Cardiovascular Emergencies and 12 Lead EKGs Condell Medical






























































































- Slides: 138

Cardiovascular Emergencies and 12 Lead EKG’s Condell Medical Center EMS System ECRN Packet Module III 2007 Prepared by: Sharon Hopkins, RN, BSN, EMT-P

Objectives Upon successful completion of this program, the ECRN should be able to: – understand the normal anatomy & physiology of the cardiovascular system – describe anatomical changes to the heart during ischemic episodes – differentiate presentations of patients with cardiorespiratory complaints

–recognize ST elevation on the 12 lead EKG – identify and appropriately state interventions for a variety of dysrhythmias – review discussion of case presentations – successfully complete the quiz with a score of 80% or better

Cardiovascular System u This system is composed of the heart and blood vessels Delivers oxygenated blood to all cells Transports hormones throughout the body Transports waste products for waste disposal u The heart is a pump – right pump is under low pressure – left pump is under high pressure

3 Components of The Circulatory System À Functioning heart Á Sufficient blood volume Intact blood vessels If any one of the above 3 are not working properly, the patient may be symptomatic and could be in need of intervention

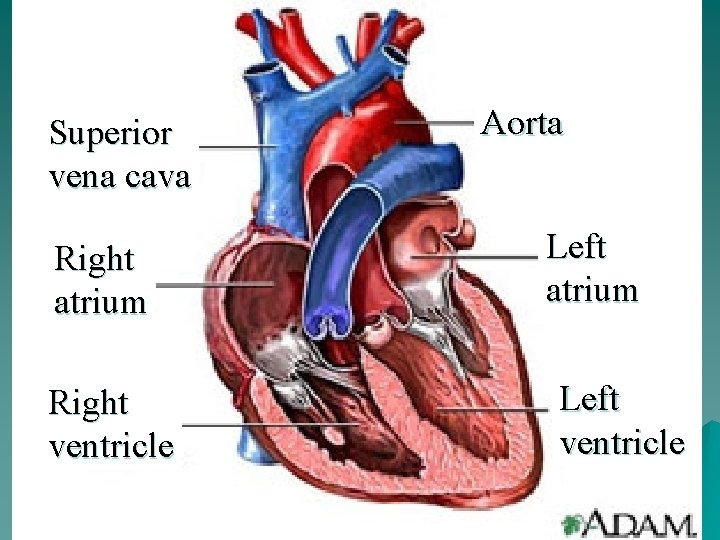
Superior vena cava Right atrium Right ventricle Aorta Left atrium Left ventricle

Myocardial Blood Flow u The heart is a muscle (myocardium) u 3 layers epicardium - smooth outer surface myocardium - thick middle layer, responsible for cardiac contraction activity endocardium - innermost layer of thin connective tissue u Myocardial blood flow – via coronary arteries immediately off aorta – heart is the 1 st structure to receive oxygenated blood - it’s that important!

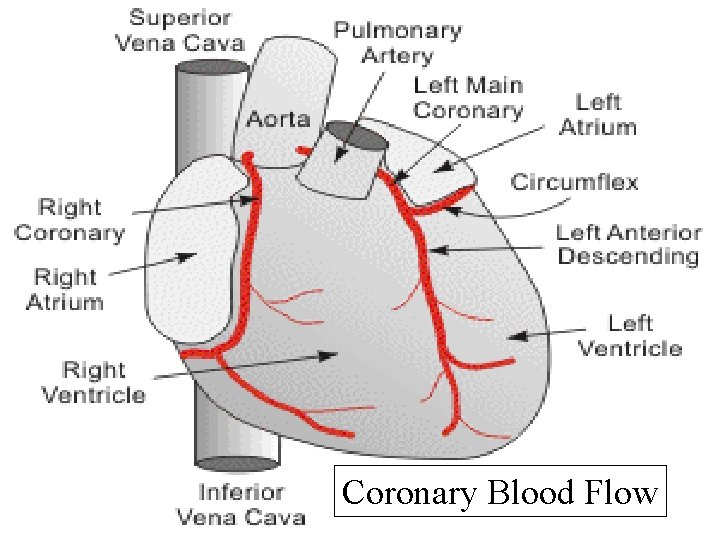
Coronary Arteries ªLeft main coronary artery –left anterior descending coronary artery (LAD) supplies left ventricle, septum –circumflex coronary artery supplies left atrium, left ventricle, septum, part of right ventricle ªRight coronary artery (RCA) supplies right atrium & ventricle

Coronary Blood Flow

Collateral Circulation u Development of new blood vessels to reroute blood flow around blockage in a coronary artery u New arteries may not be able to supply enough oxygenated blood to heart muscle in time of increased demand u Ischemia occurs when blood supply to the heart is inadequate to meet the demands

Influences of Heart Function u Preload – pressure under which a ventricle fills; volume of blood returning to fill the heart u Afterload – the resistance the ventricle has to pump against to eject blood out of the heart – the higher the afterload the harder the ventricle has to work u Ejection fraction (EF) – percentage of blood pumped by the ventricle with each contraction (healthy >55%) – damage to heart muscle decreases EF

Influences On Preload & Afterload Preload Afterload u increased oxygen u arteriosclerosis demand increases induced high B/P volume of blood can cause left returning to heart ventricle to become exhausted & stop u temporarily not a working efficiently problem u heart enlarges when preload remains increased (Frank. Starling law)

Problems That Decrease Ejection Fraction (EF) u Myocardial infarction (MI) u Congestive heart failure (CHF) u Coronary artery disease (CAD) u Atrial fibrillation u Cardiomyopathy u Anemia u Excess body weight u Poorly controlled blood pressure

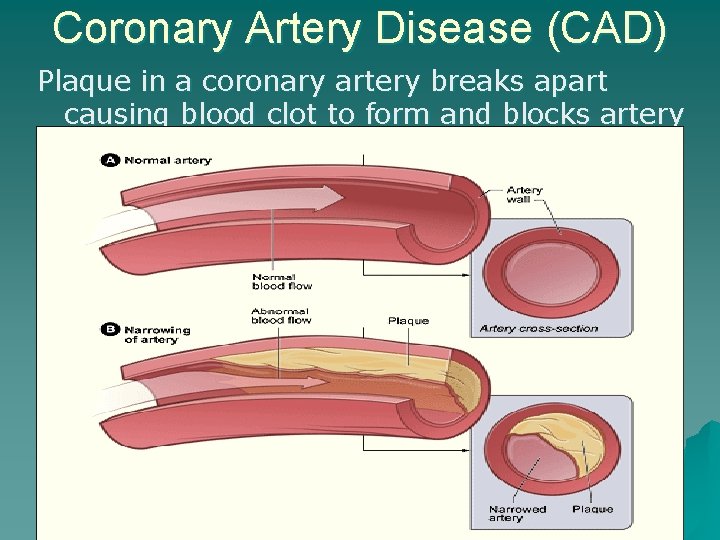
Coronary Artery Disease (CAD) u Leading cause of death in USA – Narrowing or blockage in coronary artery decreasing blood flow – Atherosclerosis - thickening & hardening of the arteries due to fatty deposits in vessels – Plaque deposits build up in arteries uarteries narrow uarteries become blocked ublood clots form u Overtime, CAD can contribute to heart failure & dysrhythmias

Coronary Artery Disease (CAD) Plaque in a coronary artery breaks apart causing blood clot to form and blocks artery

Symptoms of Cardiovascular Problems u Breathing problems – Shortness of breath (SOB) – Paroxysmal nocturnal dyspnea (PND) usuddenly awakens with shortness of breath – Orthopnea udyspnea when lying down – Breath sounds uare they clear or not clear?

u Peripheral edema – excess fluid found in tissues of the most dependent part of the body upresacral area in bedridden person ufeet and ankles in someone up and about u Syncope – fainting when cardiac output falls – fainting while lying down is considered cardiac in nature until proven otherwise u Palpitations – sensation of fast or irregular heartbeat u Pain

Initial Impression u Not necessarily important to know exactly what to “name” the patient’s problem (diagnosis) u Important to identify signs and symptoms that need to be treated – think “what’s the worse case scenario? ” u Important to recognize the possible medical condition the signs and symptoms may be representing u Important to determine the right treatment approach

Patient Assessment: OPQRST of Pain Symptoms u Onset – Sudden or gradual? – Anything like this before? u Provocation or palliation – What makes it better/worse? – What was the patient doing at the time? u Quality – What does it feel like (in patient’s own words)?

u Radiation – From where to where? u Severity – How bad is it on a scale of 0 -10? u Timing – When did it start – How long did it last? – Continuous or intermittent?

Vital Signs: Tools for Pt Assessment u Heart rate – too fast uventricle does not stay open long enough to adequately fill – too slow urate too slow to pump often enough to maintain an adequate volume output u Blood pressure – could be elevated in anxiety and pain – low in shock – serial readings (trending) tell much

u Respirations – Abnormally fast, slow, labored, noisy? Clear - hear breath sounds enter & exit unormal Crackles - pop, snap, click, crackle ufluid in lower airways Rhonchi - rattling sounds; resembles snoring umucus in the airways Wheezes - whistling sound; initially heard on exhalation unarrowing airways (ie: asthma) ¨Absence of sound - not good!!!

u Pulse oximetry (Sa. O 2) – Measures percent of saturated hemoglobin in arterial blood – <95% indicates respiratory compromise – <90% indicates dire problem – Need to evaluate reading with patient’s clinical presentation do they match?

