DIPHTHERIA The Past Present the Future Dr Cummings




































































- Slides: 84

DIPHTHERIA The Past, Present & the Future Dr Cummings Henry Consultant Paediatrician DELSUTH

PRE TEST 1. Diphtheria has been eradicated 2. The is a resurgence of diphtheria 3. The mainstay of treatment is antibiotics 4. Vaccination remain the most effective control measure.

The Past Outline n The Present n The future n

n n n Diphtheria, The Past: Introduction Epidemiology Aetio-pathogenesis Immunology Clinical Presentation Complications Differentials Investigations Treatment Prognosis Prevention

Introduction n n An ancient disease described by Hippocrates in the 5 th century BC Plagued Europe & the American colonies in the 18 th century Diphtheria is an acute toxic infectious disease A localized infection of mucous membrane &/or skin May have systemic complications/manifestations

n n Epidemiology Reservoir - Exclusively in humans - Skin infection and skin carriage constitute silent reservoir Mode of spread * primarily by airborne respiratory droplets * direct contact with; -respiratory secretions of infected individuals -exudates from infected skin lesions

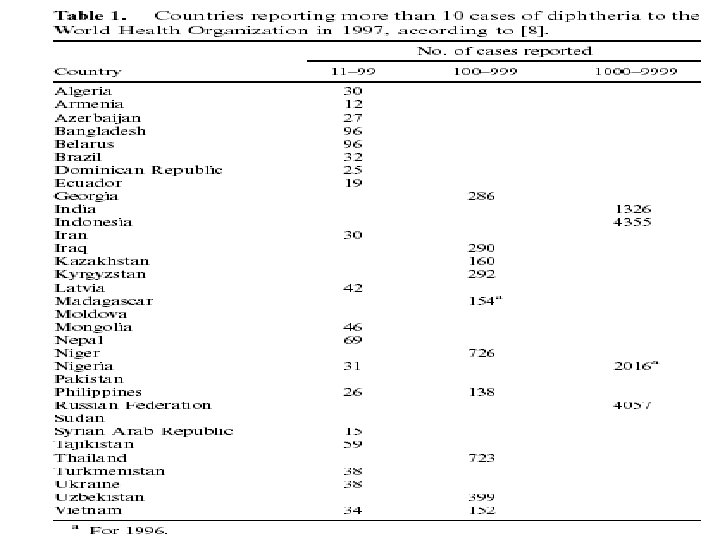
Epidemiology contd. In the U. S - Pre-vaccination era(1920 s) > 115, 000 cases and 10, 000 deaths reported annually - Recently, < 5 cases are reported annually n In Nigeria - 5, 039 cases reported in 1989 - 3, 995 cases in 2000 - 2, 468 cases in 2001 - 312 cases in 2006 (7. 8% of global report) n


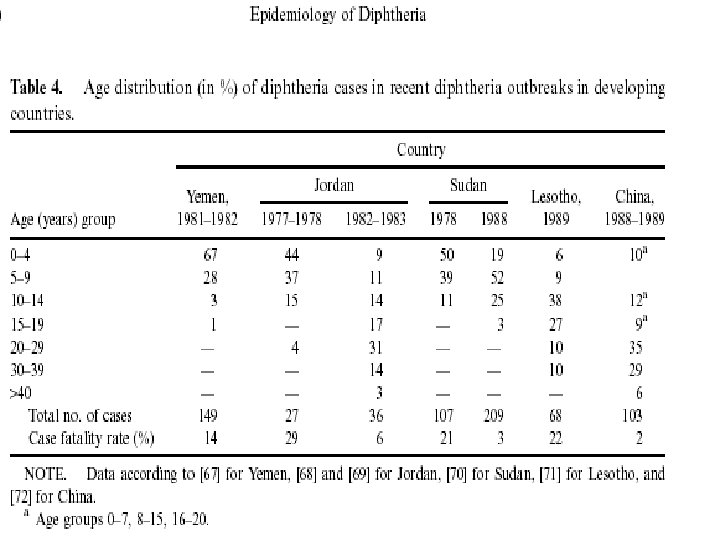
Epidemiology contd. n n Carriers are important in transmission constitute 3 -5% of healthy individuals in endemic region Estimated mortality rates→ 5 -10% (up to 20% in <5 yrs, & > 40 yrs)

