Maternity Male reproductive system Consists of those organs















































- Slides: 57

Maternity

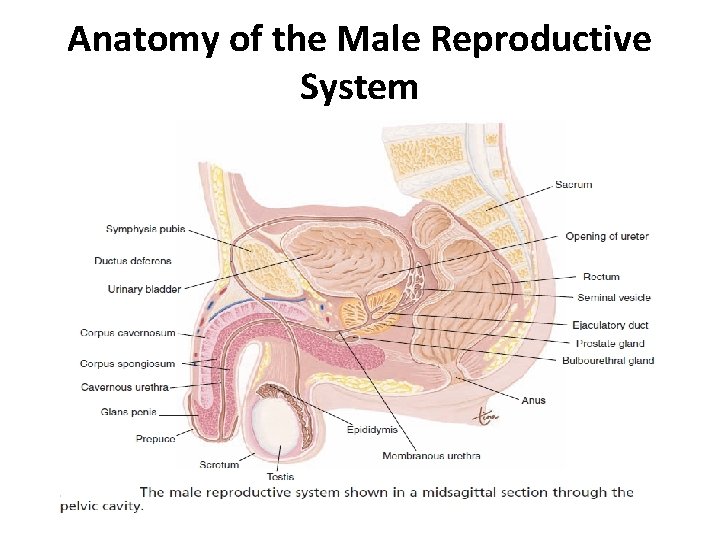
Male reproductive system • Consists of those organs functioning to produce a new individual. • The male organs are specialized to produce and maintain the male sex cells, or sperm; to transport them, along with supporting fluids, to the female reproductive system; and to secret the male hormone testosterone. • The Male reproductive organs include the two testes (Where the sperm cells and testosterone are made), the penis, the scrotum, and the Accessory organs (epididymis, vas deferens, seminal vesicles, ejaculatory duct, urethra, bulbourethral glands, and prostate gland).

Anatomy of the Male Reproductive System

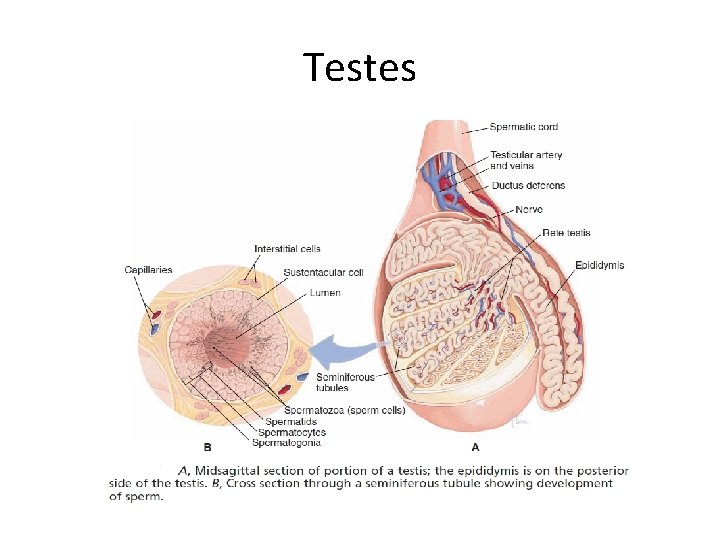
Testes • Located in the scrotum; one testis in each of the two scrotal compartments. • The left testis is lower than the right one. • Each testis is composed of several lobules which contain many seminiferous tubules and interstitial cells. • Seminiferous tubules in testis open into a series of efferent ductules that emerge from the top of the organ & enter the head of epididymis.

Testes

The functions of testes • Spermatogenesis which is formation of mature male gametes by seminiferous tubules (cells divide first by the process of mitosis). • Secretion of hormone (testosterone) by interstitial cells.

The genital Ducts • • Epididymis Vas deferens Ejaculatory duct Urethra

Epididymis • Each one is formed of a single, coiled tube enclosed in a fibrous tissue. • It lies along the top of testis & behind it. • Functions: o It is one of the ducts systems (they convey sperms to the vas deferens) o Maturation of the sperm which stays 1 -3 weeks in this segment. o Secretion of a small part of the seminal fluid.

