Nutrition and Feeding Dr Rakesh Sharma Ahmedabad Breast

Nutrition and Feeding Dr. Rakesh Sharma Ahmedabad

• Breast feeding • Complimentary feeding • Obesity 2

Infant feeding • Feeding the fetus – Feeding the pregnant mother • Feeding the infant 0 - 6 months – Exclusive breast feeding • Feeding beyond 6 months – Complementary feeding +BF 1 April 2018 3

What is Optimal Infant and Young Child Feeding? • Optimal feeding is defined as – – Exclusive breastfeeding from birth to six months of age and… – Thereafter continued breastfeeding for 2 years with adequate and safe complementary feeds to meet nutritional needs of a young child 26 February 2021 4 4

Definitions of Infant Feeding Exclusive breast feeding Only breast milk is given / No other food or drink, not even water is given • Define mixed feeding and replacement feeding. 26 February 2021 5 5
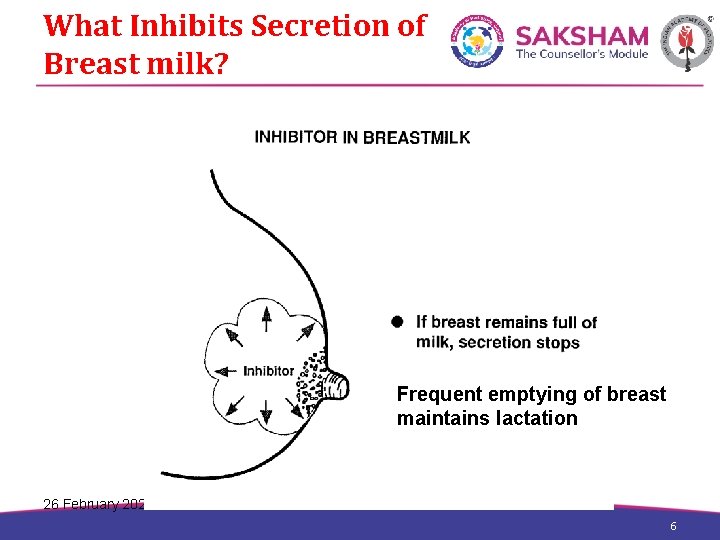
What Inhibits Secretion of Breast milk? Frequent emptying of breast maintains lactation 26 February 2021 6 6

Observe breastfeeding • Make the mother comfortable • Ask her to put the child to breast if s/he is awake or ready to feed. • Watch the mother baby pair for. . è Interaction è Signs of attachment è Signs of effective suckling è Correct position if child not well attached è Any Signs of discomfort or pain to mother • Observe the entire feed preferably or at least for 4 minutes 26 February 2021 7
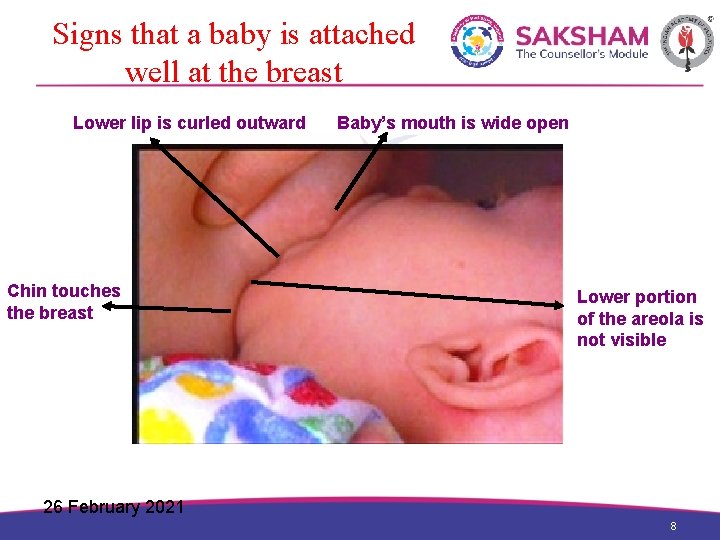
Signs that a baby is attached well at the breast Lower lip is curled outward Chin touches the breast Baby’s mouth is wide open Lower portion of the areola is not visible 26 February 2021 8

