Trauma of Urinary Tract RENAL TRAUMA Introduction Injury

























































- Slides: 93

Trauma of Urinary Tract

RENAL TRAUMA Introduction Injury to the kidney is seen in approximately 8%– 10% of patients with blunt or penetrating abdominal injuries. n The vast majority (80%– 90%) of cases involve blunt rather than penetrating injury. n

Introduction Serious renal injuries are frequently associated with injuries to other organs; multiorgan involvement occurs in 80% of patients with penetrating trauma and in 75% of those with blunt trauma n The vast majority (98%) of isolated renal injuries are classified as minor injuries n

Indications for Imaging Evaluation n n Children with blunt trauma and hematuria. blunt trauma if associated with gross hematuria microscopic hematuria and hypotension penetrating injury and hematuria. blunt trauma in patients with other injuries known to be associated with renal injury.

Imaging Modalities Computed Tomography. n Intravenous Urography. n Angiography. n Retrograde Pyelography. n Ultrasonography. n Radionuclide Renal Scintigraphy. n MR Imaging. n

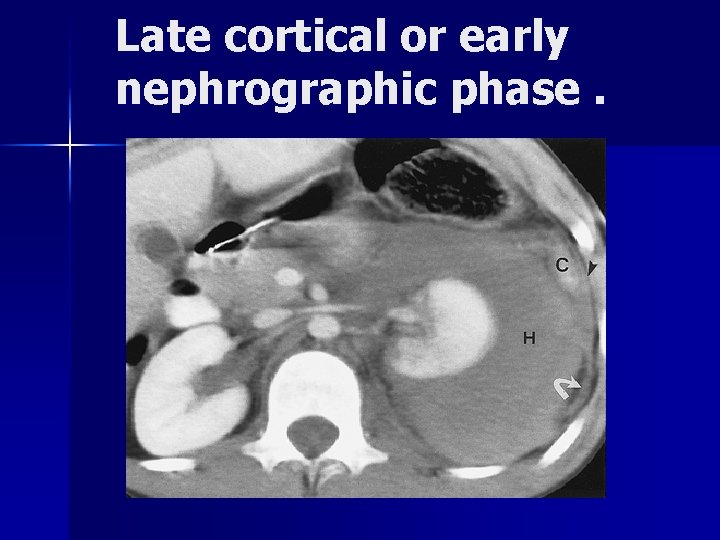
CT SCAN n n n provide precise delineation of a renal laceration. determine the presence and location of a renal hematoma. presence of active arterial extravasation. presence of urinary extravasation. presence of devascularized segments of renal parenchyma. differentiate trivial injuries from those requiring intervention.

Late cortical or early nephrographic phase.

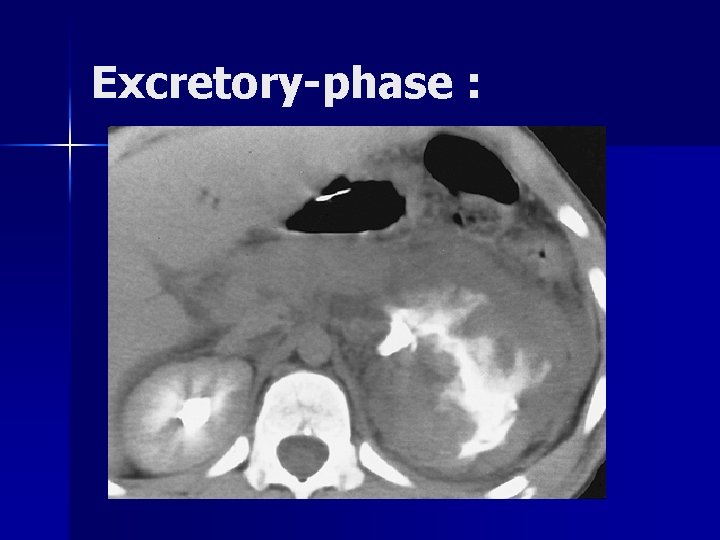
Excretory-phase :

Intravenous Urography : no longer the primary modality n primary role: assessment of gross function n evaluation of the uninjured kidney in hemodynamically unstable patients n unstable to undergo CT n already in the operating room n

Angiography most vascular injuries can be assessed with CT n can provide more detailed information regarding the exact anatomic area of vascular injury n embolization may be used for nonsurgical therapy in hemodynamically stable patients n evaluation of suspected vascular complications of injury n

Retrograde Pyelography n assessment of ureteral and renal pelvic integrity when ureteropelvic junction injury is suspected n not helpful in evaluating renal parenchymal injuries

Ultrasonography detecting hemoperitoneum in patients with suspected intraperitoneal injuries following blunt trauma n limited compared with CT in the evaluation of the renal parenchyma n comparing US with CT in this setting, several renal injuries were missed at trauma US n

Radionuclide Renal Scintigraphy helpful in documenting the presence of a functioning kidney n in patients with a contraindication for iodinated contrast material n in following up repair of renovascular trauma n

MR Imaging to assess suspected renal injury n when there is a contraindication for iodinated contrast material n when CT is not available n Like contrast-enhanced CT, MR imaging with use of intravenous gadolinium-based contrast material has proved helpful in the assessment of urinary extravasation n

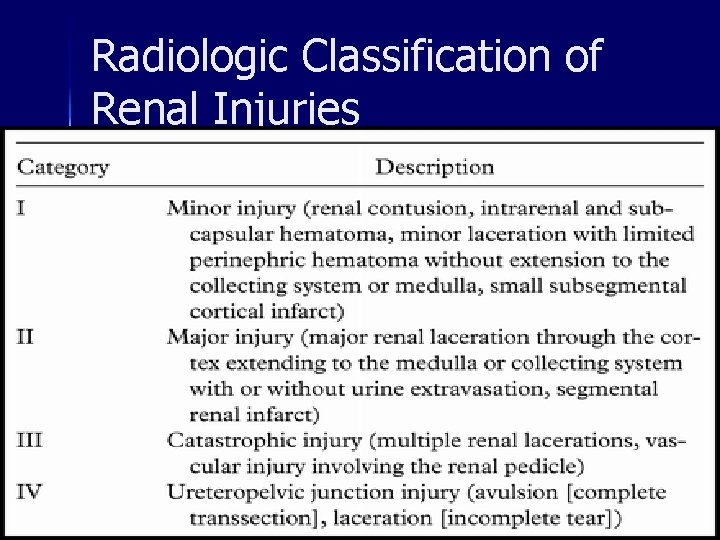
Radiologic Classification of Renal Injuries

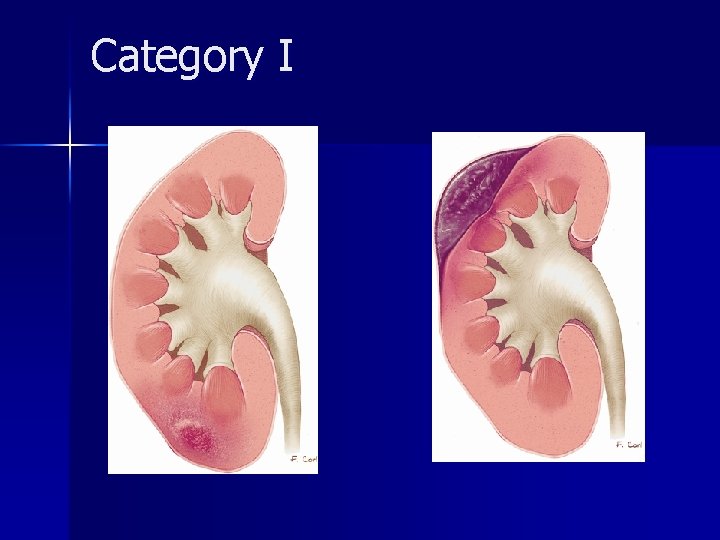
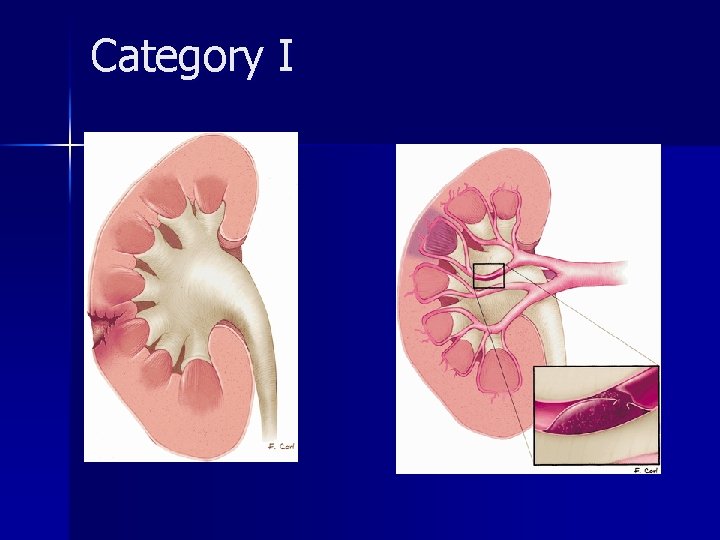
Category I

