Teaching Hematology to SecondYear Medical Students What Are


























- Slides: 31

Teaching Hematology to Second-Year Medical Students: What Are We Doing, How Are We Doing It, and Can We Improve? How Medical Education Has Changed Over the Decades William E. Winter, MD University of Florida Departments of Pathology and Pediatrics

How am I involved in teaching hematology? 2 nd Year Medical Student General and Systemic Pathology Course Director, 2004 – > present Background - Pediatrics, Pediatric endocrinology - Clinical Chemistry True confession - I am not a clinical hematologist or a hematopathologist - I teach in hematopathology - Reading a CBC - Hematopoiesis - Laboratory coagulation testing - Blood bank (basics)

2008 - The Times They Are A Changin’. . 2009 - The Times They Have Changed Come mothers and fathers Throughout the land And don't criticize What you can't understand Your sons and your daughters Are beyond your command 3

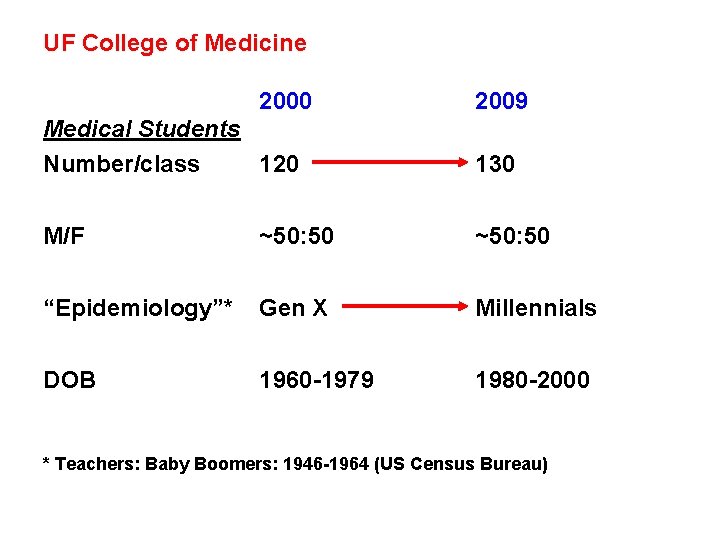
UF College of Medicine 2000 2009 Medical Students Number/class 120 130 M/F ~50: 50 “Epidemiology”* Gen X Millennials DOB 1960 -1979 1980 -2000 * Teachers: Baby Boomers: 1946 -1964 (US Census Bureau)

Have medical students changed in the last 10 years? Yes! Medical students have changed in the past ~10 years: - Independent: work at their own pace; multitask - Less appreciation for hierarchy - equality of student and teacher (disrespect? ) - yet: interested in social justice, poverty, inequity - On-demand information availability using all possible communication media interfaces - Internet, youtube, facebook, i. Phone

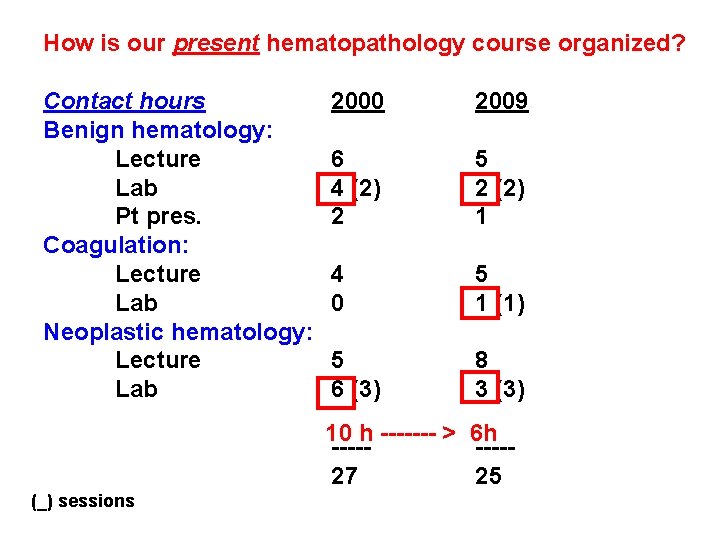
How is our present hematopathology course organized? Contact hours Benign hematology: Lecture Lab Pt pres. Coagulation: Lecture Lab Neoplastic hematology: Lecture Lab 2000 2009 6 4 (2) 2 5 2 (2) (-) 1 4 0 5 1 (1) 5 6 (3) 8 3 (3) No change ----25 Decr. total hrs. ----27 (_) sessions Added 1 lab

How is our present hematopathology course organized? Contact hours Benign hematology: Lecture Lab Pt pres. Coagulation: Lecture Lab Neoplastic hematology: Lecture Lab 2000 2009 6 4 (2) 2 5 2 (2) 1 4 0 5 1 (1) 5 6 (3) 8 3 (3) 10 h ------- > 6 h ----27 25 (_) sessions

