Urinary Tract Infections Prof Dr ar BKE Yeditepe

Urinary Tract Infections Prof. Dr. Çağrı BÜKE Yeditepe University Medical Faculty Infectious Diseases and Clinical Microbiology
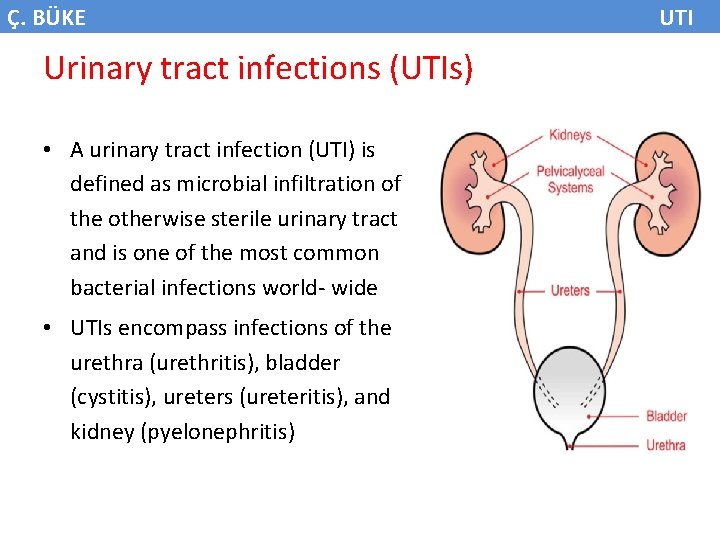
Ç. BÜKE Urinary tract infections (UTIs) • A urinary tract infection (UTI) is defined as microbial infiltration of the otherwise sterile urinary tract and is one of the most common bacterial infections world- wide • UTIs encompass infections of the urethra (urethritis), bladder (cystitis), ureters (ureteritis), and kidney (pyelonephritis) UTI

Ç. BÜKE UTI Epidemiology • UTIs are the most frequent bacterial infection seen in the outpatient setting: 1 in 3 women will develop a UTI requiring antibiotic treatment by age 24, and • UTIs are the second most common cause for prescription of antibiotics • 50% experience at least 1 UTI during their lifetime

Ç. BÜKE UTI Epidemiology • The incidence of cystitis is significantly higher in women than men, likely the result of anatomic differences • Colonization of the vaginal introitus by gastrointestinal pathogens can also increase the likelihood of urinary tract infiltration • Incidence in men rises dramatically after age 50

Ç. BÜKE UTI Epidemiology • Other factors including; urinary tract obstruction, incomplete voiding, and aberrant structural anatomy also predispose individuals to UTIs • Additional risk factors include; prior history of UTIs, vaginal intercourse within the past 2 weeks, use of contraception with spermicide, low vaginal estrogen levels, and individual genetic background

Ç. BÜKE UTI Epidemiology • Worldwide, 150 million cases / year • 90 % cystitis • 10 % pyelonephritis • 75 % sporadic • 25 % recurrent • 2 % complicated The risk of UTI in women increases after menapause After a UTI 20 – 40% will have a recurrence UTI is rare in young and middleaged men İt often occurs due to catheterisation or urological procedures

Ç. BÜKE UTI Definition • Bacteriuria; Presence of bacteria in the urine • Significant bacteriuria; Presence of bacteria in the urine ≥ 105 cfu/ml for F and 104 cfu/ml for M – Symptomatic bacteriuria – Asymptomatic bacteriuria • Contamination; Presence of bacteriuria in the urine ≤ 105 cfu/ml or 104 cfu/ml
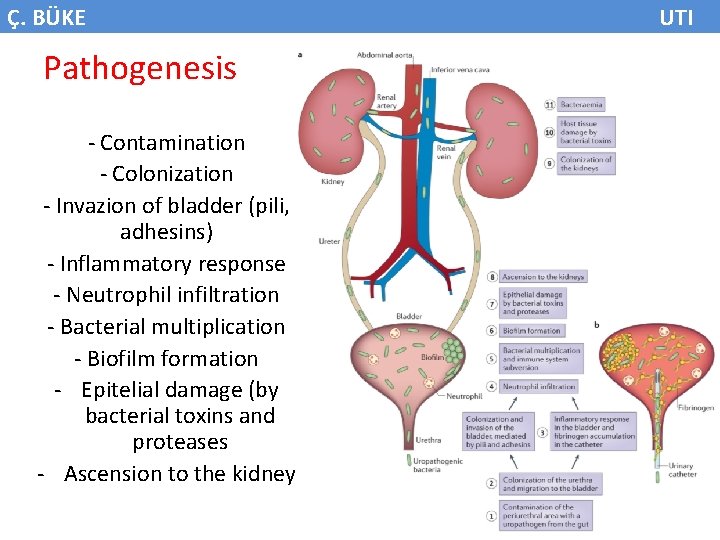
Ç. BÜKE Pathogenesis - Contamination - Colonization - Invazion of bladder (pili, adhesins) - Inflammatory response - Neutrophil infiltration - Bacterial multiplication - Biofilm formation - Epitelial damage (by bacterial toxins and proteases - Ascension to the kidney UTI

