Inflammatory and Valvular Heart Diseases Rheumatic Fever and



















































- Slides: 62

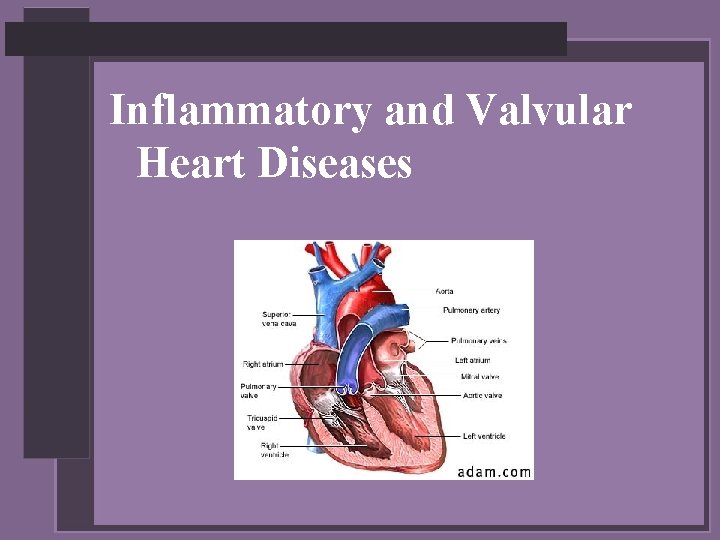
Inflammatory and Valvular Heart Diseases

Rheumatic Fever and Heart Disease • Rheumatic Fever - inflammatory disease of heart potentially involving all layers • Systemic • Abnormal immune response to group A beta hemolytic strep (“strep throat”) • Transmission to heart via lymphatic channels Most common cause of valvular heart disease

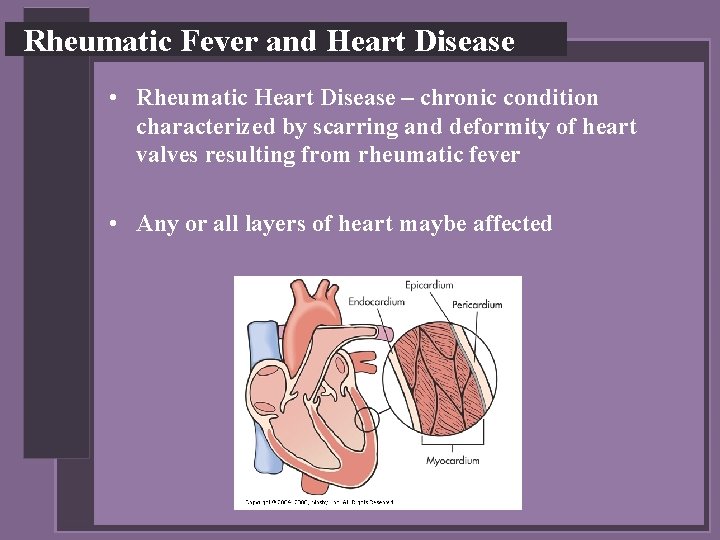
Rheumatic Fever and Heart Disease • Rheumatic Heart Disease – chronic condition characterized by scarring and deformity of heart valves resulting from rheumatic fever • Any or all layers of heart maybe affected

Rheumatic Fever and Heart Disease • Rheumatic endocarditis (most serious) • Erosion and swelling of valves (thickening) • Vegetations • Stenosis/Regurgitation • Rheumatic Myocarditis • Nodules and fibrin deposits loss of contractile power CHF • Rheumatic Pericarditis • Fibrinous Exudate and pericardial effusion

Rheumatic Fever and Heart Disease • Nursing Assessment • • Previous history of rheumatic fever Socioeconomic class Fever Cardiovascular (tachycardia; pericardial friction rub; distant heart sounds; murmurs) • Neurological: chorea • Skin: subcutaneous nodules and erythema marginatum • Musculoskeletal: Polyarthritis

Rheumatic Fever and Heart Disease • Primary Prevention • Detection and treatment of strep throat • Secondary Prevention • Prophylactic antibiotics to prevent recurrent ARF

Rheumatic Fever and Heart Disease v v Acute Intervention Antibiotics Rest Control Fever Anti-Inflammatories

Infective Endocarditis • Infection of the inner layer (endocardium) of the heart that usually affects the cardiac valves • Was almost always fatal until development of penicillin • 5, 000 -8, 000 cases diagnosed in U. S. each year

