Urinalysis Laboratory Procedures Ch 5 Urinalysis n n

Urinalysis Laboratory Procedures Ch. 5

Urinalysis n n This test is often part of an initial data base for case work up of a clinically ill patient. It is a very useful indicator of renal function, and should be performed on any animal suspected to have renal disease or urinary tract pathology

Urinalysis n A urinalysis consists of gross examination of urine, a specific gravity (SG), chemical analysis, and sediment evaluation. n Equipment required : clean glass or plastic collection container, a centrifuge and conical centrifuge tubes, chemical reagent strips, clean glass slides and coverslips, a refractometer and microscope. A sediment stain is recommended.

n The best samples for urinalysis are morning samples. These are the most concentrated. n Urine samples should be analyzed within 30 minutes to 1 hour of collection. n Physical properties of urine include volume , color, odor, transparency, and specific gravity.

Collection for analysis n n n There are several different methods of collection for urinalysis and each has its benefits and draw backs. Collection methods will often be dictated by the information that you are looking to gather. Analysis of urine samples should be performed only in samples taken before administration of therapeutic agents.

Midstream, voided or “Free Catch” n n n This collection method is often easiest for the animal but can be quite difficult for the collector. Collection is made into a container directly from the patient. This collection method will obviously contain contamination

Manual Expression: n This collection method is most often performed on small dogs and cats. It is sometimes difficult, and can result in trauma in the form of red blood cells in the urine. This method will also contain contamination from the lower urinary tract

Catheterization n Catheterization is the insertion of a polypropylene or rubber catheter into the bladder by way of the urethra This test can be used on male dogs for the assessment of urethral patentcy and upper urinary tract infection. This method often results in iatrogenic presence of red blood cells in the urine. Lubricate the catheter
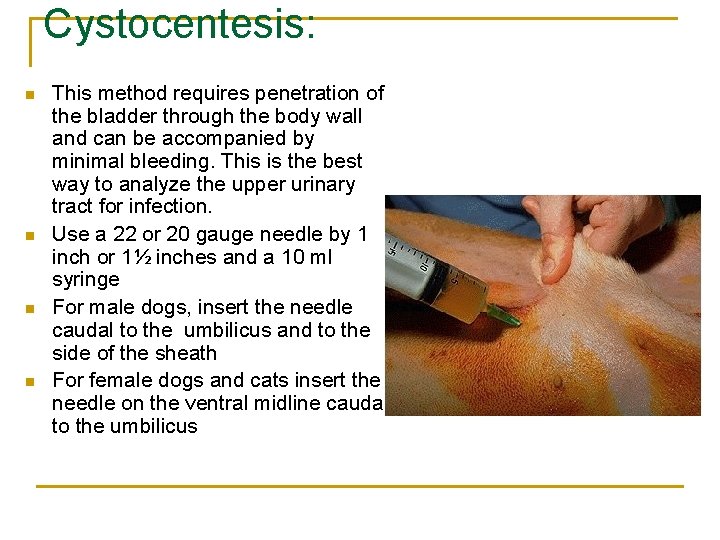
Cystocentesis: n n This method requires penetration of the bladder through the body wall and can be accompanied by minimal bleeding. This is the best way to analyze the upper urinary tract for infection. Use a 22 or 20 gauge needle by 1 inch or 1½ inches and a 10 ml syringe For male dogs, insert the needle caudal to the umbilicus and to the side of the sheath For female dogs and cats insert the needle on the ventral midline caudal to the umbilicus

Volume n n Normal 24 urine production for dogs and cats is 20 -40 ml/kg. An average sized saddle horse may produce between 5 and 15 L of urine in 24 hours. An increase in this volume is termed polyuria and may be due to physiological, pharmacological or pathological causes. Decreased urine volume is called oliguria, and occurs in dehydration, renal failure, or urinary blockages. No urine is called anuria, and is an emergency condition that may be due to renal failure, urinary blockage or ruptured bladder.

