Sleep Apnea Dr Vishal Sharma History Lugaresis 1970
















































- Slides: 124

Sleep Apnea Dr. Vishal Sharma

History • Lugaresis (1970): described OSAS • Stanford University (1972): Polysomnography • Sleep Latency Test devised in 1976 • Before 1980’s tracheostomy main treatment • Ikematsu performed first UPPP in 1952 • Fujita popularized UPPP • Kamami developed LAUP in late 1980 s

Definitions

Sleep related breathing disorders Synonym: sleep disordered breathing Consists of: A. Snoring B. Obstructive sleep apnea C. Obstructive sleep hypopnea D. Upper airways resistance syndrome

Arousal: Abrupt change from deep stage to lighter stage of NREM sleep, or from REM sleep to awakening Arousal index: Number of arousals per hour of sleep Apnea: Cessation of breathing for > 10 seconds Apnea Index: Number of apneas per hour of sleep Hypopnea: Decreased airflow (>50%) with oxygen desaturation (> 4% ) for > 10 seconds Snoring: breathing noise due to partial upper airway obstruction

Obstructive sleep apnea: Cessation of airflow for > 10 seconds even with continued respiratory effort Obstructive sleep hypopnea: Decreased airflow (>50%) with oxygen desaturation (> 4% ) for > 10 seconds even with continued respiratory effort Upper airway resistance syndrome (respiratory effort related arousal): partial airway obstruction with no apnea or hypnea, but arousal index > 15

Respiratory Distress Index: Number of apneas + hypopneas + respiratory effort related arousals per hour Obstructive sleep apnea syndrome: 30 or more episodes of obstructive sleep apnea during a 7 - hour period of sleep or apnea index > 5 or respiratory distress index > 15

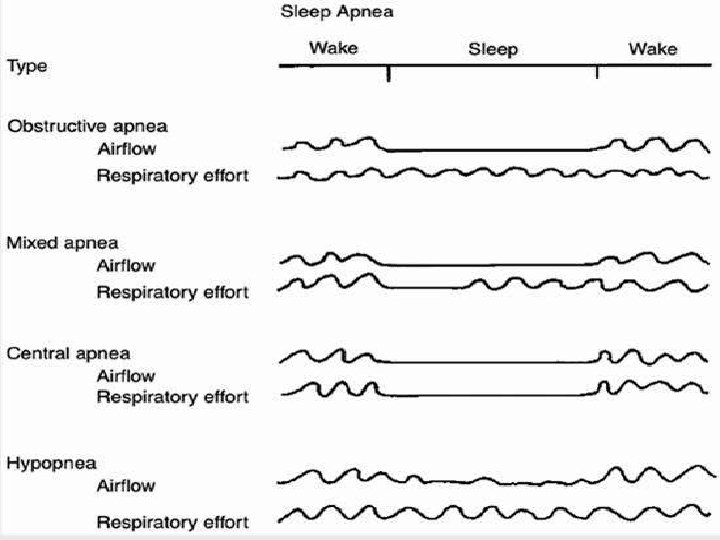
Types of sleep apnea 1. Obstructive: Normal respiratory chest wall movement 2. Central: No respiratory chest wall movement 3. Mixed: Partial respiratory chest wall movement


Grades of sleep apnea American Sleep association grading: 1. Mild ------ 5 - 20 apneas per hour 2. Moderate ----- 20 - 40 apneas per hour 3. Severe ---- more than 40 apneas per hour

Etiology of central sleep apnea

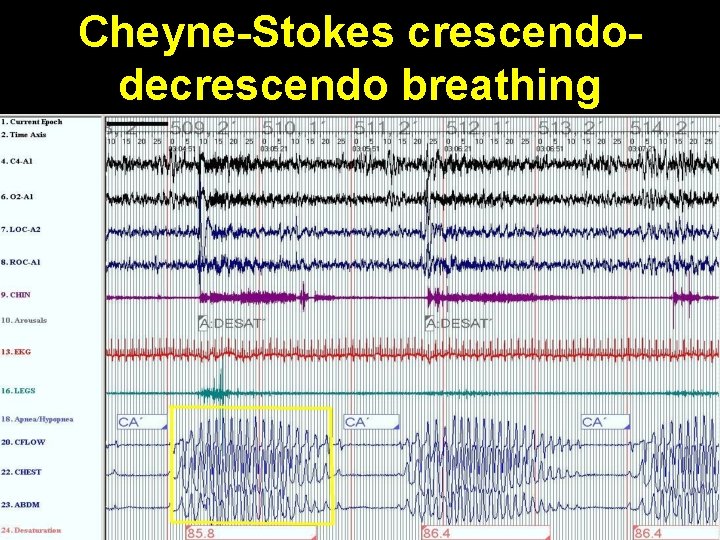
• Cheyne-Stokes breathing-central sleep apnea due to renal failure, heart failure, stroke • Diabetes mellitus, Hypothyroidism, Acromegaly, Parkinson disease, Myasthenia gravis, Idiopathic cardiomyopathy, Muscular dystrophy • Medullary tumor or infarction • Arnold-Chiari malformation • Cervical cordotomy • High-altitude periodic breathing (at > 5000 m) • Use of opiates & other CNS depressants

Cheyne-Stokes crescendodecrescendo breathing

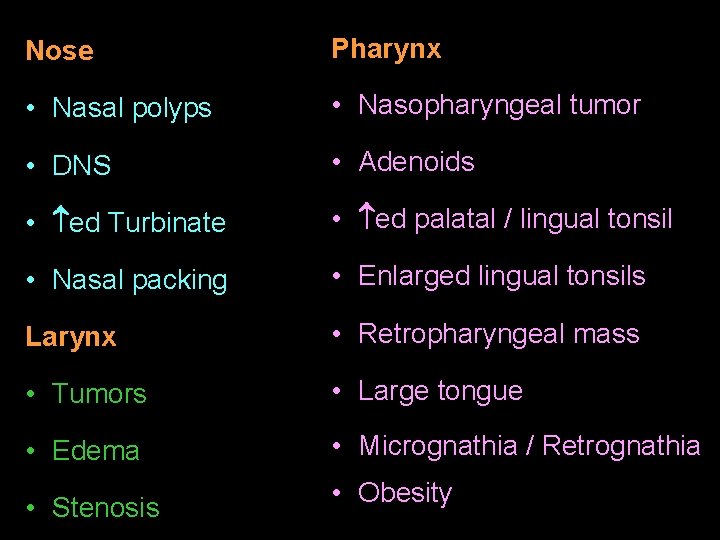
Etiology of obstructive sleep apnea

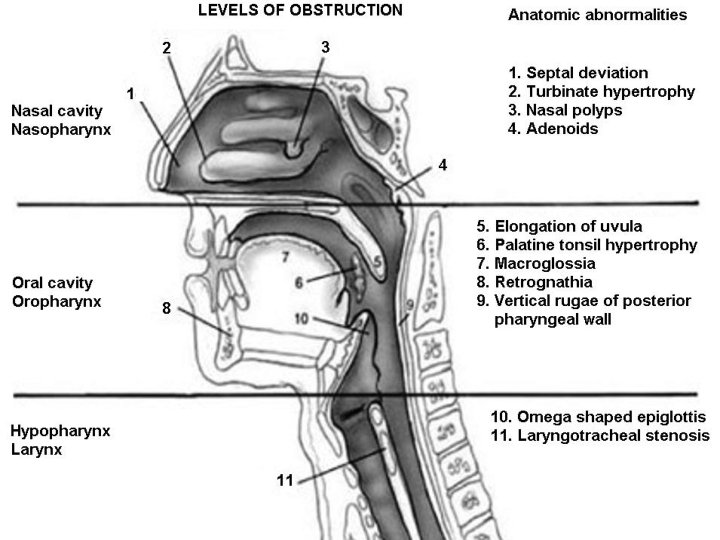
Nose Pharynx • Nasal polyps • Nasopharyngeal tumor • DNS • Adenoids • ed Turbinate • ed palatal / lingual tonsil • Nasal packing • Enlarged lingual tonsils Larynx • Retropharyngeal mass • Tumors • Large tongue • Edema • Micrognathia / Retrognathia • Stenosis • Obesity




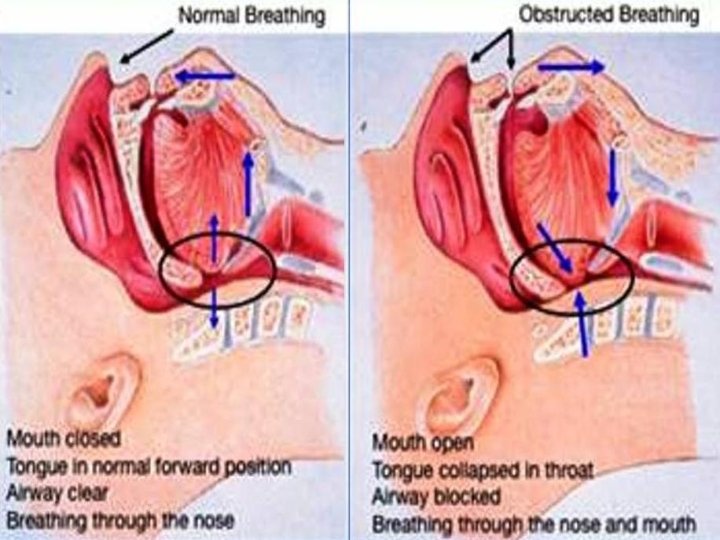
Patho-physiology

Increased compliance of pharyngeal tissues + Neuromuscular in-coordination & ed muscle tone + Anatomical abnormalities Upper airway collapse airway obstruction Hypoxia + negative intra-thoracic pressure Arousal Increased tone of upper airway muscles + upper airway obstruction clears Patient goes to sleep Upper airway collapses again causing arousal

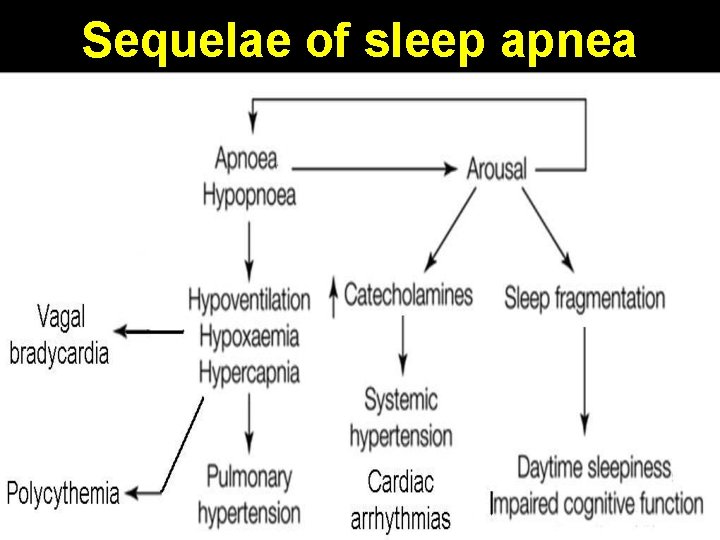
Sequelae of sleep apnea

Complications of sleep apnea Systemic hypertension Coronary artery disease Pulmonary hypertension Right heart failure Cardiac arrhythmias Cerebro-vascular accident Polycythemia Sleepiness accidents Depression Impotence Vagal bradycardia Sudden nocturnal death

Clinical Features

Snoring or sleep apnea?