Classification • Subacute form • • • Longer clinical course Insidious onset Streptococcus bovis or viridians Staphylococcus epidermidis HACEK group

Classification • Acute form • Shorter clinical course • Rapid onset • Causative organism more virulent • Streptococcus pneumoniae • Staphylococcus aureus • Streptococcus groups A, B, C • Fungi

Etiology and Pathophysiology • Vegetations • Fibrin, leukocytes, and microbes • Adhere to the valve or endocardium • Embolization of portions of vegetations into circulation

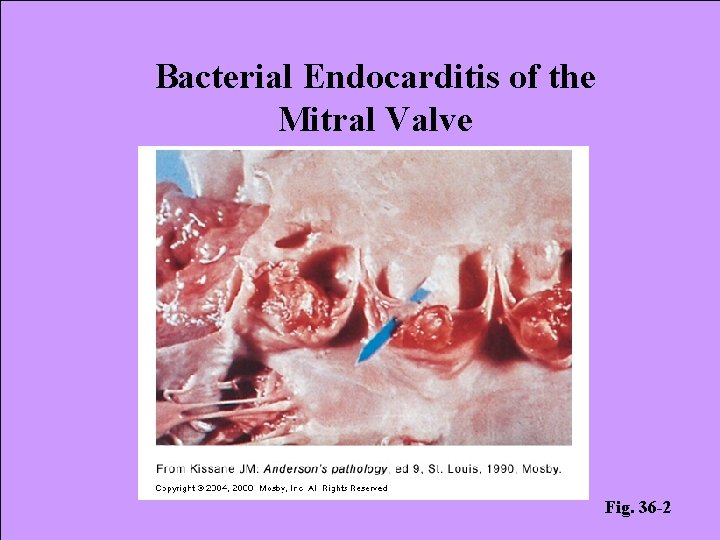
Bacterial Endocarditis of the Mitral Valve Fig. 36 -2

Etiology and Pathophysiology • Left-sided more common with bacterial infections and underlying heart disease • Right-sided lesions usually caused by IV drug abuse

Etiology and Pathophysiology • Risk Factors: • Cardiac Conditions (blood flow turbulence allows pathogen to infect previously damaged valves or other surfaces) • Rheumatic heart disease • Prosthetic valves • Aging • IV drug abuse • Invasive Medical and Dental Procedures • UTI, skin/wound infections

Clinical Manifestations • • • Nonspecific Fever occurs in 90% of patients Chills Weakness Malaise, Fatigue Anorexia

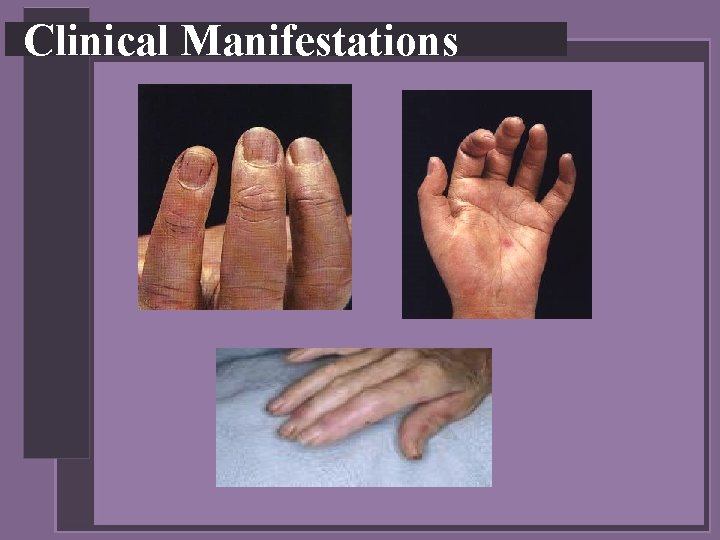
Clinical Manifestations • Vascular manifestations • • Splinter hemorrhages in nail beds Petechiae Osler’s nodes on fingers or toes Janeway’s lesions on palms or soles

Clinical Manifestations

Clinical Manifestations • Murmur in 80% of cases • CHF • in up to 80% with aortic valve endocarditis • 50% with mitral valve endocarditis • Manifestations secondary to embolism

