aminimmums ac ir ASTHMA AND PREGNANCY CASE HISTORY




























































- Slides: 65

aminim@mums. ac. ir ASTHMA AND PREGNANCY

CASE HISTORY

A 20 yr old lady presented with Hx of cough and dyspnea for 6 months 2 weeks of drug discontinuation 1 week cough, sputum and dyspnea She is 3 mo pregnant She is concerned about her chest disease during pregnancy

Is it really asthma? Why me? I had no family history. Does pregnancy cause my asthma to be exacerbated? Can my asthma be cured? Can moisturizers help me to improve? How does asthma affect my fetus? Are asthma drugs risky for my fetus? Is my child more prone to asthma? Can heartburn cause my asthma? Should I get flu shot? What should I do in the case of asthma attack? Can I do NVD for termination of pregnancy?

IS IT REALLY ASTHMA?

Recurrent episodes of wheezing Troublesome cough at night Cough or wheeze after exercise Cough, wheeze or chest tightness after exposure to airborne allergens or pollutants Colds “go to the chest” or take more than 10 days to clear


Pregnancy dyspnea Increased tidal volume Decreased ERV and FRC Intact FEV 1 Less than normal PCo 2 Above normal PO 2 The presence of cough and wheezing suggests asthma

WHY ME?

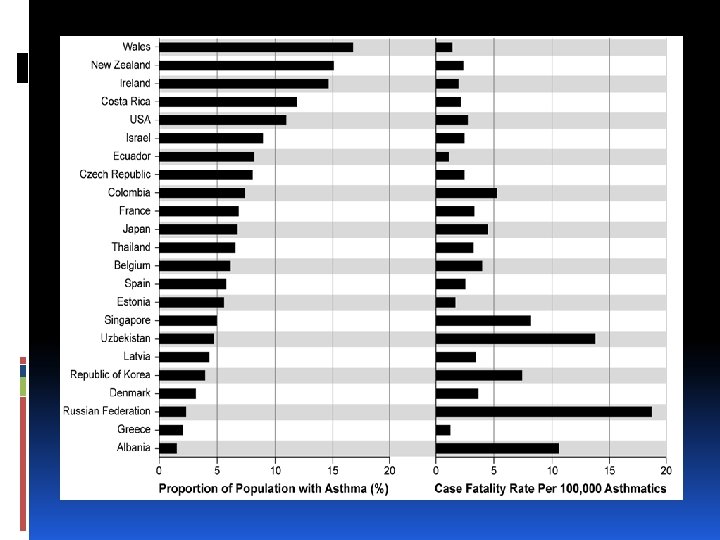
Asthma is a common disease Even more than diabetes mellitus In some countries 1 out of every 4 children has asthma


Asthma affects 4 to 8% of all pregnant women

I HAD NO FAMILY HISTORY

Asthma occurs more commonly in those with atopic history In themselves or Their 1 st degree relatives A person with allergic rhinitis has 5 times more chance of asthma

Asthma is a polygenic disease Asthma occurs in a genetically susceptible person, who exposed to specific etiologic factors It occurs more common in identical twins

DOES PREGNANCY CAUSE MY ASTHMA TO BE EXACERBATED?

Pregnant women have different courses of their asthma 1/3 aggravate 1/3 improve 1/3 does not change

The most common cause of asthma exacerbation Discontinuation of drugs Viral infections Well controlled asthma has favorable outcome in pregnancy

Poor controlled asthma has been associated with 15 to 20 % increase in Preterm delivery Preeclampsia Growth retardation Need for C/S Maternal morbidity Maternal mortality

These risks are increased 30 to 100 % those with more severe asthma Asthma is not associated with risk of congenital malformations

What is “well control”? No (or minimal) daytime symptoms No limitations of activity No nocturnal symptoms No (or minimal) need for rescue medication Normal lung function No exacerbations

In pregnant asthmatics you should confirm control by Spirometry Monthly Peak flow metry Twice daily Upon awakening After 12 hr


FEV 1 < 80% in pregnancy associated with poor pregnancy outcomes moderate to severe asthmatics Serial ultrasound examination Early in pregnancy Regularly after 32 wk After an asthma exacerbation

CAN MY ASTHMA BE CURED?

Asthma is a chronic disease We have very few diseases with such a good response to therapy as asthma Quality of life improved markedly after treatment

ARE ASTHMA DRUGS RISKY FOR MY FETUS?