Symptoms of sleep apnea Day- time Night- time Excessive sleepiness Snoring Morning headache Observed choking Intellectual deterioration Arousal from sleep Personality change Repeated waking Depression Nocturnal sweating Xerostomia Nocturnal enuresis Abnormal movements Impotence

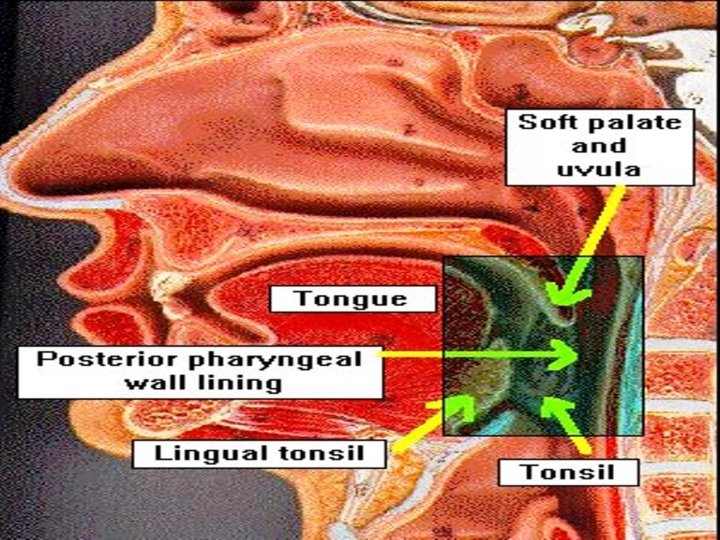
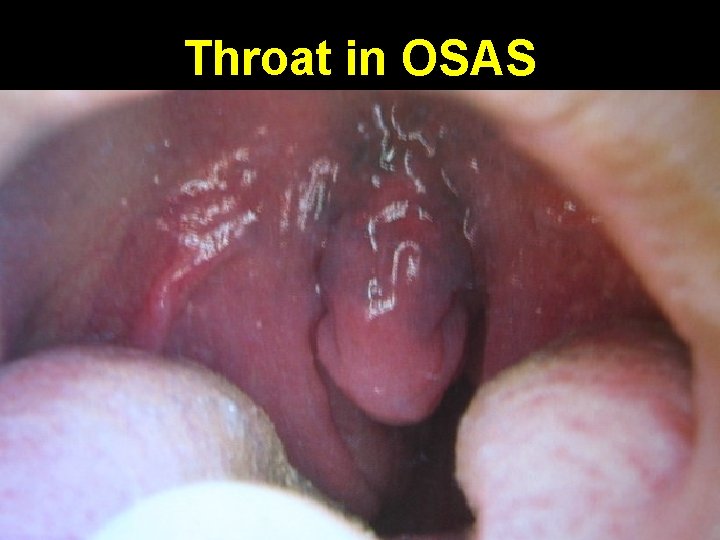
Typical OSAS patient • Synonym: Pickwickian syndrome • Middle age or elderly male with hyper somnolence • Obese with body mass index > 30 • Short neck with its circumference > 17 inches • Hypertension & right heart failure • Large bulky tongue, hypertrophied tonsils, bulky soft palate, prominent posterior pharyngeal wall rugae

Mr. Pickwick & fat boy Joe

Throat in OSAS

History from sleep partner • Bed timings • Body position • Snoring • Apnea (choking) • Arousal from sleep • Alcohol consumption • Sedative use

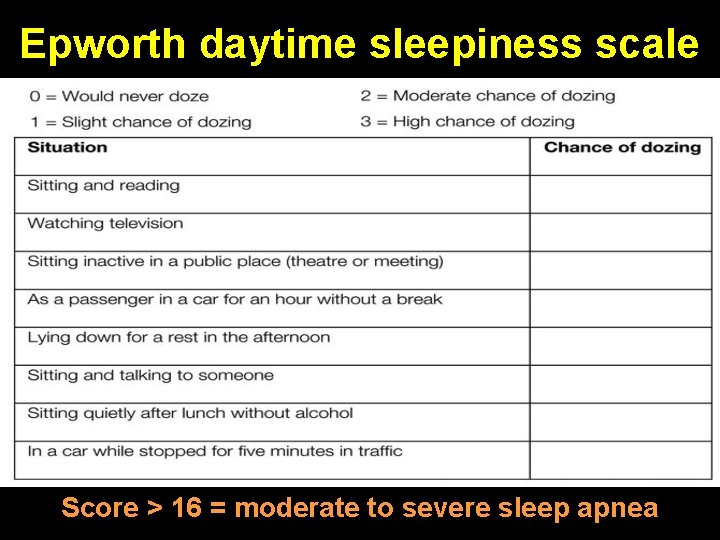
Epworth daytime sleepiness scale Score > 16 = moderate to severe sleep apnea

Physical examination General appearance, weight, body mass index Blood pressure, cardiovascular examination Cranio-facial: retrognathia, hypoplastic maxilla Nasal: airway patency, DNS, turbinate hypertrophy Tongue: macroglossia, lingual tonsil Nasopharynx: adenoids, polyp, cyst, tumor

Physical examination Oropharynx: Soft palate, palatine tonsil, base of tongue, posterior pharyngeal wall Hypopharynx: tumor Larynx: cyst, tumor, vocal cord mobility Neck: short wide neck (circumference > 17 inches) Thyroid enlargement, features of hypothyroidism

Investigations

General Investigations • Complete blood count: anemia, polycythemia • Chest x-ray: cardiomegaly, pulmonary disorder • Lung function: portable spirometry flow volume loop saw-tooth pattern • Thyroid function tests: hypothyroidism • Electro-cardiography: cardiac arrhythmias • Arterial blood gas analysis

Portable spirometer

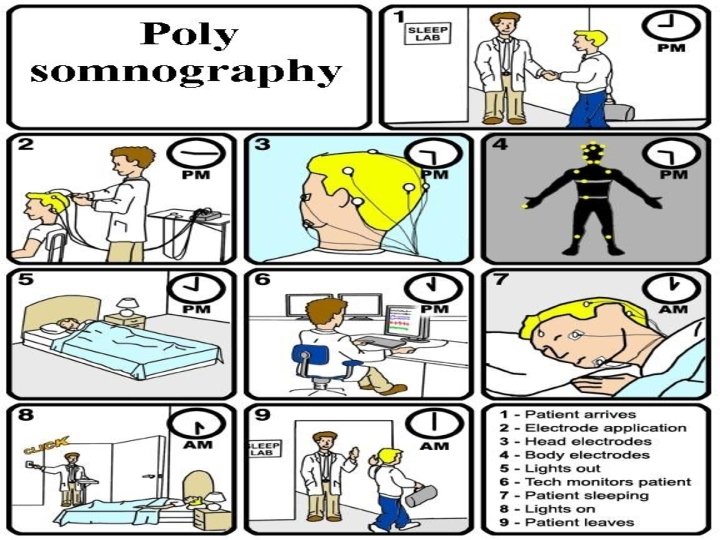
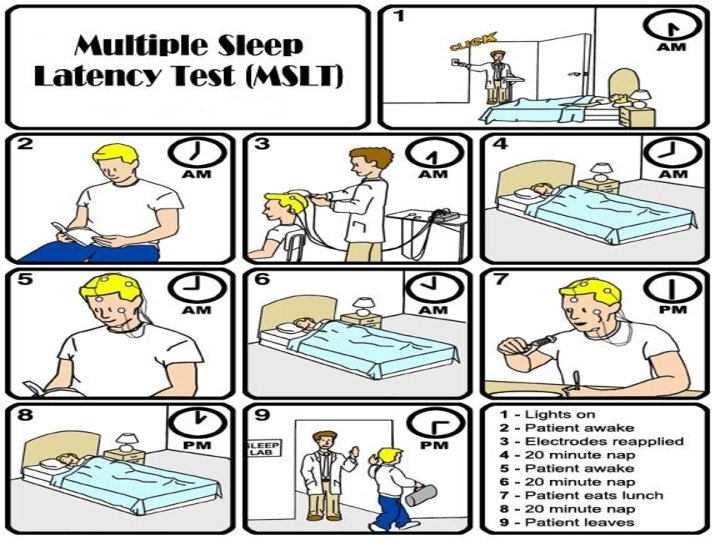
Investigations for confirmation of sleep apnea • Polysomnography • Portable sleep monitoring • Overnight pulse oximetry recording • Multiple sleep latency test

Polysomnography parameters 1. Electro-encephalogram (EEG) 2. Electro-myogram (EMG): submental, anterior tibialis 3. Electro-oculogram (EOG) / Electro-nystagmogram 4. Electro-cardiogram (ECG) 5. Oxygen saturation 6. Nasal & oral airflow 7. Chest + abdominal movement detector 8. Sleeping position detector 9. Tracheal microphone 10. Esophageal manometer


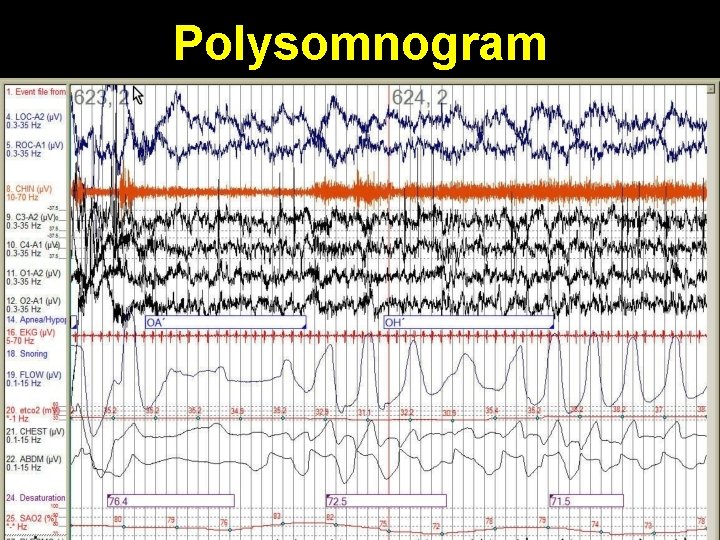
Polysomnogram

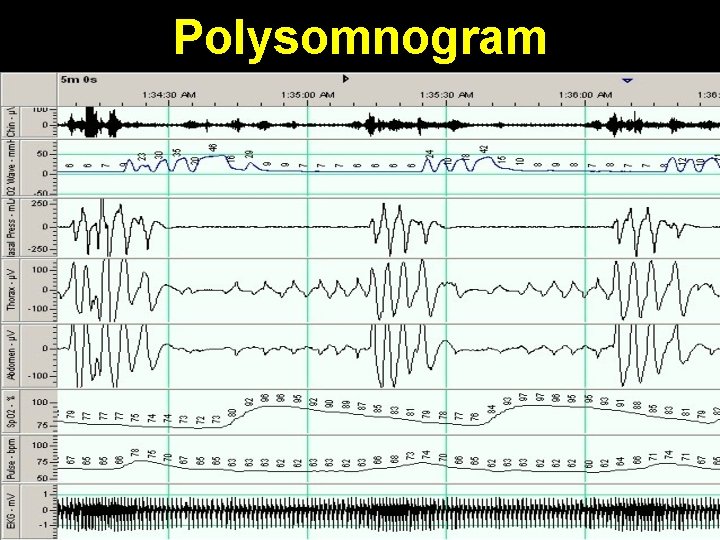
Polysomnogram

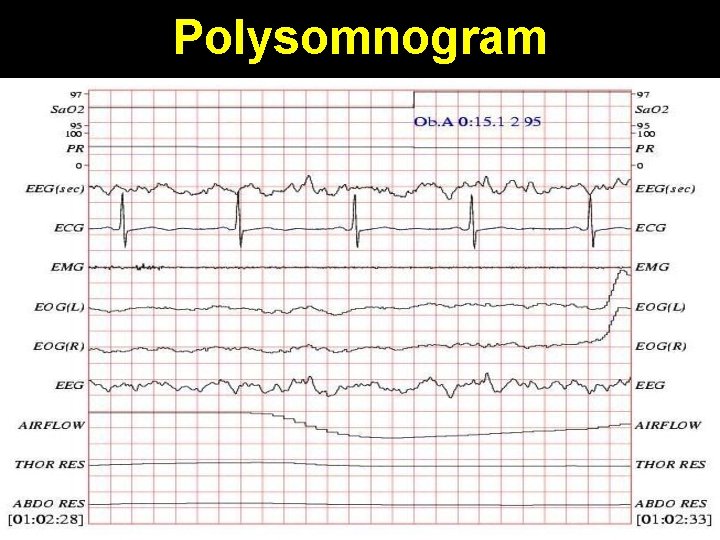
Polysomnogram

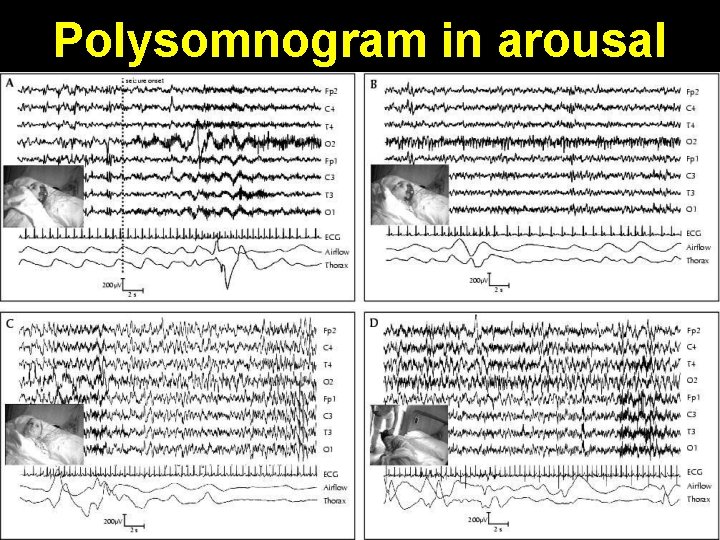
Polysomnogram in arousal

Portable polysomnogram


Investigations to assess site of airway obstruction Awake patient Sleeping patient Muller maneuver Flexible nasendoscopy Lateral cephalometry Somno-fluoroscopy C. T. scan of neck Cine C. T. scan Pharyngeal manometry

