Neck Space Infections Dr Vishal Sharma Fascial layers












































- Slides: 99

Neck Space Infections Dr. Vishal Sharma

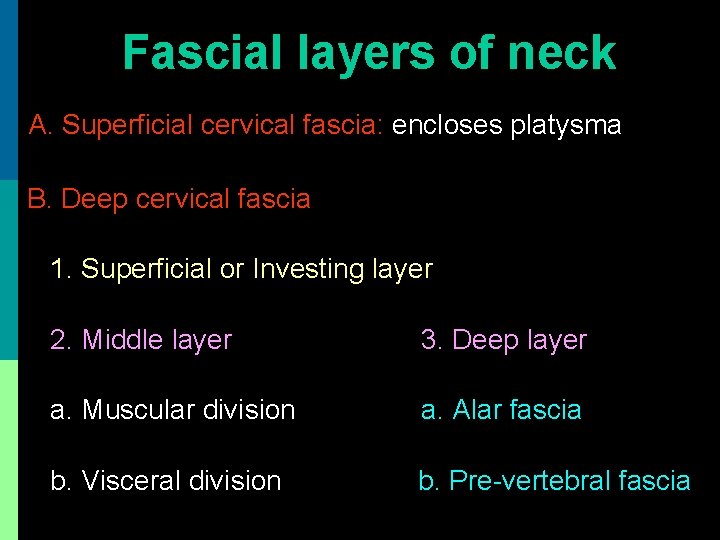
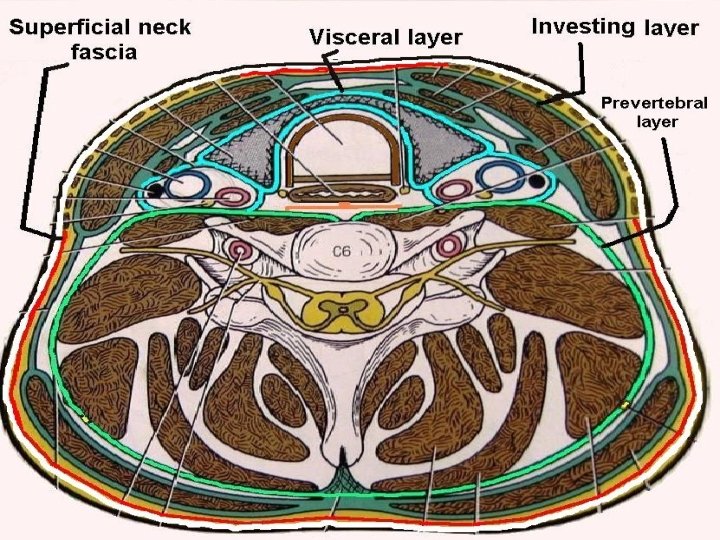
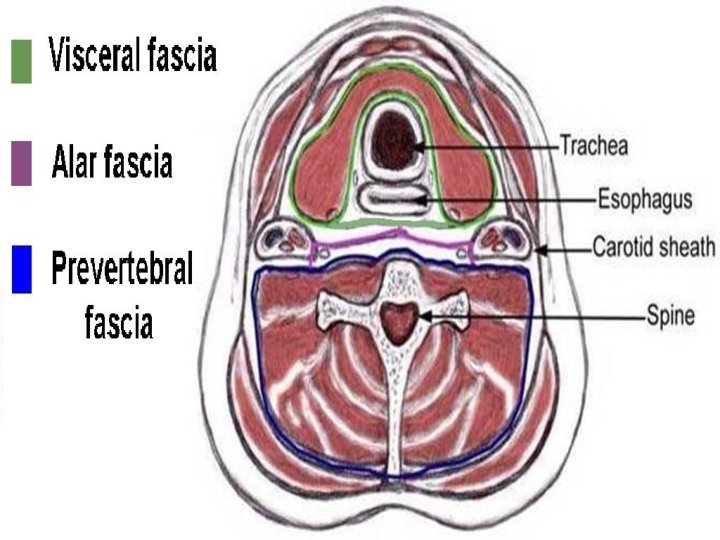
Fascial layers of neck A. Superficial cervical fascia: encloses platysma B. Deep cervical fascia 1. Superficial or Investing layer 2. Middle layer 3. Deep layer a. Muscular division a. Alar fascia b. Visceral division b. Pre-vertebral fascia

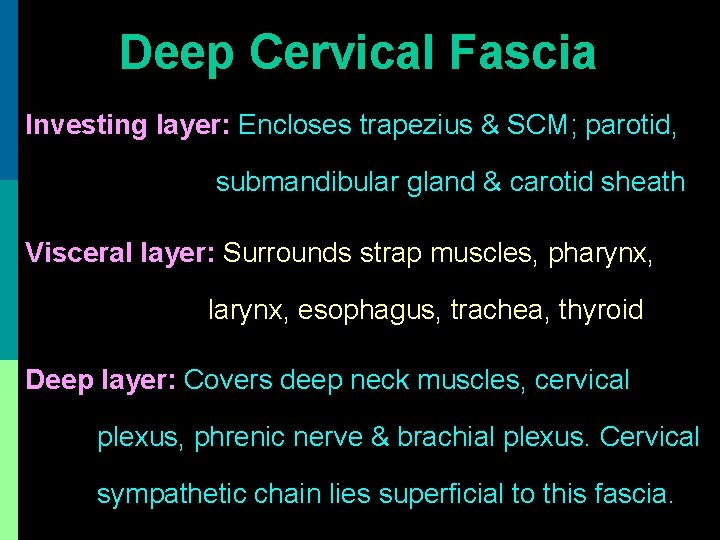
Deep Cervical Fascia Investing layer: Encloses trapezius & SCM; parotid, submandibular gland & carotid sheath Visceral layer: Surrounds strap muscles, pharynx, larynx, esophagus, trachea, thyroid Deep layer: Covers deep neck muscles, cervical plexus, phrenic nerve & brachial plexus. Cervical sympathetic chain lies superficial to this fascia.



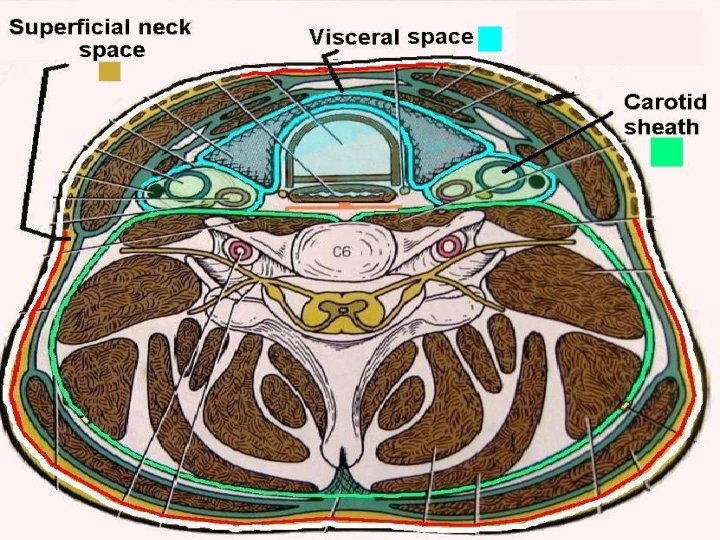
Classification of neck spaces

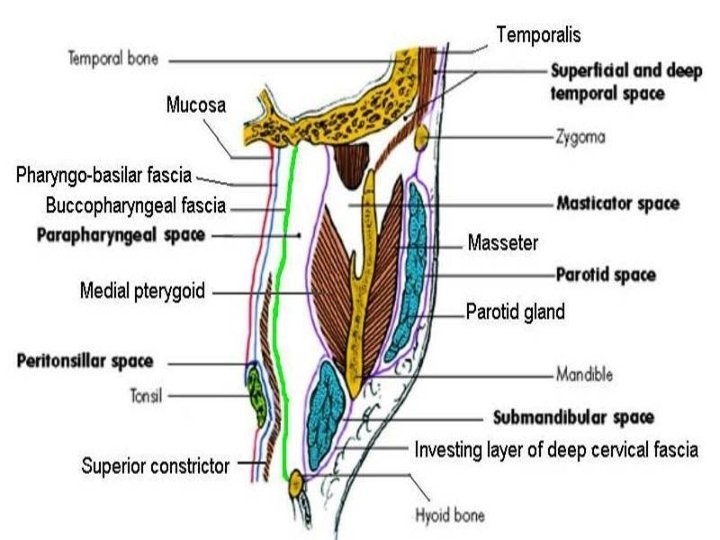
A. Involves entire neck B. Spaces above hyoid 1. Superficial neck space 1. Submental 2. Deep neck spaces 2. Submandibular a. Carotid sheath a. Sublingual b. Retro-pharyngeal b. Submaxillary c. Danger space 3. Masticator d. Pre-vertebral 4. Parotid C. Below Hyoid 5. Parapharyngeal 1. Pre-tracheal space 6. Peri-tonsillar





