Hemostasis Objectives 1 What is Hemostasis 2 Steps
Hemostasis

Objectives 1. What is Hemostasis? 2. Steps involved under Hemostasis 3. Mechnism of Hemostasis 4. Anticoagulants and their mechanism of action 5. tests and bleeding disorders

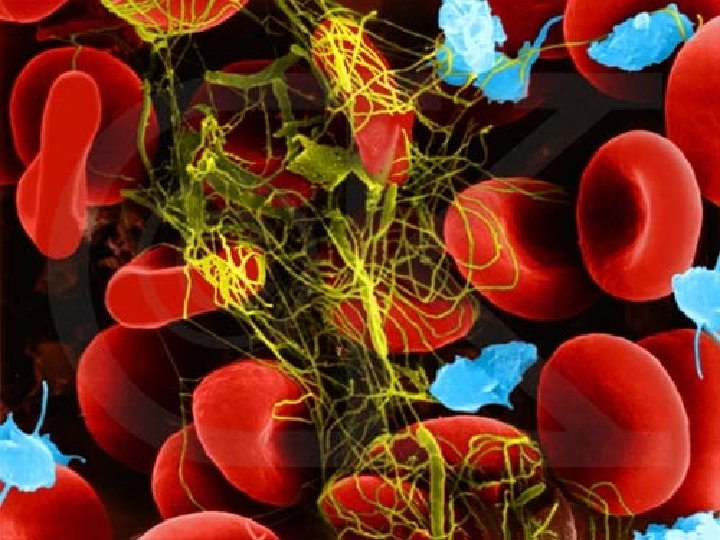
What is Hemostasis? • It is spontaneous arrest of bleeding by physiological process in small vessels • Means prevention of blood loss • Definition: Hemostasis is a process of forming clots in the walls of damaged blood vessels & preventing blood loss, while maintaining blood in a fluid state within the vascular system

Steps of haemostasis 1. Vasoconstriction 2. Temporary plug formation 3. Permanent plug formation (definite) a) formation of prothrombin activator b) convertion of prothrombin to thrombin c) conversion of fibrinogen to fibrin d) conversion of soluble fibrin monomer to insoluble fibrin polymer 4. Clot retraction 5. Clot lysis 6. Permanent repair of the damaged vessel wall

Steps involved in hemostasis : 1) Vasoconstriction 2) Formation of the platelet plug 3) Blood Coagulation /clot formation 4) Fibrous organization or dissolution of the blood clot
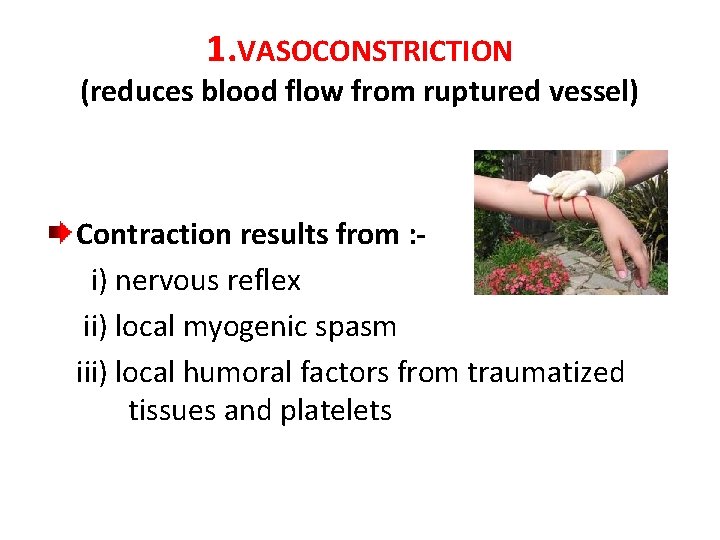
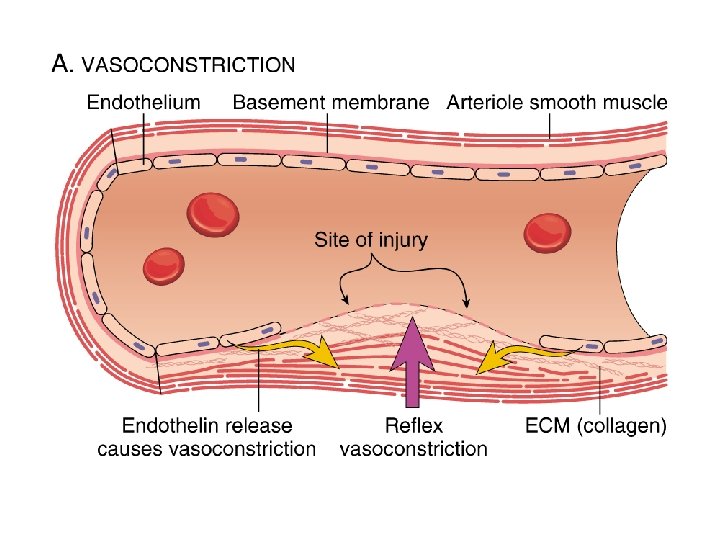
1. VASOCONSTRICTION (reduces blood flow from ruptured vessel) Contraction results from : i) nervous reflex ii) local myogenic spasm iii) local humoral factors from traumatized tissues and platelets

