FRCR Physics Lectures Diagnostic Radiology Lecture 1 An






























































- Slides: 99

FRCR: Physics Lectures Diagnostic Radiology Lecture 1 An introduction to radiography with X-rays and the X-ray tube Dr Tim Wood Clinical Scientist

Lecture aims • Revision of the physics of x-ray interactions and production • Describe how the x-ray tube is constructed and understand the importance of each component • Basic understanding of x-ray generators • Explain what factors affect the output of an x-ray tube

INTRODUCTION

A little bit of history… • Wilhelm Röntgen discovered X-rays on 8 th Nov 1895 • Took first medical X-ray of wife’s hand (22 nd Dec 1895) • Used to diagnose Eddie Mc. Carthy’s fractured left wrist on 3 rd Feb 1896 (20 min exposure) • Awarded first Nobel Prize in Physics in 1901 for his discovery of ‘Röntgen rays’

A little bit of history…

Thankfully, things improved!…

What is diagnostic radiology? ra·di·ol·o·gy The science dealing with X-rays and other highenergy radiation, especially the use of such radiation for the diagnosis and treatment of disease Origin: 1895– 1900; radio- + -logy Related forms: ra·di·ol·o·gist, noun

What is diagnostic radiology? • The underlying principle of the majority of diagnostic radiological techniques is that X-rays display differential attenuation in matter – When the X-ray beam is targeted at a patient, the different tissues in the body will remove a different number of Xrays from the beam • The resulting modified X-ray flux can then be ‘captured’ by some form of detector to produce a latent image or radiation measurement – Detection may be through film, phosphor screens, digital detectors, etc

X-ray Properties • • Electromagnetic photons of radiation Emitted with various energies & wavelengths not detectable to the human senses Travel radially from their source (in straight lines) at the speed of light Can travel in a vacuum Display differential attenuation by matter The shorter the wavelength, the higher the energy and hence, more penetrating Can cause ionisation in matter Produce a ‘latent’ image on film/detector

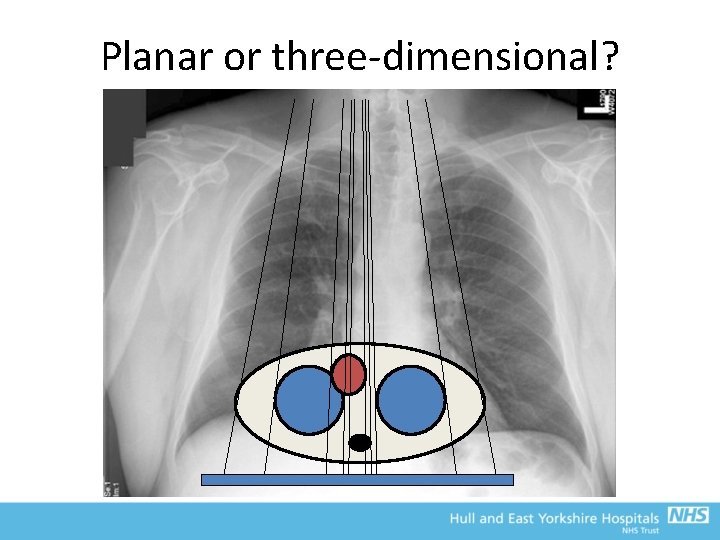
Planar or three-dimensional? • Planar imaging is the most common technique used in diagnostic radiology – – General radiography e. g. PA chest Mammography screening Intra-oral dental radiography Fluoroscopy (but some modern ones can do 3 D) • The anatomy that is in the path of the beam is all projected onto a single image plane – Tissues will overlap and may not be clearly visible – Contrast is generally poorer than in 3 D imaging techniques

Planar or three-dimensional?

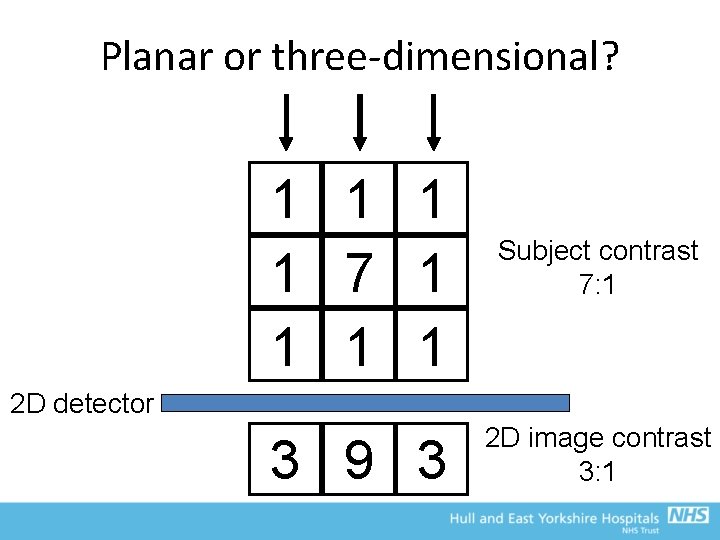
Planar or three-dimensional? 1 1 7 1 1 Subject contrast 7: 1 3 9 3 2 D image contrast 3: 1 2 D detector

Planar or three-dimensional? • 3 D imaging offers superior contrast to 2 D • More techniques are becoming available – Computed Tomography (CT), Cone beam CT, Tomosynthesis, etc • Compromise is that doses tend to be much higher than the planar image – e. g. CT chest = 6. 6 m. Sv c. f. PA chest = 0. 02 m. Sv (a factor of 330 difference!) • Hence, despite being less common, they account for a significant proportion of the UK populations exposure to medical radiation – CT accounts for 11% of examinations, but 68% of dose (HPA 2008 review)

X-ray interactions with matter • It is the physics of the interactions with matter that determine how each imaging technique works, and how it is used in clinical practice • So, a bit of revision…

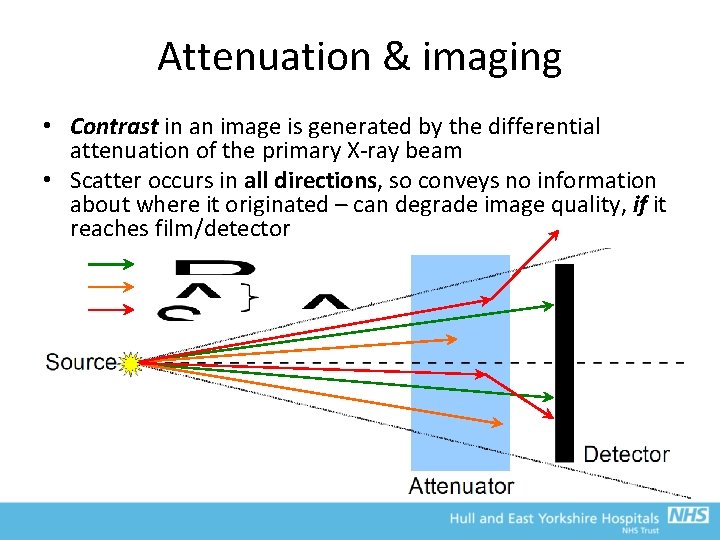
Attenuation & imaging • Contrast in an image is generated by the differential attenuation of the primary X-ray beam • Scatter occurs in all directions, so conveys no information about where it originated – can degrade image quality, if it reaches film/detector

Attenuation • For a mono-energetic photon beam: where, I = final intensity, I 0 = incident intensity, µ = attenuation coefficient, x = thickness • Equal thicknesses of material reduce the intensity by the same fraction (half-value thickness).

