Periodontal Flap Surgery Purpose 1 To gain access














- Slides: 60

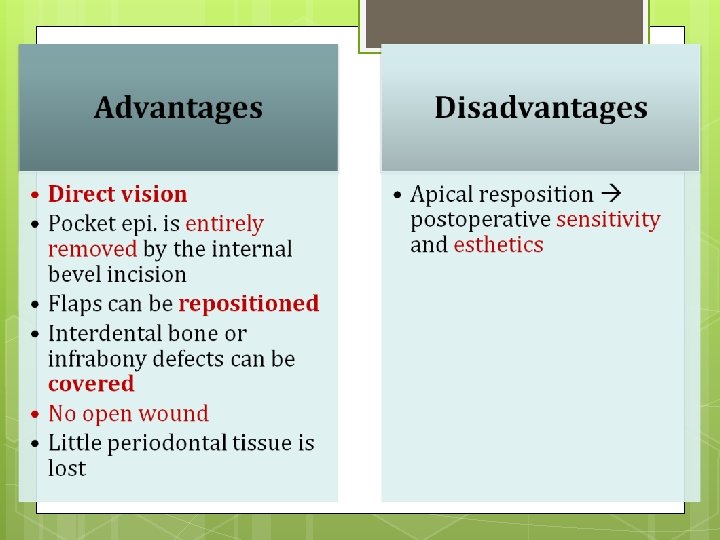
Periodontal Flap Surgery

Purpose 1. To gain access to deeper periodontal structures with direct vision. 2. Relocation of the frenulum 3. Maintenance of the attached tissue 4. Pocket elimination and regeneration

Indications • • • Pockets > 5 mm persisting after phase I therapy Bony pockets and interdental craters Bony lesions in the furcations Need for surgical crown lengthening When to open up a flap? complicated morphology like: – Deep and narrow pocket – Difficult to achieve the correct angle

Contraindications • Shallow, supraalveolar pockets – subgingival scaling/rootplaning • Esthetically sensitive areas • Fibrous thickened gingiva – gingivectomy more favorable morphology


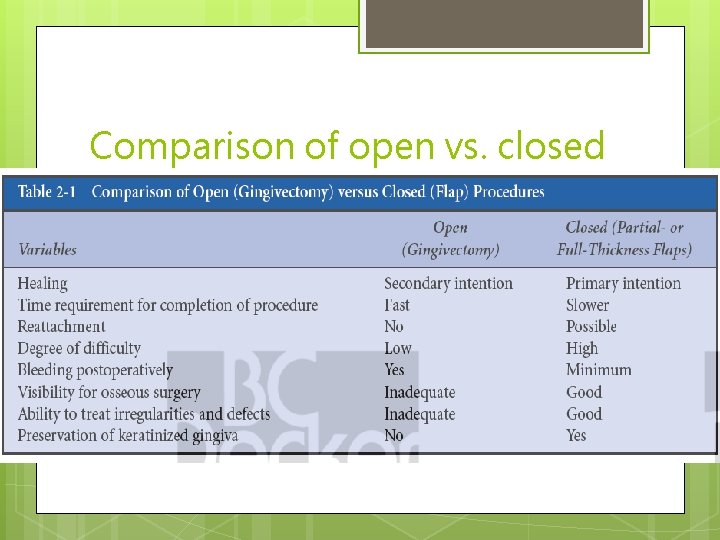
Comparison of open vs. closed

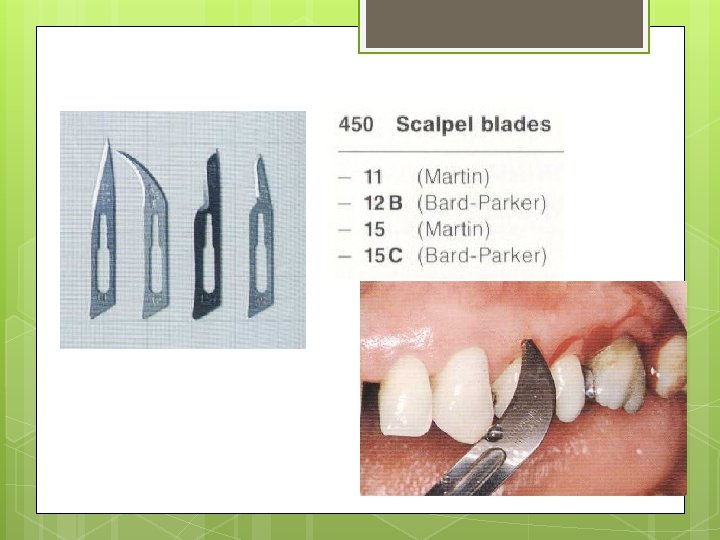
Instruments

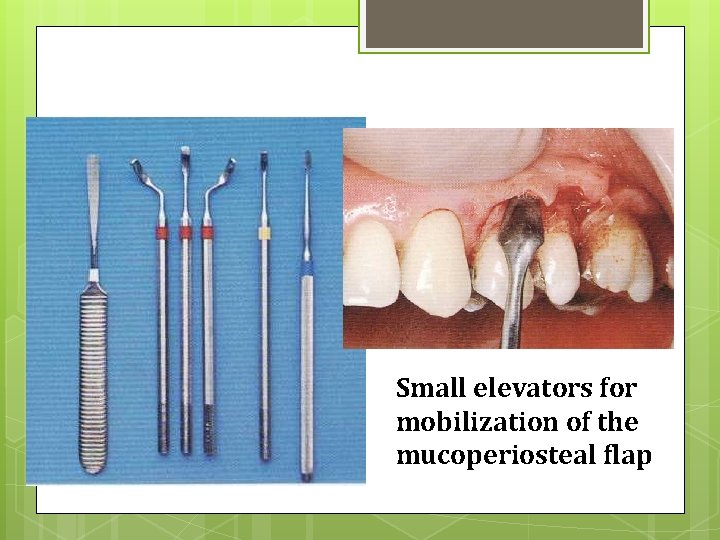
Instruments Small elevators for mobilization of the mucoperiosteal flap

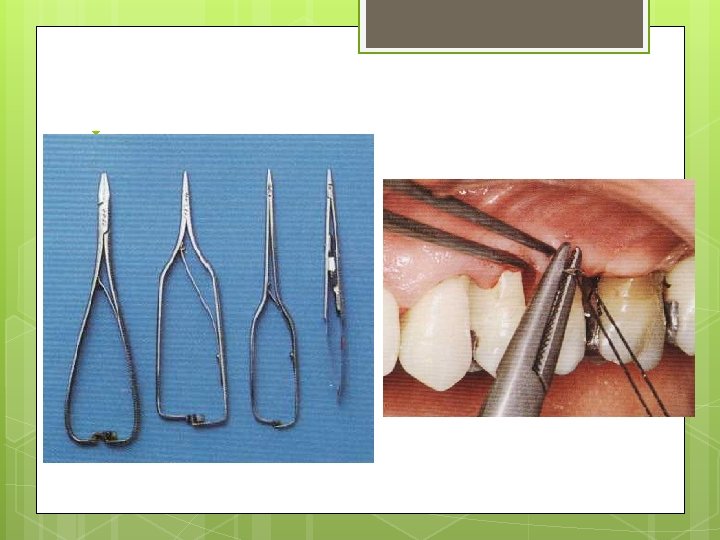
Instruments

• Principles of Flap Design Local flap 1. 2. 3. 4. 5. outlined by a surgical incision carries its own blood supply allows surgical access to underlying tissues can be replaced in the original position can be maintained with sutures and is expected to heal ü Used in oral surgical, periodontic, and endodontic procedures to gain access.