Vas deferens • It's the extension of the tail of the epididymis. • It passes up in the inguinal canal to the top of the urinary bladder, to join the seminal duct, forming the ejaculatory duct. • Function: o Ductal system connects the epididymis with ejaculatory duct. o The storage time is about 30 days & the sperm will not lose their fertility power.

Ejaculatory duct • Both ducts are short tubes. • Pass through the prostate gland to terminate in urethra and they carry the spermatozoa and the seminal fluid. • Each is formed of the union of vas deferens & seminal vesicle.

Urethra • Is a tube for micturation & semen secretion

Accessory Reproductive Glands • Seminal vesicles • Prostate gland • Bulbourethral (Cowper's) glands

Seminal vesicles • They are two pouches, lies along the lower part of the posterior surface of the bladder, directly in front of the rectum. • Function: o Secretion of an alkaline viscous liquid component of the semen (it accounts for 60% of semen volume). o It contains fructose which is considered an energy source for sperm motility after ejaculation. o Contains alkaline prostaglandin to help neutralize semen p. H.

Prostate gland • It lies just below the bladder. • is a donut-shaped structure that encircles the urethra. • Functions: o It secretes a thin, milky, alkaline fluid that is rich in zinc, citric acid, acid phosphatase, and calcium which accounts for 30% of the seminal fluid. o Its alkalinity protects the sperm from the acidity of the male urethra & female vagina.

Bulbourethral glands • Cowper's glands are small peas in size & shape. • They are just below the prostate and around the penile part of urethra. • Functions: • Secretion of an alkaline fluid. • Secretion of mucous which is lubricant for urethra.

Supporting Structure • Scrotum • Penis • Spermatic cord

Scrotum • It's a pouch covered by skin. • They protect the testis • The main function of the scrotum is to provide the optimum temperature for testes for proper spermatogenesis; it's about 3°C below normal body temperature.

Penis • It's formed of 3 cylindrical masses of erectile or cavernous tissue, enclosed in separate fibrous covering of skin. • The larger upper two are called corpora cavernosa & the smaller lower one which contains the urethra is called the corpus spongiosum. • The distal part of the corpus spongiosum overlaps the terminal ends of the two corpora cavernosa forming a slight bulging, called glans penis. • The skin is folded over it. It is called foreskin or prepuce that's cut during circumcision. • The opening of urethra at the tip of glans penis is called the external urinary meatus. • The main function of penis is erection (enlargement & rigidity of the penis) by filling of the cavernous tissue by blood for penetration of the vagina to reach the semen deeply near the women’s cervix.

Spermatic cord • It's a fibrous covering of the vas deferens, blood vessels, lymph vessels & nerves. • It extends from the top of the testis along the inguinal canal, up to the internal inguinal ring. • Note: – Sperm count is 70 million per ml of semen. – Semen volume is 3 -5 cm.

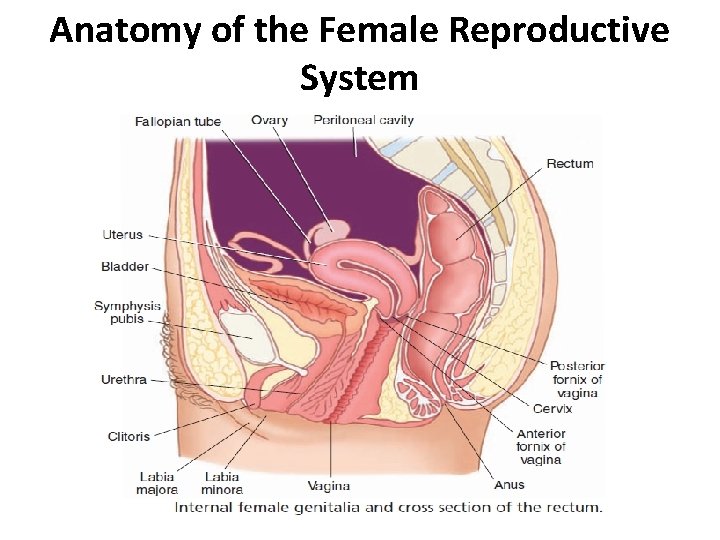
Female Reproductive System • The female reproductive system produces the female reproductive cells (the eggs, or ova and contains an organ (uterus) in which development of the fetus takes place. • The system includes the ovaries, uterus, uterine tubes, vagina, vulva, pelvis & breast.

