ANTICOAGULANTS Classes of Drugs Prevent coagulation Dissolve clots




































































































- Slides: 136

ANTICOAGULANTS

Classes of Drugs Prevent coagulation Dissolve clots Prevent bleeding and hemorrhage Hemostatic Overcome clotting deficiencies (replacement therapies)

Anticoagulant drugs to treat thromboembolism Drug Class Anticoagulant Parenteral Prototype Heparin Action Inactivation of clotting Factors Effect Prevent venous Thrombosis Anticoagulant Warfarin Decrease synthesis of Oral Clotting factors Prevent venous Thrombosis Antiplatelet drugs Aspirin Prevent arterial Thrombosis Thrombolytic Drugs Streptokinase Fibinolysis Decrease platelet aggregation Breakdown of thrombi

Heparin Sulphated carbohydrate Different sizebovine lungs Administration - parenteral- Do not inject IM only IV or deep s. c. Half-life 1 - 5 hrs - monitor a. PTT Adverse effect: hemorrhage Antidote : protamine sulphate

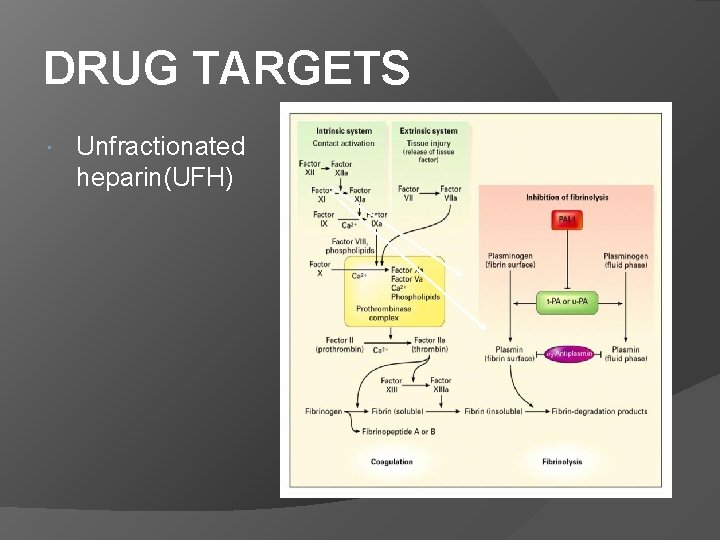
DRUG TARGETS Unfractionated heparin(UFH)

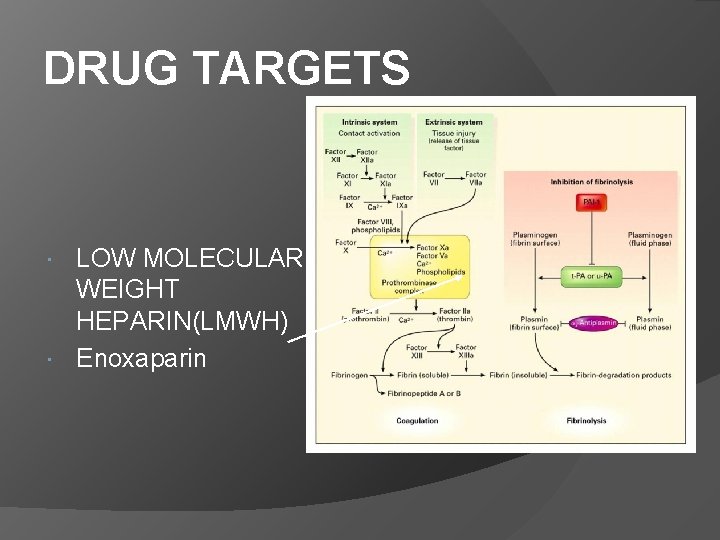
DRUG TARGETS LOW MOLECULAR WEIGHT HEPARIN(LMWH) Enoxaparin

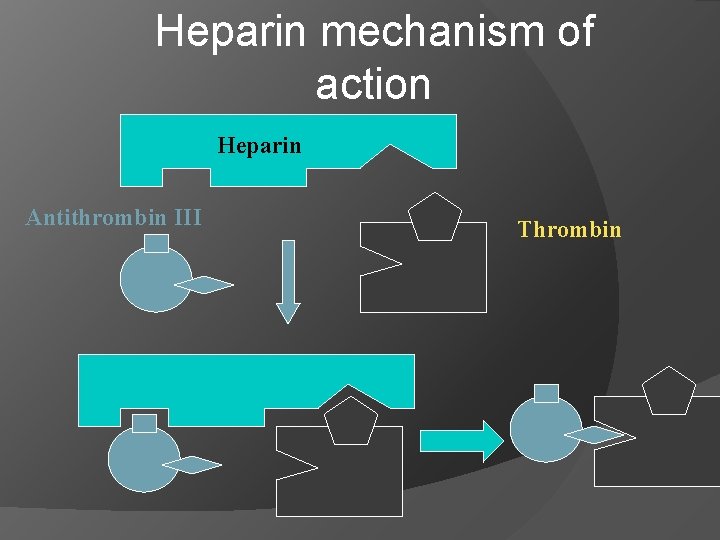
Heparin mechanism of action Heparin Antithrombin III Thrombin

Complications of Heparin Haemorrhage Heparin-induced thrombocytopaenia (HIT) Osteoporosis (long-term only)

Heparin-Induced Thrombocytopaenia Most significant adverse effect of heparin after haemorrhage Most common drug-induced thrombocytopenia A large number of patients receive heparin in the hospital environment.

Non-immune heparin-associated thrombocytopaenia (“HIT Type I”) Benign Up to 10% patients on heparin Rapid decline in platelet count within first 2 days of heparin administration Platelet count >100 000/ul Returns to normal within 5 days despite continued heparin use (or within 2 days if heparin is stopped).

Heparin-induced thrombocytopaenia: “HIT type 2” Potentially catastrophic thrombosis (Heparininduced thrombocytopenia and thrombosis) 8% of patients on heparin develop antibody without becoming thrombocytopenic 1 -5% patients on heparin develop thrombocytopaenia Of those with thrombocytopaenia, 30% develop venous and/or arterial thrombosis Bleeding uncommon

Treatment of HIT Discontinue all heparin If need to continue anti-coagulation, use danaparoid (orgaran). Avoid platelet transfusions Thrombosis: use danaparoid or thrombin inhibitor

Oral anticoagulants Examples: Coumarins - warfarin, dicumarol Structurally related to vitamin K Inhibits production of active clotting factors Clearance is slow - 36 hrs Delayed onset 8 - 12 hrs Overdose - reversed by vitamin K infusion Can cross placenta - do not use during late pregnancies

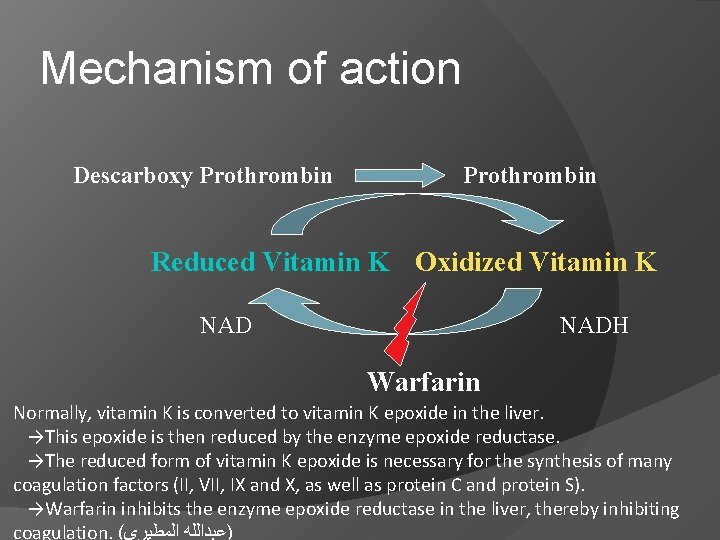
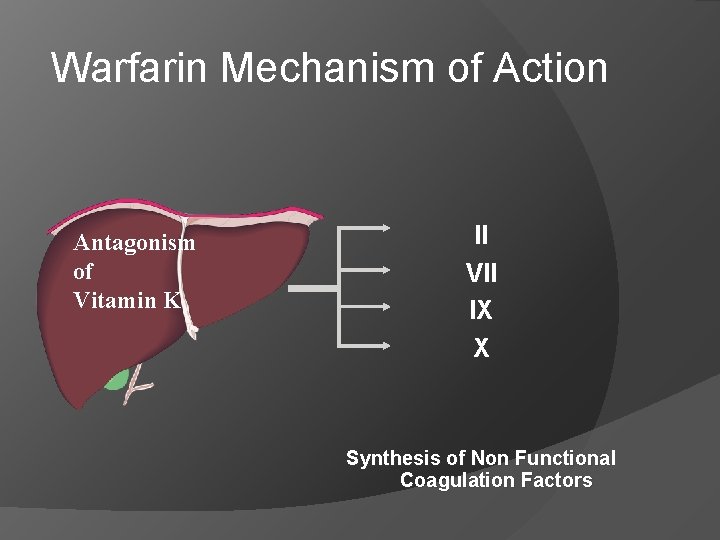
Mechanism of action Descarboxy Prothrombin Reduced Vitamin K Oxidized Vitamin K NADH Warfarin Normally, vitamin K is converted to vitamin K epoxide in the liver. →This epoxide is then reduced by the enzyme epoxide reductase. →The reduced form of vitamin K epoxide is necessary for the synthesis of many coagulation factors (II, VII, IX and X, as well as protein C and protein S). →Warfarin inhibits the enzyme epoxide reductase in the liver, thereby inhibiting coagulation. ( )ﻋﺒﺪﺍﻟﻠﻪ ﺍﻟﻤﻄﻴﺮﻱ

Antiplatelet drugs Example: Aspirin Prevents platelet aggregation /adhesion Clinical use - prevents arterial thrombus Myocardial infarction (MI), stroke, heart valve replacement and shunts Other antiplatelet drugs are - Dipyridamole, sulfinpyrazone and Ticlopidine

Mechanism of action Aspirin inhibits cyclooxygenase (COX) COX is a key enzyme involved in the synthesis of thromboxane 2 (prostaglandins) Inhibits platelet aggregation

Prophylactic use of Aspirin Low dose daily. Prevents ischemic attack (ministroke) and MI 335 mg/day reduced the risk of heart attack in patients over 50 More than 1000 mg/day NO EFFECT Contraindication - DO NOT give to patients with glucose 6 -PO 4 dehydrogenase deficiency

Definition of Anticoagulation Therapeutic interference ("blood-thinning") with the clotting mechanism of the blood to prevent or treat thrombosis and embolism.

