BETALACTAM ANTIBIOTICS GLYCOPEPTIDES AMINOGLYCOSID aminosides TETRACYCLINES Assoc Prof

• BETA-LACTAM ANTIBIOTICS • GLYCOPEPTIDES • AMINOGLYCOSID (aminosides) • TETRACYCLINES Assoc. Prof. I. Lambev (www. medpharmsofia. eu)

Antiinfective agents are among the most dr examples of the advances of modern medicin Many infectious diseases once considered inc and lethal now can be treated. The remarkably and specific activity of antimicrobial drugs is due selective toxicity for targets that are either uniqu to microorganisms or much more important in the than in animals or humans Among these target bacterial and fungal cell wall-synthesizing enzyme bacterial ribosome, the enzymes required for nuc synthesis and DNA replication, the mechanism of replication, etc. The much older and less select cytotoxic drugs are the antiseptics and disinfe

Antiinfective agents may be classified according to their antimicrobial activity: 1. Antibacterial drugs (antibiotics and synthetic drugs) 2. Antiviral drugs 3. Antifungal drugs 4. Antiprotozoal drugs 5. Anthelmintic drugs 6. Insecticides for ectoparasites 7. Antiseptics and Disenfectant (Not are drug 8. Prepartaions for Disinsection (Not are dru 9. Prepartaions for Deratisation (Not are dru 10. Vaccines, Serums, and Immunoglobulins

Antibacterial antibot • BETA-LACTAMs • Amphenicols GLYCOPEPTIDES • Macrolides • AMINOGLYCOSIDES • Lincosamides (aminosides) • Polymyxins • TETRACYCLINES • Streptogramins

Synthetic antibacterial dru • Oxazolidinones (e. g. Linezolide) • Fluoroquinilones and other quinolo • Metronidazole • Sulfonamides/Trimethoprime • Nitrofurans • Oxiquinolones etc.
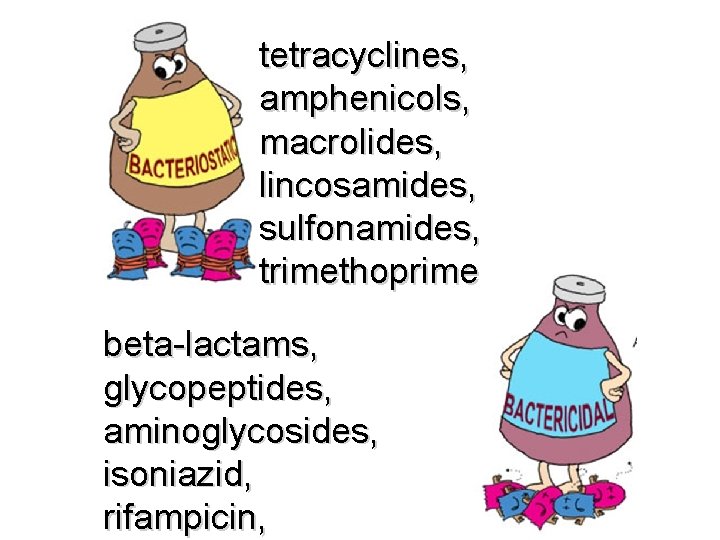
tetracyclines, amphenicols, macrolides, lincosamides, sulfonamides, trimethoprime beta-lactams, glycopeptides, aminoglycosides, isoniazid, rifampicin,

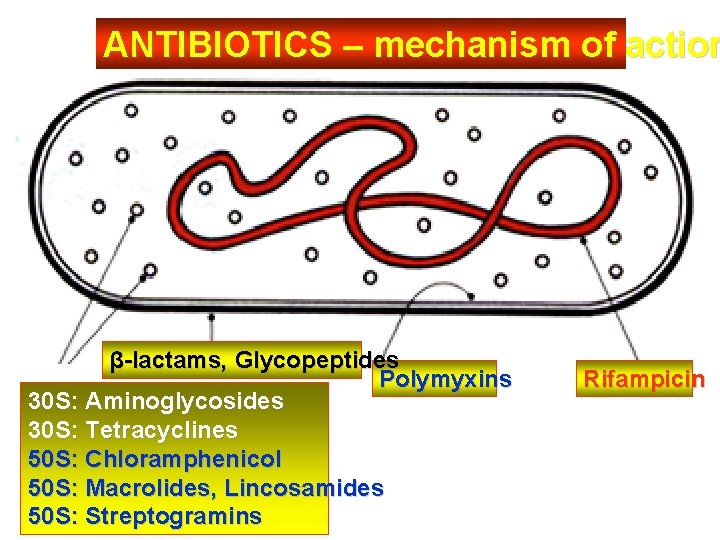
ANTIBIOTICS – mechanism of action β-lactams, Glycopeptides Polymyxins 30 S: Aminoglycosides 30 S: Tetracyclines 50 S: Chloramphenicol 50 S: Macrolides, Lincosamides 50 S: Streptogramins Rifampicin

Adverse Drug Reactions (ADRs) Antibacterial agents may cause: ●direct host toxicity (aminoglycosides) ●toxic interactions with other drugs ●interference with protective effects of norm microflora (by suppressing obligate anaero e. g selection or promotion of drug resistanc ●tissue lesions at injection sites (tetracycline ●impairment of host immune system (chloramphenicol)

●reduced phagocytosis (tetracyclines) ●inhibition of phagocytosis (aminoglycosi ●hypersensitivity reactions (penicillins, amin sulfonamides) ●hepatic microsomal enzyme induction (rifam or inhibition (chloramphenicol, metronidazo that interferes with their own metabolism as well as that of concurrent medications ●residues in animal products for human consumption (all antibacterials). NB: withdrawal periods…

Because of the potential for some antibacterials to reduce protein production, incl. antibodies (e. g. aminoglycosides, amphenicols, lincosamides, macrol tetracyclines), concurrent antibacte medications need to be selected ca when immunizing animals, espec with killed vaccines.

Selection or promotion of resista Antibacterial agents do not cause bacte become resistant but their use preferent selects resistant populations of bacteria Some genes that code for resistance have identified in bacterial cultures. The most clin important for resistance are plasmids. They genes that may benefit survival of the organism (e. g. antibacterial resistance) transmitted from one bacterium to another.

Plasmids are cytoplasmic genetic elements which transfer drug resistance to previously susceptible bacteria Acquired resistance is not a problem in all ba For example, Gram-positive bacteria (with some exceptions, incl. Staphylococcus spp) often unable to acquire resistance plasmids (and thus acquire resistance through mutatio a slower process), whereas resistance is an increasing problem in many Gram-negativ pathogens such as the Enterobacteriaceae.

