Plasma Cell Dyscrasias Miten R Patel MD Cancer


































- Slides: 41

Plasma Cell Dyscrasias Miten R. Patel, MD Cancer Specialists of North Florida

Disclosures • None

Objectives • • • Review types of Plasma cell dyscrasias Epidemiology and definitions Presenting signs and symptoms Myeloma staging Couple of cases Treatment overview

Plasma Cell Dyscrasias • Monoclonal Gammopathy of Unknown Significance (MGUS) • Smoldering Myeloma (SMM) • Multiple Myeloma (MM) • Waldenstroms Macroglobulinemia (WM) • Amyloidosis • Solitary plasmacytoma • POEMS syndrome

MGUS • Mean age at diagnosis – 70 yo • M>F, incidence increases with age, found in 1 -2% of adults • African Americans 2 -3 x > Caucasians • Present in 3% of persons >50 and 5% of persons over the age of 70 • Most cases sporadic but relatives of patients with MGUS/myeloma have an increased risk (RR 2 -3)

MGUS • Definition – Serum monoclonal protein <3 g/d. L, bone marrow plasma cells <10%, and absence of end organ damage • • Hypercalcemia Renal Failure Anemia/Thrombocytopenia Lytic bone lesions

MGUS • Non-Ig. M MGUS – Progresses to myeloma – Rarely, to AL amyloid, light chain disease or other lymphoproliferative disorder • Ig. M MGUS – Progresses to Waldenstroms macroglobulinemia – Rarely, to myeloma, AL amyloidosis or lymphoma

MGUS • Part of the spectrum of smoldering myeloma and multiple myeloma • Characterized by a monoclonal protein level of <30 g/L (m spike of 3. 0 g/d. L), <10% plasma cells in the bone marrow • Progression to MM or related disorder is about 1% per year. • Clinically asymptomatic premalignant condition

MGUS • No symptoms? – Pts. identified when undergoing testing for other conditions such as neuropathy, vasculitis, hemolytic anemia, rashes, hypercalcemia, elevated ESR, elevated total protein – Likely had existed for years before diagnosis – Finding on labs - usually elevated total protein, immunoglobulin, abnormal SPEP/UPEP, positive IFE, or abnormal light chain ratio

MGUS – Workup • Labs - CBC + diff, BMP (Cr, Ca), SPEP + IFE, Quant Igs, 24 urine IFE, B 2 microglobulin, albumin, serum free light chains • Imaging – Skeletal survey, Certain cases - MRI & PET scan • Bone Marrow biopsy & aspirate – Cytogenetics & FISH studies

MGUS • Once confirmed (Monoclonal protein <3 g/d. L, <10% plasma cells, no CRAB symptoms) – no treatment • Serial followup, every 3 -6 months, exam, assessment and labs, less often after 2 years. • Monitor for developing symptoms (bone pain, hypercalcemia, kidney dysfunction, anemia, etc) • SMM – every 3 months until progression • No treatment unless symptomatic MM

Smoldering Myeloma • Smoldering Myeloma (aka asymptomatic multiple myeloma) – Same as MM but without symptoms and • Hgb > 10. 5, • Monoclonal Ig Peak (usually > 3 g/d. L and/or >10 but <60% clonal plasma cells) • Normal serum Ca and Cr levels • No lytic bone lesions • REQUIRES NO TREATMENT • >60% plasma cells or FLC ratio >100 even without end organ damage, best classified as multiple myeloma

Multiple Myeloma • Presentation – Weakness, Fatigue, Pallor (32%) – Weight Loss (24%) – Radiculopathy, cord compression – Bone pain (58%), fractures – Recurrent infections (dysfunctional immunoglobulin) – Labs – Anemia (73%), hypercalcemia (28%), elevated total protein, kidney dysfunction (48%)

Multiple Myeloma Rouleaux Formation Elevated Sed Rate Elevated C Reactive Protein Normocytic, normochromic anemia Renal Disease, Cr > 2 mg/d. L in 19% Renal insufficiency caused by cast nephropathy (myeloma kidney) or hypercalcemia • Altered mental status caused by hypercalcemia and hyperviscosity • • •

