Male Reproductive System Organs of Male Reproduction Gonads














































- Slides: 122

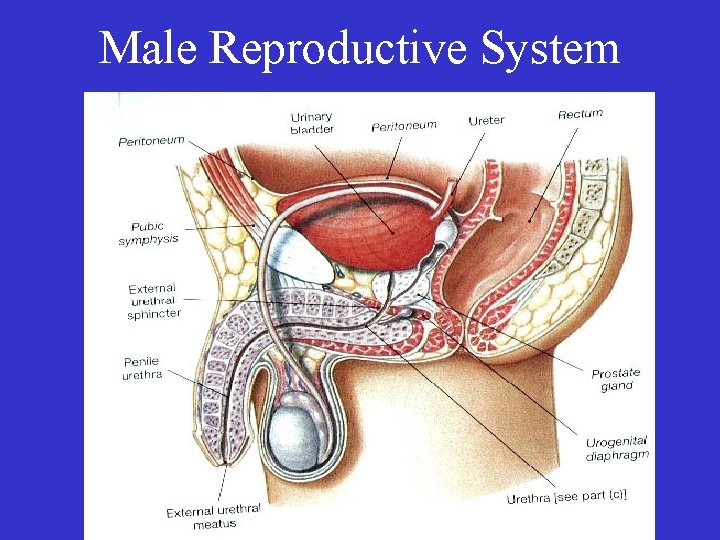
Male Reproductive System

• Organs of Male Reproduction – Gonads (Testes) • produce gametes (sperm) • secrete the sex steroid hormones

• Organs of Male Reproduction – Ducts (reproductive tract) • Store Sperm • Transport sperm

• Organs of Male Reproduction – Accessory Organs • Secrete substances that support sperm

• Organs of Male Reproduction –External genitalia • Penis • scrotum

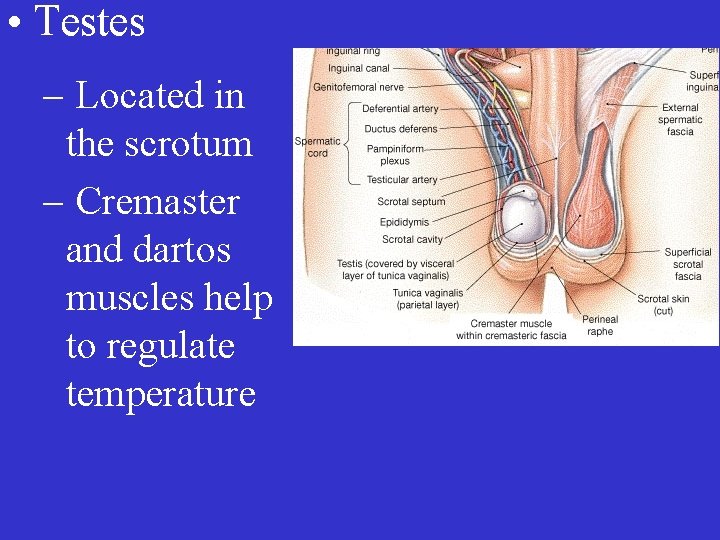
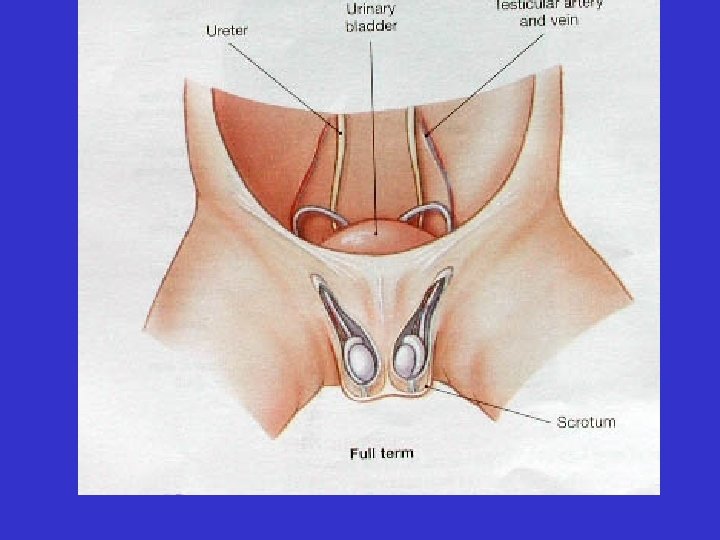
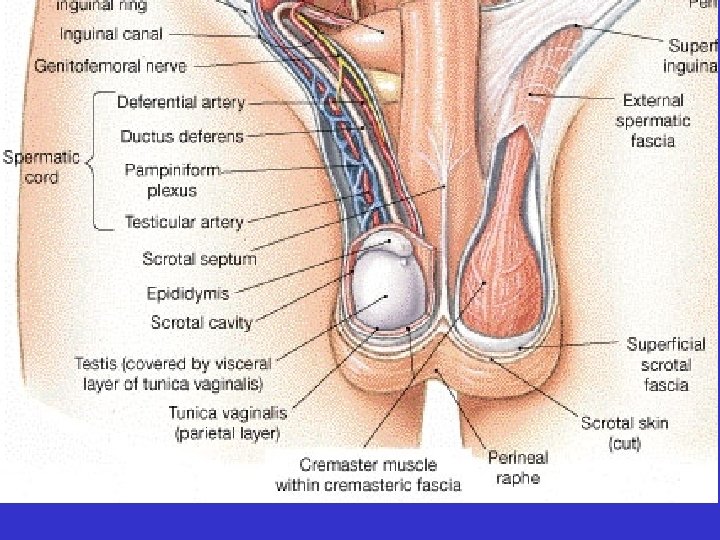
• Testes – Located in the scrotum – Cremaster and dartos muscles help to regulate temperature

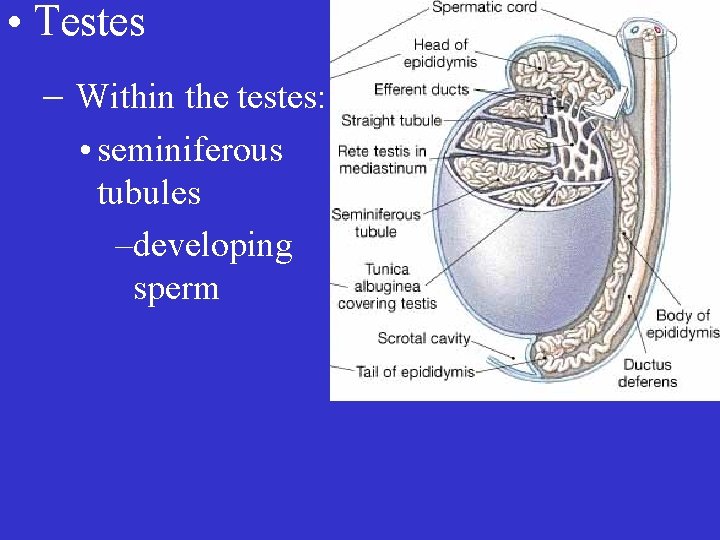
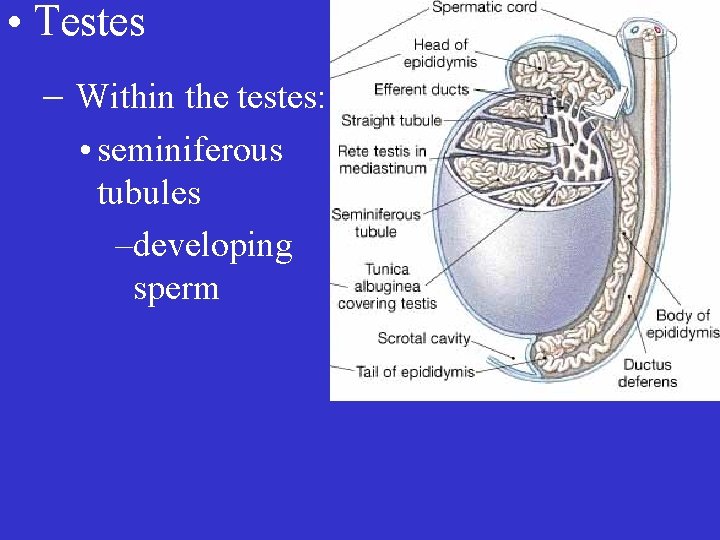
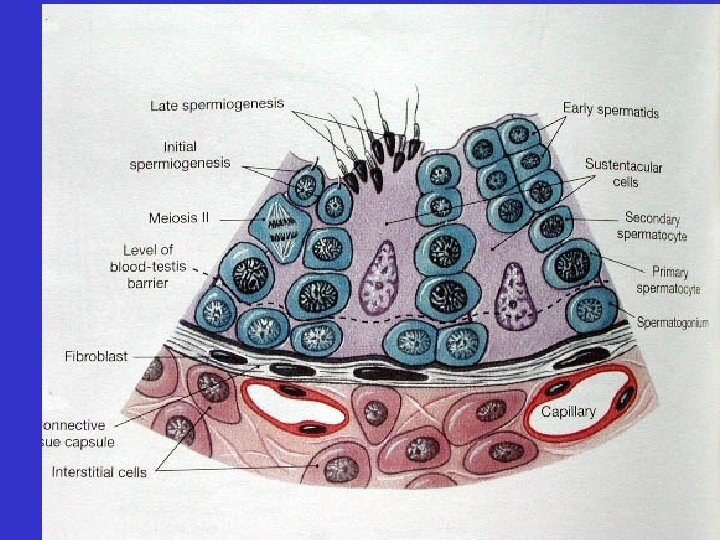
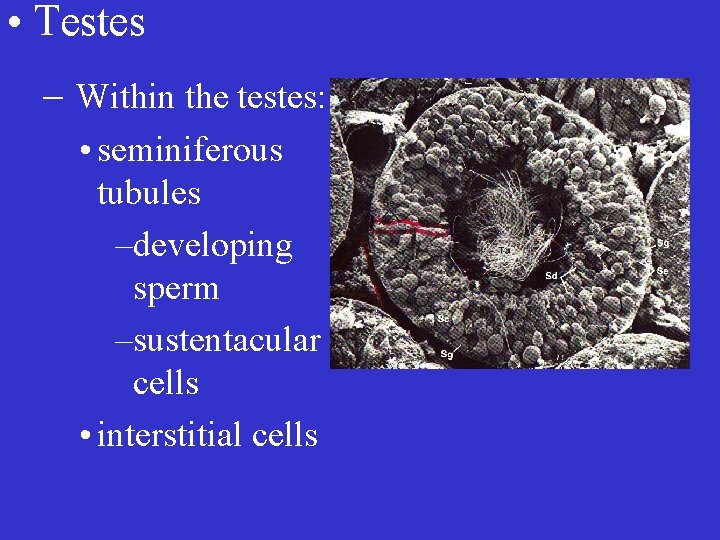
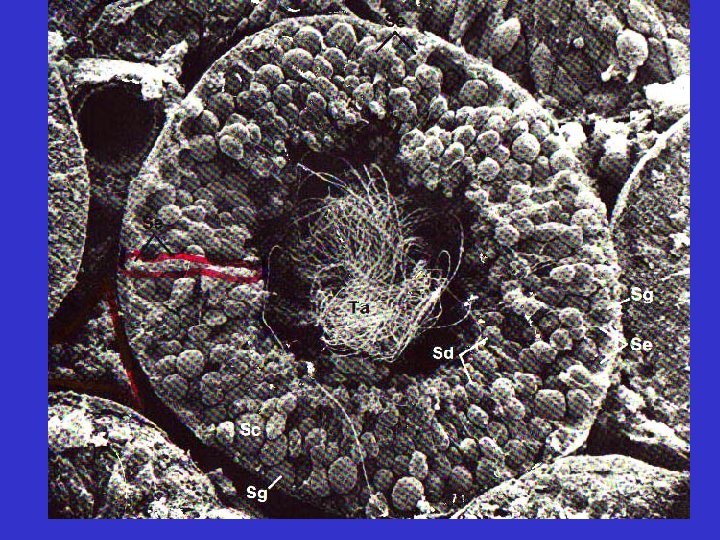
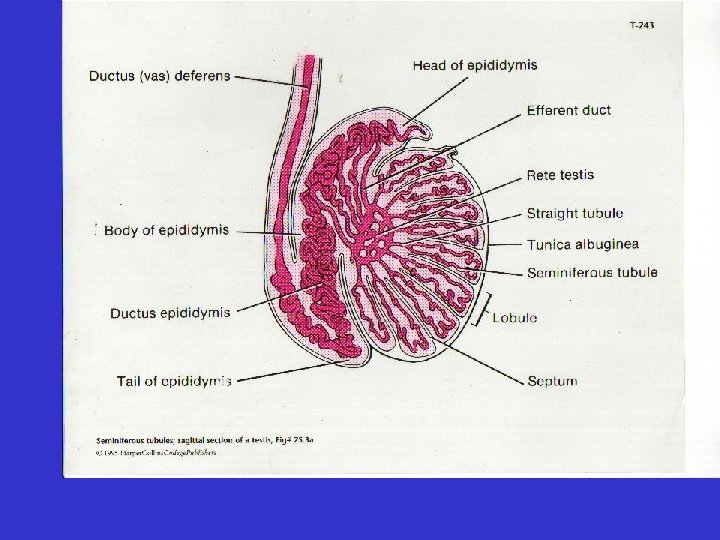
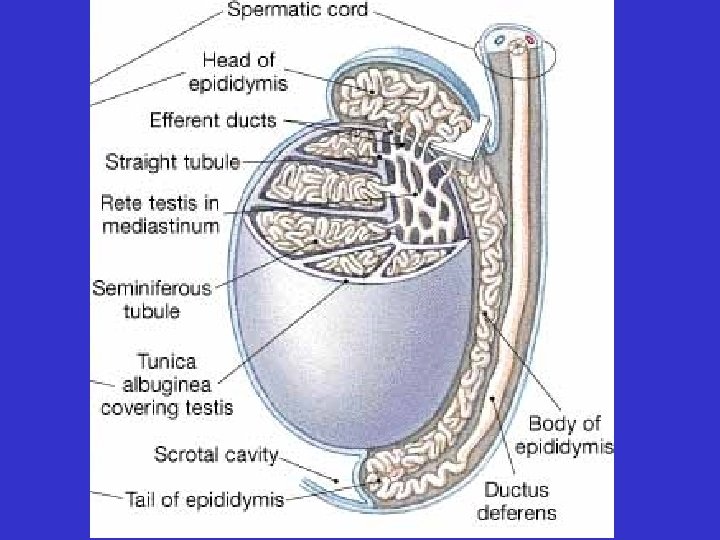
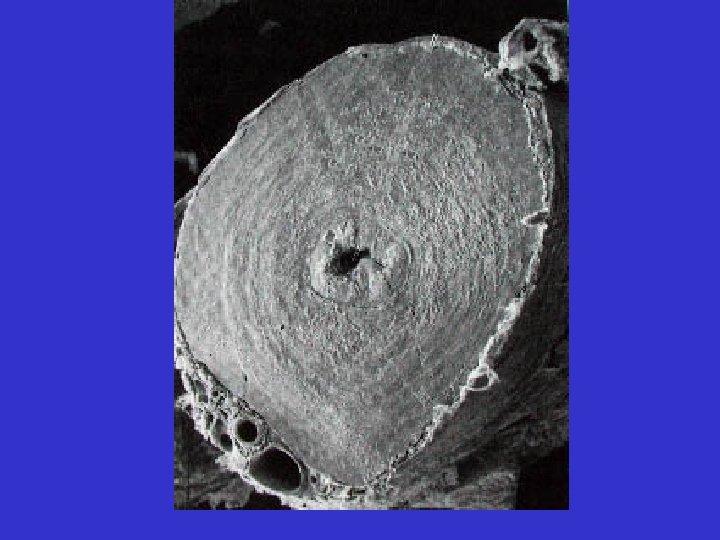
• Testes – Within the testes: • seminiferous tubules –developing sperm

