1 1 INTRODUCTION Betalactam antibiotics Bacterial cell wall

1

1. INTRODUCTION • Beta-lactam antibiotics • Bacterial cell wall synthesis inhibitors. • These are bactericidal drugs • Chemically related to penicillins • High therapeutic index. • Recognized by the inclusion of “cef” or “ceph” in their official names. 2

2. Source & Discovery: Cephalosporium acremonium, the first source of the cephalosporins, was isolated in 1948 by Italian scientist, Brotzu from the sea near a sewer outlet off the Sardinian coast. Crude filtrates from cultures of this fungus were found to inhibit the in vitro growth of S. aureus and to cure staphylococcal infections and typhoid fever in human beings. Culture fluids in which the Sardinian fungus was cultivated were found to contain three distinct antibiotics, which were named cephalosporin P, N, and C. With isolation of the active nucleus of cephalosporin C, 7 aminocephalosporanic acid, and with the addition of side chains, it became possible to produce semisynthetic compounds with antibacterial activity very much greater than that of the parent substance 3
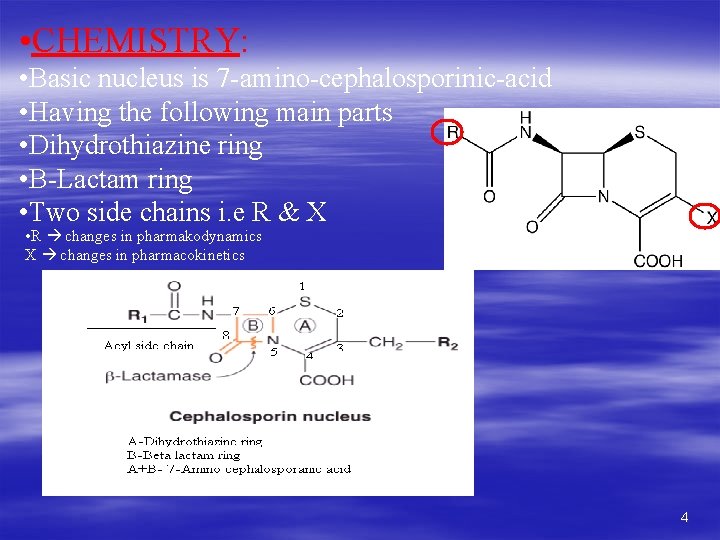
• CHEMISTRY: • Basic nucleus is 7 -amino-cephalosporinic-acid • Having the following main parts • Dihydrothiazine ring • Β-Lactam ring • Two side chains i. e R & X • R changes in pharmakodynamics X changes in pharmacokinetics 4

The nucleus of the cephalosporins, 7 -aminocephalo-sporanic acid, bears a close resemblance to 6 -amino-penicillanic acid. The intrinsic antimicrobial activity of natural cephalosporins is low, but the attachment of various R 1 and R 2 groups has yielded hundreds of potent compounds of low toxicity. Cephalosporins can be classified into four major groups or generations, depending mainly on the spectrum of their antimicrobial activity. The cephalosporin nucleus, 7 -aminocephalosporanic acid (7 -ACA), was derived from cephalosporin C and proved to be analogous to the penicillin nucleus 6 -aminopenicillanic acid, but it was not sufficiently potent for clinical use. Modification of the 7 -ACA side-chains resulted in the development of useful antibiotic agents, and the first agent cephalothin (cefalotin) was launched by Eli Lilly in 1964. 5
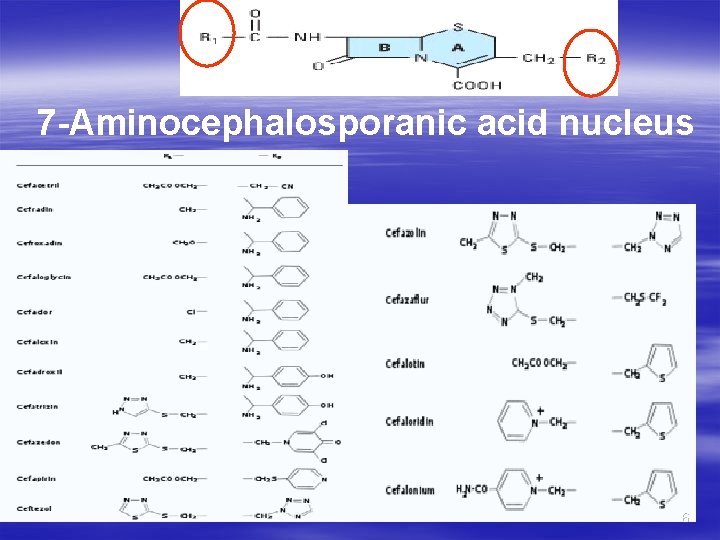
7 -Aminocephalosporanic acid nucleus 6
7

