Chronic Kidney Disease Chapter 46 Chronic Kidney Disease






































































- Slides: 73

Chronic Kidney Disease Chapter 46

Chronic Kidney Disease (CKD) • Involves progressive, irreversible loss of kidney function • More than 26 million American adults have CKD • Over half a million Americans are receiving treatment for ESRD

Chronic Kidney Disease • Defined as one of the following: • Kidney damage • Pathologic abnormalities • Markers of damage • Blood, urine, imaging tests • Low glomerular filtration rate (GFR) • <60 m. L/min for longer than 3 months

Chronic Kidney Disease • Leading causes • Diabetes- 50% • Hypertension- 25% • Individuals with CKD are frequently asymptomatic • Results in CKD being underdiagnosed and untreated

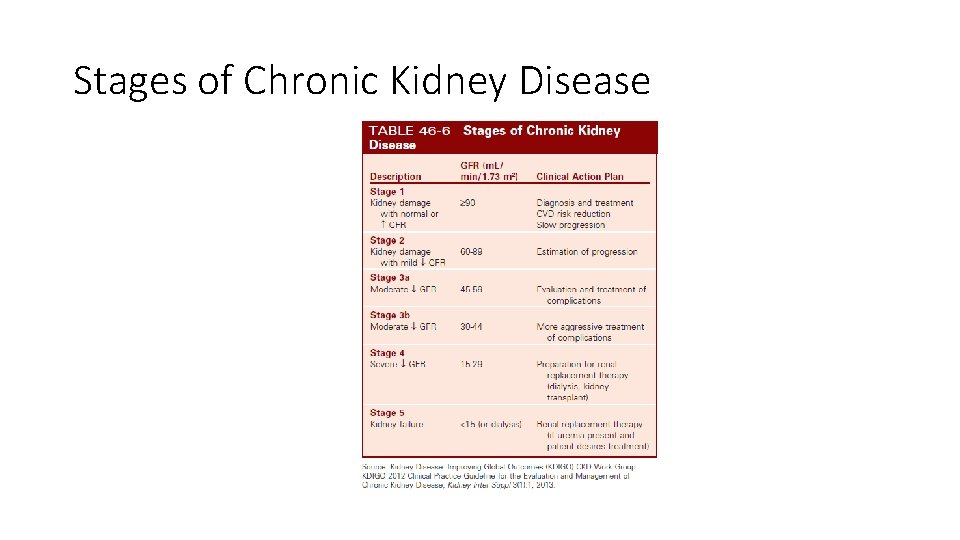
Chronic Kidney Disease • Disease staging based on decrease in GFR • Normal GFR: 125 m. L/min, which is reflected by urine creatinine clearance • Last stage of kidney failure • End-stage renal disease (ESRD) occurs when GFR <15 m. L/min

Stages of Chronic Kidney Disease

Case Study (©Purestock/Thinkstock) • K. W. , a 35 -year-old man, began to notice weakness with activities such as walking distances or running. • He also had tingling all over his body, particularly in his hands and feet.

Case Study (©Purestock/Thinkstock) • At age 5, K. W. was admitted to the hospital for hematuria, and acute glomerulonephritis was diagnosed. • At age 11, he was admitted to the same hospital, and recurring acute glomerulonephritis was diagnosed. • K. W. has had no further follow-up until this admission.

