Blood Blood Vessels Circulation 21 1 Cardiovascular System

Blood, Blood Vessels & Circulation 21 -1
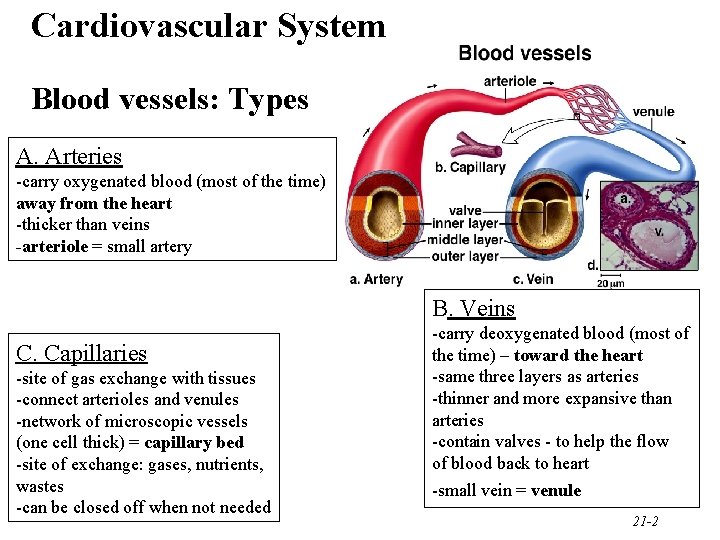
Cardiovascular System Blood vessels: Types A. Arteries -carry oxygenated blood (most of the time) away from the heart -thicker than veins -arteriole = small artery B. Veins C. Capillaries -site of gas exchange with tissues -connect arterioles and venules -network of microscopic vessels (one cell thick) = capillary bed -site of exchange: gases, nutrients, wastes -can be closed off when not needed -carry deoxygenated blood (most of the time) – toward the heart -same three layers as arteries -thinner and more expansive than arteries -contain valves - to help the flow of blood back to heart -small vein = venule 21 -2
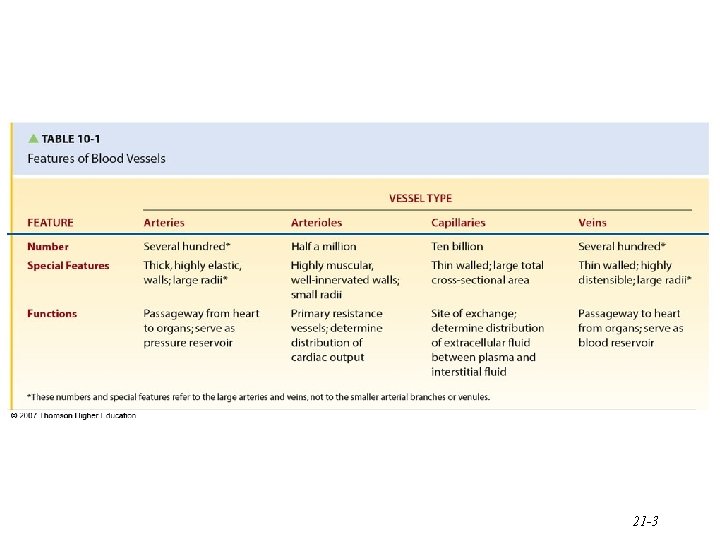
21 -3
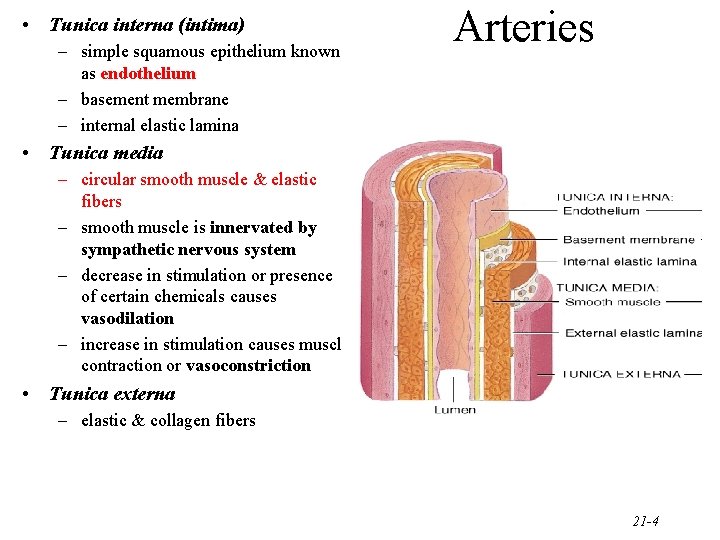
• Tunica interna (intima) – simple squamous epithelium known as endothelium – basement membrane – internal elastic lamina Arteries • Tunica media – circular smooth muscle & elastic fibers – smooth muscle is innervated by sympathetic nervous system – decrease in stimulation or presence of certain chemicals causes vasodilation – increase in stimulation causes muscle contraction or vasoconstriction • Tunica externa – elastic & collagen fibers 21 -4
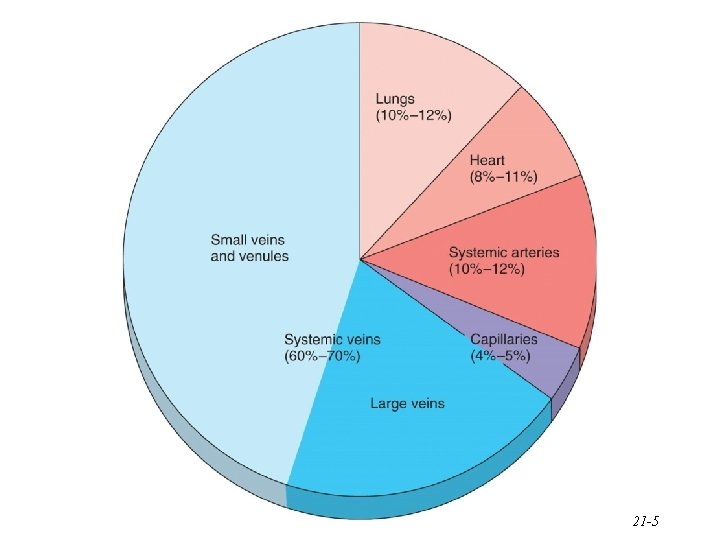
21 -5
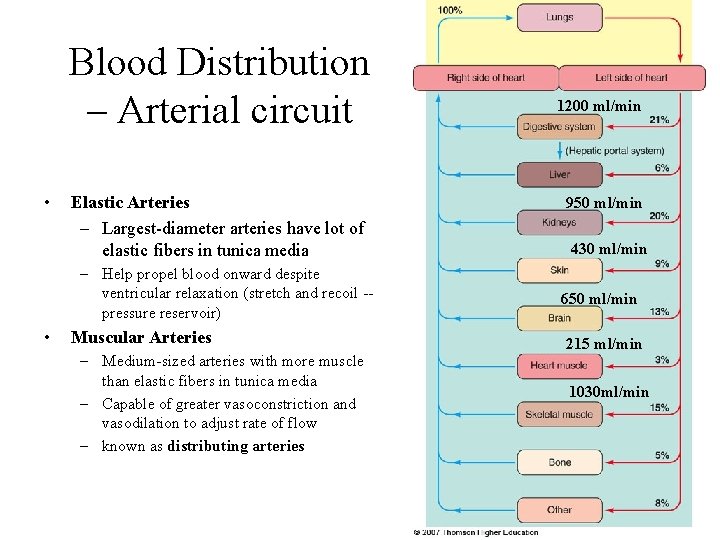
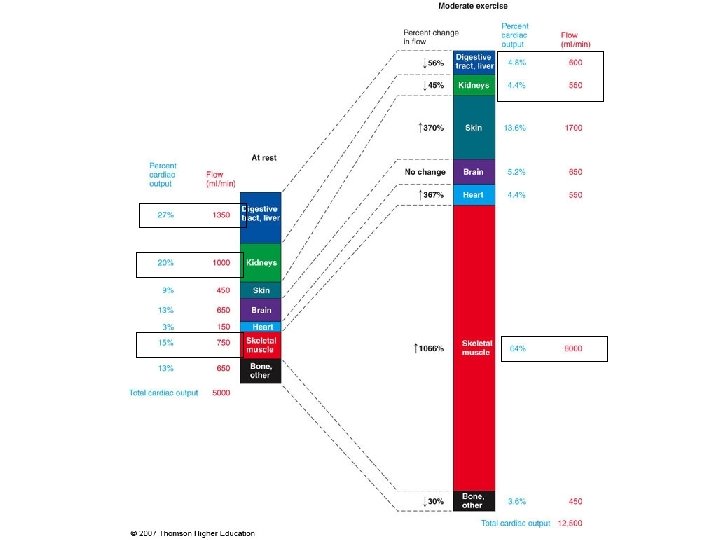
Blood Distribution – Arterial circuit • Elastic Arteries – Largest-diameter arteries have lot of elastic fibers in tunica media – Help propel blood onward despite ventricular relaxation (stretch and recoil -pressure reservoir) • Muscular Arteries – Medium-sized arteries with more muscle than elastic fibers in tunica media – Capable of greater vasoconstriction and vasodilation to adjust rate of flow – known as distributing arteries 1200 ml/min 950 ml/min 430 ml/min 650 ml/min 215 ml/min 1030 ml/min 21 -6
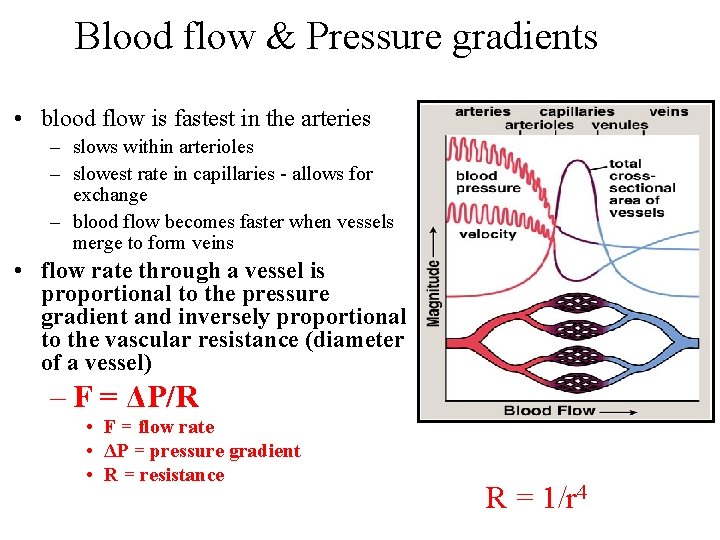
Blood flow & Pressure gradients • blood flow is fastest in the arteries – slows within arterioles – slowest rate in capillaries - allows for exchange – blood flow becomes faster when vessels merge to form veins • flow rate through a vessel is proportional to the pressure gradient and inversely proportional to the vascular resistance (diameter of a vessel) – F = ΔP/R • F = flow rate • ΔP = pressure gradient • R = resistance R = 1/r 4

