Complications of Pregnancy PreEclampsiaEclampsia Diabetes in Pregnancy Perinatal

Complications of Pregnancy Pre-Eclampsia/Eclampsia Diabetes in Pregnancy Perinatal Infections Abortion & Others

ACOG (American College of Obstetricians and Gynecologists) created a task force of experts in the management of hypertension in pregnancy ¨ Reviewed available data ¨ Published evidence based recommendations http: //www. acog. org/Resources-And-Publications/Task-Force-and. Work-Group-Reports/Hypertension-in-Pregnancy

4 Categories Used By The Task Force n Chronic Hypertension (of any cause) n Chronic Hypertension with superimposed preeclampsia n Gestational Hypertension n Preeclampsia/Eclampsia

Chronic Hypertension High blood pressure known to predate conception or detected BEFORE 20 weeks gestation

Chronic Hypertension with Superimposed Preeclampsia § § (Maternal prognosis is worse than either condition alone) HTN with proteinuria that develops after the 20 th week OR HTN and proteinuria before the 20 th week WITH (At least one): Ø Sudden increase in BP Ø Sudden manifestation of other s/s ( i. e. increase in liver enzymes to abnormal levels) Ø Platelets below 100, 000/microliter Ø Additional symptoms like RUQ pain & Severe headache Ø Pulmonary congestion or edema Ø Renal insufficiency Ø Sudden and sustained increase in protein excretion

Gestational Hypertension ¨ Transient— BP that occurs without proteinuria late in pregnancy or in the early pp period, but returns to normal BY 12 weeks pp. ¨ Chronic— BP that occurs without proteinuria late in pregnancy or in the early pp period, but remains AFTER 12 wks pp.

Pre-eclampsia/Eclampsia (Pregnancy-specific, multi-system syndrome) Hypertension that develops after the 20 th week gestation AND ¨ Proteinuria OR ¨ Thrombocytopenia ¨ Renal insufficiency ¨ Impaired liver function ¨ Pulmonary edema ¨ Cerebral or visual symptoms ¨

Blood Pressure ¨ > or = 140 systolic OR > or = to 90 diastolic on two occasions AT LEAST 4 hours apart in a woman with previously normal BP ¨> or = 160 systolic OR > or = 110 diastolic can be confirmed within a short interval to facilitate timely treatment. ¨ Increase occurs AFTER the 20 th week gestation

Proteinuria ¨ > or = 300 mg per 24 hour urine collection (GOLD STANDARD) OR ¨ Protein/creatinine ¨ Dipstick ratio > or = to 0. 3 mg/d. L reading of 1+ (used only if other quantitative methods are not available)
Thrombocytopenia ¨ Platelet count less than 100, 000/microliter Renal Insufficiency ¨ Serum creatinine > 1. 1 mg/d. L Impaired liver function Elevated blood concentrations of liver enzymes Pulmonary Edema Cerebral or Visual Symptoms

Eclampsia The Presence of new-onset grand mal seizure in a woman with preeclampsia ØCannot cause be attributed to any other

Predisposing Factors to Preeclampsia n n n Primiparity Previous preeclamptic pregnancy Chronic hypertension or chronic renal disease History of thrombophilia Multigestational pregnancies In vitro fertilization Family Hx of preeclampsia Type I DM or Type II DM Obesity Systemic lupus erythematosus Maternal age <19 or >40

Changes in Normal Pregnancy n n n n Cardiac output by 50% Blood volume by 1500 ml Peripheral vascular resistance BP Renin GFR ECF Aldosterone effects blocked
Changes in Preeclampsia (pg 382; 10 n th ed) Generalized Vasospasm ¨ Hypertension Intravascular volume placental perfusion IUGR of fetus, fetal distress ¨ renal perfusion GFR urine output (oliguria) ¨ BUN & Creatinine & uric acid ¨ proteinuria serum albumin ¨ Extravascular fluid (edema) Pulmonary, retinal, & cerebral edema ¨ Dyspnea, scotomata, CNS irritability/ hyperreflexia, HA, N& V, convulsions ¨ Hepatic perfusion Liver function tests, epigastric pain (RUQ) ¨

Preeclampsia without severe features n Signs & Symptoms ¨ BP > 140/90 ¨ Proteinuria (Mild)

Treatment of Preeclampsia w/o Severe Features ¨ Daily kick counts ¨ Ultrasound for fetal growth q 3 weeks ¨ Amniotic fluid assessment at least 1/week ¨ NST twice a week (non-reactive = BPP) ¨ Monitor daily wt for gain ¨ Monitor BP daily ¨ Lab tests: CBC, liver enzyme & serum creatinine level at least once a week. ¨ Regular diet w/ no salt restrictions ¨ Instructed to go to hospital w/worsening sx

