ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES causes 1

ACQUIRED COAGULATION ABNORMALITIES

ACQUIRED COAGULATION ABNORMALITIES - causes 1. 2. 3. Vitamin K deficiency Liver disease Clotting factor inhibitors : a) circulating anticoagulants b) complications of anticoagulant therapy 4. Incraesed consumption or loss of the clotting factors: a) disseminated intravascular coagulation ( DIC) b) fibrinogenolysis (primary fibrinolysis)

Coagulation abnormalities vitamin K deficiency dependent § vitamin K is essential for the final postribosomal carboxylation of coagulation factors II, VII, IX, X and the physiologic anticoagulants, protein C and protein S § laboratory features - prothrombin time (PT) is prolonged and decreased factors II, VII, IX, X level § activated partial thromboplastin time (a. PTT) prolonged in severe, protracted vitamin K deficiency

Vitamin K deficiency-etiology I. Inadequate supply: 1. Dietary deficiency 2. Destroying the gut flora by administration of broadspectrum antibiotics II. Impaired absorption of vitamin K: 1. Biliary obstruction (gallstone, strictures, tumor) 2. Malabsorption of vitamin K(sprue, celiac disease, ulcerative colitis) 3. Drugs (cholestyramine) III. Pharmacologic antagonists of vitamin K (coumarins, warfarin)

Abnormalities of hemostasis and coagulation in liver diseases (1) I. Decreased synthesis of coagulation factors 1. Fibrinogen, protrombin, clotting factors V, VII, IX, X, XII, XIII, prekallikrein, high molecular weight kininogen 2. Antiplasmins, antithrombin, protein C and S II. Aberrant biosynthesis : 1. Of abnormal fibrinogenu 2. Of abnormal analogues of prothrombin, factors VII, IX, X,

Abnormalities of hemostasis and coagulation in liver diseases (2) III. Deficient clearance : 1. Of fibrin monomers, fibrinogen degradation products (FDP) 2. Of activated coagulation factors (IXa, Xia) 3. Of plasminogen acivators IV. Accelerated destruction of coagulation factors: 1. Intravascular coagulation 2. Localized coagulation (hepatic cell necrosis) 3. Abnormal fibrinolysis V. Thrombocytopenia and platelet dysfunction (splenomegaly)

Circulating anticoagulants Clotting factor inhibitors are autoantibodies (usually Ig. G) or alloantibodies ( in hemophilia A) that inactivate coagulation factors and, therefore, act as anticoagulants - The laboratory test: prolonged a. PTT,

Circulating anticoagulants I. Antibodies to factor VIII (prolonged a. PTT, normal INR) 1. In hemophilia A 2. Postpartum -several months after parturition in asociation with a first pregnancy 3. Various immunologic disorders (rheumatoid arthritis, SLE, penicillin allergy ) 4. Older patients without underlying disease II. Other spontaneous inhibitors (rarely)- against factors : V, IX, XIII, fibrinogen, III. Lupus anticoagulant (in 30% SLE, rheumatoid arthritis, HIV infection, in lymphoproliferative disorders, after drugs hydralazine, quinidine, penicillin)

Disseminated intravascular coagulation - DIC is an acquired syndrome characterized by the activation of intravascular coagulation up to intravascular fibrin formation. , The process may be accompanied by secondary fibrinolysis or inhibition of fibrinolysis. This definition implies that microclot formation and consecutive organ failure and/or a hemorrhagic diathesis may occur.

DIC- ETIOLOGY 1. Infections: viral (herpes, acute hepatitis), bacterial (meningococcemia, septicemia), mycotic (aspergillosis), protozoal (malaria), 2. Abruptio placentae, septic abortion, postpartum hemolyticuremic syndrome 3. Neoplasms: carcinomas (prostate, pancreas, lung, ovary) 4. Disorders of hematopoietic system: acute leukemia (promyelocytic ) intravascular hemolysis 5. Vascular disorders: giant hemangiomas, aneurysmas, myocardial infarctioncardiac arrest, various forms of shock, 6. Massive tissue injury: large traumatic injuries and burns, 7. Miscellaneous: acute pancreatitis, graft versus host disease, diabetic acidosis,