Multiple Myeloma • Monoclonal Ig – – Ig. G 60% Ig. A 20% Light chain only 18% (K>L) Ig. M, Ig. D, Ig. E, non-secretory < 1% • For nonsecretory myeloma (no M protein) or light chain only, diagnosis is often made with bony lesions and plasmacytosis by bone marrow

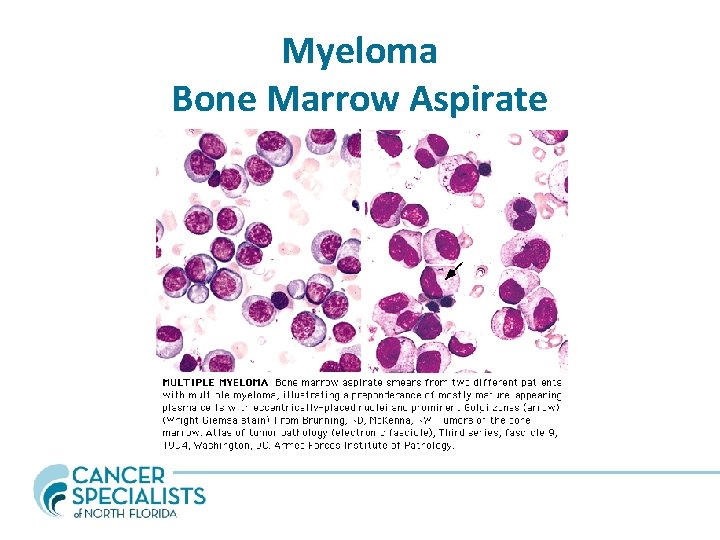
Myeloma Bone Marrow Aspirate

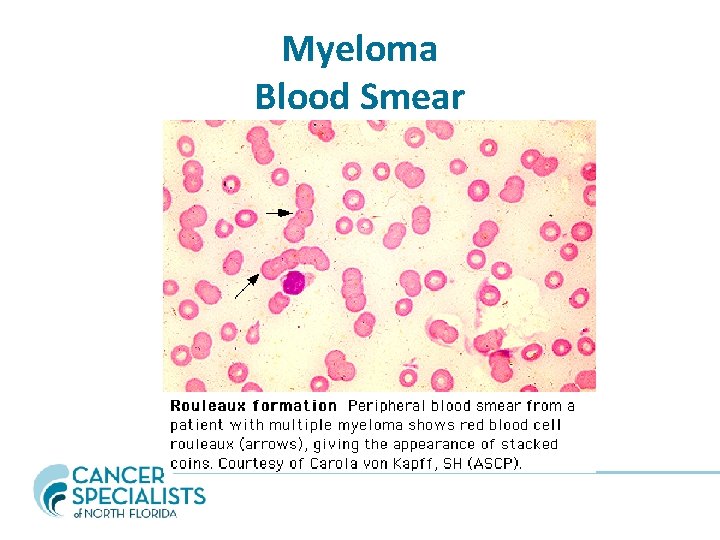
Myeloma Blood Smear

Myeloma Staging Durie Salmon • Stage 1 – Ca <12, Hgb >10, Normal skeletal survey or solitary plasmacytoma, low M protein with Ig. G <5 g/d. L or Ig. A <3 g/d. L, Bence Jones protein <4 g/24 h • Stage 2 – Neither stage 1 or 3 • Stage 3 – One of the following: Hgb <8. 5, Ca >12, multiple lytic lesions, high M component (Ig. G >7, Ig. A >5 or Bence Jones >12 gm)

• Stage 1 Myeloma Staging ISS – B 2 M ≤ 3. 5 and albumin ≥ 3. 5 • Stage 2 – B 2 M > 3. 5 but <5. 5 or albumin >3. 5 • Stage 3 – B 2 M ≥ 5. 5

Case Presentation • 41 yo WF with no symptoms goes to annual physical at office based clinic. • No symptoms other than mild fatigue • Routine annual labs drawn

