Otogenic intracranial complications Clinical examination of patients undergoing














































- Slides: 52

Otogenic intracranial complications. Clinical examination of patients undergoing otogenic intracranial complications. The etiology, pathogenesis, classification, clinical features, diagnosis, treatment and prevention. Department of ENT diseases of Tashkent Medical Akademy www. tma. uz

Otogenic intracranial complications. n n For decades, the problem of otogenic intracranial complications was one of the leaders in otolaryngology in the 20 -30 s of this century more than 25% of inpatient ENTpatients were persons with otogenic intracranial complications. A significant breakthrough in the treatment of intracranial otogenic disease occurred after the introduction of antibiotics in practical public health

n Antibiotics, providing a pronounced therapeutic effect of meningitis, meningoencephalitis, sigmoid sinus thrombosis, otogenic sepsis, were little effective in otogenic ulcers (extradural abscesses, and abscesses of the brain and cerebellum), the cranial cavity.

n The percentage of deaths in pure meningitis (meningoencephalitis) and sinus thrombosis (otogenic sepsis) in many hospitals is minimized, while at the same time, an unfavorable outcome in abscess of the brain and cerebellum remains still high - 20 to 50%

n Along with the generally accepted ways and mechanisms of the spread of toxic infection of the middle and inner ear to the cranial cavity in the genesis of intracranial complications, we attach particular importance as the blood brain barrier disruption, which in terms of physiological norm protects against accidental intracranial education and harmful substances circulating in the blood.

n Blood-brain barrier disruption is likely to contribute to other adverse external and internal factors (ported head trauma, highly virulent infections, weakened immune reactivity, etc. ).

n All varieties of otogenic intracranial complications can be divided into two groups: the large form (purulent meningoencephalitis and meningitis, sinus thrombosis and otogenic sepsis, brain abscess, and cerebellum) and small forms (extradural and subdural abscess middle and posterior cranial fossae, and nonsuppurative arachnoiditis arahnoentsefalit , focal nonsuppurative encephalitis, etc. ).

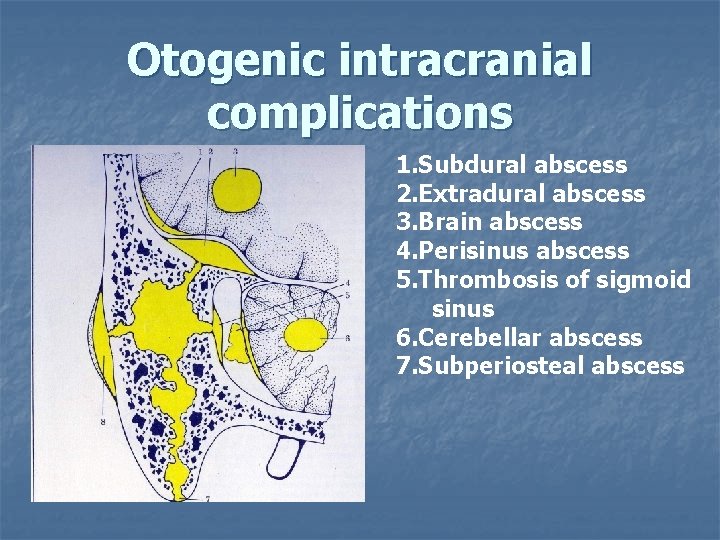
Otogenic intracranial complications 1. Subdural abscess 2. Extradural abscess 3. Brain abscess 4. Perisinus abscess 5. Thrombosis of sigmoid sinus 6. Cerebellar abscess 7. Subperiosteal abscess

