Cardiovascular Physiology I Physiology of the Heart The







































- Slides: 92

Cardiovascular Physiology I: Physiology of the Heart & The Cardiac Cycle

References: Seeley, R. , Stephens, T. , and Tate, P. , Anatomy & Physiology. 8 th ed. Mc. Graw Hill Company Inc. , (2008) l Guyton, A. , Hall, J. , Textbook of Medical Physiology. 11 th ed. WB Saunders Co. (2006) • Martini, F. , Fundamentals of Anatomy & Physiology. 6 th ed. Benjamin Cummings Inc (2003) l

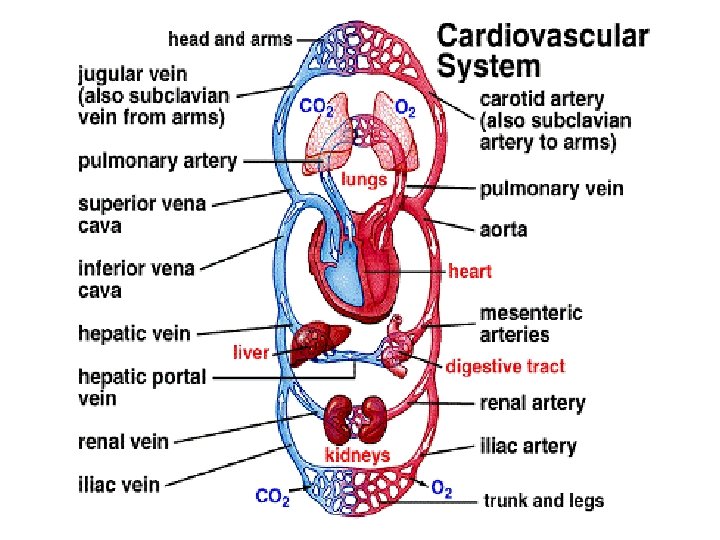
Part I FUNCTIONS OF THE CARDIOVASCULAR SYSTEM


Function of the CV System: Blood l Transport l Protection l Regulation

Function of the CV System: Heart l Generating BP l Blood routing l Ensuring one-way blood flow l Regulating blood supply

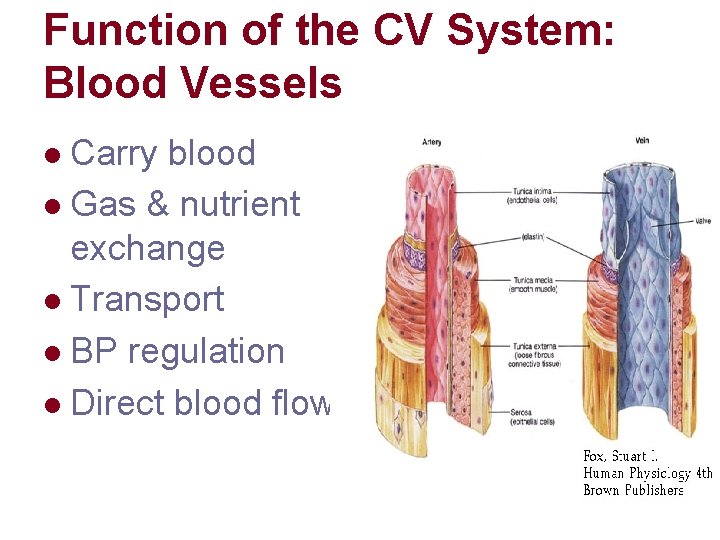
Function of the CV System: Blood Vessels Carry blood l Gas & nutrient exchange l Transport l BP regulation l Direct blood flow l

Part II THE CARDIAC CYCLE

Cardiac cycle l Events occurring from the beginning of one heartbeat to the beginning of the next l Consists of 2 periods as to the activity of the ventricles

Cardiac Cycle Systole – period of contraction l Isovolumetric contraction l Ejection l Diastole – period of relaxation l Isovolumetric Relaxation l Passive Ventricular filling l Atrial Contraction l

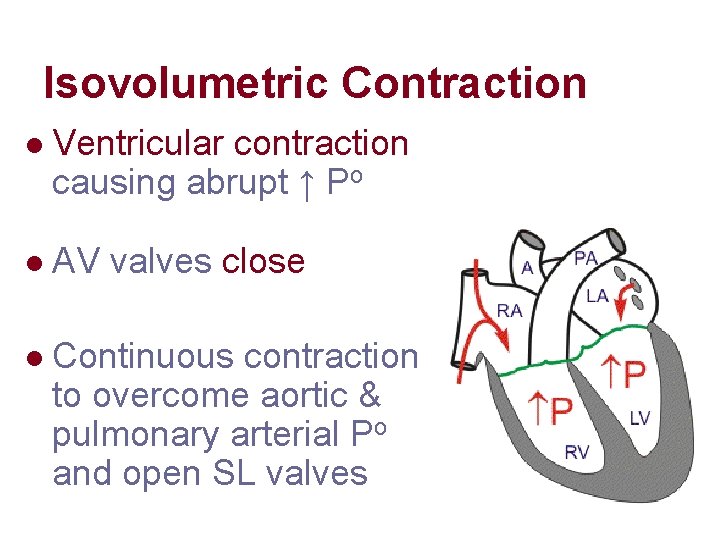
Isovolumetric Contraction l Ventricular contraction causing abrupt ↑ Po l AV valves close l Continuous contraction to overcome aortic & pulmonary arterial Po and open SL valves


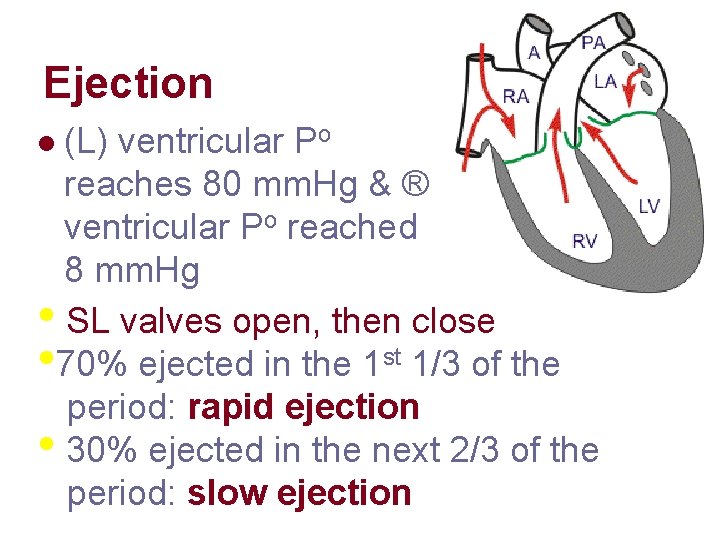
Ejection (L) ventricular Po reaches 80 mm. Hg & ® ventricular Po reached 8 mm. Hg • SL valves open, then close • 70% ejected in the 1 st 1/3 of the period: rapid ejection • 30% ejected in the next 2/3 of the period: slow ejection l


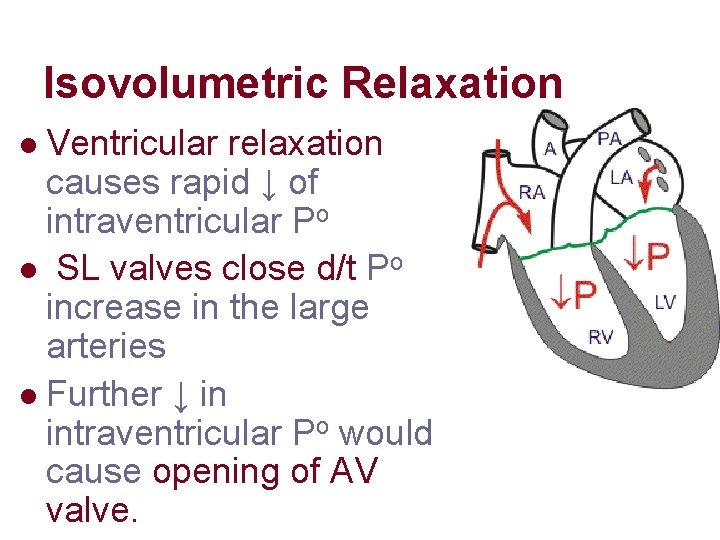
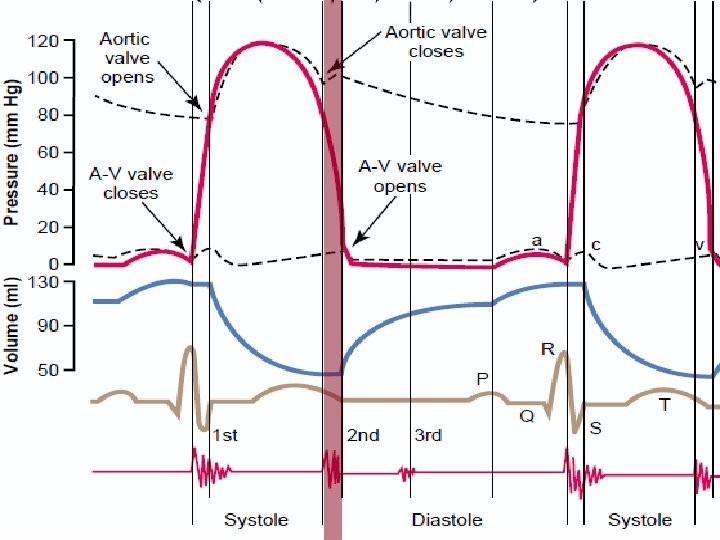
Isovolumetric Relaxation Ventricular relaxation causes rapid ↓ of intraventricular Po l SL valves close d/t Po increase in the large arteries l Further ↓ in intraventricular Po would cause opening of AV valve. l