Attenuation • Attenuation coefficient, µ, decreases with increasing photon energy (except for absorption edges) • Increases with atomic number of material, Z • Increases with density of material, ρ • Transmission of radiation @ 70 k. Vp; – 1 cm of soft tissue 66% transmitted – 1 cm bone 17% transmitted – 1 cm tooth 6% transmitted

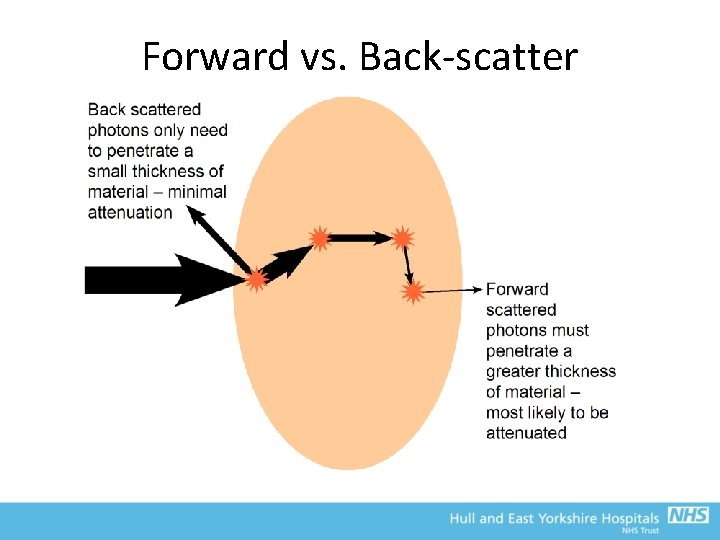
Forward vs. Back-scatter • Forward scatter is most likely, but. . . • Forward scatter is attenuated by the patient, and • Deeper layers receive a smaller intensity, so there are fewer scattering events • Overall, see more back scatter. • Advantage for image quality (less scatter, but more attenuation at the detector), but may pose a risk in terms of radiation protection

Forward vs. Back-scatter

Interaction Processes • Elastic scattering • Photoelectric effect • Compton effect

Elastic Scatter • • Photon energy smaller than BE Causes e- to vibrate – re-radiates energy No absorption, only scatter < 10% of total interactions in diagnostic range i. e. not significant

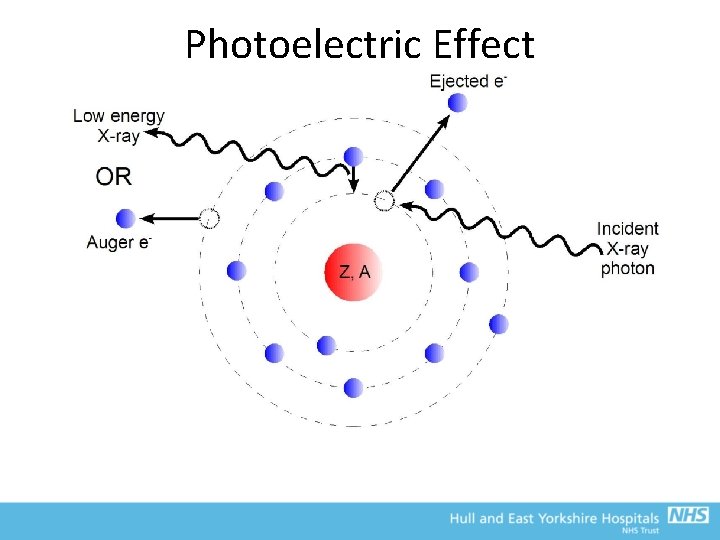
Photoelectric Effect • Process of complete absorption • ~30% of interactions in diagnostic range • Energy is transferred to bound e-, which is ejected at a velocity determined by difference in photon and BE • e- dissipates energy locally, and is responsible for biological damage • Hence, main source of radiographic contrast (and dose), and why Lead is used in protection

Photoelectric Effect

Photoelectric Effect • Leaves atom in unstable state – electronic reconfiguration results in emission of X-ray or Auger electron • Auger emission more probable for low Z material – short range in tissue (= more biological damage) • Low energy X-rays reabsorbed locally • Rapid fall-off with increasing energy

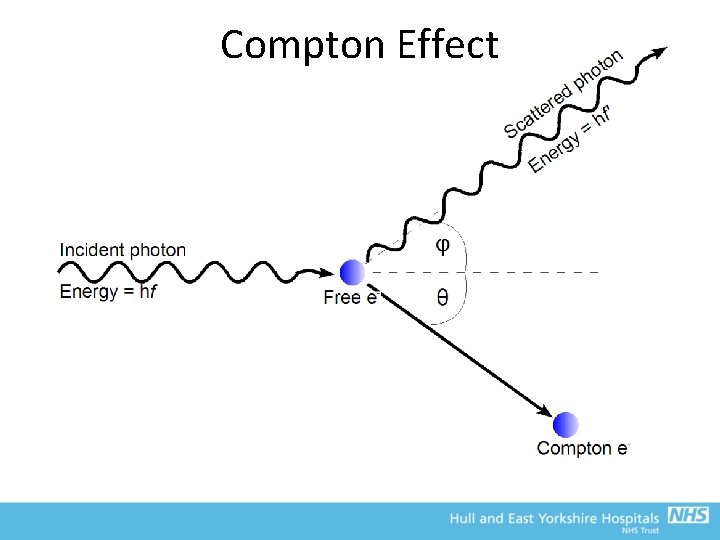
Compton Effect • Process of scatter and partial absorption – inelastic scattering • Photon collides with a free electron (photon energy >> BE) • Loses small proportion of its energy and changes direction • Energy loss depends on scattering angle and initial photon energy • Photon free to undergo further interactions until completely absorbed (Photoelectric)

Compton Effect

Compton Effect • Compton scatter mass attenuation coefficient almost independent of energy over diagnostic range • Ratio of Z/A similar for most elements of biological interest (~0. 5) – offers little in terms of radiographic contrast

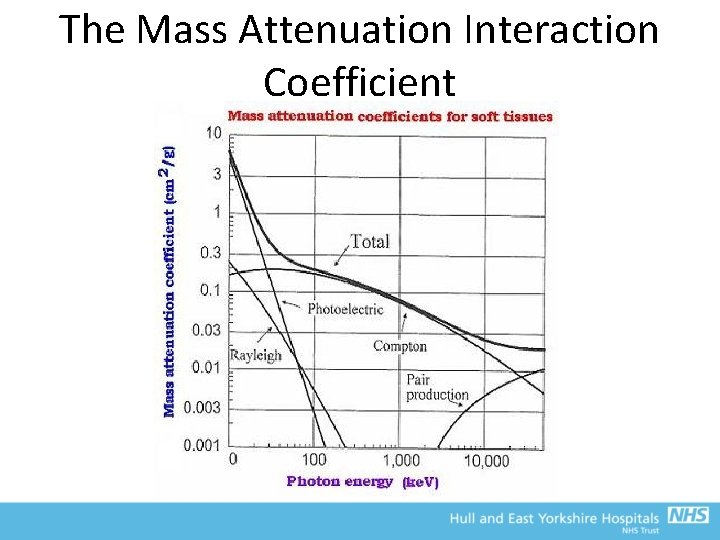
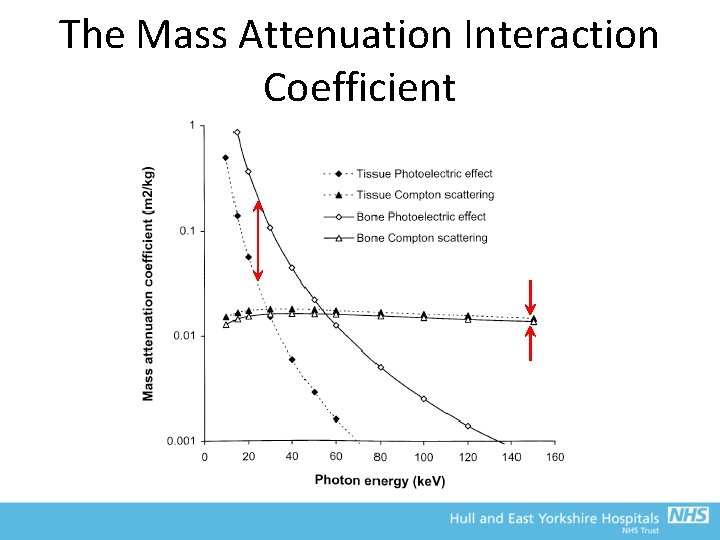
The Mass Attenuation Interaction Coefficient • Each process is independent – can add the interaction coefficients to give the total mass attenuation coefficient • Z dependence is the source of contrast in radiographic imaging

The Mass Attenuation Interaction Coefficient

The Mass Attenuation Interaction Coefficient

Maximising Radiographic Contrast • Maximise contrast due to Photoelectric absorption – use lower energy photon beams (note, it is the mean energy of the beam, not k. Vp that is important) • Use scatter rejection techniques such as scatter grids and air gaps • Limit beam to smallest area consistent with diagnostic task to minimise amount of scatter generated • BUT…

Maximising Radiographic Contrast • More Photoelectric absorption means higher patient dose • Scatter rejection techniques attenuate the primary beam, so a higher patient dose is required for acceptable image receptor dose • NEED TO BALANCE IMAGE QUALITY WITH PATIENT DOSE!!! • Hence, the principle of ALARA (As Low As Reasonably Achievable) – Use the highest energy beam that gives acceptable contrast, consistent with the clinical requirements