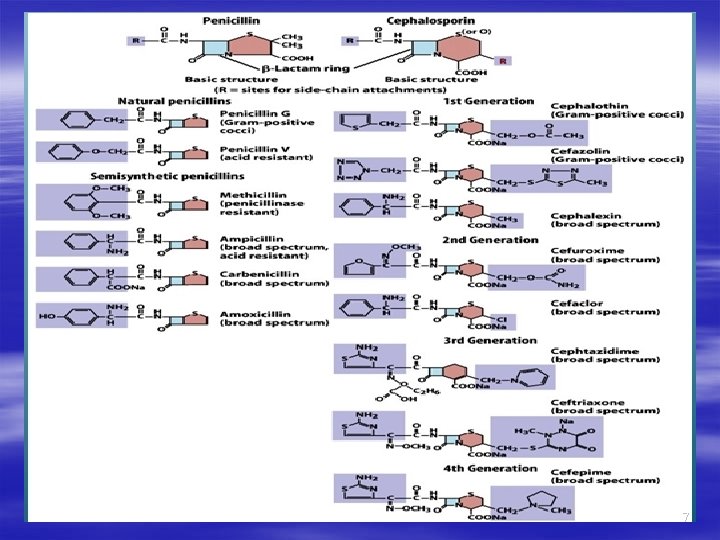
• CLASSIFICATION Cephalosporins are similar to penicillins, but more stable to many bacterial betalactamases and therefore have a broader spectrum of activity. However, strains of E. coli and Klebsiella species expressing extended-spectrum betalactamases that can hydrolyze most cephalosporins are becoming a problem. Cephalosporins are not active against enterococci and L. monocytogenes. Cephalosporins are classified (Generations/ Spectrum) as; 8

• First generation cephalosporin. • Narrow spectrum drugs G+ve & Few G-ve bacteria’s. • Can’t cross BBB except cephalothin • Highly susceptible to beta- lactamases • Drugs of this group are as follows (7 drugs) • Oral; • Cephalexin (ciporex) • Cephradine (velosef) • Cefadroxil (Duricef) • Parental; • Cefazolin • Cephalothin • Cephaloridin • cephapirin 9

Second generation cephalosporin. § § § Intermediate spectrum Can’t cross BBB Most susceptible to Betalactamase except Cefuroxime (11 drugs) Oral Paraenteral cefuroxime cephaclor cefuroxime axetil loracarbef Cephamandol Cephonicid Cephoranide Cefuroxime sodium Cephamycin • Cefmetazole • Cefotetan • Cefoxitin 10

Third generation cephalosporin. § § Extended/broad spectrum Most can cross BBB Most resistant to Beta-lactamases (10 drugs) en xime proxetil Paraenteral Ceftriaxone Ceftazidime Cefoperazone Lactamoxcef Moxalactam Cefotaxime sodium 11

Fourth generation cephalosporins. § § Extended/broad spectrum Cross BBB Highly resistant to Beta-lactamases (2 drugs) Oral Paraenteral NA Cefepime cefpirome 12
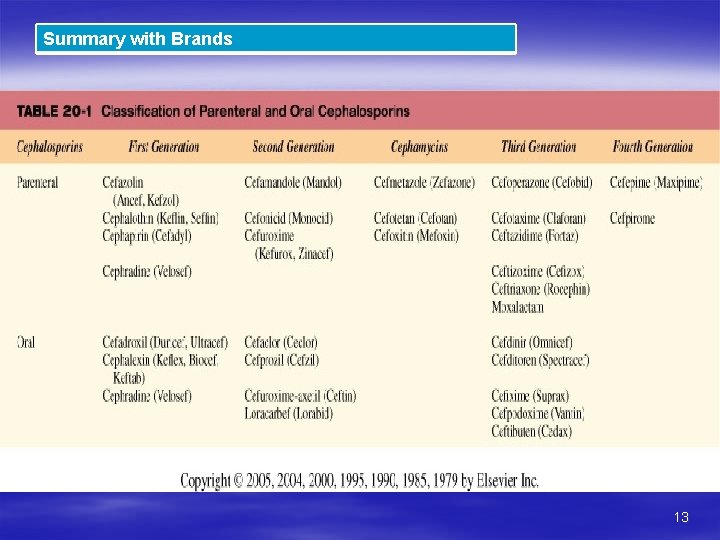
Summary with Brands 13

