Bacterial meningitis meningitis l An inflammation of the

Bacterial meningitis

meningitis l An inflammation of the leptomeninges. l bacterial meningitis is a common complication of septicemia in children and must be treated as an emergency. l Caused by : bacteria, viruses , or rarely fungi. viral infection of the CNS are much more common than bacterial infection

meningitis l Bacterial meningitis is one of the most potentially serious infection , in infants and older children. l Associated with a high rate of acute complications and risk of long-term morbidity. l The etiology of meningitis in the neonate and the treatment are generally distinct from in older children

meningitis l A limited number of bacteria are associated with meningitis in normal hosts. l the principle of supportive management and the initial choice of antibiotics can be generalized.

Etiology of meningitis l 2 month – 12 yr: S. pneumonia, N. Meningitidis , H. influenza type b is the most common cause of meningitis in children < 4 -yr

Etiology and epidemiology of meningitis l 2 month : maternal flora and environment. Group B and D. streptococci gram – negative enteric bacilli. and listeria monocytogenes. may be due H. Influenza type b and nonecapsulate and other pathogens

Etiology and epidemiology of meningitis l Lack of immunity ( Ig. M or ig. G anti capsular antibody ) to specific pathogens with young age. l recent colonization with pathogenic bacteria. l Close contact with invasive disease ( respiratory tract secration) l Crowding , poverty , black race , male. l Defect in complement (C 5 - C 8 ) associated with recurrent meningococcal infection.
Etiology and epidemiology of meningitis l ventricular-peritoneal shunts: Coagulase negative staphylococci and corynebacteria. l CSF leaks due to fracture cribriform palate or paranasal sinus ( pneumococcal ). l head trauma or neurosurgical procedures ( staphylococci )

Etiology and epidemiology of meningitis l Splenic disfunction (sickle cell anemia or asplenia ) increased risk of pneumococcal , H. influenza type b , rarely meningococcal sepsis and meningitis. l Immuno-suppressed patients with T-cell defects (AIDS, and malygnancy) : Cryptococcal and L. monocytogens. l Open neural tube defect : Meningomyelocele and lombosacral dermal sinus associated with staphylococci -Aureus and gram – negative.

pathogenesis l Bacterial meningitis is usually hematogenous. (endocarditis , pneumonia , or thrombophlebitis , burns , indwelling catheters ) l Bacteremia precedes the condition or occur at the same time. l microorganisms leads to nasopharyngeal colonization , replication , invasion , and bacteremia.
pathogenesis l Bacteria entry to the CSF through the choroid plexus. and meningeal seeding , binding to specific receptors and production of local cytokines initiates inflammation. l Neutrophilic infiltration , increase vascular premeablity , alterations of blood- brain barrier , and cerebral edema.

pathogenesis l Meningitis rarely may be follow bacterial invasive from a contiguous focus of infection ; Paranasal synusitis , otitis media , mastoiditis , orbital cellulitis, cranial osteomyelitis , penetrating cranial trauma , meningomyeloceles , More often brain abscesses or epidural or subdural empyema follows contiguous infection.

Clinical manifestation l Onset has two patterns; 1. The more dramatic and less common is sudden onset(< 1 day ) rapidly progressive of shock , purpura , DIC , and reduce level of consciousness frequntly resulting in death in 24 hr ( S. pneumoniae , or N. meningitidis ) 2. More often is preceded by several days of upper respiratory tract symptoms or GI symptoms. Subacute 2 -3 day. (H. influenzae)

Clinical manifestation 1. In the young infants: fever usually is present and irritablity , poor feeding , restlessness, may be noted. signs of meningeal inflammation may be minimal. 2. Older child : confusion , back pain , usually Kernig and Brudzinski signs in some children particularly age < 12 -18 mo are not present

Clinical manifestation l Increased ICP headache , diolopia , emesis , bulging fontanel 3 or 6 nerve paralysis, hypertension with bradicardia , apnea or hyperventilation , stupor coma ( brain herniation ) l inflammation of the meninges is associated with (headache , nausea , vomiting , irritability , nuchal regidity , photophobia ) l Arthritis , arthralgia , myalgia , anemia , petechia , purpura

Clinical manifestation l Papilledema is uncommon. intracranial abcess , subdural empyema or occlusion of a dural venous sinus l Focal neurologic signs are due to vascular occlusion (10 -20% ) l Seizures occur in 20 -30% Seizures that occure on presentation or within the first 4 days of onset are no prognostic significance


Clinical manifestation l Seizures cerebritis, infarction , electrolyte l Alteration of mental status increased ICP, cerebritis , hypotension
Clinical manifestation l Kernig sign: Flexion of the hip 90 degrees with subsequent pain with extension of the leg. l Brudzinski sign : Involuntary flexion of the knees and hips after passive flexion of the neck while supine.

diagnosis l Blood culture ( reveal responsible bacteria 50 -90% ) l LP analysis CSF for WBC count with diff , protein, glucose , Gram stain helpful in 90% , culture) CSF leukocyte count elevated >1000 and neutrophil (75 -95%) l In tramatic LP Gram stain , culture , glucose level may not be influenced.

diagnosis 1. 2. 3. 4. 5. LP should be performed in every child when bacterial meningitis is suspected. Except : when signs of increased ICP are present. Infection at the LP site. Suspicion of a mass lesion. Extreme patient instability. Thrombocytopenia is a relative contraindication.