Indications of Anticoagulant Therapy Treatment and Prevention of Deep Venous Thrombosis Pulmonary Emboli Prevention of stroke in patients with atrial fibrillation, artificial heart valves, cardiac thrombus. Ischaemic heart disease During procedures such as cardiac catheterisation and apheresis.

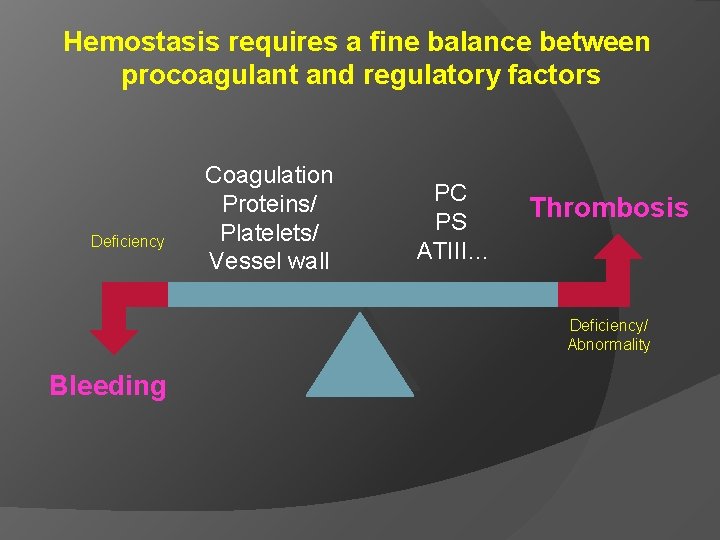
Hemostasis requires a fine balance between procoagulant and regulatory factors Deficiency Coagulation Proteins/ Platelets/ Vessel wall PC PS ATIII… Thrombosis Deficiency/ Abnormality Bleeding

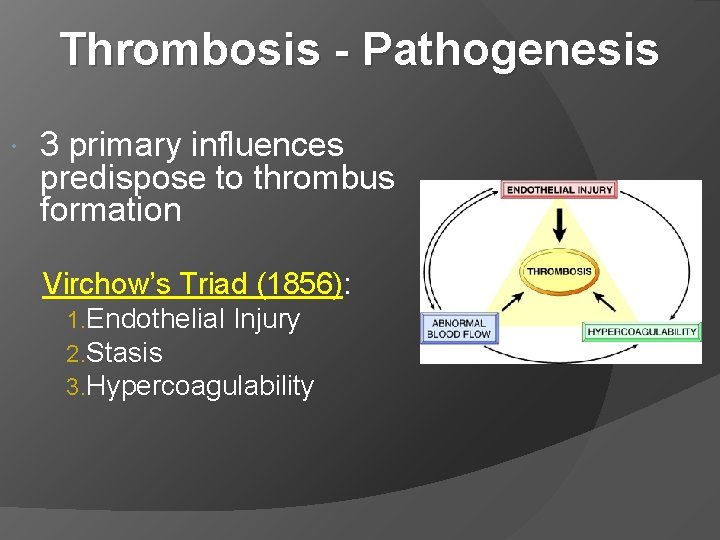
Thrombosis - Pathogenesis 3 primary influences predispose to thrombus formation Virchow’s Triad (1856): 1. Endothelial Injury 2. Stasis 3. Hypercoagulability

Clinical significance of thrombosis 1. Obstruction of arteries and veins Ischemia or necrosis of downstream tissue 2. Embolization

Deep vein thrombosis (DVT) and acute pulmonary embolism (PE) are two manifestations of venous thromboembolism (VTE). VTE contributes to significant morbidity and mortality both in the community and in hospital. The mainstay of therapy for DVT is anticoagulation, provided there is no contraindication. Following initial anticoagulation, patients with DVT are anticoagulated further to prevent future recurrences, embolism, and thrombosis-related death.

Initial anticoagulation is administered in the first 5 to 10 days following a diagnosis of DVT. Long-term anticoagulant therapy is typically administered for a finite time beyond the initial period, usually three to six months, and occasionally up to 12 months. Extended anticoagulation refers to therapy that is administered indefinitely.

Anticoagulation is the mainstay of therapy for patients with deep venous thrombosis (DVT). Anticoagulation is indicated for all patients with proximal deep venous thrombosis (DVT) and select cases of distal DVT. The decision to anticoagulate must weigh the benefits of anticoagulation against the risk of bleeding for an individual.

The primary objective of anticoagulation is the prevention of further thrombosis and of early and late complications. Major early complications of DVT include further clot extension, acute pulmonary embolus (PE), major bleeding, and death. Late complications include recurrent clot, postthrombotic (post phlebitic) syndrome and chronic thromboembolic pulmonary hypertension.

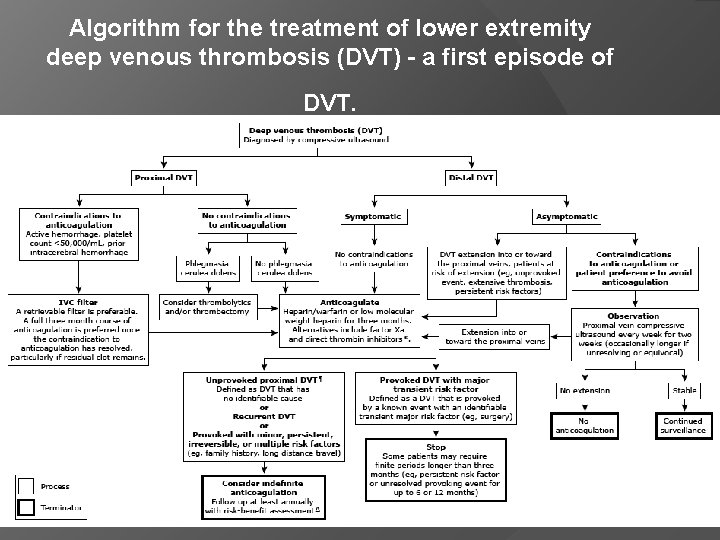
Duration of therapy — A decision regarding the optimal duration of anticoagulation must take into account the presence or absence of provoking events, risk factors for recurrence and bleeding, as well as to the individual patient's preferences and values. Although there is agreement on the minimum length of time a patient with a first episode of DVT should be treated (ie, three months), the optimal length of time is not known. For most patients with a first episode of proximal DVT (provoked and unprovoked, proximal and distal), anticoagulants should be administered for three months rather than for shorter periods (eg, four or six weeks) (algorithm 1).

Algorithm for the treatment of lower extremity deep venous thrombosis (DVT) - a first episode of DVT.

Most experts agree that extending anticoagulation beyond three months is considered in select populations, particularly in patients with provoked DVT with persistent but reversible risk factors (extended finite periods; eg, 6 to 12 months or until risk factor is resolved) and unprovoked DVT (indefinite anticoagulation). In contrast, anticoagulation beyond three months is NOT typically performed in patients with an episode of DVT provoked by a transient risk factor (eg, surgery) or in those at high risk of bleeding.

Pregnancy — Pregnancy is a risk factor for the development of DVT. Adjusted-dose subcutaneous LMW heparin is the preferred agent for initial and long-term anticoagulation in pregnant women with acute DVT. This agent is preferred, because it has a more favorable safety profile, especially when compared with warfarin. Warfarin freely crosses the placental barrier and can produce an embryopathy when given between the sixth and ninth weeks of pregnancy. Intravenous and subcutaneous forms of unfractionated heparin are alternatives to LMW heparin. Fondaparinux and oral factor Xa and direct thrombin inhibitors have not been adequately tested in pregnant women with acute DVT and as such should not be administered.

The optimal duration of anticoagulation in pregnancy is unknown and should be individualized on a case-by-case basis. In general, the total duration of anticoagulant therapy (pregnancy plus the postpartum period) should be at least three to six months for women whose only risk factors for DVT were transient (eg, pregnancy, cesarean section). Anticoagulant therapy generally continues for at least six weeks postpartum. Patients with persistent risk factors for DVT may require a longer duration of therapy.

