Presentation title Date 1 Gestational Diabetes Mellitus GDM

Presentation title Date 1 Gestational Diabetes Mellitus (GDM) Training, Madhya Pradesh 1 -2 April, 2016 Dr Sachin Chittawar DM (Endocrinology)

Presentation title Agenda 1. Diabetes – a public health crisis 2. Diabetes and maternal health and pregnancy 3. Gestational diabetes and pregnancy outcomes 4. National guidelines for diagnosis and management of GDM • Testing for GDM • Management of GDM Date 2

Presentation title Date Diabetes a public health crisis 3

Presentation title Date Globally diabetes has reached pandemic status As of 2015 415 million people have diabetes 1 318 million people have prediabetes*, 1 * Prediabetes is the number of people estimated to have impaired glucose tolerance, a precursor to developing type 2 diabetes Source: IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015 4
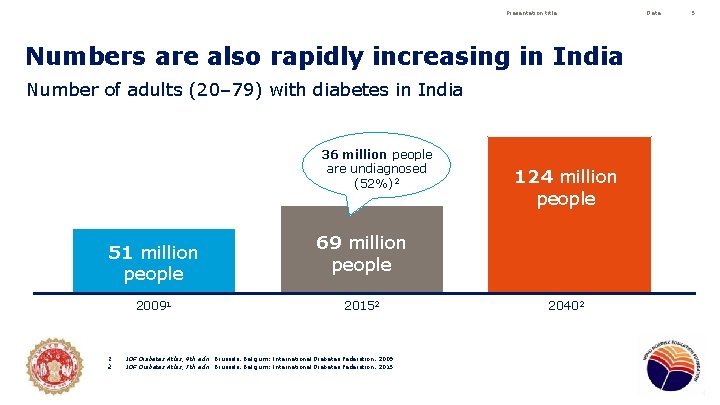
Presentation title Numbers are also rapidly increasing in India Number of adults (20– 79) with diabetes in India 36 million people are undiagnosed (52%)2 51 million people 20091 1. 2. 124 million people 69 million people 20152 IDF Diabetes Atlas, 4 th edn. Brussels, Belgium: International Diabetes Federation, 2009 IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015 20402 Date 5

Presentation title Date 6 Diabetes is associated with serious complications Consistently high blood glucose levels can lead to serious disease affecting the heart and blood vessels, eyes, kidneys and nerves STROKE Strokes are up to four times as likely BLINDNESS Diabetes is a leading cause of blindness HEART ATTACK Heart attack is three times as likely Source: IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015 KIDNEY FAILURE Total kidney failure is three times as likely AMPUTATION Diabetes is a leading cause of nontraumatic lower-limb amputations
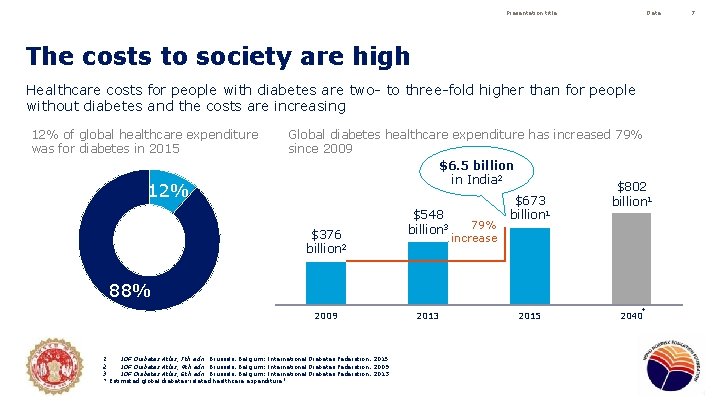
Presentation title Date The costs to society are high Healthcare costs for people with diabetes are two- to three-fold higher than for people without diabetes and the costs are increasing 12% of global healthcare expenditure was for diabetes in 2015 12% Global diabetes healthcare expenditure has increased 79% since 2009 $6. 5 billion in India 2 $802 $673 billion 1 1 $548 billion 79% 3 billion $376 increase billion 2 88% 2009 1. 2. 3. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015 IDF Diabetes Atlas, 4 th edn. Brussels, Belgium: International Diabetes Federation, 2009 IDF Diabetes Atlas, 6 th edn. Brussels, Belgium: International Diabetes Federation, 2013 * Estimated global diabetes-related healthcare expenditure 1 2013 2015 * 2040 7

Presentation title Date What does diabetes have to do with maternal health and pregnancy? 8