ACUTE DIC-CLINICAL PRESENTATION § symptoms of underlying disease § symptom of local thrombosis § hemorrhagic diathesis § shock
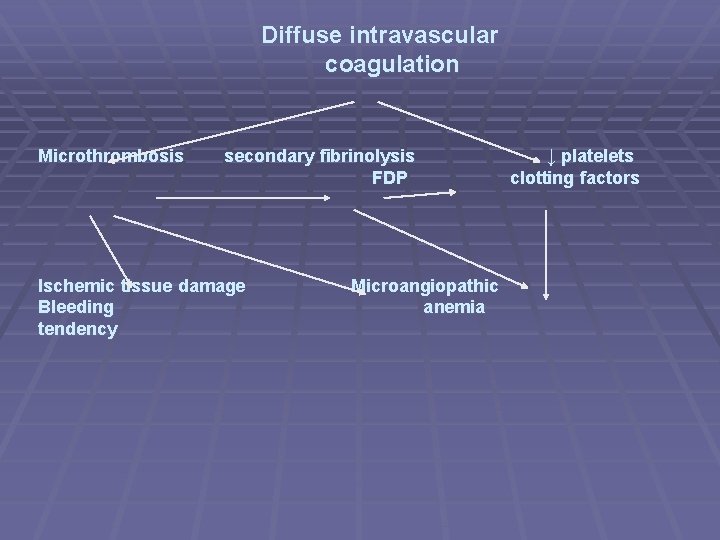
Diffuse intravascular coagulation Microthrombosis secondary fibrinolysis FDP Ischemic tissue damage Bleeding tendency Microangiopathic anemia ↓ platelets clotting factors

Acute. DIC-laboratory features § § § § § Increased D-Dimer level Increased FDP level Decreased AT level Decreased platelet level Bload smear - schistocytes Decreased fibrinogen level Prolonged thrombin time Prolonged a. PTT Prolonged prothrombin time (PT)

Acute DIC diagnosis The basis of the diagnosis is the knowledge of the underlying diseases in which DIC can occur. Because patients suffering from acute DIC need urgent therapy, DIC should always be taken into consideration if a complex coagulation defect in combination with a underlying disease is observed.

CHRONIC (compensated) DIC In chronic DIC, the activation of the hemostatic system is minimal since negative feedback mechanisms as well as inhibitors can limit the activation process so that microthrombi do not occur and bleeding episodes are rare phenomena.

Chronic DIC - etiology 1. Obstetric complications: eclampsia, the death fetus syndrom 2. Vascular disorders: giant hemangiomas (Kasabach Merrit syndrome), Leriche syndrome, Raynaud, s disease 3. Carcinomas 4. Hematology disorders: myelofibrosis, polycythemia vera, NNH 5. Collagen-vascular disorders: SLE, sclerodermia 6. Kidneys disorders: glomerulonephritis, HUS 7. Another: vasculitis allergica, diabetes mellitus

PRIMARY FIBRINOLYSIS (FIBRINOGENOLYSIS) DEFINITION: primary fibrinolysis occurs when plasmin is generated in the absence of DIC. This has been described in hepatic disorders, prostatic carcinomas, and cases without apparent cause. At present, most cases of primary fibrynolysis are iathrogenically induced during thrombolytic therapy.
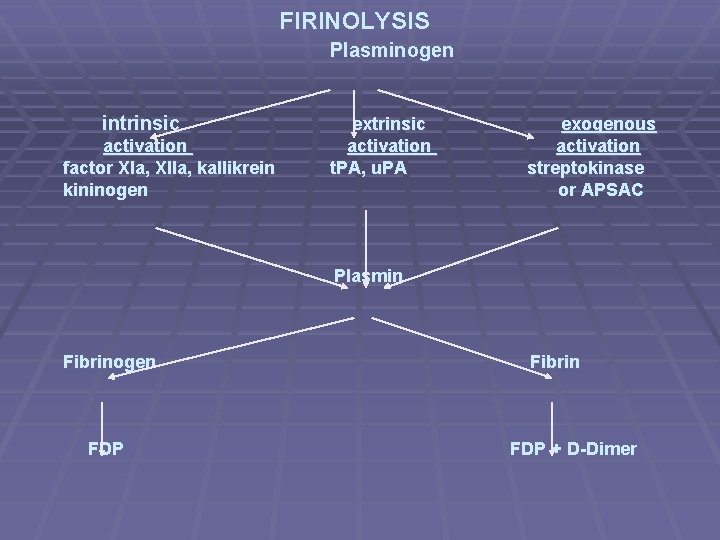
FIRINOLYSIS Plasminogen intrinsic activation factor XIa, XIIa, kallikrein kininogen extrinsic activation t. PA, u. PA exogenous activation streptokinase or APSAC Plasmin Fibrinogen FDP Fibrin FDP + D-Dimer