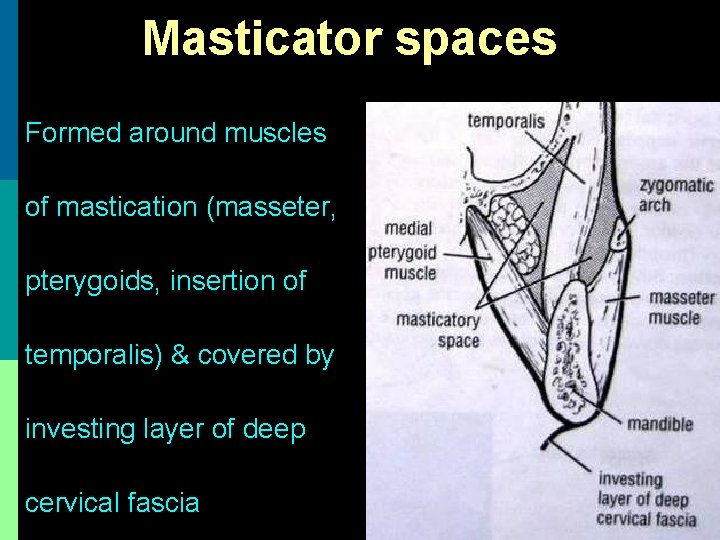
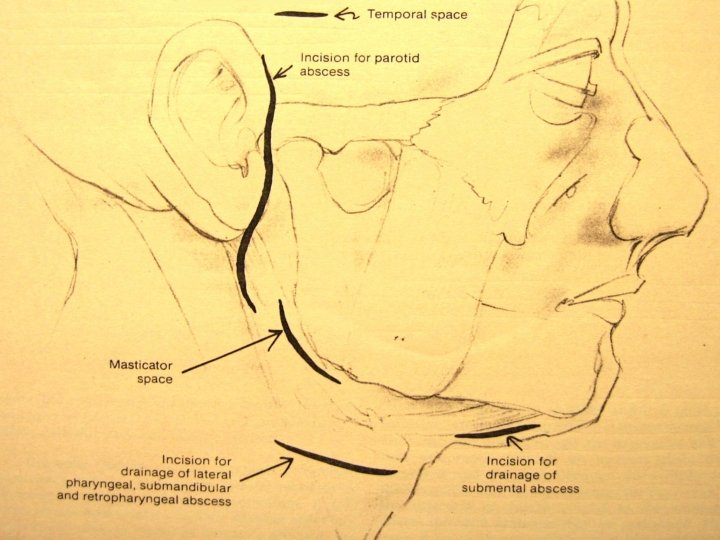
Masticator spaces Formed around muscles of mastication (masseter, pterygoids, insertion of temporalis) & covered by investing layer of deep cervical fascia

Classification of neck space infections

A. Involves entire neck B. Supra-hyoid abscess 1. Superficial space Sub-mental Necrotizing fascitis Masticator 2. Deep space abscess Parotid Carotid sheath Ludwig’s angina Retro-pharyngeal Para-pharyngeal Danger space Peri-tonsillar (quinsy) Pre-vertebral C. Infra-hyoid abscess Pre-tracheal

Necrotizing fasciitis

p Rare infection of superficial neck space causing necrosis of fascia + subcutaneous tissue, initially sparing skin & muscle p Term coined in 1952 by Wilson p Etiology: Dental infections, skin trauma, quinsy & parapharyngeal abscess p Bacteriology: β-hemolytic streptococcus, Staphylococcus aureus, anaerobes

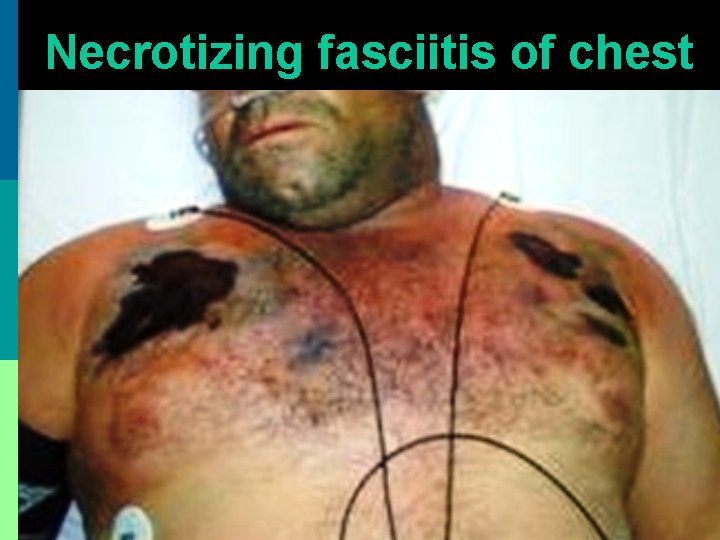
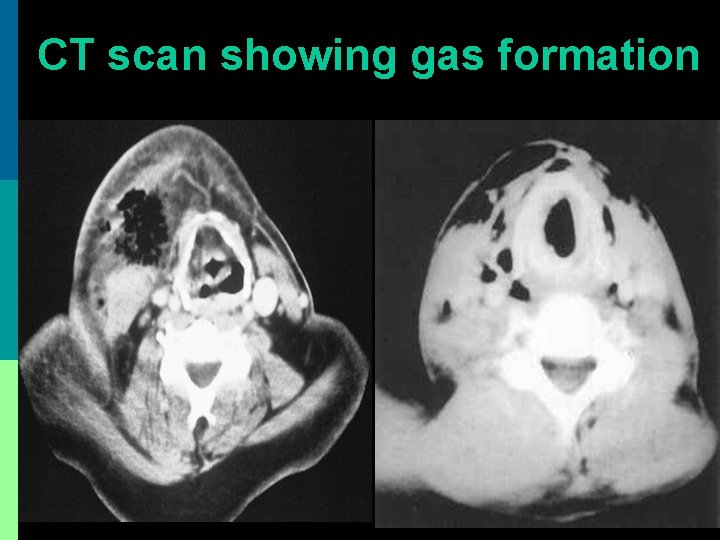
Clinical Presentation p Outer zone of erythema, intermediate zone of tender ecchymosis & central zone of vesiculation + black necrosis + ulceration p Fascial necrosis extends beyond skin necrosis p Skin anesthesia (damage of cutaneous nerves) p Soft tissue crepitus due to gas formation p Hypocalcemia, hyponatremia & dehydration

Necrotizing fasciitis of chest

CT scan showing gas formation

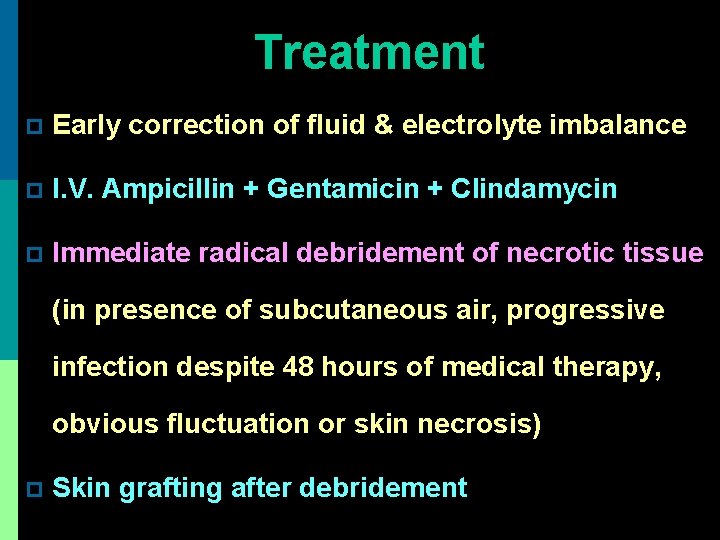
Treatment p Early correction of fluid & electrolyte imbalance p I. V. Ampicillin + Gentamicin + Clindamycin p Immediate radical debridement of necrotic tissue (in presence of subcutaneous air, progressive infection despite 48 hours of medical therapy, obvious fluctuation or skin necrosis) p Skin grafting after debridement