Enterobacteriaceae: • E. coli, Salmonella, Schige • Yersinia pestis (plugue!) • Klebsiella • Enterobacter • Serratia • Citrobacter

The intestine is a major site of transfer of antibacterial resistance. This is important wh antibacterial agents are used in animals in contact with fecal material, an enormous reservoir of intestinal bacteria. Nosocomial infections In veterinary hospitals, nosocomial infection (infection acquired during hospitalization) by resistant bacteria is an emerging problem. Bac most frequently implicated in veterinary hospit Klebsiella, Escherichia, Proteus and Pseudomonas spp.

Factors predisposing to nosocomial infections age extremes (young or old), severity of diseas duration of hospitalization, use of invasive supp systems, surgical implants, defective immune responses and prior antibacterial drug use. The drugs with greatest potential to suppress endogenous flora are those most active agains obligate anaerobic bacteria (amphenicols, lincosamides, beta-lactams) and those undergoing extensive enterohepatic recycling (chloramphenicol, lincosamides, tetracyclines). Cephalosporins are a major risk factor in huma

Hypersensitivity reactions to antibacterial age reported less frequently in VM than in human patients, where they constitute 6– 10% drug reactions. To induce an allergic response molecules must be able to form covalent bon macromolecules such as proteins. Bonding w protein carrier enables reaction with T lympho and macrophages. The reactive moiety is usu drug metabolite, e. g. the penicilloyl moiety of penicillins.

●Hypersensitivity reactions depend on the combination of antigen and antibody and are not dose related. ●Hypersensitivity reactions have been report most frequently in animals with cephalospor penicillins and sulfonamides. ●Doberman pinschers have an increased risk of sulfonamide hypersensitivity, possibly due to delayed sulfonamide metabolism.

●The probability of an anaphylactoid reaction direct histamine release that is not immunolo mediated) is increased with penicillin prepara containing methylcellulose as a stabilizer. Drug hypersensitivity manifest in differen ●Acute anaphylaxis is associated with Ig. E-tri mast cell degranulation and characterized by or more of the following signs: hypotension, bronchospasm, angioedema, urticaria, erythe pruritus, pharyngeal and/or laryngeal edema, vomiting and colic.

BETA-LACTAM ANTIBIOTICS (inhibitors of cell wall synthesis) Their structure contains a beta-lactam ring. The major subdivisions are: (a) penicillins whose official names usually include or end in “cillin” (b) cephalosporins which are recognized by the inclusion of “cef” or “ceph” in their official names. (c) carbapenems (e. g. meropenem, imipenem) (d) monobactams (e. g. aztreonam) (e) beta-lactamase inhibitors (e. g. clavulanic acid, sulbactam).

A. FLEMING (1881– 1955) • Penicillin G - P. notatum I. PENICILLINS (1929)
The fungus Penicillium chrysogenum

The cell wall completely surrounds the cyto membrane, maintains cell shape and integri prevents cell lysis from high osmotic pressu cell wall is composed of a complex cross-lin polymer of polysaccharide and peptide chain so called peptidoglycan (murein). The polysaccharide contains alternating amino s N-acetylglucosamine, and N-acetylmuramic A five-amino-acid peptide is linked to the N-acetylmuramic acid sugar. This peptide terminates in D-alanyl-D-alanine.

Penicillin-binding protein (PBP, an enzyme removes the terminal alanine in the proces forming a cross-link with a nearby peptide. Cross-links give the cell wall its structural r Beta-lactam antibiotics covalently bind the active site of PBPs. This inhibits the transpeptidation reaction, halting peptidoglycan synthesis, and the cell d Beta-lactams kill bacterial cells only when they are actively growing and synthesizing cell wall.


NARROW SPECTRUM PENICILLINS • Biosynthetic (natural) penicillins • Antistaphylococcal penicillins BROAD SPECTRUM PENICILLINS • Aminopenicillins • Antipseudomonal penicillins - Carboxypenicillins - Ureidopenicillins

1. NARROW SPECTRUM PENICILLINS a) Biosynthetic (natural) penicillins Benzylpenicillin (Penicillin G® Na or K) – Phenoxymethylpenicillin (Penicillin-VK®) – Benzathine benzylpenicillin (effect 2 to 4 b) Antistaphylococcal penicillins Isoxazolyl penicillins - Cloxacillin, Dicloxacillin - Flucloxacillin, Oxacillin Others: Methicillin, Nafcillin (crosses BB

Antibacterial spectrum of narrow-spectru biosynthetic penicillins: ●Narrow-spectrum penicillins are active aga Gram-positive aerobes and obligate anaer ●They are ineffective against most Gram-ne aerobes and Penicillase-producing Staphylococcus. Antibacterial spectrum of antistaphylococcal penicillins: ● Staphylococcus spp (without MRSA) MRSA

Clinical applications Narrow-spectrum biosynthetic penicillins: are still the drugs of choice in small animals i clostridial diseases, listeriosis, actinomyco anaerobic infections (abscess, fight wound pyothorax) and β-hemolytic streptococcal infections. Antistaphylococcal penicillins: ●Staphylococcal skin infections in dogs ●Surgical prophylaxis, especially for orthoped procedures ●Treatment of osteomyelitis, discospondylitis

Penicilline G Sodium®: 20 000 – 40 000 /IU/kg/BW q. 6– 8 h i. v. , i. m. , s. c. Penicillin-VK® (Potassium): 10 mg/kg/BW q. 8 h p. o.

Cloxacillin, Dicloxacillin, Flucloxacillin: 10 – 40 mg/kg q. 8 h p. o. 500 mg Flucloxacillin

2. BROAD-SPECTRUM PENICILLINS a) Aminopenicillins The aminopenicillins have identical spectrum and activity, but amoxicillin is better absorbed orally (70– 90%). They are effective against streptococci, enterococci, and some Gram-negative organisms (incl. H. pylori) but have variable activity against staphylococci and are ineffective against P. aeruginosa. Amoxicillin and Ampicillin


J. Robin Warren (2005) Barry J. Marshall (2005)

Clinical applications of aminopenicil ●Soft tissue non-staphylococcal infections in dogs and cats. ●Cat abscesses. ●Uncomplicated urinary tract infections, bu amoxicillin-clavulanate might be a better ●Some enteric infections. ●Amoxicillin in combination with metronida and omeprazole has been used for treatm of Helicobacter gastritis.
Cat abscesses Amoxicillin: 10 – 20 mg/kg/BW q. 8– 12 h i. v. , i. m. , s. c. p. o.