Anatomy of the Female Reproductive System

Female pelvic • Function • Allows movement of the body, especially walking and running. • Helps in child bearing • Protect the pelvic organ.

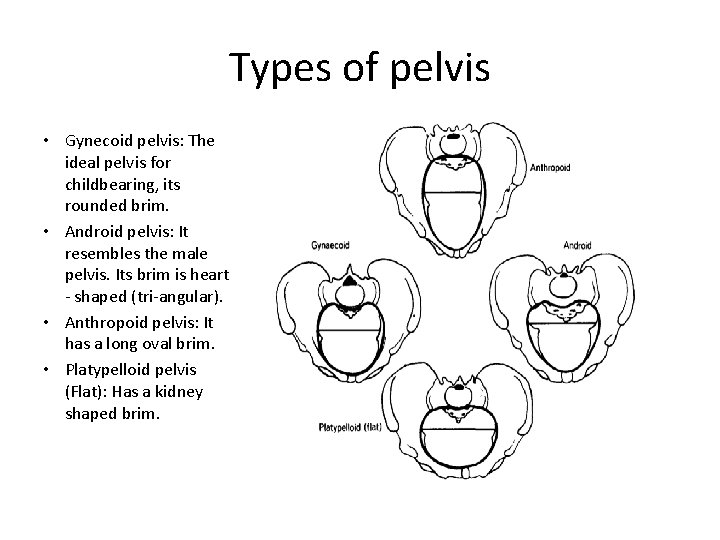
Types of pelvis • Gynecoid pelvis: The ideal pelvis for childbearing, its rounded brim. • Android pelvis: It resembles the male pelvis. Its brim is heart - shaped (tri-angular). • Anthropoid pelvis: It has a long oval brim. • Platypelloid pelvis (Flat): Has a kidney shaped brim.

Pelvic floor Function • Responsible for voluntary control of micturition and play an important part in sexual intercourse. • Allows exit to the fetus

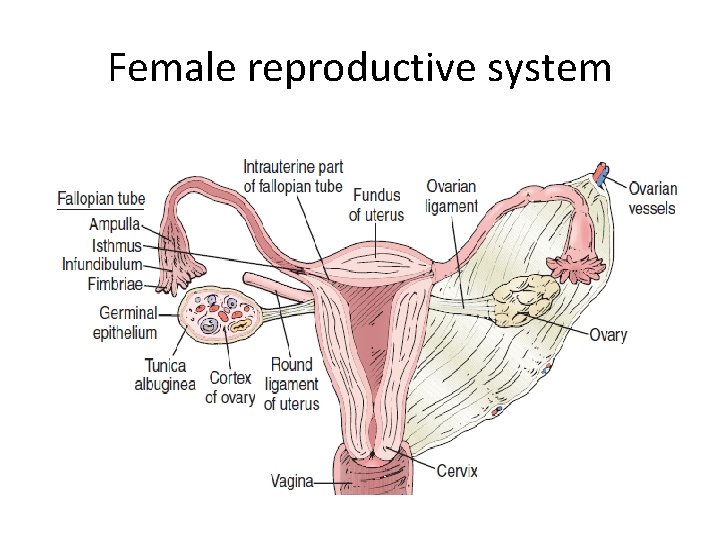
Female reproductive system

Ovaries – Both ovaries are nodular glands of uneven surface, like large almonds in size & shape. – Attached to the posterior surface of the broad ligament. – The end of the uterine tube cup is over it without actual attachment. – Functions: • Oogenesis (egg production). • Endocrine function: ovaries are the source of the female sex hormones (estrogen & progesterone) which are essential hormones in menstrual cycle & pregnancy.