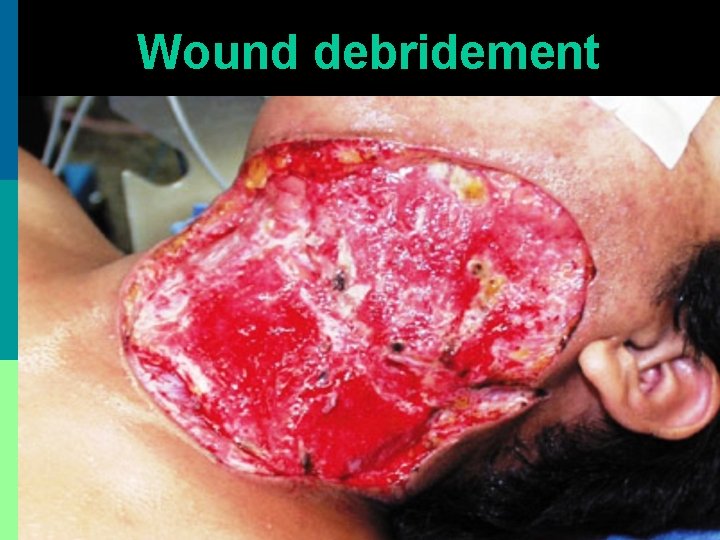
Wound debridement

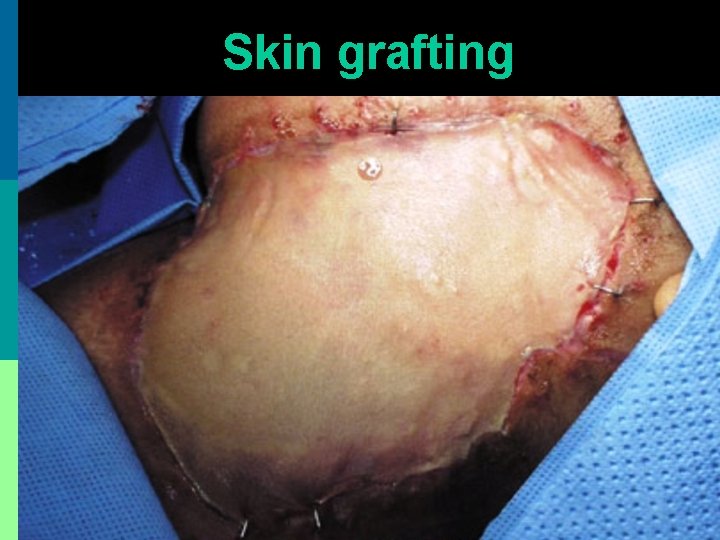
Skin grafting

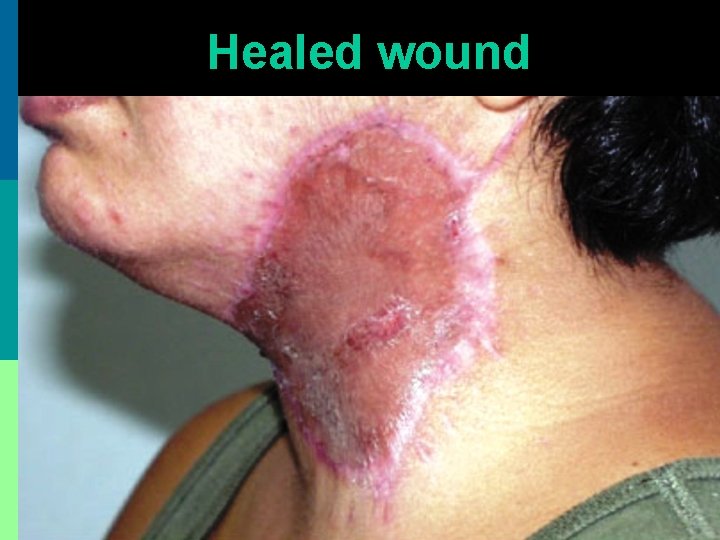
Healed wound

p Poor prognostic factors: Diabetes mellitus, atherosclerosis, chronic renal failure, obesity, immuno-suppression, malnutrition p Complications: necrosis of chest wall fascia, mediastinitis, pleural effusion, pericardial effusion, empyema, airway obstruction, arterial erosion, jugular vein thrombophlebitis, septic shock, lung abscess, carotid artery thrombosis

Ludwig’s Angina

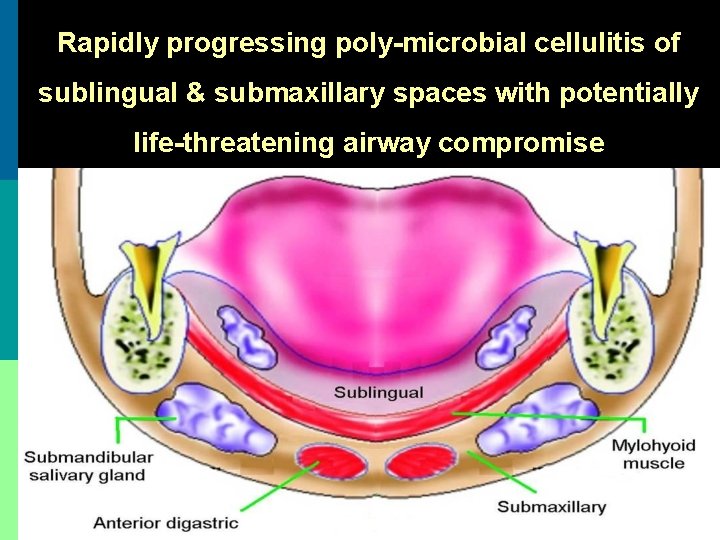
Rapidly progressing poly-microbial cellulitis of sublingual & submaxillary spaces with potentially life-threatening airway compromise

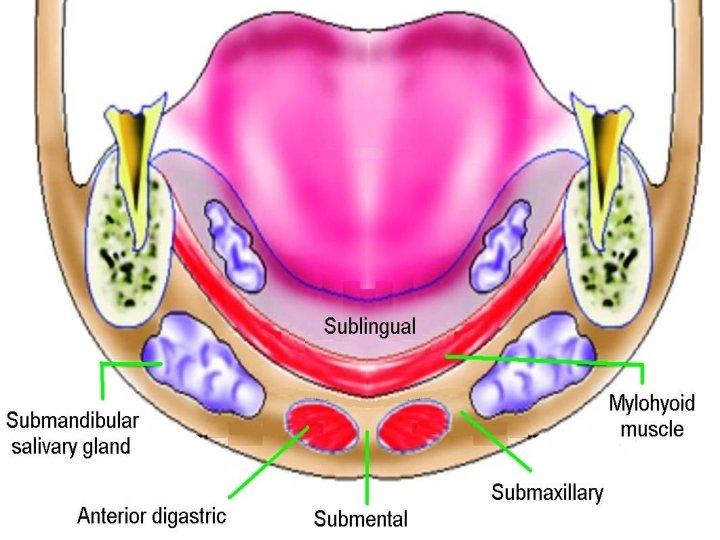
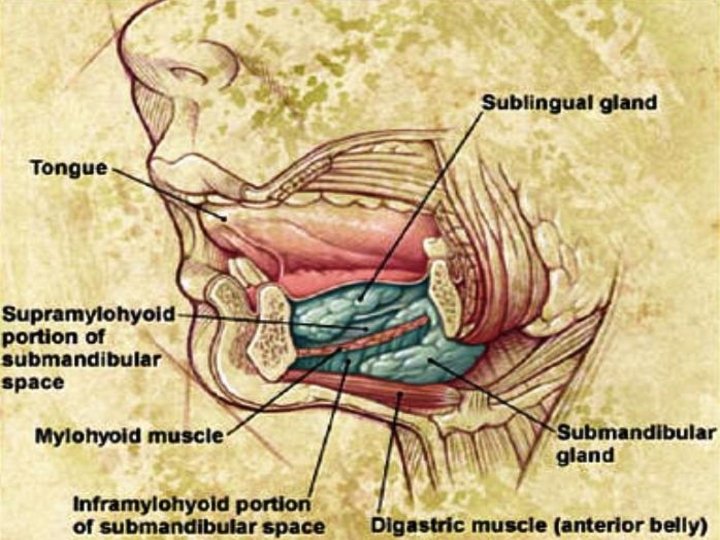
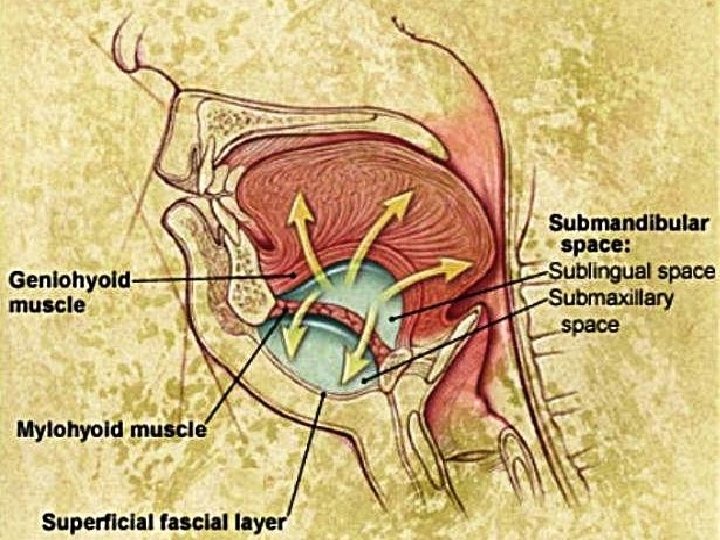
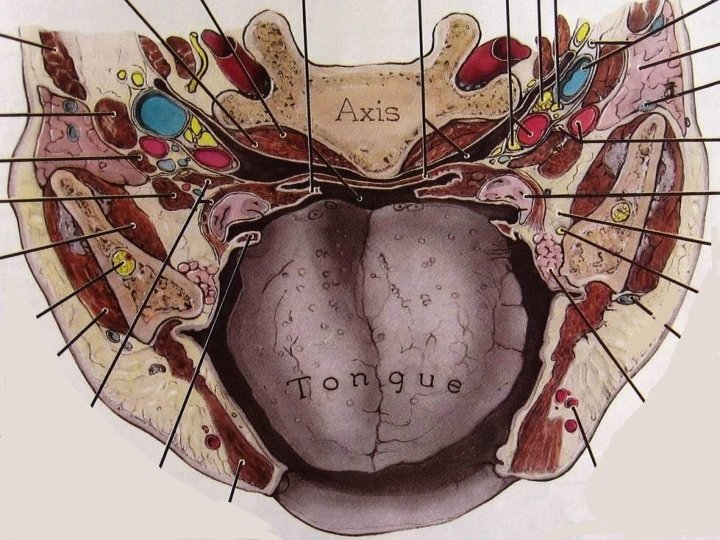
Submandibular space Boundaries: Anterior & lateral: mandible Medial: anterior belly of digastric Posterior: submandibular gland Inferior: level of hyoid bone Subdivisions: 1. Sublingual space: above mylohyoid muscle 2. Submaxillary space: below mylohyoid muscle Contents: Submandibular salivary gland, lymph nodes

Etiology of Ludwig’s angina

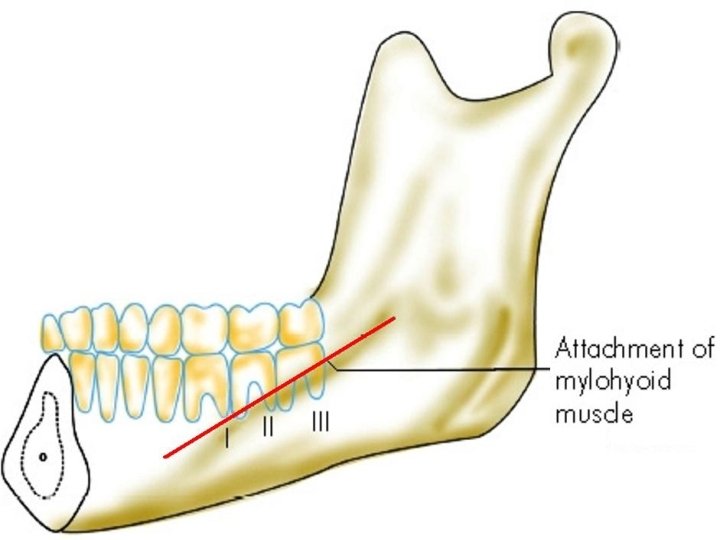
A. Lower dental or periodontal infection (80%): 1. Poor dental hygiene (caries & abscess) 2. Tooth extraction (lower molars & premolars) Roots of premolars & 1 st molar lie above mylohyoid sublingual space infection Roots of 2 nd & 3 rd molars lie below mylohyoid submaxillary space infection B. Others (20%): submandibular sialadenitis, floor of mouth trauma, mandibular fractures




