Respiratory Emergencies Victor Politi M D FACP Medical


































































- Slides: 87

Respiratory Emergencies Victor Politi, M. D. , FACP Medical Director Physican Assistant Program


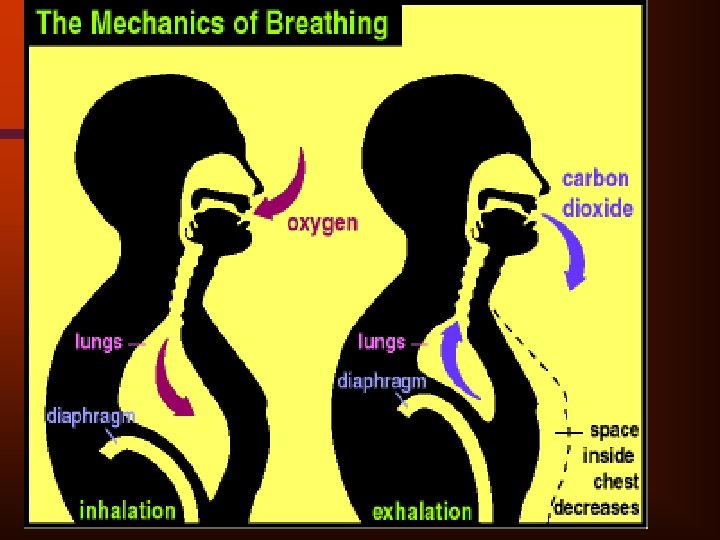
• Dyspnea • the sensation of breathlessness or inadequate breathing • the most common complaint of patients with cardiopulmonary diseases

• Dyspnea - common complaint/symptom • “shortness of breath” or “breathlessness” • Defined as abnormal/uncomfortable breathing • Multiple etiologies • 2/3 of cases - cardiac or pulmonary etiology

• When it becomes obvious to us that an individual IS breathing, and it's one of the first things that we noticed about this individual, then THAT needs to be one of the first things that we address. • Any patient who is presenting with some degree of respiratory effort is IN respiratory distress

• There is no one specific cause of dyspnea and no single specific treatment • Treatment varies according to patient’s condition • • chief complaint history exam laboratory & study results

Differential Diagnosis • Composed of four general categories • Cardiac • Pulmonary • Mixed cardiac or pulmonary • non-cardiac or non-pulmonary

Pulmonary Etiology • • • COPD Asthma Restrictive Lung Disorders Hereditary Lung Disorders Pneumonia Pneumothorax

Cardiac Etiology • • CHF CAD MI (recent or past history) Cardiomyopathy Valvular dysfunction Left ventricular hypertrophy Pericarditis Arrhythmias

Mixed Cardiac/Pulmonary Etiology • • COPD with pulmonary HTN and/or cor pulmonale Deconditioning Chronic pulmonary emboli Pleural effusion

Noncardiac or Nonpulmonary Etiology • • • Metabolic conditions (e. g. acidosis) Pain Trauma Neuromuscular disorders Functional (anxiety, panic disorders, hyperventilation) • Chemical exposure

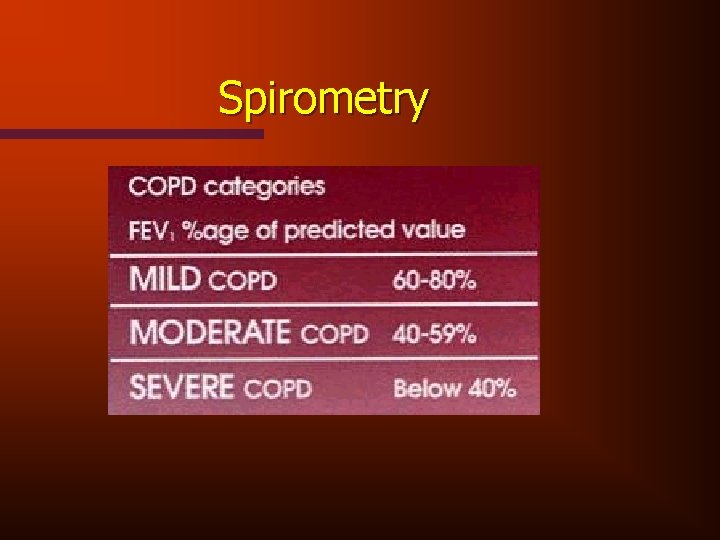
Easily Performed Diagnostic Tests • Chest radiographs • Electrocardiograph • Screening spirometry

