BRONCHIAL ASTHMA Pharmacology and Clinical Aspects DEFINITION AB
BRONCHIAL ASTHMA Pharmacology and Clinical Aspects

DEFINITION AB Asthma bronchiale is chronic inflammatory disease of airways connected with bronchial hyperreactivity and totally or partially reversible obstruction of airways, which in the most cases dissapears spontaneously or with treatment.

AB 1. Extrinsic: often allergy and atopy 2. Intrinsic: non-alergic 10 -30% (more severe, adult-onset) daily symptom variability family history no smoking

ETIOPATOGENESIS • INFLAMMATION activation of mastocytes, macrophages, eosinophils, helper Th-lymfocytes => formed and released inflammatory mediators: histamine, leucotriens, prostaglandins, bradykinin bronchoconstriction, mucus secretion, plasma exudation and bronchial hyperreactivity, airway remodelation insufficient anti-inflammatory therapy => progressive destructive changes fixing of airway obstruction to emphysematous changes

Triggers of Symptoms and Exacerbations allergens factors of air pollution (including cigarette smoke) respiratory infections, particularly viral (RSV, rhinoviruses, influenza viruses, chlamydia) physical activity and hyperventilation (by osmotic processes) wheather changes food and drugs (ASA, NSAID, -blockers) emotional stress gastroesophageal reflux

CLINICAL SYMPTOMS OF AB Emphasis on early diagnosis management begins with right analysis of symptoms - to them belong: dyspnoe cough (in younger people may be the only symptom, mostly at night) chest tightness wheezing
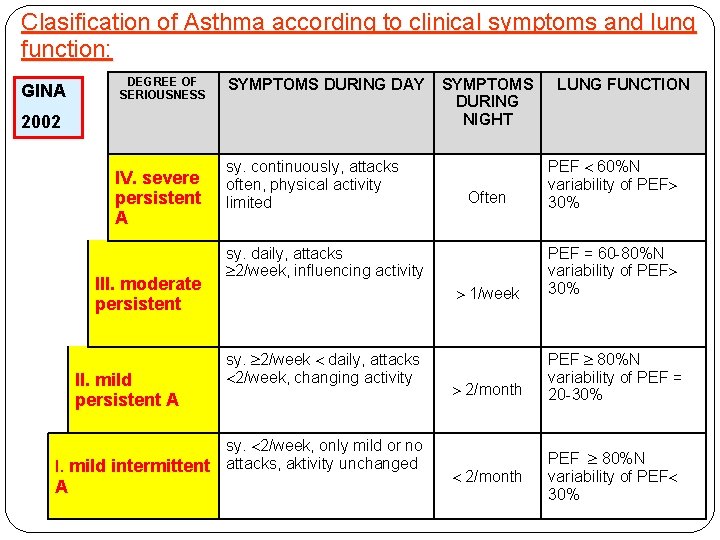
Clasification of Asthma according to clinical symptoms and lung function: GINA DEGREE OF SERIOUSNESS SYMPTOMS DURING DAY 2002 SYMPTOMS DURING NIGHT sy. continuously, attacks IV. severe often, physical activity persistent limited A III. moderate persistent II. mild persistent A sy. 2/week, only mild or no I. mild intermittent attacks, aktivity unchanged A Often PEF 60%N variability of PEF 30% 1/week PEF = 60 -80%N variability of PEF 30% 2/month PEF 80%N variability of PEF = 20 -30% sy. daily, attacks 2/week, influencing activity sy. 2/week daily, attacks 2/week, changing activity LUNG FUNCTION 2/month PEF 80%N variability of PEF 30%
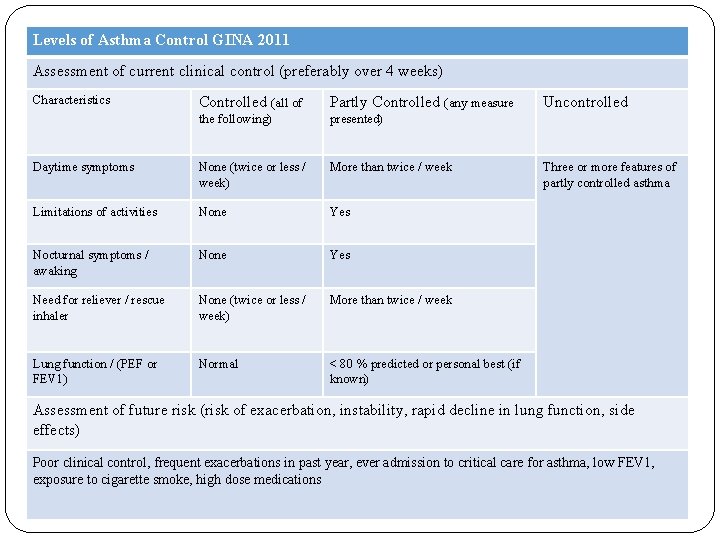
Levels of Asthma Control GINA 2011 Assessment of current clinical control (preferably over 4 weeks) Characteristics Controlled (all of Partly Controlled (any measure the following) presented) Daytime symptoms None (twice or less / week) More than twice / week Limitations of activities None Yes Nocturnal symptoms / awaking None Yes Need for reliever / rescue inhaler None (twice or less / week) More than twice / week Lung function / (PEF or FEV 1) Normal < 80 % predicted or personal best (if known) Uncontrolled Three or more features of partly controlled asthma Assessment of future risk (risk of exacerbation, instability, rapid decline in lung function, side effects) Poor clinical control, frequent exacerbations in past year, ever admission to critical care for asthma, low FEV 1, exposure to cigarette smoke, high dose medications
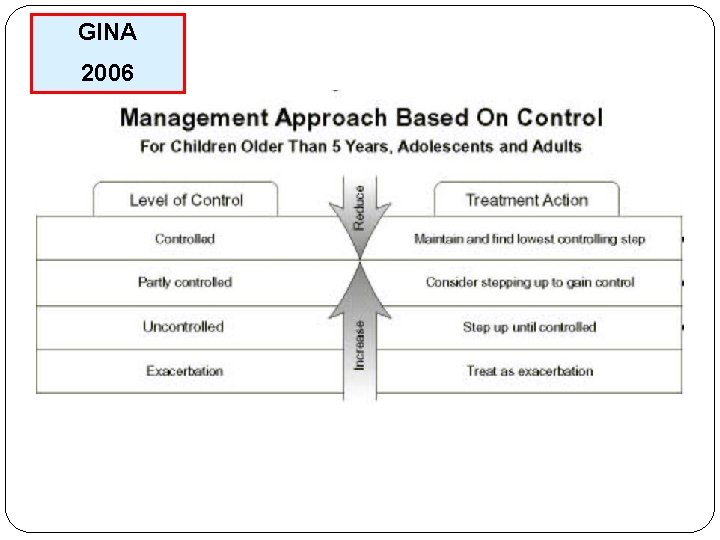
GINA 2006

