Hematology Oncology Emergencies Elizabeth Ellent LSU Hematology Oncology

Hematology Oncology Emergencies Elizabeth Ellent LSU Hematology Oncology Fellowship New Orleans Health Sciences Center July 2018 Adapted from Jennifer Slim’s 2015 and Alejandra Fuentes 2017 presentation

Overview Tumor Lysis Syndrome Hypercalcemia of Malignancy Malignant Spinal Cord Compression Acute Leukemia with Hyperleukocytosis SVC Syndrome Consumptive Coagulopathies Neutropenic Fever

Tumor Lysis Syndrome When to worry….

Metabolic Complications Cardiac Renal Insufficiency Crystallization of uric acid and calcium phosphate Seizures Sudden Death
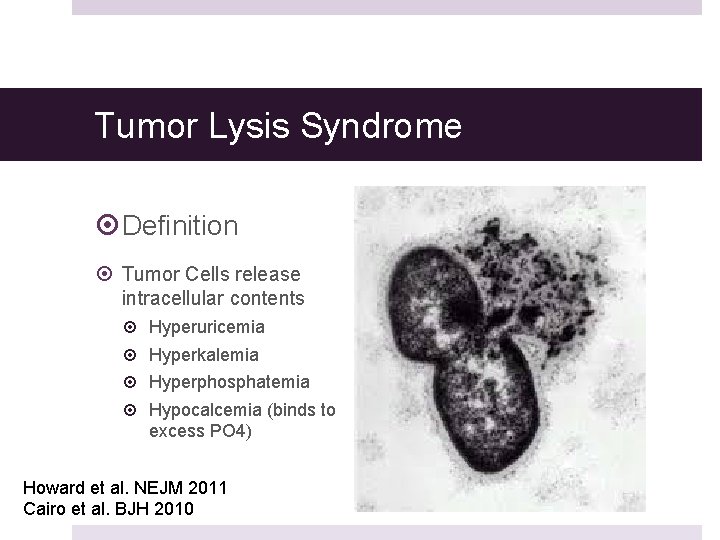
Tumor Lysis Syndrome Definition Tumor Cells release intracellular contents Hyperuricemia Hyperkalemia Hyperphosphatemia Hypocalcemia (binds to excess PO 4) Howard et al. NEJM 2011 Cairo et al. BJH 2010
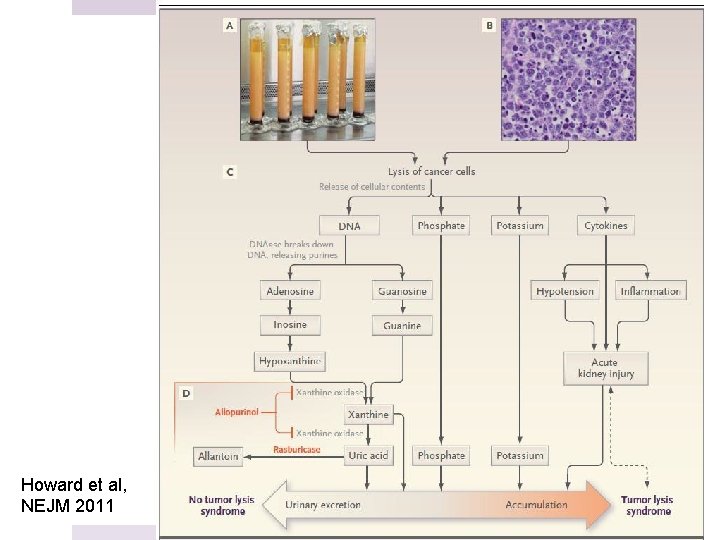
Howard et al, NEJM 2011