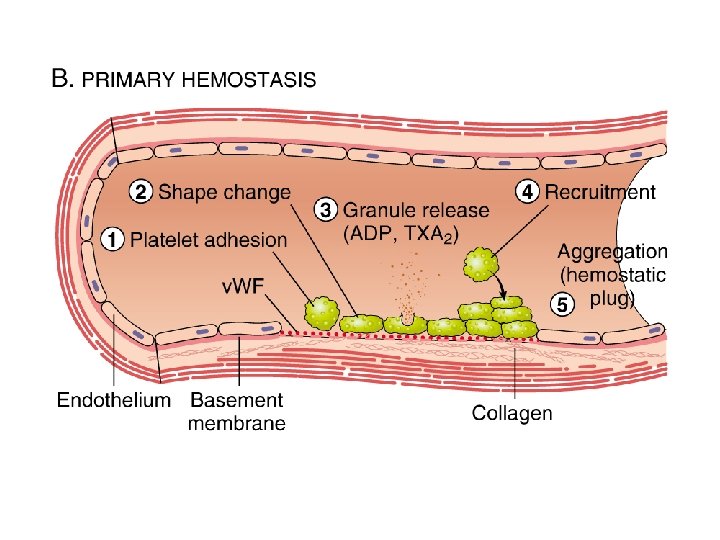
II. FORMATION OF PLATELET PLUG If the rent in the blood vessel is very small it is often sealed by a platelet plug, rather than a clot Physical and chemical characteristics of platelets § Actin, myosin, thrombosthenin § Storage of calcium ions § ADP § PGs § Fibrin-stabilizing factor § Growth factor

The surface coat of glycoproteins repulses the adherence to normal endothelium and yet causes adherence to injured areas, even more to exposed collagen. Membrane contains large amounts of Phospholipids that play several activating roles in clotting process

MECHANISM OF PLATELET PLUG Platelets come in contact with a damaged vascular surface Change their characteristics – § Swell up § Assume irregular forms with numerous radiating psudopods § Contractile proteins contract-cause the release of granules Become sticky and adhere to collagen and to von Willibrand factor Secretion of ADP and thromboxane A 2

ADP and thromboxane A 2 activate more and more platelets – forming a loose platelet plug Importance: of plug formation: Loose platelet plug is successful in blocking the blood loss in minute ruptures in very small blood vessels