• Testes – Within the testes: • seminiferous tubules –developing sperm

• Testes – Within the testes: • seminiferous tubules –developing sperm

• Testes – Within the testes: • seminiferous tubules –developing sperm –sustentacular cells


• Testes – Within the testes: • seminiferous tubules –developing sperm –sustentacular cells

• Testes – Within the testes: • seminiferous tubules –developing sperm –sustentacular cells • interstitial cells


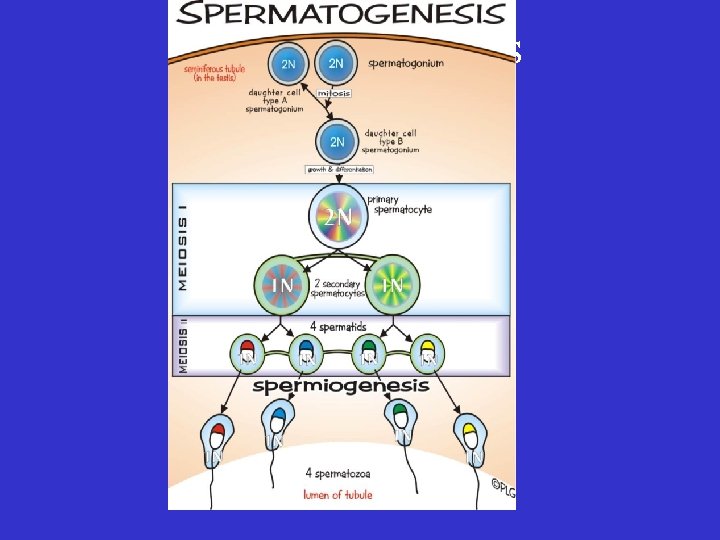
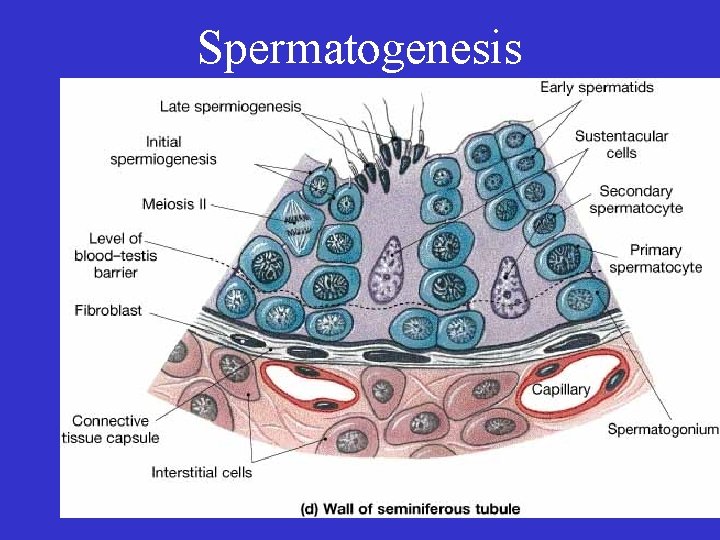
Spermatogenesis