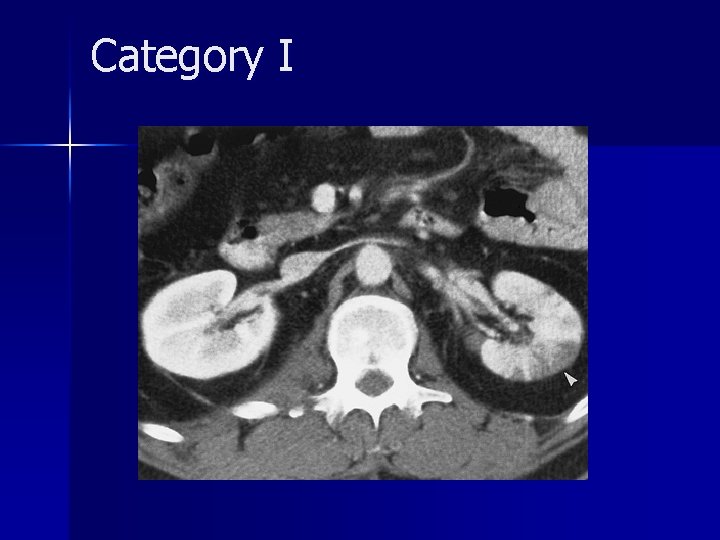
Category I

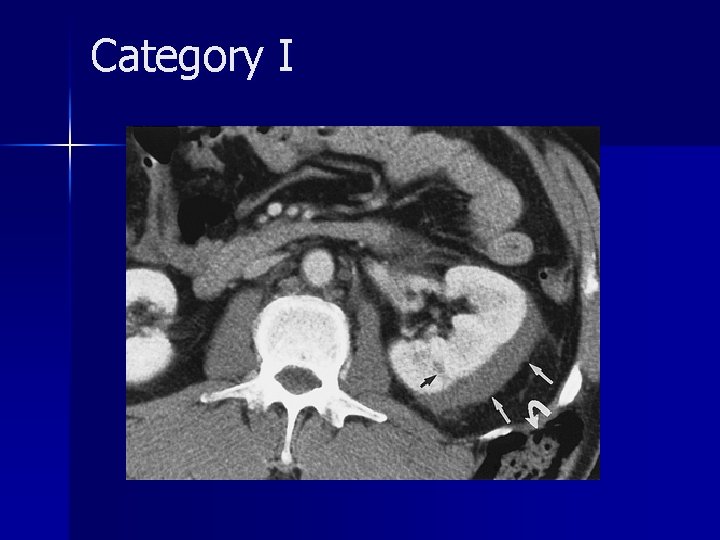
Category I

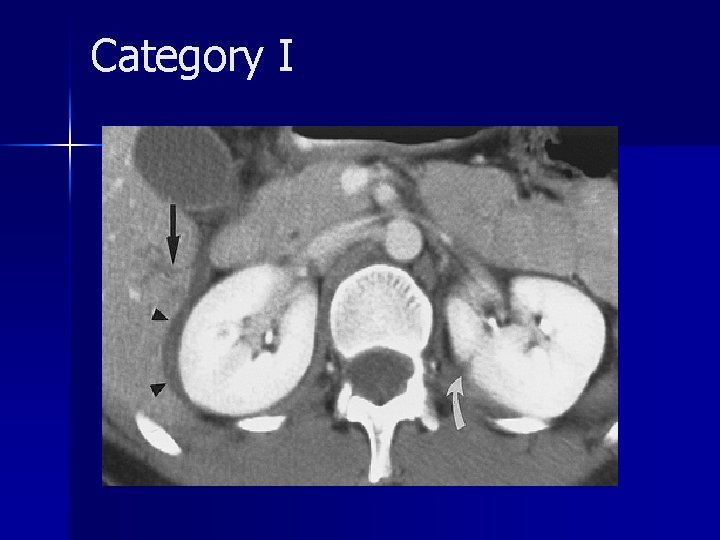
Category I

Category I

Category I n Category I renal injuries constitute 75%– 85% of all renal injuries in most series and are generally managed conservatively. n The vast majority of minor injuries represent small intrarenal hematomas (renal contusions). n Subsegmental infarcts are increasingly recognized at CT and usually they end result in scar formation.

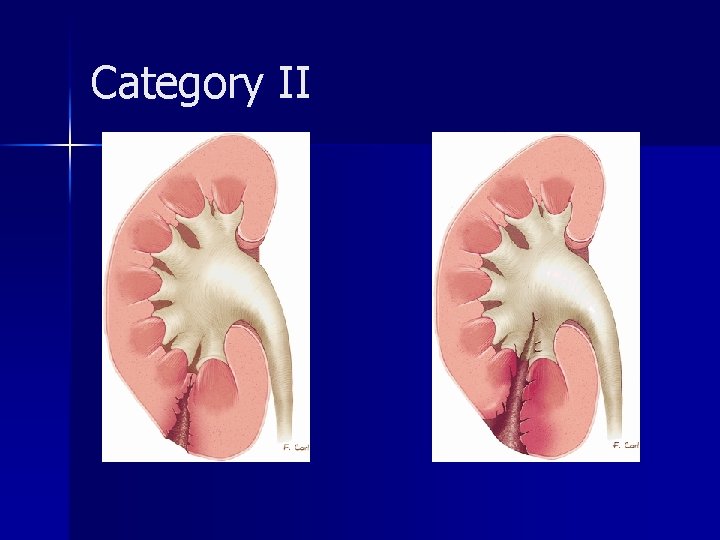
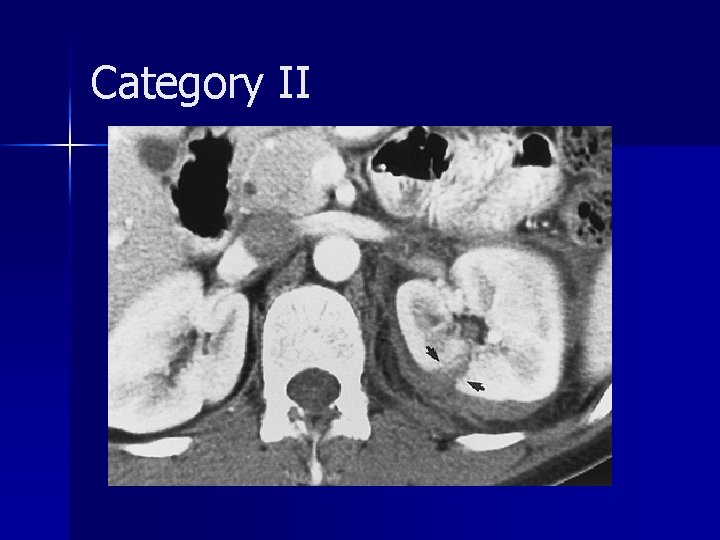
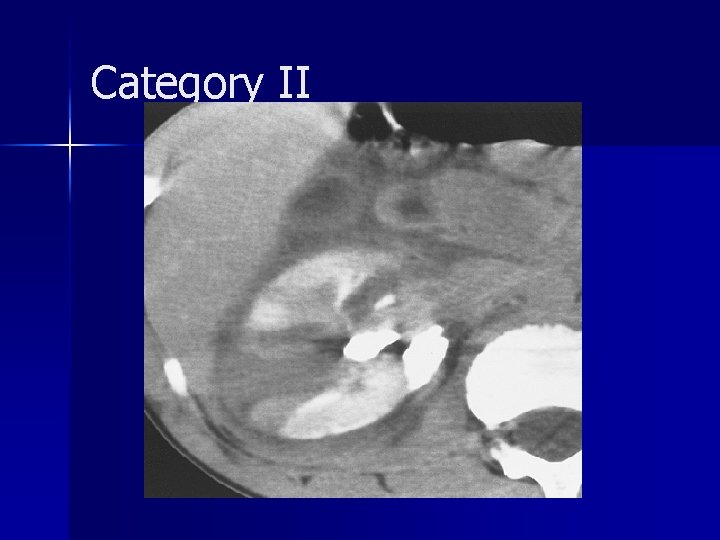
Category II