Color n n n Urine color will vary between species, but it is normally some shade of yellow depending on the concentration. Abnormal color changes in the urine could be due to drugs, increased urinary pigments or red blood cells. Red to reddish-brown could be due to either hematuria, hemoglobinuria, or myoglobinuria. Occasionally, unusual colors may be caused by dyes associated with food or drugs. urine sample exhibiting hematuria

Turbidity n n Urine is normally transparent in most animals, except for the horse. The horse has a thick viscous urine that is cloudy on examination. In small animals, turbidity suggests the presence of cells, casts, or crystals. Often refrigeration will propagate the sedimentation of crystals in the urine, producing a cloudy appearance. This is usually of no significance The sample on the left is exhibiting turbidity. The sample on the right is a normal color and clarity for canine urine

Odor n Urine has a characteristic smell that varies slightly by species and concentration of the sample. n A particularly foul odor may occur in the presence of bacteria. Thus, strong smelling urine is common in cases of cystitis. n Ketonuria produces a very sweet smell as does glucosuria. n Sweet smelling urine is commonly associated with diabetes mellitus.

Specific Gravity n n n Specific gravity measures the concentrating ability of the kidney tubules. It is the ratio of the weight of urine to the weight of an equal volume of water. Normal values range from 1. 001 -1. 060 in most of our domestic animals. If the kidneys are unable to concentrate urine the specific gravity will approach that of the glomerular filtrate, at 1. 010. A small drop of the urine sample is placed under the slide on the top of the scope, and the measurement is made by looking through the eye piece to read the value indicated.

The Chemical Analysis n n A chemical analysis of urine is performed using a commercial dip stick reagent strip. If the sample is turbid, the chemistry tests are done on the supernatant.

What is evaluated on chemical analysis? n n n Protein Glucose Ketones Blood Bilirubin Urinary p. H

p. H n Urine p. H will be affected by many things including the diet, handling of the sample, and acid-base balance of the animal. An alkaline p. H is most indicative of an infectious process. Normal p. H is between 6 and 8 for most animals depending on their diet.

Glucose n n In the normal animal there should not be glucose in the urine. If glucose is present, it is a classic response to hyperglycemia and should instigate an investigation into the possibility of diabetes in the patient.

Ketones n In the normal animal there will be no ketones in the urine. An animal that is undergoing fat metabolism or is deficient in carbohydrates will have ketones in the urine. Slight ketonuria should be expected in malnourished animals. A ketonuria also frequently accompanies diabetes mellitus.

Bilirubin n Bilirubinuria increased concentrations of bilirubin due to biliary obstruction, cholestasis, or increased bilirubin production secondary to hemolysis.

Blood n n There should not be any blood in the urine of a normal animal. Most test strips cannot differentiate between red blood cells, hemoglobin, or myoglobin, thus some care should be taken in interpretation. Hematuria is also evaluated in urine sedimentation microscopically and is reported as cells per high power field (or HPF). Remember that collection methods may also cause blood to appear in the urine. Other causes of hematuria include infection, neoplasia, or trauma.

Protein n Urine normally contains a small amount of protein, which is due to normal leakage and secretion from the urinary tract lining. This “normal” amount of protein will not show + on the dipstick. Proteinuria is an excess of serum proteins in the urine. This is an important factor of renal disease. Proteinuria can also be found in glomerulonephritis, congestive heart failure, and renal ischemia of all kinds.

Sediment n n n Urine sedimentation may contain cells, casts and crystals and is examined microscopically after centrifugation of a urine sample. A very small amount of all of the above sediments is normal. Concern begins when any of these components is significantly elevated. There are many different crystals, cell types, and casts that may be found in the urine of animals, and it varies from species to species.

Urinary Crystals

Crystals cont’d n p. H dependant n May indicate a urolith (bladder stone) n May lead to urethral obstruction
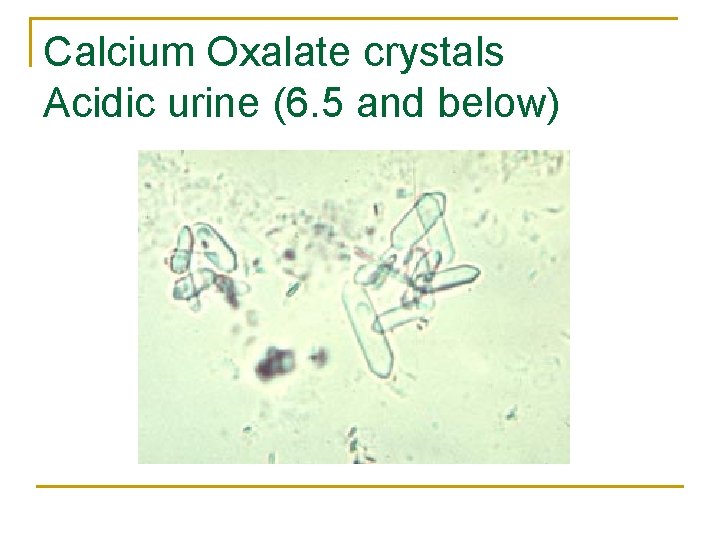
Calcium Oxalate crystals Acidic urine (6. 5 and below)