Epidemiology contd. n n Sex No significant difference in the incidence in males & females of similar immunization status Age - Commoner in 6 month-12 yrs (esp. in the pre-vaccination era)

Risk factors Incomplete or absent immunization n Low herd immunity n Travel to endemic areas or regions with current epidemic n Immunocompromised states e. g. HIV/AIDS n Low socio-economic status n Poor health care facilities n Overcrowding n

Aetio-pathogenesis Caused by toxigenic Corynebacterium diphtheriae n Types - Corynebacterium diphtheriae * mitis * intermedius * belfanti * gravis - Corynebacterium ulcerans- causes cutaneous disease n

Characteristics Gram positive n Club-shaped bacillus n Aerobic n Non-motile n Non-encapsulated n About 2 -4μm in length n Assume L &/or V configuration to each other n Form a Chinese lettering pattern n

Corynebacterium diphtheria

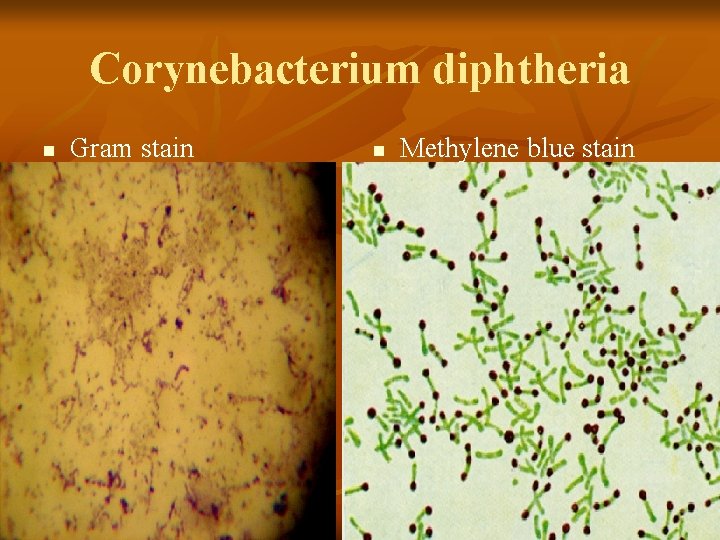
Corynebacterium diphtheria n Gram stain n Methylene blue stain

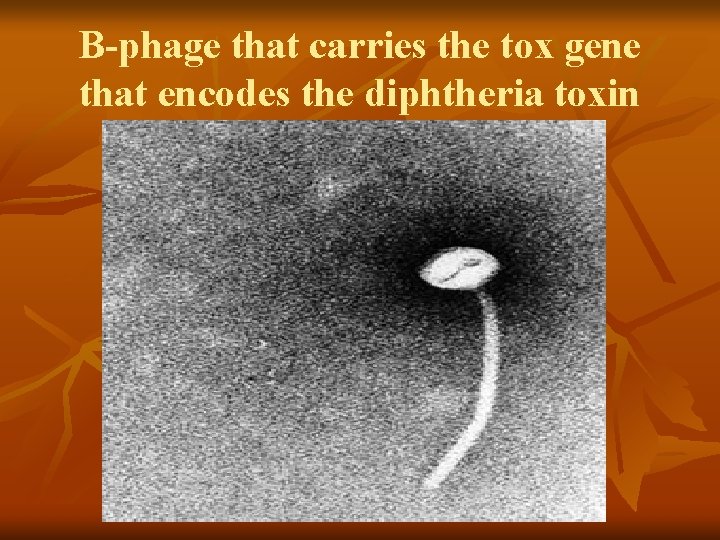
Virulence n n n Depends on the ability to produce the diphtheria toxin-an exotoxin Toxigenicity depends on the presence of a lysogenic bacteriophage Non-toxigenic strain can become toxigenic by coming in contact with toxigenic strains