Inaccurate Sa. O 2 Readings Hypotensive or cold patient (falsely low) Carbon monoxide poisoning (falsely high) Abnormal hemoglobin (sickle-cell disease) (falsely low) Incorrect probe placement (falsely low) Dark nail polish (falsely low) Anemia (falsely high - whatever hemoglobin patient has is saturated)

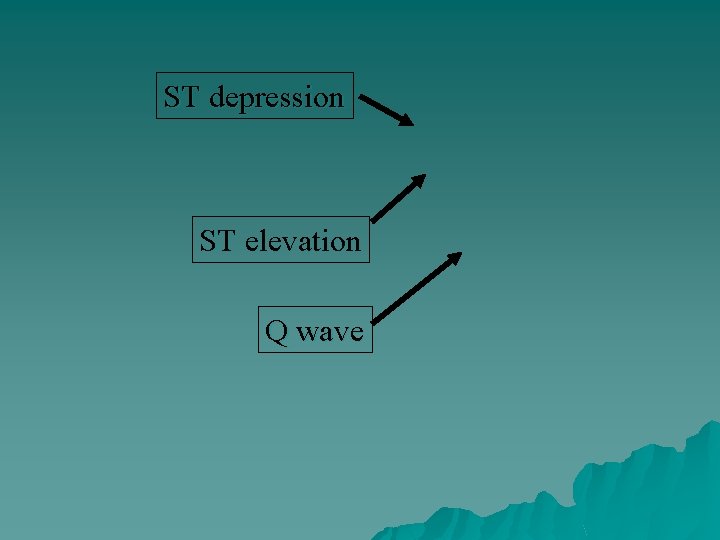
u EKG monitoring – Indicates electrical activity of the heart – Evaluate mechanical activity by measuring pulse, heart rate and blood pressure – Can indicate myocardial insult and location K ischemia - initial insult; ST depression L injury - prolonged myocardial hypoxia or ischemia; ST elevation; injury reversible L infarction - tissue death –dead tissue no longer contracts –amount of dead tissue directly relates to degree of muscle impairment –may show Q waves

ST depression ST elevation Q wave

Acute Coronary Syndrome Variety of events that represent acute myocardial ischemic pain (plaque rupture) ¬Unstable angina u. Intermediate severity of disease between stable angina and acute MI; tissue ischemia Non-Q wave infarct (NSTEMI) u. No ST elevation but MI is present with tissue necrosis (death) ®Q wave infarct (STEMI) u. ST elevation MI with tissue necrosis (death) u. Usually a large/significant infarct

Acute Myocardial Infarction u Coronary blood flow deprived so that portion of muscle dies – occlusion by a thrombus (blood clot superimposed on ruptured plaque) – spasm of coronary artery – reduction in blood flow (shock, arrhythmias, pulmonary embolism) u Location and size of infarct depends on which coronary artery is blocked & where – left ventricle most common

AMI Signs & Symptoms u Chest pain - most common especially in men – lasts >15 minutes – does not go away with rest – typically felt beneath sternum – typically described as heavy, squeezing, crushing, tight – can radiate down the arm (usually left), fingers, jaw, upper back, epigastrium u Pain not influenced by coughing, deep breathing, movement

Atypical AMI Signs & Symptoms Persons with diabetes, elderly, women, and heart transplant patients u Atypical presentation - from drop in cardiac output (CO) – sudden dyspnea – sudden lose of consciousness (syncope) or near-syncope – unexplained drop in blood pressure – apparent stroke – confusion – generalized weakness

Atypical AMI Signs & Symptoms u Women at greater risk – symptoms ignored (by patient & MD) – under-recognized – under-treated u Typical presentation in women – nausea – lightheadedness – epigastric burning – sudden onset weakness – unexplained tiredness/weakness

Region X SOP Initial Treatment Acute Coronary Syndrome u Regardless of the end diagnosis, all patients treated initially the same – IV-O 2 -monitor-vital signs-history – aspirin – nitroglycerin – morphine if necessary – 12 lead EKG obtained (transmitted to ED by EMS) u Treatment fine-tuned as more diagnostic information is obtained

Congestive Heart Failure u Heart unable to pump efficiently u Blood backs up into systemic system, pulmonary system or both – Right heart failure umost often occurs due to left heart failure ucan occur from pulmonary embolism ucan occur from long-standing COPD (esp chronic bronchitis) – Left heart failure umost commonly from acute MI ualso occurs due to chronic hypertension

Right Heart Failure u Blood backs up into systemic circulation – gradual onset over days to weeks – jugular vein distension (JVD) – edema (most visible in dependent parts of the body) from fluids pushed out of veins – engorged, swollen liver due to edema – right sided failure alone seldom a life threatening situation u Pre-hospital treatment most often symptomatic u More aggressive treatment needed when accompanied with left heart failure

Left Sided Heart Failure u Heart unable to effectively pump blood from pulmonary veins u Blood backs up behind left ventricle u Pulmonary veins engorged with blood u Serum forced out of pulmonary capillaries and into alveoli (air sacs) u Serum mixes with air to produce foam (pulmonary edema)

Progression Left Heart Failure u Think “left - lungs” u Impaired oxygenation – compensates by respiratory rate u Fluid leaks into interstitial spaces – auscultate crackles u interstitial pressure narrows bronchioles – auscultate wheezing u Dyspnea & hypoxemia panic release of adrenaline increased work load on heart

Left Heart Failure u Sympathetic nervous system response – Peripheral vasoconstriction uperipheral resistance (afterload) increases uweakened heart has to pump harder to eject blood out through narrowed vessels ublood pressure initially elevated to keep up with the demands and to pump harder against increased vessel resistance udiaphoretic, pale, cold skin

Asthma or Heart Failure? Asthma Left heart failure u younger patient u older patient u hx of asthma u poss hx heart problems u unproductive cough u orthopnea u meds for asthma u recent rapid weight gain u wheezing u cough with watery or foamy fluid u accessory muscles being used u meds for heart problems u wheezing u JVD u Pedal or sacral edema

Which Came First - CHF or AMI? u Not unusual to see the AMI patient in pulmonary edema - watch for it! u Often hard to determine which came first and triggered the development of the other problem Heart failure poor perfusion & hypoxemia myocardium suffers from inadequate blood & oxygen supply acute myocardial ischemia acute coronary syndrome AMI poor pumping performance of heart acute failure of left heart pump left heart failure

Cardiogenic Shock u Heart extensively damaged; it can no longer function as a pump u 25% of heart damage causes left heart failure u if >40% of the left ventricle is infarcted, cardiogenic shock occurs u High mortality rate

Signs & Symptoms Cardiogenic Shock u Altered level of consciousness – confusion to unconsciousness u Restless, anxious u Massive peripheral vasoconstriction – pale, cold skin, poor renal perfusion u Pulse rapid and thready u Respirations rapid and shallow u Falling blood pressure

Treatment Goals Acute Coronary Syndrome u Goals – early recognition of a possible cardiac problem – minimize size of infarction – reduce myocardial oxygen demand – decrease patient’s fear & pain (minimizes sympathetic discharge) – salvage ischemic myocardium – prevent development of dysrhythmias – improve chances of survival

Region X SOP - Acute Coronary Syndrome u Oxygen – may limit ischemic injury u Aspirin - 324 mg chewed – blocks platelet aggregation (clumping) to keep clot from getting bigger – chewing breaks medication down faster & allows for quicker absorption – hold if patient allergic or for a reliable patient that states they have taken aspirin within last 24 hours

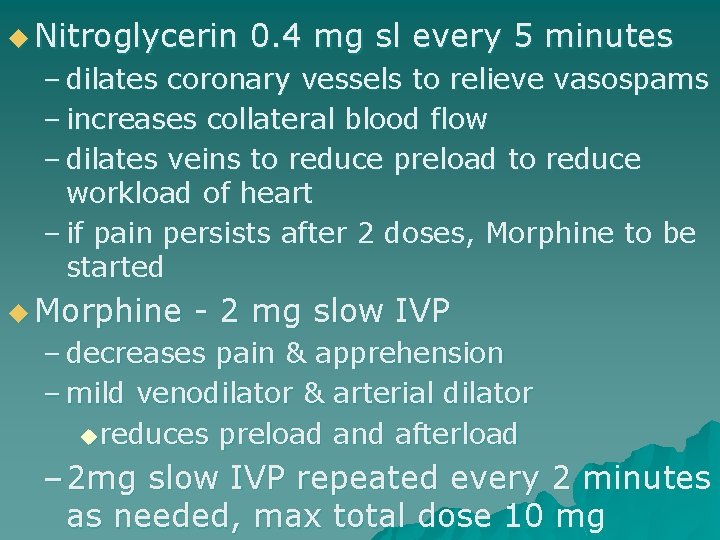
u Nitroglycerin 0. 4 mg sl every 5 minutes – dilates coronary vessels to relieve vasospams – increases collateral blood flow – dilates veins to reduce preload to reduce workload of heart – if pain persists after 2 doses, Morphine to be started u Morphine - 2 mg slow IVP – decreases pain & apprehension – mild venodilator & arterial dilator ureduces preload and afterload – 2 mg slow IVP repeated every 2 minutes as needed, max total dose 10 mg

Treatment Goals Congestive Heart Failure u Goals – improve oxygenation – decrease workload of the heart (ie: decrease preload & afterload)

Region X SOP Treatment Stable Acute Pulmonary Edema (B/P>100) u Nitroglycerin - 0. 4 mg sl – Vasodilator to create venous pooling – Reduces preload & afterload – Maximum 3 doses (repeated every 5 minutes if blood pressure remains >100) u Consider CPAP - use if indicated

Region X SOP cont’d u Lasix - 40 mg IVP – Diuretic - excess fluid excreted via kidneys – Venodilating effect to pool venous blood – Dose to 80 mg IVP if patient on Lasix at home

u Morphine - 2 mg slow IVP – Venodilator to increase pooling of blood – Anxiolytic to calm anxious patient – May repeat 2 mg dose every 2 minutes – Maximum total dose 10 mg u Albuterol - 2. 5 mg/3 ml nebulizer – Wheezing may indicate bronchoconstriction from excessive fluid – Bronchodilator could be helpful

Region X SOP cont’d u Hypotensive side effects from treatments used for stable pulmonary edema – Treatment used (NTG, Lasix, Morphine, CPAP) can all cause venodilation B/P – Blood pressure needs to be carefully monitored

Region x SOP Treatment Unstable Acute Pulmonary Edema (B/P<100) u Contact Medical Control u CPAP on orders of Medical Control u Consider Cardiogenic Shock Protocol u If wheezing (indicating bronchoconstriction), contact Medical Control for Albuterol order – if patient needs to be intubated, Albuterol to be delivered via in-line

Treatment Goals Cardiogenic Shock u Goals – Improve oxygenation – Improve peripheral perfusion – Avoid adding any workload to the heart

Region X SOP Treatment Cardiogenic Shock u Oxygen via nonrebreather mask – BVM if respirations ineffective – Intubation may become necessary u Positioning – Supine if lungs are clear – Head somewhat elevated if pulmonary edema is present (semi-fowler’s) u IV/IO fluid challenge in 200 ml increments if lung sounds are clear – The shock may include a hypovolemic component

Treatment Cardiogenic Shock u Cardiac monitor – Arrhythmias are likely u. May cause hypotension decreasing cardiac output u Dopamine Infusion - maintain B/P >100 – Effects dose related & dependent on clinical condition of patient – 5 - 20 g/kg/min has beta influence on the heart u. Increases contractility strength of heart u. To a lesser degree increases heart rate

u Dopamine cont’d – Doses >20 g/kg/min u. Alpha stimulation predominate & vasoconstriction my negatively affect circulation u Extravasation - leaking out of vessels – Can cause tissue necrosis – IV infiltration reported to ED staff; document u Dosing - start at 5 g/kg/min – Refer to table in SOP page 13 OR – Take patient’s weight in pounds, take 1 st 2 numbers, & subtract 2 (ie: 185 pounds: 18 - 2 = 16 gtts/min to start drip)

EKG Monitoring & 12 Lead EKG’s u Goal EKG monitoring – Identify a disturbance in the normal cardiac rhythm – Arrhythmias caused by u. Ischemia u. Electrolyte imbalances u. Disturbances or damage in electrical conduction system u Goal of obtaining 12 lead EKG – Early recognition Acute Coronary Syndrome u Treat clinical condition, not the monitor!

