Power Point Lecture Slides prepared by Barbara Heard

Power. Point® Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College CHAPTER 27 The Reproductive System: Part B © Annie Leibovitz/Contact Press Images © 2013 Pearson Education, Inc.

Hormonal Regulation of Male Reproductive Function • Sequence of hormonal regulatory events involving hypothalamus, anterior pituitary gland, and testes – Hypothalamic-pituitary-gonadal (HPG) axis – Regulates production of gametes and sex hormones through 3 interacting sets of hormones • Gn. RH indirectly stimulates testes via FSH & LH • FSH & LH directly stimulate testes • Testosterone & inhibin – negative feedback on hypothalamus and anterior pituitary © 2013 Pearson Education, Inc.

HPG Axis • Sequence of regulatory events – Hypothalamus releases gonadotropinreleasing hormone (Gn. RH) anterior pituitary to secrete FSH and LH – FSH causes sustentocytes to release androgen-binding protein (ABP) high concentration of testosterone near spermatogenic cells spermatogenesis – LH prods interstitial endocrine cells testosterone spermatogenesis © 2013 Pearson Education, Inc.

HPG Axis • Testosterone sex organ maturation, development/maintenance secondary sex characteristics, libido • Rising testosterone levels feedback inhibition on hypothalamus to inhibit Gn. RH and on pituitary to inhibit gonadotropin release • Inhibin (released when sperm count high) – inhibits Gn. RH and FSH release © 2013 Pearson Education, Inc.

HPG Axis • Three years to achieve balance, then testosterone and sperm production fairly stable throughout life • Without Gn. RH and gonadotropins testes atrophy; sperm and testosterone production cease © 2013 Pearson Education, Inc.
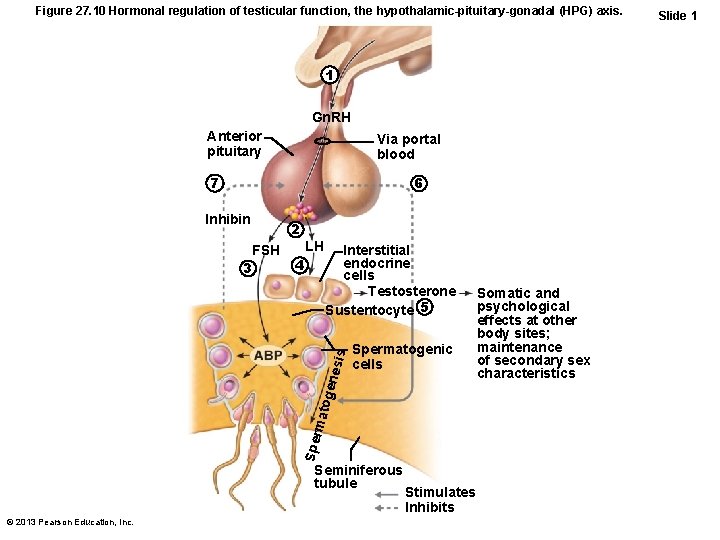
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 7 6 Inhibin LH 4 Interstitial endocrine cells Testosterone Sustentocyte 5 Spermatogenic cells Spe rma toge nesi s FSH 3 2 Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Somatic and psychological effects at other body sites; maintenance of secondary sex characteristics Slide 1
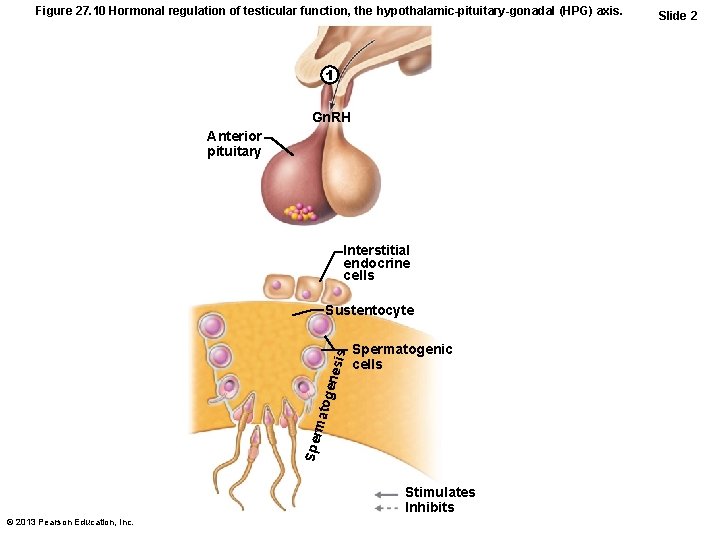
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Interstitial endocrine cells Spermatogenic cells Spe rma toge nesi s Sustentocyte Stimulates Inhibits © 2013 Pearson Education, Inc. Slide 2
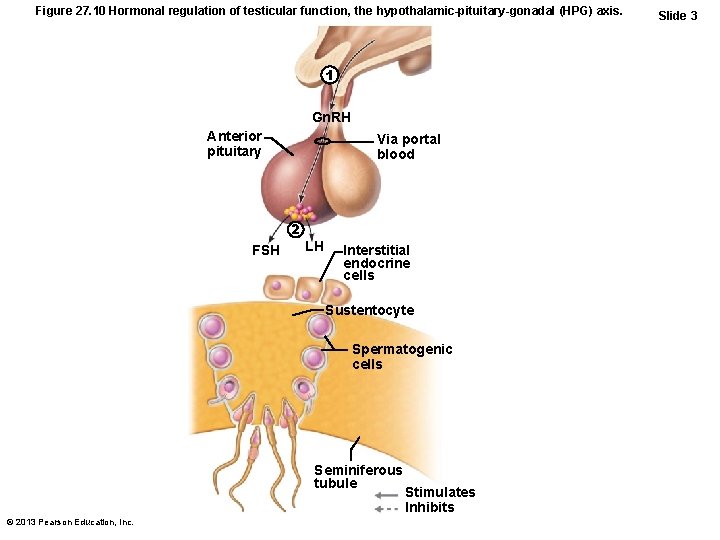
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 2 FSH LH Interstitial endocrine cells Sustentocyte Spermatogenic cells Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Slide 3
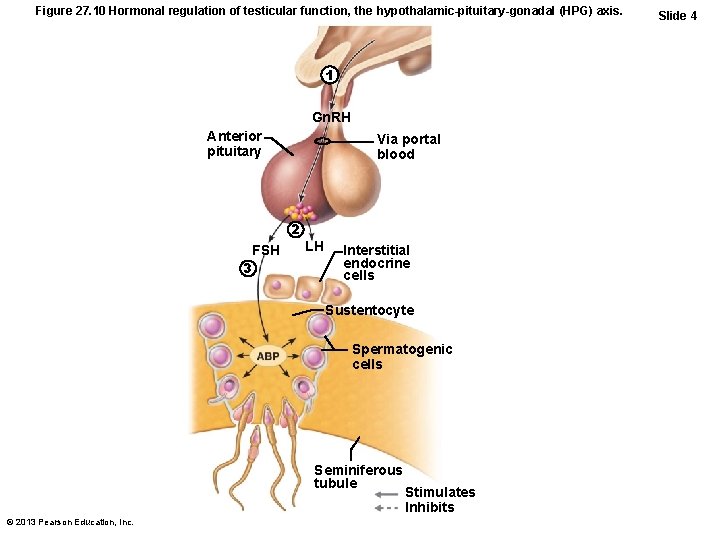
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 2 FSH 3 LH Interstitial endocrine cells Sustentocyte Spermatogenic cells Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Slide 4
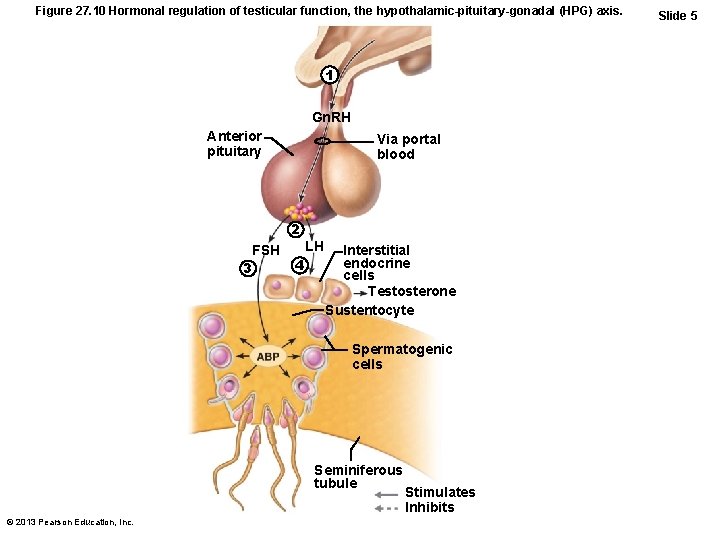
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 2 FSH 3 4 LH Interstitial endocrine cells Testosterone Sustentocyte Spermatogenic cells Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Slide 5
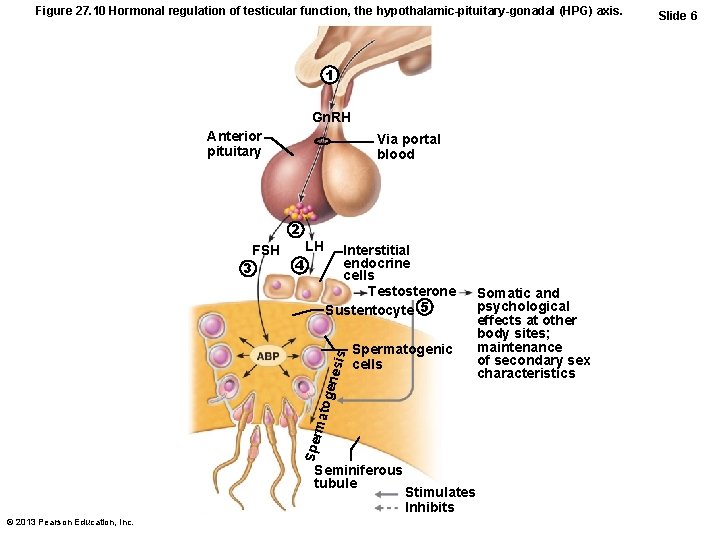
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 2 LH 4 Interstitial endocrine cells Testosterone Sustentocyte 5 Spermatogenic cells Spe rma toge nesi s FSH 3 Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Somatic and psychological effects at other body sites; maintenance of secondary sex characteristics Slide 6
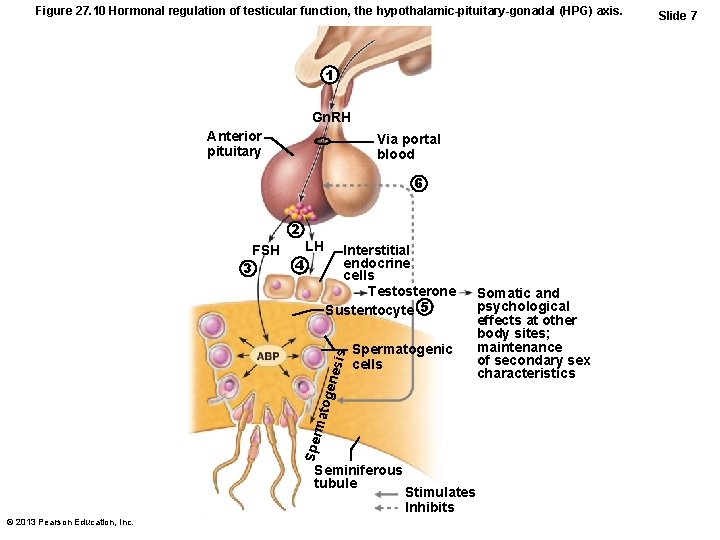
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 6 2 LH 4 Interstitial endocrine cells Testosterone Sustentocyte 5 Spermatogenic cells Spe rma toge nesi s FSH 3 Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Somatic and psychological effects at other body sites; maintenance of secondary sex characteristics Slide 7
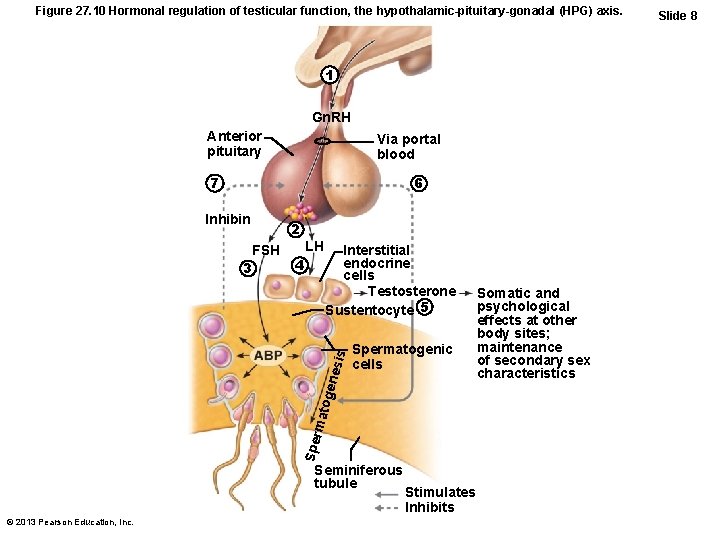
Figure 27. 10 Hormonal regulation of testicular function, the hypothalamic-pituitary-gonadal (HPG) axis. 1 Gn. RH Anterior pituitary Via portal blood 7 6 Inhibin LH 4 Interstitial endocrine cells Testosterone Sustentocyte 5 Spermatogenic cells Spe rma toge nesi s FSH 3 2 Seminiferous tubule © 2013 Pearson Education, Inc. Stimulates Inhibits Somatic and psychological effects at other body sites; maintenance of secondary sex characteristics Slide 8