Category II

Category II

Category II Comprise approximately 10% of renal injuries n Urine leakage usually occurs into the lateral perinephric space n Surgical exploration depending on hemodynamic status and the evolution of the injury n Follow-up CT may be necessary to assess interval change in the appearance of the injury n

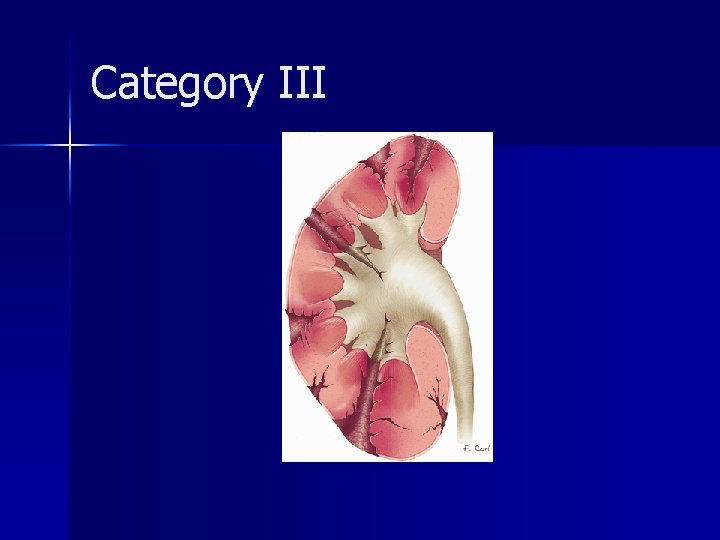
Category III

Category III

Category III

Category III

Category III

Category III

Category III

Category III

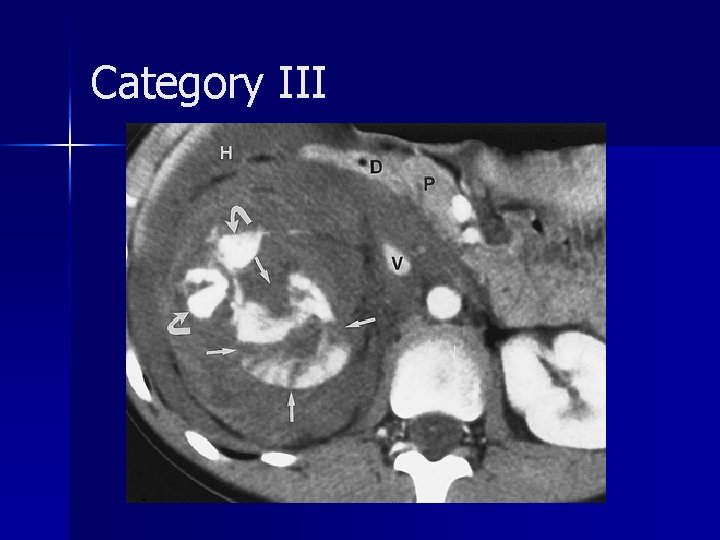
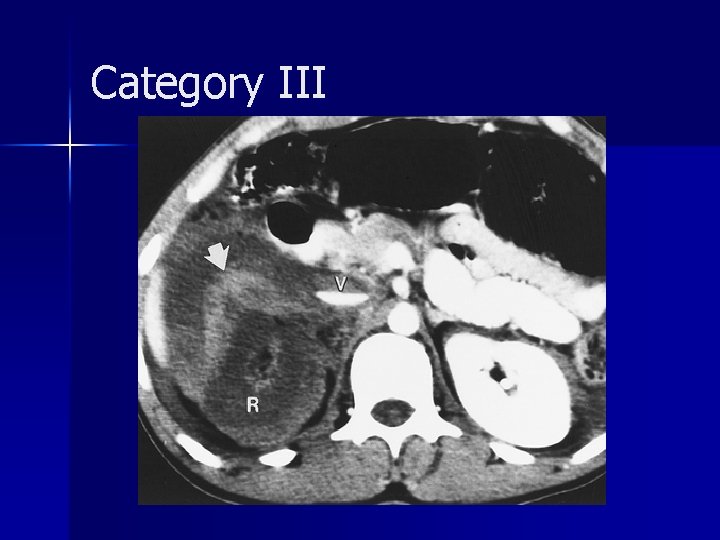
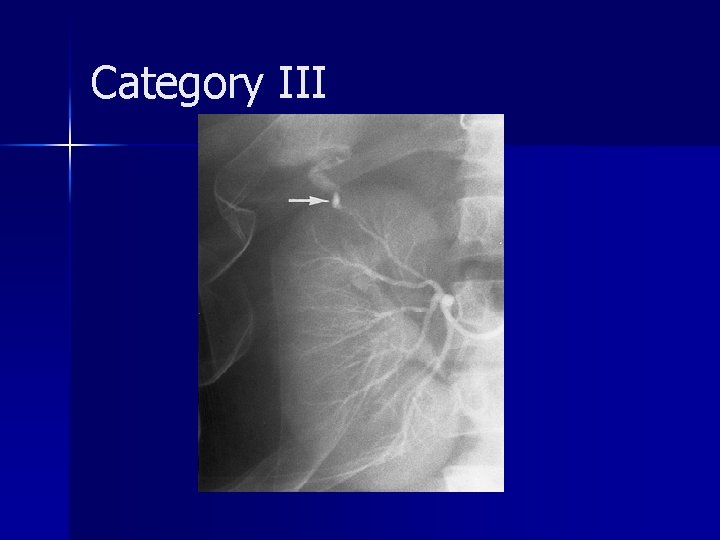
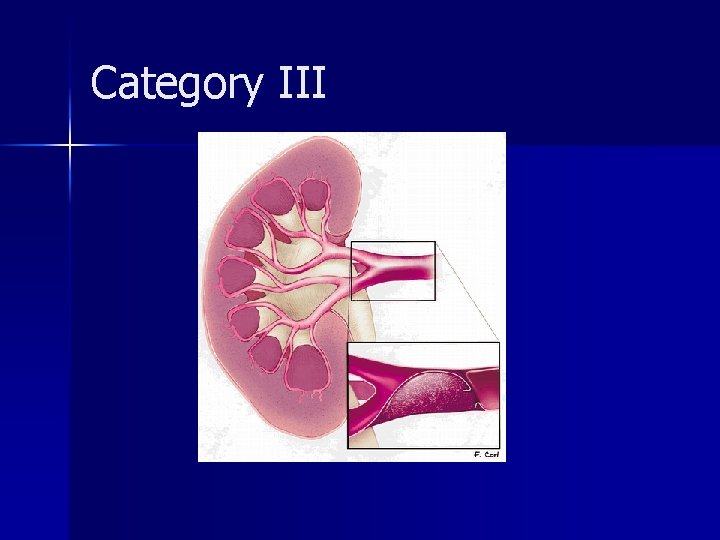
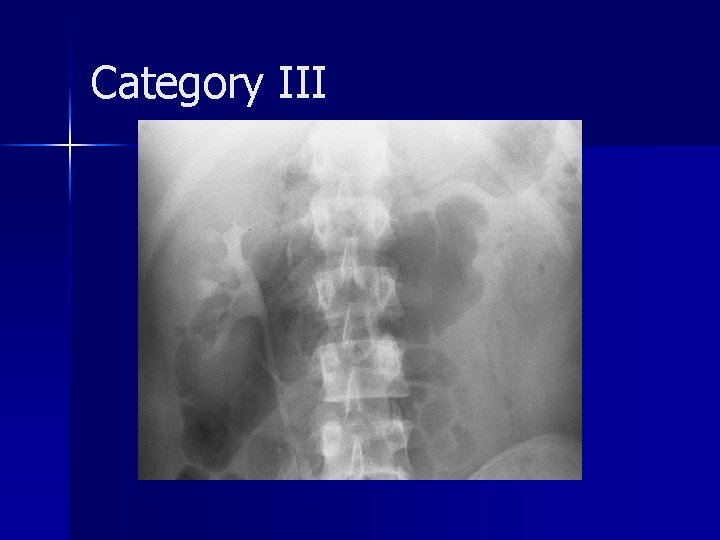
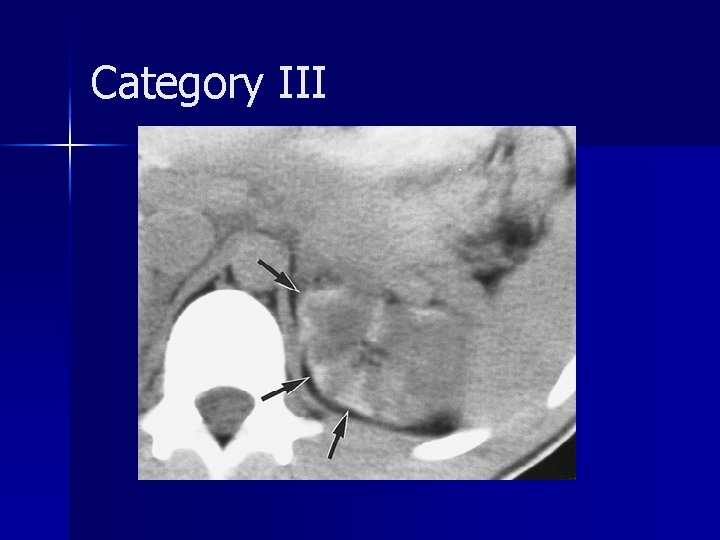
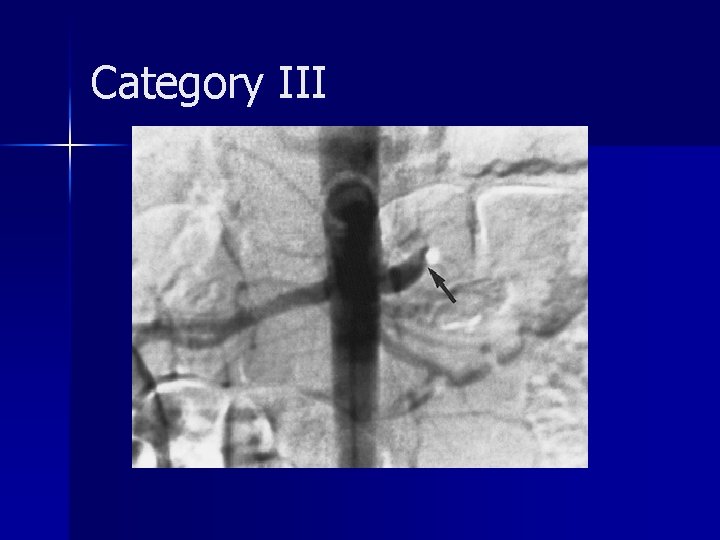
Category III account for approximately 5% of cases n generally require surgical exploration, often nephrectomy n Intraarterial embolization may be used to salvage the kidney n The absence of a perinephric hematoma is characteristic of a renal arterial occlusion n