Causative organisms Mixed aerobic & anaerobic infection p Streptococcus pyogenes p Streptococcus viridans p Streptococcus pneumoniae p Staphylococcus p Fusobacterium p Bacteroides p Peptostreptococcus

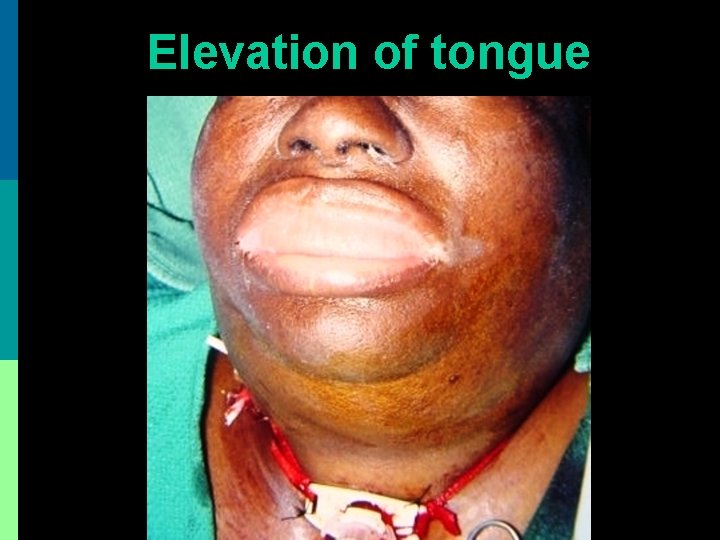
Clinical Features p Toothache, fever, odynophagia, drooling p Floor of mouth swelling + tongue elevation in sublingual space infection p Brawny / woody tender swelling below chin in submaxillary space infection p Trismus p Stridor: falling back of tongue, laryngeal edema p Initial cellulitis delayed pus formation

Elevation of tongue

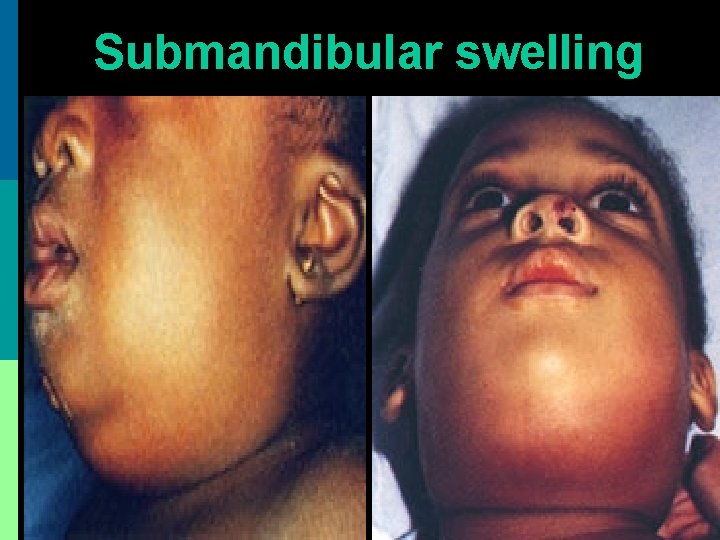
Submandibular swelling

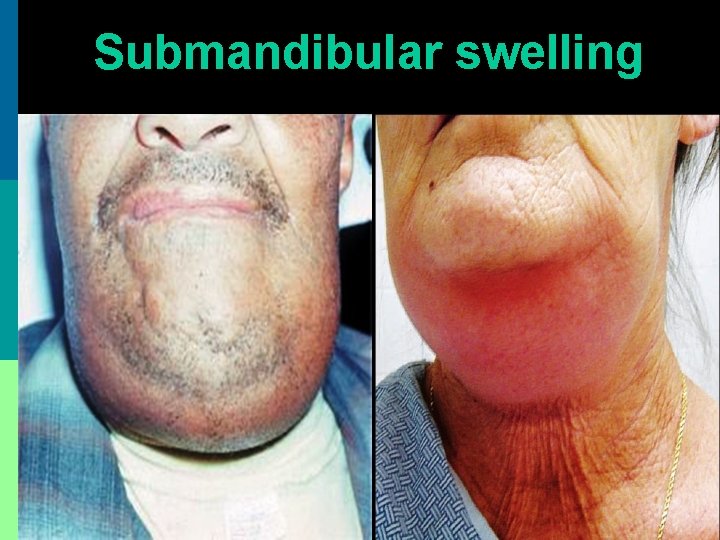
Submandibular swelling

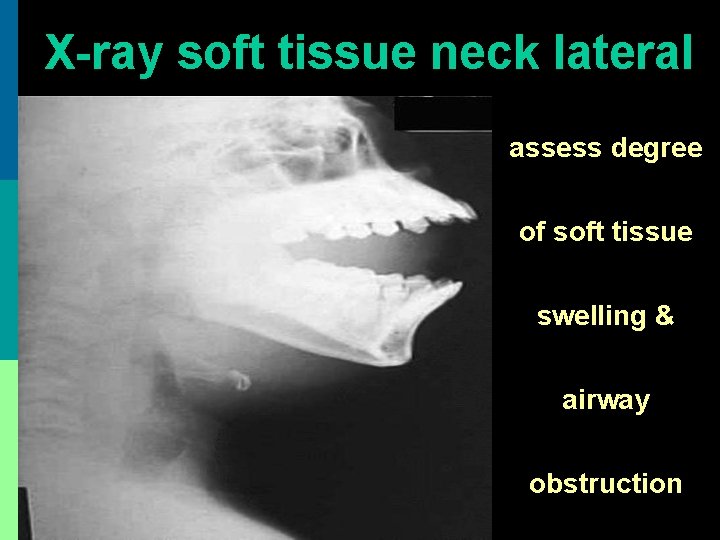
X-ray soft tissue neck lateral assess degree of soft tissue swelling & airway obstruction

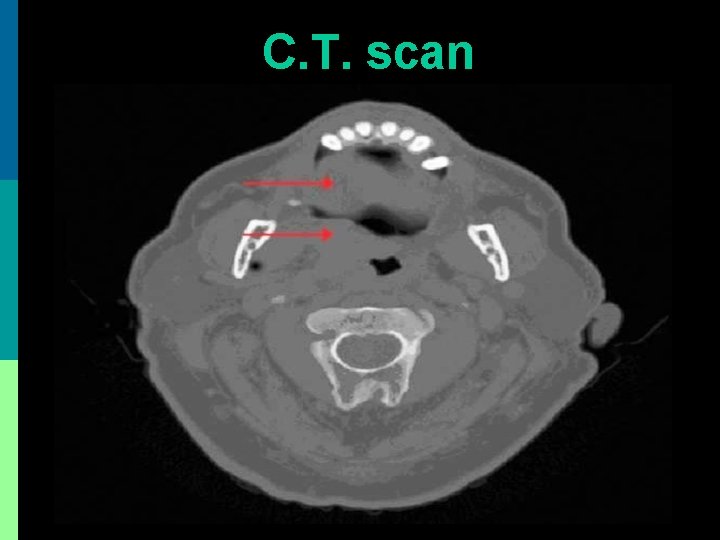
C. T. scan

Treatment of Ludwig’s angina

1. I. V. antibiotics: Cefuroxime / Ceftriaxone + Metronidazole / Clindamycin 2. Airway: endotracheal intubation / tracheostomy 3. Incision & drainage of serous fluid / pus a. Intra-oral: for sublingual space infection b. Extra-oral: for submaxillary space infection Transverse incision from one angle of mandible to opposite angle of mandible 4. IV fluid for adequate hydration 5. Periodic assessment for disease progression & airway compromise

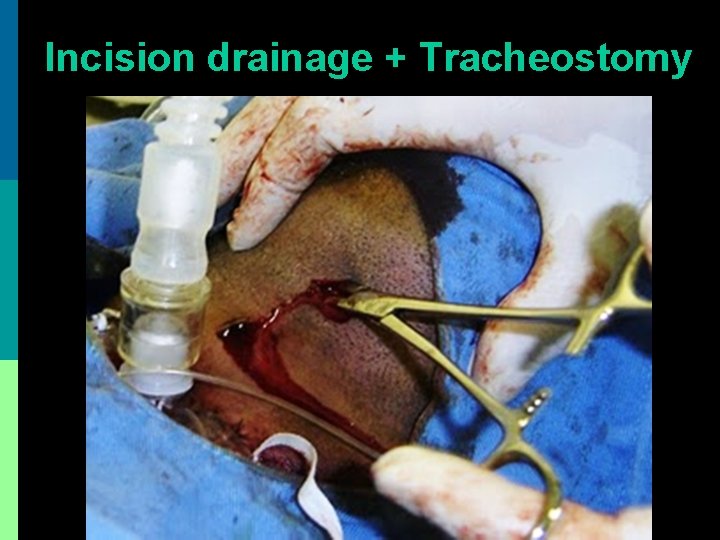
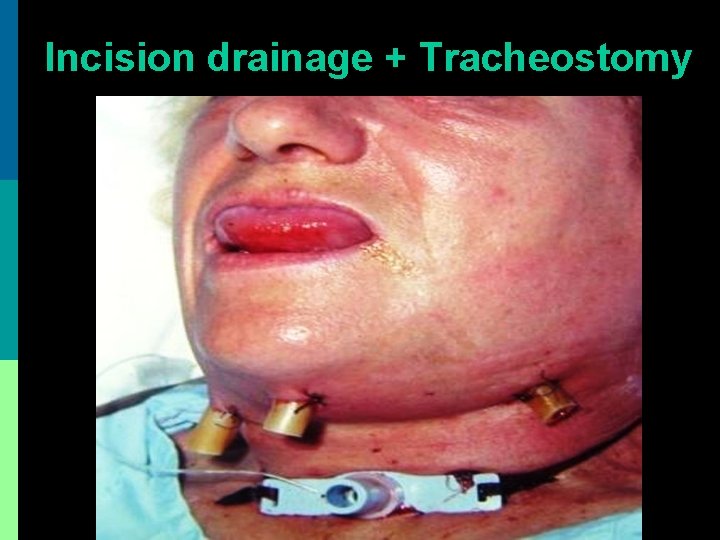
Incision drainage + Tracheostomy