Tumor Lysis Syndrome Cairo et al. BJH 2010
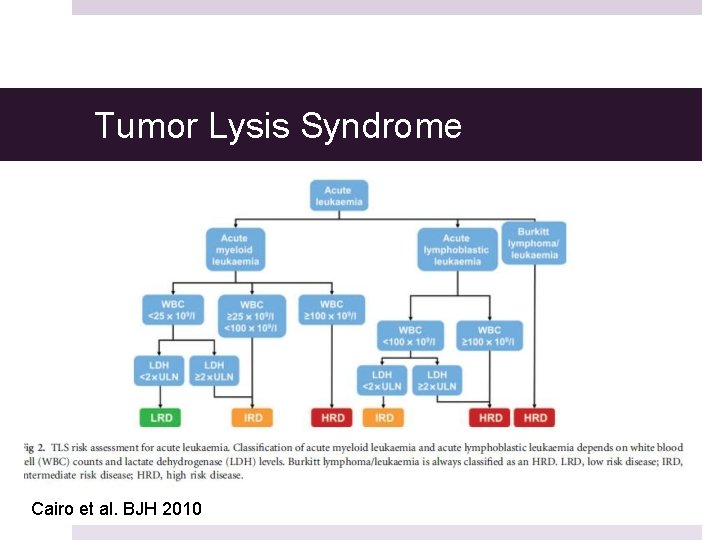
Tumor Lysis Syndrome Cairo et al. BJH 2010
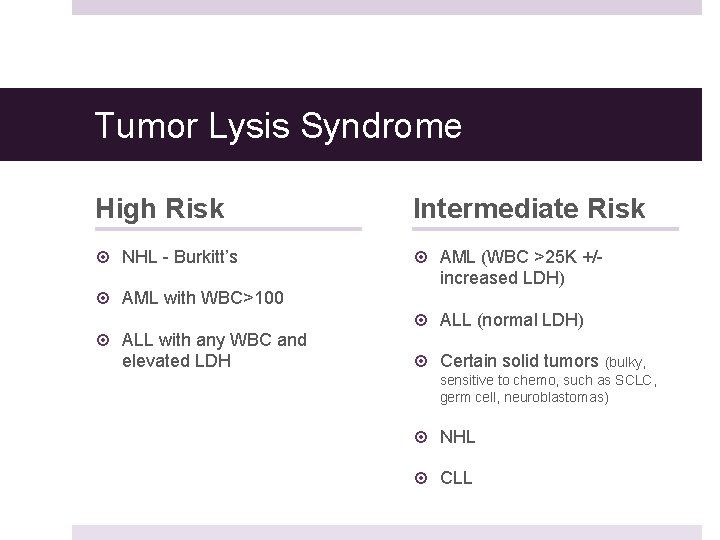
Tumor Lysis Syndrome High Risk Intermediate Risk NHL - Burkitt’s AML (WBC >25 K +/increased LDH) AML with WBC>100 ALL with any WBC and elevated LDH ALL (normal LDH) Certain solid tumors (bulky, sensitive to chemo, such as SCLC, germ cell, neuroblastomas) NHL CLL

Tumor Lysis Syndrome Important to consider and start prophylaxis / treatment Prophylaxis for intermediate/high risk malignancies: IVF and allopurinol 300 mg daily Treatment Fluids, fluids (no evidence of benefit for sodium bicarb) Uric Acid – Allopurinol or Rasburicase Electrolyte management

