Chapter 18 Innate immunity nonspecific defenses of the
























![Phagocyte migration – a picture [Insert Animation Inflammation: Overview, Steps. ] MORE VIDEOS: Margination: Phagocyte migration – a picture [Insert Animation Inflammation: Overview, Steps. ] MORE VIDEOS: Margination:](https://slidetodoc.com/presentation_image_h/203e8b44c46579f3852a150b701fac70/image-46.jpg)






![Phagocyte Migration [Insert Animation Inflammation: Overview, Steps. ] Figure 16. 8 c Phagocyte Migration [Insert Animation Inflammation: Overview, Steps. ] Figure 16. 8 c](https://slidetodoc.com/presentation_image_h/203e8b44c46579f3852a150b701fac70/image-57.jpg)

























- Slides: 100

Chapter 18 Innate immunity – nonspecific defenses of the host

From a microbe’s perspective = How do we avoid becoming a food source for microbes?

Pre quiz • What is immunity? • Distinguish innate from acquired immunity • Specify if this is part of the innate or adaptive immune system, both or neither – Red blood cell – White blood cell – T cell and B cell – Natural killer cell and phagocytes – Cytokine – Complement system – Skin, mucous and “normal” microbiota

Connections – relate these topics to disease and/or immunity (Reason or example immunity relates to …) • Cell anatomy and structure • Virus anatomy and structure • Enzymes and metabolism • Gene expression/regulation (DNA protein) • Mechanisms of pathogenicity (pathogen tools)

Human Immune System in two acts Innate Immunity (Ch 18) – non‐specific; defends against any pathogen Adaptive Immunity (Ch 19) – response to specific pathogen; detection of antigens and production of antibodies; develop throughout life and provide substantial increase in protection *Innate Immunity: recent work has shown that most components rely on pattern recognition, or detection of molecules associated with invading microbes (e. g. , lipopolysaccharide, lipoteichoic acid, peptidoglycans) Phagocytic cells engulfing bacteria

Recall from last sections • Pathogenicity – Surface proteins and lipids • Adhesion • Recognition/evasion • Endotoxin – Exotoxin – Ability to mutate • Portals of entry – Skin – Mucous membranes – parenteral

An Overview of the Body’s Defenses Figure 16. 1

Goals of innate immunity • Prevent infection • Eliminate foreign substances and pathogens • Generate acquired immune response*

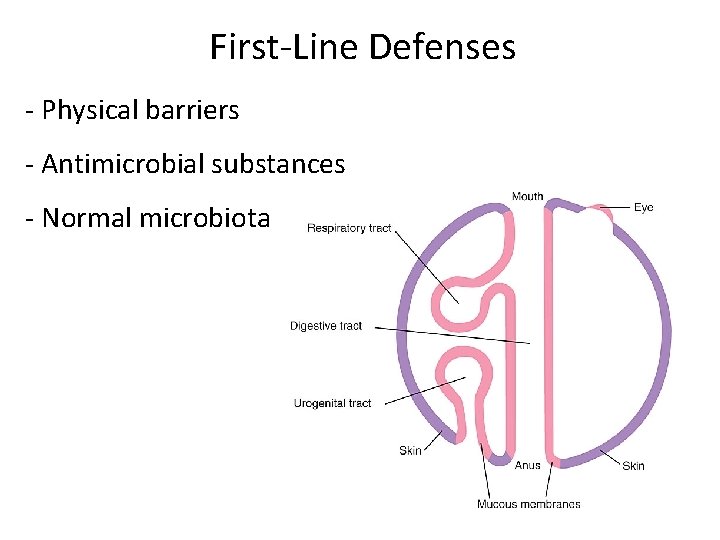
First‐Line Defenses ‐ Physical barriers ‐ Antimicrobial substances ‐ Normal microbiota

Think about • How does your skin protect you? • Mucous membranes? • Anything you know already is in your saliva or mucous that may help protect you? • How can your normal microbiota help you?

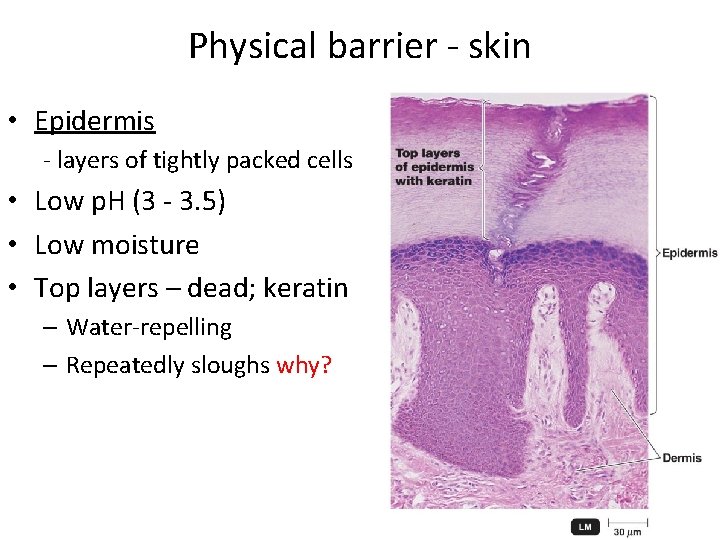
Physical barrier ‐ skin • Epidermis ‐ layers of tightly packed cells • Low p. H (3 ‐ 3. 5) • Low moisture • Top layers – dead; keratin – Water‐repelling – Repeatedly sloughs why? Figure 16. 2

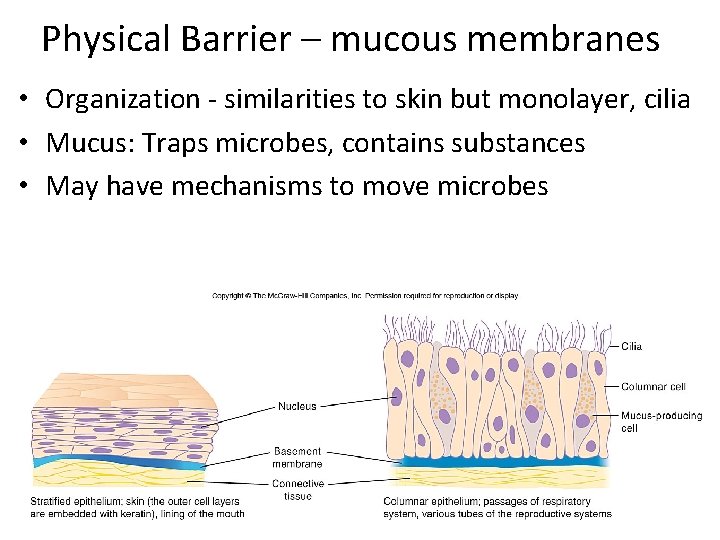
Physical Barrier – mucous membranes • Organization ‐ similarities to skin but monolayer, cilia • Mucus: Traps microbes, contains substances • May have mechanisms to move microbes

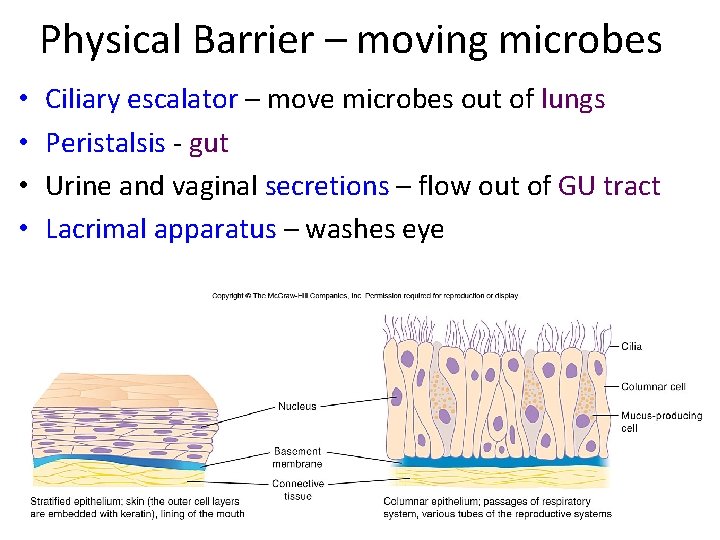
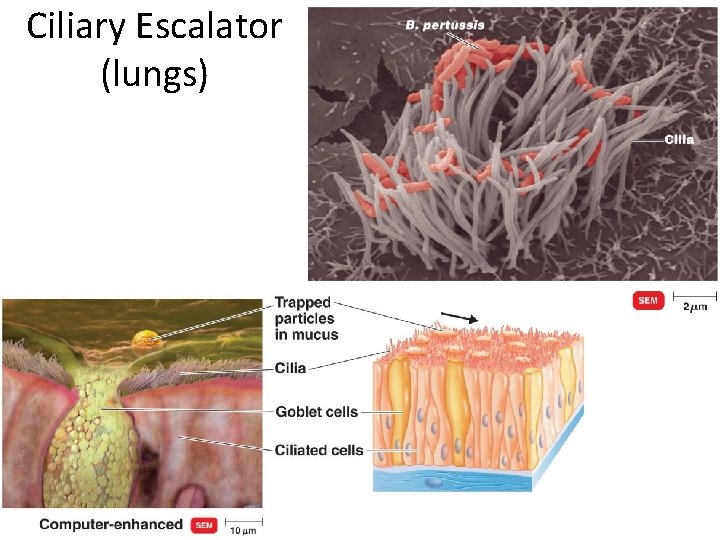
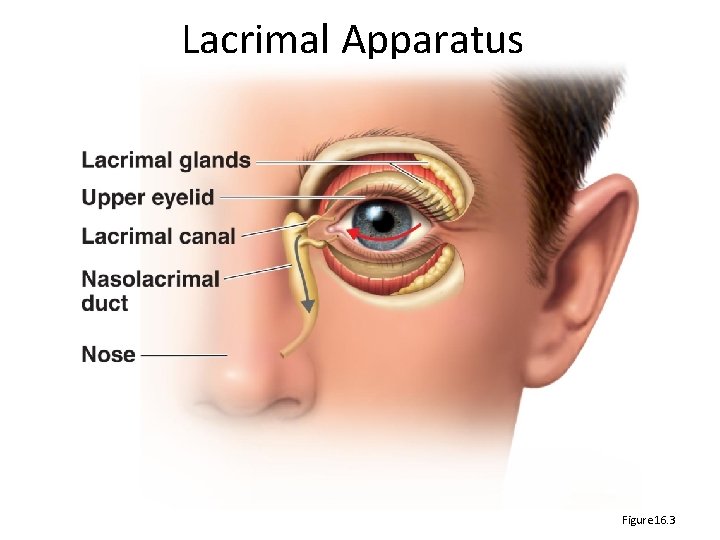
Physical Barrier – moving microbes • • Ciliary escalator – move microbes out of lungs Peristalsis ‐ gut Urine and vaginal secretions – flow out of GU tract Lacrimal apparatus – washes eye