Flow Rate & Pressure gradients • ΔP is the pressure gradient = difference in P between the beginning and end of a vessel – this is what determines flow rate – NOT the absolute pressure! – if there is no difference in the ΔP – i. e. no difference in pressure at the start of the vessel and at the end of the vessel – F will not change coming into and exiting the vessel F = ΔP/R constant R

Flow Rate & Vessel Resistance • if ΔP remains the same to change Flow rate you need to change the Resistance • R depends on one major factor: • vessel radius (r) – major determinant of R • R increases as r decreases – F will decrease (if ΔP stays the same) • R decreases as r increases – F will increase (if ΔP stays the same) – To overcome the effects of increased R - you have to increase ΔP (increase the pressure at the start of the vessel) if you want to maintain F constant ΔP
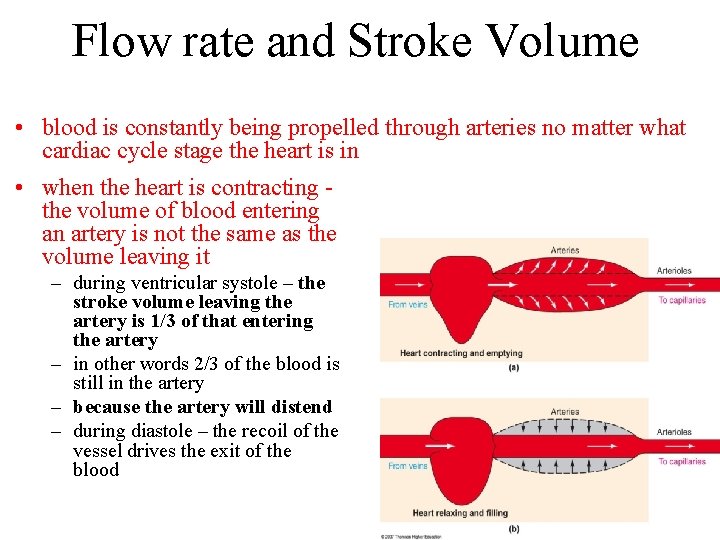
Flow rate and Stroke Volume • blood is constantly being propelled through arteries no matter what cardiac cycle stage the heart is in • when the heart is contracting the volume of blood entering an artery is not the same as the volume leaving it – during ventricular systole – the stroke volume leaving the artery is 1/3 of that entering the artery – in other words 2/3 of the blood is still in the artery – because the artery will distend – during diastole – the recoil of the vessel drives the exit of the blood 21 -10
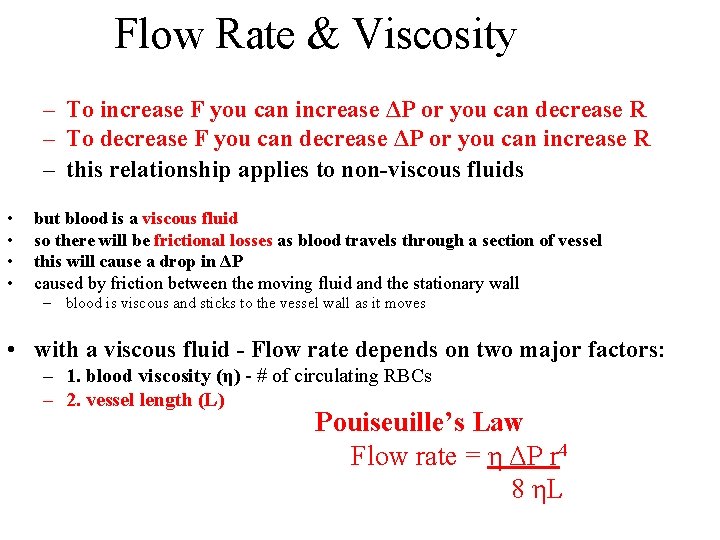
Flow Rate & Viscosity – To increase F you can increase ΔP or you can decrease R – To decrease F you can decrease ΔP or you can increase R – this relationship applies to non-viscous fluids • • but blood is a viscous fluid so there will be frictional losses as blood travels through a section of vessel this will cause a drop in ΔP caused by friction between the moving fluid and the stationary wall – blood is viscous and sticks to the vessel wall as it moves • with a viscous fluid - Flow rate depends on two major factors: – 1. blood viscosity (η) - # of circulating RBCs – 2. vessel length (L) Pouiseuille’s Law Flow rate = η ΔP r 4 8 ηL

Pouiseuille’s Law (Snooty French Guy Law) -true description of how blood flow through our vessels Flow rate = η ΔP r 4 8 ηL -notice that changing the viscosity (η) of the blood actually does NOT change the F value (go ahead try it!) -but changing the L value does -this is because thick, viscous blood “sticks” to the blood vessel wall -so the longer the vessel – the more sticking to the vessel occure and the slower the blood flows 21 -12
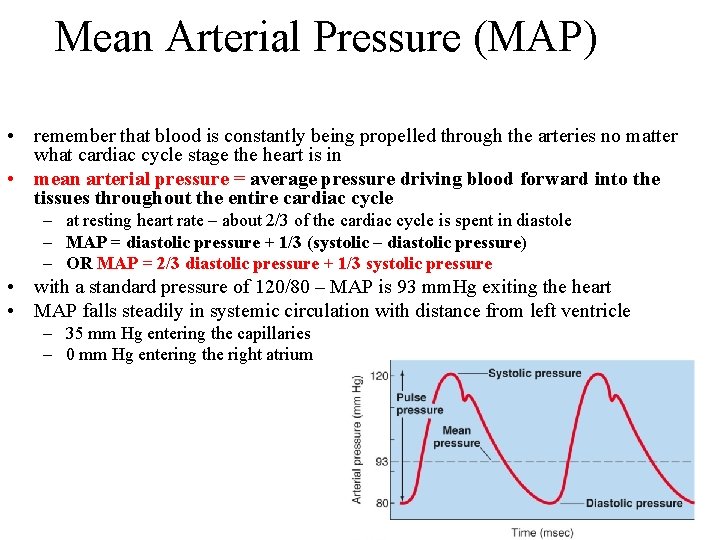
Mean Arterial Pressure (MAP) • remember that blood is constantly being propelled through the arteries no matter what cardiac cycle stage the heart is in • mean arterial pressure = average pressure driving blood forward into the tissues throughout the entire cardiac cycle – at resting heart rate – about 2/3 of the cardiac cycle is spent in diastole – MAP = diastolic pressure + 1/3 (systolic – diastolic pressure) – OR MAP = 2/3 diastolic pressure + 1/3 systolic pressure • with a standard pressure of 120/80 – MAP is 93 mm. Hg exiting the heart • MAP falls steadily in systemic circulation with distance from left ventricle – 35 mm Hg entering the capillaries – 0 mm Hg entering the right atrium
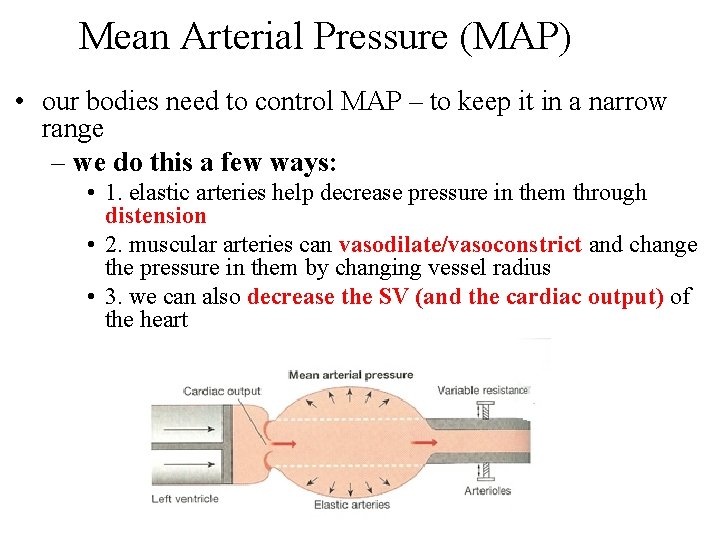
Mean Arterial Pressure (MAP) • our bodies need to control MAP – to keep it in a narrow range – we do this a few ways: • 1. elastic arteries help decrease pressure in them through distension • 2. muscular arteries can vasodilate/vasoconstrict and change the pressure in them by changing vessel radius • 3. we can also decrease the SV (and the cardiac output) of the heart