12 Lead EKG’s u EMS to transmit EKG to Medical control when following the Acute Coronary Syndrome SOP u Many patients can be monitored by a Lead II but not all patients need a 12 lead. u Some patients experiencing angina or an acute MI will not yet have any EKG changes indicated on the 12 lead.

12 Lead Transmitted From The Field u ECRN to complete the radio report u ECRN immediately after radio report to retrieve faxed copy of the field 12 lead EKG u 12 lead EKG to be immediately presented to the ED physician u 12 lead EKG from EMS is to be placed on the patient’s chart after MD review

A normal EKG DOES NOT necessarily mean there is nothing acute going on!

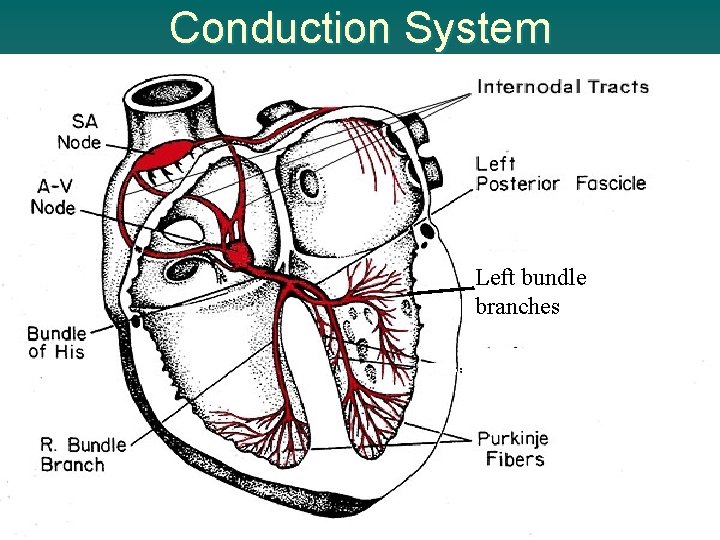
Cardiac Conduction System u SA node - dominant pacemaker – upper right atrium – blood supply from RCA u Internodal pathways – to spread electrical impulse thru-out atria u AV node in region of AV junction – in 85 -90% of people, blood supplied by RCA to AV node – in 10 -15% of people, blood supplied by left circumflex

Conduction System cont’d u bundle of His u Right and left bundle branches u Purkinje fibers - through ventricular muscle ª Changes in electrolyte concentrations influence depolarization and repolarization sodium (Na+), potassium (K+), calcium (Ca++), Magnesium (Mg++)

Conduction System LLeft bundle lbranches


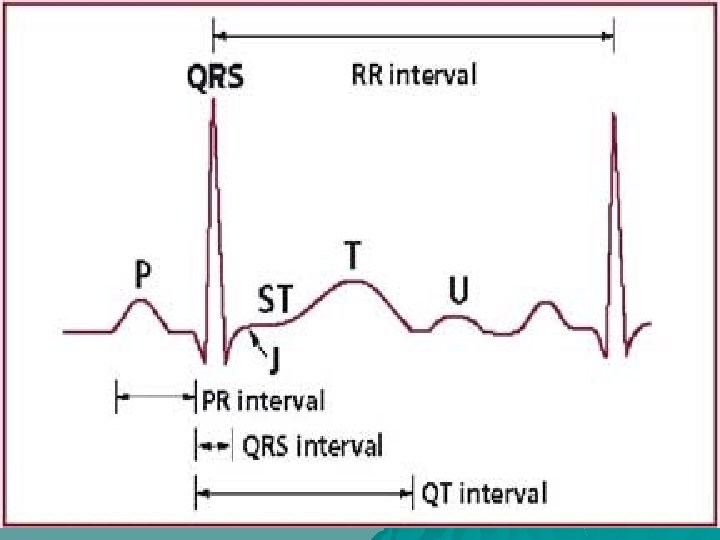
EKG Wave Forms u. P wave – depolarization of atria u PR interval – depolarization of atria & delay at AV junction – normal PR interval 0. 12 - 0. 20 seconds u QRS complex – depolarization of ventricles – normal QRS complex <0. 12 seconds u. T waves – repolarization of ventricles (and atria)

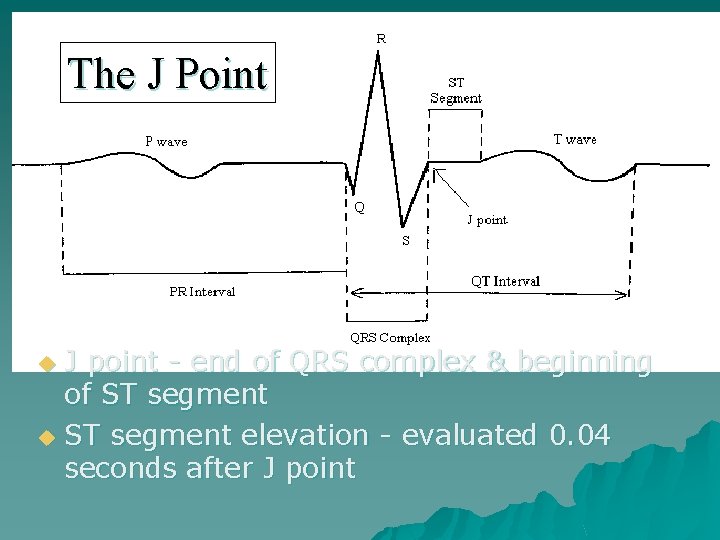
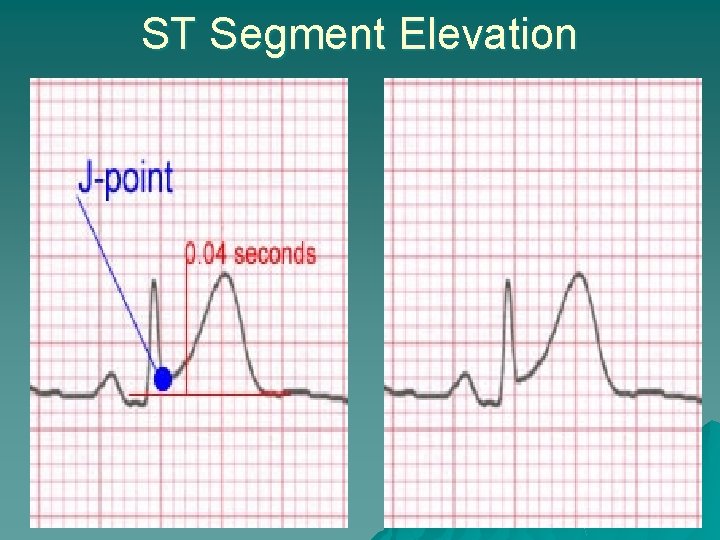
The J Point J point - end of QRS complex & beginning of ST segment u ST segment elevation - evaluated 0. 04 seconds after J point u

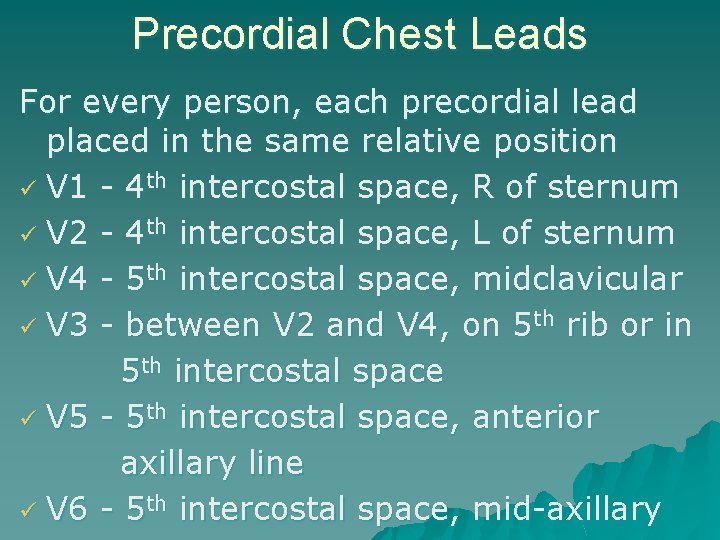
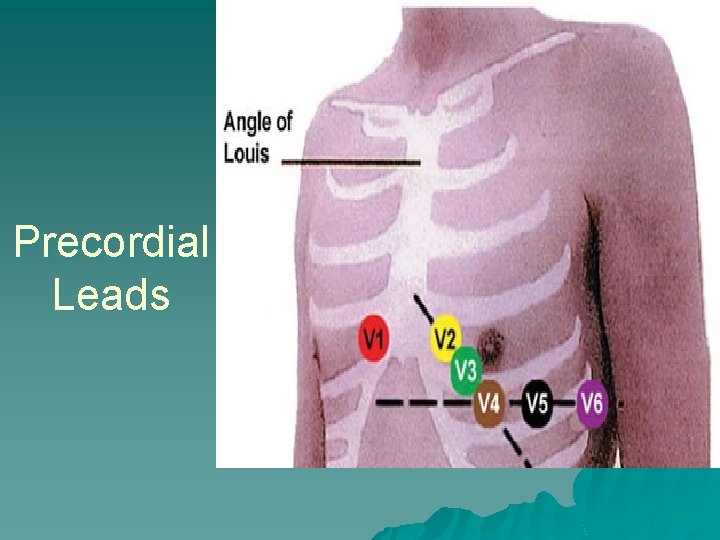
Precordial Chest Leads For every person, each precordial lead placed in the same relative position V 1 - 4 th intercostal space, R of sternum V 2 - 4 th intercostal space, L of sternum V 4 - 5 th intercostal space, midclavicular V 3 - between V 2 and V 4, on 5 th rib or in 5 th intercostal space V 5 - 5 th intercostal space, anterior axillary line V 6 - 5 th intercostal space, mid-axillary

