General concept Stable lowenergy fractures Nonsurgical management Unstable


General concept ¡ ¡ Stable, low-energy fractures Nonsurgical management Unstable and high-energy fractures ORIF l l l ¡ External fixation (uniplanar and multiplanar) Plate fixation Intramedullary nailing Open tibial shaft fractures the associated bone and soft tissue loss

Trauma Mechanism ¡ Direct or indirect trauma ¡ Low-energy trauma: l l ¡ Simple falls, twisting injuries Sports injuries High-energy trauma : l motor vehicle or motorcycle crashes

Classification ¡ Fracture classification : AO/OTA fracture classification
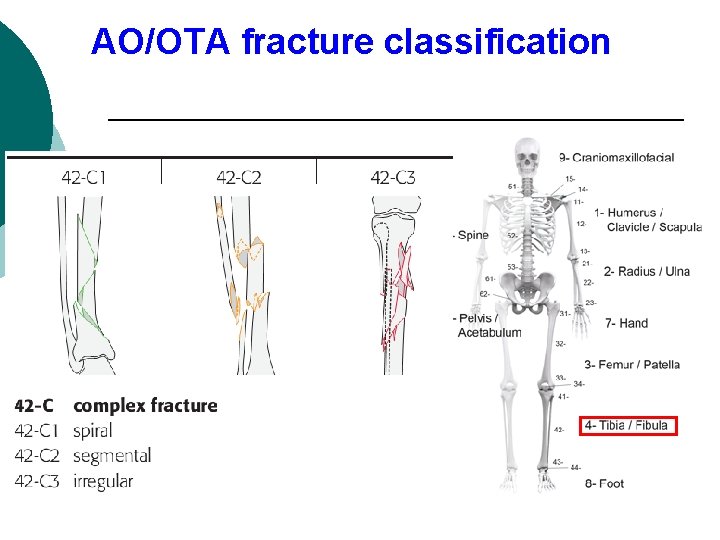
AO/OTA fracture classification

Physical examination ¡ ¡ Patient’s skin Gross deformity of the extremity Neurovascular examination : Nerve function and Pulse Identify associated injuries : ipsilateral hip, knee, and ankle Suspicion risk of compartment syndrome !!

Compartment syndrome ¡ ¡ ¡ Younger patients High-energy tibia fractures Patients with diaphyseal tibia fractures (8. 1%) 【proximal (1. 6%) and distal (1. 4%) 】 ¡ ¡ J Orthop Trauma. 2009 Aug; 23(7): 514 -8 Difficult to assess “cardinal signs – 5 P” due to fracture pain Anterior and deep posterior compartments are susceptible