Mean Arterial Pressure (MAP) – F = ΔP/R applies to the entire circulatory system in addition to a single vessel – F = cardiac output – ΔP = MAP (ΔP = difference in pressure at the beginning of the systemic circulation and the end of the systemic circulation) – R = total peripheral resistance = total resistance offered by all systemic peripheral vessels – rearrange the equation - ΔP = F X R – OR – MAP = CO X TPR (total peripheral resistance) 21 -15
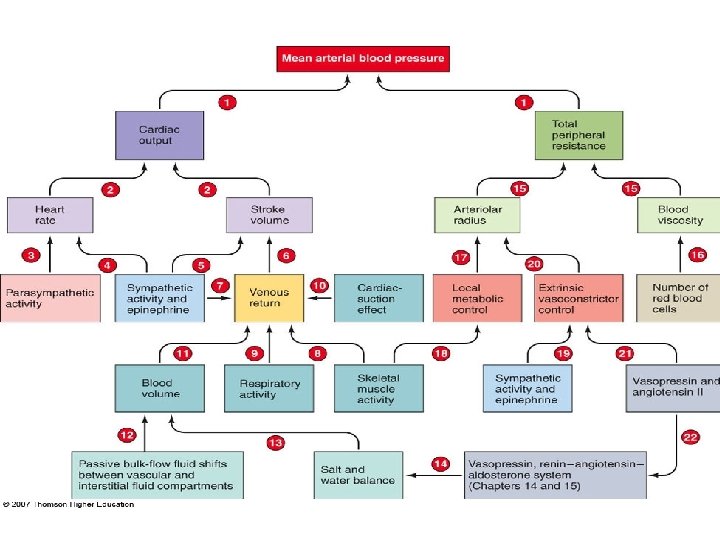
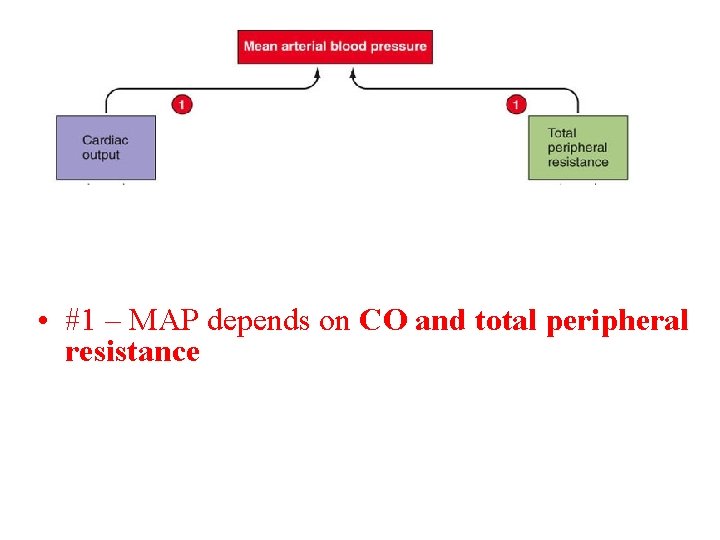
• #1 – MAP depends on CO and total peripheral resistance
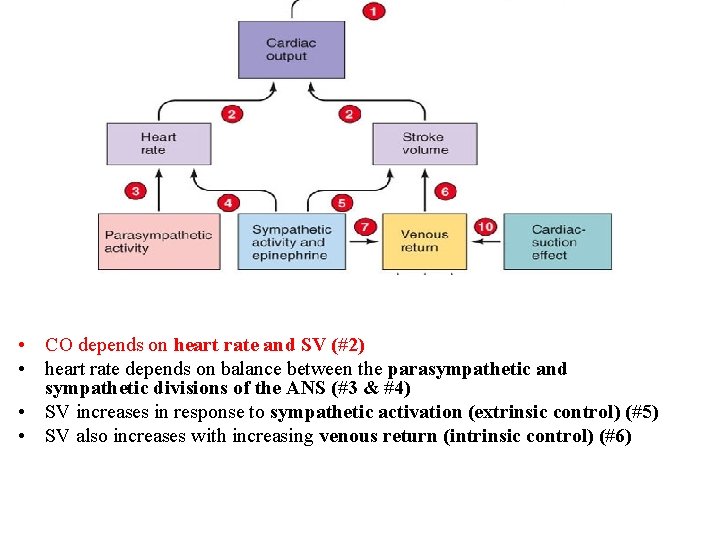
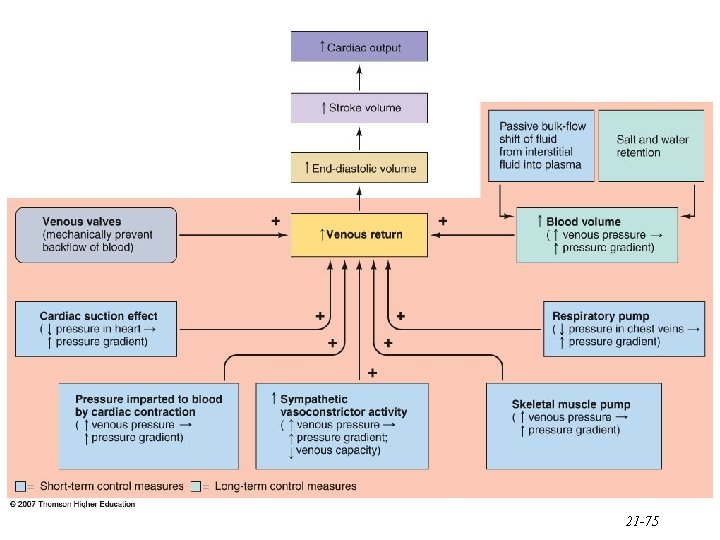
• CO depends on heart rate and SV (#2) • heart rate depends on balance between the parasympathetic and sympathetic divisions of the ANS (#3 & #4) • SV increases in response to sympathetic activation (extrinsic control) (#5) • SV also increases with increasing venous return (intrinsic control) (#6)
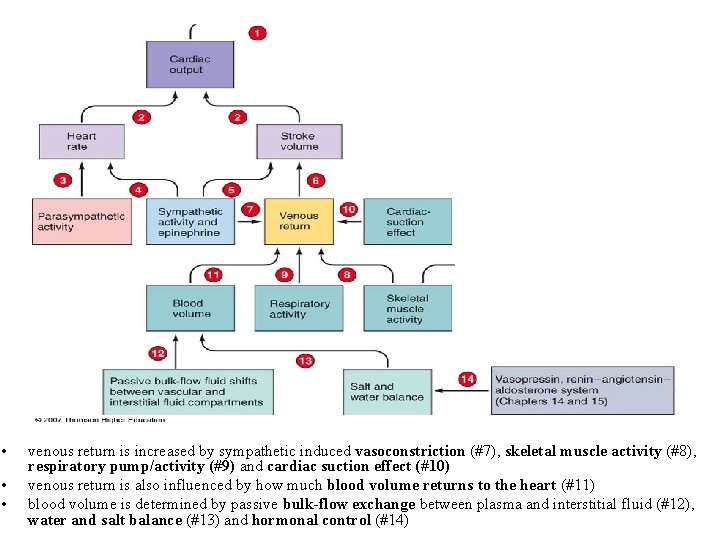
• • • venous return is increased by sympathetic induced vasoconstriction (#7), skeletal muscle activity (#8), respiratory pump/activity (#9) and cardiac suction effect (#10) venous return is also influenced by how much blood volume returns to the heart (#11) blood volume is determined by passive bulk-flow exchange between plasma and interstitial fluid (#12), water and salt balance (#13) and hormonal control (#14)
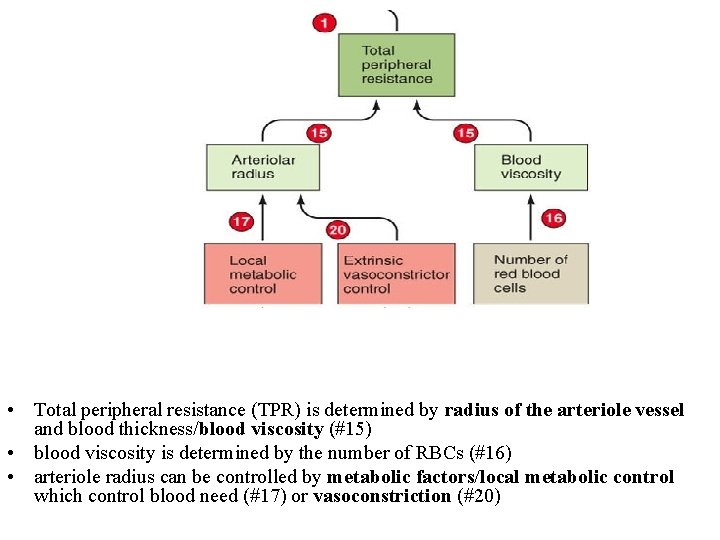
• Total peripheral resistance (TPR) is determined by radius of the arteriole vessel and blood thickness/blood viscosity (#15) • blood viscosity is determined by the number of RBCs (#16) • arteriole radius can be controlled by metabolic factors/local metabolic control which control blood need (#17) or vasoconstriction (#20)
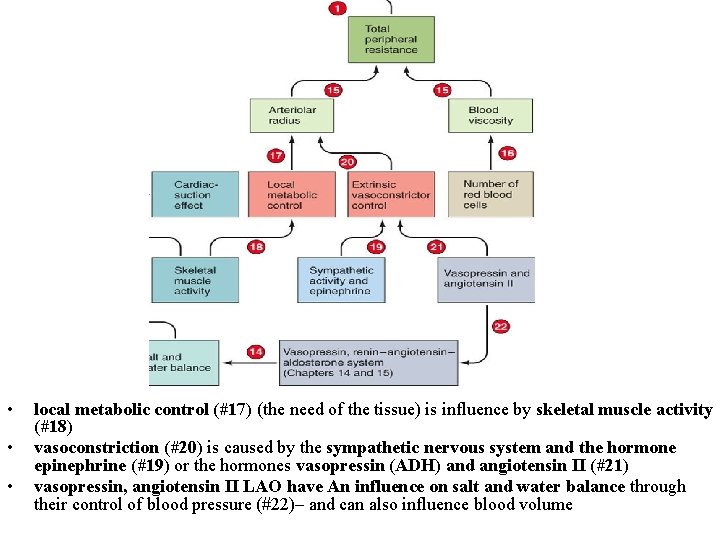
• • • local metabolic control (#17) (the need of the tissue) is influence by skeletal muscle activity (#18) vasoconstriction (#20) is caused by the sympathetic nervous system and the hormone epinephrine (#19) or the hormones vasopressin (ADH) and angiotensin II (#21) vasopressin, angiotensin II LAO have An influence on salt and water balance through their control of blood pressure (#22)– and can also influence blood volume
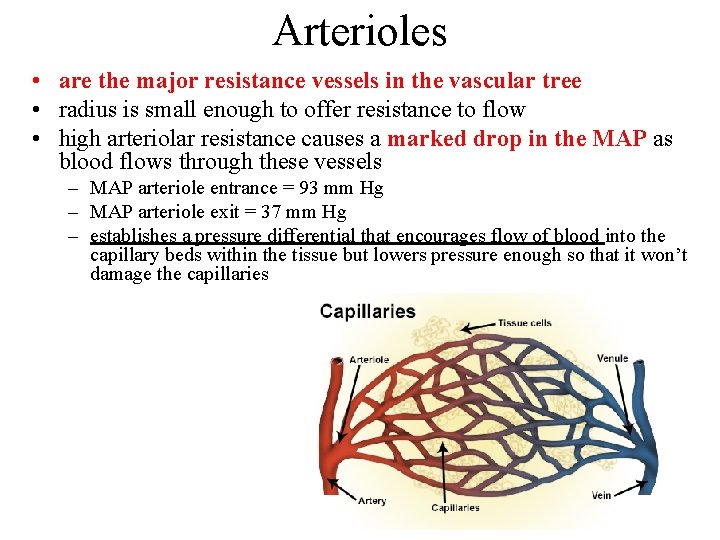
Arterioles • are the major resistance vessels in the vascular tree • radius is small enough to offer resistance to flow • high arteriolar resistance causes a marked drop in the MAP as blood flows through these vessels – MAP arteriole entrance = 93 mm Hg – MAP arteriole exit = 37 mm Hg – establishes a pressure differential that encourages flow of blood into the capillary beds within the tissue but lowers pressure enough so that it won’t damage the capillaries
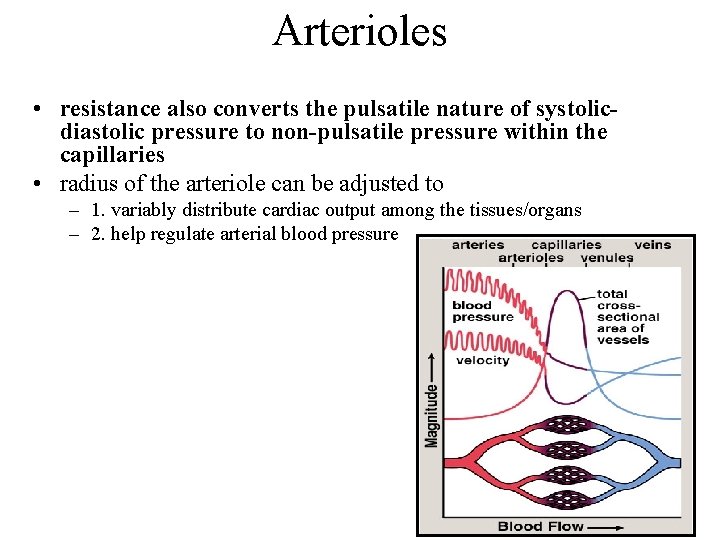
Arterioles • resistance also converts the pulsatile nature of systolicdiastolic pressure to non-pulsatile pressure within the capillaries • radius of the arteriole can be adjusted to – 1. variably distribute cardiac output among the tissues/organs – 2. help regulate arterial blood pressure
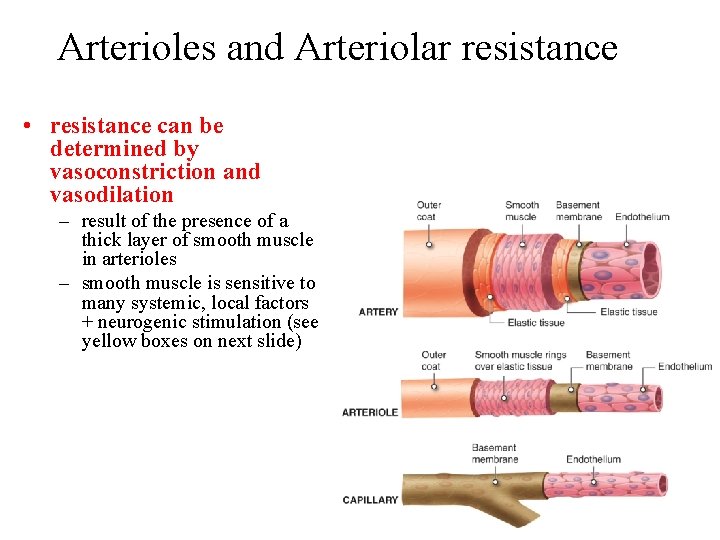
Arterioles and Arteriolar resistance • resistance can be determined by vasoconstriction and vasodilation – result of the presence of a thick layer of smooth muscle in arterioles – smooth muscle is sensitive to many systemic, local factors + neurogenic stimulation (see yellow boxes on next slide)
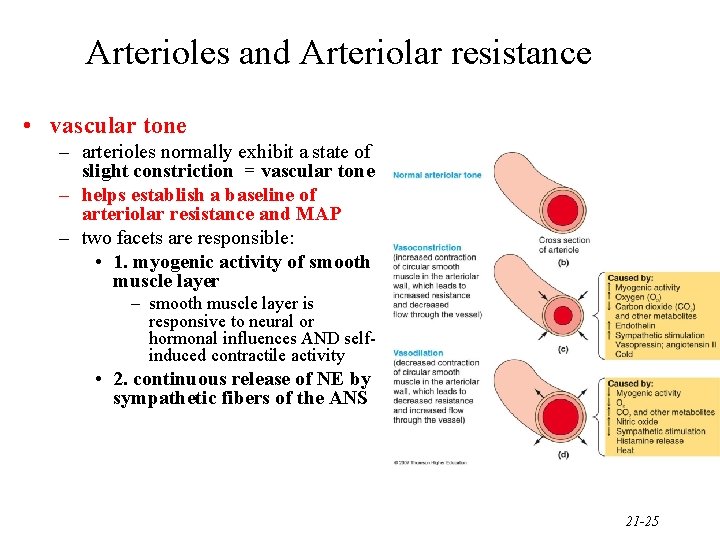
Arterioles and Arteriolar resistance • vascular tone – arterioles normally exhibit a state of slight constriction = vascular tone – helps establish a baseline of arteriolar resistance and MAP – two facets are responsible: • 1. myogenic activity of smooth muscle layer – smooth muscle layer is responsive to neural or hormonal influences AND selfinduced contractile activity • 2. continuous release of NE by sympathetic fibers of the ANS 21 -25