Mechanism and Effects of Testosterone Activity • Testosterone – Synthesized from cholesterol – Transformed to exert its effects on some target cells • Dihydrotestosterone (DHT) in prostate • Estradiol in some neurons in brain © 2013 Pearson Education, Inc.

Mechanism and Effects of Testosterone Activity • Prompts spermatogenesis • Targets all accessory organs • Has multiple anabolic effects throughout body • Deficiency leads to atrophy; semen volume declines; erection and ejaculation impaired – Treated with testosterone replacement © 2013 Pearson Education, Inc.

Male Secondary Sex Characteristics • Features induced in nonreproductive organs by male sex hormones (mainly testosterone) – Appearance of pubic, axillary, and facial hair – Enhanced growth of chest hair; deepening of voice – Skin thickens and becomes oily – Bones grow, increase in density – Skeletal muscles increase in size and mass – Boosts basal metabolic rate – Basis of sex drive (libido) in males © 2013 Pearson Education, Inc.

Male Secondary Sex Characteristics • Testosterone – Masculinizes embryonic brain – Continues to exert effect well into adulthood – Adrenal glands produce androgens in small amounts – insufficient to maintain normal testosterone-mediated functions © 2013 Pearson Education, Inc.
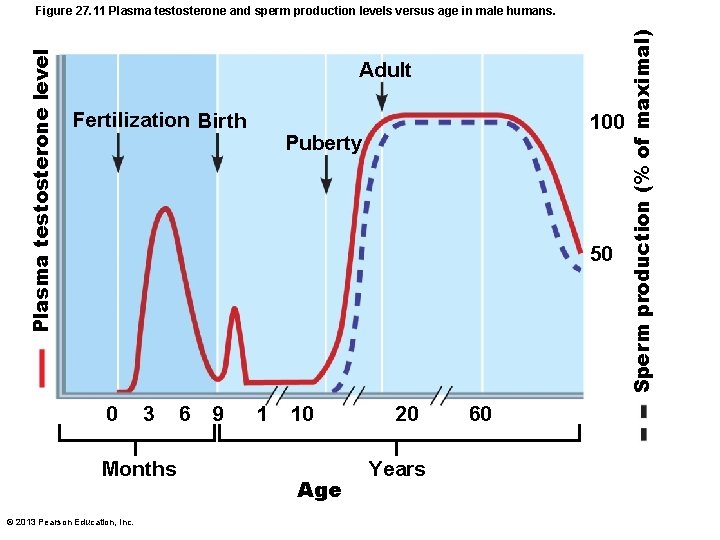
Adult Fertilization Birth 100 Puberty 50 0 3 Months © 2013 Pearson Education, Inc. 6 9 1 10 Age 20 Years 60 Sperm production (% of maximal) Plasma testosterone level Figure 27. 11 Plasma testosterone and sperm production levels versus age in male humans.