Hospital care of mild preeclampsia ¨ Bedrest, left lateral recumbent position to renal perfusion which promotes diuresis and lowers BP ¨ Diet—well balanced, nutritious, moderate protein to replenish what is spilled by kidneys

Hospital care of mild preeclampsia (Cont’d) ¨ Assessment of fetal well-being n DFMC, BPP, NST, Amniocentesis ¨ Assessment of maternal well-being n BP assessed qid or q 4 hr n Daily wt, and assessment of worsening edema n Assessment of HA, visual changes, epigastric pain, hyperreflexia n Lab tests: daily urine dipstick for protein, 24 hr protein, CBC w/ platelet count q 2 days, serum creatinine, uric acic, & liver function tests (AST, ALT, LDH, Bili)

Severe Preeclampsia n Signs and symptoms ¨ BP of 160/110 or higher on 2 occasions at least 4 hr apart while on bedrest ¨ Proteinuria 5 g/L in 24 hr or 3+ or > on 2 random urine samples 4 hrs apart ¨ Oliguria: urine output <500 ml/24 hr ¨ Cerebral or visual disturbances—HA, scotomata or blurred vision ¨ Pulmonary edema or cyanosis ¨ Epigastric or RUQ pain ¨ Impaired liver function ( AST, APT) ¨ Thrombocytopenia

Treatment of Severe Preeclampsia ¨Absolute bedrest ¨Quiet environment to reduce stimuli ¨Delivery > 34 weeks gestation
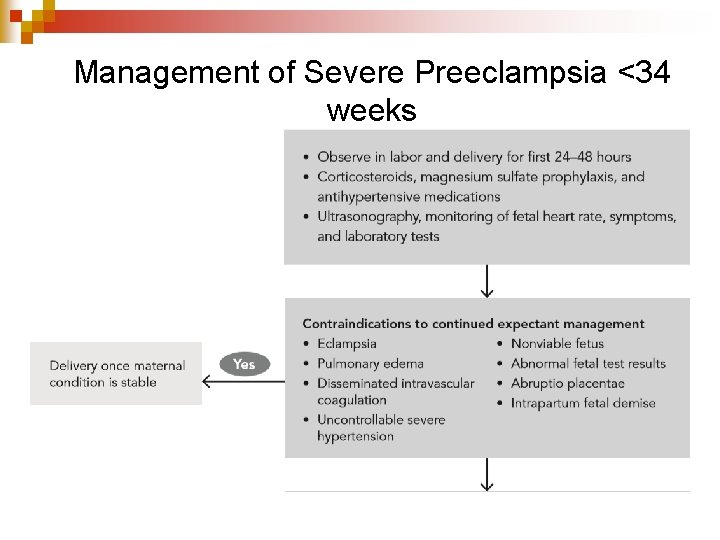
Management of Severe Preeclampsia <34 weeks



Medications used in treatment Seizure Prophylaxis n Magnesium Sulfate: Sulfate a 4 -6 gm bolus is given IV over 20 minutes, then a continuous infusion of 2 gm/hr is generally advocated. CNS depressant Ø Needs to be maintained at a therapeutic level as determined by each laboratory Ø Excessive levels lead to respiratory paralysis and cardiac arrest Ø Calcium gluconate given per MD protocol to reverse Ø

Case Study A 35 year old G 1 P 0 patient is admitted to L&D with severe preeclampsia. Her most recent blood pressure readings have been 172/108 & 176/112. She complains of seeing spots and a severe headache. You have received orders for a 4 gm IV bolus of Magnesium over 20 minutes followed by a 2 gm/hr maintenance dose. Ø If 40 grams are added to 1000 mls of LR, at what rate would you set the IV pump to administer 4 gm in 20 minutes? Ø What amount would you put in the VTBI on the pump? Ø If you are to continue to infuse at 2 gm/hr, at what rate would you set the pump? Ø What side effects can you educate your patient on? Ø What are the nursing implications? Ø What should you have available in case of Mag Sulfate toxicity? See p. 572 Davidson 10 th ed. for more info