• In cases where test results inconclusive • complete PFTs • ABGs • EKG • Standard exercise treadmill testing/ or complete cardiopulmonary exercise testing • Consultation with pulmonologist/cardiologist may be useful

ABGs • • • Commonly used to evaluate acute dyspnea can provide information about altered p. H, hypercapnia, hypocapnia or hypoxemia normal ABGs do not exclude cardiac/pulmonary dx as cause of dyspnea • Remember- ABGs may be normal even in cases of acute dyspnea - ABGs do not evaluate breathing

PULSE OX • Rapid, widely available, noninvasive means of assessment in most clinical situations • insensitive (may be normal in acute dyspnea) • • The % of Oxygen saturation does not always correspond to Pa. O 2 The hemoglobin desaturation curve can be shifted depending on the p. H, temperature or arterial carbon monoxide or carbon dioxide levels

ASTHMA

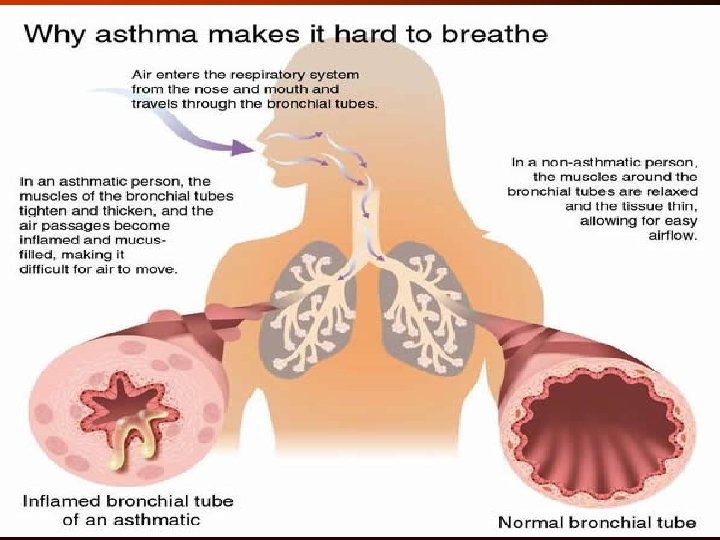
What is Asthma • A Chronic disease of the airways that may cause: • Wheezing • Breathlessness • Chest tightness • Nighttime or early morning coughing


The bronchospasm characteristic of the acute asthmatic attack is typically reversible. It improves spontaneously or within minutes to hours of treatment

• Asthma can exist by itself or coexist with chronic bronchitis, emphysema, or bronchiectasis

Symptoms/Chief Complaint • • Progressive dyspnea Cough Chest tightness Wheezing/coughing

• The rapidly reversible airflow obstruction of asthma is mainly due to bronchial smooth muscle contraction

Focus of Therapy • • Pharmacologic manipulation of airway smooth muscle Do not overlook physiologic impairment caused by mucous production and mucosal edema Bronchospasm can be reversed in minutes Airflow obstruction due to mucous plugging and inflammatory changes in bronchial walls may not resolve for days/weeks • may lead to atelectasis, infectious bronchitis, pneumonitis

Asthma Triggers • • Immunologic reaction Viral respiratory/sinus infections change in temperature/humidity Drugs/Chemicals • aspirin, NSAIDS • • Exercise GE reflux Laughing/coughing Environmental factors • strong odors, pollutants, dust, fumes

Patient Exam • Wheezing • may be audible w/o stethoscope • • • Use of accessory muscles of inspiration diaphragmatic fatigue Paradoxical respirations • - reflect impending ventilatory failure • Altered mental status • lethargy, exhaustion, agitation, confusion

