Treatment of Pulpal and Periapical Diseases 1 Case











































































- Slides: 78

Treatment of Pulpal and Periapical Diseases

1. Case Selection and Treatment Planning 病例选择与治疗计划 Pathways of the pulp, 8 th edition

Chapter Outline • Common medical findings that may influence endodontics • Dental evaluation • Treatment planning

1. 1 Common medical findings that may influence endodontics

1. 1. 1 Pregnancy • Not a contradiction to endodontics • Modified treatment plan – Defer elective dental treatment during the first trimester except emergency treatment – Provide routine dental care during the second trimester – Consult physician if necessary

1. 1. 2 Cardiovascular disease • Medically compromised patients • Consult with physicians before initiation of treatment

Myocardial infarction 心肌梗死 (heart attack) within past 6 months • Increased susceptibility to repeat infarctions and other cardiovascular complications • Contraindication to any elective dental care

Patients with a history of – Heart murmur 心脏杂音 – Mitral valve prolapse with regurgitation 二尖瓣回流 – Rheumatic fever 风心病 – Congenital heart defect 先心病 – Artificial heart valves 人 瓣膜 • Increased susceptibility to infective (bacterial) endocarditis 细菌性心内膜炎 • Potentially fatal complication • Prophylactic antibiotic therapy 预防性使用抗生素

Coronary artery bypass graft • Antibiotic prophylaxis is not needed after the first few months of recovery • Consultation is advised

1. 1. 3 Cancer Patients undergoing chemotherapy and/or radiation to the head and neck • Impaired healing responses • Consult the patient’s physician before initiation of treatment

1. 1. 4 AIDS • Infection control • Asymptomatic patients are usually candidates for endodontic treatment • Medical consultation before endodontic surgery for HIV-infected patients

1. 1. 5 Diabetes • Well controlled patients are candidates for endodontic treatment • Medical consultation for patients with serious complications or before endodontic surgery – Renal disease – Hypertension – Coronary atherosclerotic disease 冠状动脉粥样硬化

1. 1. 6 Dialysis 透析 • Bleeding tendency • Elective endodontic treatment should be postponed

1. 1. 7 Prosthetic implants – Heart valves – Vascular grafts – Pacemakers 起搏器 – Cerebrospinal fluid shunts – Prosthetic joints人 关节 • Antibiotic prophylaxis to prevent infection at the site of the prosthesis • Medical consultation highly recommended

1. 1. 8 Behavioral and psychiatric disorders Consultation before using • Sedatives镇静剂 • Hypnotics催眠药 • Antihistamines 抗组胺药

1. 2 Dental evaluation • • Periodontal considerations Restorative considerations Endodontic considerations Surgical considerations

1. 2. 1 Periodontal considerations • • Periodontal probing Mobility assessment Radiographic assessment Endodontic treatment should not be planned for teeth with poor periodontal prognosis (e. g. mobility III)

1. 2. 2 Restorative considerations • Restorative treatment planning before starting endodontic treatment in a nonemergency situation – Extensive loss of tooth structure – Subosseous root caries (crown lengthening may be needed) – Poor crown-root ratio – Lack of ferrule effect – Misaligned tooth • Consultation with a prosthodontist

1. 2. 3 Endodontic considerations – Anatomy of roots and canals – Procedural errors – Small mouth – Instruments – Operator skill – Time • To determine the level of anticipated difficulty • To identify cases that should be referred

1. 2. 4 Surgical considerations • Of particular value in the diagnosis of nonodontogenic lesions • Biopsy prior to definitive endodontic treatment


1. 3 Treatment planning Scope of endodontics • Vital pulp therapy 活髓保存 • Pulpectomy or RCT 牙髓摘除术或根管治疗 • Endodontic surgery 牙髓外科 • Retreatment 再处理 • Hemisection or root amputation 牙半切或截根术 • Bleaching 牙漂白 • Apexification or apexogenesis 根尖发育成形术或根尖诱导术