Calcium Oxalate crystals in a slightly different configuration

Struvite Crystals / Triple Phosphate Neutral to Acidic (7. 0 and above)
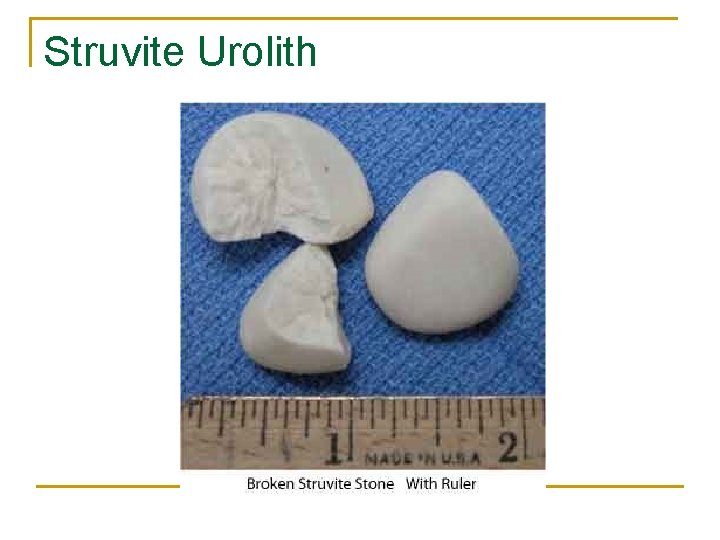
Struvite Urolith

Casts n Casts are elongated structures composed of protein from plasma and mucoprotein from the renal tubules. n In general, they form in the distal tubules, in which the urine is more concentrated and acidic. n Any structures that happen to be in the tubules at the time the casts form (RBCs, WBCs or epithelial cells), become embedded in the casts.