Patient Exam • • • Hypersonance to percussion decreased intensity of breath sounds prolongation of expiratory phase w or w/o wheezing

Patient Exam • The intensity of the wheeze may not correlate with the severity of airflow obstruction • “quiet chest” - very severe airflow obstruction

Asthma Treatment • • Nebulized B-adrenergic drugs Corticosteroids Nebulized anticholinergics Magnesium sulfate Oxygen Long acting beta-agonists Inhaled steroids

Managing Asthma: • Indications of a severe attack: • Breathless at rest • hunched forward • talking in words rather than sentences • Agitated • Peak flow rate less than 60% of normal

Treatment Goals of Severe Asthma • • • Improve airway function rapidly Avoid hypoxemia Prevent respiratory failure and death

COPD

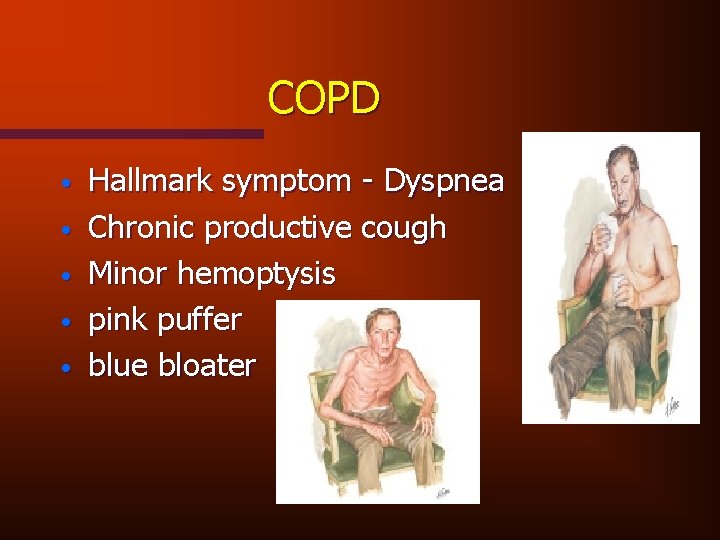
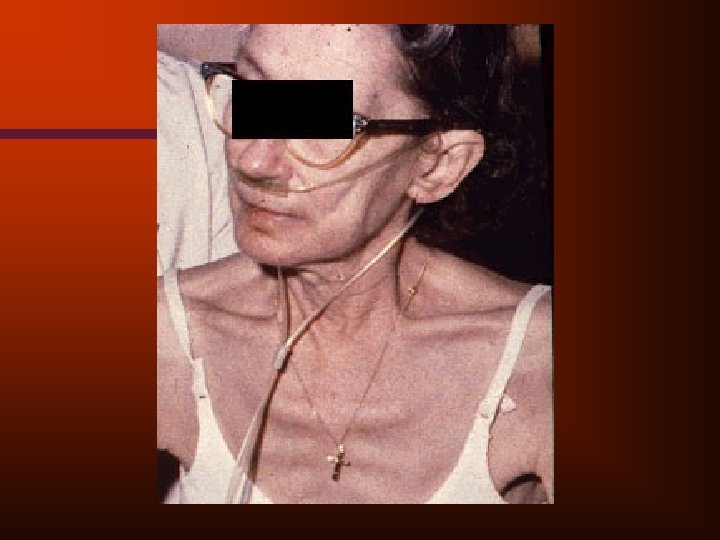
COPD • • • Hallmark symptom - Dyspnea Chronic productive cough Minor hemoptysis pink puffer blue bloater

