THE PERIODONTAL FLAP Dr Malek Abdulmatlob PERIODONTAL FLAP

THE PERIODONTAL FLAP Dr. Malek Abdulmatlob

PERIODONTAL FLAP �Definition: Asection of gingiva and/or mucosa surgically separated from the underlying tissues. �Advantages: 1 - Provides visibility & access to the bone & root surface. 2 - Allows the gingiva to be displaced to a different location.

Classification of Periodontal Flap: Based on: �Bone exposure after flap reflection Full thickness flap Partial thickness flap �Placement of the flap after surgery Displaced flap Non-displaced flap �Management of the papilla Conventional flap Papilla preservation flap
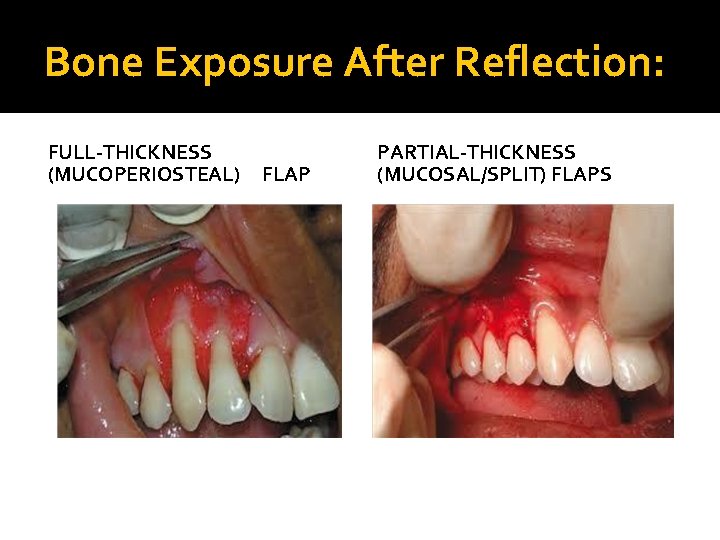
Bone Exposure After Reflection: FULL-THICKNESS (MUCOPERIOSTEAL) FLAP PARTIAL-THICKNESS (MUCOSAL/SPLIT) FLAPS
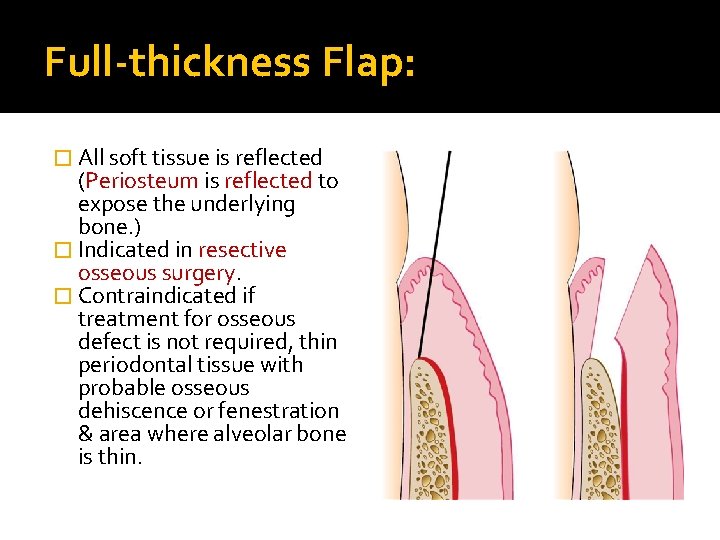
Full-thickness Flap: � All soft tissue is reflected (Periosteum is reflected to expose the underlying bone. ) � Indicated in resective osseous surgery. � Contraindicated if treatment for osseous defect is not required, thin periodontal tissue with probable osseous dehiscence or fenestration & area where alveolar bone is thin.
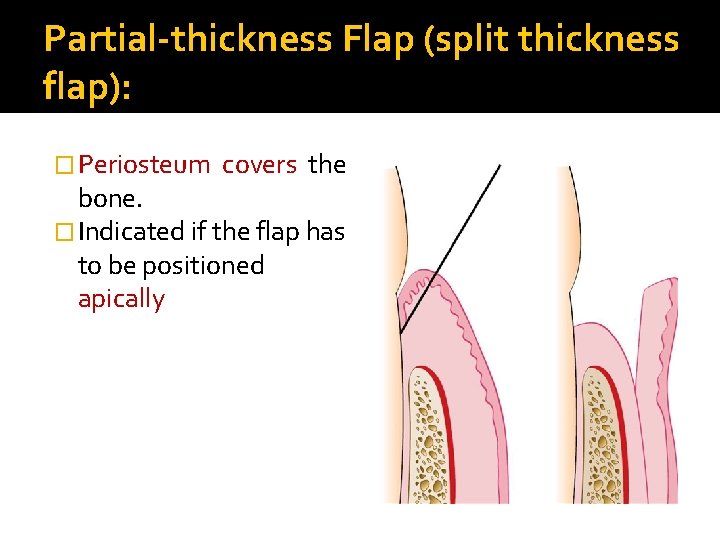
Partial-thickness Flap (split thickness flap): � Periosteum covers the bone. � Indicated if the flap has to be positioned apically

