Urinary Tract Infections Dr haiying liu department of



































































































- Slides: 104

Urinary Tract Infections Dr. haiying liu department of nephrology the second hospital of shandong university

Introduction • UTIs represent a wide variety of syndromes including urethritis, cystitis, prostatitis, and pyelonephritis. • One of the most commonly occurring infections.

Introduction • Young women are particularly susceptible, 40% of all women will suffer at least one UTI at some point. • Infection in men occurs less frequently until the age of 50, when incidence in men and women is similar.

Definition • It is the presence of microorganisms in the urinary tract that cannot be accounted for by contamination. • The organisms have the potential to invade the tissues of the UT and adjacent structures.

Definition • A UTI can manifest as several syndromes associated with an inflammatory response to microbial invasion that range from asymptomatic bacteriuria to pyelonephritis.

Classification According to anatomic site of involvement: • Lower tract infection: cystitis, urethritis, prostatitis • Upper tract infection: pyelonephritis, involving the kidneys

Classification According to Degree 1 -Uncomplicated • Occur in individuals who lack structural or functional abnormalities in the UT that interfere with the normal flow of urine. • Mostly in healthy females of childbearing age

Classification According to Degree 2 -Complicated predisposing lesion of the UT such as congenital abnormality or distortion of the UT, a stone a catheter, prostatic hypertrophy, obstruction, or neurological deficit • All can interfere with the normal flow of urine and urinary tract defenses.

Recurrent UTIs • Multiple symptomatic infections with asymptomatic periods • Reinfection: caused by a different organism than originally isolated and account for the majority of recurrent UTIs. • Relapse: repeated infections with the same initial organism and usually indicate a persistent infectious source.

Other Definitions Asymptomatic bacteriuria • Common among the elderly • Bacteriuria > 105 bacteria/ml of urine without symptoms Symptomatic abacteriuria: • Symptoms of frequency and dysuria in the absence of significant bacteriuria

Other Definitions Significant bacteriuria • More than 105 bacteria /ml (CFU) of urine in clean catch specimen • 1/3 of symptomatic women have CFU counts below this level • A bacterial count of 100 CFU/ml has a high positive predictive value of cystitis in symptomatic women

Other Definitions Count less than 105 may represent true infection in certain situations • Concurrent antibacterial drug administration • Rapid urine flow • Low urine PH • Upper tract obstruction

Etiology The microorganism that cause UTIs usually originate from the bowel flora of the host Uncomplicated UTI: • E. coli accounts for 85% • S. saprophyticus 5 -15% • K. pneumoniae, Pseudomonas, and Enterococcus 5 -10% • S. epidermidis if isolated should be considered a contamination

Etiology Complicated UTIs • More varied and generally more resistant • E. coli 50% • K. pneumoniae, Pseudomonas, Enterococcus, sp

Etiology Complicated UTIs • Enterococcus fecalis 2 nd most frequently isolated organism in hospitalized patients • SP infection is more commonly a result of bacteremia producing metastatic abscesses in the kidney • Candida is common cause of UTI in critically ill and chronically catheterized patients

Etiology • The majority of UTIs are caused by a single organism • In patients with stones , indwelling catheter, or chronic renal abscesses multiple organisms may be isolated • Although this may be due to contamination and a repeat evaluation should be done.

Predisposing factors Abnormalities in the UT that interfere with natural defenses 1 -Obstruction can inhibit urine flow, disrupting the natural flushing and voiding effect in removing bacteria from the bladder and resulting in incomplete emptying

Predisposing factors Abnormalities in the UT that interfere with natural defenses. 2 -Condition that result in residual urine volumes e. g. prostatic hypertrophy, urethral stricture, calculi, tumors, and drug such as anticholinergic agents, neurological malfunctions associated with stroke, diabetes, and spinal cord injuries.