Presentation title Date Hyperglycaemia in pregnancy can be classified as: Diabetes in Pregnancy (DIP) Diabetes detected prior to pregnancy (Type 1 and Type 2) Diabetes first detected in pregnancy (Type 1 and Type 2) Diabetes continues post delivery Gestational Diabetes (GDM) Pregnant women who have never had diabetes but who have high blood glucose levels during pregnancy Transient and disappears after birth Source: IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015 Hod M, Kapur A, Sacks DA, et al. The International Federation of Gynecology and Obstetrics (FIGO) Initiative on gestational diabetes mellitus: A pragmatic guide for diagnosis, management, and care. International Journal of Gynecology and Obstetrics: the official organ of the International Federation of Gynecology and Obstetrics. 2015; 131: S 173. 9
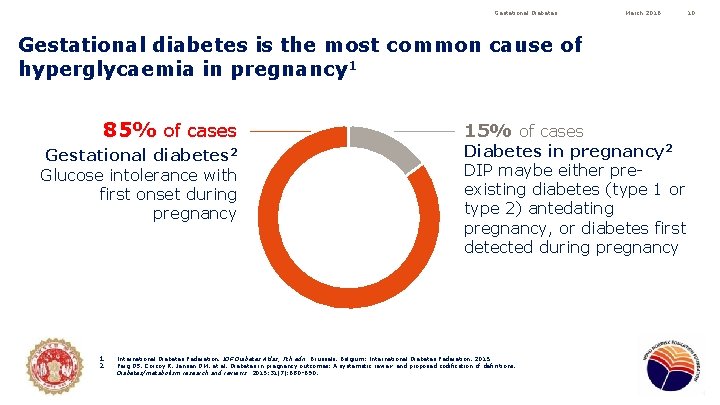
Gestational Diabetes March 2016 Gestational diabetes is the most common cause of hyperglycaemia in pregnancy 1 85% of cases Gestational diabetes 2 Glucose intolerance with first onset during pregnancy 1. 2. 15% of cases Diabetes in pregnancy 2 DIP maybe either preexisting diabetes (type 1 or type 2) antedating pregnancy, or diabetes first detected during pregnancy International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. Feig DS, Corcoy R, Jensen DM, et al. Diabetes in pregnancy outcomes: A systematic review and proposed codification of definitions. Diabetes/metabolism research and reviews. 2015; 31(7): 680– 690. 10
Gestational Diabetes March 2016 Hyperglycaemia is one of the most common medical conditions associated with pregnancy 1 Globally 20. 9 million live births are affected by hyperglycaemia in pregnancy 1 30% (6. 2 million) are in India 1 1. 2. International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. HAPO Study Cooperative Research Group. Hyperglycemia and Adverse Pregnancy Outcome (HAPO) Study associations with neonatal anthropometrics. Diabetes. 2009; 58(2): 453 -459. 11

Gestational Diabetes March 2016 Hyperglycaemia in pregnancy in India 6. 2 million GDM prevalence 27. 6%1 live births are affected by hyperglycaemia in pregnancy 1 Of which, 5. 9 million are due to GDM 1 Difference in GDM urban/rural distribution (Tamil Nadu field study 2) Urban areas 17. 8% 1. 2. Semi-urban areas 13. 8% International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. Nielsen, K. K. , Damm, P. , Kapur, A. , Balaji, V. , Balaji, M. S. , Seshiah, V. , & Bygbjerg, I. C. (2016). Risk Factors for Hyperglycaemia in Pregnancy in Tamil Nadu, India. Plo. S one, 11(3), e 0151311. Rural areas 9. 9% 12

Presentation title Date How does GDM impact pregnancy outcomes? 13

Food for thought!!! All are diabetogenic in GDM except • • • 1) 2) 3) 4) 5) h. PL Progesterone GH increase in insulin Beta cell failure.

Presentation title Date Gestational diabetes is associated with a number of maternal complications • • Pre-eclampsia Polyhydramnios Prolonged labour Obstructed labour Caesarean Section Uterine atony Postpartum haermorrhage Infection 1. Crowther CA, Hiller JE, Moss JR, Mc. Phee AJ, Jeffries WS, Robinson JS. Effect of treatment of gestational diabetes mellitus on pregnancy outcomes. New England Journal of Medicine. 2005; 352(24): 2477– 2486. 2. The HAPO Study Cooperative Research Group, Metzger BE, Lowe LP, et al. Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008; 358(19): 1991– 2002. 3. Hod M, Kapur A, Sacks DA, et al. The International Federation of Gynecology and Obstetrics (FIGO) Initiative on gestational diabetes mellitus: A pragmatic guide for diagnosis, management, and care. International Journal of Gynecology and Obstetrics: the official organ of the International Federation of Gynecology and Obstetrics. 2015; 131: S 173. 4. International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. 5. Ehrenberg HM, Durnwald CP, Catalano P, Mercer BM. The influence of obesity and diabetes on the risk of cesarean delivery. Am J Obstet Gynecol. 2004; 191(3): 969 -974. 7. Rudge MV, Calderon IM, Ramos MD, Peracoli JC, Pim A. Hypertensive disorders in pregnant women with diabetes mellitus. Gynecol Obstet Invest. 1997; 44(1): 11 - 15. 8. Yogev Y, Xenakis EM, Langer O. The association between preeclampsia and the severity of gestational diabetes: the impact of glycemic control. American journal of obstetrics and gynecology. 2004; 191(5): 1655 -1660. 15