Hyperuricemia NCCN Guidelines Coiffier et al. JCO 2008

Rasburicase

Black Box Warning WARNING: ANAPHYLAXIS, HEMOLYSIS, METHEMOGLOBINEMIA, AND INTERFERENCE WITH URIC ACID MEASUREMENTS Anaphylaxis: ELITEK can cause severe hypersensitivity reactions including anaphylaxis. Immediately and permanently discontinue ELITEK in patients who experience a serious hypersensitivity reaction. Hemolysis: Do not administer ELITEK to patients with glucose-6 -phosphate dehydrogenase (G 6 PD) deficiency. Immediately and permanently discontinue ELITEK in patients developing hemolysis. Screen patients at higher risk for G 6 PD deficiency (e. g. , patients of African or Mediterranean ancestry) prior to starting ELITEK. Methemoglobinemia: ELITEK can result in methemoglobinemia in some patients. Immediately and permanently discontinue ELITEK in patients developing methemoglobinemia. Interference with Uric Acid Measurements: ELITEK enzymatically degrades uric acid in blood samples left at room temperature. Collect blood samples in pre-chilled tubes containing heparin and immediately immerse and maintain sample in an ice water bath. Assay plasma samples within 4 hours of collection.
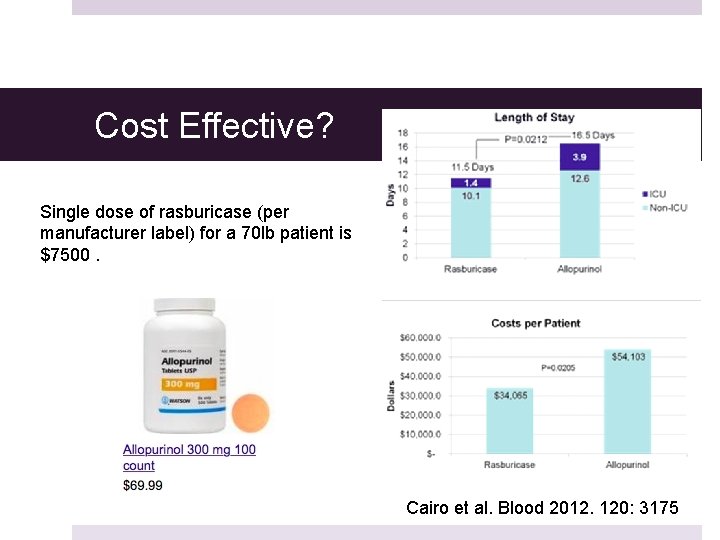
Cost Effective? Single dose of rasburicase (per manufacturer label) for a 70 lb patient is $7500. Cairo et al. Blood 2012. 120: 3175

TLS Electrolytes Hyperkalemia Depletion total body potassium Potassium binders – sodium polystyrene sulfonate Loop (lasix) Hemodialysis Shift potassium intracellular Insulin (and D 5) Beta-agonist, albuterol neb (at least 10 mg dose) Stabilize cardiac membrane Calcium gluconate

TLS Electrolytes Hyperphosphatemia Phosphate binder Aluminum carbonate Calcium acetate PO Hypocalcemia Calcium gluconate/chloride

Tumor Lysis Syndrome: recap Think about it! Order G 6 PD in high risk groups Start FLUIDS Start Allopurinol Think about Rasburicase Monitoring, Level of Care and Labs – Q 4 -6 hrs

Hypercalcemia of Malignancy When to worry and what to do…

Overview Hypercalcemia Common in Cancer about 10 -20% of malignancies Three main mechanisms PTHr. P related Osteolytic Metastases Tumor Production of calcitriol Most common associated malignancies Breast Lung Multiple Myeloma Occurs abruptly, can be severe and has a poor prognosis Ca Cancer J Clin 2011
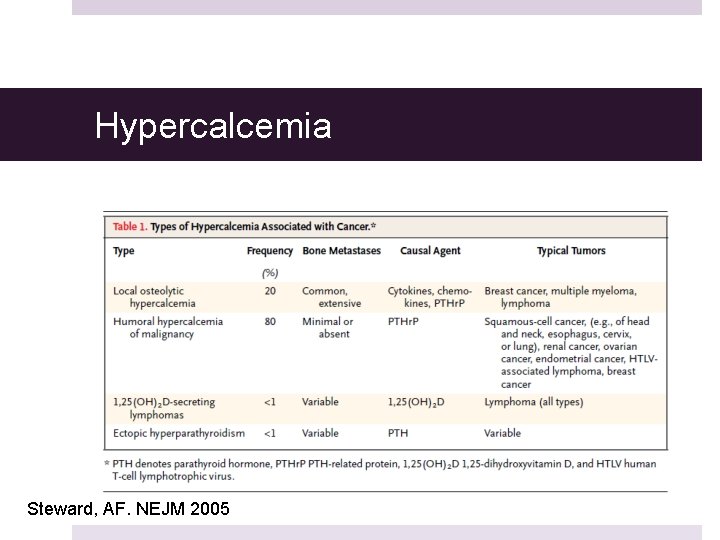
Hypercalcemia Steward, AF. NEJM 2005