Based on Flap Placement After Surgery: • Non displaced flap : The flap is returned & sutured in its original position. • Displaced flap : The flap is placed apically, coronally, or laterally to its original position. It can be a fullthickness or partial-thickness flap.
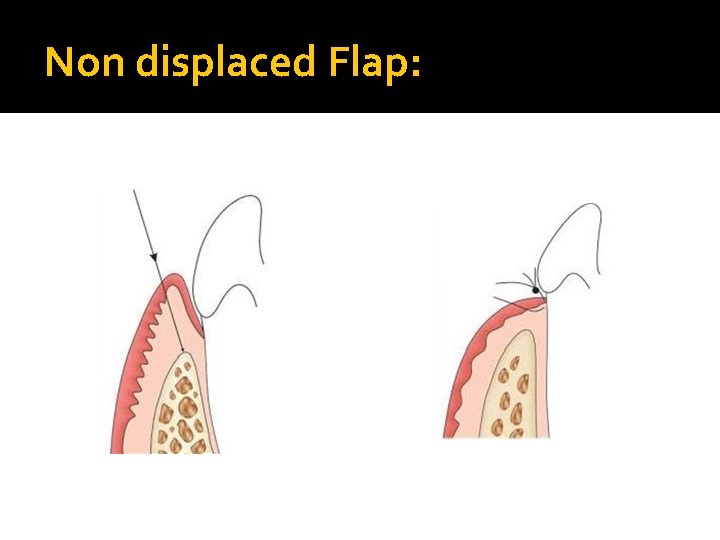
Non displaced Flap:
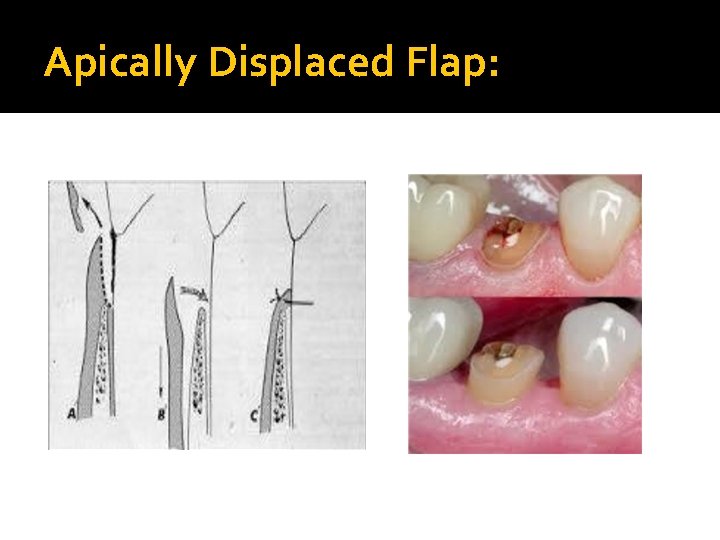
Apically Displaced Flap:
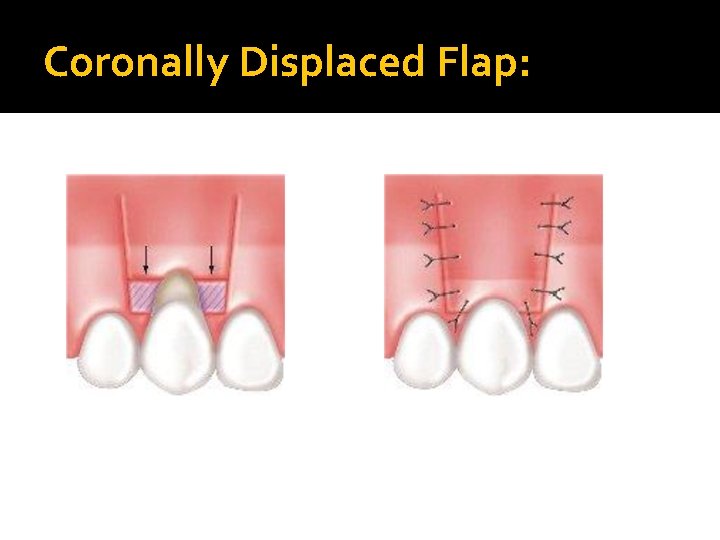