B-phage that carries the tox gene that encodes the diphtheria toxin

The Exotoxin n n A 62, 000 dalton polypeptide Composed of 2 joined major segments (A and B)

Actions of the Toxin n Segment B bind receptors on susceptible cells and facilitate entrance of segment A Segment A mediates toxic actions: - inactivates RNA translocase - inhibits protein synthesis - causing tissue necrosis n

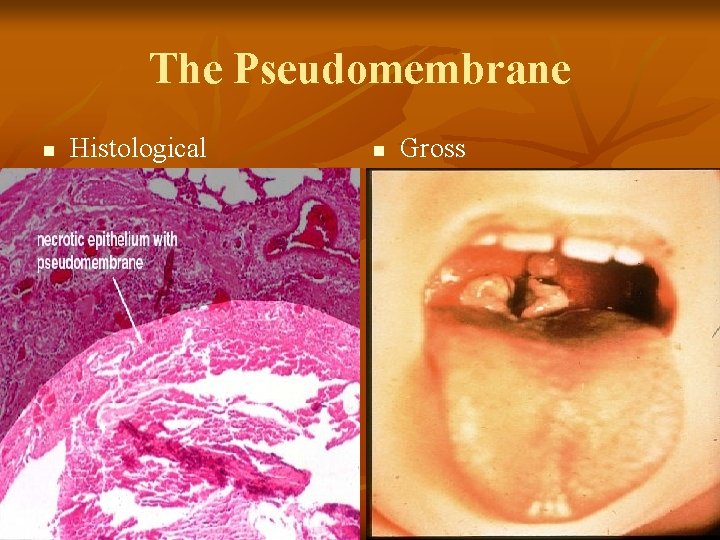
Actions of The Toxin contd. n Formation of pseudomembrane * a dense necrotic coagulum of organism, epithelial cells, fibrin, leucocytes & RBCs * grayish-white or brown in colour

The Pseudomembrane n Histological n Gross

Other effects of the toxin Paralysis of palate & hypopharynx n Systemic absorption: - renal tubules necrosis - thrombocytopenia - cardiomyopathy - demyelination of nerves - paralysis of the diaphragm n The toxin is converted to toxoid (for vaccination) when treated with formalin n

Immunology n Organisms invasion usually remain localized The main immune response is to the exotoxin n Immune response is antibody-mediated n The antibody is of the Ig. G type – Antitoxin n n Immunity does not prevent colonization rather it protects against the effects of the toxin

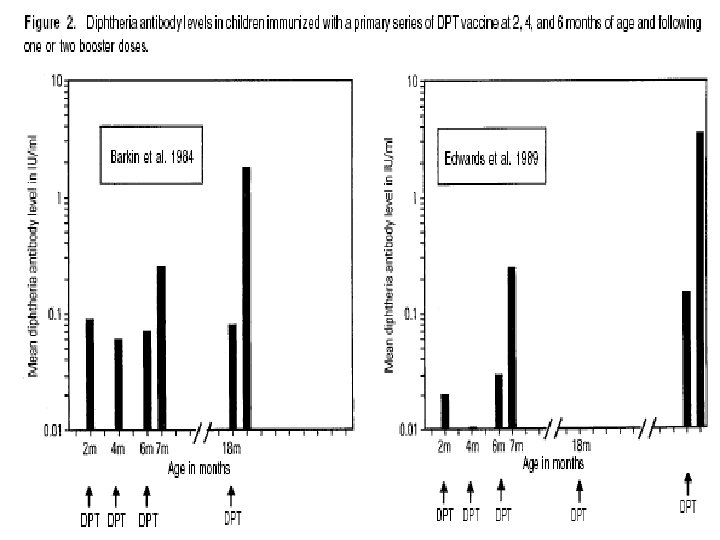
Immunology Contd. Active antibodies production may be induced by: - active disease - carrier state - vaccination with the toxoid n Passive immunity –transplacentally transferred n Immunity was previously thought to be life long n

Assessment of immunity n The Schick test: - Intradermal injection of 0. 1 ml 1: 50 dilution of toxin - positive result: inflammation appearing after 24 -36 hrs & persisting for ≥ 4 days – no antitoxin – no immunity - negative result – has antitoxin - immune