Compartment syndrome ¡ Intra-compartmental pressures l ¡ ¡ Delta pressure < 30 mm Hg (diastolic pressure - tissue pressure) Should not be measured after anesthesia (diastolic pressure ↓) Four-compartment fasciotomy l Anterior compartment is most frequently incompletely released
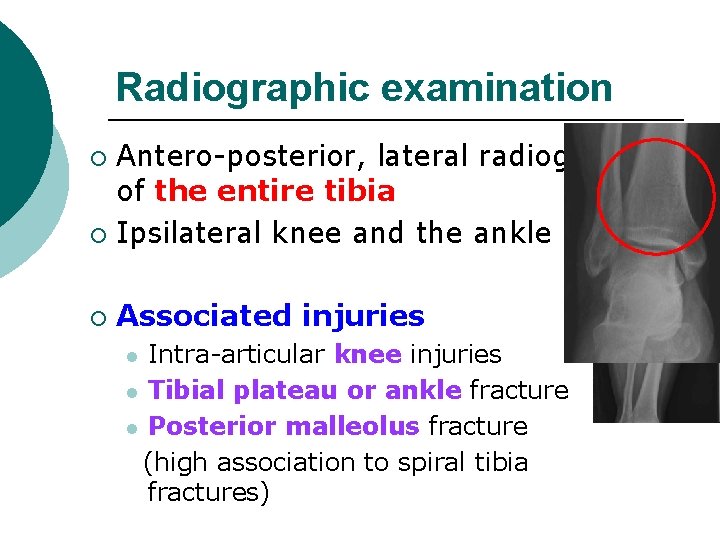
Radiographic examination Antero-posterior, lateral radiographs of the entire tibia ¡ Ipsilateral knee and the ankle ¡ ¡ Associated injuries Intra-articular knee injuries l Tibial plateau or ankle fracture l Posterior malleolus fracture (high association to spiral tibia fractures) l
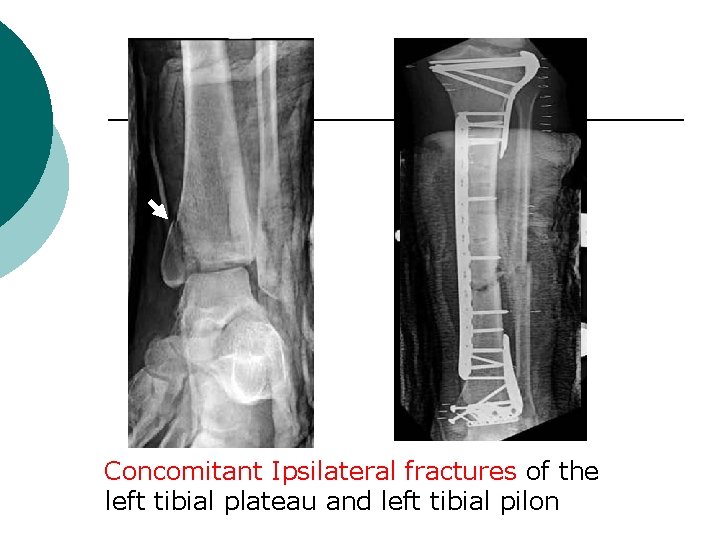
Concomitant Ipsilateral fractures of the left tibial plateau and left tibial pilon

Nonsurgical Treatment ¡ ¡ Nondisplaced, low-energy tibia fractures Initial immobilization : long leg splinting (Not casting) an ipsilateral fibula fracture is a relative contraindication Results : High union rates with angulation(<8°) and shortening(<12 mm)