Incision drainage + Tracheostomy

Complications p Parapharyngeal abscess p Retropharyngeal abscess p Acute airway obstruction (within hours): due to pushing back of tongue, laryngeal edema p Aspiration pneumonia p Septicemia p Death

Retropharyngeal abscess

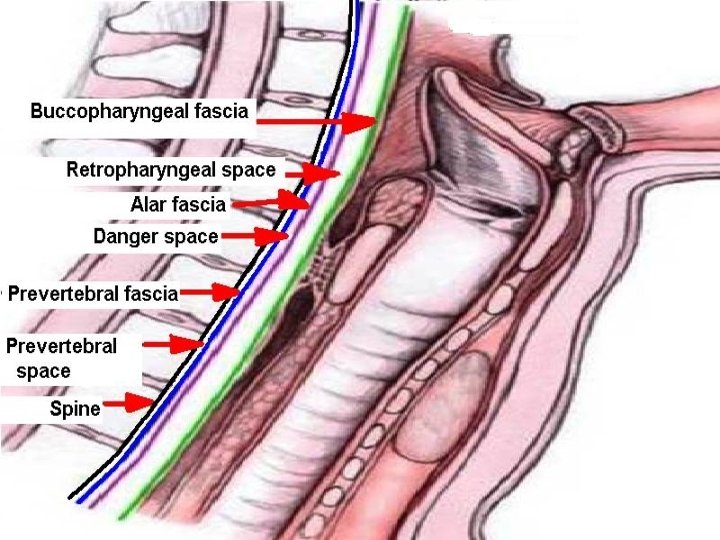
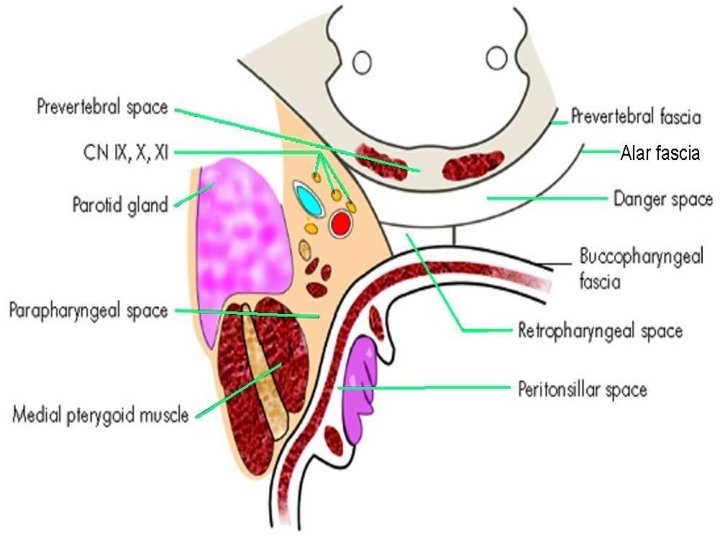
Retropharyngeal Space Superior: Base of skull Inferior: Mediastinum (till tracheal bifurcation) Anterior: Buccopharyngeal fascia Posterior: Alar fascia Lateral: Parapharyngeal spaces Divided into two lateral compartments (space of Gillette) by midline fibrous raphe


Retropharyngeal abscess Collection of pus in retropharyngeal space Classification: 1. Acute 2. Chronic Acute abscess is common in children below 3 -5 yrs as retropharyngeal nodes of Rouviere regress later

Acute Retropharyngeal Abscess

Etiology p Suppuration of retropharyngeal lymph node of Rouviere from upper respiratory tract infection p Penetrating injury of posterior pharyngeal wall (e. g. . fish bone, vertebral fracture) p Following endoscopic trauma to pharynx p Acute mastoitis: pus tracking under petrous bone

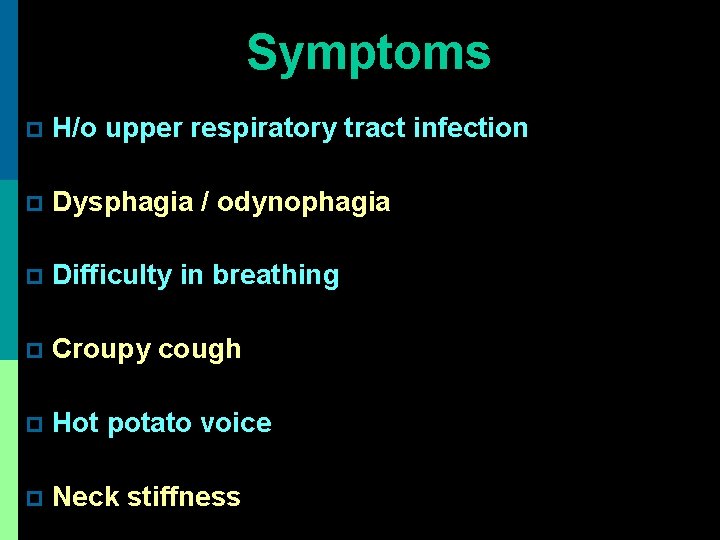
Symptoms p H/o upper respiratory tract infection p Dysphagia / odynophagia p Difficulty in breathing p Croupy cough p Hot potato voice p Neck stiffness

Signs p Febrile, ill-looking, child with drooling p Tender neck swelling + fistula p Torticollis (twisted neck) on side of abscess followed by hyperextension of neck p U/L bulge on posterior pharyngeal wall

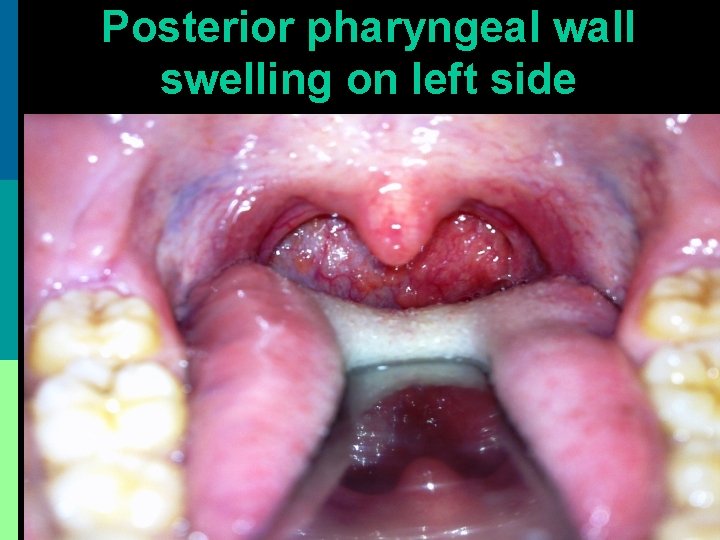
Posterior pharyngeal wall swelling on left side

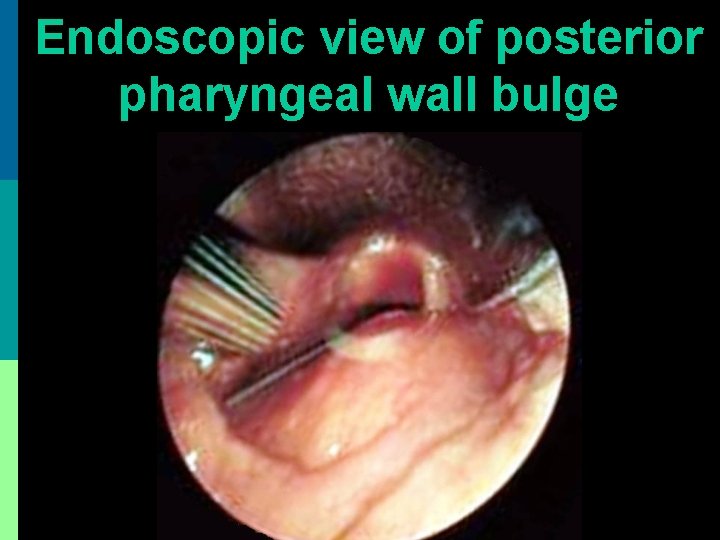
Endoscopic view of posterior pharyngeal wall bulge