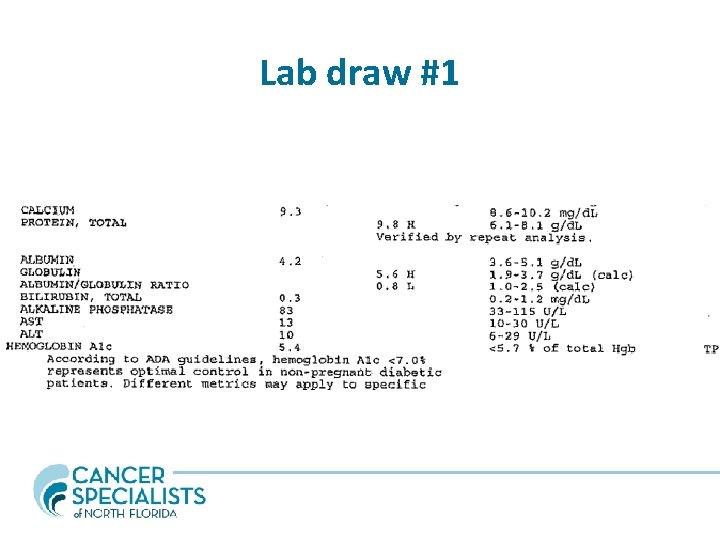
Lab draw #1

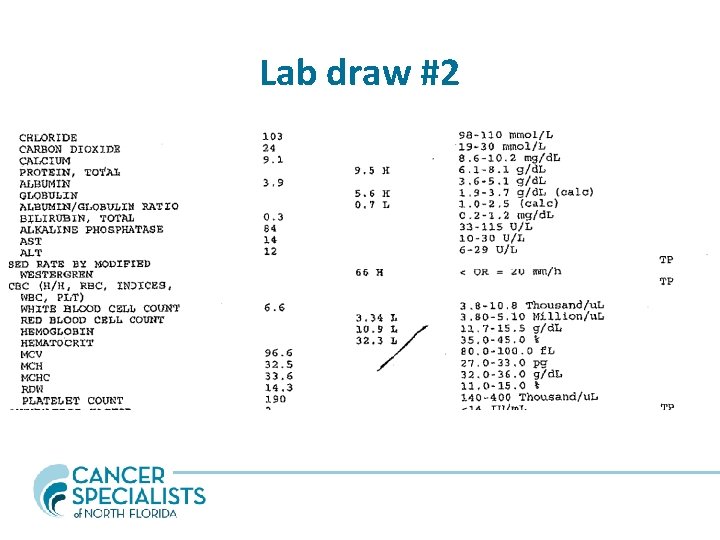
Lab draw #2

Lab draw #3

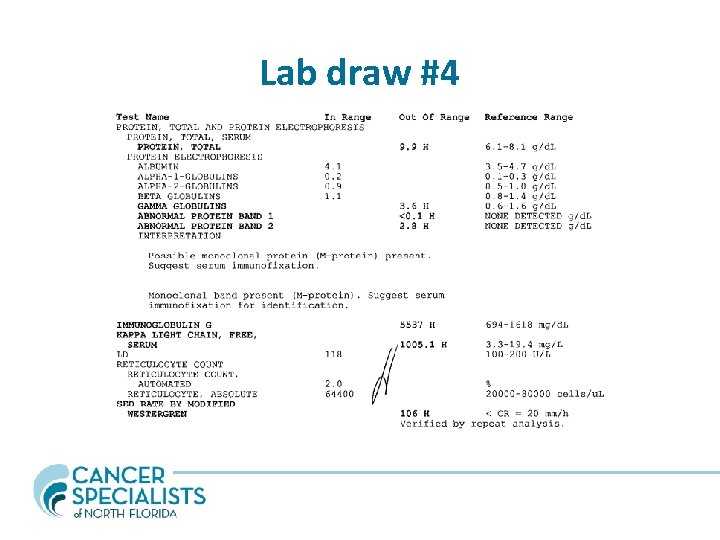
Lab draw #4

Bone Marrow Biopsy

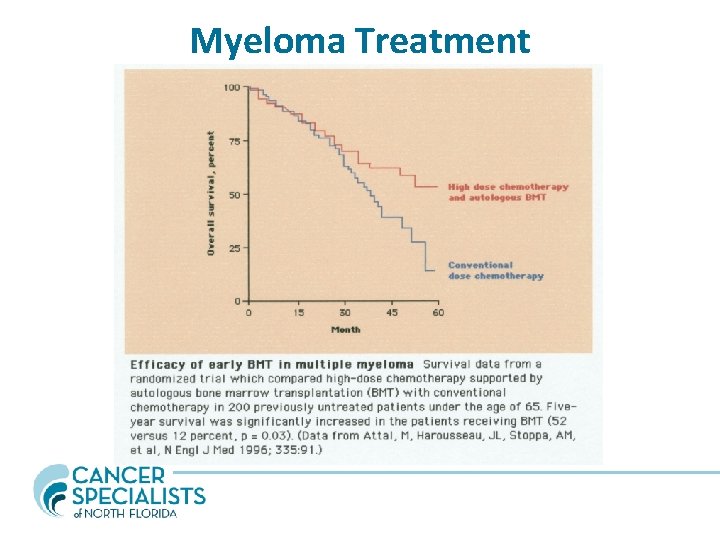
Myeloma Treatment • Determine eligibility for HDT and SCT – Age, overall health, psychological evaluation – Avoid alkylating agents (marrow toxic) – Chemotherapy to induce remission – Refer for stem cell collection and transplant – Maintenance therapy – Regular monitoring – ASCT improves median OS by >12 months

Myeloma Treatment • Transplant ineligible – Immunomodulators (Thalidomide, Revlimid, Pomalyst) • DVT risk – Proteosome inhibitors (Velcade, Kyprolis) – Chemotherapy (MP, VAD, Doxil, Hyper. CVAD) – Supportive care • Bisphonates

Myeloma Treatment