Uterus – It is centrally located in the pelvic cavity between the bladder (anteriorly) and rectum (posteriorly). – In unmarried woman, the uterus is pear shaped, measures approximately 7. 5 cm length, 5 cm in width, and 2. 5 cm in thickness. – The upper part is called the body, the bulging upper part of the body is called the fundus & the lower part is called the cervix (neck).

Uterus – Uterine wall: consists of 3 layers: • Endometrium: is the innermost layer • It is composed of three layers, and of these, two are shed with each menses. • Myometrium: • It's the thick middle layer. • The fundus has the thickest part of myometrium. • It is composed of layers of smooth muscle that extend in three directions—longitudinal, transverse, and oblique. The tridirectional formation of the muscular layers is important in facilitating effective uterine contractions during labor and birth. • Parietal peritoneum: • It's the outermost layer. • It covers all the parts except the lower fourth of the anterior surface & the cervix.

Uterus – Uterine cavity: • The cavity is small because of the thick wall. • It's flat & triangular. • The base is upward & its apex is downward, constitutes the internal os which opens into the cervical canal which narrows on its lower end forming the external os which opens into the vagina. – Blood supply of the uterus: • The uterine blood supply is generous. • The two uterine arteries are branches of the internal iliac arteries. • The uterine & vaginal veins return to the internal iliac veins.

Functions of the uterus • • • Permits sperm to ascend toward the fallopian tubes. Pregnancy site. Nutritional source for the zygote until the placental develops. Provides a safe environment that protects and nurtures the growing embryo/fetus Labor. Menstruation.

Uterine (Fallopian) Tubes – Each one is about 10 cm long, attached to the outer upper angle of the uterus. The diameter of each tube is approximately 6 mm. – The mucosa of it has free connection with the uterine cavity medially & the peritoneal cavity laterally, so any infection in the tube "salpingitis" may extend to the peritoneal region caused peritonitis.

Uterine (Fallopian) Tubes – Consists of 3 divisions: • The isthmus: the closest part to the uterus. Tubal ligation done here. • Ampulla: is the middle third, dilated part, passing over the ovary. Mostly, ovum fertilization takes place here. • Infundibulum: Is the funnel-shaped portion located at the distal end of the fallopian tube. It has a finger like processes called fimbriae with an opening that receive ovum. – Functions: • It is one of the ductal systems. • It is the site of fertilization.

Vagina – It's a collapsible tube, 7 -10 cm long. – It presents between the bladder & urethra (anteriorly) & the rectum (posteriorly). – It connects the uterus with the perennial opening. – Functions: • Receives the sperms during the sexual intercourse. • Birth canal. • Transports tissue and blood during menses to the outside,