As asthma is an inflammatory disease limited to lung airways Treatment of this disease in a topical form is More effective Less harmful

You can choose one of these categories for your asthmatic patient Relievers Controllers

If you choose the 1 st one (reliever) You treat patient's symptom, but Relievers do not work on inflammation! Your patient is prone to Asthma attack Airway remodeling

If you choose the 2 nd one (controllers) You treat your patient's disease, and You can control inflammation You reduce the risk of Asthma attack Airway remodeling in your patient

Relievers (No anti-inflammatory action) Salbutamol Atrovent Controllers (Mainly anti-inflammatory) Inhaled corticosteroids LABA cromolyn Theophylline Leukotrene antagonists

When should I start controllers? >3 times/ wk day salbutamol need >3 times/ mo night awakening >3 times/ yr salbutamol prescription >3 times/ yr exacerbation >3 times/ yr short-term corticosteroid

Safety profile of common anti-asthma drugs Drug Safety Salbutamol Safe, inhaler (labor) Inhaled corticosteroids Category B, Budesonide Cromolyn Safe Theophylline Safe (5 -12 mcg/ml) ↓ clearance in 3 rdtrimester Cord blood level the same Load 5 -6 mg/kg Maintenance 0. 5 mg/kg/hr Delayed labor

Drug Safety LABA Not reassuring Adrenaline Not for asthma Systemic steroids Pre-eclampsia, GDM Atroent Leukotrene antagonists Prematurity, LBW Safe Ziluten not assessed Zafirleukast, monteleukast probably safe

Mild intermittent PRN Salbutamol Mild persistent Inhaled corticoteroid Moderate persistent Inhaled corticoteroid + LABA Severe persistent Inhaled corticoteroid + LABA

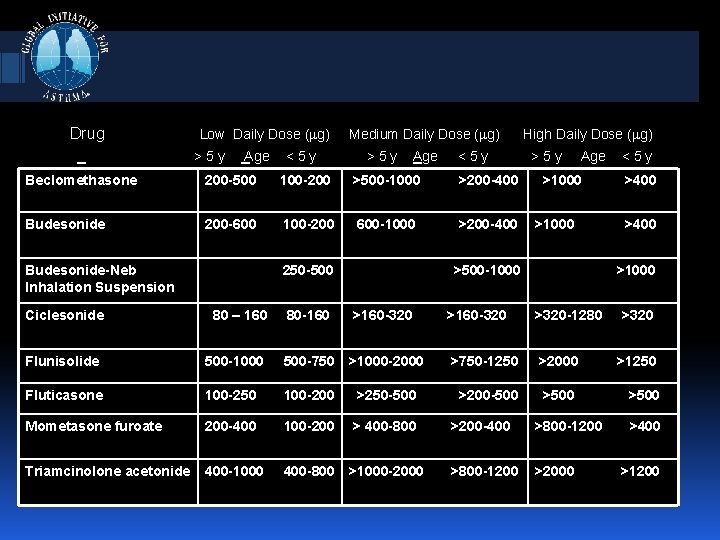
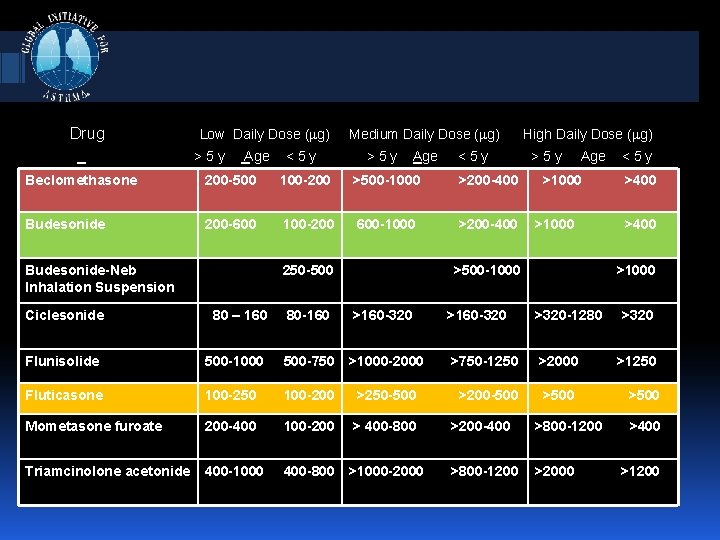
Drug Low Daily Dose ( g) >5 y Age <5 y Medium Daily Dose ( g) >5 y Age <5 y Beclomethasone 200 -500 100 -200 >500 -1000 >200 -400 Budesonide 200 -600 100 -200 600 -1000 >200 -400 Budesonide-Neb Inhalation Suspension Ciclesonide 250 -500 80 – 160 High Daily Dose ( g) >5 y Age >1000 >500 -1000 <5 y >400 >1000 80 -160 >160 -320 >320 -1280 >320 Flunisolide 500 -1000 500 -750 >1000 -2000 >750 -1250 >2000 >1250 Fluticasone 100 -250 100 -200 >250 -500 >200 -500 >500 Mometasone furoate 200 -400 100 -200 > 400 -800 >200 -400 >800 -1200 Triamcinolone acetonide 400 -1000 400 -800 >1000 -2000 >800 -1200 >2000 >400 >1200

