Urinary Tract Infection Dr Shreedhar Paudel Urinary Tract





























- Slides: 31

Urinary Tract Infection Dr. Shreedhar Paudel

Urinary Tract Infection… • Incidence equal in girls and boys till infancy • Incidence in girls increases afterwards • Organisms: – Escherichia coli ( predominant periurethral flora) – Klebsiella – Proteus – Pseudomonas – enterococcus

Urinary Tract Infection… • Risk factors: – Female – Neurogenic bladder* – Vesicoureteral reflux * – Obstructive uropathy* – Urethral instrumentation – Wiping from back to front – Pinworm infestation – Voiding dysfunction * (30 -40 % of UTI in children)

Urinary Tract Infection… • Clinical features: – Neonates → features of sepsis with fever, vomiting diarrhea, poor weight gain and lethargy – Older infants → unexplained fever, frequent micturition – Distal UTI → dysuria, hypogastric pain, frequency and urgency of micturition

Urinary Tract Infection… • Clinical features: – Pyelonephritis → flank pain, fever with chills and rigors – Excessive crying or straining during voiding, dribbling, weak stream, palpable bladder → urinary obstruction

Urinary Tract Infection… • Diagnosis: – Urine routine → more than 10 WBC/cu. Mm in uncentrifuged sample – Urine culture → comfirms ** urine obtained by suprapubic bladder aspiration or urethral catheterization in children < 2 yrs **clean catch sample in older children

Urinary Tract Infection… • Emperical therapy with antibiotics (ASAP) – Trimethoprim- sulfamethoxazole (4 mg TMP/ day) – Nitrofurantoin (5– 7 mg/kg/24 hr in three to four divided doses) – Amoxicillin (50 mg/kg/24 hr) – Modified if required once culture reports available – Treatment required for 7 -10 days • Large amount of fluids and frequent emptying of bladder to prevent stasis • A repeat urine culture -----1 wk after the termination of treatment of any UTI • 1– 2 yr FOLLOW UP EVEN IF THE URINE IS STERILE

Vesicoureteral Reflux(VUR) • Retrograde flow of urine from the bladder to the upper urinary tract • Rise in intravesical pressure occuring during micturition is freely transmitted to ureter, renal pelvis, papillary collecting ducts and renal tubules • Pathogenic organism gain access to renal parenchyma → renal inflammation and scarring (Reflux nephropathy)

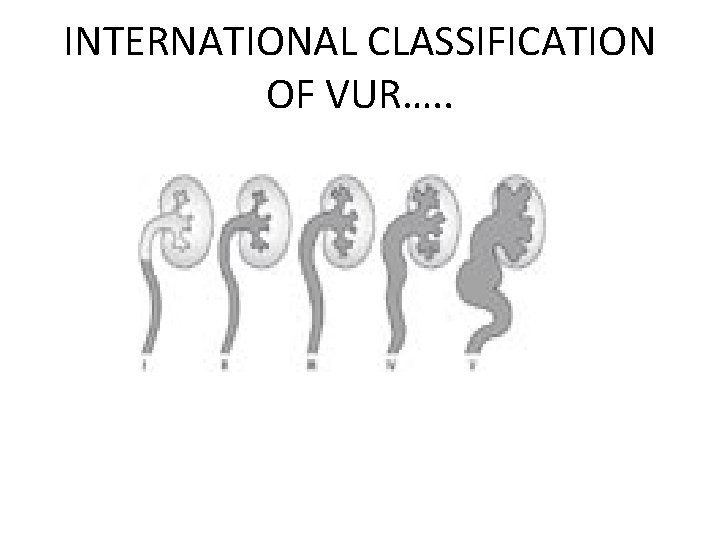
INTERNATIONAL CLASSIFICATION OF VUR • Grade I – reflux into non-dilated ureter • Grade II – reflux into the renal pelvis and calyces without dilatation • Grade III – mild/moderate dilatation of the ureter, renal pelvis and calyces with minimal blunting of the fornices • Grade IV – dilation of the renal pelvis and calyces with moderate ureteral tortuosity • Grade V – gross dilatation of the ureter, pelvis and calyces; ureteral tortuosity; loss of papillary impressions

INTERNATIONAL CLASSIFICATION OF VUR…. .