Presentation title Date 16 Gestational diabetes is associated with a number of consequences for the foetus • • • Congenital anomalies Intra Uterine Growth Restriction (IUGR) Increase in still-births Macrosomia Increased respiratory problems Jaundice Shoulder dystocia Birth injuries Neonatal hypoglycaemia Infant respiratory distress syndrome 1. Crowther CA, Hiller JE, Moss JR, Mc. Phee AJ, Jeffries WS, Robinson JS. Effect of treatment of gestational diabetes mellitus on pregnancy outcomes. New England Journal of Medicine. 2005; 352(24): 2477– 2486. 2. The HAPO Study Cooperative Research Group, Metzger BE, Lowe LP, et al. Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008; 358(19): 1991– 2002. 3. Hod M, Kapur A, Sacks DA, et al. The International Federation of Gynecology and Obstetrics (FIGO) Initiative on gestational diabetes mellitus: A pragmatic guide for diagnosis, management, and care. International Journal of Gynecology and Obstetrics: the official organ of the International Federation of Gynecology and Obstetrics. 2015; 131: S 173. 4. International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. 5.

Presentation title Date Gestational diabetes also increases the risk for type 2 diabetes in both mother and child Approximately 50% of women with GDM go on to develop type 2 diabetes within five year of pregnancy. Children born to mothers with GDM are up to 8 -times more likely to develop type 2 diabetes and obesity in their teens or early adulthood. SOURCES: 1. Kim C, Newton KM, Knopp RH. Gestational Diabetes and the Incidence of Type 2 Diabetes: A Systematic Review, Diabetes Care 25, 2002. 2. Clausen TD, Mathiesen ER, Hansen T, et al. High prevalence of type 2 diabetes and pre-diabetes in adult offspring of women with gestational diabetes mellitus or type 1 diabetes the role of intrauterine hyperglycemia. Diabetes care. 2008; 31(2): 340 -346 3. Hod M, Kapur A, Sacks DA, et al. The International Federation of Gynecology and Obstetrics (FIGO) l of Gynecology and Obstetrics. 2015; 131: S 137 4. International Diabetes Federation. IDF Diabetes Atlas, 7 th edn. Brussels, Belgium: International Diabetes Federation, 2015. 17

Presentation title Date All of this goes hand in hand with a general rise of the diabetes pandemic 18

Presentation title Date 19 Gestational diabetes risk factors Globally recognised risk factors • • • Personal history of IGT or GDM in a previous pregnancy Ethnicity Family history of diabetes, especially in first degree relatives BMI >30 kg/m 2 Maternal age >25 years of age Previous delivery of a baby >9 pounds (4. 1 kg) • • • Previous unexplained perinatal loss Glycosuria at the first prenatal visit Medical condition/setting associated with development of diabetes, such as metabolic syndrome, polycystic ovary syndrome (PCOS), current use of glucocorticoids, hypertension Risk increases when multiple risk factors are present SOURCES: 1. Solomon, et al. (1997). A prospective study of pregravid determinants of gestational diabetes mellitus. Jama, 278(13), 1078 -1083. 2. Kim, C, et al. (2009). Does frank diabetes in first-degree relatives of a pregnant woman affect the likelihood of her developing gestational diabetes mellitus or nongestational diabetes? . American journal of obstetrics and gynecology, 201(6), 576 -e 1. 2. Hedderson, et al. (2008). Body mass index and weight gain prior to pregnancy and risk of gestational diabetes mellitus. American journal of obstetrics and gynecology, 198(4), 409 -e 1.

Food for thought!!! Exercise increases all except • Insulin secretion. • Insulin independent glucose consumption. • Am. P kinase activity. • Insulin resistance. • Insulin sensitivity.

Presentation title Date GDM risk factors In a recent study (2015) from Tamil Nadu, globally recognised risk factors were not significant: 1 Although risk factors, to some extent, point to additional risk among certain women, testing according to risk factors would imply missing out on 20 -30% of hypoglycaemia in pregnancy cases 1 Source: Nielsen, K. K. , Damm, P. , Kapur, A. , Balaji, V. , Balaji, M. S. , Seshiah, V. , & Bygbjerg, I. C. (2016). Risk Factors for Hyperglycaemia in Pregnancy in Tamil Nadu, India. Plo. S one, 11(3), e 0151311. 21

Presentation title Date GDM risk factors “In India… studies indicate that GDM may be associated with increasing socio-economic status, and similar trends have been found for type 2 diabetes. ” “…among women attending the rural health centre a doubling in income caused an 80% increased risk of HIP [hyperglycaemia in pregnancy]. ” Source: Nielsen, K. K. , Damm, P. , Kapur, A. , Balaji, V. , Balaji, M. S. , Seshiah, V. , & Bygbjerg, I. C. (2016). Risk Factors for Hyperglycaemia in Pregnancy in Tamil Nadu, India. Plo. S one, 11(3), e 0151311. 22