Spectrum of first Generation 14
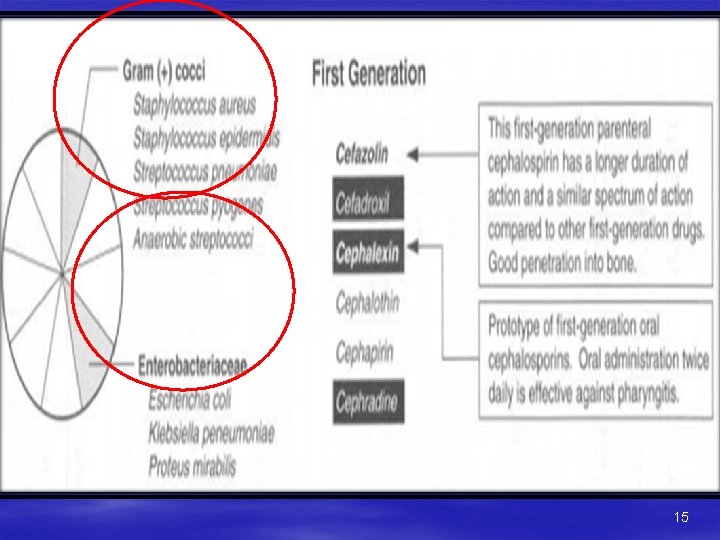
15

Spectrum of Second Generation The second-generation display greater activity against three additional gram-negative organisms. H. influenzae, Enterobacter aerogenes, and some Neisseria species, whereas activity against gram-positive organisms is weaker. • First generation µ-organisms (SSPEK)+ • Moraxella catarrhallis • H- influenza • Anaerobes esp Bacteroid fragilis 16
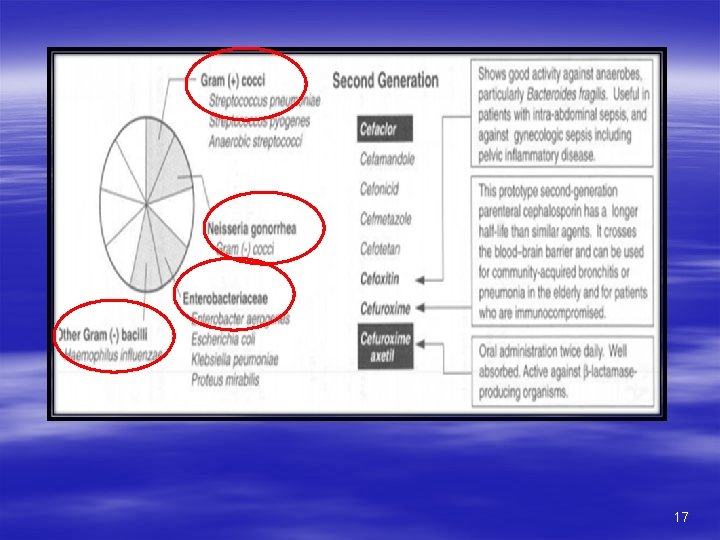
17

Spectrum of Third Generation • First generation (SSPEK) + • Second generation (MEHN) + • Pseudomonas aerogenosa • Certain enteriobacteriacea • Salmonella typhae • Vibrio cholera The third-generation cephalosporins have enhanced activity against gram-negative bacilli, including those mentioned above, as well as most other enteric organisms plus Serratia marcescens. Ceftriaxone have become agents of choice in the treatment of meningitis. 18

19

Spectrum of Fourth Generation • First generation + • Second generation + • Third generation Cefepime is classified as a fourth-generation cephalosporin and must be administered parenterally. Cefepime has a wide antibacterial spectrum being active against streptococci and staphylococci. Cefepime is also effective against aerobic gram-negative organisms, such as enterobacter, E. coli, K. pneumoniae P. mirabilis, and P. aeruginosa (mostly for resistant case 20

Cephalosporins: Mechanisms of Resistance • Mechanism Same as that of penicillins § i) Antibiotic Destruction by Betalactamases (Enterobacteraciae) § ii) Alteration in the PBP target resulting in reduced binding affinity (MRSA) § iii) Reduced penetration of the antibiotic through the LPS membrane 21

