Rheumatic Fever By Dr alazar W Rheumatic Fever

Rheumatic Fever By: Dr alazar W.

Rheumatic Fever • is a non-suppurative acute inflammatory complication of group A streptococcal (GAS) pharyngeal infections, causing chronic progressive damage to the heart & its valves • It is a multisystem disease resulting from delayed autoimmune response to GAS infection • characterized by an exudative and proliferative inflammatory lesion of the connective tissue • It involves: the heart, joints, CNS, skin, blood vessels and subcutaneous tissue 3/8/2021 Dr. Alazar W.

Epidemiology • Even though the overall incidence of RF and RHD in developed countries has sharply declined, RF is still the commonest cause of heart disease in developing countries. • In those developing countries > 50% of heart disease is accounted for rheumatic heart disease (RHD) • 95% of ARF cases & RHD deaths occur in developing countries • The annual incidence of ARF among school children < 1 per 100, 000 (Developed), 150 per 100, 000 (Developing) • With the peak age of 5 -15 years, and Rare >30 yrs 3/8/2021 Dr. Alazar W.

Cont. • In adults the risk of developing RF is about 3% following GAS Pharyngitis (0. 3– 3% of individuals with GAS pharyngitis develop RF) • The high attack rate of GAS pharyngitis in families, institutions and military recruits is the result of contact among susceptible persons living closely • Risk factors: low socioeconomic status with associated over crowded living condition. • RF is not associated with streptococcal skin infection (pyoderma) 3/8/2021 Dr. Alazar W.

RHD Prevalence 15 - 19 million (worldwide) F > M Peak: 25 - 40 years 3/8/2021 Dr. Alazar W.

Pathophysiology • ARF is a sequele of a previous GAS infection, usually of the upper respiratory tract. • Rheumatogenicity of GAS is important factor as • Not all GAS pharyngitis is associated with development of RF • One beta-streptococcal serotype (e. g. M types 3, 5, 18, 19, 24) is linked directly to ARF. • Shares structural homology with myocardial cells (myosin, tropomyosin, keratin and laminin) • RF follows pharyngitis within the interval of 2 -3 wks 3/8/2021 Dr. Alazar W.

v The mechanism is not clear, but the following are proposed ones: • Dysfunction of the immune Response • Antigenic Mimicry üSimilarity b/n the carbohydrate moiety of GAS and glycoprotein of heart valve üMolecular similarity b/n some Streptococcal antigens and sarcolema or other moiety of myocardial cells. 3/8/2021 Dr. Alazar W.

Clinical Manifestation • ARF is associated with 2 distinct patterns of presentation • The 1 st is sudden onset • typically begins as polyarthritis 2 -6 weeks after pharyngitis, and it is usually characterized by fever and toxicity • The 2 nd is insidious or subclinical and the initial abnormality is mild carditis. • Age at onset influences the order of complications. • Younger children tend to develop carditis first, while • older patients tend to develop arthritis first. 3/8/2021 Dr. Alazar W.

Diagnosis • Requires a high index of suspicion • Relies on - presence of a combination of typical CF, evidence of preceding GAS infection and exclusion of other dx • No definitive diagnostic laboratory test is available • Clinical examination remains the basis of a Dx • Jones criteria is still a universal standard for the dx of RF It is reviewed and modified by the AHA & WHO 3/8/2021 Dr. Alazar W.

1) Carditis: ≈ in 40 -60% of patients. The only abnormality that can cause permanent damage and may manifest as: a) New murmur (early MR ± AR, lately MS ± AS ) b) Cardiomegaly c) CHF d) Pericarditis, which resolve without squeale e) Valvular damage: is the hallmark of rheumatic carditis, where mitral and aortic valves are commonly affected (MV > AV >>TV) 3/8/2021 Dr. Alazar W.

Cont. v. Recurrent episodes → leaflet thickening, scarring, calcification and valvular stenosis v. Healing of valvulitis will lead into fibrous thickening and adhesion progressive valvular damage v. But, about 80% of mild valvulitis would resolve. v. There is increased risk of developing infective endocarditis on a damaged valve 3/8/2021 Dr. Alazar W.