Predisposing factors Abnormalities in the UT that interfere with natural defenses. 3 -Other risk factors include: urinary catheter, mechanical instrumentation, pregnancy, and the use of spermicidies and diaphragms

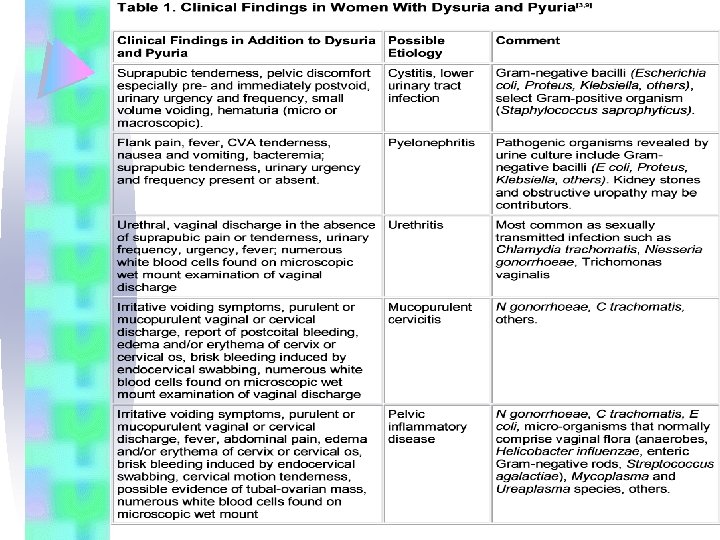
Clinical presentations Lower tract infection: • Include dysuria, urgency, frequency, nocturia, suprapubic heaviness, and hematuria in women. • No systemic symptoms Upper tract infection: • Flank pain, costovertebral tenderness, abdominal pain, fever, nausea, vomiting and malaise.

Clinical presentations Elderly patients: • Frequently do experience specific urinary symptoms • Altered mental status, change eating habits, or GI symptoms Patients with catheters • Will have no lower tract symptoms • Just flank pain and fever

Laboratory findings • Symptoms alone are unreliable for diagnosis • Examination of the urine is the cornerstone of diagnosis Collection of urine: • Mid stream clean catch method is preferred method

Laboratory findings Collection of urine: • Catheterization for patient who are uncooperative or unable to void, but introduction of bacteria in the bladder occurs at 1 -2% • Suprapubic aspiration bypasses the contaminating organism in the urethra, safe and painless.

Diagnosis: • Based on isolation of significant numbers of bacteria from a urine specimen Microscopic examination • is performed by preparing a gram stain that indicates the morphology of the organism and help direct the selection of an appropriate AB.

Diagnosis: Microscopic examination • The presence of one organism per oil-immersion field in an un centrifuged sample correlates with 100, 000 bacteria/ml

Diagnosis: Hematuria, non-specific, may indicate other disorders such as calculi or tumor Protenuria is found in the presence of infection

Diagnosis: Pyuria: WBC > 10 WBC/mm 3 • it only signifies the presence of inflammation Sterile pyuria is associated with urinary tuberculosis, chlamydial, and fungal infections

