Surgical Management of Renal Stone Abbas Hassanpour MD

ﺍﻟﻠ ﺍﻟ ﻣ ﺍﻟ ﺣﻴ Surgical Management of Renal Stone Abbas Hassanpour, MD Assistant Proffessor of Urology Jahrom College of Medicine

Historical Aspects of stone Disease n Bladder & Kidney stones 4800 BC (Egypt) n Nobel Prize in Physiology & Medicine for studies on Oxalate (Gunter Blobel, 1999)

HIPPOCRATIC OATH : “I Will not cut, even for the stone, but leave such procedures for the practitioners of the craft”

COMPARATIVE INCIDENCES OF FORMS OF URINARY LITHIASIS Form of Lithiasis India USA Japan UK Pure Calcium Oxalate 86. 1 33 17. 4 39. 4 Mixed Calcium Oxalate and Phosphate 4. 9 34 50. 8 20. 2 Magnesium Ammonium Phosphate (Struvite ) 2. 7 15 17. 4 15. 4 Uric Acid 1. 2 8. 0 4. 4 8. 0 Cystine 0. 4 3. 0 1. 0 2. 8

Cause of Stone Disease n Supersaturation of urine is the key to stone formation n Intermittent supersaturation - Dehydration n Nucleation, Crystal growrth, Crystal aggregation n Anatomic Abnormailities – UPJ , MSK n Bacterial Infection n Defects in transport of Calcium and Oxalate by Renal epithelia E. Coli infection increases matrix content in urine. Proteus makes urine alkaline

Inhibitors & Promoters of Stone Formation in Urine INHIBITORS Inhibits crystal Growth n Citrate – complexes with Ca n Magnesium – complexes with oxalates n Pyrphosphate complexes with Ca n Zinc Inhibits crystal Aggregation n Glycosaminoglycans n Nephrocalcin n Tamm- Horsfall Protein PROMOTERS n Bacterial Infection n Matrix n Anatomic Abnormalities – UPJ obst. , MSK n Altered Ca and oxalate transport in renal epithelia n Prolonged immobilisation n Increased uric acid levels I. e taking increased purine subs– promotes crystalisation of Ca and oxalate n ? ? Nanobacteria – seen in 97% of renal stones

SOME DISEASES ASSOCIATED WITH HYPERCALCAEMIA & HYPERCALCIURIA Hyperparathyroidism Leukemia Sarcoidosisa Lymphoma Multiple myeloma Hyperthyroidism Adrenal Metastatic Malig. Neoplasm's Vit. D Intoxication

Uncommon Stones XANTHINE STONES – (Autosomal Recessive. Def of Xanthine Oxidase leading to Xanthinuria) DIHYDROXYADENINE STONE – ( Def. of enzyme adenine phospo ribosyl transferase ) Sl. LICATE STONES – Rare in humans ( excess intake of Antacid with Mg Trisilicate. Mostly in cattle due to ingestion of Sand ) MATRIX - Infection by Proteus - Radiolucent (all calculi have some amt ( 3%) of matrix but matrix calculus has 65% Matrix content in calculi)

Uncommon Stones TRIAMTERENE – Anti-hypertensive used with hydroclorothiazide – spare Potassium. Mostly found as a nucleus in Ca oxalate or uric acid calculus Indinavir Stones - Drug to treat AIDS (4 to 13%) Ephedrine or Guifenesin – Cough medicine - Radiolucent

Stones – Chemical Constituents n Whewelite – Calcium Oxalate Monohydrate – Ca. C 2 O 4 -H 2 O n Weddelite - Calcium Oxalate dihydrate – Ca. C 2 O 4 -2 H 2 O n Brushite – Calcium Hydrogen phosphate dihydrate – Ca. HPO 4 2 H 2 O n Whitlockite - Tri. Calcium Phosphate – Ca 2(PO 4)2 n Struvite – Magnesium Ammonium hexahydrate – Mg. NH 4 PO 46 H 2 O

OXALATE (CALCIUM OXALATE) n ALSO CALLED MULBERRY STONE n COVERED WITH SHARP PROJECTIONS n SHARP Proj. MAKES KIDNEY BLEED (HAEMATURIA) n VERY HARD n RADIO - OPAQUE Under microscope looks like Hourglass or Dumbbell shape if monohydrate and Like an Envelope if Dihydrate