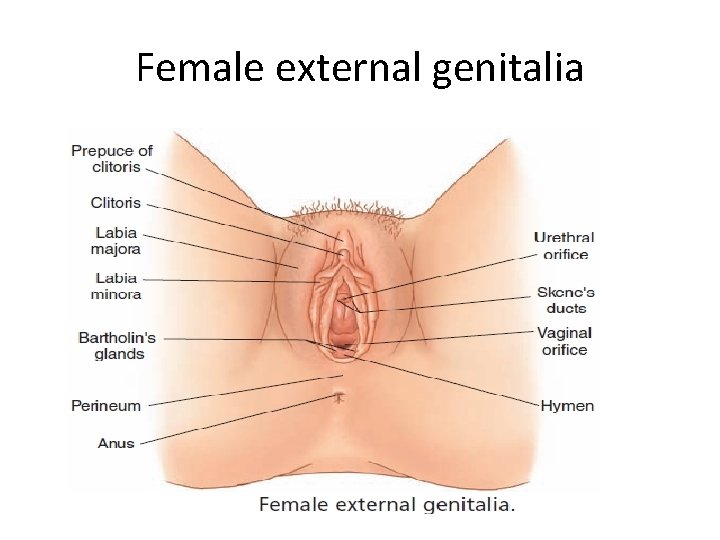
Female external genitalia

Vulva – Is the external genitalia which include mons pubis, labia majora, labia minora, urethral meatus, vaginal orifice, and bartholin's glands. » Mons pubis: is a skin – covered pad of fat over the symphysis pubis. » Labia majora (large lips): • The two folds of tissue that lie lateral to the genitalia and serve to protect the delicate tissues between them. • The external labia are covered with pubic hair while the medial surfaces, which are moist and pink, are without pubic hair. • It's formed mainly of connective tissue & fat with numerous sweat & sebaceous glands. » Labia minora (small lips): • They are hairless folds of skin. • They contain a number of sebaceous glands that provide lubrication and protective bacteriocidal secretions • The area in between the labia minora is called the vestibule.

Clitoris • It's a small erectile tissue and it’s sensitive during sexual intercourse. • It presents just behind the anterior junction of the labia minora. • Urinary meatus (urethral orifice): o Is a small opening of the urethra, between clitoris & vaginal orifice.

Greater vestibular gland (Bartholin's gland) • • • It's bean-shaped, one on each side of the vaginal orifice. Each opens by a long duct in a space between labia minora & the hymen They secrete mucus which lubricates the vaginal opening.

Hymen • A small portion of tissue surrounds the opening of the vagina. • It typically forms a border around the entrance of the vagina in premenstrual girls. • Hymenal tissue does not completely cover or occlude the vagina. • Ultimately the hymen becomes widened, sometimes by tearing, which may be accompanied by bleeding.

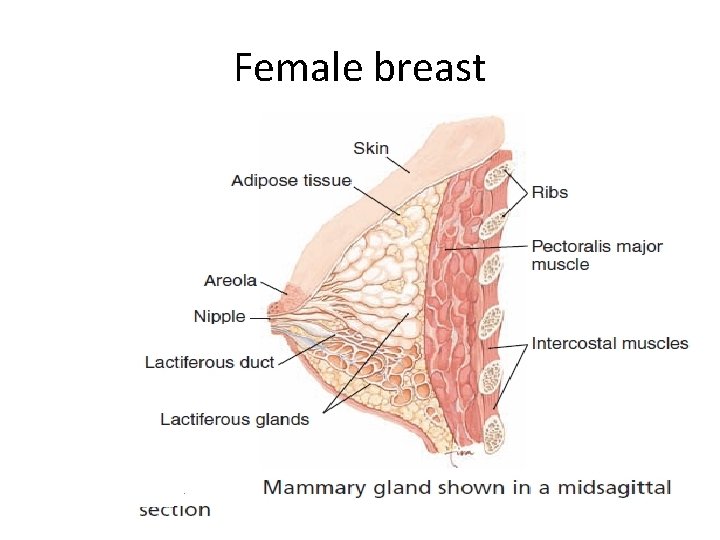
Female breast

Breasts • Breasts lay over the pectoralis muscles, connected to them by fibrous tissue and their size depend on the amount of fat deposited. • At puberty, development of an adolescent’s breasts is controlled by the hormones estrogen and progesterone. • Interestingly, in most women, the left breast is often larger than the right.

Breasts • Breast tissue is formed of two major organs: 1. Mammary systems: which include : – Lactating glands: which are formed of distal alveoli, forming lobules, united to form lobes, arranged in grape like clusters. – Ductal system: The ducts from the various lobules unite forming a single lactiferous (milk carrying) duct for each lobe, each enlarges slightly before reaching the nipple into small lactiferous sinuses, each duct terminates in a tiny opening on the surface of the nipple, each nipple is bordered by a circular pigmented area called areola, which contains many sebacious glands. 2. The connective tissue & fat: Which form the bulk of the breast, it is made mainly of fat, and the skin is anchored to the pectoral fascia by many fibrous suspensory ligaments.

Breast function • The function of the breast is lactation, the factors affecting milk production are: 1. Estrogen hormones promote the ductal growth. 2. Progestrone stimulates the alveolar system. 3. Prolactin stimulates milk secretion. 4. Oxytocin stimulates milk ejection from the breast.