Hypercalcemia Bones, moans, stones and groans CNS Confusion Seizures lethargy GI Nausea/vomiting Abdominal pain Constipation GU Renal failure Osmotic diuresis Cardiovascular EKG changes Sudden death

Then Add…. Hypercalcemia concentrates water s/s include nausea / vomiting Further adds to dehydration Further decrease in GFR and Reduced Calcium excretion

Making the Diagnosis: LABS Total serum calcium Calcium is bound to albumin Multiple Myeloma also produces excess immunoglobulins which also bind calcium Ionized calcium, Check it – this is your best test and can usually be completed rapidly Look outside the malignancy box PTH Consider 1, 25(OH)2 D when thinking sarcoid, granulomatous disease

When to Worry? ? ? Rapid Rise – not good Severe >14 mg/d. L Moderate 12 -13. 9 mg/d. L Mild Elevated – but <12 mg/d. L

Treatment IVFS – Normal Saline 200 -500 cc hourly After volume replete Now add loop diuretics while you continue fluids Based on studies with Lasix 80 -100 mg IV and 10 L NS daily Most recommend 20 – 40 mg BID for naïve patients 9 patients in this study – 7 responded to therapy Don’t forget to STOP THIAZIDES Calcif Tissue Int. 1992; 50(2): 107.

Calcitonin Increases renal calcium excretion Interferes with osteoclast activity. Will decrease serum levels 1 -2 mg/d. L and works for about 48 hours Tachyphylaxis Receptor down regulation Nasal application does not lower calcium Ann Intern Med. 2008; 149(4): 259.

Bisphonates Proportion of patients achieving a complete response by treatment group. Pierre Major The Oncologist 2002; 7: 481 -491 © 2002 by Alpha. Med Press

Treatment Recap Lewis et al. CA Cancer J Clin 2011
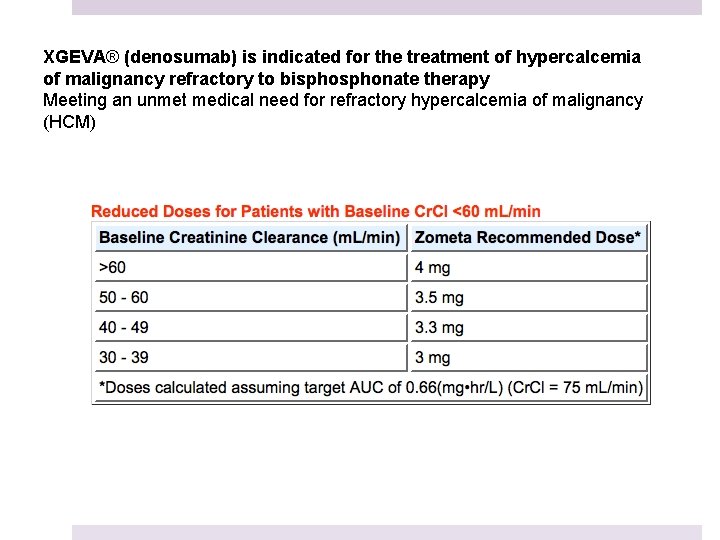
XGEVA® (denosumab) is indicated for the treatment of hypercalcemia of malignancy refractory to bisphonate therapy Meeting an unmet medical need for refractory hypercalcemia of malignancy (HCM)

And the Calcium goes Back Up! Denosumab (Xgeva) In an open-label, single-arm trial of patients with HCM (N=33), approximately 64% achieved CSC ≤ 11. 5 mg/d. L by day 10 Approved by the FDA for Hypercalcemia of Malignancy refractory to Bisphonate therapy Administer 120 mg every 4 weeks with additional 120 mg doses on Days 8 and 15 of the first month of therapy. Administer subcutaneously in the upper arm, upper thigh, or abdomen J Clin Endocrinol Metab. 2014; 99: 3144 -3152.
Spinal Cord Compression Brain Mets When to wake up your neurosurgeon and/or radiation oncologist