Check for attachment (4 signs of attachment) 1. Chin touching breast 2. Mouth wide open 3. Lower lip turned outwards 4. More areola visible above than below the mouth Remember… o All of these signs should be present in a well attached baby o An infant who is not able to feed or is not sucking may be having serious illness and needs immediate treatment 26 February 2021 9
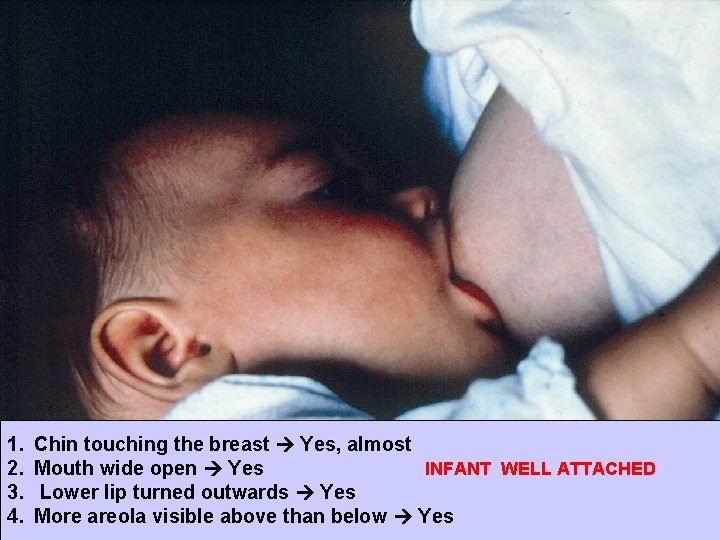
1. 2. 3. 4. Chin touching the breast Yes, almost Mouth wide open Yes INFANT WELL ATTACHED Lower lip turned outwards Yes 5/1 26 February 2021 More areola visible above than below Yes 10
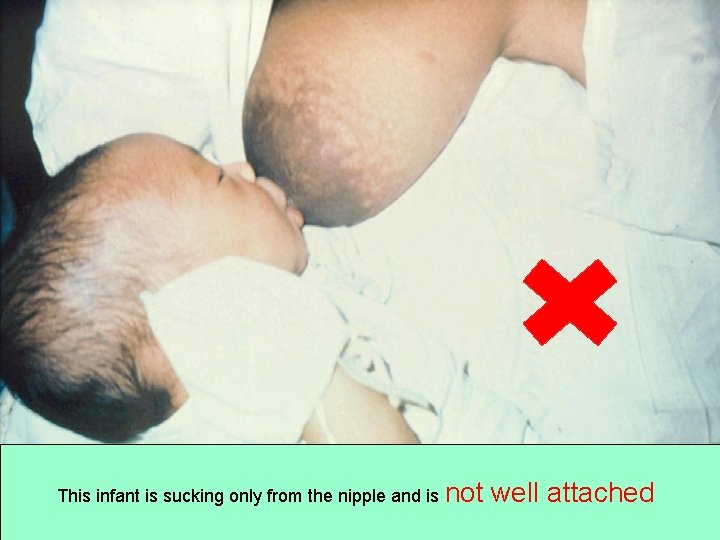
This infant is sucking only from the nipple and is not well attached 5/5