Mechanisms of breast function • A high blood concentration of estrogen during pregnancy inhibits anterior pituitary secretion of prolactin, so no milk will be made during pregnancy. • Shedding of placenta, after labor leads to marked decrease in estrogen level in the blood that stimulates anterior pitutary to secrete prolactin. • Sucking movements of a baby stimulates the anterior pituitary to secrete prolactin, and the posterior pituitary to secrete oxytocin to increase milk ejection.

Female reproductive cycles • There are many periodical changes in female during the years between the onset of the menses (menarche) and their cessation (menopause) on the level of endometrium, ovarian, myometrial & gonadotropic cycle.

1. Ovarian Cycle • Before birth, the ovarian tissue begins a meiosis division; it reduces the number of chromosomes in the daughter cell by half. • When a child is born, her ovaries contain many primary follicles, each contains an oocytes that have temporarily suspended the meiotic process before it's complete, once each month, on about the first day of menstruation, the oocytes within many primary follicles resume meiosis, one of them matures & migrates to the surface of the ovary, to be expelled from the ruptured wall of the mature follicle during ovulation.

1. Ovarian Cycle • Ovulation usually occurs 14 days before the next menstrual period begins. • Immediately after ovulation, cells of the ruptured follicle enlarged & transformed into a golden colored body which called corpus luteum. • The corpus luteum which grows for 7 -8 days, during this period will secrete high amount of progesterone. • Then the corpus luteum will be nonfunctioning white scar, called corpus albicans which moves to the center of the ovary & finally disappears.

2. Endometrial (menstrual) cycle • During menstruation, parts of compact & spongy layers of the endometrium slough off, leaving denuded areas. • After menstruation, this cell layer will proliferate causing the endometrium to reach a thickness of 2 -3 mm by the time of ovulation. • Part of this is secreting a nutrient fluid during the time between ovulation & the next menses.

2. Endometrial (menstrual) cycle • A day before menstruation starts again, a drop in progesterone level causes contraction of the muscle layer of the arteries that supply the tissues, producing endometrial ischemia, leading to the death of the tissue, and sloughing of the endometrium (bleeding). • So we can divide menstrual cycle into phases: • Menses: occurs on days 1 -5 of a new cycle. • Postmenstrual phase (between the end of menses & ovulation), so it can be described as "preovulatory phase" it starts from the 6 th to 13 th day of a 28 days-cycle. This period is called estrogenic or follicular or proliferative phase. • Ovulation: occurs on cycle day 14 in a 28 - day cycle. • Premenstrual phase (postovulatory) between ovulation & the onset of menses, it's secretory or luteal phase so progesterone will be secreted, it takes from day 14 to day 28 in a 28 -day cycle.

3. Myometrial cycle: • Myometrium contracts mildly but with increasing frequency during the two weeks preceding ovulation, to decrease or stop during ovulation & after that. 4. Gonadotropic cycle: • The anterior pituitary gland secretes two hormones, LH & FSH.

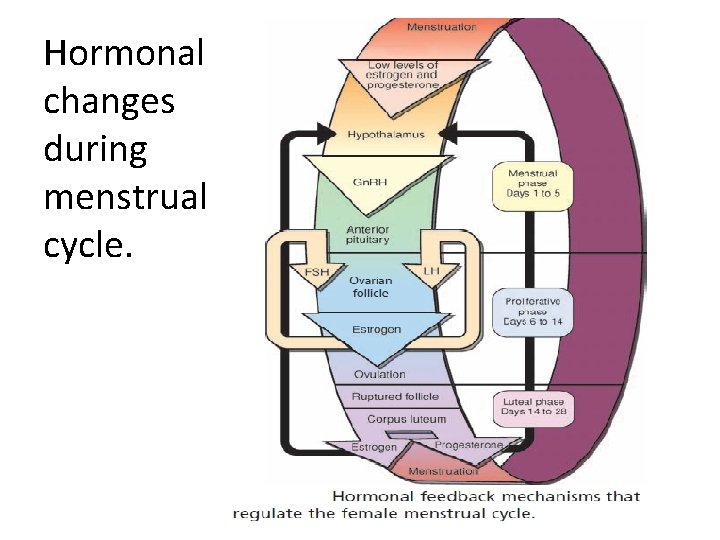
Control of female reproductive cycles • The menstrual cycle is hormonally mediated through events that take place in the hypothalamus, anterior pituitary gland, and the ovaries. • The hypothalamus stimulates the anterior pituitary gland to produce gonadotropin. FSH, one of these hormones, stimulates the growth and development of the graafian follicle, which secretes estrogen. • Estrogen stimulates proliferation of the endometrial lining of the uterus. • After ovulation, the anterior pituitary gland secretes LH, which stimulates development of the corpus luteum.