Principles of Flap Design • Complications A. Flap necrosis B. Flap Dehiscence C. Flap Tearing D. Injury to Local Structures

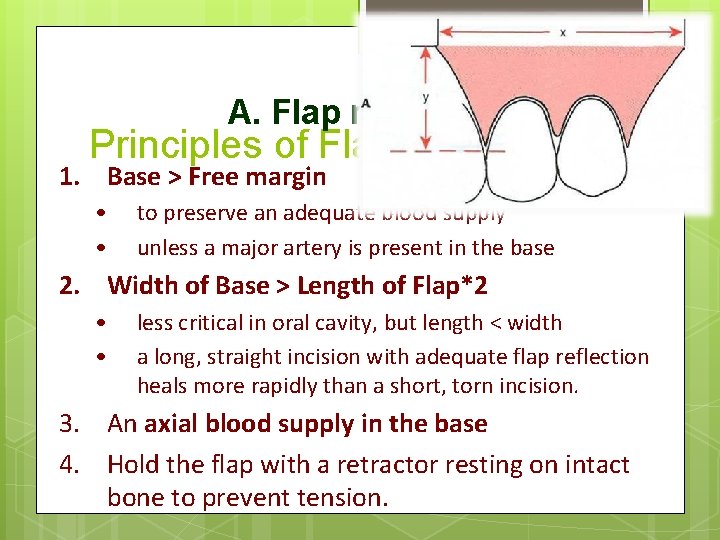
A. Flap necrosis Principles of Flap Design 1. Base > Free margin • • to preserve an adequate blood supply unless a major artery is present in the base 2. Width of Base > Length of Flap*2 • • less critical in oral cavity, but length < width a long, straight incision with adequate flap reflection heals more rapidly than a short, torn incision. 3. An axial blood supply in the base 4. Hold the flap with a retractor resting on intact bone to prevent tension.

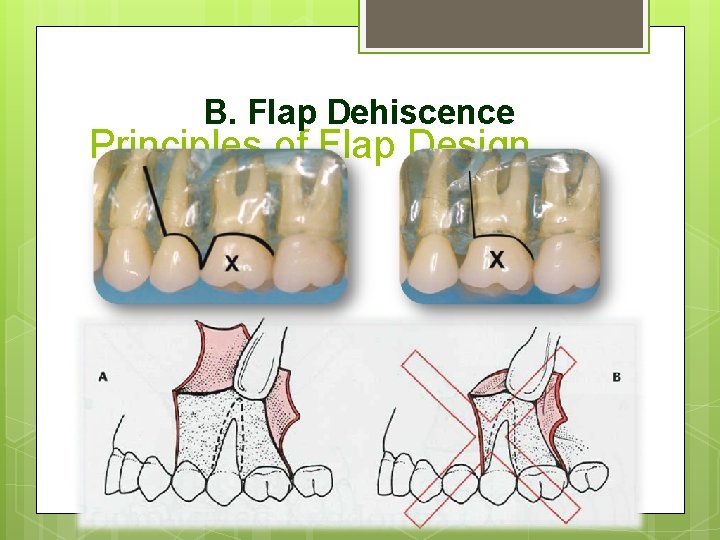
B. Flap Dehiscence Principles of Flap Design 1. The incisions must be made over intact bone 2. If the pathologic condition has eroded the buccocortical plate, the incision must be at least 6 or 8 mm away from it. 3. The incision is 6 to 8 mm away from the bony defect created by surgery. 4. Gently handle the flap's edges 5. Do not place the flap under tension 6. Do not cross bony prominences, ex: canine eminence

B. Flap Dehiscence Principles of Flap Design

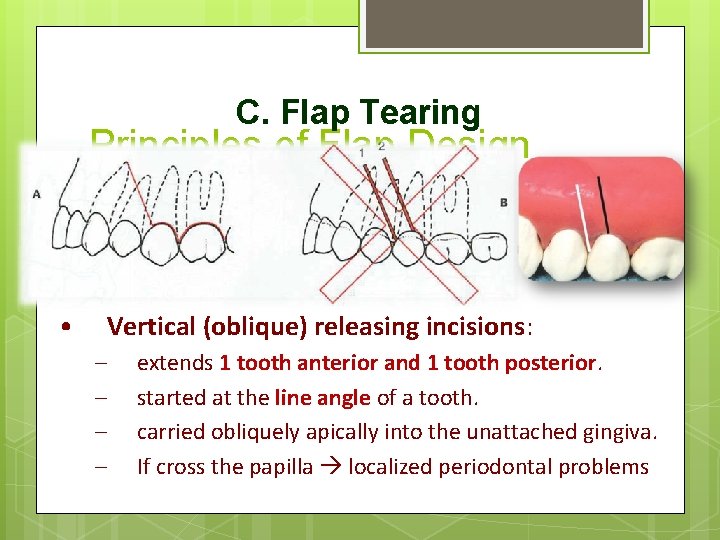
C. Flap Tearing • Principles of Flap Design Envelope flaps – – an incision around the necks of several teeth. extends 2 teeth anterior and 1 tooth posterior. If not provide sufficient access… • Vertical (oblique) releasing incisions: – – extends 1 tooth anterior and 1 tooth posterior. started at the line angle of a tooth. carried obliquely apically into the unattached gingiva. If cross the papilla localized periodontal problems

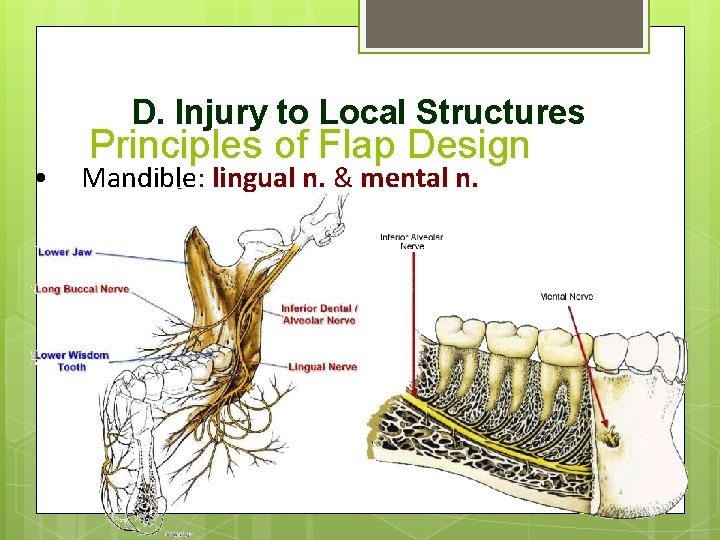
D. Injury to Local Structures • Principles of Flap Design Mandible: lingual n. & mental n.

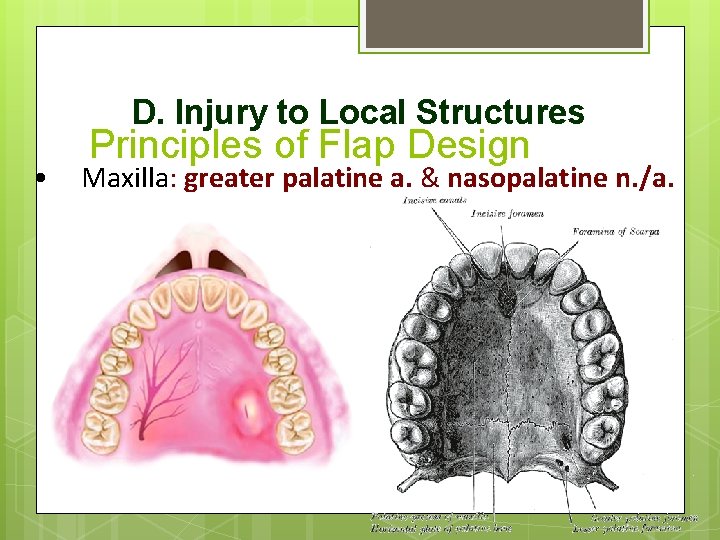
D. Injury to Local Structures • Principles of Flap Design Maxilla: greater palatine a. & nasopalatine n. /a.

