Pediatrics Respiratory Emergencies Respiratory Emergencies n 1 cause



















































- Slides: 56

Pediatrics Respiratory Emergencies

Respiratory Emergencies n #1 cause of – – Pediatric hospital admissions Death during first year of life except for congenital abnormalities

Respiratory Emergencies Most pediatric cardiac arrest begins as respiratory failure or respiratory arrest

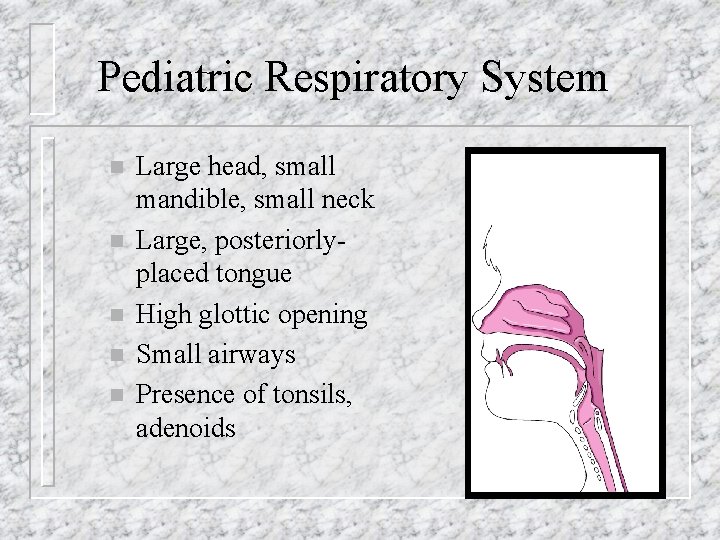
Pediatric Respiratory System n n n Large head, small mandible, small neck Large, posteriorlyplaced tongue High glottic opening Small airways Presence of tonsils, adenoids

Pediatric Respiratory System Poor accessory muscle development n Less rigid thoracic cage n Horizontal ribs, primarily diaphragm breathers n Increased metabolic rate, increased O 2 consumption n

Pediatric Respiratory System Decrease respiratory reserve + Increased O 2 demand = Increased respiratory failure risk

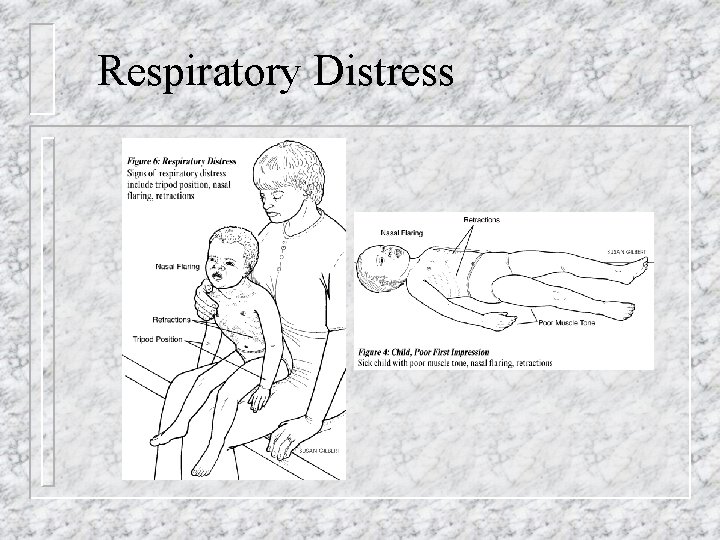
Respiratory Distress

Respiratory Distress n n Tachycardia (May be bradycardia in neonate) Head bobbing, stridor, prolonged expiration Abdominal breathing Grunting--creates CPAP

Respiratory Emergencies Croup n Epiglottitis n Asthma n Bronchiolitis n Foreign body aspiration n

Laryngotracheobronchitis Croup

Croup: Pathophysiology n n n Viral infection (parainfluenza) Affects larynx, trachea Subglottic edema; Air flow obstruction

Croup: Incidence 6 months to 4 years n Males > Females n Fall, early winter n

Croup: Signs/Symptoms “Cold” progressing to hoarseness, cough n Low grade fever n Night-time increase in edema with: n – – n Stridor “Seal bark” cough Respiratory distress Cyanosis Recurs on several nights

Croup: Management n Mild Croup – – Reassurance Moist, cool air

Croup: Management n Severe Croup – – – Humidified high concentration oxygen Monitor EKG IV tko if tolerated Nebulized racemic epinephrine Anticipate need to intubate, assist ventilations

Epiglottitis

Epiglottitis: Pathophysiology Bacterial infection (Hemophilus influenza) n Affects epiglottis, adjacent pharyngeal tissue n Supraglottic edema n Complete Airway Obstruction