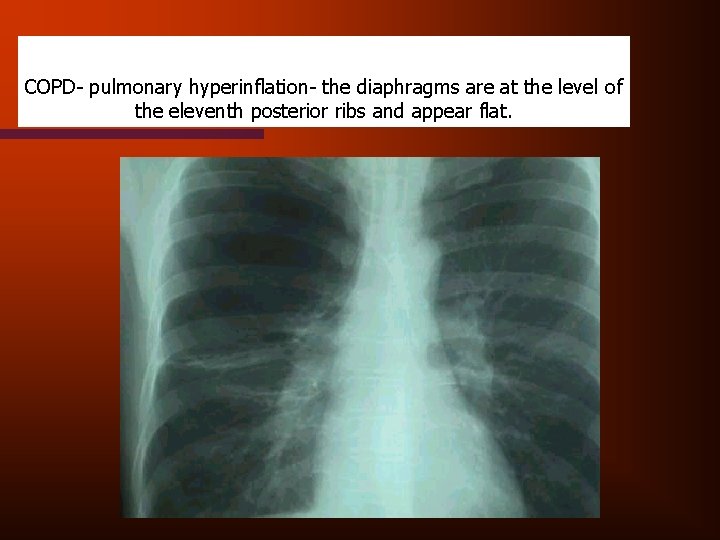
COPD- pulmonary hyperinflation- the diaphragms are at the level of the eleventh posterior ribs and appear flat.

COPD - Physical Findings • • Tachypnea Accessory respiratory muscle use Pursed lip exhalation Weight loss due to poor dietary intake and excessive caloric expenditure for work of breathing


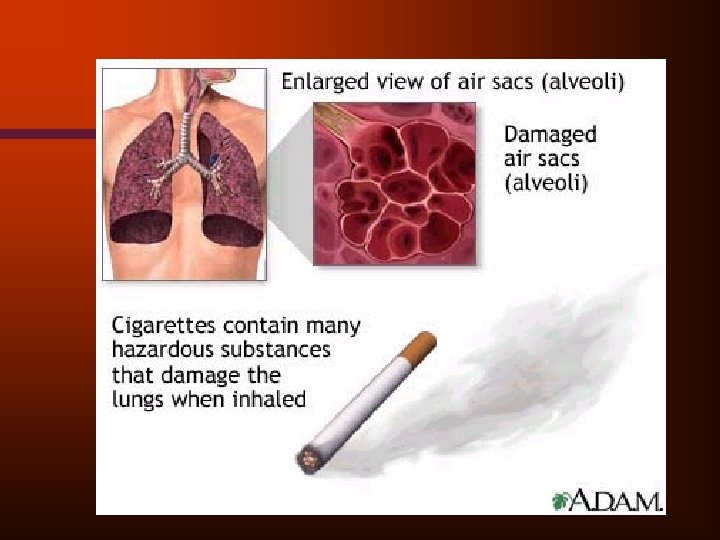
Dominant Clinical Forms of COPD • • Pulmonary emphysema Chronic bronchitis • Most patients exhibit a mixture of symptoms and signs

COPD - Advanced Dx • • • secondary polycythemia cyanosis tremor somnolence and confusion due to hypercarbia Secondary pulmonary HTN w or w/o cor pulmonale

COPD Treatment Strategy • • • Elimination of extrinsic irritants bronchodilator & glucocorticoid therapy Antibiotics Mobilization of secretions “respiratory vaccines” Oxygen therapy - if oxygen saturation <90% at rest on room air

Spirometry


PNEUMONIA

• 6 th leading cause of death in the US • Respiratory viruses & mycoplasma responsible for greater than 1/3 of cases

Common types of respiratory infections • • Tracheobronchitis Pneumonia Effusions Empyema Abscess Cavitary lesions post-obstructive

Common Respiratory Viruses • • Influenza A & B Parainfluenza 1& 3 Respiratory Syncytial Virus Adenovirus Cytomegalovirus Herpes Simplex & Zoster/varicella Hanta Virus Infection