Control of female reproductive cycles • Progesterone secreted by the corpus luteum prompts further development of the lining of the uterus in preparation for the fertilized ovum. • When pregnancy does not occur, the corpus luteum degenerates, and the levels of estrogen and progesterone decline. • The decreased levels of estrogen and progesterone cause the uterus to shed its lining during menstruation. • The decrease in estrogen and progesterone triggers a negative feedback to the hypothalamus, which stimulates the anterior pituitary gland to secrete FSH once again.

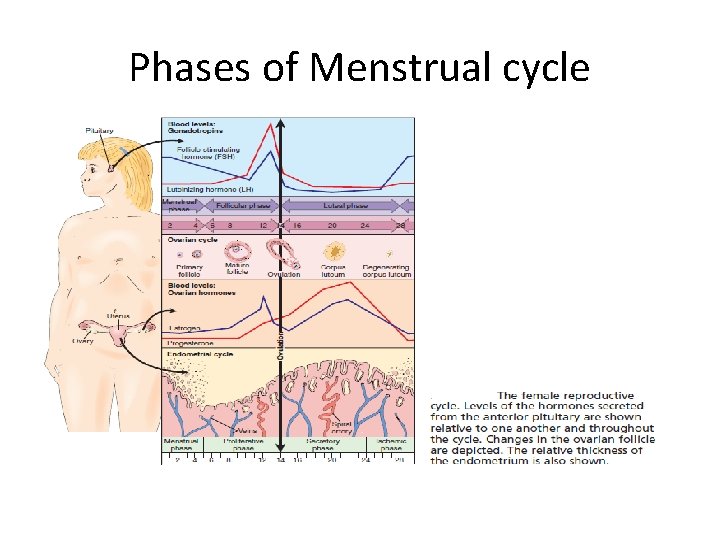
Phases of Menstrual cycle

Hormonal changes during menstrual cycle.

Increase of estrogen during the post menstrual phase will cause • • Proliferation of the endometrium cells. Growth of the endometrial glands. Increase in endometrium water content. Increase in myometrial contraction.

Increase of progesterone during the premenstrual phase will cause • Increase secretion by endometrial glands. • Increase in the endometrium water content. • Decrease in myometrial contraction

Importance of female reproductive cycles • Production of ovum is the main role. • Preparing the uterine endometrium for suitable implantation, so constant renewable of the endometrium makes successful implantation. • Notes: – Menarche: is the first flow of menstruation, at puberty, at about the age of 13 years, with many variations. – Menopause (climacteric) is the cessation of menstruation from about the age 45 -50 years. – After menopause, estrogen concentration decreases dramatically, which causes negative feedback response that increases the gonadotropin levels.

Notes – After ovulation, the ovum can be fertilized for 12 -24 hours. – After ejaculation, sperm can fertilize an egg for up to 48 hours. – Less than 200 sperms actually reach the egg and only one will fertilize it. – Fertilization occurs in the ampullary portion of the fallopian tube. – The fertilized ovum reaches the uterine cavity approximately 2 -3 days after fertilization – Implantation begins 2 -3 days after the fertilized ovum enters the uterine cavity – Human chorionic gonadotropin (h. CG) is produced by the conceptus at about the time of implantation.