CLINICAL SIGNS OF AB depends on the stage of asthma intermittent attacks of expiration type dyspnoe, ich worsening at night and at dawn wheezing: intermittent, more significant at expiration cough: usually not productive, can be basic sign anxiety, pressure, chest tightness, dyspnoe sputum production usually little, if than deep mucus prodromal signs prior attack: itching under the chin, discomfort between shoulder, fear, anxiety typical is vanishing of signs after b-dilators or antiinflammatory therapy, unsuccessful ATB th.

DIAGNOSIS PRINCIPLE: simple examinations made repeatedly are more usefull than complete examinations made at one time or during long intervals limitation of expiratory flow at asthma has variable character findings may vary from completely normal to absolutely pathological Functional diagnostics Allergologic diagnostics Specifying of inflammation markers

EXAMINATIONS AT AB • SPIROMETRY • BRONCHODILATION TESTS (BDT) – it verifies the degree of obstruction reversibility • BRONCHOPROVOKING TEST (BKT) – BKT with histamine, ACh, adenosine, excercise, cold. . . – negative BKT excludes dg. of AB (absence of bronchial negative excludes dg. of AB hyperreactivity. . . ) • PEF variability by výdychomerom (self monitoring) • ARTERIAL BLOOD GASES (at exacerbation) • Determination of NO in exhaled air (early marker of asthmatic inflammation) • SPUTUM EXAMINATION – eosinophils and their effective products, Curshmann´s spirals, Charcot-Leyden´s crystalls

SPIROMETRY • simple, reproductible • gives informations about restriction of air flow • – FVC (forced vital capacity) – FEV 1 (sec. vital cap. ) – FEV 3 (forced expiratory flow at 50% expiration) – FEV 1/VC – Tiffaneau´s index (FEV 3/VC) – PEF (peak expiratory flow in l/min)

DIFERENTIAL DIAGNOSIS chronic obstructive pulmonary disease asthma cardiale at older adults viral bronchiolitis at children hyperventilatory syndrom fixed obstacles in the airways (tumors, extramural compression, foreign particles) diffuse interstitial lung processes pneumothorax chest wall diseases (kyphoscoliosis, neuromuscular diseases)

COPD 95% are or have been cigarette smokers less common causes: exposure to air polution, inherited alfa 1 -antiprotease deficiency symptoms: persistent airflow obstruction, which can be reversible or irreversible and slowly progressive → progressive breathlessness and cough (often productive and worse in the morning), repeated respiratory infections, can lead to emphysema particularly affects the peripheral airways
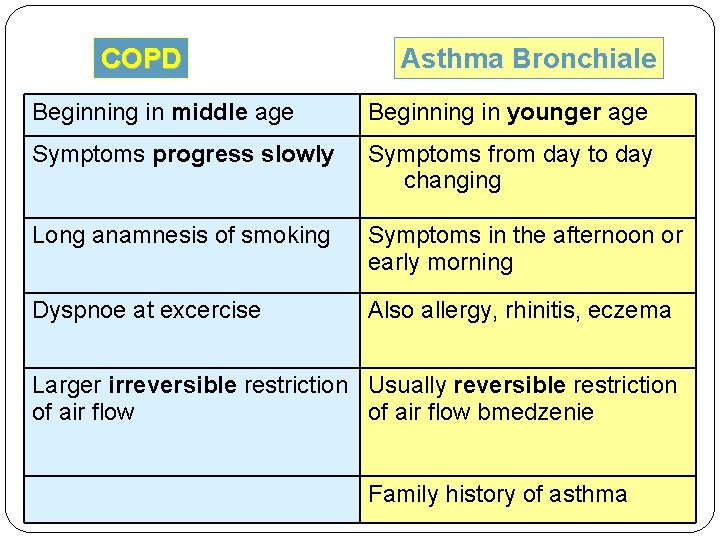

COPD Asthma Bronchiale Beginning in middle age Beginning in younger age Symptoms progress slowly Symptoms from day to day changing Long anamnesis of smoking Symptoms in the afternoon or early morning Dyspnoe at excercise Also allergy, rhinitis, eczema Larger irreversible restriction Usually reversible restriction of air flow bmedzenie Family history of asthma
COPD Pulmonary functions Symptoms
ASTHMA Symptoms Pulmonary functions

GOALS of Optimal AB Control elimination or significant reduction of symptoms prevention of exacerbations maintaining lung functions closest to physiological values functions maintaining normal physical and living activity absence of treatment adverse effects prevention of irreversible bronchial obstruction (remodelation of lower airways) - preventing asthma mortality -

THERAPY OF AB Nonpharmacological • – – Patients´ education avoiding risk factors and triggers- Pharmacological • – ANTIINFLAMMATORY • • – relieves inflammation and bronchial hyperreactivity regular, long-term use B R O N CH O D I L A T O R Y • • eliminates the symptoms of expiratory flow limitation rescue therapy in exacerbation

Administration of Drugs at AB peroral parenteral by inhalation directly to the site of action J fast beginning of action J maximum efficacy J lower therapeutic doses = minimalise risk of AE L limitations from the site of patient (technique of from the site of patient inhalation, cooperation. . . ) L inspiratory resistance, needs to be overcomed inspiratory resistance J