Ç. BÜKE UTI Pathogenesis Inoculum size Virulence • Ascending route most common 90% Adherence • Colonization of urethra and peri-urethral tissue is the initial event • More in woman than man due to short female urethra, so urethral organisms enter bladder in close proximity to perianal areas • Once in the bladder, multiply, then pass up the ureters to the renal pelvis and parenchyma • Hematogenous seeding less frequent 10%

Ç. BÜKE Host protective factors in UTIs • Mechanical – Dilution and flow of urine – Length of urethra • Interference – Normal bacteria flora (meatus) • Chemical – Osmolality and p. H of urine – Prostatic fluid • Anti-adherence mechanisms in bladder – Urinary immunoglobulins – Mucosal antibacterial activity UTI

Ç. BÜKE Host factors complicating bacteriuria • Residual bladder urine after voiding • Turbulent urethral flow (stricture) • Foreign bodies • Stones • Atrophic vaginal mucosa • Vesico-ureteral reflux • Sexual intercourse (insertive rectal sex) • Antibiotics • Spermicides UTI

Ç. BÜKE Host factors complicating bacteriuria • Urinary stasis – Neurologic bladder – Reflux into the ureters (pregnancy) – Obstruction • Congenital anatomical abnormalities • Prostate hypertrophy (age) • Stones, tumor • Diabetes mellitus • Foreign materials – Stones – Stents – Catheters UTI

Ç. BÜKE UTI Bacterial virulence factors in UTI • E. coli strains expressing O-antigens cause high proportion of infections • Capsular antigens of E. coli associated with clinical severity (antiphagocytic) • P-fimbriae enhance attachment of E. coli to uroepithelial cells • Motile bacteria ascend the ureter against urine flow

Ç. BÜKE Bacterial virulence factors in UTI • Bacterial urease (Proteus) alkalinizes urine, stone formation and survival of bacteria within stones • Gram (-) endotoxin decreases ureteral peristalsis • Hemolysin damages renal tubular epithelium and promotes invasive infection • Aerobactin of E. coli promote iron accumulation for bacterial replication UTI

Ç. BÜKE Types of urinary tract problems • Asymptomatic bacteriuria • Dysuria • Cystitis – Acute uncomplicated cystitis – Recurrent cystitis • Complicated UTI – Pyelonephritis – UTIs in men, pregnant women, children – Prostatitis • Other – Catheter associated UTI – Candida in urine – Sterile pyuria UTI
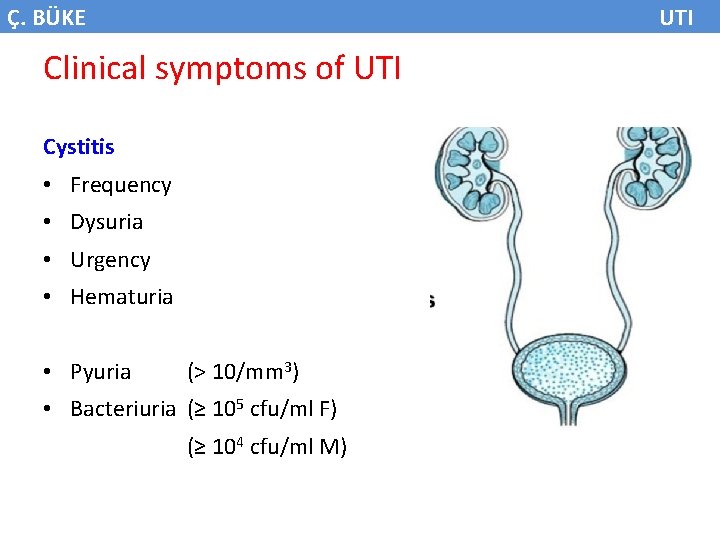
Ç. BÜKE UTI Clinical symptoms of UTI Cystitis • Frequency • Dysuria • Urgency • Hematuria • Pyuria (> 10/mm 3) • Bacteriuria (≥ 105 cfu/ml F) (≥ 104 cfu/ml M)