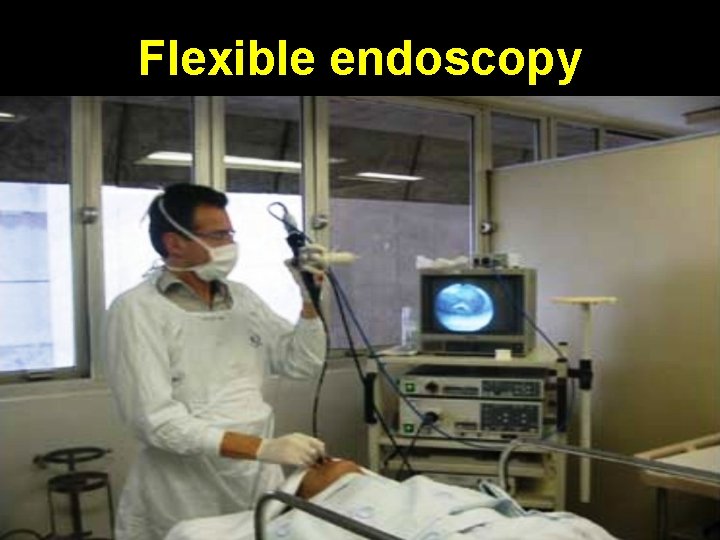
Flexible endoscopy

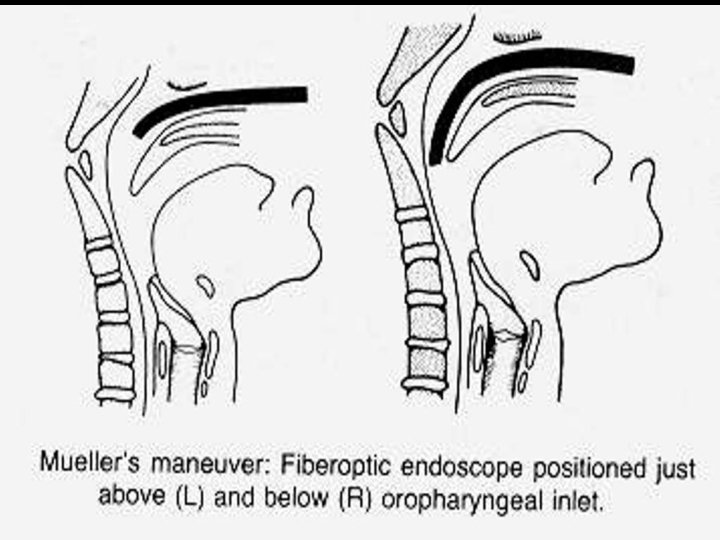
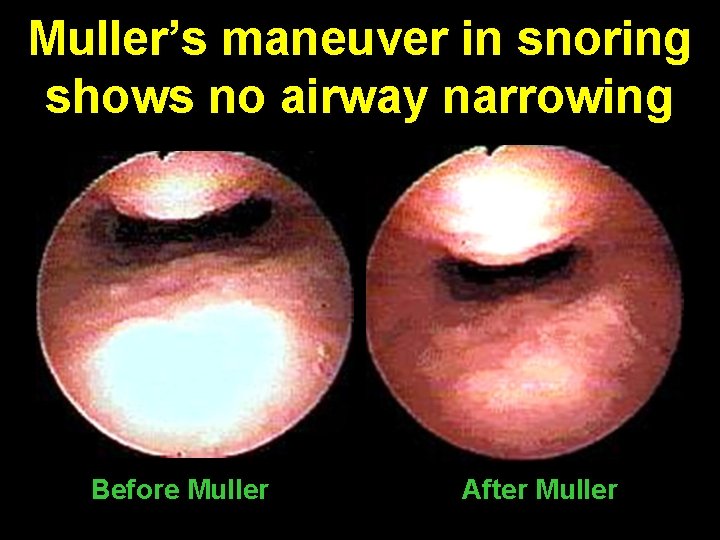
Muller’s maneuver • After a forced expiration, pt attempts inspiration with closed mouth & nose, whereby negative pressure leads to collapse of airway • Previously introduced flexible endoscope (via nasal cavity) identifies weakened sections of airway at levels of soft palate & tongue base, during this maneuver


Muller’s maneuver in snoring shows no airway narrowing Before Muller After Muller

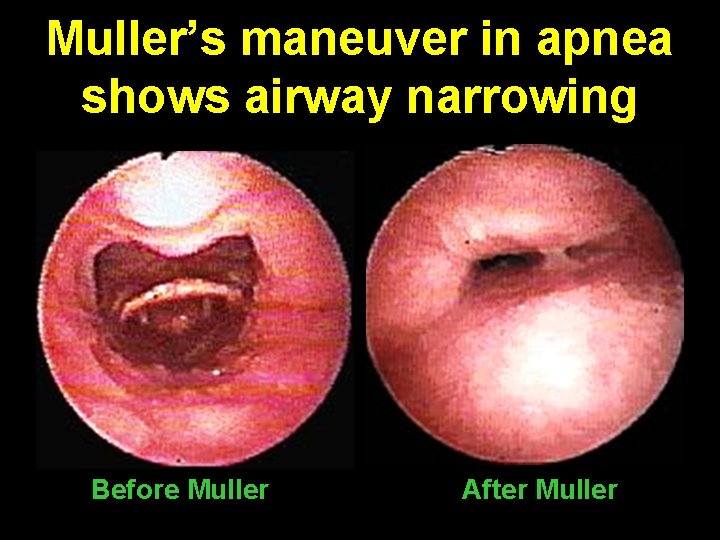
Muller’s maneuver in apnea shows airway narrowing Before Muller After Muller

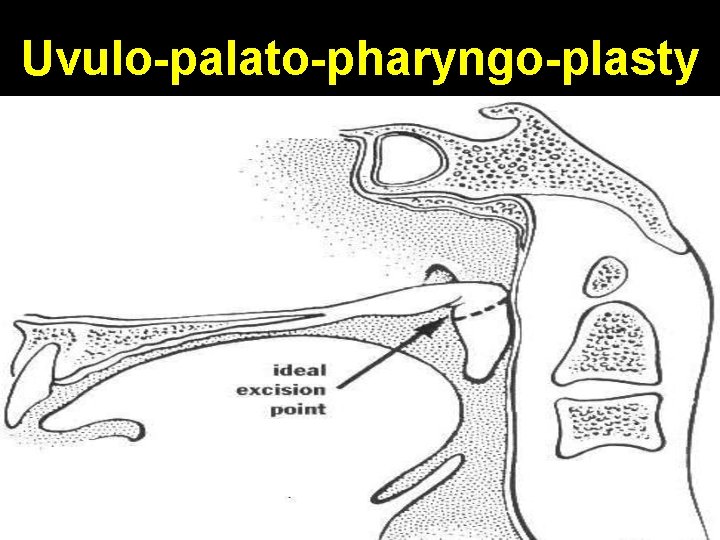
Degree of airway obstruction 0 = no collapse 1+ = minimal collapse 2+ = collapse es cross-sectional area by 50% 3+ = collapse es cross-sectional area by 75% 4+ = collapse obliterates airway 3+ or 4+ score at soft palate level with 0 score at tongue base level is ideal for UPPP Score of > 2+ at tongue base level is not suitable for Uvulo-palato-pharyngo-plasty (UPPP)

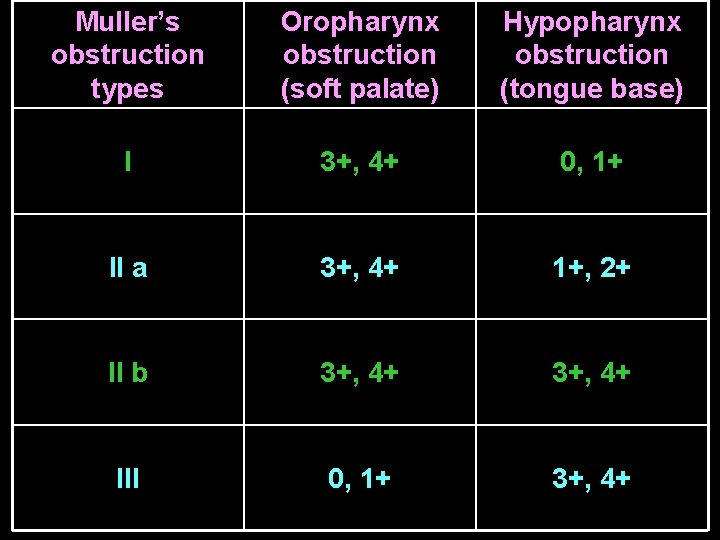
Muller’s obstruction types Oropharynx obstruction (soft palate) Hypopharynx obstruction (tongue base) I 3+, 4+ 0, 1+ II a 3+, 4+ 1+, 2+ II b 3+, 4+ III 0, 1+ 3+, 4+

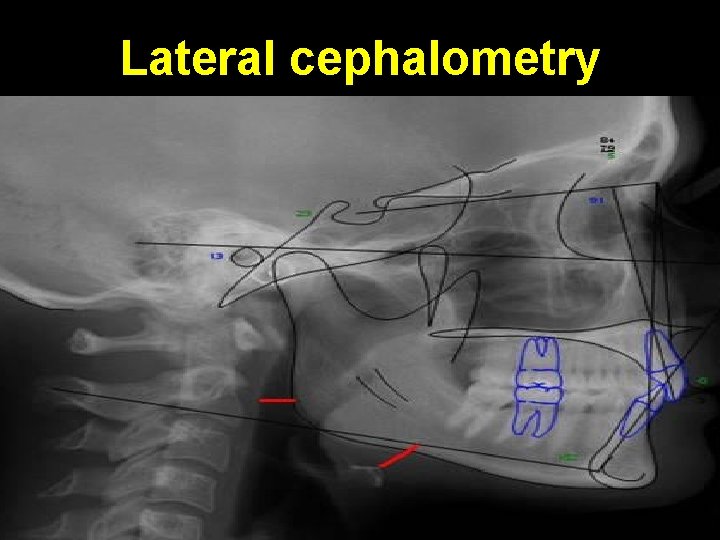
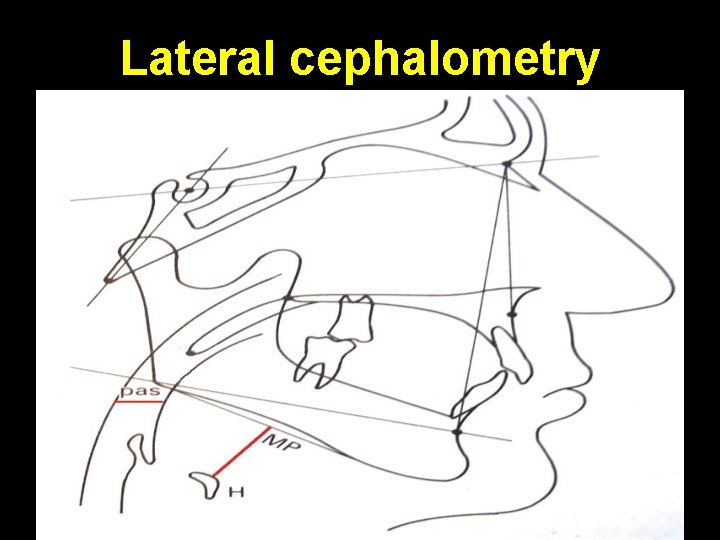
Lateral cephalometry

Lateral cephalometry

Lateral cephalometry Measurements in obstructive sleep apnea: • Posterior airway space (PAS) or narrowest width of hypopharynx is < 5 mm • Distance b/w mandibular plane to hyoid bone (MP-H) is > 24 mm

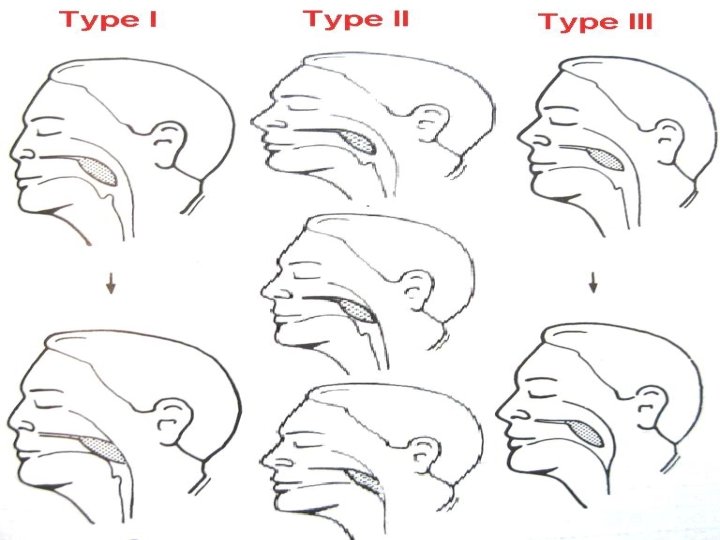
Somno-fluoroscopy Sleeping pt observed with polysomnography & during apneic episode visualized with fluoroscopy for upper airway obstruction • Type I = obstruction at soft palate level only • Type II = obstruction at soft palate level followed by obstruction at tongue base level • Type III = obstruction at tongue base level


Cine C. T. scan: • Rapid CT scanning of 8 cm of upper airway in 240 msec during apneic episode to study anatomical changes during apneic episode. Research tool. Pharyngeal manometry: • Measurement of intra-luminal pressure at level of soft palate, tongue base & hypopharynx

D/D of excessive daytime sleepiness (hyper somnolence) Sleep apnea syndrome Narcolepsy Sleep deprivation Hypoglycemia Hypothyroidism Severe anemia Cerebral tumors Depression Sedative drugs Nocturnal myoclonus Idiopathic

Non-surgical Tx for OSAS • Lifestyle modifications • Sleep hygiene • Medications • Nasal valve dilator • Positioning device • Nasal positive airway pressure device