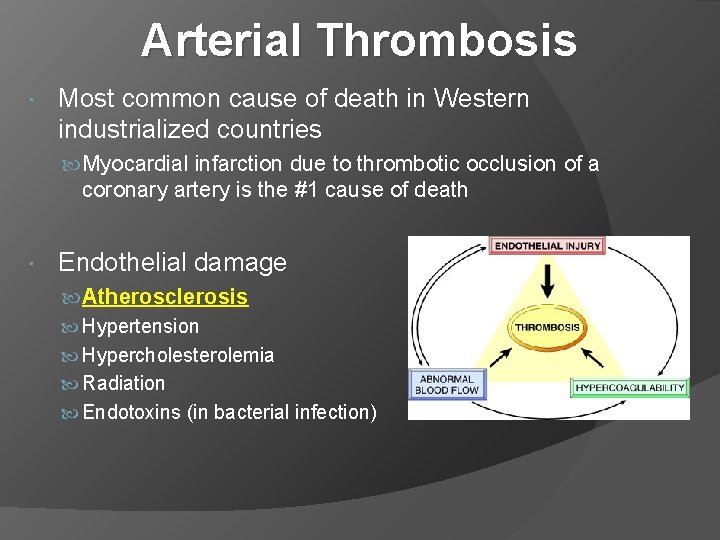
Arterial Thrombosis Most common cause of death in Western industrialized countries Myocardial infarction due to thrombotic occlusion of a coronary artery is the #1 cause of death Endothelial damage Atherosclerosis Hypertension Hypercholesterolemia Radiation Endotoxins (in bacterial infection)

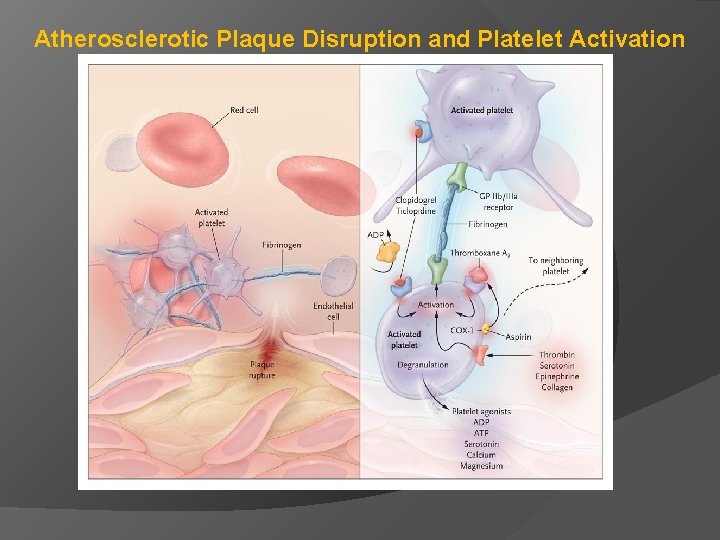
Atherosclerotic Plaque Disruption and Platelet Activation

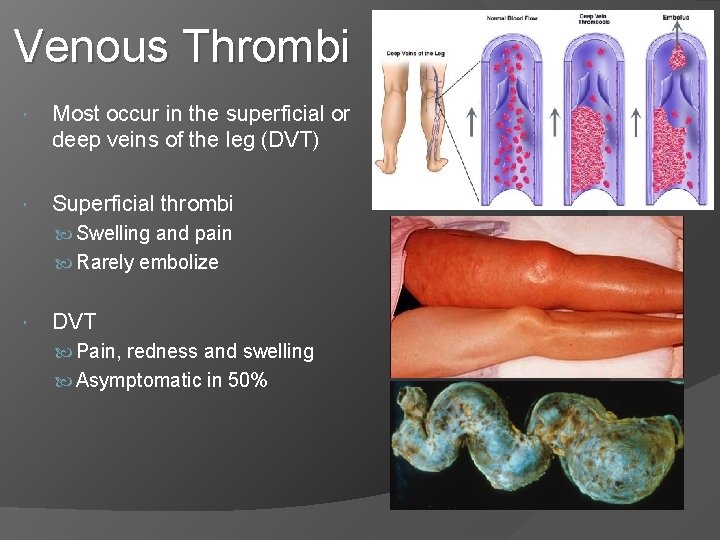
Venous Thrombi Most occur in the superficial or deep veins of the leg (DVT) Superficial thrombi Swelling and pain Rarely embolize DVT Pain, redness and swelling Asymptomatic in 50%

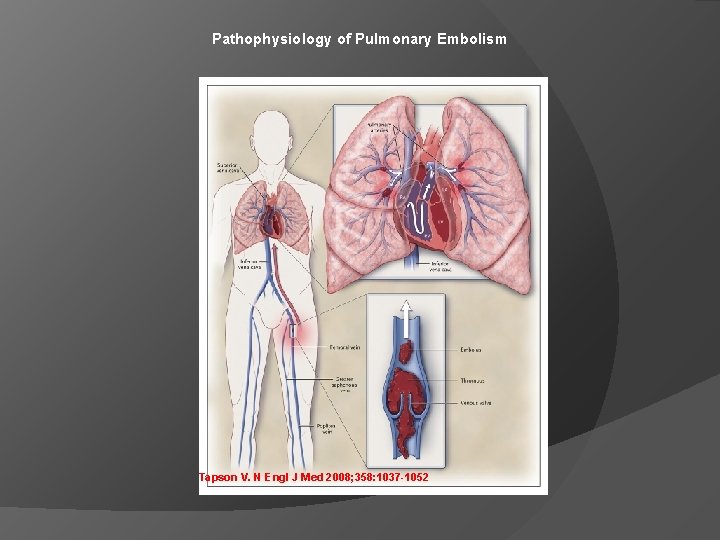
Pathophysiology of Pulmonary Embolism Tapson V. N Engl J Med 2008; 358: 1037 -1052

Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE)

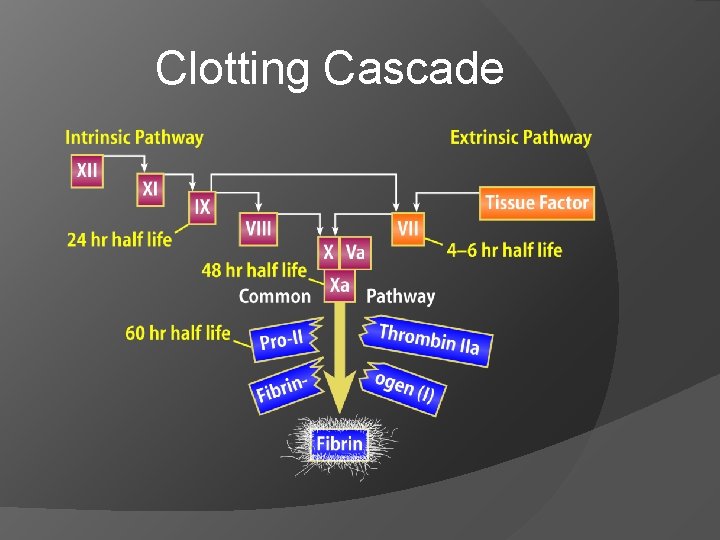
Clotting Cascade

Warfarin Mechanism of Action Antagonism of Vitamin K II VII IX X Synthesis of Non Functional Coagulation Factors

Virchow’s Triad

Antithrombotic Agents: Mechanism of Action Anticoagulants: prevent clot formation and extension Antiplatelet drugs: interfere with platelet activity Thrombolytic agents: dissolve existing thrombi

Warfarin: Indications Prophylaxis and/or treatment of: Venous thrombosis and its extension Pulmonary embolism Thromboembolic complications associated with AF and cardiac valve replacement Post MI, to reduce the risk of death, recurrent MI, and thromboembolic events such as stroke or systemic embolization Prevention and treatment of cardiac embolism

Warfarin: Major Adverse Effect Hemorrhage Factors that may influence bleeding risk: Intensity of anticoagulation Concomitant clinical disorders Concomitant use of other medications Quality of management

High risk categories: Any patient with the following must be considered as a high risk of bleeding when on warfarin and the reversal of warfarin may be considered at a lower INR. • Age >65 • Uncontrolled hypertension • Diabetes • Renal failure • Hepatic failure • Trauma and recent surgery • Anti platelet drugs • Previous major bleeding

Special Considerations in the Elderly—Bleeding Increased age associated with increased sensitivity at usual doses Comorbidity Increased drug interactions ? Increased bleeding risk independent of the above

Prothrombin Time (PT) Historically, a most reliable and “relied upon” clinical test However: Proliferation of thromboplastin reagents with widely varying sensitivities to reduced levels of vitamin K-dependent clotting factors has occurred Concept of correct “intensity” of anticoagulant therapy has changed significantly (low intensity) Problem addressed by use of INR (International Normalized Ratio)

INR: International Normalized Ratio A mathematical “correction” (of the PT ratio) for differences in the sensitivity of thromboplastin reagents Relies upon “reference” thromboplastins with known sensitivity to antithrombotic effects of oral anticoagulants INR is the PT ratio one would have obtained if the “reference” thromboplastin had been used Allows for comparison of results between labs and standardizes reporting of the prothrombin time

INR Equation INR = International Normalized Ratio ISI = International Sensitivity Index

Potential Problems with the INR Limitations Unreliable during induction Loss of accuracy with high ISI thromboplastins Incorrect ISI assignment by manufacturer Incorrect calculation of INR due to failure to use proper mean normal plasma value to derive PT ratio Solutions Use thromboplastin reagents with low ISI values (less than 1. 5) Use thromboplastin reagents with low ISI values and use plasma calibrants with certified INR values Use “mean normal” PT derived from normal plasma samples for every new batch of thromboplastin reagent

Warfarin: Dosing Information Individualize dose according to patient response (as indicated by INR) Use of large loading dose not recommended May increase hemorrhagic complications Does not offer more rapid protection Low initiation doses are recommended for elderly/frail/liverdiseased/malnourished patients