Precordial Leads

Lead Placement u The more accurate the lead placement, the more accurate the 12 -lead interpretation when interpreted from all other EKG’s taken on this patient u 12 -leads are often evaluated on a sequential basis, each interpretation made trying to consider the previous one u V 4 -6 should be in a straight line

12 Lead Printout u Standard format 81/2 x 11 paper u 12 lead views printed on top half I a. VR V 1 V 4 II a. VL V 2 V 5 III a. VF V 3 V 6 u Additional single view of rhythm strips usually printed on bottom of report u Machines can analyze data obtained but humans must interpret data

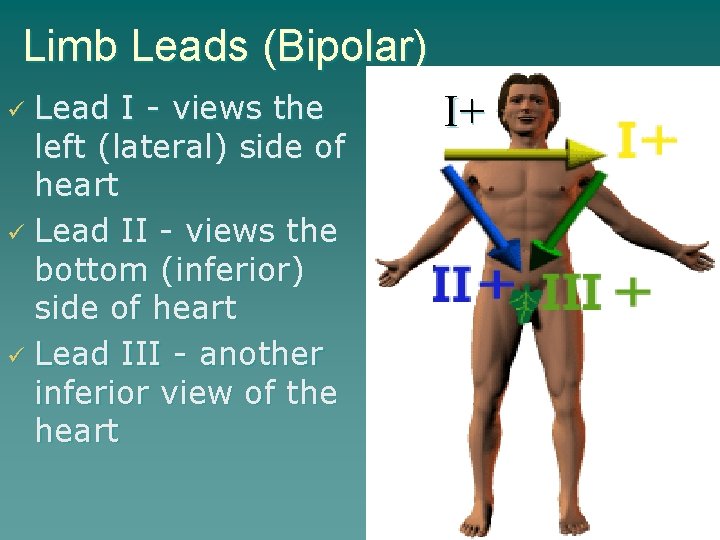
Limb Leads (Bipolar) Lead I - views the left (lateral) side of heart Lead II - views the bottom (inferior) side of heart Lead III - another inferior view of the heart I+

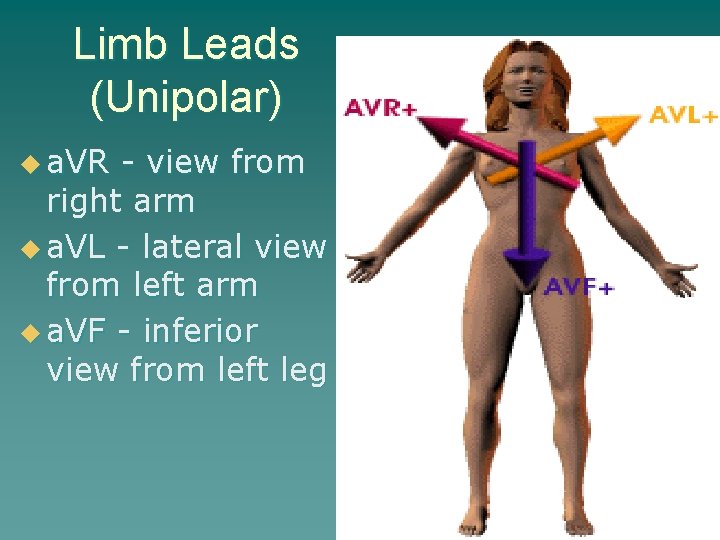
Limb Leads (Unipolar) u a. VR - view from right arm u a. VL - lateral view from left arm u a. VF - inferior view from left leg

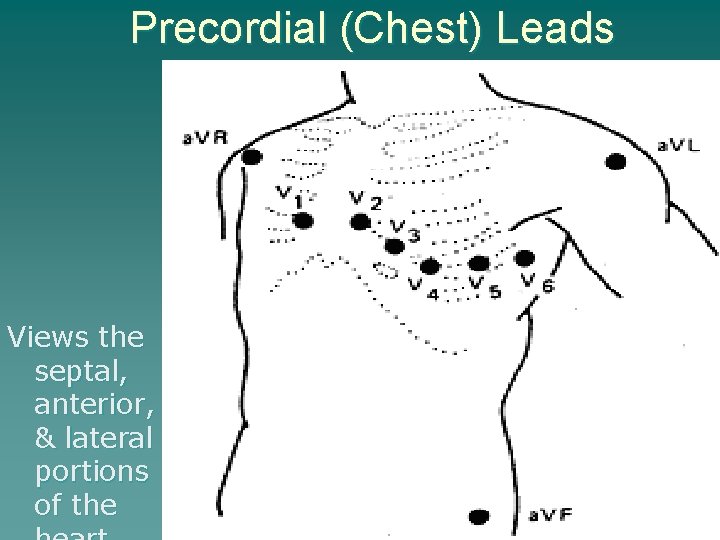
Precordial (Chest) Leads Views the septal, anterior, & lateral portions of the

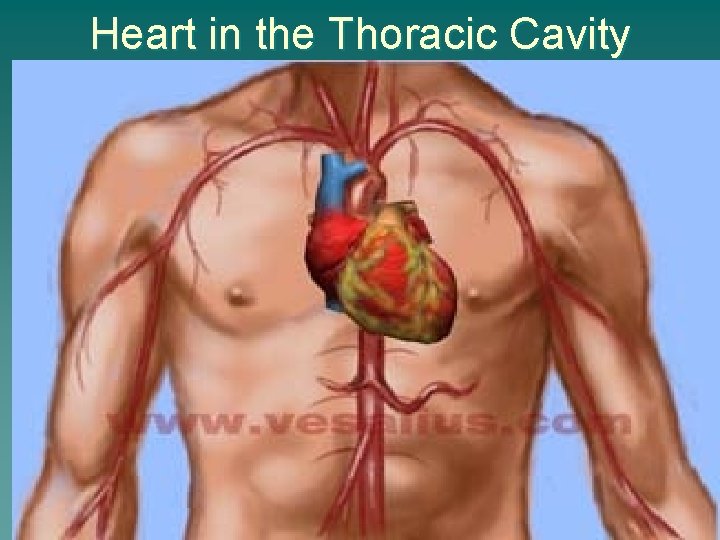
Heart in the Thoracic Cavity

Myocardial Insult u Ischemia – lack of oxygenation – ST depression or T wave inversion – permanent damage avoidable u Injury – prolonged ischemia – ST elevation – permanent damage avoidable u Infarct – death of myocardial tissue – may have Q wave

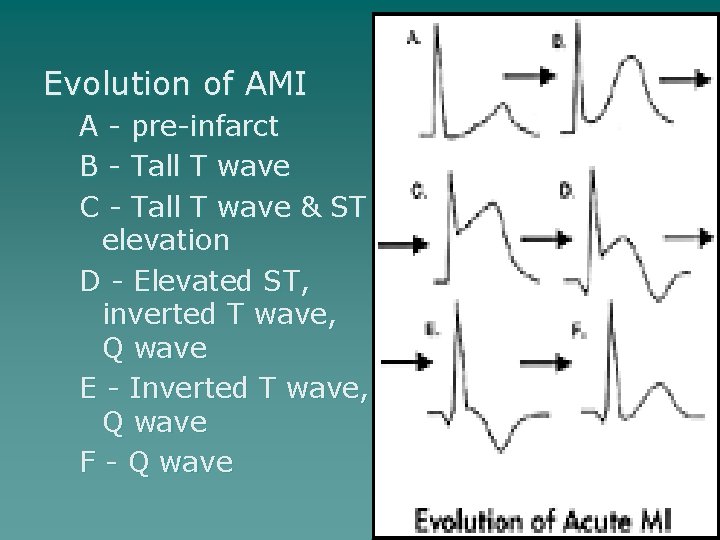
Evolution of AMI A - pre-infarct B - Tall T wave C - Tall T wave & ST elevation D - Elevated ST, inverted T wave, Q wave E - Inverted T wave, Q wave F - Q wave

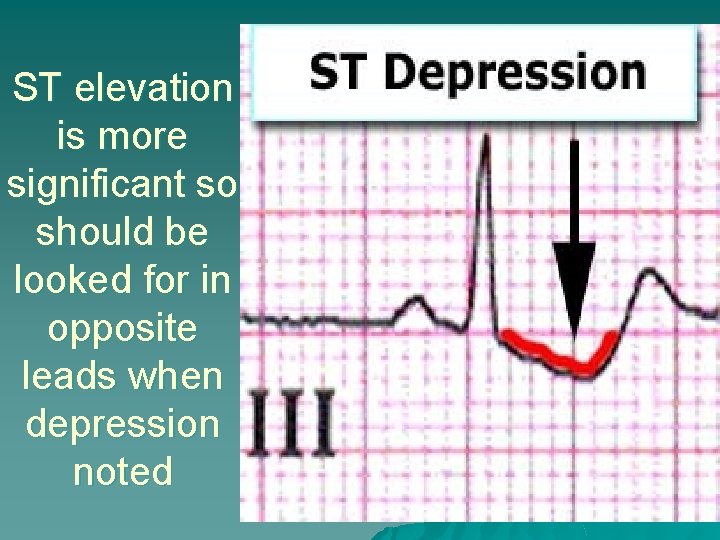
ST Depression u Can indicate ischemia electrolyte abnormality rapid heart rate digitalis influence reciprocal changes to ST elevation u ST depression measurement – 1 mm (1 small box) below baseline measured 2 mm (2 small boxes) after end of QRS

ST elevation is more significant so should be looked for in opposite leads when depression noted

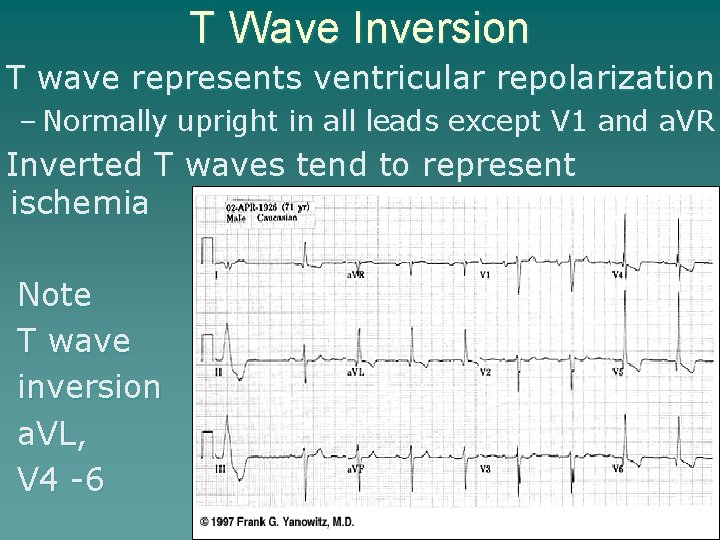
T Wave Inversion T wave represents ventricular repolarization – Normally upright in all leads except V 1 and a. VR Inverted T waves tend to represent ischemia Note T wave inversion a. VL, V 4 -6

ST Segment Elevation u Myocardium exposed to prolonged hypoxia or ischemia u Finding indicates injury or damage u Injury probably due to occluded coronary artery u Muscle can still be salvaged u If corrective intervention not taken in timely manner, tissue necrosis/death is likely (infarction) TIME IS MUSCLE!