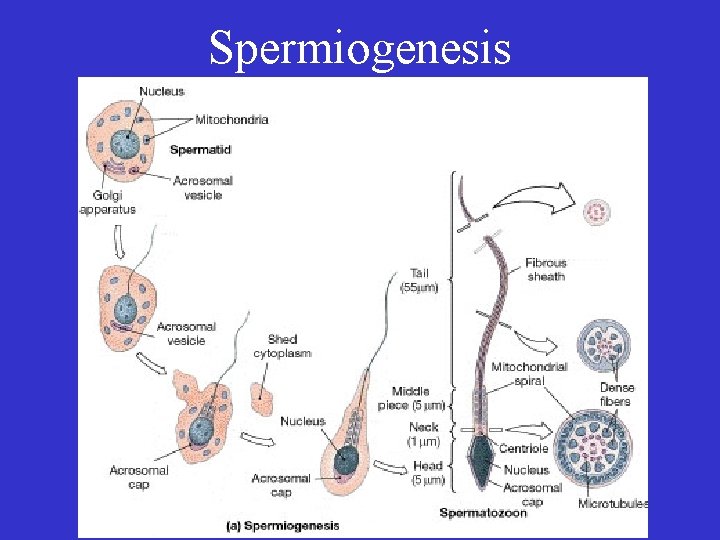
Spermiogenesis

Spermatogenesis



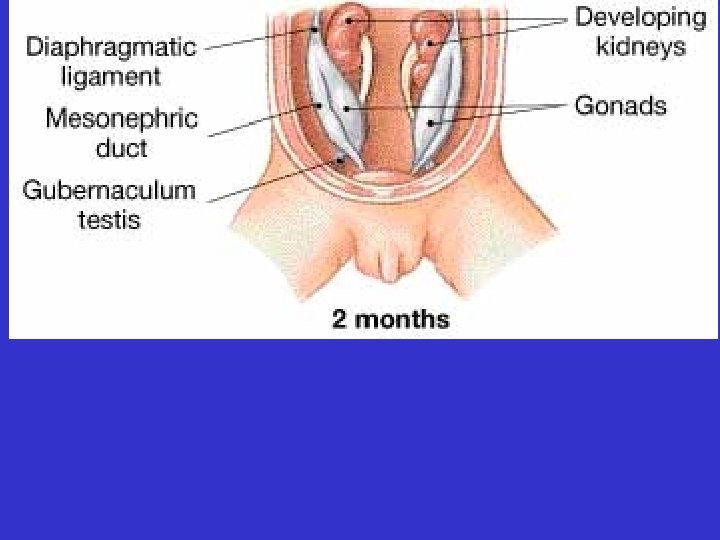
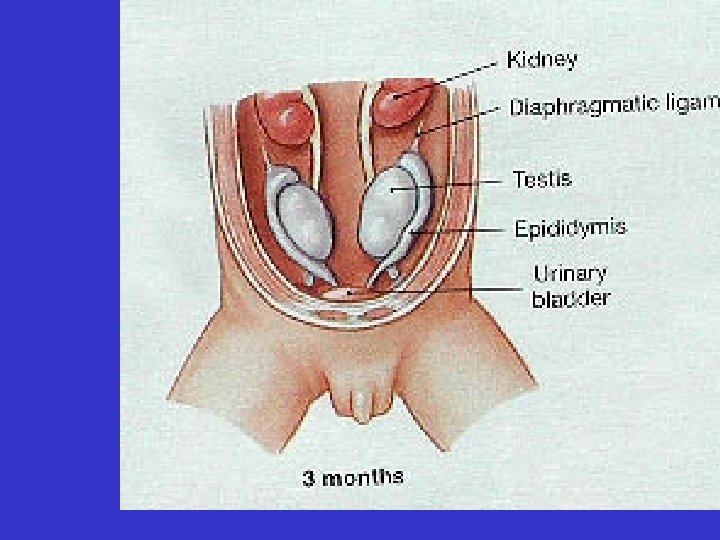
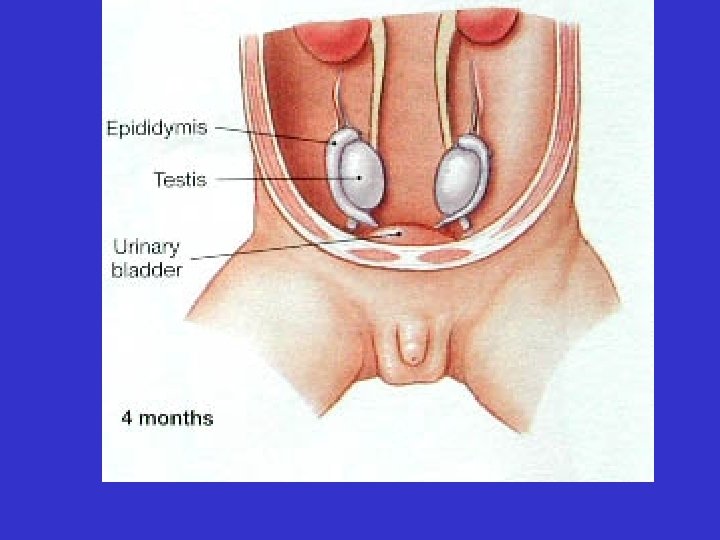
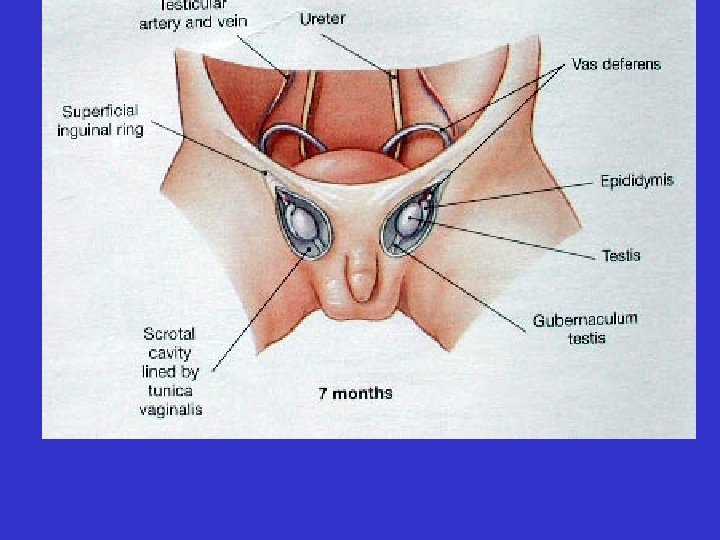
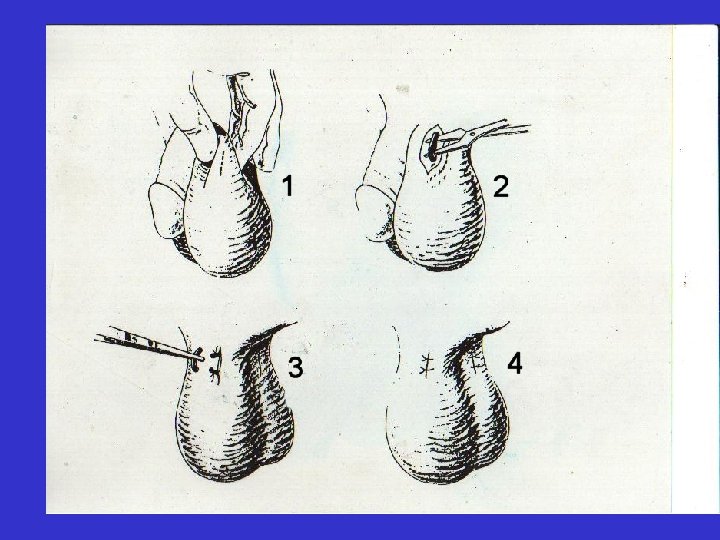
• The testes descend from the abdomen during fetal development






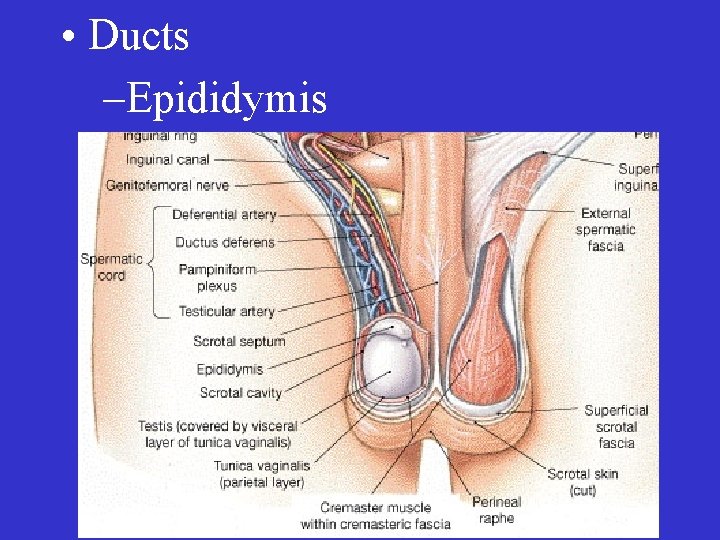
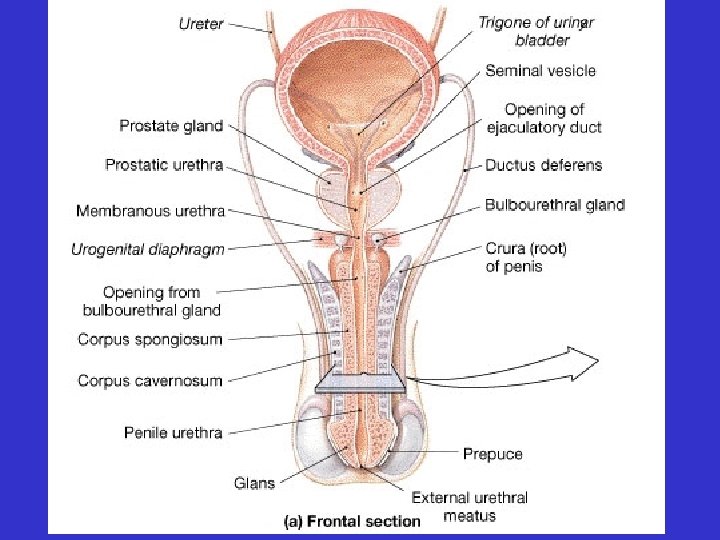
• Ducts

• Ducts –Epididymis


• Ducts –Epididymis

• Ducts –Epididymis – Vas deferens











• Ducts –Epididymis – Vas deferens

• Ducts –Epididymis – Vas deferens – Ejaculatory duct


• Ducts –Epididymis – Vas deferens – Ejaculatory duct

• Ducts –Epididymis – Vas deferens – Ejaculatory duct – Urethra


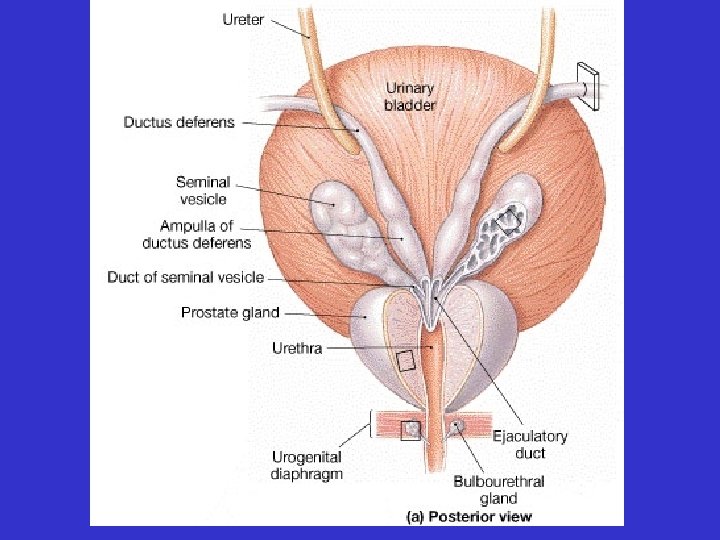
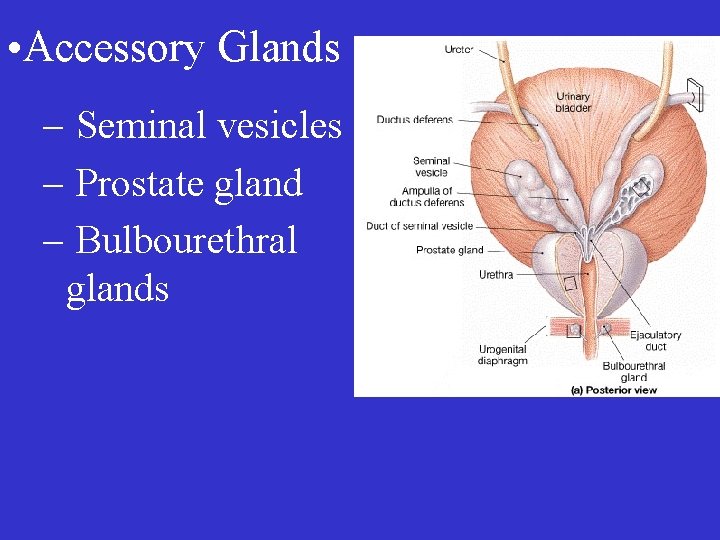
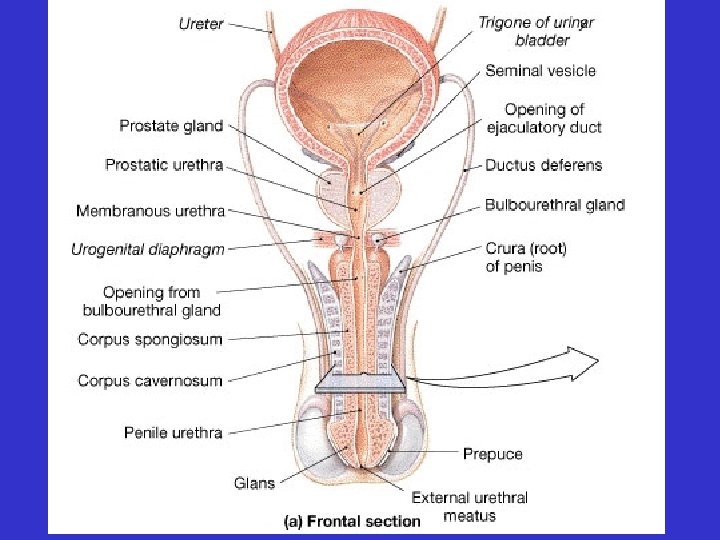
• Accessory Glands – Seminal vesicles – Prostate gland – Bulbourethral glands

• Semen

• Semen – sperm plus seminal fluid

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml – includes prostaglandins,

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml – includes prostaglandins, bicarbonate,

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml – includes prostaglandins, bicarbonate, fructose,

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml – includes prostaglandins, bicarbonate, fructose, antibiotics,

• Semen – sperm plus seminal fluid – 20 -150 million sperm/ml – includes prostaglandins, bicarbonate, fructose, antibiotics, & enzymes that activate sperm

