The optimal choice of gonadotrophin in Gn RH























- Slides: 37

The optimal choice of gonadotrophin in Gn. RH antagonist protocols Prof Dr P Devroey

Recent trends in ART practice • Increasing use of Gn. RH antagonists with lower doses of gonadotrophin • Increasing use of ICSI over the last decade • Increasing use of single embryo transfer • Increasing use of embryo culture to blastocyst stage • Increasing use of vitrification instead of slow-freezing

Why the MEGASET trial? • MEGASET compares HP-h. MG (MENOPUR®) with r. FSH (PUREGON®) in a setting that addresses these recent trends in ART practice • Randomised, assessor-blind, parallel groups, multicentre trial to demonstrate non-inferiority of HPh. MG compared to r. FSH with respect to ongoing pregnancy rates

Participating clinics 25 clinics in 7 countries

Key design features • • • Women 18– 34 years BMI 18– 24. 9 kg/m 2 Gn. RH antagonist No programming 150 IU starting dose ICSI Blastocyst culture Single blastocyst transfer on Day 5 2 weeks luteal support Vitrification Replacement of a single warmed blastocyst in a natural cycle

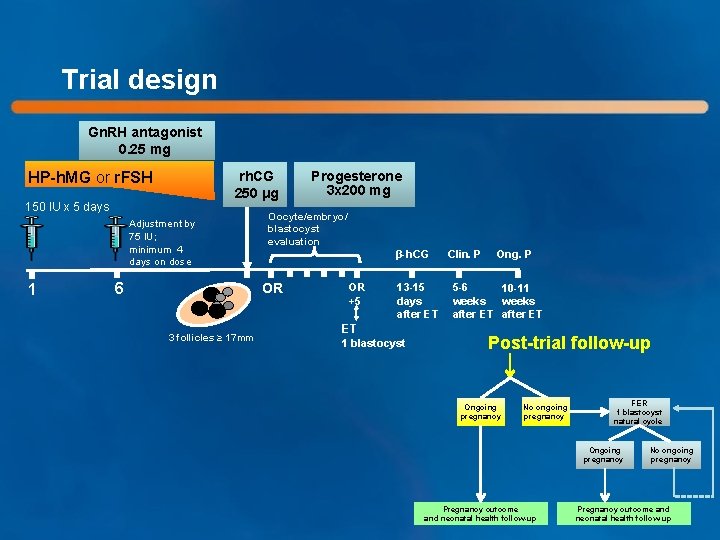
Trial design Gn. RH antagonist 0. 25 mg HP-h. MG or r. FSH rh. CG 250 μg 150 IU x 5 days Adjustment by 75 IU; minimum 4 days on dose 1 6 Oocyte/embryo/ blastocyst evaluation β-h. CG OR 3 follicles ≥ 17 mm Progesterone 3 x 200 mg OR +5 13 -15 days after ET ET 1 blastocyst Clin. P Ong. P 5 -6 10 -11 weeks after ET Post-trial follow-up Ongoing pregnancy No ongoing pregnancy FER 1 blastocyst natural cycle Ongoing pregnancy Pregnancy outcome and neonatal health follow-up No ongoing pregnancy Pregnancy outcome and neonatal health follow-up

Investigations: All patients • Endocrine profile • Follicular development • Ovarian response • Endometrial profile • Pregnancy rates • Cumulus mass appearance • Oocyte maturation, fertilisation • Embryo quality • Blastocyst quality

Additional investigations: Subgroups of patients • Early-mid follicular phase endocrine profile • Intrafollicular endocrine profile • Uterine contractility • Modelling of follicles • Modelling of endometrium • Gene expression in cumulus cells (mechanical dissection and enzymatic denudation)

METHODOLOGY

Primary endpoint of the study • Ongoing pregnancy rates beyond 10– 11 weeks after ET in a fresh cycle

Power calculation • Estimated ongoing pregnancy rate of 30% was derived from previous studies on single blastocyst transfer • Non-inferiority margin was set at – 10% (absolute) • At least 660 cycles was required to achieve a study power of 80%