Casts n The presence of increased numbers of casts helps to localize the renal disease to the tubules, but the numbers to not necessarily correlate with the severity of the disease. n The five main types of casts are : Hyaline, Cellular, Granular, Waxy and Fatty
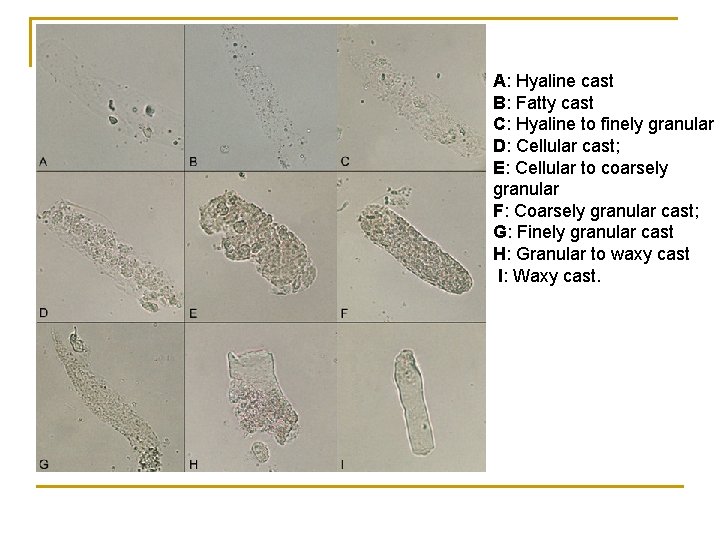
Cast Compilation The image below represents different casts seen in urine at the same magnification and lighting. Shown are hyaline, fatty, granular and waxy casts. Hyaline casts can be quite difficult to see in wet preparations of urine sediments with light microscopy, even with the condenser of the microscope racked down. They are much easier to visualize using phase contrast, however phase is usually not available on most microscopes. They become more visible with regular light microscopy if fat sticks to the protein matrix (Tamm-Horsfall mucoprotein) that makes up the hyaline cast (image B) or particulate material from degenerating cells is present within the cast matrix (image C). Cellular casts have distinct cells within the protein matrix - if the cells are of epithelial origin (i. e. , not WBCs or RBCs), they are called epithelial casts (images D and E). As cells within the protein cast matrix break down, the cast becomes coarsely (image E and F) then finely granular (image G). Waxy casts are the final stage of cast degeneration (usually originating from cellular and granular casts). Compared to hyaline casts, they are readily observable because they have a smooth appearance, no internal texture, and are more refractile than the surrounding urine. Legend: A: Hyaline cast; B: Fatty cast; C: Hyaline to finely granular cast; D: Cellular cast; E: Cellular to coarsely granular cast; F: Coarsely granular cast; G: Finely granular cast; H: Granular to waxy cast, I: Waxy cast. A: Hyaline cast B: Fatty cast C: Hyaline to finely granular D: Cellular cast; E: Cellular to coarsely granular F: Coarsely granular cast; G: Finely granular cast H: Granular to waxy cast I: Waxy cast.
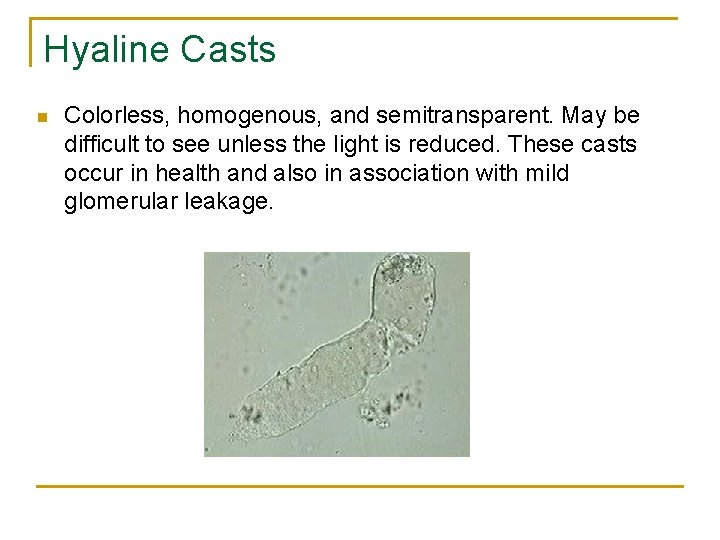
Hyaline Casts n Colorless, homogenous, and semitransparent. May be difficult to see unless the light is reduced. These casts occur in health and also in association with mild glomerular leakage.
Cellular Casts n n Contain recognizable cells embedded in the protein matrix. Cellular casts may be epithelial cell casts that contained sloughed tubular epithelial cells, RBC casts that indicate renal hemorrhage, or WBC casts that indicate renal inflammation of pyelonephritis.
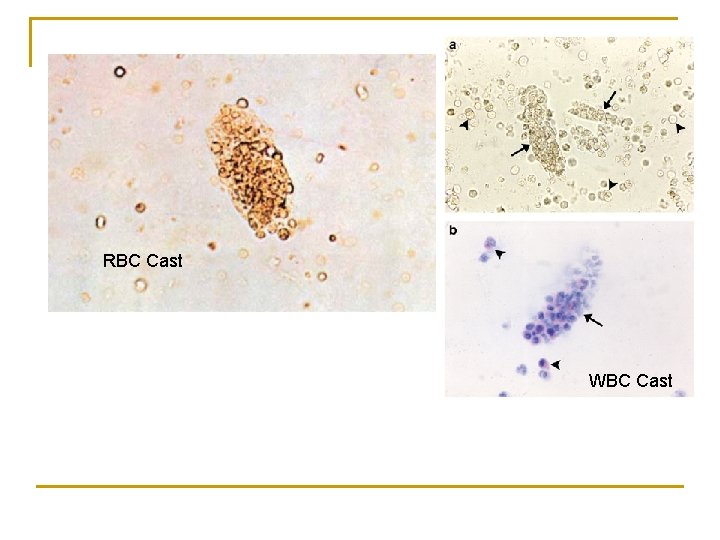
RBC Cast WBC Cast