Significant ST Elevation u ST segment elevation measurement – 0. 04 seconds after J point u ST elevation – > 1 mm (1 small box) in 2 or more contiguous chest leads (V 1 -V 6) – >1 mm (1 small box) in 2 or more anatomically contiguous leads u Contiguous lead – limb leads that “look” at the same area of the heart or are numerically consecutive chest leads

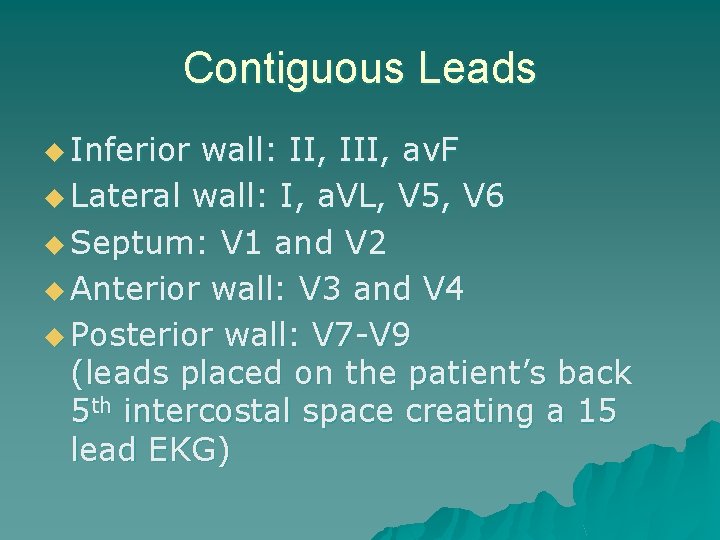
Contiguous Leads u Inferior wall: II, III, av. F u Lateral wall: I, a. VL, V 5, V 6 u Septum: V 1 and V 2 u Anterior wall: V 3 and V 4 u Posterior wall: V 7 -V 9 (leads placed on the patient’s back 5 th intercostal space creating a 15 lead EKG)

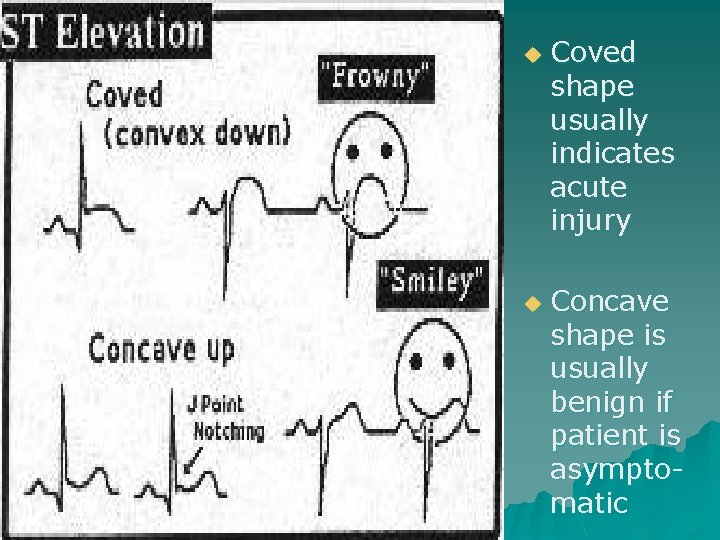
ST Segment Elevation

u u Coved shape usually indicates acute injury Concave shape is usually benign if patient is asymptomatic

Groups of EKG Leads u Inferior wall - II, III, a. VF u Septal wall - V 1, V 2 u Anterior wall - V 3, V 4 u Lateral wall - I, a. VL, V 5, V 6 u a. VR is not evaluated in typical groups u Standard lead placement does not look at posterior wall or right ventricle of the heart - need special lead placement for these views

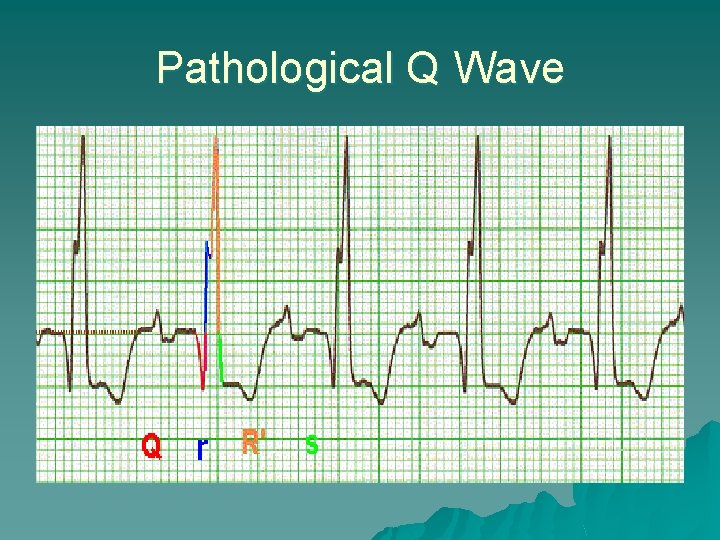
Pathological Q Waves - Infarction u Death of tissue u Pathological Q wave – >0. 04 seconds wide or – 1/ of R wave height 3 – when seen with ST elevation indicates ongoing myocardial infarction u Remember: ST segment probably single most important element on EKG when looking for evidence of AMI

Pathological Q Wave

Reciprocal Changes u Changes seen in the wall of the heart opposite the location of the infarction u Observe ST segment depression u Usually observed at the onset of infarction u Usually a short lived change u Lead Reciprocal changes II, III, a. VF I, a. VL, V 5, V 6 II, III, a. VF V 1 -V 4 V 7 -V 9

Acute MI Locator Table

Acute Myocardial Infarction Acute myocardial infarction (AMI) is part of a spectrum of disease known as acute coronary syndrome (ACS) u ACS – Larger term to cover a group of clinical syndromes compatible with acute myocardial ischemia – Chest pain is due to insufficient blood supply to the heart muscle that results from coronary artery disease (CAD) – Clinical conditions include unstable angina to non-Q wave MI and Q wave MI u

Common Complications of AMI u V 1 -2: septal wall - infranodal heartblock, BBB u V 3 -4: anterior wall - LV dysfunction, CHF, BBB, 3 rd degree HB, PVC’s u I, a. VL, V 5 -6: lateral wall -LV dysfunction, AV nodal block in some u II, III, a. VF: inferior & posterior wall LV - hypotension, sensitivity to Nitroglycerin & Morphine

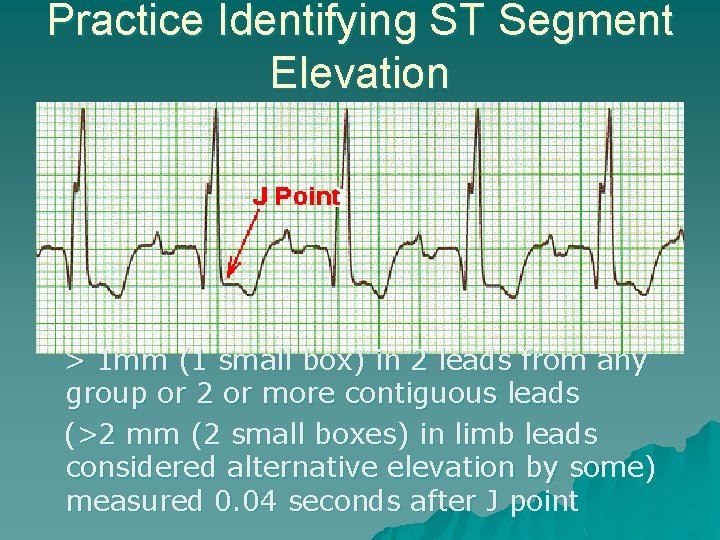
Practice Identifying ST Segment Elevation > 1 mm (1 small box) in 2 leads from any group or 2 or more contiguous leads (>2 mm (2 small boxes) in limb leads considered alternative elevation by some) measured 0. 04 seconds after J point

Think Pattern Recognition Inferior Wall MI

Think Pattern Recognition Lateral Wall MI

Think Pattern Recognition Anterior Wall MI

Think Pattern Recognition Septal Wall MI

Test Yourself What pattern would indicate an anterior/septal wall MI?