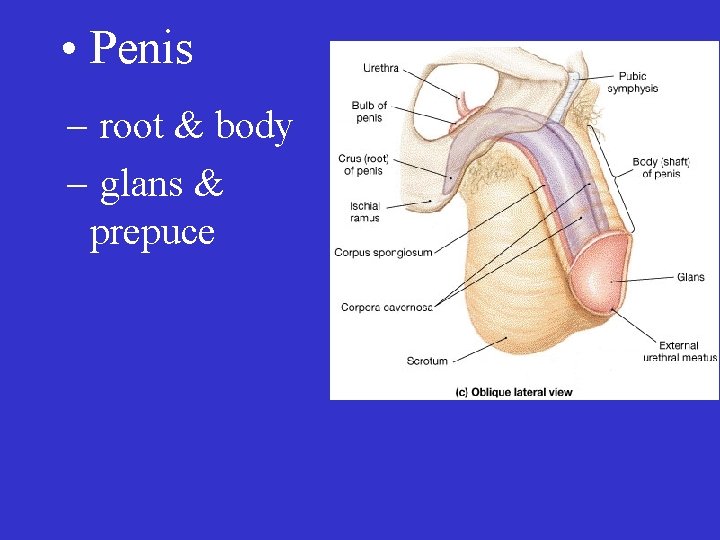
• Penis – root & body – glans & prepuce

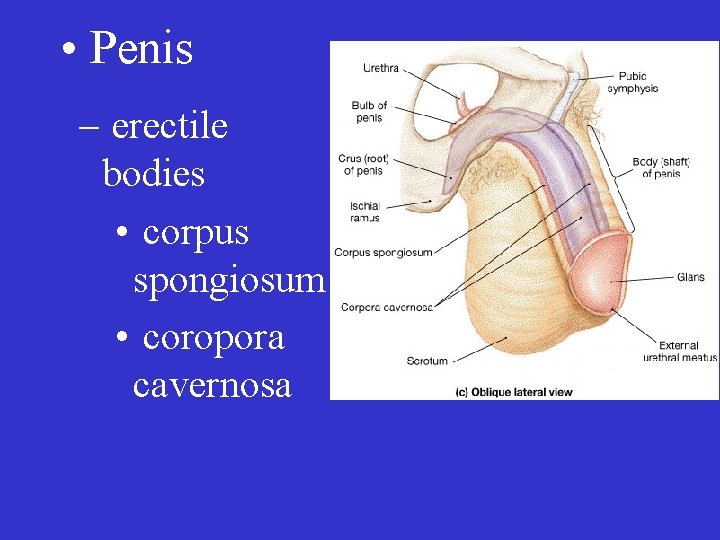
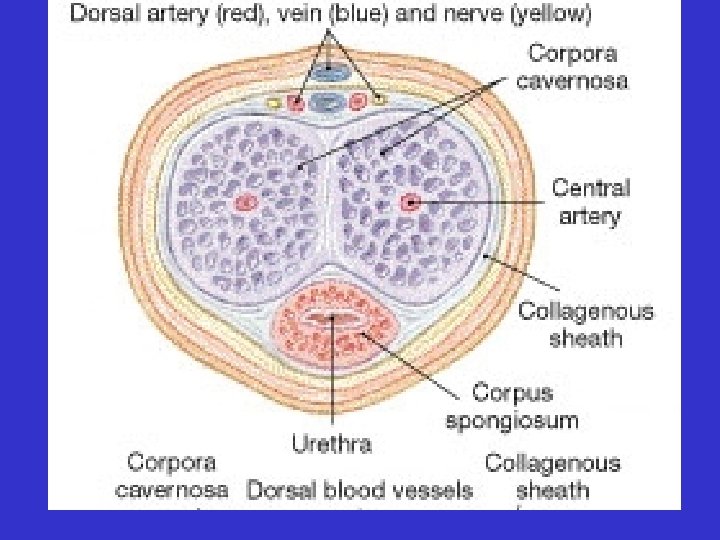
• Penis – erectile bodies • corpus spongiosum • coropora cavernosa

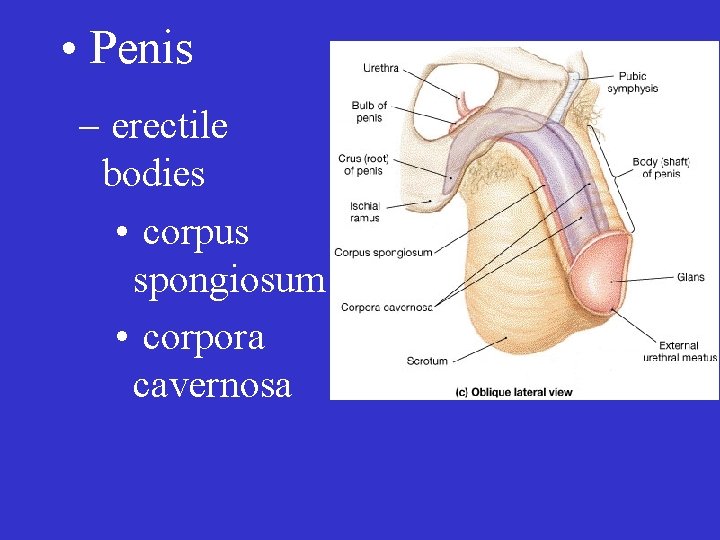
• Penis – erectile bodies • corpus spongiosum • corpora cavernosa



• Penis –erections under the control of parasympathetic stimulation – ejaculation: sympathetic

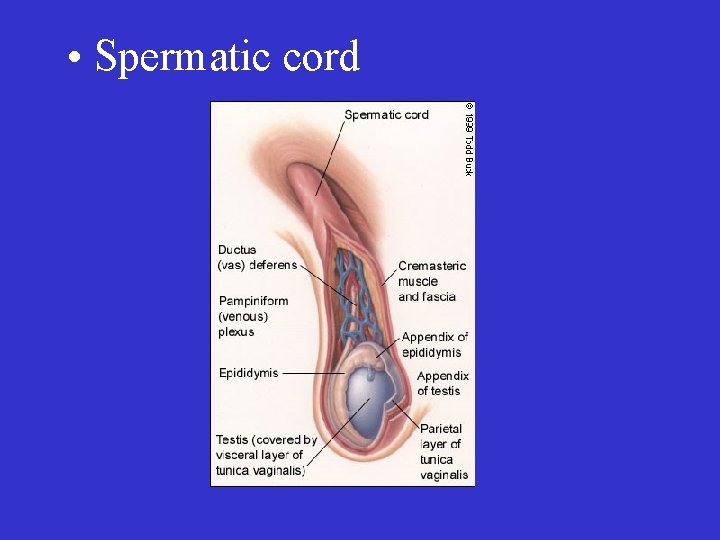
• Spermatic cord

Hormone Control of Male Reproduction Gonadotropin releasing hormone FSH & LH (ICSH) Sperm production Testosterone release

• Other Functions of Testosterone – development, growth, & maintenance of male sex organs – bone and muscle growth – 2 o sex characteristics – aggression? – libido

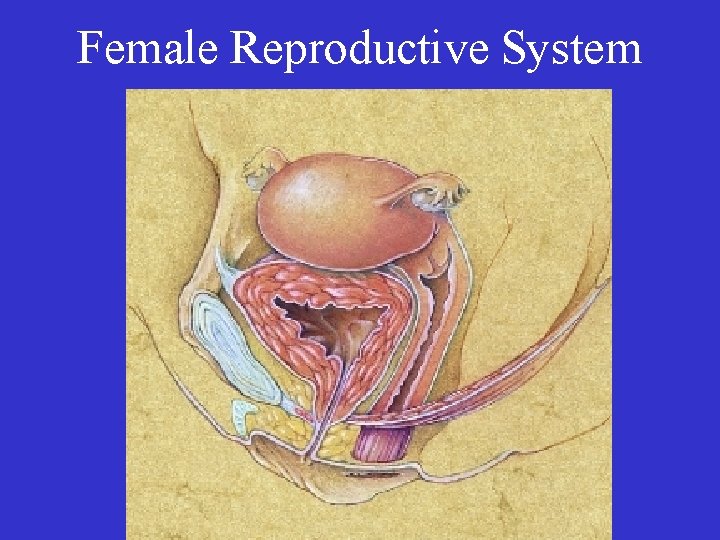
Female Reproductive System

• Organs of Female Reproduction – Gonads (Ovaries)

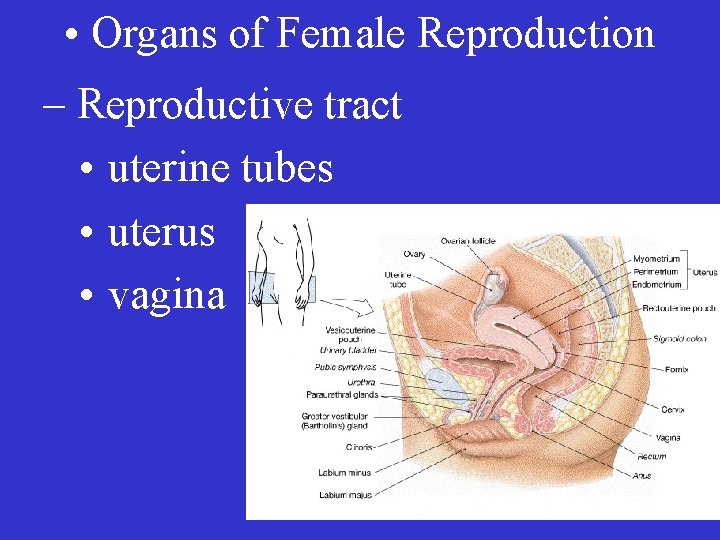
• Organs of Female Reproduction – Reproductive tract • uterine tubes • uterus • vagina

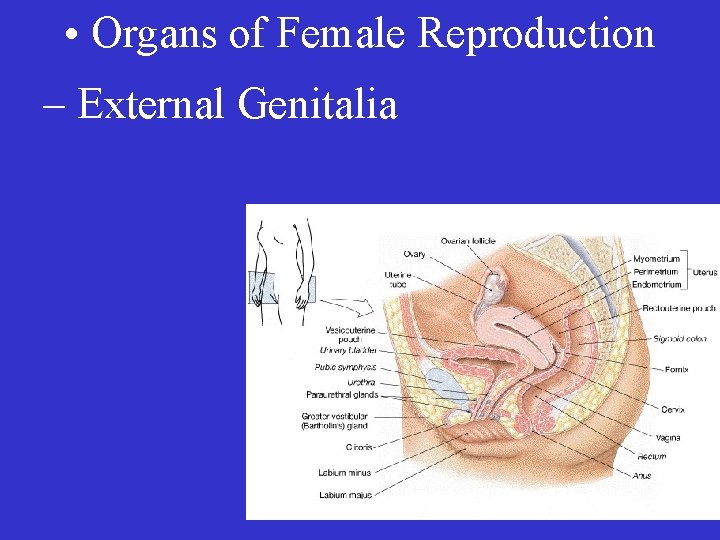
• Organs of Female Reproduction – External Genitalia

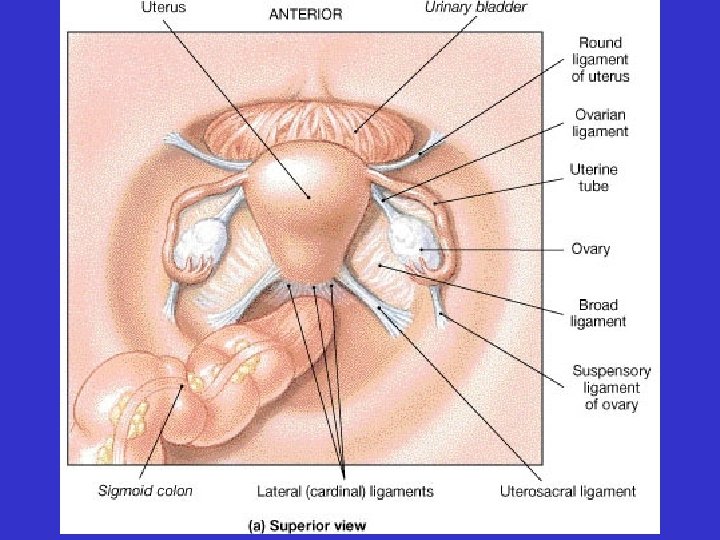
• Ovaries –Held in place by ligaments • ovarian ligaments • suspensory ligaments