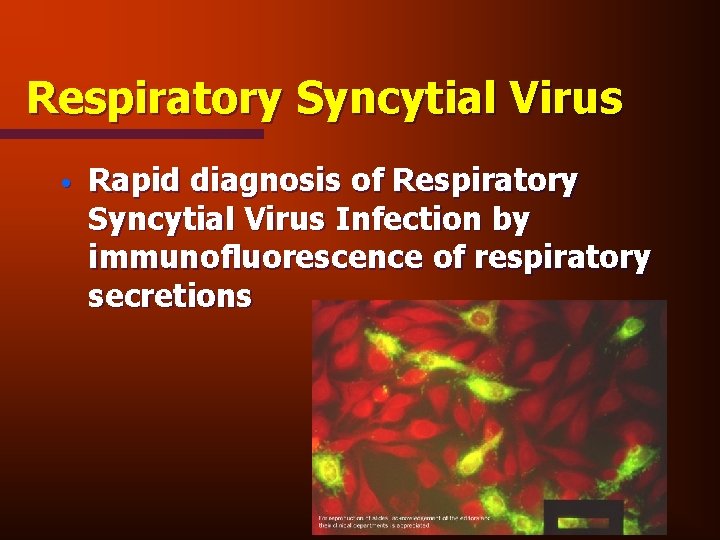
Respiratory Syncytial Virus • Rapid diagnosis of Respiratory Syncytial Virus Infection by immunofluorescence of respiratory secretions

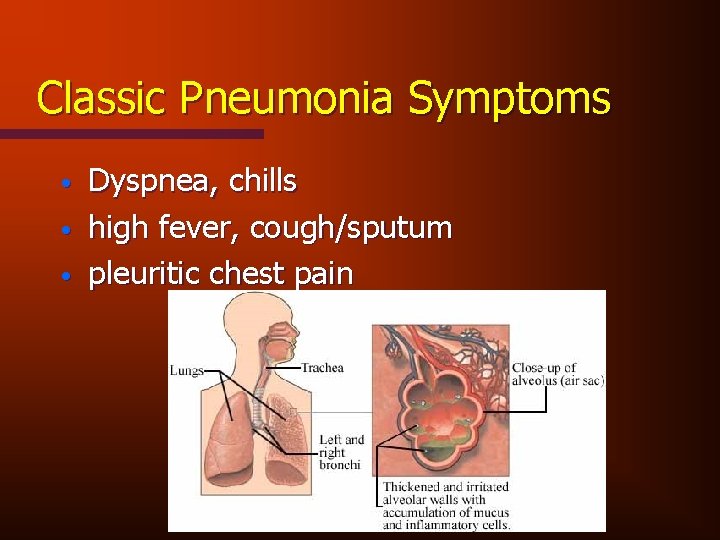
Classic Pneumonia Symptoms • • • Dyspnea, chills high fever, cough/sputum pleuritic chest pain

Viral Pneumonia - symptoms • • Chest Pain Fever Dyspnea Prodrome - malaise, upper respiratory symptoms, and other GI symptoms

Viral pneumonia Clinical Findings • • Minimal/variable Chest exam - may reveal wheezing Fine rales if heard can signify interstitial involvement Chest x-ray - patchy densities or interstitial involvement

Viral pneumonia Management /Prophylaxis • • • Supportive treatment - decrease severity of symptoms bed rest analgesics expectorants Patients w/ • airway obstruction - treat w/bronchodilators • secondary bacterial infection - antibiotics

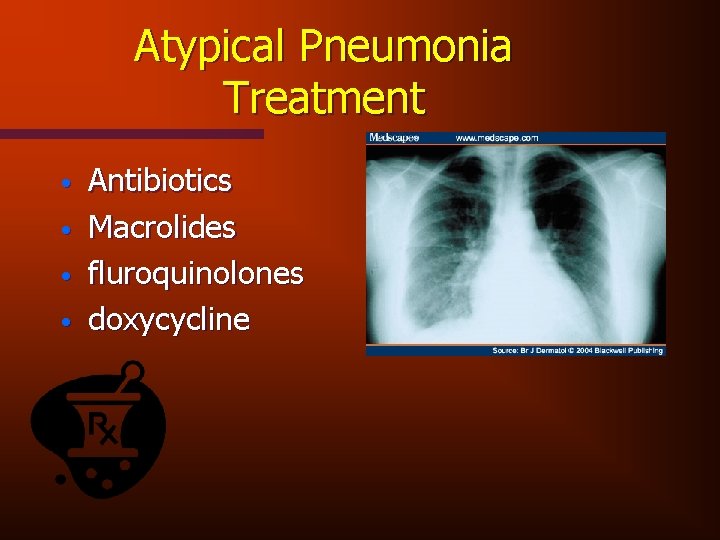
Atypical Pneumonia • • • Accounts for 25% of community acquired pneumonias Mycoplasma/chlamyda/legionella can case extrapulmonary manifestations • meningitis, encephalitis, pericarditis, hepatitis, hemolytic anemia • typically bilateral infiltrates on chest x-ray • primarily effects younger persons