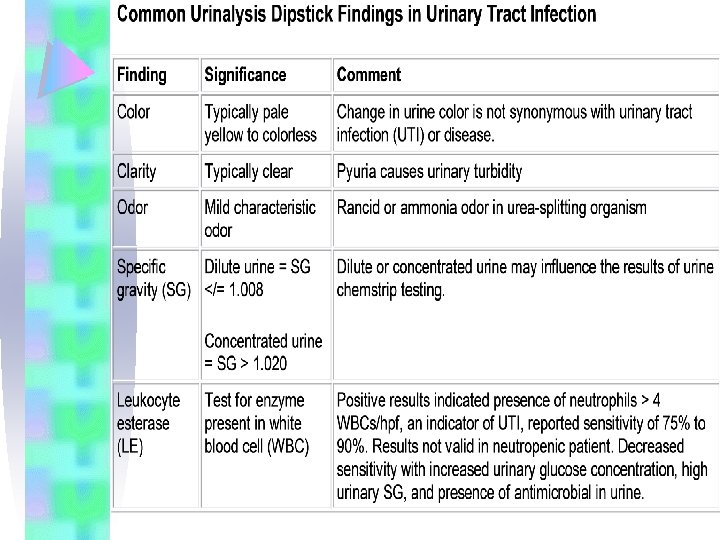
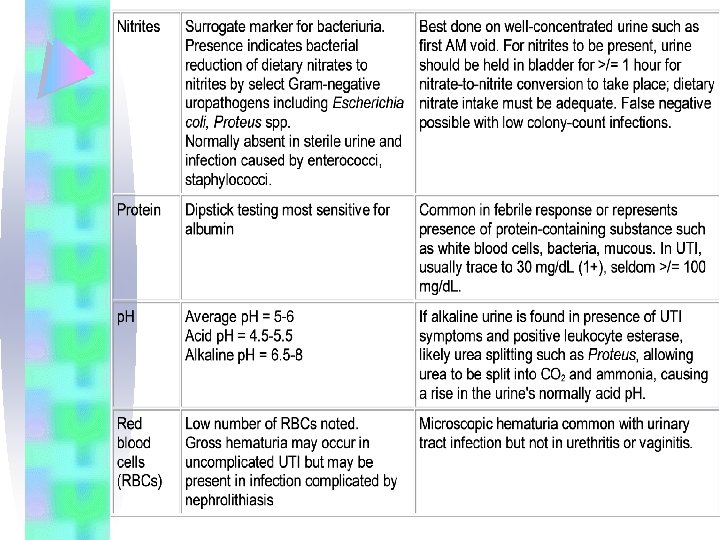
Diagnosis Biochemical tests 1 -dipstick test for nitrite: bacteria in the urine reduce nitrate→ nitrite • false –negatives are common and caused by • gm+ve or pseudomonas that do not reduce • low urinary PH • frequent voiding and dilute urine

Diagnosis Biochemical tests 2 - leukocyte esterase dipstick test • rapid screening test for detecting the presence of pyuria • LE is found in neutrophills


Diagnosis Quantitative urine culture • Based on properly collected urine • Urine is normally sterile • Determines the number of bacteria present in a urine sample • 1/3 of symptomatic women have bacteria < 105


Diagnosis Quantitative urine culture • one organism per oil immersion field correlates with 100, 000 CFU/ml by culture Susceptibility • determine bacterial susceptibility to different antimicrobials

Treatment Desired outcome • Prevent or treat systemic consequences of infection • Eradicate the invading organism • Prevent reoccurrence of infection

Treatment Non-specific therapies 1 -fluid hydration: • rapid dilution of bacteria and removal of infection through increased voiding

Acute uncomplicated cystitis Most common form of UTI? • Occur in women of childbearing age • Can be explained by – – sexual activity anatomy (short urethra) delay in micturation use of diaphragm and spermicidal Causes • Mostly cause E. coli • Other causes : S. saprophyticus. K. pneumonia, Proteus mirabilis

Treatment Non-specific therapies 3 -urinary analgesics • phenazopyridine • has little clinical role in infection because symptoms respond rapidly to antimicrobial therapy


Acute uncomplicated cystitis Management: • Urinanalysis including microscopic examination, cell count, and LE test • urine culture add little to the choice of empiric therapy

• Regarding the use of laboratory tests to diagnose urinary tract infections, which of the following statements is correct? • A. In a patient with suspected cystitis, urine dipstick results should be confirmed with a urinalysis B. The urine should always be cultured in outpatients with acute cystitis C. Urine dipstick results usually provide the laboratory information needed to manage young otherwise healthy patients with acute cystitis D. The use of urine dipsticks should be avoided; urinalysis is the test of choice.