Questions of importance: If there is more to teach, how could we teach more in less time? How could we reduce lab time without reducing content? Why should students participate in lecture and lab? COURSE REVISIONS -- > were not directed at reducing contact time -- > reduced contact time was a result of our course “renovations”

If there is more to teach, how could we teach more in less time? 1) Students have a better understanding of molecular biology than in the past (HS students study recombinant DNA technology & molecular biology) 2) Teach from the physiology -- > pathophysiology (disease follows the physiology) - Benign hematology is extremely logical - Neoplastic hematology is becoming more logical 3) Lectures and labs emphasize problem solving (recall is used as a “tool” to solve problems and is not an educational end in itself)

If there is more to teach, how could we teach more in less time? 4) Reduced the number of lecturers (selected better educators) 5) Frequent references to material previously taught (e. g. , inflammation & repair, immunology & immunopathology) (educators know the student’s course work) [“integration”]

If there is more to teach, how could we teach more in less time? 6) Teach what is important for an MS 2 (and little more) - Refer to a standard MS textbook (Robbins) 7) Emphasize clinical presentations and differential diagnosis 8) Treatment is not the 10 goal of the pathology course - Treatment is discussed but specifics should be discussed in pharmacology, oncology, MS 3+

If there is more to teach, how could we teach more in less time? Linked labs directly to topics / problem-solving focus Neoplastic HP Introduction to HP (technologies) Lymphadenopathy/ lymphoma (I) Lymphoma (II) Lab: Lymphadenopathy/ lymphoma Problem solving Leukemias (I) Leukemias (II) Lab: Leukemias Problem solving MDS/MPD Lab: MDS/MPD Problem solving

What is “problem solving? ” An example from the coag lab --- > A 5 y/o boy presents with a swollen, tender knee 12 hours following trauma. The knee is taped and bloody fluid is removed. Is this most consistent with a defect in primary hemostasis or secondary hemostasis? Secondary hemostasis

For the 5 year old boy, what 2 clotting tests are most important to initially order? PT and a. PTT PT Reference interval (sec) 10. 5 - 13. 5 a. PTT 23 - 33 Pt result 12 42 What factor(s) could be deficient, dysfunctional or inhibited? Factors XI, IX, VIII Why isn’t FXII included on this list? Factors XII deficiency does not cause bleeding

If there is more to teach, how could we teach more in less time? Link: Physiology – Lab testing – Pathophysiology – Pt Evaluation Coagulation Introduction to coagulation testing Pathophysiology of bleeding diatheses Pathophysiology of thrombotic disorders Approach to the patient who is bleeding Approach to the patient with thrombosis Lab: Coagulation cases Problem solving

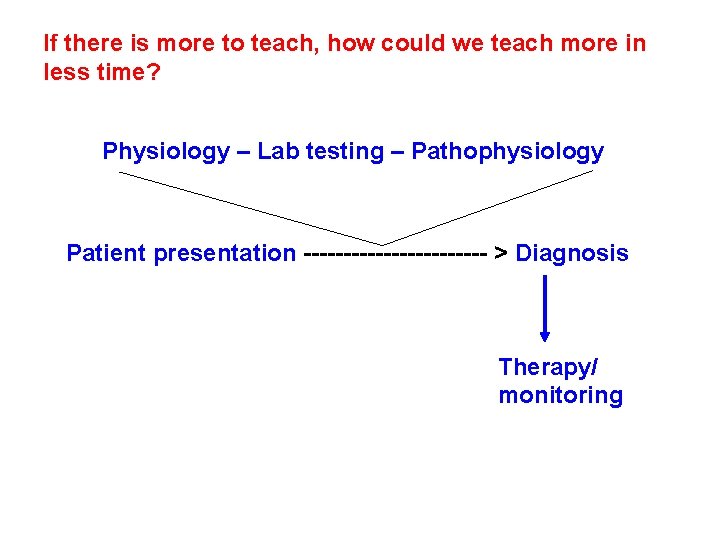
If there is more to teach, how could we teach more in less time? Physiology – Lab testing – Pathophysiology Patient presentation ------------ > Diagnosis Therapy/ monitoring