Medications used in treatment Anti-hypertensives Given for sustained BP’s >160/110 n n First Line for Acute Hypertension Ø Labetalol: 20 mg IV over 2 min, can give q 10 min if needed (max 300 mg) – avoid with asthma or CHF Ø Hydralazine: 5 mg IV over 1 -2 min, can give q 20 min if needed (max 30 mg) Expectant management Ø n Oral Labetalol, Nifedipine, or Methyldopa NO diuretics or ACE inhibitors

Eclampsia— occurs in 1600 pregnancies n Symptoms of impending seizure: ¨ Persistent occipital or frontal headaches ¨ Blurred vision ¨ Photophobia ¨ Epigastric or right upper quadrant pain ¨ Altered mental status ¨ Hyperreflexia— 4+ ¨ Scotomata—dark spots or flashing lights ¨ Vomiting ¨ Neurologic hyperactivity ¨ Pulmonary edema ¨ Cyanosis

Safety precautions ¨ Quiet environment—no phone calls, TV, lights, pulled shades, etc. ¨ Padded side rails in bed ¨ O 2 ready and available ¨ Suction ready and available

Refer to Nursing Care Plan pp. 389 -391 Davidson et al, 10 th ed. Note importance of careful monitoring of mother and fetus throughout hospitalization with severe pre-eclampsia n Prevention of complications is key to healthy management n

HELLP Syndrome Hemolysis n Elevated Liver Enzymes n Low Platelets (< 100, 000/mm 3) n ¨ Sometimes associated with severe preeclampsia ¨ Sx: N & V, malaise, flu-like sx, or epigastric pain with or without HTN ¨ Persons presenting with these sx should have CBC with platelets and liver enzymes drawn ¨ These pts should be managed at tertiary care centers ¨ Corticosteroids: while usually given to foster fetal maturity, they have been found to stabilize platelet counts and hepatic enzymes and LDH levels. Dexamethasone is often chosen for HELLP syndrome.

Diabetes In Pregnancy Did it exist BEFORE Pregnancy? n Pregestational Diabetes Mellitus ¨ Type 1 ¨ Type 2 ¨ 1/2000 pregnancies n Gestational Diabetes ¨ Any degree of glucose intolerance with the onset or first recognition occurring during pregnancy ¨ 2 -5% of all pregnancies n n 90% of all cases of diabetes in pregnancy 25% of these women will develop Type 2 diabetes later in life

Normal CHO Metabolism in PG Goal of changes is to provide adequate glucose to fetus for growth n Maternal glucose crosses the placenta n Maternal insulin does NOT n KEY CONCEPT TO UNDERSTAND n

CHO Metabolism— 1 st Trimester in E & P stimulate Beta cells of Pancreas to Insulin production n = use of glucose in serum glucose levels (FBS ) n in tissue glycogen stores n in liver glycogen production n = Pregestational Diabetics Hypoglycemia n

CHO Metabolism-2 nd & 3 rd Trimester Pregnancy is a “diabetogenic” state n Hormones levels lead to tolerance to glucose n insulin resistance n ¨ HPL-Human n Insulin antagonist—Won’t let insulin work ¨ Placental n Placental Lactogen Insulinase Breakdown insulin at placental site

Net Result = Changes in Insulin Needs for Type 1 Diabetic Mother during Pregnancy n 1 st trimester = ¨ need for insulin production, N&V, transfer to fetus food intake, 2 nd Trimester = Gradual n 3 rd Trimester = 2 -4 times higher need for insulin by 36 week, then levels off til labor n Soon After delivery = glucose/insulin balance OK by 7 -10 days n

Risks to Mother n Pregestational Diab. ¨ If poor control very early in PG Miscarriage ¨ Macrosomic baby C/S ¨ Pre-eclampsia ¨ PTL ¨ Infections (UTI’s, Vag) ¨ Polyhydramnios ¨ Ketoacidosis / Hypogylecemia n Gestational-Onset ¨ 2 X likely to have preeclampsia ¨ Macrosomic baby C/S

Risks to Baby n Pregestational ¨ Congenital n Defects Heart, Skeletal, CNS ¨ Same as Gestational n Gestational ¨ Macrosomia Birth Trauma ¨ Hypoglycemia ¨ RDS ¨ Hypocalcemia ¨ Hyperbilirubinemia ¨ Thrombocytopenia ¨ Polycythemia

Management of Pre-gestational Diabetes n Pre-conceptual Counseling ¨ Establish glycemic control BEFORE PG ¨ Understand the VERY close monitoring Blood glucose levels 4 -8 times a day. n Frequent MD visits n ¨ If Type 2—Some oral hypoglycemic agents are teratogenic Insulin SQ during pregnancy