AMOXICILLIN

b) Antipseudomonal penicillins These drugs retain activity against streptococci and possess additional effects against Gram-negative organisms, including various Enterobacteriaceae (E. coli, Salmonella, Schigella, Proteus) and Pseudomonas. • Carboxypenicillins - Carbenicillin (out…) - Ticarcillin • Ureidopenicillins - Azlocillin - Mezlocillin - Piperacillin

Clinical applications in VM ●For topical treatment of otitis externa due aeruginosa resistant to other drugs. ●For systemic treatment infections by Pseudomonas spp, usually in combi with an aminosides to delay the emergen of resistance. ●When combined with clavulanate, ticarcill effective against many β-lactamase prod strains of otherwise resistant Gram-nega bacteria and Staphylococcus.

Known drug interactions ●Penicillins are often said to be synergistic aminoglycosides against many Gram-posi microorganisms, incl. Staphylococcus aure ●Narrow-spectrum penicillins such as penic are synergistic with drugs that bind β-lacta enzymes, including cloxacillin, clavulanate some cephalosporins.

Antibacterial drugs have been classified broadly into: 1. Bacteriostatic, i. e. those that act prim pri by arresting bacterial multiplication, suc tetracyclines, amphenicols, macrolides, lincosamides, sulfonamides, trimetrhop 2. Bactericidal, i. e. those which act prim by killing bacteria, such as beta-lactams glycopeptides, aminoglycosides, isoniaz rifampicin, fluoroquinolones, metronidaz

Adverse effects The main hazard with the penicillins is allergic rea These include itching, rashes (eczematous or urti fever, and angioedema. Rarely (about 1 in 10 000 is anaphylactic shock which can be fatal (about 1 100 000 treatment courses). Allergies are least likely when penicillins are given orally and m likely with local application. Metabolic opening of β-lactam ring creates a highly reactive penicilloyl which polymerizes and binds with tissue proteins the major antigenic determinant. The anaphylactic reaction involves specific Ig. E antibodies which ca detected in the plasma of susceptible patients.


There is cross-allergy between all the vario forms of penicillin, probably due in part to the common structure, and in part to the degrada products common to them all. Partial cross-allergy exists between penicil and cephalosporins (a maximum of 10%) wh is of particular concern when the reaction to group of antimicrobials has been angioedem anaphylactic shock. Carbapenems and the monobactams have a much lower risk of cross-reactivity.

When the history of allergy is not clear and i necessary to prescribe a penicillin, the presence of Ig. E antibodies in serum is a useful indicator of reactions mediated these antibodies, i. e. immediate (type 1) rea Additionally, an intradermal test for allergy be performed; appearance of wheal reaction indicates a positive response. Only about 10% of patients with a his of “penicillin allergy” respond positiv

Other (nonallergic) ADRs include diarrhoea du alteration in normal intestinal flora which may pro Clostridium difficile-associated diarrhoea. Neutro is a risk if penicillins or other β-lactam antibiotics used in high dose and usually for a period of long 10 days. Rarely penicillins cause anaemia, some hemolytic, and thrombocytopenia or interstitia nephritis. Penicillins are presented as their sodi or potassium salts. Extremely high plasma penic concentrations cause convulsions. Co-amoxicla flucloxacillin, or oxacillin given in high doses for prolonged periods in the elderly may cause hepatic toxicity.

Antibacterial drugs have been classified broadly into: 1. Bacteriostatic, i. e. those that act prim pri by arresting bacterial multiplication, suc tetracyclines, amphenicols, macrolides, lincosamides, sulfonamides, trimetrhop 2. Bactericidal, i. e. those which act prim by killing bacteria, such as beta-lactams glycopeptides, aminoglycosides, isoniaz rifampicin, fluoroquinolones, metronidaz

Adverse effects The main hazard with the penicillins is allergic rea These include itching, rashes (eczematous or urti fever, and angioedema. Rarely (about 1 in 10 000 is anaphylactic shock which can be fatal (about 1 100 000 treatment courses). Allergies are least likely when penicillins are given orally and m likely with local application. Metabolic opening of β-lactam ring creates a highly reactive penicilloyl which polymerizes and binds with tissue proteins the major antigenic determinant. The anaphylactic reaction involves specific Ig. E antibodies which ca detected in the plasma of susceptible patients.

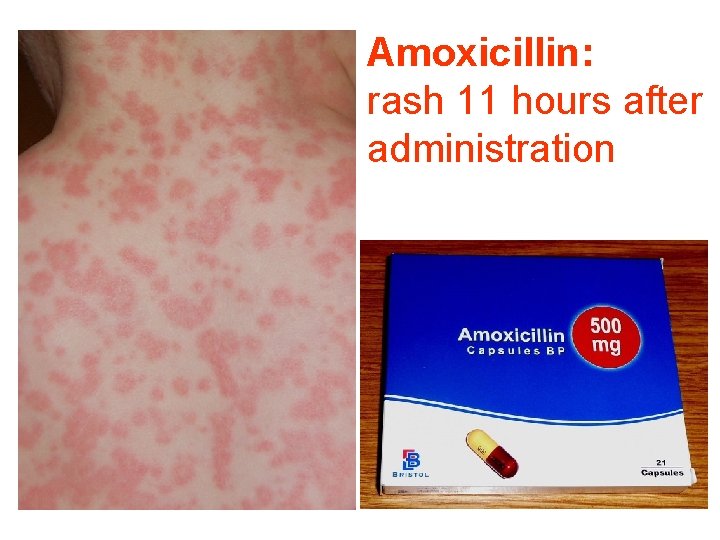
Amoxicillin: rash 11 hours after administration

There is cross-allergy between all the vario forms of penicillin, probably due in part to the common structure, and in part to the degrada products common to them all. Partial cross-allergy exists between penicil and cephalosporins (a maximum of 10%) wh is of particular concern when the reaction to group of antimicrobials has been angioedem anaphylactic shock. Carbapenems and the monobactams have a much lower risk of cross-reactivity.

When the history of allergy is not clear and i necessary to prescribe a penicillin, the presence of of Ig. E antibodies in seru is a useful indicator of reactions mediated these antibodies, i. e. immediate (type 1) rea Additionally, an intradermal test for allergy be performed; appearance of wheal reaction indicates a positive response. Only about 10% of patients with a his of “penicillin allergy” respond positiv

Other (nonallergic) ADRs include diarrhoea du alteration in normal intestinal flora which may pro Clostridium difficile-associated diarrhoea. Neutro is a risk if penicillins or other β-lactam antibiotics used in high dose and usually for a period of long 10 days. Rarely penicillins cause anaemia, some hemolytic, and thrombocytopenia or interstitia nephritis. Penicillins are presented as their sodi or potassium salts. Extremely high plasma penic concentrations cause convulsions. Co-amoxicla flucloxacillin, or oxacillin given in high doses for prolonged periods in the elderly may cause hepatic toxicity.