Position of the baby in relation to the mother 4 signs of correct positioning are. . 1. The baby’s whole body facing the mother 2. The baby’s entire body including head and neck supported 3. The baby’s head & neck in a straight line with his body 4. Baby’s abdomen touching mother’s abdomen, to be very close to the mother 26 February 2021 12
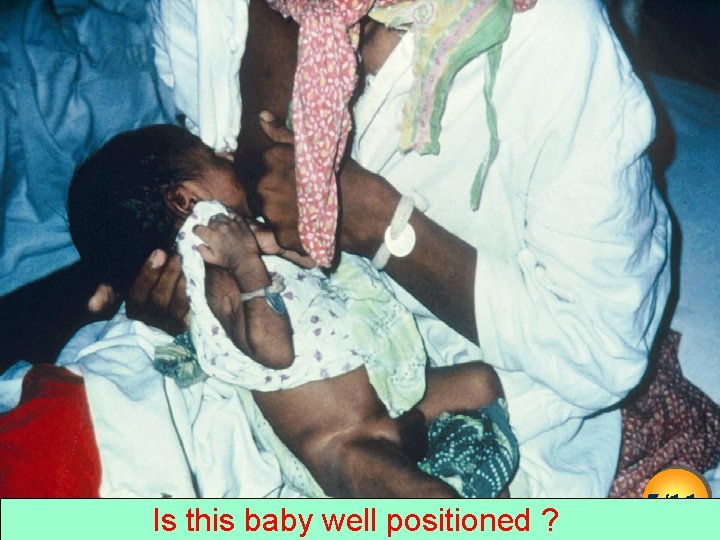
Is this baby well positioned ? 5/11
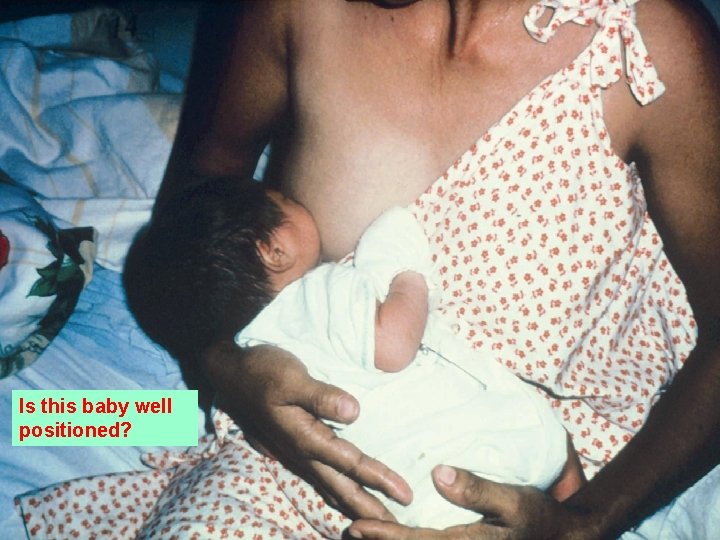
Is this baby well positioned?

Formation of Teat • For effective suckling the baby does not take just the nipple but a mouthful of the areola and the breast tissue beneath, which contains the lactiferous sinuses 26 February 2021 15 15