Lifestyle modifications Weight reduction for obese patients • Body mass index = weight in kg / (height in metres)2 • Ideal BMI: male < 27. 8; Stop smoking Stop alcohol consumption Avoid sedative drugs female < 27. 3

Sleep hygiene • Elevate head-end of bed by 300: decreases pressure of abdominal contents on diaphragm & improves upper airway patency • Avoid lying supine: T-shirt with tennis ball at back • Avoid sleep deprivation • Have regular sleep cycle

Medications • Amitriptyline & Protriptyline: suppress REM sleep, respiratory stimulant, increase pharyngeal muscle tone • Nasal decongestant, antihistamine, steroid spray • Fenfluramine to reduce obesity • Thyroxin for hypothyroidism

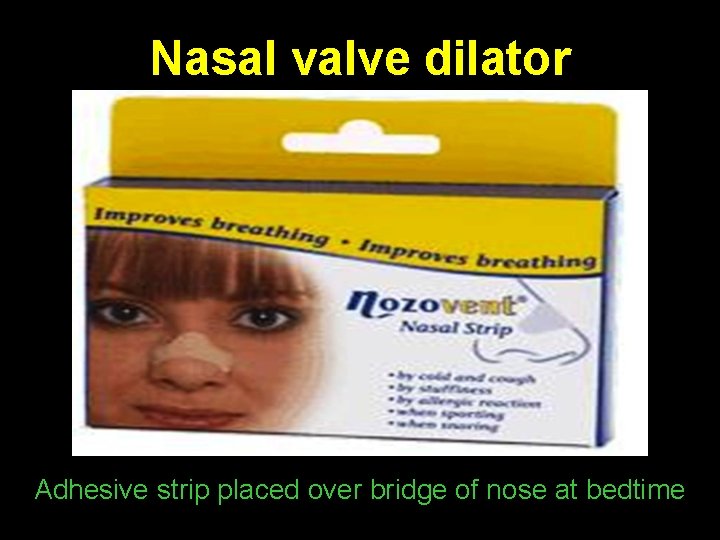
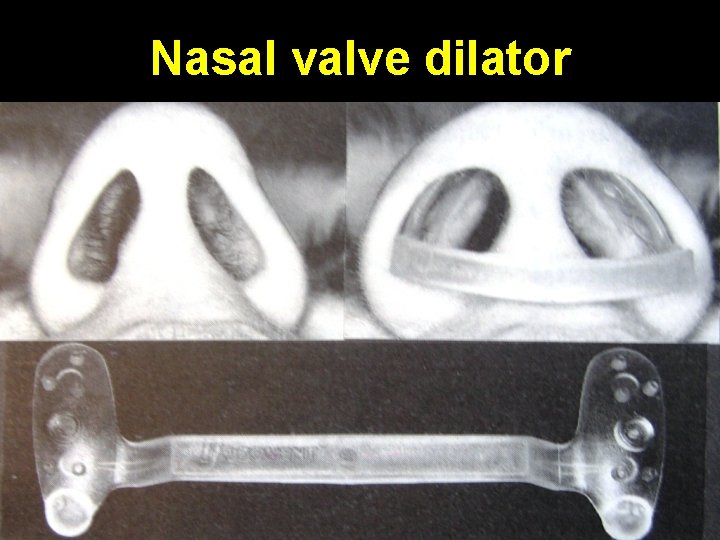
Nasal valve dilator Adhesive strip placed over bridge of nose at bedtime

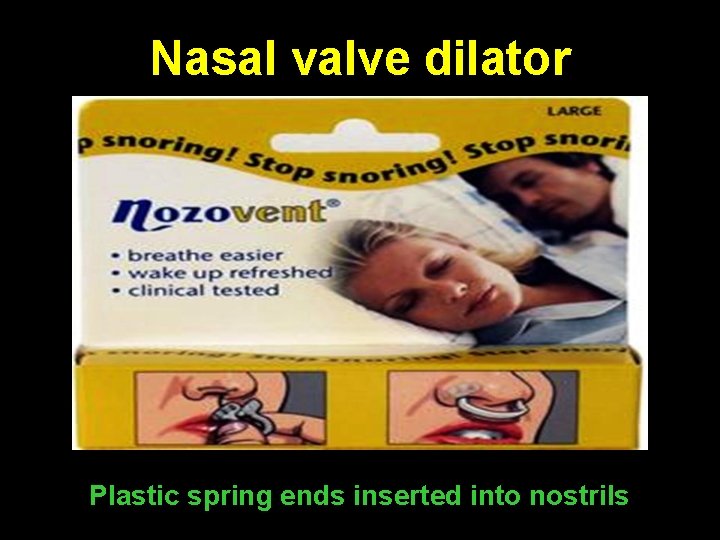
Nasal valve dilator Plastic spring ends inserted into nostrils

Nasal valve dilator

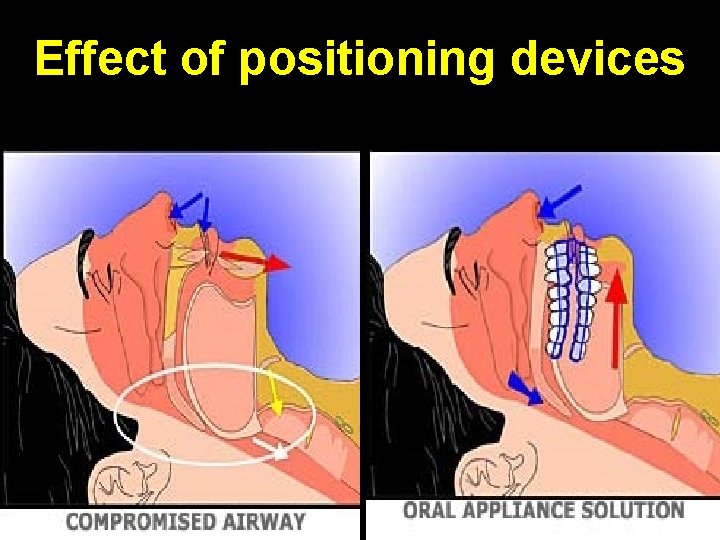
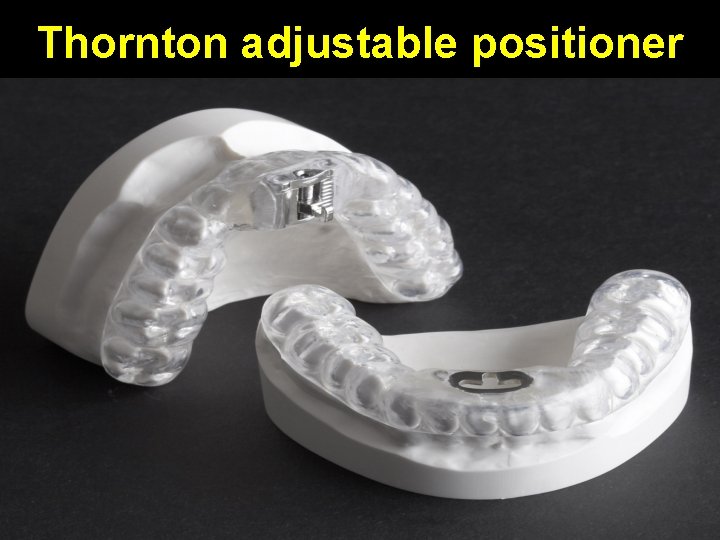
Positioning devices • Tongue retaining device • Mandibular advancement device • Optimized mandible retention • Thornton adjustable positioner

Effect of positioning devices

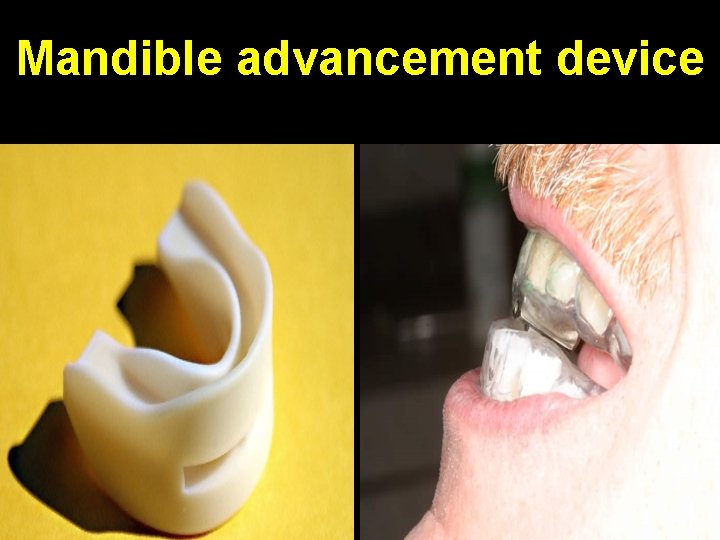
Mandible advancement device

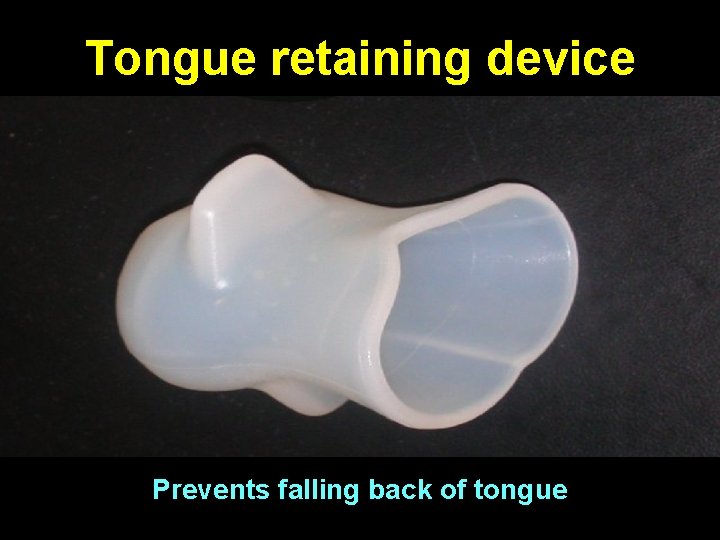
Tongue retaining device Prevents falling back of tongue

Optimized mandible retention

Thornton adjustable positioner

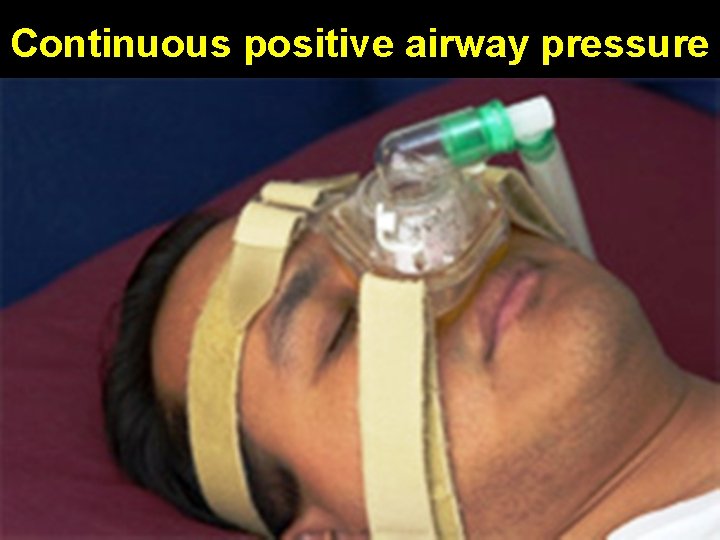
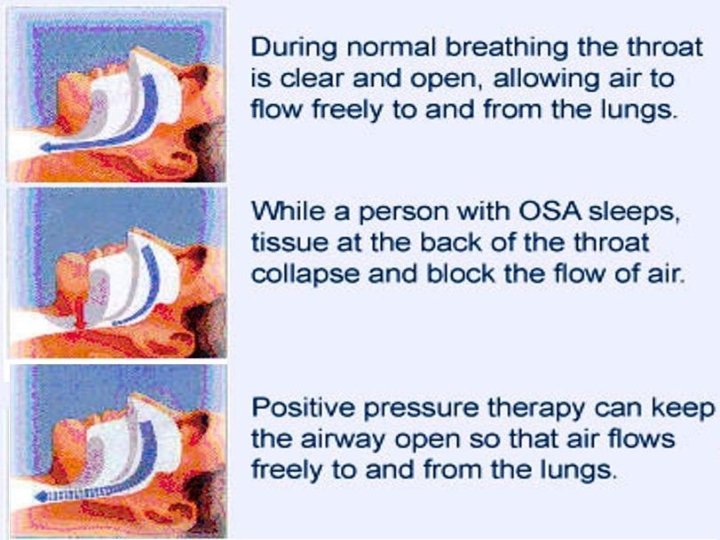
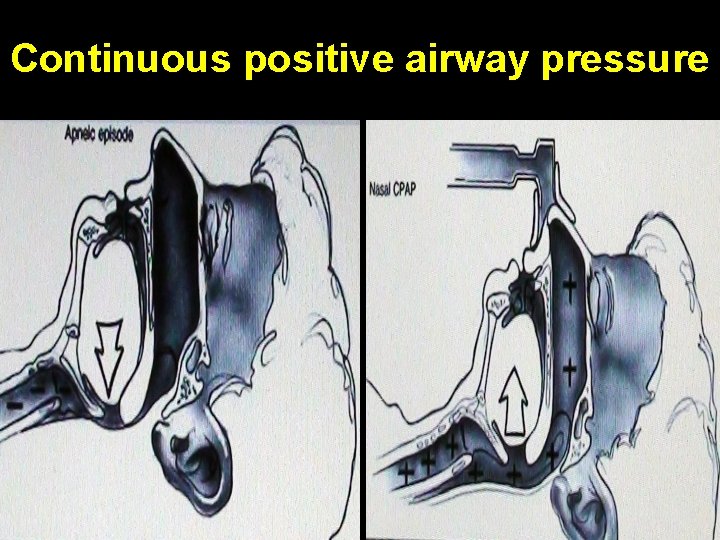
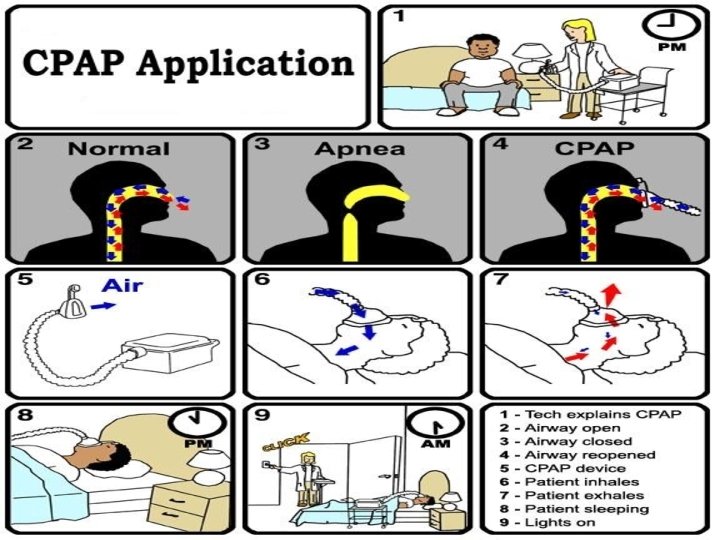
Positive airway pressure devices • Gold standard treatment • Prevents apneas in 99 -100% patients • C. P. A. P. : Continuous positive airway pressure • Bi. P. A. P. : Bi-level positive airway pressure (less pressure given during expiration) • A. P. : Automatic positive airway pressure (adjusts pressure breath by breath)