Category III A review of the literature showed that only five (14%) of 35 patients with unilateral posttraumatic occlusion of the renal artery who underwent revascularization had return of normal renal function; in all five patients, the duration of the ischemia was less than 12 hours n revascularization may be attempted in patients with only one kidney or with bilateral renal arterial thrombosis n

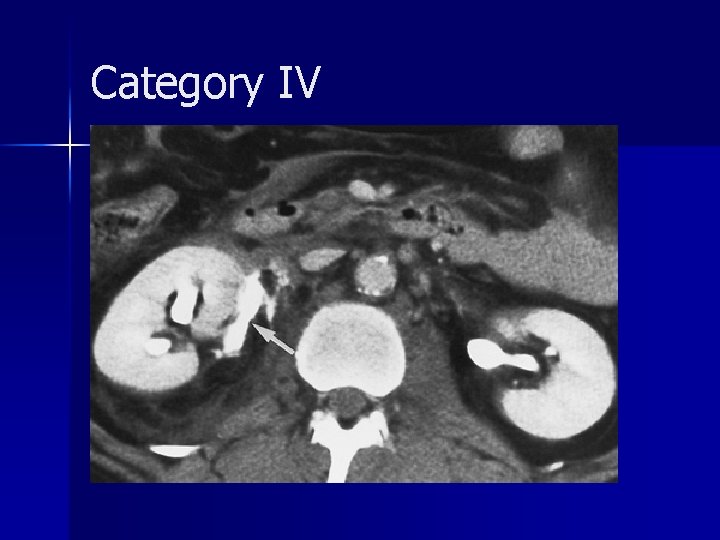
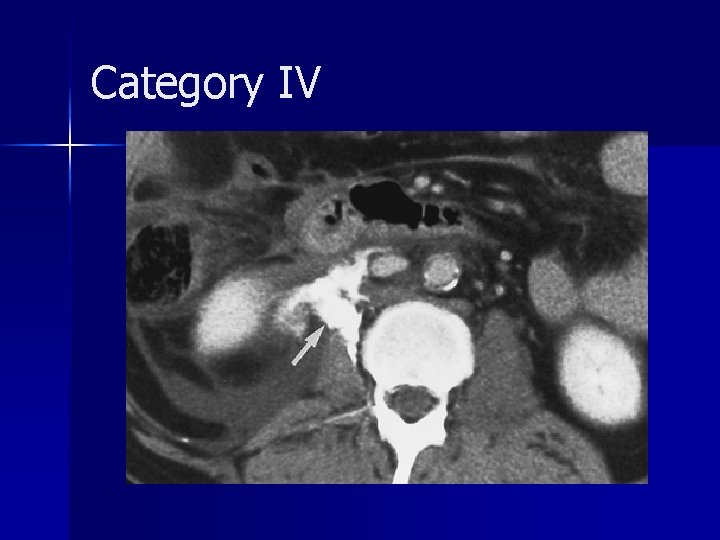
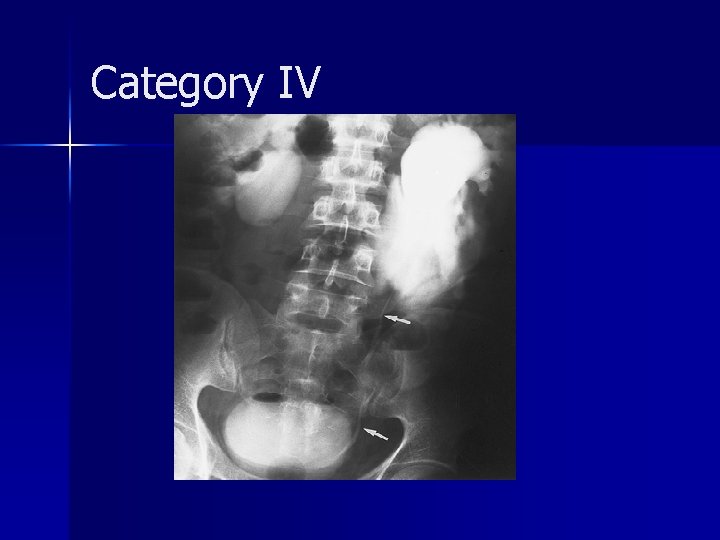
Category IV