Resistance Organisms • Resistance to Cephem antibiotics. L 2 AME L 2 Legionella pneumophila Listeria monocytogenes A Atypical microbes • Mycoplasma • Mycobacterium • Spirochetes M MRSA E Enterococci • Fragilis • Liquefaciens • Durans • Zymogen 22
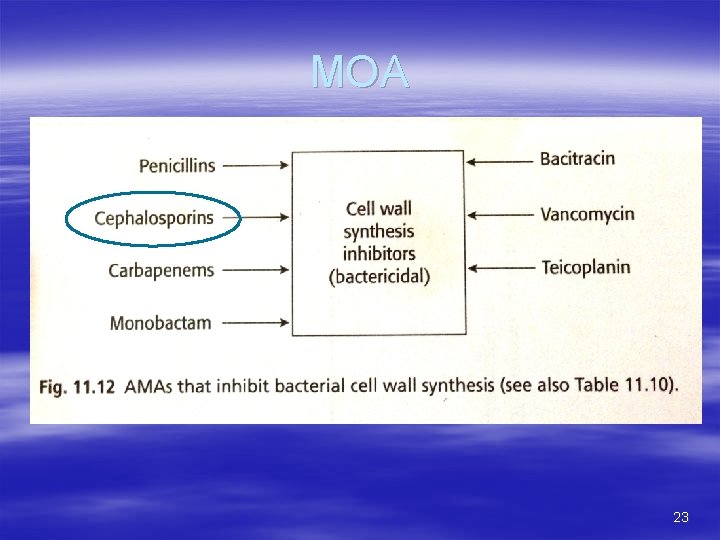
MOA 23
24

COMPARATIVE STUDY OF CEPHALOSPORINS 25

COMPARATIVE STUDY OF CEPHALOSPORINS 26
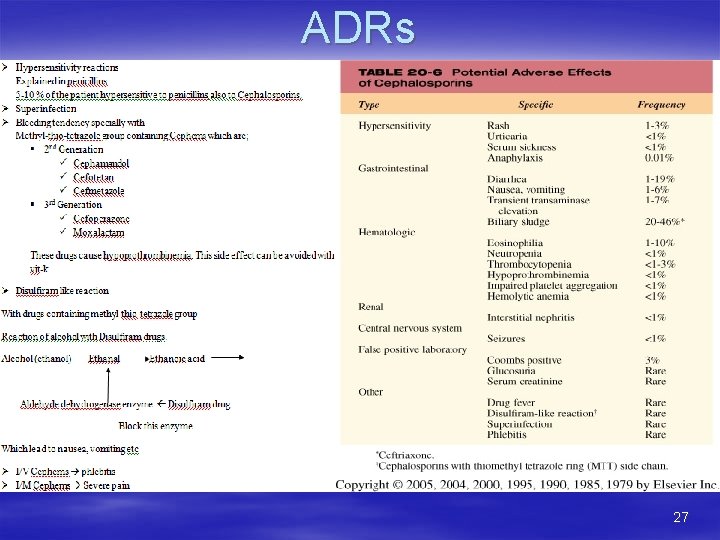

ADRs 27

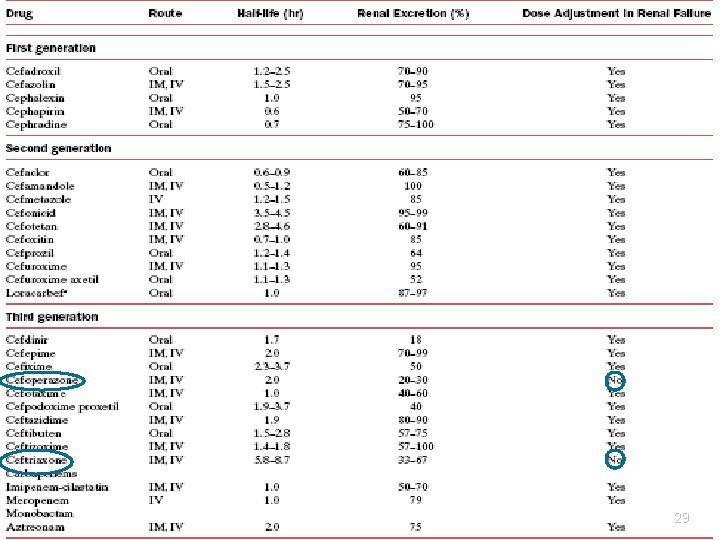
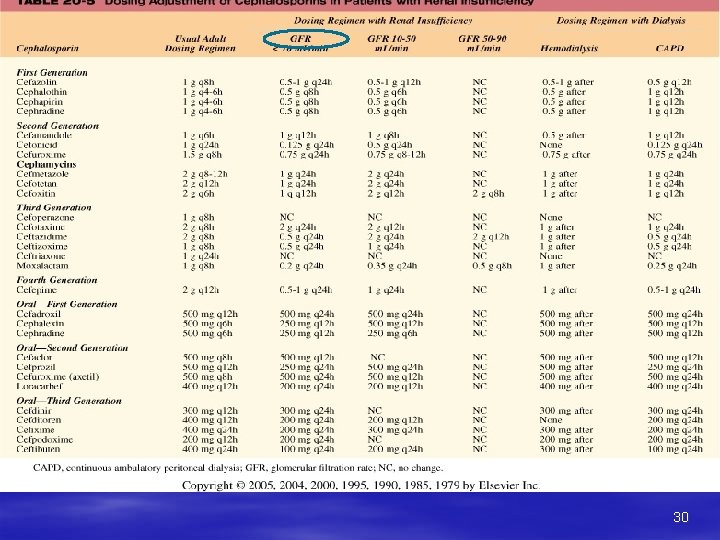
Cephalosporin prescribing in Renal Impairment § Most, apart from Ceftriaxone, need dose adjustment. 28
29
30