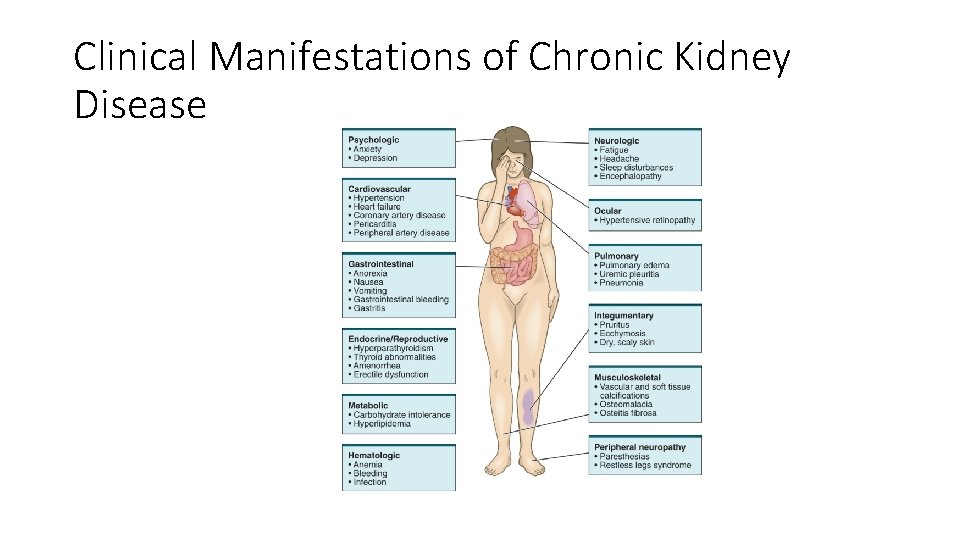
Clinical Manifestations • Result of retained substances • • • Urea Creatinine Phenols Hormones Electrolytes Water

Clinical Manifestations • Uremia • Syndrome in which kidney function declines to the point that symptoms occur in multiple body systems • Often occurs when GFR is ≤ 15 m. L/min

Clinical Manifestations of Chronic Kidney Disease

Case Study (©Purestock/Thinkstock) • K. W. says he had an increase in urine production several months ago and was concerned about the possibility of diabetes. • History reveals grandmother and aunt have diabetes; no family history of renal disease.

Case Study (©Purestock/Thinkstock) • He states that he has recently developed a severe decrease in urine output.

Clinical Manifestations Urinary System • Early stages • No change in urine output • Polyuria may be present related to diabetes. • As CKD progresses patients have increasing fluid retention • After a period on dialysis, patients may become anuric

Clinical Manifestations Urinary System • Early stages • No change in urine output • Polyuria may be present related to diabetes. • As CKD progresses patients have increasing fluid retention • After a period on dialysis, patients may become anuric

Clinical Manifestations Metabolic Disturbances • Altered carbohydrate metabolism • Caused by impaired glucose metabolism • From cellular insensitivity to normal action of insulin

Clinical Manifestations Metabolic Disturbances • Defective carbohydrate metabolism • Patients with diabetes who develop uremia may require less insulin than before the onset of CKD • Excretion of insulin dependent on kidneys • Insulin dosing must be individualized

Clinical Manifestations Metabolic Disturbances • Elevated triglycerides • Hyperinsulinemia stimulates hepatic production of triglycerides • Altered lipid metabolism • ↓ Levels of enzyme lipoprotein lipase • Important in breakdown of lipoproteins

Clinical Manifestations Metabolic Disturbances • Elevated triglycerides • Hyperinsulinemia stimulates hepatic production of triglycerides • Altered lipid metabolism • ↓ Levels of enzyme lipoprotein lipase • Important in breakdown of lipoproteins

Clinical Manifestations Electrolyte/Acid-Base Imbalances • Potassium • Hyperkalemia • Most serious electrolyte disorder in kidney disease • Fatal dysrhythmias • When serum potassium level reaches 7 to 8 m. Eq/L (7 to 8 mmol/L) When serum potassium level

Clinical Manifestations Electrolyte/Acid-Base Imbalances • Sodium • May be elevated, normal, or low • Because of impaired excretion, sodium along with water is retained • Dilutional hyponatremia may occur • Edema • Hypertension • HF

Clinical Manifestations Electrolyte/Acid-Base Imbalances • Calcium and phosphate alterations • Magnesium alterations • Hypermagnesemia • Related to ingestion of magnesium • Can result in absence of reflexes, decreased mental status, cardiac dysrhythmias, hypotension, respiratory failure

