Male Reproductive Anatomy of Cattle By C Kohn

Male Reproductive Anatomy of Cattle By C. Kohn, Waterford WI
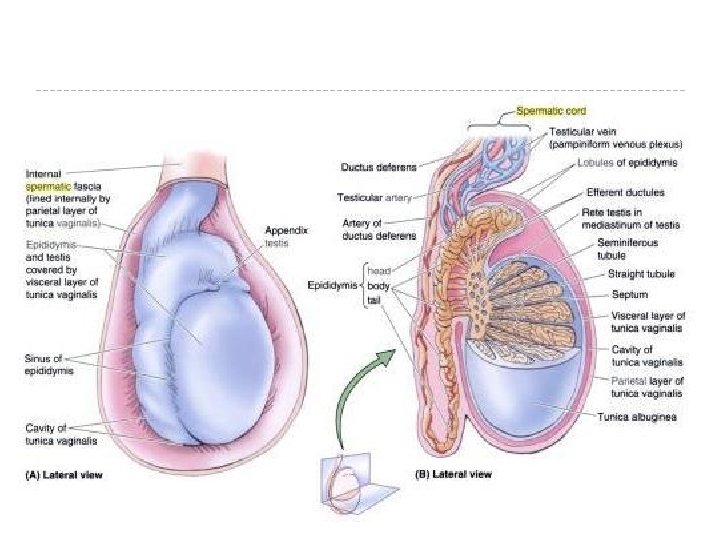
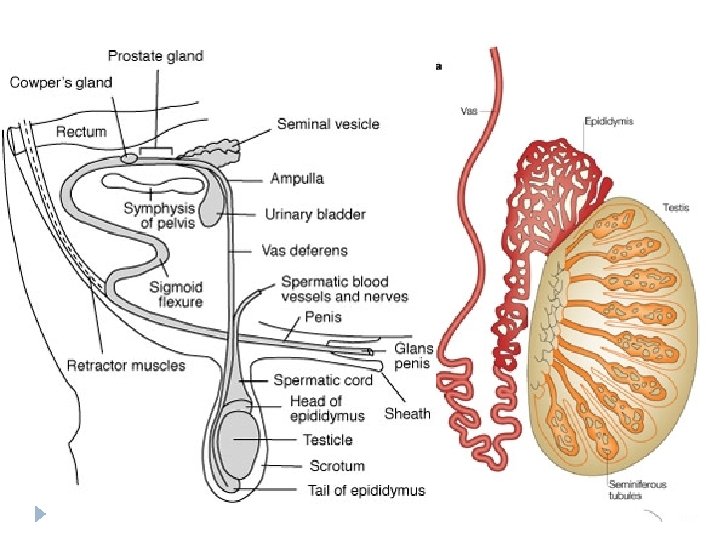
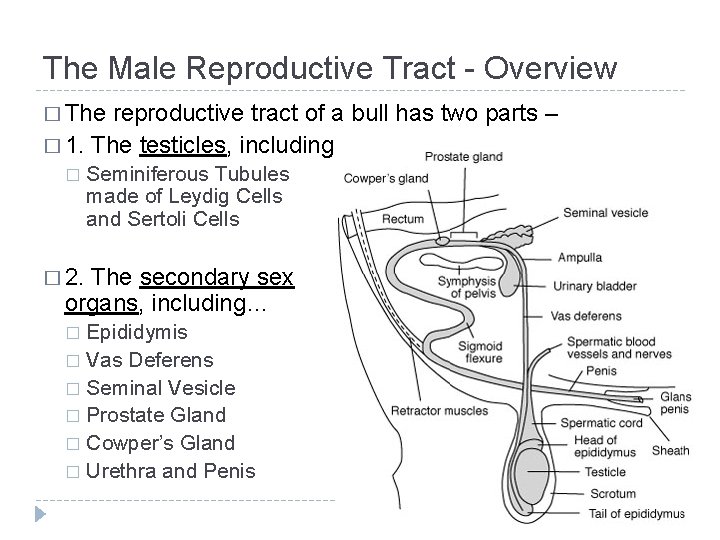
The Male Reproductive Tract - Overview � The reproductive tract of a bull has two parts – � 1. The testicles, including � Seminiferous Tubules made of Leydig Cells and Sertoli Cells � 2. The secondary sex organs, including… Epididymis � Vas Deferens � Seminal Vesicle � Prostate Gland � Cowper’s Gland � Urethra and Penis �
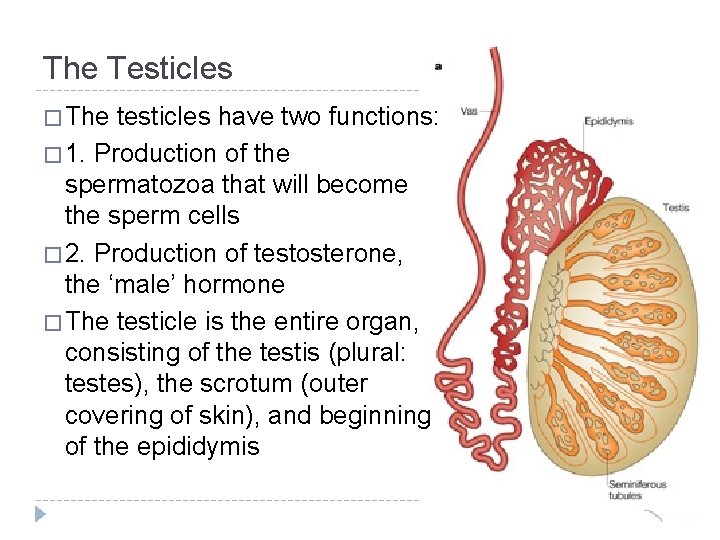
The Testicles � The testicles have two functions: � 1. Production of the spermatozoa that will become the sperm cells � 2. Production of