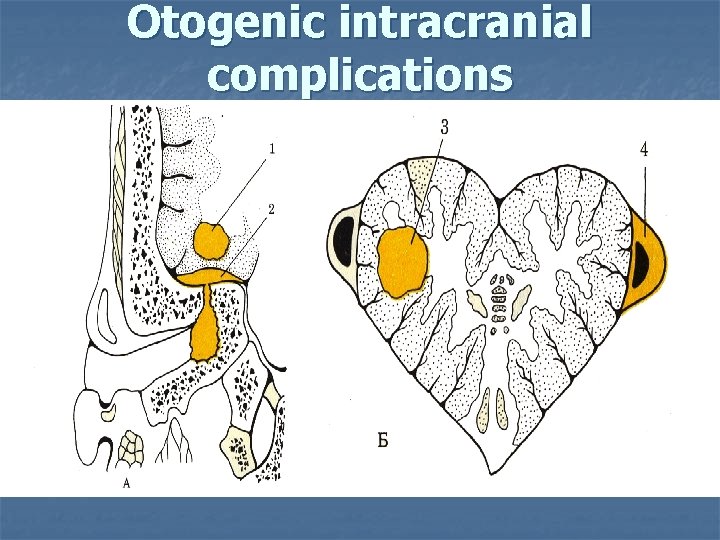
Otogenic intracranial complications

Otogenic purulent meningitis n n n Otogenic purulent meningitis inflammation of the soft and arachnoid meninges with the formation of a purulent exudate, and increased intracranial pressure that occurs with chronic or acute purulent otitis media. Etiology Pathogens are usually identical to the microorganisms causing acute and chronic otitis media.

WAYS of infection in the cranial cavity n n n Pin or the duration of -On pre-existing (preformed) pathways -Labirintogenny -Hematogenous -Lymphogenous Degistsentsii-through

Stages of infection n n The first stage - extradural abscess; The second stage - subdural abscess; Third stage - purulent meningitis; The fourth stage - an abscess of the cerebral hemispheres and cerebellum

Types of Meningitis otogenic n n Primary - due to the spread of infection from the ear to the meninges in different ways. SECONDARY - a consequence of other intracranial complications.

Meningial symptoms in otogenic meningitis n Stiff neck n Upper, lower symptom of Brudzinsk n Kernig's sign n When you join encephalitis marked pyramidal signs (Babinsk, Oppenheim)

Focal symptoms of meningitis n n Of the eye - the optic disc hyperemia, increased stress and veins. Liquor - high pressure (300 -600 millimeter of water), muddy color, low CSF pleocytosis, the presence of protein.

Treatment n n Surgical treatment is aimed at the elimination of the purulent focus in the middle ear (acute otitis media - antromastoidotomy, chronic otitis media extended obschepolostnaya radical surgery); Antibiotic therapy - the use of broad-spectrum antibiotics that penetrate the blood-brain barrier (cephalosporins of the 3 rd generation, metronidazole, penicillin, etc. ). Also, antibiotics are introduced into the spinal canal;

Treatment n n n Disintoxication therapy (reopolyglucin, native plasma, etc. ); Dehydration therapy (Lasix, 40% glucose, etc. ); Antihistamines intramuscularly (diphenhydramine, suprastin, etc. ); Parenteral corticosteroids; Symptomatic therapy.

Common symptoms of purulent labyrinthitis and cerebellar abscess. n n n And for purulent labyrinthitis, and cerebellar abscess is characterized by the following: a) vertigo b) nystagmus c) incoordination d) skeletal muscle dysfunction

Criteria for differential diagnosis of purulent labyrinthitis and cerebellar abscess. n n a) Nystagmus and its characteristics (plane, strength, speed oscillating cycles, the amplitude of the rhythm) b) Koordinator test (tonic deviation of the reaction of the limbs): paltsenosovaya - patient spreads his hands apart and open at first and then with eyes closed trying to touch the tip of his nose, finger - the patient is alternately left and right hand index finger should go in forefinger doctor at arm's length at first open and then with eyes closed, knee-heel - the patient must be with closed eyes lying on her back with one leg to the shin the other foot on the level of the knee and back down

n n Stability in the Romberg position - is surveyed, brought together by the feet so that your heels and toes touching, arms extended forward at chest level, fingers spread apart, eyes closed. d) The nature of gait in a straight line (the patient with eyes closed makes 5 steps forward in a straight line and, without turning, 5 steps back) and flank (the right patient dismiss his right foot, puts the left and does so five steps, and then similarly returns to the lef.