Granular Casts n n n Casts derived from degenerating cells or cellular casts. Characterized by a nonspecific granular matrix and are designated as either coarsely or finely granular. This is the most common type of cast found in animals.
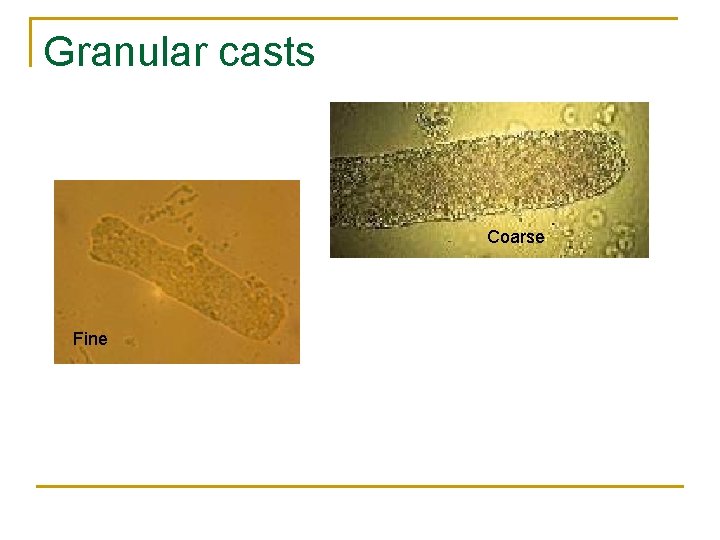
Granular casts Coarse Fine
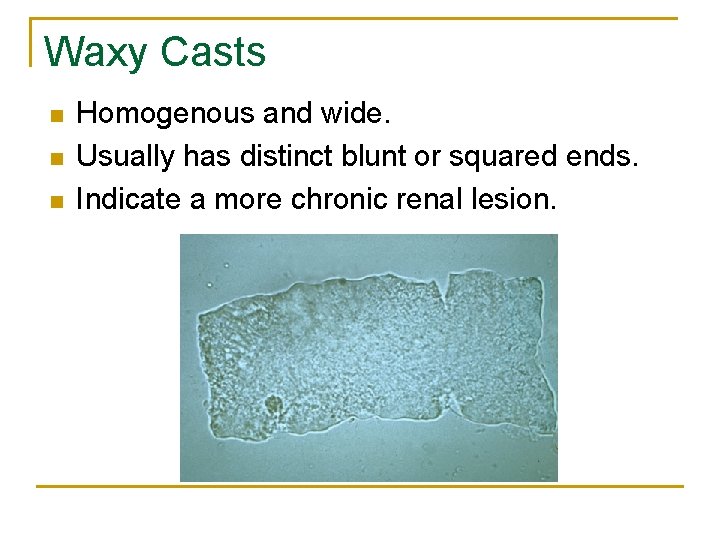
Waxy Casts n n n Homogenous and wide. Usually has distinct blunt or squared ends. Indicate a more chronic renal lesion.
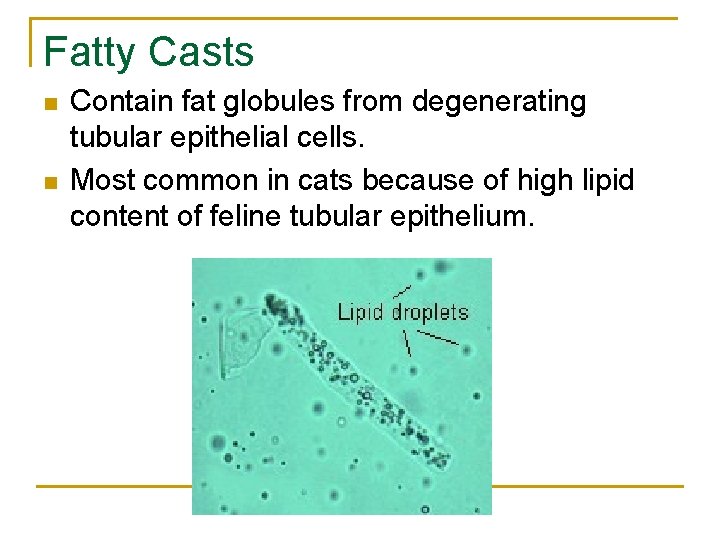
Fatty Casts n n Contain fat globules from degenerating tubular epithelial cells. Most common in cats because of high lipid content of feline tubular epithelium.