testosterone, the ‘male’ hormone � The testicle is the entire organ, consisting of the testis (plural: testes), the scrotum (outer covering of skin), and beginning of the epididymis
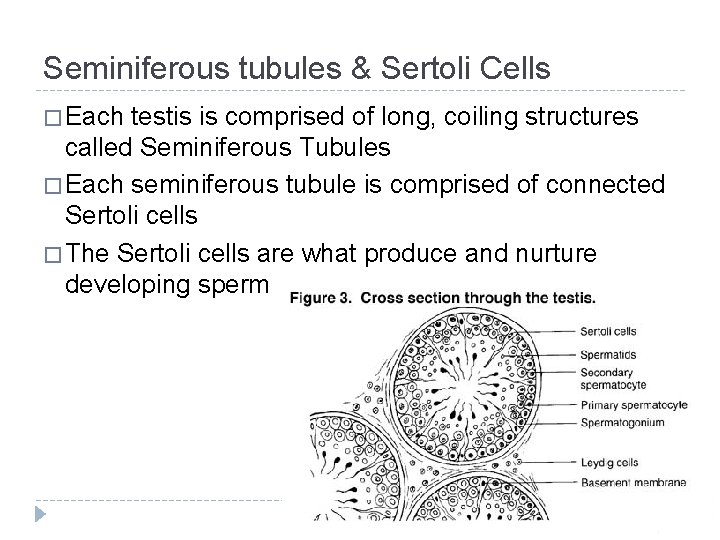
Seminiferous tubules & Sertoli Cells � Each testis is comprised of long, coiling structures called Seminiferous Tubules � Each seminiferous tubule is comprised of connected Sertoli cells � The Sertoli cells are what produce and nurture developing sperm
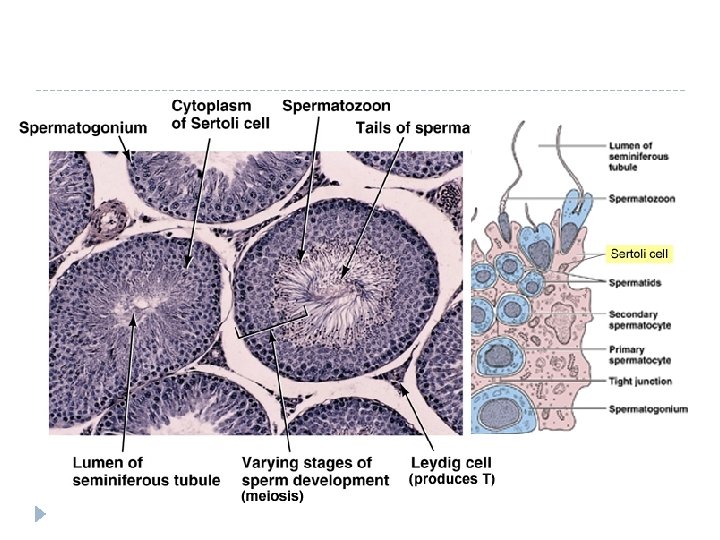
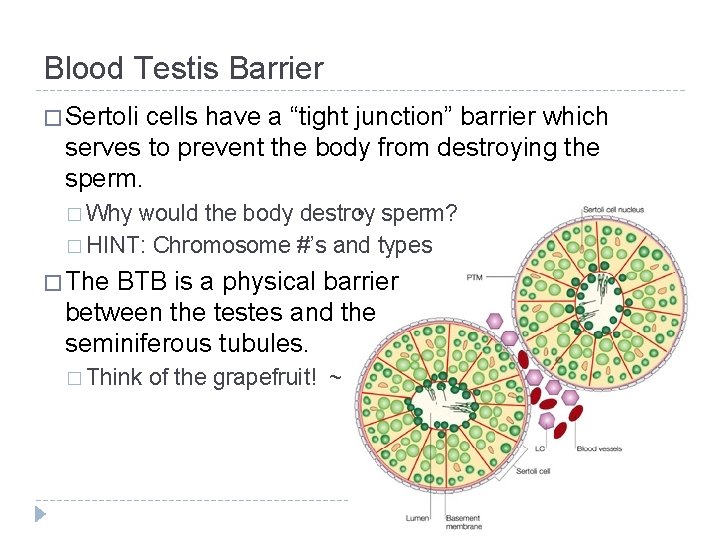
Blood Testis Barrier � Sertoli cells have a “tight junction” barrier which serves to prevent the body from destroying the sperm. � Why would the body destroy sperm? � HINT: Chromosome #’s and types � The BTB is a physical barrier between the testes and the seminiferous tubules. � Think of the grapefruit! ~
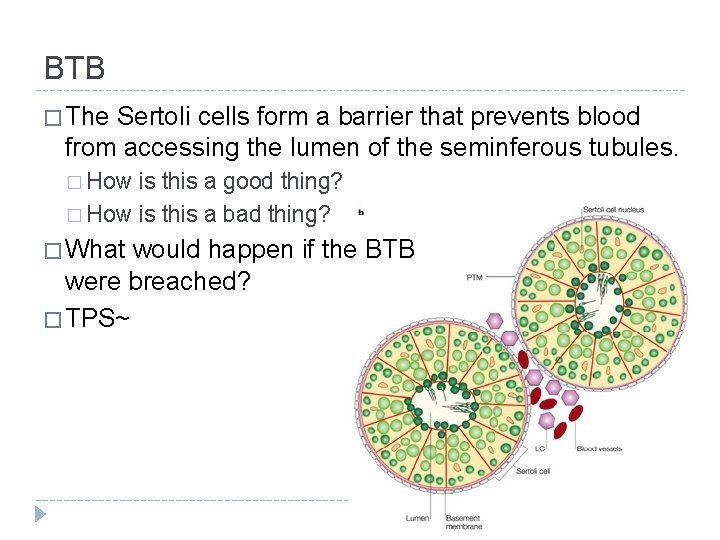
BTB � The Sertoli cells form a barrier that prevents blood from accessing the lumen of the seminferous tubules. � How is this a good thing? � How is this a bad thing? � What would happen if the BTB were breached? � TPS~
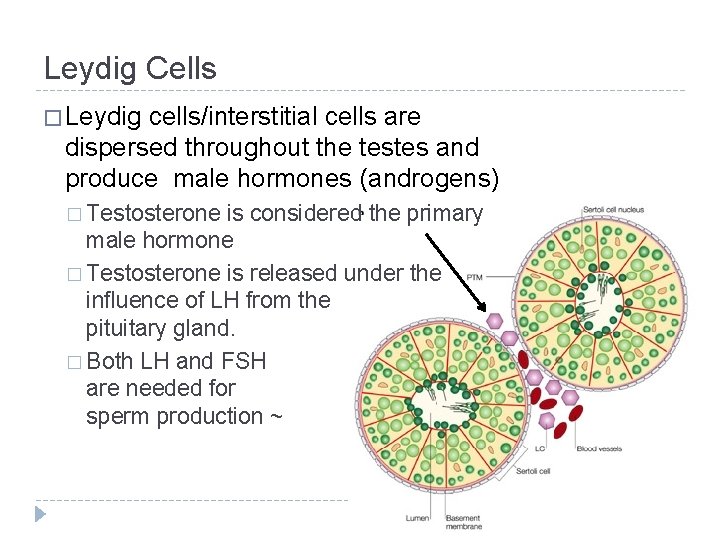
Leydig Cells � Leydig cells/interstitial cells are dispersed throughout the testes and produce male hormones (androgens) � Testosterone is considered the primary male hormone � Testosterone is released under the influence of LH from the pituitary gland. � Both LH and FSH are needed for sperm production ~