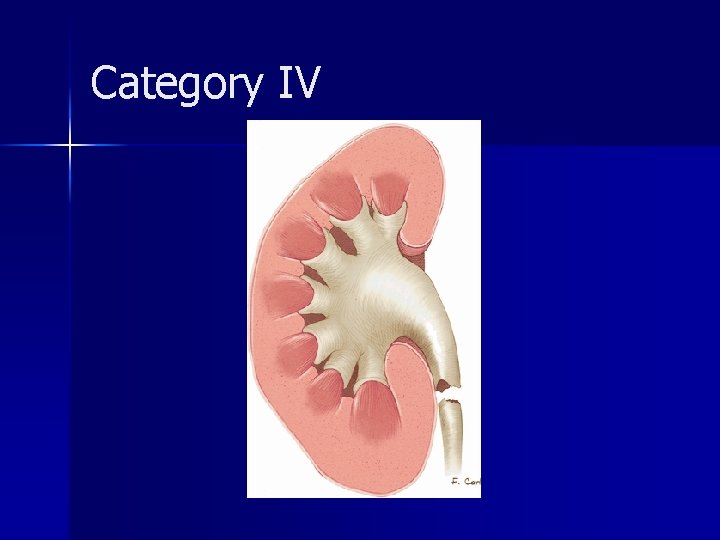
Category IV Rare consequence of blunt trauma and are caused by sudden deceleration. n The diagnosis may be delayed because hematuria is absent in one-third of patients. n Medial perinephric urinary extravasation. n A circumferential (circumrenal) urinoma may be seen around the affected kidney, but typically there is no perinephric hematoma. n Two groups: avulsion (complete transection) and laceration (incomplete tear). n

Category IV

Category IV

Category IV

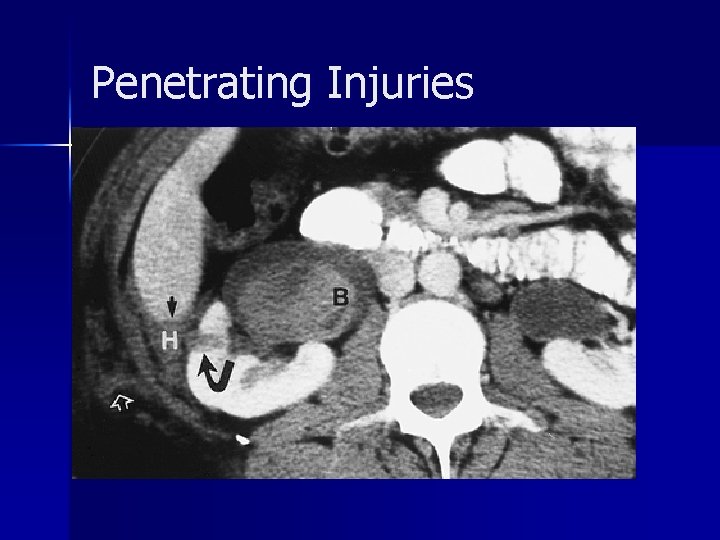
Penetrating Injuries

Penetrating Injuries n CT is not usually performed in patients with an anterior stab wound because these patients generally require exploratory laparotomy due to the high prevalence of bowel injury associated with this form of trauma.

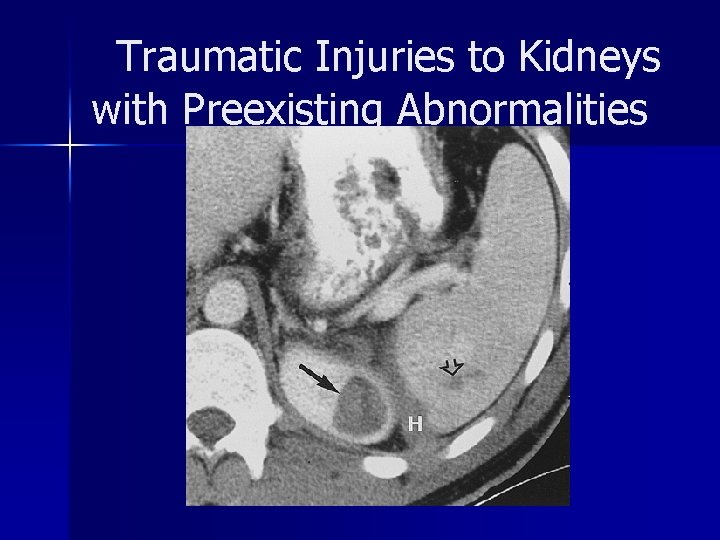
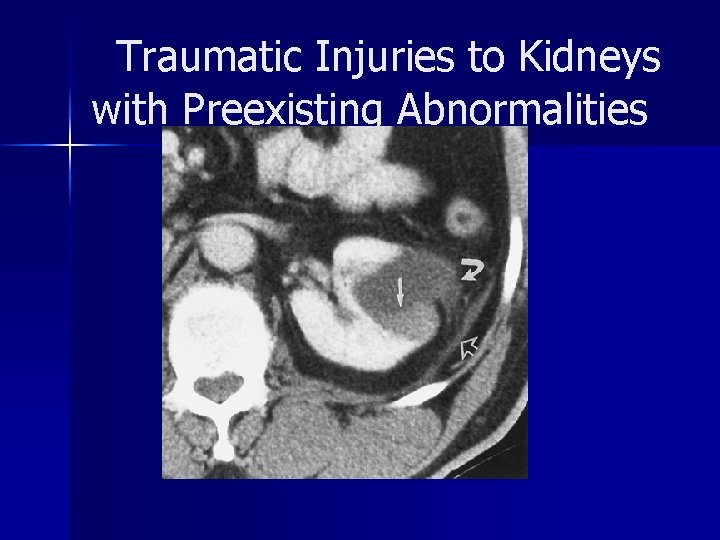
Traumatic Injuries to Kidneys with Preexisting Abnormalities disruption of the renal pelvis or ureteropelvic junction in patients with hydronephrosis or an extrarenal pelvis n intracystic hemorrhage or rupture of a renal cyst with or without communication with the collecting system n rupture of a tumor. n

Traumatic Injuries to Kidneys with Preexisting Abnormalities laceration of poorly protected ectopic or horseshoe kidneys n laceration of fragile, infected kidneys n CT provides more specific and clinically useful information than excretory urography in this context n