Ciliary Escalator (lungs)

Q&A During one year, nosocomial infections occurred in 74 patients in one hospital. All 74 patients were intubated and mechanically ventilated. The infections were caused by Burkholderia cepacia transmitted in nonsterile mouthwash. Why did these patients develop infections while others who used the mouthwash were not infected?

Lacrimal Apparatus Figure 16. 3

First line defenses: antimicrobial secretions • Fungistatic fatty acid in sebum • Salt – on skin what can survive on high salt? • Low p. H why is this helpful – (3– 5) of skin – (1. 2– 3. 0) of gastric juice – Low p. H (3– 5) of vaginal secretions • Lysozyme what does this target – in sweat, tears, saliva, and urine • Other factors – peroxidase and transferin in saliva which does what?

lysozyme • Where have you seen this enzyme before? – Phage infections – injection and lysis! – Secreted by normal microbiota to discourage interlopers • What does it do? – Hydrolyzes peptidoglycan – link NAG to NAM – WHY does this make SENSE • Where is it found? – Sweat, tears, saliva, mucus, blood, tissue fluids

peroxidase • What does it do? – Oxidizes things using H 2 O 2 – creates toxic oxygen species – General reaction: reduced acceptor + H 2 O 2 → oxidized acceptor + H 2 O – Specific examples: • thiocyanate (SCN−) → hypothiocyanite (OSCN−) • bromide (Br−) → hypobromite (Br. O−) • iodide (I−) → hypoiodite (IO−) • Where is it found? – Saliva, milk, respiratory secretions

Others? • • Yes Lactoferrin Transferrin defensins

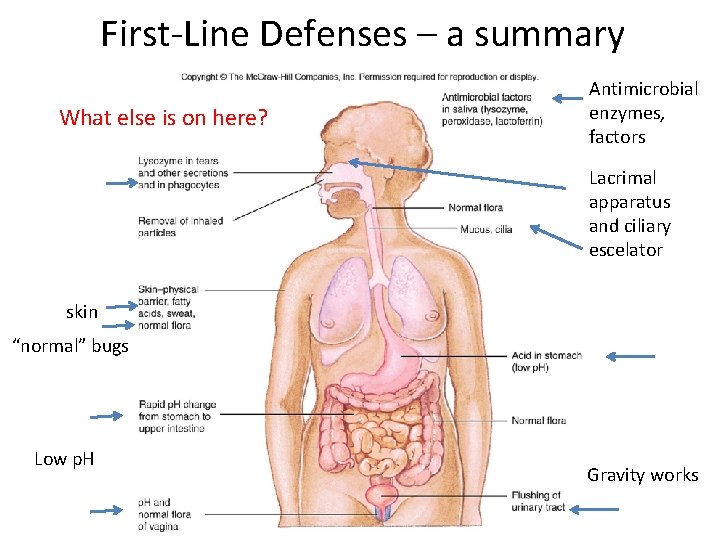
First‐Line Defenses – a summary What else is on here? Antimicrobial enzymes, factors Lacrimal apparatus and ciliary escelator skin “normal” bugs Low p. H Gravity works

First line defenses ‐ Normal Microbiota • Competitively exclude pathogens – Cover binding sites, consume nutrients • Alter the environment – Make wastes, antimicrobial compounds, toxins • Commensal microbiota: – One organism (microbe) benefits; other (host) unharmed – May be opportunistic pathogens • Antibiotics disrupt normal microbiota – Allow pathogens or opportunistic pathogens to take hold

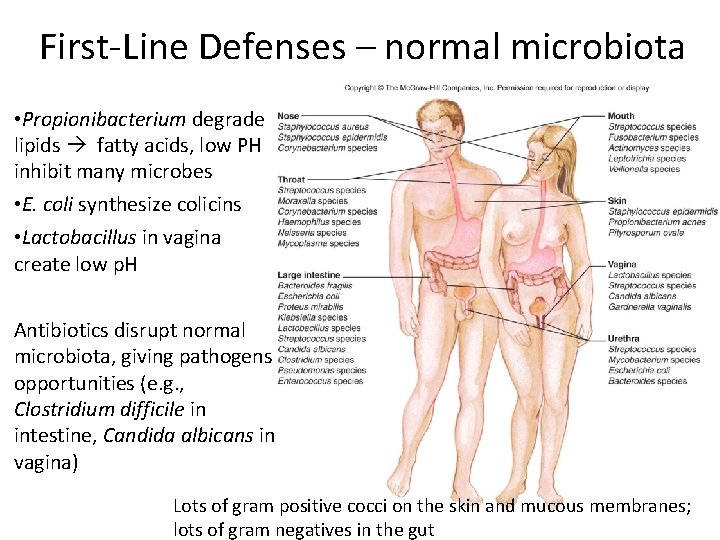
First‐Line Defenses – normal microbiota • Propionibacterium degrade lipids fatty acids, low PH inhibit many microbes • E. coli synthesize colicins • Lactobacillus in vagina create low p. H Antibiotics disrupt normal microbiota, giving pathogens opportunities (e. g. , Clostridium difficile in intestine, Candida albicans in vagina) Lots of gram positive cocci on the skin and mucous membranes; lots of gram negatives in the gut

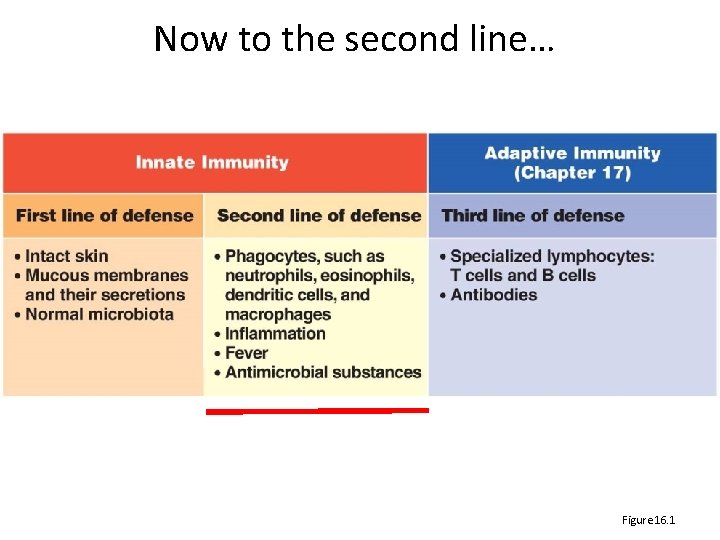
Now to the second line… Figure 16. 1

Goals of the second line • Recognition of “us” vs “them” and safe vs danger • Pattern recognition – Molecules unique to pathogens – Molecules indicating tissue damage – Binding of receptors

Second line of defense • • • Cells of the immune system Circulation ‐ blood and lymph Process of inflammation Fever Antimicrobial proteins in circulation

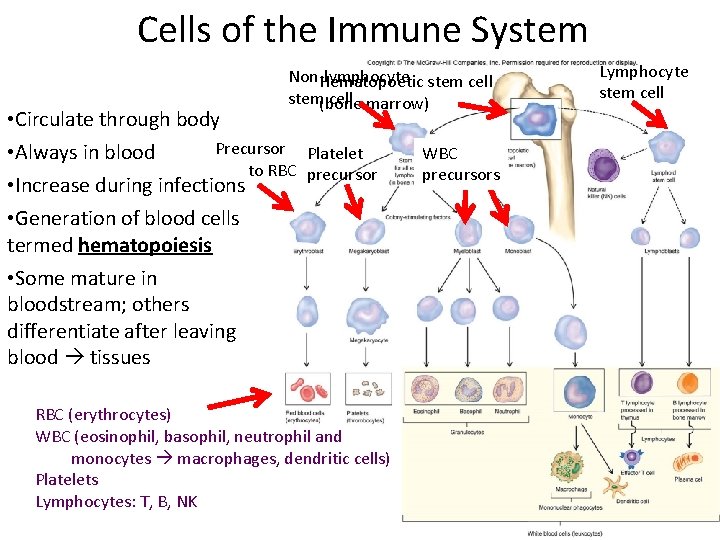
Cells of the Immune System Non‐lymphocyte Hematopoetic stem cell (bone marrow) • Circulate through body Precursor • Always in blood to RBC • Increase during infections • Generation of blood cells termed hematopoiesis • Some mature in bloodstream; others differentiate after leaving blood tissues Platelet precursor RBC (erythrocytes) WBC (eosinophil, basophil, neutrophil and monocytes macrophages, dendritic cells) Platelets Lymphocytes: T, B, NK WBC precursors Lymphocyte stem cell