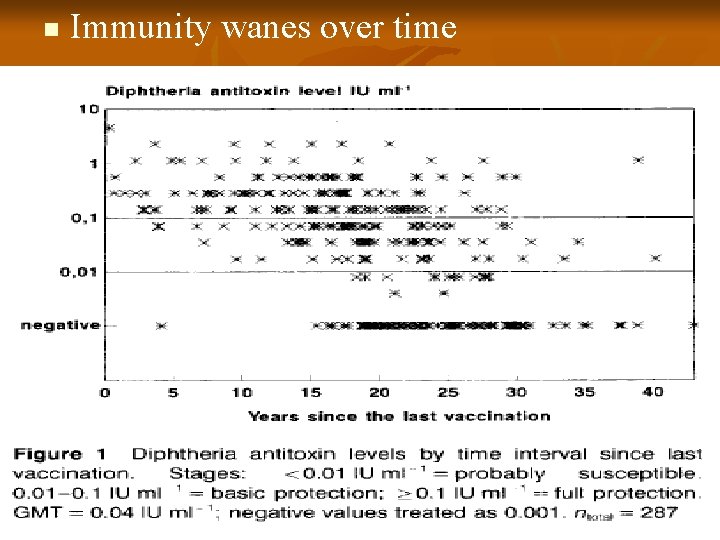
Immunity assessment contd. n Assay of serum level of antitoxin - full protection: ≥ 0. 1 IU/m. L - basic protection: ≥ 0. 01 - <0. 1 IU/m. L - no protection : < 0. 01 IU/m. L N. B: Epidemic outbreak is likely when > 90% of the population has < 0. 01 IU/m. L of antitoxin

Clinical Presentation n Incubation: usually 2 -4 days with a range of 1 -7 days n Classified into: - Respiratory Tract Diphtheria - Non-Respiratory Tract disease - Complicated disease

Respiratory tract diphtheria n Nasal Diphtheria - commoner in infants - little or no constitutional symptoms - serosanguineous nasal discharge - epistaxis

Nasal Diphtheria contd. - - purulent foul smelling discharge - shallow ulcers +/- pseudomembrane - unilateral or bilateral - may persist for several weeks - major source of transmission

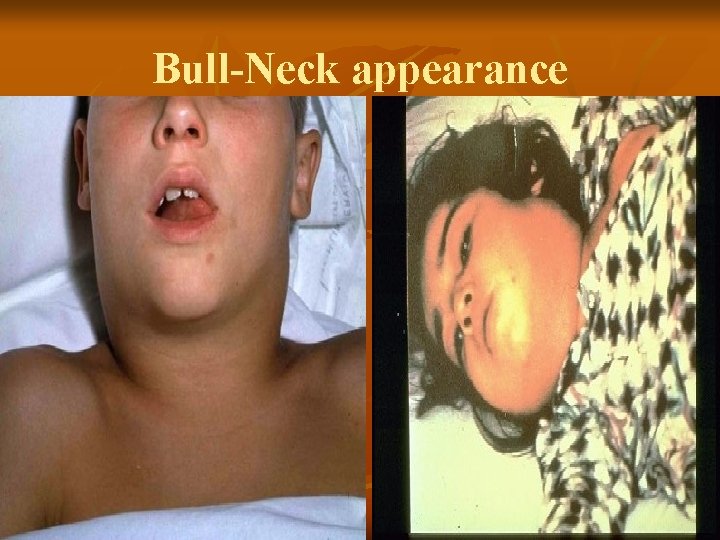
Tonsilo-Pharyngeal Most common (90% of cases) n Malaise n Fever – mild to moderate n Sore throat – drooling, odynophagia +/dysphagia n Bull-neck appearance n Pseudomembrane of variable extent n