First Things First Spinal Cords Compression = Surgical EMERGENCY Surgery MUST evaluate this patient right away. If not a surgical candidate, get rad-onc on board. Think about appropriate level of care CT scan in the ER MRI

Symptoms Back pain 83 -95% Motor weakness 60 -85% Sensory changes Autonomic dysfunction

What to do…. Bolus Steroids (Dexamethasone) 10 mg IV x 1 dose Maintenance 4 -6 mg Q 6 -8 hours with a goal of 16 mg/ daily IV preferred awaiting surgical considerations Supportive Care PPI for GI prophylaxis Heimdal et al. J Neurooncol 1992 Sorensen et al. Eur J Cancer 1994 Vecht et al, Neurology 1989 Maranzano et al. Am J Clin Oncol 1996
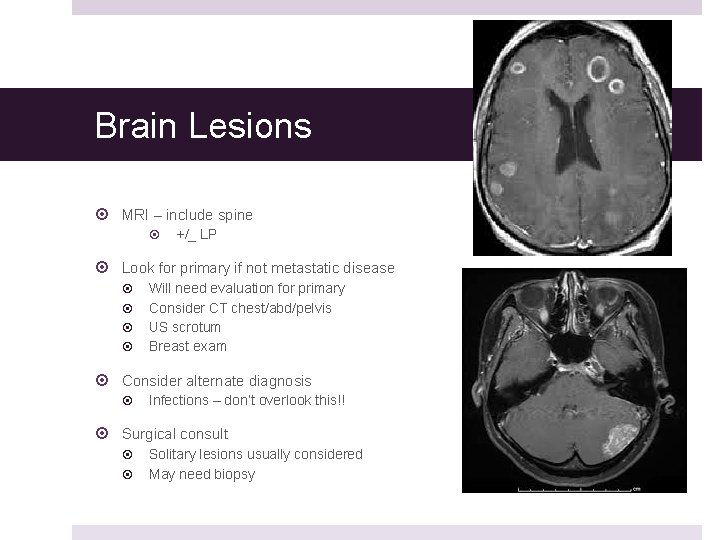
Brain Lesions MRI – include spine +/_ LP Look for primary if not metastatic disease Will need evaluation for primary Consider CT chest/abd/pelvis US scrotum Breast exam Consider alternate diagnosis Infections – don’t overlook this!! Surgical consult Solitary lesions usually considered May need biopsy

Recap: Early recognition and appropriate imaging Steroids Supportive care Radiation vs Surgery Chemotherapy / treat underlying issue
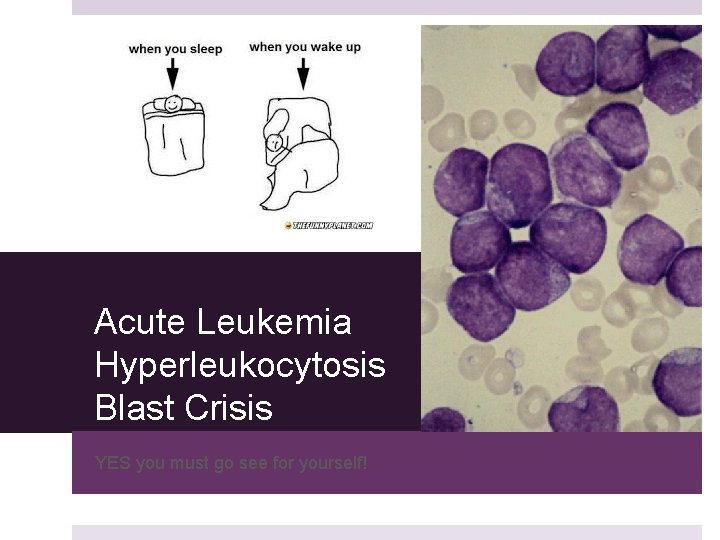
Acute Leukemia Hyperleukocytosis Blast Crisis YES you must go see for yourself!