Analysis of data • Modified Intention-to-treat (ITT) analysis – All subjects who have been randomised and exposed to at least one dose of investigational medicinal product were analysed according to the actual treatment • Per protocol analysis – All subjects from the modified ITT, except those who are excluded because of a major protocol deviation were analysed

EMBRYO ASSESSMENT

Embryo morphology assessment and grading • Local embryologists only; no central evaluation • Interobserver agreement and intraobserver reproducibility were validated in the MERi. T trial showing good–excellent agreement on overall embryo morphology assessment and grading 1 • Embryos were graded according to the Gardner and Schoolcraft classification system 2 1. Arce et al. Hum Reprod 2006; 21: 2141– 2148 2. Gardner and Schoolcraft. In: Towards reproductive certainty (Eds Jansen & Mortimer). The plenary proceedings of the 11 th world congress on in vitro fertilization and human reproductive genetics. The Parthenon Publishing Group. 1999. Pp 378– 388

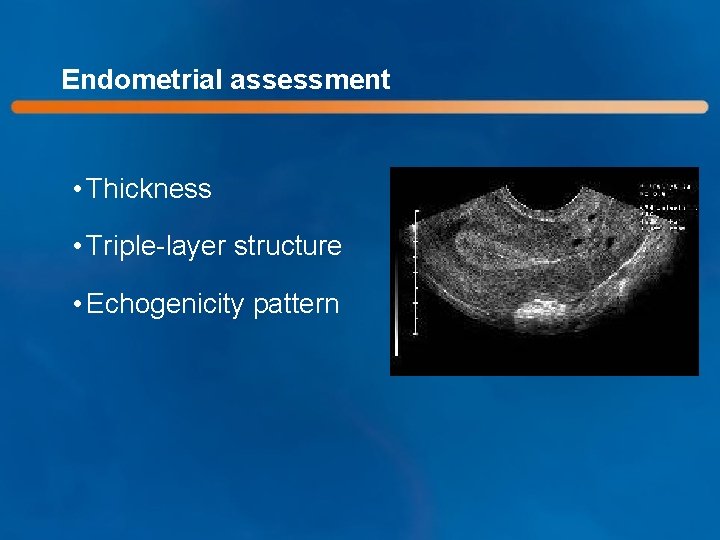
Endometrial assessment • Thickness • Triple-layer structure • Echogenicity pattern

SUBJECT DISPOSITION

Consort diagram Screened (N=810) Randomised and exposed (n=749) HP-h. MG (ITT; N=374) r. FSH (ITT; N=375) Oocyte retrieval N=362 Embryo transfer N=305 Embryo transfer N=316 β-h. CG visit N=305 β-h. CG visit N=316 Ongoing pregnancy visit N=107

BASELINE PARAMETERS

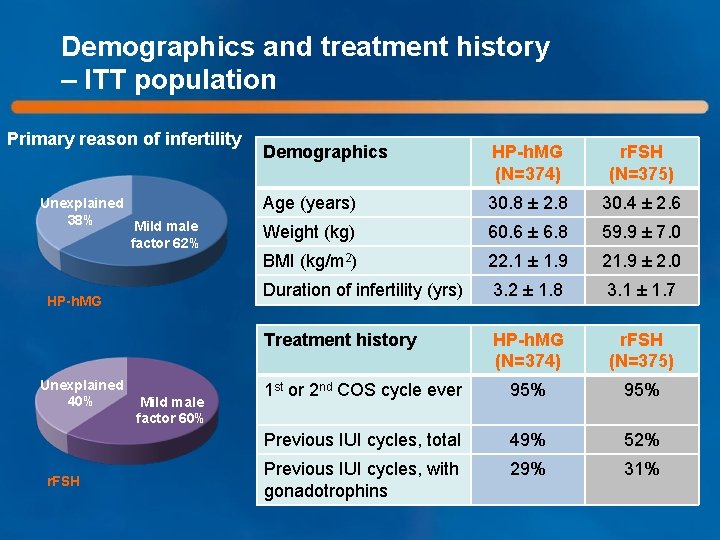
Demographics and treatment history – ITT population Primary reason of infertility Unexplained 38% Mild male factor 62% HP-h. MG Unexplained 40% r. FSH Mild male factor 60% Demographics HP-h. MG (N=374) r. FSH (N=375) Age (years) 30. 8 ± 2. 8 30. 4 ± 2. 6 Weight (kg) 60. 6 ± 6. 8 59. 9 ± 7. 0 BMI (kg/m 2) 22. 1 ± 1. 9 21. 9 ± 2. 0 Duration of infertility (yrs) 3. 2 ± 1. 8 3. 1 ± 1. 7 Treatment history HP-h. MG (N=374) r. FSH (N=375) 1 st or 2 nd COS cycle ever 95% Previous IUI cycles, total 49% 52% Previous IUI cycles, with gonadotrophins 29% 31%