Clotting factors FACTORS NAMES I fibrinogen II prothrombin III thromboplastin IV calcium V proaccelerin/labile factor VII proconvertin/stable factor VIII antihemophilic factor A IX christmas factor/antihemophilic factor B X stuart-prower factor XI thromboplastin antecedent XII hageman’s factor XIII fibrin stabilizing factor
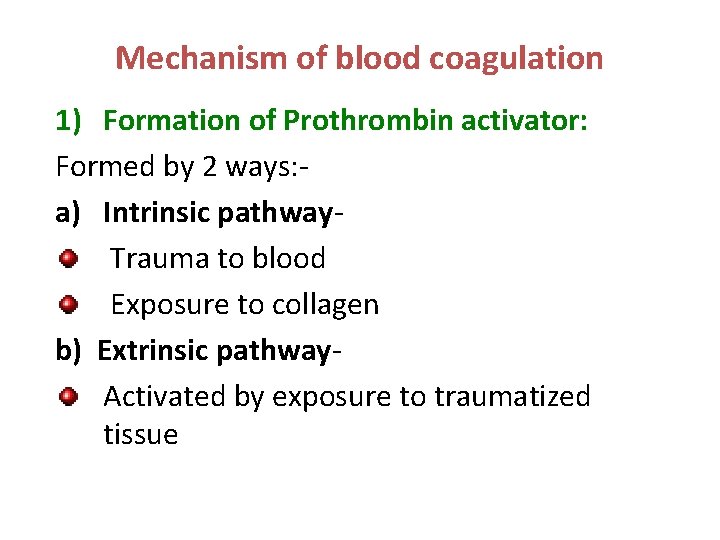
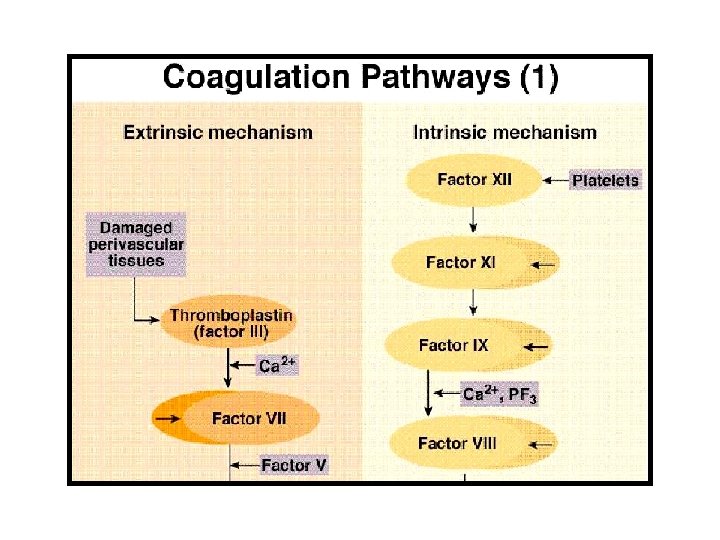
Mechanism of blood coagulation 1) Formation of Prothrombin activator: Formed by 2 ways: a) Intrinsic pathway. Trauma to blood Exposure to collagen b) Extrinsic pathway. Activated by exposure to traumatized tissue
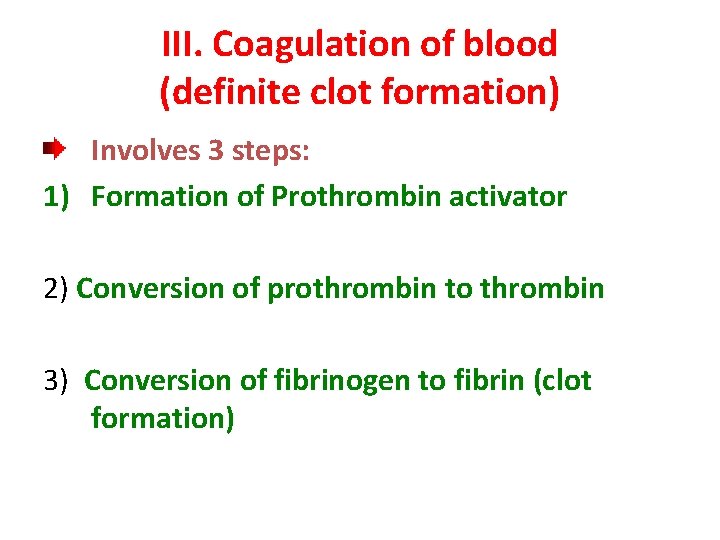