Device For Delivery of Drugs in AB Pressurised metered-dose inhaler The most common device The inhaler should be shaken before use
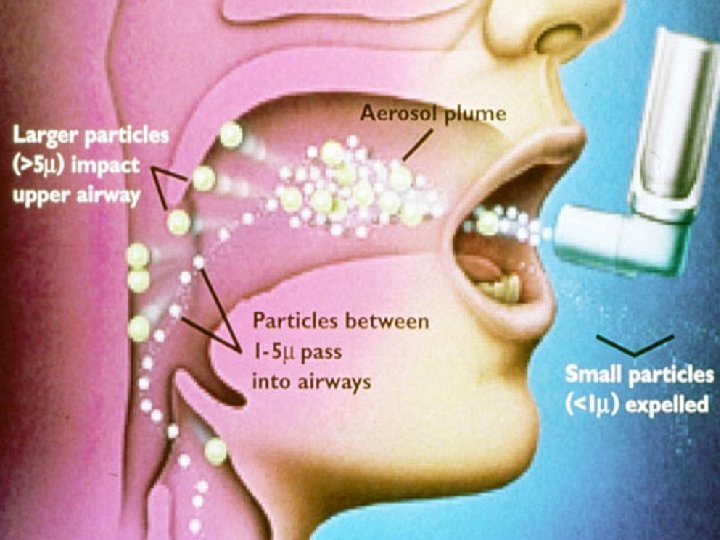

Device For Delivery of Drugs in AB Pressurised metered-dose inhaler with spacer Spacer = plastic reservoir Removes the need to coordinate aerosol activation and inspiration (young children)

Device For Delivery of Drugs in AB Breath-actuated metered-dose inhaler Several types; activated by inhalation Deliver either an aerosol or dry powder Cannot be used with spacer

Device For Delivery of Drugs in AB Dry-powder inhaler Some devices use a single dose capsule, others are multidose (the sourse is a bulk powder with the device metering the dose)
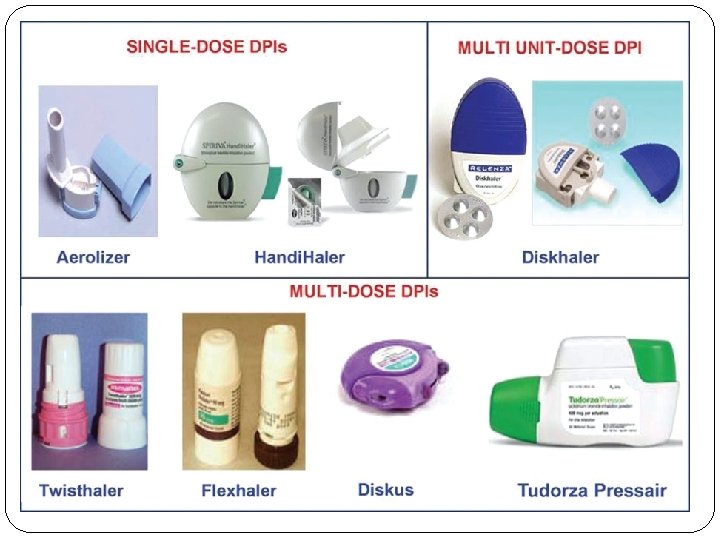

Device For Delivery of Drugs in AB Multi-dose liquid inhaler New delivery device High drug delivery to the lungs

Device For Delivery of Drugs in AB Nebulisers Are used with facemask or mouthpiece to deliver drug from reservoir solution Up to 10 times the amount of drug is required in nebuliser to produce the same effect as MDI 1. Jet nebulisers Use compressed air or oxygen

Device For Delivery of Drugs in AB Nebulisers 2. Ultrasonic nebulisers Produce more uniform particle size, but are more expensive Use piezoelectric crystal vibrating (do not require gass flow)

THERAPY OF AB A: Bronchodilators 1 st choice: ß 2 - sympathomimetics 2 nd choice: anticholinergics 3 rd choice: methylxantines B: Anti-inflammatory drugs 1 st choice: ICS 2 nd choice: leukotriene receptor antagonists severe asthma: monoclonal antibodies

INFLUENCE OF AUTONOMIC NERVOUS SYSTEM IN THE TREATMENT OF ASTHMA ß 2 - SYMPATHOMIMETICS ANTICHOLINERGICS ADMINISTRATION BY INHALATION
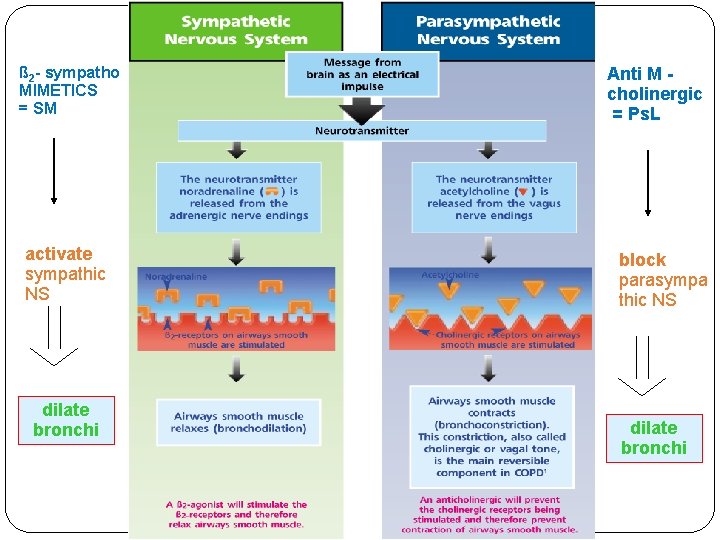
ß 2 - sympatho MIMETICS = SM activate sympathic NS dilate bronchi Anti M cholinergic = Ps. L block parasympa thic NS dilate bronchi
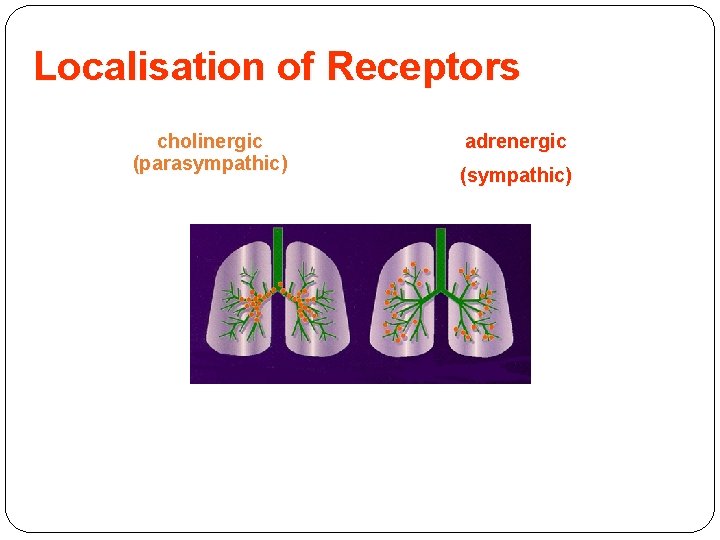
Localisation of Receptors cholinergic (parasympathic) adrenergic (sympathic)