End 31

Cephalosporins are group of broad spectrum antibiotics, which are grouped into 4 generation with increasing activity against gram – ve bacteria and some what decreasing activity against gram + bacteria. They are more active against most streptococci except enterococci spp (which are intrinsically resistant). Importantly, they have no activity against listeria and Methicillin resistant Staphylococci. Most penicillin allergic patients will tolerate cephalosporins but this group of antibiotics should be avoided if there 32

is definitive history of anaphylaxis after penicillin administration. In general third generation cephalosporins are less active against staphylococci than 1 st and 2 nd generation cephalosporins. The intrinsic antimicrobial activity of cephalosporins is low, but the attachment of various R 1 and R 2 groups yeilded drugs of good therapeutic activity. The cephalosporins are a class of β-lactam antibiotics originally derived from Acremonium, which was previously known as "Cephalosporium". Together with cephamycins they constitute a subgroup of β-lactam antibiotics called cephems 33
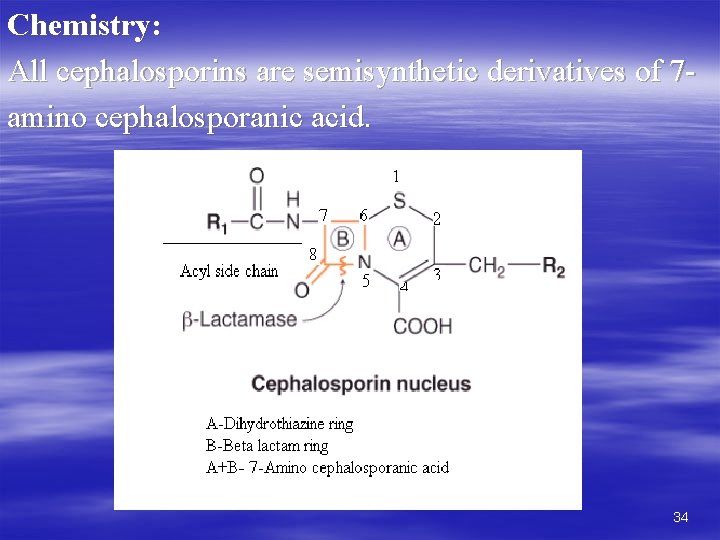
Chemistry: All cephalosporins are semisynthetic derivatives of 7 amino cephalosporanic acid. 34

Classification Cephalosporins are grouped into generations by their antimicrobial properties. The cephalosporins were designated first generation, while latter more extended were classified as 2 nd generation cephalosporins. Significantly each newer generation has greater gram – ve coverage than the preceding generation. Conversely, The older generations of cepalosporins have greater gram +ve coverage (Strep & Staph) coverage than the newer generation. 1. Gram + ve coverage diminishes as gram -ve Coverage im of cephalosporins. proves with successive 35

generations of cephalosporins. 2. Total daily dosage of individual cephalosporins is similar within each generation. 3. Frequency of dosing decreases with increase in generation. 4. Palatibility increases with increase in generation. 5. Most 2 nd and third generations are approved for use in patients less than 6 month of age. 36

The first cephalosporins were designated first generation, whereas later, more extended spectrum cephalosporins were classified as second-generation cephalosporins. Each newer generation of cephalosporins has significantly greater Gram negative antimicrobial properties than the preceding generation, in most cases with decreased activity against Gram-positive organisms. Fourth-generation cephalosporins, however, have true broad spectrum activity. 37

Classifiaction: (Lippon cots) 1. First generation cephalosporins 1. Cefadroxil 2. Cefazolin 3. Cephalexin 4. Cephapirin 5. Cephradine 6. Cephalothin Spectrum: Staphylococci (Except MRSA), Streptococci (Not enterococci), E. Coli, Proteus, Klebsiella 2. Second generation cephalosporins 1. Cefaclor 2. Cefamandole 3. Cefmetazole 4. Cefonicid 38

5. Cefotetan 6. Cefoxitin 7. Cefprozil 8. Cefuroxime 9. Cefuroxime axetil 10. Loracarbef (is a carbacepem class) Spectrum: As in first generation plus Haemophilus (Beta lactamase producing bacteria) 6. Cefoxitin (As for 1 st and 2 nd generation + Bacteroides) 3. Third generation 1. Cefdinir 2. Cefixime 3. Cefoperazone 39