• Ovaries – Produce gametes (ova) – Secrete the sex steroid hormones


• Ovaries – Contain thousands of follicles – Each follicle contains one ovum


• Ovaries – each month one follicle matures – at ovulation: a mature follicle releases an ovum

• Ovaries – hormones secreted include • estrogens • progestins (progesterone)

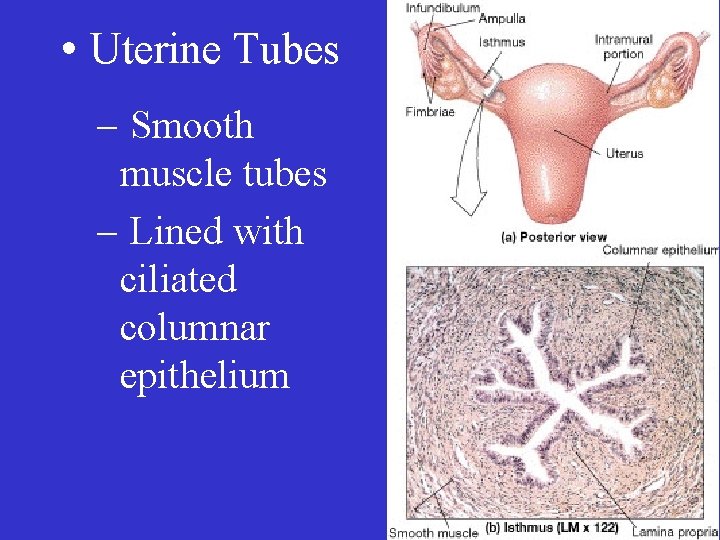
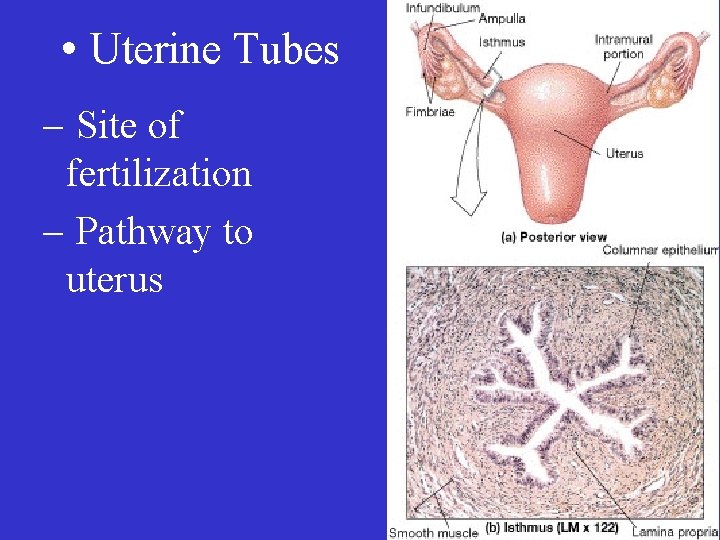
• Uterine Tubes – Smooth muscle tubes – Lined with ciliated columnar epithelium

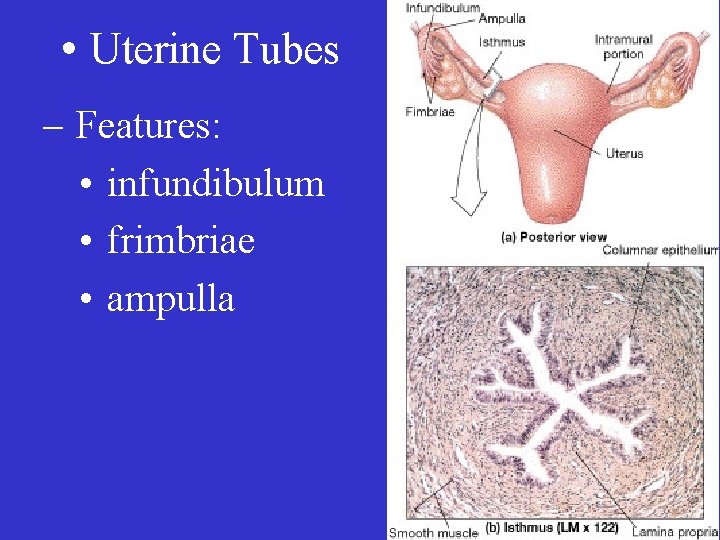
• Uterine Tubes – Features: • infundibulum • frimbriae • ampulla

• Uterine Tubes – Site of fertilization – Pathway to uterus

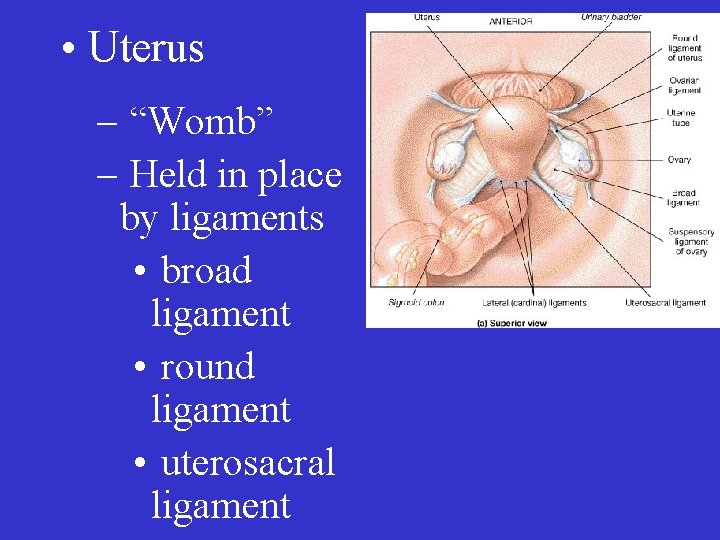
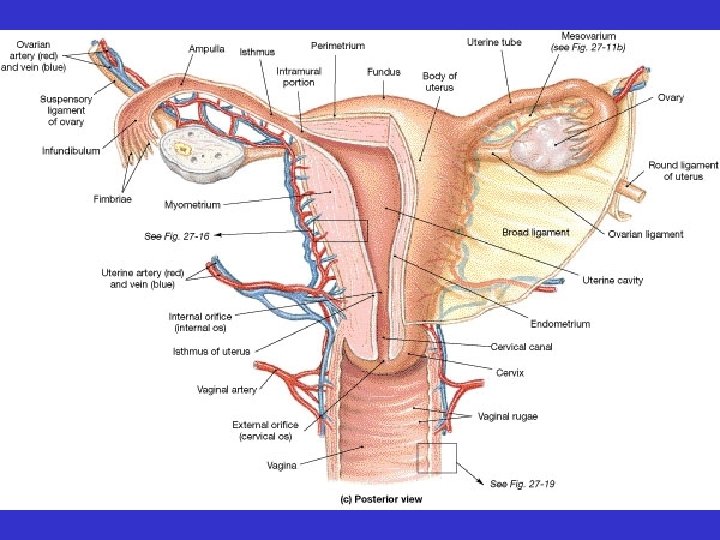
• Uterus – “Womb” – Held in place by ligaments • broad ligament • round ligament • uterosacral ligament

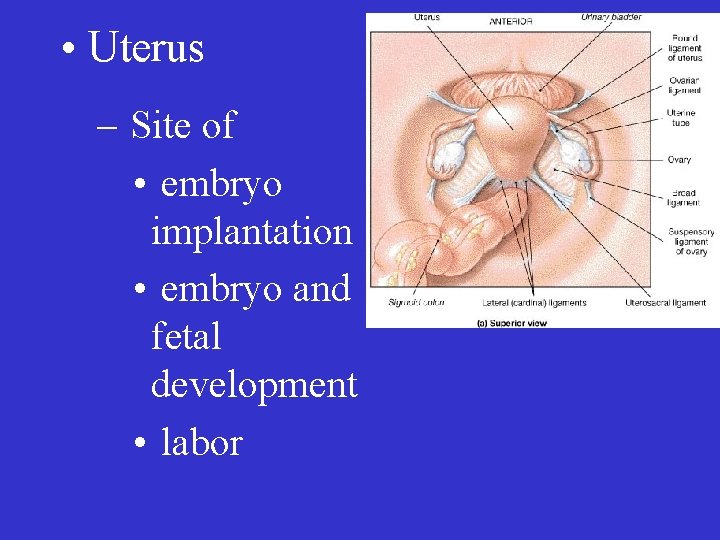
• Uterus – Site of • embryo implantation • embryo and fetal development • labor

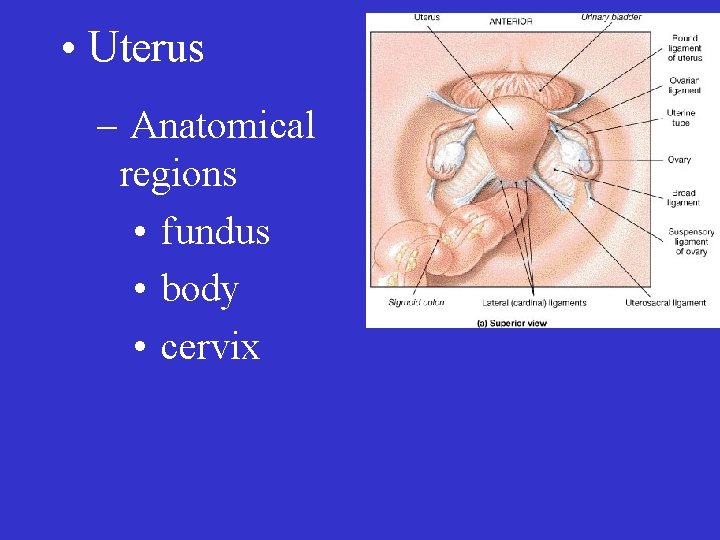
• Uterus – Anatomical regions • fundus • body • cervix


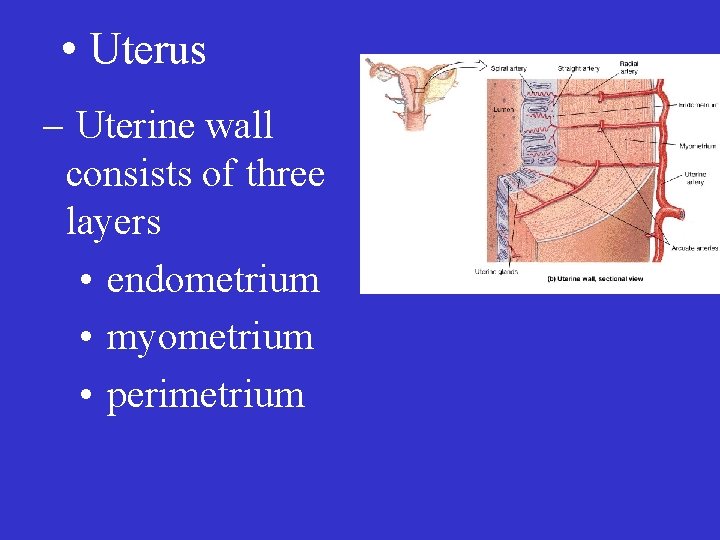
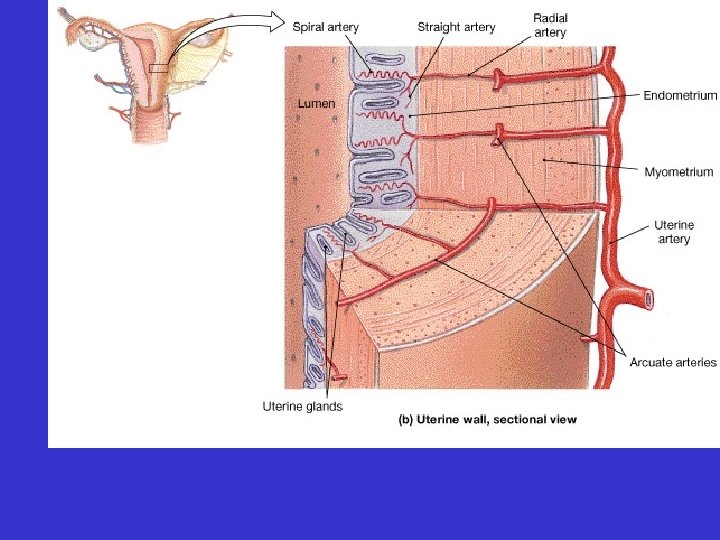
• Uterus – Uterine wall consists of three layers • endometrium • myometrium • perimetrium