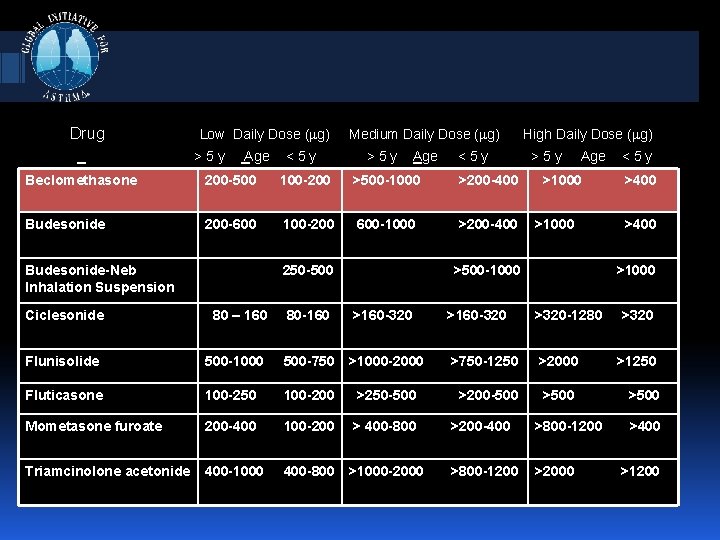
Drug Low Daily Dose ( g) >5 y Age <5 y Medium Daily Dose ( g) >5 y Age <5 y Beclomethasone 200 -500 100 -200 >500 -1000 >200 -400 Budesonide 200 -600 100 -200 600 -1000 >200 -400 Budesonide-Neb Inhalation Suspension Ciclesonide 250 -500 80 – 160 High Daily Dose ( g) >5 y Age >1000 >500 -1000 <5 y >400 >1000 80 -160 >160 -320 >320 -1280 >320 Flunisolide 500 -1000 500 -750 >1000 -2000 >750 -1250 >2000 >1250 Fluticasone 100 -250 100 -200 >250 -500 >200 -500 >500 Mometasone furoate 200 -400 100 -200 > 400 -800 >200 -400 >800 -1200 Triamcinolone acetonide 400 -1000 400 -800 >1000 -2000 >800 -1200 >2000 >400 >1200

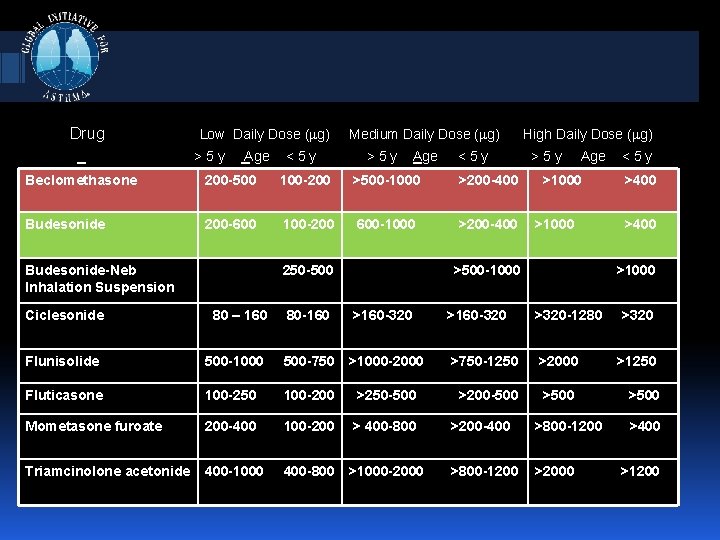
Drug Low Daily Dose ( g) >5 y Age <5 y Medium Daily Dose ( g) >5 y Age <5 y Beclomethasone 200 -500 100 -200 >500 -1000 >200 -400 Budesonide 200 -600 100 -200 600 -1000 >200 -400 Budesonide-Neb Inhalation Suspension Ciclesonide 250 -500 80 – 160 High Daily Dose ( g) >5 y Age >1000 >500 -1000 <5 y >400 >1000 80 -160 >160 -320 >320 -1280 >320 Flunisolide 500 -1000 500 -750 >1000 -2000 >750 -1250 >2000 >1250 Fluticasone 100 -250 100 -200 >250 -500 >200 -500 >500 Mometasone furoate 200 -400 100 -200 > 400 -800 >200 -400 >800 -1200 Triamcinolone acetonide 400 -1000 400 -800 >1000 -2000 >800 -1200 >2000 >400 >1200

