T Cymes Stage 3 student doctor University of










- Slides: 13

T. Cymes Stage 3 student doctor University of Cambridge Paediatrics Respiratory system

Plan �Examination tips differences from adults red flags �Asthma �Bronchiolitis �Pneumonia �Cystic fibrosis �Other diseases

Examination – how to survive �Get to their level! �Let young children play with your stethoscope Great toy! Lets them get used to it �Let parents undress the child only when needed �Start with least invasive examination �Show on parents, toy etc �Auscultate early �Save percussion until the end ▪ Start on arm or knee – they get used to it!

Examination – difference from adults �Position Infants – lying on couch Toddler – on parent's lap Pre-school – while at play �Initial impression important ? unwell child �Look for dysmorphic features �Percussion can be omitted Little information in infants

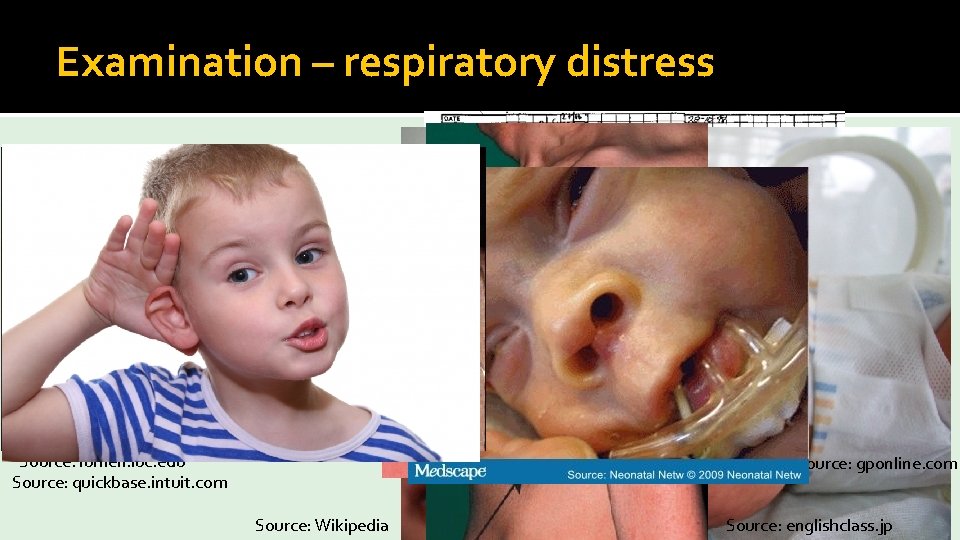
Examination – respiratory distress � Tachypnoea / tachycardia � Accessory muscles � Intercostal recessions � Wheeze � Harrison’s sulcus � Stridor � Cyanosis � Grunting � Nasal flaring � Silent chest Source: lumen. luc. edu Source: quickbase. intuit. com Source: gponline. com Source: Wikipedia Source: BMJ Source: englishclass. jp

Asthma � Epidemiology � Examination out of attack 15% prevalence ± wheeze Associated with atopy Reduced PEFR � History � Examination during attack Wheeze & cough Signs of respiratory distress Worse a night Hyperexpansion Ask about Ascultate ▪ Triggers ▪ Frequency ▪ Interval symtpoms Reduced PEFR Sp. O 2

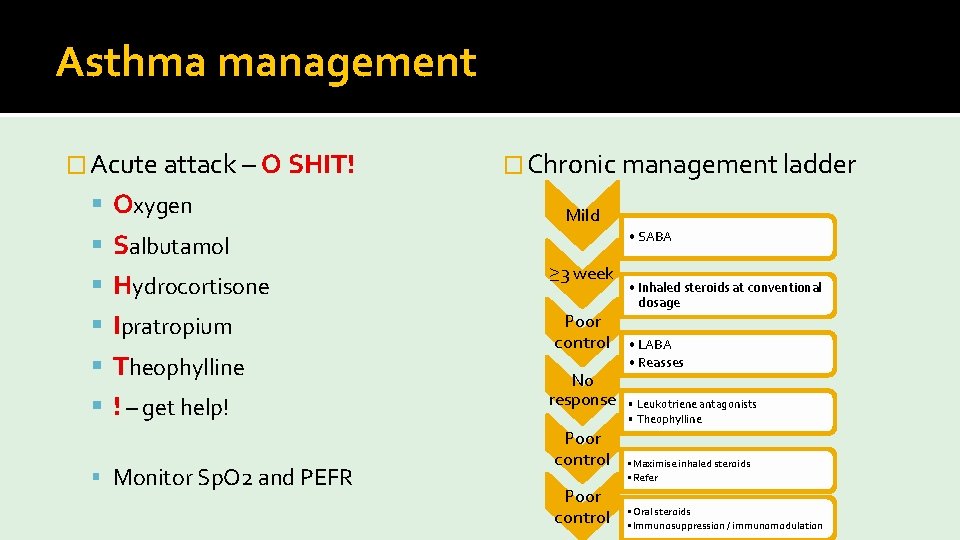
Asthma management � Acute attack – O SHIT! Oxygen � Chronic management ladder Mild Salbutamol • SABA Hydrocortisone ≥ 3 week Ipratropium Poor control Theophylline ! – get help! Monitor Sp. O 2 and PEFR No response Poor control • Inhaled steroids at conventional dosage • LABA • Reasses • Leukotriene antagonists • Theophylline • Maximise inhaled steroids • Refer • Oral steroids • Immunosuppression / immunomodulation