Conversion from Heparin to Warfarin May begin concomitantly with heparin therapy Heparin should be continued for a minimum of four days Time to peak antithrombotic effect of warfarin is delayed 96 hours (despite INR) When INR reaches desired therapeutic range, discontinue heparin (after a minimum of four days)

Warfarin: Dosing and Monitoring Start low Initiate 5 mg daily* Educate patient Stabilize Titrate to appropriate INR Monitor INR frequently (daily then weekly) Adjust as necessary Monitor INR regularly (every 1– 4 weeks) and adjust * Elderly, frail, liver disease, malnourished: 2 mg/day

Relative Contraindications to Warfarin Therapy Pregnancy Situations where the risk of hemorrhage is greater than the potential clinical benefits of therapy Uncontrolled alcohol/drug abuse Unsupervised dementia/psychosis

Signs of Warfarin Overdosage Any unusual bleeding: Blood in stools or urine Excessive menstrual bleeding Bruising Excessive nose bleeds/bleeding gums Persistent oozing from superficial injuries Bleeding from tumor, ulcer, or other lesion

Warfarin - Adverse Effects Bleeding is the main concern, risk depends on: Intensity of therapy Patient’s underlying disorder Concomitant use of aspirin or antiplatelet drugs. Patient’s age - risk > 65 yrs old, hx of stroke, hx of GI bleeding Bleeding with an INR < 3, usually due to some occult cause, GI or renal lesion

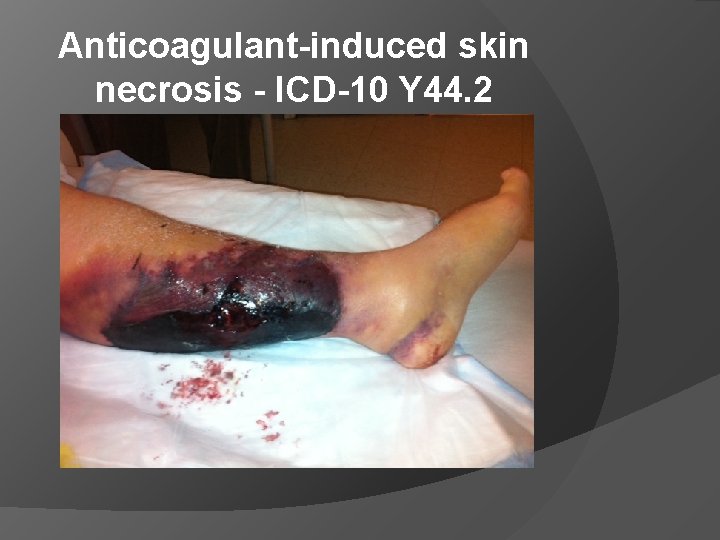
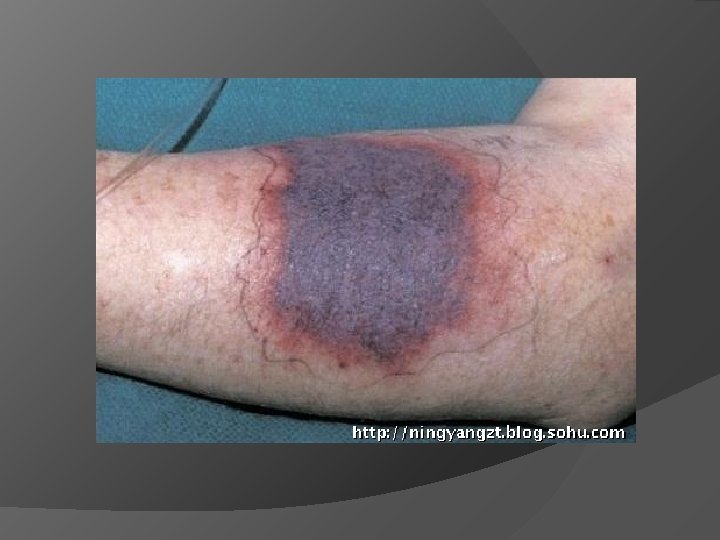
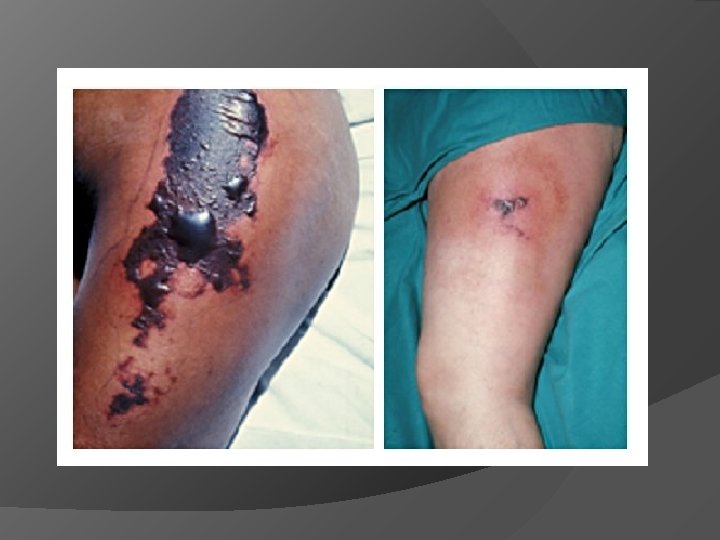
Warfarin - Adverse Effects Most important non-hemorrhagic effect is skin necrosis Occurs on 3 rd to 8 th day of dosing Due to excessive thrombosis of venules and capillaries in subcutaneous fat May be associated with Protein C deficiency - initiation of warfarin therapy can induce a rapid decline in protein C because of its short half life (7 hours) resulting in a parodoxical syndrome of transient hypercoagulation and microthrombus formation beginning before effective anticoagulation is achieved.

Anticoagulant-induced skin necrosis - ICD-10 Y 44. 2



Factors which Influence PT/INR Significant variations in INR results occur for a variety of reasons including drug interaction, diet, and disease state.

Drugs and Herbal Preparation Prior to prescribing any new drug, interaction with warfarin should be considered. This includes over the counter drugs. Warfarin circulates bound to albumin in plasma, and other drugs which bind to albumin can displace warfarin increasing its therapeutic effect. Conversely, removal of drugs which bind to albumin can decrease warfarin’s therapeutic effect. Drugs which induce or are metabolized by the hepatic microsomal cytochrome P 450 system wil also alter the effect of warfarin, as the potent S‐isomer of the drug is metabolized by this enzyme. For patients taking warfarin or other vitamin K antagonists, the formulary should be consulted before starting the patient on a new drug or before changing the dose of any other drug

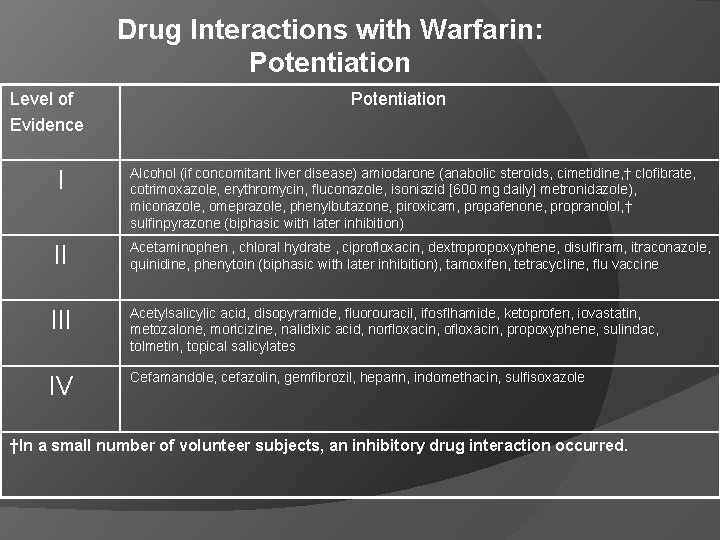
Drug Interactions with Warfarin: Potentiation Level of Evidence Potentiation I Alcohol (if concomitant liver disease) amiodarone (anabolic steroids, cimetidine, † clofibrate, cotrimoxazole, erythromycin, fluconazole, isoniazid [600 mg daily] metronidazole), miconazole, omeprazole, phenylbutazone, piroxicam, propafenone, propranolol, † sulfinpyrazone (biphasic with later inhibition) II Acetaminophen , chloral hydrate , ciprofloxacin, dextropropoxyphene, disulfiram, itraconazole, quinidine, phenytoin (biphasic with later inhibition), tamoxifen, tetracycline, flu vaccine III Acetylsalicylic acid, disopyramide, fluorouracil, ifosflhamide, ketoprofen, iovastatin, metozalone, moricizine, nalidixic acid, norfloxacin, ofloxacin, propoxyphene, sulindac, tolmetin, topical salicylates IV Cefamandole, cefazolin, gemfibrozil, heparin, indomethacin, sulfisoxazole †In a small number of volunteer subjects, an inhibitory drug interaction occurred.