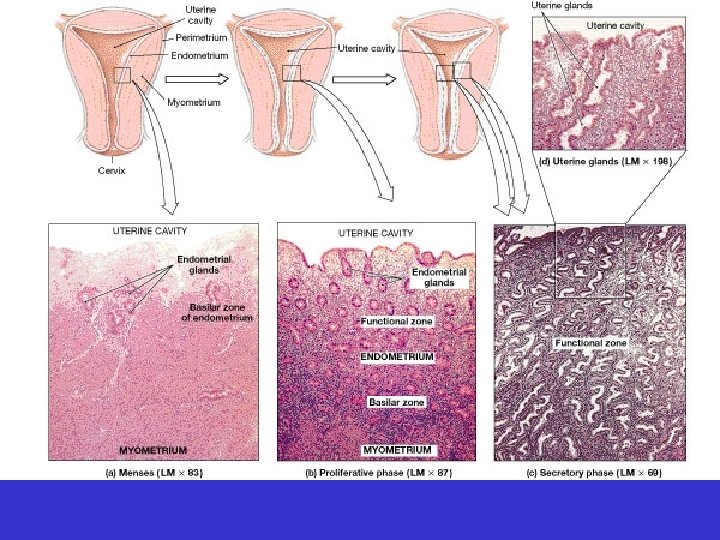
• Uterus – Endometrium divided into • functional zone • basilar zone


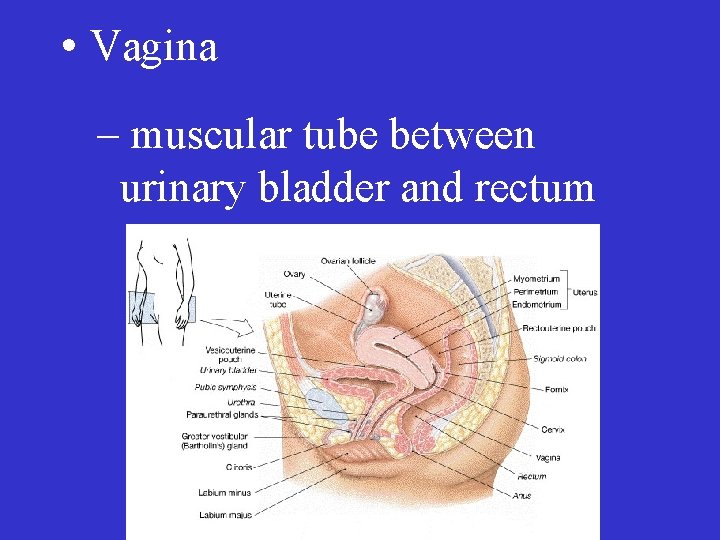
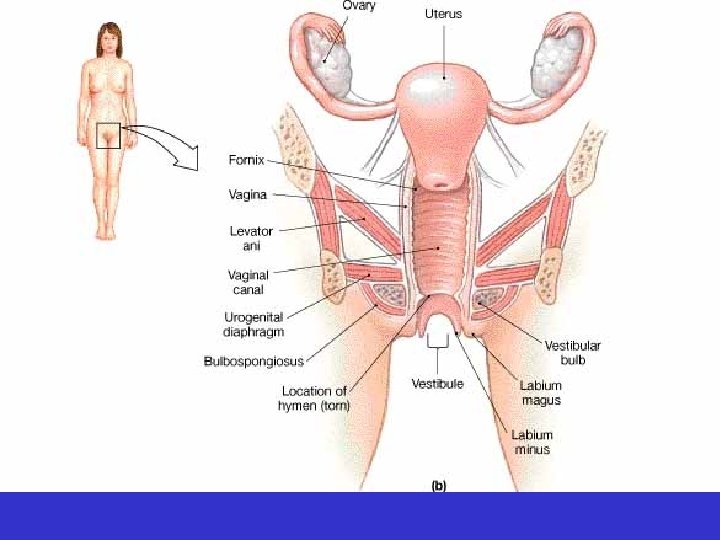
• Vagina – muscular tube between urinary bladder and rectum

• Vagina – pathway for sperm – pathway for menstrual flow – birth canal – vaginal opening may be partially covered by the hymen


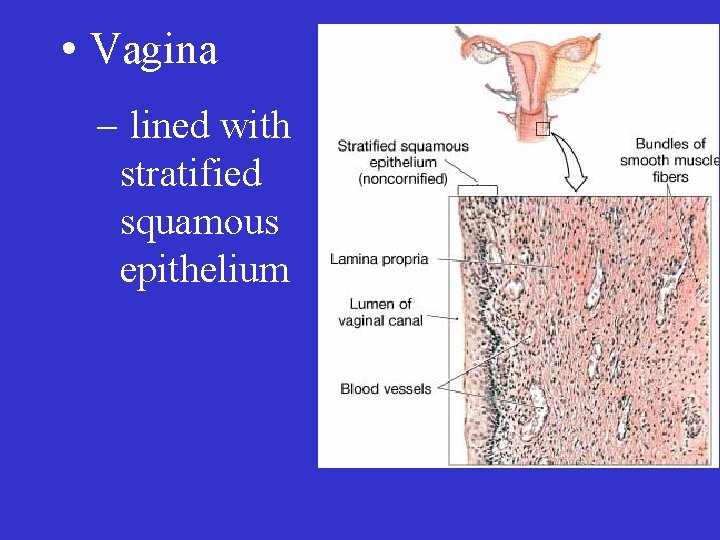
• Vagina – lined with stratified squamous epithelium

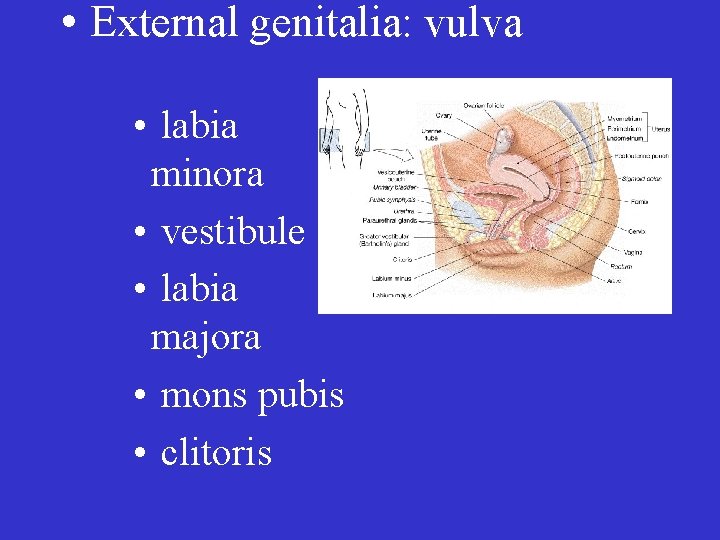
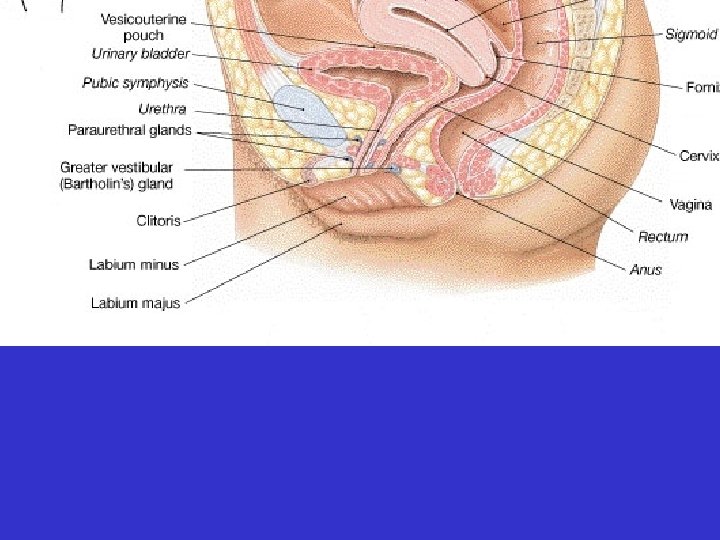
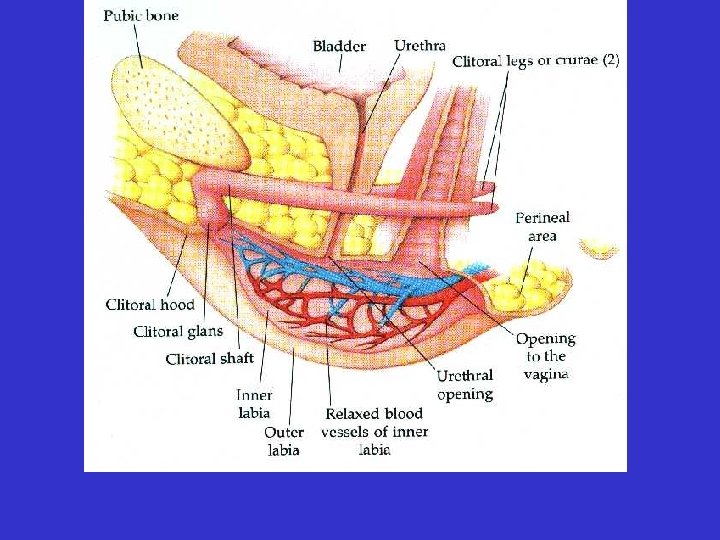
• External genitalia: vulva • labia minora • vestibule • labia majora • mons pubis • clitoris



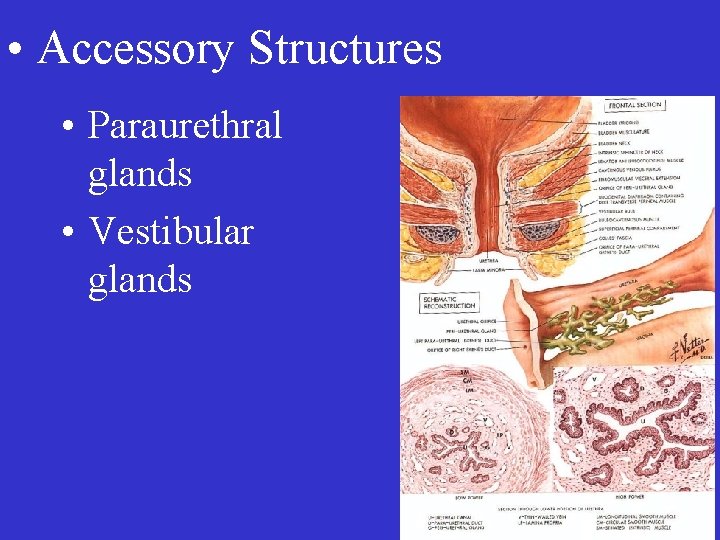
• Accessory Structures • Paraurethral glands • Vestibular glands