Pathophysiology of CALCIUM OXALATE stone n n n Hypercalciuria: Absorptive(I, II &III) Renal Resorptive Idiopathic Hypercalcemia Hyperoxaluria: Primary(Rare- genetic defect) Enteric(Short bowl) Idiopathic Hyperuricosuria(High protein diet) Hypocitaturia(Acidosis) Hypomagnesemia(IBD)

Medical Management of CALCIUM OXALATE stone n n n n n High fluid Low protein Nl calcium diet Low sodiom Low oxalate? Thiasides Orthophosphate Allopurinol Citrate Magnesium

LIQUIDS & FOODS Containing Oxalate Moderate Amounts : High Amounts : Apple Juice Cocoa Beer Fresh Tea Coffee Cola FOODS : Almonds, Asparagus, Cashew Nuts, Currants, Greens, Plums, Raspberries, Spinach

Struvite stones Composed of magnesium ammonium phosphate “triple phosphate” crystals n Precipitate at alkaline p. H created by urease producing bacteria such as Proteus or Klebsiella n Urease Urea NH 3 + H 20 2 NH 3 + CO 2 NH 4+ + OH-

Magnesium ammonium phosphate crystals – orthorhombic shape

Struvite stones cont. Occur 3: 1 ratio female: male n More common in those anatomically predisposed to infection such as with neurogenic bladder or urinary diversion n Staghorn calculi may also contain mixed calcium/struvite or all calcium stones n The presence of calcium warrants metabolic workup for cause of stones n

Struvite stone symptoms n n n Often no symptoms directly related to stone May present with UTI, flank pain, hematuria Passage of struvite stone is rare Can rapidly grow and lead to chronic pyelonephritis and parenchymal scarring Struvite stones are radiopaque and can be seen on X-Ray and CT
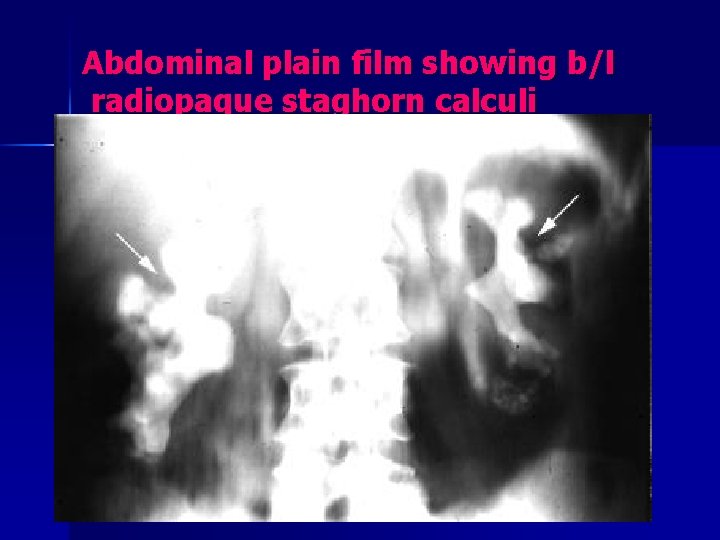
Abdominal plain film showing b/l radiopaque staghorn calculi
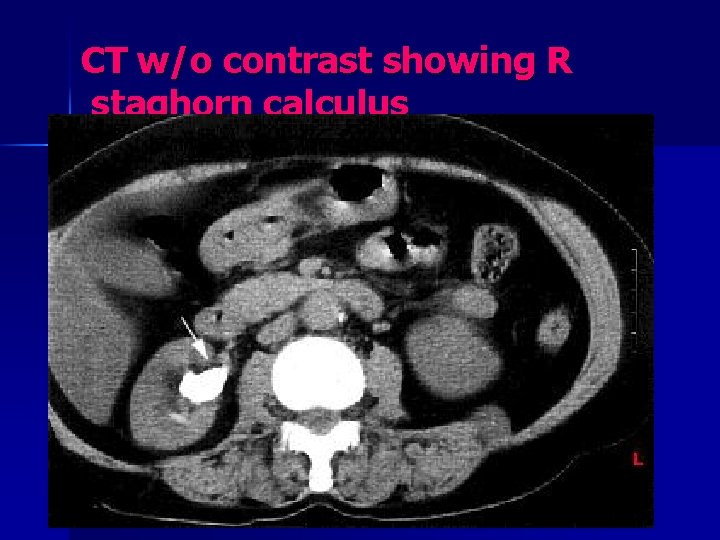
CT w/o contrast showing R staghorn calculus