Solitary Plasmacytoma • Approx 3% of myeloma patients • No or very low myeloma protein in serum or urine • MR must be done to evaluate patient as it may detect other bone lesions (upstage the patient to myeloma) • Presence of monoclonal protein >1 yr after irradiation denotes progression to myeloma • Treat with XRT (at least 45 Gy). • MM manifests overtime, only 20% remain disease free at 10 yrs • Median time to progression is 2 yrs

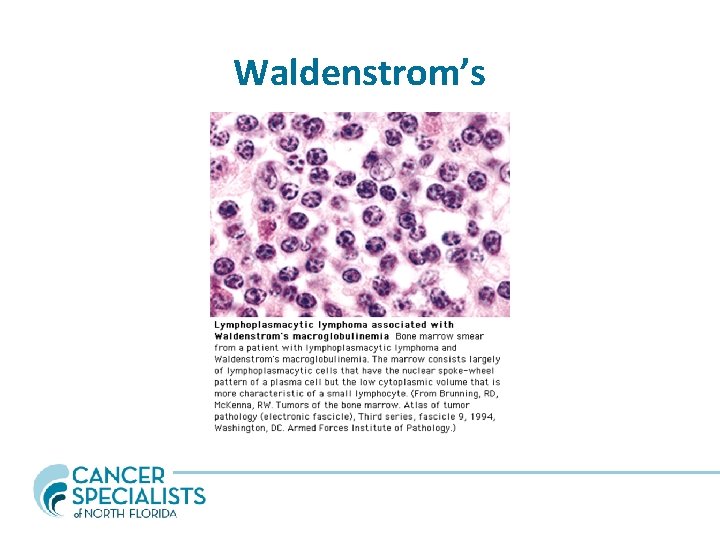
Waldenstrom’s • • • Lymphoplasmacytic bone marrow infiltration Malignant B lymphocytes producing monoclonal Ig. M Median age 65; Whites > Blacks; M>F 1500 cases in the US per year Hyperviscosity syndromes – neurologic complaints including vision change, headache, vertigo, nystagmus, dizziness, deafness, diplopia and ataxia • 10 -20% of pts. Have a cryoglobulin (Type I) which precipitates at high T >22 C on cold exposure may cause symptoms such as Raynauds phenomenon, urticaria, purpura and acral cyanosis. • Diarrhea and Steatorrhea (Ig. M infiltration into GI tract)