Coronally Displaced Flap:
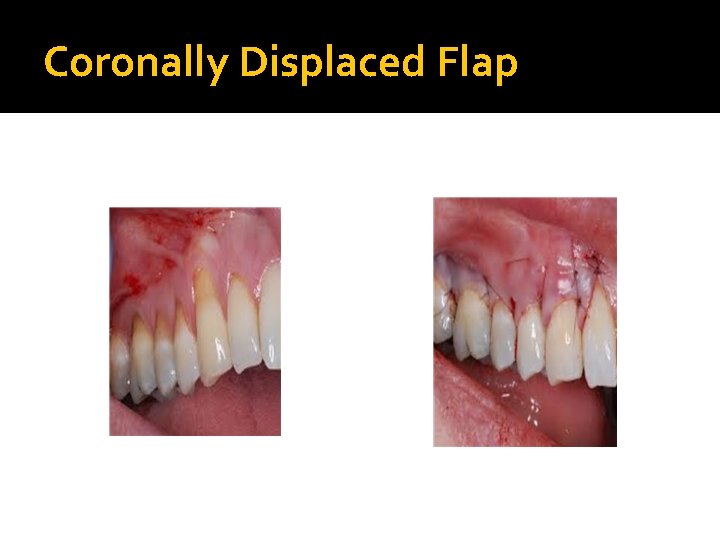
Coronally Displaced Flap
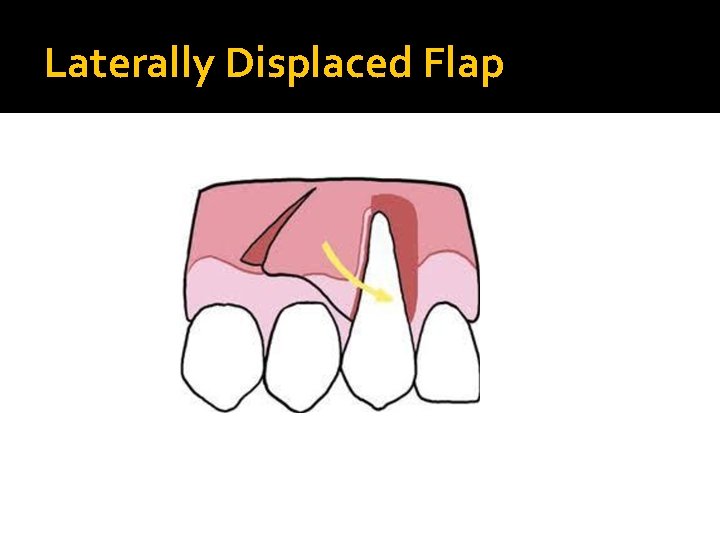
Laterally Displaced Flap
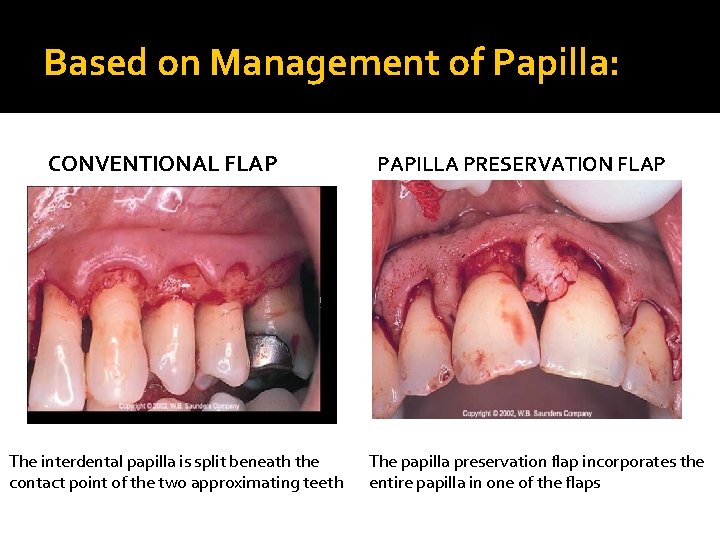
Based on Management of Papilla: CONVENTIONAL FLAP The interdental papilla is split beneath the contact point of the two approximating teeth PAPILLA PRESERVATION FLAP The papilla preservation flap incorporates the entire papilla in one of the flaps