The X-ray tube

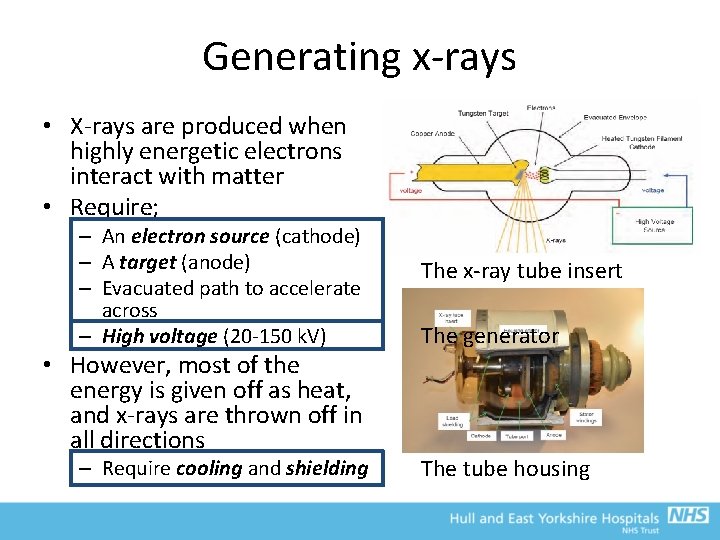
Generating x-rays • X-rays are produced when highly energetic electrons interact with matter • Require; – An electron source (cathode) – A target (anode) – Evacuated path to accelerate across – High voltage (20 -150 k. V) • However, most of the energy is given off as heat, and x-rays are thrown off in all directions – Require cooling and shielding The x-ray tube insert The generator The tube housing

A bit of revision… THE PHYSICS OF X-RAY PRODUCTION

The physics of X-ray production • Electron reaches the anode with kinetic energy equivalent to the accelerating potential (k. Vp) • Electrons penetrate several micrometres below the surface of the target and lose energy by a combination of processes – Large number of small energy losses to outer electrons of the atoms = heat – Account for about 99% of all energy dissipated from e- beam in the diagnostic range – Relatively few, but large energy loss X-ray producing interactions with inner shell electrons or the nucleus

Heat generating processes • When an electron (e-) strikes the target, most likely interaction is with loosely bound e-s that surround nuclei • Relatively weak interactions – slight deflection, ionisation or excitation • Small amount of energy transfer (per interaction) – observed as heat • However, accounts for ~99% of all energy dissipated from e- beam in the diagnostic range

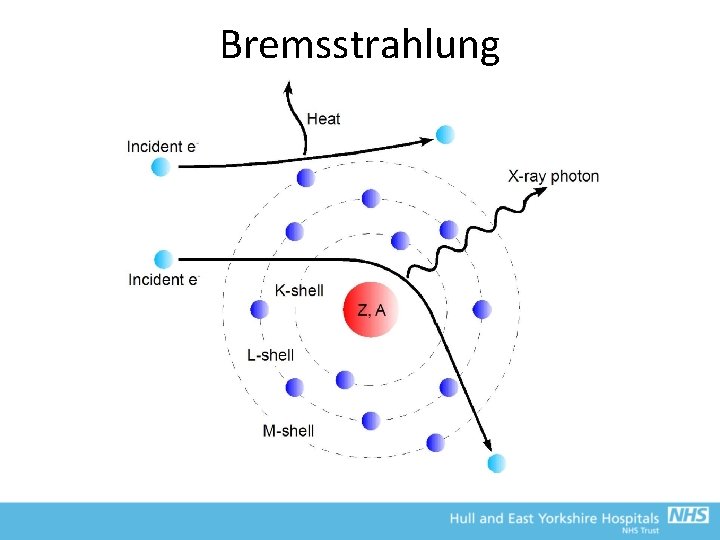
Bremsstrahlung

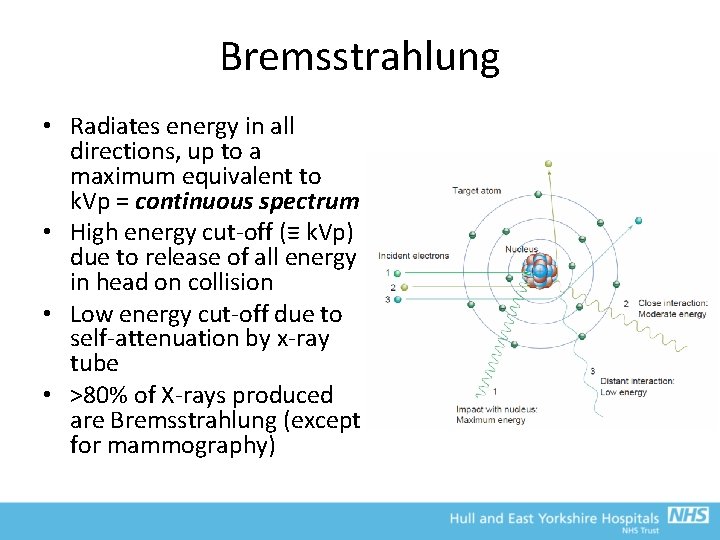
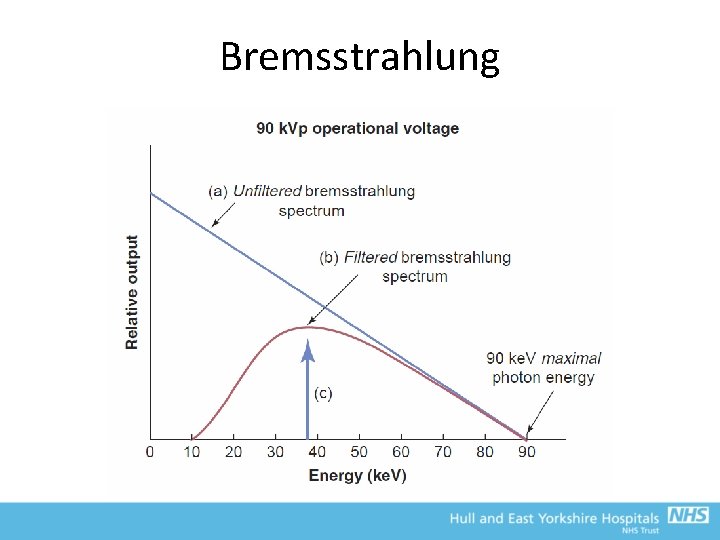
Bremsstrahlung • Radiates energy in all directions, up to a maximum equivalent to k. Vp = continuous spectrum • High energy cut-off (≡ k. Vp) due to release of all energy in head on collision • Low energy cut-off due to self-attenuation by x-ray tube • >80% of X-rays produced are Bremsstrahlung (except for mammography)

Bremsstrahlung

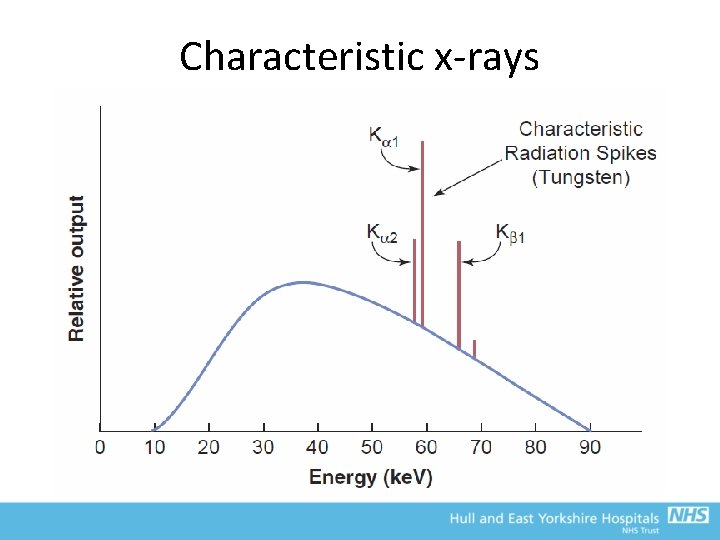
Characteristic x-rays • Interactions with tightly bound e- (typically K-shell) • If energy of e- exceeds binding energy (BE) → ionisation • Vacancy leaves atom unstable – e- from higher state drops down, releasing X-ray photon (energy = difference in BE) • Gives characteristic peaks on X -ray spectrum that are specific to the target – For Tungsten target, Kα = 58 -59 ke. V and Kβ = 67 ke. V – Not observed below 70 k. Vp