Breast & Nipple problems • If the mother reports pain or difficulty while feeding, examine breast and nipple and look for… o o o Sore / cracked nipple Retracted (inverted) nipple Breast engorgement Examine every mother for nipple and breast issues as well as observe the mother giving breastfeeding 26 February 2021 16
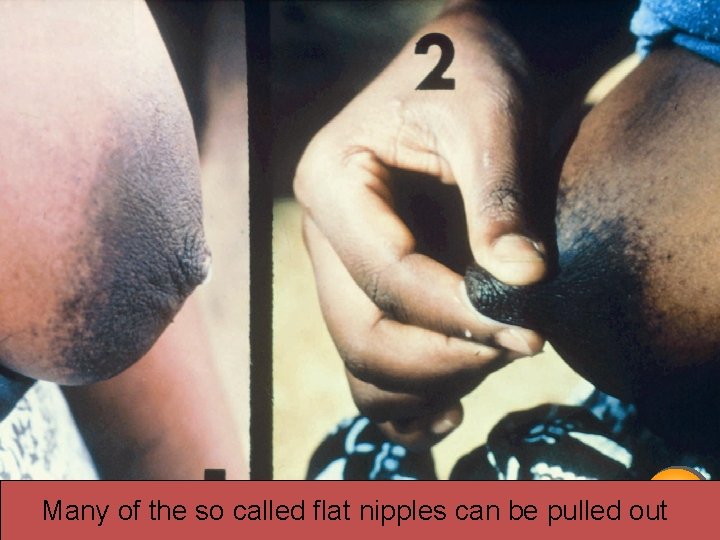
14/2 26 February 2021 Many of the so called flat nipples can be pulled out 17
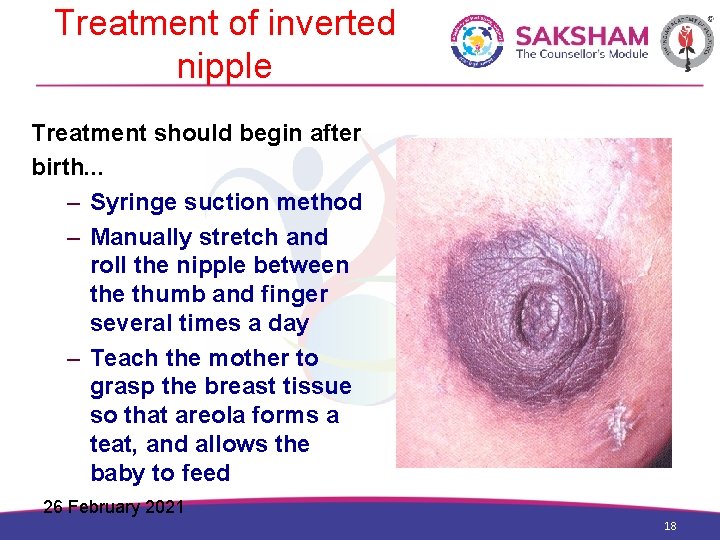
Treatment of inverted nipple Treatment should begin after birth. . . – Syringe suction method – Manually stretch and roll the nipple between the thumb and finger several times a day – Teach the mother to grasp the breast tissue so that areola forms a teat, and allows the baby to feed 26 February 2021 18
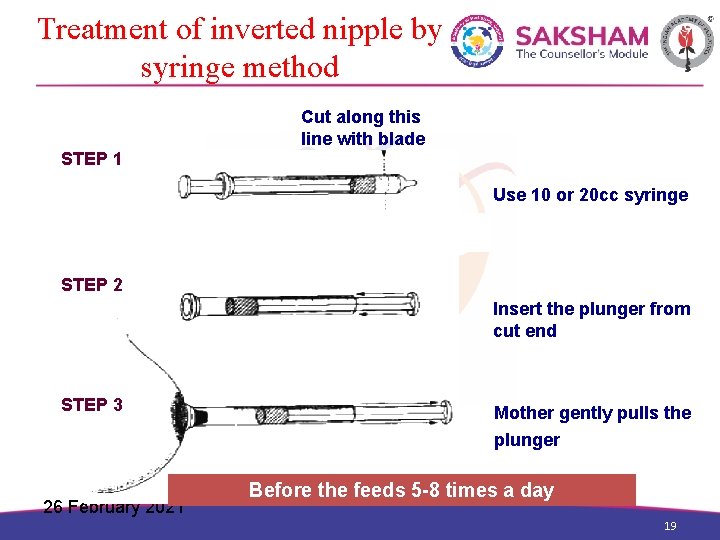
Treatment of inverted nipple by syringe method Cut along this line with blade STEP 1 Use 10 or 20 cc syringe STEP 2 Insert the plunger from cut end STEP 3 26 February 2021 Mother gently pulls the plunger Before the feeds 5 -8 times a day 19
Sore nipple Causes o Incorrect attachment : Nipple suckling o Frequent use of soap and water o Candida (fungal) infection Treatment • Continue breast feeding and correct the position & attachment • Apply hind milk to the nipple after feeds • Expose the nipple to air between feeds • EBM, if severe discomfort 26 February 2021 20
Breast engorgement Causes v Delayed and infrequent breastfeeds v Incorrect latching of the baby Treatment o Give analgesics to relieve pain o Apply warm packs locally o Gently express milk prior to feed o Put the baby frequently to the breast 26 February 2021 21

Remember… o Baby needs mother’s help initially to take the breast into his mouth o Keeping baby and mother together makes breastfeeding successful o More suckling makes more milk o For sustained milk secretion, it is essential to breastfeed frequently 26 February 2021 22 22
Advantages of Breastfeeding to the infant Breastfeeding Breastmilk l Perfect nutrients l Easily digestible l Ready to serve l Protects against infection l Protects against adult onset diseases (heart disease/ diabetes/ lymphoma) 26 February 2021 l Helps bonding and development l Helps in adequate growth and development l Enhances brain & visual development l Prevents hypothermia 23 23

Advantages of Breastfeeding to the mother l Reduces post delivery bleeding and anemia (helps in involution of uterus) l Delays next pregnancy l Protects against breast and ovarian cancer l Prevent obesity, helps in regaining figure l Convenient, decreases mother’s workload & saves time and energy l Provides sense of satisfaction and feeling of accomplishment to mother 26 February 2021 24 24

26 February 2021 25 25

Storage of Breast milk Room temperature for 6 -8 hours Refrigerator for 24 hours. Preferably in stainless steel containers 26
Disadvantages of Artificial Feeding l More diarrhea, ARI and other infections Infant l Interferes with bonding l More allergy and intolerance milk l Requires preparation l Not easy to digest l l Lacks balance of nutrients Increased risk of some chronic diseases l Overweight babies l More likely to die from infection & malnutrition l l May become pregnant sooner 26 February 2021 Increased risk of anemia, osteoporosis, ovarian and breast cancer Mother 27 27

Prerequisites for successful breastfeeding – A willing and motivated mother – An active and sucking newborn – A motivator who can bring both mother and newborn together ( health professional or relative ) 26 February 2021 28 28