Practice Identifying Leads Showing ST Elevation Evaluate the top 3 rows of the 12 -lead EKG Answers follow the 12 lead


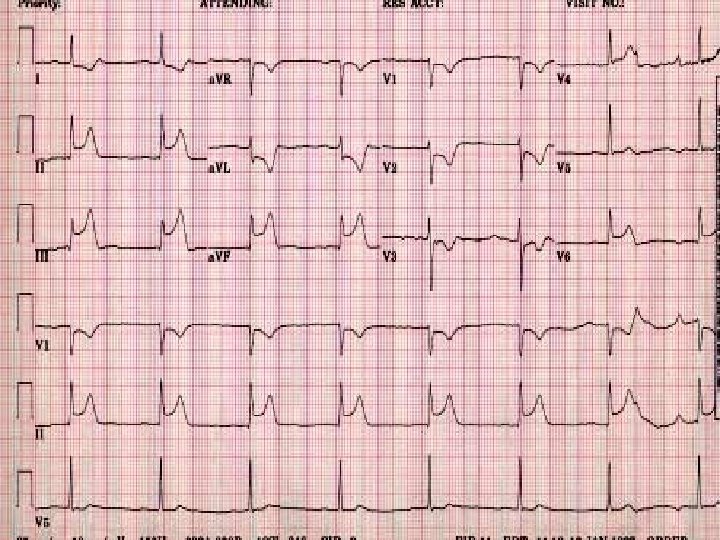
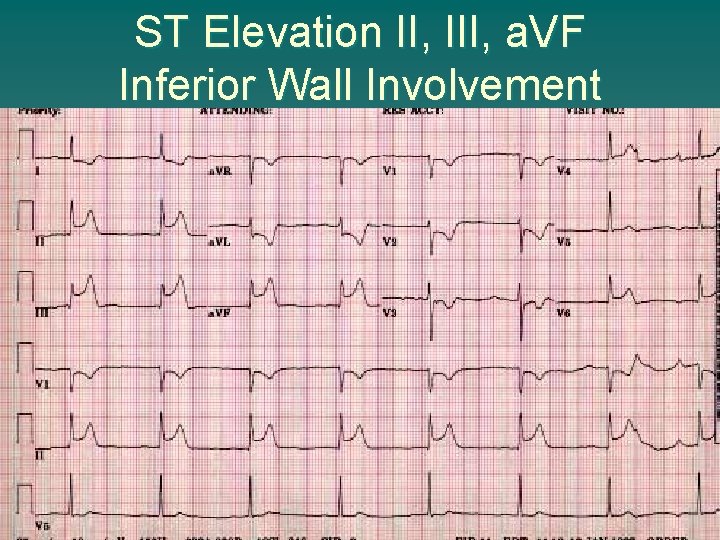
ST Elevation II, III, a. VF Inferior Wall Involvement


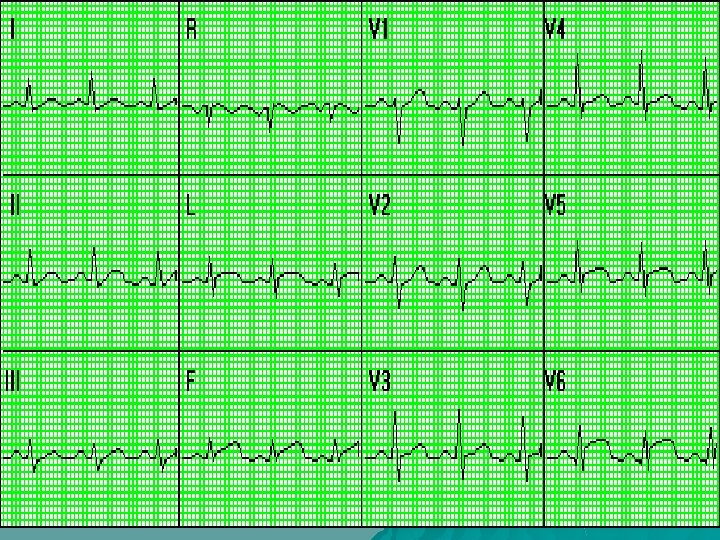
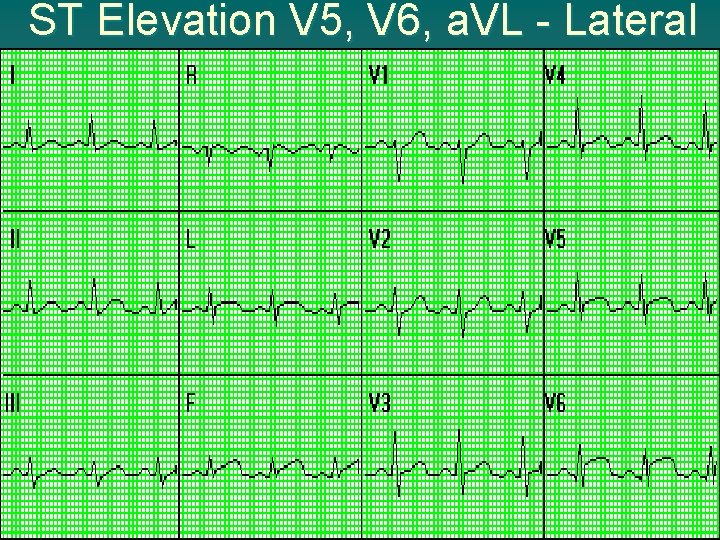
ST Elevation V 5, V 6, a. VL - Lateral


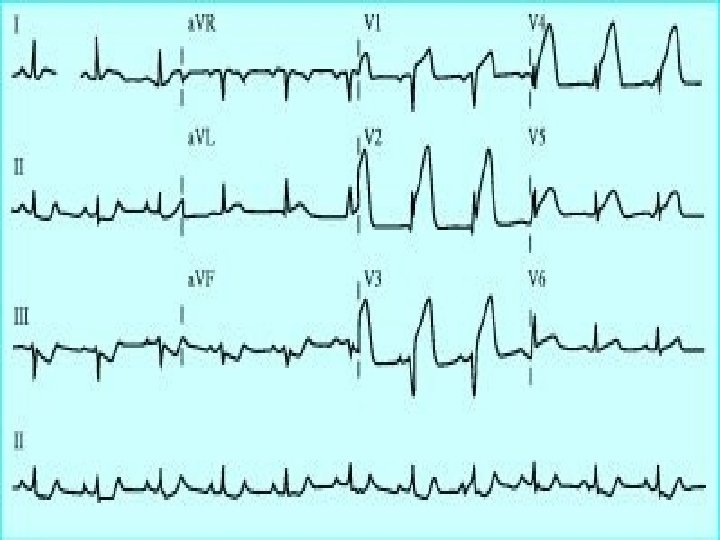
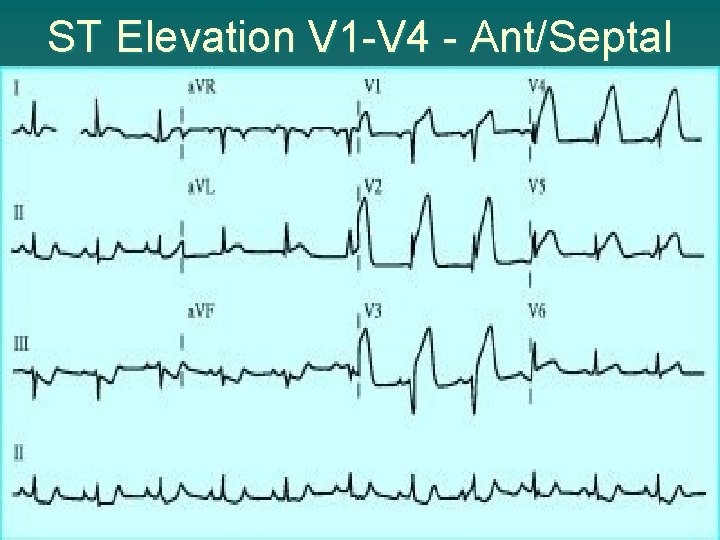
ST Elevation V 1 -V 4 - Ant/Septal


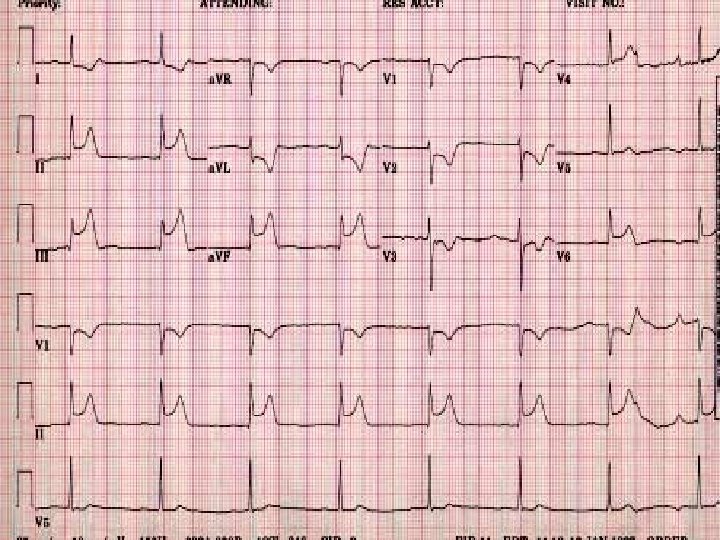
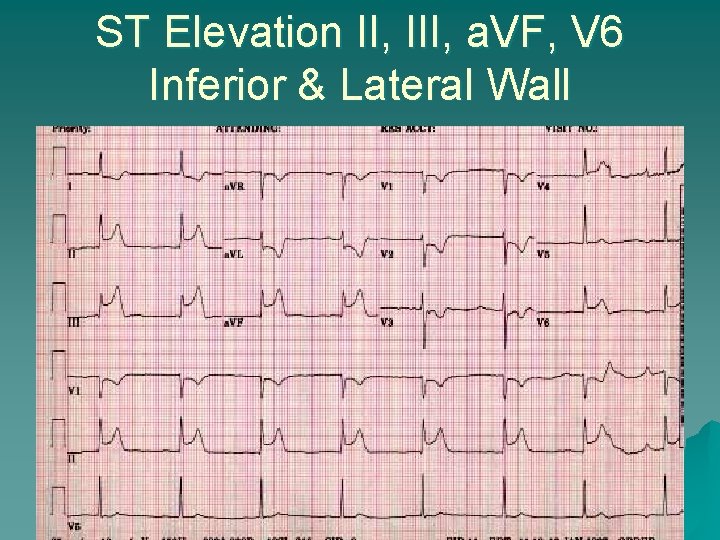
ST Elevation II, III, a. VF, V 6 Inferior & Lateral Wall