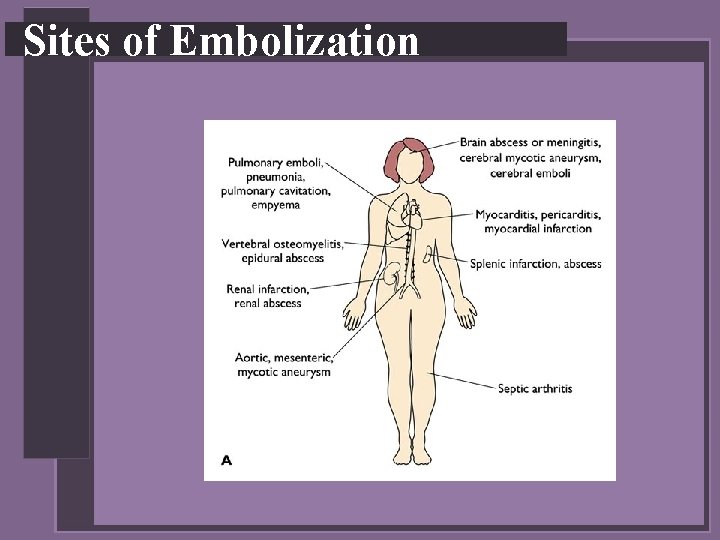
Sites of Embolization

HISTORY • Recent dental, urologic, surgical, or gynecologic procedures • Heart disease • Recent cardiac catheterization • Skin, respiratory, or urinary tract infections

Diagnostic Studies • Labs • Blood cultures • Echocardiography (detects valvular vegetations, abscesses) • Chest x-ray

Collaborative Care • Prophylactic treatment for patients having: • Removal of drainage of infected tissue • Indwelling pacemakers • Renal dialysis • Ventriculoatrial shunts

Collaborative Care • Antibiotic administration • Monitor antibiotic serum levels • Antipyretics • Subsequent blood cultures • REST • Valve repair/replacement

Nursing Assessment • Subjective • History of valvular, congenital, or syphilitic cardiac diseases • Previous endocarditis • Staph or strep infection • Immunosuppressive therapy

Nursing Assessment • Recent surgical procedures or invasive procedures • IV drug abuse • Weight changes • Chills • Diaphoresis

Nursing Assessment • • Bloody urine Exercise intolerance Generalized weakness Fatigue Cough Dyspnea on exertion Night sweats Chest, back, abdominal pain

Nursing Assessment • Objective • • • Olser’s nodes Splinter hemorrhages Janeway’s lesions Petechiae Clubbing

Nursing Assessment • • Tachypnea Crackles Arrhythmias Leukocytosis Increased ESR and cardiac enzymes Positive cultures ECG showing chamber enlargement

Nursing Diagnoses v. Decreased cardiac output v. Activity intolerance v. Ineffective health maintenance

Acute Pericarditis • • Caused by inflammation of pericardial sac Etiologies: Infectious vs Non-Infectious S&S: dyspnea, CP, pericardial friction rub Complications • Pericardial effusion • Cardiac tamponade • Treatment • • • Antibiotics NSAIDS Corticosteroids Positioning head at 45 degree angle Pericardiocentesis

Valvular Heart Disease

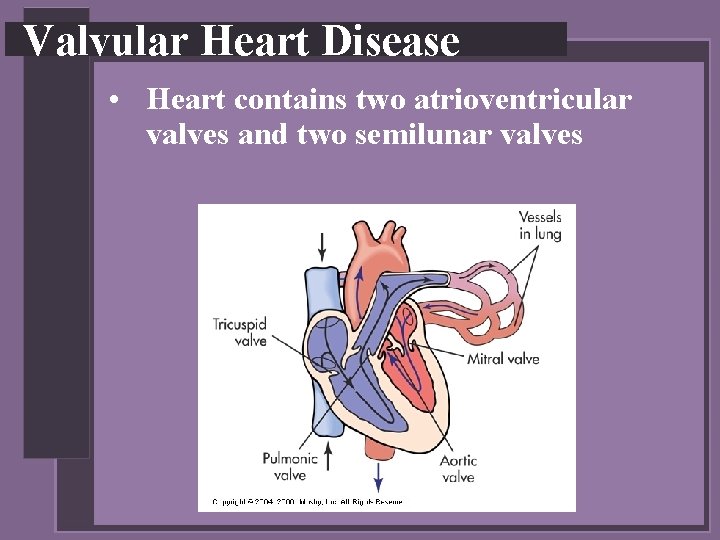
Valvular Heart Disease • Heart contains two atrioventricular valves and two semilunar valves