Cont. 2) Migratory polyarthritis: ≈ in 60 -75% of cases and involves many joints at a time. • Asymmetric + Migratory • larger joints are mainly affected. • lasts about 1 month without Rx • inflamed joint, tenderness out of proportion to findings • leaves no pathological / functional residue 3/8/2021 Dr. Alazar W.

3) Subcutaneous nodules: ≈ in 10% of patients • firm painless nodules on the extensor surfaces or on bony prominences of wrists, elbows, and knees. ümobile üLasts from days to 3 wks üusually associated with carditis üare not pathognomonic of RF 3/8/2021 Dr. Alazar W.

Cont. 4) Erythema marginatum: in ≈ 5% of cases • Bright pink papule / macular rash • Clear centrally, a serpiginous spreading edge • Temporary • Blanches with pressure • Trunk >> proximal limb (never on the face) • Migratory pattern. • Leaves no residual scar • associated with carditis 3/8/2021 Dr. Alazar W.

5) Sydenham’s chorea: a characteristic movement disorder that occurs in 5 -10% of cases • It manifest as: rapid, purposeless, involuntary movements in the extremities & face, Facial ticks & grimaces, Darting tongue, Disappear with sleep § Onset may be delayed for several months to years § Resolves completely (6 weeks) 3/8/2021 Dr. Alazar W.

In general: üArthritis is often the only major manifestation in adolescents & adults üCarditis & chorea: less common in older age groups üPolyarthritis & Sydenham’s chorea: never occur simultaneously üArthritis & Carditis: frequently coexist during an ARF episode with an inverse relationship b/n the severity of arthritis and carditis 3/8/2021 Dr. Alazar W.

Investigations • CBC – Leukocytosis, mild anemia • Blood cultures (if febrile) • ECG: P-R interval prolongation is seen in 25% of all cases • CXR (if carditis ) • Isolate GAS via throat swab culture which has 20 -40% yield. • Acute phase reactants: elevated ESR and CRP • Streptococcal antibody tests: reveal preceding infection üASO titer: positive in 80% of cases üAnti DNAase β and Anti hyaluronidase is positive in 95% of cases 3/8/2021 Dr. Alazar W.

Jones Criteria Major Criteria Minor Criteria Supportive evidence of recent GAS infection Carditis Migratory polyarthritis Subcutaneous nodules Erythema marginatum Sydenham’s Chorea Fever Arthralgia Elevated ESR/CRP Prolonged PR interval A positive throat culture or rapid antigen test for GAS; and/or elevated or rising ASO or other streptococcal antibody v. Diagnosis of ARF requires Supportive evidence + 2 major OR Supportive evidence + 1 major + 2 minor 3/8/2021 Dr. Alazar W.

Management General Measures • Hospital admission for - Confirming the Dx & instituting treatment - Educating patients and family - Monitoring for the onset of carditis • Bed–rest Until arthritis subsides At least 4 wks for pts with carditis • Pts with chorea must be placed in a protective env’t • NO treatment that has been proven to alter the likelihood of developing or the severity of RHD 3/8/2021 Dr. Alazar W.

Treatment 1. Treat GAS infection v. All pts with ARF should be given appropriate antibiotic, whether or not pharyngitis is present at the time of Dx v. Eradication of GAS Ø Avoids repetitive exposures to streptococcal antigens üAmpicillin 500 mg, PO, QID or üAmoxicillin 500 mg, PO, TID for 10 days or üBenzathin penicillin 1. 2 million IU IM stat (for > 27 kg) or üErythromycin 500 mg, PO, QID for 10 days (for penicillin allergy) 3/8/2021 Dr. Alazar W.

2. Treat manifestations q. For severe Carditis § Steroids- may reduce the acute inflammation and result in more rapid resolution of failure • Prednisolone: 60 -80 mg/day (1– 2 mg/kg/d), to be tapered as patient improves. Duration: 3 wks (max. ) • Start Aspirin during tapering phase to be given for 4 -6 wks But, both have no influence on the future development of VHD 3/8/2021 Dr. Alazar W.