Female Reproductive Anatomy • Ovaries - female gonads – Produce female gametes (ova) – Secrete female sex hormones, estrogen (estradiol, estrone, estriol) and progesterone • Accessory ducts include – Uterine tubes – Uterus – Vagina © 2013 Pearson Education, Inc.

Female Reproductive Anatomy • Internal genitalia – in pelvic cavity – Ovaries – Uterine tubes – Uterus – Vagina • External genitalia – External sex organs © 2013 Pearson Education, Inc.
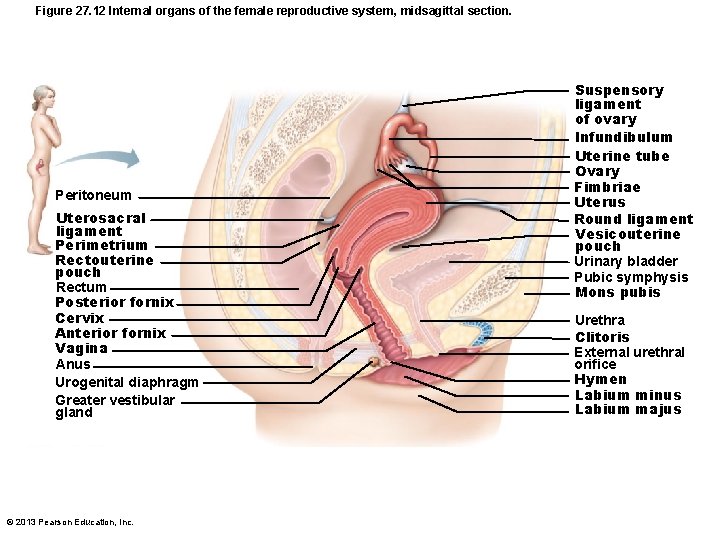
Figure 27. 12 Internal organs of the female reproductive system, midsagittal section. Peritoneum Uterosacral ligament Perimetrium Rectouterine pouch Rectum Posterior fornix Cervix Anterior fornix Vagina Anus Urogenital diaphragm Greater vestibular gland © 2013 Pearson Education, Inc. Suspensory ligament of ovary Infundibulum Uterine tube Ovary Fimbriae Uterus Round ligament Vesicouterine pouch Urinary bladder Pubic symphysis Mons pubis Urethra Clitoris External urethral orifice Hymen Labium minus Labium majus

Ovaries • Held in place by several ligaments – Ovarian ligament - anchors ovary medially to uterus – Suspensory ligament - anchors ovary laterally to pelvic wall – Mesovarium - suspends ovary • Suspensory ligament and mesovarium part of broad ligament – supports uterine tubes, uterus, and vagina © 2013 Pearson Education, Inc.
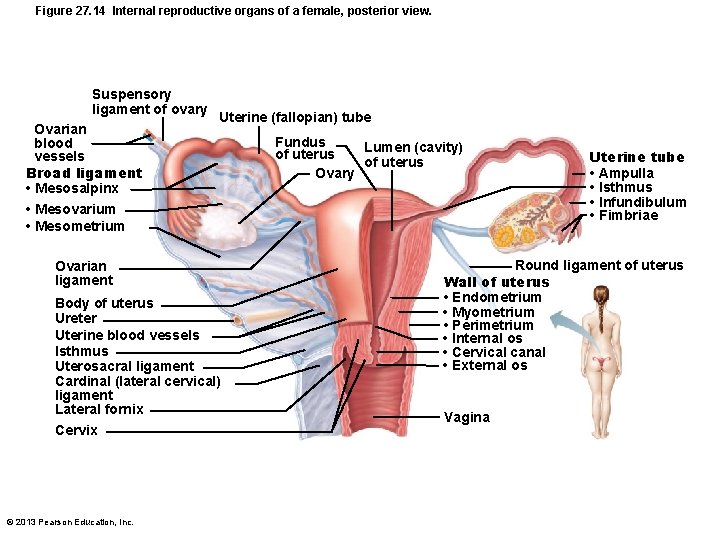
Figure 27. 14 Internal reproductive organs of a female, posterior view. Suspensory ligament of ovary Ovarian blood vessels Broad ligament • Mesosalpinx • Mesovarium • Mesometrium Uterine (fallopian) tube Ovarian ligament Body of uterus Ureter Uterine blood vessels Isthmus Uterosacral ligament Cardinal (lateral cervical) ligament Lateral fornix Cervix © 2013 Pearson Education, Inc. Fundus Lumen (cavity) of uterus Ovary Uterine tube • Ampulla • Isthmus • Infundibulum • Fimbriae Round ligament of uterus Wall of uterus • Endometrium • Myometrium • Perimetrium • Internal os • Cervical canal • External os Vagina

Ovaries • Blood supply - ovarian arteries and ovarian branch of the uterine arteries • Surrounded by fibrous tunica albuginea • Germinal epithelium - outer layer • Two poorly defined regions – Outer cortex – houses forming gametes – Inner medulla - large blood vessels and nerves © 2013 Pearson Education, Inc.

Ovaries • Embedded in cortex – Ovarian follicles • Immature egg (oocyte) surrounded by – Follicle cells (one cell layer thick) – Granulosa cells (more than one layer present) © 2013 Pearson Education, Inc.

Follicles • Several stages of development – Primordial follicle – single layer of follicle cells + oocyte – More mature follicles – several layers of granulosa cells © 2013 Pearson Education, Inc.

Ovaries • Vesicular (antral or tertiary) follicle – fully mature follicle – Fluid-filled antrum forms; follicle bulges from ovary surface • Ovulation – Ejection of oocyte from ripening follicle • Corpus luteum develops from ruptured follicle after ovulation © 2013 Pearson Education, Inc.
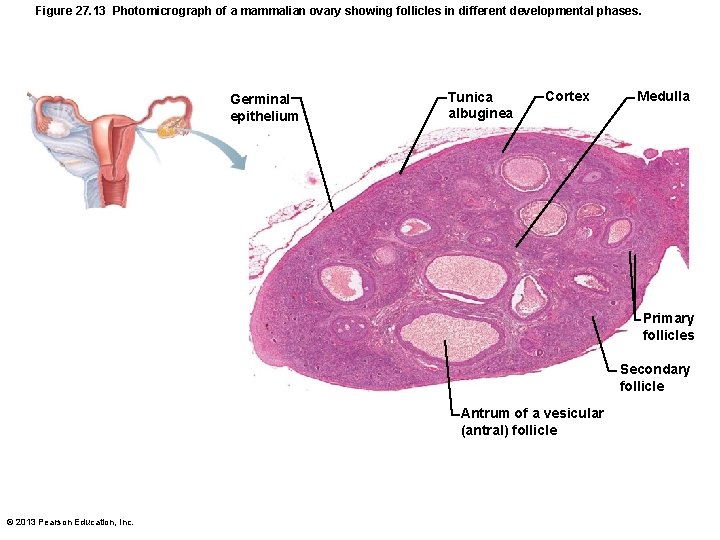
Figure 27. 13 Photomicrograph of a mammalian ovary showing follicles in different developmental phases. Germinal epithelium Tunica albuginea Cortex Medulla Primary follicles Secondary follicle Antrum of a vesicular (antral) follicle © 2013 Pearson Education, Inc.

Female Duct System • Ducts have no contact with ovary – Oocyte cast into peritoneal cavity; some lost there • Uterine (fallopian) tubes or oviducts • Uterus • Vagina © 2013 Pearson Education, Inc.

Uterine Tubes • Receive ovulated oocyte; usual site of fertilization • Isthmus - constricted region where tube joins uterus • Ampulla • Distal expansion with infundibulum near ovary – Ciliated fibriae of infundibulum create currents to move oocyte into uterine tube © 2013 Pearson Education, Inc.