II. CEPHALOSPORINS The nucleus of the cephalosporins, 7 -aminoce sporanic acid, bears a close resemblance to 6 penicillanic acid. The intrinsic antimicrobial ac of natural cephalosporins is low, but the attach of various R 1 and R 2 groups has yielded hun of potent compounds of low toxicity. Cephalos can be classified into four major generations, depending mainly on their antibacterial sp and some pharmacokinetic properties.
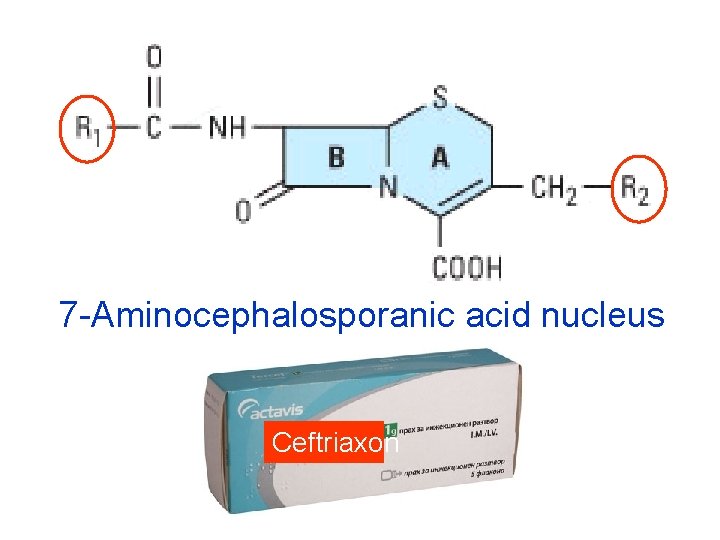
7 -Aminocephalosporanic acid nucleus Ceftriaxon
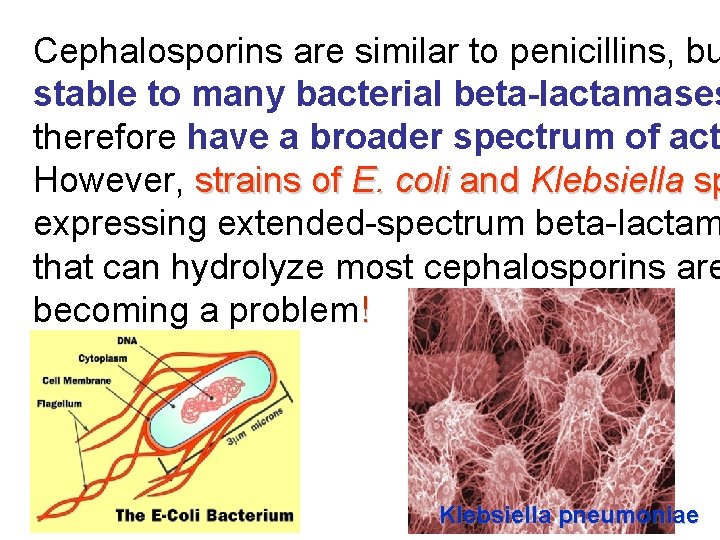
Cephalosporins are similar to penicillins, bu stable to many bacterial beta-lactamases therefore have a broader spectrum of act However, strains of E. coli and Klebsiella sp expressing extended-spectrum beta-lactam that can hydrolyze most cephalosporins are becoming a problem! Klebsiella pneumoniae

1. First-generation cephalosporins ●cefadroxil, cefalonium, cefazolin, ●cefalotin, cefapirin, cefradine These drugs are very active against Gram-po cocci (pneumococci, streptococci, and Staphylococci). Cephalosporins are not ac against MRSA. E. coli, K. pneumoniae, an P. mirabilis are often sensitive. Anaerobic are usually sensitive except Bacteroides frag They do not cross BBB.

Clinical applications First-generation ●Osteomyelitis ●Skin infections caused by Staphylococcus (but not MRSA) ●Soft tissue infections due to susceptible orga ●Urinary tract infections (but not prostatis) ●Discospondylitis ●Bacterial conjunctivitis (cefalonium)

Cefalonium (Cepravin™): 250 mg Carton – 8 cows: 32 syringes) • Long-acting cephalosporin • Cure existing infections at dry off • Protect against mastitis and reduce new infections at calving

4 nipples In USA there are 9. 5 000

Cefalonium (Cepravin™): 250 mg in spray syringes (jeringas – spanish): intrammary Indications: In conjunction with teat spraying and proper managem cow during the drying off period, the careful administra Cepravin Dry Cow at drying off reduces new infection dry period and treats subclinical mastitis. Dosage 1 syringe per quarter (3 months) immediately after fina Withholding Period Milk: Treatment to be at least 49 days before calving. Milk from the first 8 milkings after calving must be disc Meat: 30 days

2. Second-generation cephalosporin • cefaclor, cefalexin, cefamandole, • cefuroxime, cefotetan, cefoxitin They are active against organisms inhibited by firs ration drugs, but in addition they have extended G negative coverage. Klebsiellae (incl. those resista cefalotin) are usually sensitive. Cefamandole, cefuroxime, and cefaclor are active against H. infl but not against serratia or B. fragilis. In contrast, c and cefotetan are active against B. fragilis and so serratia strains but are less active against H. influ

Cefalexin p. o. • Cats: 22 – 50 mg/kg q. 8– 12 h • Dogs: 20 – 40 mg/kg q. 8– 12 h

Clinical applications Second-generation ●Orally active cephalosporins in dogs and ●In veterinary institutions the human-appro formulation cefuroxime is used for sur prophylaxis for orthopedic surgery.

Cefuroxime Zinacef™: 20– 50 mg/kg/BW q. 8– 12 h i. v. , i. m. , s. c.
Cefoxitin 10– 30 mg/kg q. 6– 8 h i. v. , i. m. , s. c.

3. Third-generation cephalosporins • cefoperazone, cefpodoxime, cefotaxim • cefovecin, ceftriaxone Compared with second-generation agents drugs have extanded Gram-negative cove and some are able to cross the BBB. Thi generation drugs are active against Citrob Serratia marcescens, and Providencia. Th also effective against β-lactamase-prod strains of Haemophilus and Neisseria.

Clinical applications ●Third-generation cephalosporins should reserved in small animal practice for ser infections caused by Gram-negative aerob and facultatively anaerobic bacteria, espe Enterobactericaceae. ●They may also be indicated for the treatm of urinary tract infections.