III. Coagulation of blood (definite clot formation) Involves 3 steps: 1) Formation of Prothrombin activator 2) Conversion of prothrombin to thrombin 3) Conversion of fibrinogen to fibrin (clot formation)
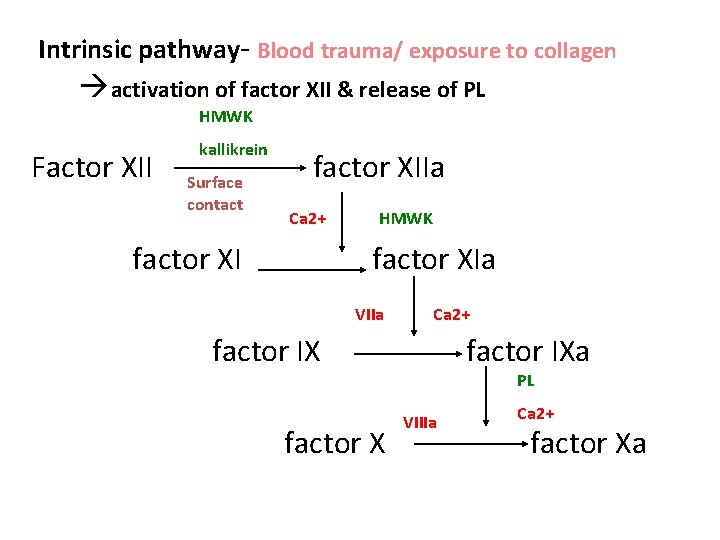
Intrinsic pathway- Blood trauma/ exposure to collagen activation of factor XII & release of PL HMWK Factor XII kallikrein Surface contact factor XIIa Ca 2+ factor XI HMWK factor XIa VIIa Ca 2+ factor IXa PL VIIIa Ca 2+ factor Xa
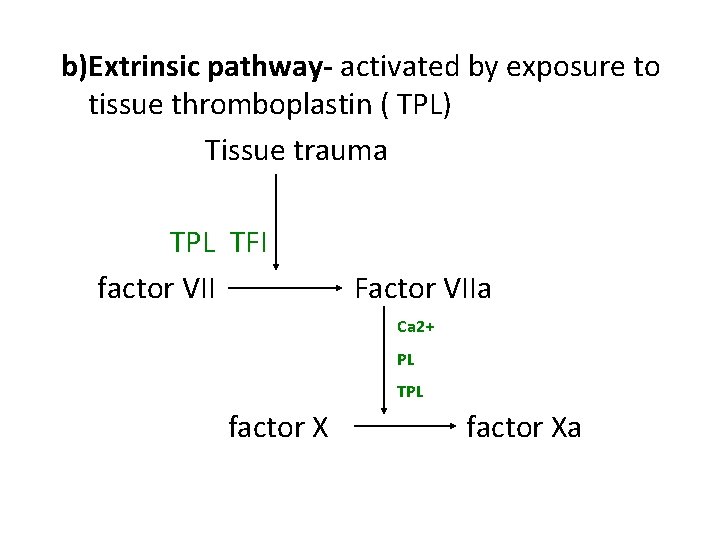
b)Extrinsic pathway- activated by exposure to tissue thromboplastin ( TPL) Tissue trauma TPL TFI factor VII Factor VIIa Ca 2+ PL TPL factor Xa
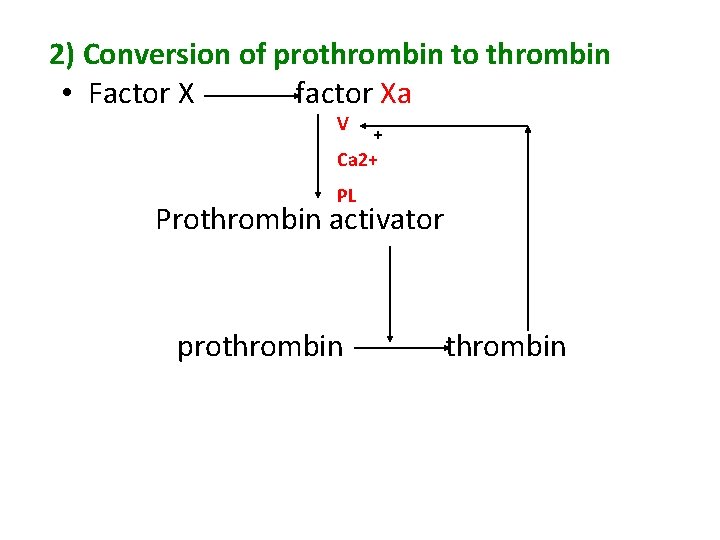
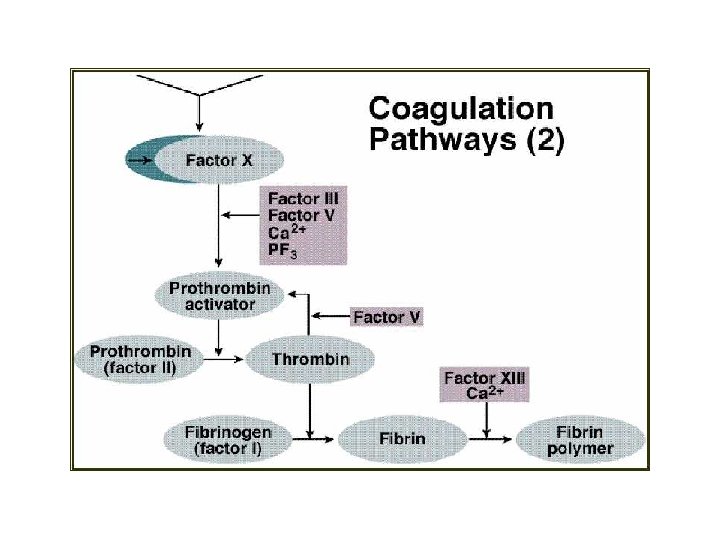