Uterine Tubes • Oocyte carried along by peristalsis and ciliary action • Nonciliated cells nourish oocyte and sperm • Covered externally by peritoneum • Mesosalpinx - mesentery that supports uterine tubes © 2013 Pearson Education, Inc.
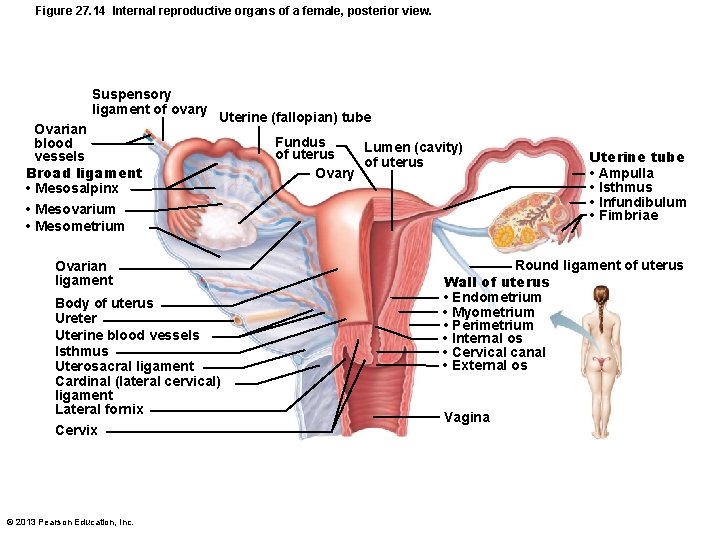
Figure 27. 14 Internal reproductive organs of a female, posterior view. Suspensory ligament of ovary Ovarian blood vessels Broad ligament • Mesosalpinx • Mesovarium • Mesometrium Uterine (fallopian) tube Ovarian ligament Body of uterus Ureter Uterine blood vessels Isthmus Uterosacral ligament Cardinal (lateral cervical) ligament Lateral fornix Cervix © 2013 Pearson Education, Inc. Fundus Lumen (cavity) of uterus Ovary Uterine tube • Ampulla • Isthmus • Infundibulum • Fimbriae Round ligament of uterus Wall of uterus • Endometrium • Myometrium • Perimetrium • Internal os • Cervical canal • External os Vagina

Homeostatic Imbalance • Ectopic pregnancy – Oocyte fertilized in peritoneal cavity or distal uterine tube begins developing there • Normally abort naturally with substantial bleeding • Pelvic inflammatory disease (PID) – Spread of infection from reproductive tract to peritoneal cavity • May cause scar tissue infertility © 2013 Pearson Education, Inc.

Uterus • Hollow, thick-walled, muscular organ • Function – Receive, retain, nourish fertilized ovum • Anteverted – inclined forward; retroverted – inclined backward • Body - major portion • Fundus - rounded superior region • Isthmus - narrowed inferior region © 2013 Pearson Education, Inc.

Uterus • Cervix - narrow neck, or outlet; projects into vagina • Cervical canal communicates with – Vagina via external os – Uterine body via internal os • Cervical glands secrete mucus that blocks sperm entry except during midcycle © 2013 Pearson Education, Inc.

Homeostatic Imbalance • Cervical cancer – 450, 000 women worldwide each year – killing half – Most common between 30 – 50 – Risks – frequent cervical inflammations, STIs, multiple pregnancies – Papanicolaou (Pap) smear for detection • Every two years 21 – 30; every year > 30; discontinue at 65 if negative for 10 years © 2013 Pearson Education, Inc.

Homeostatic Imbalance • Pap smear results inconclusive – Test for human papillomavirus – cause of most cervical cancers • Gardasil – three-dose vaccine; protects against HPV – Recommended for 11 - and 12 -year-old girls © 2013 Pearson Education, Inc.

Supports of the Uterus • Mesometrium—lateral support: portion of broad ligament • Cardinal (lateral cervical ) ligaments – from cervix and superior vagina to lateral walls of pelvis • Uterosacral ligaments secure uterus to sacrum • Round ligaments bind to anterior wall © 2013 Pearson Education, Inc.
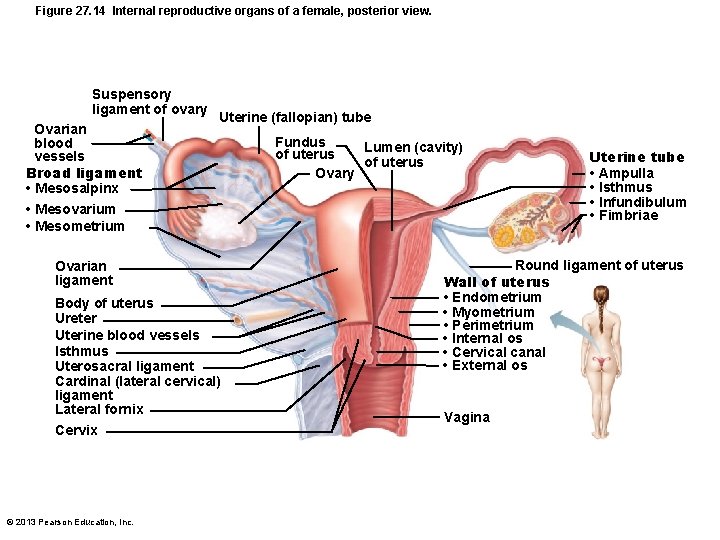
Figure 27. 14 Internal reproductive organs of a female, posterior view. Suspensory ligament of ovary Ovarian blood vessels Broad ligament • Mesosalpinx • Mesovarium • Mesometrium Uterine (fallopian) tube Ovarian ligament Body of uterus Ureter Uterine blood vessels Isthmus Uterosacral ligament Cardinal (lateral cervical) ligament Lateral fornix Cervix © 2013 Pearson Education, Inc. Fundus Lumen (cavity) of uterus Ovary Uterine tube • Ampulla • Isthmus • Infundibulum • Fimbriae Round ligament of uterus Wall of uterus • Endometrium • Myometrium • Perimetrium • Internal os • Cervical canal • External os Vagina

Peritoneal Pouches • Sacs of peritoneum exist around uterus – Vesicouterine pouch between bladder and uterus – Rectouterine pouch between rectum and uterus © 2013 Pearson Education, Inc.

Uterine Wall • Three layers – Perimetrium - serous layer (visceral peritoneum) – Myometrium - interlacing layers of smooth muscle – Endometrium - mucosal lining © 2013 Pearson Education, Inc.

Endometrium • Stratum functionalis (functional layer) – Changes in response to ovarian hormone cycles – Shed during menstruation • Stratum basalis (basal layer) – Forms new functionalis after menstruation – Unresponsive to ovarian hormones © 2013 Pearson Education, Inc.