Treatment planning • Treatment or extraction? • What kind of treatment ? – Endodontic – Periodontal – Restorative • • Who will be the operator? Single-visit or multi-visit? Cost Prognosis

2. Preparation for treatment • Infection control – Universal precautions (operatory preparation) – Instrument sterilization – Tooth isolation 患牙隔离 • Patient preparation – Informed consent 知情同意 – Pain control

2. 1 Infection Control • Dental personnel are at risk of exposure to a host of infectious organisms • Risk of cross-contamination in the dental environment

Effective infection control procedures • Reduce the number of micro-organisms in the working environment • Protect patients and the dental team • Improve the outcome of endodontic treatment

Universal precautions • American Dental Association (ADA) recommendation • Each patient is considered potentially infectious • The same strict infection control policies applied to all patients

Infection control guidelines • • • Dental personnel vaccinated against hepatitis B Thorough and updated patient medical history Proper barrier techniques for dental personnel – Masks, protective eyewear, disposable latex gloves – Hands, wrists and lower forearms washed with soap – Use of vacuum suction (high-volume evacuation) for high-speed handpiece, water spray or ultrasonics – Use of rubber dam

Cross-contamination related with handpieces • Surface contamination 表面污染 • Air contamination 空气污染 • Suction contamination 回吸污染

Rubber Dam 橡皮障 Routine placement of the rubber dam is considered the standard of care in USA

Reasons for use of rubber dam • Protection – aspiration or swallowing of instruments or irrigants – Soft tissue injury caused by instruments • Efficiency – Improve visibility (dry field and reduced mirror fogging) – Minimize patient conversation – Minimize the need for frequent rinsing • Reduced risk of cross-contamination • Legal considerations

Components of rubber dam system • • • Rubber dam (sheet) 橡皮障 Frame 橡皮障架 Retainers (clamps) 橡皮障夹 Punch 橡皮障打孔器 Forceps 橡皮障钳

2. 2 Informed consent • Continuous rise in dental litigation • For consent to be informed – The procedure and prognosis must be described – Alternatives to the recommended treatment must be presented along with their respective prognoses – Foreseeable risks must be described – Patients must have the opportunity to have questions answered


2. 3 Pain control • Local anesthesia • Divitalization 失活法

2. 3. 1 Local anesthesia (LA) • When to anesthetize – LA should be given at each appointment • Three misconceptions – Necrotic teeth may be instrumented without LA (vital tissue may exists periapically) – Patient’s sense aids the clinician to determine working length 根管 作长度 – LA is unnecessary during obturation phase (obturation pressure and extrusion of sealer may produce pain)

local anesthetics Lidocaine 利多卡因 Articaine 阿替卡因


Techniques • Conventional techniques – Supraperiosteal injection (local infiltration) – Regional nerve block • Supplemental techniques – Periodontal ligament (PDL) injection – Intrapulpal injection – Intraseptal injection – Intraosseous (IO) injection

• Maxillary posterior teeth – Posterior superior alveolar (PSA) block for molars – Buccal infiltration for premolars – Palatal infiltration for rubber dam retainer (optional) • Maxillary anterior teeth – Labial infiltration – Palatal anesthsia for rubber dam retainer (optional)

• Mandibular teeth – Inferior alveolar nerve (IAN) block for anterior and posterior teeth – Incisive nerve block for premolars and anterior teeth – Labial infiltration for anterior teeth

Periodontal ligment (PDL) injection • 27 -gauge/short or 30 -gauge/ultrashort needle • Placed into the periodontal space between the root and the interseptal bone • Bevel facing the root • 0. 2 m. L of anesthetic slowly deposited on the distal of each root of the tooth

• Index of successful PDL injection – Presence of resistance to anesthetic deposition – Ischemia of the soft tissue at the site of injection • Contraindications – Presence of infection or inflammation in the area of needle insertion (e. g. acute apical abscess)