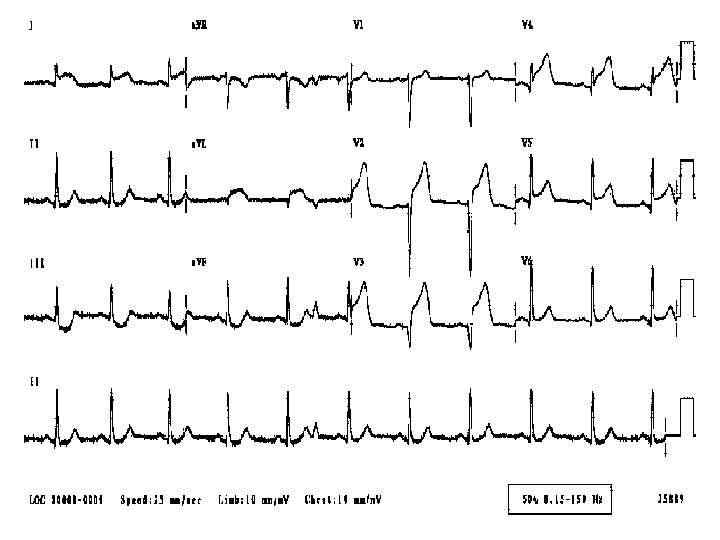
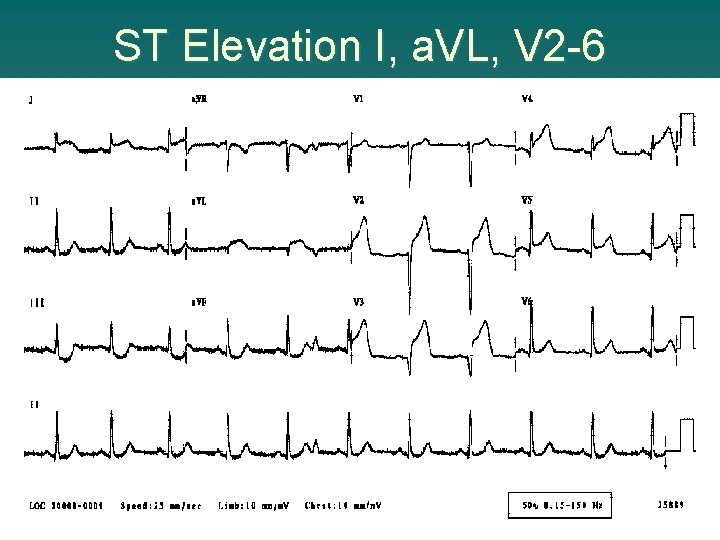
ST Elevation I, a. VL, V 2 -6


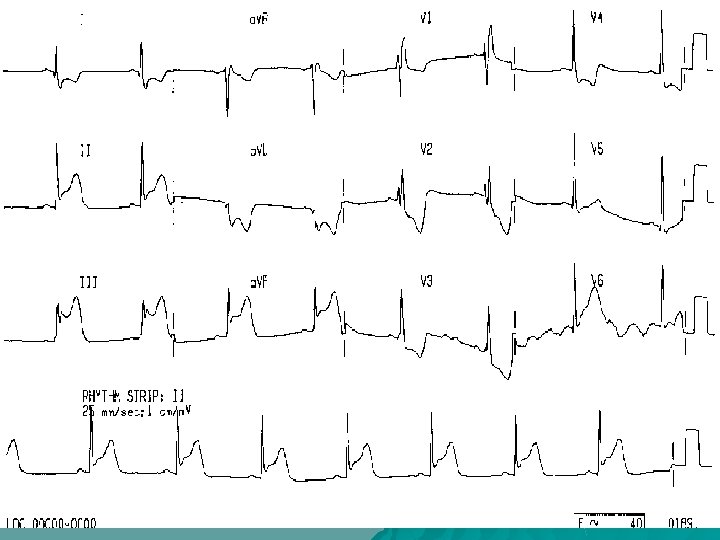
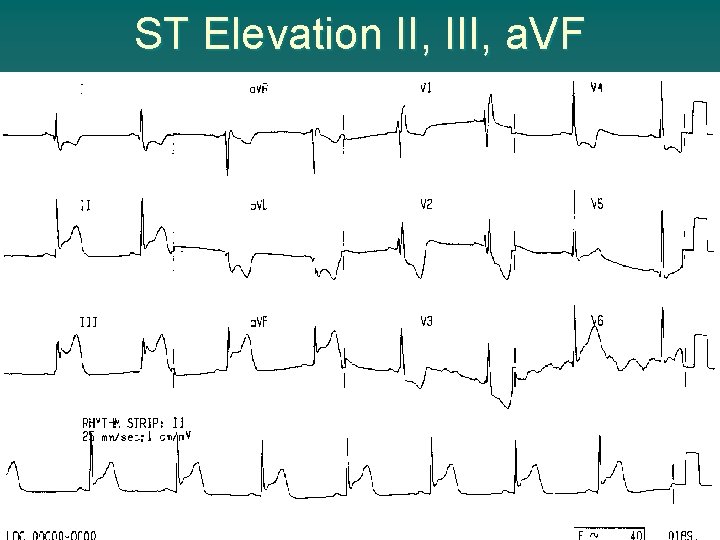
ST Elevation II, III, a. VF

Case Discussion #1 u 66 year-old male presents with “indigestion” for past 2 hours, frequent belching, nausea, paleness, diaphoresis, left arm discomfort u Vital signs – 102/76 HR 98 RR 20 u What Sa. O 2 98% is your impression and what initial treatment is indicated in the prehospital setting?

Case #1 u Impression: possible AMI (assume and treat for the worse) u SOP: Acute Coronary Syndrome u Prehospital treatment: – IV-O 2 -monitor-pulse ox – Vitals stable – History unremarkable – Aspirin chewed (any contraindications? ) – Nitroglycerin sl (ask about Viagra use) – Morphine if pain unrelieved after 2 NTG – 12 lead transmitted to ED for interpretation

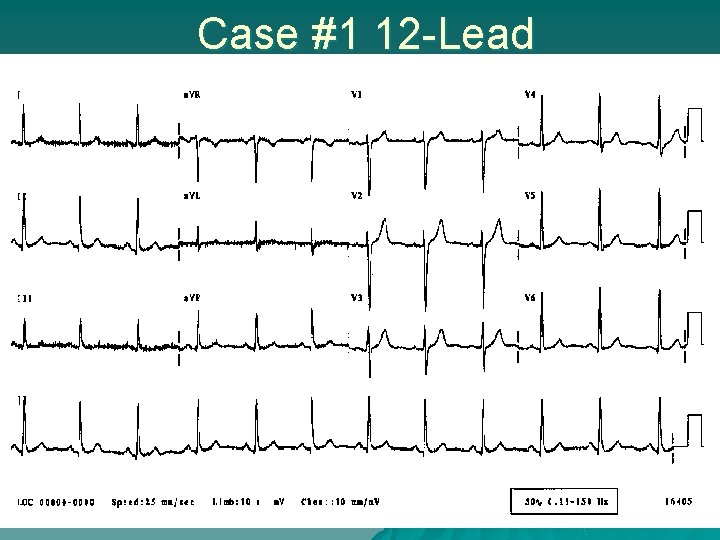
Case #1 12 -Lead

Case #1 u Impression of 12 lead? – no ST segment elevation noted u Does lack of ST segment elevation change field treatment for this patient? – Normal EKG does not preclude that acute myocardial event is occurring – Acute Coronary Syndrome SOP to be followed

Case Discussion #2 u 77 year-old female with history of CABG, hypertension, cholesterol, and long standing diabetes u Presents with vague complaints of not feeling well, very tired & no energy over the last day u Meds: – Aspirin, Isoptin, Toprol, Hydrochlorothiazide, Lipitor, Glucophage

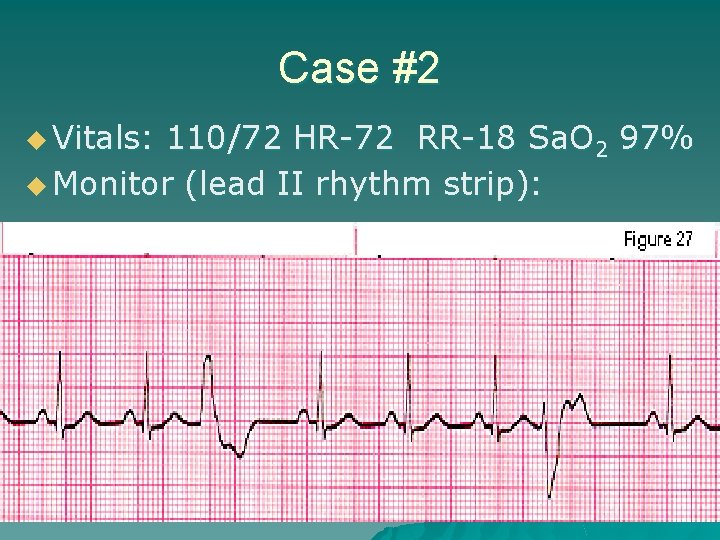
Case #2 u Vitals: 110/72 HR-72 RR-18 Sa. O 2 97% u Monitor (lead II rhythm strip):

Case #2 u What is your initial impression? u Need to at least consider possible MI u Remember: – women, elderly, and long standing diabetics report the most atypical complaints u Remember: – a lead II only looks at one view of the heart – a normal EKG does not rule out AMI

Case #2 u Prehospital treatment: – IV-O 2 -monitor (SR with PVCs)-vitals – Aspirin appropriate? – Nitroglycerin indicated? – 12 lead EKG necessary? – What about antidysrhythmic for the PVC’s? ucall Medical Control for guidance uoxygen is often enough to suppress PVC activity

Case #2 u Aspirin – if patient reliable and took own dose within last 24 hours, can omit, document why omitted and when taken u Nitroglycerin – patient not having chest pain. Defer to Medical Control for orders – no contraindications noted (B/P >100; no viagra type drug used within past 24 hours - ask, don’t assume!) u 12 lead should be obtained on high index of suspicion

Case #3 u 81 year-old female complaining of shortness of breath for past 2 days. Unable to tolerate lying flat; JVD noted u History of CHF, angina, arthritis, and mild COPD u Vitals: 126/92 HR-170 RR-24 Sa. O 2 97% u Medications: nitroglycerin PRN, – Lasix 40 mg daily – Potassium – Aspirin, one daily – Proventil inhaler PRN