Bacteria / Microorganisms n Bacteria in a voided sample are usually not clinically significant = contamination from distal urinary tract. n Bacteria in a catheterized or cystocentesis sample = clinical significance. n Bacteria in a sample is most often correlated with the presence of WBC.
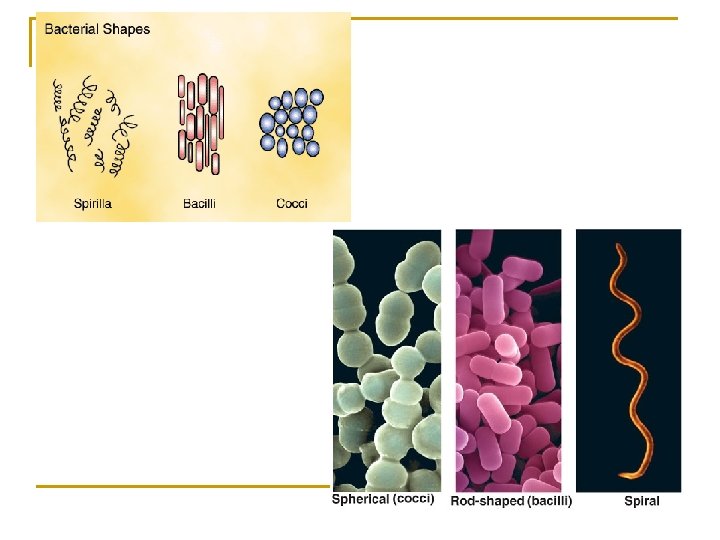
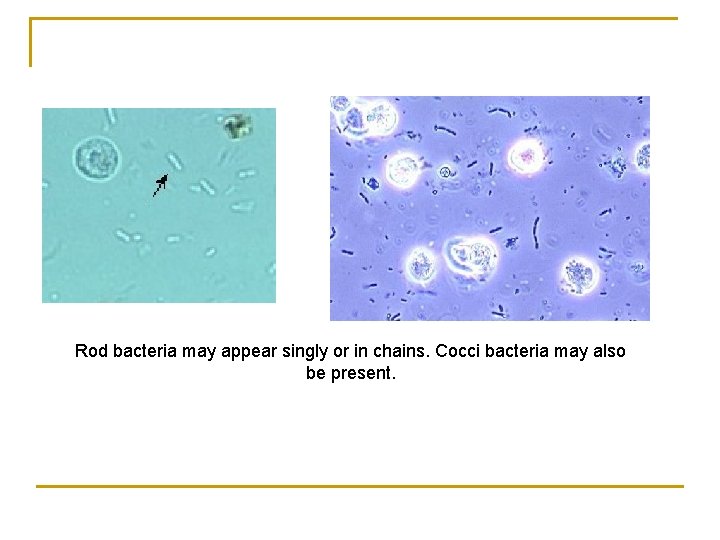
Rod bacteria may appear singly or in chains. Cocci bacteria may also be present.

Bacteria Video You. Tube - Bacteria In Urine

How to Microscopically Examine Urinary Sediment n A sample of well-mixed urine (usually 10 -15 ml) is centrifuged in a test tube at relatively low speed (about 2 -3, 000 rpm) for 5 -10 minutes. The supernatant is decanted and a volume of 0. 2 to 0. 5 ml is left inside the tube. The sediment is resuspended in the remaining supernatant by flicking the bottom of the tube several times. A drop of re-suspended sediment is poured onto a glass slide and coverslipped. Another drop is stained using urinary sediment stain.

n The sediment is first examined under low (10 X) power to identify most crystals, casts, squamous cells, and other large objects. The numbers of casts seen are usually reported as number of each type found per low power field (LPF). Since the number of elements found in each field may vary considerably from one field to another, several fields are averaged.

n Next, examination is carried out at high (40 X 100 X) power to identify crystals, cells, and bacteria. The various types of cells are usually described as the number of each type found per average high power field (HPF). Example: 1 -5 WBC/HPF.


RBCs Red Blood Cells n Red cells may also contaminate the urine from the vagina in menstruating dogs or from trauma produced by bladder catherization. Theoretically, no red cells should be found, but some find their way into the urine even in very healthy animals. However, if one or more red cells can be found in every high power field, and if contamination can be ruled out, the specimen is probably abnormal. n