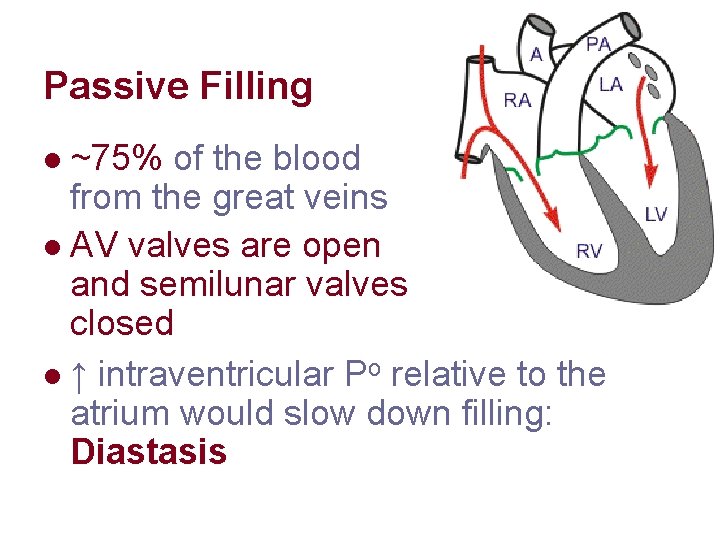
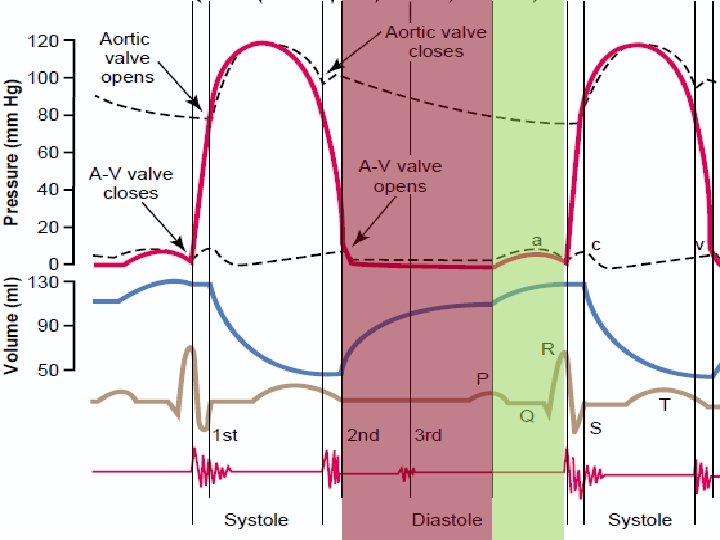
Passive Filling ~75% of the blood from the great veins l AV valves are open and semilunar valves closed l ↑ intraventricular Po relative to the atrium would slow down filling: Diastasis l

Atrial Contraction of atria will eject the remaining 25% into the ventricles


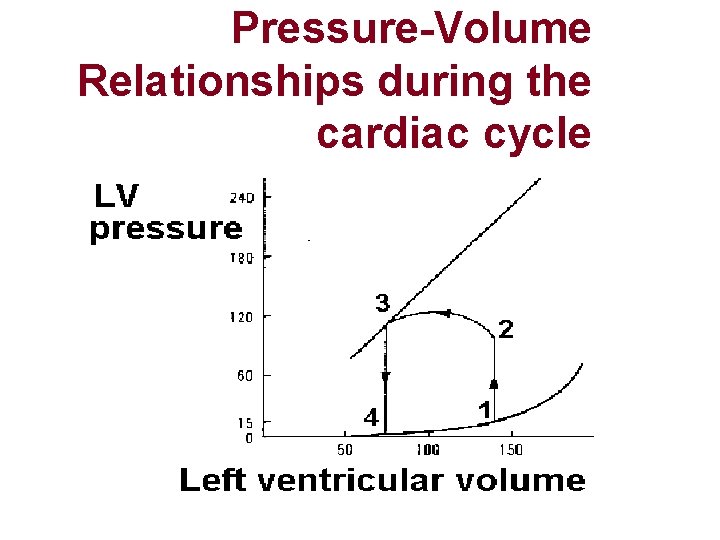
Ventricular Volumes Relative to Systolic and Diastolic contractions Volume of Blood in the Ventricle END-DIASTOLIC VOLUME STROKE VOLUME OUTPUT END SYSTOLIC VOLUME EJECTION FRACTION (110 -120 m. L) (-70 m. L) What remains after systole (40 -50 m. L) Usually 60%

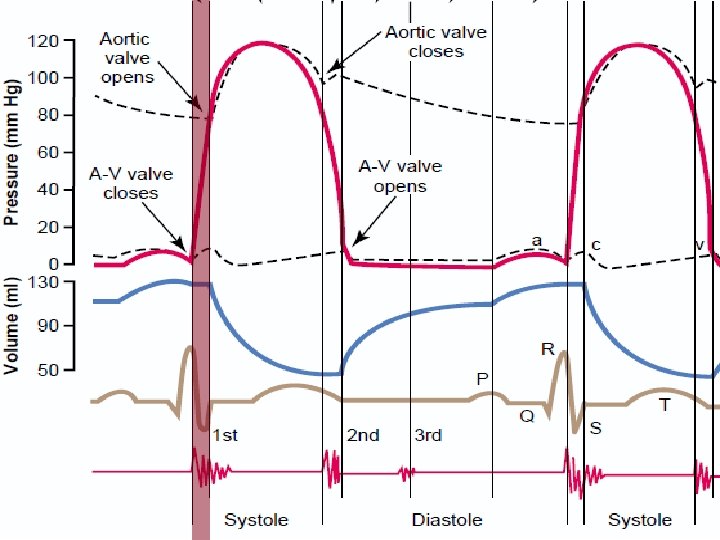
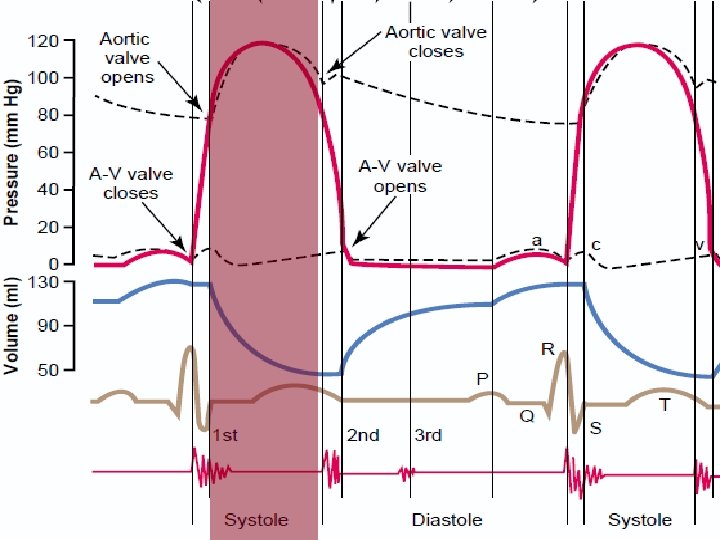
Pressure-Volume Relationships during the cardiac cycle