Ceftriaxone 15 – 50 mg/kg q. 12– 24 h i. v.

Cefpodoxime 5 – 10 mg/kg q. 12– 24 h

●Ceftriaxone and cefotaxime are approved for the treatment of meningitis, including meningitis caused by pneumococci, meningococci, H. influenzae, and susceptible enteric Neisseria meningitidis ●Ceftazidime and cefoperazone are the only two drugs with useful activity against P. aeruginos

●Cefovecin is registered in some markets for use in canine skin and soft tissue infectio associated with Staph. intermedius, β-hemolyt streptococci, Escherichia and Pasteurella mult canine urinary tract infections associated with Escherichia and Proteus spp; feline skin and s tissue infections associated with Pasteurella m cida, Fusobacterium spp, Bacteroides spp, Pre oralis, β-hemolytic streptococci and Staphylococcus intermedius; and feline urinary tract infections associated with Escherichia.

4. Fourth-generation cephalospo • cefepime, cefpirome ●Are used in human medicine for treatme nosocomial or community-acquired lowe respiratory tract infections, bacterial men and urinary tract infections.
III. CARBAPENEMS • Doripenem • Ertapenem • Meropenem • Tienam (imipenem/cilastatin)

Imipenem has a wide spectrum with goo activity against many Gram-negative rods including P. aeruginosa, Gram-positive organisms, and anaerobes. It is resistant to most β-lactamases. Imipenem is inactivated by dehydropeptid in renal tubules, resulting in low urinary concentrations. It is administered togethe with an inhibitor of renal dehydropepti (Cilastatin) for clinical use.

● The most common ADRs of carbapenem are nausea, vomiting, diarrhea, skin rashe and reactions at the infusion sites. Excess levels of imipenem in patients with renal failure may lead to seizures. ● Meropenem and ertapenem are less lik cause seizures than imipenem. Patients a to penicillins may be allergic to carbapene

Clinical applications of carabapenems in VM ●For serious and multiresistant bacterial infect Known drug interactions ●Additive or synergistic antibacterial effects ma against some bacteria when imipenem is used aminoglycoside. ●Antagonism of antibacterial effects may occur with other β-lactams. ●Synergy may occur against Nocardia when us combination with Co-Trimoxazole. ●Chloramphenicol may antagonize the antibac efficacy of imipenem.

IV. MONOBACTAMS • Aztreonam Monobactams are drugs with a monocyclic βring. They are relatively resistant to beta-lacta and active against Gram-negative rods (incl Pseudomonas and Serratia). They have no against Gram-positive bacteria or anaerobes. Aztreonam is given i. v. Penicillin-allergic patients tolerate aztreonam.
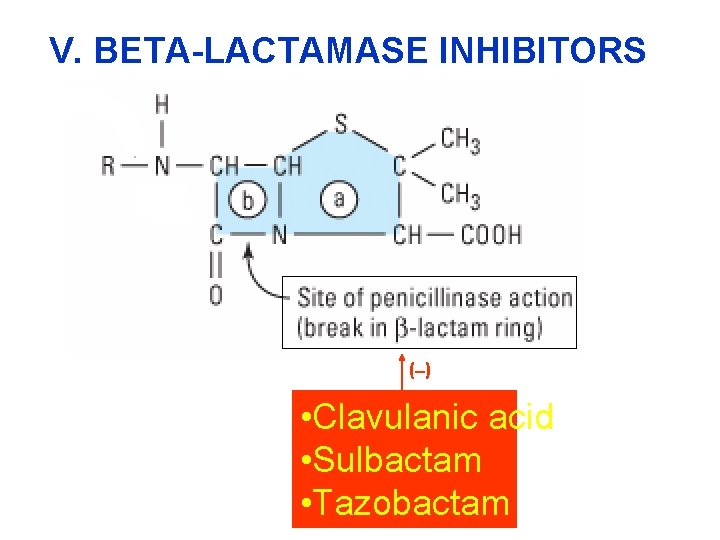
V. BETA-LACTAMASE INHIBITORS ( ) • Clavulanic acid • Sulbactam • Tazobactam

Ampicillin, amoxicillin, ticarcillin, and piperacillin are also available in combinat with one of several beta-lactamase inhibit clavulanic acid, sulbactam, or tazobactam The addition of a beta-lactamase inhibitor extends the activity of these penicillins to beta-lactamase-producing strains of S. a (without MRSA), E. coli, K. pneumoniae, P. aeruginosa, Proteus, H. influenzae).

• CO-AMOXICLAV (amoxicillin + clavulanic acid) Augmentin • SULTAMICILLIN (ampicillin + sulbactam) • PIPERACILLIN + TAZOBACTA Tazocin • CEFOPERAZONE + SULBACT Sulperazon

●Amoxicillin-clavulanate has many application small animal practice because of its broad spe and excellent activity against Staphylococcus. often the drug of first choice for infections in sk tissue and urinary tract and for surgical prophy ●A combination of ampicillin and sulbactam (a β-lactamase inhibitor) is available in some cou and has similar uses. ●The indication for ticarcillin-clavulanate is usu for systemic treatment of susceptible P. aerugi infections resistant to other antibacterials.

Co-Amoxiclave (BAN): Amoxicillin & Clavulanate • Augmentin® • Clavulox® Antibacterial spectru for amoxicillinclavulanate * MRSA

Amoxicillin & Clavulanate (Augmentin®, Clavulox®) 12. 5– 25 mg/kg q. 8– 12 h p. o. , i. m. , s. c.
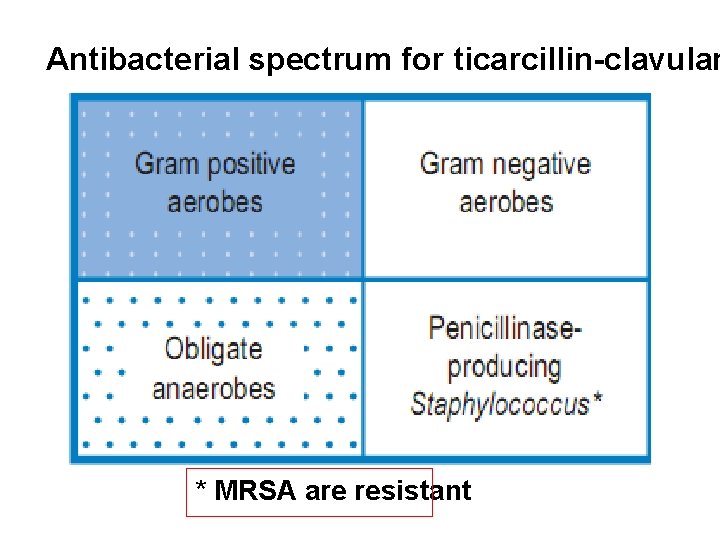
Antibacterial spectrum for ticarcillin-clavulan * MRSA are resistant


GLYCOPEPTIDES Glycopeptides inhibit synthesis of cell wall peptidoglycan and inhibit bacterial cell mem permeability: Teicoplanin, Vancomycin, Aviparcin and Bacitracin has activity against Gram-positiv organisms but is markedly nephrotoxic. It i restricted to topical and ophthalmic use in combination with polymyxin and/or neomyc (e. g. Bivacin®, Topocin®, etc. ).