Cont. q For Arthritis, arthralgia, fever • ASA (the DOC) 2 gm, PO, QID for 4 -6 weeks q For Sydenham’s chorea • In majority of the cases it is self-limiting • But in symptomatic patients benzodiazepines (diazepam) or phenothiazines (haloperidol) may be helpful in controlling Sxs • Mild - Rest & quiet room • Severe - Carbamazepine or Sodium valproate Medication should be continued for 1– 2 wks after Sxs subside 3/8/2021 Dr. Alazar W.

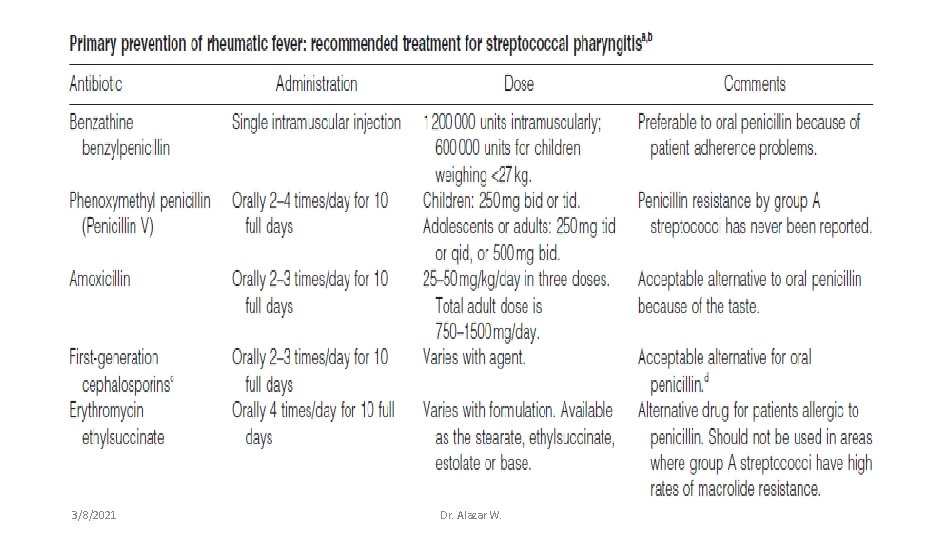
3. Prevention Primary Prevention A. Eliminate major risk factors for GAS infection Overcrowding and unhygienic conditions B. Primary prophylaxis - The mainstay of primary prevention - Proper identification & adequate antibiotic Rx of GAS tonsilopharyngitis to prevent initial attack of RF. - If commenced within 9 days of sore throat onset, it will prevent almost all cases of ARF - Best accomplished by clinical judgment & Dx tests. 3/8/2021 Dr. Alazar W.
3/8/2021 Dr. Alazar W.

Secondary Prophylaxis: Rationale • Prior attack of RF increases risk of recurrence after subsequent GAS pharyngitis - The risk of ARF after the first attack is 0. 3 -3% - The risk of ARF after subsequent infection is 25 -75% • Recurrent carditis tends to be more severe. • Most effective strategy to avoid the mortality & chronic cardiac disability • GAS infection need not be symptomatic to trigger a recurrence • Recurrence can occur even when a symptomatic infection is treated optimally 3/8/2021 Dr. Alazar W.

Secondary Prophylaxis… • B. penicillin G, IM every 4 wks OR • B. penicillin G, IM every 2 to 3 wks In populations where incidence of RF is high Recurrent RF despite adherence to a regimen of Q 4 wks • Prophylactic antibiotics should be initiated immediately at the end of therapeutic antibiotic course 3/8/2021 Dr. Alazar W.

Duration of Secondary Prophylaxis Category of Patient Duration of Prophylaxis RF without carditis For 5 years after the last attack or upto 21 years of age RF with carditis but no residual valvular disease For 10 years after the last attack, or upto 21 years of age RF with persistent valvular disease For 10 years after the last attack, or 40 years of age or Sometimes lifelong 3/8/2021 Dr. Alazar W.

THANK U All!!! 3/8/2021 Dr. Alazar W.
- Slides: 28