Presentation title Date Screening and diagnostic testing for diabetes are performed because identifying pregnant women with diabetes followed by appropriate therapy can decrease feotal and maternal morbidity, particularly macrosomia, shoulder dystocia, and pre-eclampsia. Universal testing for GDM is recommended 1 Sources: 1. National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 23

Food for thought!!! • What is optimal blood sugars in pregnancy? • • • Fasting >100, PP >150. Fasting >95, PP >140. Fasting <95, PP <140. Fasting ≤ 92, PP ≤ 120. None of the above.

Presentation title Date Are there national guidelines for diagnosis and management of GDM? 25

Presentation title Date 26 National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus Available at: www. nrhmorissa. gov. in/writereaddata/Upload/Doc uments/National%20 Guidelines%20 for%20 Diagno sis%20&%20 Management%20 of%20 Gestational% 20 Diabetes%20 Mellitus. pdf

Presentation title Testing for GDM Date 27

Presentation title Date Testing for GDM Considering the high prevalence of GDM in India and the maternal & foetal morbidity associated with untreated GDM all pregnant women should be tested for GDM • • Testing for GDM is recommended twice during antenatal care (ANC) • First testing done during first ANC contact • Second testing done during 24 -28 weeks of pregnancy if first test is negative • There should be at least 4 weeks gap between the two tests • If a woman presents beyond 28 weeks of pregnancy only one test is done If the test is positive at any point, protocol management should be followed Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 28

Presentation title Date Testing for GDM – protocol of investigations All pregnant women in the community Testing for GDM at 1 st Antenatal visit (75 g oral glucose - 2 hr Plasma Glucose value) Positive (2 hr PG ≥ 140 mg/dl) Manage as GDM as per guidelines Negative (2 hr PG <140 mg/dl) Repeat Testing at 24 -28 weeks Positive (2 hr PG ≥ 140 mg/dl) Negative (2 hr PG < 140 mg/dl) Manage as GDM as per guidelines Manage as normal ANC Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 29

Presentation title Date Methodology: Test for diagnosis • Single step testing using 75 g Oral Glucose Tolerance Test (OGTT) and measuring plasma glucose 2 hours after ingestion • 75 g glucose to be given orally after dissolving in approximately 300 ml water whether woman comes in fasting or non-fasting state • Intake of solution has to be completed within 5 min. • A plasma standardised glucometer should be used to evaluate blood glucose 2 hours after the oral glucose load • If vomiting occurs within 30 min of oral glucose intake the test has to be repeated the next day. If vomiting occurs after 30 minutes the test continues • The threshold plasma glucose level of ≥ 140 mg/d. L is taken as cut off for diagnosis of GDM Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 30

Food for thought!!! True about insulin resistance (IR) ? 1 ) Increases by 50 -60 % in 2 -3 rd trimester. 2) Insulin sensitivity increases by 50 -60 % in 2 -3 3) IR increases in late first trimester. 4) IR decreases in third trimester.

Presentation title Date Management of GDM 32
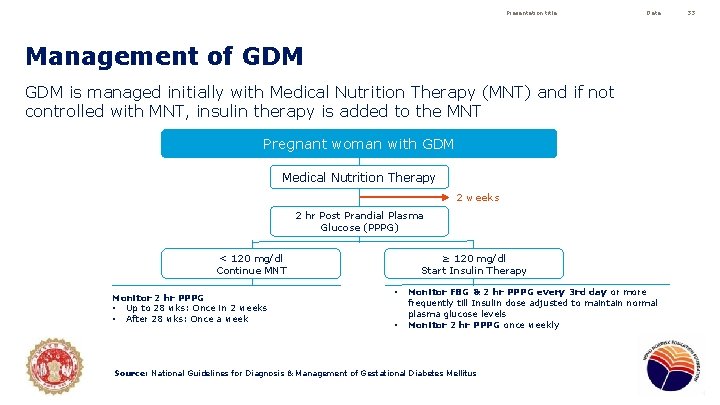
Presentation title Date Management of GDM is managed initially with Medical Nutrition Therapy (MNT) and if not controlled with MNT, insulin therapy is added to the MNT Pregnant woman with GDM Medical Nutrition Therapy 2 weeks 2 hr Post Prandial Plasma Glucose (PPPG) < 120 mg/dl Continue MNT Monitor 2 hr PPPG • Up to 28 wks: Once in 2 weeks • After 28 wks: Once a week ≥ 120 mg/dl Start Insulin Therapy • • Monitor FBG & 2 hr PPPG every 3 rd day or more frequently till Insulin dose adjusted to maintain normal plasma glucose levels Monitor 2 hr PPPG once weekly Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 33