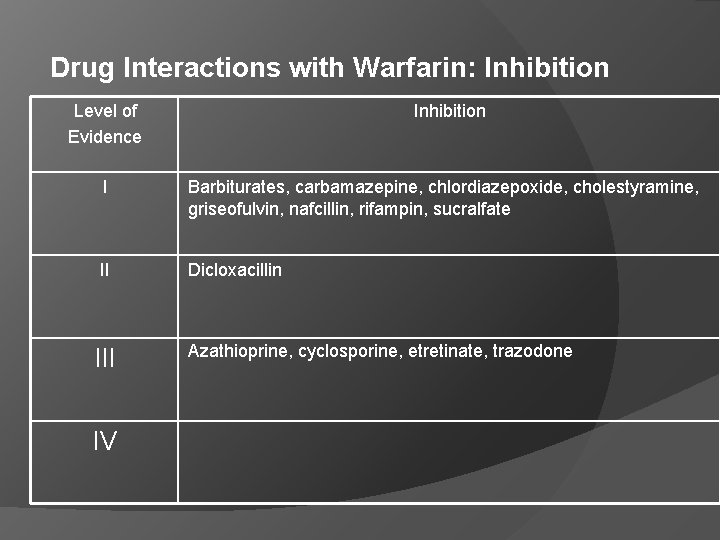
Drug Interactions with Warfarin: Inhibition Level of Evidence Inhibition I Barbiturates, carbamazepine, chlordiazepoxide, cholestyramine, griseofulvin, nafcillin, rifampin, sucralfate II Dicloxacillin III IV Azathioprine, cyclosporine, etretinate, trazodone

Drug Interactions with Warfarin: No Effect Level of Evidence No Effect I Antacids, atenolol, bumetadine, enoxacin, famotidine, fluoxetine, ketorolac metoprolol, naproxen, nizatidine, psyllium, ranitidine‡ II Ibuprofen, ketoconazole III IV Diltiazem, tobacco, vancomycin

Diet Since warfarin functions as a vitamin K antagonist, its clinical effect varies with the vitamin K content of the diet. Dietary vitamin K is largely derived from plant phyloquinones, and fluctuations in intake of green vegetables can alter the INR. In general, leafy green vegetables and oils contain high amounts of vitamin K - broccoli, brussels sprouts, cabbage, collard greens, endive, green scallion, kale, lettuce, mustard greens, spinach, turnip greens, watercress, large quantities of mayonnaise, canola, salad, and soybean oils - liver

Physicians should educate their patients about the impact of drugs, herbal preparation and diet on therapeutic effect of warfarin, and to recognize the signs and symptoms of excessive anticoagulation.

Alcohol and warfarin Binge drinking – decreases the metabolism of warfarin, increases INR and increases risk of bleeding Chronic drinking (3 or more drinks daily) – increases metabolism of warfarin, decreases risk of clotting Alcohol also increases risk of stomach bleeding

Smoking and Warfarin Smoking causes the liver to break warfarin down more quickly - it’s the smoke, not the nicotine! People that are smoking often require higher dose of warfarin

Patient - What if I miss a dose? Take it as soon as possible. If it is the next day, skip the missed dose and carry on. Do not double doses. Record the date of your missed dose (on warfarin record sheet) and be sure to tell your doctor before next INR reading.

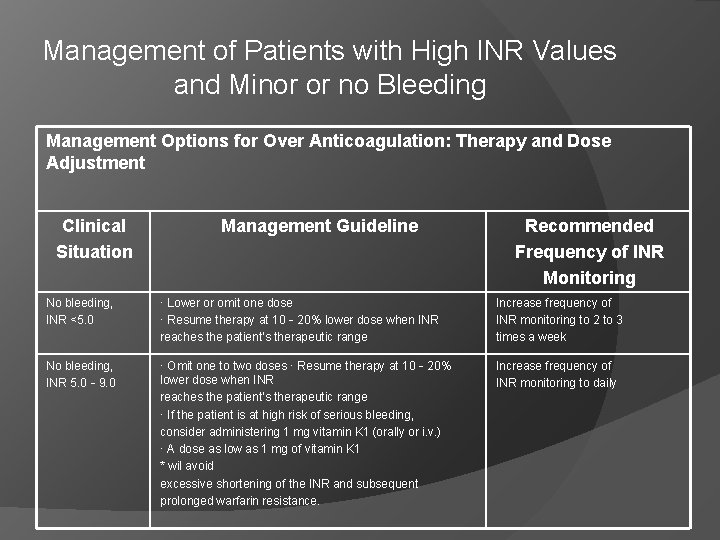
Management of Patients with High INR Values and Minor or no Bleeding Management Options for Over Anticoagulation: Therapy and Dose Adjustment Clinical Situation Management Guideline Recommended Frequency of INR Monitoring No bleeding, INR <5. 0 · Lower or omit one dose · Resume therapy at 10‐ 20% lower dose when INR reaches the patient’s therapeutic range Increase frequency of INR monitoring to 2 to 3 times a week No bleeding, INR 5. 0‐ 9. 0 · Omit one to two doses · Resume therapy at 10‐ 20% lower dose when INR reaches the patient’s therapeutic range · If the patient is at high risk of serious bleeding, consider administering 1 mg vitamin K 1 (orally or i. v. ) · A dose as low as 1 mg of vitamin K 1 * wil avoid excessive shortening of the INR and subsequent prolonged warfarin resistance. Increase frequency of INR monitoring to daily

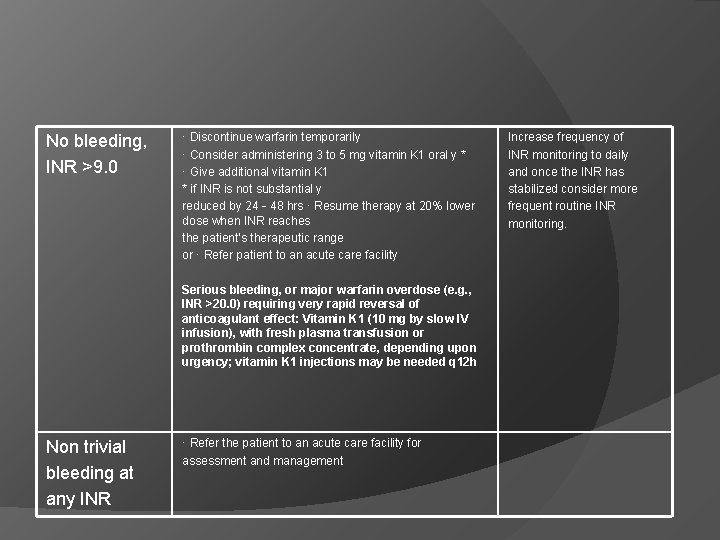
No bleeding, INR >9. 0 · Discontinue warfarin temporarily · Consider administering 3 to 5 mg vitamin K 1 oral y * · Give additional vitamin K 1 * if INR is not substantial y reduced by 24‐ 48 hrs · Resume therapy at 20% lower dose when INR reaches the patient’s therapeutic range or · Refer patient to an acute care facility Serious bleeding, or major warfarin overdose (e. g. , INR >20. 0) requiring very rapid reversal of anticoagulant effect: Vitamin K 1 (10 mg by slow IV infusion), with fresh plasma transfusion or prothrombin complex concentrate, depending upon urgency; vitamin K 1 injections may be needed q 12 h Non trivial bleeding at any INR · Refer the patient to an acute care facility for assessment and management Increase frequency of INR monitoring to daily and once the INR has stabilized consider more frequent routine INR monitoring.

Life-threatening bleeding or serious warfarin overdose Continuing warfarin therapy indicated after high doses of vitamin K 1 Prothrombin complex concentrate, with vitamin K 1 (10 mg by slow IV infusion); repeat if necessary, depending upon the INR Heparin, until the effects of vitamin K 1 have been reversed, and patient is responsive to warfarin

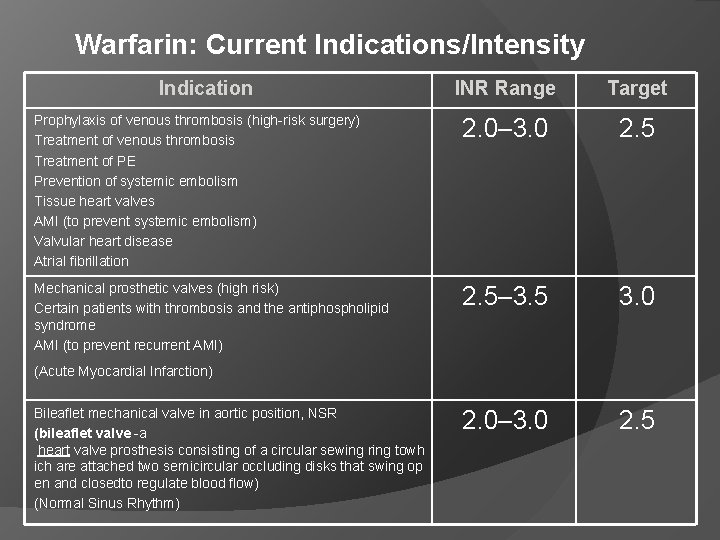
Warfarin: Current Indications/Intensity Indication INR Range Target Prophylaxis of venous thrombosis (high-risk surgery) Treatment of venous thrombosis Treatment of PE Prevention of systemic embolism Tissue heart valves AMI (to prevent systemic embolism) Valvular heart disease Atrial fibrillation 2. 0– 3. 0 2. 5 Mechanical prosthetic valves (high risk) Certain patients with thrombosis and the antiphospholipid syndrome AMI (to prevent recurrent AMI) 2. 5– 3. 5 3. 0 2. 0– 3. 0 2. 5 (Acute Myocardial Infarction) Bileaflet mechanical valve in aortic position, NSR (bileaflet valve -a heart valve prosthesis consisting of a circular sewing ring towh ich are attached two semicircular occluding disks that swing op en and closedto regulate blood flow) (Normal Sinus Rhythm)