Hyperleukocytosis Acute Leukemia with white count >100 K Leukostasis Hyperleukocytosis with symptoms Intravascular accumulation/adhesion of blasts malperfusion Ganzel et al Blood Reviews 2012

Leukostasis Signs and Symptoms: Pulmonary: dyspnea, hypoxia, infiltrates on CXR CNS: confusion, lethargy, stupor, HA vision changes, retinal vein Fever Extremities, renal dysfunction Santis et al, Journ Clin Apher 2011

Treatment: STAFF supervised Minimize transfusions Emergency – judicious phlebotomies Hydroxyurea Ok to start at diagnosis Zuckerman et al. Blood; 120 (10) Sep 6, 2012.

Leukopheresis Use of leukopheresis is a matter of debate. It has not been shown to provide early or long-term clinical benefit. 1 Apheresis guidelines name it a category 2 (i. e second line) and grade 1 b (strong) recommendation. It can be attending or institution-dependent. NOT for APL treatment, >100 k for AML and >300 K for ALL Usually requires 2 procedures that are 12 to 24 hours apart Goal WBC <50 K 1. Rollig et al. Blood 2015; 125: 3246 -52. 2. Schwartz et al. J Clin Apheresis 2016; 31: 149 -338.
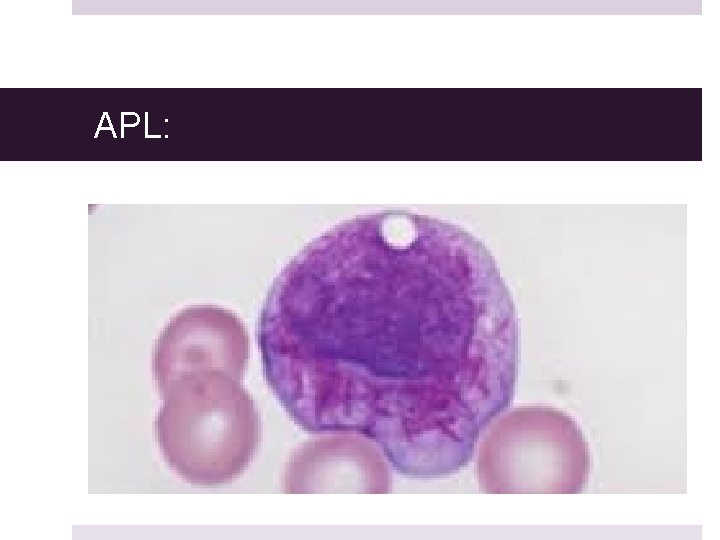
APL:

Take Home Get out of BED You NEED to recognized this quickly Come to the hospital LOOK at the SMEAR Evaluate your Patient Call YOUR STAFF
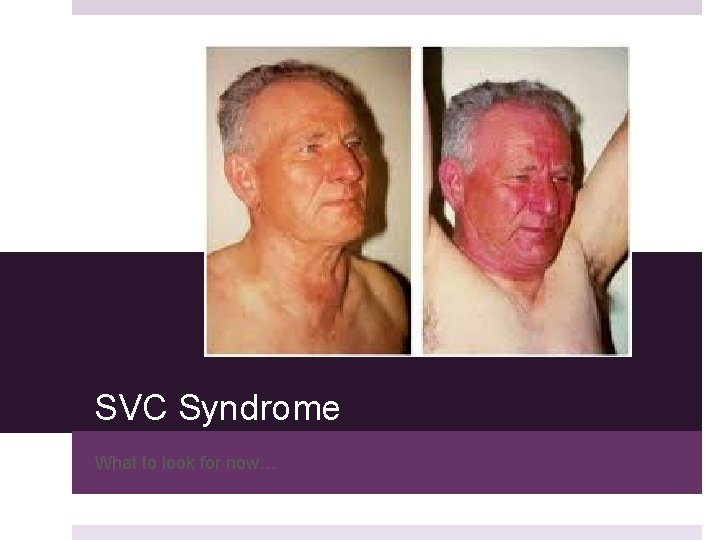
SVC Syndrome What to look for now…