●The most common indication of Vancomyci would be MRSA infections or multidrug-resis Enterococcus. ●Teicoplanin is administered IM but can also b given by rapid IV injection. ●Vancomycin and Teicoplanin are not abso orally. They are drug of choice for the oral tre of bowel inflammations occurring as a complic antibiotic therapy (pseudomembranous entero caused by Clostridium difficile) in human.

AMINOGLYCOSIDES Aminoglycosides have a hexose ring, either streptidine (in streptomycin) or 2 -deoxystrep (in other aminoglycosides), to which various sugars are attached by glycosidic linkages. They are water-soluble, stable in solution more active at alkaline than at acid p. H. Aminoglycosides have polar groups in th molecules and do not absorb in GIT.
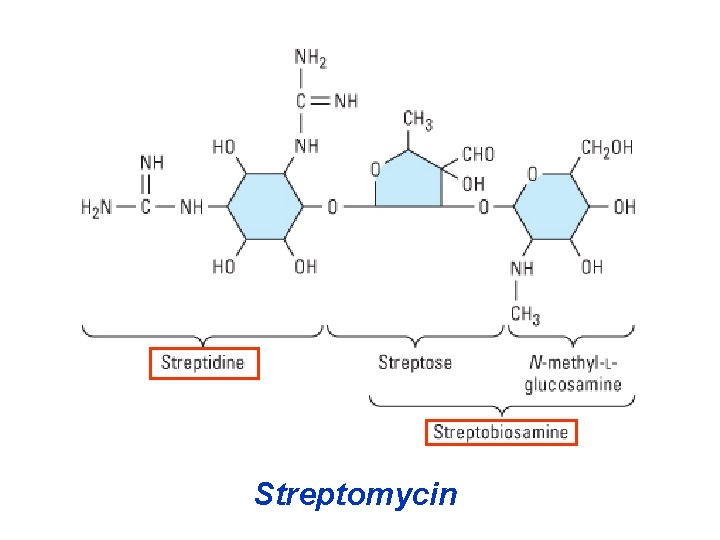
Streptomycin

Streptomycin. Its antibacterial activit is due to its binding to the 30 S subunit of bacterial ribosome and inhibiting of prote synthesis. It has a wide spectrum of antibacterial activity but is primarily used treat mycobacterial infections (i. m. ). • The main problems are eighth nerve toxicity (vestibulotoxicity more than deafness), nephrotoxicity, allergic react
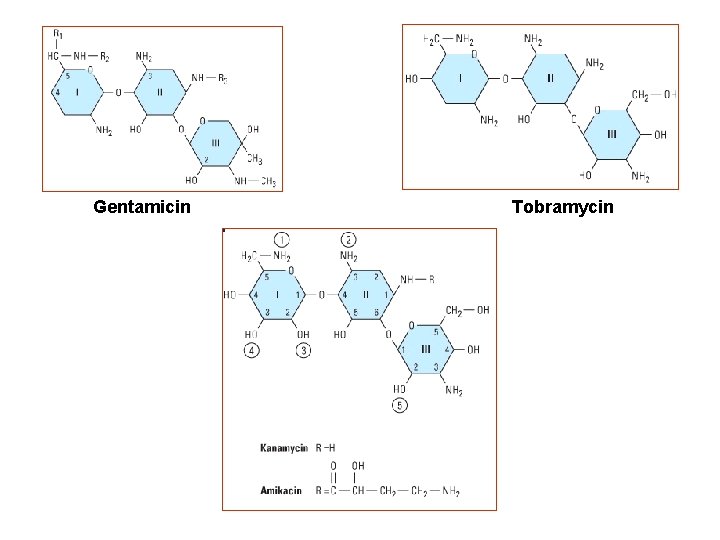
Gentamicin Tobramycin

Mechanisms of action Inside the cell, aminoglycosides bind to spe 30 S-subunit ribosomal proteins and inhibit protein synthesis in at least three ways: (1) interference with the initiation complex of peptide formation; (2) misreading of m. RNA, which causes incorp of incorrect amino acids into the peptide, re in a nonfunctional or toxic protein; (3) breakup of polysomes into nonfunctional monosomes.


Aminoglycosides act bactericidal on dividing and non-dividing extracelular microorganisms. They are in general active against staphylococci and aerobic Gram-negative organisms including P. aeruginosa and almost all the Enterobacteriac

Aminoglycosides are mostly used against G negative enteric bacteria almost always used combination with a β-lactams to extend cover to include potential Gram-positive pathogens to take advantage of the synergism between these two classes of drugs. Penicillin-aminoglycoside combinations also a used to achieve bactericidal activity in the trea of enterococcal endocarditis and to shorten d of therapy for viridans streptococcal and staphylococcal endocarditis.
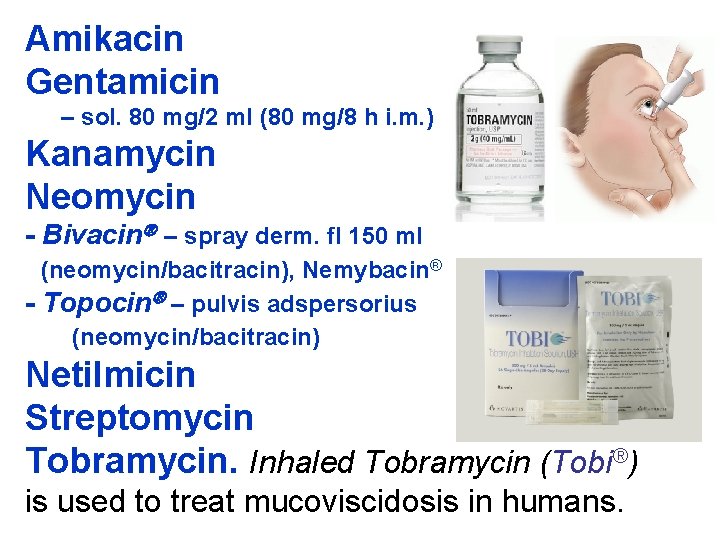
Amikacin Gentamicin – sol. 80 mg/2 ml (80 mg/8 h i. m. ) Kanamycin Neomycin - Bivacin – spray derm. fl 150 ml (neomycin/bacitracin), Nemybacin® - Topocin – pulvis adspersorius (neomycin/bacitracin) Netilmicin Streptomycin Tobramycin. Inhaled Tobramycin (Tobi®) is used to treat mucoviscidosis in humans.