What are these for? • • Red blood cell Platelet White blood cell Macrophage Dendritic cell Natural killer T cell B cell

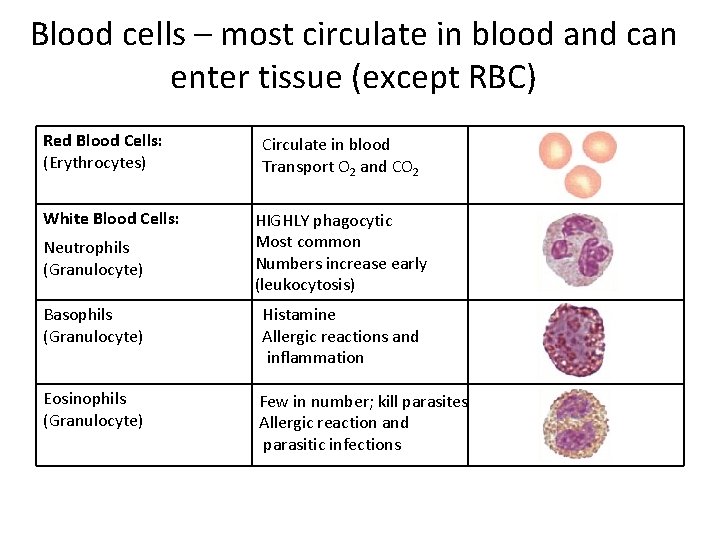
Blood cells – most circulate in blood and can enter tissue (except RBC) Red Blood Cells: (Erythrocytes) Function? Circulate in blood Transport O 2 and CO 2 White Blood Cells: HIGHLY phagocytic Most common Numbers increase early (leukocytosis) Neutrophils (Granulocyte) Basophils (Granulocyte) Histamine Allergic reactions and inflammation Eosinophils (Granulocyte) Few in number; kill parasites Allergic reaction and parasitic infections

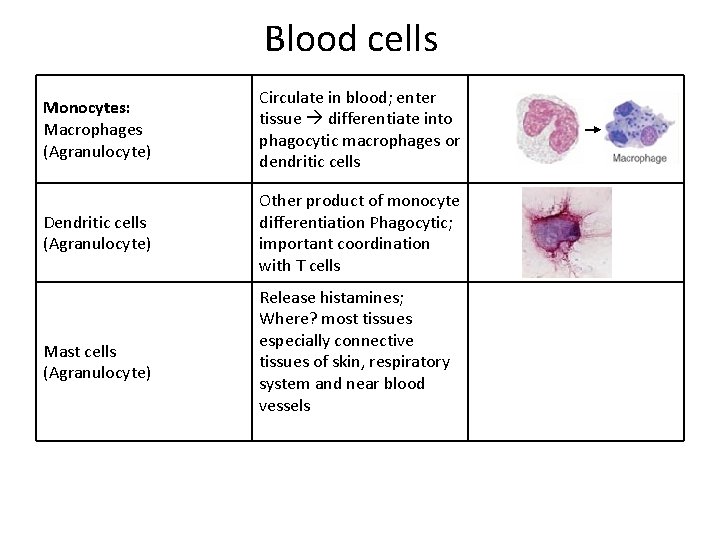
Blood cells Monocytes: Macrophages (Agranulocyte) Circulate in blood; enter tissue differentiate into phagocytic macrophages or dendritic cells Dendritic cells (Agranulocyte) Other product of monocyte differentiation Phagocytic; important coordination with T cells Lymphocytes: Natural killer cells (Agranulocyte ‐ Mast cells lymphocyte) (Agranulocyte) Release histamines; Where? most tissues Destroy target cells especially connective tissues of skin, respiratory system and near blood vessels

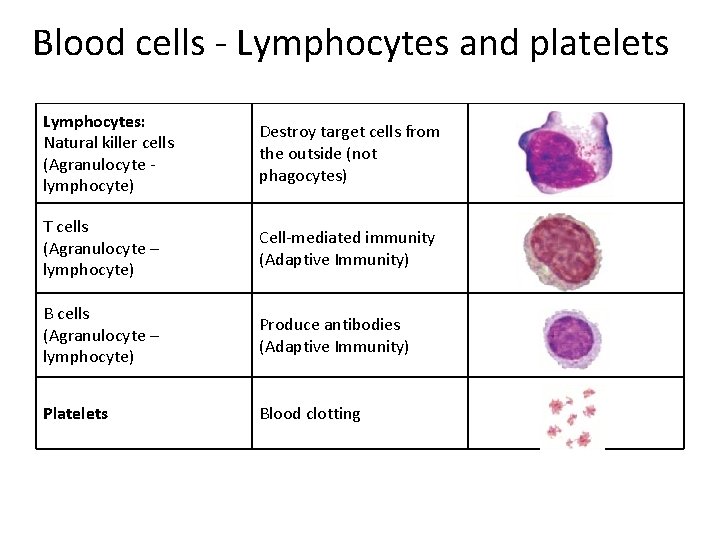
Blood cells ‐ Lymphocytes and platelets Lymphocytes: Natural killer cells (Agranulocyte ‐ lymphocyte) Destroy target cells from the outside (not phagocytes) T cells (Agranulocyte – lymphocyte) Cell‐mediated immunity (Adaptive Immunity) B cells (Agranulocyte – lymphocyte) Produce antibodies (Adaptive Immunity) Platelets Blood clotting

Differential White Cell Count • % each type white cells in a sample of 100 Neutrophils 60– 70% Basophils 0. 5– 1% Eosinophils 2– 4% Monocytes 3– 8% Lymphocytes 20– 25%

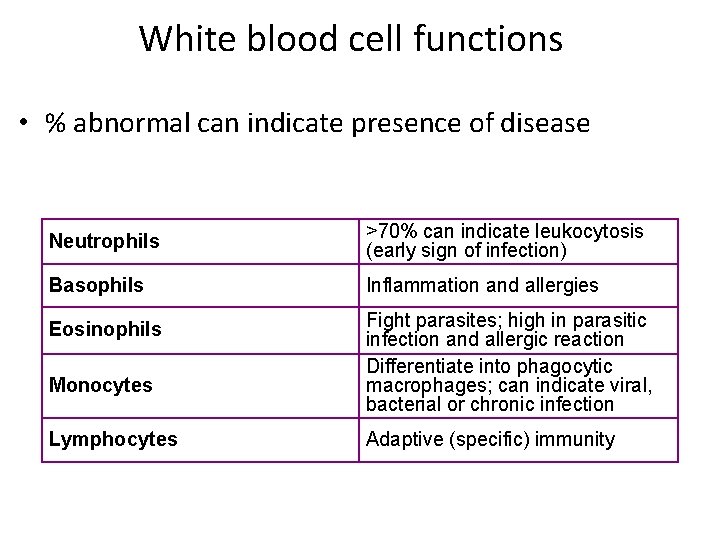
White blood cell functions • % abnormal can indicate presence of disease Neutrophils >70% can indicate leukocytosis (early sign of infection) Basophils Inflammation and allergies Eosinophils Fight parasites; high in parasitic infection and allergic reaction Differentiate into phagocytic macrophages; can indicate viral, bacterial or chronic infection Monocytes Lymphocytes Adaptive (specific) immunity

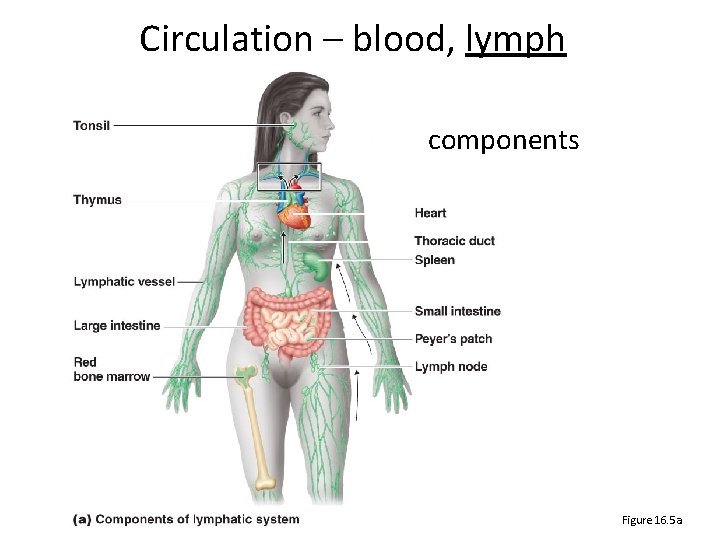
Circulation – blood, lymph components Figure 16. 5 a

