Heat IllnessHyperthermia Victor Politi M D FACP Medical
































- Slides: 35

Heat Illness/Hyperthermia Victor Politi, M. D. , FACP Medical Director – St. Johns University-Physician Assistant Program


Risk factors for heat illness Obesity Fatigue Drugs Alcohol Sunburn Unacclimatized Fluid deficit Previous history of heat injury Many medical conditions Febrile illness Cystic fibrosis Diabetes Malnutrition

Heat Illness Classification • Heat Rash • Heat syncope • Heat cramps • Heat exhaustion • Heat stroke


Minor Heat Illness Heat Cramps • Brief, intermittent, often severe muscular cramps typically occurring in muscles that are fatigued by heavy work • Usually occur after exertion • Copious hypotonic fluid replacement during exertion

Minor Heat Illness Heat Cramps • Related to salt deficiency • Victims exhibit -hyponatremia, hypochloremia, low urinary sodium and chloride levels • Usually rapidly relieved by salt solutions

Minor Heat Illness Heat Syncope • Individuals at risk should be warned to move frequently, flex leg muscles repeatedly whenever standing • Scintillating scotomata, tunnel vision, vertigo, nausea, diaphoresis, and weakness are prodromal symptoms of syncope • Adequate oral volume replacement may prevent some conditions

Minor Heat Illness - Prickly Heat AKA miliaria rubra, lichen tropicus, heat rash • Acute phase – Produces intensely pruritic vesicles on an erythematous base – Rash confined to clothed areas – Effected area completely anhydrotic • – may persist for weeks – chronic dermatitis -frequent complication

Heat Exhaustion - two types classically described – Water depletion heat exhaustion • inadequate fluid replacement by persons in heat “ voluntary dehydration” • weakness, fatigue, frontal headache, impaired judgement, vertigo, nausea/vomiting, occasional muscle cramps, sweating, body temperature near normal • orthostatic dizziness/syncope may occur • results in progressive hypovolemia • Untreated can progress to heat stroke

Heat Exhaustion - two types classically described • Salt depletion heat exhaustion – takes longer to develop than water depletion form – systemic symptoms occur – hyponatremia, hypochloremia, low urinary sodium and chloride concentrations – Symptoms similar to water depletion type, body temperature remains near normal

Heat Exhaustion: Diagnosis • Vague malaise, fatigue, headache • Core temperature often normal; if elevated less than 1040 F • Mental function essentially intact; no coma or seizures • Tachycardia, orthostatic hypotension, clinical dehydration (may occur) • Other major illness ruled out • If in doubt, --- treat as heat stroke !!


Heat Exhaustion - Treatment • Rest • cool environment • Assess volume status (orthostatic changes, BUN, hematocrit, serum sodium) • Fluid replacement • Consider admission if patient is elderly, has significant electolyte abnormalities or would be at risk of recurrence if d/c

Hyperthermia A patient presents to the ED with elevated body temperature 1 st thought ? ? ? Infectious etiologies/severe infection but some patients with elevated temperature, including some with extreme pyrexia, do not have fever at all, they have hyperthermia !

Fever versus Hyperthermia • Body temperature can become elevated through either of two very different processes • In fever, thermoregulation remains intact while hyperthermia represents thermoregulation failure


Causes of Hyperthermia. Disorders of excessive heat production – Exertional hyperthermia – Heatstroke – Malignant hyperthermia of anesthesia – Neuroleptic malignant syndrome – Thyrotoxicosis / Pheochromocytoma – Salicylate intoxication / Delirium tremens – Cocaine, amphetamines, other drugs of abuse – Status epilepticus /Generalized tetanus

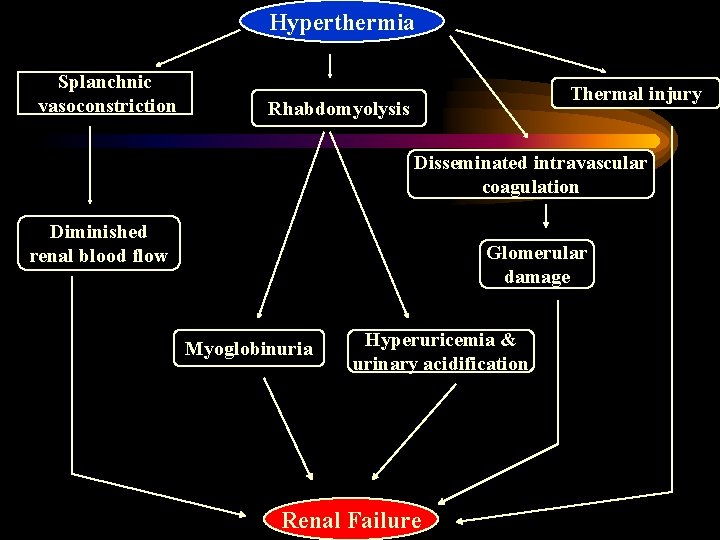
Hyperthermia Splanchnic vasoconstriction Thermal injury Rhabdomyolysis Disseminated intravascular coagulation Diminished renal blood flow Glomerular damage Myoglobinuria Hyperuricemia & urinary acidification Renal Failure