Basic Incisions • Can be sulcular, crestal, or inverse bevel

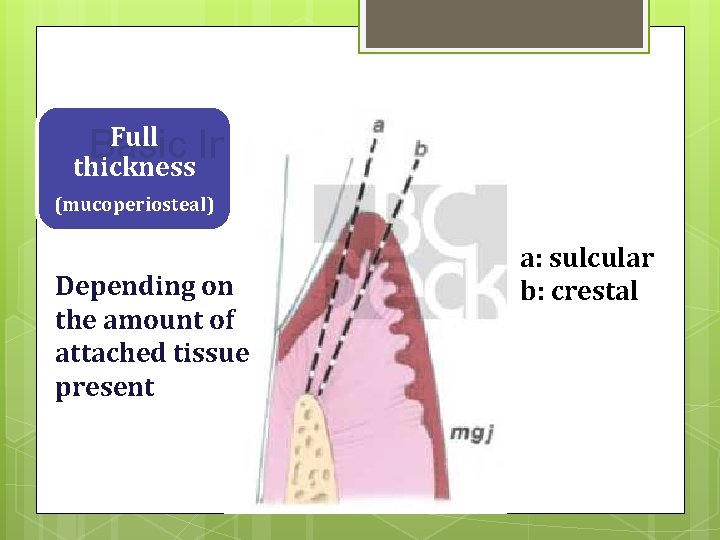
Full Incisions Basic thickness (mucoperiosteal) Depending on the amount of attached tissue present a: sulcular b: crestal

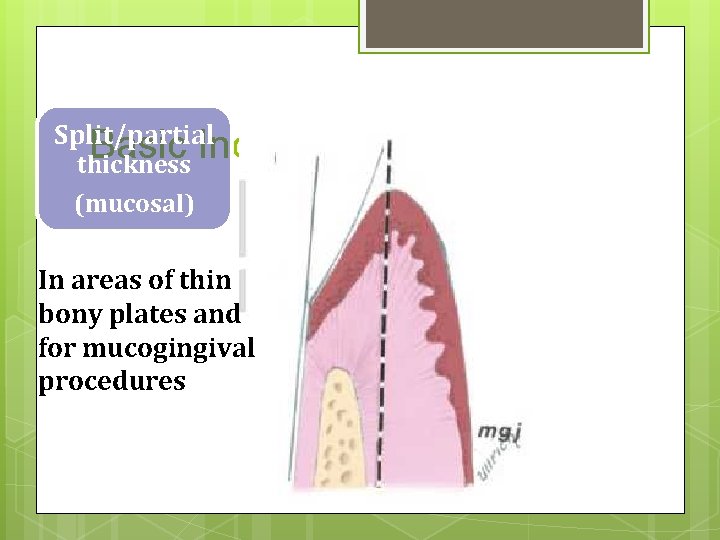
Split/partial Basic Incisions thickness (mucosal) In areas of thin bony plates and for mucogingival procedures

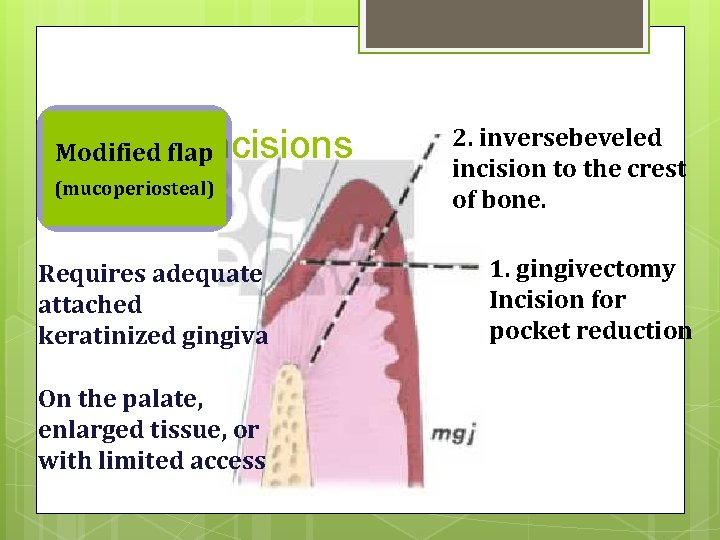
Basicflap. Incisions Modified (mucoperiosteal) Requires adequate attached keratinized gingiva On the palate, enlarged tissue, or with limited access 2. inversebeveled incision to the crest of bone. 1. gingivectomy Incision for pocket reduction

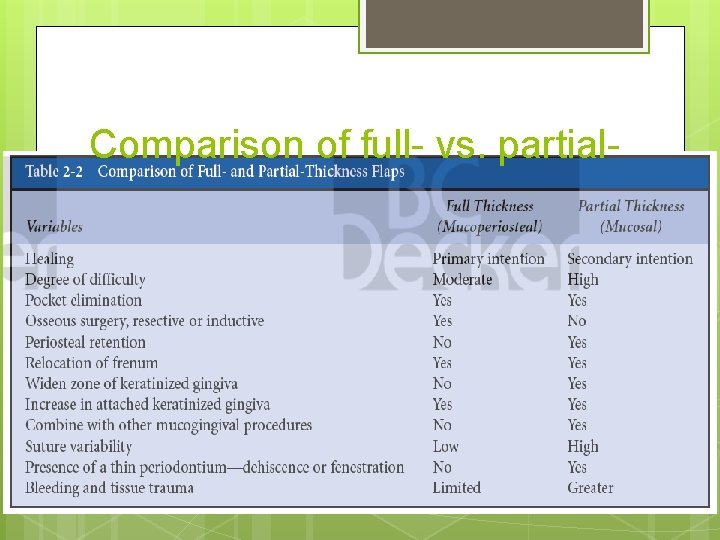
Comparison of full- vs. partial-

Types of Mucoperiosteal Flaps 1. Envelope/sulcular incision 2. Envelope with one releasing incision (threecorner flap) 3. Envelope with two releasing incisions (fourcorner flap) Full-thickness mucoperiosteal flap

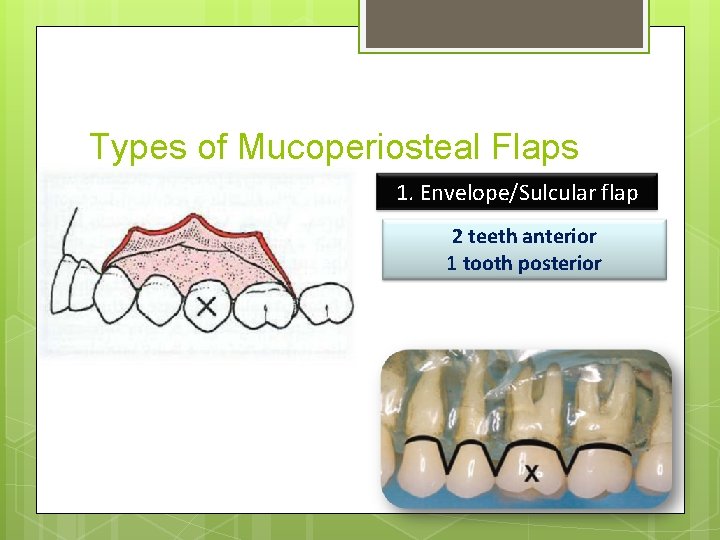
Types of Mucoperiosteal Flaps 1. Envelope/Sulcular flap 2 teeth anterior 1 tooth posterior

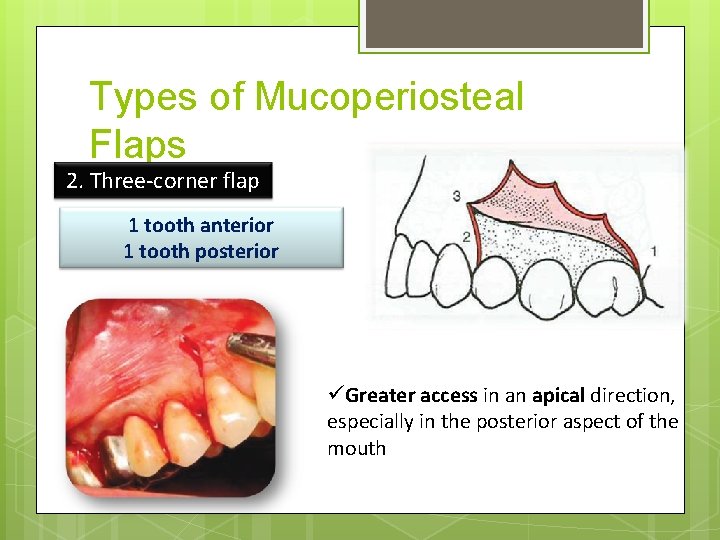
Types of Mucoperiosteal Flaps 2. Three-corner flap 1 tooth anterior 1 tooth posterior üGreater access in an apical direction, especially in the posterior aspect of the mouth