Bull-Neck appearance

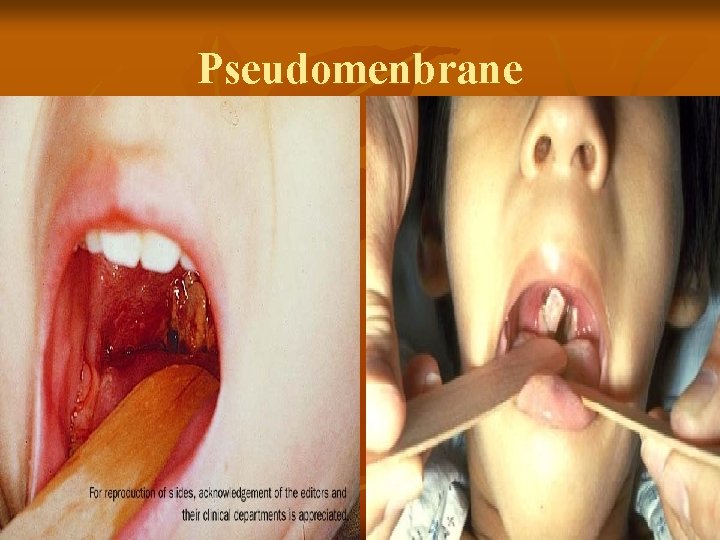
Pseudomenbrane

Laryngeal Diphtheria n Usually an extension of pharyngeal disease n Hoarseness of voice n Cough n Inspiratory stridor

Laryngeal Diphtheria contd. n n Suprasternal, substernal & subcostal recessions Symptoms & signs of sudden airway obstruction n Sudden death n May require intubation/tracheotomy

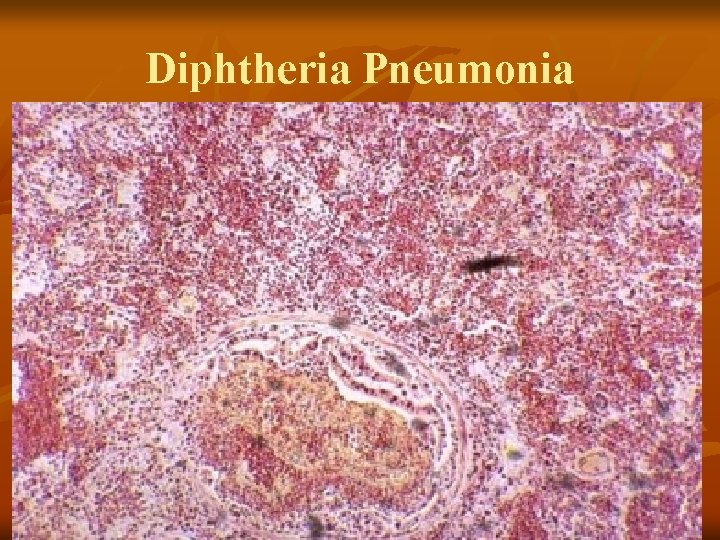
Tracheo-bronchial diphtheria n Usually an extension from pharynx & larynx n Diphtheria pneumonia – hemorrhagic n Bronchiolar pseudomembrane n Airway obstruction/sudden death

Diphtheria Pneumonia

Non-Respiratory disease

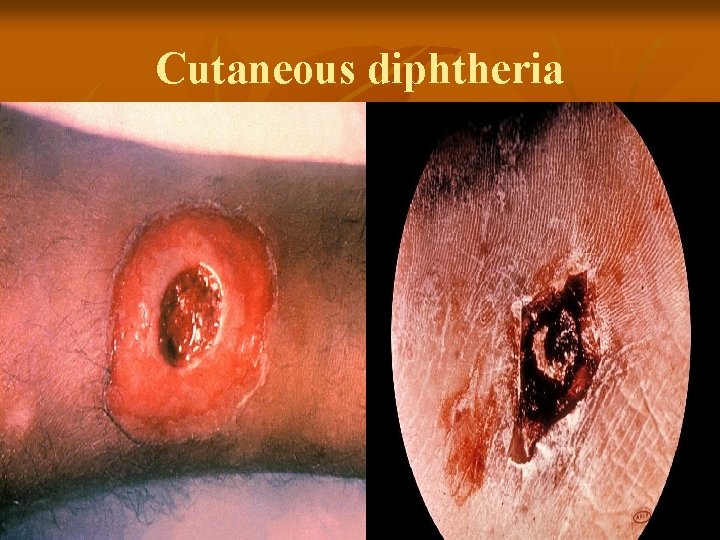
Cutaneous diphtheria

Cutaneous diphtheria superficial, non-healing ulcers n well defined margins n pseudomembrane on floor of ulcer n erythema & tenderness of surrounding skin n important in transmission in the community n