Acute uncomplicated cystitis Management: 1 - Single dose therapy • 65 -100% cure rate with SMXTMP, amoxicillin advantages of single does: • less expensive • better compliance • low side effects • low potential for development of resistance

Acute uncomplicated cystitis 1 - Single Dose Therapy • Not all agents are effective as single dose • 2 DS TMP/SMX is most effective • β-lactam are less effective due to increasing resistance and because they are eliminated rapidly and do not achieve high urine concentrations

Acute uncomplicated cystitis 2 -Three day course • single dose Tx was blamed for high rate of recurrence within six weeks • this may be due to failure to eradicate gm-ve bacteria from the rectum • TMP/SMX is superior to single dose • Amoxicillian, nitrofurantion, are not appropriate due to increasing resistance of E. coli

Acute uncomplicated cystitis Management: Short course therapy is not appropriate for • Patient with previous infection with a resistant bacteria • Male patients • Complicated UTI

Acute uncomplicated cystitis Management: • If symptoms do not respond or they reoccur, a urine culture should be obtained and conventional therapy started

Acute uncomplicated cystitis Management: 3 -Seven-day course • in pregnant women • diabetic women • women who have had symptoms for more than one week and are at higher risk for pyelonephritis

Symptomatic abacteriuria Acute urethral syndrome • In females, present with dysuria and pyuria • Urine culture reveals < 105 bacteria /ml • Accounts for half the complaints of dysuria in women • Most likely infected with a small number of bacteria

Symptomatic abacteriuria Causes: • E. coli, S. saprophyticus • Other causes: • Most patients will require short course therapy as above

Symptomatic abacteriuria 1 g of azithromycin or doxycycline 100 mg bid for 7 days • Concomitant treatment of sexual partner is required to cure this infection and prevent recurrence

Asymptomatic bacteriuria • Patients with no urinary symptoms • Have two consecutive urine cultures with > 105 • The majority are elderly and female

Asymptomatic bacteriuria • Aggressive treatment does not affect infection, complications or mortality • Also present in pregnant women • Relapse and reinfection are common and chronicity occurs which is difficult to eradicate

Asymptomatic bacteriuria Management Groups who benefit from treatment: • pregnant women • patient with renal transplant • Patient who will undergo urinary procedure

Asymptomatic bacteriuria Management • Depend on age and whether they are pregnant • In children: conventional treatment because of greater risk for renal damage • In non-pregnant female: controversial

Asymptomatic bacteriuria Management • In elderly: two groups – Persistent bacteriuria: – Intermittent bacteriuria • Mostly seen as a benign disease and does not warrant treatment • Two cultures should be obtained to confirm the presence of bacteria

Asymptomatic bacteriuria Management • Only 50% remained free of bacteria for 1 year • Hospitalized patients: therapy in non-efficacious

Case 1 • A 24 -year-old woman comes to the clinic to discuss recent laboratory results. She went to a local walk-in clinic asking to be screened for a urinary tract infection. She comes to the clinic to review them with you. She is asymptomatic and has no past medical history. She is married and has a 3 year-old boy. Her physical exam is unremarkable. A urinalysis showed 1+ leukocyte esterase; a urine culture revealed >100000 CFU of Escherichia coli.

Case 1 Which of the following management strategies is the most appropriate for this patient? • A. Explain that even though the urine culture was positive she does not need treatment B. Start oral ciprofloxacin for three days C. Repeat a urine dipstick, and if the presence of pyuria is confirmed start treatment D. Start oral ampicillin for seven days

Case 1 • The IDSA guidelines recommend screening for and treatment of asymptomatic bacteriuria in only three circumstances: pregnancy, before invasive urologic procedures that are associated with mucosal bleeding, and in women who are found to have catheter-acquired bacteriuria that persists 48 hours after the catheter is removed

Complicated UTI • Accurate urine culture and susceptibility is necessary to target the pathogen • Treatment duration at least 10 -14 days