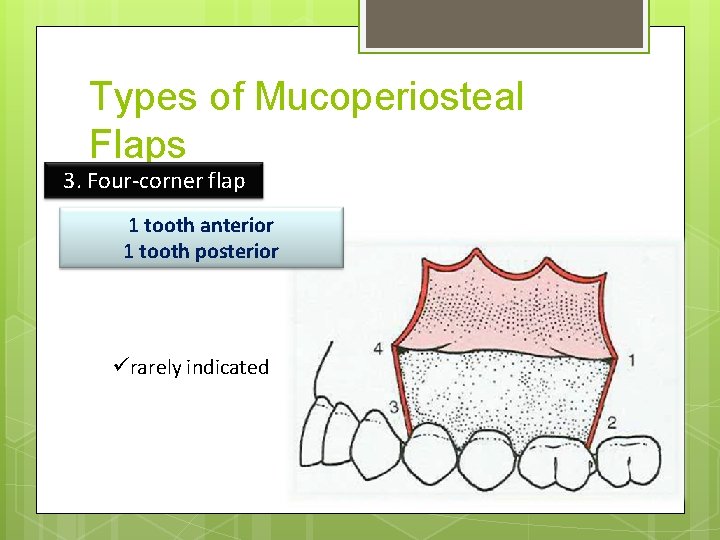
Types of Mucoperiosteal Flaps 3. Four-corner flap 1 tooth anterior 1 tooth posterior ürarely indicated

Common Periodontal Flap

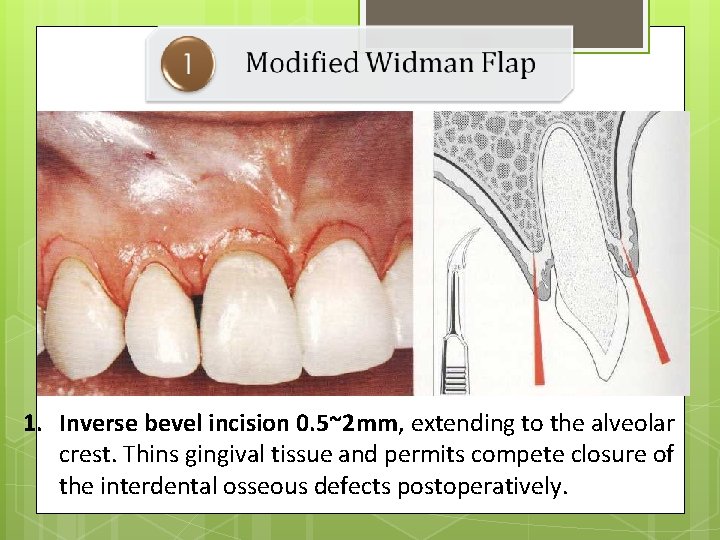
1. Inverse bevel incision 0. 5~2 mm, extending to the alveolar crest. Thins gingival tissue and permits compete closure of the interdental osseous defects postoperatively.

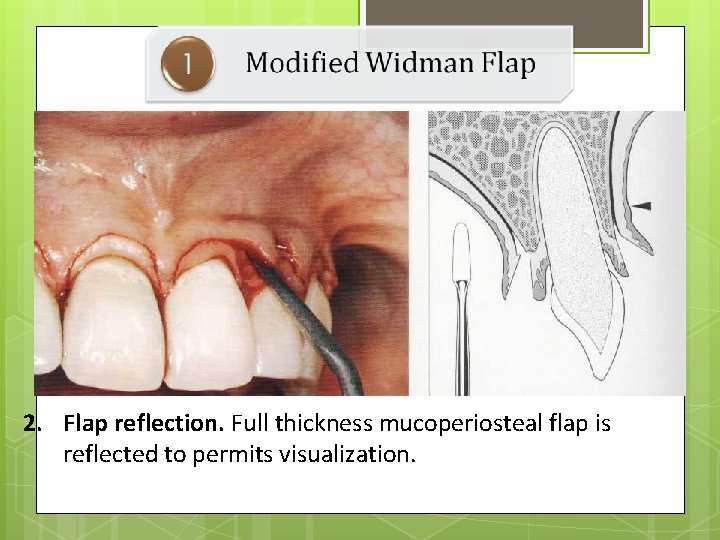
2. Flap reflection. Full thickness mucoperiosteal flap is reflected to permits visualization.

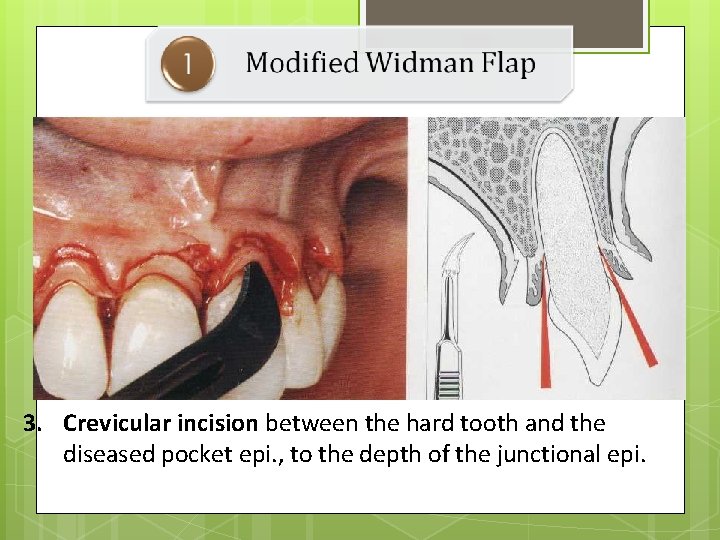
3. Crevicular incision between the hard tooth and the diseased pocket epi. , to the depth of the junctional epi.

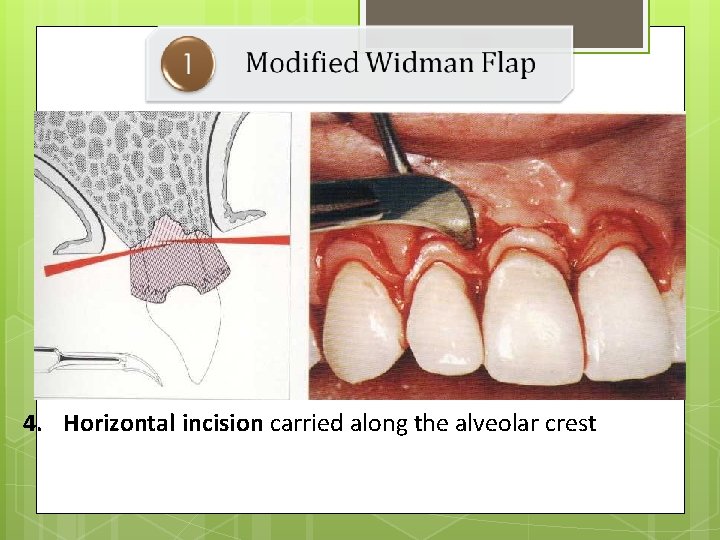
4. Horizontal incision carried along the alveolar crest