Male Hormones � Male Hormones are necessary for: � Onset and maintenance of sperm production � Sex drive (libido) � Development and maintenance of secondary sex characteristics (organs and features) ~ � After puberty, spermatozoa formation is a continuous process. � This � FSH process is controlled by the endocrine system. and LH are important in stimulating the testes to produce spermatozoa and testosterone. ~
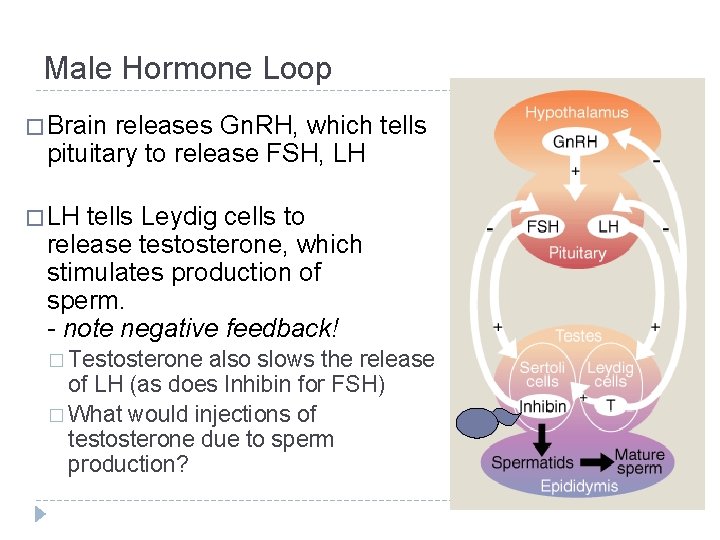
Male Hormone Loop � Brain releases Gn. RH, which tells pituitary to release FSH, LH � LH tells Leydig cells to release testosterone, which stimulates production of sperm. - note negative feedback! � Testosterone also slows the release of LH (as does Inhibin for FSH) � What would injections of testosterone due to sperm production?