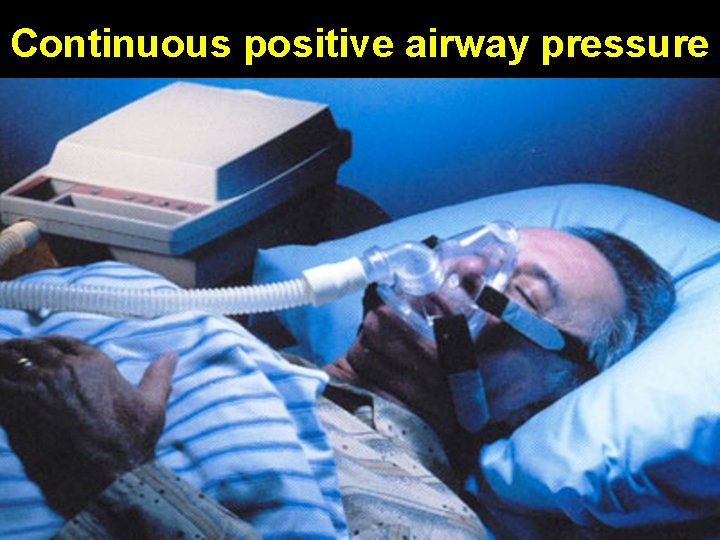
Continuous positive airway pressure


Continuous positive airway pressure


Continuous positive airway pressure

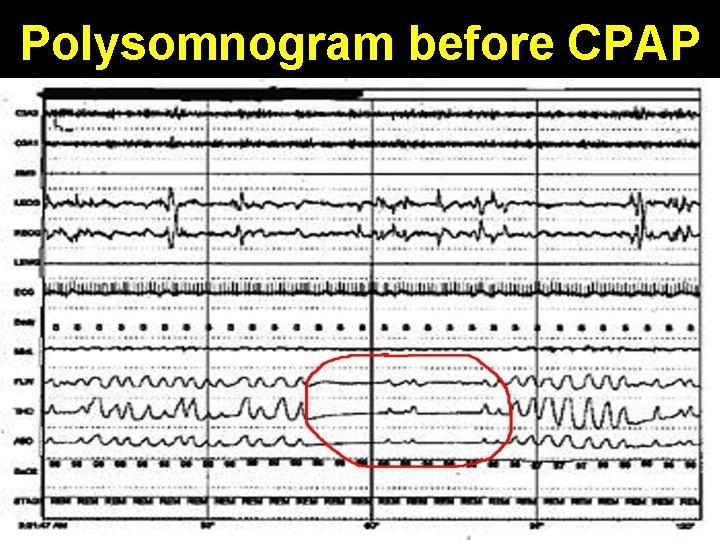
Polysomnogram before CPAP

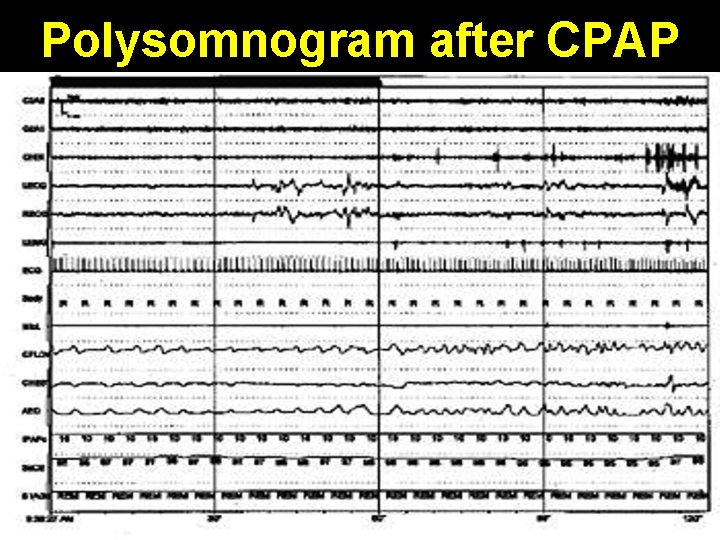
Polysomnogram after CPAP

Surgical Tx of OSAS 1. Nasal surgery 2. Palatal surgery 3. Tongue base surgery 4. Maxillo-facial surgery 5. Tracheostomy: last resort, 100% cure; relieves all levels of airway obstruction

Nasal & nasopharyngeal surgery More effective for snoring than sleep apnea 1. Septo-turbinoplasty 2. Radio-frequency turbinate somnoplasty 3. Nasal polypectomy 4. Nasal valve reconstruction 5. Nasal mass excision 6. Adeno-tonsillectomy

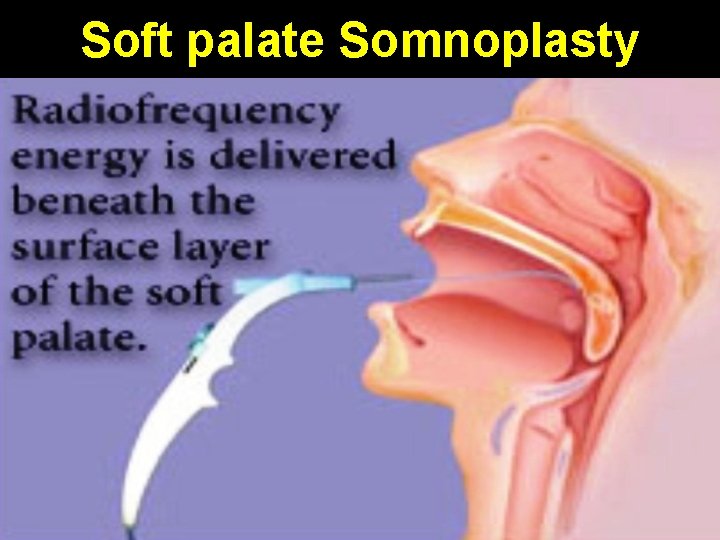
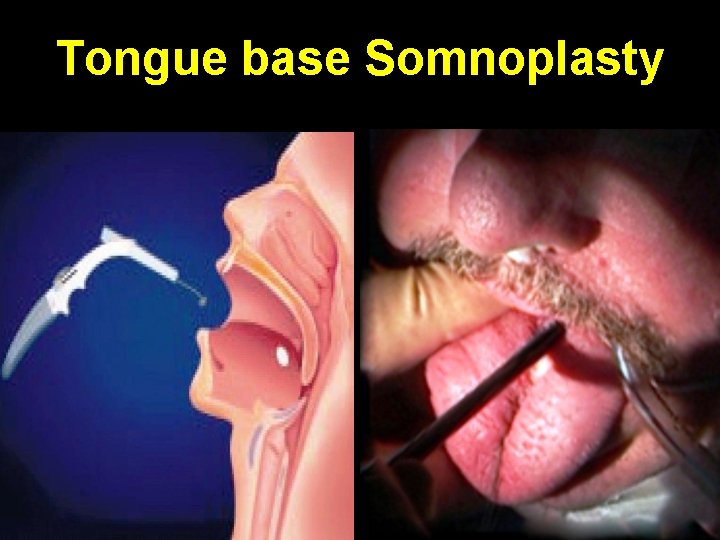
Somnoplasty • Small probe delivers radiofrequency energy into tissue bulk, causing coagulative lesions which shrink on healing • Body absorbs these lesions over 4 -8 weeks leading to tissue volume reduction • Used for enlarged base of tongue / soft palate / turbinates causing snoring / sleep apnea

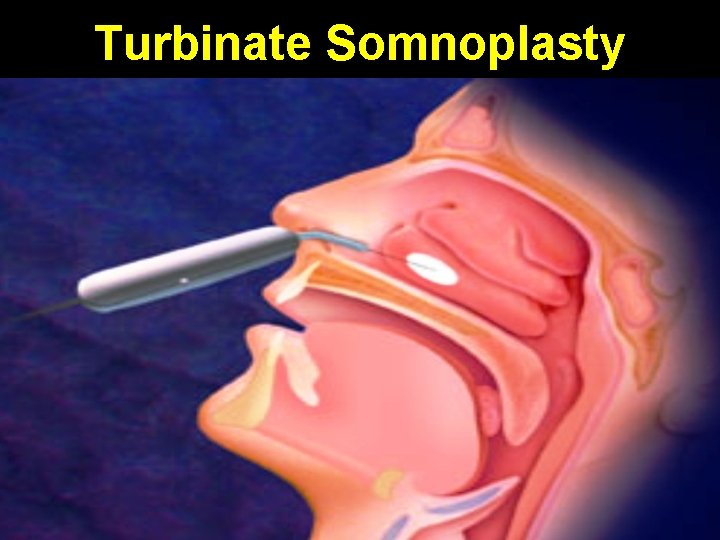
Turbinate Somnoplasty

Palatal Surgery Relieve palato-pharyngeal level obstruction 1. Uvulo-palato-pharyngo-plasty (UPPP) 2. Laser-assisted Uvulo Palato-plasty (LAUP) 3. Radio-frequency uvulo-palato-plasty (RFUP) 4. Uvulo-palatal flap 5. Lateral pharyngoplasty 6. Palatal stiffening operations