Waldenstrom’s

Waldenstrom’s Treatment • Goal to reduce hyperviscosity (Ig. M is a pentamer!) and lymphoproliferation – Pheresis if symptoms from the hyperviscosity causing severe neurologic deficits • Chemotherapy – Chlorambucil, other CCU, Cladribine and Fludarabine, Rituxan, IFN, Thalidomide, Ibrutinib, Velcade

Case #2 • 73 yo WF presenting with neuropathy, dizziness, 40 lb weight loss, Ig. M 5454, immediately hospitalized due to neurologic symptoms, started plasma exchange

Case #2 • Bone Marrow – Bone marrow, flow cytometric immunophenotypic analysis: Monoclonal plasma cells and lymphocytes identified, consistent with Waldenstrom's macroglobulinemia.

Case #2 • Dramatic decline in Ig. M (>5000 to <2000) after plasma exchange • Symptoms have improved • Treated with Rituxan and Velcade, Ig. M started rising again. • Changed to Ibrutinib, symptoms remain improved, Ig. M stabilized below 1500 • Ig. M stable for > 2 years now

Amyloidosis • Occurs in 10% of patients with MM • Infiltrative process resulting from amyloid fibril deposition in organs • Fibril is made from the terminal amino acid residue (NH 2) of the variable portion of the light chain Ig molecule • Produced by clonal plasma cells

Amyloidosis • Renal disease - asymptomatic proteinuria to nephrotic syndrome • Cardiomyopathy • Hepatomegaly • Neuropathy • Pseudohypertrophy of muscles • Bleeding problems (Factor X def, Liver dz) • Lung and Skin infiltration

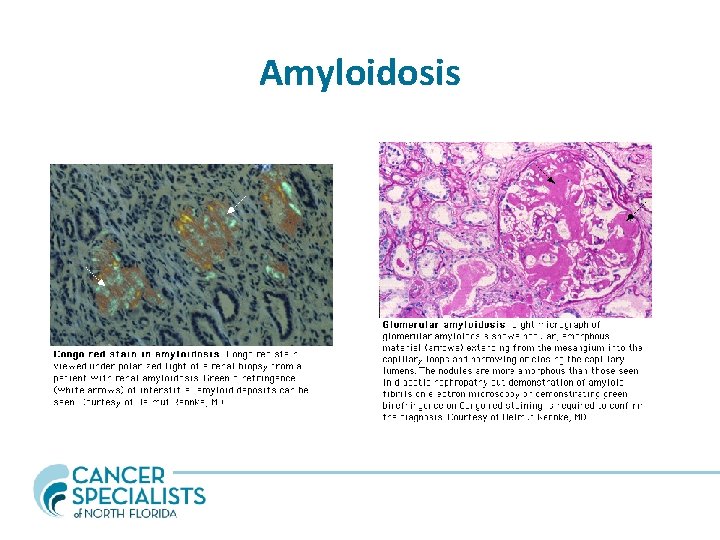
Amyloidosis

Amyloidosis • AL should be suspected in patients with plasma cell dyscrasia history • Biopsy results as shown • SPEP/UPEP - confirms monoclonal protein (plasma cell population) • Treatment - treat underlying plasma cell dyscrasia

Summary • MGUS, SMM and MM are a spectrum of the same disease process • MGUS and SMM patients need close observation • WM patients present with hyperviscosity symptoms and very high Ig. M, total protein • Amyloidosis (AL) is characterized by fibril deposition in organs with damage (most commonly heart/liver/kidney) • Treatment is dependant on the disease process

Questions Miten R. Patel, MD Office 904 -516 -3737 Cell phone 904 -451 -9820 miten. patel@csnf. us