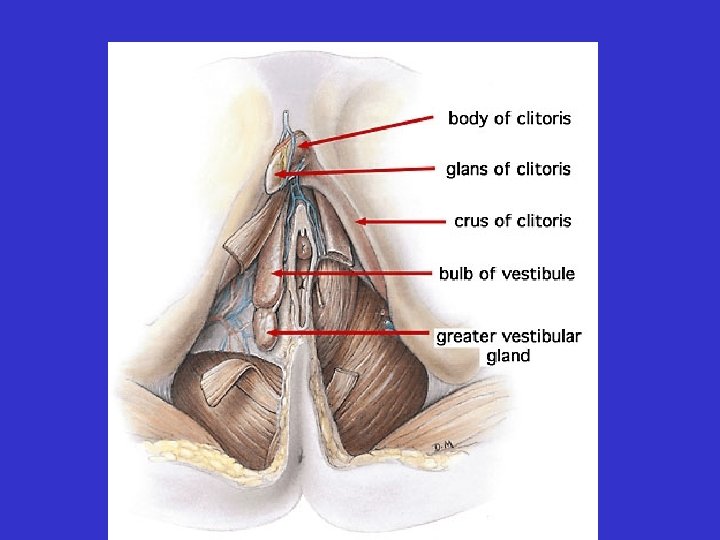
• Accessory Structures • Vestibular Bulb


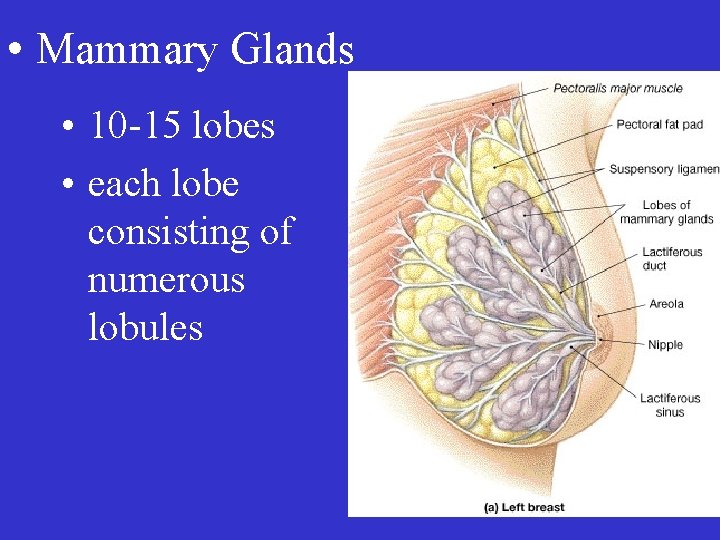
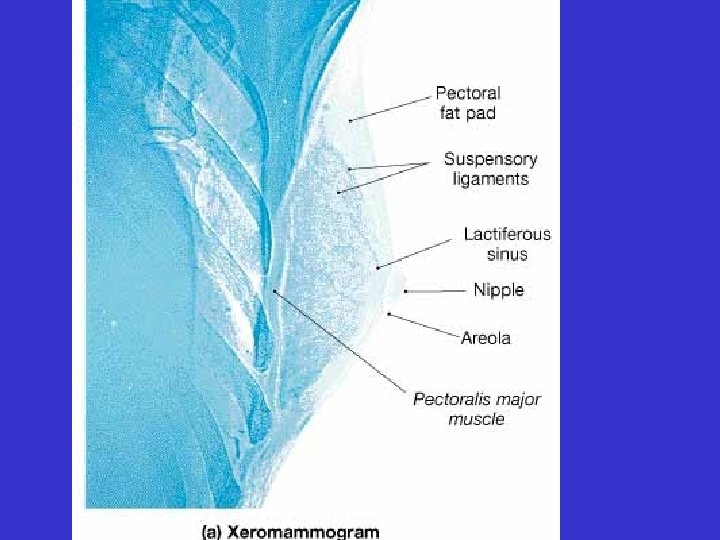
• Mammary Glands • 10 -15 lobes • each lobe consisting of numerous lobules

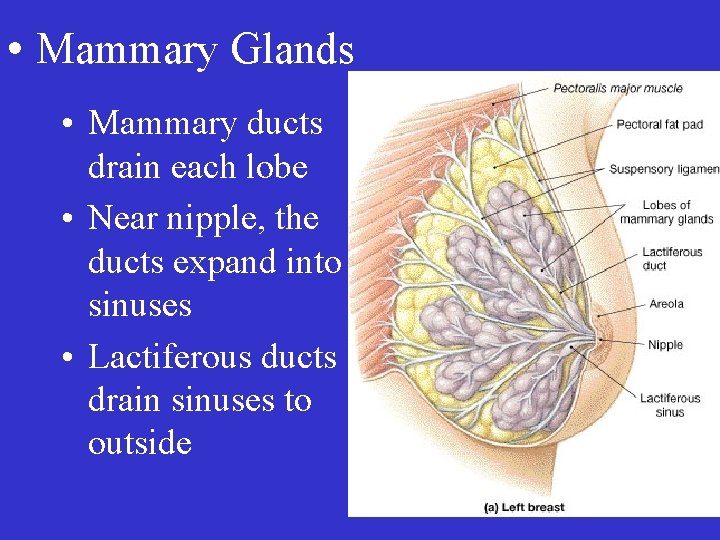
• Mammary Glands • Mammary ducts drain each lobe • Near nipple, the ducts expand into sinuses • Lactiferous ducts drain sinuses to outside

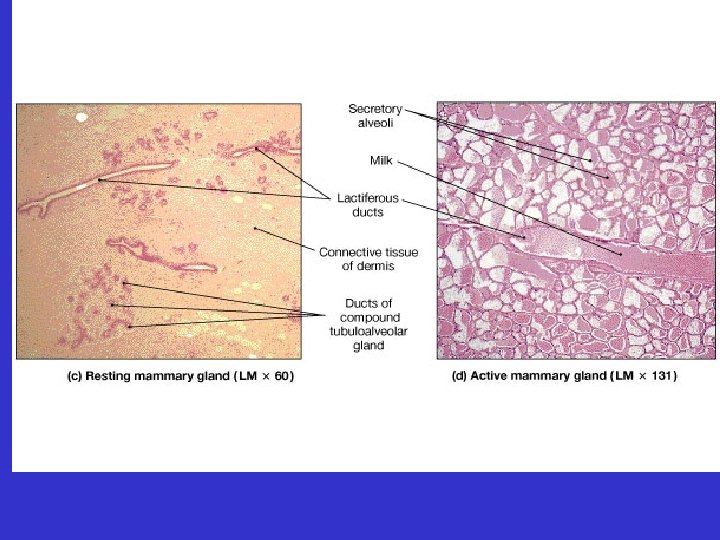
• Mammary Glands • Ducts and lobules associated with myoepithelial cells

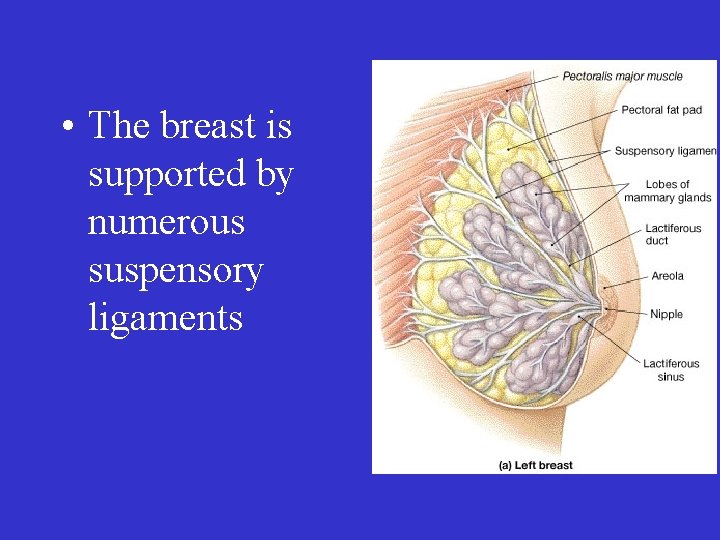
• The breast is supported by numerous suspensory ligaments




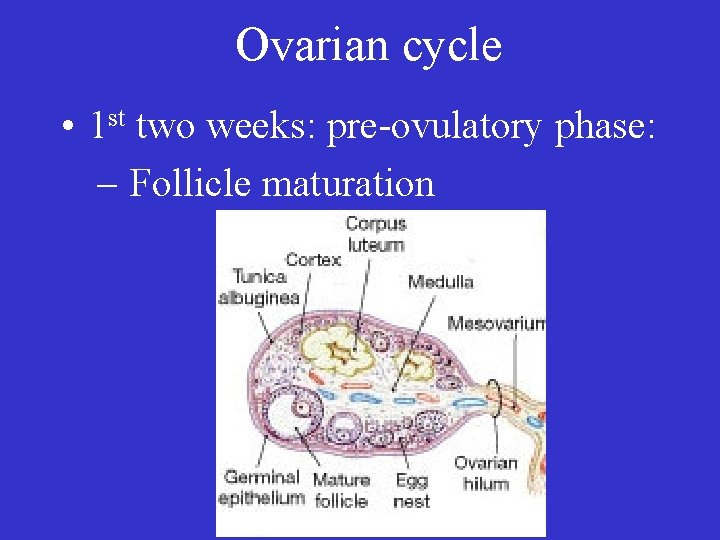
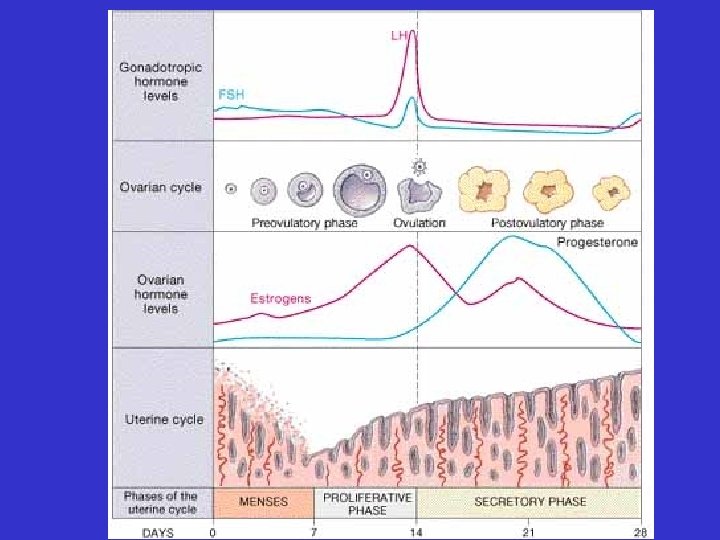
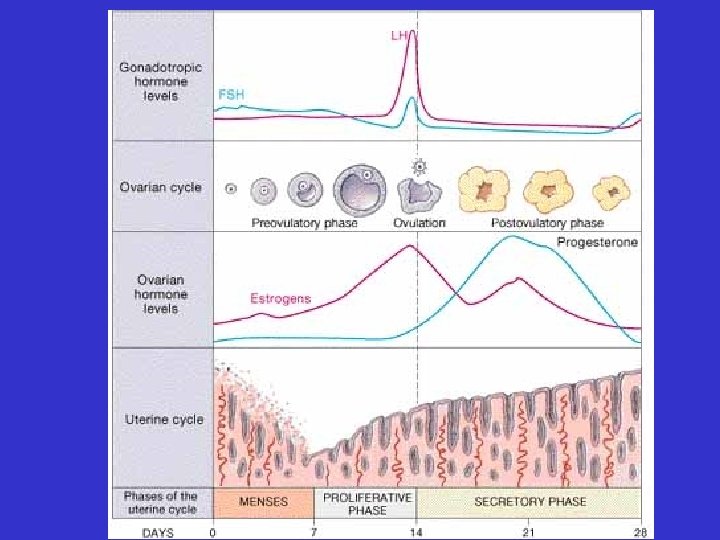
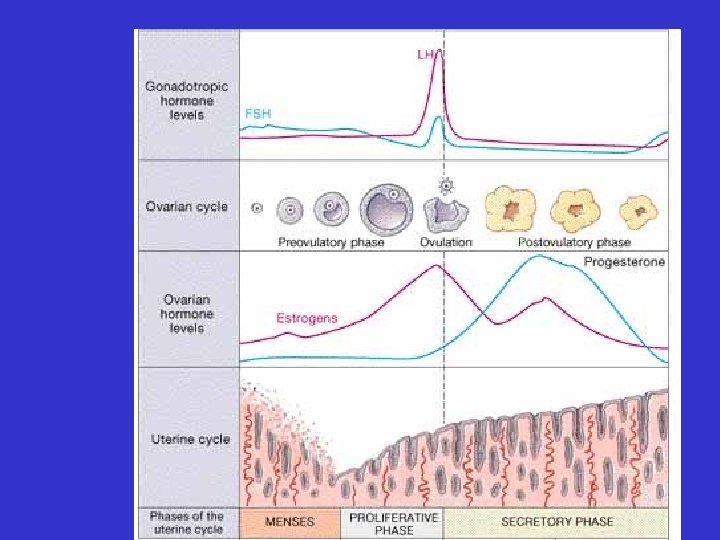
Ovarian cycle • 1 st two weeks: pre-ovulatory phase: – Follicle maturation