A catastrophic life-threatening medical emergency --- HEAT STROKE

Heat Stroke Diagnosis • Exposure to heat stress, endogenous or exogenous • Signs of severe CNS dysfunction (coma, seizures, delirium • Core temperature usually 410 C (105. 80 F) or more, • Dry, hot skin frequent, • Marked elevation of hepatic transaminases


Classic Heatstroke • Occurs primarily in epidemics during summer heat waves • Most likely to effect the elderly and patients with serious underlying illnesses • Infants also at risk • Typical victim confined at home w/no fan or A/C • Dehydration - predisposing factor

Classic Heatstroke • Other risk factors - obesity, neurologic or cardiovascular disease, use of diuretics, neuroleptics, or medications with anticholinergic properties that interfere with sweating • Alcohol use may be a risk factor

Exertional Heat Stroke • Like classic heat stroke- occurs during hot, humid weather • Occurs sporadically - effecting young, healthy persons engaged in strenuous physical activity

Initial Treatment of Heat Stroke • Immediate cooling • Protect airway (intubate if comatose or seizing) • IV line with 0. 9% Na. Cl or Ringer’s lactate • CVP or Swan Ganz catheter in hypotensive patients • Foley catheter; monitor output

Initial Treatment of Heat Stroke • • Rectal probe - monitor temperature Oxygen, 5 -10 L/min ABGs Labs - CBC, electrolytes, BUN, glucose, SGOT, LDH, CPK, calcium phosphate, lactate, PT/PTT, fibrin degradation products • Check glucose by dextrostix method & treateadminister D 50 if hypoglycemia present

Cooling Modalities to lower body temperature in heat stroke • Ice-water immersion • Evaporative cooling using large circulating fans and skin wetting • Ice packs • Peritoneal lavage • Rectal lavage • Gastric lavage • Cardiopulmonary bypass • Alcohol sponge baths (caution) • Phenothiazines (caution)

Treatment of early complications of Heat Stroke • • • Shivering Convulsions Myoglobinuria Acidosis Hypokalemia Hypocalcemia


Heat Illness Prevention • A Crucial issue • Counsel persons with any risk factors regarding symptoms of heat stroke – Elderly persons – persons with chronic diseases – those on medications predisposing them to heat illness

Heat Illness Prevention • Exertional heat stroke is most likely to strike young, healthy persons involved in strenuous physical activity – many of these people have risk factors for heat illness -commonly obesity, diarrhea, febrile illness – other variables to consider- hydration, salt intake, clothing, and climatic conditions

Heat Illness Prevention • Fluid intake is the most critical variable


Questions ?
 Dr victor politi
Dr victor politi Victor politi
Victor politi Victor politi
Victor politi Victor politi
Victor politi Rachel politi
Rachel politi Latent heat dimension
Latent heat dimension Typically involves high heat with 300°f or hotter
Typically involves high heat with 300°f or hotter Thermal capacity
Thermal capacity Difference between medical report and medical certificate
Difference between medical report and medical certificate Torrance memorial map
Torrance memorial map Ptal california medical board
Ptal california medical board Cartersville medical center medical records
Cartersville medical center medical records Gbmc medical records
Gbmc medical records Caracterizarea personajului realist
Caracterizarea personajului realist Victor manuel castaño
Victor manuel castaño Victor hurtig
Victor hurtig Escultor benjamin victor
Escultor benjamin victor Victor bocangel puclla
Victor bocangel puclla Un deseo victor hugo
Un deseo victor hugo Victor vocabulary
Victor vocabulary Didtica
Didtica Victor adamchik
Victor adamchik Victor veliadis
Victor veliadis Victor hsiao
Victor hsiao Victor spinski
Victor spinski Vector victor meaning
Vector victor meaning Victor le grand
Victor le grand Victor pestov
Victor pestov Tabela bidimensional
Tabela bidimensional Victor waldmann
Victor waldmann Universitatea de medicină și farmacie victor babeș
Universitatea de medicină și farmacie victor babeș Victor molev
Victor molev Casa doru
Casa doru Les contemplations aurore
Les contemplations aurore Victor shoup
Victor shoup Victor oder die kinder an der macht
Victor oder die kinder an der macht