Uterine Vascular Supply • Uterine arteries arise from internal iliacs; branch into • Arcuate arteries in myometrium; branch into • Radial arteries in endometrium; branch into • Straight arteries stratum basalis • Spiral arteries stratum functionalis – Degenerate and regenerate; spasms shedding of functionalis layer during menstruation © 2013 Pearson Education, Inc.
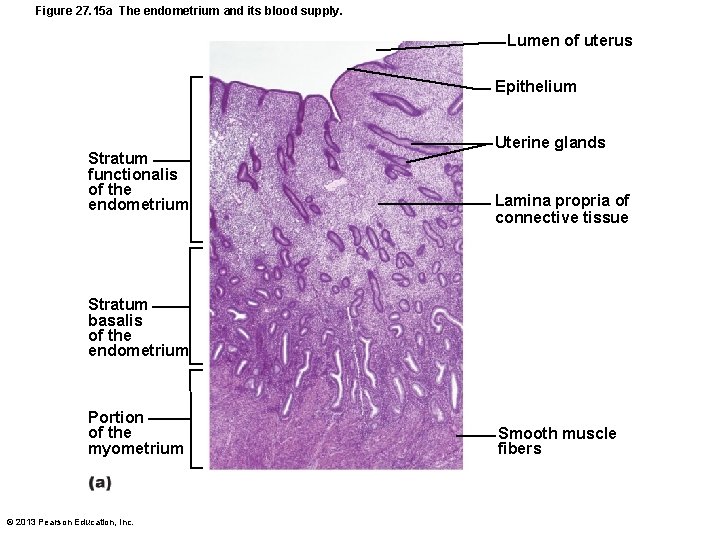
Figure 27. 15 a The endometrium and its blood supply. Lumen of uterus Epithelium Stratum functionalis of the endometrium Uterine glands Lamina propria of connective tissue Stratum basalis of the endometrium Portion of the myometrium © 2013 Pearson Education, Inc. Smooth muscle fibers
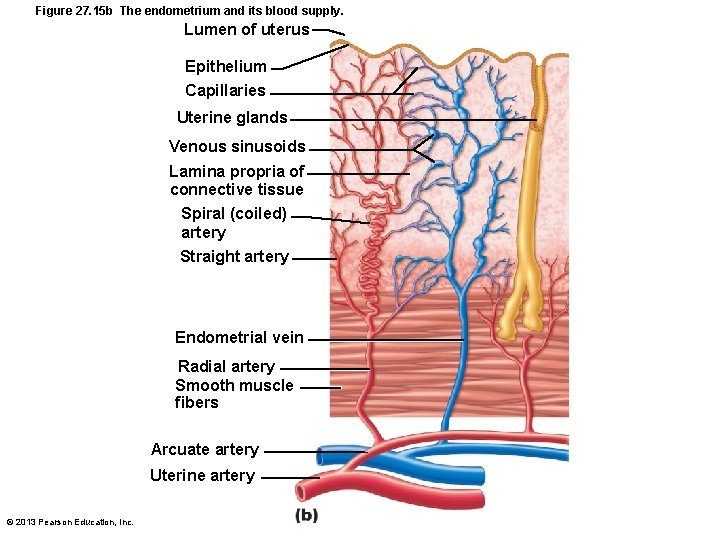
Figure 27. 15 b The endometrium and its blood supply. Lumen of uterus Epithelium Capillaries Uterine glands Venous sinusoids Lamina propria of connective tissue Spiral (coiled) artery Straight artery Endometrial vein Radial artery Smooth muscle fibers Arcuate artery Uterine artery © 2013 Pearson Education, Inc.

Vagina • Thin-walled tube 8 -10 cm in length • Birth canal and organ of copulation • Extends between bladder and rectum from cervix to exterior • Urethra parallels course anteriorly; embedded in anterior wall © 2013 Pearson Education, Inc.

Vagina • Layers of wall – Fibroelastic adventitia – Smooth muscle muscularis – Stratified squamous mucosa with rugae • Dendritic cells in mucosa may provide route for HIV transmission • Mucosa near vaginal orifice forms incomplete partition called hymen – ruptures with intercourse • Vaginal fornix - upper end of vagina surrounding cervix © 2013 Pearson Education, Inc.
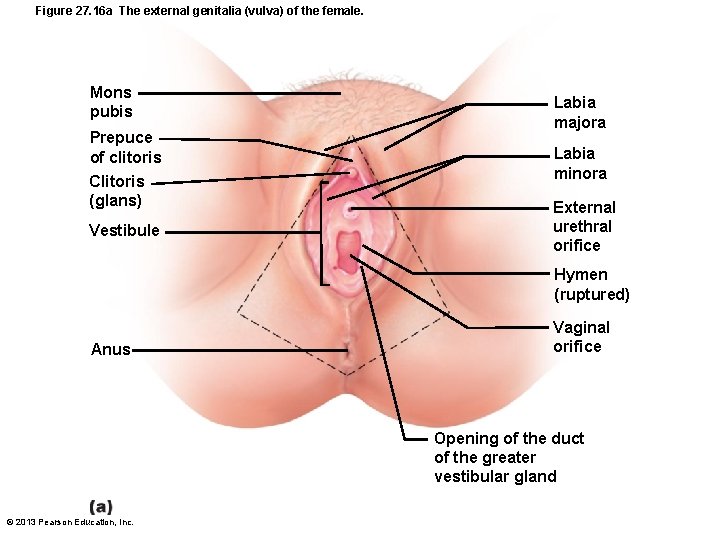
Figure 27. 16 a The external genitalia (vulva) of the female. Mons pubis Prepuce of clitoris Clitoris (glans) Vestibule Labia majora Labia minora External urethral orifice Hymen (ruptured) Anus Vaginal orifice Opening of the duct of the greater vestibular gland © 2013 Pearson Education, Inc.

External Genitalia (Vulva or Pudendum) • Mons pubis - fatty area overlying pubic symphysis • Labia majora - hair-covered, fatty skin folds – Counterpart of male scrotum • Labia minora - skin folds lying within labia majora – Join at posterior end of vestibule fourchette – Vestibule - recess within labia minora © 2013 Pearson Education, Inc.

External Genitalia • Greater vestibular glands – Flank vaginal opening – Homologous to bulbourethral glands – Release mucus into vestibule for lubrication © 2013 Pearson Education, Inc.

External Genitalia • Clitoris – anterior to vestibule – Glans of the clitoris - exposed portion – Prepuce of the clitoris – hoods glans – Counterpart of penis • Perineum – Diamond-shaped region between pubic arch and coccyx – Bordered by ischial tuberosities laterally © 2013 Pearson Education, Inc.
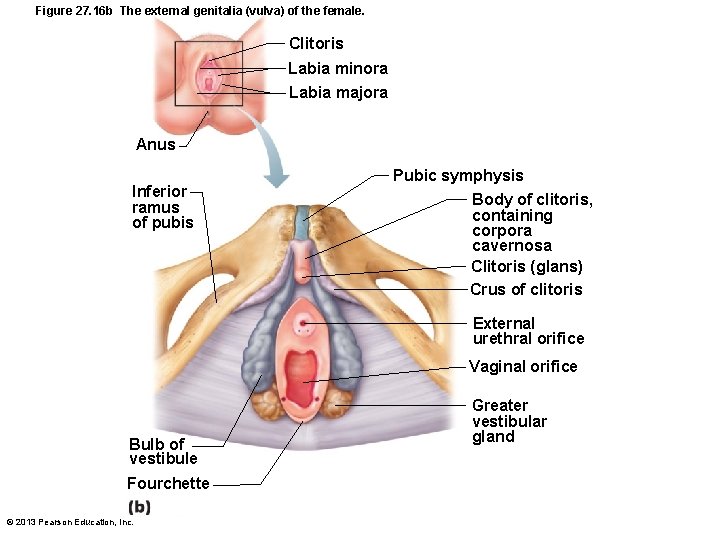
Figure 27. 16 b The external genitalia (vulva) of the female. Clitoris Labia minora Labia majora Anus Inferior ramus of pubis Pubic symphysis Body of clitoris, containing corpora cavernosa Clitoris (glans) Crus of clitoris External urethral orifice Vaginal orifice Bulb of vestibule Fourchette © 2013 Pearson Education, Inc. Greater vestibular gland

Mammary Glands • Modified sweat glands consisting of 15– 25 lobes • Function in milk production • Areola - pigmented skin surrounding nipple • Suspensory ligaments – attach breast to underlying muscle • Lobules within lobes contain glandular alveoli that produce milk © 2013 Pearson Education, Inc.