ENDOCRINE PROFILE

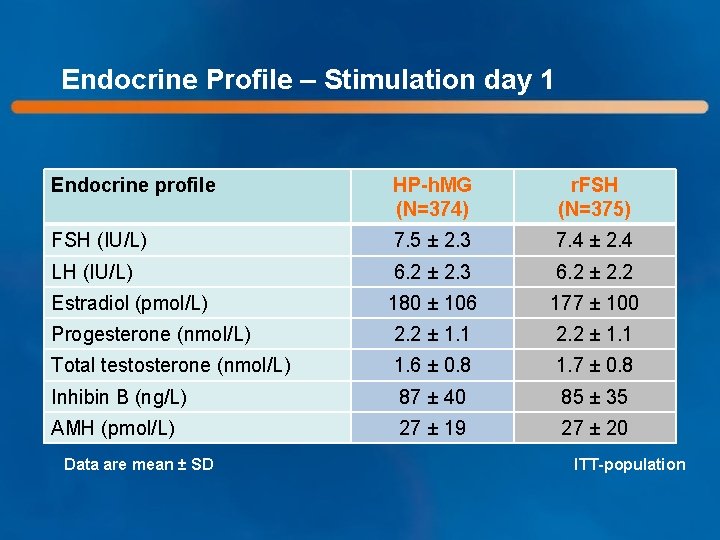
Endocrine Profile – Stimulation day 1 Endocrine profile HP-h. MG (N=374) r. FSH (N=375) FSH (IU/L) 7. 5 ± 2. 3 7. 4 ± 2. 4 LH (IU/L) 6. 2 ± 2. 3 6. 2 ± 2. 2 Estradiol (pmol/L) 180 ± 106 177 ± 100 Progesterone (nmol/L) 2. 2 ± 1. 1 Total testosterone (nmol/L) 1. 6 ± 0. 8 1. 7 ± 0. 8 Inhibin B (ng/L) 87 ± 40 85 ± 35 AMH (pmol/L) 27 ± 19 27 ± 20 Data are mean ± SD ITT-population

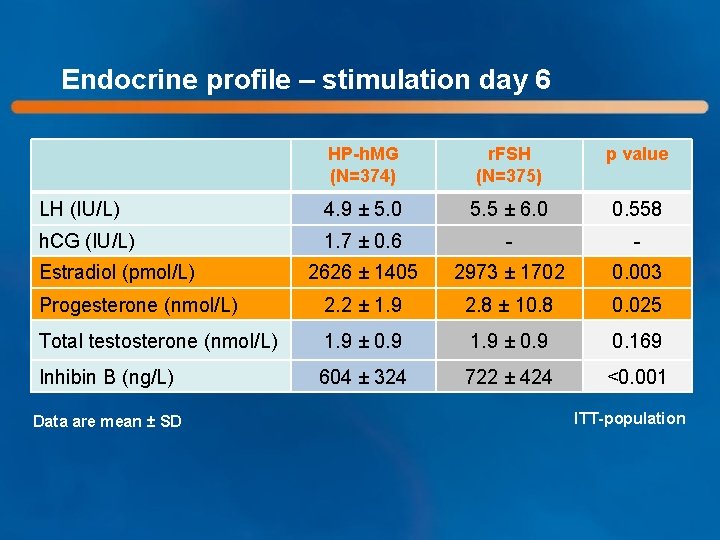
Endocrine profile – stimulation day 6 HP-h. MG (N=374) r. FSH (N=375) p value LH (IU/L) 4. 9 ± 5. 0 5. 5 ± 6. 0 0. 558 h. CG (IU/L) 1. 7 ± 0. 6 - - 2626 ± 1405 2973 ± 1702 0. 003 Progesterone (nmol/L) 2. 2 ± 1. 9 2. 8 ± 10. 8 0. 025 Total testosterone (nmol/L) 1. 9 ± 0. 9 0. 169 Inhibin B (ng/L) 604 ± 324 722 ± 424 <0. 001 Estradiol (pmol/L) Data are mean ± SD ITT-population