Presentation title Medical Nutrition Therapy (MNT) Overall Principles • In most cases GDM can be managed by Medical Nutrition Therapy (MNT) • Principles of MNT • MNT for GDM primarily involves a carbohydrate controlled balanced meal plan • Nutrition assessment should be individualised • Maternal weight gain is the important measure in follow up visits to determine whether energy intake is adequate to support fetal growth Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus, page 11. Date 34

Presentation title Date Medical Nutrition Therapy (MNT) Careful Selection of Carbohydrates • Carbohydrate foods are essential for a healthy diet for mother and baby. • Once digested, carbohydrate foods are broken down to glucose, which goes into the blood stream. The type, amount and frequency of carbohydrate intake has a major influence on blood glucose readings. • Large amounts of carbohydrate foods eaten at one time will lead to high blood glucose level and should be avoided. It is better to spread carbohydrate foods over 3 small meals and 2 -3 snacks each day than taking 3 large meals. • Complex carbohydrates (e. g. whole grain cereals) should be preferred over simple carbohydrates like foods with lots of added sugar or honey or foods that are made from refined white flour. • Counting the number of carbohydrates serves that a mother eats during the days will help her to eat the right amount. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus, page 11. 35

Presentation title Date Medical Nutrition Therapy (MNT) Understanding Fat Intake During Pregnancy • Saturated fat intake (ghee, butter, coconut oil, palm oil, red meat, organ meat, full cream milk etc. ) should be less than 10% of total calories and dietary cholesterol should be less than 300 mg/day. In obese and overweight patients, a lower fat diet overall can help slow down the rate of weight gain. • Recommendations • • Use less fat in cooking and avoid frying of foods Using low-fat dairy products in place of whole milk or full cream products • Choose low-fat snack (e. g. fresh fruit) instead of high-fat snacks (cakes, biscuits etc. ) • Use lean mean instead of read meat For more details, see: Sample Diet Chart and Food Exchange Chart for MNT in the National GDM Guidelines. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 36

Presentation title Insulin Therapy • When and What • • • Insulin therapy is the accepted medical management of pregnant women with GDM not controlled on MNT in 2 weeks The National Guidelines recommend the use of Human Premix insulin 30/70. Oral tablets for diabetes treatment in pregnancy are not to be given as they are not considered safe. All pregnant women in whom MNT fails to achieve a 2 hr PPPG <120 mg/d. L are started on insulin, along with MNT • In case of very high 2 hr PPPG: • • • If 2 hr PPPG is >200 mg/d. L at diagnosis, starting dose of insulin should be 8 units pre-mixed insulin The dose to be adjusted on follow-up and at the same time MNT has been followed. Frequency of monitoring to be decided by the treating Physician/Gynaecologist/Medical Officer. If the pregnant women requires more than 20 units insulin/day, she should be referred to a higher healthcare centre. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus Date 37