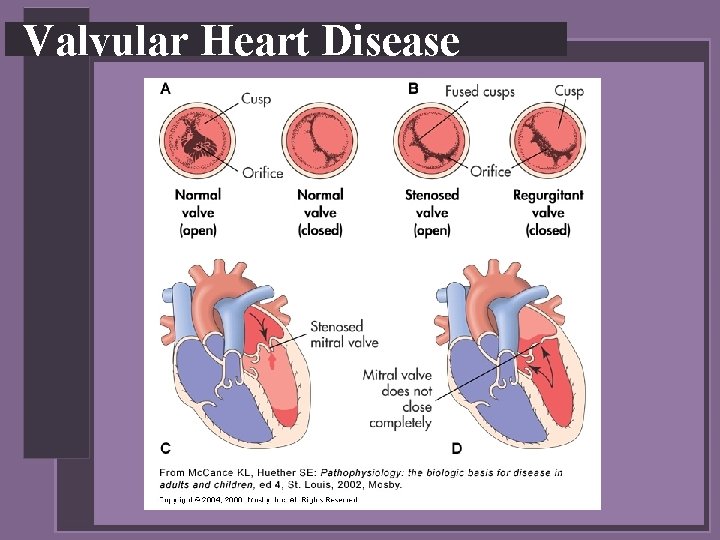
Valvular Heart Disease • Types of valvular heart disease depends on: • Valve or valves affected • Two types of functional alterations • Stenosis • Regurgitation

Valvular Heart Disease • Stenosis • • Valve orifice is restricted Impending forward blood flow Creates a pressure gradient across open valve Degree of stenosis reflected in pressure gradient differences • Regurgitation • • Incomplete closure of valve leaflets Results in backward flow of blood

Mitral Valve Stenosis • Due to rheumatic heart disease • Causes scarring of valve leaflets and chordae tendineae • Contractures develop with adhesions between commissures of the leaflets • Stenotic mitral valve assumes funnel shape due to thickening and shortening of valve structures

Mitral Valve Stenosis • Pathophysiology: • Incomplete emptying of LA Increased LA pressure LA dilatation and hypertrophy • Increased LA pressure Elevated pulmonary pressure pulmonary congestion • Incomplete emptying of LA insufficient volumes to ventricles decreased C. O. • Afib is common risk of embolism

Clinical Manifestations • Dyspnea • Occasionally accompanied by hemoptysis • Primary symptom because of reduced lung compliance • • Palpitations from atrial fibrillation Fatigue Opening snap Low-pitched rumbling diastolic murmur Chest pain Seizures (from emboli) Stroke • Emboli can arise from stagnant blood in left atrium

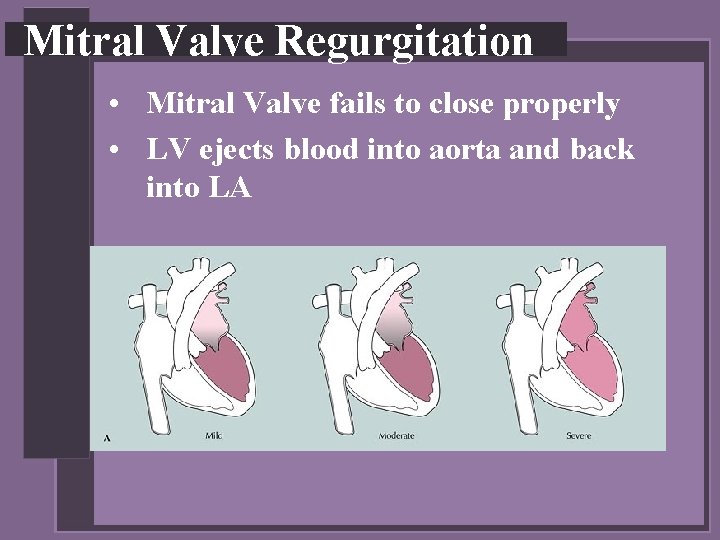
Mitral Valve Regurgitation • Mitral Valve fails to close properly • LV ejects blood into aorta and back into LA

Mitral Valve Regurgitation • Majority of cases attributed to: • MI (MI with left ventricular failure places patient at risk for rupture of chordae tendineae) • Chronic rheumatic heart disease • Isolated rupture of chordae tendineae • Mitral valve prolapse • Ischemic papillary muscle dysfunction • Infectious endocarditis

Mitral Valve Regurgitation • Acute Onset (e. g. papillary dysfunction due to M. I. ) • Backward flow increased LA pressure Increased Pulmonary Pressure Pulmonary Edema • Chronic Onset • Backward flow LA dilates and hypertrophies Increased pulmonary pressures pulmonary congestion right sided failure