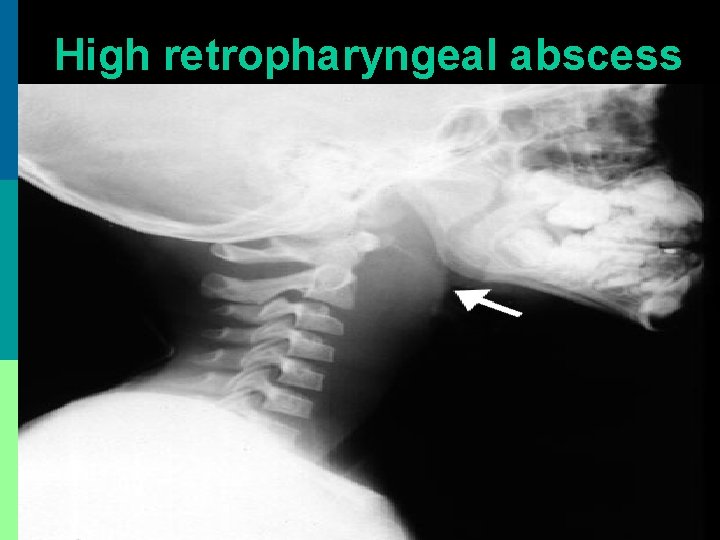
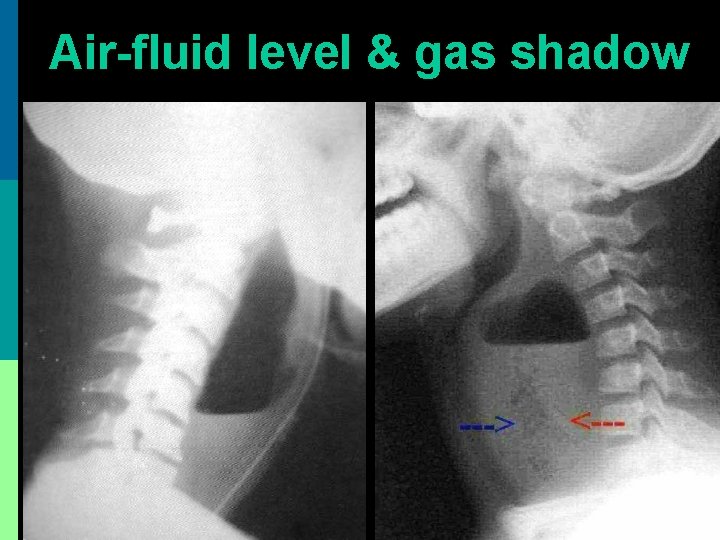
X-ray soft tissue neck (lateral) 1. Widened pre-vertebral soft tissue shadow a. > 7 mm at C 2 vertebra b. > 14 mm at C 6 vertebra below 14 years c. > 22 mm at C 6 vertebra above 14 years 2. Presence of air-fluid level & / gas (acute cases) 3. Homogenous pre-vertebral shadow (chronic) 4. Straightening of cervical spine curve due to spasm of pre-vertebral muscles

High retropharyngeal abscess

Air-fluid level & gas shadow

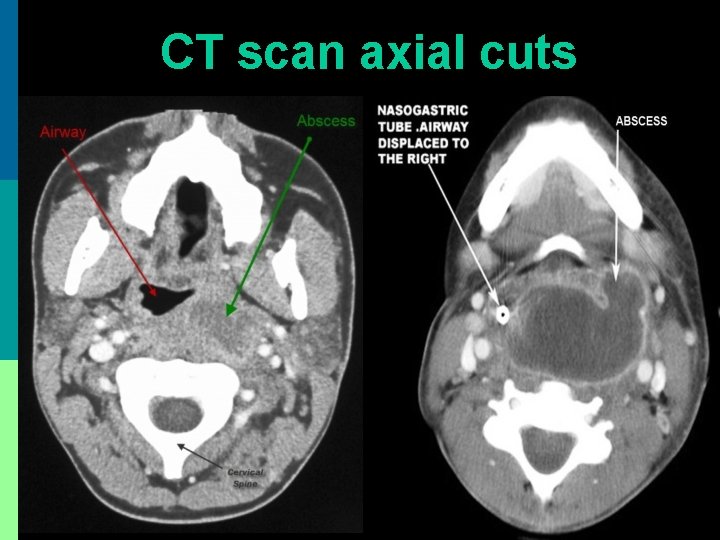
CT scan axial cuts

Treatment 1. IV antibiotics: Ceftriaxone + Metronidazole 2. Incision & drainage: p No anesthesia (as it may rupture abscess) or very careful endotracheal intubation p Supine with head hanging low from table p Vertical or horizontal incision on fluctuant area p Incision + immediate suction of pus 3. Tracheostomy for airway obstruction

Chronic Retropharyngeal Abscess

Etiology p Caries of cervical spine: presents as central posterior pharyngeal wall swelling p Tubercular infection of retropharyngeal lymph nodes from infected deep cervical nodes: presents as lateral posterior pharyngeal wall swelling true retropharyngeal abscess p Post traumatic: vertebral fracture p Spread from parapharyngeal abscess

Clinical Features p Chronic mild dysphagia p Pain is absent due to cold abscess p Bulge of posterior pharyngeal wall with fluctuant swelling (central or lateral) Investigations p As in acute retropharyngeal abscess p Ziehl Neelsen stain of pus after aspiration

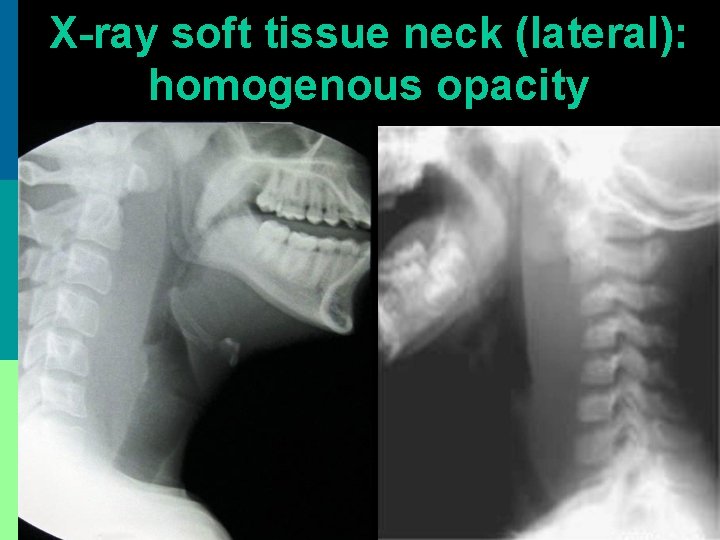
X-ray soft tissue neck (lateral): homogenous opacity

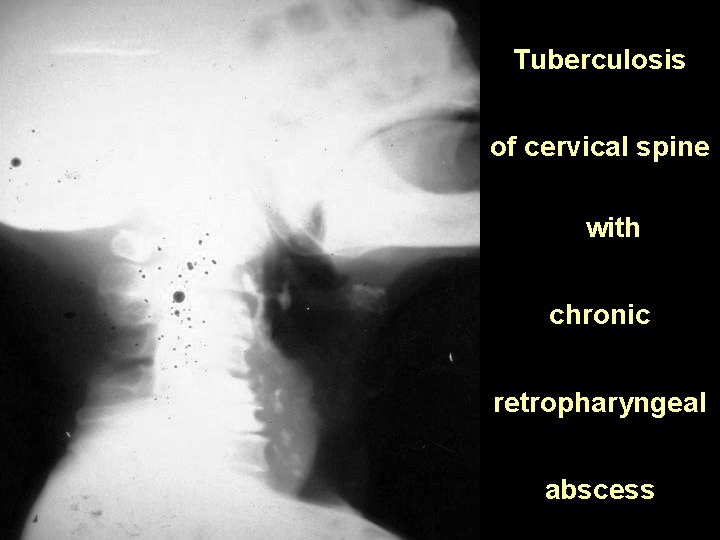
Tuberculosis of cervical spine with chronic retropharyngeal abscess

Treatment 1. I. V. antibiotics: Ceftriaxone + Metronidazole 2. Incision & drainage: p Low abscess: along anterior border of sternocleidomastoid muscle p High abscess: along posterior border of sternocleidomastoid muscle 3. Anti-tubercular therapy for 9 - 12 months

Complications 1. Airway obstruction: mechanical obstruction laryngeal edema 2. Spread of abscess to other neck spaces 3. Spontaneous rupture of abscess 4. Septicemia 5. Death

Parapharyngeal abscess

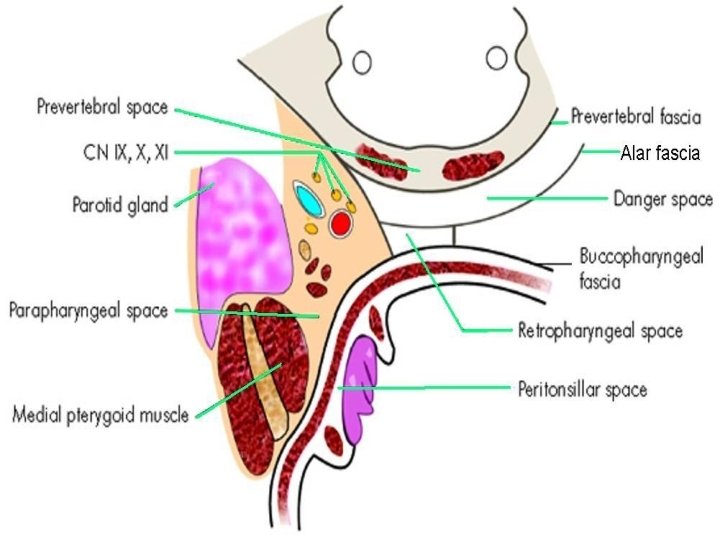
Parapharyngeal space Base & superior limit: Skull Base Apex: Lesser cornu of hyoid Lateral: Mandible ramus, Medial Pterygoid, Parotid Medial: Bucco-pharyngeal fascia, superior constrictor Anterior: Pterygo-mandibular raphe Posterior: Pre-vertebral fascia Inferior: Deep cervical fascia lateral to mandible angle