Epiglottitis: Incidence n n n Children > 4 years old Common in ages 4 - 7 Pedi incidence falling due to Hi. B vaccination Can occur in adults, particularly elderly Incidence in adults is increasing

Epiglottitis: Signs/Symptoms Rapid onset, severe distress in hours n High fever n Intense sore throat, difficulty swallowing n Drooling n Stridor n Sits up, leans forward, extends neck slightly n One-third present unconscious, in shock n

Epiglottitis Respiratory distress+ throat+Drooling = Epiglottitis Sore

Epiglottitis: Management High concentration oxygen n IV tko, if possible n Rapid transport n Do not attempt to visualize airway n

Epiglottitis Immediate Life Threat Possible Complete Airway Obstruction

Asthma

Asthma: Pathophysiology n Lower airway hypersensitivity to: – – – Allergies Infection Irritants Emotional stress Cold Exercise

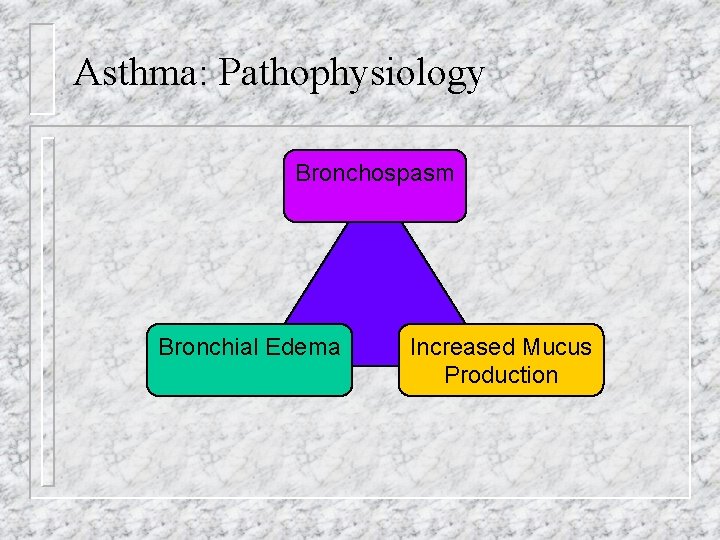
Asthma: Pathophysiology Bronchospasm Bronchial Edema Increased Mucus Production

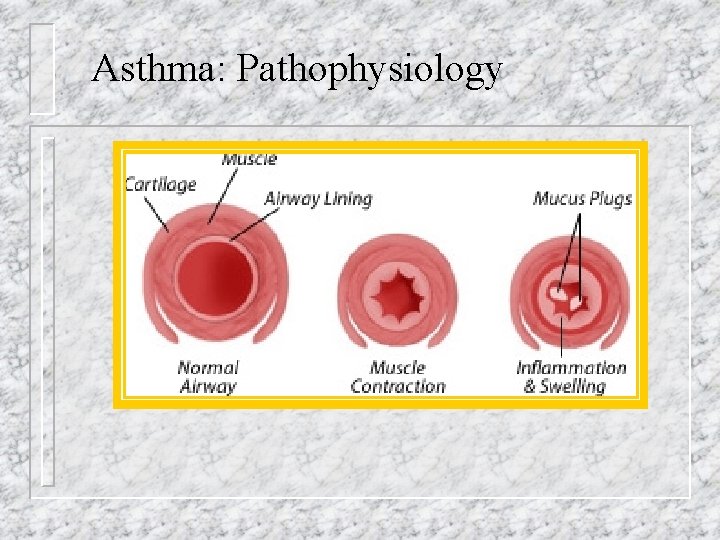
Asthma: Pathophysiology

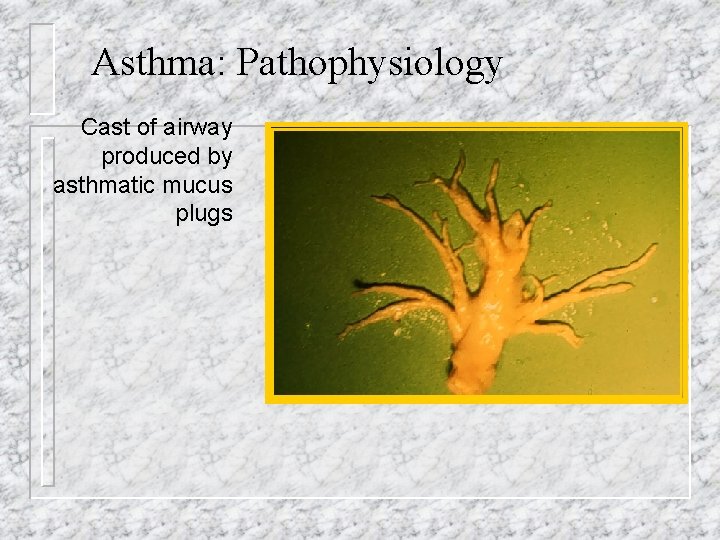
Asthma: Pathophysiology Cast of airway produced by asthmatic mucus plugs