Conventional Flap: The interdental papilla is split beneath the contact point of the two approximating teeth to allow reflection of buccal and lingual flaps. Indications: 1 -Narrow interdental spaces that prevents papilla preservation 2 -When the flap is to be displaced. • Types: Modified Widmanflap Non displaced flap Apically displaced flap The flap for reconstructive procedures.

Incisions

Incisions: Types: 1 - Horizontal incisions: Can be used without vertical incisions if the flap reflection ensures sufficient access & if displaced flap is not needed. 2 - Vertical (oblique) releasing incisions: Can be used on one or both ends of the horizontal incision, depending on the design and purpose of the flap (eg. vertical incisions at both ends are necessary for apically displaced flap).

Horizontal Incisions: Are directed along the margin of the gingiva in a mesial or a distal direction. • Types: A- Internal bevel incision : starts at a distance from the gingival margin and is aimed at near the bone crest. B- Crevicular incision: starts at the base of the pocket and is directed to the bone crest. C-Interdental incision is performed after the flap is elevated.
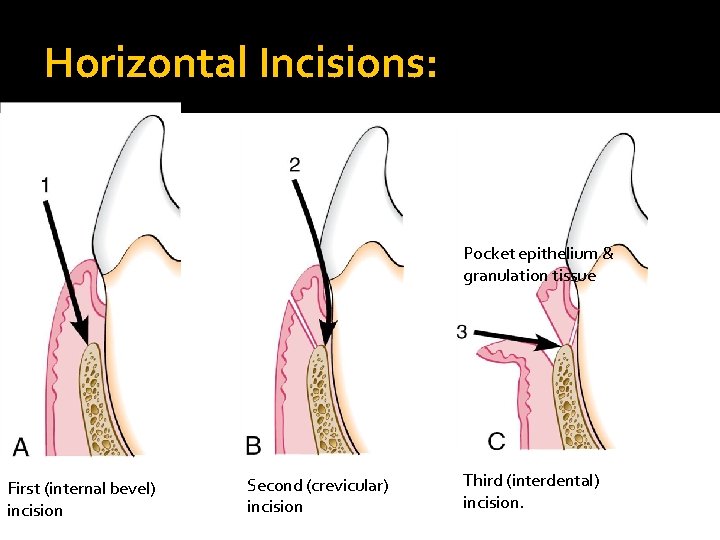
Horizontal Incisions: Pocket epithelium & granulation tissue First (internal bevel) incision Second (crevicular) incision Third (interdental) incision.
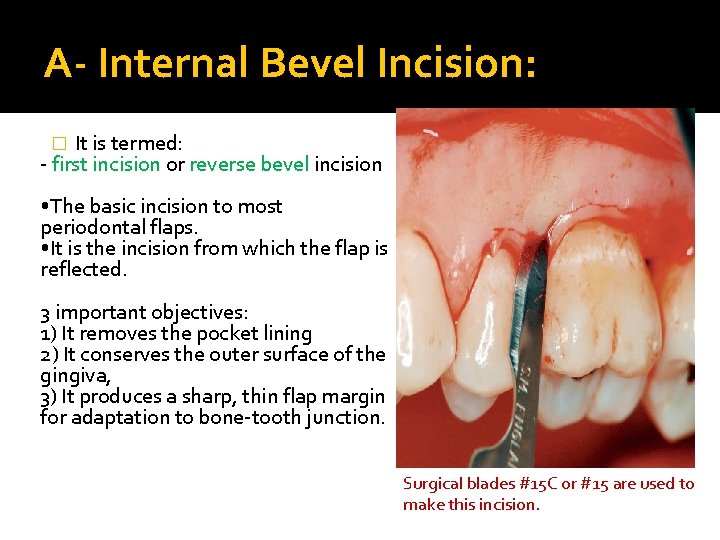