Mitral Valve Regurgitation Clinical Manifestations • Asymptomatic for years until development of some degree of left ventricular failure • Initial symptoms include: • Weakness • Fatigue • Dyspnea that gradually progress to orthopnea, paroxysmal nocturnal dyspnea, and peripheral edema

Aortic Valve Stenosis • Usually discovered in childhood, adolescence, or young adulthood • Those seen later in life usually have aortic stenosis from rheumatic fever or senile fibrocalcific degeneration of a normal valve

Aortic Valve Stenosis • Results in obstruction of flow from LV to aorta during systole • Effect is left ventricular hypertrophy and increased myocardial oxygen consumption because of increased myocardial mass • Leads to reduced CO and pulmonary hypertension

Aortic Valve Stenosis Clinical Manifestations • Symptoms of angina pectoris • Syncope • Heart failure • Occurs when valve orifice is 1/3 normal size

Aortic Valve Stenosis • Poor prognosis when experiencing symptoms and valve obstruction is not relieved • Why would Nitroglycerine be contraindicated with aortic valve stenosis?

Aortic Valve Regurgitation • May result from disease of aortic valve leaflets, aortic root, or both • Caused by: • Bacterial endocarditis • Trauma • Aortic dissection • Constitutes life-threatening emergency • Chronic aortic regurgitation results from: • • Rheumatic heart disease Congenital bicuspid aortic valve Syphilis Chronic rheumatic heart conditions

Aortic Valve Regurgitation • Physiologic consequence: • Retrograde blood flow from ascending aorta to left ventricle • Elevated LV pressures • LV dilatation and hypertrophy • Results in volume overload

Tricuspid Valve Disease • Tricuspid valve stenosis • Seen in IV drug users • Right atrial output is obstructed • Results in right atrial enlargement and elevated systemic venous pressure

Tricuspid Valve Disease Clinical Manifestations • • Peripheral edema Ascites Hepatomegaly Murmur

Collaborative Care • Drug therapy • Digitalis • Diuretics • Antiarrhythmics • b-blockers • Anticoagulants • Low-sodium diet

Collaborative Care • Percutaneous transluminal balloon valvuloplasty to split open fused commissures • Surgical therapy for valve repair • Annuloplasty • Valvuloplasty • Commissurotomy • Valve Replacement • Mechanical Vs. Biological

Nursing Assessment • Objective • • • Fever Diaphoresis Peripheral edema Crackles Wheezes Abnormal heart sounds Ascites Hepatomegaly Cardiomegaly Valve calcification Pulmonary congestion on x-ray

Nursing Assessment • Diagnostic Tests: • Calcification or vegetation of leaflets or prolapse • Chamber enlargement • Arrhythmias • Conduction deficits on ECG

Nursing Implementation • Prevention of rheumatic valvular disease by diagnosing and treating streptococcal infection and providing prophylactic antibiotics for patients with history • Patient with history of endocarditis must also be treated with prophylactic antibiotics

Nursing Implementation • • • Teach when to seek medical treatment Design activity to patient’s limitations Discourage smoking Avoid strenuous activity Nursing assessment to monitor effectiveness of medications

Nursing Implementation • Medic Alert bracelet • Teach importance of completing antibiotic regimen • Teach drug side effects • INR for anticoagualtion therapy • Follow-up care

Case Study • Patient Profile: • Mrs. S. , a 54 -year-old Hispanic woman, is admitted to the hospital for valvular heart disease. • Subjective Data • Was told she had streptococcal throat infection as a child • Was diagnosed 10 years ago with rheumatic heart disease • Has shortness of breath at rest; cannot get out of bed without becoming dyspneic • Takes digoxin (0. 25 mg once a day) • Objective Data • Physical Examination • • Ankle edema Irregular pulse Crackles at lung bases Murmurs of mitral stenosis, mitral insufficiency, and aortic insufficiency • Diagnostic Studies • Chest x-ray and ECG indicate enlarged left atrium

Case Study: Question #1 • Explain the cause of Mrs. S. ’s valvular heart disease. What valves are most likely to become involved with rheumatic heart disease?

Case Study: Question #2 • Differentiate between the characteristics of mitral stenosis and mitral regurgitation.

Case Study: Question #3 • What other conservative treatment measures might be initiated for Mrs. S. (in addition to digoxin? )

Case Study: Question #4 • On the basis of the assessment data provided, write one or more nursing diagnoses.

Case Study: Question #5 • What are important nursing measures for Mrs. S. ?