ß 2 - SYMPATHOMIMETICS Mechanism of action = agonistic, activating influence on ß 2 receptors of sympathic NS 1. Long-acting ß 2 SM (long-acting betaagonists ) = LABA Controllers – to long-term, regular bronchodilation 2. Short-acting ß 2 SM (short-acting betaagonists ) = SABA Relievers – to short-term, acute management of exacerbation

ß 2 - SYMPATHOMIMETICS Mechanism of action: Influence of ß 2 -receptors in lungs (↑c. AMP, aktivation of PKA, phosphorylation of proteins that regulate smooth muscle tone) The regular use can enhance Th 2 Inflammatory pathways and also down-regulate ß 2 -receptors (regular use of ß 2 sympathomimetics without ICS is not advised)
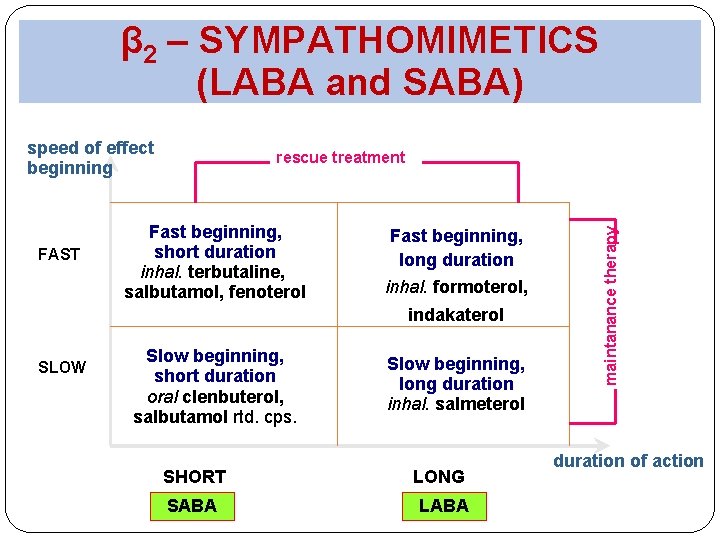
β 2 – SYMPATHOMIMETICS (LABA and SABA) speed of effect beginning Fast beginning, short duration inhal. terbutaline, salbutamol, fenoterol Fast beginning, long duration inhal. formoterol, indakaterol SLOW Slow beginning, short duration oral clenbuterol, salbutamol rtd. cps. SHORT SABA Slow beginning, long duration inhal. salmeterol LONG LABA maintanance therapy FAST rescue treatment duration of action

SABA basic relievers used ad hoc to relieve or to remove symptoms no reason for regular administration salbutamol (Ventolin) fenoterol /Australia – deregistered for AE CVS/

LABA C the best, fast and intense acting b-dilatans duration of action >12 hours MA: Bronchodilation through β 2 => relaxation of smooth muscle Improve mucociliar clearens Lower vascular permeability Modulate release of mediators from mastocytes a bazophils Provide long-term safety against bronchoconstriction Length of this bronchodilation effect at long-term regular administration decreases sign of tollerance for down regulation of β 2 receptors => inhibition = concomitant administration of ICS LABA in long-term therapy of asthma never can administer lonely, without ICS!
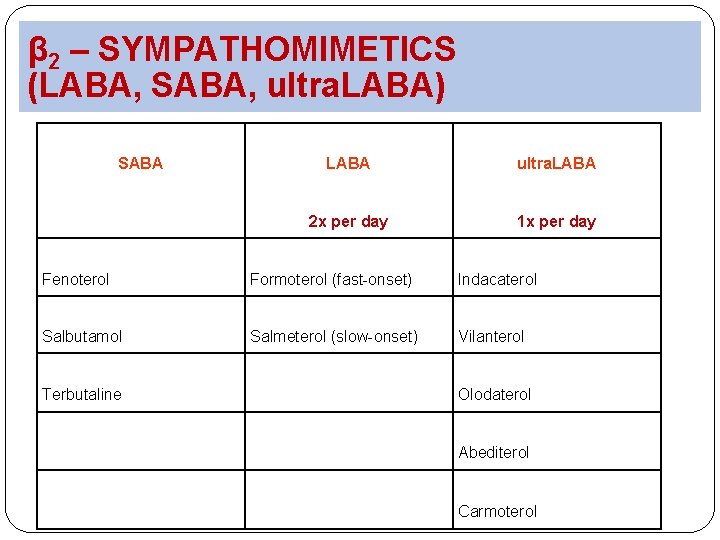
β 2 – SYMPATHOMIMETICS (LABA, SABA, ultra. LABA) SABA LABA ultra. LABA 2 x per day 1 x per day Fenoterol Formoterol (fast-onset) Indacaterol Salbutamol Salmeterol (slow-onset) Vilanterol Terbutaline Olodaterol Abediterol Carmoterol
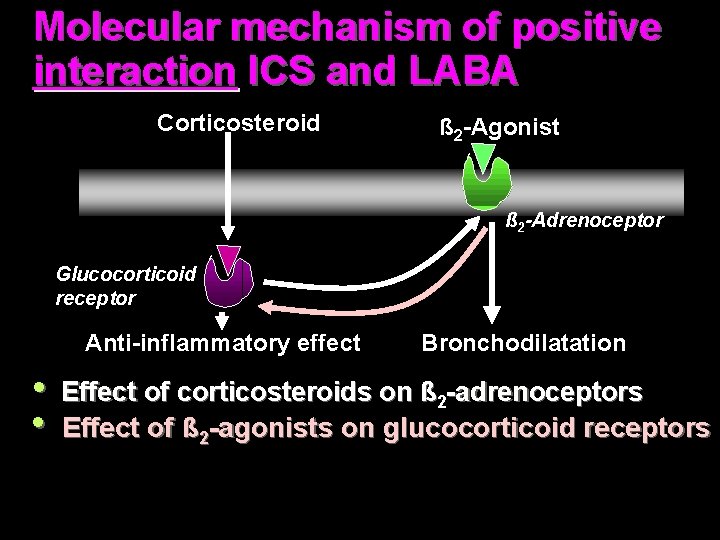
Molecular mechanism of positive interaction ICS and LABA Corticosteroid ß 2 -Agonist ß 2 -Adrenoceptor Glucocorticoid receptor Anti-inflammatory effect Bronchodilatation • Effect of corticosteroids on ß 2 -adrenoceptors • Effect of ß 2 -agonists on glucocorticoid receptors