Symptoms Facial edema, plethora Arm edema Distended neck veins, chest veins Visual symptoms Dyspnea, Cough, Hoarseness, Stridor Syncope, Headaches, Dizziness, Confusion, Obtundation

Treatment Supportive / Symptom Management Elevate head Corticosteroids – debatably helpful. Biopsy first if concerned for lymphoma. Think about thrombotic etiology – thrombolysis/anticoagulation. IR helpful: venogram, thrombolysis, stents for emergency. Radiation – for lung etiology Chemotherapy (need tissue, SCLC, lymphoma, germ-cell very chemo-sensitive) Lewis et al. CA Cancer J Clin 2011; 61: 287 -314.

Crit Care Med 2012

Recap: Diagnosis REQUIRED Get the tissue SLCL, Germ Cell, Lymphoma chemotherapy NSCLC Radiation Temporize / supportive care

Consumptive Coaguloapathies Thrombocytopenia When to drive in….

Thrombocytopenia Platelet level < 150 K Think about spontaneous bleeding Around < 10 -20 K Think about secondary causes – HIV, Hep C, cirrhosis/splenomegaly, infections/sepsis, drugs, Et. OH Look for other cytopenias – marrow infiltration (e. g. leukemia, lymphoma, metastatic carcinoma, HLH, PNH), aplastic anemia Isolated thrombocytopenia: Plt clumping, ITP, TTP/HUS, DIC, HIT, HELLP/pregnancy
Hemolysis Concurrent hemolysis with thrombocytopenia, think consuption/microangiopathic hemolytic anemia (MAHA)! Must look at smear: schistocytes? DIC – coags/fibrinogen will be off. TTP/HUS – all you need is MAHA + thrombocytopenia without readily apparent cause to call the path lab plasmapheresis
Hemolysis Labs Ensure decline in RBC’s Base line, bleeding etc. Haptoglobin LDH Bilirubin D-dimer, PTT, fibrinogen Schistocytes?
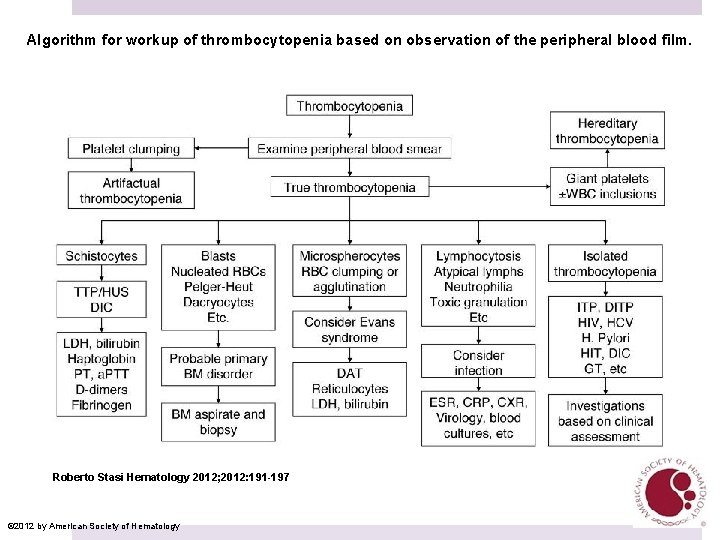
Algorithm for workup of thrombocytopenia based on observation of the peripheral blood film. Roberto Stasi Hematology 2012; 2012: 191 -197 © 2012 by American Society of Hematology
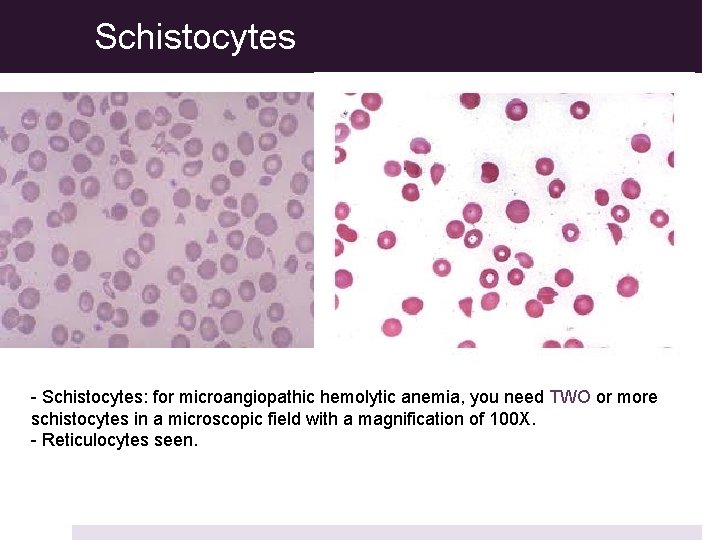
Schistocytes - Schistocytes: for microangiopathic hemolytic anemia, you need TWO or more schistocytes in a microscopic field with a magnification of 100 X. - Reticulocytes seen.
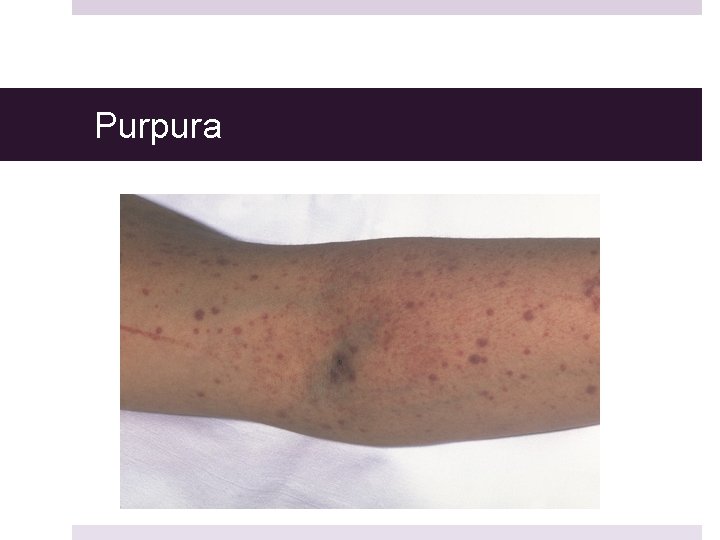
Purpura
TTP Consumption of platelets Lack of ADAMTS 13 enzyme activity High Mortality if not treated Plasmapheresis Follow the LDH