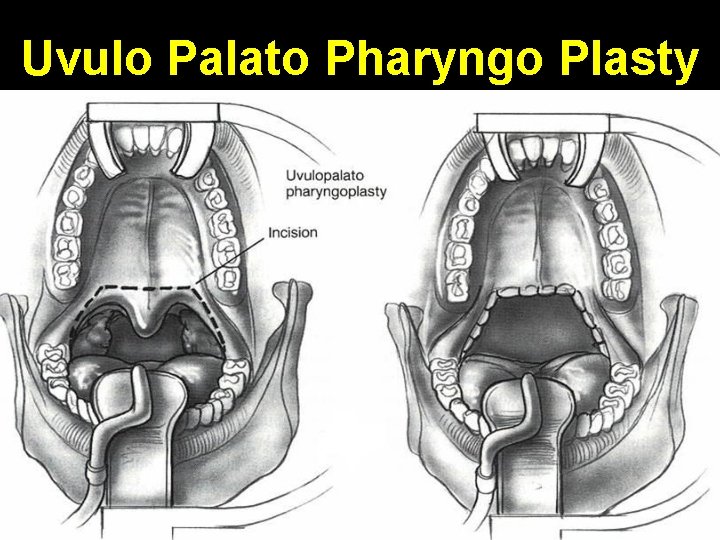
Uvulo Palato Pharyngo Plasty

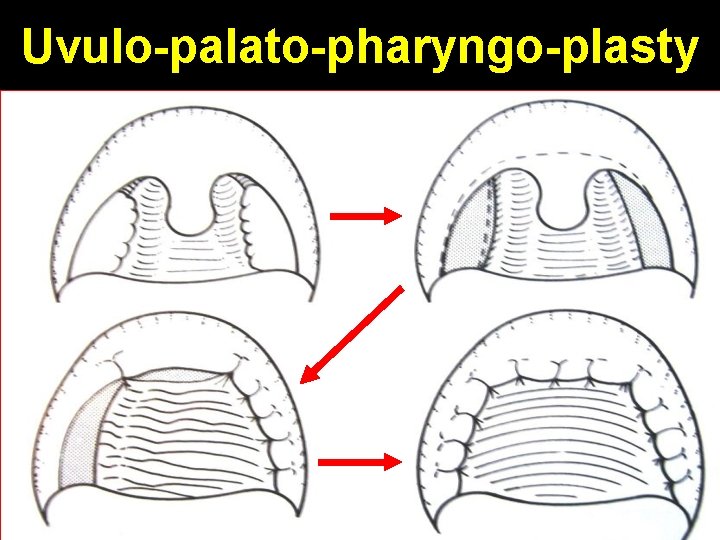
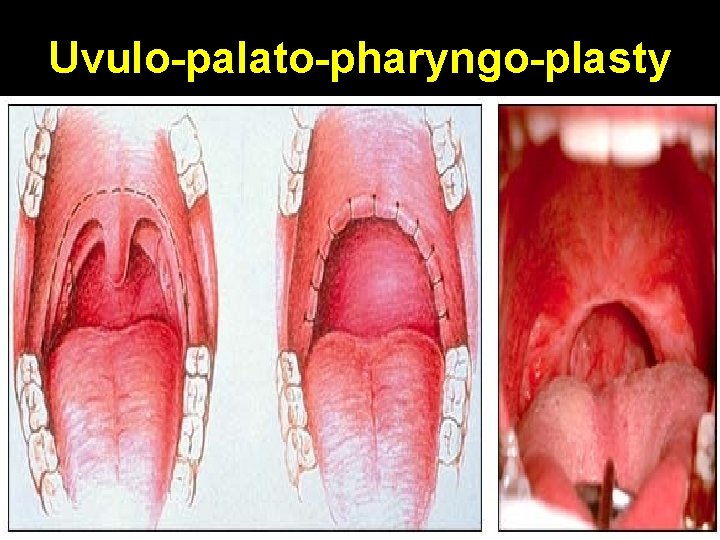
Uvulo Palato Pharyngo Plasty • Remove palatine tonsils • Trim tonsillar pillars (optional) • Remove uvula & variable amount of soft palate • Suture posterior tonsillar pillar to anterior tonsillar pillar • Suture posterior soft palate mucosa to anterior soft palate mucosa

Uvulo-palato-pharyngo-plasty

Uvulo-palato-pharyngo-plasty

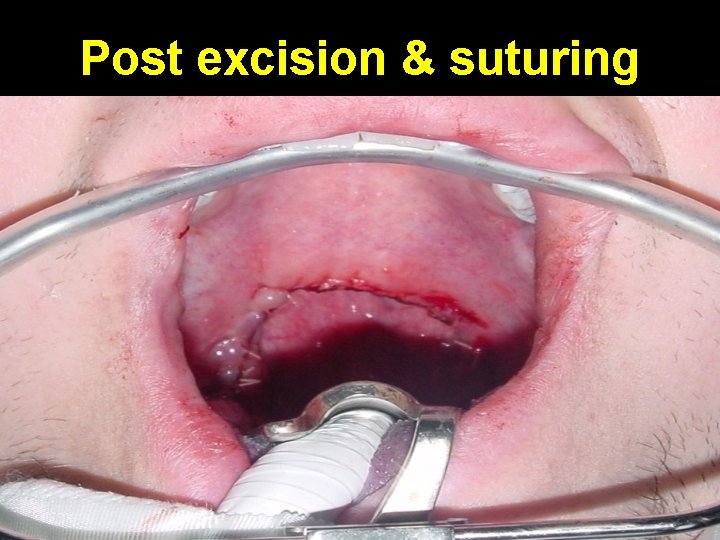
Post excision & suturing

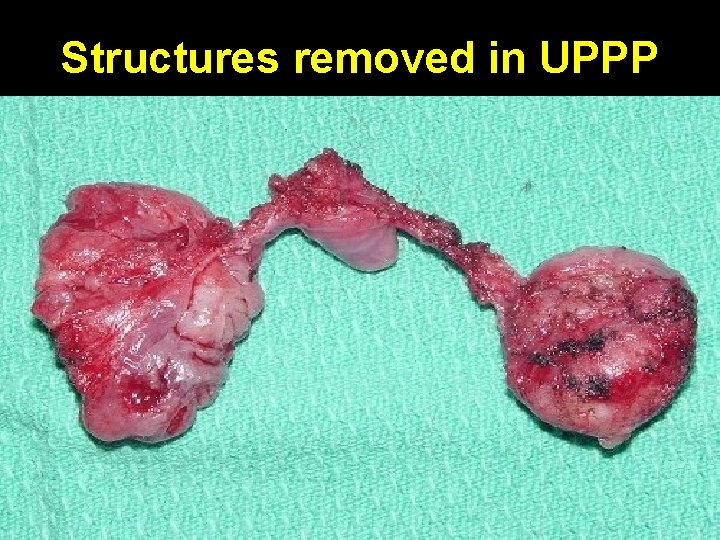
Structures removed in UPPP

Uvulo-palato-pharyngo-plasty

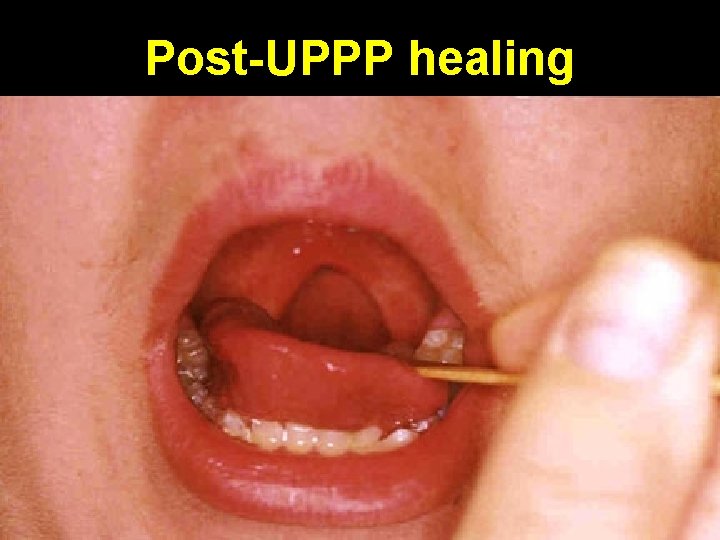
Post-UPPP healing

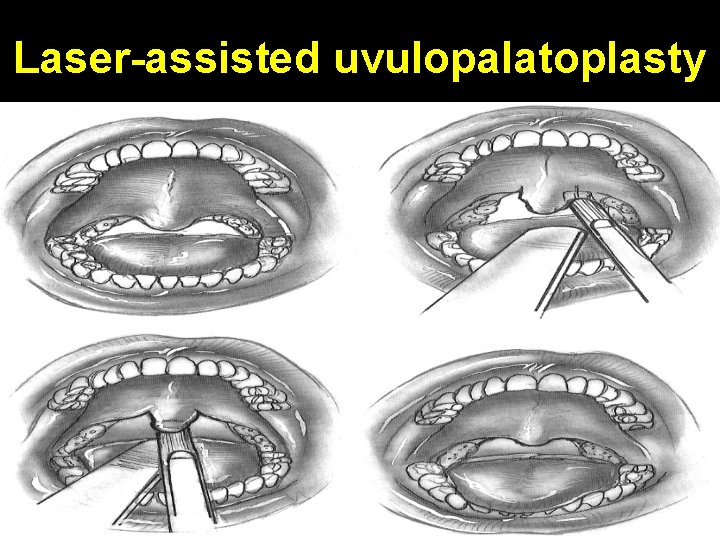
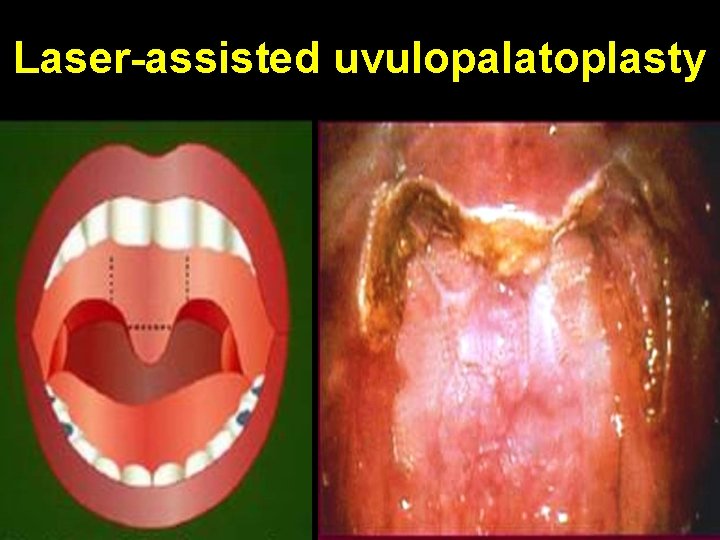
Laser-assisted uvulopalatoplasty

Laser-assisted uvulopalatoplasty

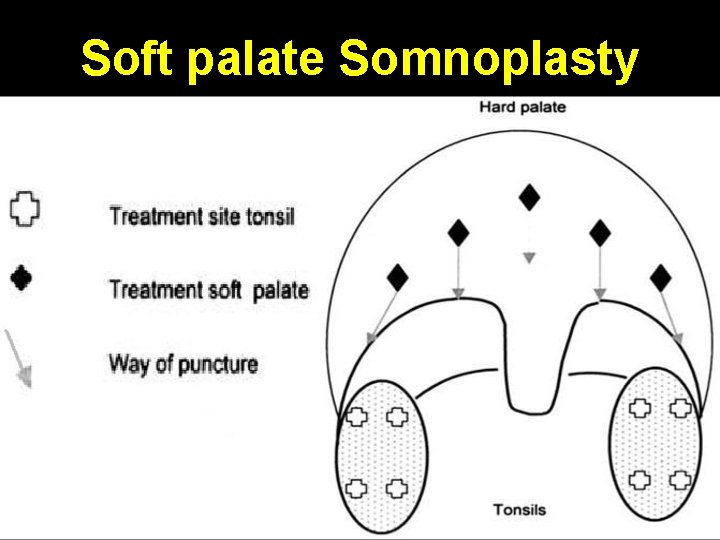
Soft palate Somnoplasty

Soft palate Somnoplasty

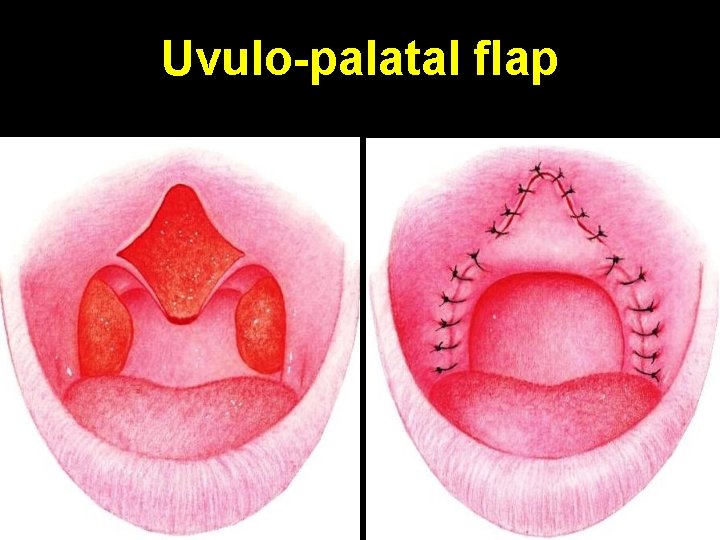
Uvulo-palatal flap

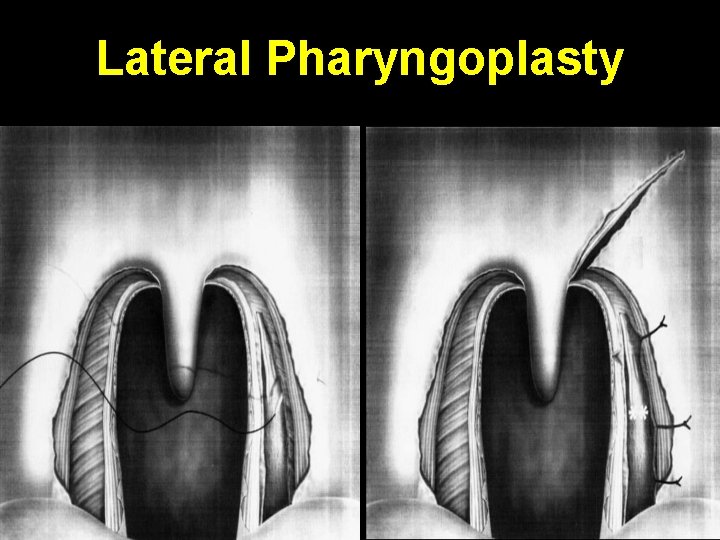
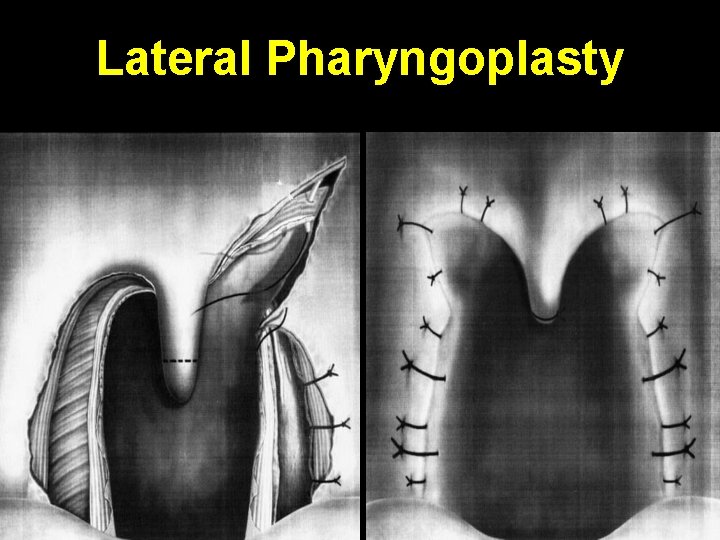
Lateral Pharyngoplasty