Arteriolar diameter • Local (or intrinsic) changes – at the tissue, organ specific – 1. local chemical factors • metabolic factors • vasoactive mediators – 2. histamine – 3. local physical factors • hot/cold • passive stretch of arteriole • shear stress within arteriole • Extrinsic factors – 1. sympathetic nervous system – 2. hormones

#1 - Local Chemical Changes: Metabolic Factors • the most important local chemical influences on arteriolar smooth muscle are local changes in metabolism within that organ • local metabolic changes can affect the diameter of an arteriole without neural influence • active hyperemia = local arteriolar vasodilation that increases blood flow into an organ – arterioles are found within an organ and can be directly affected by that organ – during increased metabolism (e. g. increased skeletal muscle contraction) local concentrations of chemicals change within the organ • e. g. local concentrations of oxygen decrease as the organs begins to increase its metabolic use of glucose – this can result in vasodilation 21 -27

Local Chemical Changes: Metabolic Factors • local metabolic factors – – decreased/increased oxygen = vasodilation/vasoconstriction increase carbon dioxide = vasodilation increased carbonic acid= vasodilation increased K+ - repeated APs that outpace the Na/K pump’s ability to correct ionic changes = vasodilation – increased osmolarity – concentration of solutes accumulates in actively metabolic cells = vasodilation – adenosine release – cardiac muscle – release in response to increased metabolic activity = vasodilation – prostaglandin release = vasodilation • relative concentration of these factors can determine the state of arteriolar muscle tone • local metabolic factors cause vasodilation/vasoconstriction through the production of vasoactive mediators 21 -28

Local Metabolic Factors Act through Vasoactive Mediators • these local chemical changes do not act directly on smooth muscle but act on the endothelial cells • Endothelial cells – simple squamous epithelia cells – found lining the inside of the arteriole and capillary • in response to local metabolic changes - ECs release chemical factors called vasoactive mediators – e. g. endothelin = vasoconstriction – e. g. nitric oxide = vasodilation by relaxing arteriolar smooth muscle • inhibits entrance of calcium into the smooth muscle which inhibits the opening of the foot proteins on the sarcoplasmic reticulum

#2 – Local Changes: Histamine • • NOT released by metabolic changes NOT produce by endothelial cells only released upon pathology released by connective tissue cells within the organ or by circulating white blood cells (mast cells, basophils) • usually released in response to organ damage • causes vasodilation to increase blood flow and speed healing

#3 - Local Changes: Local Physical factors • application of heat or cold – heat causes localized arteriolar vasodilation • increases blood flow – cold – induces vasoconstriction • shear stress – blood flowing over the endothelial lining creates friction = shear stress – increase in shear stress can cause increased release of NO from the endothelial cells – promotes vasodilation – increased blood flow now reduces shear stress

#3 - Local Changes: Local Physical factors • myogenic response to stretch – increased MAP drives more blood into the arteriole which pushes out against the vessel wall = passive stretch – SO extent of passive stretch is related to the volume of blood through the vessel • leads to vasoconstriction to reduce this blood volume • arteriolar smooth muscle responds to passive stretch by increasing its tone through vasoconstriction – arterial occlusion can block blood flow and reduce myogenic stretch since the arterioles will dilate in response • called reactive hyperemia Incr. MAP

Extrinsic control over arteriolar diameter • extrinsic control includes both neural and hormonal control • sympathetic division innervates arteriolar smooth muscle everywhere except the brain • NO parasympathetic innervation of arteriolar smooth muscle! – exception – clitoris and penis • sympathetic activity contributes to arteriolar vascular tone – through production of norepinephrine (vasoconstrictor) – epinephrine made by the adrenal gland is a vasodilator! • BUT increased sympathetic activity to certain arterioles (heart and muscle) can induce vasodilation drops arteriolar resistance (TPR) and changes MAP • main area of the brain to adjust sympathetic output = cardiovascular control center • other brain regions involved – hypothalamus

Hormonal control: Epinephrine and Norepinephrine • • Epinephrine and Norepinephrine are released from the adrenal medulla (sympathetic activity) only NE is released from neurons (sympathetic activity) – NE binds to a 1 -adrenergic receptors on ALL arteriolar smooth muscle to increase vasoconstriction • secreted normally at a low level in your body & results in vascular tone • Epi can bind these receptors also – less affinity – Epi binds to b 2 -adrenergic receptors in smooth muscle in heart and muscle arterioles to cause vasodilation • cerebral arterioles do NOT have a 1 -adrenergic receptors !!! -influenced entirely by local physical and chemical changes (intrinsic changes)

Hormonal control: Epinephrine and Norepinephrine • during the “flight or fight” response - Epi is more abundant and has more affinity for their b 2 -adrenergic receptors which are expressed in large amounts on arteriolar smooth muscle supplying skeletal and cardiac muscle • so overall effect is of Epi vasodilation to heart and skeletal muscles Epi and NE can cause vasoconstriction or vasodilation!!! depends on receptor and its location FIGHT Or FLIGHT 21 -35

Hormonal control: Angiotensin II and Vasopressin • angiotensin II – converted from angiotensin I by the enzyme ACE (produced in the lungs) – regulates body’s salt balance – causes the release of aldosterone from the adrenal cortex – increased salt reabsorption – powerful vasoconstrictor • vasopressin (ADH) – released from the posterior pituitary in response to changes in water volume – drop in water content, release of vasopressin, decreased urine volume, increased water retention – also constriction of peripheral vessels = vasoconstrictor – plays a role in reducing hemorrhage
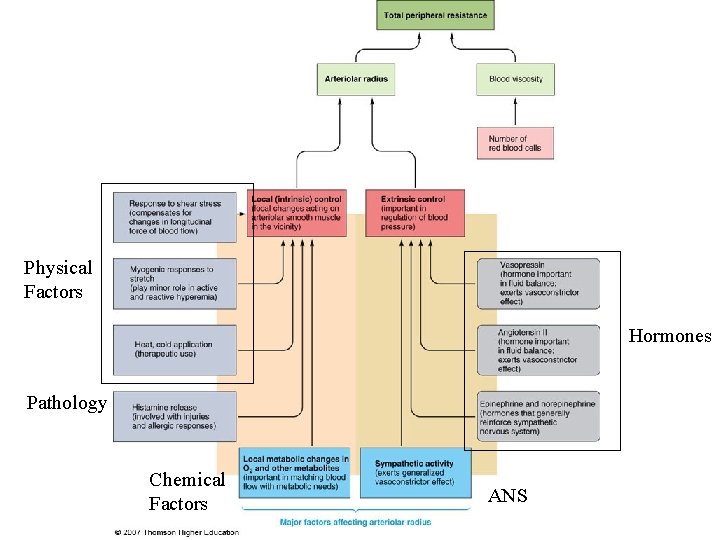
Physical Factors Hormones Pathology Chemical Factors ANS