Clinical Manifestations Electrolyte/Acid-Base Imbalances • Metabolic acidosis • Results from • Kidneys’ impaired ability of to excrete excess acid (primary ammonia) • Defective reabsorption and regeneration of bicarbonate • Plasma bicarbonate level usually falls to approximately 16 to 20 m. Eq/L (16 to 20 mmol/L)

Clinical Manifestations Hematologic System • Anemia • Due to ↓ production of erythropoietin • From ↓ of functioning renal tubular cells • Also decreased iron stores • Folic acid lost in dialysis • Bleeding tendencies • Defect in platelet function

Clinical Manifestations Hematologic System • Infection • Changes in WBC function • Altered immune response and function • Hyperglycemia and external trauma

Clinical Manifestations Cardiovascular System • CV disease and CKD closely linked • Traditional CV risk factors • Hypertension • Elevated lipids • Nontraditional CV risk factors • Vascular calcification • Arterial stiffness

Clinical Manifestations Cardiovascular System • Calcium deposits associated with stiffness of blood vessels • Vascular smooth muscle cells change • Chondrocytes or osteoblastlike cells • High calcium and phosphate totals • Impaired renal excretion • Drug therapies to treat bone disease

Clinical Manifestations Cardiovascular System • Hypertension • Both a cause and a consequence of CKD • Aggravated by sodium and water retention • Increased renin production may contribute • Lead to left ventricular hypertrophy and HF

Clinical Manifestations Cardiovascular System • Hypertension • Both a cause and a consequence of CKD • Aggravated by sodium and water retention • Increased renin production may contribute • Lead to left ventricular hypertrophy and HF

Clinical Manifestations Gastrointestinal System • Every part of GI system is affected • Cause: excessive urea • • • Stomatitis with ulcerations Uremic fetor (urinous odor of breath) Gastrointestinal system Diabetic gastroparesis GI bleeding Constipation

Clinical Manifestations Neurologic System • Expected as kidney disease progresses • Result of • • ↑ Nitrogenous waste products Electrolyte imbalances Metabolic acidosis Atrophy and demyelination of nerve fibers

Clinical Manifestations Neurologic System • CNS depression • • Lethargy, apathy Decreased ability to concentrate Fatigue, irritability Altered mental ability Seizures Coma Hypertensive encephalopathy

Clinical Manifestations Neurologic System • Slowing of nerve conduction • Restless legs syndrome • Paresthesias • Motor involvement • • Foot drop Muscle weakness and atrophy Loss of deep tendon reflexes Peripheral neuropathy

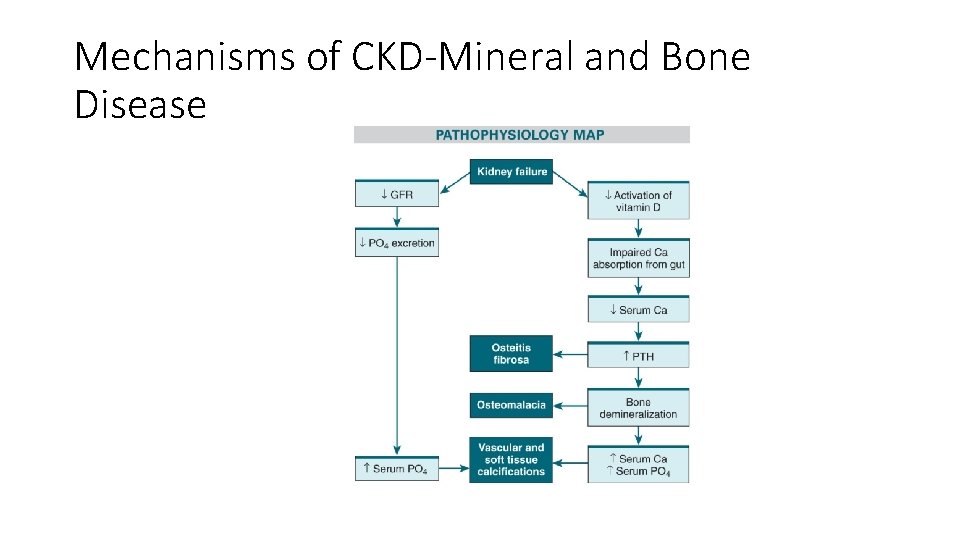
Clinical Manifestations Musculoskeletal System • CKD mineral and bone disorder • Systemic disorder of mineral and bone metabolism • Results in • Skeletal complications (osteomalacia, osteitis fibrosa) • Soft tissue complications (vascular calcifications)