Acute pyelonephritis • Perform uniranalysis, gram stain, C&S Severely ill patients • Should be hospitalized and treated with IV Abs • Use broad spectrum directed at bacteremia or sepsis

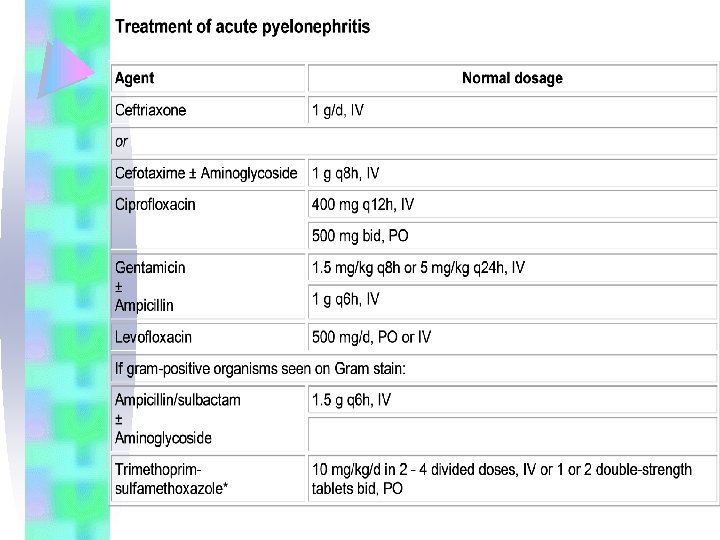
Acute pyelonephritis Empiric therapy: • 3 rd generation cephalosporin with antipseudomanl activity as ceftazidime, cefoperazone • Ampicillian + gentamicin • TMP/SMX • B-lactamase inhibitor combination: ampicillian/Sulbactam • imipenem

Acute pyelonephritis If the patient has been hospitalized for > 6 months: • Consider P. aeruginosa and enterococci, and multiple organisms Empiric therapy: • Piperacillin/tazobactam • imipenem

Acute pyelonephritis Management • ceftazidime, cefepime, piperacillin/tazobactam, and aztreonam. • They have reliable activity against many nosocomially acquired gramnegative rods, including P aeruginosa.

Acute pyelonephritis Management Carbapenems, imipenem-cilastatin and meropenem. have extremely broad-spectrum coverage and should be reserved for only the most severe forms of nosocomial infections, such as multiresistant pathogens, sepsis syndrome, overwhelming intra-abdominal infections, or septic shock

Acute pyelonephritis • Effective therapy should stabilize patient within 12 -24 hrs • Bacterial load should reduce in 48 hrs If the patient fails to respond in 3 -4 days further investigation is necessary to • Exclude bacterial resistance • Exclude obstruction • Or other disease process

Acute pyelonephritis • Oral therapy can be started when the patient is non febrile for 24 hrs • Oral therapy should be continued for 2 wks • Follow-up urine cultures should be obtained 2 wks after end of therapy

Acute pyelonephritis Mild cases: • can be treated orally as outpatients for at least 2 w ks • Gram –ve bacilli: TMP/SMX ;Gram +ve: cocci: consider enterococcus fecalis, DOC Ampicillin


Case 2 22 year-old woman without any significant past medical history presents to the emergency room with 2 days of worsening fever, urinary frequency, back pain, nausea and vomiting. She is not able to keep food or liquids down. On physical examination she is febrile and tachycardic. The abdominal exam is normal except for the presence of moderate costovertebral angle tenderness. A blood pregnancy test is negative. A urinalysis is obtained and reveals >50 PMN per high power field and 10 -25 red blood cells. Blood cultures are sent to the lab.

Case 2 Which of the following management strategies is the most appropriate for this patient? A. Order an ultrasound to confirm your clinical impression, and start intravenous antibiotics if needed B. Admit the patient for administration of intravenous antibiotics, and obtain imaging studies only if the patient does not improve after a few days C. Start intravenous antibiotics, and order abdominal CT scan to rule out complicated pyelonephritis D. Discharge the patient home on an oral fluoroquinolone

Infection in males • Infection in males are considered complicated • Occur in presence of functional or structural abnormalities that disrupt the normal defense mechanism of urinary tract.