Medical management of struvite calculi n n n Dietary phosphorus reduction Antibiotics rarely successful at eradicating bacteria in struvite stone Acetohydoxamic acid (AHA, Lithostat) is a urease inhibitor that has been shown to stop stone growth in 80% vs. 40% on placebo. Use is limited by frequent side effects including palpitations, nausea, and hemolytic anemia

PHOSPHATE STONE n USUALLY ® CALCIUM PHOSPHATE n SOMETIMES ® CALCIUM MAGNESIUM AMMONIUM PHOSPHATE OR TRIPLE PHOSPHATE n SMOOTH ® MINIMUM SYMPTOMS n DIRTY WHITE n The most RADIO - OPAQUE Calcium Phosphate also called ‘Brushite’ appears like Needle shape under microscope

PHOSPHATE STONES IN ALKALINE URINE ¯ ENLARGES RAPIDLY ¯ TAKE SHAPE OF CALYCES ¯ STAGHORN ® Struvite can form Stag-horn and appear like coffin lid under microscope

CALCIUM PHOSPHATE STONES n Hyperparathyroidism Ca P Renal Tubular Acidosis K Urine PH n Medullary Sponge Kidney n PTH Hormone Promotes renal production of 1 -25 dihyroxycholecalciferol – active Vit. D and also increases absorption of Calcium and decreases Phosphorus absorption from Kidneys

URIC ACID & URATE STONE n Relatively HARD & SMOOTH n MULTIPLE or STAGHORN n YELLOW OR RED-BROWN n RADIO - LUCENT (USE ULTRASOUND) Under microscope appear like irregular plates or rosettes p. Ka of uric acid 5. 75 – at this p. H 50% of uric acid insoluble. If p. H falls further - uric acid more insoluble

Pathophysiology & Medical Management of Uric Acid stone Defect on Hypoxanthine cycle n High fluid n Low purine diet n Alkaline urine n Allopurinol n

CYSTINE STONE n AUTOSOMAL RECESIVE DISORDER n USUALLY IN YOUNG GIRLS n DUE TO CYSTINURIA - n CYSTINE NOT ABSORBED BY TUBULES n MULTIPLE n SOFT OR HARD – can form stag-horns n PINK OR YELLOW n RADIO-OPAQUE (ground-glass appearance) Under microscope appears like hexagonal or benezene ring – ask for first morning sample

CYSTINE STONE - Management n High Fluid Intake and Alkalanise Urine – dissolve most of the smaller cystine stones n D-Pencillamine or MPG (Mercaptopropionylglycine) binds to cystine that is soluble in urine tiopronin, and captopril n Side effects of Pencillamine restricts it use – Allergic rashes, GI problems- Nausea, Vomiting, Diarrhoea n MPG better tolerated n Large obstructive stones – Surgery required first p. Ka of cystine is 8. 3, hence alkalinisisation above p. H 7. 5 helps to dissolve t Cyanide Nitroprusside Calorimeteric Test for detecting Cystinuria. If positive do amino acid chromatography

Medical Evaluation Management(General) n n 63% of adult men with a single stone episode will form further stones Patients with a single stone have the same incidence and severity of metabolic derangements as recurrent stone formers A metabolic cause can be found in approximately 97% of those evaluated Cost and inconvenience of metabolic evaluation must be balanced against risk of further stones

Medical Management(General) n Therefore one solution is to reserve full evaluation for high risk patients – Middle aged men with a family history of stones – Patients with chronic diarrhoeal states, pathological fractures, osteoporosis, gout, UTIs – Any patient with cystine, uric acid, or struvite (infection) stones – All children