Drug Low Daily Dose ( g) >5 y Age <5 y Medium Daily Dose ( g) >5 y Age <5 y Beclomethasone 200 -500 100 -200 >500 -1000 >200 -400 Budesonide 200 -600 100 -200 600 -1000 >200 -400 Budesonide-Neb Inhalation Suspension Ciclesonide 250 -500 80 – 160 High Daily Dose ( g) >5 y Age >1000 >500 -1000 <5 y >400 >1000 80 -160 >160 -320 >320 -1280 >320 Flunisolide 500 -1000 500 -750 >1000 -2000 >750 -1250 >2000 >1250 Fluticasone 100 -250 100 -200 >250 -500 >200 -500 >500 Mometasone furoate 200 -400 100 -200 > 400 -800 >200 -400 >800 -1200 Triamcinolone acetonide 400 -1000 400 -800 >1000 -2000 >800 -1200 >2000 >400 >1200

Choice of drug categories in pregnancy Category Drug of choice SABA Salbutamol LABA Salmetrol ICS Budesonide

CAN MOISTURIZERS HELP ME TO IMPROVE?

About 80 % of asthma patients have allergic (extrinsic) asthma Allergens, especially indoor allergens Mites Fungi Can cause asthma or allergic rhinitis to become worse Room humidity of > 50% speed up growth of mites and fungi

Avoidance from allergens, irritants and air pollution Is necessary for any asthmatic pregnant woman

Allergen immunotherapy can be continued during pregnancy But, should not be started for the 1 st time in a pregnant woman

IS MY CHILD MORE PRONE TO ASTHMA?

There is no association to mother asthma during fetal period and development of asthma in childhood period. Albeit asthma is a genetic disease

CAN HEARTBURN CAUSE MY ASTHMA?

Comorbid conditions in asthma Gastro-esophageal reflux disease (GERD) Allergic rhinitis (AD)

Be suspicious to GERD if Your asthmatic patient become poorly controllable Your asthmatic patient is worse at night Your asthmatic patient has symptoms when lies down Patient complains of GERD symptoms

Treatment of heartburn can improve asthma symptoms Continue anti GERD drugs for at least 2 -3 months

Be suspicious to AD if Your asthmatic patient complains of seasonal nose or sinus symptoms

Treat AD with Intranasal corticosteroids Antihistamines (2 nd generation in pregnancy) Allergen avoidance

SHOULD I GET FLU SHOT?

Influenza vaccination is necessary for Pregnant women with 2 nd and 3 rd trimester In cold months

WHAT SHOULD I DO IN THE CASE OF ASTHMA ATTACK?

Treatment of asthma attack is the same as non-pregnant woman Aggressive monitoring of mother and fetus Oxygen 3 -4 l/min by cannula Goal of Po 2 > 70 Sat > 95

Pco 2 > 35 mm. Hg Po 2 < 70 mm Hg Are abnormal during pregnancy IV fluid (dextrose) initially 100 ml/hour Seated position Fetal monitoring

Dosage of glucocorticoids is not different IV aminophylline NOT generally recommended IV Mg sulfate may be beneficial Concomitant hypertension Preterm contraction

Respiratory infections in asthmatic patients Usually viral If indicated in a pregnant woman I V Ceftriaxone Erythromycin

LABOR: C/S OR NVD?

No difference PG F 2 analogues should not be used in asthmatics for termination of pregnancy Morphine and meperidine should be avoided Fentanyl is an appropriate alternative

In the case of emergency cesarean section Epidural anesthesia is the favoured anesthesia Decreses O 2 consumption and minute ventilation If general anesthesia required Ketamine is preferred Ergot derivatives for pertiprtum bleeding, headache, should be avoided

Summary Careful assessment and monitoring Avoidance and controll of triggers Maintenance rather than symptomatic therapy Aggressive treatment of exacerbations

THANK YOU