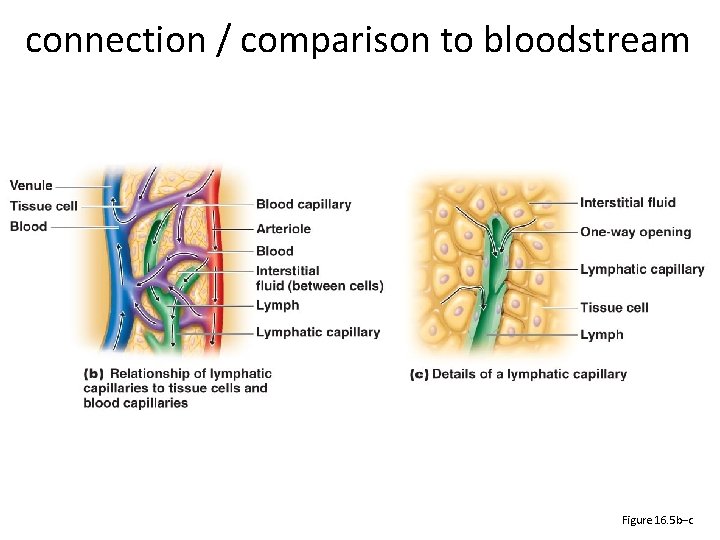
connection / comparison to bloodstream Figure 16. 5 b–c

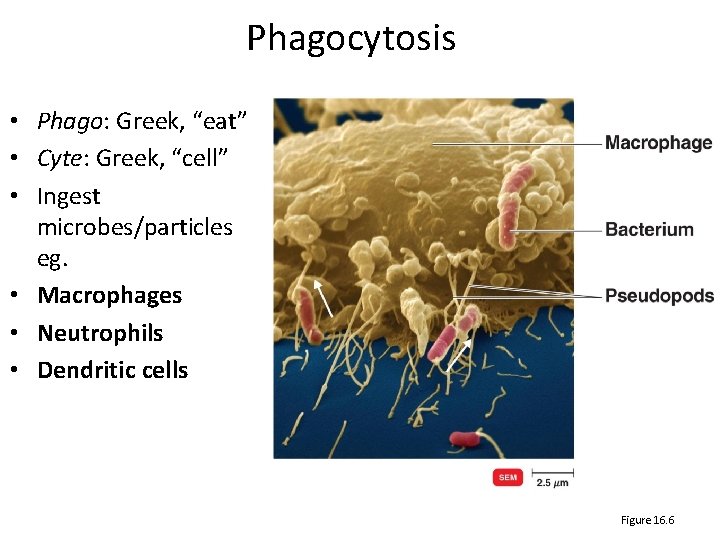
Phagocytosis • Phago: Greek, “eat” • Cyte: Greek, “cell” • Ingest microbes/particles eg. • Macrophages • Neutrophils • Dendritic cells Figure 16. 6

A demonstration • https: //www. youtube. com/watch? v=VAh. M 9 O x. ZDk. U

Phagocytes ‐ macrophages THE INCREDIBLE HULK (with apologies for the specific cultural reference…. ) Damaging to tissues; so usually inactivated Activated by T cells (cooperation innate ‐adaptive immunity) Engulf and destroy microbes OR If fail to destroy microbes, many macrophages fuse to form granulomas to isolate organisms that can’t be destroyed (eg. tuberculosis) lesions, reservoir

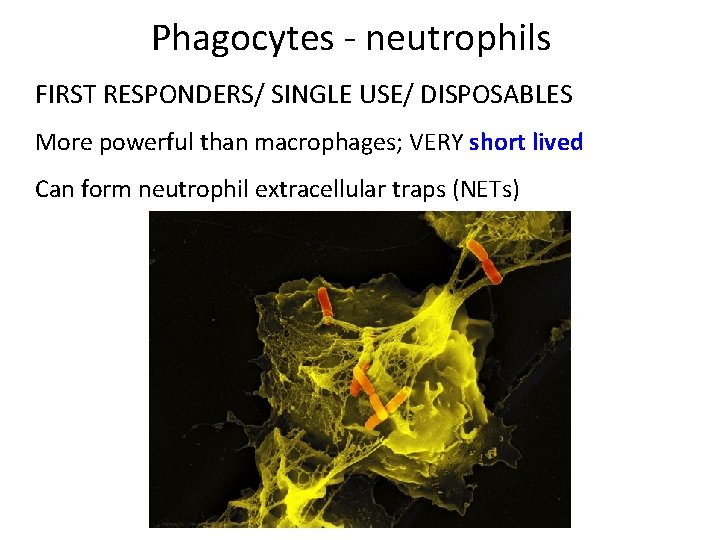
Phagocytes ‐ neutrophils FIRST RESPONDERS/ SINGLE USE/ DISPOSABLES More powerful than macrophages; VERY short lived Can form neutrophil extracellular traps (NETs)

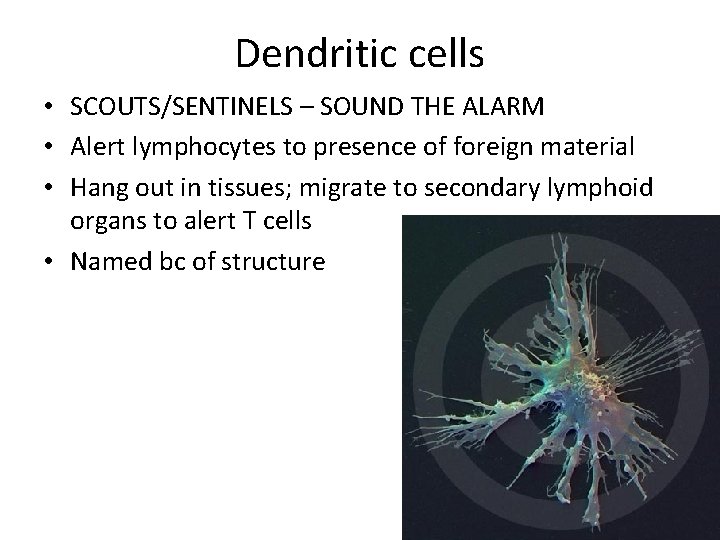
Dendritic cells • SCOUTS/SENTINELS – SOUND THE ALARM • Alert lymphocytes to presence of foreign material • Hang out in tissues; migrate to secondary lymphoid organs to alert T cells • Named bc of structure

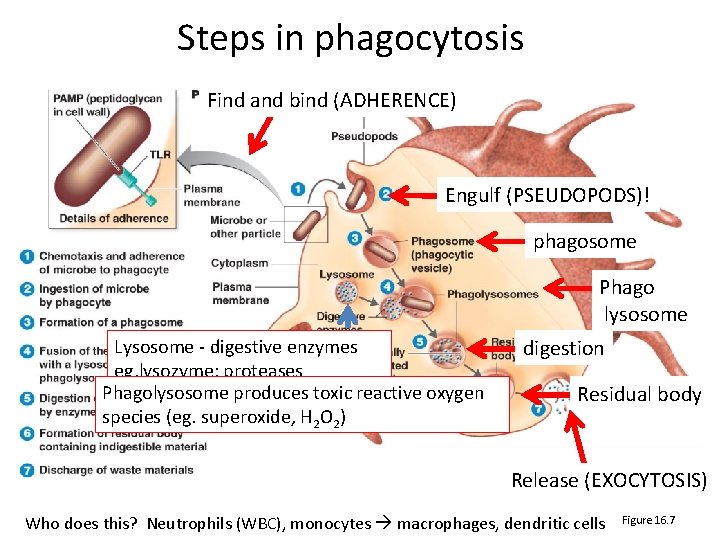
Steps in phagocytosis Find and bind (ADHERENCE) Engulf (PSEUDOPODS)! phagosome Phago lysosome Lysosome ‐ digestive enzymes eg. lysozyme; proteases Phagolysosome produces toxic reactive oxygen species (eg. superoxide, H 2 O 2) digestion Residual body Release (EXOCYTOSIS) Who does this? Neutrophils (WBC), monocytes macrophages, dendritic cells Figure 16. 7

Are phagocytes always successful? • What helps some bacteria avoid being eaten? • HINT : remember bacterial structures lab • What would you do?

Microbial Evasion of Phagocytosis Inhibit adherence: M protein, capsules Streptococcus pyogenes, S. pneumoniae Kill phagocytes: Leukocidins Staphylococcus aureus Lyse phagocytes: MAC attack (membrane attack complex) Listeria monocytogenes Escape phagosome Shigella, Rickettsia Prevent phagosome-lysosome HIV, Mycobacterium tuberculosis fusion (granuloma formation) Survive in phagolysosome Coxiella burnettii

How do they get there? (eg. neutrophil migration) https: //www. youtube. com/watch? v=0 Tv. Tyj 5 FAa. Q Figure 16. 8 c

Steps in phagocyte migration 1. circulating in blood 2. endothelial cells receive signals from tissue 3. margination (roll along inside vessel) 4. chemotaxis (chemical attraction) 5. diapedesis (WBC squeezes out between endothelial cells of the blood vessel tissue) • 6. more chemotaxis • • •
![Phagocyte migration a picture Insert Animation Inflammation Overview Steps MORE VIDEOS Margination Phagocyte migration – a picture [Insert Animation Inflammation: Overview, Steps. ] MORE VIDEOS: Margination:](https://slidetodoc.com/presentation_image_h/203e8b44c46579f3852a150b701fac70/image-46.jpg)
Phagocyte migration – a picture [Insert Animation Inflammation: Overview, Steps. ] MORE VIDEOS: Margination: https: //www. youtube. com/watch? v=Xyl. Vh. CR QATk Margination and diapedesis: https: //www. youtube. com/watch? v=R 8 Vzqu. H dw. Zw Figure 16. 8 c

This begs the question • How did the tissue send out those signals?