Mammary Glands • Milk lactiferous ducts lactiferous sinuses open to outside at nipple • Breast size due to amount of fat deposits © 2013 Pearson Education, Inc.
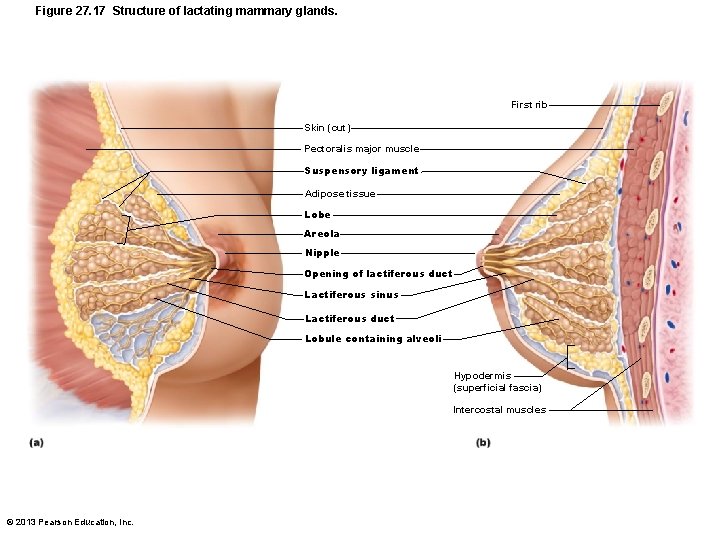
Figure 27. 17 Structure of lactating mammary glands. First rib Skin (cut) Pectoralis major muscle Suspensory ligament Adipose tissue Lobe Areola Nipple Opening of lactiferous duct Lactiferous sinus Lactiferous duct Lobule containing alveoli Hypodermis (superficial fascia) Intercostal muscles © 2013 Pearson Education, Inc.

Breast Cancer • Invasive breast cancer most common malignancy, second most common cause of cancer death in U. S. women • 13% will develop condition © 2013 Pearson Education, Inc.

Breast Cancer • Usually arises from epithelial cells of smallest ducts; eventually metastasize • Risk factors include – Early onset of menstruation and late menopause – No pregnancies or first pregnancy late in life – No or short periods of breast feeding – Family history of breast cancer • 70% of women with breast cancer have no known risk factors © 2013 Pearson Education, Inc.

Breast Cancer • 10% due to hereditary defects, including mutations to genes BRCA 1 and BRCA 2 – 50 – 80% develop breast cancer – Greater risk of ovarian cancer as well © 2013 Pearson Education, Inc.

Breast Cancer: Diagnosis • Early detection via self-examination and mammography – X-ray examination – American Cancer Society recommends screening every year for women 40 and over – U. S. Prevention Services Task Force on Breast Cancer Screening recommends 50 and over © 2013 Pearson Education, Inc.

Breast Cancer: Treatment • Treatment depends upon characteristics of lesion – Radiation; chemotherapy; surgery, often followed by radiation or chemotherapy to destroy stray cells – Drugs for estrogen-responsive cancers • Trastuzumab – for aggressive cancer cells • Tamoxifen – improves outcome for premenopausal women with early- or late-stage • Letrozole – reduces recurrence © 2013 Pearson Education, Inc.

Breast Cancer: Treatment • Radical mastectomy – removes breast, all underlying muscles, fascia, associated lymph nodes • Lumpectomy – excises only cancerous lump • Simple mastectomy – removes only breast tissue, sometimes some axillary lymph nodes • Some have breast reconstruction © 2013 Pearson Education, Inc.
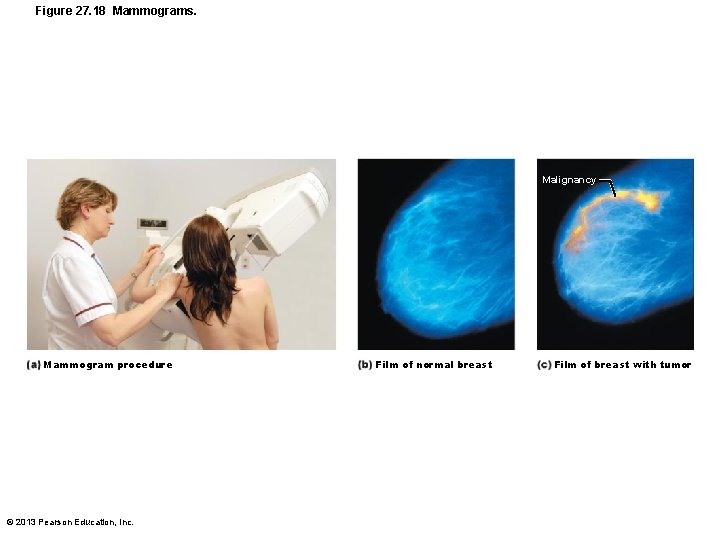
Figure 27. 18 Mammograms. Malignancy Mammogram procedure © 2013 Pearson Education, Inc. Film of normal breast Film of breast with tumor

Physiology of the Female Reproductive System • Always assumed females total supply of eggs determined at birth • New evidence stem cells can arise from epithelial cells at ovary surface • May overturn previous assumption © 2013 Pearson Education, Inc.

Oogenesis • Production of female gametes – Takes years to complete • Begins in fetal period – Oogonia (2 n ovarian stem cells) multiply by mitosis and store nutrients – Primary oocytes develop in primordial follicles – Primary oocytes begin meiosis; stall in prophase I © 2013 Pearson Education, Inc.

Oogenesis • At birth female presumed to have lifetime supply of primary oocytes • Each month after puberty, a few primary oocytes activated • One "selected" each month to resume meiosis I • Result is two haploid cells of different sizes – Secondary oocyte – large cell with ~ all cytoplasm and organelles of original cell – First polar body – small cell © 2013 Pearson Education, Inc.

Oogenesis • Secondary oocyte arrests in metaphase II; ovulated ovum • If not penetrated by sperm - deteriorates • If penetrated by sperm second oocyte completes meiosis II, yielding – Ovum (functional gamete) – Second polar body © 2013 Pearson Education, Inc.
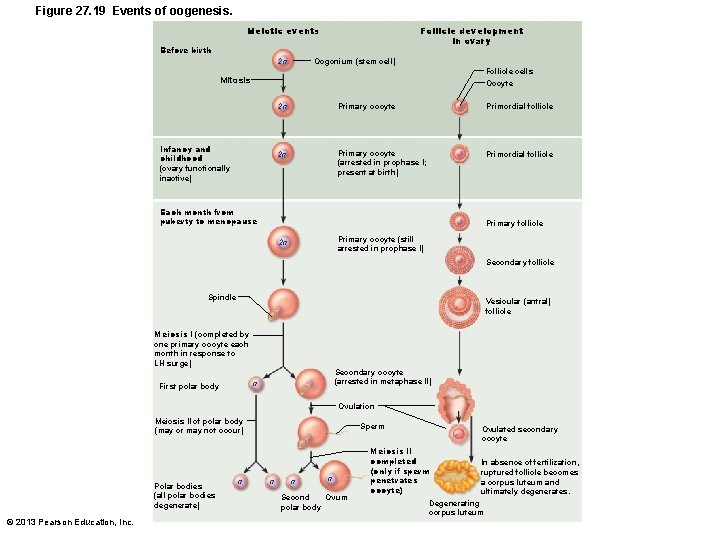
Figure 27. 19 Events of oogenesis. Follicle development in ovary Meiotic events Before birth Oogonium (stem cell) 2 n Follicle cells Oocyte Mitosis Infancy and childhood (ovary functionally inactive) 2 n Primary oocyte Primordial follicle 2 n Primary oocyte (arrested in prophase I; present at birth) Primordial follicle Each month from puberty to menopause Primary follicle Primary oocyte (still arrested in prophase I) 2 n Secondary follicle Spindle Vesicular (antral) follicle Meiosis I (completed by one primary oocyte each month in response to LH surge) Secondary oocyte (arrested in metaphase II) n First polar body Ovulation Meiosis II of polar body (may or may not occur) Polar bodies (all polar bodies degenerate) © 2013 Pearson Education, Inc. n Sperm n n n Second Ovum polar body Ovulated secondary oocyte Meiosis II completed (only if sperm penetrates oocyte) In absence of fertilization, ruptured follicle becomes a corpus luteum and ultimately degenerates. Degenerating corpus luteum

Comparison of Oogenesis and Spermatogenesis • Spermatogenesis 4 viable sperm • Spermatogenesis – error rate of 3 -4% • Oogenesis 1 viable gamete; 3 polar bodies • Oogenesis – error rate of 20% • Unequal divisions ensure oocyte has ample nutrients for 6 -7 day journey to uterus • Polar bodies degenerate and die © 2013 Pearson Education, Inc.