Surgical indication ¡ Absolute indications l l ¡ ¡ Open fractures Concomitant vascular injuries or compartment syndrome, Irreducible or unstable fractures Failure of closed treatment Displacement : > 50% of shaft Angulation : > 5° to 10° Rotation : > 10° Shortening : > 1 cm
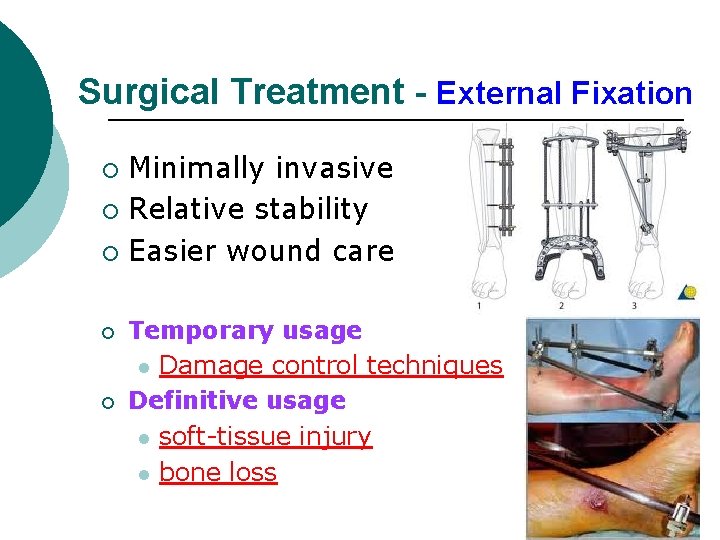
Surgical Treatment - External Fixation Minimally invasive ¡ Relative stability ¡ Easier wound care ¡ ¡ ¡ Temporary usage l Damage control techniques Definitive usage l soft-tissue injury l bone loss
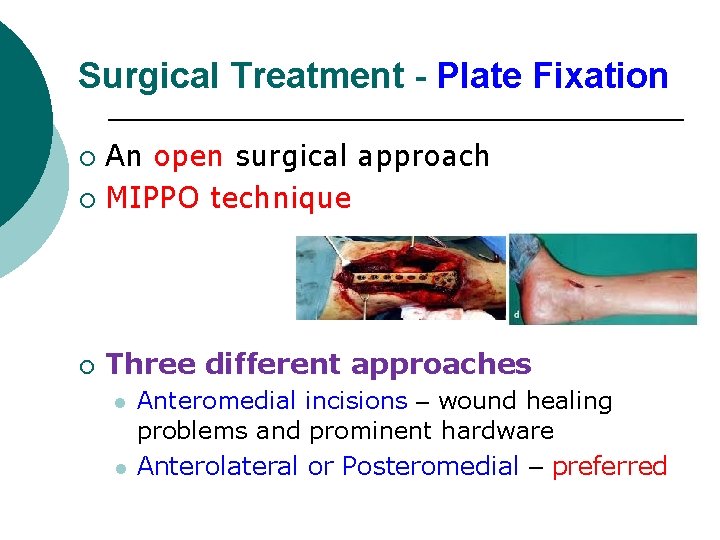
Surgical Treatment - Plate Fixation An open surgical approach ¡ MIPPO technique ¡ ¡ Three different approaches l l Anteromedial incisions – wound healing problems and prominent hardware Anterolateral or Posteromedial – preferred

Minimally invasive percutaneous plating ¡ Medial or anteromedial plating ¡ Hardware, wound breakdown, and saphenous vein and nerve injury Anterolateral percutaneous plating l injury to the superficial peroneal nerve (distal screws) l ¡ For comminuted fractures bridge plating techniques

Surgical Treatment - Plate Fixation ¡ Higher rates of complications (19% to 30%) and worse outcomes ¡ For specific indications l l l Periprosthetic fractures Open physes Too small of a medullary canal s/p cruciate ligament reconstruction Open wound provides the surgical exposure
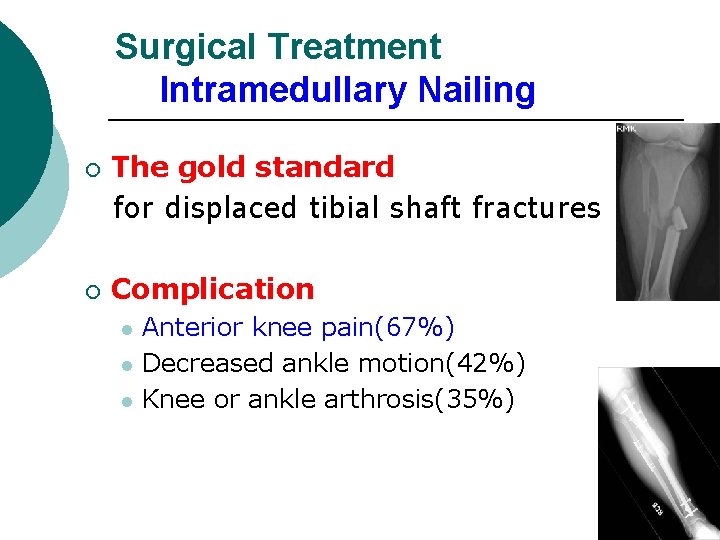
Surgical Treatment Intramedullary Nailing ¡ ¡ The gold standard for displaced tibial shaft fractures Complication l l l Anterior knee pain(67%) Decreased ankle motion(42%) Knee or ankle arthrosis(35%)
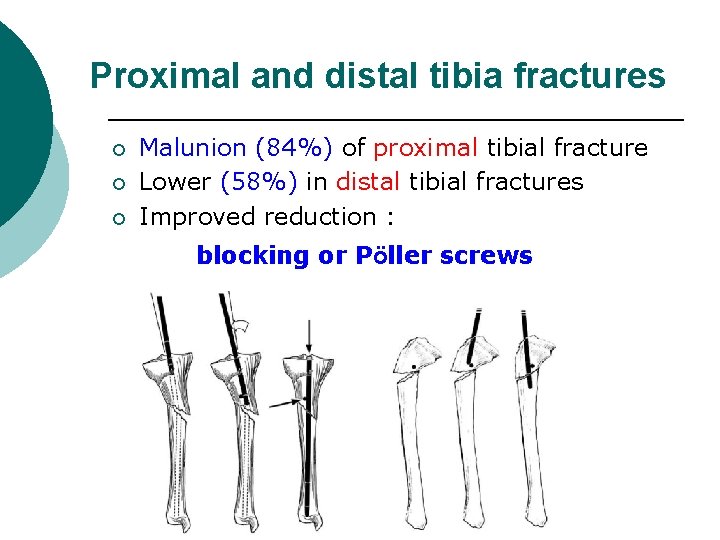
Proximal and distal tibia fractures ¡ ¡ ¡ Malunion (84%) of proximal tibial fracture Lower (58%) in distal tibial fractures Improved reduction : blocking or Pöller screws