LABA formoterol salmeterol Monotherapy LABA: effectivity of LABA vs. ICS improving sleeping, but without effect to pulmonary functions discontinuation ICS and adding LABA at persistent asthma loosing control good controlled patient with asthma with persistent asthma at low dose ICS replacement by LABA loosing control ( e. No and Eo in sputum) without effect on inflam. in airways (biopsia)

ß 2 - SYMPATHOMIMETICS - ADRs Fine skeletal muscle tremor Tachycardia and arrhythmias (high doses, oral or parenteral administration) Hypokalaemia with high doses Paradoxical bronchospasm Headache Tolerance (avoids use of ICS)

FDA – LABA drug safety communication 2011 In February 2010, the agency announced it was requiring manufacturers to revise their drug labels because of an increased risk of severe exacerbation of asthma symptoms, leading to hospitalizations, in pediatric and adult patients, as well as death in some patients using LABAs for the treatment of asthma.

FDA – LABA drug safety communication 2011 The new recommendations in the updated labels state: Use of a LABA alone without use of a long-term asthma control medication, such as an inhaled corticosteroid, is contraindicated (absolutely advised against) in the treatment of asthma. LABAs should not be used in patients whose asthma is adequately controlled on low or medium dose inhaled corticosteroids. LABAs should only be used as additional therapy for patients with asthma who are currently taking but are not adequately controlled on a long-term asthma control medication, such as an inhaled corticosteroid. Once asthma control is achieved and maintained, patients should be assessed at regular intervals and step down therapy should begin (e. g. , discontinue LABA), if possible without loss of asthma control, and the patient should continue to be treated with a long-term asthma control medication, such as an inhaled corticosteroid. Pediatric and adolescent patients who require the addition of a LABA to an inhaled corticosteroid should use a combination product containing both an inhaled corticosteroid and a LABA, to ensure adherence with both medications.

INHALED ANTIMUSCARINIC DRUGS Relievers of the second choice, at AE competitive antagonists on M 1, M 2 and M 3 receptors of parasympathicus cholinergic tonus Division: with short-lasting effect: ipratropium bromide short-lasting with long-lasting effect: tiotropium bromide (CHOPD) long-lasting

FDA – LABA drug safety communication 2011 In February 2010, the agency announced it was requiring manufacturers to revise their drug labels because of an increased risk of severe exacerbation of asthma symptoms, leading to hospitalizations, in pediatric and adult patients, as well as death in some patients using LABAs for the treatment of asthma.

FDA – LABA drug safety communication 2011 The new recommendations in the updated labels state: Use of a LABA alone without use of a long-term asthma control medication, such as an inhaled corticosteroid, is contraindicated (absolutely advised against) in the treatment of asthma. LABAs should not be used in patients whose asthma is adequately controlled on low or medium dose inhaled corticosteroids. LABAs should only be used as additional therapy for patients with asthma who are currently taking but are not adequately controlled on a long-term asthma control medication, such as an inhaled corticosteroid. Once asthma control is achieved and maintained, patients should be assessed at regular intervals and step down therapy should begin (e. g. , discontinue LABA), if possible without loss of asthma control, and the patient should continue to be treated with a longterm asthma control medication, such as an inhaled corticosteroid. Pediatric and adolescent patients who require the addition of a LABA to an inhaled corticosteroid should use a combination product containing both an inhaled corticosteroid and a LABA, to ensure adherence with both medications.
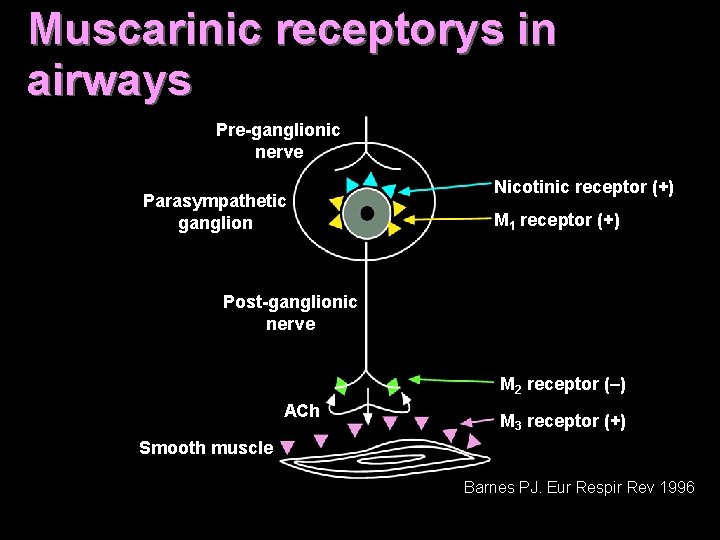
Muscarinic receptorys in airways Pre-ganglionic nerve Parasympathetic ganglion Nicotinic receptor (+) M 1 receptor (+) Post-ganglionic nerve M 2 receptor (–) ACh M 3 receptor (+) Smooth muscle Barnes PJ. Eur Respir Rev 1996

INHALED ANTIMUSCARINIC DRUGS Mechanism of action: M 3 receptors: mediate bronchoconstriction, mucus secretion M 2 receptors: inhibit cilliary activity, also presynaptic receptors Ipratropium (non-selective) Tiotropium (selective for M 3 receptors)

INHALED ANTIMUSCARINIC DRUGS decrease n. vagus tone cause relaxation but no bronchoprotective action are in general less effective than β 2 – mimethics and have a little slower beginning of action advantageous combinations v 1 inhalation system: ipratropium+fenoterol
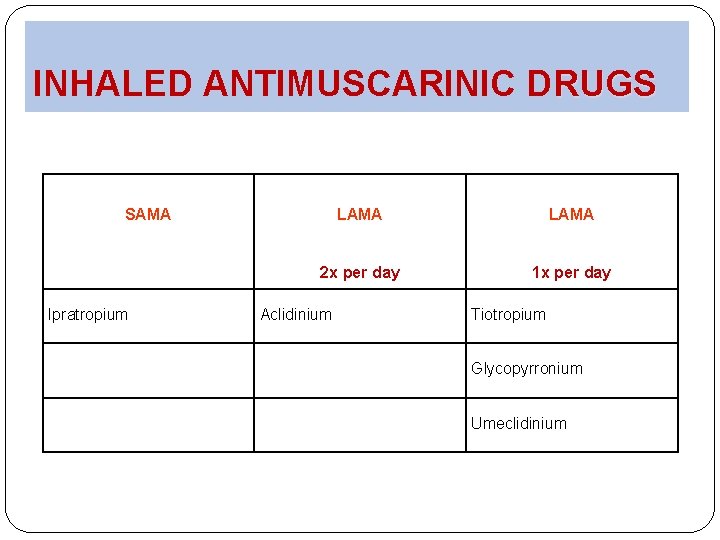
INHALED ANTIMUSCARINIC DRUGS SAMA Ipratropium LAMA 2 x per day 1 x per day Aclidinium Tiotropium Glycopyrronium Umeclidinium