Avoid bottle feeding • Bottle feed baby develops nipple confusion and refuses to feed on breast • Single session lesser the chances of successful breast feeding. • Increases chances of dental caries and serious illness like diarrhea and pneumonia. • Risk of overweight and obesity • Also discourage Pre lacteal feeds like Honey, glucose water and other things. 29

Disadvantages of cow’s milk o o o Bacterial contamination likely No active anti-infective substances Too high in protein & casein Low in cystine & deficient in taurine Too much of saturated fats & inadequate amounts of cholesterol & essential fatty acids like linoleic acid Deficient in lipase Inadequate amount of lactose Too much of salts ( sodium, potassium & chloride ) Too much of minerals like calcium & phosphates Low in iron which is poorly absorbed Deficient in vitamins 26 February 2021 30 30

Complementary feeding 31

Adequacy (Quality) • Staples: Cereals (Rice, wheat, maize, millets) and Legumes • Fats (Vegetable oils/butter/ghee; 1 g ~ 9 Kcal) and sugars to improve energy density and taste • Foods of animal origin (Milk, curd, eggs, meat, fish) to provide good quality proteins, vitamin A and calcium. • Vegetables and Fruits to provide micronutrients e. g. iron and vitamins. Supplements e. g. iron might be required. 32 32

Other Attributes of Complementary Foods p Right consistency p Soft p Easy to digest p Inexpensive p Locally available p Culturally acceptable p Easily prepared at home 33 33

Energy density in foods given to infants and young children can be increased in four different ways 1. By adding a teaspoonful of oil or ghee to the child's food. Fat is a concentrated source of energy and substantially increases energy content of food without increasing the bulk. There is no reason to feel that a child can not digest visible fat when added to food. 2. By adding a teaspoonful of sugar or jaggery to the child's food. Children need more energy and hence adequate amounts of sugar or jaggery can be added to their food. 3. By giving malted foods. Malting reduces the viscosity of foods and hence a child can eat more at a time. Malting is germinating whole grain cereals or pulses, drying it after germination and grinding. Infant Food Mixes prepared after malting the cereal or pulse will provide more energy. Flours of malted food when mixed with other foods help in reducing the viscosity of that food. Amylase Rich Flour (ARF) is the scientific name given to flours of malted foods and must be utilized in infant foods. 4. By feeding thick but smooth mixtures. Thin gruels do not provide enough energy. A young infant particularly during 6 -9 months requires thick but smooth mixtures as hard pieces in the semi-solid food may cause difficulty if swallowed. Semi-solid foods for young infants can be passed through a sieve by pressing with a ladle to ensure that the mixed food is smooth and uniform without any big pieces or lumps. • 34

Variety of Foods o Start at 6 m with small amounts of food; increase quantity with age, maintaining frequent breast feeding o Increase food consistency & variety with age § Can feed mashed & semi-solids (e. g. porridge) at 6 m § Can feed finger foods by 8 -9 m § By 12 m, family foods can be eaten o Combine foods (e. g. rice and legumes) to provide good mixture of amino acids 35 35

Foods to Avoid § Tea & coffee: interfere with iron absorption § Aerated beverages: No nutritional value § Too much sugary drinks & Fruit juices: cause decreased appetite for other nutritious foods and also may cause loose stools. 36 36

Adequacy (Frequency & Amount) 6 -12 months Give at least one katori (150 -200 m. L) serving* at a time • Khichdi or dalia or sooji (semolina) with added oil/ghee • Mashed roti/rice/bread mixed in thick dal or sweeetened undiluted milk • Add cooked/pureed vegetables or meat also in the servings • Sevian/dalia/halwa/kheer/biscuits@ prepared in milk or any cereal porridge cooked in milk • Mashed boiled/fried potatoes • Mashed banana, sapota, mango, papaya *3 times per day if breastfed; 5 times per day if not breastfed @ Only when fresh food is not available 37 37

Feeding Techniques • Feed infants directly & assist older toddlers eat; be sensitive to hunger & satiety cues • Feed patiently; encourage, but don’t force • If child refuses, experiment with different food combinations, tastes, textures • Minimize distractions during meals • Talk to child during feeding; maintain eye contact 38 38

Responsive feeding 39 39

Obesity 40

Causes of obesity in children • • • Increase intake of junk foods & colas. Decreased intake of fruits & vegetables. Decreased physical activity at school & at home. Increased timing of schools & tuitions, leading to sedentary lifestyle. Increased screen time (TV, computer, mobile etc. ) Ignorance of seriousness of the condition. 41