How do cells communicate • Can cells really talk? • Cell surface proteins – Membrane spanning proteins • Receptors and ligands – “voices” – Chemical signals sent between cells • Adhesion molecules – “hands” – Endothelial cells bind to phagocytes forcing them to roll

Chemical signals • • • Cytokines are the “voices” of the cells Released by one, received by another Recipient has cytokine receptor Can act locally or systemically Groups of cytokines can have a specific effect – Eg. pro‐inflammatory cytokines • Induce changes – Growth, differentiation, migration or death

Types of cytokines • Chemokines – Stimulate chemotaxis • Colony stimulating factors (CSFs) – Growth and differentiation (make more, this kind) • Interferon (IFN) – Control of viral infection, – Active • Interleukins (Ils) – Made by leukocytes; innate and adaptive immunity • Tumor necrosis factor (TNFs) – Inflammation and apoptosis (cell suicide)

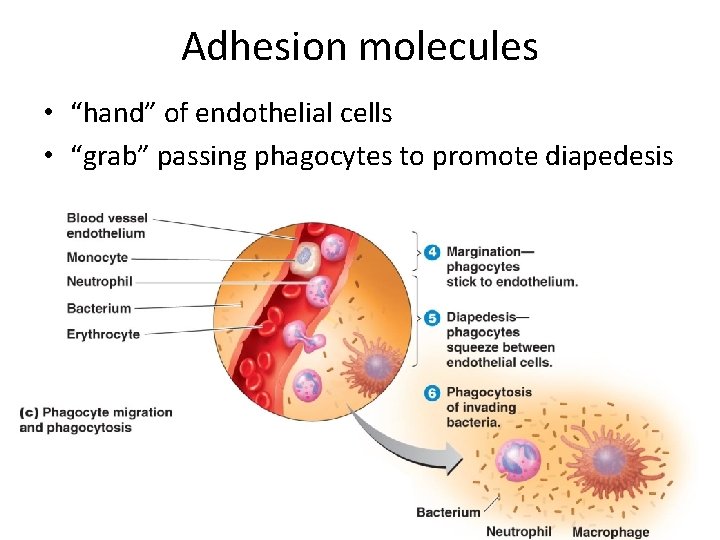
Adhesion molecules • “hand” of endothelial cells • “grab” passing phagocytes to promote diapedesis

An Overview of the Body’s Defenses ‐ what is inflammation? Figure 16. 1

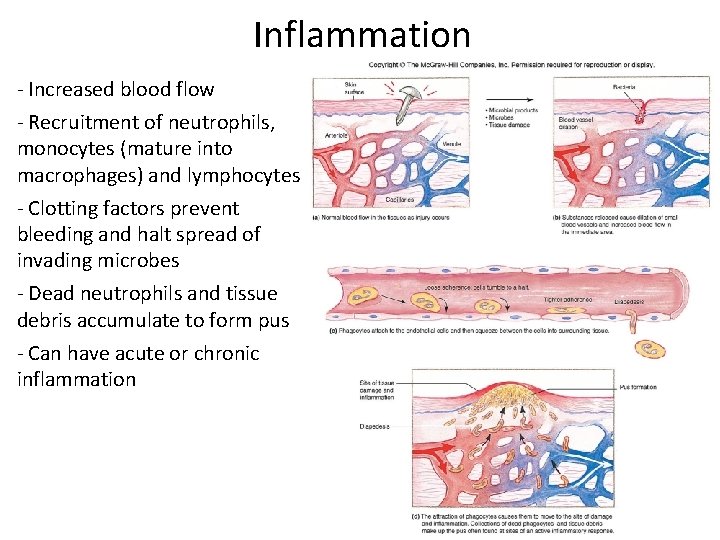
Inflammation ‐ Increased blood flow ‐ Recruitment of neutrophils, monocytes (mature into macrophages) and lymphocytes ‐ Clotting factors prevent bleeding and halt spread of invading microbes ‐ Dead neutrophils and tissue debris accumulate to form pus ‐ Can have acute or chronic inflammation

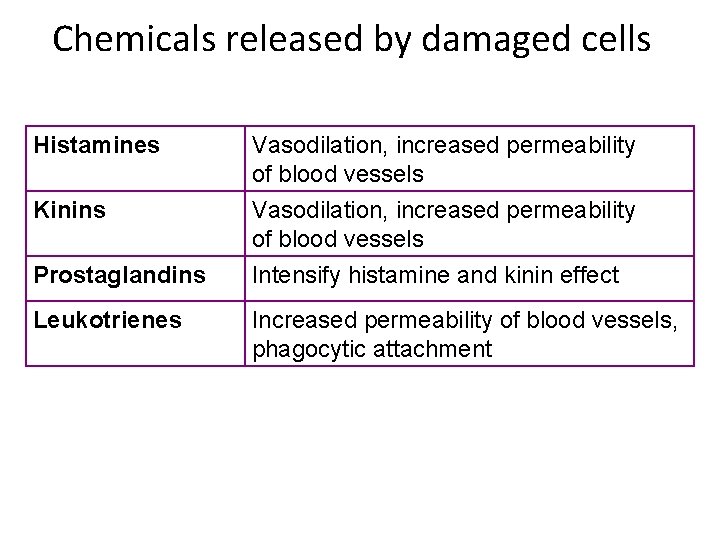
Inflammation ‐ hallmarks • Acute‐phase proteins activated – (complement, cytokines) • Vasodilation – (histamine, kinins, prostaglandins, leukotrienes) • Effects – Redness – Swelling (edema) – Pain – Heat

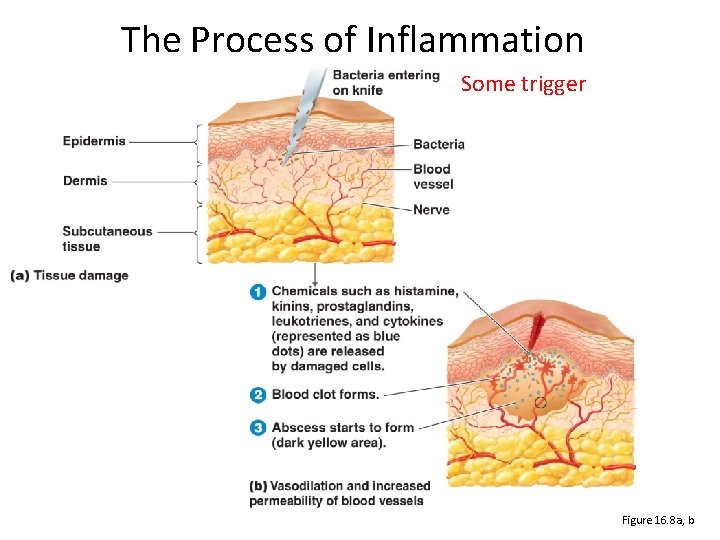
The Process of Inflammation Some trigger Figure 16. 8 a, b

Chemicals released by damaged cells Histamines Vasodilation, increased permeability of blood vessels Kinins Vasodilation, increased permeability of blood vessels Intensify histamine and kinin effect Prostaglandins Leukotrienes Increased permeability of blood vessels, phagocytic attachment
![Phagocyte Migration Insert Animation Inflammation Overview Steps Figure 16 8 c Phagocyte Migration [Insert Animation Inflammation: Overview, Steps. ] Figure 16. 8 c](https://slidetodoc.com/presentation_image_h/203e8b44c46579f3852a150b701fac70/image-57.jpg)
Phagocyte Migration [Insert Animation Inflammation: Overview, Steps. ] Figure 16. 8 c

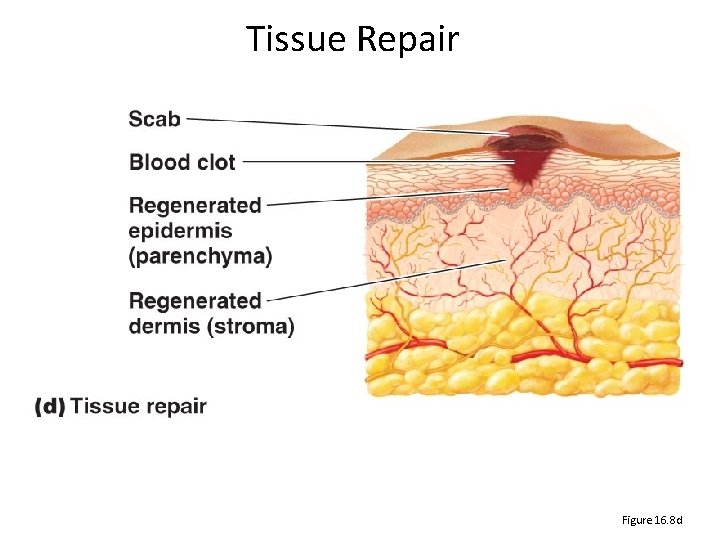
Tissue Repair Figure 16. 8 d

Inflammation is not fever • What’s the difference?