Summary of Pressure Volume Relationships l CARDIAC CYCLE TABLE SUMMARY. pdf

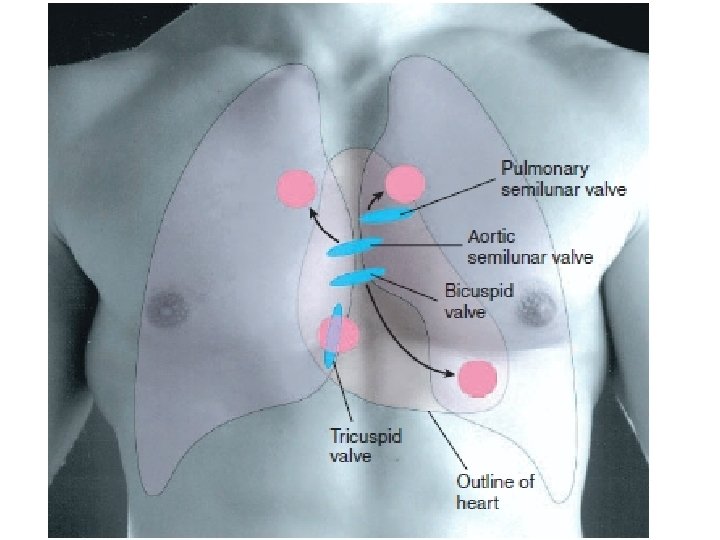
Heart Valves l Atrioventricular valves l l Prevent back flow of blood between ventricles and atria Semilunar valves l Prevent back flow of blood between aorta (and pulmonary artery) and ventricles

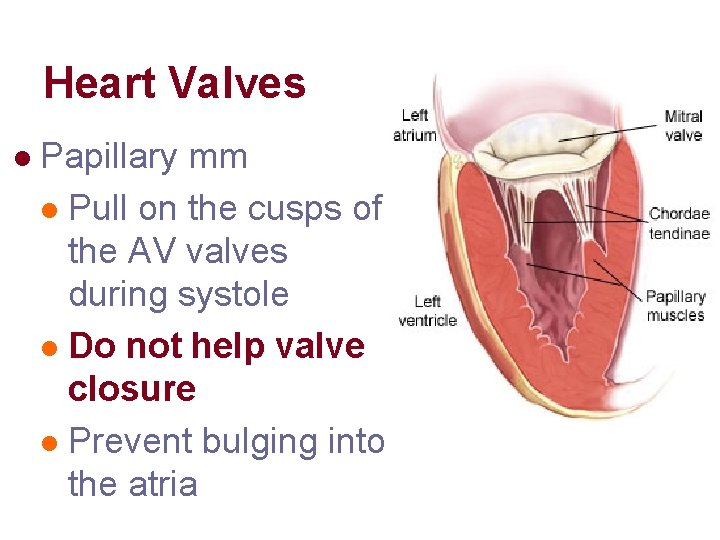
Heart Valves l Papillary mm l Pull on the cusps of the AV valves during systole l Do not help valve closure l Prevent bulging into the atria

Heart Valves and Heart Sounds l 1 st heart sound: Lub l closure of the AV valves l Heard during systole l Relatively low in pitch and long l 2 nd heart sound: Dup l Closure of the SL valves l Heard during diastole l Rapid snap l Shorter

Heart Valves and Heart Sounds l 3 rd heart sound l Mid-diastole l Blood oscillation as it rushes from the aorta l Weak rumbling sound l 4 th heart sound l Atrial contraction l Inrush of blood into the ventricles l Low frequency sound


Heart Valves and Abnormal Heart Sounds l Murmurs: Abnormal Heart Sounds l Valvular Stenosis: Opening is too small l Valvular Regurgitation: Valve does not close completely

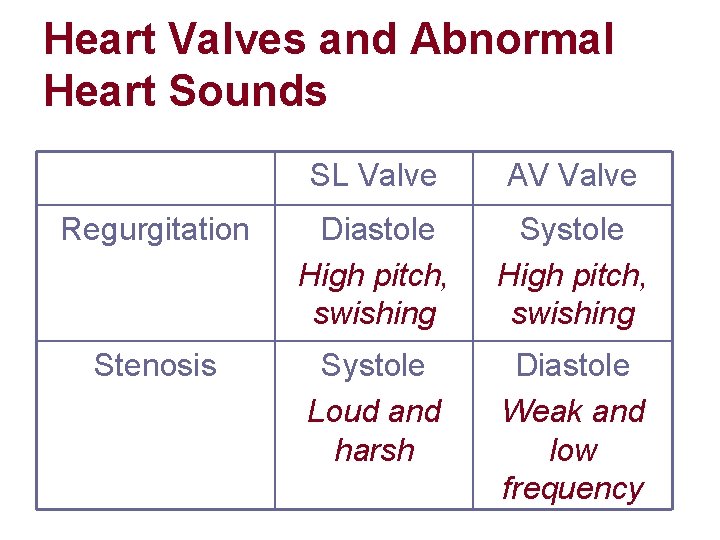
Heart Valves and Abnormal Heart Sounds SL Valve AV Valve Regurgitation Diastole High pitch, swishing Systole High pitch, swishing Stenosis Systole Loud and harsh Diastole Weak and low frequency

Part III CARDIAC ELECTROPHYSIOLOGY


Let’s review!

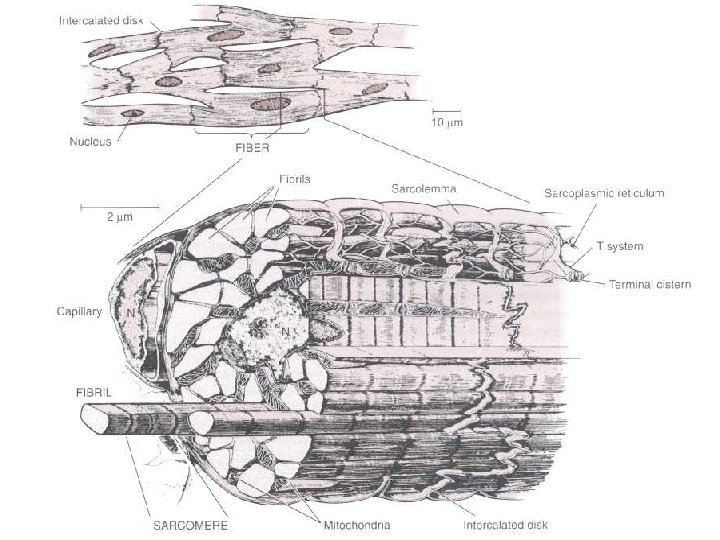
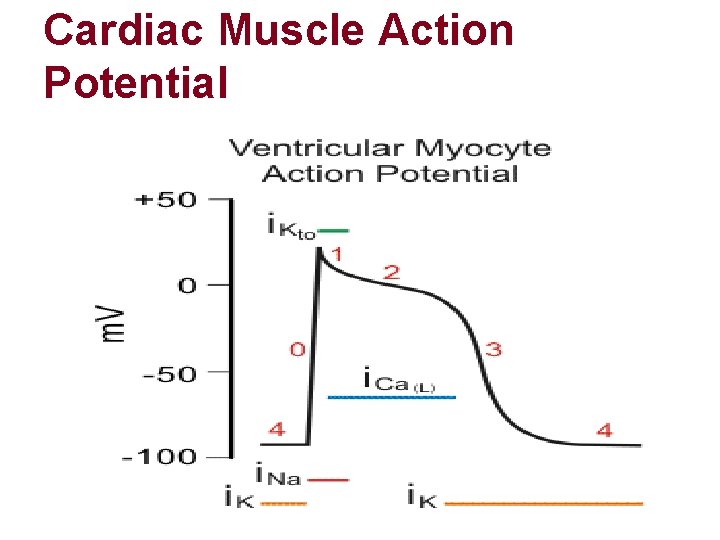
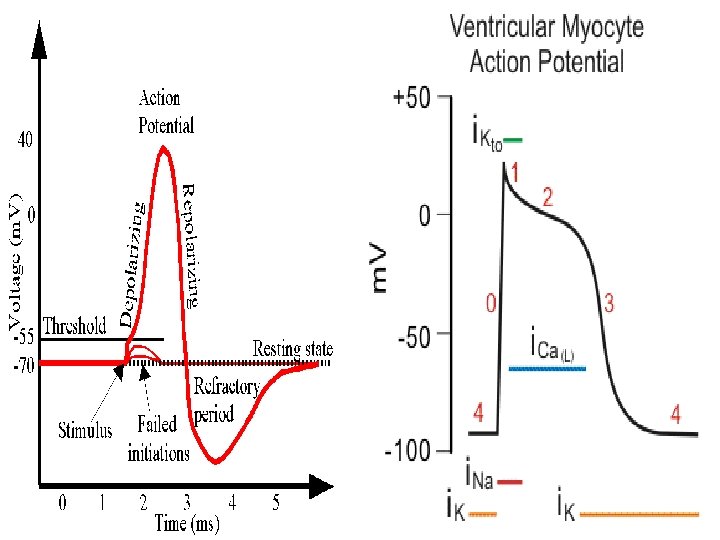
Cardiac Muscle Action Potential


Cardiac Muscle Action Potential l RMP of cardiac muscle: -90 m. V l Overshoots until ~+20 m. V