Gentamicin (Spelt with an “i”) ●Probably now the most commonly used amin for severe infections caused by Gram (–) aerob bacteria in dogs with oft-treated ear infection Tobramycin: More active against Pseudomonas than gen Amikacin is particularly important in treating serious Pseudomonas and other Gra infections in immunosuppressed patients. I administered for 2– 3 weeks at recommended d with less risk of nephrotoxicity than with gen

Gentamicin: 6 mg/kg q. 24 h i. m. , i. v. , s. c. Tobramycin: 1– 2 mg/kg q. 8 h i. m. , i. v. , s. c.

ADRs: Ototoxicity and nephrotoxicity are more likely be encountered when therapy is continued for than 5 days, at higher doses, in the elderly, an in the setting of renal insufficiency. Concurren use with loop diuretics (e. g. furosemide, ethac acid) or other nephrotoxic antimicrobial agents (vancomycin, amphotericin) can potentiate nep toxicity. Ototoxicity can manifest as auditory damage, resulting in tinnitus and high-frequen hearing loss initially, or as vestibular damage evident by vertigo, ataxia, and loss of balance

• Streptomycin and gentamicin are the most vestibulotoxic agents. • Neomycin, kanamycin, and amikacin are the most cochlear toxic agents. • Neomycin, tobramycin, and gentamicin are the most nephrotoxic agents. • In very high doses, aminoglycosides can produ a curare-like effect with neuromuscular blockade that results in respiratory paralysis. T paralysis is usually reversible by calcium gluco (given promptly i. v. ) or galantamine (or neosti • Hypersensitivity occurs infrequently.

Mechanisms of resistance ●mutation of the organisms, resulting in alte ribosomes that no longer bind the drug ●reduced permeability of the bacteria to the ●inactivation of the drug by bacterial enzym Pharmacokinetics ●Aminoglycosides are not significantly abso from the gut, so must be given parenterall treat systemic infections. ●All have poor tissue penetration (including and eye) as they are highly hydrophilic.

●They are eliminated almost exclusively by glomerular filtration. ●Half-lives are short in plasma (40– 60 min much longer (>30 h) for tissue-bound drug ●Aminosides have a prolonged postantibio effect. Once-daily dosing is now recommended to reduce toxicity. ●The bactericidal action of aminosides is enh in an alkaline medium and may be reduced by acidity secondary to tissue damage. ●All aminoside bind to and are inactivated by


Spectinomycin is structur related to aminoglycosides ●Has limited clinical application because resistance develops readily. ●Is marketed in combination with lincom which marginally enhances activity against Mycoplasma.
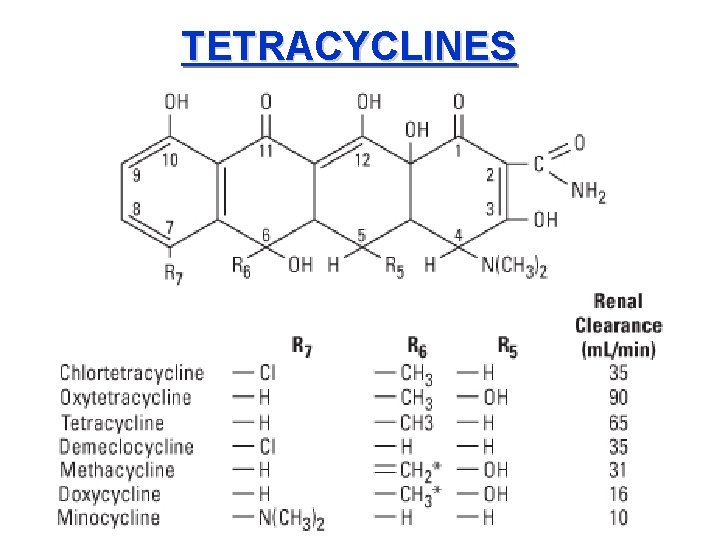
TETRACYCLINES

Tetracyclines enter microorganisms in part by diffusion and in part by an energy-dependent p of active transport. Susceptible cells concentrat drug intracellularly. Once inside the cell, tetrac bind reversibly to the 30 S subunit of the bac ribosome, blocking the binding of aminoacyl-t. R to the acceptor site on the m. RNA-ribosome com This prevents addition of amino acids to the gro peptide. Tetracyclines are broad-spectrum bacteriostatic antibiotics that inhibit protein synthesis.


●Tetracyclines have activity against many Gram (+) and Gram (–) aerobic bacteria bu acquired resistance limits their activity agai many species, such as Staphylococcus, Enterobacteriaceae (includin Enterobacter, Escherichia, Proteus and Salmonella, Shigella). ●Atypical bacterial species (Rickettsia, Bo Chlamydia and Mycoplasma) are generally susceptible, though some Mycoplasma (M. bovis) are resistant.

●In VM tetracyclines are used most frequen for atypical bacterial diseases due to Chlamyd (in cats), Borrelia, Rickettsia and Mycoplasma ●Tetracyclines are the drugs of choice for Ehrlichia canis and Rickettsia infections. ●Brucellosis is commonly treated with tetracyc in combination with rifampicin or streptomycin ●Tetracyclines have antiinflammatory prop that are independent of their antibacterial action, particularly in the case of doxycycl minocycline.
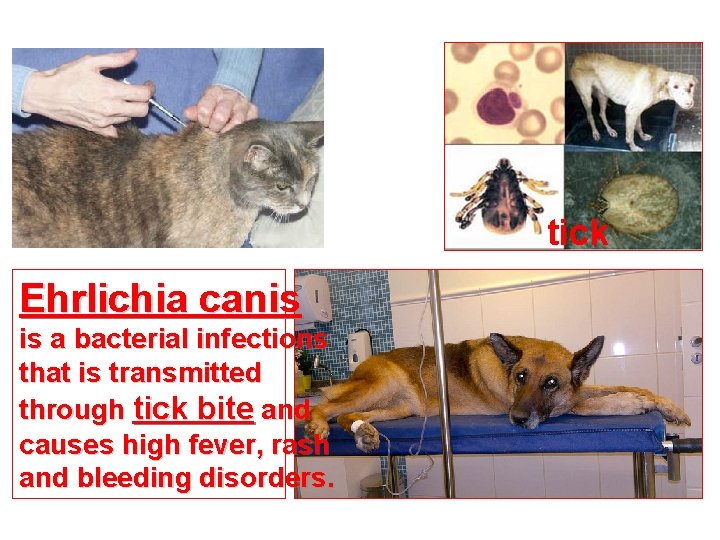
tick Ehrlichia canis is a bacterial infections that is transmitted through tick bite and causes high fever, rash and bleeding disorders.