Intrapulpal injection • 27 -gauge/short needle • Inserted into the pulp chamber or canal • Resistance met and 0. 2~0. 3 m. L of the solution expressed • In lack of a snug fit of the needle – warm gutta percha牙胶 inserted around the needle – Injection under pressure after cooling







3. Vital Pulp Therapy 活髓保存治疗 • Indirect pulp capping 间接盖髓术 • Direct pulp capping 直接盖髓术 • Pulpotomy 牙髓切断术 “Principles and practice of endodontics” 2 th edition

3. 1 Indirect pulp capping Indications – deep carious lesions – No history of pulpalgia – No signs of irreversible pulpitis – No pulp exposure after excavation of carious dentine

Pulp Capping Materials Calcium hydroxide 氢氧化钙 • The most commonly-used (direct) pulp-capping material – Water-based calcium hydroxide – Resin-based Calcium hydroxide e. g. Dycal, Timeline

Zinc oxide-eugenol cement (Zn. OE) • Only for indirect pulp capping • Bactericidal effect and hermetic marginal seal • Cytotoxicity-use of Zn. OE as a liner in deep carious lesions is still controversial

Procedures 1. Remove all softened, mushy or leathery dentine 2. Either ZOE or Ca(OH)2 placed on the remaining dentin to kill or suppress bacteria 3. Base 4. Temporary or permanent restoration

3. 2 Direct pulp capping Indications: • Accidental or mechanical pulp exposure (normal pulp) – Cavity preparation – Placement of pins – Trauma • Mainly for immature permanent teeth with recent (<24 hr) traumatic pulp exposure or mechanical exposure during cavity preparation

Should mature teeth be pulp capped? • Size of exposure limited to 1 mm • Contraindicated for carious tooth with pulp involvement Enamel-dentin fracture with pulpal involvement Direct pulp capping

Hemostatic reagents 止血剂 • • Saline 盐水 Hydrogen peroxide 双氧水 Diluted sodium hypochlorite 次氯酸钠 Chlorhexidine 洗必泰

Pulp capping materials • Calcium hydroxide • Mineral trioxide aggregates (MTA) 矿化三氧化聚合物

Procedures 1. Ca(OH)2 applied to the exposure to stimulate differentiation of new odontoblast-like cells and formation of secondary dentin 2. Temporary restoration placed over Ca(OH)2 3. Follow-up 4. Permanent restoration 5. Pulpotomy or endodontic treatment for symptomatic tooth

3. 3 pulpotomy Indication: Immature permanent teeth

Procedures • Removal of all carious dentin and pulp tissue to the level of the radicular pulp • Vital pulp stump capped with Ca(OH)2 • Temporary restoration • Follow-up • Asymptomatic: permanent restoration • Symptomatic: endodontic treatment

Potential problems with pulpotomy as a permanent treatment • Impossible to determine whether all disease tissue has been removed • The remaining radicular pulp tissue may undergo mineralization – Making further endodontic treatment difficult or impossible • Internal resorption

Conclusions • The vital pulp therapies are predictable in teeth with traumatic or mechanical pulp exposure. • Direct pulp capping is contraindicated for teeth with carious pulp exposure. Pulpotomy might be the choice but is considered unproven. • When – for financial or other reasons – extraction is the only alternative, pulpotomy certainly should be considered for the benefit of the patient.

4. Emergency Treatment Pretreatment emergency • Irreversible pulpitis without acute apical periodontitis • Irreversible pulpitis with acute apical periodontitis • Pulp necrosis with acute apical periodontitis Pathways of the pulp, 8 th edition Principles and practice of endodontics, 2 th edition

4. 1 Irreversible pulpitis without AAP Principles: • Complete pulp removal • Total cleaning and shaping (C/S) of the root canal system 根管清理和成形 • Pulpectomy is the best to achieve pain relief

Pulpectomy • Complete removal of the vital pulp tissue followed by cleaning , shaping and filling of the root canal(s). • Indicated for tooth with pulpitis