Cutaneous diphtheria contd. Predisposing factors: - pre-existing dermatoses - laceration - burns - bites - impetigo n

Other non-respiratory disease Ear- otitis externa n Eye – purulent and ulcerative conjunctivitis n Genital tract – purulent and ulcerative vulvo-vaginitis n Rarely septicaemia n

Complications n Toxic Cardiomyopathy - commonly myocarditis, rarely endocarditis - usually occurs at the end of 2 nd wk of illness - tachycardia out of proportion to fever - arrhythmias - symptoms & signs of CCF - occurs in 10 -25% of patients - accounts for 50 -60% of deaths

Toxic Cardiomyopathy contd. n n ECG findings: - prolonged PR interval - ST segment elevation - 1 st, 2 nd, or 3 rd degree heart block Echocardiogram: - dilated cardiomyopathy - hypertrophic cardiomyopathy - vegetations

Toxic Neuropathy n Usually occurs at 3 -4 wks n Affects mainly motor functions n Paralysis of soft palate &pharyngeal wall - nasal voice - difficulty in swallowing (esp. fluids)

Toxic Neuropathy contd. n n n Occulomotor N. & cillary paralysis - strabismus &/or blurred vision Peripheral neuritis – diminished DTR & paralysis - occasionally glove & stockings neuropathy ( like GBS) Paralysis of the diaphragm

Airway obstruction n Commoner in laryngeal disease n May be sudden n n Usually due to dislodgement of Pseudomembrane May require intubation/tracheotomy & mechanical ventilation

Differentials Tonsillo-Pharyngitis n Viral Croup n Epiglottitis n Peritonsilar abscess n Angioedema n Myocarditis (other causes) n Peripheral neuropathy 2 o GBS n

Laboratory Studies n Methylene blue &/or gram staining n Culture using tellurite-Loeffler media n Toxigenicity test: - Elek test - PCR

Laboratory studies contd. n FBC – moderate leucocytosis n Urinalysis – transient proteinuria n Serum assay of antibodies – immunity n Serum assay of troponin 1 – myocarditis

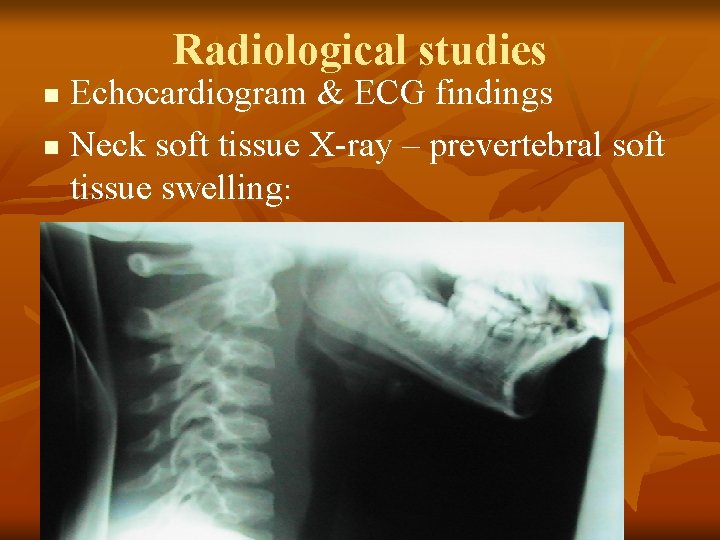
Radiological studies Echocardiogram & ECG findings n Neck soft tissue X-ray – prevertebral soft tissue swelling: n