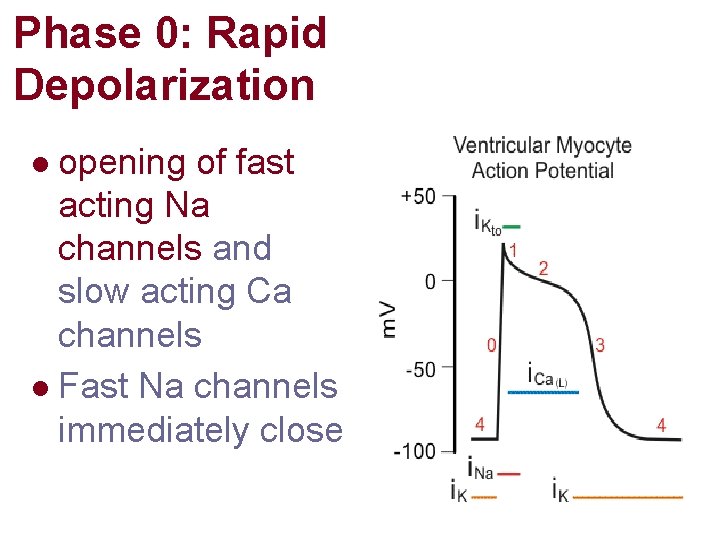
Phase 0: Rapid Depolarization opening of fast acting Na channels and slow acting Ca channels l Fast Na channels immediately close l

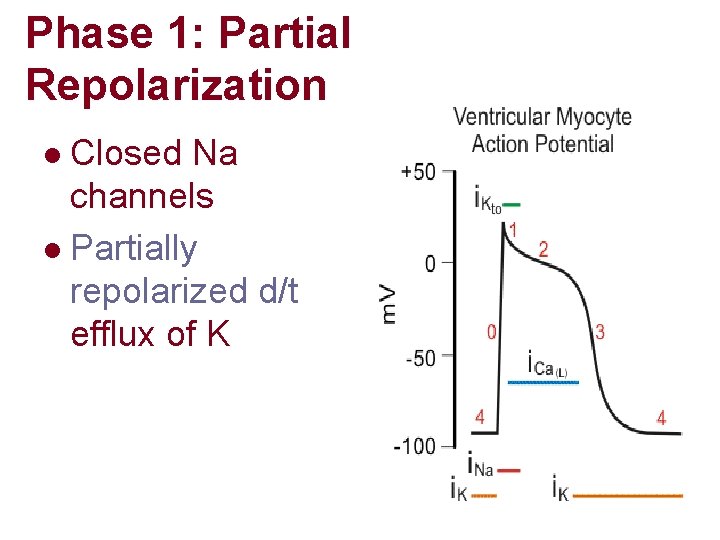
Phase 1: Partial Repolarization Closed Na channels l Partially repolarized d/t efflux of K l

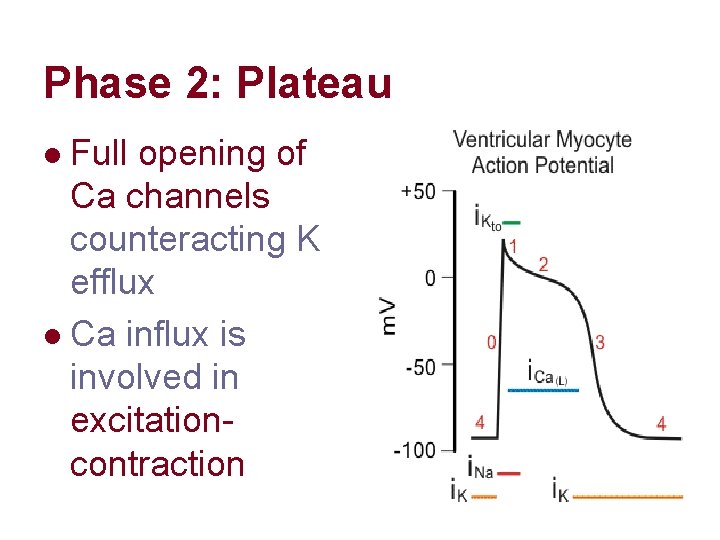
Phase 2: Plateau Full opening of Ca channels counteracting K efflux l Ca influx is involved in excitationcontraction l

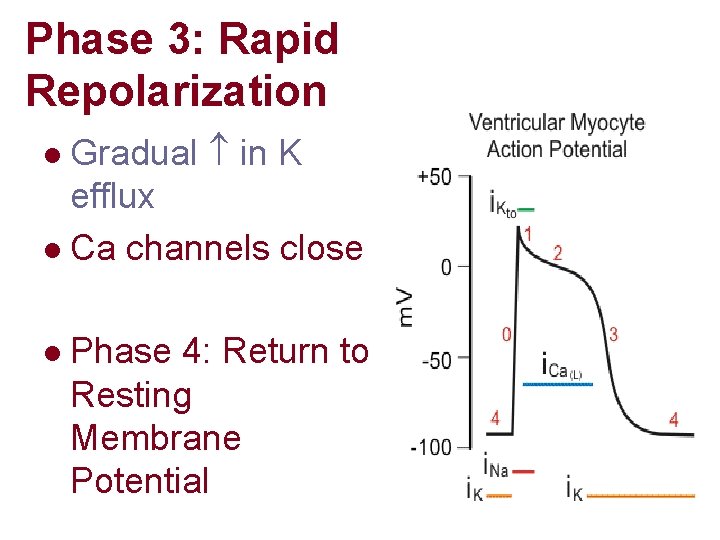
Phase 3: Rapid Repolarization Gradual in K efflux l Ca channels close l l Phase 4: Return to Resting Membrane Potential

Cardiac Muscle Excitation. Contraction Coupling l Phase 2 l Action potential spreads to interior via T-tubules l Excitation of T-tubules promote Ca release from sarcoplasmic reticulum adding to Ca influx l Actin-Myosin binding

Cardiac Muscle Excitation – Contraction Coupling l Phase 3 l Ca influx is cut l Ca ions are pumped back into the sarcoplasmic reticulum l relaxation

Part IV CONDUCTING SYSTEM OF THE HEART

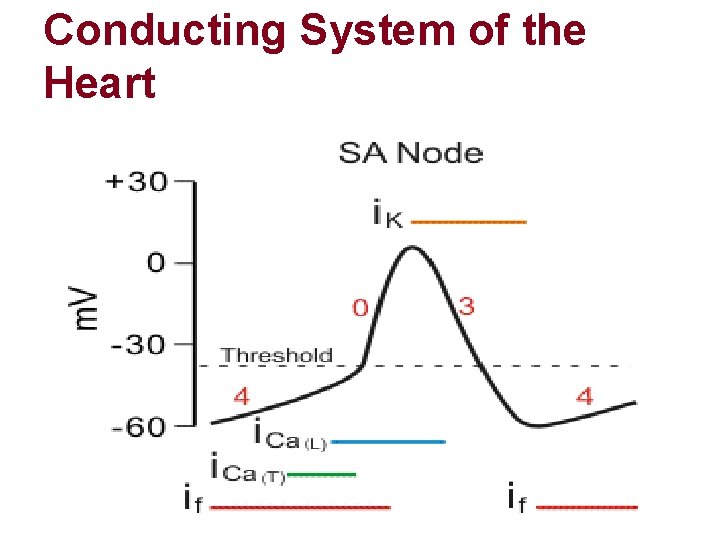
Conducting System of the Heart l Sinoatrial Node l Superior posterolateral wall of ® atrium, below and lateral to SVC opening l Non-contractile l Self excitatory

Conducting System of the Heart l Sinoatrial node l RMP of -55 to -60 m. V l Firing level of -40 m. V l Depolarization only by opening of slow Na-Ca channels

Conducting System of the Heart

Conducting System of the Heart Internodal pathways l Anterior Tract of Bachman l Middle Tract of Wenckebach l Posterior Tract of Thorel l Impulses converge on the Atrioventricular node l

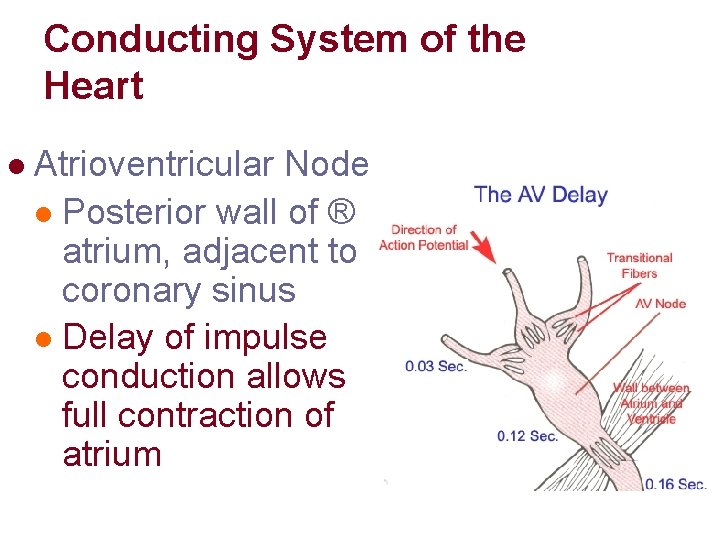
Conducting System of the Heart l Atrioventricular Node l Posterior wall of ® atrium, adjacent to coronary sinus l Delay of impulse conduction allows full contraction of atrium