Mechanisms of CKD-Mineral and Bone Disease

Clinical Manifestations Integumentary System • Pruritus • Itching may be intense • Leads to bleeding or infection • Uremic frost • Urea crystalizes on skin

Clinical Manifestations Reproductive System • Infertility and decreased libido • Experienced by both sexes • Low sperm counts • Sexual dysfunction • Pregnancy poses significant risk to mother and infant

Clinical Manifestations Psychologic Changes • Personality and behavioral changes • Emotional lability • Withdrawal • Depression

Case Study (©Purestock/Thinkstock) • K. W. states that he has had difficulty with itchy skin and assumed that it was simply related to winter dryness. • He also recently received a diagnosis of restless legs syndrome.

Diagnostic Studies • History and physical examination • Dipstick evaluation of protein • Urinalysis • Renal ultrasound/ biopsy • Albumin-to-creatinine ratio (first morning void) • GFR

Interprofessional Care • Overall Goals • • Preserve existing kidney function Reduce risks of CV disease Prevent complications Provide for patient’s comfort

Case Study (©Purestock/Thinkstock) • K. W. undergoes a renal biopsy, which shows severe damage of nephrons. • His BP is 154/88. • He receives a diagnosis of chronic glomerulonephritis. • He has stage 4 chronic kidney disease and begins conservative therapy.

Interprofessional Care Conservative Therapy • Correction of extracellular fluid volume overload or deficit • Nutritional therapy • Erythropoietin therapy • Calcium supplementation, phosphate binders

Interprofessional Care Conservative Therapy • Antihypertensive therapy • Measures to lower potassium • Adjustment of drug dosages to degree of renal function

Interprofessional Care Drug Therapy • Hyperkalemia • • • Restriction of high-potassium foods and drugs IV glucose and insulin IV 10% calcium gluconate

Interprofessional Care Drug Therapy • Hyperkalemia • • • Restriction of high-potassium foods and drugs IV glucose and insulin IV 10% calcium gluconate

Interprofessional Care Drug Therapy • Hypertension • • Weight loss (if indicated) Therapeutic lifestyle changes Diet recommendations (DASH Diet) Administration of antihypertensive drugs

Interprofessional Care Drug Therapy • Hypertension • Antihypertensive drugs • ACE inhibitors • ARB agents

Interprofessional Care Drug Therapy • CKD-Mineral and bone disease (MBD) • Phosphate not restricted until patient requires renal replacement therapy • Phosphate intake then restricted to < 1 g/day

Interprofessional Care Drug Therapy • CKD-MBD • Phosphate binders • Calcium acetate (Phos. Lo) • Calcium carbonate (Caltrate) • Bind phosphate in bowel and then excreted • Sevelamer hydrochloride (Renagel) • Lowers cholesterol and LDL levels

Interprofessional Care Drug Therapy • CKD-MBD • Phosphate binders • Should be administered with each meal • Side effect: constipation

Interprofessional Care Drug Therapy • CKD-MBD • Avoid aluminum preparations • Supplementing vitamin D • Calcitriol • Serum phosphate level must be lowered before calcium or vitamin D is administered

Interprofessional Care Drug Therapy • CKD-MBD • Controlling secondary hyperparathyroidism • Calcimimetic agents • Cinacalcet (Sensipar) • ↑ Sensitivity of calcium receptors in parathyroid glands • Subtotal or total parathyroidectomy

Interprofessional Care Drug Therapy • Anemia • Erythropoietin (EPO) • • • Epoetin alfa (Epogen, Procrit) Darbepoeitin alfa (Aranesp) Administered IV or subcutaneously Increased hemoglobin and hematocrit in 2 to 3 weeks Side effects: thromboembolism, hypertension