Treatment n Diphtheria Antitoxin - mainstay of treatment - give at clinical diagnosis - can only neutralize free toxins - efficacy diminishes with delay - only available from CDC/WHO - preferably given IV - dosage depends on site involved & duration of illness

Dosage of Antitoxin (units) n n n n n • Site and extent of lesion Nasal One tonsil Both tonsils+/Pharyngeal Laryngeal or Combined types Very extensive Disease illness<72 hrs 10, 000 -20, 000 illness >72 hrs 10, 000 -20, 000 -40, 000 -60, 000 40, 000 -80, 000 60, 000 -80, 000 -100, 000 N. B. Test for sensitivity before administration and desensitized if necessary

Testing for Sensitivity Skin test: - Intradermal injection of 0. 1 m. L of 1: 10 dilution of antiserum in saline - read in 20 mins - a wheal ≥ 1 cm – positive – sensitive n Conjunctiva test: - conjunctivitis & lacrimation – positive n Caution! Ensure adrenalin is available n

Desensitizing n n n 0. 1 ml of a 1: 20 dilution subcut. 0. 1 ml of a 1: 10 dilution subcut. 0. 1 ml undiluted subcut. 0. 3 ml undiluted IM 0. 5 ml undiluted IM - wait 20 mins wait 20 mins If no reaction has occurred the rest of the dose can be given IM

Antimicrobial therapy Role: - halt toxin production - treat localized infection - prevent transmission n Drugs/dosage - IV/IM penicillin * iv xtapen 100, 000/kg/day in 6 hrly dosing * im procaine pen. 25, 000 iu/kg/day, 12 hrly - Oral erythromycin, 40 mg/kg/day 6 hrly n

Antimicrobial contd. n n n Other drugs that can be used: - Clindamycin - Tetracycline Give for 10 – 14 days Elimination of organism should be confirmed by at least 2 successive negative culture obtained 24 hrs apart.

Treatment contd. Isolation - respiratory isolation for respiratory disease - contact isolation for cutaneous disease n n Bed rest n Secure airway if necessary n NG tube feeding – palatal/pharyngeal paralysis

Treatment contd. n IV fluid administration if needed n Vaccinate – 10 series &/or boosters n Disease notification n Contact tracing

Contact tracing & Care n n n The risk of developing the disease after household exposure to a case is ≈ 2% The risk of disease after exposure to a carrier is ≈ 0. 3% Types of contacts: - asymptomatic case contact - carrier

Asymptomatic case contact monitor for illness n culture n Antimicrobial prophylaxis n Vaccinate nprimary schedule. nbooster dose n

Carrier n The reported rate of carriage in household contacts of case patients is 0 -25% Antimicrobial prophylaxis x 7 days n Isolation n Monitor n Vaccination n

Prognosis Depends on: n Virulence of the organism. Gravis has the highest fatality followed by intermedius and the least is mitis. n Age; higher mortality rates in individuals < 5 yrs and those > 40 yrs. n Immunization status: worse in the unimmunized

n n Prognosis (contd. ) Site of infection/involvement; mortality occur in: n < 1% of cutaneous disease n ≈ 10% of uncomplicated respiratory disease n 30 – 40% of bacteremic disease n 60 - 90% of those with cardiac involvement. Speed of administration of antitoxin; worse with delay

Prevention n Immunization is the mainstay of prevention n Given as DPT n Immunization schedule (NPI) - DPT 1 – 6 wks - DPT 2 – 10 wks - DPT 3 – 14 wks

The Present

Emerging Issues n Changing epidemiology - recent re-emergence in some developed and developing countries - Shifting of the disease into the older population