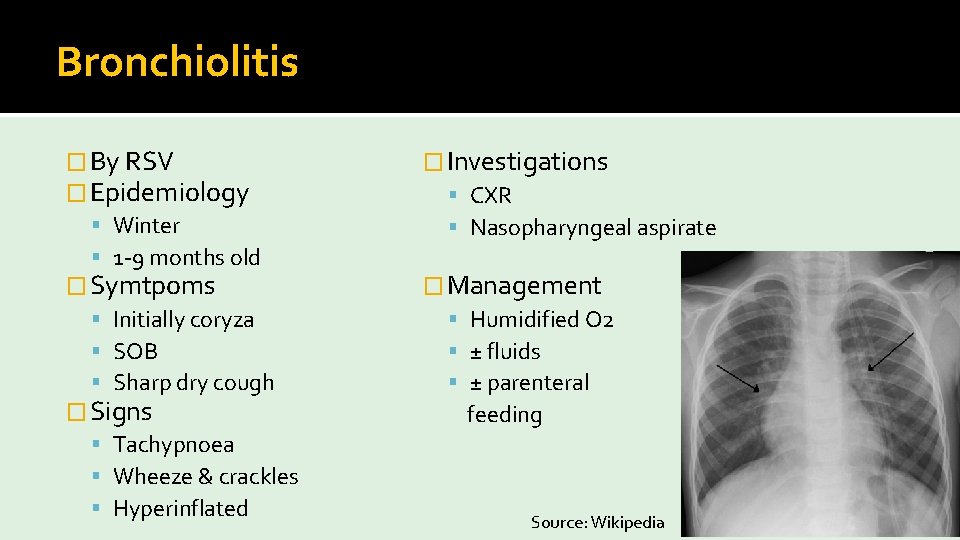
Bronchiolitis � By RSV � Epidemiology Winter 1 -9 months old � Symtpoms Initially coryza SOB Sharp dry cough � Signs Tachypnoea Wheeze & crackles Hyperinflated � Investigations CXR Nasopharyngeal aspirate � Management Humidified O 2 ± fluids ± parenteral feeding Source: Wikipedia

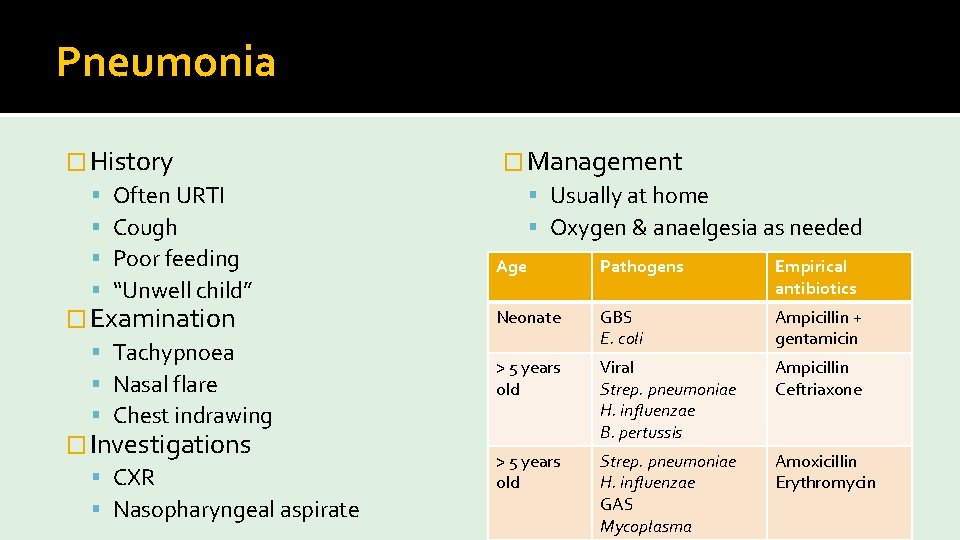
Pneumonia � History Often URTI Cough Poor feeding “Unwell child” � Examination Tachypnoea Nasal flare Chest indrawing � Investigations CXR Nasopharyngeal aspirate � Management Usually at home Oxygen & anaelgesia as needed Age Pathogens Empirical antibiotics Neonate GBS E. coli Ampicillin + gentamicin > 5 years old Viral Strep. pneumoniae H. influenzae B. pertussis Ampicillin Ceftriaxone > 5 years old Strep. pneumoniae H. influenzae GAS Mycoplasma Amoxicillin Erythromycin

Cystic fibrosis � Part of Guthrie test � Autosomal recessive 1: 2500 live births 1: 25 are carriers � History Meconium ileus (10 -20%) Persistent cough Recurrent/chronic chest infection Bronciectasis in children Malabsorption failure to thrive Male infertility � Signs Hyperinflated Wheeze Coarse crackles � Management Monitor lung function Prophylactic + rescue antibiotics Physiotherapy Bilateral lung transplant when end-stage Nutrtional ▪ Pancreatic enzyme supplements ▪ 150% healthy calorie intake

Other diseases � Croup � Acute epiglottitis Parainfluenza virus H. influenzae type b URTI barking cough + stridor Very painful throat Improve over 24 h Sits up with open mouth Symptomatic management Drooling ? Steroids DON’T examine throat Intubate, then: ▪ Blood culture ▪ Cefuroxime IV

Other diseases � Whooping cough � Acute otitis media B. pertussis RSV, pneumococci, Hib, GBS Coryza Earache in older children Coughing paroxysms Fever ▪ Inspiratory whoop Erythromycin Exclude via otoscopy in any ill oddler Management ▪ Symptomatic ▪ amoxicillin

Thank you!