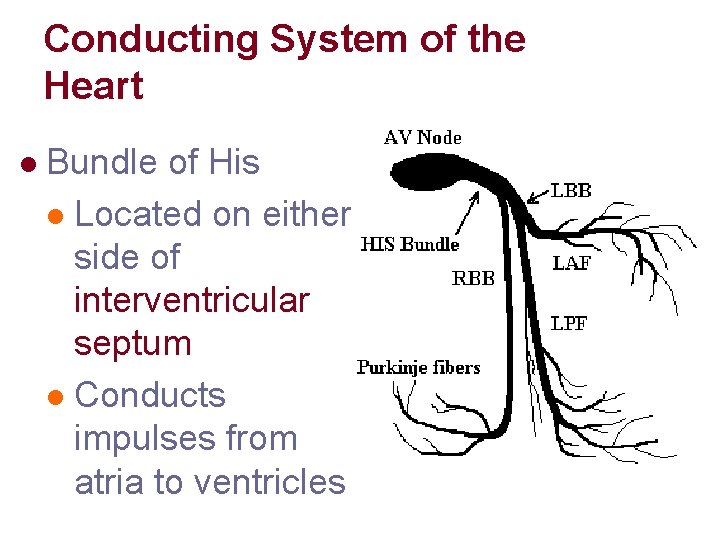
Conducting System of the Heart l Bundle of His l Located on either side of interventricular septum l Conducts impulses from atria to ventricles

Conducting System of the Heart l Purkinje Fibers l Conducting tissues of the ventricles

Conducting System of the Heart l l Why is the SA node the pacemaker of the heart? Frequency of impulse production is faster Structure Impulses/min SA 70 -80 AV 40 -60 Purkinje Fibers 15 -40 Greater rhythmicity depresses other potential pacemakers

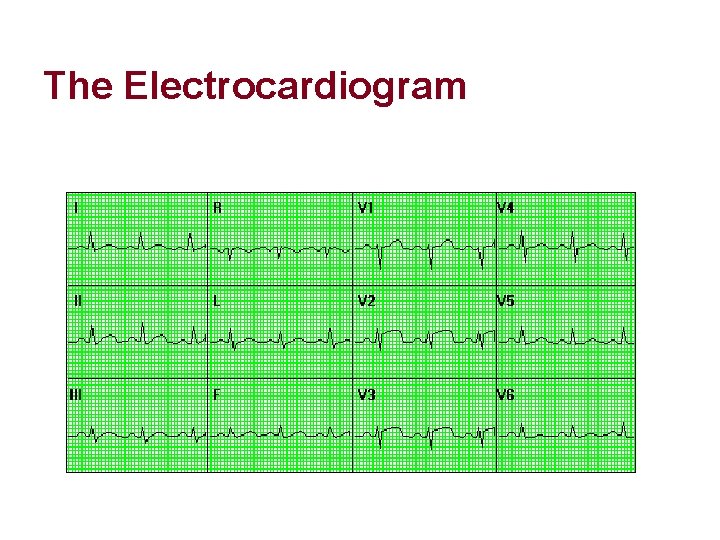
The Electrocardiogram l a graphic representation of the electrical activity generated by the atria and ventricles.

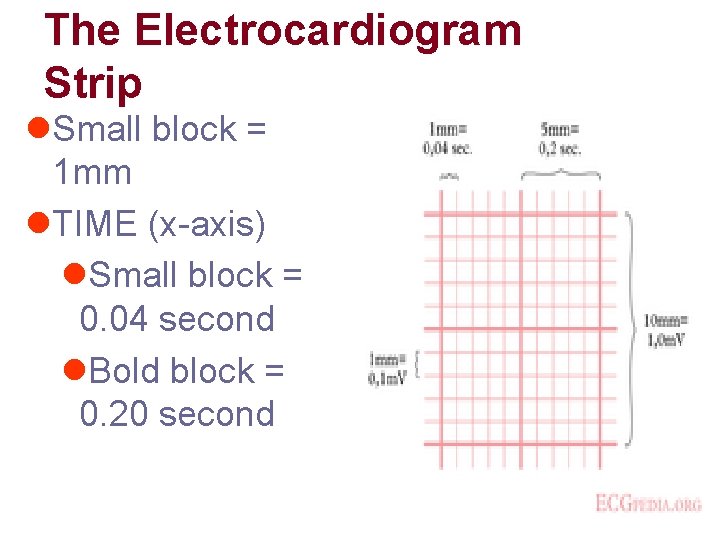
The Electrocardiogram Strip l. Small block = 1 mm l. TIME (x-axis) l. Small block = 0. 04 second l. Bold block = 0. 20 second

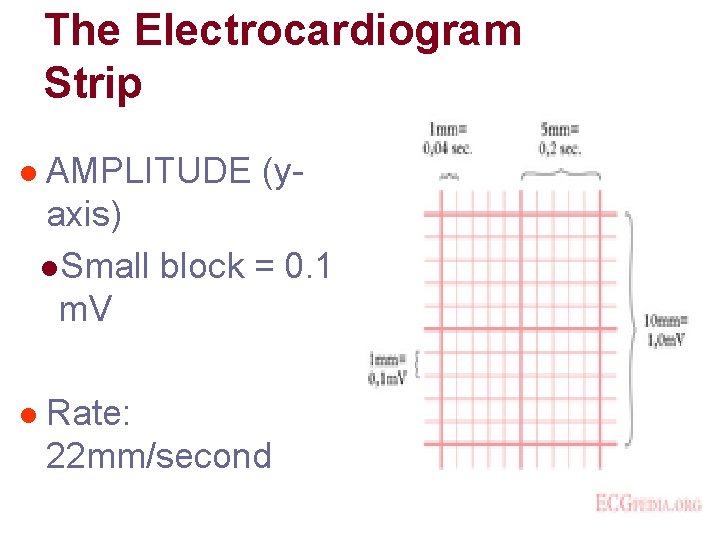
The Electrocardiogram Strip l AMPLITUDE (yaxis) l. Small block = 0. 1 m. V l Rate: 22 mm/second

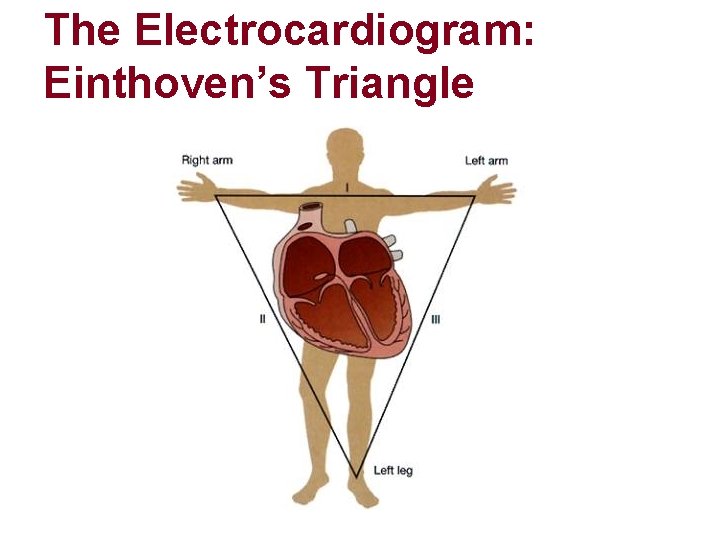
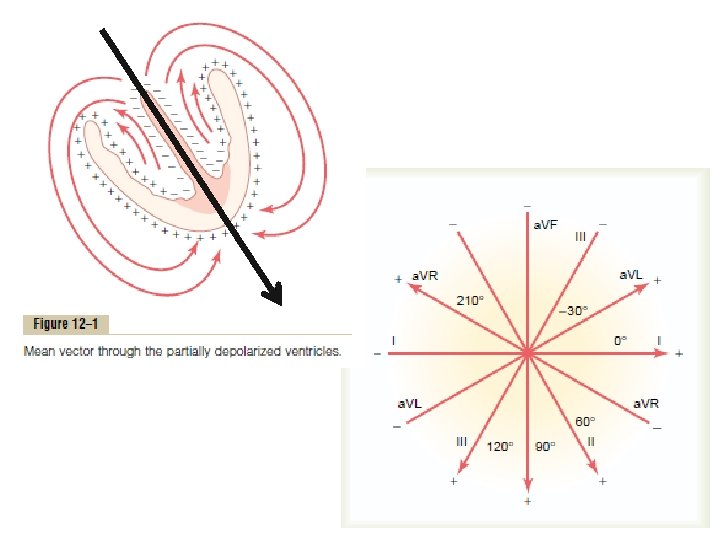
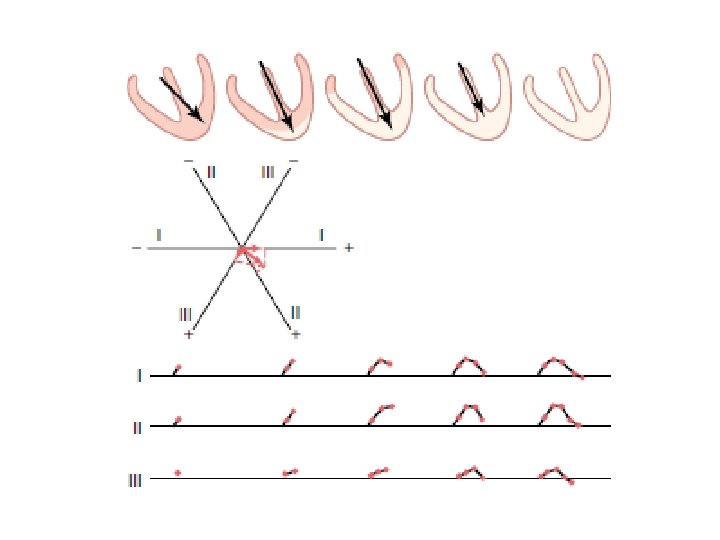
The Electrocardiogram: Einthoven’s Triangle