n RBC's may appear normally shaped, swollen by dilute urine (in fact, only cell ghosts and free hemoglobin may remain), or crenated by concentrated urine. Both swollen, partly hemolyzed RBC's and crenated RBC's are sometimes difficult to distinguish from WBC's in the urine. In addition, red cell ghosts may simulate yeast.
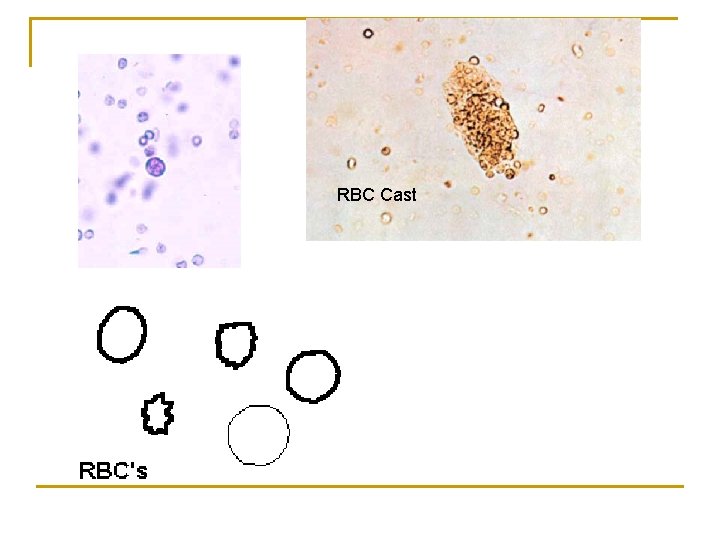
RBC Cast