n n e) Test for diadohokinez - the patient with eyes closed stretches out his hands and makes a quick change of supination and pronation e) The characteristics of vertigo d) Samples for detection of latent vestibular disorders (caloric, rotational) - can be applied only in cases of doubt, when it is necessary for definitive diagnosis e) Laboratory and instrumental methods of analysis: blood count, examination of the cerebrospinal fluid, blood pressure measurement;

Features of the clinic abscess of the cerebellum. n n 1. The gradual development of a process with signs of intracranial space-occupying lesions (hypertensive symptoms): a) until a pronounced local unbearable headache in the occipital region, worse in the afternoon and at night (the dominant symptom) b) nausea and vomiting at the height of a headache c) bradycardia (45/min to)

Features of the clinic abscess of the cerebellum. n n n d) refractory to medical therapy rise in blood pressure Characterized by a forced position of the head with a slope on one side 2. Vertigo abscesses of the cerebellum is not pronounced rotational vertigo. Patients prefer to lie on the affected side with a healthy side angled eyes, as this vertigo and nystagmus somewhat inhibited. The direction of the fall of the patient for dizziness does not change depending on the position of the head.

n n n 3. Cerebellar ataxia: a) The finger-nose (the most specific, because the preferential localization of otogenic abscesses of the hemispheres of the cerebellum upper front), heel-knee, finger test - the patient misses a "sick" side (toward the lesion) b) Romberg patient is unstable and falls toward the affected hemisphere of the cerebellum

c) adiadohokinez - on the affected side there is a sharp gap hand n d) violation of the flank of gait in the direction of destruction n 4. Nystagmus horizontal large sprawling, constant or growing, is directed towards the lesion. In rare cases, nystagmus vertical. n

5. Hypotonia of the muscles on the affected side, slow speech, its "blurring" and chanting (at the expense of muscle tone of the language). n 6. Perhaps a combined lesion of the facial (peripheral facial paresis, and paralysis of muscles) and abducens (esotropia, diplopia) due to increased compression of the cerebellum in the cerebellopontine angle n

n n n 7. Characterized by progressive stagnation nipples optic nerves, visual disturbance and change in visual fields. 8. Inflammatory changes in the blood (the shift to the left of the formula, the increase in ESR, leukocytosis). 9. In the study of cerebrospinal fluid: high blood pressure, elevated protein and lymphocytic pleocytosis predominantly mild (protein-cell dissociation).

n n 10. Severe symptoms of intoxication (lethargy, weakness, fatigue, lack of appetite, drowsiness, pale skin). Low-grade temperature, with occasional rises above 38 C, accompanied by a fever. The discrepancy between heart rate (bradycardia) and temperatures (a symptom of scissors). 11. Characterized by meningeal symptoms (most often neck stiffness, Kernig's symptom in the absence of or with mild symptoms of Kernig’s)

STAGE otogenic brain abscess n n Initial Latent Explicit Terminal

INITIAL PHASE n Lasts 1 to 2 weeks. Accompanied by a mild headache, rise in body temperature to 37. 5 C, vomiting, and poor health.

Latent stage n This stage of the poor of symptoms the patient lethargy, paleness, poor appetite, recurrent headache.

Explicit STAGE n Manifested by a sudden apparent satisfactory overall condition of the patient. The dynamics of the process tends to be a gradual deterioration. Increased body temperature depends on the concomitant purulent otitis media. The pulse rate is usually 5060 bpm. in min. , ie observed bradycardia.

End-stage n At this stage there are gross violations of the cardiovascular system due to intoxication, cerebral edema with paralysis of the vascular center.

Otogenic brain abscess and cerebellar n n n The main pathway Pin, is mainly formed by a single abscess. Location otogenic brain abscesses most often the temporal, temporoparietal lobe.

Extradural abscess n n Extradural abscess - a collection of pus between the dura and bone. This is the result of the spread of the inflammatory process of the mastoid and tympanic cavity in the skull cavity. Located in the middle or in the posterior fossa

Subdural abscess n Subdural ABSTs. ESSf. SUBDURALNY abscess - a complication of chronic suppurative otitis media, especially holesteatomnogo, much less acute. Located in the middle or posterior fossa.