Tripple therapy – COPD glycopyronium (LAMA) + formoterol fumarate (LABA) + beclometasone dipropionate (ICS)

Tripple therapy – COPD

Methylxanthines CONTROLLERS, to long-lasting control of symptoms Improvement of clinical symptomatology bronchodilation - without signif. increase of FEV 1/ improvement of lung function parameters through inhibition of fosfodiesterase I. to IV. => c. AMP antiinflam. , immunomodulatory effects positive effect on phenomenon of „corticoid resist. “ AE: cephalea, nausea, vomiting, tachycardia, palpitations, plasm. conc. (TDM) arrhytmias, epileptic spasms even death potential toxicity, profile of AE BRONCHODILATORS OF THE THIRD CHOICE

Methylxanthines Proven benefit bring only drug forms providing longlasting action with controlled release - p. o. aminophylline, theophylline for using during day time always + ICS – less effective than ICS+LABA with short-lasting ef. - p. o. , i. v. aminophylline

INHALED CORTICOIDS ICS the most effective antiinflammatory antiasthmatics to long-term use at all forms of AB Mechanism of action: 1. inhibition of cytokine transcription antiinflam. ef. 2. inhibition of mediators of inflam. release 3. decrease of airways reactivity 4. restriction of vasodilation antioedematic ef. 5. affect synthesis of eikosanoids 6. control activation of adhesive molecules 7. increase of susceptibility resp. protection of increase of susceptibility 2 receptors against down-regulation at long-term treatment with 2 mimetics

ICS The most effective contollers of symptoms in chronic asthma Relatively ineffective in COPD Mechanism of action: supress inflammation and immune response No bronchodilators

ICS AE locally can reduce with the use of attachments and rinsing the mouth with Na. HCO 3 oropharyngeal candidosis dysphonia seldomly irritation to cough risk of systemic AE is , depends on dose systemic , efficacy and pharmacokinetic of steroid inflammation in airways, bronchial inflammation hyperreactivity and obstruction of airways ction risk of AE (acute exacerbations) AE and control symptoms of disease
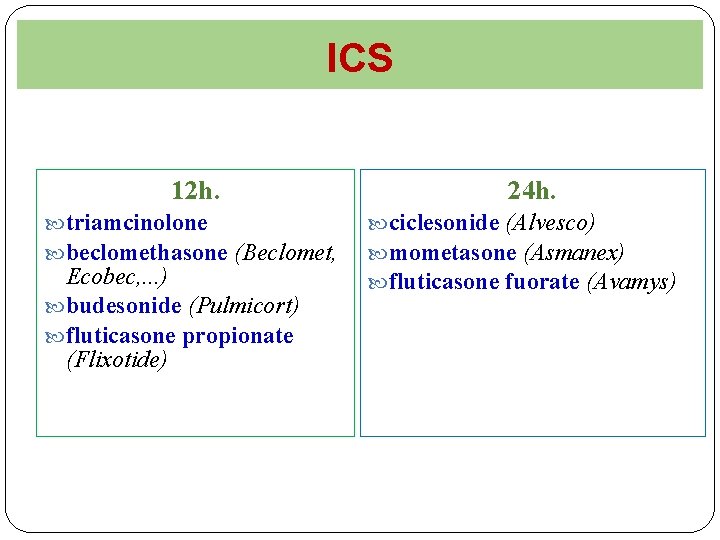
ICS 12 h. triamcinolone beclomethasone (Beclomet, Ecobec, . . . ) budesonide (Pulmicort) fluticasone propionate (Flixotide) 24 h. ciclesonide (Alvesco) mometasone (Asmanex) fluticasone fuorate (Avamys)

Principles of Treatment with ICS 1. ICS need to be administered at each new dg. AB 2. Treatment is essential to start early 3. We administer attack doses of ICS 4. Reduction of dose only after longer stabilisation (6 months) – than minimal effective dose 5. If not sufficient ICS, we add as the drug of the first choice LABA, alternatives are leucotriene modifiers ( the first choice add-on therapy for children younger than 5 years), methylxanthines, slow release β 2 -agonists tablets 6. To adult patients are administered max. 200 -800 mcg BDP/day and to children max. 400 mcg BDP/day, than you should start on with add-on therapy

ICS in the Treatment of AB – „exacerbations“ the best to add high dose of ICS to regular to maintenance therapy ICS+LABA at severe AE systemic CS AE

Adverse effects of systemically administered corticosteroids 1. Infections 2. The long-term use may increase blood 3. 4. 5. 6. pressure, cause fluid retention and salt retention in the body (oedema), increased excretion of calcium and potassium Worse and longer wound healing Rash and acne Hyperglycaemia They increase the risk of gastrointestinal perforation

Adverse effects of systemically administered corticosteroids 7. Increased appetite and weight gain 8. Osteoporosis (↓ absorption of calcium, ↑ its excretion) 9. Muscle pain, muscle weakness and muscle cramps (especially ↑ loss of potassium, ↓ calcium level in the blood) 10. Cataract, increased intraocular pressure, optic nerve damage, eye infections 11. CNS: irritability, mood and personality changes, depression, headaches, dizziness

Leukotriene receptor antagonists CONTROLLERS, for long-term control of symptoms antagonists of leukotriene 1 (Cys. LT 1) receptors montelukast, zafirlukast, pranlukast inhibitors of 5 -lipooxygenase zileuton taken perorally MA: - additive antiinflam. effect to ICS - reduce tissue eosinophilia - mild bronchodilation ef. - bronchoprotective ef.