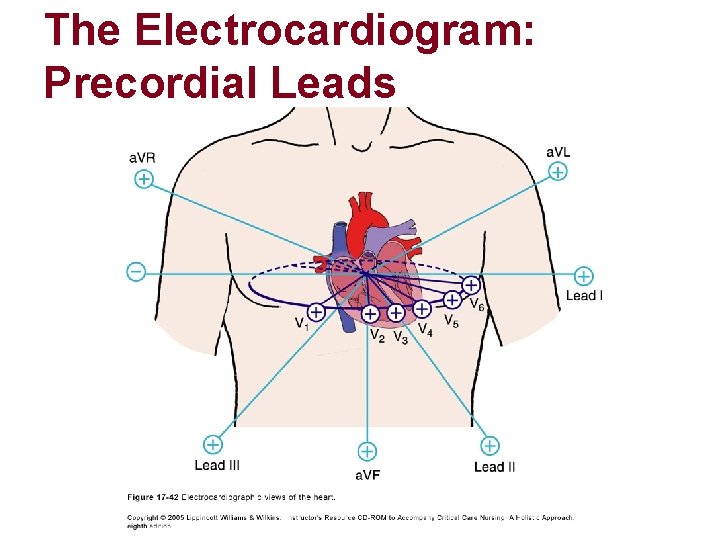
The Electrocardiogram: Precordial Leads

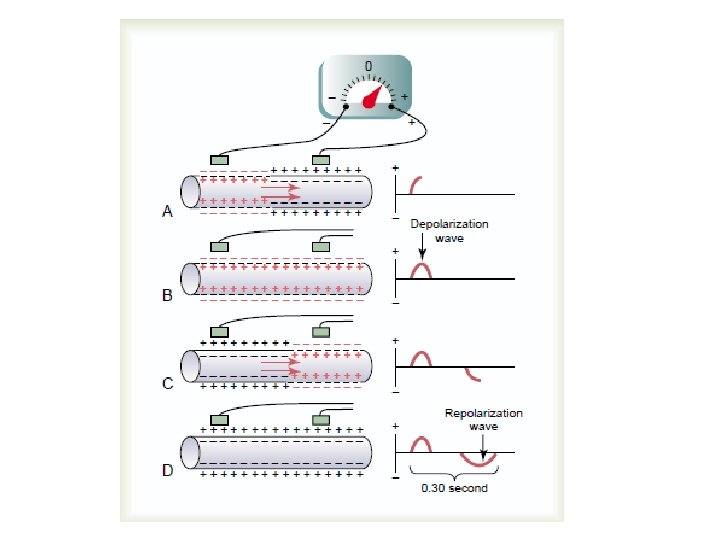
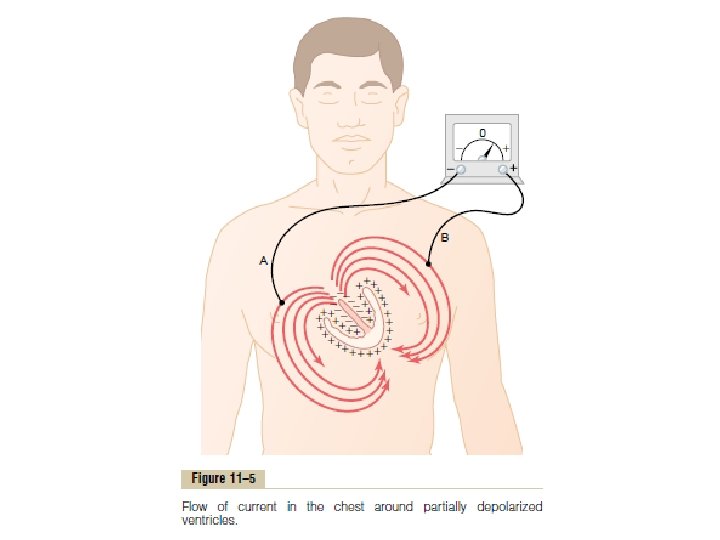
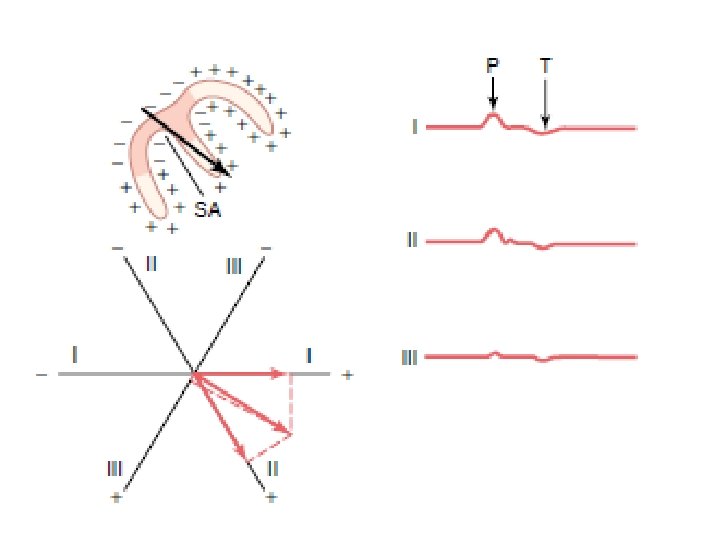
The Electrocardiogram When a positive wave of depolarization within the heart cells moves toward a positive skin electrode, there is an upward deflection on the ECG




The Electrocardiogram

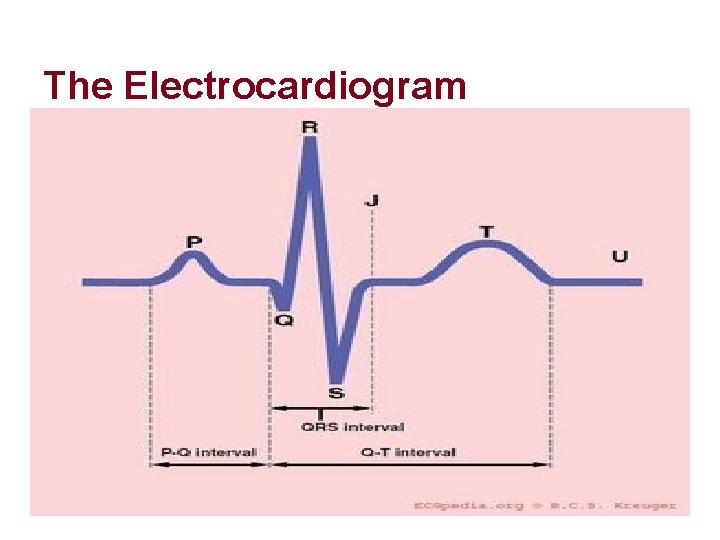
The Electrocardiogram

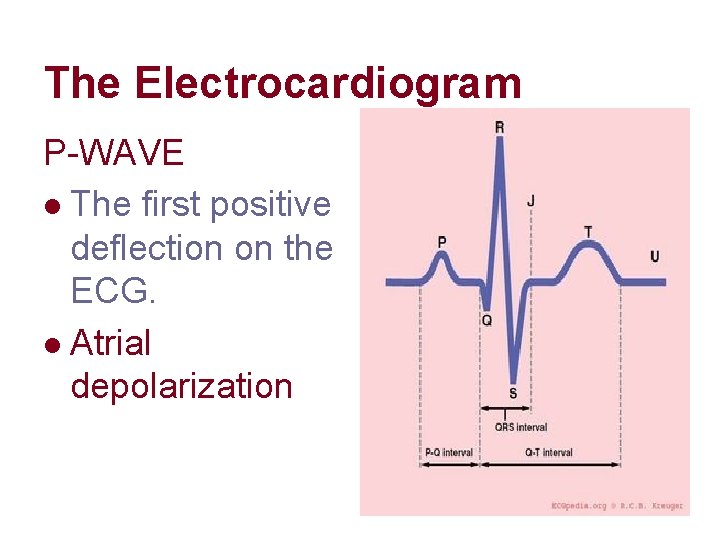
The Electrocardiogram P-WAVE l The first positive deflection on the ECG. l Atrial depolarization