• the sympathetic nervous system essentially maintains an appropriate driving pressure to each organ (i. e. MAP) but the organ itself controls the amount of blood that actually enters it. • NE/sympathetic control over arteriolar vascular tone slightly constricts most arterioles to ensure adequate MAP throughout the systemic circuit • BUT the organ can override the sympathetic control using local arteriolar control mechanisms – analogy = water pressure in pipes
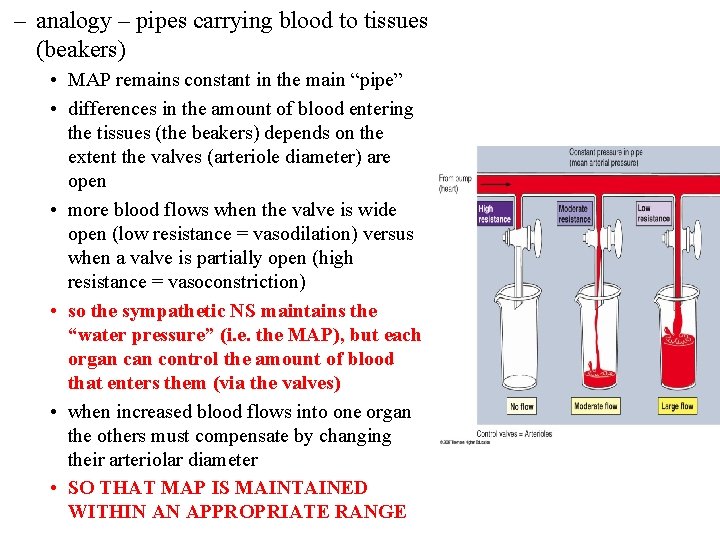
– analogy – pipes carrying blood to tissues (beakers) • MAP remains constant in the main “pipe” • differences in the amount of blood entering the tissues (the beakers) depends on the extent the valves (arteriole diameter) are open • more blood flows when the valve is wide open (low resistance = vasodilation) versus when a valve is partially open (high resistance = vasoconstriction) • so the sympathetic NS maintains the “water pressure” (i. e. the MAP), but each organ control the amount of blood that enters them (via the valves) • when increased blood flows into one organ the others must compensate by changing their arteriolar diameter • SO THAT MAP IS MAINTAINED WITHIN AN APPROPRIATE RANGE
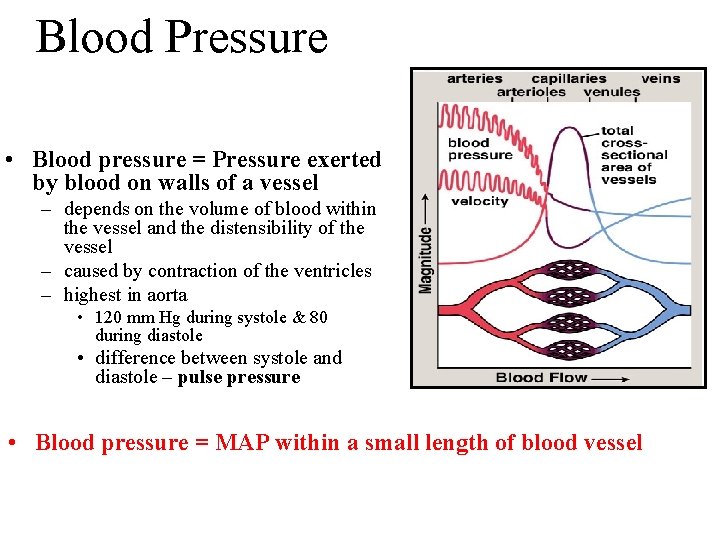
Blood Pressure • Blood pressure = Pressure exerted by blood on walls of a vessel – depends on the volume of blood within the vessel and the distensibility of the vessel – caused by contraction of the ventricles – highest in aorta • 120 mm Hg during systole & 80 during diastole • difference between systole and diastole – pulse pressure • Blood pressure = MAP within a small length of blood vessel

Evaluating Blood Pressure • Pulse is a pressure wave – alternate expansion & recoil of elastic artery after each systole of the left ventricle – pulse rate is normally between 70 -80 beats/min • tachycardia is rate over 100 beats/min/bradycardia under 60 • Measuring blood pressure with sphygmomanometer – Korotkoff sounds are heard while taking pressure – systolic blood pressure from ventricular contraction – diastolic blood pressure during ventricular contraction • provides information about systemic vascular resistance – pulse pressure is difference between systolic & diastolic – normal ratio is 3: 2: 1 -- systolic/diastolic/pulse pressure 21 -42
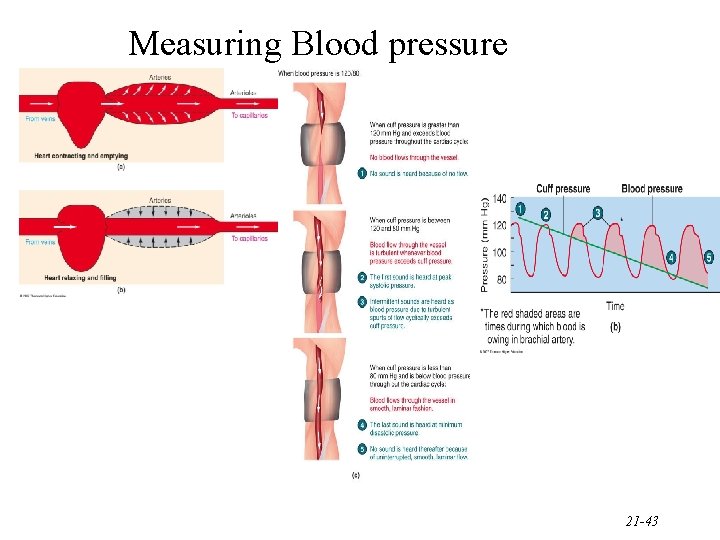
Measuring Blood pressure 21 -43
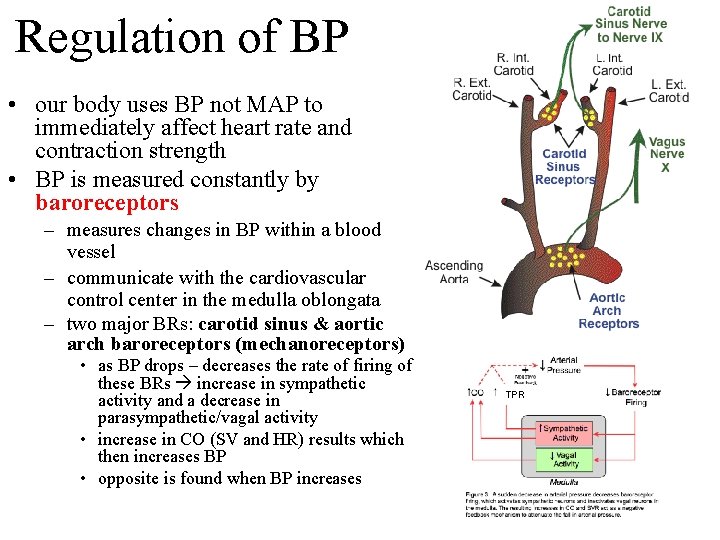
Regulation of BP • our body uses BP not MAP to immediately affect heart rate and contraction strength • BP is measured constantly by baroreceptors – measures changes in BP within a blood vessel – communicate with the cardiovascular control center in the medulla oblongata – two major BRs: carotid sinus & aortic arch baroreceptors (mechanoreceptors) • as BP drops – decreases the rate of firing of these BRs increase in sympathetic activity and a decrease in parasympathetic/vagal activity • increase in CO (SV and HR) results which then increases BP • opposite is found when BP increases TPR

Regulation of BP • Proprioceptors – physical activity increases BP via increased sympathetic activity and decreased parasympathetic activity • Central Chemoreceptors – central = in the medulla oblongata – monitor the p. H of the CSF – peripheral chemoreceptors= out in the body - located in the carotid and aortic arteries – monitor p. H of blood, the p. O 2 and p. CO 2 of blood as well – also have an effect on respiratory function – both types increase BP via increased sympathetic activity and decreased parasympathetic activity