DIC LABS Low Fibrinogen (if early in course, it may not be) High D-dimer Smear PT/PTT prolonged Treatment Fix / optimize underlying issue Supportive care fibrinogen >150 (cryoprecipitate) and FFP for prolonged PT/PTT Platelets > 20 K

Isolated Thrombocytopenia Secondary Treat underlying condition ITP – no other cytopenias, Dx of exclusion (HIV, Hep C, smear is all you need before trial of steroids) Primary treatment Dexamethasone 40 mg x 4 days now proven better than prednisone, best results if you do 3 cycles every 2 -4 wks. 1, 2 IVIg 1 g/kg (may repeat for two daily doses) – if refractory to steroids or when quicker responses are needed. If actively bleeding, okay to transfuse. Refractory: Rituxan, splenectomy, thrombopoetin receptor agonists. 1. 2. Wei et al. Blood 2016; 127: 296 -302. Mazzucconi et al. Blood 2007; 109: 1401 -7.

Neutropenic Fever Yes – this one is ours… well chemotherapy related
Neutropenic Fever Neutropenia >101 F ANC < 500 cells Sustained >100. 4 over 1 hour ANC <1000 with further decline anticipated In select patients AML – watch out – their neutrophils are the problem!!! Most chemotherapy protocols ANC nadir 7 -10 days

Management GNR Coverage Cefepime 2 Gm Q 8 hours (Cat 1 NCCN V 2. 2015) Imipenem/cilastatin (cat 1) Meropenem (cat 1) Zosyn (Cat 1) Must be started within 1 hour of presentation GET CULTURES Think about Vancomycin use Antibiotic prophylaxis if anticipate neutropenia > 5 days.
- Slides: 61