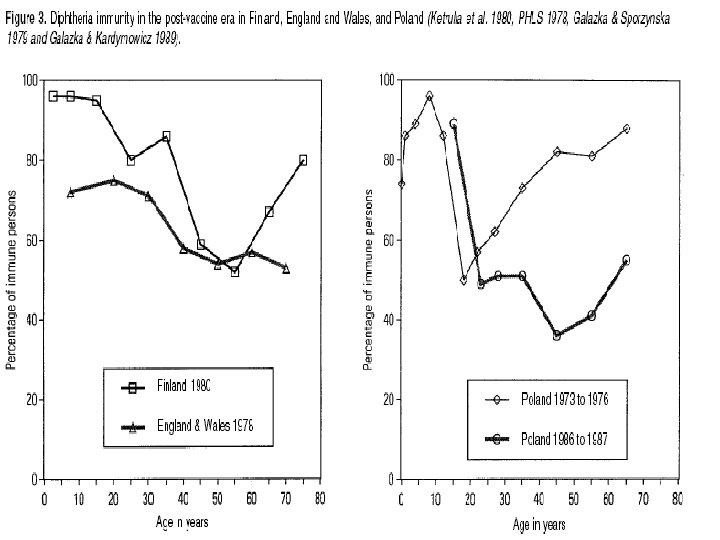
n Immunity wanes over time


Other Epidemiological issues n Questionable Notification from Nigeria Erratic values: - In 1996 reported 2016 cases - In 1997 , , 31 cases *DPT 3 coverage in 1996 – 30%

Inconsistent figures n In 2003 & 2004 – no case reported * In 2003 Nigeria had the worst immunization coverage in the world DPT 1 coverage – 43. 2% DPT 3 coverage – 24. 8% Only 12. 8% were fully immunized

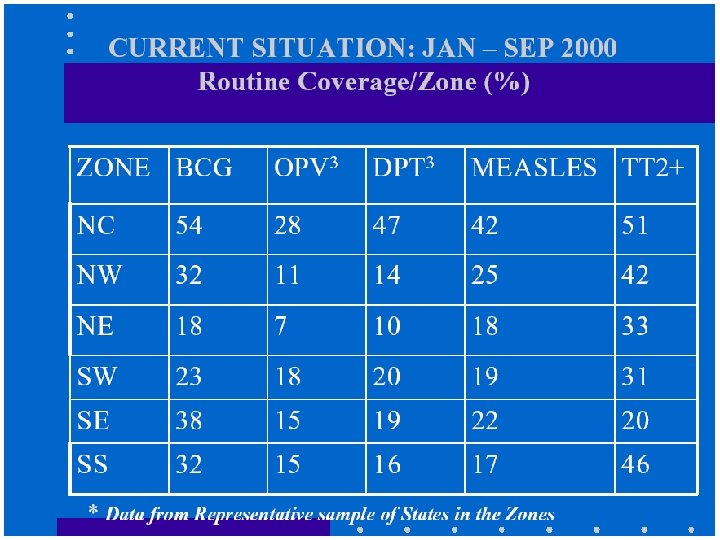
Latest Immunization Coverage n n n Global: 79% estimated DPT 3 coverage Current coverage in Nigeria: - DPT 1 is ≈ 65% - DPT 3 is ≈ 77% WHO proposed coverage is ≥ 90%



Changes In Immunization strategies n n Effect of passive immunity on 10 series Commencing 1 O series later e. g. - In the US DPT 1 – 2 mth DPT 2 – 4 mth DPT 2 – 6 mth

New Immunization Strategies contd. n Boosters: - Given at *18 mths *5 yrs *adolescence *every 10 yrs thereafter


New Formulations of the Toxoid Td - tetanus toxoid with lower dose of diphtheria toxoid - adult type *for adolescence & beyond - less side effects n Tdap - tetanus toxoid + smaller dose diphtheria + acellular pertusis vaccine - may be used for pregnant women n

Other Emerging Issues n Antitoxin for Carriers: * To give or not to give ? n The need for vaccination of pregnant women

The Future

Recommendations n n n Improve coverage of 10 schedule to 90% at least 4 th & 5 th DPT doses at 18 mths & 5 yrs respectively Improve disease Surveillance and notification

Recommendations contd. n Research to evaluate the need to - delay commencement of the primary series - give booster doses at adolescence & thereafter every 10 yrs, using Td - give Td or Tdap to pregnant women

Conclusion n The global goal is to eradicate diphtheria. This may only be achieved by not only making the right policies but also ensuring that these policies are completely and effectively implemented.

THANK YOU