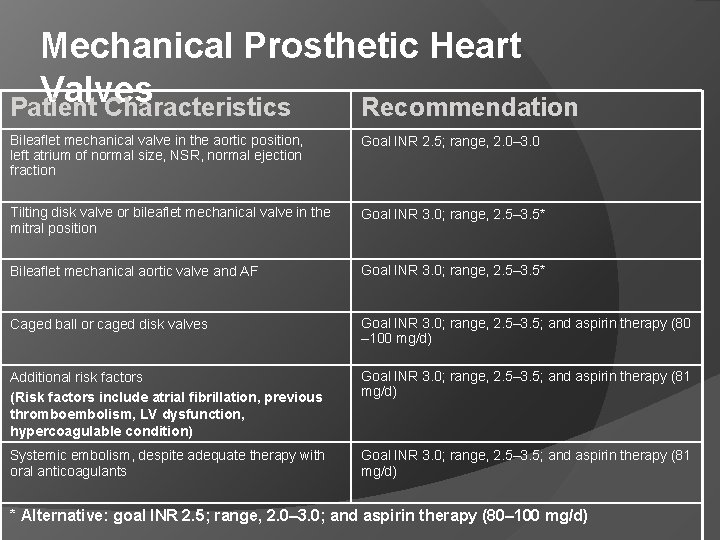
Mechanical Prosthetic Heart Valves Patient Characteristics Recommendation Bileaflet mechanical valve in the aortic position, left atrium of normal size, NSR, normal ejection fraction Goal INR 2. 5; range, 2. 0– 3. 0 Tilting disk valve or bileaflet mechanical valve in the mitral position Goal INR 3. 0; range, 2. 5– 3. 5* Bileaflet mechanical aortic valve and AF Goal INR 3. 0; range, 2. 5– 3. 5* Caged ball or caged disk valves Goal INR 3. 0; range, 2. 5– 3. 5; and aspirin therapy (80 – 100 mg/d) Additional risk factors (Risk factors include atrial fibrillation, previous thromboembolism, LV dysfunction, hypercoagulable condition) Goal INR 3. 0; range, 2. 5– 3. 5; and aspirin therapy (81 mg/d) Systemic embolism, despite adequate therapy with oral anticoagulants Goal INR 3. 0; range, 2. 5– 3. 5; and aspirin therapy (81 mg/d) * Alternative: goal INR 2. 5; range, 2. 0– 3. 0; and aspirin therapy (80– 100 mg/d)

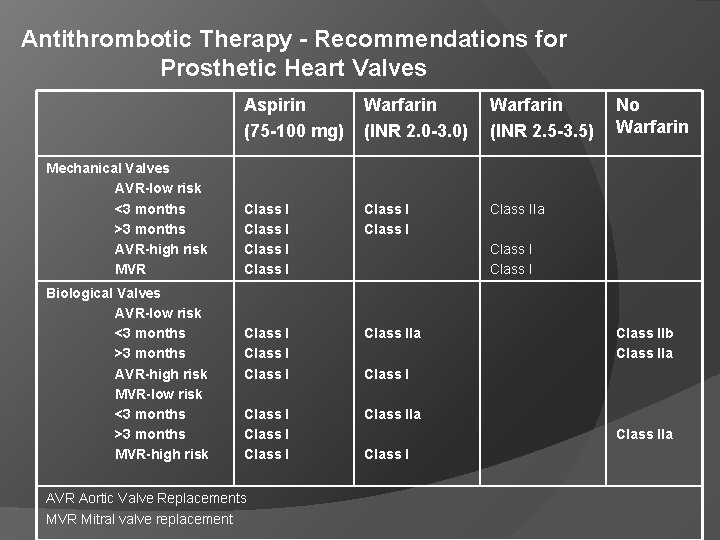
Antithrombotic Therapy - Recommendations for Prosthetic Heart Valves Mechanical Valves AVR-low risk <3 months >3 months AVR-high risk MVR Biological Valves AVR-low risk <3 months >3 months AVR-high risk MVR-low risk <3 months >3 months MVR-high risk Aspirin (75 -100 mg) Warfarin (INR 2. 0 -3. 0) Warfarin (INR 2. 5 -3. 5) Class I Class I Class I Class IIa AVR Aortic Valve Replacements MVR Mitral valve replacement No Warfarin Class IIb Class IIa Class I

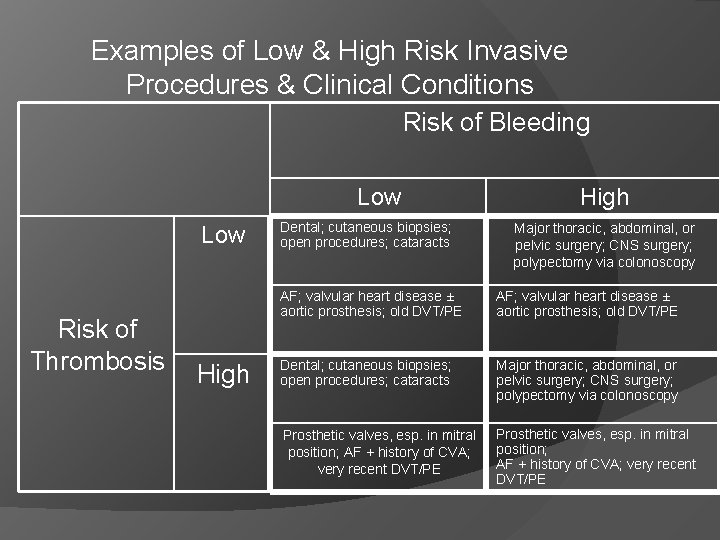
Examples of Low & High Risk Invasive Procedures & Clinical Conditions Risk of Bleeding Low Risk of Thrombosis High Dental; cutaneous biopsies; open procedures; cataracts High Major thoracic, abdominal, or pelvic surgery; CNS surgery; polypectomy via colonoscopy AF; valvular heart disease ± aortic prosthesis; old DVT/PE Dental; cutaneous biopsies; open procedures; cataracts Major thoracic, abdominal, or pelvic surgery; CNS surgery; polypectomy via colonoscopy Prosthetic valves, esp. in mitral position; AF + history of CVA; very recent DVT/PE

Warfarin in pregnancy Crosses the placenta Produces characteristic embryopathy, CNS abnormalities, fetal bleeding • Embryopathy consists of: nasal hypoplasia stippled epiphyses agenesis of corpus callosum ventral midline dysplasia - optic atrophy

Effective Patient Education Teach basic concepts of safe, effective anticoagulation Discuss importance of regular INR monitoring Counsel on use of other medications, alcohol Develop creative strategies for improving compliance

New Anticoagulation Drugs Direct Thrombin Inhibitors Ximelagatran, hirudin, bivalirudin (Angiox), and argatroban (not available in Poland) Synthetic pentasaccharide Acivated Protein C Tissue Factor Pathway Inhibitor (TFPI)

Why do we need new anticoagulation drugs? Heparin-induced thrombocytopenia Heparin prophylaxis is imperfect Heparin-associated osteoporosis Warfarin takes several days for its effect Warfarin is not as effective in some situations e. g antiphospholipid syndrome Warfarin interacts with many other drugs Warfarin is dangerous if not monitored

Synthetic Pentasaccharide ? ? ? E. g Fonaparinux Synthetic, single molecular entity Targets Factor Xa Does not cause thrombocytopenia Shown promise in DVT prevention during orthopedic procedures. Also being examined in ischaemic heart disease

Ximelagatran ? ? ? Promising oral direct thrombin inhibitor Converted to the active form melagatran in vivo No dosing problems No monitoring needed. Recent atrial fibrillation study showed it to possibly be superior to warfarin.

New oral anticoagulants in Poland Dabigatran - Pradaxa 110 mg, 150 mg >300 zł/monthly Apixaban – Eliquis 2, 5 mg - >400 zł/monthly Rivaroxaban – Xarelto 10 mg, 15 mg, 20 mg - >400 zł/monthly But Warfarin - <20 zł/monthly

Pregnancy Direct thrombin inhibitors and direct factor Xa inhibitors are not used during pregnancy, due to lack of clinical experience in this setting; LMW heparin is preferred in most pregnant women who require an anticoagulant. If a patient taking a one of these agents becomes pregnant, she should be switched to LMW heparin immediately.

The use of any anticoagulant is associated with an increased risk of bleeding, and bleeding complications can be life-threatening. Bleeding is especially concerning with the target-specific oral anticoagulants (TSOACs) because antidotes or specific reversal agents for TSOACs are lacking. Additionally, routine coagulation tests cannot be used to determine the degree of anticoagulation, making it more challenging to determine when the anticoagulant effect has resolved.

Perioperative management of patients receiving anticoagulants The management of anticoagulation in patients undergoing surgical procedures is challenging because interrupting anticoagulation for a procedure transiently increases the risk of thromboembolism. At the same time, surgery and invasive procedures have associated bleeding risks that are increased by the anticoagulant(s) administered for thromboembolism prevention. If the patient bleeds from the procedure, their anticoagulant may need to be discontinued for a longer period, resulting in a longer period of increased thromboembolic risk. A balance between reducing the risk of thromboembolism and preventing excessive bleeding must be reached for each patient.

For patients taking a vitamin K antagonist (eg, warfarin), it takes several days until the anticoagulant effect is reduced and then reestablished perioperatively; the risks and benefits of "bridging" with a shorter acting agent, such as heparin, during this time are unclear. The newer target-specific oral anticoagulants (eg, direct thrombin inhibitor dabigatran, factor Xa inhibitors rivaroxaban, apixaban, edoxaban) have shorter halflives, making them easier to discontinue and resume rapidly, but they lack a specific antidote or reversal strategy, which raises concerns about treatment of bleeding and management of patients who require an urgent procedure.