Acquired coagulation abnormalities diagnostics I History II Physical examination III Laboratory features - morphology - blood smear - bleeding time - prothrombin time (PT), INR - a. PTT - thrombin time (TT) - fibrinogen - fibrin(ogen) degradation products (FDP) - D-dimer - antithrombin
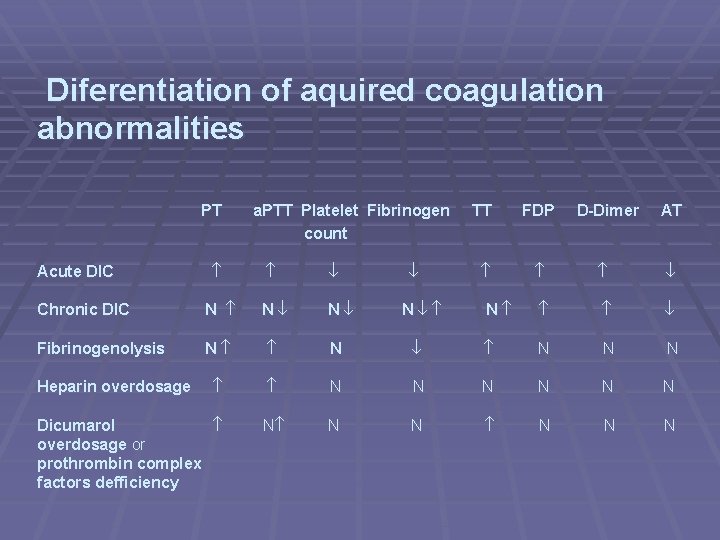
Diferentiation of aquired coagulation abnormalities PT a. PTT Platelet Fibrinogen count FDP D-Dimer AT N Chronic DIC N N N Fibrinogenolysis N N N N N Acute DIC Heparin overdosage Dicumarol overdosage or prothrombin complex factors defficiency TT N

ACA – THERAPY (1) I Vitamin K deficiency - Vit. K i. m. / i. v. 10 -20 mg/doba - severe bleeding - Vit. K i. v. + FFP(�) 10 -15 ml/kg II Liver disease - Vit. K - severe bleeding: FFP or prothrombin complex concentrates (FEIBA, Autoplex) III Warfarin overdosage - withhelt anticoagulant on 1 -2 d, reduction of dosage - moderate complications – Vit, . K - severe bleeding – FFP or prothrombin complex concentrates, FFP

ACA- Therapy (2) IV Bleeding disorders of circulating inhibitors - factor VIII inhibitor - massive FVIII replacement , cryoprecipitate - FVIII porcin - immunosuppressive therapy - plasmapheresis and high –dose i. v. Ig. G - activated FVII V Heparin-induced hemorrhage: stop the heparin infusion, intravenous protamin administration at the dosage of 1 mg/100 U of heparin, FFP

ACA – DIC THERAPY 1. Treatment of the underlying disorder 2. Treatment of shock 3. Replacement therapy - platelet concentrates - RBC - FFP - Cryoprecipitate (fibrinogen) - activated protein C 4. Heparin treatment (unfractioned heparin or low-molecular weight heparin (acrocyanoza, purpura fulminans, dermal necrosis, venous thromboembolism)
- Slides: 23