Leukotriene receptor antagonists role in therapy of AB - still unclear are less effective than low doses of ICS as additive drugs (in combination with ICS) reduce the need of steroid dose at severe asthma again less effective than standard ICS+LABA advantageous – aspirin asthma, by excercise induced asthma, „preschool wheezing“ compliance at taking tablet form

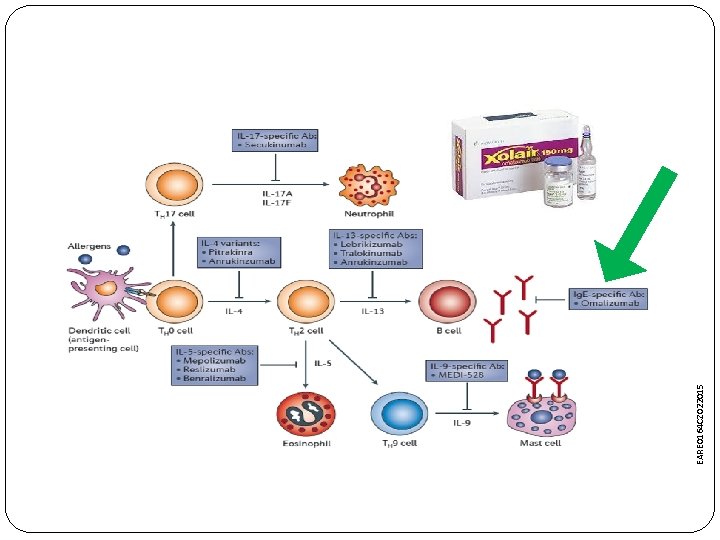
BIOLOGIC THERAPY ASTHMA BRONCHIALE = imunotherapy
Anti-Ig. E monoclonal antibody EMA approval from 2008 OMALIZUMAB anti-Ig. E monoclonal antibodyanti-Ig. E monoclonal . antibody Indications: adults, children from 6 years – severe persistent AB – severe urticaria
EARE 0164 CZ 022015
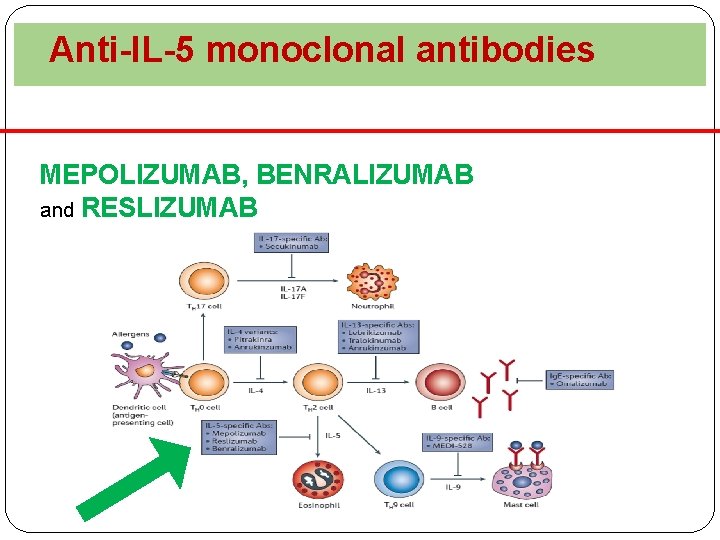
Anti-IL-5 monoclonal antibodies MEPOLIZUMAB, BENRALIZUMAB and RESLIZUMAB
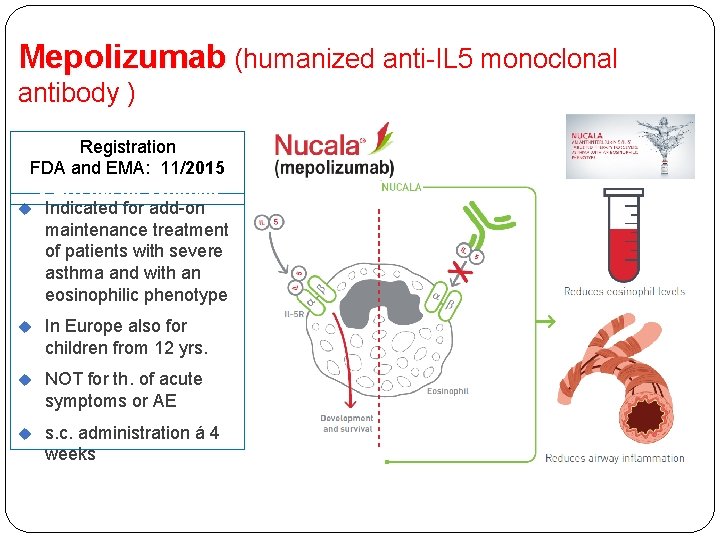
Mepolizumab (humanized anti-IL 5 monoclonal antibody ) Registration FDA and EMA: 11/2015 V SR: t. č. na výnimku Indicated for add-on maintenance treatment of patients with severe asthma and with an eosinophilic phenotype In Europe also for children from 12 yrs. NOT for th. of acute symptoms or AE s. c. administration á 4 weeks

Anti-IL-4/13 receptor MAb DUPILUMAB a LEBRIKIZUMAB Lebrikizumab is an Ig. G 4 humanized m. Ab that specifically binds to IL-13, inhibiting its function. Dupilumab blocks the transduction signal activated by IL-13 and IL-4 and has been evaluated in patients with persistent asthma (moderate-tosevere) and airway or peripheral eosinophilia.

A: PREVENTERS inhalatory corticoids ICS long-acting 2 -sympathomimetics (long-acting betaagonists ) LABA, (8 -15 h. ) antileukotriens LTRAs leukotriene receptor antagonists inhibitors of 5 -lipooxygenase (zileuton) retard methylxanthines cromones