Characteristic x-rays

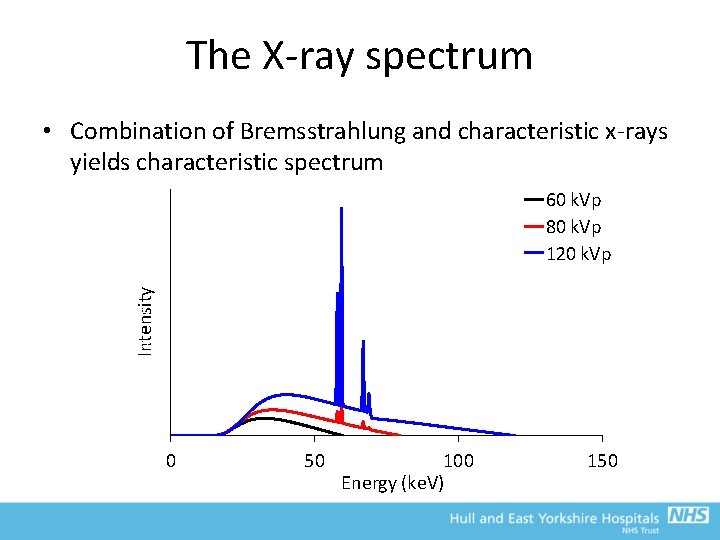
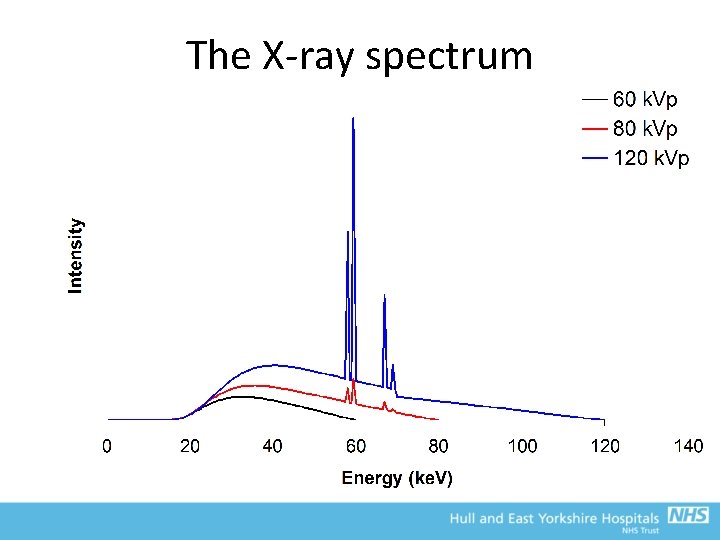
The X-ray spectrum • Combination of Bremsstrahlung and characteristic x-rays yields characteristic spectrum 4. 00 E+05 60 k. Vp 80 k. Vp 120 k. Vp 3. 50 E+05 3. 00 E+05 Intensity 2. 50 E+05 2. 00 E+05 1. 50 E+05 1. 00 E+05 5. 00 E+04 0. 00 E+00 0 50 100 Energy (ke. V) 150

The X-ray spectrum • The peak of the continuous spectrum is typically one third to one half of the maximum k. V • The average (or effective) energy is between 50% and 60% of the maximum – e. g. a 90 k. Vp beam can be thought of as effectively emitting 45 ke. V X-rays (NOT 90 ke. V) • Area of the spectrum = total output of tube – As k. Vp increases, width and height of spectrum increases – For 60 -120 k. Vp, intensity is approximately proportional to k. Vp 2 x m. A

Controlling the X-ray spectrum – Exposure factors • Increasing k. Vp shifts the spectrum up and to the right – Both maximum and effective energy increases, along with the total number of photons • Increasing m. As (the tube current multiplied by the exposure time) does not affect the shape of the spectrum, but increases the output of the tube proportionately • k. V waveform – three-phase or high frequency generators will have more high energy photons than single phase. Hence, output and effective energy are higher

Quality & Intensity Definitions: • Quality = the energy carried by the X-ray photons (a description of the penetrating power) • Intensity = the quantity of x-ray photons in the beam • An x-ray beam may vary in both its intensity and quality

Quality • Describes the penetrating power of the X-ray beam, and is governed by the kilo-voltage (k. Vp) • Usually described by the Half-Value Thickness – i. e. the thickness (in mm) of Al required to half the beam intensity for a given k. Vp • Typically >2. 5 mm Al for general radiography • Changing the quality of the beam will change the contrast between different types of tissue. • A highly penetrating beam is referred to as ‘Hard’ and a poorly penetrating beam as ‘Soft’

Intensity • Intensity - is the quantity of energy flow onto a given area over a given time; the ‘brightness’ of an x-ray beam • The tube current (m. A) is a measure of X-ray beam intensity • Intensity is directly proportional to m. A. – i. e. Double the m. A, double the dose (quality not affected) • Intensity is also affected by k. Vp

The mechanics of making an x-ray THE X-RAY TUBE

X-ray tubes – an overview • The x-ray tube insert is where we make the x-rays used in x-ray imaging systems – Cathode, anode, glass/metal enclosure under vacuum • The x-ray tube housing supports and shields the tube insert • The x-ray generator supplies the power • k. V, m. A and exposure time are selectable by the operator

THE X-RAY TUBE INSERT

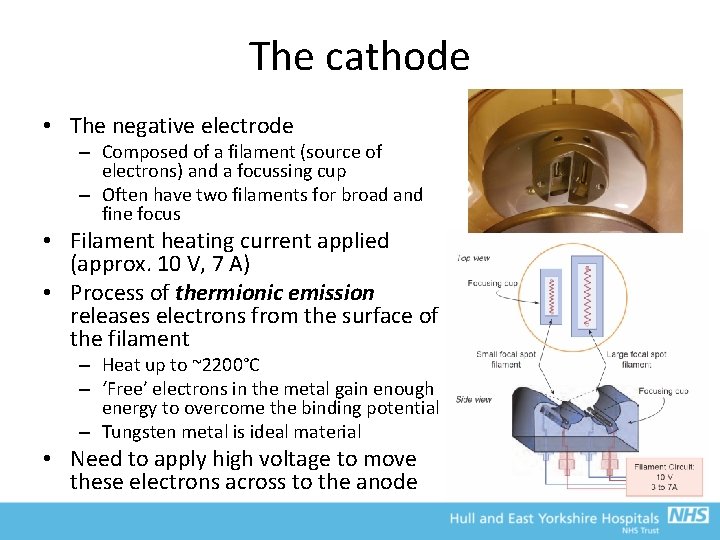
The cathode • The negative electrode – Composed of a filament (source of electrons) and a focussing cup – Often have two filaments for broad and fine focus • Filament heating current applied (approx. 10 V, 7 A) • Process of thermionic emission releases electrons from the surface of the filament – Heat up to ~2200°C – ‘Free’ electrons in the metal gain enough energy to overcome the binding potential – Tungsten metal is ideal material • Need to apply high voltage to move these electrons across to the anode

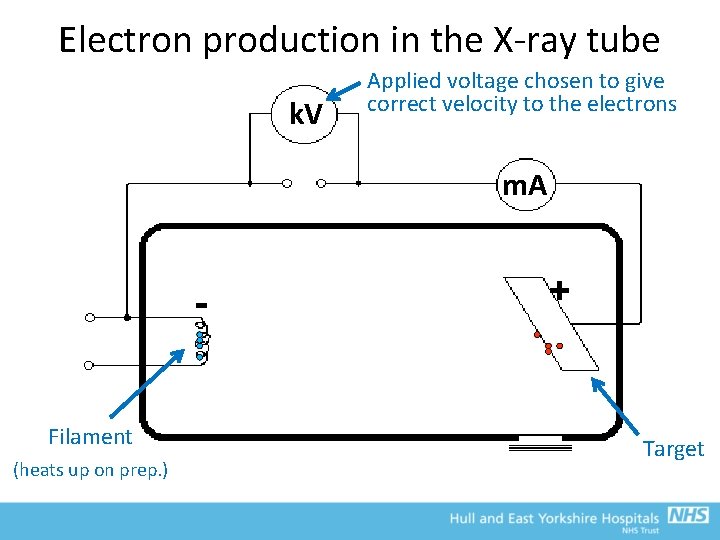
Electron production in the X-ray tube k. V Applied voltage chosen to give correct velocity to the electrons m. A Filament (heats up on prep. ) + Target

The anode • Metal target electrode, held at a large positive potential difference relative to the cathode • Electrons strike the anode and convert kinetic energy to mostly heat, with relatively few x-rays released – So to get an acceptable output from the tube, a lot of heat must be generated that has to be dealt with – Don’t want to blow the tube up! • Limits are placed on exposure factors to avoid damage • Choice of material important – Alloys of 10% rhenium and 90% tungsten are resistant to surface damage – good for general x-ray tubes • Also other design features used to limit heat damage…