Ç. BÜKE UTI Cystitis in male • Young men (rare in men under 50) – Anatomic abnormalities – Anal insertive sex, toys • Older men – Calculi – Enlarged prostate (obstruction) – Chronic prostatitis • Organisms differ – E. coli accounts for 40 -50% – Proteus and Providencia species accounting for next most frequent cause • Most common cause of relapsing UTI is chronic bacterial prostatitis
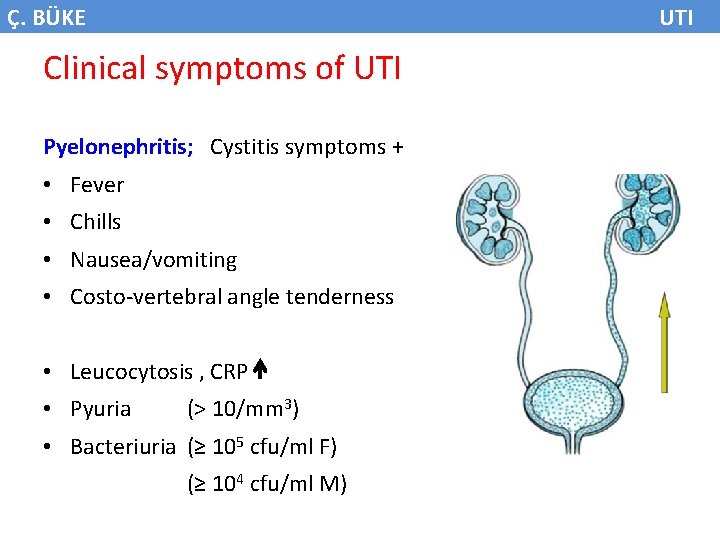
Ç. BÜKE UTI Clinical symptoms of UTI Pyelonephritis; Cystitis symptoms + • Fever • Chills • Nausea/vomiting • Costo-vertebral angle tenderness • Leucocytosis , CRP • Pyuria (> 10/mm 3) • Bacteriuria (≥ 105 cfu/ml F) (≥ 104 cfu/ml M)

Ç. BÜKE Recurrent UTIs • Relapse: same organism in <2 weeks • Suggests uneradicated focus – Ab resistance – Non compliance • Reinfection: may be same or different organism: Interval >2 weeks • Hygiene/wiping • Post-coital • Vaginal atrophy • Post-void residual (prolapse) UTI

Ç. BÜKE UTI Complicated urinary tract infection • May involve the bladder or kidneys • Symptomatic urinary infection in individuals with functional or structural abnormalities of the urinary tract • Child, male, pregnant female • Kidney involvement, 2 nd bacteraemia • Abnormality • Urologic procedure • Catheterization • Unusual or resistant organisms

Ç. BÜKE UTI Etiology • The most common bacterial cause of uncomplicated community-acquired UTI is uropathogenic Escherichia coli (UPEC), representing >80% of infections • Other pathogens commonly associated with uncomplicated UTI include; Staphylococcus saprophyticus, Klebsiella species, Proteus mirabilis, and Enterococcus faecalis •

Ç. BÜKE Diagnosis of UTIs History • Dysuria – Frequency - Urgency – Vaginitis -no pyuria and <102 cfu/ml) • Candida • Trichomonas • atrophy of vaginal tissues – Urethritis –pyuria and • Chlamydia • Neisseria gonorrhoeae – Cystitis – pyuria and >104 -5 cfu/ml, onset abrupt – Pyelonephritis - pyuria and >104 -5 cfu/ml, UTI

Ç. BÜKE UTI Diagnosis of UTIs • Physical examination • Laboratory parameters Urin sample – In adults, mid stream urine sample usually reliably represents the urine in the bladder – The most reliable sample is obtained via suprapubic puncture – Urine in bladder > 4 hours – Samples from urinary bags or bedpans should not be used as they invariably will be contaminated

Ç. BÜKE UTI Diagnosis of UTIs • Urinalysis – Microscopy – Dipstick • Leukocyte esterase: rapid screening test for detecting pyuria – Patients with symptoms and negative LE should have a urine microscopic examination for pyuria • Urinary nitrite – Nitrite is formed when bacteria reduce the nitrate that is normally found in the urine – False negatives common, but false positives are rare

Ç. BÜKE Diagnosis of UTIs • Quantitative culture • Specialized cultures (TB, fungi) UTI
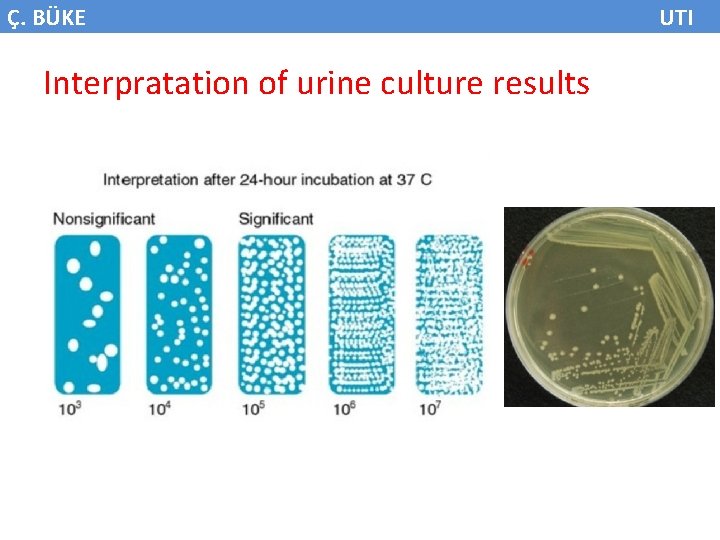
Ç. BÜKE Interpratation of urine culture results UTI