Atypical Pneumonia Treatment • • Antibiotics Macrolides fluroquinolones doxycycline


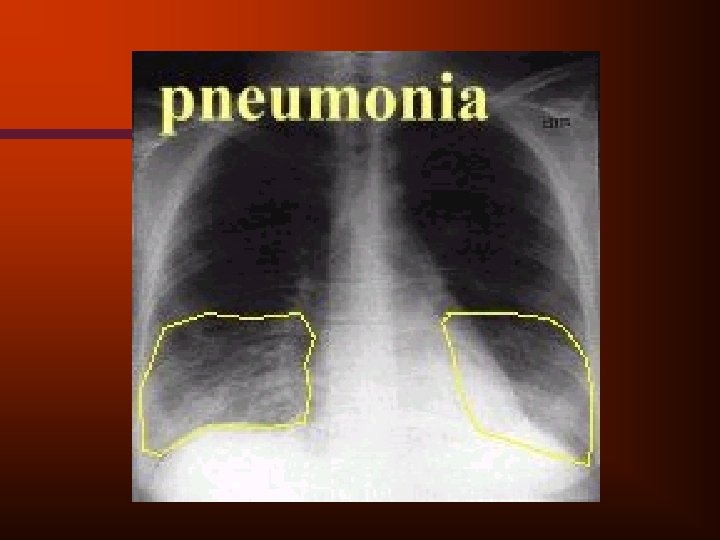
Bacterial pneumonia • • • 3. 3 million cases yearly in US responsible for 10% of hospital admissions unilateral infiltrate on x-ray high mortality in elderly population most common cause pneumococcal followed by haemophilus influenza

• Pneumococcus pneumonia accounts for up to 90% of all bacterial pneumonias • Patients with a chronic Dx are at an increased risk of contracting pneumonia

Bacterial pneumonia presentation • • acute shaking - chills tachypnea tachycardia malaise anorexia myalgias flank or back pain vomiting

Lab Tests • • WBC Chest X-ray Pulse Ox ABGs Sputum exam Blood cultures pleural fluid exam

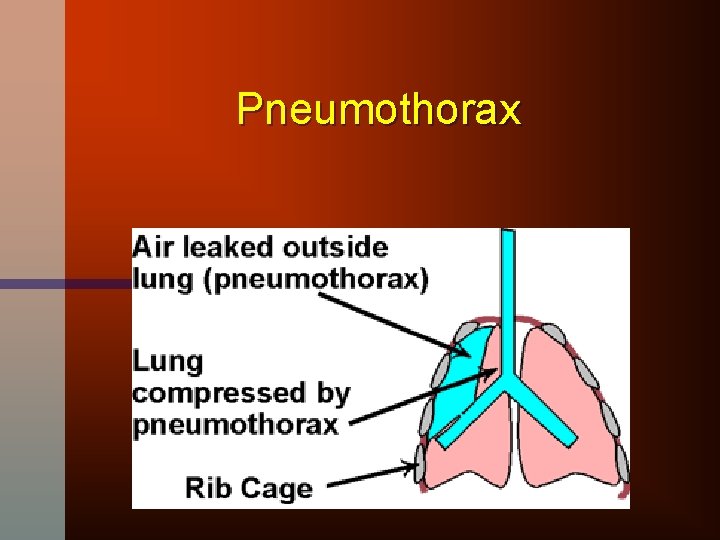
Pneumothorax

Causes of Spontaneous Pneumothorax • Pleural blebs • Bullae • Emphysema • Interstitial lung disease • Alpha 1 antitrypsin deficiency

Traumatic and Iatrogenic Causes • • Penetrating wounds Line placements Lung biopsies Mechanical ventilation