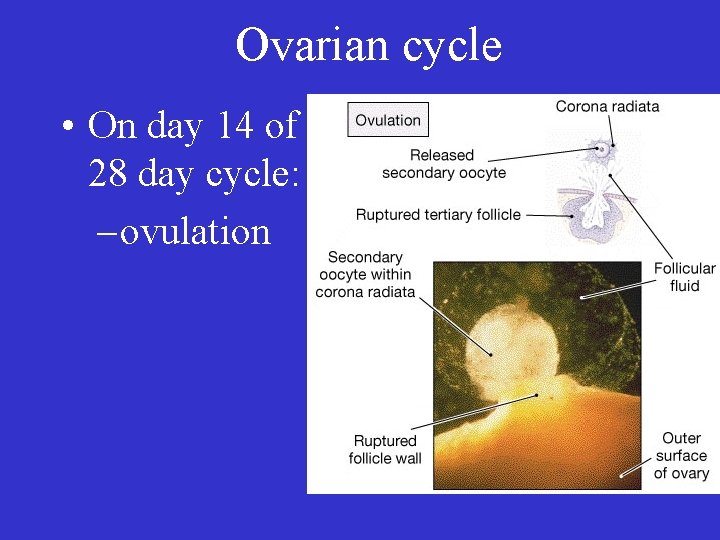
Ovarian cycle • On day 14 of a 28 day cycle: – ovulation


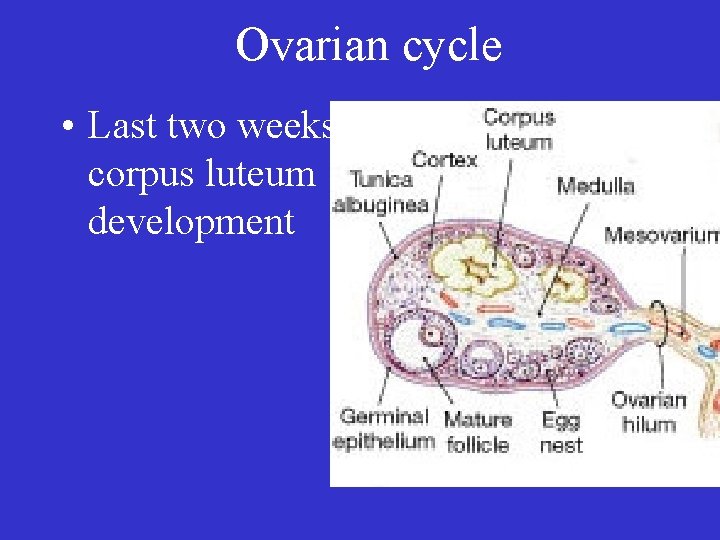
Ovarian cycle • Last two weeks: corpus luteum development


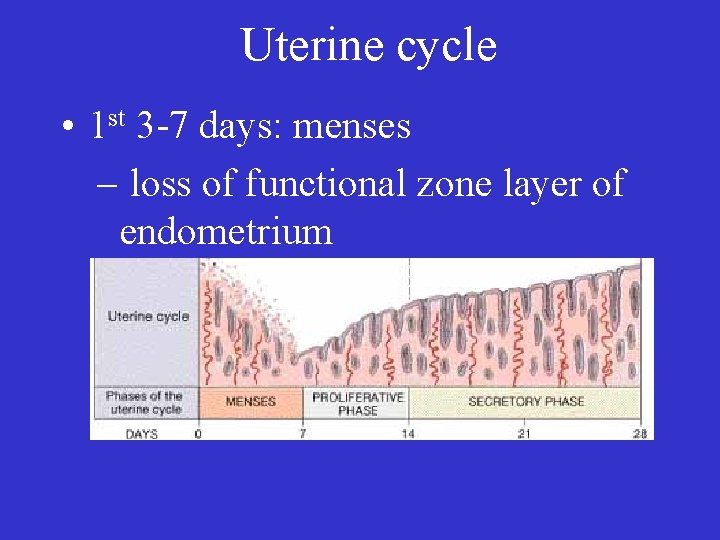
Uterine cycle • 1 st 3 -7 days: menses – loss of functional zone layer of endometrium

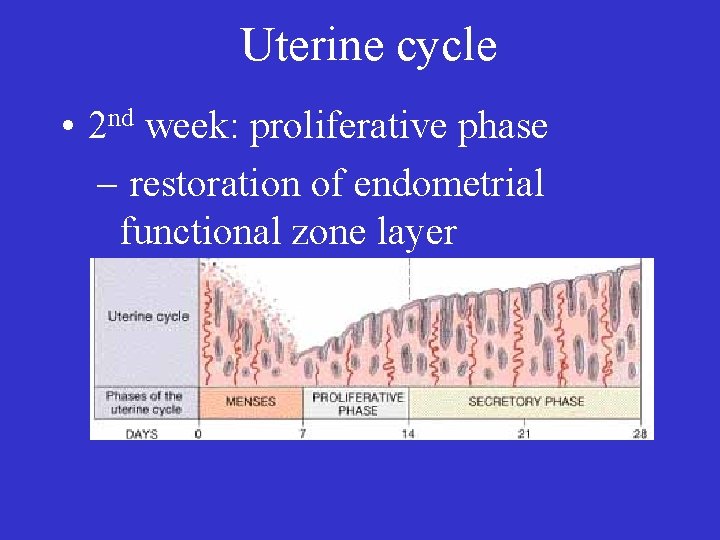
Uterine cycle • 2 nd week: proliferative phase – restoration of endometrial functional zone layer

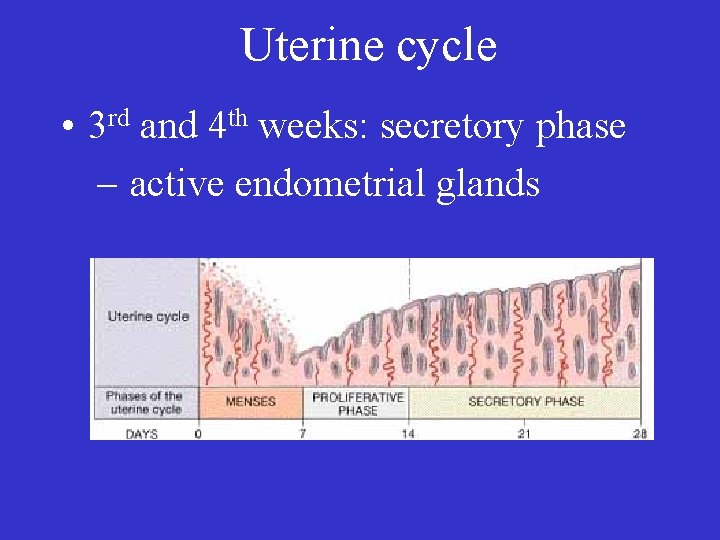
Uterine cycle • 3 rd and 4 th weeks: secretory phase – active endometrial glands

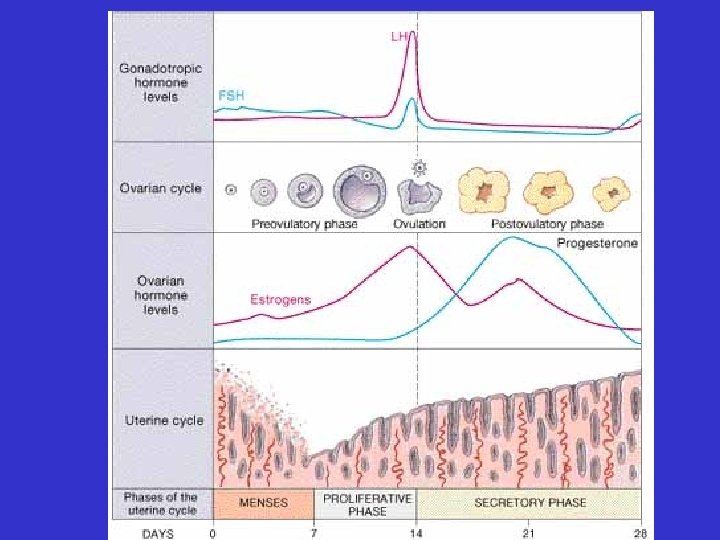
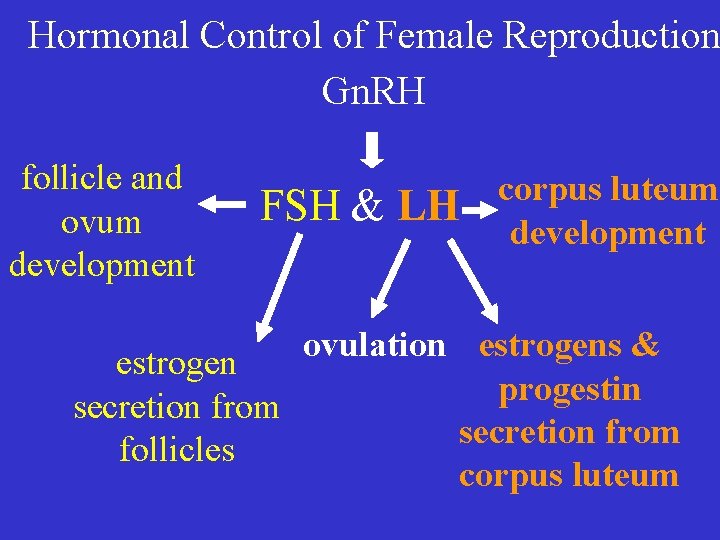
Hormonal Control of Female Reproduction Gn. RH follicle and ovum development FSH & LH corpus luteum development ovulation estrogens & estrogen progestin secretion from follicles corpus luteum

follicle and ovum development FSH & LH estrogen secretion from follicles ovulation E stimulates regrowth of endometrium corpus luteum development estrogens & progestin secretion from corpus luteum E & P stimulate endometrial gland secretion


• If (after two weeks) no pregnancy: – corpus luteum shuts down. – E & P secretion stops – endometrium loses hormonal support – menses begins

• If a successful fertilization occurs: – corpus luteum does not shut down. – E & P secretion continues – endometrium is maintained – pregnancy continues

• Why doesn’t the corpus luteum shut down if an early embryo is present?

• Other Functions of Estrogen – development, growth, & maintenance of female sex organs – bone and muscle growth – 2 o sex characteristics – libido

• General Function of Progestins – preparation of the body for pregnancy


Thank you ulnar nerve.