Regulation of BP • Hypothalamus – osmoreceptors control salt and water balance and therefore longterm regulation of BP via determining blood volume – also controls arteriole responses in fight or flight response, sexual orgasm, blushing – controls cutaneous arterioles for temperature regulation • this supercedes the cardiovascular center’s control over these vessels for regulating BP • therefore BP can fall dramatically as arteries dilate to allow cooling • Higher brain centers such as cerebral cortex & limbic system – anticipation of competition
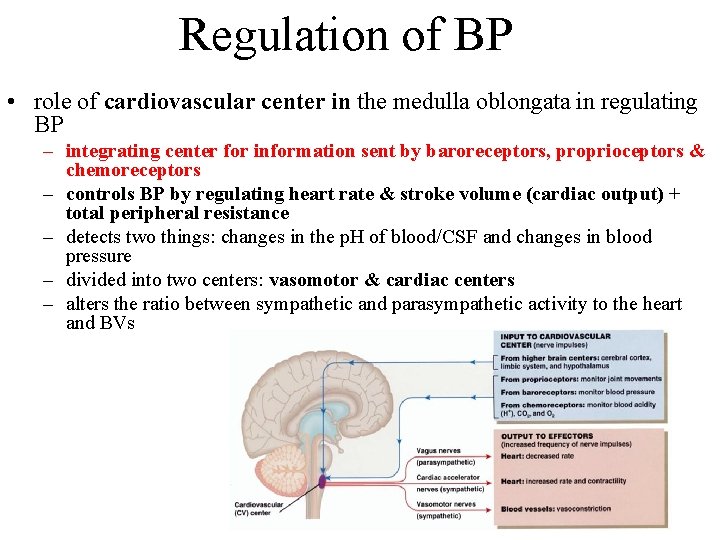
Regulation of BP • role of cardiovascular center in the medulla oblongata in regulating BP – integrating center for information sent by baroreceptors, proprioceptors & chemoreceptors – controls BP by regulating heart rate & stroke volume (cardiac output) + total peripheral resistance – detects two things: changes in the p. H of blood/CSF and changes in blood pressure – divided into two centers: vasomotor & cardiac centers – alters the ratio between sympathetic and parasympathetic activity to the heart and BVs
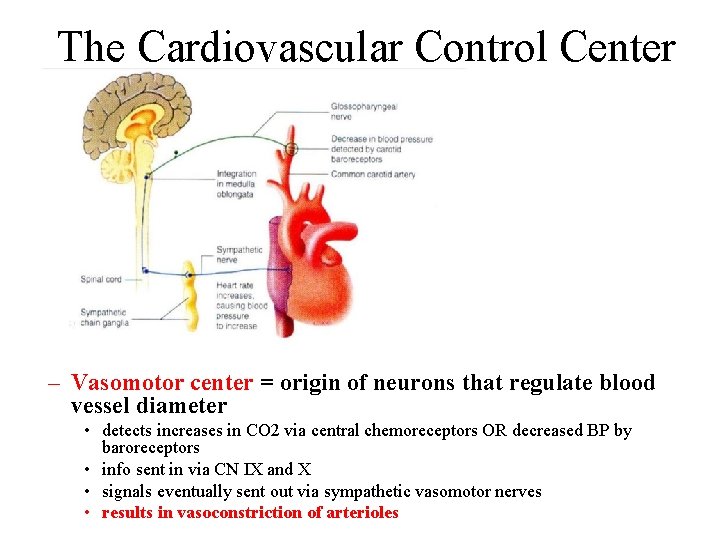
The Cardiovascular Control Center – Vasomotor center = origin of neurons that regulate blood vessel diameter • detects increases in CO 2 via central chemoreceptors OR decreased BP by baroreceptors • info sent in via CN IX and X • signals eventually sent out via sympathetic vasomotor nerves • results in vasoconstriction of arterioles
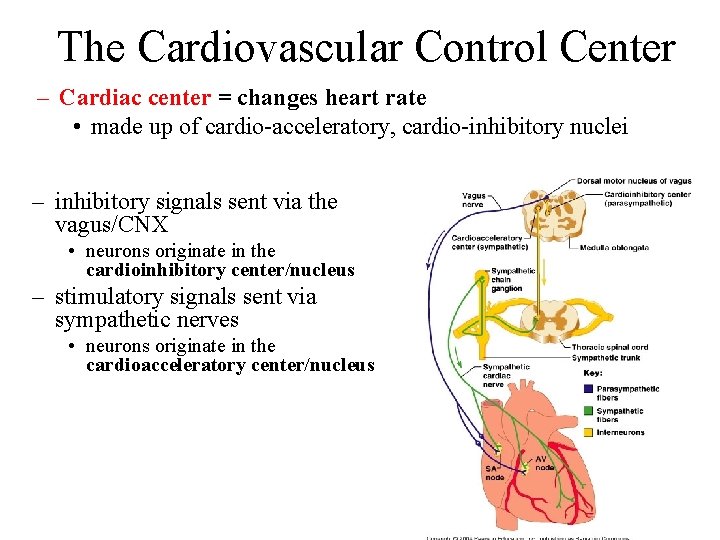
The Cardiovascular Control Center – Cardiac center = changes heart rate • made up of cardio-acceleratory, cardio-inhibitory nuclei – inhibitory signals sent via the vagus/CNX • neurons originate in the cardioinhibitory center/nucleus – stimulatory signals sent via sympathetic nerves • neurons originate in the cardioacceleratory center/nucleus
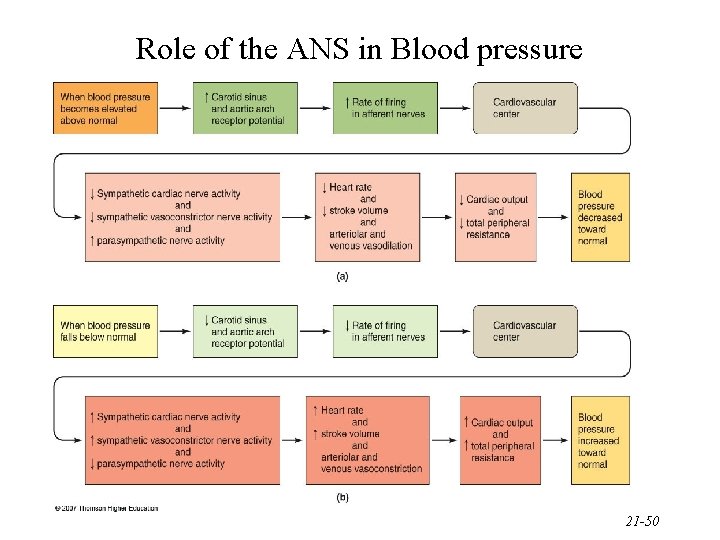
Role of the ANS in Blood pressure 21 -50

Medical application: Hypertension • primary and secondary hypertension • primary hypertension: caused by a variety of reasons – defects in salt management by kidneys – accumulation of salt and water in blood – excessive salt intake – salt osmotically retains water and expands plasma volume – diets low in fruits, vegetables and dairy products – low K+ and Ca+ • K+ from fruits and vegetables may relax artery walls • role of calcium is still unclear • secondary hypertension: occurs secondary to another disorder – 1. renal hypertension – artherosclerotic lesions in the renal artery or other disruptions to the flow of blood into the kidney • • kidney responds by releasing renin – initiates the renin-angiotensin II-aldosterone pathway increased salt and water retention increases blood volume – increases BP angiotensin II is also a powerful vasoconstrictor – 2. endocrine hypertension • tumors of the adrenal glands can cause excessive secretion of epinephrine and NE – increase cardiac output – 3. neurogenic hypertension • erroneous neural control 21 -51
Capillaries • Microscopic vessels that connect arterioles to venules • Found near every cell in the body but more extensive in highly active tissue (muscles, liver, kidneys & brain) – entire capillary bed fills with blood when tissue is active – lacking in epithelia, cornea and lens of eye & cartilage • Function is exchange of nutrients & wastes between blood and tissue fluid • Structure is single layer of simple squamous epithelium and its basement membrane 21 -52
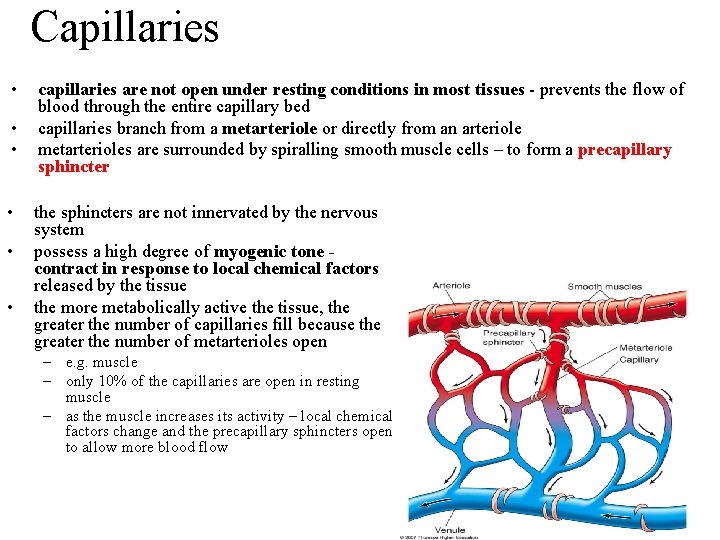
Capillaries • • • capillaries are not open under resting conditions in most tissues - prevents the flow of blood through the entire capillary bed capillaries branch from a metarteriole or directly from an arteriole metarterioles are surrounded by spiralling smooth muscle cells – to form a precapillary sphincter the sphincters are not innervated by the nervous system possess a high degree of myogenic tone contract in response to local chemical factors released by the tissue the more metabolically active the tissue, the greater the number of capillaries fill because the greater the number of metarterioles open – e. g. muscle – only 10% of the capillaries are open in resting muscle – as the muscle increases its activity – local chemical factors change and the precapillary sphincters open to allow more blood flow 21 -53
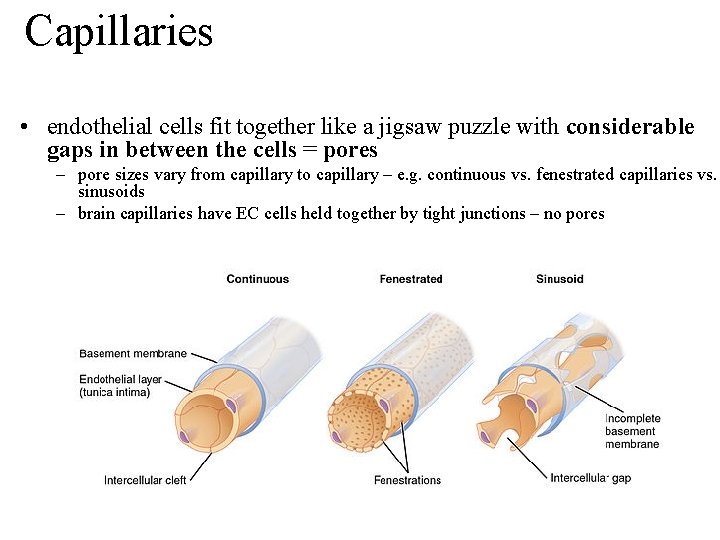
Capillaries • endothelial cells fit together like a jigsaw puzzle with considerable gaps in between the cells = pores – pore sizes vary from capillary to capillary – e. g. continuous vs. fenestrated capillaries vs. sinusoids – brain capillaries have EC cells held together by tight junctions – no pores
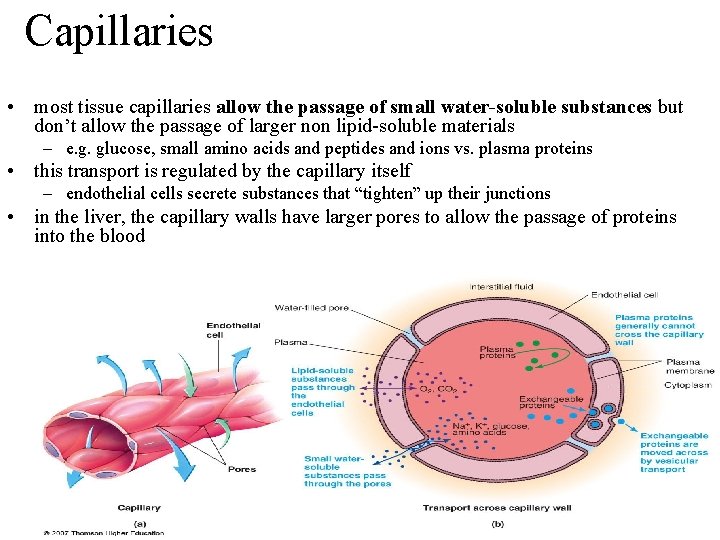
Capillaries • most tissue capillaries allow the passage of small water-soluble substances but don’t allow the passage of larger non lipid-soluble materials – e. g. glucose, small amino acids and peptides and ions vs. plasma proteins • this transport is regulated by the capillary itself – endothelial cells secrete substances that “tighten” up their junctions • in the liver, the capillary walls have larger pores to allow the passage of proteins into the blood 21 -55
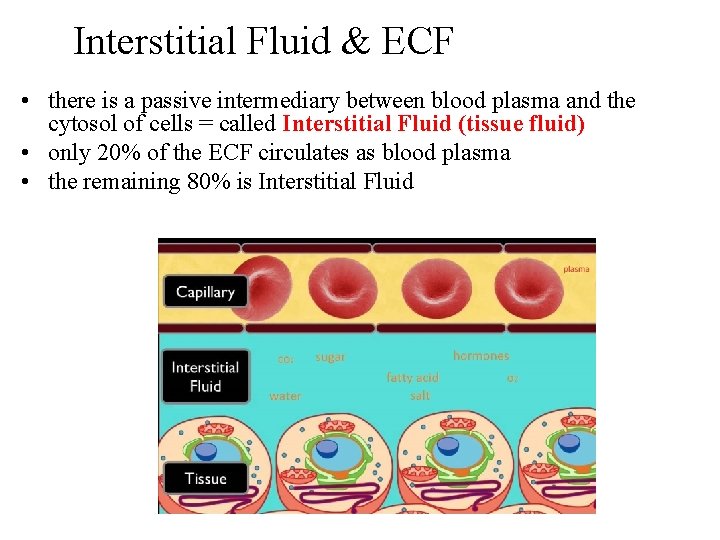
Interstitial Fluid & ECF • there is a passive intermediary between blood plasma and the cytosol of cells = called Interstitial Fluid (tissue fluid) • only 20% of the ECF circulates as blood plasma • the remaining 80% is Interstitial Fluid
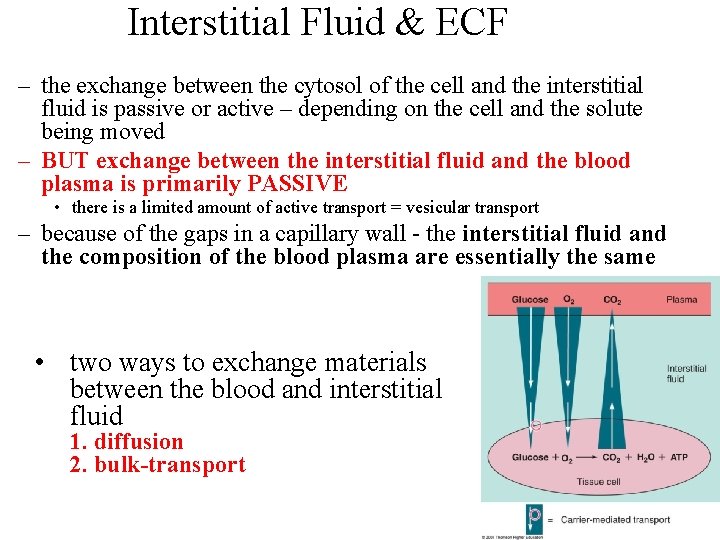
Interstitial Fluid & ECF – the exchange between the cytosol of the cell and the interstitial fluid is passive or active – depending on the cell and the solute being moved – BUT exchange between the interstitial fluid and the blood plasma is primarily PASSIVE • there is a limited amount of active transport = vesicular transport – because of the gaps in a capillary wall - the interstitial fluid and the composition of the blood plasma are essentially the same • two ways to exchange materials between the blood and interstitial fluid 1. diffusion 2. bulk-transport 21 -57