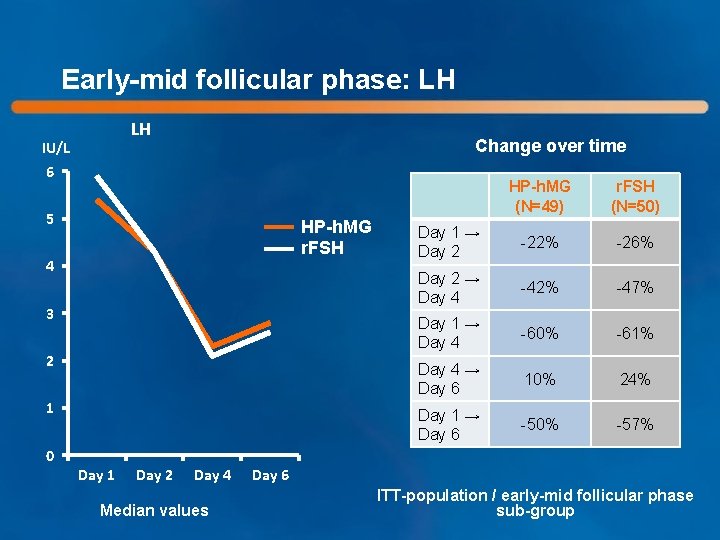
Early-mid follicular phase: LH LH IU/L Change over time 6 5 HP-h. MG r. FSH 4 3 2 1 HP-h. MG (N=49) r. FSH (N=50) Day 1 → Day 2 -22% -26% Day 2 → Day 4 -42% -47% Day 1 → Day 4 -60% -61% Day 4 → Day 6 10% 24% Day 1 → Day 6 -50% -57% 0 Day 1 Day 2 Day 4 Median values Day 6 ITT-population / early-mid follicular phase sub-group

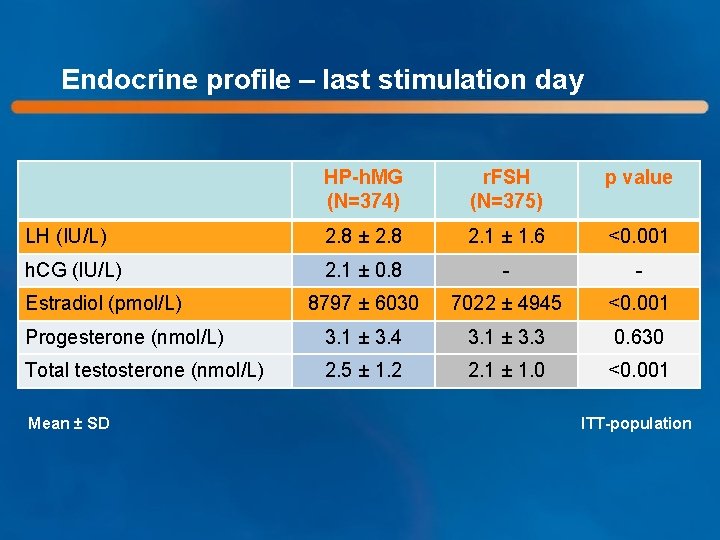
Endocrine profile – last stimulation day HP-h. MG (N=374) r. FSH (N=375) p value LH (IU/L) 2. 8 ± 2. 8 2. 1 ± 1. 6 <0. 001 h. CG (IU/L) 2. 1 ± 0. 8 - - 8797 ± 6030 7022 ± 4945 <0. 001 Progesterone (nmol/L) 3. 1 ± 3. 4 3. 1 ± 3. 3 0. 630 Total testosterone (nmol/L) 2. 5 ± 1. 2 2. 1 ± 1. 0 <0. 001 Estradiol (pmol/L) Mean ± SD ITT-population