DIAGNOSIS Abscess n n Computed tomography - the most accurate method of diagnosis. Ehoelektroentsefalography - an important and simple method for the study. Angiography - is widely used in neurosurgical practice. Ventriculography - only in a neurosurgical hospital.

SINUSTRAMBOS n At a depth of 2. 5 - 3 cm from the edge of the ear canal is located sigmoid sinus. It flows into the bulb of the jugular vein. When the disease process comes to a wall, there is an inflammation of the outer wall of the sinus, followed by a contact in the inflammatory process involves the intima. There is an infected blood clot in the main vessel.

Arachnoiditis n Arachnoiditis - an inflammatory disease of the arachnoid (arachnoid) with involvement in the process of pia mater. Occurs when the etiology of common infections (influenza, pneumonia, measles, etc. ), foci of focal infections (sinusitis, tonsillitis, sinusitis, otitis, etc. ), traumatic brain injury. In some cases, patients develop encephalitis (arahnoentsefalit), myelitis (arahnomielit).

Pathogenesis n In arachnoid develops reactive inflammation due to exposure to the pathogen, its toxins, brain edema, disorders of the blood and lymph circulation. Depending on the nature and location changes distinguish Adhesive, cystic-adhesive, cerebral (basal-and convexital optohiazmalny, posterior fossa, bridge-cerebellar angle) and spinal arachnoiditis. Latest in children is rare. By the nature of the flow may be acute (rare), subacute and chronic.

The clinical picture n With cerebral arachnoiditis with subacute and chronic observed moderate cerebral disorders: headache Expander or oppressive character, nausea and sometimes vomiting, and dizziness. Headache - a constant symptom arachnoiditis.

The clinical picture n It usually is permanent, periodically amplified under the influence of physical and mental overexertion, hypothermia, overheating, and other causes. At the height of a headache to vomiting. There is a general weakness, fatigue, emotional lability

n Focal neurologic deficits depend on the preferential localization of the lesion. When convexital arachnoiditis often arise focal seizures which may become generalized with loss of consciousness. Also observed diffuse or focal neurological symptoms.

n Optohiazmalnogo for arachnoiditis is characteristic slowly progressive or rapidly occurring decrease of one or both sides. In the fundus may be stagnation or neuritis, atrophy of the optic nerve, optic nerve atrophy. May be double vision, ptosis. In some cases, developing hypothalamic metabolic disorders (diabetes insipidus, obesity, etc. ).

n n n Arachnoiditis posterior fossa shows an intense, periodically increasing headache with nausea and vomiting, may develop hydrocephalus. Characterized by cerebellar disorders muscular hypotonia, incoordination, nystagmus. May be stagnant in the fundus.

n The disease often resembles a brain tumor. The most characteristic symptoms of arachnoiditis cerebellopontine angle - a unilateral hearing loss, facial nerve lesion, later joined by cerebellar disorders.

Diagnosis n The diagnosis is substantiated data neurological examination and finally confirmed by pneumoencephalography or computed tomography. You should avoid overdiagnosis of arachnoiditis.

Treatment n In acute disease course shows antibiotics: penicillin, semisynthetic penicillins (methicillin, ampioks) in high therapeutic doses. n For the treatment of sub-acute and chronic arachnoiditis appointed dehydrating - diakarb, furosemide, absorbable - aloe extract, plazmol, vitreous lidazy; n

n Treatment bracing (vitamins, ATP) and symptomatic agents. You can use iodine electrophoresis on an orbital-occipital technique. n In the presence of seizures appointed anticonvulsants. Is the treatment of focal infection. In the case of cystic arachnoiditis sometimes shown neurosurgical treatment. n

Treatment of otogenic intracranial complications n n n Extended operation sanifying ear. Antibiotic therapy. Pathogenetic therapy. Disintoxication therapy. Symptomatic therapy.

Prophylaxis n Early diagnosis and treatment of acute infectious diseases, prevention of infectious disease outbreaks focal infections, traumatic brain injury.

Department of ENT diseases of Tashkent Medical Academy www. tma. uz