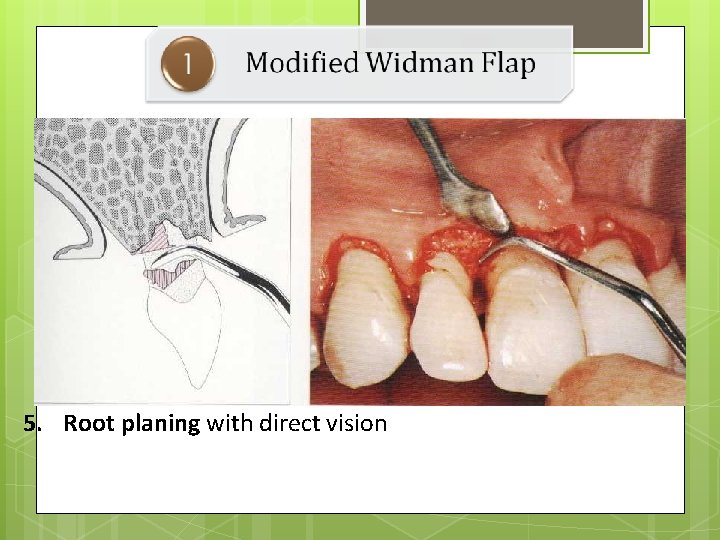
5. Root planing with direct vision

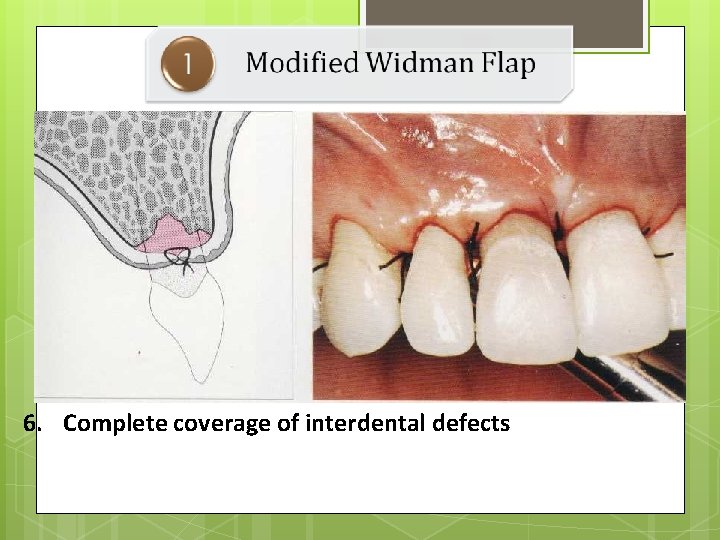
6. Complete coverage of interdental defects

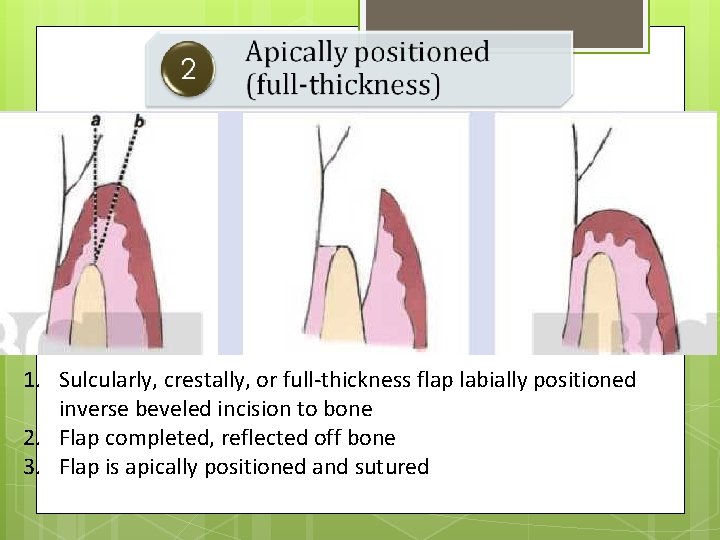
1. Sulcularly, crestally, or full-thickness flap labially positioned inverse beveled incision to bone 2. Flap completed, reflected off bone 3. Flap is apically positioned and sutured

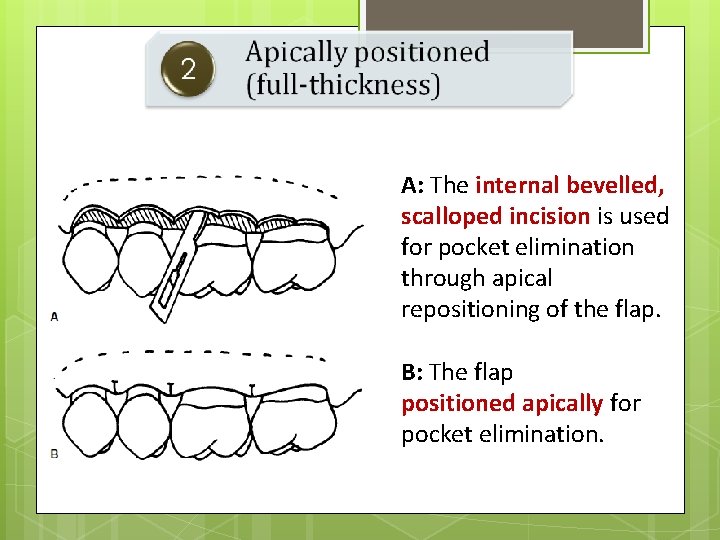
A: The internal bevelled, scalloped incision is used for pocket elimination through apical repositioning of the flap. B: The flap positioned apically for pocket elimination.

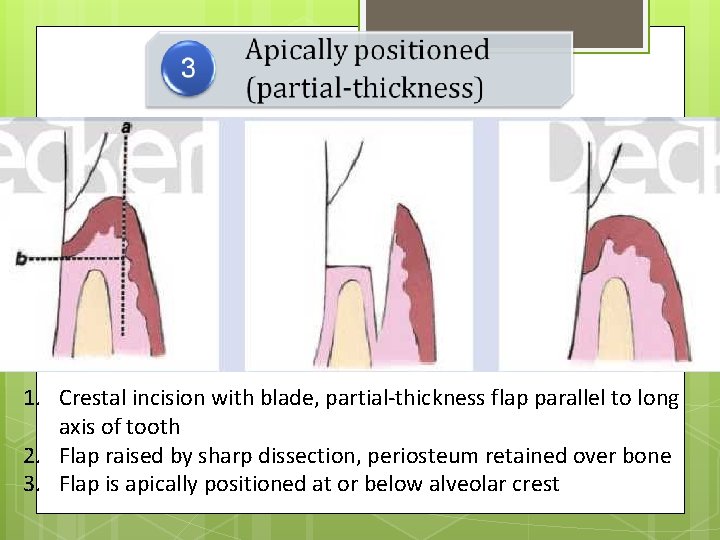
1. Crestal incision with blade, partial-thickness flap parallel to long axis of tooth 2. Flap raised by sharp dissection, periosteum retained over bone 3. Flap is apically positioned at or below alveolar crest

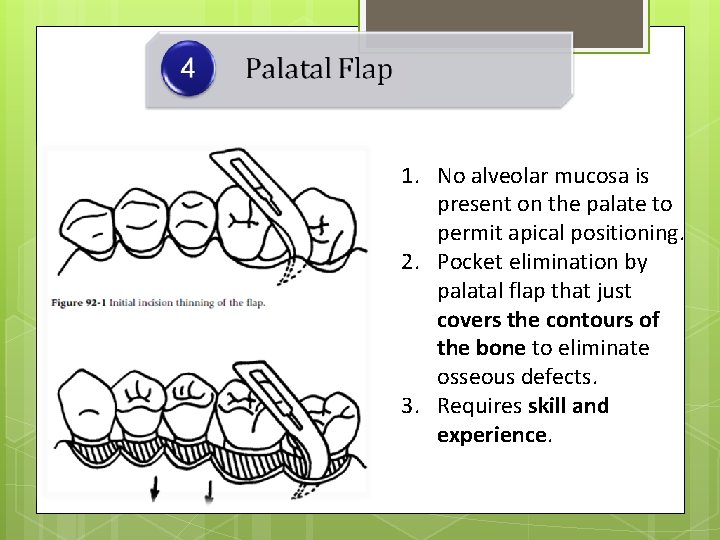
1. No alveolar mucosa is present on the palate to permit apical positioning. 2. Pocket elimination by palatal flap that just covers the contours of the bone to eliminate osseous defects. 3. Requires skill and experience.