Asthma: Signs/Symptoms Dyspnea n Signs of respiratory distress n – – Nasal flaring Tracheal tugging Accessory muscle use Suprasternal, intercostal, epigastric retractions

Asthma: Signs/Symptoms Coughing n Expiratory wheezing n Tachypnea n Cyanosis n

Asthma: Prolonged Attacks Increase in respiratory water loss n Decreased fluid intake n Dehydration n

Asthma: History How long has patient been wheezing? n How much fluid has patient had? n Recent respiratory tract infection? n Medications? When? How much? n Allergies? n Previous hospitalizations? n

Asthma: Physical Exam Patient position? n Drowsy or stuporous? n Signs/symptoms of dehydration? n Chest movement? n Quality of breath sounds? n

Asthma: Risk Assessment n n n n Prior ICU admissions Prior intubation >3 emergency department visits in past year >2 hospital admissions in past year >1 bronchodilator canister used in past month Use of bronchodilators > every 4 hours Chronic use of steroids Progressive symptoms in spite of aggressive Rx

Asthma n SILENT CHEST= DANGER OF RESPIRATORY FAILURE

Golden Rule ALL THAT WHEEZES IS NOT ASTHMA Pulmonary edema n Allergic reactions n Pneumonia n Foreign body aspiration n

Asthma: Management Airway n Breathing n – – Sitting position Humidified O 2 by NRB mask n Dry – – O 2 dries mucus, worsens plugs Encourage coughing Consider intubation, assisted ventilation

Asthma: Management n Circulation – – IV TKO Assess for dehydration Titrate fluid administration to severity of dehydration Monitor ECG

Asthma: Management n Obtain medication history – – Overdose Arrhythmias

Asthma: Management n Nebulized Beta-2 agents – Albuterol

Asthma: Management n Subcutaneous beta agents – Epinephrine 1: 1000 --0. 1 to 0. 3 mg SQ POSSIBLE BENEFIT IN PATIENTS WITH VENTILATORY FAILURE

Asthma: Management Use EXTREME caution in giving two sympathomimetics to same patient n Monitor ECG n

Asthma: Management n Avoid – Sedatives n Depress – respiratory drive Antihistamines n Decrease – LOC, dry secretions Aspirin n High incidence of allergy

Status Asthmaticus Asthma attack unresponsive to -2 adrenergic agents

Status Asthmaticus Humidified oxygen n Rehydration n Continuous nebulized beta-2 agents n Atrovent n Corticosteroids n Aminophylline (controversial) n Magnesium sulfate (controversial) n

Status Asthmaticus Intubation n Mechanical ventilation n – – n Large tidal volumes (18 -24 ml/kg) Long expiratory times Intravenous Terbutaline – – Continuous infusion 3 to 6 mcg/kg/min

Bronchiolitis

Bronchiolitis: Pathophysiology Viral infection (RSV) n Inflammatory bronchiolar edema n Air trapping n

Bronchiolitis: Incidence Children < 2 years old n 80% of patients < 1 year old n Epidemics January through May n

Bronchiolitis: Signs/Symptoms n n n Infant < 1 year old Recent upper respiratory infection exposure Gradual onset of respiratory distress Expiratory wheezing Extreme tachypnea (60 - 100+/min) Cyanosis

Asthma vs Bronchiolitis n Asthma – – – Age - > 2 years Fever - usually normal Family Hx - positive Hx of allergies - positive Response to Epi - positive n Bronchiolitis – – – Age - < 2 years Fever - positive Family Hx - negative Hx of allergies - negative Response to Epi - negative

Bronchiolitis: Management Humidified oxygen by NRB mask n Monitor EKG n IV tko n Anticipate order for bronchodilators n Anticipate need to intubate, assist ventilations n

Foreign Body Airway Obstruction FBAO

FBAO: High Risk Groups > 90% of deaths: children < 5 years old n 65% of deaths: infants n

FBAO: Signs/Symptoms n Suspect in any previously well, afebrile child with sudden onset of: – – – Respiratory distress Choking Coughing Stridor Wheezing

FBAO: Management Minimize intervention if child conscious, maintaining own airway n 100% oxygen as tolerated n No blind sweeps of oral cavity n Wheezing n – – Object in small airway Avoid trying to dislodge in field

FBAO: Management n Inadequate ventilation – – Infant: 5 back blows/5 chest thrusts Child: Abdominal thrusts