Fever • Abnormally high body temperature • Hypothalamus normally set at 37°C • Gram‐negative endotoxin cause phagocytes to release interleukin– 1 (IL– 1) • Hypothalamus releases prostaglandins that reset the hypothalamus to a high temperature • Body increases rate of metabolism and shivering which raise temperature • Vasodilation, sweating: Body temperature falls (crisis)

Fever • Advantages – Increases transferrins – Increases IL– 1 activity – Produces Interferon • Disadvantages – Tachycardia – Acidosis – Dehydration – 44– 46°C fatal

Antimicrobial substances • • Complement Interferons Transferrins Antimicrobial proteins (AMPs)

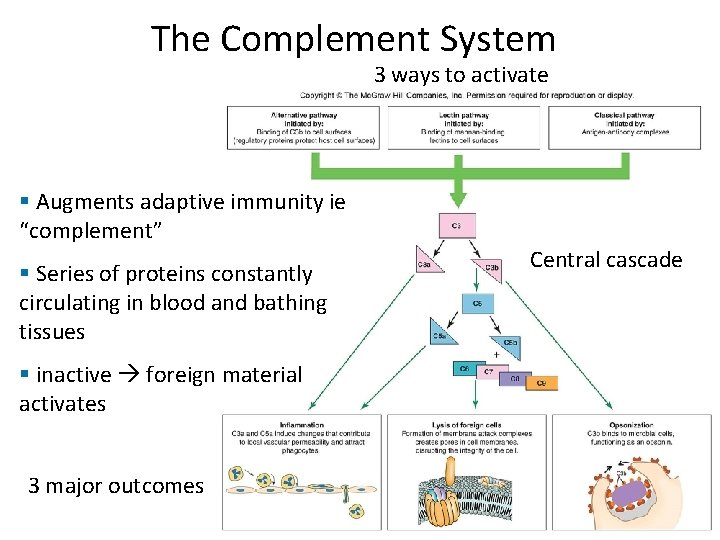
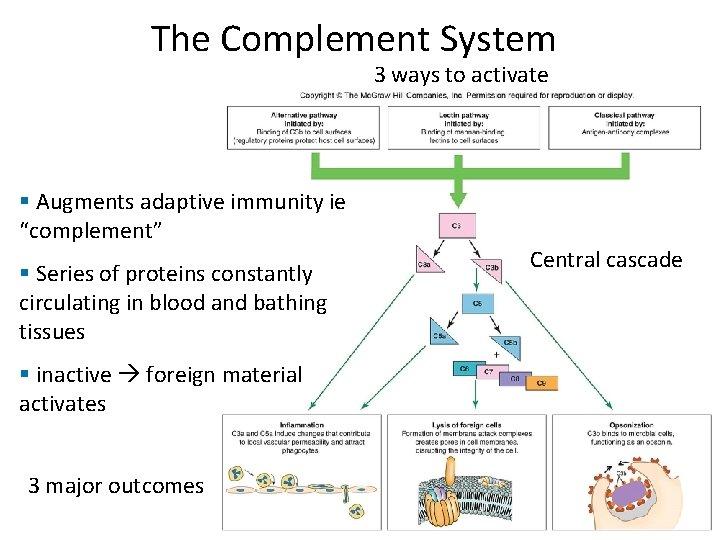
The Complement System 3 ways to activate § Augments adaptive immunity ie “complement” § Series of proteins constantly circulating in blood and bathing tissues § inactive foreign material activates 3 major outcomes Central cascade

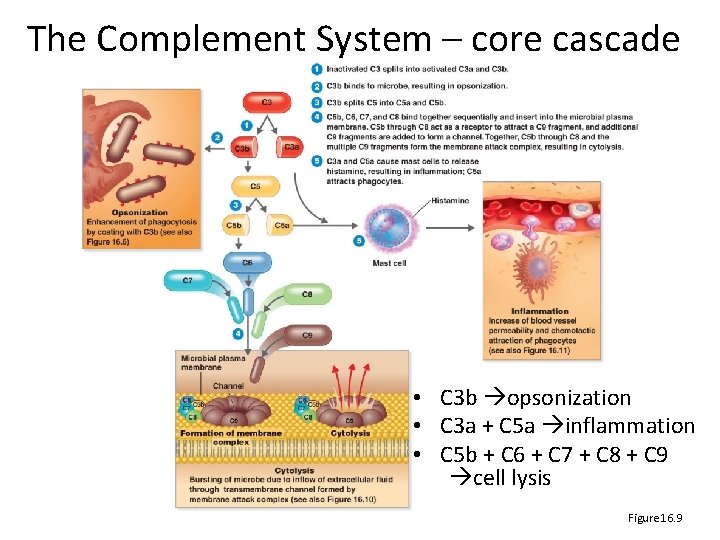
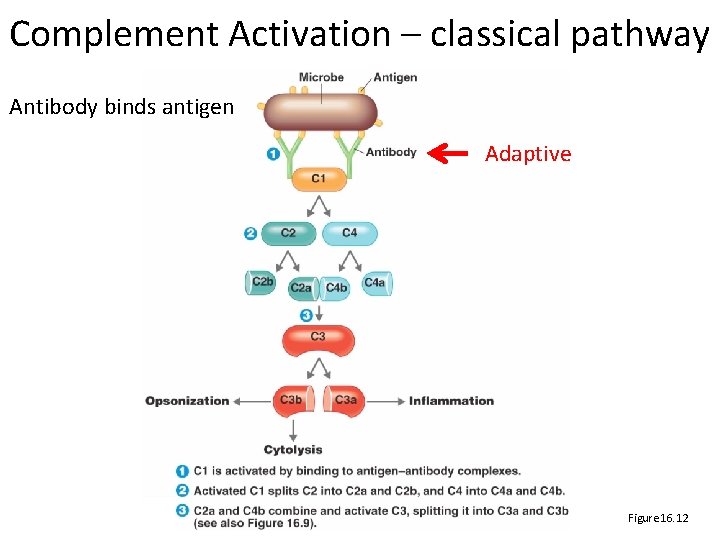
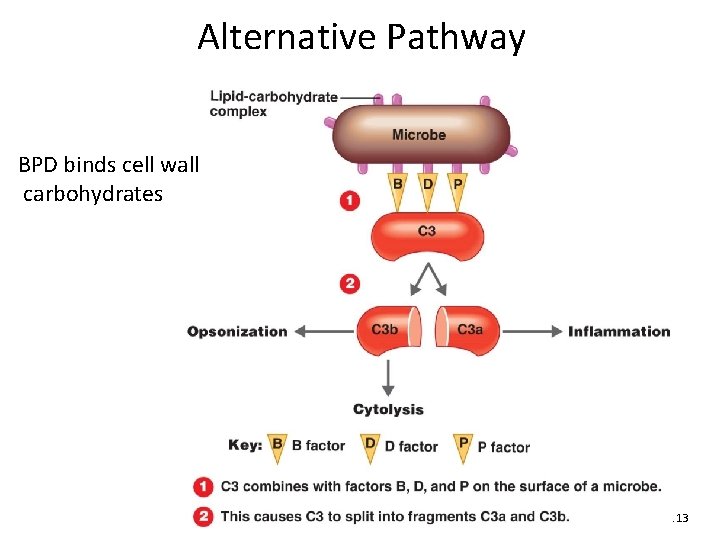
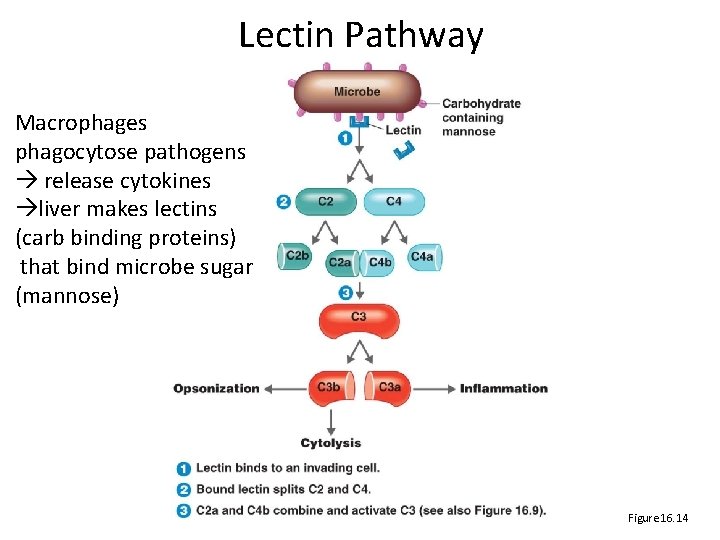
The Complement System • Normally inactive – Serum proteins normally inactive, circulating – Activated rapidly, transiently in a cascade • Activated by – Antigen‐antibody reaction (classic) – Proteins C 3, B, D, P binding a pathogen (alternative) – Lectins binding mannose on a pathogen (lectin) • Effects of activation – C 3 b causes opsonization – C 3 a + C 5 a cause inflammation – C 5 b + C 6 + C 7 + C 8 + C 9 cause cell lysis

The Complement System – core cascade • C 3 b opsonization • C 3 a + C 5 a inflammation • C 5 b + C 6 + C 7 + C 8 + C 9 cell lysis Figure 16. 9

Complement activation • How to get to C 3

Complement Activation – classical pathway Antibody binds antigen Adaptive Figure 16. 12

Alternative Pathway BPD binds cell wall carbohydrates Figure 16. 13

Lectin Pathway Macrophages phagocytose pathogens release cytokines liver makes lectins (carb binding proteins) that bind microbe sugar (mannose) Figure 16. 14