White Blood Cells n Pyuria refers to the presence of abnormal numbers of leukocytes that may appear with infection in either the upper or lower urinary tract or with acute glomerulonephritis. Usually, the WBC's are granulocytes. n If two or more leukocytes per each high power field appear in non-contaminated urine, the specimen is probably abnormal. Leukocytes have lobed nuclei and granular cytoplasm.
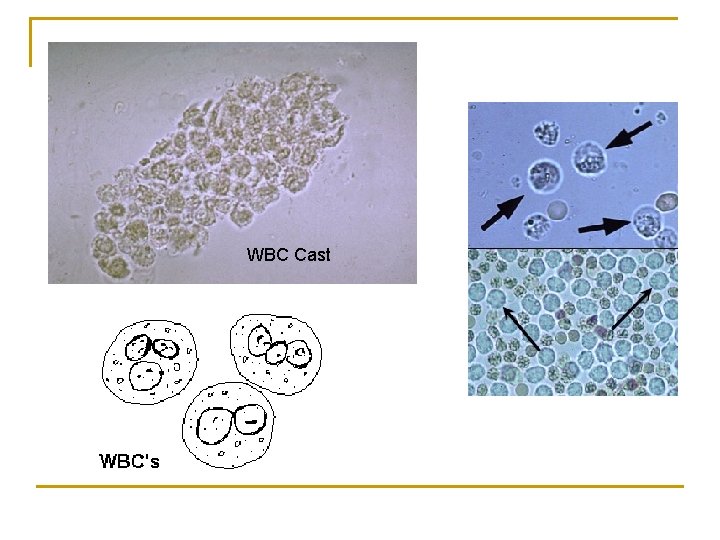
WBC Cast
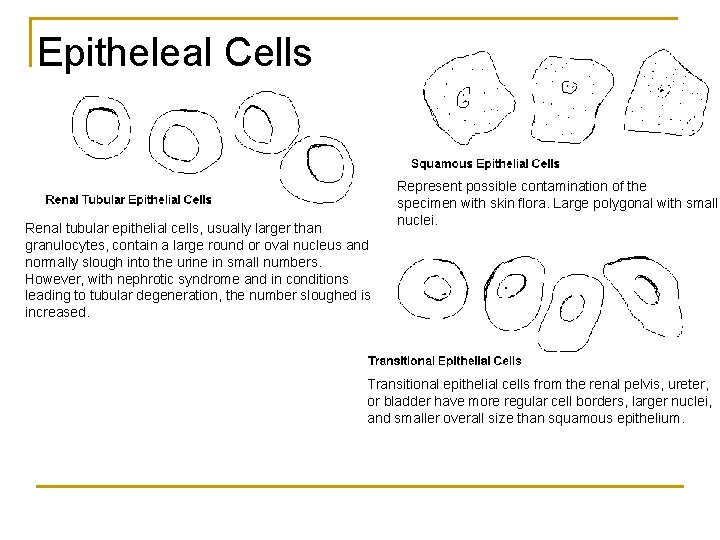
Epitheleal Cells Renal tubular epithelial cells, usually larger than granulocytes, contain a large round or oval nucleus and normally slough into the urine in small numbers. However, with nephrotic syndrome and in conditions leading to tubular degeneration, the number sloughed is increased. Represent possible contamination of the specimen with skin flora. Large polygonal with small nuclei. Transitional epithelial cells from the renal pelvis, ureter, or bladder have more regular cell borders, larger nuclei, and smaller overall size than squamous epithelium.
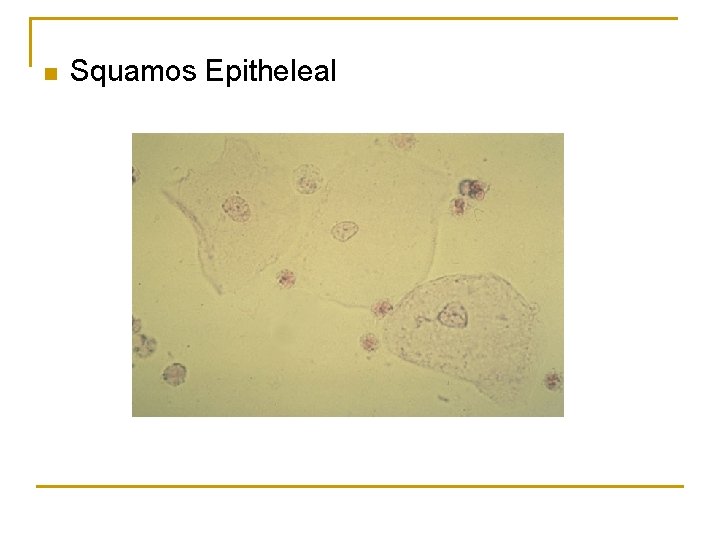
n Squamos Epitheleal
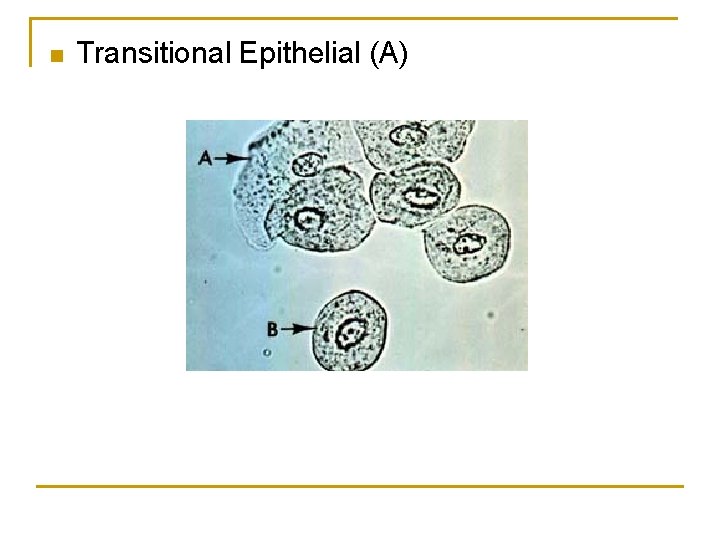
n Transitional Epithelial (A)
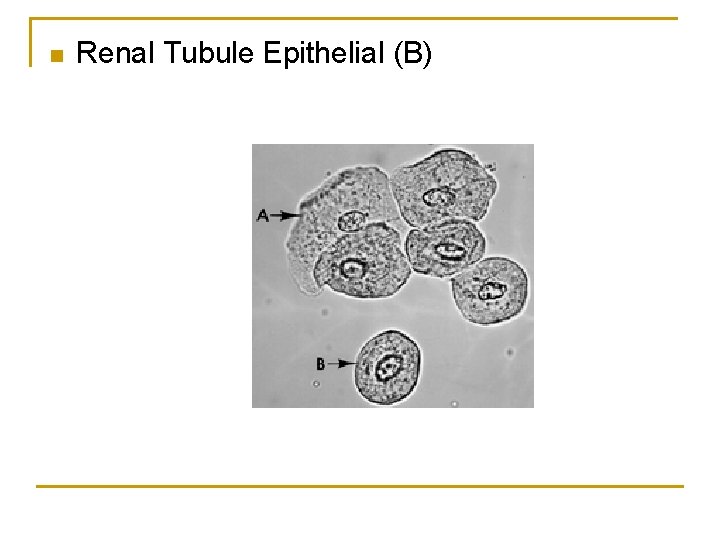
n Renal Tubule Epithelial (B)
- Slides: 56