Infection in males The most common causes are • Instrumentation • Catheterization • Renal and urinary stones • In the elderly the most common cause is bladder outlet obstruction due prostatic hypertrophy.

Infection in males Treatment • Urine culture is needed because causative organism is not easily predictable • A urine culture with>100 CFU/ml is best sign of infection • If Gm –ve is TMP/SMX • Duration therapy should be 10 -14 days

Case 3 • A 53 year-old man with history of benign prostatic hypertrophy comes to the emergency room complaining of burning with urination and increased urinary frequency. He is afebrile, denies back pain, nausea or vomiting. His past medical history is also significant for hypertension and diabetes. He takes hydrochlorothiazide, enalapril, aspirin, metformin and terazosin. On physical examination his prostate is enlarged, but is not tender. Urine dipstick shows 3+ leukocyte esterase.

Case 3 • A 53 year-old man with history of benign prostatic hypertrophy comes to the emergency room complaining of burning with urination and increased urinary frequency. He is afebrile, denies back pain, nausea or vomiting. His past medical history is also significant for hypertension and diabetes. He takes hydrochlorothiazide, enalapril, aspirin, metformin and terazosin. On physical examination his prostate is enlarged, but is not tender. Urine dipstick shows 3+ leukocyte esterase.

Case 3 Which of the following interventions is the most appropriate for this patient? • A. Start ciprofloxacin, and order urine culture B. Start Levofloxacin, and order urine culture only of the patient fails to improve after five days of symptoms. C. Start nitrofurantoin empirically D. Admit the patient for intravenous piperacillin/tazobactam

Recurrent infection Reinfections: • Infection by an organism different from the initial infection • Mostly occurs in females where reinfection rate is 20% Factors contributing to infection: 1 -sexual intercourse 2 -diaphram and spermicidal use 3 - postmenopausal women

Recurrent infection Divided into two groups: 1 -Those with less than 2 or 3 episodes per year • Each episode should be treated as a separate infection • Short course therapy is appropriate • Can be self administered

Recurrent infection Divided into two groups: 2 -Those with more than 3 episodes per year • Long-term prophylaxis may be needed • Patient should be treated conventionally before prophylaxis is started

Recurrent infection Regimen: • TMP/SMX • Nitrofurantion 50 -100 mg OD • Continued for 6 months • Urine cultures followed monthly • If symptomatic episodes develop they should be treated with a full course

Recurrent infection Infection related to sexual activity: • Voiding after intercourse • Single-dose prophylactic with TMP/SMX taken after intercourse In postmenopausal women • Recurrent episodes related to decreased estrogen and changes in bacterial flora

Relapses • Persistence of the infection with the same organism after therapy • Usually indicate structural abnormality, renal involvement, or chronic bacterial prostatitis

Relapses In women: • If relapse after short course treat with 2 week course • In-patient who relapse after 2 wk course continue for another 2 -4 wks • If relapse after 6 wks of therapy, urologic evaluation and any obstruction corrected • May need therapy for 6 months

Relapses In males • Relapse usually indicate bacterial prostaitis • TMP/SMX appear to be highly effective for relapses

Case 4 • A 26 -year-old woman comes to the clinic complaining of recurrent cystitis. Over the previous year she has had 5 episodes of cystitis that were treated with antibiotics. The symptoms improved rapidly after each course of therapy. The episodes have happened once every two to three months for the last year. Her past medical history is otherwise unremarkable. She uses oral contraceptives for contraception. She has had two urine cultures done during the previous year that showed pansusceptible Escherichia coli. The patient asks for ways to prevent these infections from coming back.