In humans also against - Plasmodium falciparum - Yersinia pestis (plague!) Doxycycline: 5– 10 mg/kg/12 h p. o.

Minocycline: 5– 15 mg/kg/12 h p

Oxytetracycline: 20 mg/kg/8 h p

Oxyvet® 5% or 10% − Oxytetracycline injectable solution Cattle, Horse, Goat, Sheep, Dog and C Recommended dose is 5 − 10 mg/kg b Oxytetracycline has activity against most mycoplasma, spirochetes (including the Lyme disease organism Chlamydia and Rickettsia.

Tetraoleandomycin: p. o. pulvis

Sacets: 300, 150 and 1000 g. Packs: 45 and 25 kg. For prevention and treatment of actinobacil Pleuropneumonia, Dysentery (bloody diarrh ileitis and Spirochetosis of the colon etc in

Pharmacokinetics Absorption after oral administration is approxim 60– 70% for tetracycline, oxytetracycline, and methacycline; and 95– 100% for doxycycline an minocycline. A portion of an orally administered of tetracycline remains in the gut lumen, modifi intestinal flora, and is excreted in the feces. Absorption occurs mainly in the upper small int and is impaired by food and same cations (Ca 2 Fe 2+, Fe 3+ or Al 3+), by dairy products, antacids alkaline p. H.

Tetracyclines are 40– 80% bound by serum pro They are distributed widely to tissues and body except for CSF. Minocycline reaches very high concentrations in tears and saliva, which make useful for eradication of the meningococcal car state. Tetracyclines cross the placenta to reach the fetus and are also excreted in milk. As a re chelation with calcium, tetracyclines are bound damage – growing bones and teeth. Carbamaz phenytoin, barbiturates, and chronic alcohol ing may shorten the half-life of doxycycline by 50% induction of hepatic enzymes that metabolize th

Tetracyclines are excreted mainly in bile and Concentrations in bile exceed those in serum From 10 to 50% of various tetracyclines is excreted into the urine, mainly by glomerular filtration. From 10% to 40% of the drug is exc in feces. Doxycycline, in contrast to other tetracyclines, is eliminated by nonrenal mechanisms, do not accumulate significantly and require no dosage adjustment in renal fai Tetracyclines and macrolides have a good intracellular distribution.
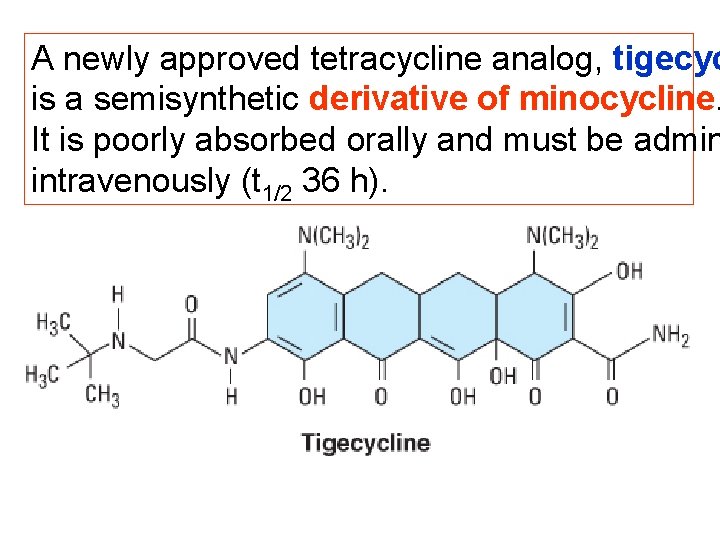
A newly approved tetracycline analog, tigecyc is a semisynthetic derivative of minocycline. It is poorly absorbed orally and must be admin intravenously (t 1/2 36 h).
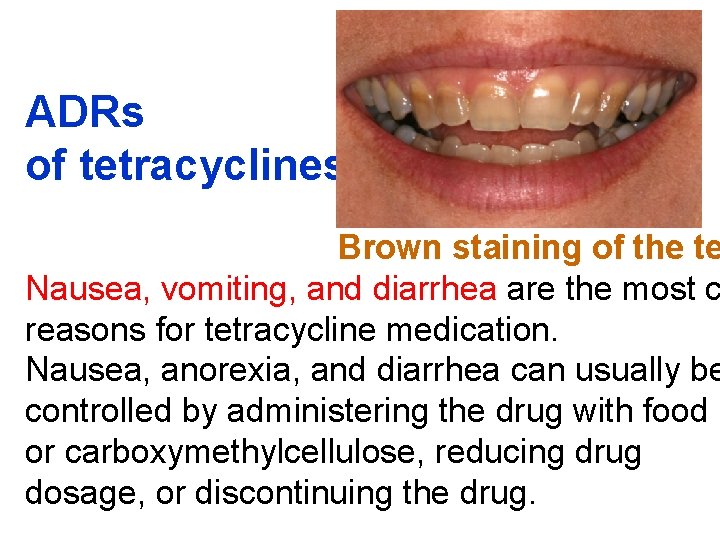
ADRs of tetracyclines Brown staining of the te Nausea, vomiting, and diarrhea are the most c reasons for tetracycline medication. Nausea, anorexia, and diarrhea can usually be controlled by administering the drug with food or carboxymethylcellulose, reducing drug dosage, or discontinuing the drug.

Tetracyclines modify the normal flora and overg of pseudomonas, proteus, staphylococci, resistan coliforms, clostridia, and candida. This can result intestinal disturbances, anal pruritus, vaginal or o candidiasis, or enterocolitis with shock and death Tetracyclines are readily bound to calcium depo in newly formed bone or teeth. When a tetracycline is given during pregnancy, it be deposited in the fetal teeth, leading to fluoresc discoloration, and enamel dysplasia; it can be de in bone, where it may cause deformity or growth inhibition.

The main mechanisms of resistan to tetracyclines and its analogs ar (1) impaired influx or increased efflux b active transport protein pump; (2) ribosome protection due to product of proteins that interfere with tetrac binding to the ribosome; (3) enzymatic inactivation.
- Slides: 126