Open Tibia Fractures ¡ Urgent management l l l Early antibiotic Wound coverage - sterile Tetanus prophylaxis Surgical débridement Fracture stabilization

Open Tibia Fractures ¡ Choice of antibiotics : Gustilo-Anderson classification l l Type 1 or 2 – gram(+) bacteria, a 1 st or 2 nd generation cephalosporin Type 3 – gram(-) bacteria, Aminoglycoside ¡ With soil contamination, Penicillin (gram(+) anaerobes)

Open Tibia Fractures ¡ ¡ ¡ Fracture stabilization l Soft-tissue healing l Prevention of infection External fixation : an excellent alternative to nailing or plating Conversion to nailing : < 2 weeks

Open Tibia Fractures ¡ Immediate nailing : up to type IIIB fractures (reamed or unreamed) Plating : a higher rate of infection ¡ Soft tissue coverage ¡ l l Split-thickness skin grafts (STSG) Flaps reconstruction – bone, nerves… Proximal : rotational gastrocnemius flap ¡ middle third : a soleus flap ¡ Distal defects : a sural flap or free flap ¡

Complication - Nonunion ¡ 定義 : Not healed at 6 months or no progressive healing for 3 consecutive months Patient factors : n. Smoking or medical comorbidities (diabetes) n. Poor nutrition n. Underlying metabolic or endocrine disorders Surgeon factors : n. Distraction of the fracture n. Excessive soft-tissue stripping n. Excessive reaming

Complication - Nonunion Surgical treatment ¡ Hypertrophic non-unions : Exchange nail ¡ Atrophic non-unions : bone graft or orthobiologics ¡ Infected nonunions - ring (Ilizarov) E. F

Tibial Plafond Fractures (Pilon fractures)

Tibial Plafond Fractures Higher energy with axial load ¡ Significant articular damage ¡ More compromised soft-tissue envelopes ¡ High complication rate ¡

At Emergency Room ¡ ¡ Clinical evaluation : associated injuries l Associated fracture (calcaneus…. . ) l Neurologic or vascular compromise l Compartment syndrome Radiographic evaluation l X-ray : AP, mortise, and lateral view l CT scan : useful l The timing of CT : after external fixation X

Classification ¡ ¡ Ruedi and Allgöwer system : articular displacement and comminution AO/OTA system : base on continuity to the tibial shaft Type III Ruedi and Allgöwer system