Management of Pre-gestational Diabetes n Hgn A 1 c ¨ Good control = 2. 5% to 5. 9 % ¨ Fair Control = 6% - 8% ¨ Poor Control = > 8% n Diet VERY CAREFULLY BALANCED ¨ Should n be followed by Registered Dietician Exercise ¨ Not vigorous, Best time is after meals

Management of Pre-gestational Diabetes-Insulin n Multiple daily injections needed ¨ Mixed of longer-acting and rapid-acting in AM and PM Humulin or Novolin, NOT pork or beef insulins n Humalog, if newly diagnosed n

Management of Pre-gestational Diabetes-Insulin n GOAL—keep blood sugar in narrow margin ¨ Fasting = 60 -90 mg/dl ¨ 2 -hour postprandial = 90 -120 mg/dl

Management of Pre-gestational Diabetes-Delivery Careful determination of ACTUAL due date n Amniocentesis Fetal lung maturity n Induce 39 -40 wks-NO LATER THAN 40 WKS n If estimated fetal weight > 4000 -4500 Gms C/S n In L&D- Watch maternal glucose levels every 2 hours n

Gestational Diabetes-Screening n Low-risk ¨< 25 y/o ¨ No family Hx ¨ Normal BMI ¨ Not in High-Risk group ¨ No Hx of Abnormal GTT n Hi-Risk ¨ Hx of gestational Diabetes ¨ Overweight/Obese BMI ¨ High-risk group n n African-American Native-American Latina Pacific-Islander

Gestational Diabetes-Screening n First pre-natal visit ¨ 50 gm glucose load -> draw serum 1 hour later Negative < 140 mg/dl n Positive > 140 mg/dl n n Screen again 24 -28 weeks gestation

Gestational Diabetes-Screening If positive do 3 -hour GTT (100 g of glucose) n Positive for GDM = 2 or more levels are met or exceeded n ¨ Fasting ¨ 1 -hr ¨ 2 -hr ¨ 3 -hr < 95 mg/dl < 180 mg/dl < 155 mg/dl < 140 mg/dl

Gestational Diabetes Management n n n GOAL Keep blood sugars within levels for Pregestational diabetes GDM should be managed first with diet and exercise, exercise and medications should be added if needed. http: //care. diabetesjournals. org/content/38/Supplement_1/S 77 (Jan. 2015) Insulin— 20% will need insulin during PG; safest Glyburide (oral hypoglycemic agent) is being used with caution but not yet approved by ACOG Blood glucose monitoring ¨ Frequently done in MD office or at home

Gestational Diabetes Management n Target Blood Sugars: Recommended daily target blood glucose numbers for most pregnant women with diabetes are ¨ Before meals, at bedtime, and overnight: 90 or less ¨ 1 hour after eating: 130 to 140 or less https: //www. niddk. nih. gov/healthinformation/diabetes-pregnancy 3 ¨ 2 hours after eating: 120 or less ¨ n n n Delivery ¨ Frequent NST/BPP in last 2 months of pregnancy ¨ Deliver by 40 weeks Excellent resource link from the National Diabetes Education Program with handouts. Another great resource with tables from Merck Manual

Perinatal Infections n Group-B Hemolytic Streptococcus ¨ Major cause of perinatal infections ¨ Found in Vagina and Urine ¨ Increase fetal mortality and morbidity ¨ Screen 35 -37 wks with vaginal and rectal cultures. (CDC Recommendations) n If Positive –Treat in Labor Penicillin: 5 million Units IV x 1; 2. 5 -3 million units every 4 hours ¨ Ampicillin: 2 GMs IV x 1; 1 GM every 4 hours ¨ Clindamycin 900 mg IV q 8 hr OR Erythromycin 500 mg IV q 6 hr till delivery if allergic to Penicillin. ¨

Perinatal Infections n If GBS status unknown—Prophylactic trx is indicated if: ¨ Previous infant with GBS ¨ GBS bacturia during this pregnancy ¨ PTL ¨ Temp in labor > 100. 4 F ¨ Membranes ruptured > 18 hours

Other Perinatal infections Syphyllis n Gonorrhea n Chlamydia n TORCH p. 394 -400; 10 th ed. n ¨ Toxoplasmosis ¨ Rubella ¨ Cytomegalovirus ¨ Herpes, Human B 19 Parvovirus

Hemorrhagic Complications Abortion = loss of pregnancy BEFORE 20 weeks gestation n spontaneous (miscarriage) or induced n 10% of all pregnancies end in a miscarriage n Most in 1 st Trimester n

