Diabetes and Kidney Normal Kidney Diabetic Kidney Diabetic

Diabetes and Kidney
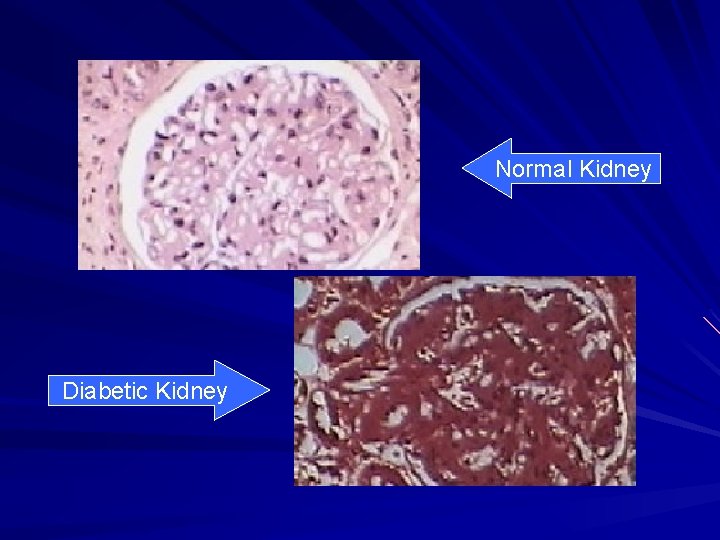
Normal Kidney Diabetic Kidney

Diabetic nephropathy Commonest cause of Renal failure 50 % of dialysis patients have DM 30 % of patients with type 1 & 2 develop renal failure This number will increase as the diabetic population is increasing

Risk factors for developing Diabetic Nephropathy Poor control of blood glucose, Long duration of Diabetes, Presence of other diabetic complication, Ethnicity (Asian, Pima Indians), Pre-existing High BP, Family h/o of Diabetic Nephropathy, Family h/o Hypertension.

Diabetic Nephropathy Clinical syndrome consisting of – Protein in urine – High BP – Decline in renal function If > 25 years elapse - unlikely to develop nephropathy.
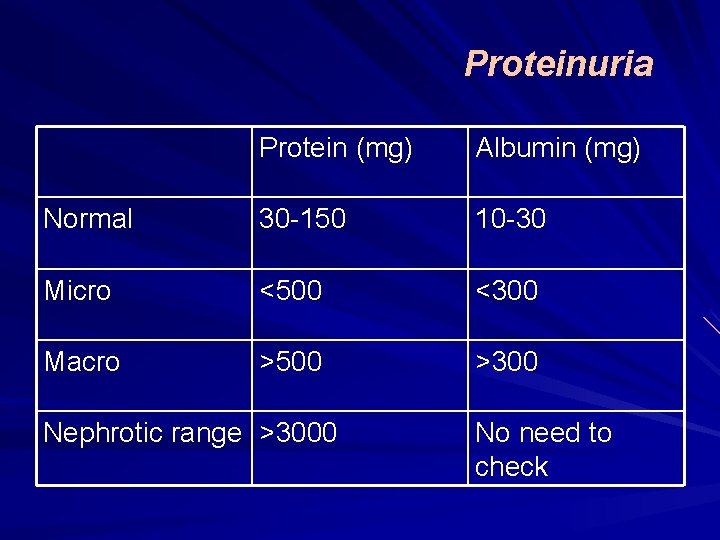
Proteinuria Protein (mg) Albumin (mg) Normal 30 -150 10 -30 Micro <500 <300 Macro >500 >300 Nephrotic range >3000 No need to check

Microalbuminuria Called micro… because it is not detectable by normal urine dip stick Urinary albumin (30 - 300 mg/day) Becomes irreversible when reaches 300 Detected by newer generation dipstix (micral)