Articular Surface Fracture ¡ ¡ ¡ A : anterolateral or Chaput fragment M : medial malleolar fragment P : posterior malleolar or Volkmann fragment Primary fracture lines ※ Additional articular pieces are created via secondary fracture lines J Bone Joint Surg 2005; 87: 692 -697

Surgical Treatment n n n Immediate ORIF External Fixation Staged ORIF

Immediate ORIF Principles ¡ ¡ Reconstruction of the fibula Anatomic reconstruction of the articular surface Cancellous grafting of defects Plating via the medial aspect of the tibia

Immediate ORIF Complication l l l ¡ (Ruedi and Allgöwer type III ) Wound dehiscence Infection Hardware failure Related to l l Energy associated with the injury Experience of the surgeons !!

External Fixation With/Without Limited ORIF For complex Pilon fractures ¡ The goal of preventing major complications ¡ Worse quality of reduction ¡ ¡ Timing to open surgery “ Wrinkle sign “
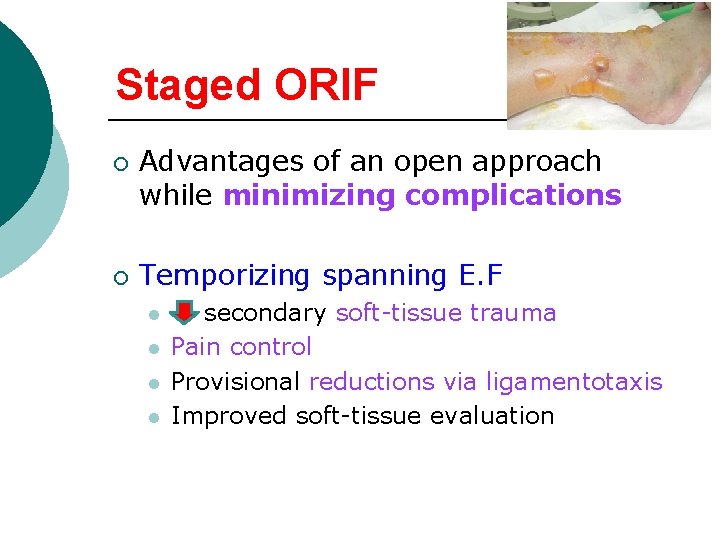
Staged ORIF ¡ ¡ Advantages of an open approach while minimizing complications Temporizing spanning E. F l l secondary soft-tissue trauma Pain control Provisional reductions via ligamentotaxis Improved soft-tissue evaluation

Staged ORIF ¡ Approaches – medial / lateral With the no-touch technique (no retraction of the soft tissues) ¡ Approach 的選擇 : ¡ l l l Fracture pattern: Articular/Metadiaphysis Direction of talar displacement Soft-tissue quality Necessity of fibular fixation Surgeon preference Orthopedics, October 2010, 33 (10), p 734 -8

Staged ORIF Multiple approaches ¡ Maximizing the interval between the approaches ¡ may be safely less than 7 cm apart ¡ Wound complications/infection J Orthop Trauma 2008; 22(5): 299 -305
Complications Wound-healing and deep infections ¡ Malunions and nonunions ¡ Postoperative scarring and stiffness ¡ Hardware prominence ¡ Posttraumatic arthritis ¡

How to get Better outcome ? ¡ Changes in treatment techniques and implant design l Staged management l Soft-tissue handling l Less extensile approaches l Indirect reduction techniques l Lower profile plates l definitive external fixation Honest assessments of individual capabilities ! (該轉就轉 !!)

Take home message Poor soft tissue envelope around ankle ¡ Be aware of compartment syndrome ¡ Respect soft tissue in surgery “No touch technique” ¡ Choose correct treatment strategy ¡ Honest assessments of individual capabilities ! (該轉就轉 !!)

Thanks for your attentions !!
- Slides: 40