B: RELIEVERS inhalatory short-acting 2 -sympathomimetics (short- acting betaagonists ) SABA (till 4 -6 h. ) inhalatory anticholinergics short-acting systemic corticoids p. o. /i. v. („rescue“ treatment) some sources – controllers fast acting methylxantines
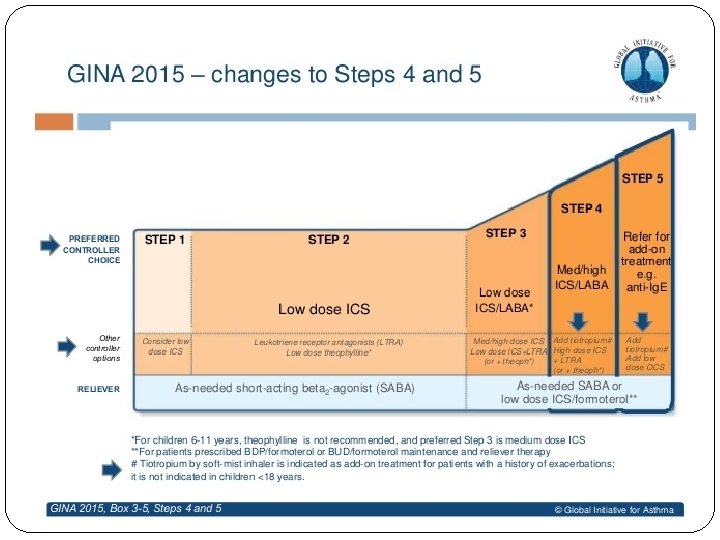
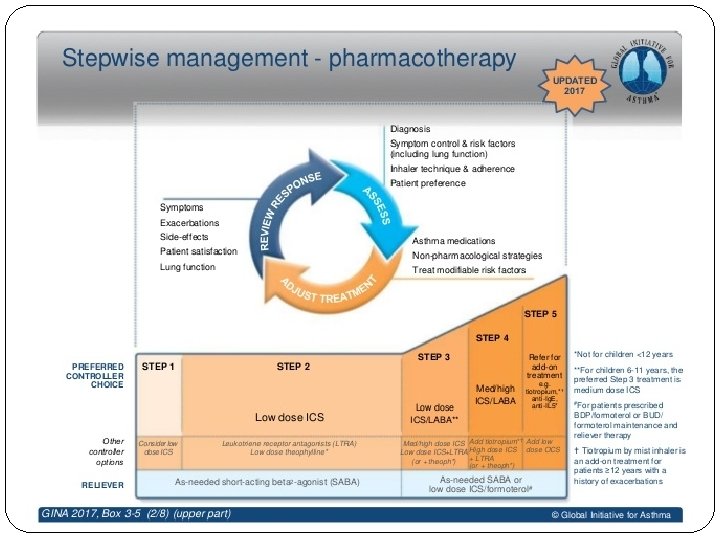
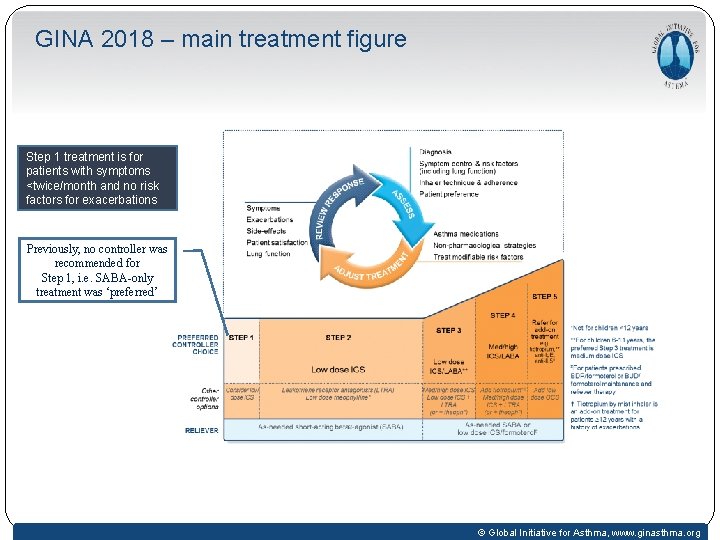
GINA 2018 – main treatment figure Step 1 treatment is for patients with symptoms <twice/month and no risk factors for exacerbations Previously, no controller was recommended for Step 1, i. e. SABA-only treatment was ‘preferred’ GINA 2018, Box 3 -5 (2/8) (upper part) © Global Initiative for Asthma, www. ginasthma. org

7 May 2019
ANTIHISTAMINES
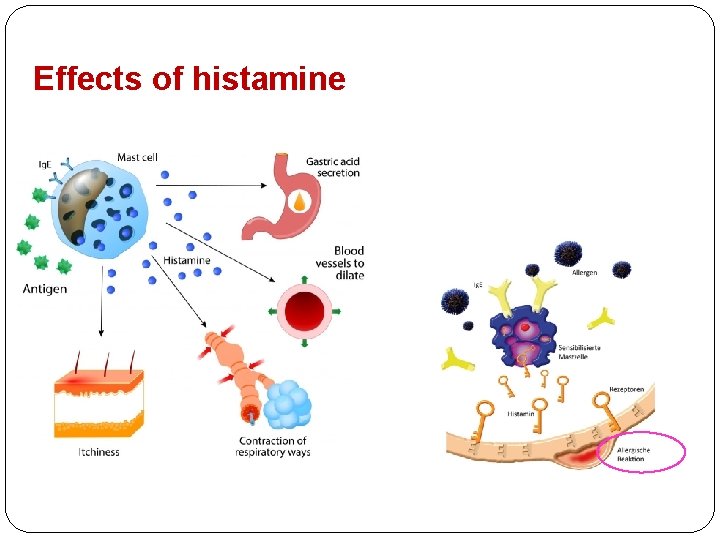
Effects of histamine

H 1 receptor antagonists (Antihistamines) 1 st generation = sedating antihistamines 2 nd generation = non-sedating antihistamines Histamine = local hormone (autacoid) important in pathophysiology of allergic reactions

H 1 receptor antagonists (Antihistamines) 1 st generation 2 nd generation Non-selective From the 1980 s onwards H 1, M, 5 -HT, Ach, D and other receptors High selectivity for H 1 rec. => Less ADRs – anticholinergic, sedative. . . Lipophobic, relat. big Mn => Lipofil, small Mn => Little cross HEB Easy cross HEB Bisulepine (Dithiaden) Dimetindene (Fenistil) Moxastine (Kinedryl) Promethazine (Protazín) Ketotifen (Zaditen) Cyproheptadine (Peritol) Tietylperazine (Torecan) Cetirizine (Zyrtec) Loratadine (Claritine) Modern antihistamines: Desloratadine (Aerius) Fexofenadine (Fixit) Levocetirizine (Xyzal) Bilastine (Omarit) Rupatadine (Rupafin)

Topical antihistamines EYES, NOSE Azelastine (Allergodil) Levocabastine (Livostin) Olopatadine (Opatanol)
- Slides: 85