Ovarian Cycle • Monthly series of events associated with maturation of egg • Two consecutive phases (in 28 -day cycle) – Follicular phase - period of follicle growth (days 1– 14) – Ovulation occurs midcycle – Luteal phase - period of corpus luteum activity (days 14– 28) © 2013 Pearson Education, Inc.

Ovarian Cycle • Only 10 – 15% women have 28 -day cycle • Follicular phase varies • Luteal phase constant – always 14 days from ovulation to end of cycle © 2013 Pearson Education, Inc.

Follicular Phase • Primordial follicle becomes primary follicle – Squamouslike cells become cuboidal; oocyte enlarges • Primary follicle becomes secondary follicle – Stratified epithelium (granulosa cells) forms around oocyte – Granulosa cells and oocyte guide one another's development via gap junctions © 2013 Pearson Education, Inc.
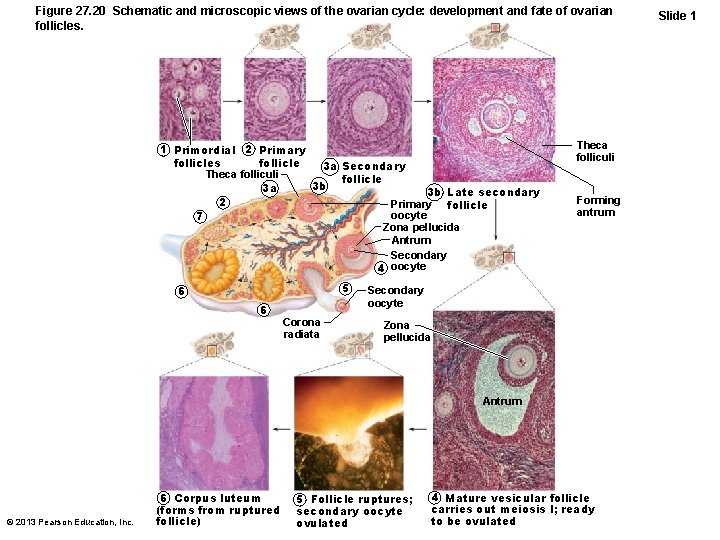
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. 1 Primordial 2 Primary follicles 3 a Secondary Theca folliculi follicle 3 b 3 a 3 b Late secondary 2 Primary follicle oocyte 7 Zona pellucida Antrum Secondary 4 oocyte 5 6 6 Corona radiata Theca folliculi Forming antrum Secondary oocyte Zona pellucida Antrum © 2013 Pearson Education, Inc. 6 Corpus luteum (forms from ruptured follicle) 5 Follicle ruptures; secondary oocyte ovulated 4 Mature vesicular follicle carries out meiosis I; ready to be ovulated Slide 1
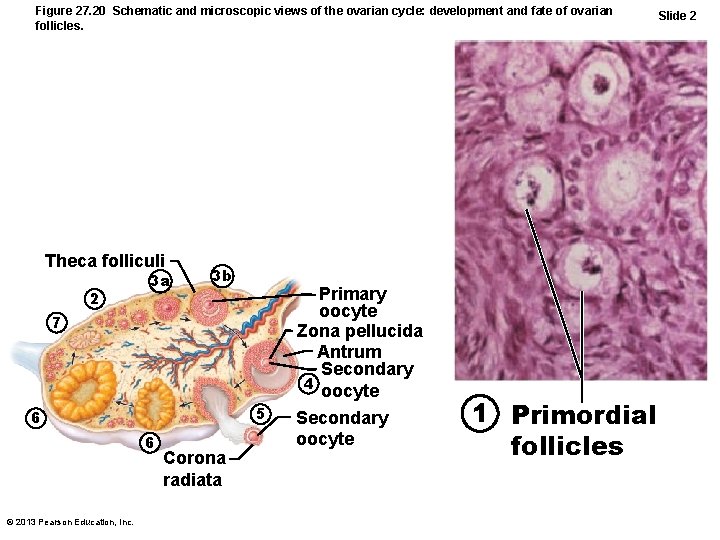
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 2 3 a 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Corona radiata Secondary oocyte 1 Primordial follicles Slide 2
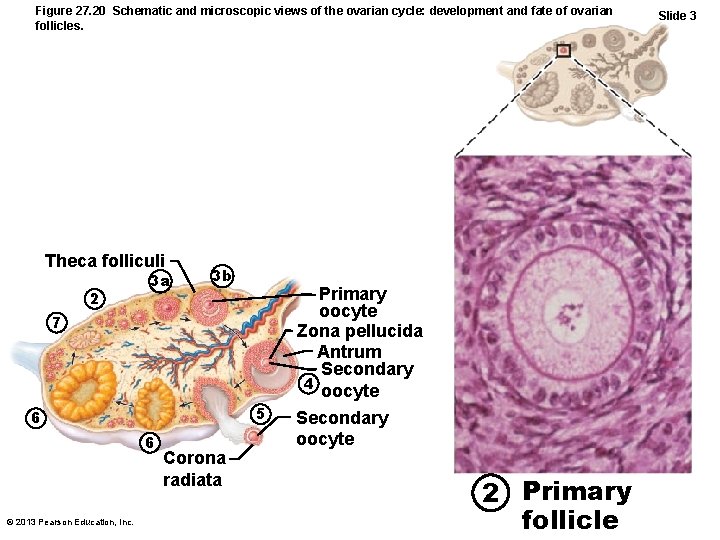
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 2 3 a 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Corona radiata Secondary oocyte 2 Primary follicle Slide 3
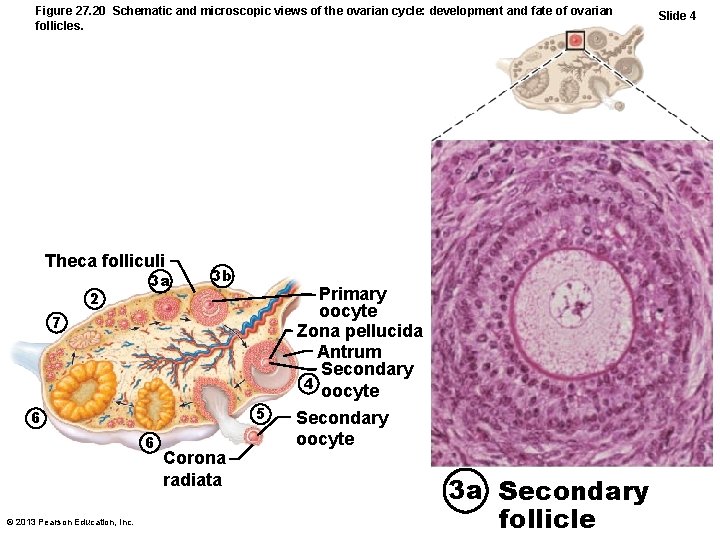
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 2 3 a 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Corona radiata Secondary oocyte 3 a Secondary follicle Slide 4

Follicular Phase • Secondary follicle becomes late secondary follicle – Connective tissue (theca folliculi) and granulosa cells cooperate to produce estrogens – Inner thecal cells produce androgens in response to LH – Zona pellucida forms around oocyte – Fluid accumulates between granulosa cells © 2013 Pearson Education, Inc.
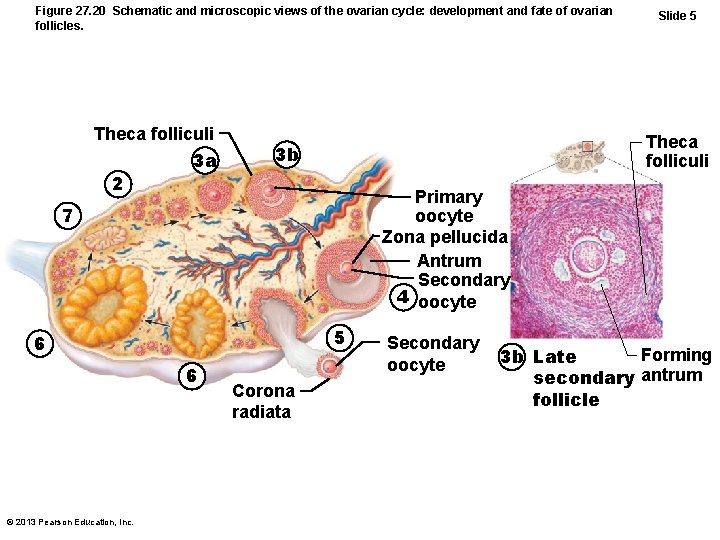
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 3 a 2 Theca folliculi 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Slide 5 Corona radiata Secondary oocyte Forming 3 b Late secondary antrum follicle