5. Cefotaxime 6. Cefpodoxime 7. Ceftazidime 8. Ceftibuten 9. Ceftizoxime 10. Ceftriaxone 11. Carbapenems 12. Imipenem 13. Meropenem 14. Monobactam 15. Aztreonam Spectrum: As for 2 nd generation plus most gram –ve bacilli except pseudomonas. 7. Ceftazidime As for above plus pseudomonas. 40

4 th generation 1. Cefipime 2. Cefpirome Spectrum: As for above plus pseudomonas. 41

Classifiaction: (Antibiotic guide) 1. First generation cephalosporins 1. Cefadroxil 2. Cefazolin 3. Cephalexin 4. Cephapirin 5. Cephradine 6. Cephalothin Spectrum: Staphylococci (Except MRSA), Streptococci (Not enterococci), E. Coli, Proteus, Klebsiella 2. Second generation cephalosporins 1. Cefaclor 2. Cefoxitin 3. Cefprozil 42

4. Cefuroxime 5. Cefuroxime axetil 6. Loracarbef (is a carbacepem class) 7. Cefamendole Spectrum: As in first generation plus Haemophilus (Beta lactamase producing bacteria) 2. Cefoxitin (As for 1 st and 2 nd generation + Bacteroides) 3. Third generation 1 Cefixime 2. Cefotaxime 43

3. Cefpodoxime 4. Ceftazidime 5. Ceftibuten 6. Ceftriaxone Spectrum: As for 2 nd generation plus most gram –ve bacilli except pseudomonas. 4. Ceftazidime As for above plus pseudomonas. 44

4 th generation 1. Cefipime 2. Cefpirome Spectrum: As for above plus pseudomonas. 45

Classifiaction: (Bhattachyra) 1. First generation cephalosporins 1. Cefadroxil 2. Cefazolin 3. Cephalexin 4. Cephapirin 5. Cephradine 6. Cephalothin 7. Cephaloridine 2. Second generation cephalosporins 1. Cefaclor 2. Cefamandole 3. ceforanide 3. Cefmetazole 4. Cefonicid 5. Cefotetan 6. Cefoxitin 7. Cefprozil 46

8. Cefuroxime 9. Cefuroxime axetil 10. Loracarbef (is a carbacepem class) 3. Third generation 1. Cefdinir 2. Cefixime 3. Cefoperazone 4. Cefotaxime 5. Ceftriaxone 6. Cefpodoxime 7. Ceftazidime 8. Ceftibuten 9. Ceftizoxime 10. Moxalactam 11. Latamocef 47

12. Proxetil 13. cefditoren 14. pivoxil 4 th generation 1. Cefipime Note: The antibacterial spectrum of first generation cephalosporins is similar to that of penicillinase resistant pencillins with slightly greater gram – ve coverage. 2. Cefazolin is the only first-generation parenteral cephalosporin still in general use. 48

PK 1. PK characteristics are similar to penicillins. 2. Some third generation Cephalosporins pass into CS and are drug of choice for meningitis. Drugs are eliminated in urine by glomerular filtration and tubular secretion. Probenecid increases the plasma half life of cephalosporins. Dose of cephalosporins should be reduced in renal dysfunction. However two third generation drugs (Cefoperazone and ceftriaxone) are mainly excreted through bile, and hence no dose adjustment is required in renal dysfuction. 49

Antimicrobial spectrum: 1. First generation Cephalosporins These cephalosporins are active against Gram + cocci, some gram – ve bacteria-E. Coli, Klebsiella, proteus and some anaerobes. Inactive against pseudomonas, B. fragilis and in meningitis. They are used in UTI, bronchitis and minor infections. 2. Second generation cephalosporins They are effective against organisms affected by first generation drugs but less potent aginst gram + ve bacteria. Some of these are active against H. Influenzae (cefuroxime, cefaclor, cefamendole), and 50

Some others against B. fragilis and N. Gonorrhoea. They are inactive against pseudomonas. They can be used against beta lactamase producing bacteria and anaerobes. 3. Third generation cephalosporins: These drugs provide extended coverage against gram -ve organisms and most of these reach CNS. They are also active pseudomonas, Hemophilus and nesseiria. Ceftizoxime and moxalactam act against B. fragilis. They are used to treat meningitis caused by pneumococci, meningococci and Hemophilus influenzae, resistant UTI and penicillin resistant 51

Gonococci. 4. Fourth generation cephalosporins: Cefipime is more active against beta lactamase producing bacteria. It has good activity against enterobacter, P. aeruginosa, S. aureus and S. pneumoniae. 52