Male Hormone Cycle � 1. Brain releases Gn. RH � 2. Gn. RH causes release of LH, FSH � 3. LH causes release of testosterone from Leydig Cells � 4. Testosterone causes production of sperm in Sertoli Cells (as well as production of Inhibin) � 5. Testosterone reduces production of LH; Inhibin reduces production of FSH

Temperature Control � The testicles must located outside of the male’s body as normal sperm formation occurs at a temperature several degrees below normal body temperature � Very cold temperatures can also damage the scrotum. � To keep the testicles at the proper temperature, the cremaster muscle suspends or retracts to move the testicles closer to or further from the body � Testosterone causes this response; no testosterone, no cremaster function � This muscle can be damaged or other injury or malformation can prevent one or both testicles from descending. This condition is called cryptorchidism � An individual with this condition will be partially or fully sterile and this individual should not be allowed to breed.

Causes of sterility � Conditions other than cryptorchidism can also cause sterility in males, including � - excessive fat deposits in the scrotum � - a very high fever or high fever over several days � - very hot weather for an extended period of time � If the male was producing sperm prior to these occurrences, sperm production may resume after 610 weeks.
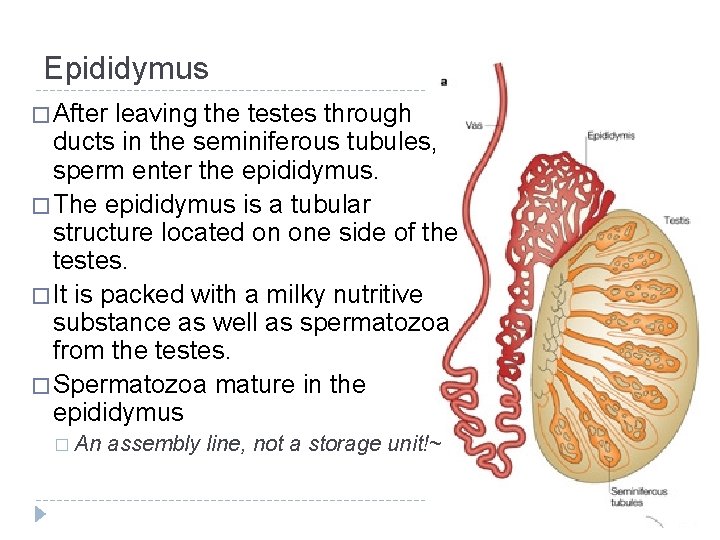
Epididymus � After leaving the testes through ducts in the seminiferous tubules, sperm enter the epididymus. � The epididymus is a tubular structure located on one side of the testes. � It is packed with a milky nutritive substance as well as spermatozoa from the testes. � Spermatozoa mature in the epididymus � An assembly line, not a storage unit!~
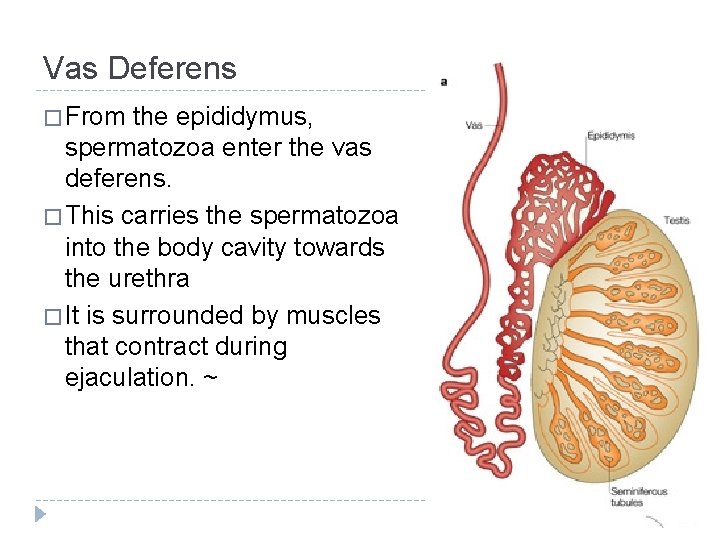
Vas Deferens � From the epididymus, spermatozoa enter the vas deferens. � This carries the spermatozoa into the body cavity towards the urethra � It is surrounded by muscles that contract during ejaculation. ~

Ampullae of Henle, Urethra �The vas deferens enlarges inside the pelvis to form the ampullae � Where spermatozoa are stored and mixed with a nutritive substance. �During copulation, sperm is moved into the urethra. � This is a common pathway for both urine and semen (the mix of the products of the testes and accessory glands. ) ~
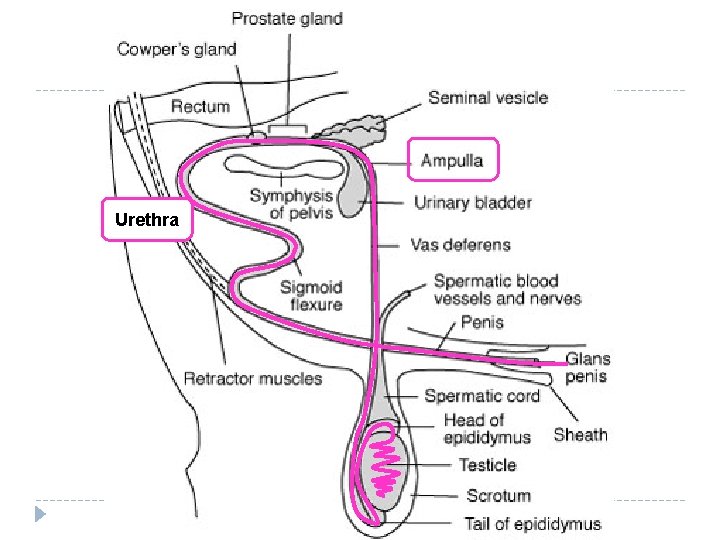
Urethra