Renal Colic The ureter is narrow at 3 points n A. at the ureteropelvic junction n B. at the point where the ureter crosses over the iliac vessels 4 mm n C. in the ureterovesical zone 1 -5 mm n
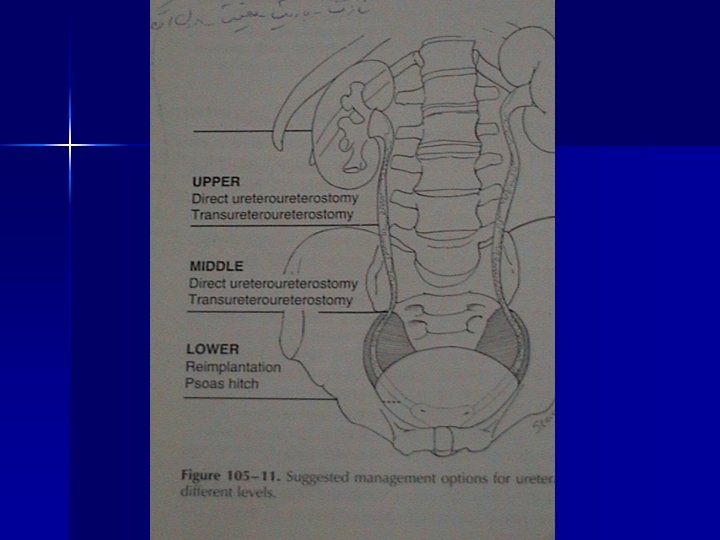

Renal Colic n n n The causes of pain? Typically occurs at night / early morning. Abrupt onset, affecting patient at rest Begins in flank, radiates around abdomen. As stone progresses down ureter may get pain in groin and testes / labia Nausea, vomiting, intestinal ileus common Pale, sweating, tachycardic ? Strangury

Differential Diagnosis of renal colic Gastro-enteritis n Acute appendicitis n Diverticulitis n Salpingitis n Cholecystitis n Pyelonephritis n Ruptured Aortic Aneurysm n

Renal Colic How much waiting for spontaneous passage of stones? Chance of spontaneous passage: Age, Stone passers, Degree of HUN, Impaction, Size, site, Fluid? , diuretics? , Alpha-Blockers?

Management of Acute Renal Colic n n n Narcotic NSAIDs: 1 - local pain control 2 - Decrease RBF and intrapelvis pressure 3 - Central pain relief Anticholinergics Diuretics Sedative & Hypnotics PDE inhibitors

Obstruction and Fever n n A true Urologic emergency No specific sign or symptom Clues: Hx of stone Not responsive to Antibiotics Toxic During evaluation of complicated UTI Management: Proper Antibiotic and Relief of the Obstruction as soon as possible

INVESTIGATIONS for Renal Colic U/A, U/C n CBC n RFT n KUB X-Ray n IVU n CT Scan n Isotope Scan n

INVESTIGATIONS… IVU OR IVP (INTRA VENOUS UROGRAM) n Not Mandatory n 1 in 40, 000 patients die due to anaphylactic reaction to contrast n Useful for radio-lucent stones & to detect Congenital Anomalies in Urinary tracts
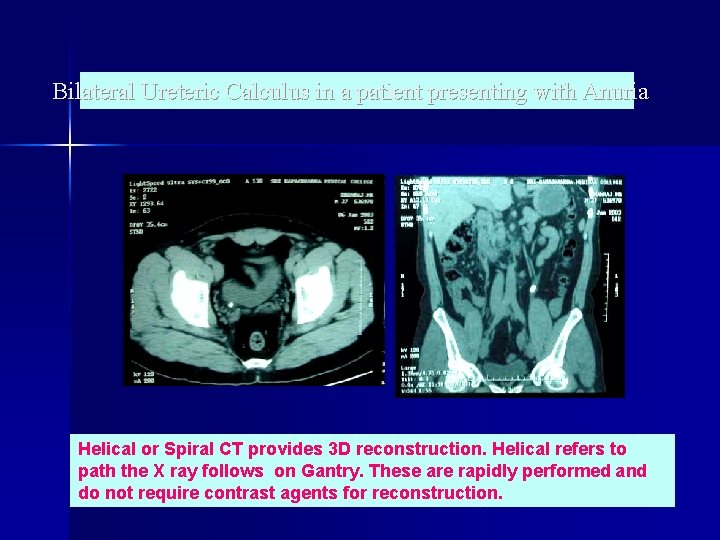
Bilateral Ureteric Calculus in a patient presenting with Anuria Helical or Spiral CT provides 3 D reconstruction. Helical refers to path the X ray follows on Gantry. These are rapidly performed and do not require contrast agents for reconstruction.