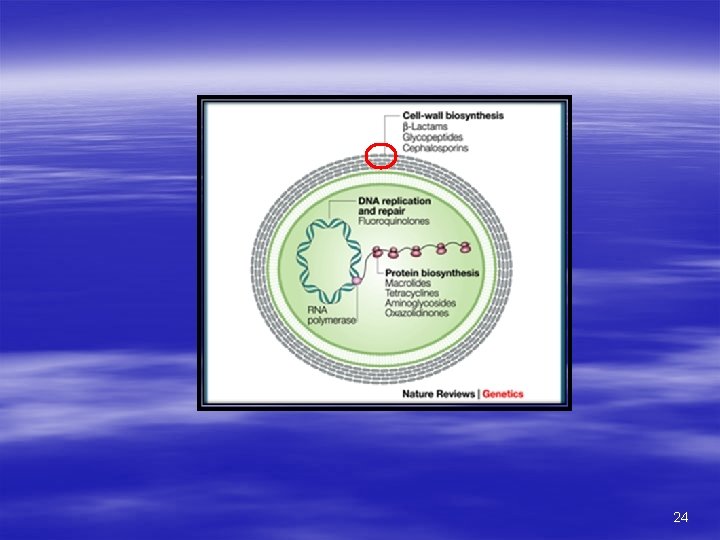
Mechanism of action; All beta lactam antibiotics have similar mechanism of action and inhibit bacterial cell wall synthesis by; 1. Attachment to specific penicillin-binding proteins (PBPs) called transpeptidase enzyme of bacteria. 2. Blocking the Transpeptidation of peptidoglycan of the bacterial cell wall and 3. Activation of autolytic enzyme of the cell wall. B/C of the mode of action, Beta lactam antibiotics are only effective against multiplying micro-organism when the cell wall is being synthesized. Beta lactam antibiotics are bactericial in nature. 53

Clinical uses: 1. Septicemia (Cefuroxime, Cefoxitime) 2. Pneumonia due to susceptible organisms 3. Meningitis (Ceftrioxone and Cefotoxime) 4. Biliary tract infections 5. Urinary tract infections 6. Sinusitis (Cefadroxil) 54

Adverse drug reactions: 1. Hypersensitivity reaction very similar to those that occur with penicillins. 2. Blood dyscrasias: (neutropenia and thrombocytopenia) 3. Nephrotoxicity (Cephradine) 4. Sometimes disufiram like reaction are seen on the ingestion of alcohol. 5. Prolog use of 2 nd and 3 rd generation cephalosporins may lead to superinfection with resistant Staphylococci, enterococci and candida. 6. Nausea, diarrhoea, rashes, electtrolyte disturbance 55

Pain at the site of injection 8. Others; Pseudomembranous colitis, superinfection and eosinophilia. 9. Certain cephalosporins (Cefamendole, Cefoperazone) may cause disulfiram like reaction 56

1. First generation cephalosporins 1. Cephalexin 0. 25 -1 g q. i. d oral 2. Cefazolin 0. 5 -2 g q. i. d i. v. 3. Cefadroxil 0. 5 -1 g o. d/b. i. d oral 2. Second generation cephalosporins 1. Cefaclor 0. 25 -0. 5 g t. i. d oral 2. Cefuroxime 0. 25 -0. 5 g b. i. d i. v 3. Cefuroxime axetil 0. 25 -0. 5 g b. i. d oral 57

3. Third generation 1. Cefixime 0. 1 -0. 2 g o. d/b. i. d oral 2. Cefoperazone 1 -2 g b. i. d im/i. v 3. Cefotaxime 1 -2 g b. i. d im/iv 4. Ceftriaxone 1 -2 g o. d/b. i. d i. v 5. Ceftazidime 0. 5 -2 g t. i. d/b. i. d i. v 58

4 th generation 1. Cefipime 0. 5 -2 g b. i. d i. v 59

Mechanism of resistance: 1. Inability of the drug to reach the site of action i. e poor penetration by the drug. 2. Alteration in the antibiotic binding proteins so that interaction does not occur. 3. Degradation of the drug by Beta lactamases. 4. Failure of activation of autolytic enzymes in the cell Wall. . 60

Septicemia: It the presence of bacteria in the blood and is often associated with severe disease. Pneumonia: It the inflammatory illness of the lungs. It is described as lung alveolar inflammation and abnormal alveolar filling with fluid. Signs and Symptoms: 1. Cough producing yellow or greenish sputum or Phelgm 2. High grade fever characterized by shaking chills. 3. Shortness of breath. 61