Stationary or rotating? • Simple x-ray tubes (e. g. dental) have tungsten insert on a solid copper block – Conducts heat away from focal spot – Limited to low tube currents as heat builds quickly • Rotating anodes used for most diagnostic applications Bevelled disc on a rotor assembly Spins 3, 000 -10, 000 rpm Spread the heat out over a large area Allows greater loading and higher x-ray output – Tube does not energise until the disc is up to speed – Cooled via radiative emission transferring heat to tube insert and surrounding oil bath – –

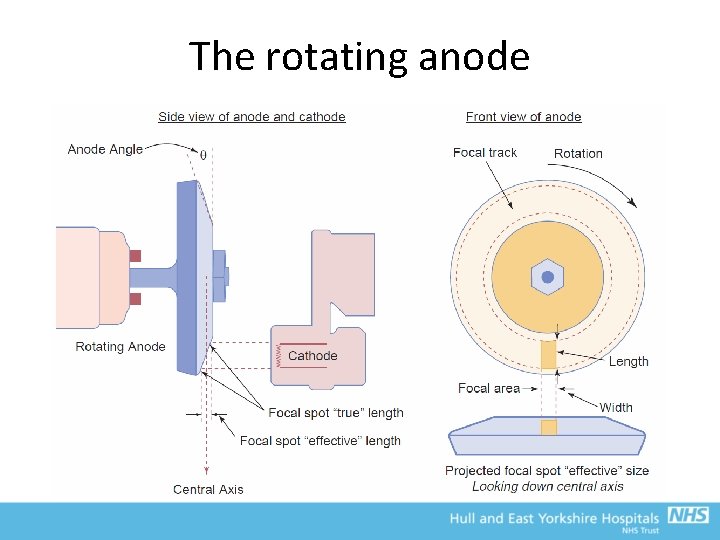
The rotating anode

The rotating anode

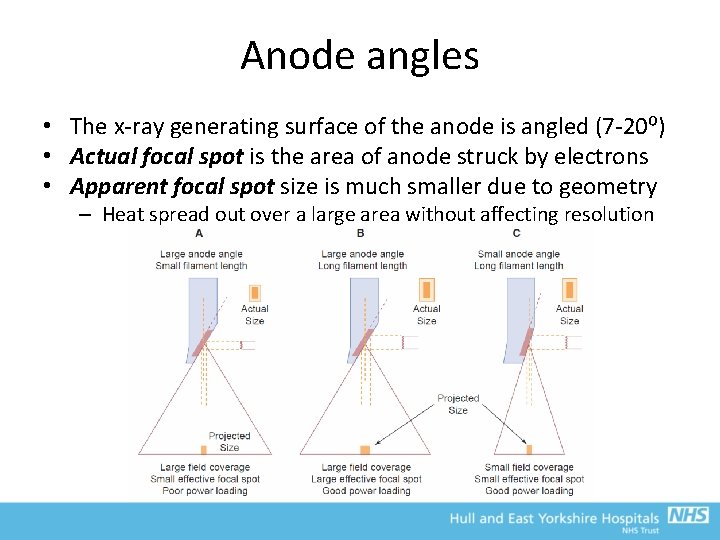
Anode angles • The x-ray generating surface of the anode is angled (7 -20⁰) • Actual focal spot is the area of anode struck by electrons • Apparent focal spot size is much smaller due to geometry – Heat spread out over a large area without affecting resolution

Anode angles • Smaller angles allow greater tube loading and finer resolution • BUT, limits maximum field size due to cut-off on anode side • Focal spot size varies across the image field – Anode side = shorter effective focal spots – Cathode side = elongated effective focal spot • Optimal target angle depends on clinical application

The focal spot • Typical focal spot sizes are – – 0. 15 -0. 3 mm for mammography 0. 6 -1. 2 mm for general radiography 0. 6 mm for fluoroscopy 0. 6 -1. 0 mm for CT

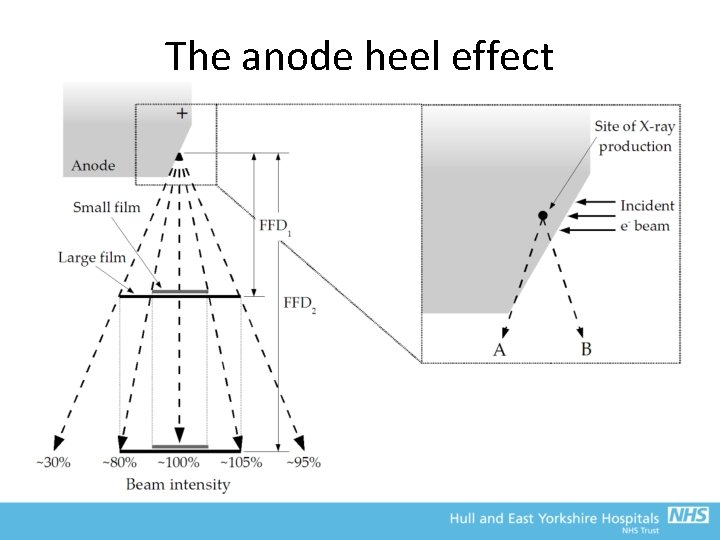
The anode heel effect • Ideally, the X-ray beam would be uniform across whole image • However, this is not the case due to the anode heel effect – The steeper the target angle, the worse the effect • The electrons penetrate a few micrometres below the surface of the anode before generating X-rays – Hence, the X-rays that are generated in the target may be attenuated on their way out • X-rays travelling towards the anode edge of the field (A) will pass through more of the target before exiting the tube – Hence, attenuation will be greater on this edge, and beam intensity will be lower than on the Cathode side of the field (B) – Roughening of the anode surface as the tube ages make this worse • Generally noticeable on most images • Can be minimised by using greater focus-to-detector distances, smaller fields and shallower target angles

The anode heel effect

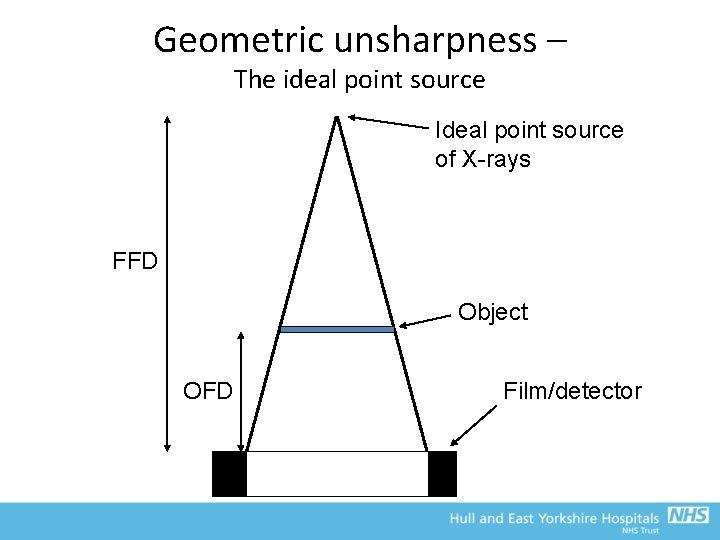
Geometric unsharpness and the focal spot • Spatial resolution is dependent upon : – Geometrical unsharpness – Motion unsharpness – Absorption unsharpness • Geometric unsharpness is related to the fact that we cannot (and in fact do not want to) produce an ideal point source of X-rays – The focal spot of the X-ray tube has a finite size that results in blurring across the edge of structures – Can be reduced by using a smaller focal spot, decreasing the object-film distance (OFD) or using a longer focus-tofilm distance (FFD)

Geometric unsharpness – The ideal point source Ideal point source of X-rays FFD Object OFD Film/detector

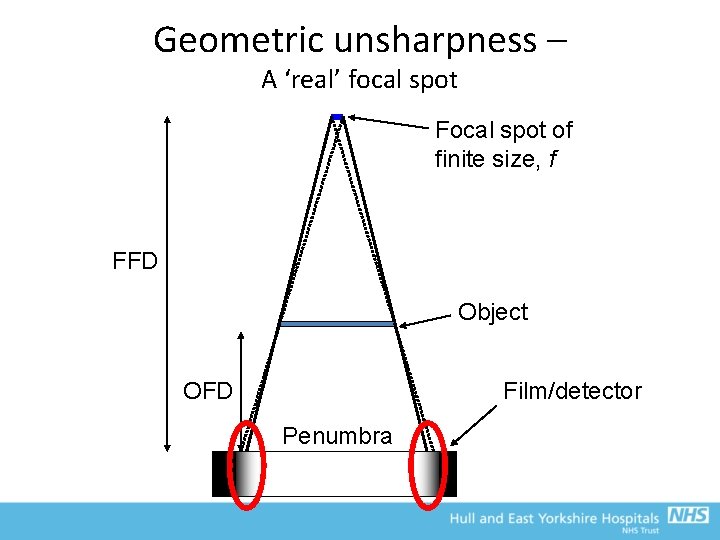
Geometric unsharpness – A ‘real’ focal spot Focal spot of finite size, f FFD Object OFD Film/detector Penumbra