Interprofessional Care Drug Therapy • Anemia • Iron supplements • If plasma ferritin level is <100 ng/m. L • Side effects: gastric irritation, constipation • May make stool dark in color

Interprofessional Care Drug Therapy • Anemia • Folic acid supplements • Needed for RBC formation • Removed by dialysis • Avoid blood transfusions • Increase the development of antibodies • May lead to iron overload

Interprofessional Care Drug Therapy • Dyslipidemia • Statins (HMG-Co. A reductase inhibitors) • Most effective for lowering LDL level • atorvastatin (Lipitor) • Fibrates (fibric acid derivitives) • Used to lower triglyceride levels • gemfibrozil

Interprofessional Care Drug Therapy • Complications • Drug toxicity • • Digoxin Diabetic agents Antibiotics Opioid medications

Case Study (©Purestock/Thinkstock) • K. W. is started on the following medications: • • Darbepoetin alfa (Aranesp) weekly HCTZ 25 mg PO daily Captopril 25 mg PO bid Calcium carbonate 600 mg PO bid

Interprofessional Care Nutritional Therapy • Designed to maintain good nutrition • Monitor laboratory parameters • Protein intake • Normal for HD patient • Increased for PD patient • Fluid restriction • Intake depends on daily urine output

Interprofessional Care Nutritional Therapy • Sodium restriction • Diets vary from 2 to 4 g/day • Salt substitutes should be avoided because they contain potassium chloride

Interprofessional Care Nutritional Therapy • Potassium restriction • Limit: 2 to 3 g • High-potassium foods should be avoided

Interprofessional Care Nutritional Therapy • Phosphate restriction in ESRD • Limit: 1 g/day • Foods high in phosphate • Meat • Dairy products • Most foods high in phosphate are also high in protein • Phosphate binders essential

Nursing Management Nursing Assessment • Complete history of any existing kidney disease, family history • Long-term health problems • Drugs and herbal preparations • Dietary habits • Support systems

Nursing Management Nursing Diagnoses • Excess fluid volume • Risk for electrolyte imbalance • Risk for injury • Imbalanced nutrition: less than body requirements

Nursing Management Planning • Overall Goals • • Demonstrate knowledge and ability to comply with therapeutic regimen Participate in decision making Demonstrate effective coping strategies Continue with activities of daily living within physiologic limitations

Nursing Management Nursing Implementation • Health Promotion • Identify individuals at risk for CKD • • Diabetes mellitus Hypertension History or family history of kidney disease Repeated urinary tract infection • Regular checkups and changes in urinary appearance, frequency, and volume should be reported

Nursing Management Nursing Implementation • Acute Care • Most care for CKD occurs on an outpatient basis • In-hospital care required for management of complications and for kidney transplantation

Nursing Management Nursing Implementation • Ambulatory Care • Teach patient and caregiver about • Diet • Drugs • Common side effects • Pill organizer • Avoid over-the-counter drugs • Take daily BP • Identify signs of fluid overload, electrolyte imbalances

Nursing Management Nursing Implementation • Ambulatory Care • Patient can complete evaluation for kidney transplant • Explain what is involved in PD or HD, home dialysis modalities, transplantation, palliative care

Case Study (©Purestock/Thinkstock) • K. W. ’s condition stabilizes, and he is ready for discharge. • Peritoneal dialysis versus hemodialysis is discussed with him as a possibility in the future. • He begins asking if kidney transplantation will cure his chronic kidney disease.

Nursing Management Evaluation • The patient with CKD will maintain • Fluid and electrolyte levels within normal ranges • An acceptable weight with no more than a 10% weight loss

Audience Response Question The nurse teaches a patient with chronic kidney disease about prevention of complications. What should the nurse include in the teaching plan? a. Monitor for proteinuria daily with a urine dipstick. b. Perform self-catheterization every 4 hours to measure urine. c. Take calcium-based phosphate binders on an empty stomach. d. Check weight daily and report a gain of greater than 4 pounds.