Traumatic Injuries to Kidneys with Preexisting Abnormalities

Traumatic Injuries to Kidneys with Preexisting Abnormalities

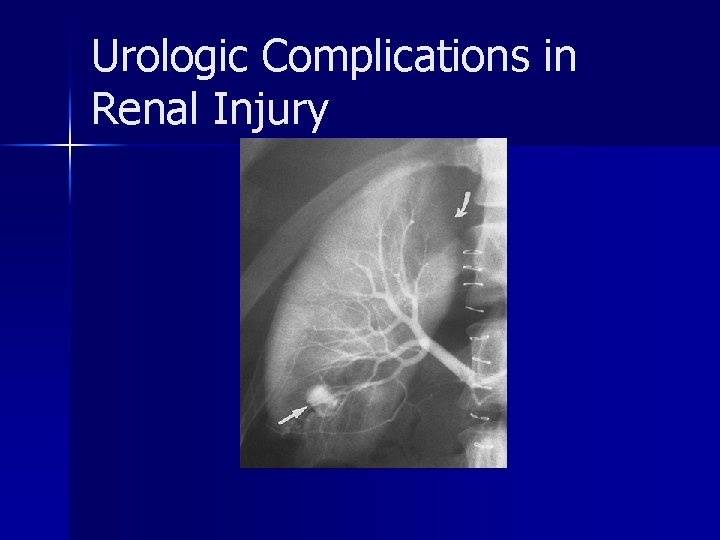
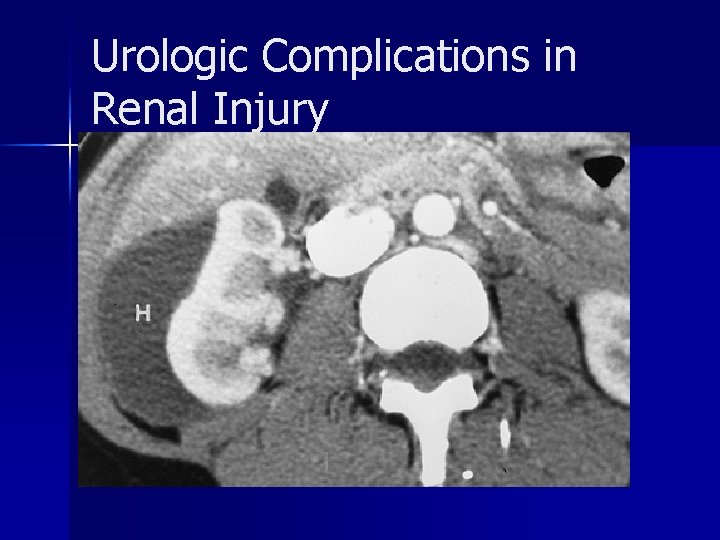
Urologic Complications in Renal Injury n Early: include urinary extravasation and urinoma formation, delayed bleeding, infected urinoma, perinephric abscess, sepsis, arteriovenous fistula, pseudoaneurysm and hypertension n Late: include hydronephrosis, hypertension, calculus formation, and chronic pyelonephritis

Urologic Complications in Renal Injury delayed urologic complications occur more frequently in patients with a devascularized fragment than in those with vascularized fragments. n Infected urinomas and perinephric abscesses frequently occur in patients with an unrepaired, devitalized renal segment and concomitant injury to the pancreas or bowel n

Urologic Complications in Renal Injury

Urologic Complications in Renal Injury

Conclusions CT plays a major role in assessing patients with renal injuries n Understanding the radiologic classification of traumatic renal injuries is helpful in patient triage n The imaging findings in renal injury should be integrated with clinical information to assist in developing a treatment plan n

Lower Genitourinary Trauma Introduction n It is not life threatening per se, but their association with other potentially more significant injuries necessitates an organized approach to diagnosis and management n Other injuries often take priority over injuries to the GU system and may initially interfere or postpone a complete urologic assessment n Initial evaluation should not differ from that of other trauma patients

Pathophysiology n n n The lower GU tract comprises the urinary bladder, urethra, and external genitalia (penis and scrotum). Blunt, penetrating and iatrogenic Bladder injury is rare owes to the bladder's protected position deep within the bony pelvis. Most bladder injuries occur in association with blunt trauma. (extra-, intraperitoneal, or combined) 85% of bladder injuries occur with pelvic fractures especially pubic ramus fractures (95%). Intraperitoneal rupture usually occur due to blow

Pathophysiology. . . n n Urethral injury is predominantly a male problem. 60% blunt, 40% iatrogenic and penetrating In males, the urethra is divided into the proximal (posterior) segment and the distal (anterior) segment by the urogenital diaphragm. The posterior urethra extends from the bladder to the urogenital diaphragm. - prostatic - membranous (sphenctiric)

Pathophysiology. . . n Posterior urethra injuries: mostly secondary to pelvic fractures. n Anterior urethral injuries (bulbous & pendulous) – straddle-type (e. g. bicycles, skateboards) – penetrating (often self-inflicted) injuries. n Anterior urethral injuries are most often isolated

Pathophysiology. . . External genitalia injuries are usually secondary to injuries caused by: - Gun-shots or penetration - Blunt trauma - Vigorous sexual activity - Suction device cleaners - Mutilation (self-inflicted or otherwise).

Main causes of bladder injuries – – – Motor Vehicle Accidents Bicycle accidents Stabbings Impalements Gunfire Iatrogenic

Main causes of urethral injuries – Straddle-type mechanism (e. g. bicycles, skateboards, falls onto the perineum) – Mutilation (self-inflicted or otherwise) – Gunfire – Stabbings – Iatrogenic

History. . . n n n Bladder trauma: SP pain Hematuria - in blunt trauma 95%-100% have gross hematuria - in penetrating trauma often microscopic Inability to void after the injury. If the patient can not provide such information and gross hematuria is present, suspect bladder injury. i. e. Patients with any degree of hematuria after lower abdominal penetrating injury should undergo complete diagnostic evaluation for bladder and ureteral injury.

History. . . Urethral trauma – Knowledge of associated injuries that can cause urethral injury is required for diagnosis. – Bleeding per urethra (urethrarhagia) – A history of inability to void indicates the possibility of urethral trauma. External genitalia trauma n a history of psychiatric problems n use of penile rings n excessive sexual activity n A history of popping sound, sudden pain, loss of erection, and swelling after trauma to the erect penis is important (penile)

n Penile trauma – Loss of skin – Swelling and ecchymosis – Angulation – Palpable corporal defect – "rolling sign, " in which clot lying near the fracture site is palpable as a firm, immobile, discrete swelling over which the penile skin can be rolled. – hugely deformed ecchymotic penis ("eggplant deformity"), a sign that is highly diagnostic of # – Level of mutilation – Viability of mutilated segment

Scrotal trauma – Edema – Loss of skin – Discoloration – Tenderness – Condition of testes

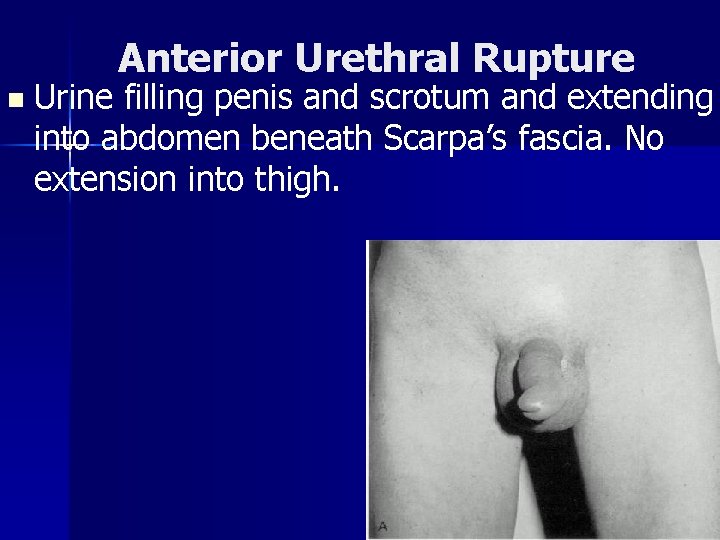
Anterior Urethral Rupture n Urine filling penis and scrotum and extending into abdomen beneath Scarpa’s fascia. No extension into thigh.

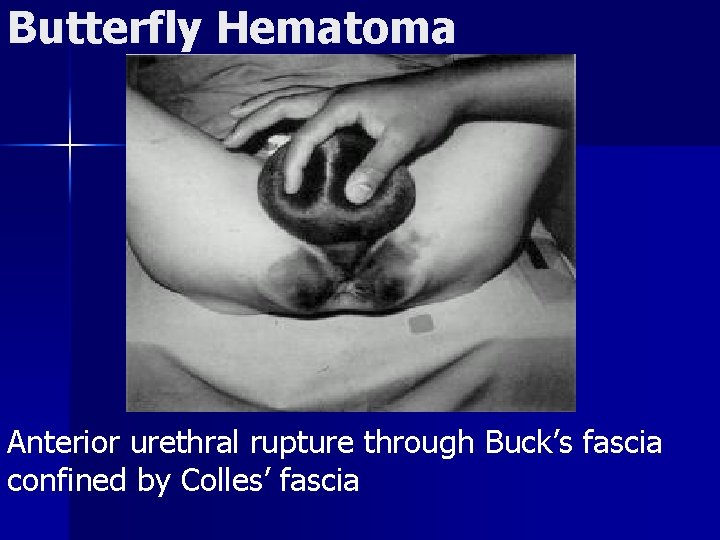
Butterfly Hematoma Anterior urethral rupture through Buck’s fascia confined by Colles’ fascia

Lab Studies: n CBC to obtain a hematocrit and a platelet count n PT and a PTT to check for coagulopathy n Blood type and cross matching n Urinalysis to assess for hematuria.