Modalities of Treatment 1. Diet 2. Exercises 3. Screen time 4. Pharmacotherapy 5. Surgical treatment 42

Role of Parents • Healthy attitudes towards the food and Nutrition, Regular family meal. • Concern about own body image! Role model • Talk with Kids about eating habits, emphasis on health and not on weight • Love-Unconditionally(No battles over food) • Involve Kids in food preparations; • Stocking Up on Healthy Foods 43
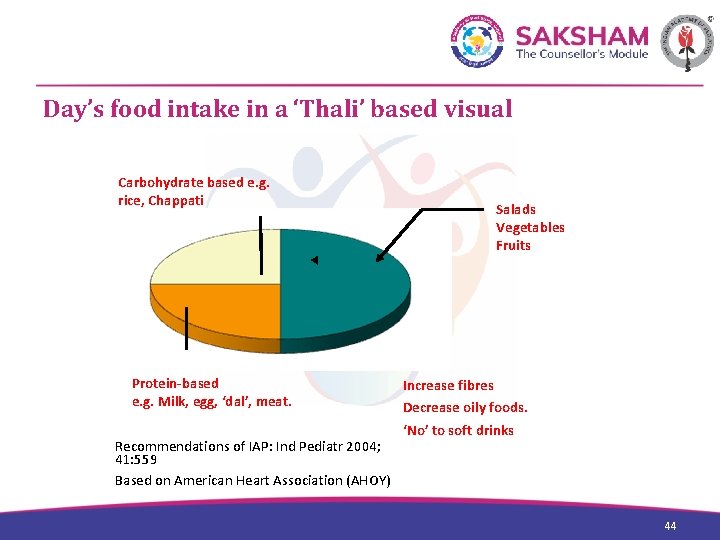
Day’s food intake in a ‘Thali’ based visual Carbohydrate based e. g. rice, Chappati Protein-based e. g. Milk, egg, ‘dal’, meat. Recommendations of IAP: Ind Pediatr 2004; 41: 559 Based on American Heart Association (AHOY) Salads Vegetables Fruits Increase fibres Decrease oily foods. ‘No’ to soft drinks 44

No Substitute to a wholesome diet 45

Healthy Eating Habits • Small, regular meals • Select portion sizes • Eat slowly, chew well, take smaller bites • Make the right choices, read food labels • Do not combine meal times with other activities such as TV viewing, reading, etc. 46

EXERCISE Physical Activity • 60 minutes a day • Formal exercises – Running / jogging – Brisk walking – Sports • Micro-exercise – Not using lift – Household chores 47

Exercise Is Important • Improves strength and endurance • Helps build healthy bones and muscles • Helps control weight & menstrual problems • Be physically active for at least 30 minutes most days of the week 48
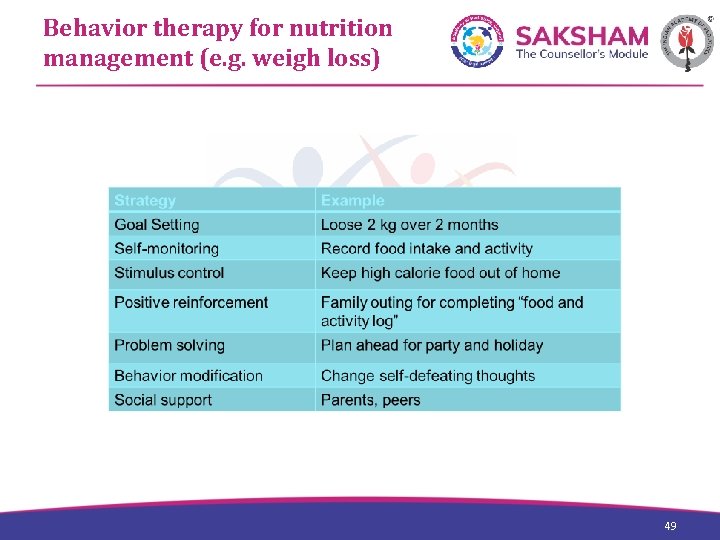
Behavior therapy for nutrition management (e. g. weigh loss) 49

REMEMBER 6 M • • • Moderation Make at home Mindful eating Modeling Maternal education Modification 50

Hope you enjoyed this session Thanks 51

- Slides: 52