Food for thought!!! Insulin approved in Pregnancy are all except ? • Lispro( Humalog, Humalog mix 25, Humalog mix 50) • Aspart • Detemir , NPH. • Glargine , Gluilisin(Apidra), Degludec, Rizodeg.
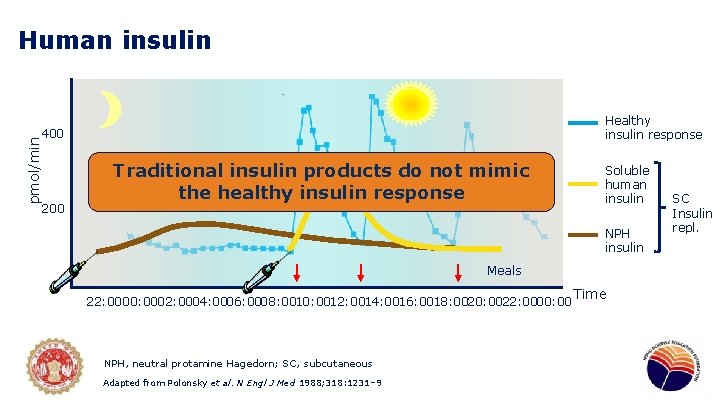
Human insulin Healthy insulin response pmol/min 400 200 Traditional insulin products do not mimic the healthy insulin response Soluble human insulin NPH insulin Meals 22: 0000: 0002: 0004: 0006: 0008: 0010: 0012: 0014: 0016: 0018: 0020: 0022: 0000: 00 NPH, neutral protamine Hagedorn; SC, subcutaneous Adapted from Polonsky et al. N Engl J Med 1988; 318: 1231– 9 Time SC Insulin repl.
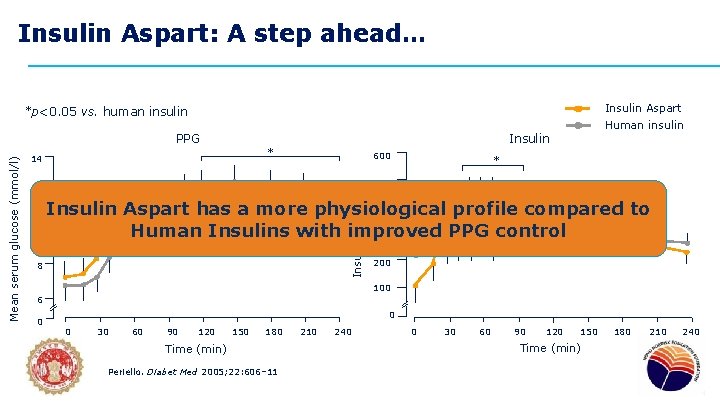
Insulin Aspart: A step ahead… Insulin Aspart *p<0. 05 vs. human insulin * 14 Human insulin Insulin 600 * 500 12 Insulin (pmol/l) Mean serum glucose (mmol/l) PPG 400 Insulin Aspart has a more physiological profile compared to 10 Human Insulins with improved PPG control 300 8 200 100 6 0 0 0 30 60 90 120 150 180 Time (min) Periello. Diabet Med 2005; 22: 606– 11 210 240 0 30 60 90 120 150 Time (min) 180 210 240
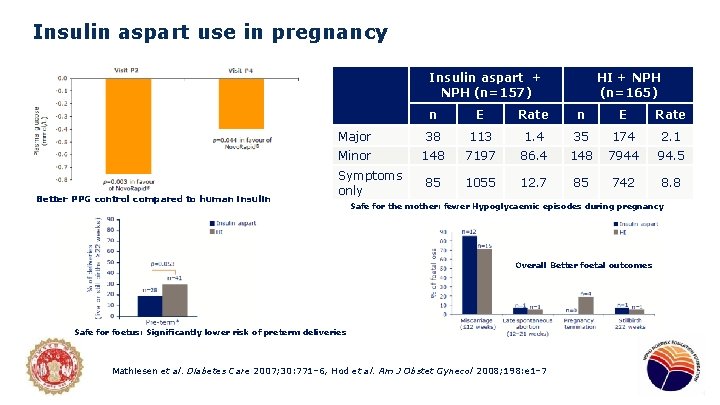
Insulin aspart use in pregnancy Insulin aspart + NPH (n=157) Better PPG control compared to human insulin HI + NPH (n=165) n E Rate Major 38 113 1. 4 35 174 2. 1 Minor 148 7197 86. 4 148 7944 94. 5 85 1055 12. 7 85 742 8. 8 Symptoms only Safe for the mother: fewer Hypoglycaemic episodes during pregnancy Overall Better foetal outcomes Safe for foetus: Significantly lower risk of preterm deliveries Mathiesen et al. Diabetes Care 2007; 30: 771– 6, Hod et al. Am J Obstet Gynecol 2008; 198: e 1– 7

Another Question Which is correct as per color coding of insulin syringe? 1. Red color is 40 IU syringe. 2. Orange for 100 IU syringe. 3. Blue for 500 IU syringe. 4. None of the above 5. All of the above

Presentation title Date Hypoglycaemia How to Recognise Hypoglycaemia • Any pregnant woman on insulin can develop hypoglycaemia at any time • Hypoglycaemia is diagnosed when blood glucose level is < 70 mg/dl • Important to recognise symptoms of hypoglycaemia & treat immediately • Early symptoms - Tremors of hands, sweating, palpitations, hunger, easy fatigability, headache, mood changes, irritability, low attentiveness, tingling sensation around the mouth/lips or any other abnormal feeling • Severe - Confusion, abnormal behaviour or both, visual disturbances, nervousness or anxiety, abnormal behaviour. • Uncommon - Seizures and loss of consciousness Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 43