2) Conversion of prothrombin to thrombin • Factor X factor Xa V + Ca 2+ PL Prothrombin activator prothrombin
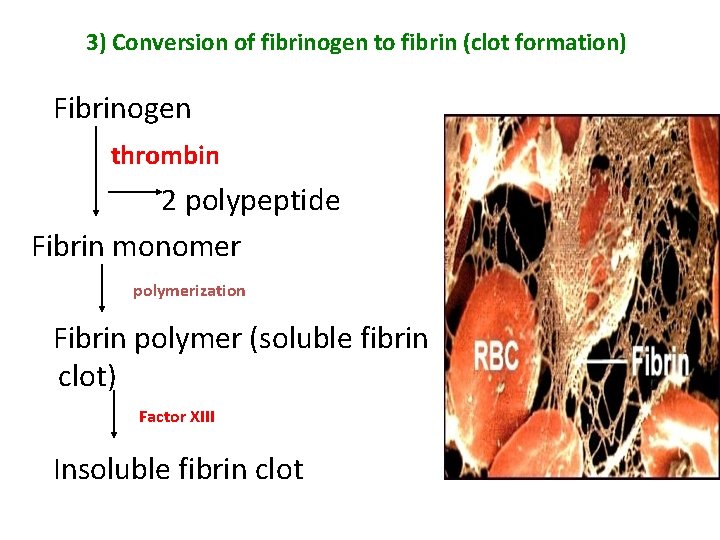
3) Conversion of fibrinogen to fibrin (clot formation) Fibrinogen thrombin 2 polypeptide Fibrin monomer polymerization Fibrin polymer (soluble fibrin clot) Factor XIII Insoluble fibrin clot
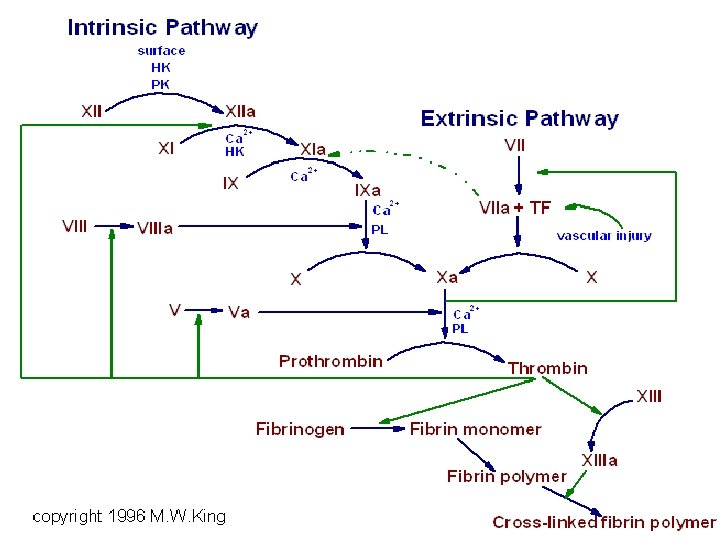
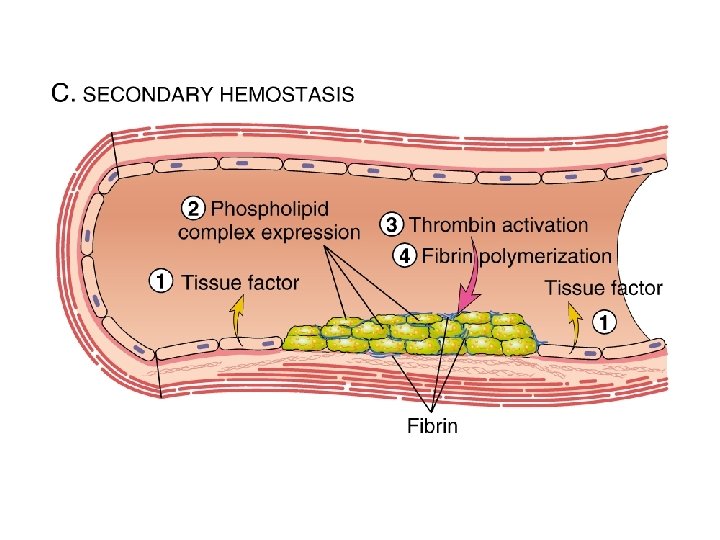
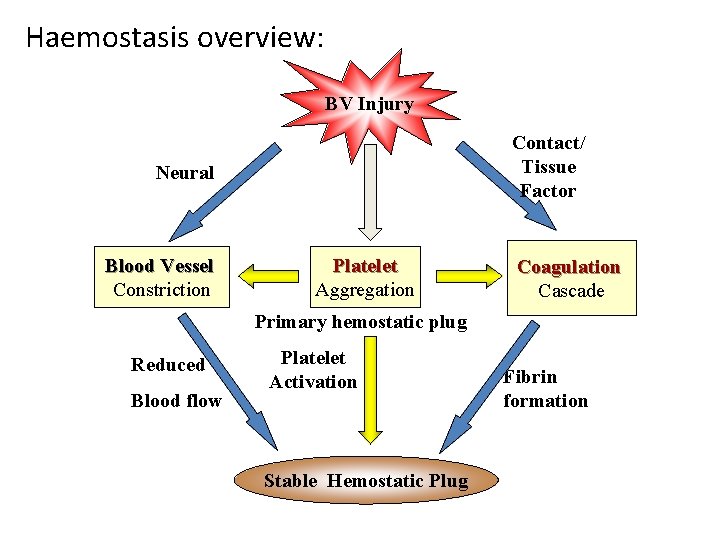
Haemostasis overview: BV Injury Contact/ Tissue Factor Neural Blood Vessel Constriction Platelet Aggregation Coagulation Cascade Primary hemostatic plug Reduced Blood flow Platelet Activation Stable Hemostatic Plug Fibrin formation