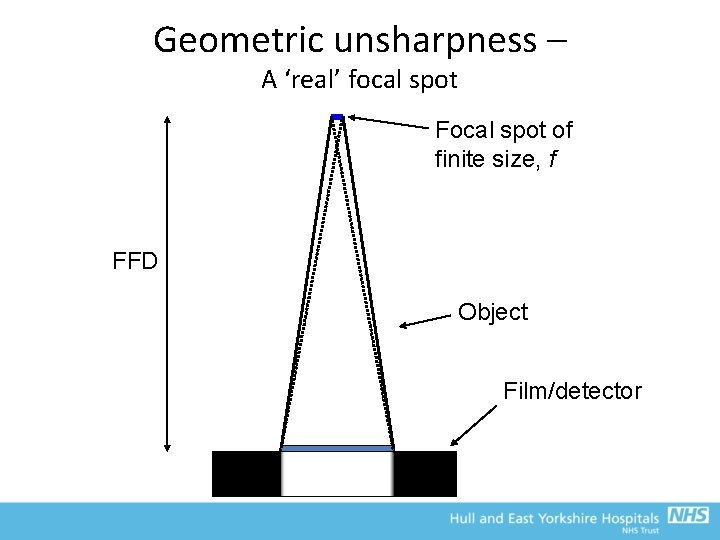
Geometric unsharpness and the focal spot • So, to minimise geometric unsharpness – The smallest focal spot should be used, especially if magnification imaging is to be performed (but be careful not to blow the tube!) – The patient should be positioned as close to the detector as possible (unless magnification imaging) – Largest possible focus-to-detector distances to reduce magnification and blurring (within practical limits!)

Geometric unsharpness – A ‘real’ focal spot Focal spot of finite size, f FFD Object Film/detector

X-ray tube design – dual focus

THE X-RAY TUBE HOUSING

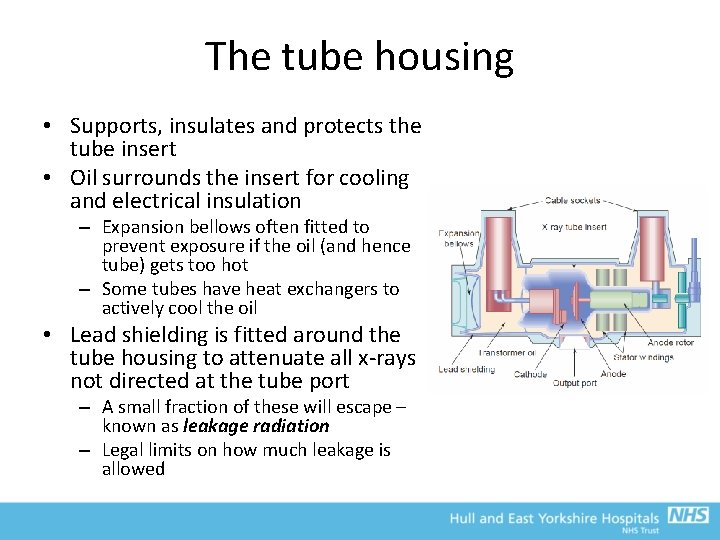
The tube housing • Supports, insulates and protects the tube insert • Oil surrounds the insert for cooling and electrical insulation – Expansion bellows often fitted to prevent exposure if the oil (and hence tube) gets too hot – Some tubes have heat exchangers to actively cool the oil • Lead shielding is fitted around the tube housing to attenuate all x-rays not directed at the tube port – A small fraction of these will escape – known as leakage radiation – Legal limits on how much leakage is allowed

Collimators • Adjust the size and shape of the x-ray beam • Two pairs of parallel blades of high attenuation material that can be adjusted to define the required rectangular field size • Has a light beam system for visualisation

Filtration • Filtration is the removal of x-ray photons as the beam passes through material • The x-ray tube has inherent filtration due to the anode, glass/metal envelope, cooling oil, etc • Added filtration is the sheets of metal deliberately inserted in the beam to reduce the number of low energy photons in the beam – Reduce the dose to the patient – Minimum standards on how much should be present in the beam (depending on application) • Can also have beam shaping filters to compensate for patient shape and to equalize the signal on the detector e. g. ‘bow-tie’ filters in CT

X-RAY GENERATORS

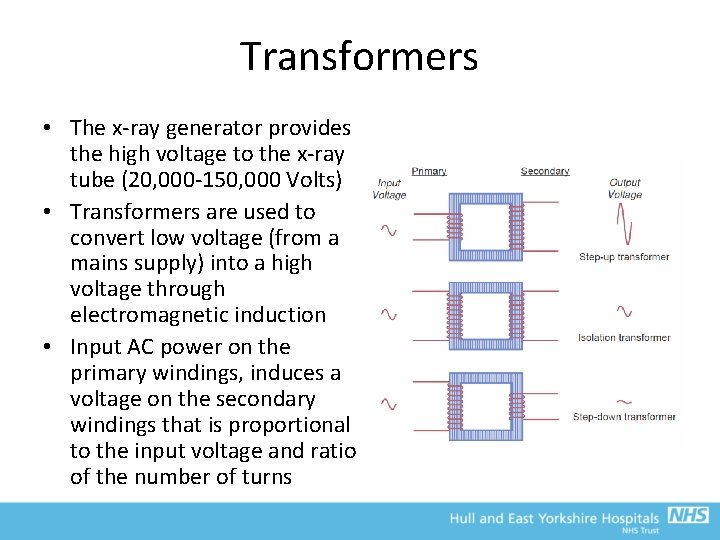
Transformers • The x-ray generator provides the high voltage to the x-ray tube (20, 000 -150, 000 Volts) • Transformers are used to convert low voltage (from a mains supply) into a high voltage through electromagnetic induction • Input AC power on the primary windings, induces a voltage on the secondary windings that is proportional to the input voltage and ratio of the number of turns

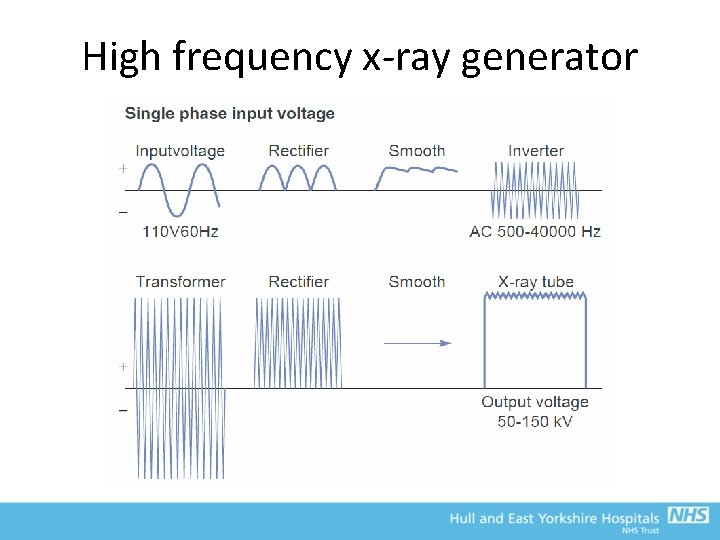
Transformers • However, to accelerate electrons across the tube, need anode to always be positive relative to cathode – AC waveforms change polarity every half-cycle • Rectifiers can prevent this • The high frequency generator is the now the most common type of generator – Takes a low voltage, low frequency input and converts to low voltage DC via rectifier and smoothing – An inverter creates a high frequency AC waveform from this – A transformer creates the high voltage – Rectified and smoothed again to provide high voltage DC to tube • A number of feedbacks are continuously checked during exposure to ensure appropriate k. V and m. A

High frequency x-ray generator

Ripple • Ideal voltage would be constant • Real voltages tend to vary, and this depends on the type of generator used • Ripple describes variation in k. V during exposure – Single phase = 100% ripple – High frequency = low ripple • Ripple reduces the output of the x-ray tube compared with what would otherwise be expected