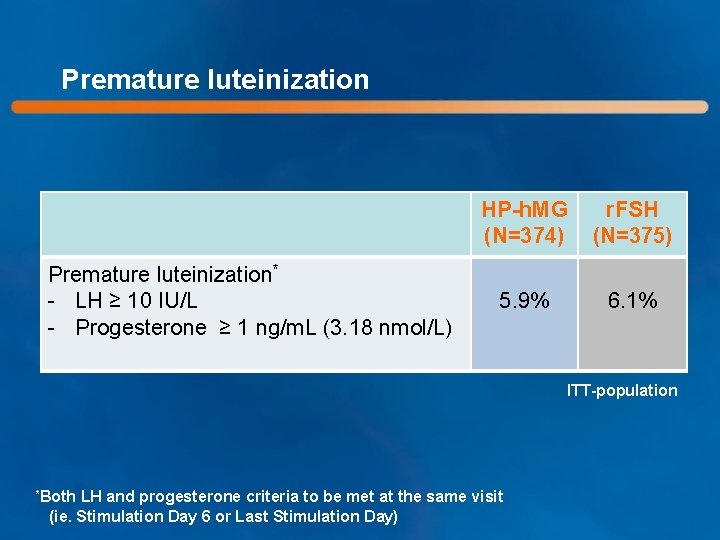
Premature luteinization* - LH ≥ 10 IU/L - Progesterone ≥ 1 ng/m. L (3. 18 nmol/L) HP-h. MG (N=374) r. FSH (N=375) 5. 9% 6. 1% ITT-population *Both LH and progesterone criteria to be met at the same visit (ie. Stimulation Day 6 or Last Stimulation Day)

TREATMENT EFFICIENCY

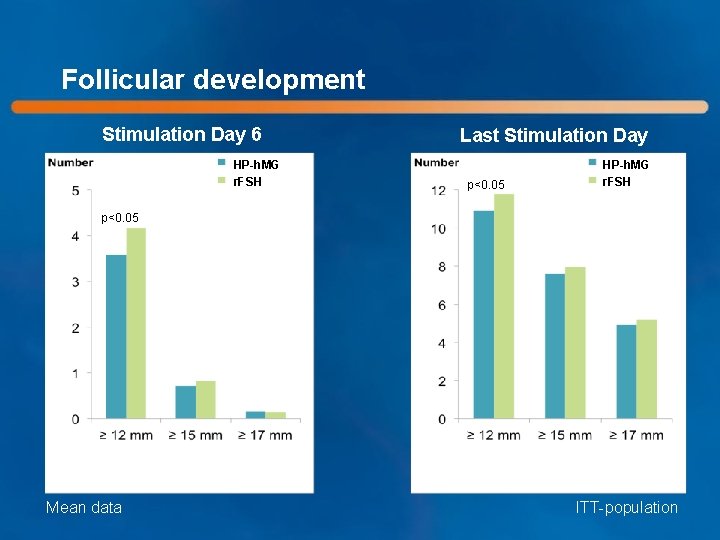
Follicular development Stimulation Day 6 HP-h. MG r. FSH Last Stimulation Day p<0. 05 HP-h. MG r. FSH p<0. 05 Mean data ITT-population