Imaging Studies: n Plain radiograph of the pelvis to assess presence and extent of bony injury n Retrograde urethrogram – Indicated prior to the insertion of a Foley catheter when urethral injury is suspected and in all patient with penetrating penile injury (involve the urethra in 50%) – Urethrography is performed with water-soluble contrast material and preferably under fluoroscopy – If fluoroscopy is unavailable, multiple plain films are obtained with 10 -m. L injections of contrast material into the distal urethra

– Perivesical hematomas may be seen on cystograms as compression or displacement of the bladder. (Tear drop appearance) – Gross hematuria without extravasation indicates bladder contusion. – Extravasation of contrast material into the bowel lumen or into the vagina is possible in penetrating trauma.

Imaging Studies. . . Ultrasonography – Used as a screening tool to indicate bladder wall abnormalities or presence of fluid in the abdomen but suffers from low sensitivity in excluding bladder injury. – It is also used in assessing the condition of the testes. (contraversial) – May be useful in the acute setting of abdominal trauma as part of the focused abdominal sonography in trauma (FAST) examination of the injured patient. – Unclear rule in penile fracture n CT scan of abdomen and pelvis – CT cystography is Specific in aiding in the diagnosis of bladder injuries but carries low sensitivity. – Because most of these patients already require CT to evaluate pelvic fracture or intra-abdominal injury, CT cystography saves time.

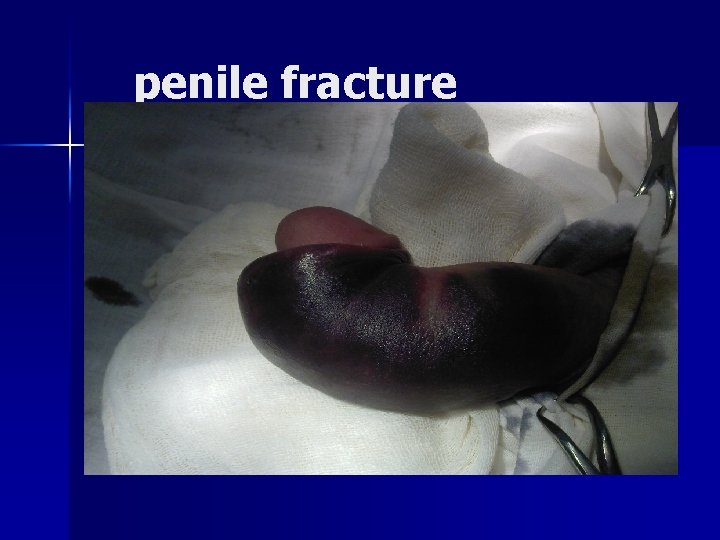
penile fracture

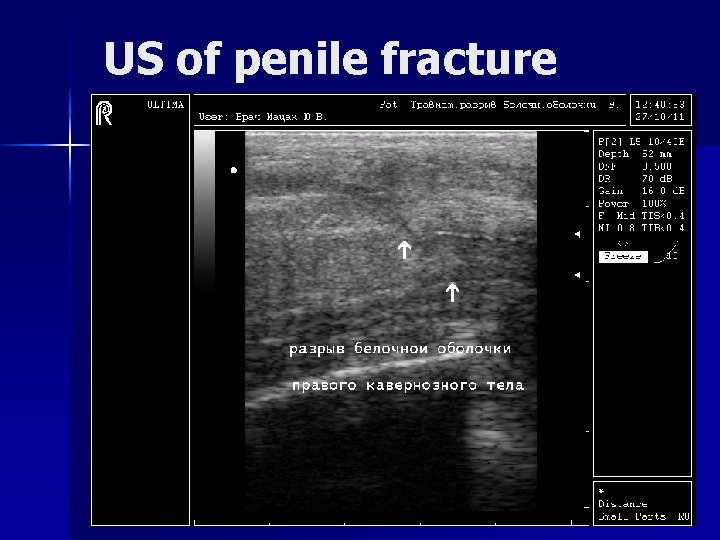
US of penile fracture

Management of Bladder Trauma Bladder contusion – Adequate drainage of the bladder should result in resolution within a few days. – Follow-up cystography is recommended to assess integrity of the bladder wall. Extraperitoneal rupture n Can most commonly be managed with adequate bladder drainage and broad-spectrum antibiotics. n Cystogram should be performed after 10 -14 days n The catheter should be removed if extravasation has resolved (76% to 87%) , but if the extravasation is persistent, cystography is repeated at 21 days (all heal by 3 weeks. surgical intervention is required if persist. n Persistent severe hematuria and infection of the pelvic hematoma are contraindications to conservative therapy.

Management of Bladder Trauma Extraperitoneal rupture n n n Another relative indication for repair of extraperitoneal rupture is found in patients undergoing laparotomy for other reasons Surgical repair is performed by opening the dome of the bladder and repairing the laceration from the inside in one layer. At open repair, careful inspection for associated lower urinary tract injuries is mandatory so as not to miss urethral disruption, prostate injury, bladder neck injury, or unexpected intraperitoneal injuries. If the bladder has been repaired, a cystogram is obtained 7 to 10 days after surgery some authors have supported open repair of extraperitoneal bladder rupture.

Management of Bladder Trauma Intraperitoneal rupture n Surgically repaired with a watertight two-layer closure with absorbable suture and perivesical drain placement. n Adequate drainage with a urethral catheter and suprapubic cystostomy catheter for 10 days. n A cystogram should be performed to assess the integrity of the repair before removing catheters. n The urethral catheter should be removed and the postvoid residuals should be checked for to ensure adequate bladder evacuation before removing the suprapubic cystostomy catheter the following day.

n 1. 2. n There are several reasons for this approach: Intraperitoneal ruptures are often much larger than suggested on cystography and are unlikely to heal spontaneously. They cause urinary leakage into the abdominal cavity with resultant peritonitis, which can be fatal. Prophylactic Antimicrobial Agents

Management of Bladder Trauma Penetrating injuries n The preferred method is surgical intervention; open the dome of the bladder and perform a full inspection. n Indigo carmine IV injection is used to help identify distal ureters.

Management of posterior Urethral Injury I. II. Primary Realignment (stenting) Suprapubic Cystostomy (p/c or open) 1. Failed primary realignment 2. Unstable patient 3. Always (96%) develop a urethral stricture requiring posterior urethroplasty III. Delayed Reconstruction (3 -12 M) 1. At 3 months, scar tissue at the urethral disruption site is stable and mature 2. After the associated injuries are stabilized and the patient is ambulatory.