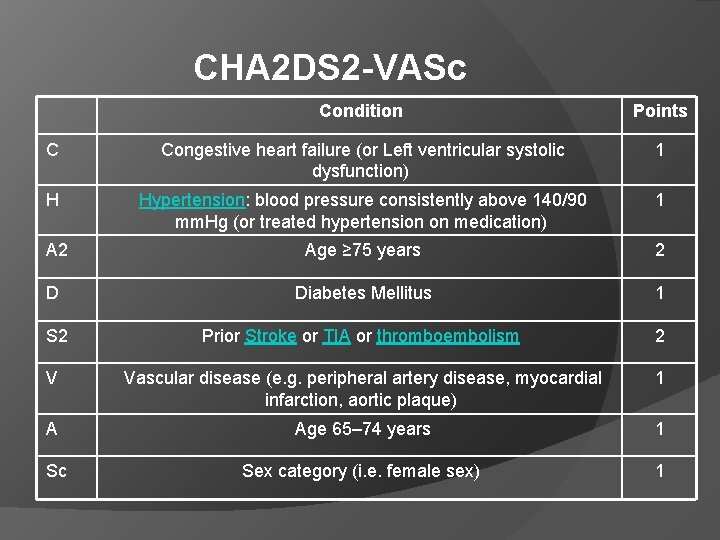
CHA 2 DS 2 -VASc Score for Atrial Fibrillation Stroke Risk CHA 2 DS 2 -VASc score (Birmingham 2009) was developed after identifying additional stroke risk factors in patients with atrial fibrillation. Warfarin anticoagulation titrated to an INR of 2. 0 -3. 0 is recommended for the average patient with a CHA 2 DS 2 VASc score ≥ 2 unless contraindicated (e. g. , history of frequent falls, clinically significant bleeding, inability to obtain regular INR). Either Warfarin or Aspirin can be used for the average patient with a CHA 2 DS 2 -VASc score of 1 depending on physician discretion and patient preference. Aspirin 325 mg daily is recommended for the average patient with a CHA 2 DS 2 -VASc score of 0.

CHA 2 DS 2 -VASc Condition Points C Congestive heart failure (or Left ventricular systolic dysfunction) 1 H Hypertension: blood pressure consistently above 140/90 mm. Hg (or treated hypertension on medication) 1 A 2 Age ≥ 75 years 2 D Diabetes Mellitus 1 S 2 Prior Stroke or TIA or thromboembolism 2 V Vascular disease (e. g. peripheral artery disease, myocardial infarction, aortic plaque) 1 A Age 65– 74 years 1 Sc Sex category (i. e. female sex) 1

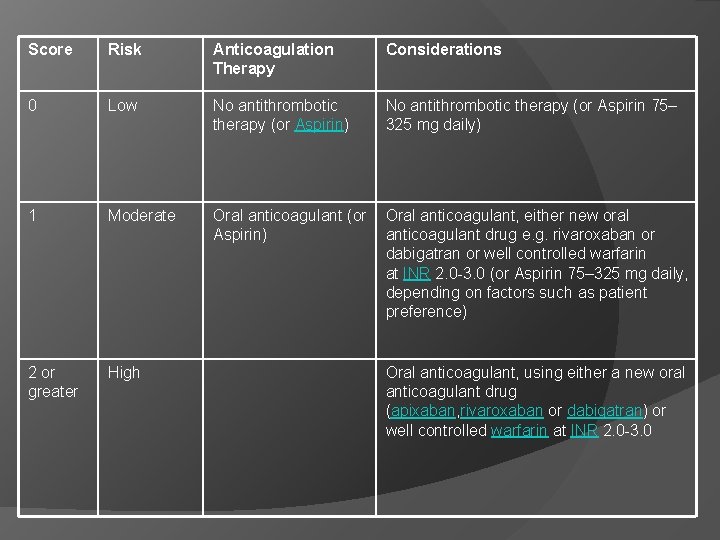
Score Risk Anticoagulation Therapy Considerations 0 Low No antithrombotic therapy (or Aspirin) No antithrombotic therapy (or Aspirin 75– 325 mg daily) 1 Moderate Oral anticoagulant (or Aspirin) Oral anticoagulant, either new oral anticoagulant drug e. g. rivaroxaban or dabigatran or well controlled warfarin at INR 2. 0 -3. 0 (or Aspirin 75– 325 mg daily, depending on factors such as patient preference) 2 or greater High Oral anticoagulant, using either a new oral anticoagulant drug (apixaban, rivaroxaban or dabigatran) or well controlled warfarin at INR 2. 0 -3. 0

Today’s Topics Diagnoses for which anticoagulation is necessary Duration of therapy INR goal Starting warfarin Sources of evidenced based medicine Drug/Drug interactions System wide protocol Work up of PE/DVT

Diagnoses requiring warfarin Atrial fibrillation - sometimes Valvular Heart Disease Prosthetic heart valves DVT PE Hypercoagulable States - sometimes THR, TKA, hip fracture repair Pulmonary Hypertension

Case 1 46 y. o. male continuity patient with allergic rhinitis, found on exam to have irregular pulse. No other medical problems. Pulse irreg. 76 bpm, BP 132/76 EKG shows a-fib

Question 1 Does the patient need anticoagulation?

Answer No Provide proof for your answer

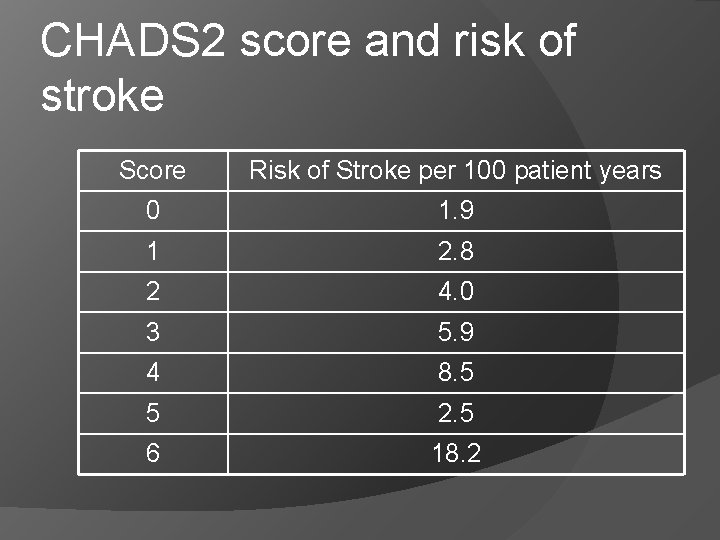
Atrial Fibrillation CHADS 2 score is an easy to use clinical tool for determining who needs warfarin C – CHF- 1 point H – treated HTN - 1 point A – age >75 – 1 point D – diabetes – 1 point S – prior history of stroke or TIA-2 points

CHADS 2 score and risk of stroke Score Risk of Stroke per 100 patient years 0 1. 9 1 2. 8 2 4. 0 3 5. 9 4 8. 5 5 2. 5 6 18. 2

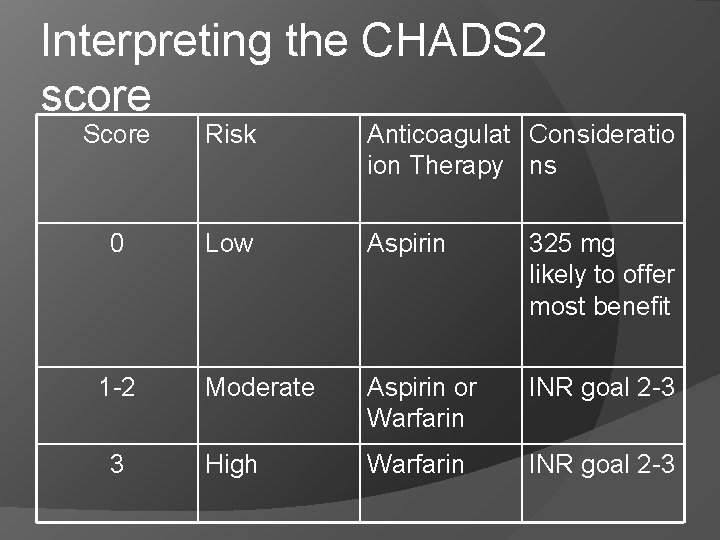
Interpreting the CHADS 2 score Score Risk Anticoagulat Consideratio ion Therapy ns 0 Low Aspirin 325 mg likely to offer most benefit Moderate Aspirin or Warfarin INR goal 2 -3 High Warfarin INR goal 2 -3 1 -2 3

Exception to CHADS 2 Although a patient with a prior stroke and no other risk factors would only have a score of 2 and calculates out as a moderate risk, they are truly high risk and should be treated with warfarin in the absence of contraindications.

Case 2 54 y. o. man with HTN well controlled on HCTZ and metoprolol, found to have irregular pulse EKG shows a-fib Echo one year ago EF 60%

Question 2 Does this patient need warfarin?