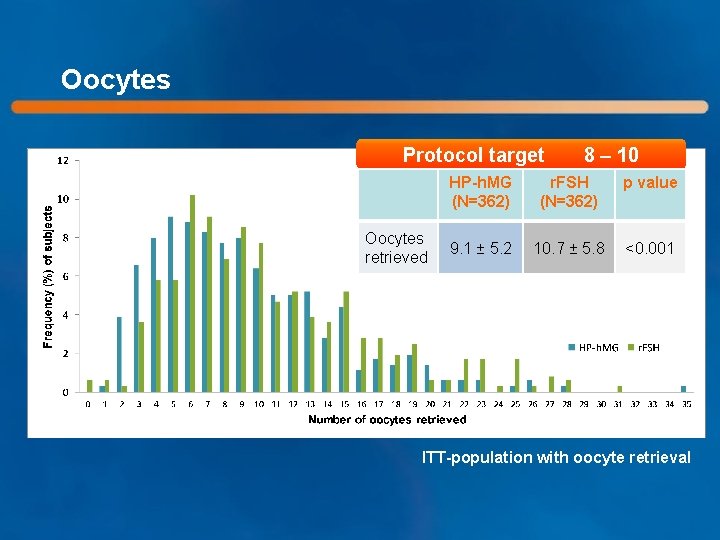
Oocytes Protocol target Oocytes retrieved 8 – 10 HP-h. MG (N=362) r. FSH (N=362) p value 9. 1 ± 5. 2 10. 7 ± 5. 8 <0. 001 ITT-population with oocyte retrieval

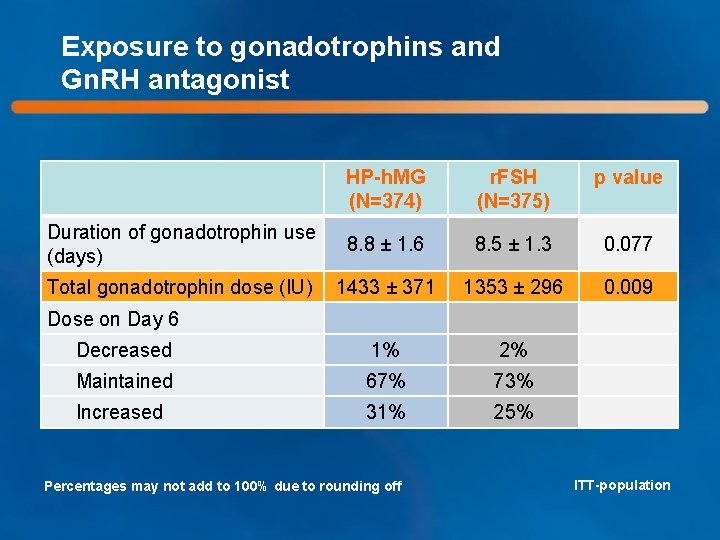
Exposure to gonadotrophins and Gn. RH antagonist HP-h. MG (N=374) r. FSH (N=375) p value Duration of gonadotrophin use (days) 8. 8 ± 1. 6 8. 5 ± 1. 3 0. 077 Total gonadotrophin dose (IU) 1433 ± 371 1353 ± 296 0. 009 Decreased 1% 2% Maintained 67% 73% Increased 31% 25% Dose on Day 6 Percentages may not add to 100% due to rounding off ITT-population

Endometrial pattern – Day of embryo transfer HP-h. MG (N=374) r. FSH (N=375) p value 11. 1 ± 2. 1 11. 1 ± 2. 2 - 53% 54% 0. 873 Hypoechogenic 5% 6% Isoechogenic 17% Hyperechogenic 73% Not possible to evaluate 5% 4% Endometrial thickness (mm) Triple-layer structure Echogenic pattern 0. 983 ITT-population

Availability of blastocysts on the day of ET ITT-population HP-h. MG r. FSH Subjects with blastocysts 82% 85% Subjects with frozen blastocysts 55% 58%