Meningitis: It is the inflammation of protective membrane covering the brain and spinal cord, collectively known as Meningitis. Signs and symptoms: 1. Severe headach 2. Nuchal rigidity (Neck is stiff i. e unable to flex neck forward) 3. High grade fever 4. Altered mental status 5. Photophobia (Unable to tolerate light) 6. Phonophobia ((Unable to tolerate loud noise) 62

Sinusitis: It is the inflammation of paranasal sinuses (Air filled spaces communicating with nasal cavity within the bones of skull and face) Superinfection: It is an infection following previous infection, especially when caused by micro-organisms that are resistant or become rsistant to antibiotic used earlier. It is produced by sudden growth of type of bacterai etc. different from original offenders in a wound or lesion or area under treatment. 63

Pseudomemranous colitis: It is the infection of the colon caused by clostridium difficile. Signs and symptoms: 1. Offensive swelling diarrhoea 2. Fever 3. Abdominal pain DD-Transpeptidase: It is a bacterial enzyme that cross links the peptidoglycan chains to form rigid cell wall. Also known as DD-Peptidase, DD trans. Peptidase, D-alanyl D-alanine, Carboxypeptidase, and serine type D-Ala 64

D-Ala carboxypeptidase. 1. Narrow spectrum drugs: As the name implies, these are only active against relatively small number of micro-organisms. In general narrow spectrum antibiotics are effective against the gram +ve bacteria. 2. Moderate spectrum drugs: These drugs are effective against gram +ve and most systemic, enteric and urinary tract gram – ve bacteria. 3. Broad spectrum: These are drugs that are effective against all prokaraytes with two exceptions 1. Mycobacterium 2. Pseudomonas 65

4. Extended spectrum; Effective against both Gram positive, Gram negative bacteria and other bacteria such as pseudomonas, clebsiella etc. 66

Cephamycins are a group of beta-lactam antibiotics. They are very similar to cephalosporins, and the cephamycins are sometimes classified as cephalosporins. Like cephalosporins, cephamycins are based upon the cephem nucleus. Cephamycins were Originally produced by Streptomyces, but synthetic ones have been produced as well. Cephamycins possess a methoxy group at the 7 -alpha position. & Include 1. Cefoxitin 2. Cefotetan 3. Cefmetazole 67

Note 1. Persons allergic to penicillins can be given azreotenam with little likehood of allergic reactions. 2. As with the penicillins, the cephalosporin –lactam Ring is the chemical group associated with Antibacterial activity. 2. Cephalosporins have been associated with superinfections with Clostridium difficile, enterococci, MRSA, coagulasenegative staphylococci, P. aeruginosa, and Candida albicans. Overgrowth by toxigenic C. difficile occasionally causes pseudomembranous colitis in patients treated with cephalosporins. Some third-generation 68

Cephalosporins induce production of extended spectrum lactamases (ESBLs) in P. aeruginosa. The ESBLs can transfer to various Enterobacteriaceae and produce organisms resistant to almost all –lactam antibiotics. 3. Drugs with the methylthiotetrazole ring can also Cause severe disulfiram-like reactions; consequently, Alcohol and alcohol-containing medications must be avoided. 69

Clinical Uses The first-generation cephalosporins have activity against most of the bacterial pathogens that colonize skin and infect wounds. Consequently, first-generation cephalosporins are useful in antimicrobial prophylaxis before surgery. Second-generation cephalosporins are used to treat infections caused by susceptible organisms. For example, cefoxitin and cefotetan have Good anaerobic activity, and they have utility in the Treatment and prophylaxis of lower abdominal and Gynecological infection. A broad spectrum of antibacterial activity makes third-generation 70

cephalosporins important in the treatment of a wide range of infections, including Lyme disease, pneumonia, peritonitis, and sepsis syndrome. 71

BACITRACIN Bacitracin is a cyclic peptide mixture first obtained from the Tracy strain of Bacillus subtilis in 1943. It is active against gram-positive microorganisms. Bacitracin inhibits cell wall formation by interfering with dephosphorylation in cycling of the lipid carrier that transfers peptidoglycan subunits to the growing cell wall. There is no cross-resistance between bacitracin and other antimicrobial drugs. Bacitracin is highly nephrotoxic when administered systemically and is only used topically. 72

Bacitracin is poorly absorbed. Topical application results in local antibacterial activity without systemic toxicity. Bacitracin, 500 units/g in an ointment base (often combined with polymyxin or neomycin), is indicated for the suppression of mixed bacterial flora in surface lesions of the skin, in wounds, or on mucous membranes. Solutions of bacitracin containing 100200 units/m. L in saline can be used for irrigation of joints, wounds, or the pleural cavity. 73
Others cell wall synthesis inhibitors 1. Cycloserine 2. Fosfomycin 3. Daptomycin 4. Teicoplanin 74
- Slides: 74