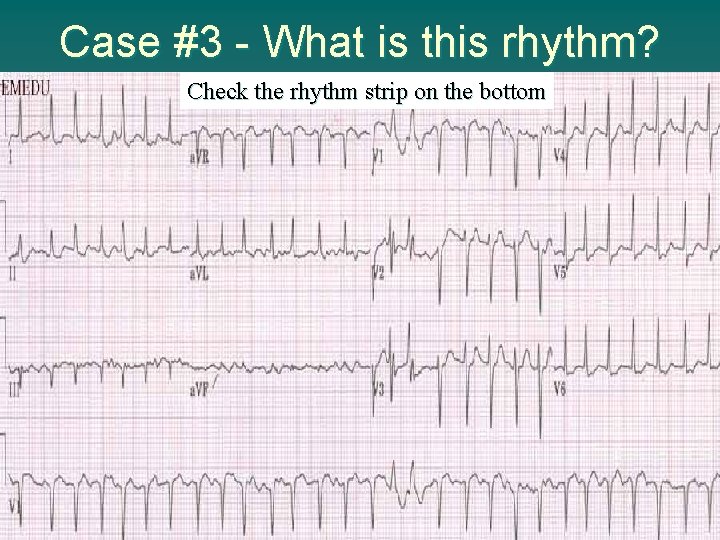
Case #3 - What is this rhythm? Check the rhythm strip on the bottom

u Rhythm Case #3 Rapid atrial fibrillation u Initial impression? Rapid atrial fibrillation u heart rate ineffective pumping cardiac output u Prehospital treatment initiated IV-O 2 -monitor-vitals-history u Goal of therapy - slow down heart rate u Is patient stable or unstable? – Stable - B/P >100, alert & cooperative

Case #3 u Prehospital ALS treatment – If Diltiazem not available, then what? u Verapamil – 5 mg IVP slowly over 2 minutes – If no response after 15 minutes and B/P remains >100, repeat 5 mg slow IVP u Carefully monitor patient for development of further deterioration and increased difficulty breathing u Position of comfort - usually sitting up

Verapamil / Isoptin® Action u Calcium channel blocker u Slows conduction thru AV node to control ventricular rate u Relaxes vascular smooth muscle u Dilates coronary arteries

Region X SOP - Verapamil Indications u Alternative to Diltiazem/cardizem u SVT not responsive to 2 doses of Adenosine - to terminate rhythm u Stable rapid atrial flutter/fibrillation to control heart rate Dosing u 5 mg IVP slowly over 2 minutes u If no response after 15 minutes and B/P >100, may repeat Verapamil 5 mg IVP slowly over 2 minutes

Verapamil Side Effects u Headache, dizziness u B/P from vasodilation u nausea & vomiting Contraindications u B/P u Wide complex tachycardias of uncertain origin u Heart block without implanted pacemaker u WPW, short PR & sick sinus syndromes

Case #4 u 32 year-old male patient with complaints of chest tightness, shortness of breath, and just not feeling well for past 2 days. Also states sore throat and ear pain. Very anxious & scared. u No history, no meds u Jogs 2 -3 miles 5 times per week u Vitals: 110/70 HR-68 RR-20 Sa. O 2 98% u Lungs clear; skin warm, dry & pink

Case #4 u Initial impression Cardiac? Musculoskeletal (what has patient been doing)? Viral illness (sore throat & ear pain)? u What treatment would EMS begin? Cardiac - can give Aspirin but call Medical Control for NTG or Morphine Normal EKG cannot rule out ACS process

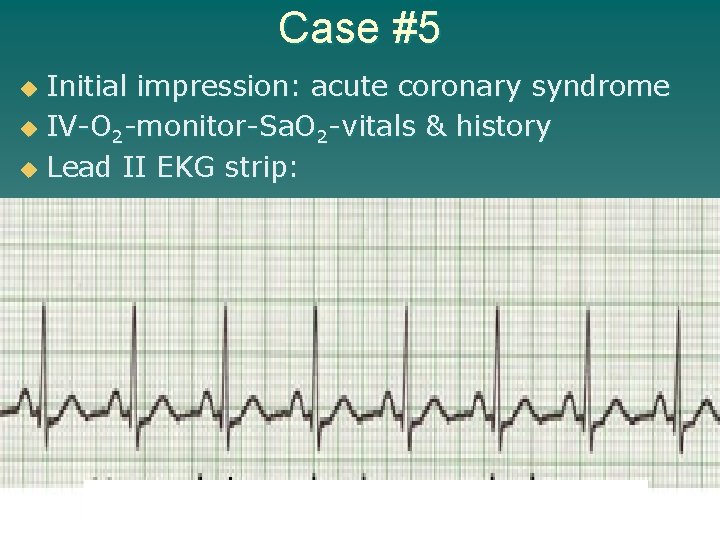
Case #5 u 68 year-old male called 911 due to non -radiating chest discomfort (not relieved with 3 of the patient’s own nitroglycerin) with some minor shortness of breath u History: – stable angina – GERD – hypertension (controlled with medications) – Type II diabetic (recently diagnosed)

Case #5 u Allergies - aspirin u Medications – nitroglycerin PRN – isordil – nexium – verapamil – glucophage u Vital signs – 136/78 HR-78 RR-18 Sa. O 2 99% u What is the initial impression & what prehospital treatment is initiated?

Case #5 Initial impression: acute coronary syndrome u IV-O 2 -monitor-Sa. O 2 -vitals & history u Lead II EKG strip: u

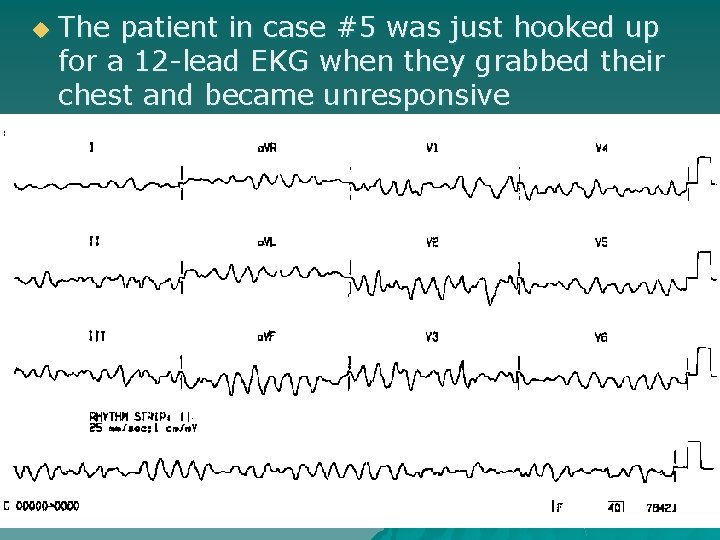
u The patient in case #5 was just hooked up for a 12 -lead EKG when they grabbed their chest and became unresponsive

Case #5 u What is this rhythm strip? u What action needs to be taken by EMS?

Case #5 - VF u Confirm no breathing, no pulse u Begin CPR until the defibrillator is ready and is charged to maximum joules u Clear the patient & deliver 1 shock u Immediately resume CPR for 2 minutes (5 cycles of 30: 2) u Check rhythm, defibrillate u Meds: vasopressor (Epinephrine) antidysrhythmic (choose 1) u 1 shock in between meds & 2 min CPR

VF/Pulseless VT SOP Meds u Epinephrine 1 mg every 3 -5 minutes IV/IO for duration of arrest u Antidysrhythmic: Amiodarone 300 mg IV/IO 1 st dose OR Lidocaine 1. 5 mg/kg IV/IO 1 st dose u Repeat dose antidysrhythmic x 1 in 5 min: If Amiodarone given, then 150 mg IV/IO OR If Lidocaine given, then 0. 75 mg/kg IV/IO

Antidysrhythmics in VF/VT u Amiodarone to the vein) needs to be diluted (irritable – total of 20 ml syringe (med mixed with saline) – rapid push in VF/VT (slow if pt has pulse!) u Lidocaine - – if unsuccessful defibrillation ucontact Medical Control for 3 rd dose order – if defib successful & bolus given < 10 min, begin drip 2 mg/min (30 mcgtts) – if defib successful & bolus given >10 min, give Lido 0. 75 mg/kg IV/IO & start drip

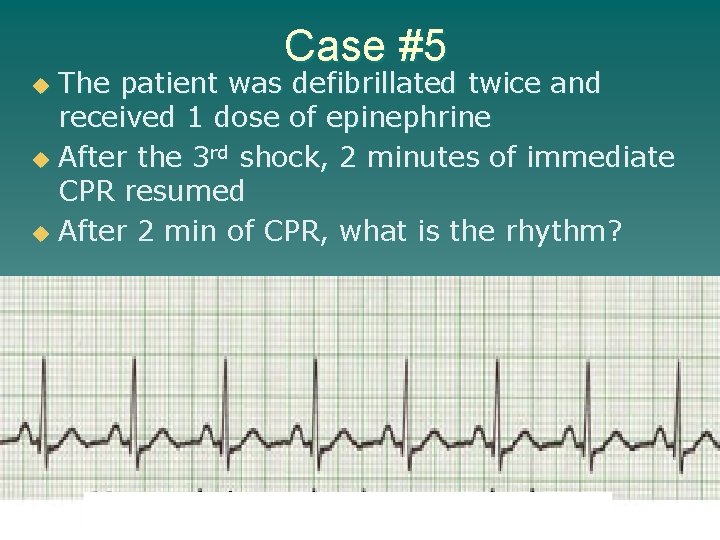
Case #5 The patient was defibrillated twice and received 1 dose of epinephrine u After the 3 rd shock, 2 minutes of immediate CPR resumed u After 2 min of CPR, what is the rhythm? u

Case #5 u Rhythm: sinus rhythm u EMS action? – Determine if there is a pulse (yes!!!) – Reevaluate airway, breathing, circulation-B/P – Medications: ubecause no antidysrhythmic were given, need to call Medical Control for direction if Lidocaine, usually 0. 75 mg/kg IV/IO if Amiodarone, 150 mg diluted into 100 ml bag D 5 W; run thru mini-drip tubing; run piggyback at rapid drip over 10 minutes u. May not want any antidysrhythmic given

ETT Route u Endotracheal tube route is discouraged, not eliminated. u Absorption found to be unpredictable u ETT drugs if this route is used L - Lidocaine E- Epinephrine A- Atropine N - Narcan u Double the calculated amount for the IV/IO route

Bibliography u American Heart Association Guidelines CPR ECC 2005 u Beasley, B. , West, M. Understanding 12 Lead EKG. Pearson Ed, 2001. u Caroline, Nancy. Emergency Care in The Streets, Jones & Bartlett, 2008. u Page, B. 12 -Lead EKG, Pearson, 2005. u Phalen, T, Aehlert, B. The 12 -Lead EKG in Acute Coronary Syndromes, 2006. u www. clevelandclinic. org u www. nhlbi. nih. gov/health/dci/Diseases