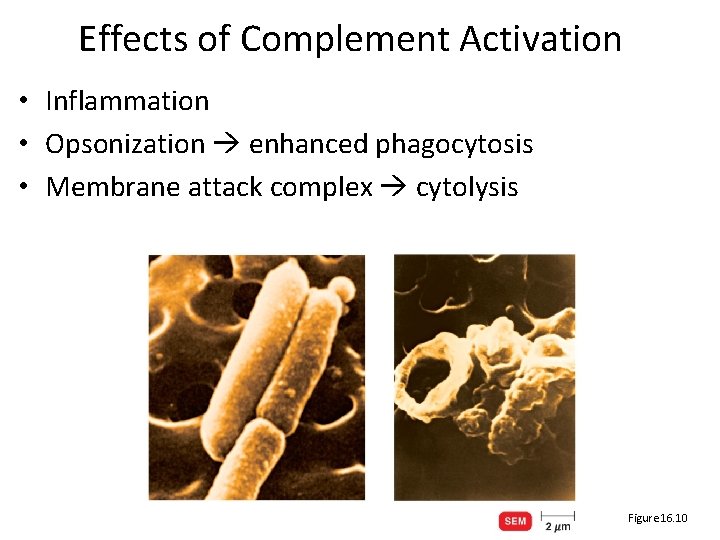
Effects of Complement Activation • Inflammation • Opsonization enhanced phagocytosis • Membrane attack complex cytolysis Figure 16. 10

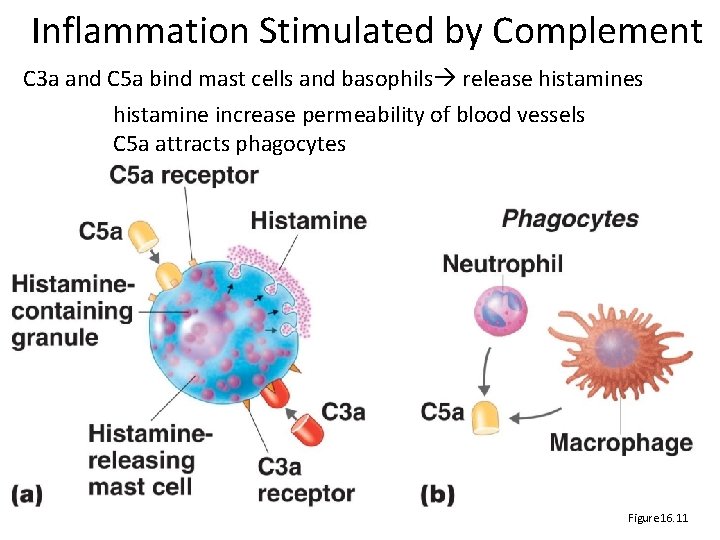
Inflammation Stimulated by Complement C 3 a and C 5 a bind mast cells and basophils release histamines histamine increase permeability of blood vessels C 5 a attracts phagocytes Figure 16. 11

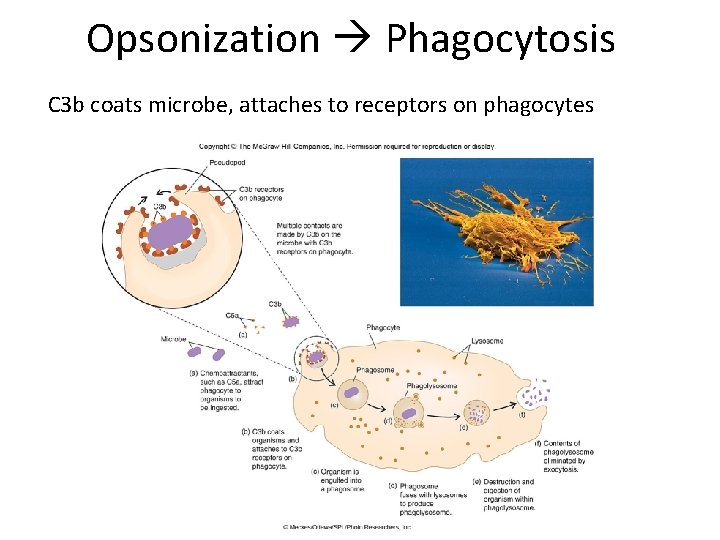
Opsonization Phagocytosis C 3 b coats microbe, attaches to receptors on phagocytes

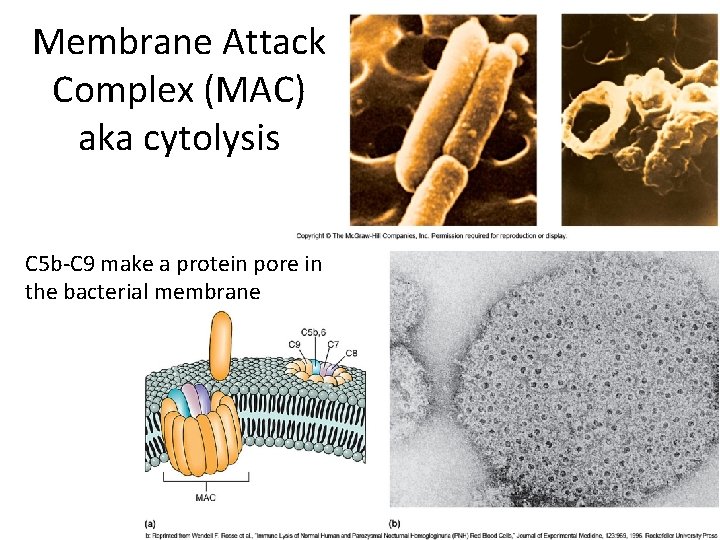
Membrane Attack Complex (MAC) aka cytolysis C 5 b‐C 9 make a protein pore in the bacterial membrane

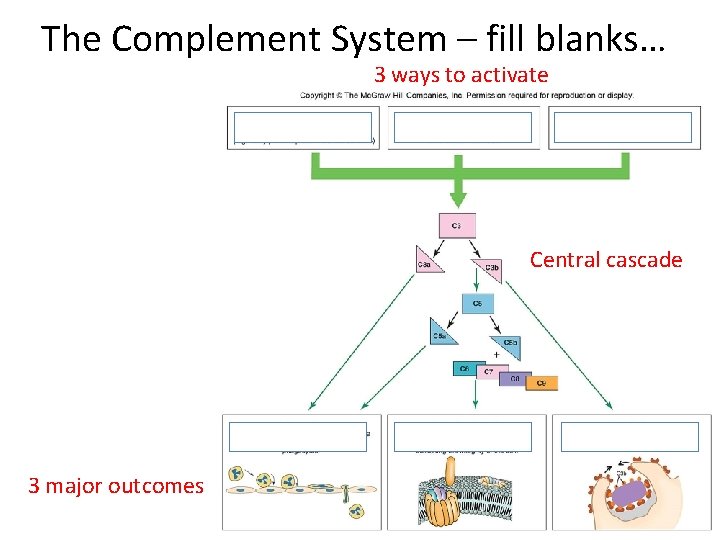
The Complement System – fill blanks… 3 ways to activate Central cascade 3 major outcomes

The Complement System 3 ways to activate § Augments adaptive immunity ie “complement” § Series of proteins constantly circulating in blood and bathing tissues § inactive foreign material activates 3 major outcomes Central cascade

So… • A patient with a genetic disorder resulting in defective complement would be most affected by a mutation in which of these? – C 1 – C 3 – C 5 – C 9

Subverting the complement system • Capsules prevent complement activation – Sialic acid inhibits MAC formation and opsonization – (also found in lipid A of LPS of some Gram negatives) • Surface lipid‐carbohydrates prevent membrane attack complex (MAC) formation – (e. g. , Salmonella with long O polysaccharide of LPS) • Enzymatic digestion – Gram positive cocci release enzyme that degrades C 5 a • Some viruses can attach to complement receptors on body cells to initiate their life cycle

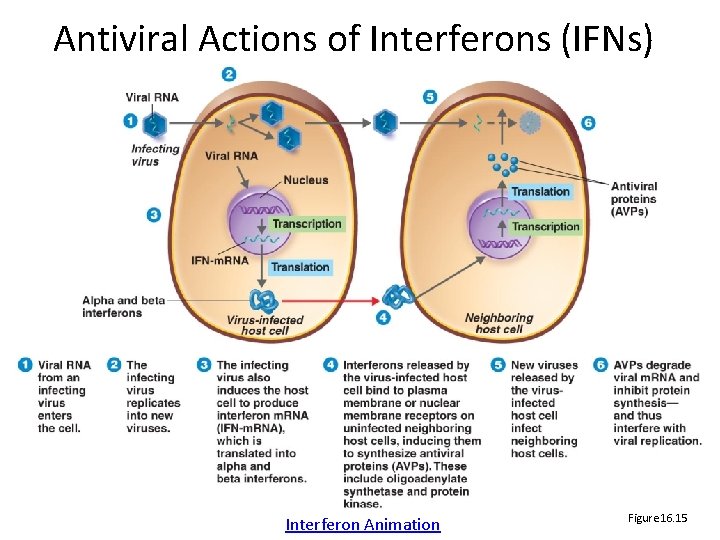
Interferons (IFNs) • IFN‐ and IFN‐ : produced by virally‐infected cells in small amounts, diffuse very localy and cause neighbor cells to produce antiviral proteins – enzymes that inhibit viral replication • Gamma IFN: produced by lymphocytes; induces neutrophils & macrophages to phagocytize bacteria

Antiviral Actions of Interferons (IFNs) Interferon Animation Figure 16. 15

Innate Immunity • Transferrins – Bind serum iron – Deprive microbes • Antimicrobial peptides – Lyse bacterial cells – Short chains ~12‐ 50 a. a. – Over 600 AMPs known so far – Activity against viruses, bacteria, fungi, parasites – Toll‐like receptors activate cells to produce

Pathogens fight back • Transferrins • Antimicrobial peptides – Bind serum iron – Deprive microbes • Pathogens – Secrete siderophores – Directly uptake human iron‐binding proteins – Release hemolysin lyse RBC (eg. S. pyogenes) – Lyse bacterial cells – Short chains ~12‐ 50 a. a. – >600 AMPs known so far – Activity against viruses, bacteria, fungi, parasites – Toll‐like receptors activate cells to produce


And now for some problem solving

Which of the following is the best definition for innate immunity? A. A response that requires specialized cells with “memory” B. A response that is directed only against a particular microbe C. A system that protects us against trauma and disease D. Several defenses present in all humans from the time of birth

Application question Smoking cigarettes is known to paralyze the cilia that line the upper respiratory tract. What effect will this have on the immune system? a. Pathogens not removed from airway b. Adaptive immune system compromised c. Innate immune system compromised d. A and B e. A and C

A word about Salmonella • Salmonella species are Gram‐negative, flagellated facultatively anaerobic bacilli characterized by O, H, and Vi antigens. There are over 1800 known serovars which current classification considers to be separate species.