Coagulation: • • • Fibrinogen to Fibrin – Coag. Cascade Several factors – proenzymes-activation. Enzyme amplication – Plasma, Endothelium & Platelets Stable hemostatic plug. Clot lysis – starts soon after clot formation.
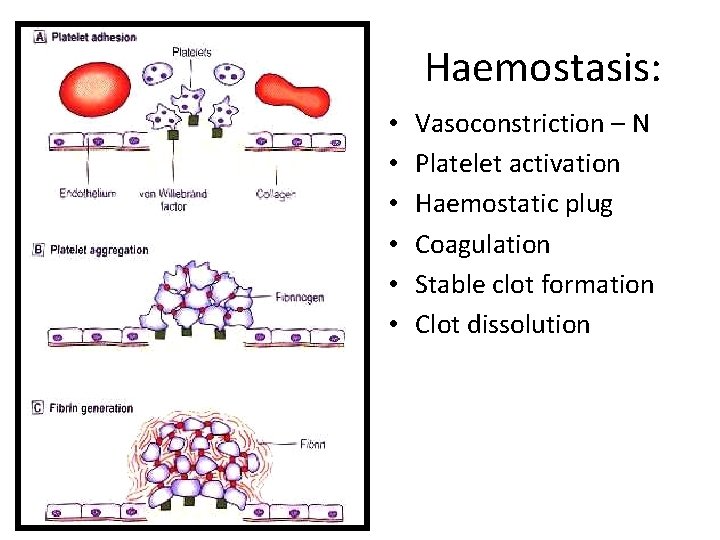
Haemostasis: • • • Vasoconstriction – N Platelet activation Haemostatic plug Coagulation Stable clot formation Clot dissolution
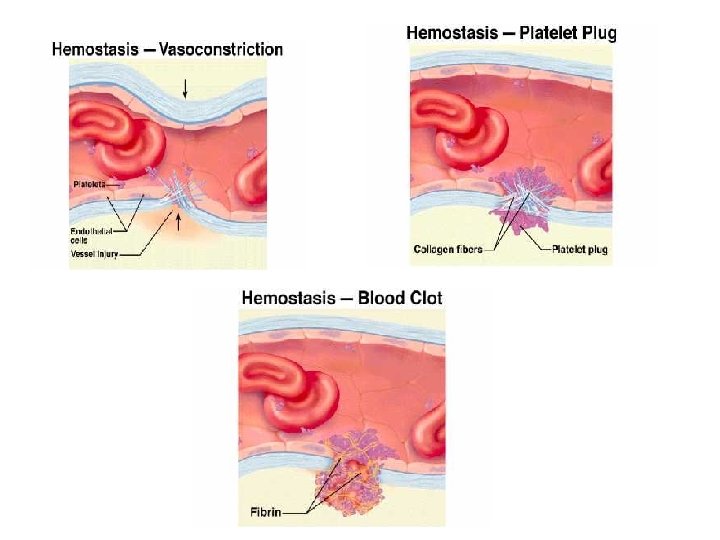