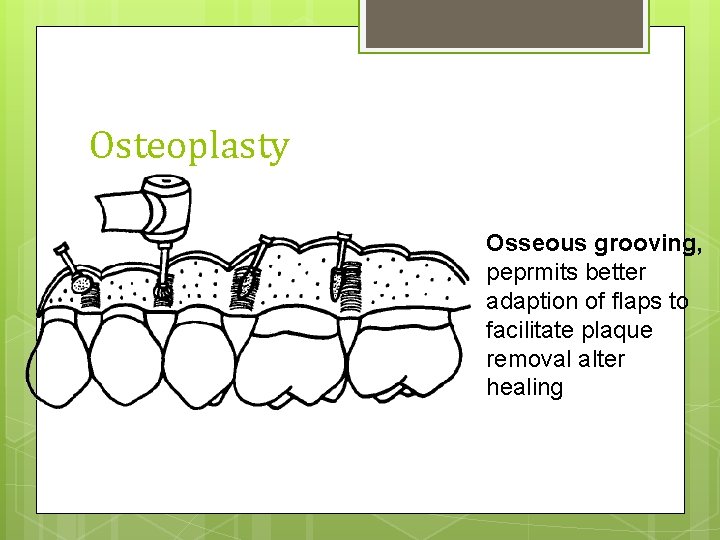
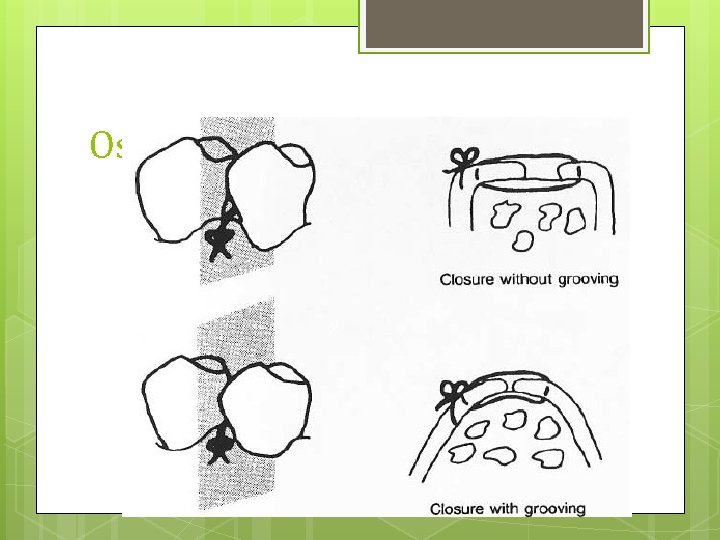
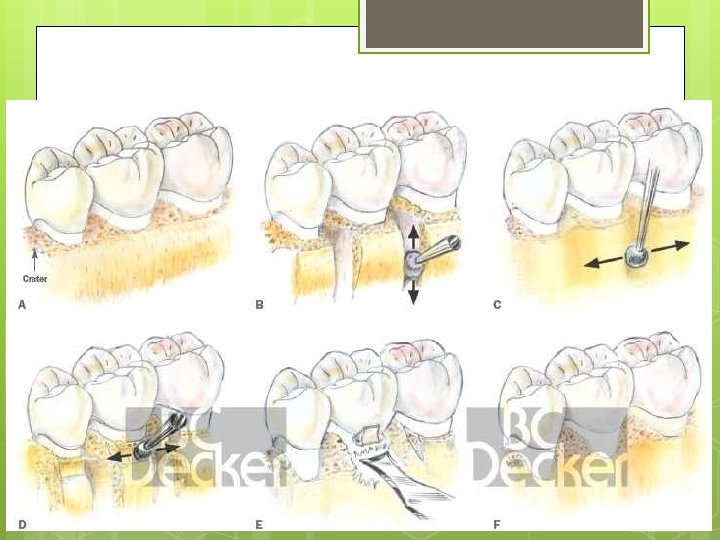
Osteoplasty Osseous grooving, peprmits better adaption of flaps to facilitate plaque removal alter healing