Lateral Pharyngoplasty

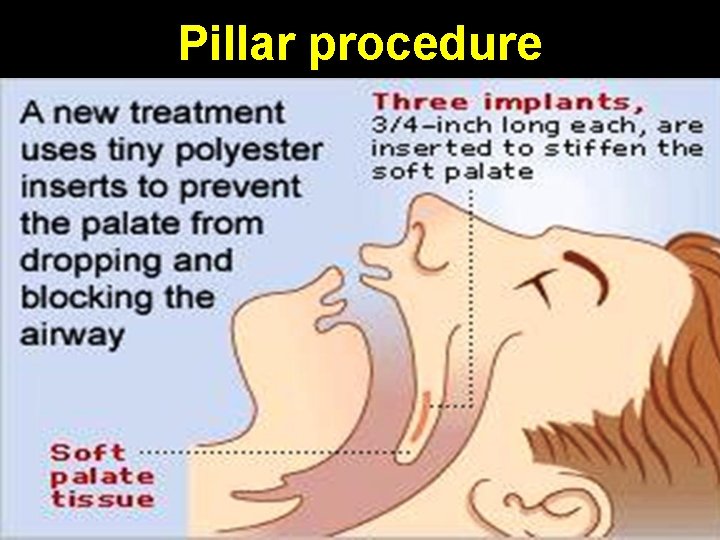
Palatal stiffening surgery Done primarily for snoring • Injection of sclerosing agents into soft palate • Laser-assisted palatal stiffening operation: longitudinal strip of palatal mucosa removed lesion heals by scarring • Cautery-assisted palatal stiffening operation • Pillar procedure

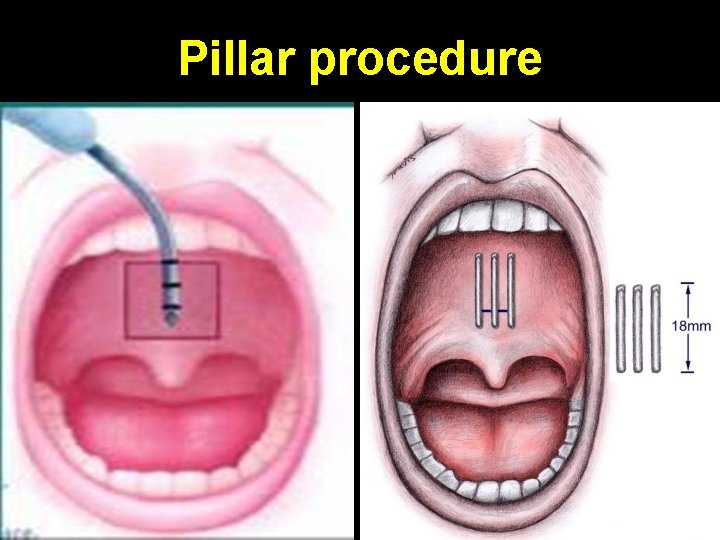
Pillar procedure

Pillar procedure

Tongue base surgery 1. Radiofrequency tongue base somnoplasty 2. Submucosal Minimally Invasive Lingual Excision or Coblation tongue base ablation 3. Laser–assisted tongue base ablation 4. Lingual tonsillectomy 5. Linguloplasty 6. Tongue base suspension

Tongue base Somnoplasty

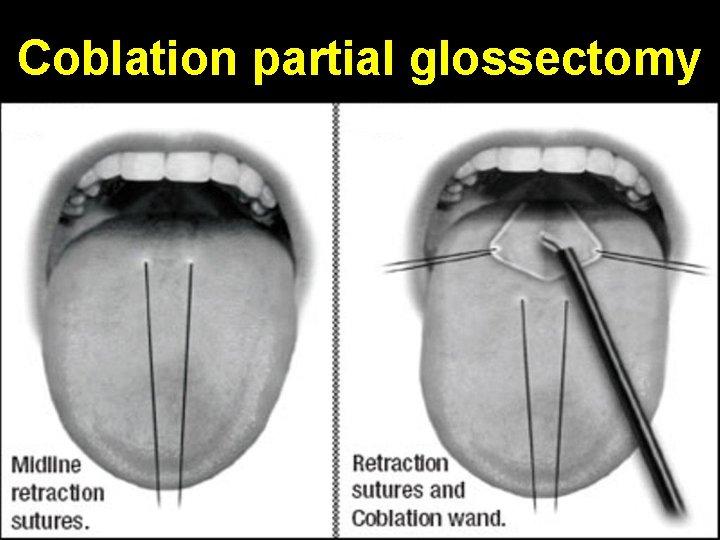
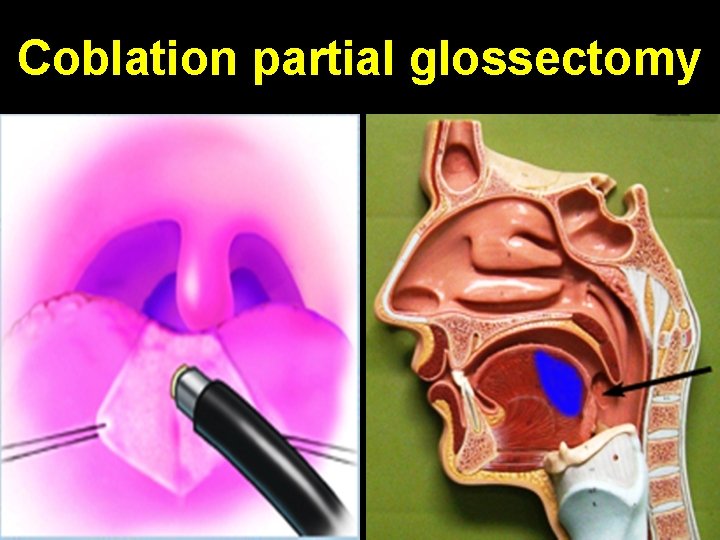
Coblation partial glossectomy

Coblation partial glossectomy

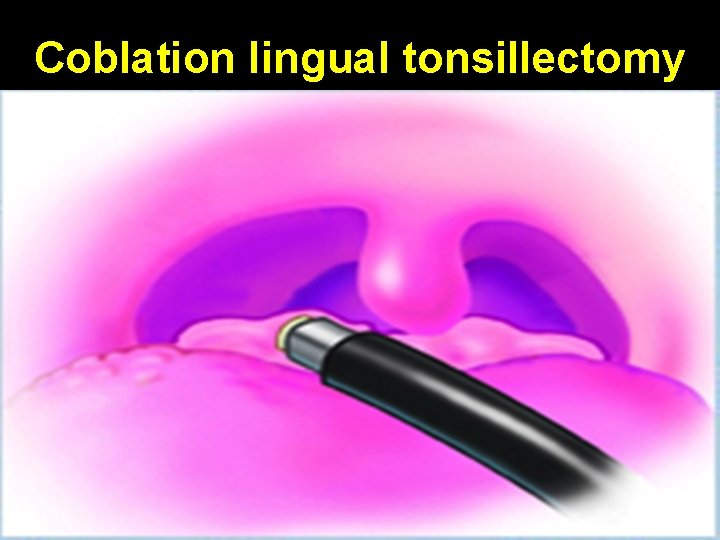
Coblation lingual tonsillectomy

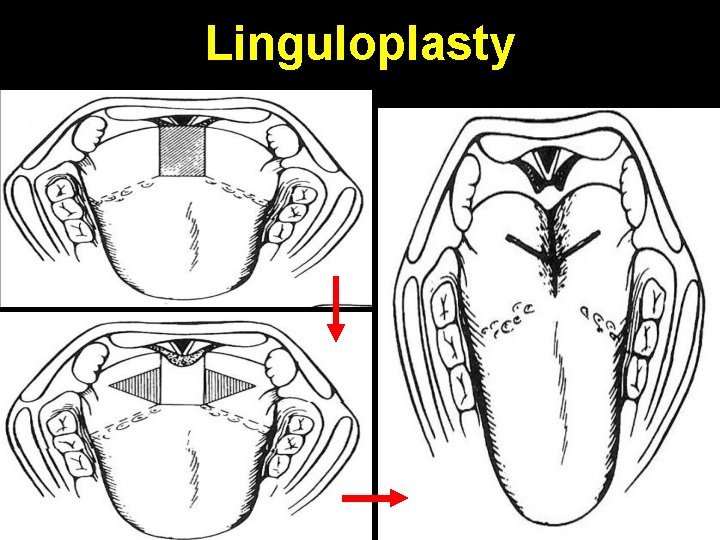
Linguloplasty

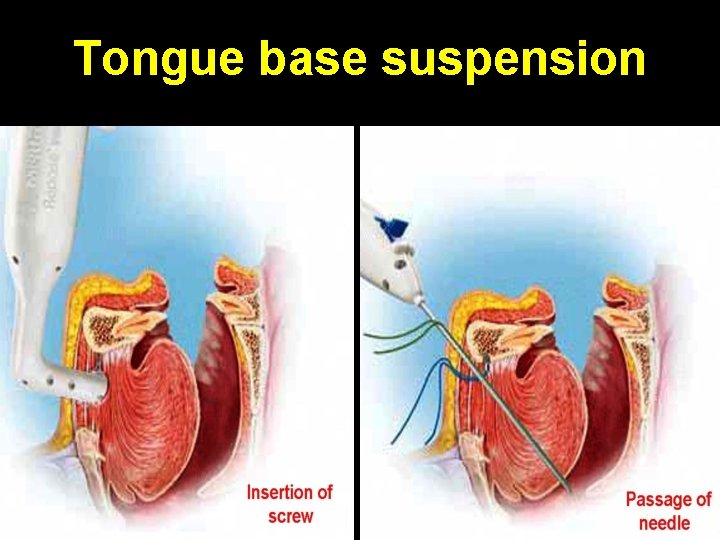
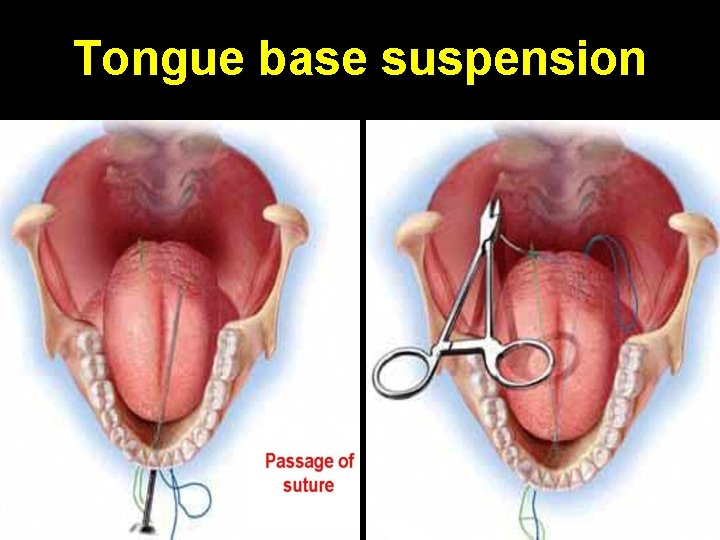
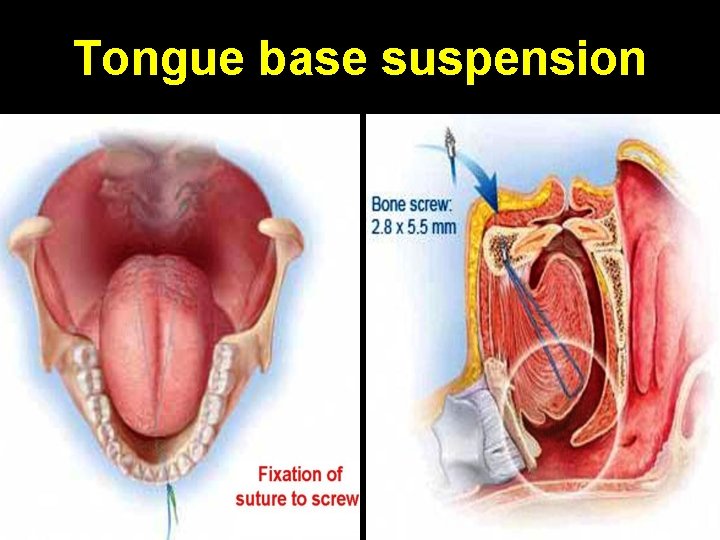
Tongue base suspension