Diffusion • the movement of individual solutes between blood plasma and interstitial fluid – e. g. O 2, CO 2 • diffusion is promoted by several factors: – 1. short distance of travel • 1. thinness of the capillary wall – 1 um in thickness (simple squamous epithelium + basement membrane) • 2. narrowness of the capillary – thinner than the RBC so the cells must pass through one at a time • 3. proximity to cells – every cell is approximately 0. 01 cm from a capillary – 2. total surface area – 10 to 40 billion capillaries available for exchange • produces a tremendous surface area for exchange = 600 m 2
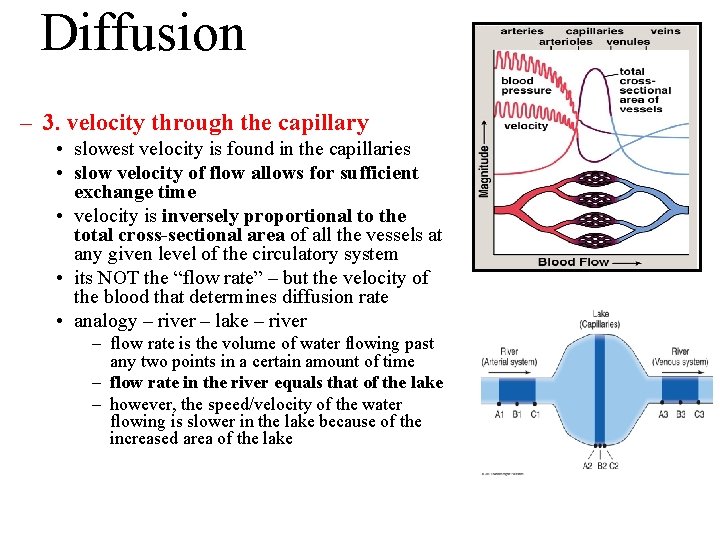
Diffusion – 3. velocity through the capillary • slowest velocity is found in the capillaries • slow velocity of flow allows for sufficient exchange time • velocity is inversely proportional to the total cross-sectional area of all the vessels at any given level of the circulatory system • its NOT the “flow rate” – but the velocity of the blood that determines diffusion rate • analogy – river – lake – river – flow rate is the volume of water flowing past any two points in a certain amount of time – flow rate in the river equals that of the lake – however, the speed/velocity of the water flowing is slower in the lake because of the increased area of the lake
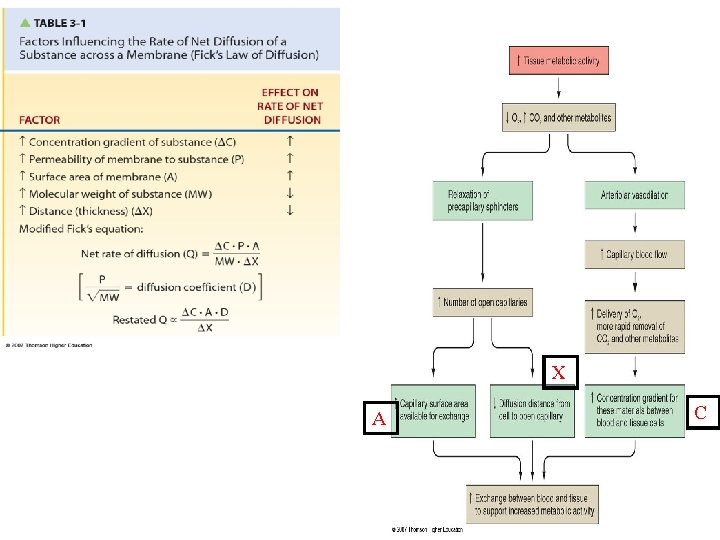
X A C

Bulk-flow • occurs when a volume of protein-free plasma filters out of the capillary and mixes with the surrounding interstitial fluid and then is reabsorbed = bulk flow • bulk flow: movement of plasma into the interstitial fluid – the various components are moved in bulk in contrast to the movement of individual components as seen in diffusion • determines the composition of interstitial fluid of your tissues • Net exchange pressure = (Pc + πIF) – (πP + PIF)

Bulk-flow: The Important Factors • factors affecting bulk flow – 1. Pc = capillary blood pressure • fluid or hydrostatic pressure exerted on the inside of the capillary wall by blood • “outward” force - tends to force fluid OUT of the capillaries into the interstitial fluid – 2. πP = plasma osmotic pressure (oncotic pressure) • osmotic pressure encourages inward movement of fluid into the blood plasma • “inward” force • doesn’t change over the length of the vessel

Bulk-flow: The “Not” Important Factors • factors affecting bulk flow – 3. PIF = interstitial fluid hydrostatic pressure • fluid pressure exerted on the outside of the capillary wall by interstitial fluid • “inward” force – 4. πIF = interstitial fluid-colloid osmotic pressure (πIF is close to zero) • does not normally contribute significantly to bulk flow • caused by the osmotic pressure of proteins in the interstitial fluid • “outward” force • these values “normally” do not change and are negligible
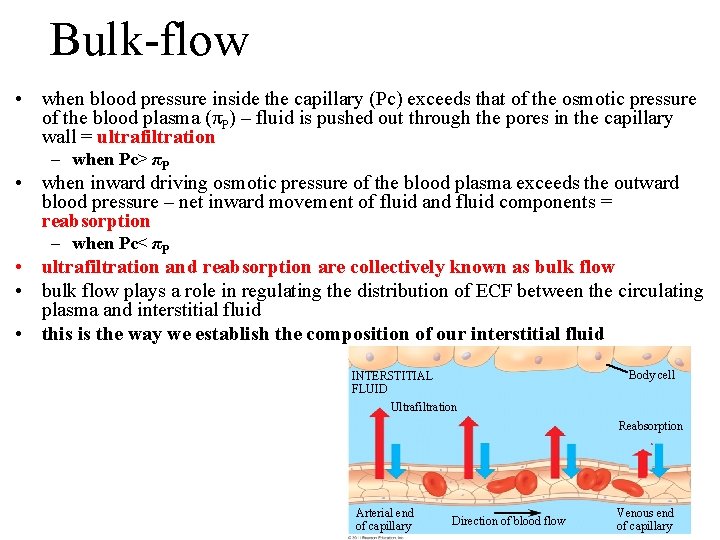
Bulk-flow • when blood pressure inside the capillary (Pc) exceeds that of the osmotic pressure of the blood plasma (πP) – fluid is pushed out through the pores in the capillary wall = ultrafiltration – when Pc> πP • when inward driving osmotic pressure of the blood plasma exceeds the outward blood pressure – net inward movement of fluid and fluid components = reabsorption – when Pc< πP • ultrafiltration and reabsorption are collectively known as bulk flow • bulk flow plays a role in regulating the distribution of ECF between the circulating plasma and interstitial fluid • this is the way we establish the composition of our interstitial fluid Body cell INTERSTITIAL FLUID Ultrafiltration Reabsorption Arterial end of capillary Direction of blood flow Venous end of 21 -64 capillary