Osteoplasty

Osteoplasty

Suturing for Flap Surgery

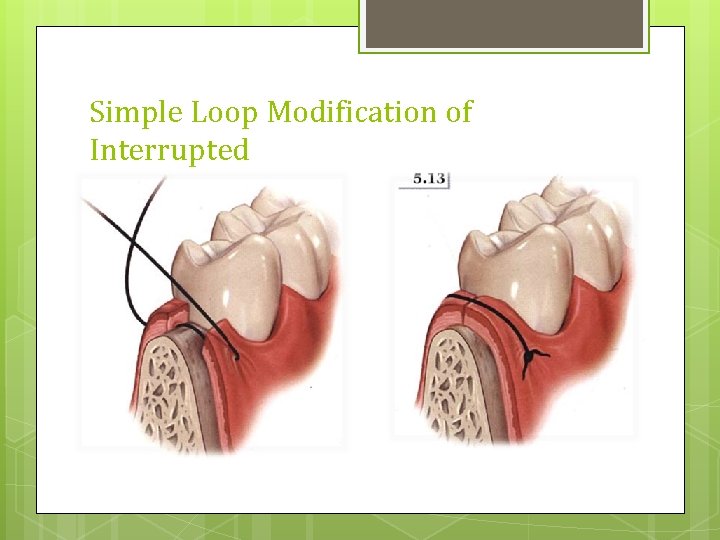
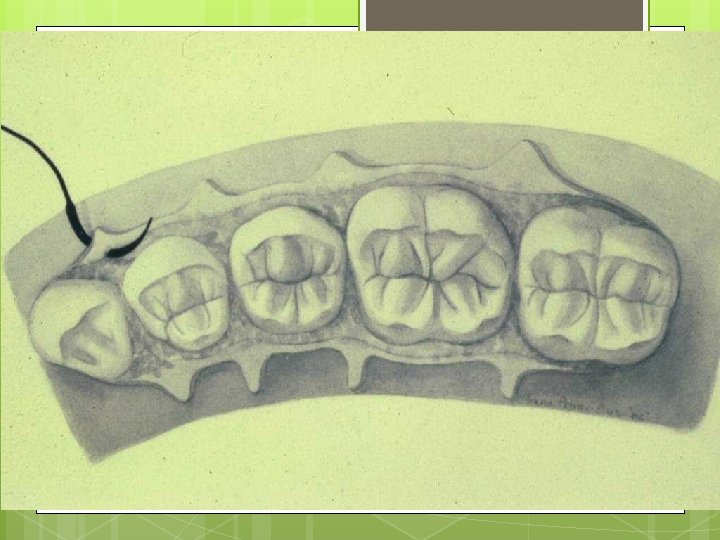
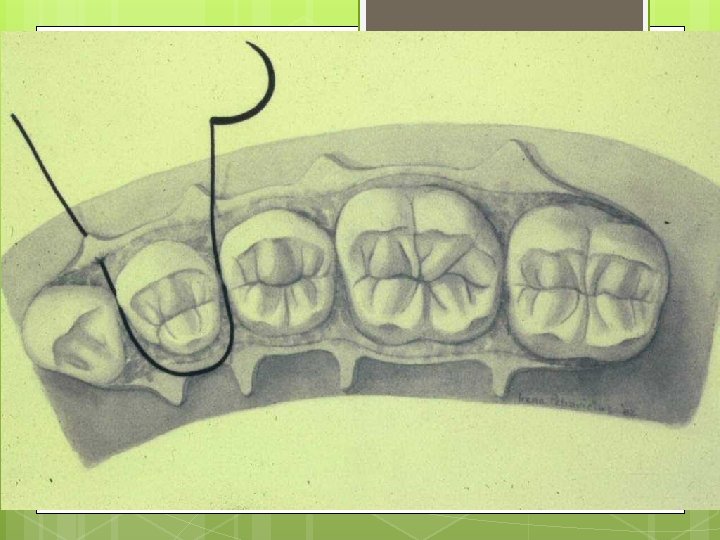
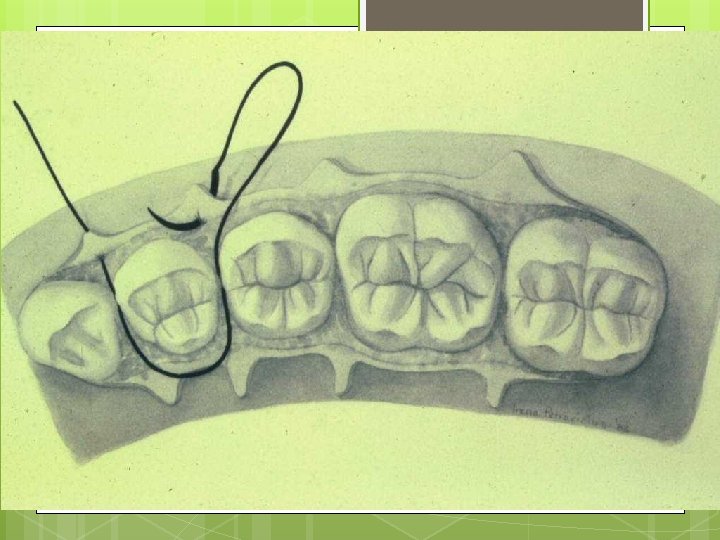
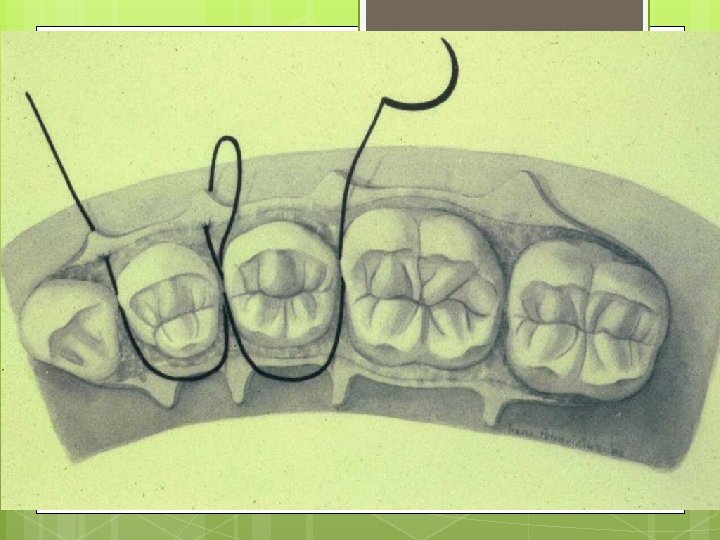
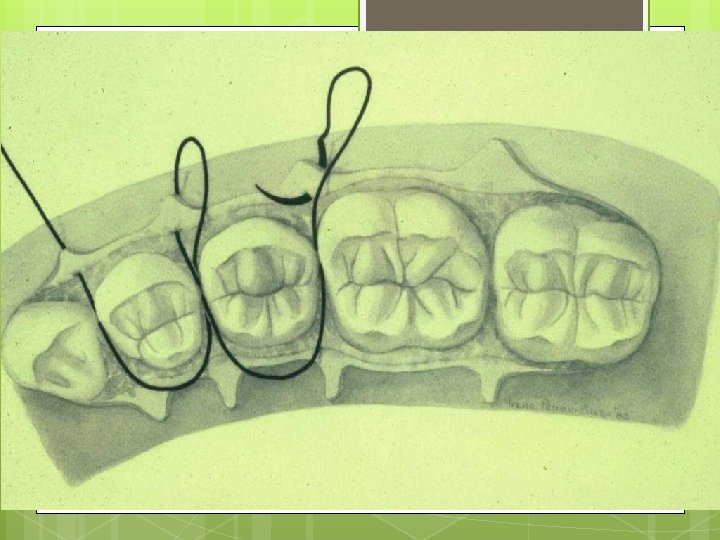
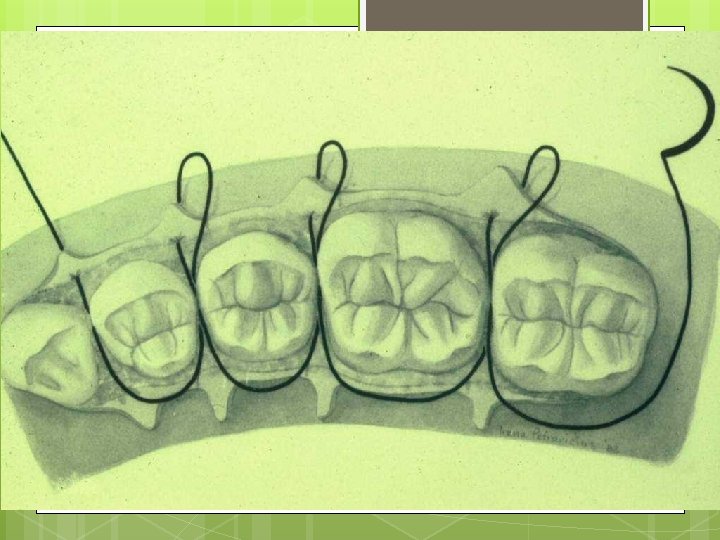
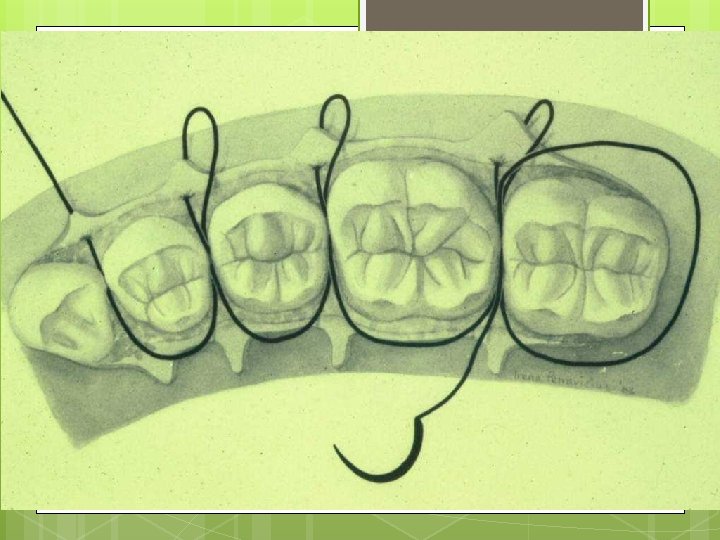
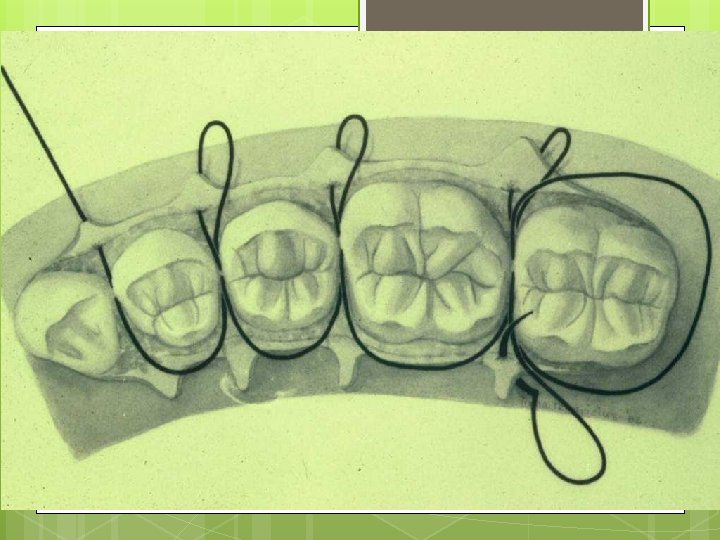
Simple Loop Modification of Interrupted