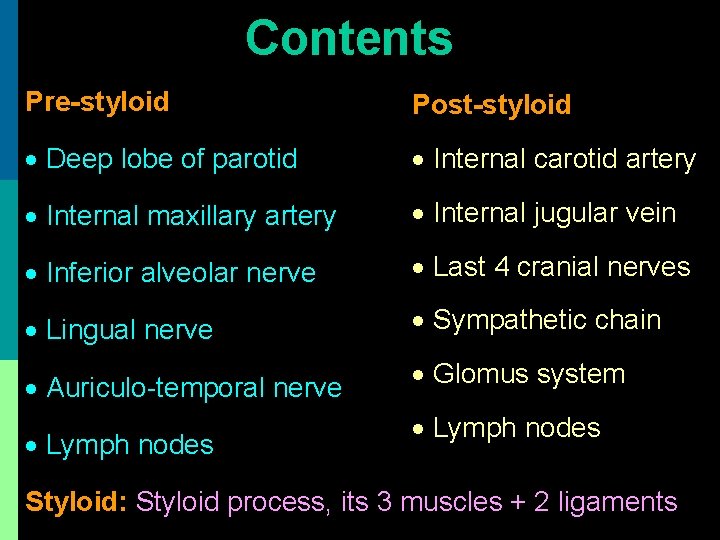
Contents Pre-styloid Post-styloid Deep lobe of parotid Internal carotid artery Internal maxillary artery Internal jugular vein Inferior alveolar nerve Last 4 cranial nerves Lingual nerve Sympathetic chain Auriculo-temporal nerve Glomus system Lymph nodes Styloid: Styloid process, its 3 muscles + 2 ligaments

Etiology p Pharynx: acute tonsillitis, peritonsillar abscess p Teeth: dental infection (esp. lower last molar) p Ear: Bezold’s abscess p Spread from other neck abscess: parotid, retropharyngeal, submandibular p Penetrating neck injuries

Clinical Features 1. Fever, sore throat, odynophagia, torticollis 2. Anterior compartment involvement: a. Tonsils pushed medially b. Trismus c. Neck swelling behind angle of mandible 3. Posterior compartment involvement: a. Medial bulge behind posterior pillar of tonsil b. Paralysis of IX, X, XII & sympathetic chain

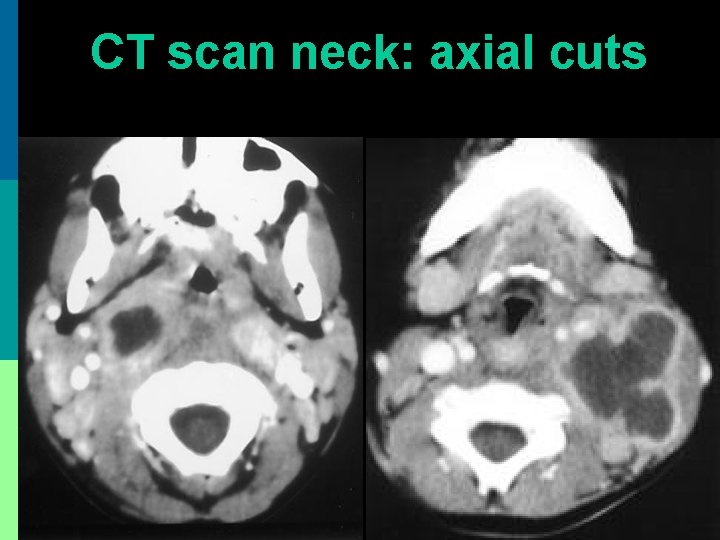
CT scan neck: axial cuts

Treatment 1. IV antibiotics: Ceftriaxone + Metronidazole 2. Incision & drainage: p Under GA with endotracheal intubation p Horizontal incision made 3 cm below angle of mandible p Trans-oral drainage avoided to prevent injury to carotid artery & internal jugular vein 3. Tracheostomy for airway obstruction / trismus


Peritonsillar abscess (Quinsy)

Etio-pathogenesis Pus present between tonsillar capsule & superior constrictor muscle Pathology: aerobic + anaerobic organisms 1. Acute tonsillitis blockage of crypts intra tonsillar abscess peritonsillitis quinsy 2. Abscess of Weber's salivary gland in supra tonsillar fossa quinsy

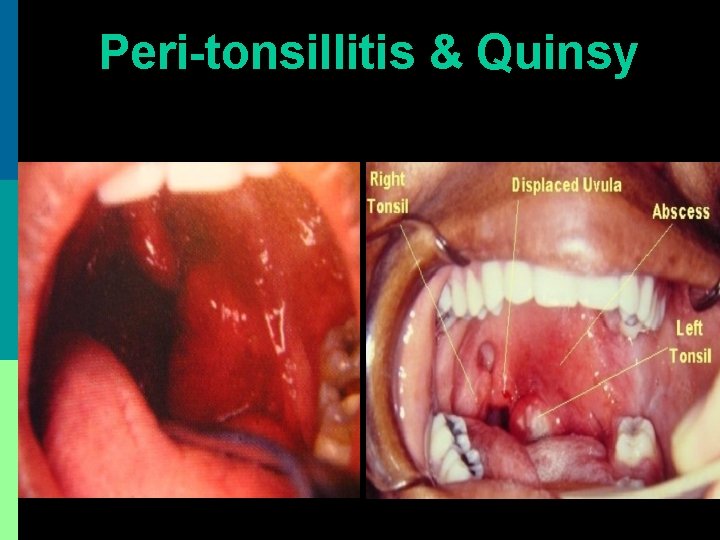
Clinical features Symptoms: Young adult with severe odynophagia, fever, halitosis & muffled voice Signs: 1. Para-tonsil area swollen & congested 2. U/L tonsil ed, pushed medially, congested 3. Jugulo-digastric lymph node tender, enlarged 4. Trismus 5. Torticollis

Peri-tonsillitis & Quinsy

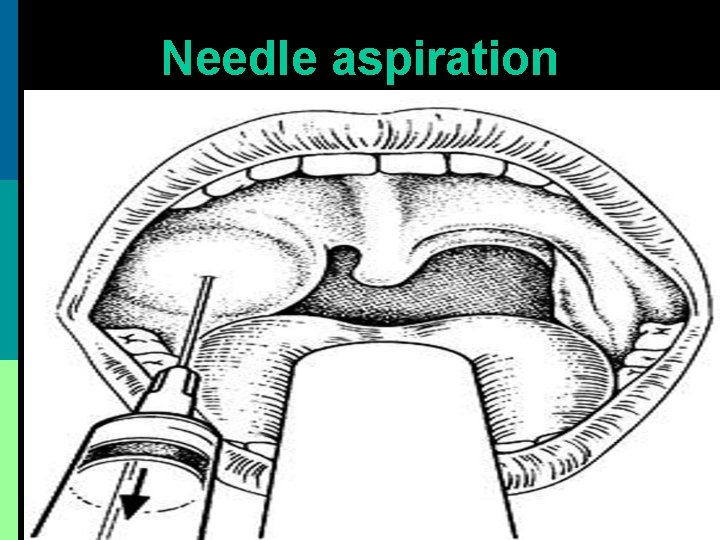
Management Diagnosis: Needle aspiration reveals pus Medical treatment: 1. Urgent admission, I. V. fluids 2. I. V. Cefotaxime + Metronidazole 3. Antihistamine - decongestant + analgesic 4. Betadine gargle

Needle aspiration

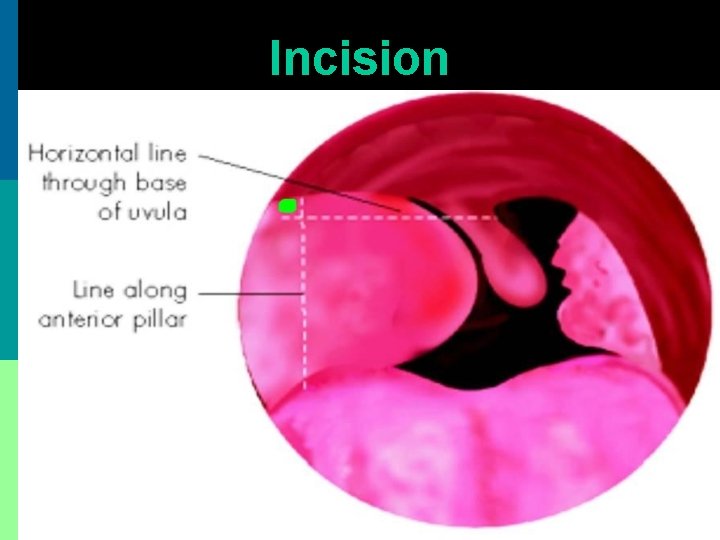
Incision

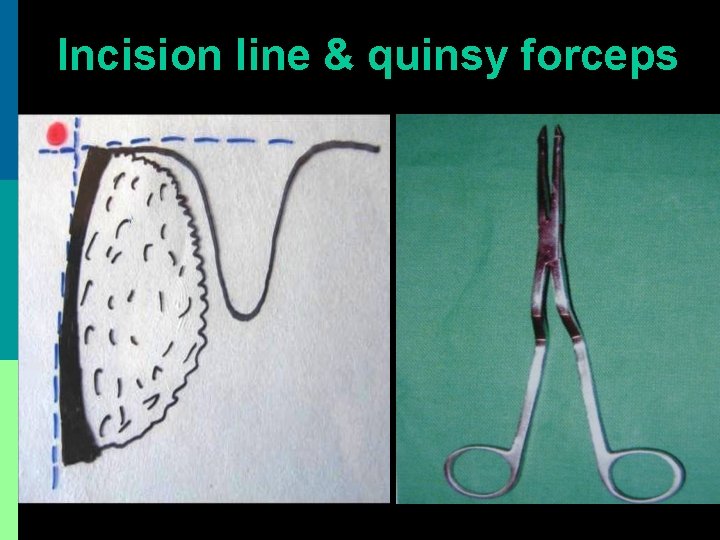
Incision line & quinsy forceps

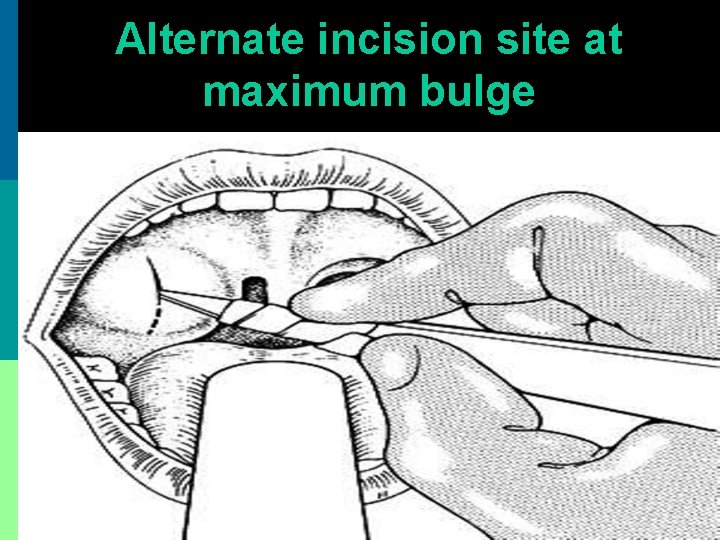
Alternate incision site at maximum bulge