Management of anterior Urethral Injury n Initial S. P. C. is the treatment of choice for straddle injuries or blunt crushing injuries to the anterior urethra and secondary repair is planned 3 months post injury n most experts have recommended primary surgical repair of urethral gunshot injuries (low-velocity) n Initial suprapubic urinary diversion is recommended after high-velocity gunshot wounds to the urethra, followed by delayed reconstruction

Management of penile injury (amputation) n every attempt should be made to do replantation, even against the patient's wishes at the time n The amputated penis should be wrapped in sterile gauze wetted with sterile saline and placed within a sterile plastic bag in a second container of ice and water. (This combination solution prevents contact cold ischemic injury. ) n Success has been reported after 16 hours of cold ischemia, and after 6 hours of warm ischemia n If the amputated segment is not available for replantation, then penile resection, with closure of the corpora and formation of a spatulated urethral neomeatus, is performed

Management of penile injury (amputation) n n n Later, if the patient desires reconstruction, several options exist to lengthen the remaining penile stump: (1) releasing the suspensory ligament (2) defatting the pubis (3) placing a rigid penile prosthesis after multiple relaxing incisions in the corpora cavernosa (4) Total free flap penile reconstruction may also be required

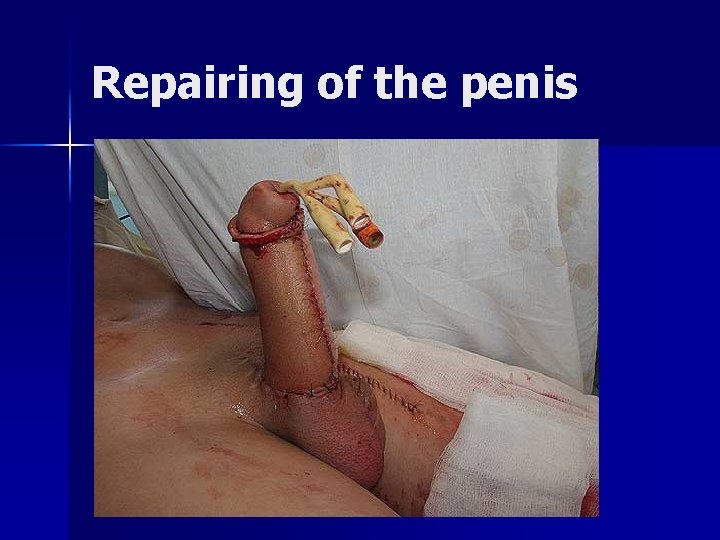
Repairing of the penis

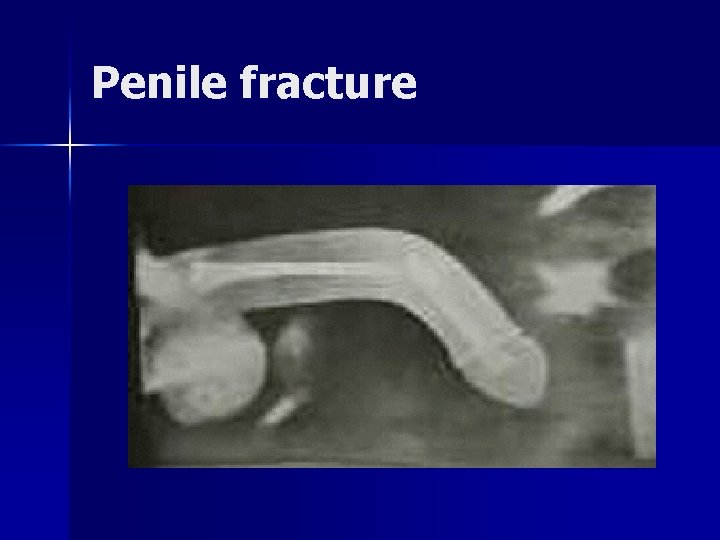
Penile fracture

Management of penile injury (Penile Fracture ) n n Due to rupture of the corpus cavernosum from trauma to the erect penis Conservative treatment involving sedatives, ice packs, and pressure bandages is condemned because of: – – – – prolonged hospitalization (4 to 71 days), healing with deformity in as many as 10%, prolonged penile pain, sometimes for months penile pulsatile hematoma, huge penile residual mass, pulsatile cavernosal diverticulum, and expanding penile hematoma

Dangerous postures»

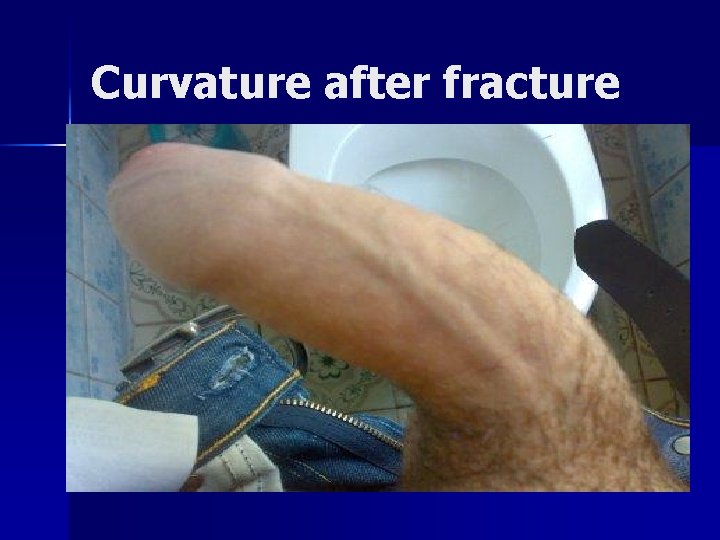
Curvature after fracture

Management of penile injury (Penile Fracture) n Because of the unacceptable complication rate associated with non-operative treatment, we advocate immediate repair of penile fracture n faster recovery, shorter hospitalization, less morbidity, and less penile deformity n Sub-coronal approach is recommended because it allows excellent exposure of the entire penis, as required in large or bilateral ruptures or associated urethral injury n A high suspicion for associated urethral injury must be maintained during open inspection of the injury

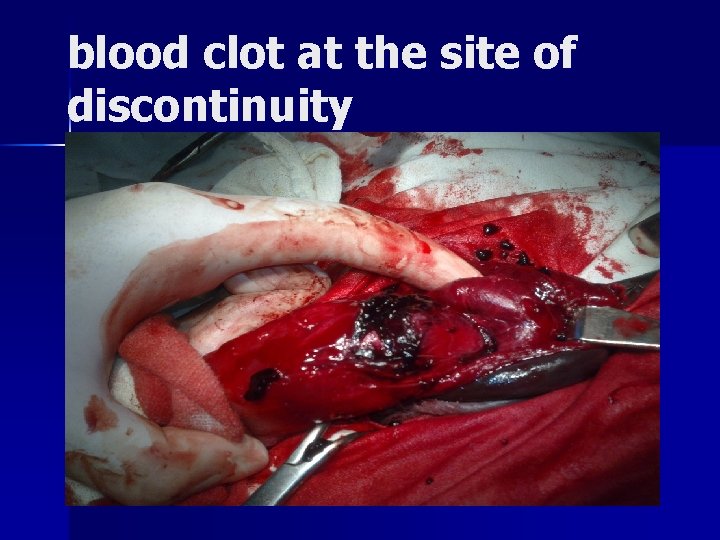
blood clot at the site of discontinuity

suturing of rapture tunica albuginea and urethra

Management of testicular injury n Explore and repair all cases of significant hematocele, intratesticular hematoma, or frank rupture of the tunica albuginea. n Lack of evidence for tunical rupture on ultrasound is not a sufficient reason to delay exploration because it results in increased orchidectomy rates n When gunshot wounds involve the testicle or spermatic cord, the testicle can be salvaged in only 35% to 65% n In blunt injury, significant intratesticular hematoma should be drained because increased intratesticular pressure from these collections can result in testicular atrophy and appearance of ASAT

Management of testicular injury n Significant, mutilating injuries of the scrotum, such as those that occur after close-range shotgun blast, should be treated in a staged fashion n Conservative therapy results in higher orchiectomy rates when the patient's condition ultimately forces delayed scrotal exploration

Complications n Bladder injuries – Urinomas – Fistulization (rectum, vagina, bowel, cutaneous) – Pelvic hematoma infection – Difficulties voiding – Distal ureteral obstruction

Complications n Urethral injuries – Strictures – Incontinence – Impotence n Penile injury – Angulation – Painful erection – Impotence

Complications Scrotal injuries – Infection – Loss of testes – Skin necrosis – Testicular atrophy – Infertility n Prognosis for patients with lower GU tract injuries is related to their associated injuries n