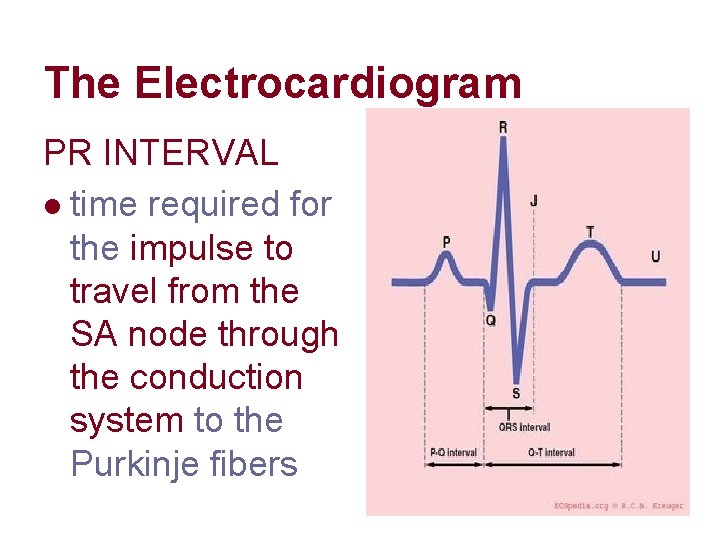
The Electrocardiogram PR INTERVAL l time required for the impulse to travel from the SA node through the conduction system to the Purkinje fibers

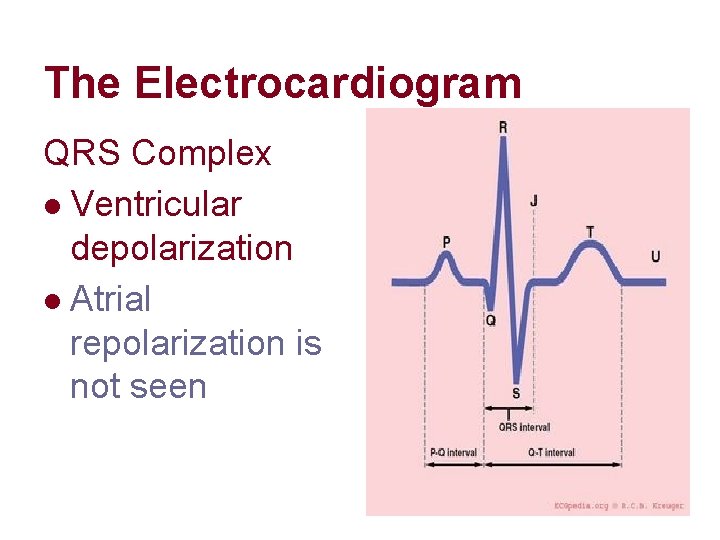
The Electrocardiogram QRS Complex l Ventricular depolarization l Atrial repolarization is not seen

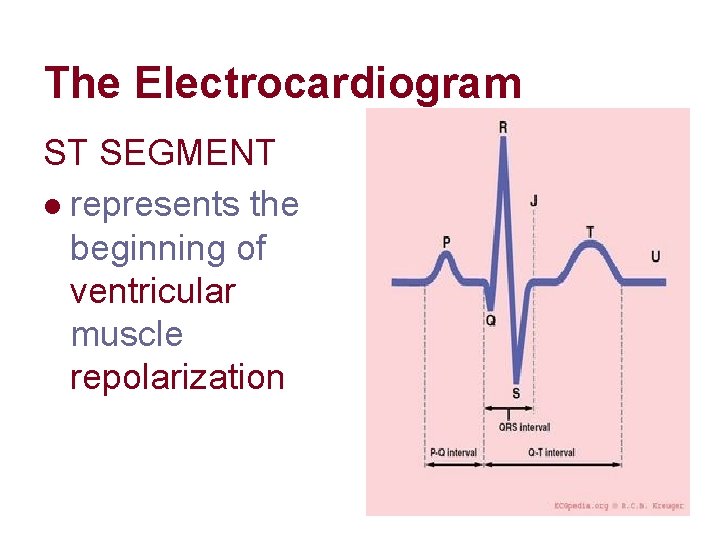
The Electrocardiogram ST SEGMENT l represents the beginning of ventricular muscle repolarization

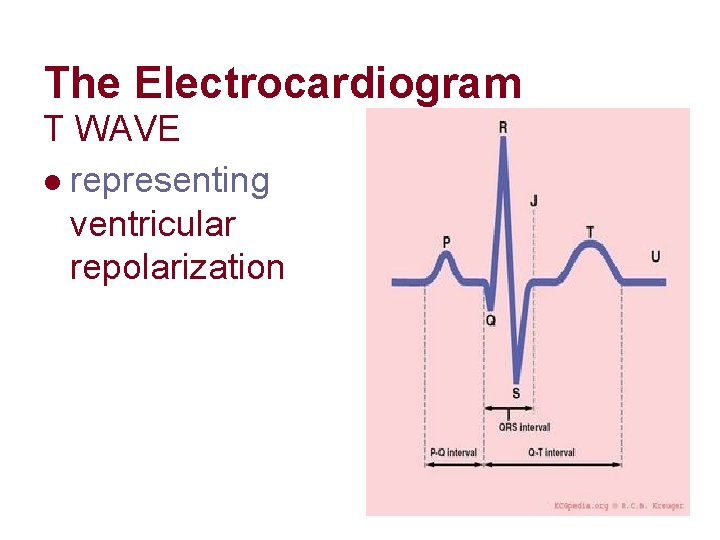
The Electrocardiogram T WAVE l representing ventricular repolarization


The Electrocardiogram

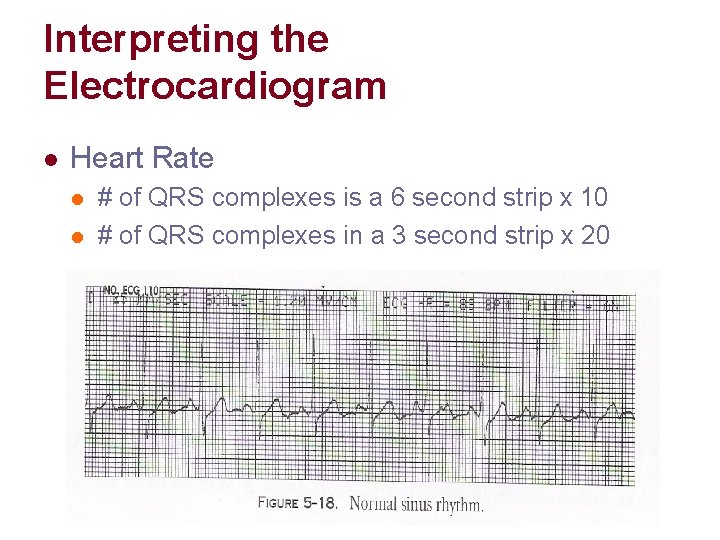
Interpreting the Electrocardiogram l Heart Rate l l # of QRS complexes is a 6 second strip x 10 # of QRS complexes in a 3 second strip x 20

Interpreting the Electrocardiogram l Heart Rate = 300 / # of big squares between 2 QRS complex l Triplicate system 300 – 150 – 100 – 75 – 60 - 50

Anatomic Representation in the ECG l Inferior wall l II, III, AVF l Anterior Wall l V 1, V 2, V 3, V 4 l Lateral Wall l I, AVL, V 5, V 6 l Superior Wall l AVR