Vesicoureteral Reflux(VUR)… • Treatment: – A) Medical therapy: • Continuous antibiotic prophylaxis • Cotrimoxazole/ Nitrofurantoin a single bedtime dose • Breakthrough infections during prophylaxis are treated with appropriate antibiotics – B) Surgical correction: indicated in • • Severe (grade 4 or 5) reflux persisting beyond 2 yrs of age Non compliance or intolerance to drugs Deterioration of renal functions/ new renal scars Multiple recurrent UTI despite prophylaxis

Vesicoureteral Reflux(VUR)… • Treatment: – General measures: • Liberal fluid intake • Regular and complete bladder emptying • Constipation should be avoided

Vesicoureteral Reflux(VUR)… • LONGTERM ANTIBIOTICS PROPHYLAXIS indications: • < 3 yrs child who have received treatment for the first UTI and being investigated for underlying etiology • >3 UTI episode in a yr in a child with normal urinary tract and no VUR– prophylaxis continued for at least 6 mo after free of UTI • UTI with VUR--- prophylaxis till the child is free from reflux for 6 months

ARF • Life threatening situation with abrupt impairment of renal function resulting in ---retention of nitrogeneous wastes -- inappropriate regulation of fluid and electrolyte homeostatis • Oliguria ( urine flow less than 1 ml/kg/hr)– prominent feature

ARF • Causes: – Prerenal– hypoperfusion – Intrinsic/ renal – Post renal – mechanical obstruction in collecting system • Diagnostic approach: – Important task is to differentiate between prerenal and intrinsic renal failure

ARF • Diagnostic approach: – Pre-renal → intact renal tubular function so urine is highly concentrated with low sodium – Intrinsic → impaired tubular function leads to increased sodium excretion and failure to concentrate urine

ARF • Clinical features: – Anuria or severe oliguria • Investigations: – CBC – Serum urea, creatinine, electrolytes – EKG – to examine for evidence of hyperkalemia

ARF • Management: – Fluid and electrolytes • Fluid therapy guided by intake and output analysis, weight and serum sodium – Diet • Adequate nutritional support (as patients with ARF have increased metabolic needs – Treatment of complications • Early detection and management

ARF • Treatment of complications: • Fluid overload – Pulmonary edema and CHF should be treated with diuretics • Metabolic acidosis – Treated with sodium bicarbonate • HTN – Treated with antihypertensive drugs • Hyponatremia – Fluid restricition ( as hyponatremia is due to excessive fluid rather than salt loss)

ARF • Treatment of complications: • Hyperkalemia →Serious emergency -- its cardiotoxicity can cause sudden death – Calcium antagonizes the cardiotoxicity of hyperkalemia – Calcium gluconate IV (0. 5 -1 ml/kg of 10% calcium gluconate over 10 minutes) – Sodium bicarbonate -- increases the potassium uptake by the cells – Nebulised Salbutamol – IV Glucose with insulin – facilitates intracellular uptake of potassium – Calcium resonium – binds with potassium – Dialysis

ARF • Supportive care – Managed under intensive care – Daily intake and output chart maintainence – Prompt detection and treatment of infections • Dialysis – To remove endogeneous and exogenous toxin, maintain fluid, electrolyte and acid base balance until renal function recovers

CRF • Permanent severe decrease in renal function • End stage renal disease (ESRD) → decline of renal function to a degree when life can not be sustained without chronic dialyses or transplantation

CRF • Causes: – Glomerulonephritis – Reflux nephropathy – Obstructive uropathy – Developmental anomalies– renal hypoplasia, dysplasia – Others – amyloidosis, renal vein thrombosis, renal cortical necrosis

CRF • Management: – Diet – adequate calorie – HTN – be treated with B- blockers, CCB – Anemia – recombinant human erythropoietin – Infections – early detection and treatment

CRF • • RENAL REPALCEMENT THERAPY CHRONIC PERITONEAL DIALYSIS CHRONIC HEMODIALYSIS RENAL TRANSPLANTATION

Hemolytic-Uremic Syndrome (HUS) • • microangiopathic hemolytic anemia thrombocytopenia Uremia thrombotic thrombocytopenic purpura

HUS… • Etiology : • Diarrhea --Shiga toxin–producing Escherichia coli 0157: H 7 – D+ HUS • verotoxin • Shigella, Salmonella, Campylobacter, Streptococcus pneumoniae, Bartonella • viral (coxsackievirus, echovirus, influenza, varicella, HIV, Epstein-Barr) infections. • oral contraceptives, mitomycin, cyclosporine

HUS…. • Clinical Manifestations: – children younger than age 4 yr – onset usually preceded by a gastroenteritis characterized by fever, vomiting, abdominal pain, and diarrhea that is often bloody – Less commonly, patients may present after an upper respiratory tract infection.

HUS • Clinical Manifestations: – Sudden onset of pallor, irritability, weakness, lethargy, and oliguria usually occurs 5– 10 days after the initial gastrointestinal or respiratory illness – Physical examination may reveal dehydration, edema, petechiae, hepatosplenomegaly, and marked irritability

HUS • Investigations: – Blood film – broken and distorted red cells – Thrombocytopenia – Urine – microscopic hematuria, mild proteinuria – Serum urea and creatinine elevated

HUS • Treatment: – Is supportive – Proper nutriton – Plasmapheresis and infusion of FFP in some patients – Management of • • ARF HTN Dyselectrolytemia Correction of anemia