Coagulation: • Contact activation-Intrinsic system • Tissue factor activation – Extrinsic • Common pathamplification • Fibrin formation • Fibrin lysis.

Bleeding disorders

Coagulation factor disorders • Inherited bleeding disorders – Hemophilia A and B – von. Willebrands disease – Other factor deficiencies • Acquired bleeding disorders – Liver disease – Vitamin K deficiency/warfarin overdose – DIC

Vitamin K deficiency • Source of vitamin K Green vegetables Synthesized by intestinal flora • Required for synthesis Factors II, VII, IX , X Protein C and S • Causes of deficiency Malnutrition Biliary obstruction Malabsorption Antibiotic therapy • Treatment Vitamin K Fresh frozen plasma

Disorders of Hemostasis • Vascular disorders – Scurvy, easy bruising, • Platelet disorders – Low Number or abnormal function • Coagulation disorders – Factor deficiency. • Mixed/Consumption: DIC

purpura • This is a condition where there is a tendency to a “spontaneous” hemorrhages, usually beneath the skin from various mucous membrane & in internal organs.

A) Primary (idiopathic) B) Secondary purpura 1. Thrombocytopenia – platelet count <50000/µl 2. Thromboasthenia – deficiancy of platelet function 3. Acquired a. allergy b. Vit C deficiancy c. Infection d. Intolerance to drugs e. Cancer Treatment: whole blood transfusion splenectomy

haemophilia • It is a clotting disorder that occurs almost exclusively in males. Inherited sex-linked anomaly invariably transmitted females.

Cause: Haemophilia A (classical haemophilia): 85% Deficiency of factor VII Haemophilia B ( christmas disease): 15% Deficiency of factor IX Haemophilia C: rare Deficiency of factor XI Severe bleeding occurs after injury of any kind even of the most trivial character Tretment: Fresh plasma Cryo precipitate of clotting factors
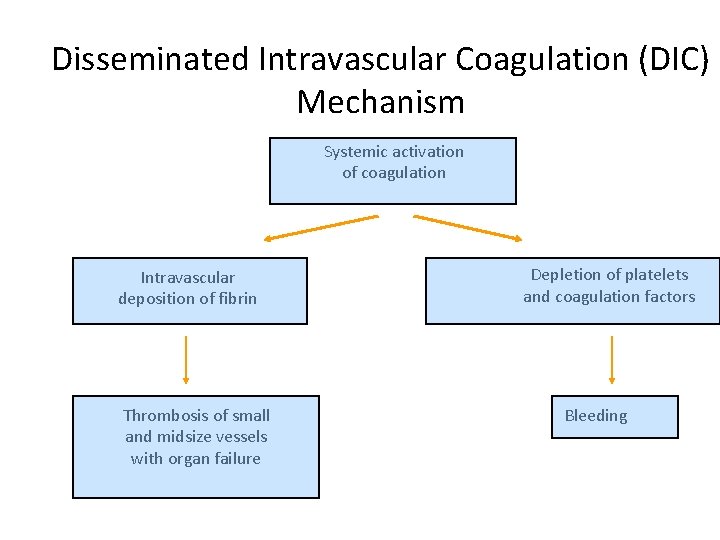
Disseminated Intravascular Coagulation (DIC) Mechanism Systemic activation of coagulation Intravascular deposition of fibrin Thrombosis of small and midsize vessels with organ failure Depletion of platelets and coagulation factors Bleeding
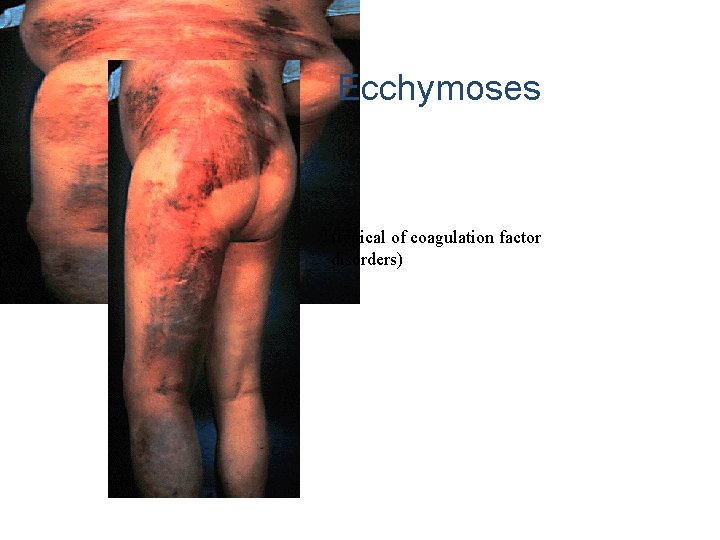
Ecchymoses (typical of coagulation factor disorders)
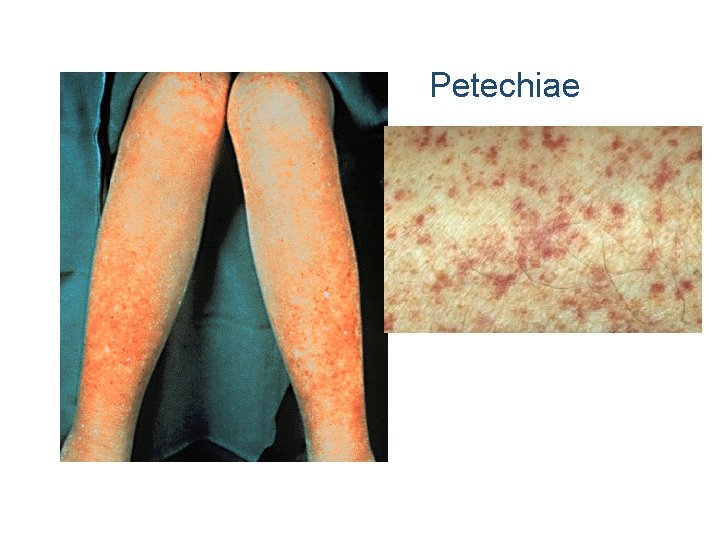
Petechiae