Tongue base suspension

Tongue base suspension

Maxillofacial Procedures Relieve tongue base level obstruction 1. Maxillo-mandibular osteotomy & advancement 2. Genioglossus advancement 3. Maxillary expansion 4. Mandibular expansion 5. Infra-hyoid myotomy & superior suspension 6. Supra-hyoid myotomy & anterior advancement

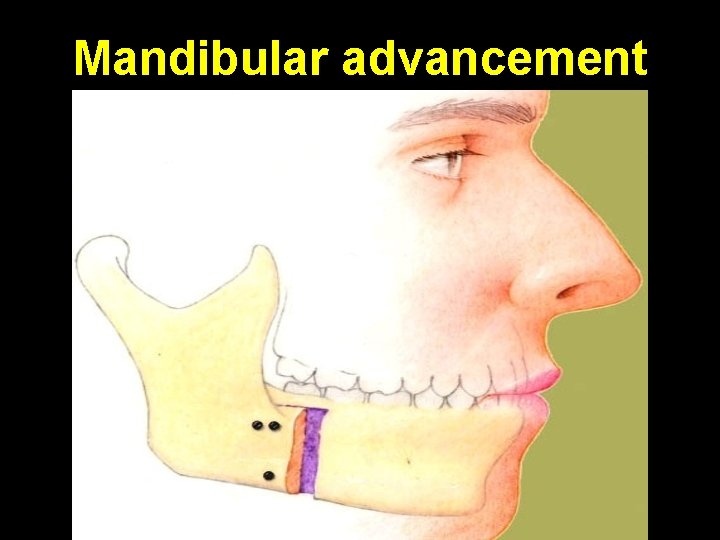
Mandibular advancement

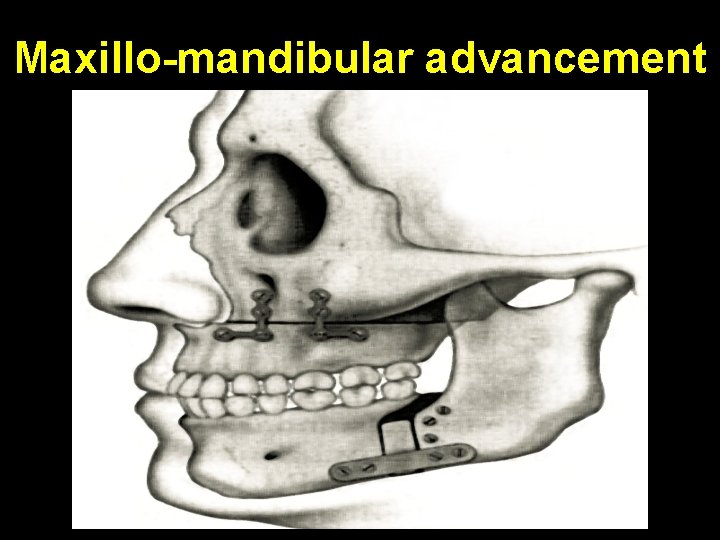
Maxillo-mandibular advancement

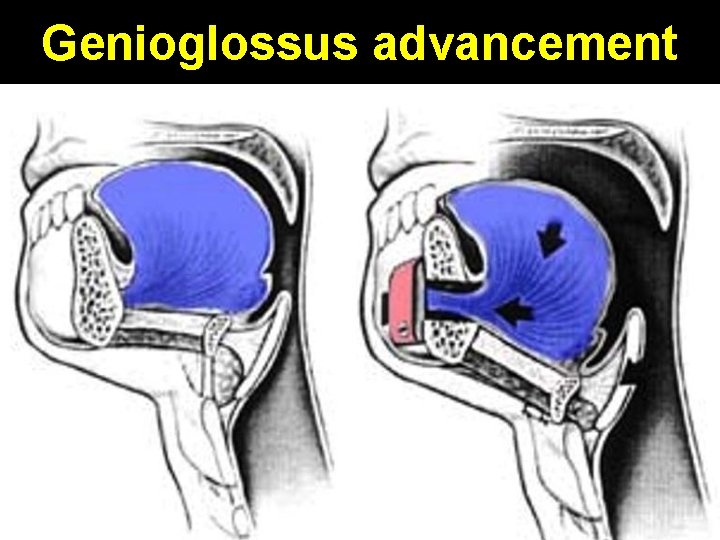
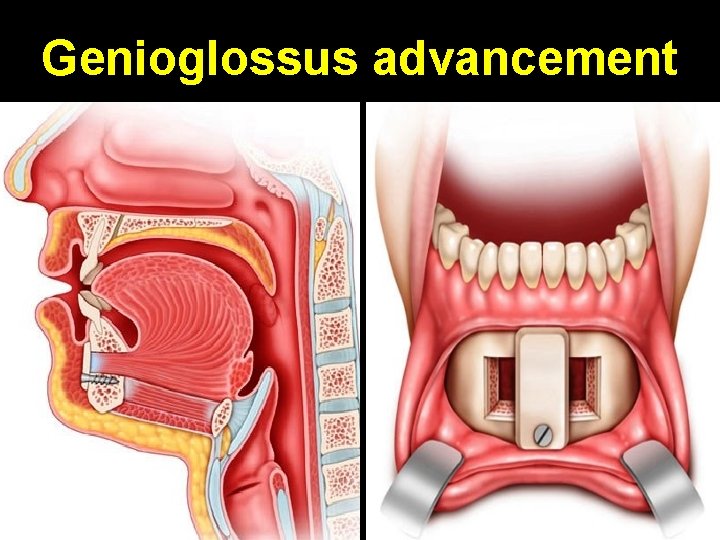
Genioglossus advancement

Genioglossus advancement

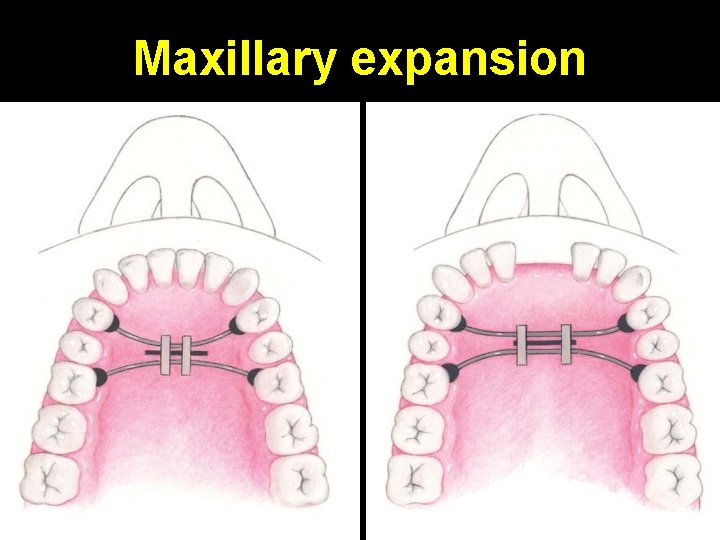
Maxillary expansion

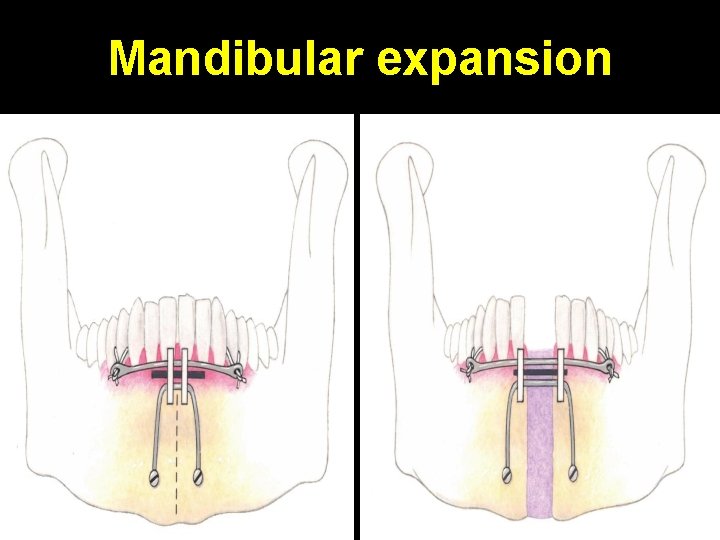
Mandibular expansion

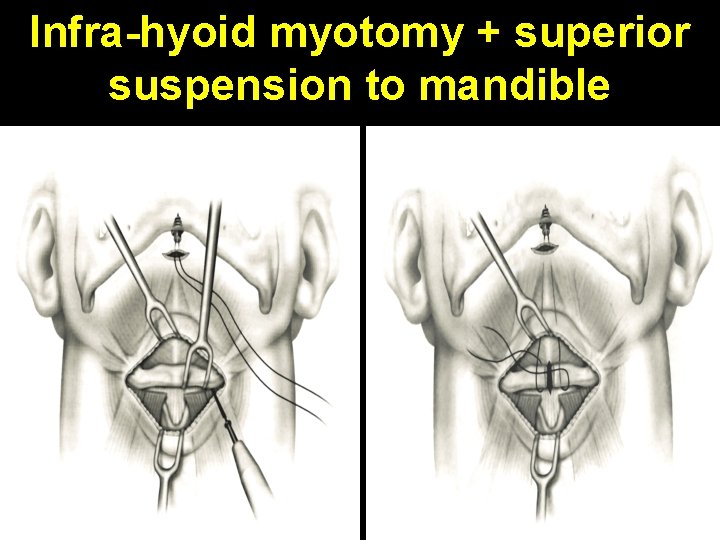
Infra-hyoid myotomy + superior suspension to mandible

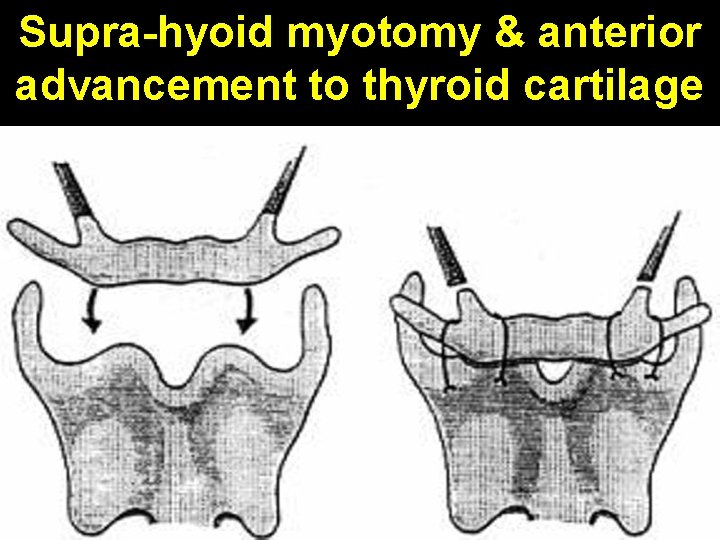
Supra-hyoid myotomy & anterior advancement to thyroid cartilage

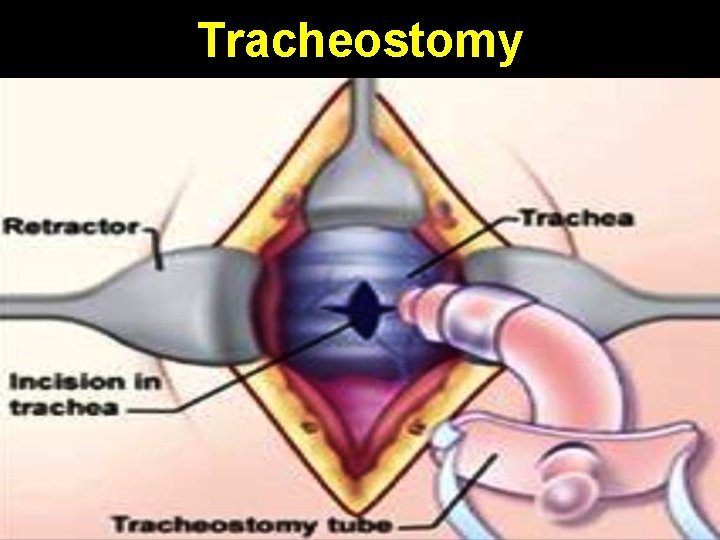
Tracheostomy

Treatment of central sleep apnea • Acetazolamide: induces metabolic acidosis & increases baseline ventilation • Theophylline: respiratory stimulant • Zolpidem: sedative hypnotic, consolidates sleep • Continuous positive airway pressure • Adaptive servo ventilation: provides a fixed CPAP of 5 cm water. Better than nasal CPAP.

Thank You