A- Internal Bevel Incision: It is termed: - first incision or reverse bevel incision � • The basic incision to most periodontal flaps. • It is the incision from which the flap is reflected. 3 important objectives: 1) It removes the pocket lining 2) It conserves the outer surface of the gingiva, 3) It produces a sharp, thin flap margin for adaptation to bone-tooth junction. Surgical blades #15 C or #15 are used to make this incision.
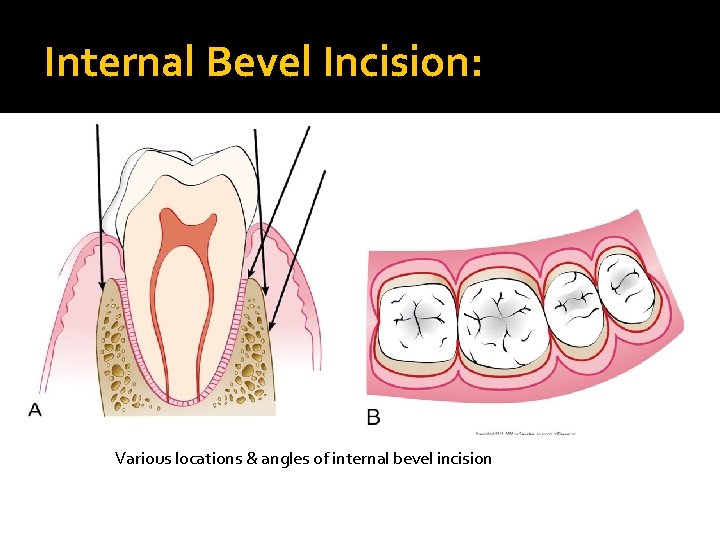
Internal Bevel Incision: Various locations & angles of internal bevel incision
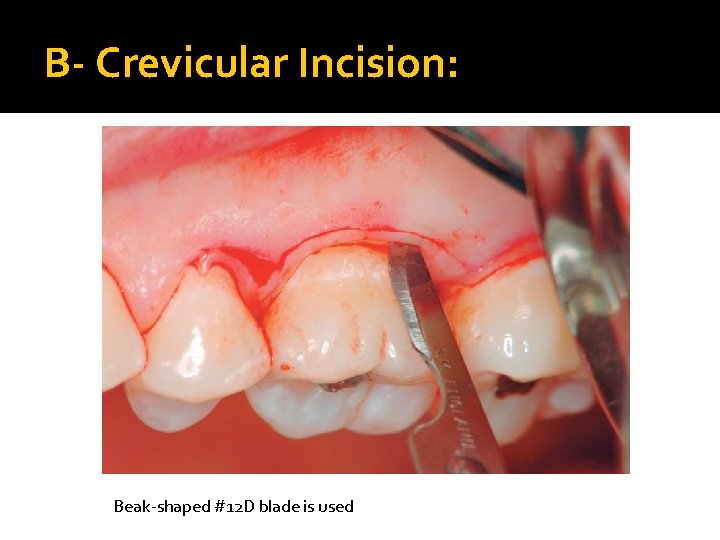
B- Crevicular Incision: Beak-shaped #12 D blade is used
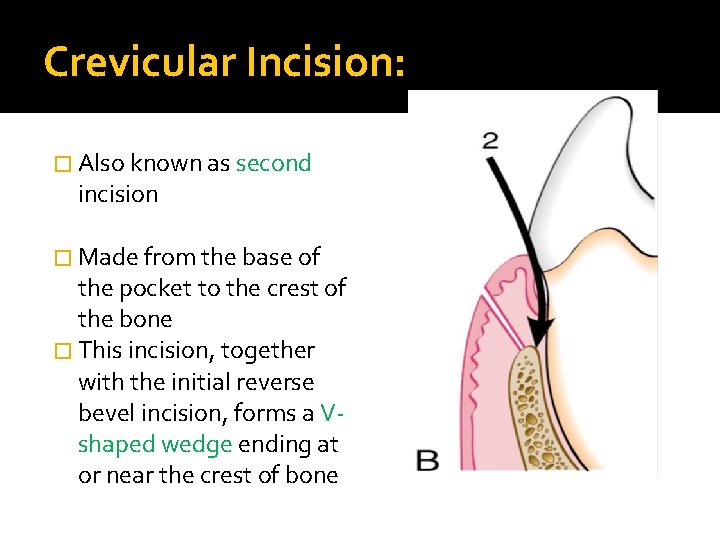
Crevicular Incision: � Also known as second incision � Made from the base of the pocket to the crest of the bone � This incision, together with the initial reverse bevel incision, forms a Vshaped wedge ending at or near the crest of bone
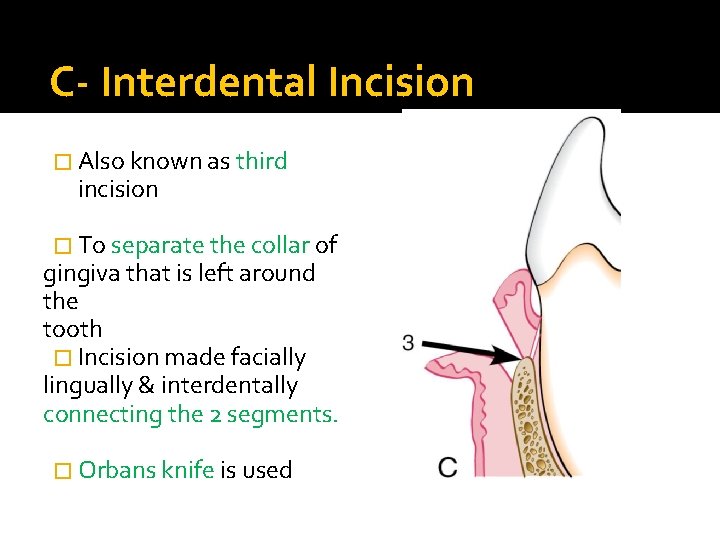
C- Interdental Incision � Also known as third incision � To separate the collar of gingiva that is left around the tooth � Incision made facially lingually & interdentally connecting the 2 segments. � Orbans knife is used
Incision Procedure: 1. Surgical blade #15 or #15 C to do internal bevel incision. 2. Beak-shaped # 12 D blade to do crevicular incision. 3. Periosteal elevator is inserted into the internal bevel incision & the flap is separated from the bone. 4. Orban knife to do interdental incision around facially, lingually & interdentally connecting the facial &lingual segments to free the gingival collar. 5. Curette or a large scaler (U 15/30) to remove the gingival collar. 6. The remaining connective tissue is carefully curetted to observe the entire root and adjacent bone.