Two most common symptoms • • Dyspnea Chest pain

Physical Examination • • • Decreased breath sounds hyperresonance to percussion decreased tactile fremitus • In patients with emphysema - clinical findings may be subtle

Chest X-ray to Confirm Dx • 500 ml of air required to visualize pneumothorax on x-ray • Characterized by • hyperlucency and lack of lung markings at the periphery of the lung and appearance of fine line that represents the retraction of the visceral from the parietal pleura

Treatment Options • • • Observation - if pneumothorax involves < 15 -20% of hemithorax and patient relatively asymptomatic Tube thoracostomy Simple Aspiration

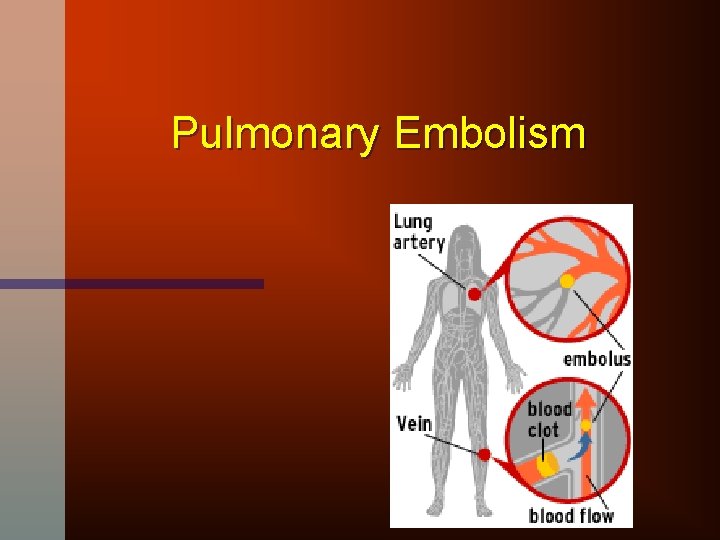
Pulmonary Embolism

PE History • PE is so common and deadly that the dx should be considered in any patient who presents with chest symptoms that cannot be proven to have another cause

PE Risk Markers • • Hypercoagulable states Prior hx of DVT or PE Recent surgery or pregnancy Prolonged immobolization Underlying malignancy smoking birth control pills trauma

Classic triad of signs/symptoms Hemoptysis Dyspnea Chest Pain • These symptoms are not sensitive or specific and occur in fewer than 20% of patients diagnosed with PE

PE Physical Exam • • • Massive PE causes hypotension due to acute cor pulmonale Physical findings in early submassive PE may be completely normal Initially, abnomal findings are absent in most patients with PE

Massive PE - Signs/Symptoms • • • Tachypnea -96% Rales - 58% Accentuated second heart sound - 53% Tachycardia - 44% Fever - 43% S 3 or S 4 gallop - 34% signs/symptoms suggestive of thrombophlebitis - 32% Lower extremity edema - 24% Cardiac murmur - 23% Cyanosis - 19%

Massive PE Diagnostic Studies • • VQ scan Pulmonary angiography CT Echocardiography (TEE) Pulmonary artery catheterization Diagnostic algorithm D-dimer blood gases increased A-a gradient

A-a gradient = predicted p. O 2 – observed PO 2 PAO 2 = (FIO 2 X 713) – (Pa. CO 2/0. 8) at sealevel PAO 2 = 150 -(Pa. CO 2/0. 8) at sealevel on room air Normal range 10 -15 mm > 30 years of age Normal range 8 mm < 30 years of age Increased A-a. DO 2=diffusion defect Right to left shunt V/Q mismatch

Examples • • • A doubel overdose brings two 30 yr old patients to the ED. Both have ingested substantial amounts of barbiturates and diazepam. Blood gases drawn on room air revealed these values: patient 1 - p. H =7. 18, PCO 2 = 70 mm. Hg, PO 2=50 mm. Hg, HCO 3=24 m. Eq/L; patient 2 - p. H =7. 31, PCO 2=50 mm. Hg, PO 2=50 mm. Hg, HCO 3=25 m. Eq/L

Comment • • The A-a gradient calculation for patient 1 is as follows: A-a DO 2 = PAO 2 – Pa. O 2 PAO 2 = 150 – (1. 25 x PCO 2) PAO 2 = 150 – (1. 25 x 70) PAO 2 = 62 A-a =62 – 50 A-a = 12

Comment • The calculation reveals a normal gradient, indicating that the etiology for hypoxemia and hypoventilation is extrinsic to the lung itself.