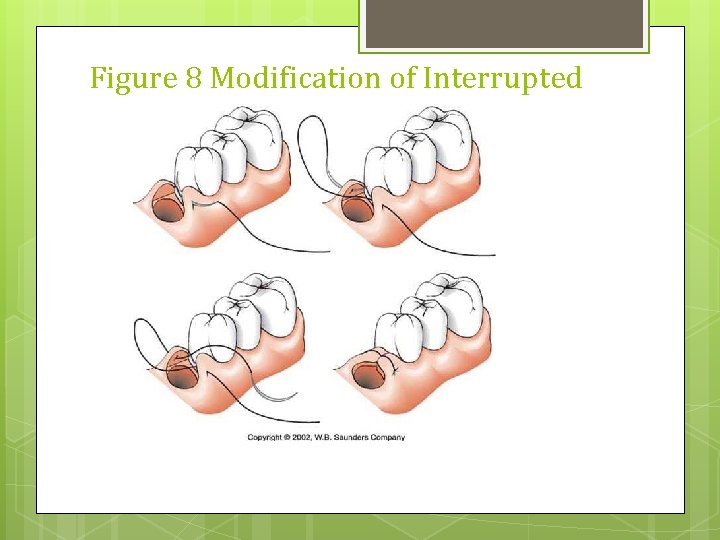
Figure 8 Modification of Interrupted

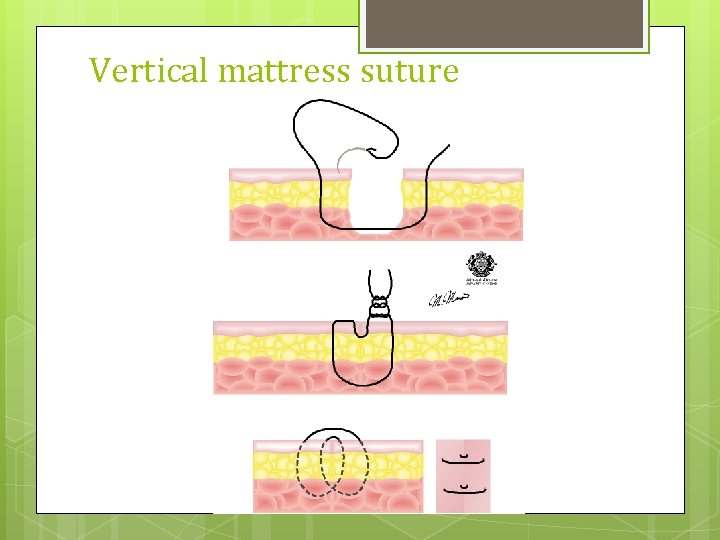
Vertical mattress suture

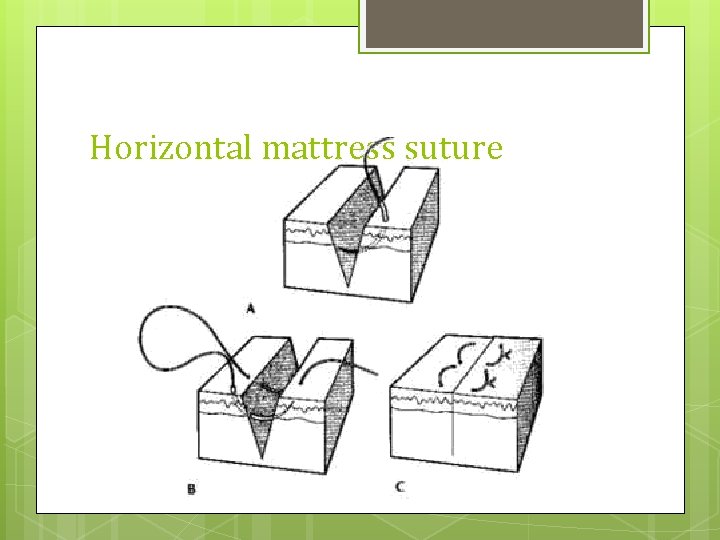
Horizontal mattress suture

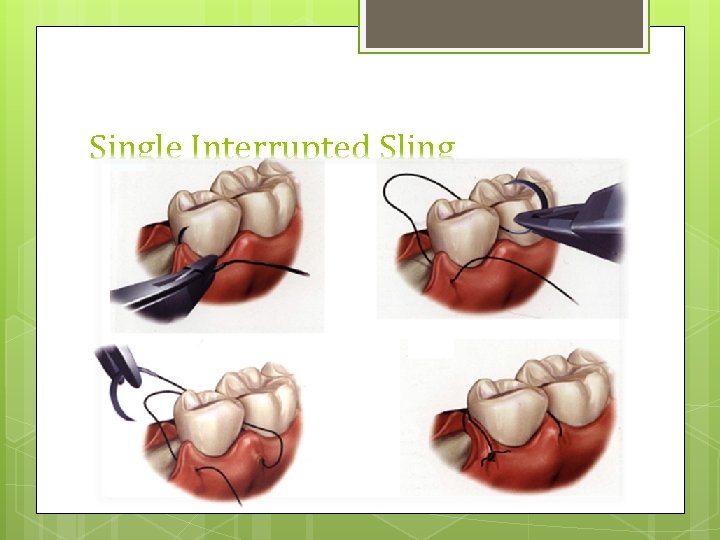
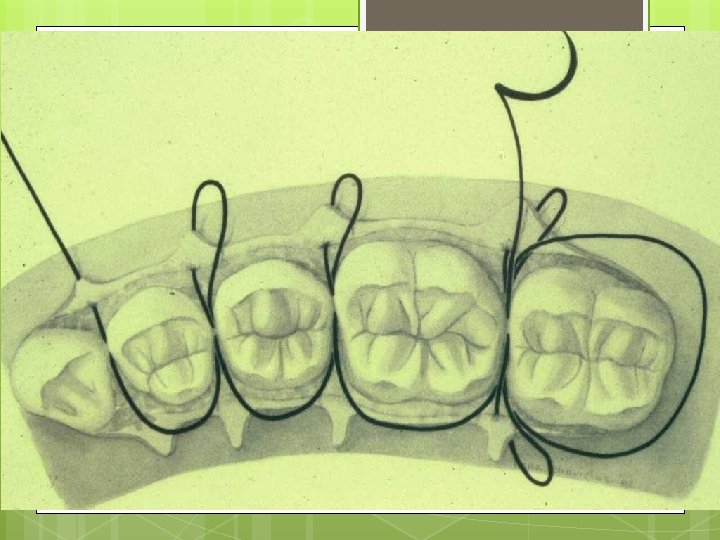
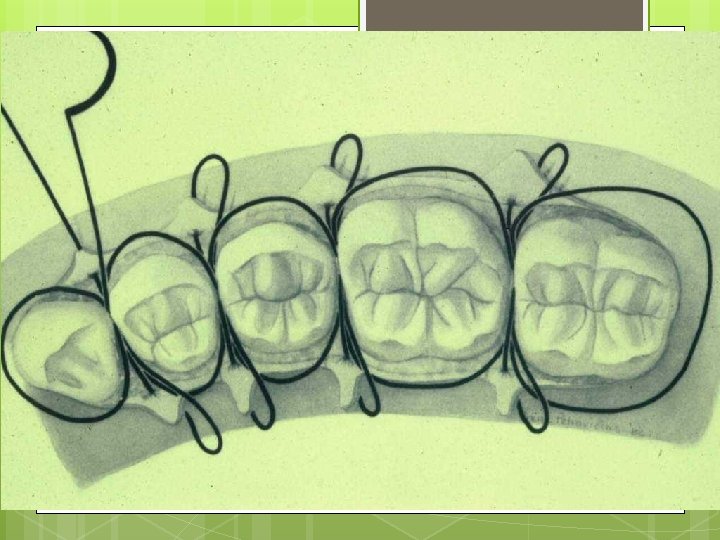
Single Interrupted Sling














Reference 1. 2. 3. 4. 5. 6. 7. Contemporary Oral and Maxillofacial Surgery, 4 th Edition, Larry J Peterson, DDS, MS, Edward Ellis, III, DDS, MS, James R Hupp, DMD, JD, FACS and Myron R Tucker, DDS Peterson's principles of oral and maxillofacial surgery, Michael Miloro, G. E. Ghali, Peter Larsen, Peter Waite An atlas of minor oral surgery: principles and practice, David A. Mc. Gowan Manual of minor oral surgery for the general dentist, Karl R. Koerner Critical Decisions in Periodontology, 4 th Edition, WALTER B. HALL, BA, DDS, MSD Color Atlas of Periodontology, Klaus H. & Edith M. Rateitschak Atlas of Cosmetic and Reconstructive Periodontal Surgery 3 rd edition, EDWARD S. COHEN, DMD