Presentation title Date Hypoglycaemia How to Manage Hypoglycaemia • Ask the pregnant women to take 3 TSF of glucose powder (15 -20 grams) dissolved in a glass of water • After taking oral glucose, she must take rest & avoid any physical activity • 15 minutes after taking glucose, she must eat one chapati with vegetable/rice/one • glass of milk/idli/fruits/anything eatable which is available • If hypoglycaemia continues, repeat same amount of glucose and wait • If glucose is not available, take one of the following: Sugar - 6 TSF in a glass of water/fruit juice/honey/anything which is sweet/any food • Take rest, eat regularly and check blood glucose if possible • If the pregnant woman develops >1 episode of hypoglycaemia in a day, she should consult any doctor • immediately Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 44
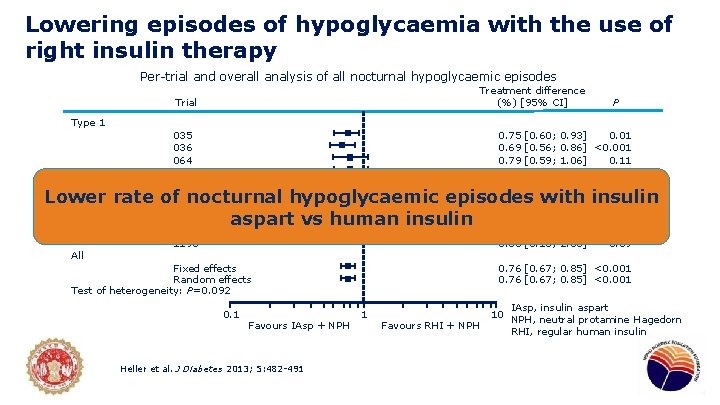
Lowering episodes of hypoglycaemia with the use of right insulin therapy Per-trial and overall analysis of all nocturnal hypoglycaemic episodes Treatment difference (%) [95% CI] Trial P Type 1 035 036 064 065 066 0. 75 0. 69 0. 79 0. 83 [0. 60; [0. 56; [0. 59; [0. 50; 0. 93] 0. 01 0. 86] <0. 001 1. 06] 0. 12 1. 38] 0. 48 037 1198 0. 54 [0. 24; 1. 22] 0. 68 [0. 16; 2. 85] Type 1 and Type 2 Lower rate of 1634 nocturnal hypoglycaemic episodes with insulin 0. 97 [0. 59; 1. 58] 0. 89 Type 2 aspart vs human insulin All Fixed effects Random effects Test of heterogeneity: P=0. 092 0. 1 Favours IAsp + NPH Heller et al. J Diabetes 2013; 5: 482 -491 0. 14 0. 59 0. 76 [0. 67; 0. 85] <0. 001 1 Favours RHI + NPH 10 IAsp, insulin aspart NPH, neutral protamine Hagedorn RHI, regular human insulin

Presentation title Date Special Obstetric Care for Women with GDM Antenatal Care • • Antenatal care of a pregnant woman with GDM should be provided by a gynaecologist, if available. If GDM is diagnosed before 20 weeks of pregnancy, a foetal anatomical survey by USG should be performed at 18 -20 weeks. For all pregnancies with GDM, a foetal growth scan should be performed at 28 -30 weeks gestation & repeated at 34 -36 weeks gestation. There should be at least 3 weeks gap between the two ultrasounds and it should include fetal biometry & amniotic fluid estimation. Pregnant women with GDM in whom blood glucose level is well controlled and there are no complications, should go for routine antenatal care as per Go. I guidelines. In pregnant women with GDM having uncontrolled blood glucose level or any other complication of pregnancy, the frequency of antenatal visits should be increased to every 2 weeks in second trimester and every week in third trimester. Monitor for abnormal foetal growth (macrosomia/growth restriction) and polyhydramnios at each ANC visit PW with GDM to be diligently monitored for hypertension in pregnancy, proteinuria and other obstetric complications In pregnant women with GDM between 24 -34 weeks of gestation and requiring early delivery, antenatal steroids should be given as per Go. I guidelines i. e. Inj. Dexamethasone 6 mg IM 12 hourly for 2 days. More vigilant monitoring of blood glucose levels should be done for next 72 hours following injection. In case of raised blood glucose levels during this period, adjustment of insulin dose should be made accordingly. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 46

Presentation title Date 47 Foetal surveillance in pregnant woman with GDM • Pregnant women with GDM are at an increased risk for foetal death in utero and this risk is increased in PW requiring medical management. Hence vigilant foetal surveillance is required. • Foetal heart should be monitored by auscultation on each antenatal visit. • The pregnant woman should be explained about Daily Fetal Activity Assessment • Woman to lie down on her side after a meal and note how long it takes for the foetus to kick 10 times. • If the foetus does not kick 10 times within 2 hrs, she should immediately consult a healthcare worker and if required should be referred to a higher centre for further evaluation. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus

Presentation title Date Labour and Delivery • • Pregnant women with GDM with good control of blood glucose (2 hr PPPG < 120 mg/dl) levels may be delivered at their respective health facility. Pregnant women with GDM on insulin therapy with uncontrolled blood glucose levels (2 hr PPPG ≥ 120 mg/dl) or insulin requirement >20 U/day should be referred for delivery at CEm. OC centres under care of gynaecologist at least a week before the planned delivery. • Such referred cases must get assured indoor admission or can be kept in a birth waiting home with round the clock availability of medical staff for monitoring. Timing of delivery • • • GDM pregnancies are associated with delay in lung maturity of the foetus; so routine delivery prior to 39 weeks is not recommended. If a woman with GDM with well controlled plasma glucose has not already delivered spontaneously, induction of labour should be scheduled at or after 39 weeks of pregnancy. In woman with GDM with poor plasma glucose control, those with risk factors like hypertensive disorder of pregnancy, previous still birth and other complications should be delivered earlier. The timing of delivery should be individualised by the obstetrician accordingly. Vaginal delivery should be preferred and LSCS should be done for obstetric indications only. In case of foetal macrosomia (estimated foetal weight > 4 Kg) consideration should be given for a primary caesarean section at 39 weeks to avoid shoulder dystocia. Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 48
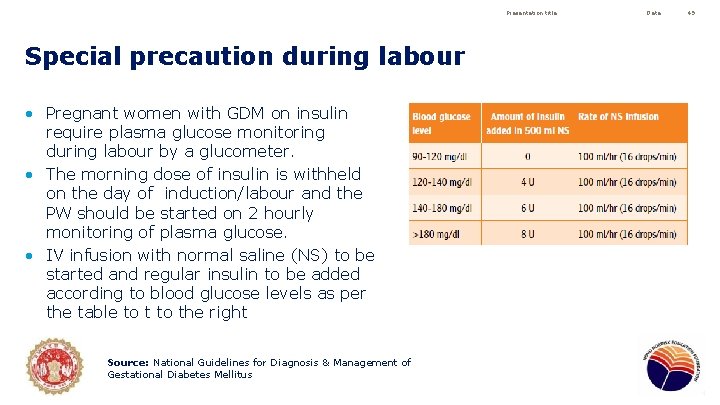
Presentation title Special precaution during labour • Pregnant women with GDM on insulin require plasma glucose monitoring during labour by a glucometer. • The morning dose of insulin is withheld on the day of induction/labour and the PW should be started on 2 hourly monitoring of plasma glucose. • IV infusion with normal saline (NS) to be started and regular insulin to be added according to blood glucose levels as per the table to the right Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus Date 49

Presentation title Date Immediate neonatal care for baby of mother with GDM • • All babies born to mothers with GDM are at risk for development of hypoglycaemia irrespective of treatment whether they are on insulin or not and should be observed closely. All babies are, hence, to be checked for hypoglycaemia at or within one hour of delivery by glucometer. All neonates should receive immediately essential newborn care with emphasis with early breastfeeding to prevent hypoglycaemia. If required, the sick neonates should be immediately resuscitated as per Go. I guidelines. Newborn should be monitored for hypoglycaemia (capillary blood glucose <44 mg/dl). Monitoring should be started at 1 hour of delivery and continued every 4 hours (prior to next feed) till four stable glucose values are obtained. Neonate should be also be evaluated for other neonatal complications like respiratory distress, convulsions, hyperbilirubinaemia. Further details are found in the National Guidelines Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 50

Presentation title Date Post-delivery follow-up of women with GDM • Immediate postpartum care women with GDM is not different from women without GDM but these women are at high risk to develop Type 2 Diabetes mellitus in future. • Maternal glucose levels usually return to normal after delivery. • Nevertheless, a FPG & 2 hr PPPG is performed on the 3 rd day of delivery at the place of delivery. For this reason, GDM cases are not discharged after 48 hours unlike other normal PNC cases. • 6 weeks post partum: 75 g GTT at 6 weeks to evaluate glycaemic status of woman. • Cut offs for normal blood glucose values are: • Fasting plasma glucose: ≥ 126 mg/dl • 75 g OGTT 2 hour plasma glucose • Normal: < 140 mg/dl • IGT: 140 -199 mg/dl • Diabetes: ≥ 200 mg/dl Source: National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus 51

Food for thought!!! DM after pregnancy(post delivery) ? • • upto 50 % 10% 5% 1%

Presentation title Date Patient Education - Key to good outcomes Bringing blood glucose in good control is almost entirely in the hands of the pregnant woman with GDM It is important that: • The pregnant woman understands both the short- and the long-term potential consequences of her condition (for her and her unborn child) • Her family (husband in-laws) understand what GDM is and why a change in the woman’s/family’s dietary habits may be necessary • The pregnant woman understands the importance of attending the clinic for observation and follow-up • The pregnant woman understands that, while GDM is transitional, both her and her child at at increased risk of type 2 diabetes in the future 53

Presentation title Date 54 Additional and detailed information and guidance is available National Guidelines for Diagnosis & Management of Gestational Diabetes Mellitus Includes detailed information on: • Evidence • Technical guidelines on testing & management of GDM • Operational aspects of GDM Programme • Records & Registers • Monitoring and Quality Assurance • Outcome measures to be assessed • Tools and resources related to: • MNT, reporting, Migration form, Referral slip, Glucometer specifications and calibration Available at: www. nrhmorissa. gov. in/writereaddata/Up load/Documents/National%20 Guidelines %20 for%20 Diagnosis%20&%20 Manage ment%20 of%20 Gestational%20 Diabetes %20 Mellitus. pdf

Presentation title Date Together we can ensure better maternal health and pregnancy outcomes…. . . and curb the increasing type 2 diabetes epidemic 55
- Slides: 55