Accessory Glands (3) � There � are three accessory glands: 1. Seminal Vesicles – secrete a fluid high in sugars (fructose) to nourish the spermatozoa – feels like a bag of grapes (palpation) � This fluid also dilutes sperm at ejaculation and serves to activate motility – the bulk of fluid production occurs here � Rich in proteins, fructose, enzymes. � Secretes prostaglandins, causing uterine contractions � 2. Prostate glands – Creates a basic p. H of 7. 5 -8 – protects sperm � 3. Cowper’s gland – lubricating & cleansing substance � Cleanse male and female reproductive tracts prior to passage of spermatozoa (King Sperm’s archers) � These secretions are released almost instantaneously � Yellowed cloudy semen secretions may indicated an infection in these glands
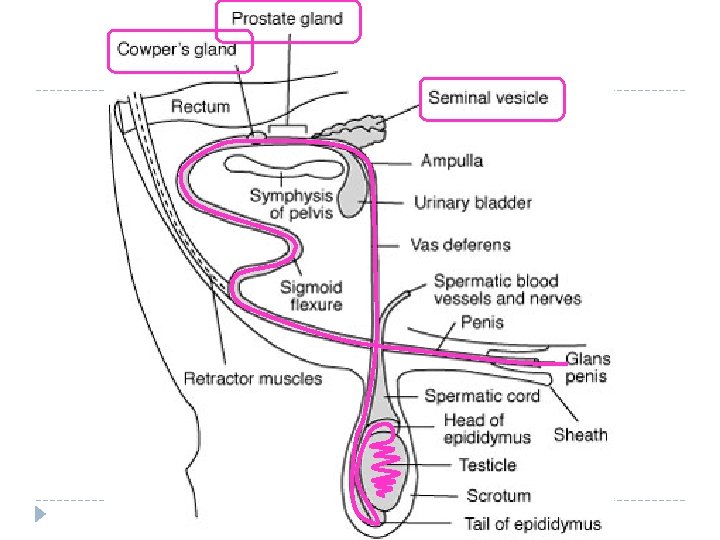

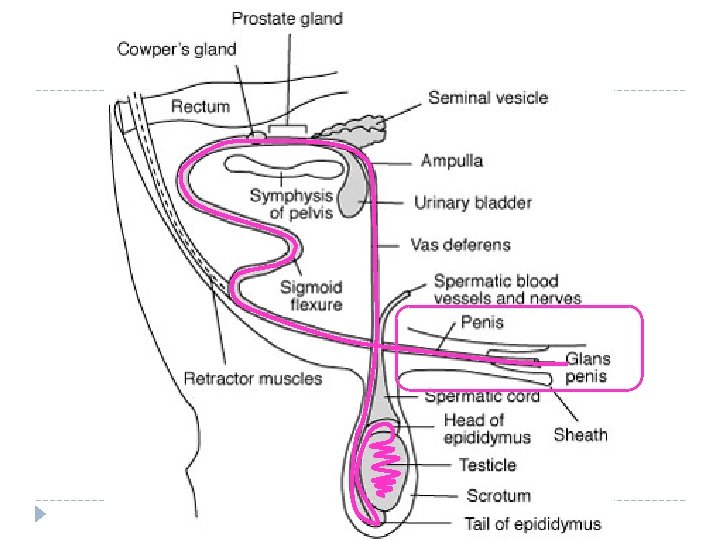
Urethra and Penis �The urethra extends to the tip of the penis, where it exits the body. �Urethra surrounded by smooth muscle – crucial for ejaculation. �Penis is composed of sponge-like blood tissue �Under sexual stimulation, this tissue fills with blood, enlarging it and enabling it to be inserted into a female’s vagina. � Otherwise, species ~ it is kept inside the body cavity in most

Briefly – EDC’s � Endocrine Disrupting Chemicals are a serious concern today. � These chemicals have similar chemical conformations to sex hormones and mimic their effects in the body. � What impact would this have on a body; remember negative feedback! ~

EDC’s � “To date, in vitro and in vivo studies have identified several antiandrogenic toxicants including vinclozolin, procymidone, linuron, several phthalate esters, and p, p’-DDE, all of which alter male rat sex differentiation. ” � Emerging Issues Related to Endocrine Disrupting Chemicals and Environmental Androgens and Antiandrogens � Gray, et. al. , US Environmental Protection Agency ~

A Concern � In humans and other mammals, male fertility has dropped significantly. � This has also been seen in cattle; it is much harder to breed a cow today than it was 50 years ago. � Furthermore, cases of sexual abnormalities have increased in amphibians and reptiles. � Is this genetic or environmental? ~

Sperm Situations �Sperm are not hardy; they are rather fragile cells �They are very susceptible to: � Heat � Jarring � Radiation � Poor Nutrition � Infrequent ejaculation (increases abnormalities) �A mature bull can ejaculate as much as 7 consecutive times without a severe reduction in spermatozoa

Infertility � Infertility is not immediately recognizable! � Symptoms may show 2. 5 -3 mo’s after! � It takes ~70 days to produce sperm, and over two weeks to travel through the epididymus. �A mature bull should produce 70 billion sperm/week. � The heavier the testes, the more sperm is produced.
- Slides: 28