diagnosis l Patient in the flexed lateral decubitus position. l Intervertebral space L 3 -L 4 or L 4 -L 5. Turbid CSF when CSF leukocyte count >200 -400. l Pleocytosis may be absent and is a poor prognostic sign. l Pleocytosis with a lymphocytosis may be present during early stage of acute meningitis

Differential diagnosis l Acute viral meningoencephalytis( PMN may be prodominant) l Partial treatment of a acute bacterial meningitis. (glucose , protein , neutrophile are not aletread) l TB , fungal , spirochete , , brain abcess , encephalitis bacterial endocarditis with embolism , subdural empyema , subarachnoid hemmorhage , l Careful examination CSF , and additional laboratory tests are important.
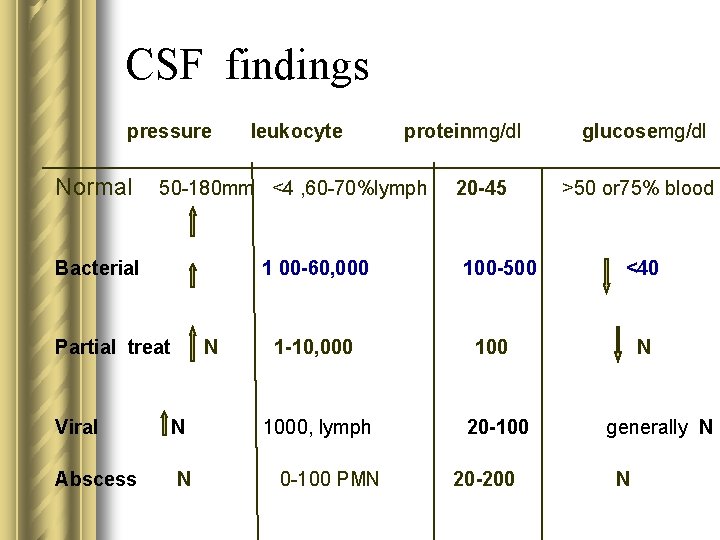

CSF findings pressure Normal leukocyte proteinmg/dl 50 -180 mm <4 , 60 -70%lymph Bacterial 1 00 -60, 000 Partial treat N Viral N Abscess N 20 -45 100 -500 1 -10, 000 1000, lymph 20 -100 PMN 20 -200 glucosemg/dl >50 or 75% blood <40 N generally N N

treatment 1. Decreasing CSF damage caused by the inflammation response with dexamethasone 0. 6 mg/kg/24 hr for 2 days 2. 3. Sterilization of CSF. Supportive therapy : Maintenance of adequate CNS systemic perfusion. Treatment shock , DIC, SAIDH , seizures , ICP increased , apnea , arrhythmia , coma.

complication l Seizure , increased ICP , nerves palsies , stroke , cerebral or cerebellar herniation , thrombosis venous sinuses, l Subdural effusion : in 10 -30% that asymtomatic in 85 -90%. In Symptomatic patient with increased ICP depressed consciousness aspiration must be done. Fever alone is not indication of aspiration.

treatment l Empirical choice must cover S. pneumoniae. l Many of which are Relatively resistance to penicillin (mic 0. 1 -1) is more common than high – level resistance. l Cefotaxime (200 -300 mg/kg/24) or ceftrixone (100 mg/kg/24) plus vancomycin (60 mg/kg/24). l Cefotaxime and ceftrixone also cover N. meningitidis or H. influenza type b. l if L-monocytogenes is suspected ( infant<2 mo ) Ampicillin 200/kg/24 hr plus ceftriaxone.

Duration of treatment l S. Pneumoniae ( 10 -14 days) l N. Meningitidis ( 7 days) l H. influenza (10 days) l Gram negative meningitis should be treated for 3 WK or 2 WK after CSF sterilization. l Patients with evidence of acute bacterial meningitis but no identifiable pathogen cetrixone for 7 -10 days.
repeat CSF examination l Repeat LP indicated ; 1. 2. 3. in neonate Gram negative meningitis In β – lactam resistance S, pneumoniae. l CSF should be sterile within 24 - 48 hr

Prevention in meningococcal meningitidis l Chemoprophylaxis: for all close contacts of patients with meningococcal meningitis. with the rifampin 10 mg/kg every 12 hr for 2 days (600 mg) l Close contacts : household, daycare , direct exposure with oral secration ,

Prevention ( H, influenza) l Rifampin should be given to all close family. 20 mg/kg /24 hr once each day for 4 days.

prognosis l Mortality rate H, influenza 8% , meningococcal 15%, for pneumococcal 25%. l 35% survivors have some sequelae; Deafness: is the most common neurologic sequelae. 30% with pneumococcal meningitis and 10%meningococ , 520% H. influ. seizures , learning disability , blindness , paresis , ataxia , hydrocephallus , mental retardation
Poor prognosis l Young age. (< 6 mo) l long duration of illness before antibiotic therapy. l late –onset seizure (>4 days). l shock , coma, focal neurologic sign l low or absent CSF WBC in the presence of visible bacteria on gram stain of CSF. l immuno compromised status.

Thanks… But it’s not the end !!
- Slides: 34