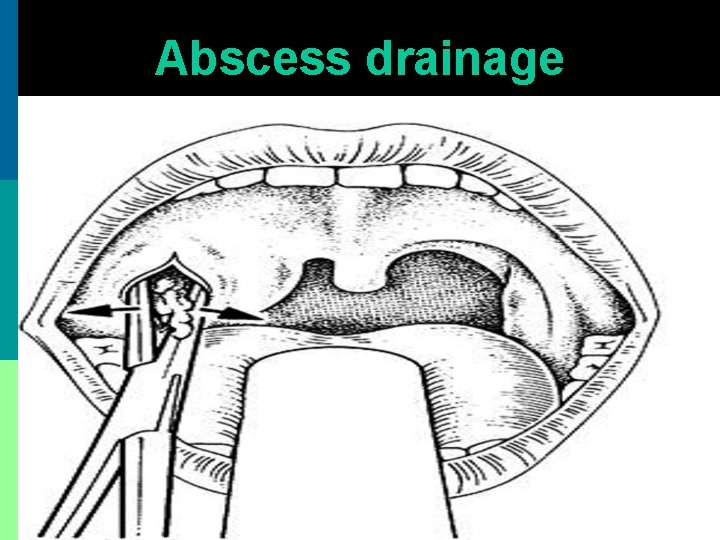
Abscess drainage

Incision & drainage p Incision made with # 11 blade or Thilenius peritonsillar abscess drainage forceps p Nick made above & lateral to junction of 2 imaginary lines. Horizontal along base of uvula, vertical along anterior tonsillar pillar. p Incision widened with sinus forceps & pus drained. No anesthesia is required.

Surgical treatment 1. Interval tonsillectomy after 4 – 6 wk. 2. Hot tonsillectomy or abscess tonsillectomy is avoided as it leads to: more bleeding septicemia

Complications of quinsy 1. Parapharyngeal abscess 2. Retropharyngeal abscess 3. Laryngitis & laryngeal edema 4. Lung abscess 5. Internal jugular vein thrombosis 6. Septicemia

Parotid abscess

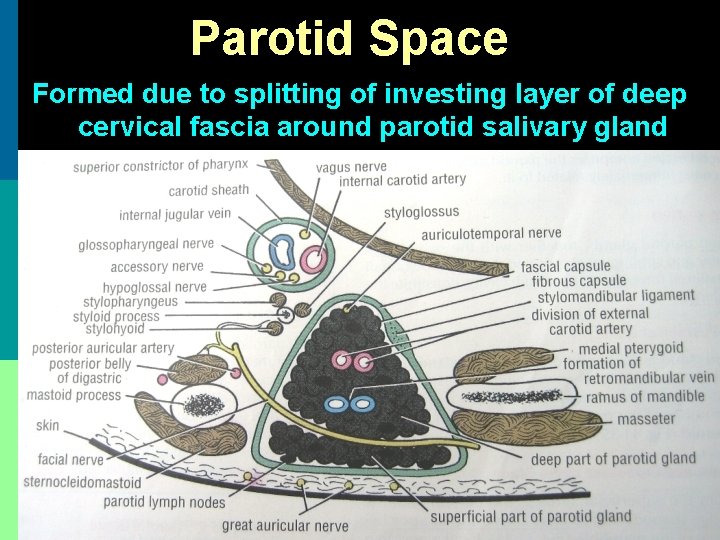
Parotid Space Formed due to splitting of investing layer of deep cervical fascia around parotid salivary gland

Etiology p Ascent of bacterial infection (Staphylococcus, Haemophillus, Streptococcus) to a dehydrated parotid gland along parotid duct from oral cavity p Suppuration of intra-parotid lymph nodes p Spread of infection from EAC via cartilaginous fissures of Santorini or bony foramen of Huschke

Causes of parotid dehydration 1. Post-operative patient (surgical mumps) 2. Medications that decrease salivary flow: p Antihistamines p Tricyclic antidepressants p Barbiturates p Diuretics p Parasympathomimetics

Parotid abscess p Pain + induration over parotid gland p Pitting edema of parotid area differentiates parotid abscess from simple parotitis p Parotid massage expresses pus from parotid duct into oral cavity (opposite upper 2 nd molar)

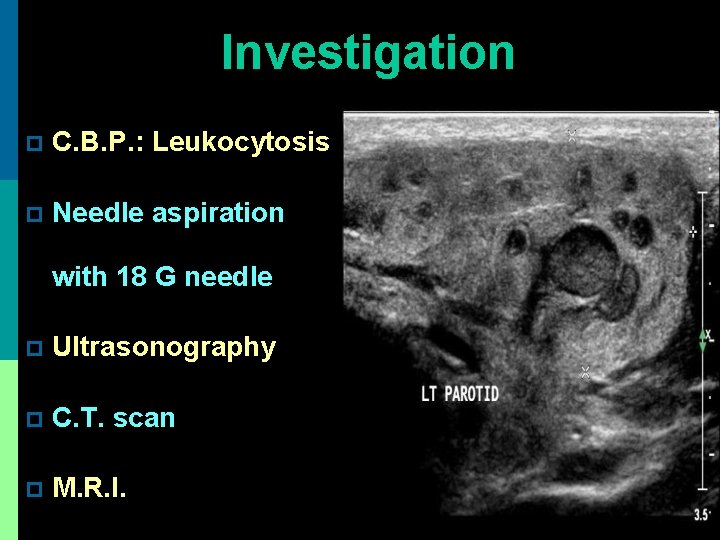
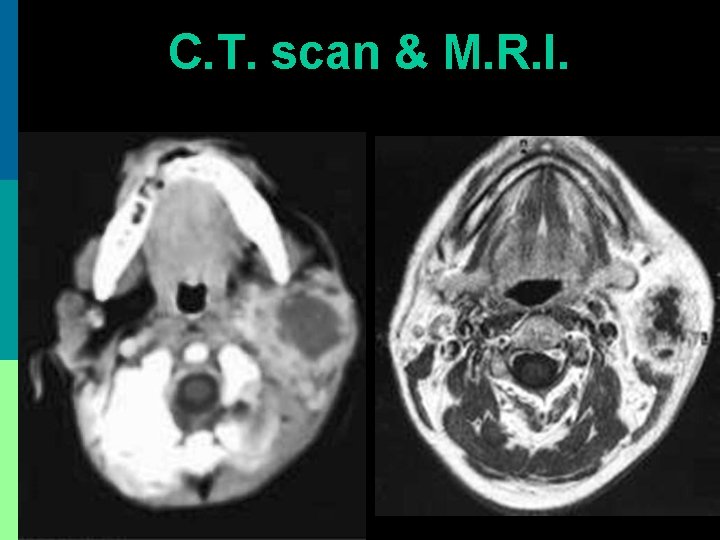
Investigation p C. B. P. : Leukocytosis p Needle aspiration with 18 G needle p Ultrasonography p C. T. scan p M. R. I.

C. T. scan & M. R. I.

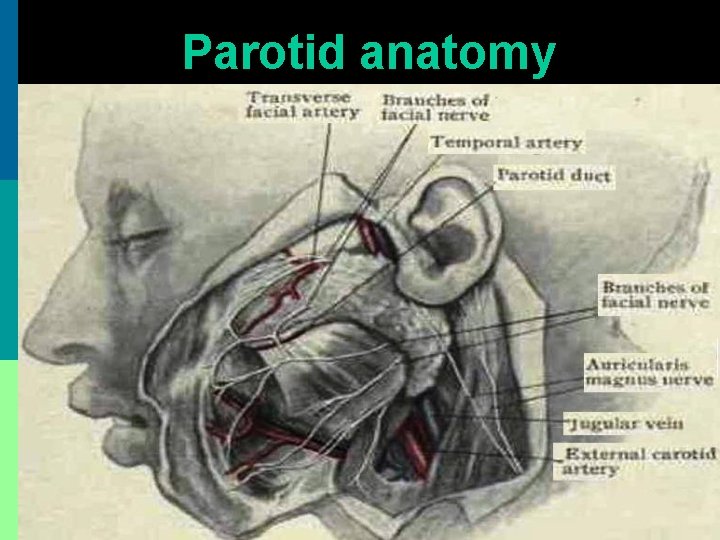
Parotid anatomy

Treatment 1. IV fluid for dehydration 2. IV Ampicillin + Gentamicin + Metronidazole 3. Incision drainage: a. Blair’s incision made b. Multiple incisions made through fascia, parallel to facial nerve branches c. Blunt dissection to evacuate pus. Drains placed.

Thank You