Screening for microalbuminuria Whom to screen – Type 1 DM, from 5 years from diagnosis, – Annually from diagnosis Abnormal tests – Exclude recent vigourous exercise, fever, heart failure, urine infection, Prostatitis and menstruation, – Confirm observation twice, – Look for hypertension
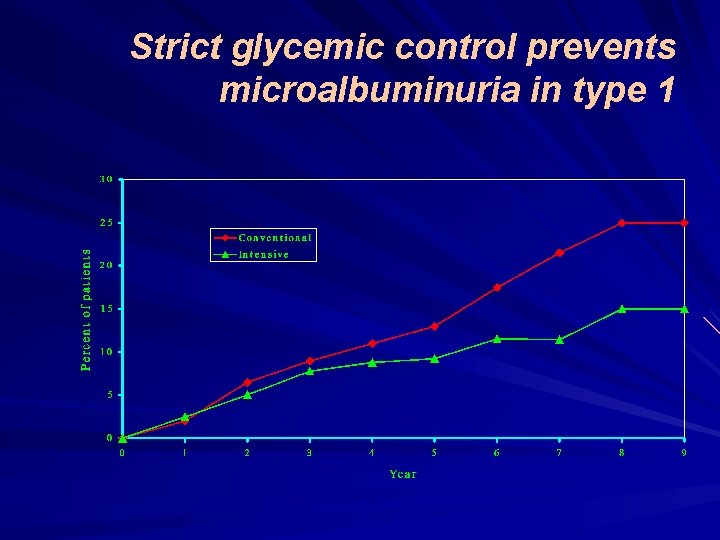
Strict glycemic control prevents microalbuminuria in type 1

Hypertension BP of < 130 / 80 is ideal – Prevents progression of Renal Failure – myocardial hypertrophy ACE I / ARBs - drugs of choice Use with caution if S. Creatinine > 3 mg Choice depends on comorbid conditions too – b blocker in CAD

Diet Calories - 35 K cal / kg Proteins of high quality - 0. 8 gm / kg Salt - 4 - 5 gm / day Potassium - 50 - 60 meq/day Lipids 30 % of calorie intake.

Fluid management Many diabetics have nephrotic state and severe edema and need rigorous salt & fluid restriction Severe edema. Mild to moderate No edema losses 600 - 800 ml / day equal to UOP + insensible

Ca - PO 4 metabolism To be tackled early to prevent secondary hyperparathyroidism AIM – Ca ~ 10, PO 4 < 5. 5 , Ca X PO 4 < 55 – Ca supplementation 1 - 1. 5 gm / day Ca. CO 3 - 40 % elemental Ca Ca acetate 20 % Ca with meals will act as PO 4 binder To be given empty stomach for Ca suppl. – Vit D 3 0. 25 – 1 mg /day If PO 4 very high, to be reduced first

Anaemia May occur when GFR < 50 % & almost always present when GFR < 30 % Correct deficiencies – Iron, Folic acid, Vit B 12, Pyridoxine Erythropoietin 75 - 150 iu/kg SC – – – With Iron supplements Expensive therapy Rs. 8 - 10, 000 / month Hb % maintained at 11 - 12 > 13 in pts with CAD

Others Lipid lowering - diet, statins Low dose aspirin Avoid nephrotoxic drugs & contrast procedures Prevent & treat infections energetically Hepatitis B immunization – Early immunization ideal – if Cr. > 3 double & more frequent dosing

Options of Renal Replacement Therapies Dialysis – Hemodialysis – Peritoneal dialysis Continuous Ambulatory Peritoneal Dialysis Continuous Cyclic Peritoneal Dialysis Renal Transplantation Simultaneous Pancreas Kidney Transplantation

Renal replacement therapy Very expensive Hemodialysis (HD) Rs. 12 - 15000 / mo Peritoneal dialysis (PD) Rs. 20000 / mo Renal Transplantation 3 - 3. 5 Lakhs for first year k. Not funded by the Government k. Not covered by insurance Hence the real need to prevent diabetic ESRD

Conclusion Pathogenesis and progression of Renal Disease in Diabetics is multifactorial and intervention should be multi-pronged Glycemic control Hypertension control Treat dyslipdemia Others – Diet, Smoking cessation, Exercise etc.
- Slides: 18