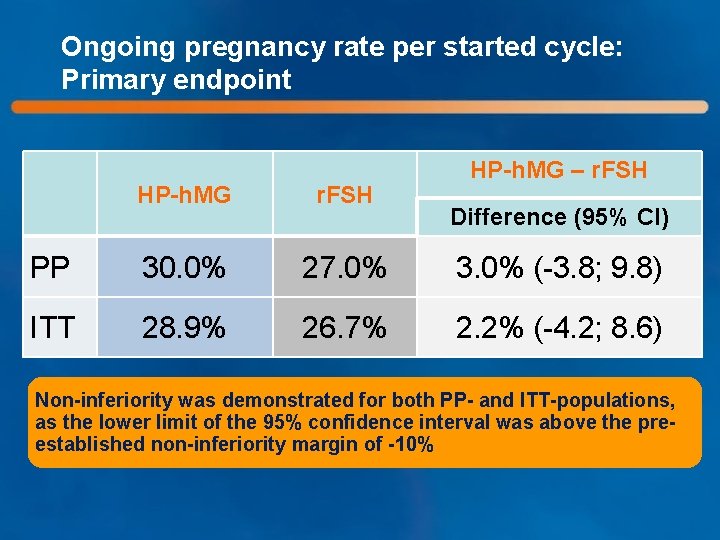
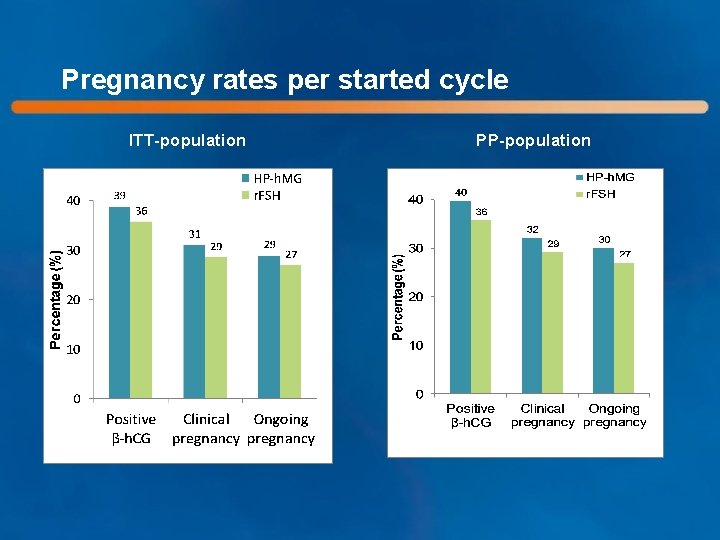
Ongoing pregnancy rate per started cycle: Primary endpoint HP-h. MG – r. FSH HP-h. MG r. FSH PP 30. 0% 27. 0% 3. 0% (-3. 8; 9. 8) ITT 28. 9% 26. 7% 2. 2% (-4. 2; 8. 6) Difference (95% CI) Non-inferiority was demonstrated for both PP- and ITT-populations, as the lower limit of the 95% confidence interval was above the preestablished non-inferiority margin of -10%

Pregnancy rates per started cycle ITT-population PP-population

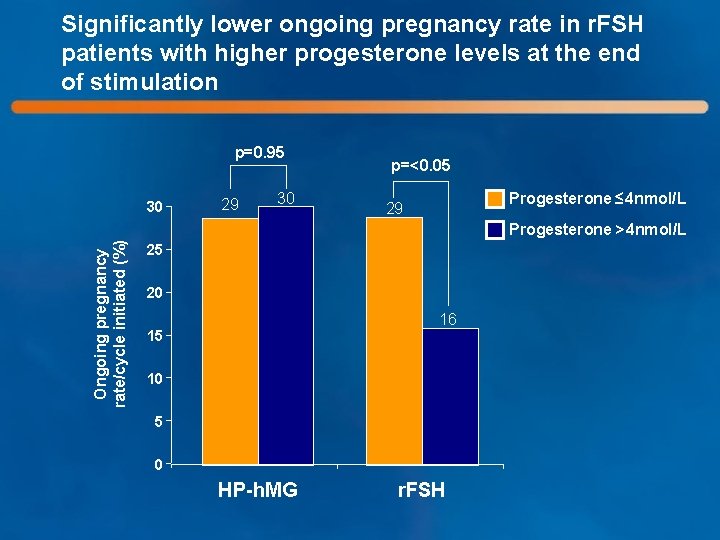
Significantly lower ongoing pregnancy rate in r. FSH patients with higher progesterone levels at the end of stimulation p=0. 95 30 29 30 p=<0. 05 Progesterone ≤ 4 nmol/L 29 Ongoing pregnancy rate/cycle initiated (%) Progesterone >4 nmol/L 25 20 16 15 10 5 0 HP-h. MG r. FSH