Part V CARDIAC REGULATION

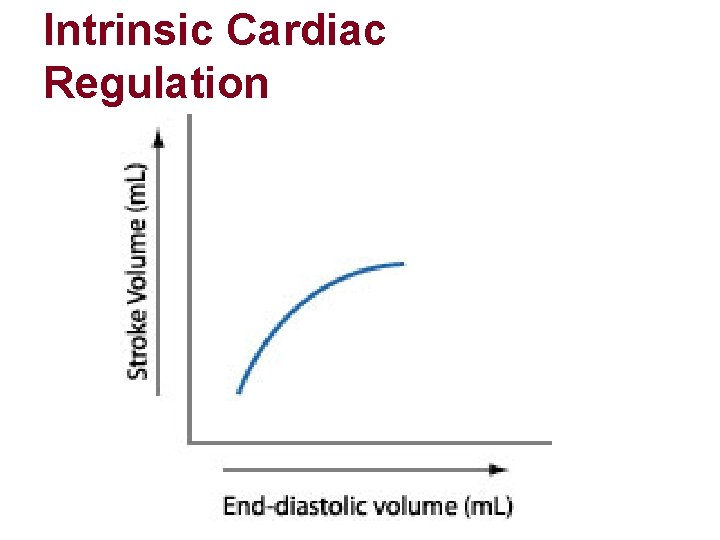
Intrinsic Cardiac Regulation l Largely determined by Preload l The degree to which the ventricular walls are stretched at the end of diastole l Determined by venous return (amount of blood returning to the heart)

Intrinsic Cardiac Regulation l Starling’s Law of the Heart l Relationship between preload and force of cardiac contraction l preload = contraction force = SV

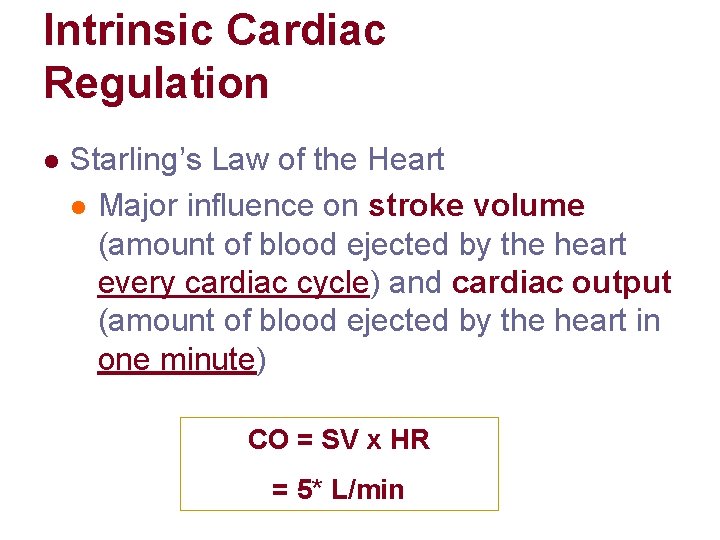
Intrinsic Cardiac Regulation l Starling’s Law of the Heart l Major influence on stroke volume (amount of blood ejected by the heart every cardiac cycle) and cardiac output (amount of blood ejected by the heart in one minute) CO = SV x HR = 5* L/min

Stroke Volume and Inotropic regulation l Inotropic effects l Force of Contraction l ↑ inotropic effect = ↑ force of contraction = ↑ amount of blood ejected

Intrinsic Cardiac Regulation

Intrinsic Cardiac Regulation l Afterload l pressure against which the ventricles must pump blood l afterload= work of cardiac mm = SV

Extrinsic Cardiac Regulation l Hormonal l Catecholamines l Neuronal l Autonomic nervous system l Cardiorespiratory centers of the medulla

Extrinsic Cardiac Regulation l Other control mechanisms l Barorecpetor and chemoreceptor l Temperature l Electrolyte levels (K, Na, Ca)

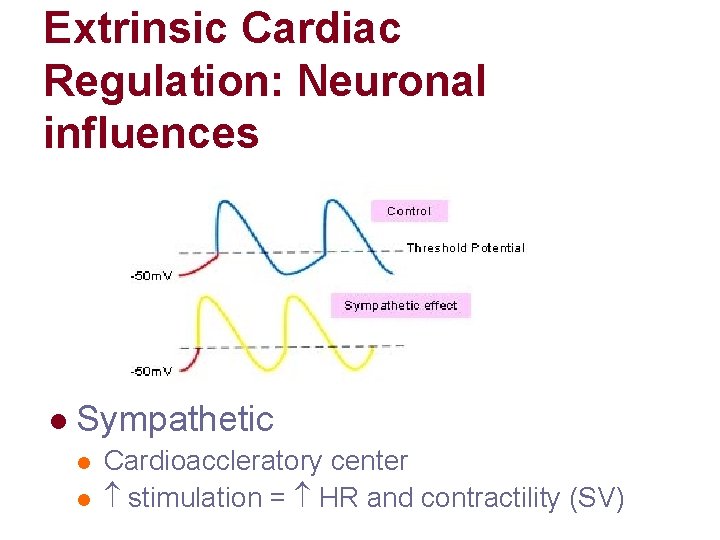
Extrinsic Cardiac Regulation: Neuronal influences l Sympathetic l l Cardioaccleratory center stimulation = HR and contractility (SV)

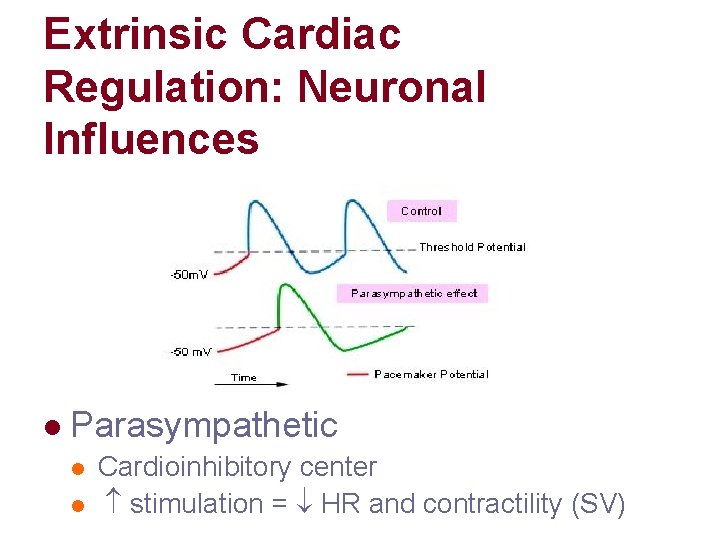
Extrinsic Cardiac Regulation: Neuronal Influences l Parasympathetic l l Cardioinhibitory center stimulation = HR and contractility (SV)

Extrinsic Cardiac Regulation: Hormonal influences l Catecholamines l Norepinephrine and Epinephrine : sympathetic stimulation

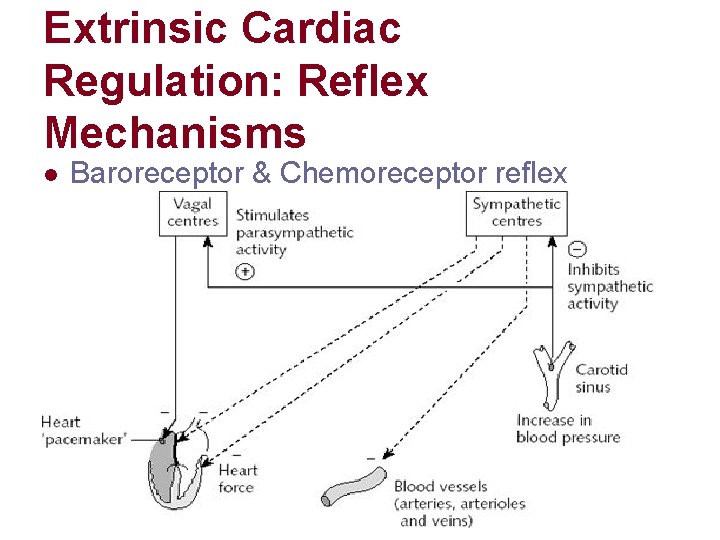
Extrinsic Cardiac Regulation: Reflex Mechanisms l Baroreceptor & Chemoreceptor reflex

Extrinsic Cardiac Regulation: Other Control Mechanisms l Na & Ca levels l Direct relation with HR l K levels l Inverse relation with HR

Extrinsic Cardiac Regulation: Other Control Mechanisms l Temperature l 1 o. C = 4 bpm l Coronary blood flow l coronary blood flow = contractility

Extrinsic Cardiac Regulation: other Control Mechanisms l Bainbridge reflex l relationship of venous return with heart rate l VR = HR

Heart Rate and Chronotropic Regulation l Chronotropic effects l Speed of contraction l ↑ chronotropic effects = ↑ speed of contraction = ↑ amount of blood ejected

Ejection Fraction and Heart Function l Determines how much of the blood entering the ventricles is pumped (End-Diastolic ventricular Volume - Endsystolic ventricular volume) End diastolic ventricular volume l (N) 63 -77% for males and 55 -75% for females

The Hypoeffective Heart Inhibition of nervous excitation l Ab. N heart rhythm l Valvular heart disease l Hypertension l Cardiac anoxia l Myocardial damage l

THE END