Hemorrhagic Complications n Types of Abortions (know the differences) ¨ Threatened ¨ Imminent ¨ Incomplete ¨ Missed ¨ Habitual
Other Hemorrhagic Complications n Ectopic Pregnancy ¨ Egg n implants outside of uterus ¨ Lots of pain and internal bleeding –manifested by sx of shock—lifethreatening ¨ Surgical intervention needed ¨ Link with photos Hydatidiform Mole ¨ No fetus, Fluid filled vesicles ¨ N&V, No FHT’s, 2 nd trimester bleeding— Prune-juice ¨ D&C ¨ Not get pregnant for 1 year ¨ Choriocarcinoma, if HCG elevated
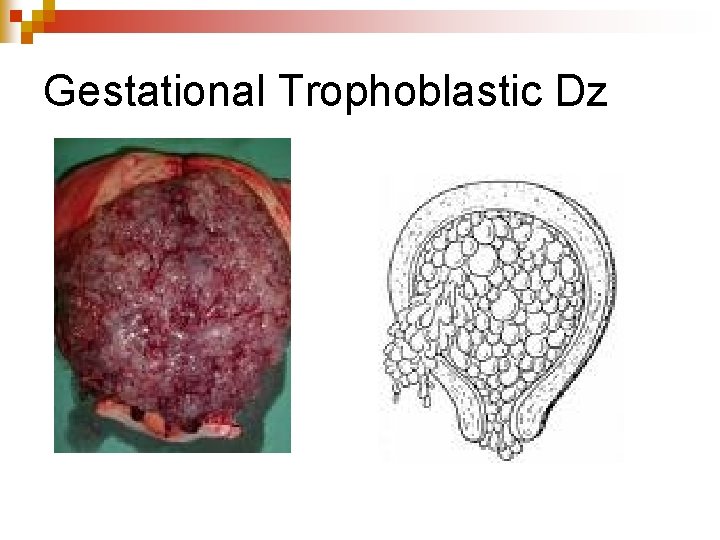
Gestational Trophoblastic Dz

Other Pregnancy Complications n Cervical Insufficiency (Incompetent Cervix) may lead to premature delivery ¨ Cerclage— Mc. Donald’s or Shirodkar procedure n 10 -14 weeks gestation n NO Intercourse, Prolonged standing, heavy lifting n On bedrest as much as possible for 24 -48 hr. n Teach signs of Preterm Labor n Take tocolytics as ordered n Home uterine monitoring ¨ Remove suture at 37 weeks vaginal ¨ Leave suture in C/Sec
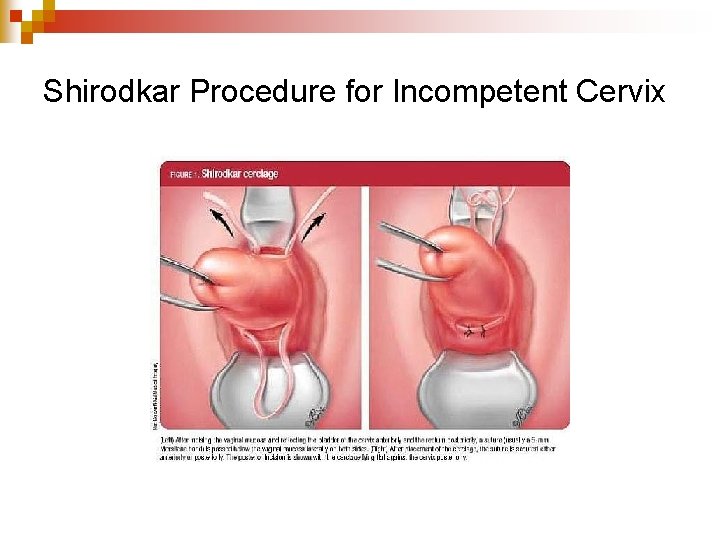
Shirodkar Procedure for Incompetent Cervix

Other Complication of Pregnancy Hyperemesis Gravidarum n n Intractable Vomiting in Pregnancy 5% loss of body weight, dehydration, ketosis, metabolic alkalosis, Rule out Gestational Trophoblastic Dz by ultrasound Medical Management/Nursing Care ¨ If doesn’t respond to small, frequent meals, then needs hospitalization: NPO, IV fluids with KCl to prevent hypokalemia, B-vitamin replacement (B 1 and B 6 especially) ¨ If still unable to eat, may need TPN temporarily

There you have it! Refer to other supplement for more detail on these complications
- Slides: 58