Group Activity Try to explain the symptoms of Salmonella enterica infection based on this information and knowledge of innate immune response • Usually ingested (contaminated food or fecal‐‐‐oral) • Survive gastric juice, mucous, lactoferrin, lysozyme • Bacterial cells enter the epithelial cells of the intestine • Vomiting, nausea, diarrhea, pain, gastrointestinal inflammation, fever • Cooking prevents illness

answers Meat and dairy may harbor Salmonella since they are in animal intestine Initial response ‐mucous and AMP production (antimicrobial peptide) Then, leukocytes come to the intestine to attack bacterial cells but also cause damage to intestinal epithelium causing diarrhea Neutrophils induce inflammatory responses: cytokines Interestingly S typhi cells actually thrive on some of the byproducts of inflammation (ROS) Resistant to many of the AMPs

Which of the following is antiviral? • • • AMPs MAC attack Transferrin Lysozyme Interferon –a Interferon ‐g

Which of the following is antiviral? • • • AMPs ‐ some MAC attack – NO; this attacks cells Transferrin – NO this relates to metabolism Lysozyme Interferon –a Interferon –g – NO; this is different from a, b

PREVIEW!!! • Adaptive immunity – antibodies and antigens

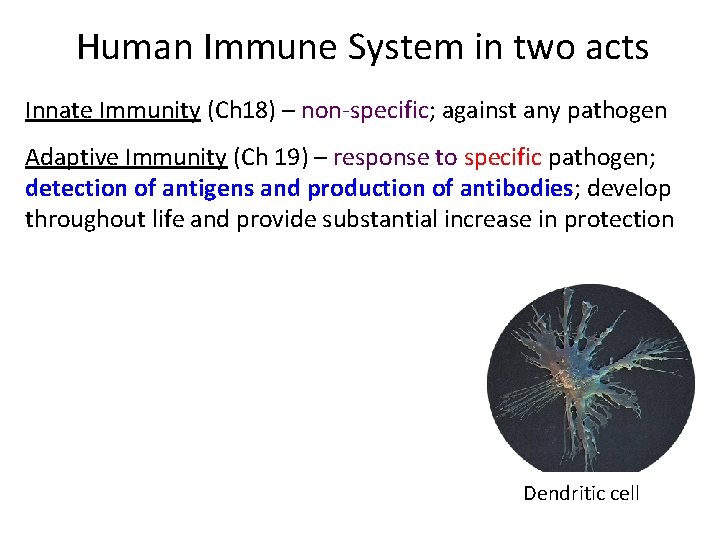
Human Immune System in two acts Innate Immunity (Ch 18) – non‐specific; against any pathogen Adaptive Immunity (Ch 19) – response to specific pathogen; detection of antigens and production of antibodies; develop throughout life and provide substantial increase in protection Dendritic cell

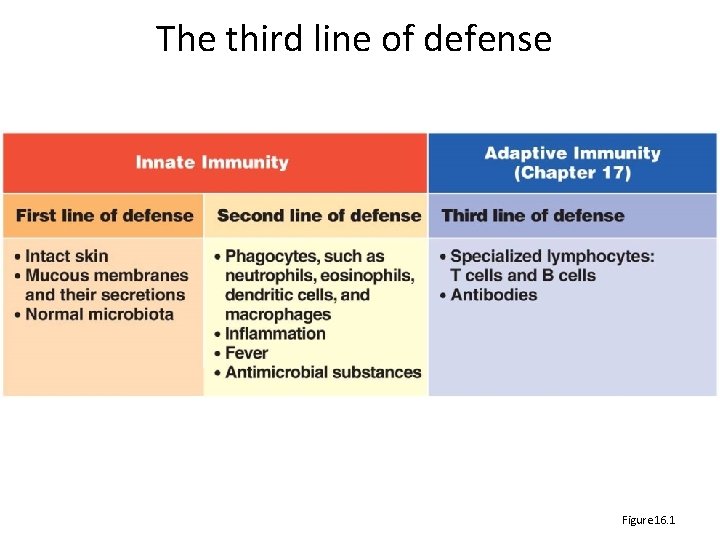
The third line of defense Figure 16. 1

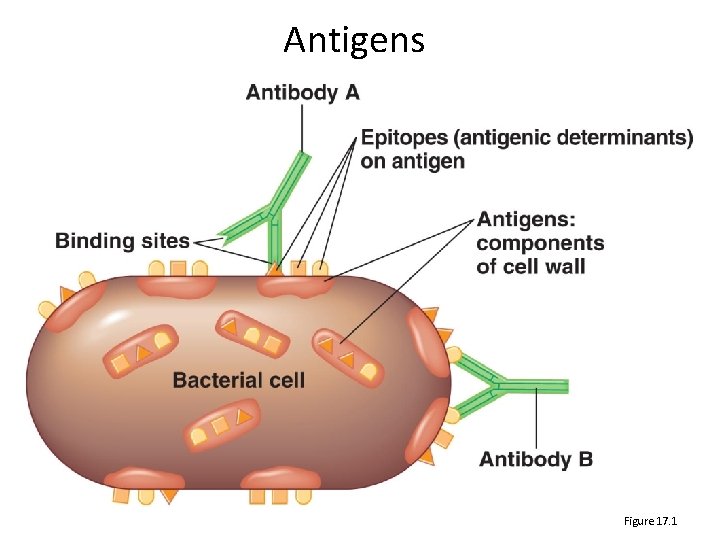
The Nature of Antigens • Antigen (Ag): A substance that causes the body to produce specific antibodies – Typically a protein or polysaccharide (not lipid) – Antibodies (Ab) interact with epitopes aka antigenic determinants, a small part of the antigen

Antigens Figure 17. 1

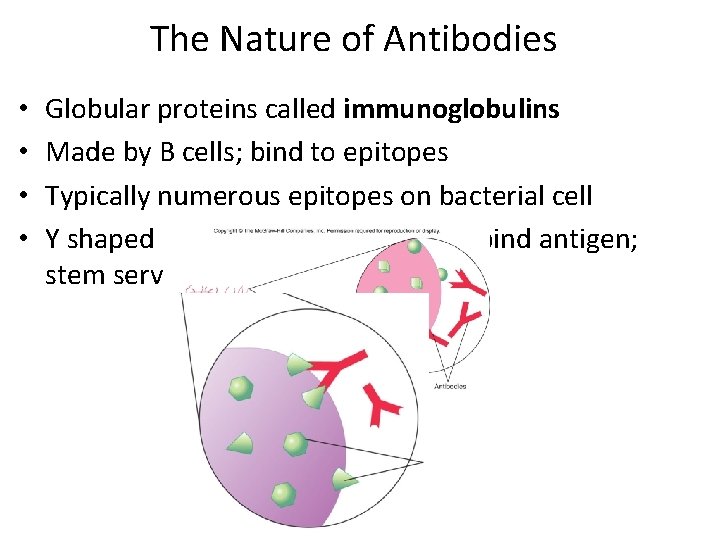
The Nature of Antibodies • • Globular proteins called immunoglobulins Made by B cells; bind to epitopes Typically numerous epitopes on bacterial cell Y shaped proteins; 2 identical arms bind antigen; stem serves as “flag”

Primary and secondary antibodies • That “stem” is animal‐specific • Antibody against antigen X is “primary” • Antibody against stem of primary is “secondary” • Eg. inject rabbit with botulism toxoid primary antibody “anti‐botulism” • Inject primary antibody into mouse secondary antibody “anti‐rabbit” • DRAW on board

ELISA • • • Detect antigen / exposure in patient serum DIRECT INDIRECT SANDWICH Movie!! https: //www. youtube. com/watch? v=n. Njl. BCn p. GZ 4

Direct ELISA • Serum – bind to plastic tube • Add known antibody to the antigen you’re looking for, attached to an enzyme • Wash (will the antibody stick? Why/not? ) • Add substrate for enzyme color • Color is +ve meaning what?

ELISA is a test in your pharmacy… • Examples? • Pregnancy test – Test HCG levels (human chorionic gonadotropin) – Levels high in urine/blood ~10 d after conception – How would you look for this? – DIRECT – use known antibody against HCG