Vertical Incisions: �Can be used on one or both ends of the horizontal incision �Must extend beyond the mucogingival line, reaching the alveolar mucosa, to allow for the release of the flap to be displaced. �Facial vertical incisions should be made at the line angles to prevent splitting of a papilla or incising directly over a radicular surface.
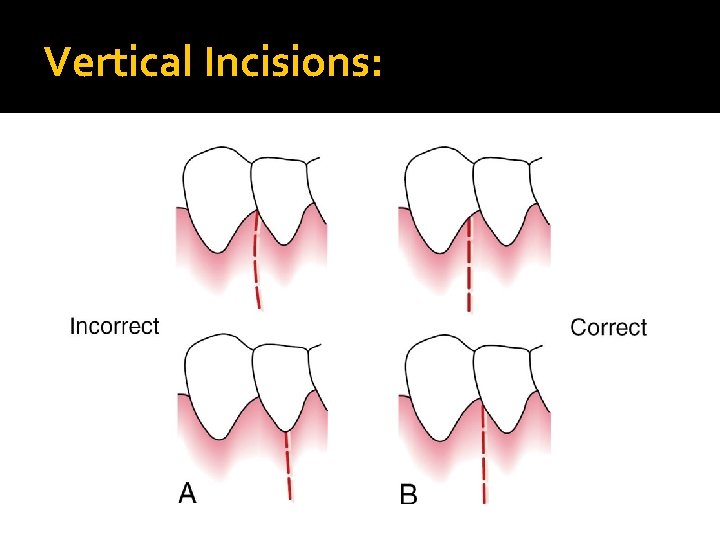
Vertical Incisions:

Flap Design

Flap Design Depends on: • Surgical judgment of the operator • Objectives of the procedure. • Necessary degree of access to the underlying bone and root • Final position of the flap • Good blood supply Requires: Careful planning that includes the type of flap, exact location, type of incisions, management of the underlying bone, and final closure of the flap and sutures.

Flap Design: Depending on papilla preservation • Conventional flap (split the papilla). • Papilla preservation flap (preserve papilla). Depending on the types of incisions: • Envelope Flap: it is released horizontally & has no vertical releasingi ncision(s). • Pedicle Flap: Two vertical releasing incisions are included in the flap design • Triangular Flap: One vertical releasing incision is included in the flap design.

Flap Design: �Envelope Flap: A flap that is released in a linear fashion at the gingival margin but has no vertical releasing incision(s). �Pedicle Flap: If two vertical releasing incisions are included in the flap design. �Triangular Flap: If one vertical releasing incision is included in the flap design.
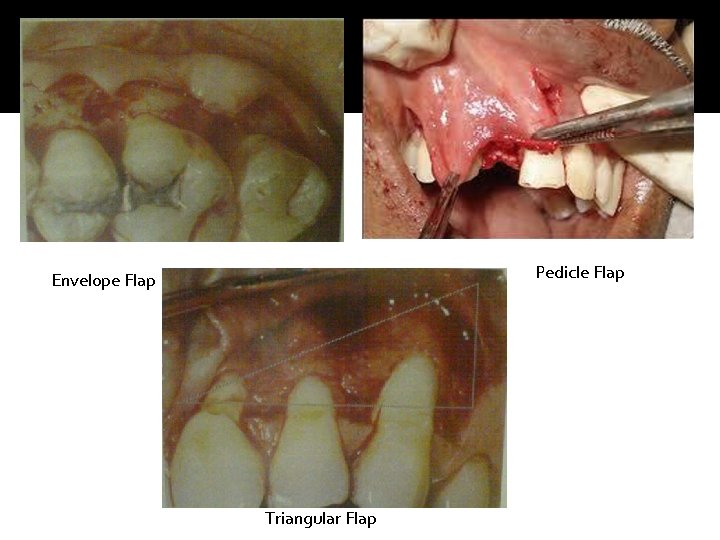
Pedicle Flap Envelope Flap Triangular Flap