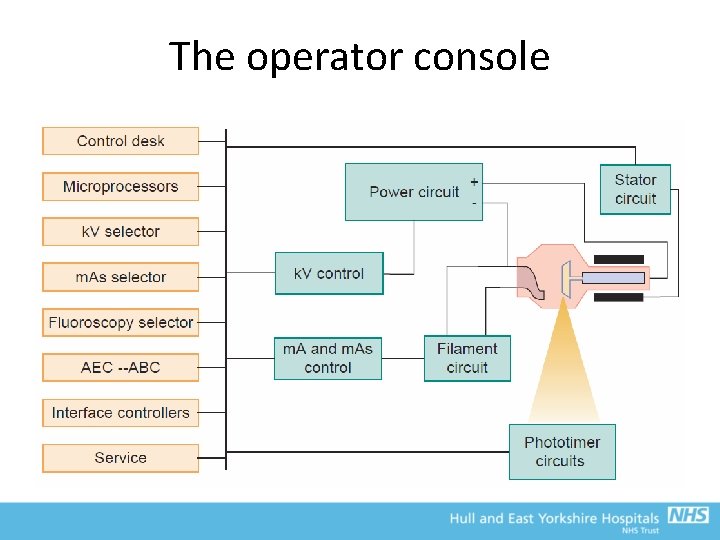
The operator console • The operator can select tube voltage (k. V), tube current (m. A), exposure time (s) or the product of m. A and time (m. As) • Focal spot selections on some systems – Choice depends on resolution requirements vs damage to x-ray tube • May also have controls for the automatic exposure control – The AEC determines how long exposures should be based on the transmission of x-rays through the subject • Pre-programmed techniques can also be found on the operator console • In fluoroscopy, manual k. V and m. A control not practical, so automatic control systems are used

The operator console

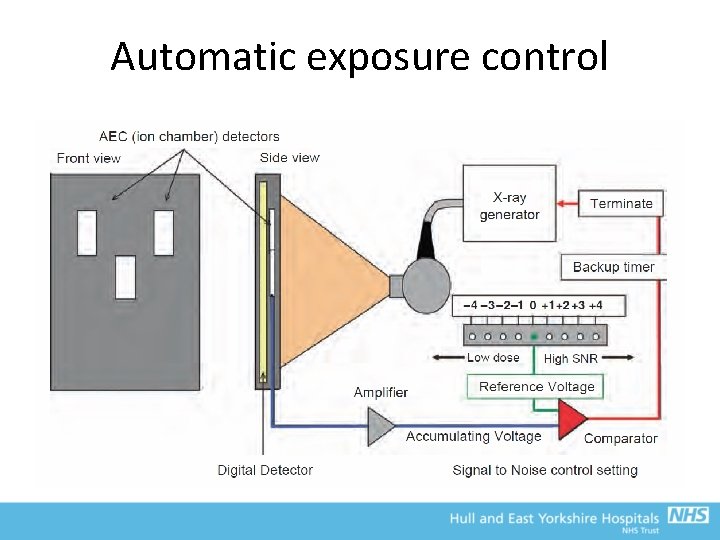
Automatic exposure control • AEC measures amount of radiation incident on the detector and terminates exposure when a pre-defined limit is reached • Compensates for different size patients and variations in attenuation • Can have some measure of manual control by using ‘fine density’ controls to force the system terminate a little earlier or later, depending on image quality requirements • Usually have a choice of ion chambers that can be selected in different configurations depending on clinical application – e. g. central chamber, left-right chambers, all three chambers

Automatic exposure control

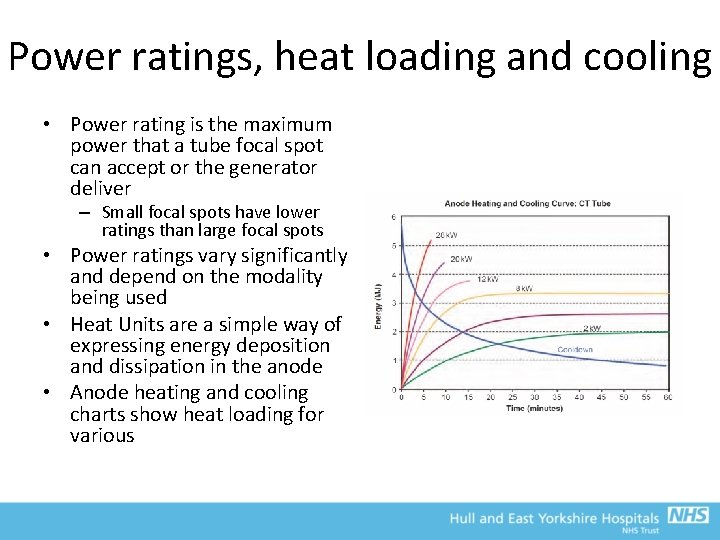
Power ratings, heat loading and cooling • Power rating is the maximum power that a tube focal spot can accept or the generator deliver – Small focal spots have lower ratings than large focal spots • Power ratings vary significantly and depend on the modality being used • Heat Units are a simple way of expressing energy deposition and dissipation in the anode • Anode heating and cooling charts show heat loading for various

Heat rating • k. V, m. A and exposure time should be such that the temperature of the anode does not exceed its safe limit – The control system is designed to prevent exposures that exceed the tube rating • Require much higher tube ratings for CT and interventional fluoroscopy units

FACTORS AFFECTING X-RAY TUBE OUTPUT

X-ray tube output • Output of an x-ray tube can be described in terms of; – Quality: Penetrating power of x-ray beam (HVL) – Quantity: Number of photons in x-ray beam • Six major factors determine x-ray tube output; – – – Anode target material Tube kilovoltage Tube current Exposure time Beam filtration Generator waveform

Target material • The efficiency of Bremsstrahlung production depends on the atomic number of the anode material – Incident electrons more likely to interact with high Z materials • The anode material also determines the energy of the characteristic x-rays • Target material affects both quantity and quality of the x-ray beam

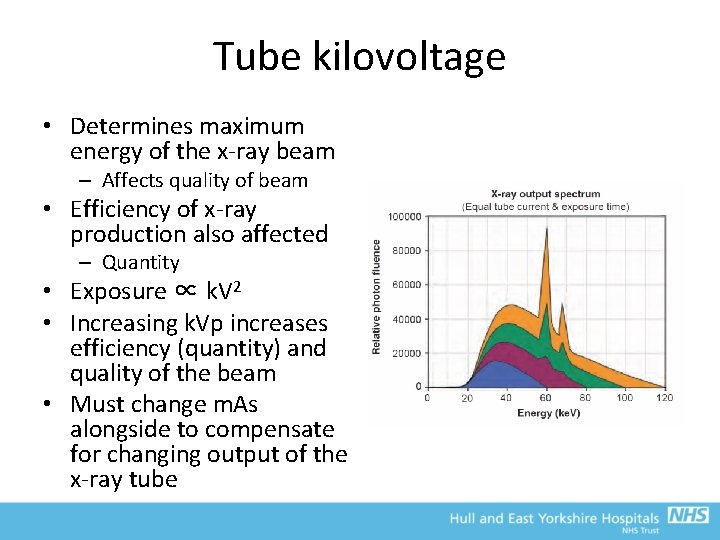
Tube kilovoltage • Determines maximum energy of the x-ray beam – Affects quality of beam • Efficiency of x-ray production also affected – Quantity • Exposure ∝ k. V 2 • Increasing k. Vp increases efficiency (quantity) and quality of the beam • Must change m. As alongside to compensate for changing output of the x-ray tube

The X-ray spectrum

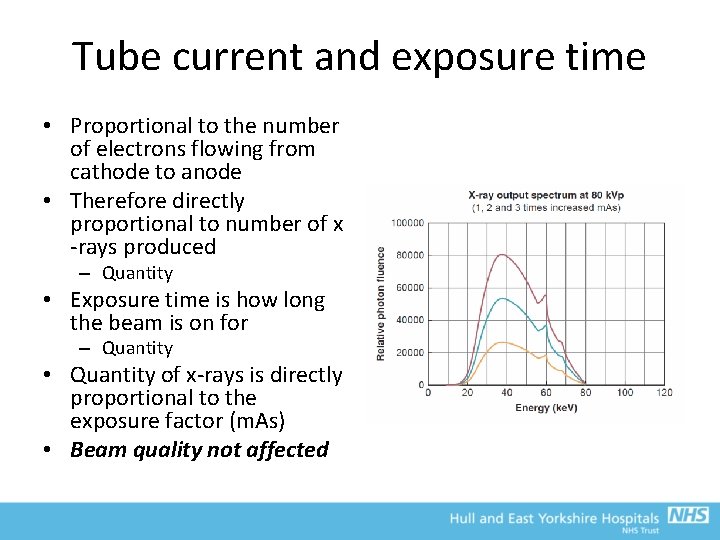
Tube current and exposure time • Proportional to the number of electrons flowing from cathode to anode • Therefore directly proportional to number of x -rays produced – Quantity • Exposure time is how long the beam is on for – Quantity • Quantity of x-rays is directly proportional to the exposure factor (m. As) • Beam quality not affected