Petechiae, Purpura
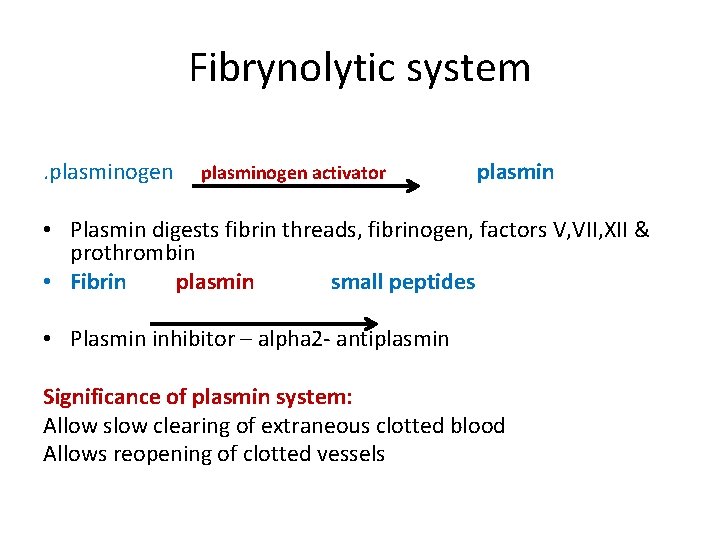
Fibrynolytic system. plasminogen activator plasmin • Plasmin digests fibrin threads, fibrinogen, factors V, VII, XII & prothrombin • Fibrin plasmin small peptides • Plasmin inhibitor – alpha 2 - antiplasmin Significance of plasmin system: Allow slow clearing of extraneous clotted blood Allows reopening of clotted vessels

• Anticoagulant factors 1. Physical characteristics of endothelium 2. High blood flow rate 3. Natural anticoagulants - Antithrombin III - Heparin - Proteinc C & protein S - Alpha 2 - macroglobulin - Fibrinolytic system Procoagulant factor 1. All clotting factors 2. Collagen 3. Reduced blood flow 4. Platlets phospholipids

1. Physical charecteristics of endothelium: Endothelial surface factors • Smoothness of endothelium • Layer of glycocalyx • Thrombomodulin + thrombin slows the clotting process also activates protein C Acts as an anticoagulant by *Inactivating factor V & factor VII *Activates plasminogen activator
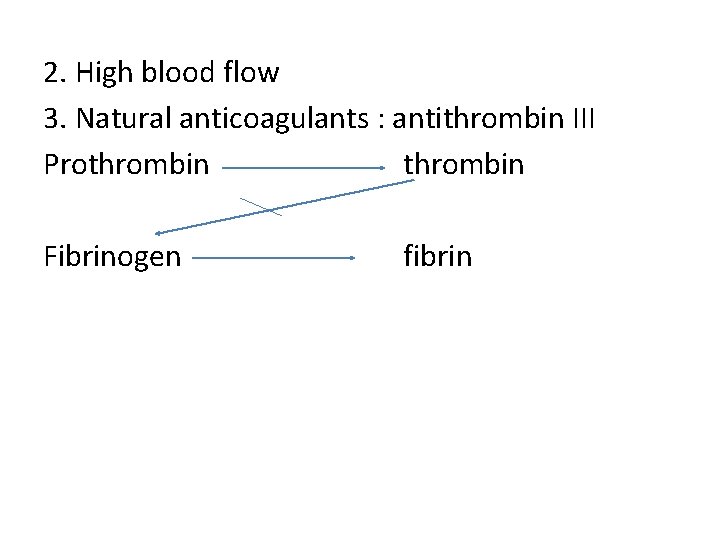
2. High blood flow 3. Natural anticoagulants : antithrombin III Prothrombin Fibrinogen fibrin

• Heparin: • Facilitate the action of antithrombin III & inhibiting the active forms of clotting factors IX, X, XII • Source: granuels of basophil & mast cells Heparin + antithrombin III s effectiveness of antithrombin III 100 – 1000 folds Also remove factor IX, X, XII
- Slides: 46