Case 4 Based on the history and test results, which of the following interventions is indicated on this patient? A. Ask the patient to report the onset of infection as soon as possible, and start treatment if a urine dipstick is positive B. Offer antibiotic prophylaxis C. Change her contraception to spermicides and diaphragms D. Obtain abdominal ultrasound to look for a secondary cause of recurrent UTIs E. Perform an immunologic evaluation to rule out an underlying immune deficiency

Pregnancy Predisposing factors: • Dilation of the renal,pelvis and ureters • Decrease urethral peristalsis • Reduced bladder tone • All lead to urine stasis and reduced defenses against reflex of bacteria to the kidney • Hormonal changes predispose to infection

Pregnancy • Asymptomatic bacteriuria Occur in 4 -7% • 20 -40% will develop acute pyelonephritis • Routine screening for bacteriuria should be performed at the initial prenatal visit and at 28 wks

Pregnancy • Significant bacteriuria should be treated regardless of symptoms • Organism is the same for uncomplicated UTI • Therapy should be for 7 days

Pregnancy Regimen • amxoicillin • augmentin • cephalexin • nitrofurantion • Follow up urine culture 1 -2 wk after completing therapy, then monthly until gestation

Catheterized patients • Most common cause of hospital aquired UTI • diagnosis is difficult, – patients often have some degree of pyuria – Virtually all patients with catheters for 1 to 2 wks exhibit bacteriuria, making differentiation of infection from colonization difficult. – often lack symptoms • Occur in 5% of patients

Catheterized patients Etiology • often polymicrobial. • Causative agents include P aeruginosa and nosocomial gm –ve rods, with more resistant susceptibility profiles; enterococci; and Candida species. • Diagnosed with > 100 CFU/ml of urine from catheter • Urinalysis and urine cultures should always be obtained.

Catheterized patients Management 1 -Asymptomatic, • Remove the catheter Do not treat unless • immunosuppresed patient • Patient at risk of endocarditis • Patient who will undergo urinary tract instrumentation

Catheterized patients Management 2 -Symptomatic • Remove the catheter and treat as complicated UTI

Vancomycin-Resistant Enterococci • VRE are often isolated from urine cultures of patients who have been hospitalized for a prolonged period. • Most commonly, a urinary catheter is present. • If the organism is E. faecalis, then penicillin/ampicillin susceptibility is frequently maintained, and ampicillin is the treatment of choice.

VRE • However, most VRE are E. faecium that are also resistant to ampicillin (VARE) and to multiple other antimicrobials. • Many VARE are susceptible to nitrofurantoin, and it can be used as long as the patient has a Cr. CL >60 m. L/min

VRE • Chloramphenicol or novobiocin, with or without other drugs, have been used. • Two newer antibiotics, quinupristin/dalfopristin and linezolid, have been marketed for gram-positive infections and have activity against VARE.

Fungal Infection • Many patients with a long-term catheter will have colonization of their bladder with Candida species or, rarely, other fungi.

Fungal Infection • Usually funguria in the absence of pyuria should not be treated, and the catheter should be removed. • Funguria should be treated in – renal transplant recipients – those undergoing an elective urologic procedure.

Fungal Infection Diagnosis • pyuria (> 20 WBC/hpf) • > 105 fungal organisms / ml of urine. • Patients may or may not have systemic findings, such as fever and leukocytosis.

Fungal Infection Treatment • The catheter should be removed, since this will result in cure in some patients. • If C. albicans infection, then oral fluconazole, 100 mg/d, should be prescribed for a 2 - to 5 -days • IV fluconazole should be reserved for patients without the ability to take oral medications or in those with ileus or bowel obstruction.

Fungal Infection Treatment • Non-albicans Candida species, including C. glabrata, and C. krusei, are becoming more common. • should be either low-dose IV amphotericin B (0. 1 mg/kg/d) or continuous amphotericin B bladder irrigation. • Both regimens are effective when given for 2 to 5 days.