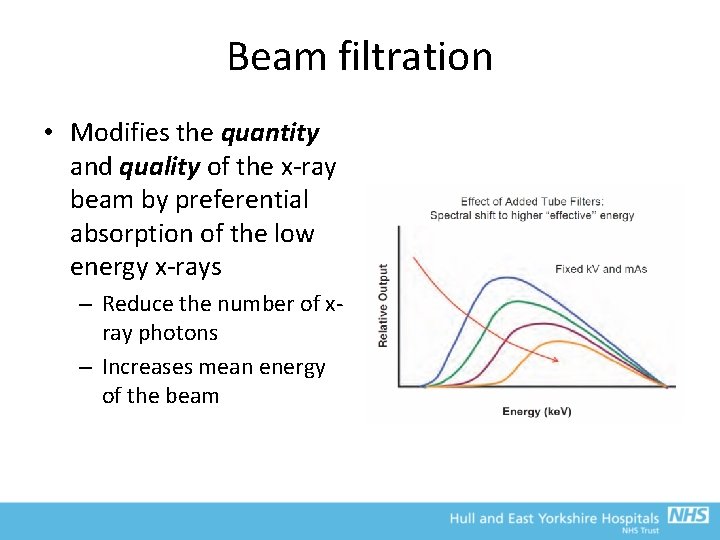
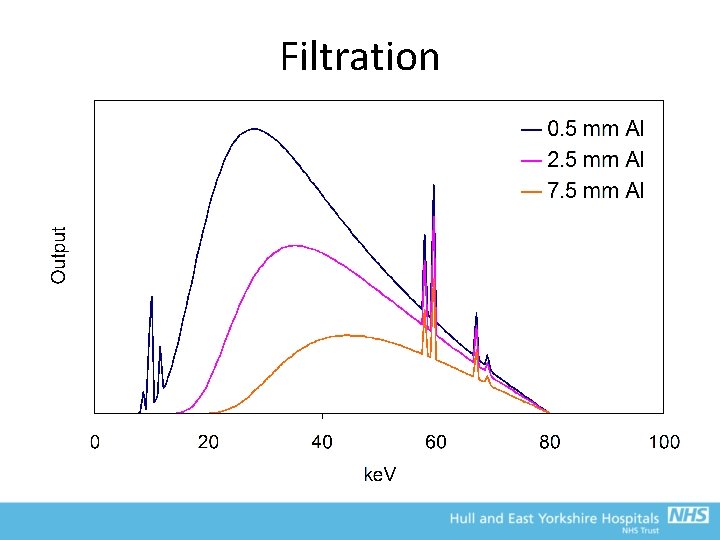
Beam filtration • ‘Soft x-rays’ contribute to patient dose without contributing to image production • Placing Al filters in the beam will increase beam quality – this is known as ‘Beam Hardening’ – Alternative materials may be used for filtration in specialised applications e. g. mammography (Mo, Rh, Ag) and fluoroscopy (Cu) • Lowest energy photons are most readily absorbed as photoelectric absorption dominates (proportional to the E 3) • As the beam passes the Al, the proportion of low energy photons is reduced, and the average photon energy increases

Filtration

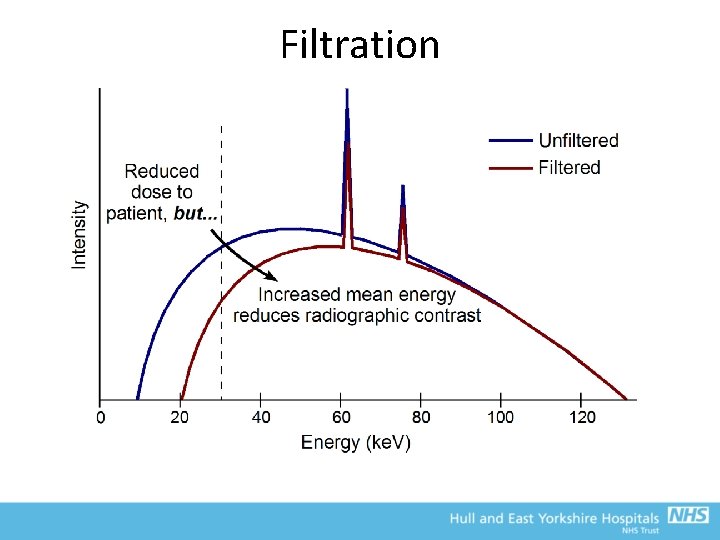
Beam filtration • Modifies the quantity and quality of the x-ray beam by preferential absorption of the low energy x-rays – Reduce the number of xray photons – Increases mean energy of the beam

Filtration

Beam filtration • Hence, Patient dose is reduced with little affect on the radiation reaching the detector • However; • Radiographic contrast is reduced due to the higher mean energy of the beam • Greater exposure factors required to yield satisfactory dose at film/detector (have to drive the tube harder, and hence tube life may be reduced) • The X-ray beam is also filtered by the target that they are produced in, the coolant oil and the window of the housing • ‘Inherent filtration’ equivalent to about 1 mm Al

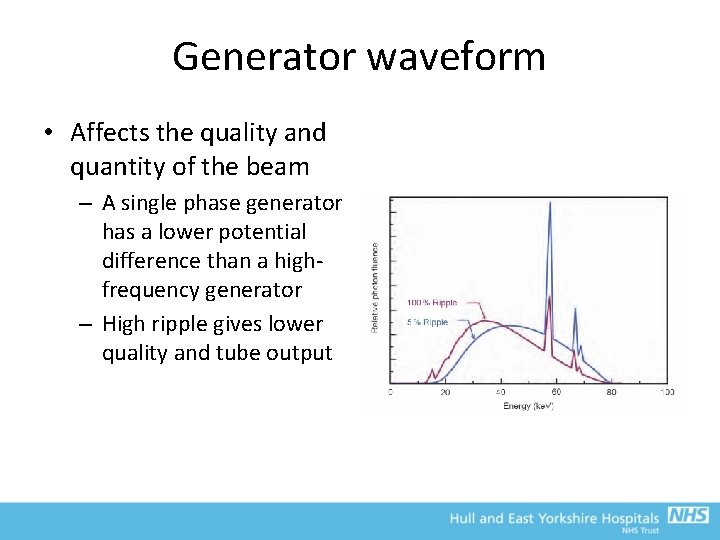
Generator waveform • Affects the quality and quantity of the beam – A single phase generator has a lower potential difference than a highfrequency generator – High ripple gives lower quality and tube output

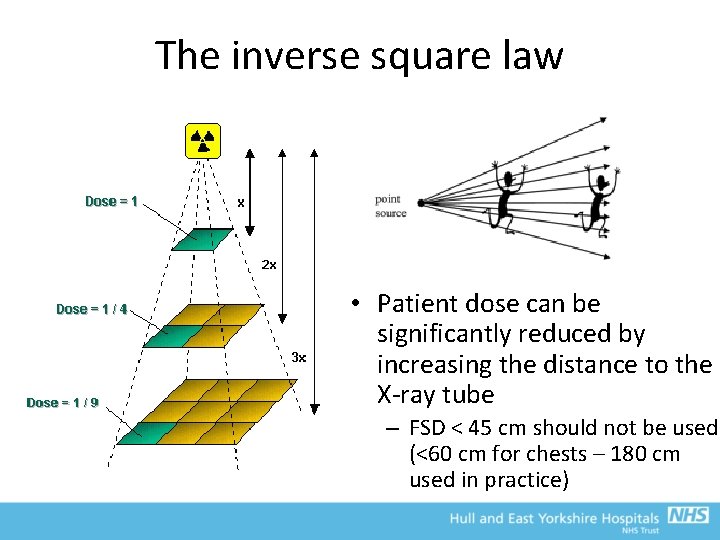
Focus-to-skin Distance: The Inverse Square Law • For a point source, and in the absence of attenuation, intensity decreases as the inverse of the square of the distance • This is a statement of the conservation of energy

The inverse square law • Patient dose can be significantly reduced by increasing the distance to the X-ray tube – FSD < 45 cm should not be used (<60 cm for chests – 180 cm used in practice)

SUMMARY

Summary • X-rays are generated in the x-ray tube • A broad spectrum of energies are produced through Bremsstrahlung and characteristic x-rays • Heat generation is a significant problem in the xray tube • A number of factors affect the output of the x-ray tube, and these must all be considered and understood to enable the best possible image to be acquired (for the minimum radiation dose to the patient)