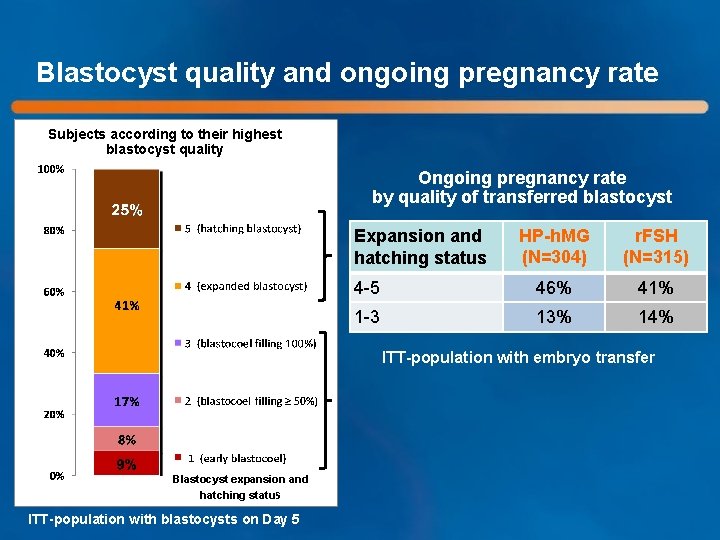
Blastocyst quality and ongoing pregnancy rate Subjects according to their highest blastocyst quality Ongoing pregnancy rate by quality of transferred blastocyst HP-h. MG (N=304) r. FSH (N=315) 4 -5 46% 41% 1 -3 13% 14% Expansion and hatching status ITT-population with embryo transfer Blastocyst expansion and hatching status ITT-population with blastocysts on Day 5

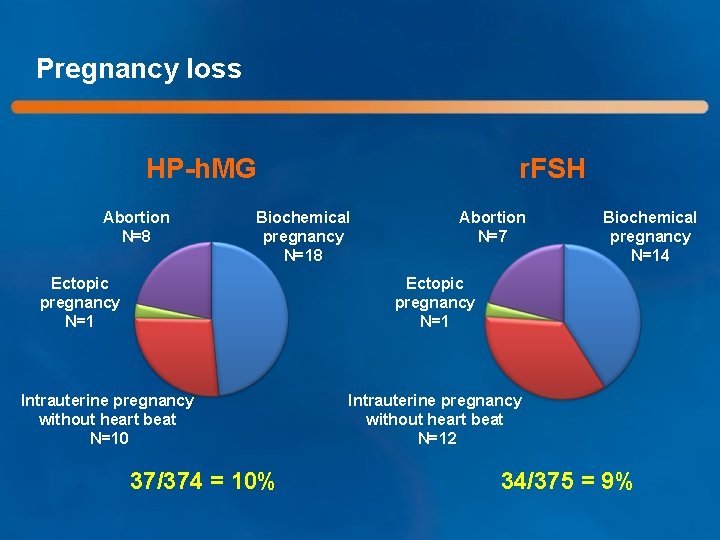
Pregnancy loss HP-h. MG Abortion N=8 r. FSH Biochemical pregnancy N=18 Ectopic pregnancy N=1 Abortion N=7 Biochemical pregnancy N=14 Ectopic pregnancy N=1 Intrauterine pregnancy without heart beat N=10 37/374 = 10% Intrauterine pregnancy without heart beat N=12 34/375 = 9%

Conclusions • Primary endpoint of MEGASET study was achieved • Largest multicentre, multinational RCT of HP-h. MG vs r. FSH addressing new trends in ART in a robust, high quality innovative trial with ICSI • Demonstrates single blastocyst transfer is effective with mild stimulation and lower number of oocytes • Reinforces the importance of progesterone during the late follicular phase – Higher pregnancy rate with HP-h. MG than r. FSH when progesterone >4 nmol/L