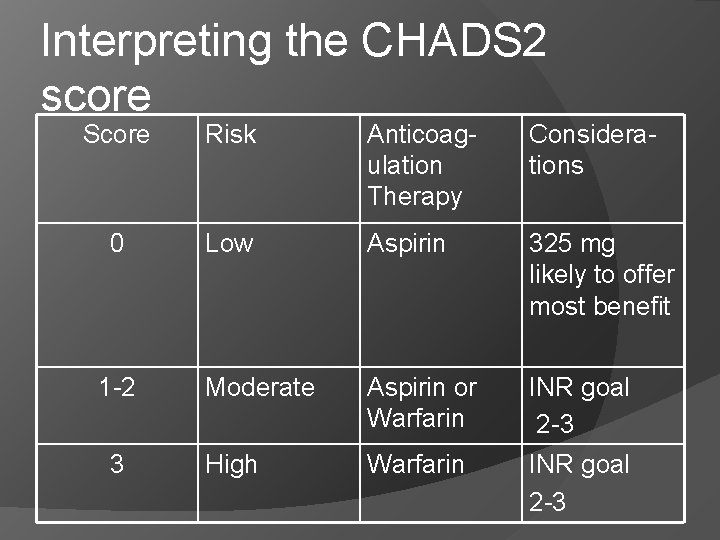
Interpreting the CHADS 2 score Score Risk Anticoagulation Therapy Considerations 0 Low Aspirin 325 mg likely to offer most benefit Moderate Aspirin or Warfarin INR goal 2 -3 High Warfarin INR goal 2 -3 1 -2 3

Valid contraindications to warfarin Patient refusal Non-compliance with INR monitoring Alcohol consumption Bleeding diathesis History of major bleeding

Question 3 56 y. o. woman with MVP admitted 4 mos ago for TIA Does she need warfarin?

Answer Only if she is an ASA failure MVP with h/o stroke or TIA –ASA dose of 50 -160 mg daily If fails ASA – then warfarin

Valvular Disease MVP with h/o stroke or embolization – ASA 50160 mg MVP with ASA failure – warfarin – long-term range 2 -3 Rheumatic heart disease – mitral valve – with a-fib and/or prior history of stroke – lifetime use of warfarin with a goal of 2 -3 Rheumatic Mitral Valve disease and NSR with Left Atrial size >5. 5 cm – lifetime warfarin goal 2 -3

Question 4 60 y. o. man with prosthetic aortic valve, echo shows nl EF. He has never had a stroke or TIA. He has a bi-leaflet valve. What is his INR goal?

Prosthetic Heart Valves Goals Aortic position – NSR, NL LA size, bi-leaflet or tilting disc prosthesis - INR 2. 0 -3. 0 Aortic position – other risk factors* INR 2. 5 -3. 5 Mitral position – 2. 5 -3. 5 Duration – lifetime if mechanical, 12 weeks post surgery if bio-prosthetic (porcine)

AVR + Other Risk Factors = INR 2. 5 -3. 5 Atrial Fibrillation Myocardial infarction Left atrial enlargement > 5. 5 cm Endocardial damage Low ejection fraction Caged ball or caged disc valve

Question 5 Patient with AVR tells you his brother just had an MI at 49 y. o. He picked up a new habit, smoking, since you last saw him. Would you start ASA for primary prevention of CV disease?

Answer Yes

Aspirin Plus Warfarin? When? Only proven benefit is in patients with Prosthetic Valves and increased CV risk or previous MI WARIS II ASPECT 2 Dose should be 81 mg

Next Case 28 y. o. woman presents to the ER on one of your call days with a unilateral swollen leg Doppler reveal a DVT History reveals she just had breast reduction surgery 2 weeks ago

Question 6 What is her INR goal? How long would you treat her?

Deep Vein Thrombosis INR goal is 2. 0 -3. 0 Duration depends on clinical scenario

Classifying Patients First-episode DVT secondary to a transient risk factor First-episode DVT and concurrent cancer First-episode idiopathic DVT First-episode DVT associated with a prothrombotic genotype Recurrent DVT CHEST 2003

st 1 DVT, Transient Risk Factor Treat to INR 2 -3 for 3 months Transient Risk factors include Surgery Pregnancy Hospitalization Trauma Fracture

Next Case 67 y. o. male continuity patient seeing you after hospital discharge, comes to clinic for follow up. He was admitted for a UE DVT. During admission he was found to have widely metastatic liver cancer. What is your anticoagulant of choice? How long do you treat him?

DVT in the setting of Cancer LMWH is recommended the in CHEST guidelines for the first 3 -6 months of long term therapy LMWH is recommended for advanced and metastatic cancers LMWH is recommended during chemotherapy In select patients with localized disease, warfarin can be considered

Next Case 37 y. o. man in your clinic comes in acutely complaining of leg pain and swelling. He denies, travel, recent surgery, hospitalization, prolonged immobilization. You are able to obtain dopplers. He has a DVT

Question 7 What is his INR goal? How long do you treat him?

First Idiopathic VTE At least 6 months (6 -12 months) PREVENT trial – after 3 months of anticoagulation, 508 patients randomized to continuation of warfarin (INR 1. 5 -2. 0) vs. placebo. Trial stopped after 4. 3 years when there was a significantly lower rate of recurrent VTE in the warfarin group (2. 6 versus 7. 2 per 100 patient-years, hazard ratio [HR] 0. 36, 95% CI 0. 19 -0. 67) ELATE – after 3 months of INR 2. 0 -3. 0, 738 patients randomized low dose warfarin INR 1. 5 -1. 9 vs. 2. 03. 0. f/u 2. 4 yrs. Recurrent VTE was significantly lower in the higher dose warfarin group (1. 9 versus 0. 7 per 100 patient-years, HR 2. 8, 95% CI 1. 1 -7. 0).

After six months Risks and benefits need to be reviewed with the patient Risk of minor bleeding with continued anticoagulation 12. 8 per 100 pt years, major bleeding is 2. 7 per 100 patient-years, with a case fatality rate of 9. 1 percent (95% CI 2. 5 -22) Ann Intern Med 2003 Dec 2; 139(11): 893 -900. Risk of recurrent VTE on no warfarin 7. 2 -8. 4 per 100 pt years in PREVENT and THRIVE III trials, low dose warfarin 1. 9 -2. 6 per 100 pt years (ELATE and PREVENT), and. 7 episodes per 100 pt years on full dose warfarin (ELATE)

Case Continued His 6 months of warfarin therapy are over You discuss the risks and benefits of treating him for a year vs. stopping now He opts to stop the warfarin Should you test him for acquired and hereditary thrombophilias? Are there any other tests to determine his individual risk?

Screening for Thrombophilias Controversial – there is no consensus Arguments against screening – excessive, not cost effective, does not impact treatment Arguments for screening – some patients (1 -2%) have very high risk profiles, knowledge could help manage risky situations such as surgery and pregnancy Helps in screening of family members

Inherited Thrombophilias Require life long anticoagulation only in the following cases: Two or more spontaneous thromboses or one spontaneous thrombosis in the case of antithrombin deficiency or the antiphospholipid syndrome One spontaneous life-threatening thrombosis (e. g. , nearfatal pulmonary embolism; cerebral, mesenteric, or portal vein thrombosis) One spontaneous thrombosis at an unusual site (e. g. , mesenteric or cerebral vein) One spontaneous thrombosis in the presence of more than a single genetic defect predisposing to a thromboembolic event Up. To. Date

Consider screening In Strongly Thrombophilic patients – First idiopathic VTE prior to 50 y. o. History of recurrent thrombotic episodes First-degree relative with thrombotic episode prior to the age of 50

When not to screen Recent major surgery, trauma, or immobilization Active malignancy Systemic lupus erythematosus Inflammatory bowel disease Myeloproliferative disorders Heparin-induced thrombocytopenia with thrombosis Preeclampsia at term Retinal vein thrombosis

Individual Risk Assessment D-dimer testing – 4 studies have shown an increased risk of recurrent VTE in patients with elevated D-dimers after 3 months of anticoagulation HR 2 -2. 5 One of the studies showed only 5 patients out of 186 with a normal D-dimer with a recurrent VTE, this give a negative predictive value of >96%. Thromb Haemost 2002 Jan; 87(1): 7 -12.

Recurrent VTE Trials are ongoing to determine the optimal duration of treatment, but for now recommendations say “indefinite” unless there is a reversible cause If reversible cause – then treat until the risk factor is no longer an issue

Upper Extremity Thrombosis General consensus is that this represents a more thrombogenic patient No randomized controlled trials to determine the most appropriate length of therapy If a reversible cause – can treat for 3 -6 months If not – long term anticoagulation

Next Case You are called to the ER to see one of your clinic patients. She is 42 y. o. c/o SOB for 1 day, she is breathing rapidly and is tachycardic, her O 2 sats are 88%. CXR is negative. WBCs are normal. She is not hypotensive. You order a PE protocol CT. It is positive. How long will this patient need to be treated for her PE?

Treatment for PE Treatment goals are the same as DVT Duration the same as DVT Exception is “massive PE” which is defined as “shock” or requiring pressors – this would constitute a reason for lifelong anticoagulation

Other Considerations Compression Stockings should be prescribed at 30 -40 mm Hg at the ankle in all patients with DVT within a month after Dx and continued for 1 -2 years. This has been proven to reduce the incidence of post-thrombotic syndrome by 50% Lancet 1997; 349, 759 -762 Patients should be on “ambulation as tolerated” NSAIDs are not recommended during the acute treatment of DVT

Total Hip Replacement Low Molecular Weight Heparin (LMWH) or Warfarin with a target INR of 2. 0 -3. 0 or Fondaparinux 2. 5 mg daily Duration: 28 -35 days

Hip Fracture Surgery Same recommendations as Total Hip Replacement

Total Knee Arthroplasty (TKA) LMWH at high risk doses or Warfarin with INR goal 2. 0 -3. 0 or Fondaparinux Duration: 10 days