SURGICAL MANAGEMENT OF UROLITHIASIS n Non-invasive approach to urinary calculas. HALLMARK of last 20 yrs. Lithotripters – 1. Extra Corporeal Shock wave 2. Intra Corporeal n Better fiber optics – Miniturisation of Telescopes n

Surgical Management of Stones n n n n Extra corporeal Shock Wave Lithotripsy (ESWL) Percutaneous Nephrolithotomy (PCNL) Ureteroscopy (TUL) Open procedures(OSS) Management of stones in Pregnancy Bladder stones Urethral Stones

Conservative Management Is the initial management of most stones n Analgesia and antiemetics +/- IV fluids (no benefit from forced diuresis) n Size of stone dictates outcome Diameter (mm) % of stones passing spontaneously <4 90 4 -6 50 >6 10 n

Extracorporeal Shock Wave Lithotripsy(ESWL) n n n First described by Christian Chaussy in 1982 Now the treatment of choice for the majority of renal and ureteric stones Performed on a day case or outpatient basis Minimal complication rate High success rates, though repeat procedures usually necessary

Shock-wave Generator n Electrohydrolic Advantage: effective in breaking stones disadvantage: 1 -Pressure fluctuation from shock to shock 2 -Short electrode life

Shock-wave Generator n Electromagnetic Advantage: 1 -more controllable 2 -repeatable 3 -less pain Disadvantage: subcapsular hematoma

Shock-wave Generator n Piezoelectric Advantages: 1 -The least pain 2 -Focusing accuracy 3 -Long service life Disadvantages : Insufficient power

Mechanism of Stone Fragmentation by ESWL n n On Front Surface – Compresive or positive Forces On Back Surface Of The Stone. Reflection Of Compression Pulse Creates Negative Or Tensile Wave That Travel Back Ward Through Calculi Once Tensile Force Exceeds “ Cohesive Strength” Of Calculi- Fragmentation Occurs Cavitation – Small air bubbles

ESWL COMPLICATIONS n n n Haematuria – is quite common ( short term antibiotics Recommended ) Incomplete stone Fragmentation & Obstruction Sepsis Transient renal dysfunction “Stienstrasse” ( stone street ) usually due to a large “ Leading fragment” ( Stents Recommended prior to ESWL for Calculi > 1. 5 cm ) Theoretical risk of Hypertension - unproven
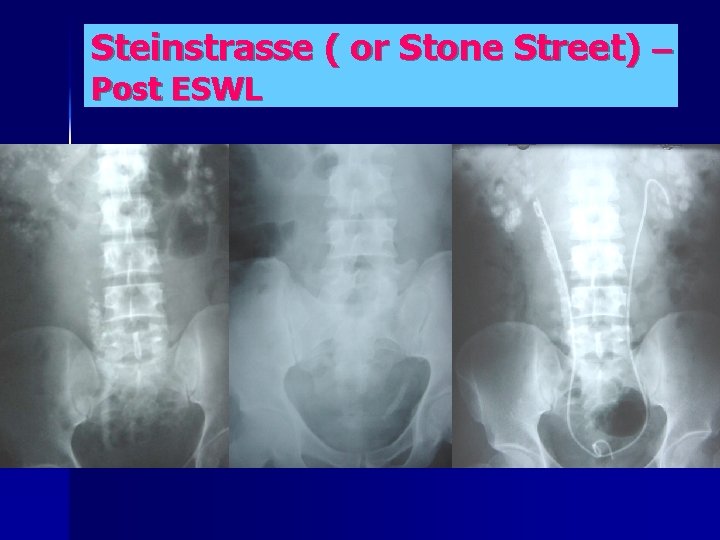
Steinstrasse ( or Stone Street) – Post ESWL

ESWL indicatons n n n Upper & middle calyx<2 cm Pelvis<2 cm Lower calyx <1 cm 1 -2 cm >2 cm UPJ & Upper ureter Middle & Lower Ureter Bladder Calculi

ESWL Contraindications Absolute Contra-indication. Pregnancy Relative Contra-Indications for ESWL – n Renal Colic n Urinary obstruction n Infection n Declining Renal Function n Significant Hematuria