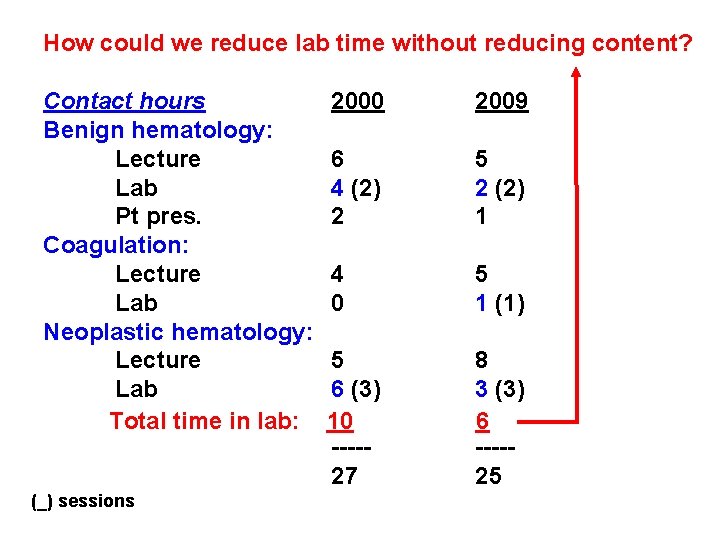
How could we reduce lab time without reducing content? Contact hours Benign hematology: Lecture Lab Pt pres. Coagulation: Lecture Lab Neoplastic hematology: Lecture Lab Total time in lab: (_) sessions 2000 2009 6 4 (2) 2 5 2 (2) 1 4 0 5 1 (1) 5 6 (3) 10 ----27 8 3 (3) 6 ----25

How could we reduce lab time without reducing content? Improved the relevance of the labs -- > the labs are all case-based and authentic, diagnostic, problem-solving exercises Labs: 2000: Histopathology (+) ASH cases (too complex for MS 2’s) 2009: De-emphasized histopathology* Created clinical cases appropriate for MS 2’s - ex. : benign hematology: M. Zumberg, MD * we are training generalists (not pathology residents)

How could we reduce lab time without reducing content? Cases: Powerpoint format (“serial reveal”) Socratic method: Question and answer Not all answers provided during lab* Students make diagnostic decisions * Faculty/staff available to provide answers

How could we reduce lab or lecture time without reducing content? Provide self-taught exercises [Millinneals are independent (? )] - Examples: - Aplastic anemia H/O (3 pages) What is aplastic anemia? What are the consequences of aplastic anemia? What is the appearance of the BM in aplastic anemia? What are the causes of aplastic anemia? What is an idiosyncratic reaction? What is the differential diagnosis of pancytopenia? What is pure red cell aplasia? What is a myelophthisic anemia?

How could we reduce lab time without reducing content? Provide self-taught labs - Examples: - Anemia self study

A Case 1 woman of reproductive age reports menorrhagia and tiredness. Her heart rate is 105 bpm. She is pale. Her stool tests negative for occult blood. Pertinent results from her CBC are displayed below. RBC count Reference interval 4. 15 - 4. 90 x 106/mm 3 Pt results 3 x 106/mm 3 Hgb (females) 12 -16 g/d. L 9 g/d. L Hct (females) 37 -48% 27% MCV 80 -100 fl 75 fl

I S THE PATIENT ANEMIC? YES NO H ANEMIA OW DO YOU DESCRIBE HER ____? MICROCYTIC NORMOCYTIC MACROCYTIC “Clinical decision making”

Why do our labs emphasize problem solving and not recall? Problem-solving: medicine is “all about” solving & treating problems key to learning: active learning - valid (vital!) for clinical care of patients - valid for exam (case-based, non-recall Q’s) Testing will drive learning

How could we reduce lab time without reducing content? All students work in 3 - 4 person teams in pathology (August -- > Feb) Students are tasked to teach one another

How could we reduce lab time without reducing content? All students work in 3 - 4 person teams in pathology (August -- > Feb) Teams are efficient W/o excessive # of slides -- > focus on problem-solving cases Abundant faculty/fellows/pathology residents available to assist students Reduced lab time: 2 hrs -- > 1 hr

How could we improve the faculty / student ratio and reduce noise and crowding in lab? 2009: Divided all lab sessions in half 2000 2009 No. students / session 120 65* * hold 2 lab sessions for each single lab Faculy-staff / student ratio: DOUBLED! More efficient use of time -- > reduced lab time “We can’t do more -- > we need to do better!”

How could we reduce our contact hours AND improve the course at the same time? Provided sufficient time for important topics Coagulation Added: coagulation testing lecture Added: coagulation lab Multiple myeloma Taught in immunology: SPE, IFE MGUS versus MM vs. Waldenstrom Myelodysplastic syndromes / myeloproliferative disorders 1 lecture –split-- > 2 lectures

Why should students participate in lecture and lab? Concepts for your consideration: Education is a “real time” experience W/ an interactive lecture style, students must think! Listening to the lecture at 2 x speed -- > enforces “consumption” of facts and not “processing” of information Active learning -- > engagement through problem solving

Why should students participate in lecture and lab? Concepts: Lab: You must be able to work successfully in groups (e. g. , lab teams) Recorded lectures can be available as a supplement to attendance -- > does not replace attendance* * You can’t take you patients home; expectation of attendance must begin before 3 rd year (professionalism)

Summary Physiology V Pathophysiology (+) Patient’s Hx / PE V Differential diagnosis v Definitive testing V Diagnosis V Therapy Goal of 2 nd year pathology: Train students to undertake this process!!!