Periodontal Flap Elevation
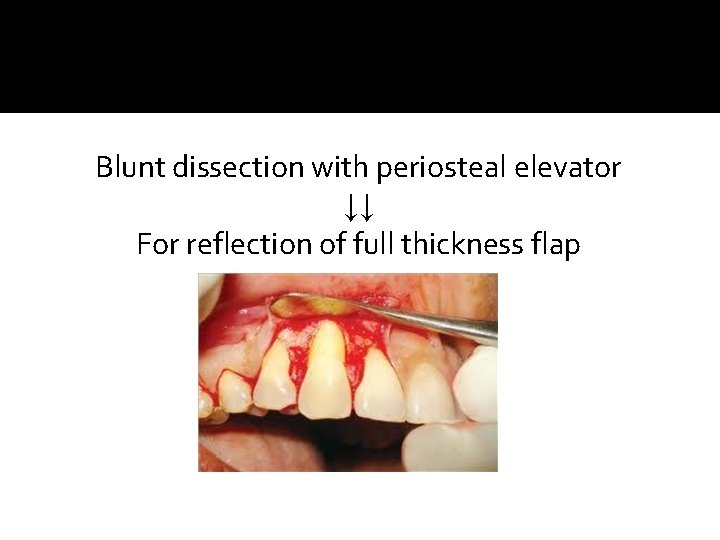
Blunt dissection with periosteal elevator ↓↓ For reflection of full thickness flap
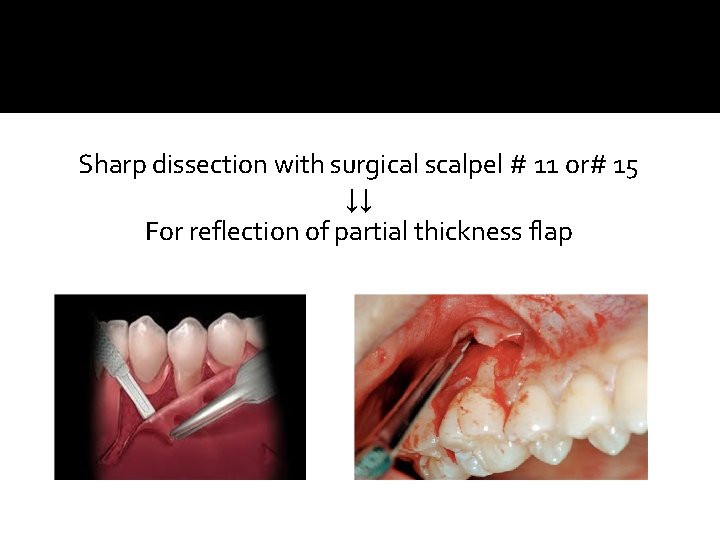
Sharp dissection with surgical scalpel # 11 or# 15 ↓↓ For reflection of partial thickness flap

Healing After Flap Surgery
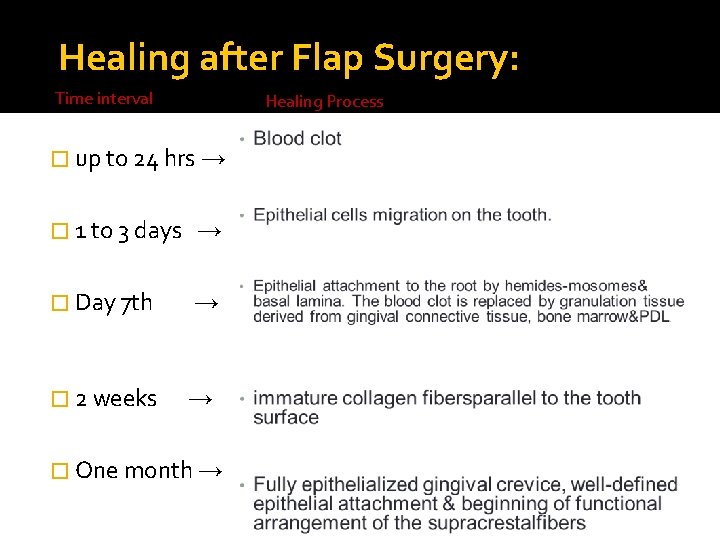
Healing after Flap Surgery: Time interval Healing Process � up to 24 hrs → � 1 to 3 days → � Day 7 th → � 2 weeks → � One month →

Healing after Flap Surgery �In full-thickness flaps: �Superficial bone necrosis (at 1 to 3 days) →→osteoclastic resorption (peak at 4 to 6 days) resulting in >1 mm bone loss if the bone is thin. �In osteoplasty: areas of bone necrosis & reduction in bone height, remodeled later by new bone formation.

Thank you
- Slides: 38