Comment • • • The A-a gradient calculation for patient 2 is as follows: PAO 2 = 150 – (1. 25 x PCO 2) PAO 2 = 150 – (1. 25 x 50) PAO 2 = 150 – 63 PAO 2 = 87 Therefore, A-a = 87 – 50 =37 (an abnormally increased gradient)

Comment • • We can be reasonably confident that patient 1 suffered hypoventilation due to the effect of the ingested drugs on the brain stem. Temporary mechanical ventilation restored this patient’s gas exchange.

Comment • • Patient 2, on the other hand, had an increased A-a gradient, indicating a lung problem in addition to any central cause for hypoventilation. The chest x-ray film revealed that this patient’s overdose was complicated by aspiration pneumonitis and that the patient required treatment with antibiotics in addition to mechanical ventilation.

Treatment Strategies • • • Fluid administration anticoagulation Vena caval interruption Thrombolytics oxygen pulse ox

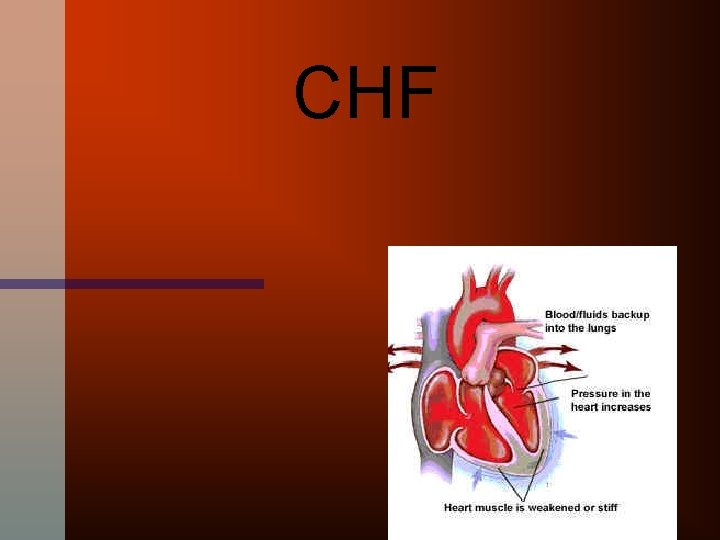
CHF

Left sided Failure • Blood/fluid back-up into the lungs result in • SOB • Fatigue • Cough (especially at night) • PND • orthopnea

Right sided Failure • Build-up of fluid in the veins • Edema of feet, legs and ankles • may effect liver/portal circulation and 3 rd spacing into soft tissue/ascites/pleural effusion

Causes of CHF • Variety of cardiac diseases • Most common cause of CHF - CAD • other causes - valvular heart dx, HTN, cardiomyopathies, myocarditis, renal dx, fluid overload, liver dx w/loss of protein and osmotic forces, high altitude and many others

Physical Findings • • • Peripheral edema JVD tachycardia tachypnea, using accessory muscles of respiration Skin - diaphoretic/cold/gray/cyanotic Wheezing/rales on ausculation Apical impulse displaced laterally ascites hepatosplenomegaly

Diagnostic Work-Up • • History Physical exam EKG Echo Chest x-ray BNP ABG/pulse ox

Treatment • • • Diuretics Digitalis Peripheral vasodilators/NTG Positive inotropic agents ACE inhibitors Beta blockers Oxygen MS 04 BNP

• Respiratory distress is FRIGHTENING! • Feelings of confinement, claustrophobia, restlessness, and anxiety accompany a realization that DEATH may be imminent. • All of this, in a patient that is, most likely, normally mentated and aware of what is happening. • If you never before had any reason to "dig deep" and draw out true human compassion for a patient, THIS IS THE TIME TO DO IT!

Questions ?