Ç. BÜKE Asemptomatic bacteriuria • Positive urine culture repeatedly (105 cfu/ml) in the absence of signs of UTIs • Pyuria does not affect interpretation • Tretment of asemptomatic bacteriuria only in – Pregnant women – Prior to urological invasive procedures • Prevalance varies 1 -5% to 100% • Screening for and treatment of asymptomatic bacteriuria is not indicated • Treatment does not prevent further episodes of asemptomatic bacteriuria UTI

Ç. BÜKE Asemptomatic bacteriuria • The risk of pyelonephritis is increased 20 -30 fold during pregnancy • Increased risk for premature delivery and to have low birthweight infants • Treatment of bacteriuria decreases the risks • Screen for bacteriuria by urine culture at least once in early pregnancy and treat for 3 -7 days if positive UTI

Ç. BÜKE UTI Asemptomatic bacteriuria • In patients with urinary catheter, antimicrobial therapy not associated with decrease in rate of symptomatic infection • High incidence of recurrence, usually with more resistant organisms • Asymptomatic bacteriuria or funguria should not be screened for or treated in patients with indwelling urethral catheter

Ç. BÜKE UTI Treatment of UTIs Acute uncomplicated UTIs (Cystitis) • TMP-SMX (160/800 mg tablet twice daily for 3 days) – > 20% resistance to TMP-SMX • Nitrofurantoin monohydrate/macrocrystals (100 mg twice daily for 5 days); – 1 -20% resistance to nitrofurantoin • Fosfomycin trometamol (3 g powder single dose • Amoxicillin (500 mg three times a day) – 30% resistance to amoxicillin • Fluoroquinolones (ciprofloxacin 500 mg twice daily) are highly effective in 3 -day regimens

Ç. BÜKE UTI Treatment of UTIs Acute pyelonephritis • Mild to moderately ill patients – Amox/clav 1 g twice daily – Cefuroxime 500 mg three times a day – Fluoroquinolone: ciprofloxacin, levofloxacin 500 mg once a day – TMP-SMX – Patients usually improve in 48 -72 hours – Treat for 1 -2 weeks

Ç. BÜKE Treatment of UTIs Acute pyelonephritis • Severely ill patients – Ceftriaxon 1 g twice daily – Floroquinolon – Ampicillin + aminoglycoside – IV therapy until patient afebrile for 48 -72 hours – Treat for 2 weeks • If fever persists and all children and men: – Renal US, CT or MR ± IVP • Look for perinephric abscess • Exclude urinary obstruction UTI

Ç. BÜKE Treatment of UTIs in pregnancy • Ampicillin 500 mg three times a day for 7 -10 days • Amok/klav 1 g twice daily for 7 - 10 days • Sefaleksin 250 mg BID-QID for 7 - 10 days • Nitrofurantoin 50 -100 mg QID for 7 - 10 days UTI

Ç. BÜKE UTI Urethritis • Neisseria gonorrhoeae • Chlamydia • Ureoplasma • Antibiotic therapy should cover both gonococcal urethritis and nongonococcal urethritis (NGU) • If concomitant treatment for NGU is not provided, the risk of postgonococcal urethritis is approximately 50%.

Ç. BÜKE Urethritis • For uncomplicated gonococcal urethritis; – Ceftriaxone, 250 mg IM single dose • For treatment of NGU; – Azithromycin, 1 g orally in a single dose, or – Doxycycline, 100 mg orally twice a day for 7 days Alternatives; – Erythromycin base 500 mg orally four times a day for 7 days – Levofloxacin 500 mg orally once daily for 7 days UTI

Ç. BÜKE UTI Prostatitis • Fever, chills • Dysuria, pain • Marked local tenderness • Excellent penetration by most antibiotic classes-easily cured • Ciprofloxacin • Levofloxacin • TMP-SMX 500 mg twice daily for 6 -8 weeks 500 mg once a day for 6 -8 weeks 160/800 mg twice a day for 6 -8 weeks

Ç. BÜKE Urinary tuberculosis • Hematogenous seeding can occur in cortex and forms granuloma • Seeding in the medulla • In both sites – Granulomas form – Erosion into collecting system – Further spread to ureters, bladder, prostate… • Requires high index of suspicion – Clinical disease insidious • Dysuria, renal functional defects • Key finding is sterile pyuria – PPD skin testing UTI
- Slides: 37