Percutaneous Nephrolithotomy(PCNL) For renal, or upper ureteric stones too large for ESWL>2 cm n Initial management of choice for Staghorn stones where renal function worth preserving(Sandwich therapy) n Stones fragmented under direct vision n

Ureteroscopy n n Made much safer and easier by development of miniature ureteroscopes Ureteroscopy performed under GA Trauma to ureter from ureteroscope is main complication Stone may be – removed by Dormia Basket – Fragmented by ultrasound, laser, Lithoclast

Open Procedures n Now restricted to: – Stones that cannot be removed by other means – In a morbidly obese patient (other procedures technically impossible) – In a patient whose poor health precludes other (lengthier) procedures – For large, complex, staghorn calculi

Management of stones in Pregnancy n n Stones neither more nor less common during pregnancy Most of the usual symptoms of stones are also common in pregnancy - therefore imaging required to confirm stones IVU relatively contraindicated U/S may show hydronephrosis - compatible with normal pregnancy

Management of stones in Pregnancy… Most symptomatic stones in pregnancy are ureteric n Management in most cases is conservative since the majority of stones will pass spontaneously n If stones remain symptomatic then ureteric stenting is most common outcome n

Management of stones in Pregnancy… Other choices include percutaneous nephrostomy tube drainage, and open lithotomy n ESWL is considered contraindicated (? effects on foetus, use of x rays) n Open surgery is contraindicated in last half of pregnancy for lower ureteric stones n

DD of Radiolucent filling defect on IVU in Ureter or Kidney Must Know n n n n Uric Acid Calculus Matrix Calculus Sloughed Papilla Blood Clots TCC Renal Cysts Vascular Lesions Know For Brownie Points n n n n n Xanthine Calculus Hydroxyadenine Calculus Ephederine Calculus Infection due to gas forming Org. Fungal Ball Tuberculoma Malacoplakia Hypertrophied Papilla Renal pseudo-tumour

Conclusions The Investigation and modern management of urinary stones, though challenging, has been transformed by recent technological advances n ESWL remains the initial treatment for most stones n Overall success rates for stone treatments are very good n

Conclusions n n The management of stones in pregnancy remains a challenge to the Urologist Limited metabolic evaluation is worthwhile in the majority of patients

VESICAL STONE Relatively painless. Terminal haematuria, dysuria and interruption of urine flow are due to impaction of the stone in the internal urinary meatus during micturition. n Risk factors 1 -BOO 2 -Malnutrition 3 -Foriegne body n

Management of bladder stones n Choice of procedures – ESWL – Lithotripsy – Litholopaxy – Open Lithotomy
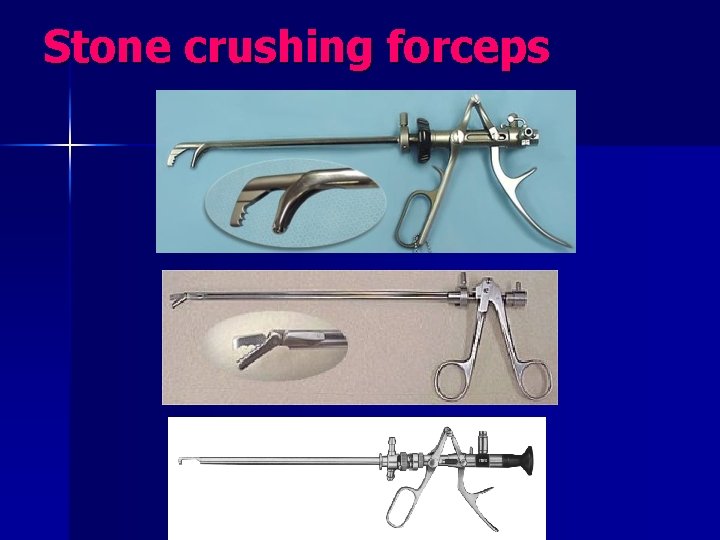
Stone crushing forceps

Urethral Calculi n Symptoms: 1. Sudden stoppage of urination 2. Dribbling of the urine 3. Refferal pain may be radiated to the glans penis

Urethral Calculi Treatment is influenced by the size, shape and position of the calculus and by the status of the urethra n Proximal, bulbar & pendolous Urethra n


- Slides: 68