• Multirooted teeth at the emergency visit – Pulpotomy (removal of the coronal pulp) or patial pulpotomy (removal of the pulp from the widest canal) acceptable but less predictable in pain relief

Procedure • C/S of the root canal system • A dry cotton pellet placed in the pulp chamber • Complete caries removal and effective temporary coronal seal to prevent contamination • Occlusal reduction 咬合调整

4. 2 Irreversible pulpitis with AAP Combination of pulpal and periapical symptoms • Complete pulp removal and C/S • Ca(OH)2 medication in canals to prevent bacterial regrowth • Effective temporary coronal seal • Occlusal reduction • Oral analgesic medication when necessary

4. 3 Pulp necrosis with AAP • • • Without swelling With localized swelling With diffuse swelling

Without swelling • Thorough removal of necrotic pulp • Complete C/S of the root canal – Introducing a small file (#10/15) slightly beyond the apex to establish drainage from the periapical tissues • Ca(OH)2 dressing between visits to help eliminate remaining bacteria • Oral analgesics

With swelling • Principle: debridement清理 and drainage • Three ways to resolve swelling and infection – Drainage through the root canal – Drainage by incising a fluctuant swelling (incision and drainage, I&D) – Antibiotic treatment

Localized swelling Firstly try to establish drainage from root canals • C/S of the root canal – Introducing a small file (size 10/15) slightly beyond the apex to establish drainage – No I&D in case of good drainage • Ca(OH)2 medication • Access seal – If pus continues to drain through the canal and cannot be dried within a reasonable period of time, the tooth may be left open for <24 hrs

Incision and drainage • Indicated for localized fluctuant soft tissue swelling • Principles – Incise at the site of the greatest fluctuance – Dissect gently and extend to the roots – Keep wound clean with hot saltwater mouth rinses or CHX mouth rinse

Diffuse swelling • Possible to turn into a medical emergency and lifethreatening condition • Principles – Thorough C/S of the canals – Apical patency achieved whenever possible – Tooth left open – I&D in the absence of drainage through the canals with a rubber dam drain inserted or sutured (2~3 days) – Referral to oral surgeons

Antibiotic therapy • Indicated for patients with – Diffuse swelling regardless of the establish of drainage – Spreading infections or systemic signs • Penicillin (1 st choice) or clindamycin or erythromycin + Metronidazole

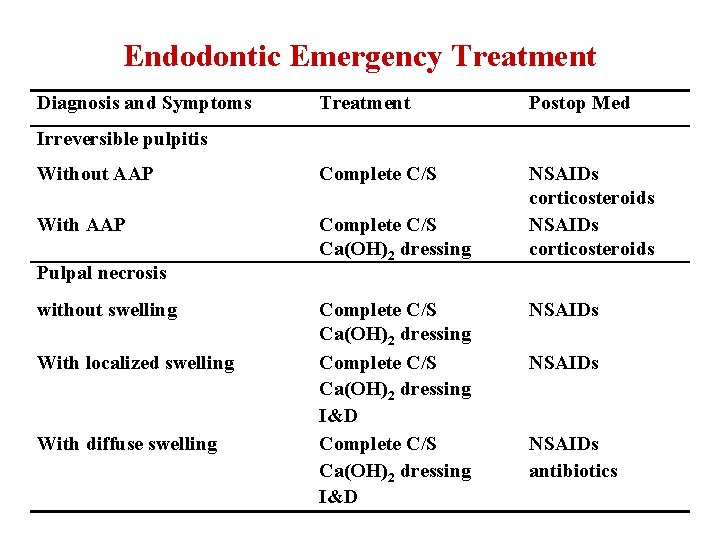
Endodontic Emergency Treatment Diagnosis and Symptoms Treatment Postop Med Without AAP Complete C/S With AAP Complete C/S Ca(OH)2 dressing NSAIDs corticosteroids Irreversible pulpitis Pulpal necrosis without swelling With localized swelling With diffuse swelling Complete C/S Ca(OH)2 dressing I&D NSAIDs antibiotics