Follicular Phase • Late secondary follicle becomes vesicular follicle – Antrum forms; expands to isolate oocyte with corona radiata on stalk – Vesicular follicle bulges from external surface of ovary – Primary oocyte completes meiosis I secondary oocyte and first polar body © 2013 Pearson Education, Inc.
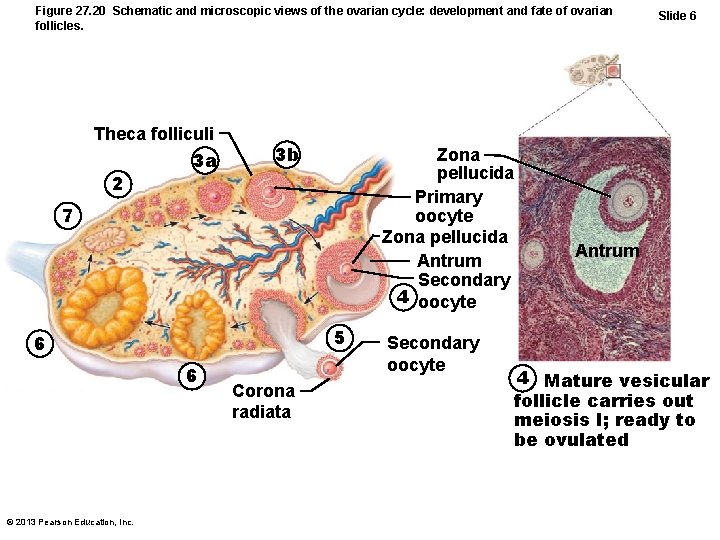
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 3 a 2 3 b Zona pellucida Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Corona radiata Secondary oocyte Slide 6 Antrum 4 Mature vesicular follicle carries out meiosis I; ready to be ovulated 4

Ovulation • Ovary wall ruptures, expels secondary oocyte with its corona radiata to peritoneal cavity • Mittelschmerz - twinge of pain sometimes felt at ovulation • 1– 2% of ovulations release more than one secondary oocyte, which, if fertilized, results in fraternal twins • Identical twins result from fertilization of one oocyte, then separation of daughter cells © 2013 Pearson Education, Inc.
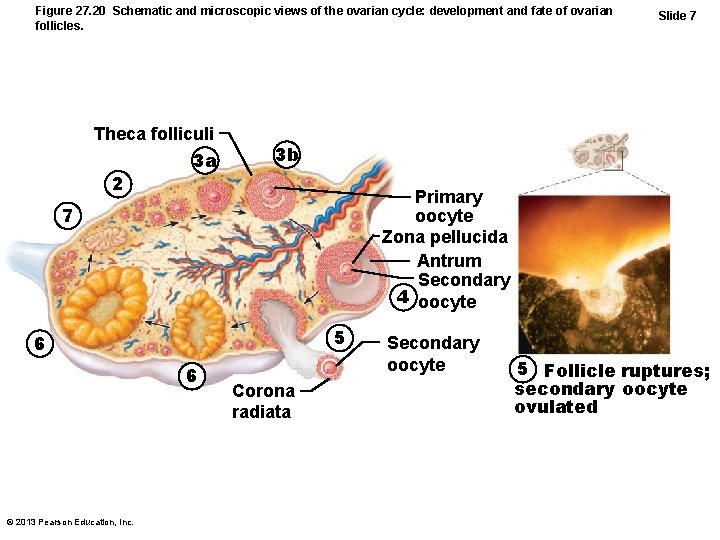
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 3 a 2 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Slide 7 Corona radiata Secondary oocyte 5 Follicle ruptures; secondary oocyte ovulated

Luteal Phase of the Ovarian Cycle • Ruptured follicle collapses; antrum fills with clotted blood – corpus hemorrhagicum • Granulosa cells and internal thecal cells form corpus luteum • Corpus luteum secretes progesterone and some estrogen © 2013 Pearson Education, Inc.

Luteal Phase • If no pregnancy, corpus luteum degenerates into corpus albicans (scar) in 10 days • If pregnancy occurs, corpus luteum produces hormones that sustain pregnancy until placenta takes over at about 3 months © 2013 Pearson Education, Inc.
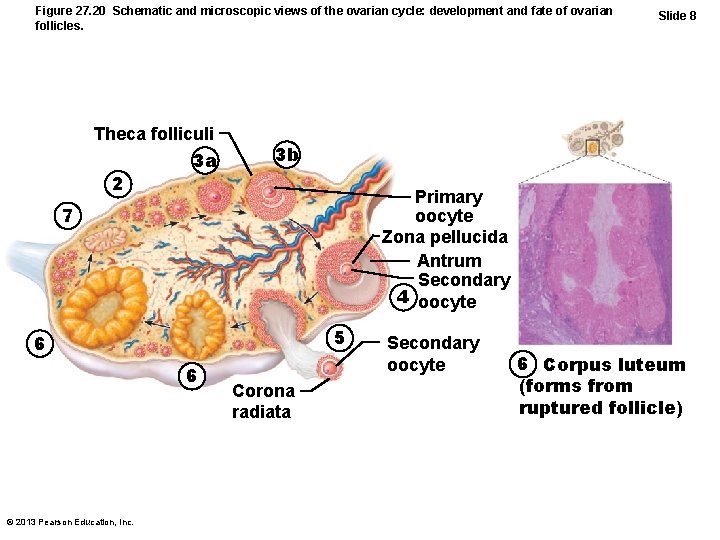
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. Theca folliculi 3 a 2 3 b Primary oocyte Zona pellucida Antrum Secondary 4 oocyte 7 5 6 6 © 2013 Pearson Education, Inc. Slide 8 Corona radiata Secondary oocyte 6 Corpus luteum (forms from ruptured follicle)
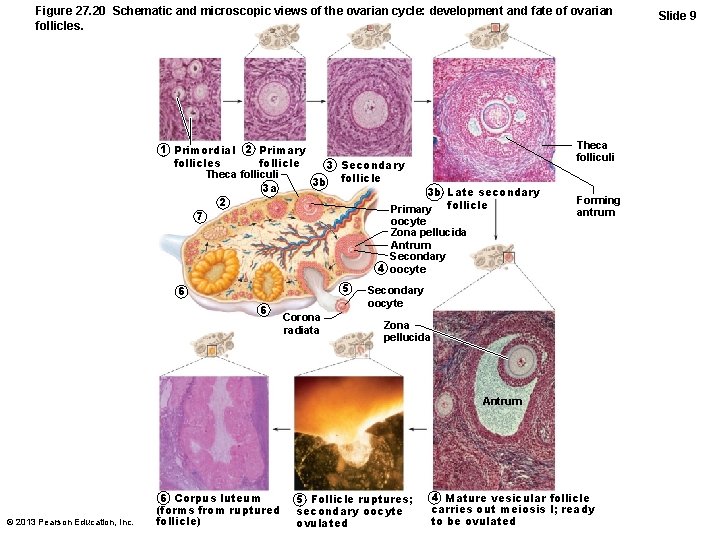
Figure 27. 20 Schematic and microscopic views of the ovarian cycle: development and fate of ovarian follicles. 1 Primordial 2 Primary follicles 3 Secondary Theca folliculi 3 b follicle 3 a 3 b Late secondary 2 Primary follicle 7 oocyte Zona pellucida Antrum Secondary 4 oocyte 5 6 6 Corona radiata Theca folliculi Forming antrum Secondary oocyte Zona pellucida Antrum © 2013 Pearson Education, Inc. 6 Corpus luteum (forms from ruptured follicle) 5 Follicle ruptures; secondary oocyte ovulated 4 Mature vesicular follicle carries out meiosis I; ready to be ovulated Slide 9
- Slides: 85