Bulk-flow • as blood flows into the capillary – the blood pressure/Pc is greater than osmotic pressure/OP of the blood plasma (πP) and more blood plasma moves out into the interstitial fluid then moves back in • as blood continues to move along the capillary – Pc drops • at the venule end of the capillary – Pc has dropped enough so that plasma OP (πP) is now greater than Pc and more blood moves back into the plasma than is pushed out INTERSTITIAL FLUID Body cell Bulk Flow = Ultrafiltration – Reabsorption Ultrafiltration • Ultrafiltration is driven by blood pressure (Pc) • Reabsorption is driven by OP (πP) Reabsorption Arterial end of capillary Direction of blood flow Venous end of capillary
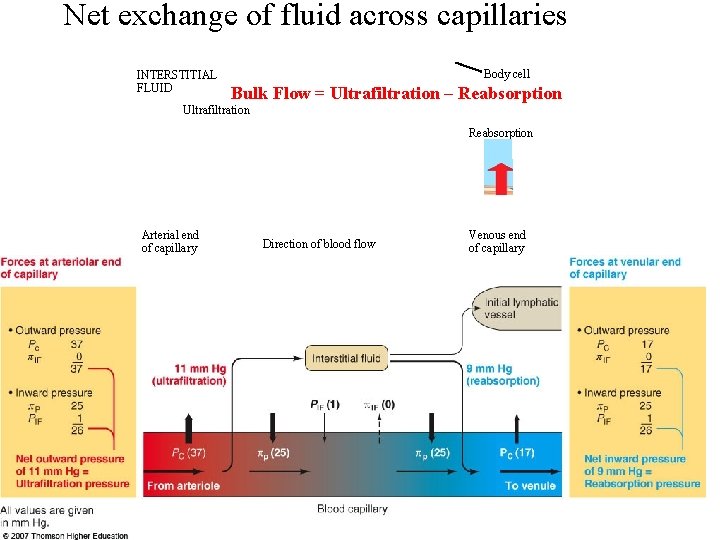
Net exchange of fluid across capillaries INTERSTITIAL FLUID Body cell Bulk Flow = Ultrafiltration – Reabsorption Ultrafiltration Reabsorption Arterial end of capillary Direction of blood flow Venous end of capillary 21 -66
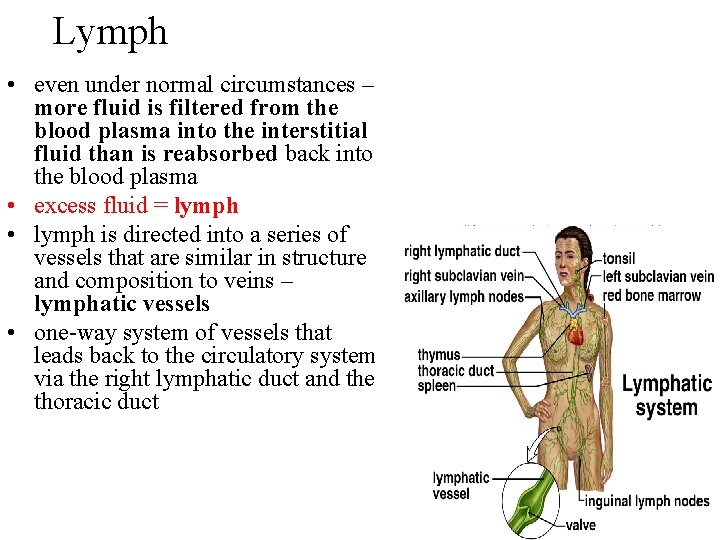
Lymph • even under normal circumstances – more fluid is filtered from the blood plasma into the interstitial fluid than is reabsorbed back into the blood plasma • excess fluid = lymph • lymph is directed into a series of vessels that are similar in structure and composition to veins – lymphatic vessels • one-way system of vessels that leads back to the circulatory system via the right lymphatic duct and the thoracic duct 21 -67
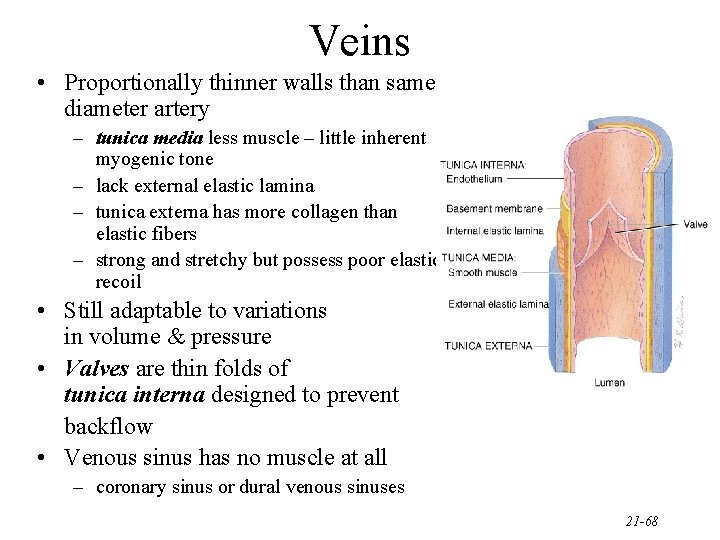
Veins • Proportionally thinner walls than same diameter artery – tunica media less muscle – little inherent myogenic tone – lack external elastic lamina – tunica externa has more collagen than elastic fibers – strong and stretchy but possess poor elastic recoil • Still adaptable to variations in volume & pressure • Valves are thin folds of tunica interna designed to prevent backflow • Venous sinus has no muscle at all – coronary sinus or dural venous sinuses 21 -68

Blood Distribution • 60% of blood volume at rest is in systemic veins and venules – veins function as blood reservoir – venous capacity = volume of blood the veins can accommodate – body at rest – many capillary beds are closed; much of the blood enters the veins – blood stretches the walls of the distensible veins and allows more blood into these vessels – but the blood moves slower in veins vs. arteries – lower pressure circuit – blood is diverted from the veins in times of need • increased muscular activity produces venoconstriction • hemorrhage causes venoconstriction to help maintain blood pressure 21 -69

Venous Return • veins & venules have little tone and resistance • the arteriole communicates chemically with the venule to ensure that inflow and outflow surrounding the capillary region matches 21 -70

Venous Return • venous return: volume of blood entering the right atria from veins – much of the driving force on the blood (blood pressure) has been lost as it enters the veins – but there is a small driving force – respiratory pump • • venous BP = 17 mm Hg SVC blood pressure = 0 mm Hg • venous return is enhanced by many extrinsic factors: 1. sympathetic activity – venous smooth muscle has an abundant sympathetic nervous innervation • their release of NE can produce a small amount of venoconstriction • produces a driving force to return blood to the heart
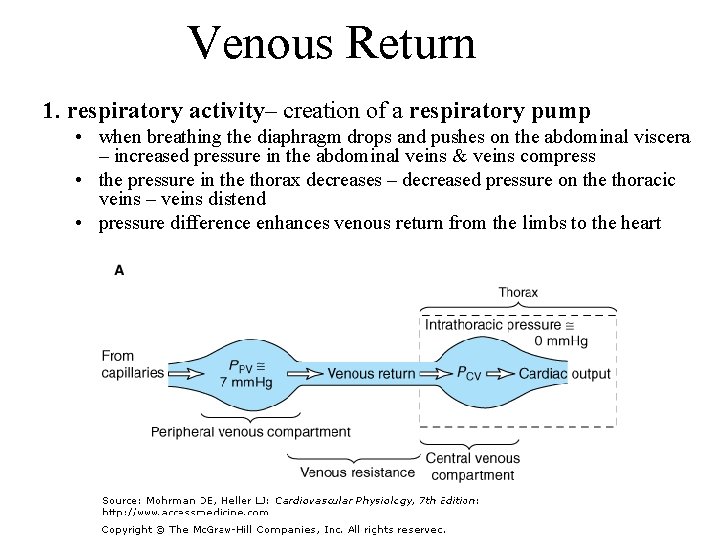
Venous Return 1. respiratory activity– creation of a respiratory pump • when breathing the diaphragm drops and pushes on the abdominal viscera – increased pressure in the abdominal veins & veins compress • the pressure in the thorax decreases – decreased pressure on the thoracic veins – veins distend • pressure difference enhances venous return from the limbs to the heart
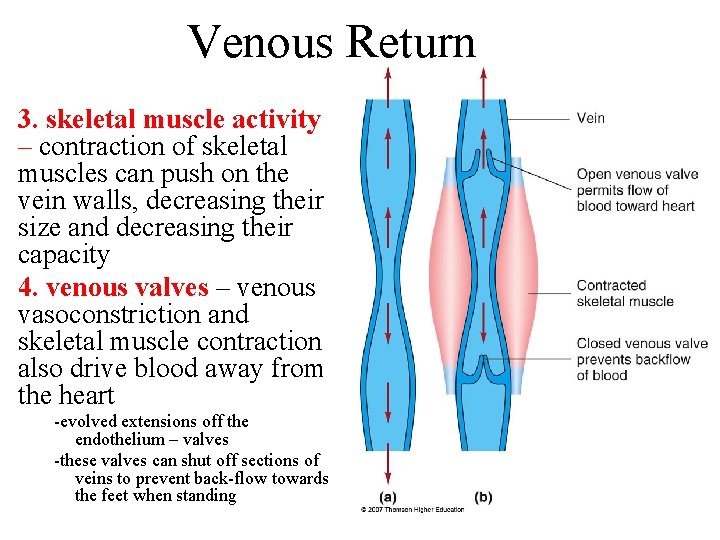
Venous Return 3. skeletal muscle activity – contraction of skeletal muscles can push on the vein walls, decreasing their size and decreasing their capacity 4. venous valves – venous vasoconstriction and skeletal muscle contraction also drive blood away from the heart -evolved extensions off the endothelium – valves -these valves can shut off sections of veins to prevent back-flow towards the feet when standing
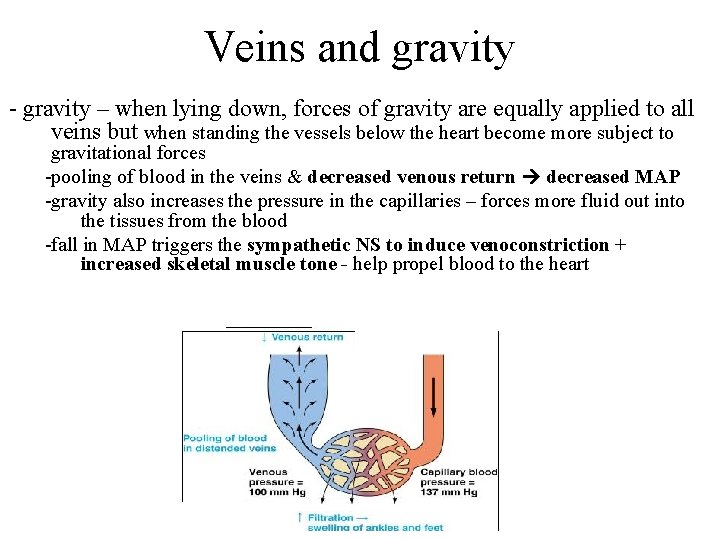
Veins and gravity - gravity – when lying down, forces of gravity are equally applied to all veins but when standing the vessels below the heart become more subject to gravitational forces -pooling of blood in the veins & decreased venous return decreased MAP -gravity also increases the pressure in the capillaries – forces more fluid out into the tissues from the blood -fall in MAP triggers the sympathetic NS to induce venoconstriction + increased skeletal muscle tone - help propel blood to the heart
21 -75
- Slides: 75