Tutorial 6 Obstetrics Dr Adeela Ashraf Academic FY

Tutorial 6: Obstetrics Dr Adeela Ashraf Academic FY 1 North Central and East London Adeela. ashraf 1@nhs. net 14 March 2021

Labour and Delivery • • • Normal Labour Problems in Labour Pain Management in Labour Foetal Distress Induction of Labour Instrumental Delivery Operative Delivery Pre-term Prelabour Rupture of Membranes Amniotic Fluid Embolism Shoulder Dystocia

Labour and Delivery 1 Which is the largest diameter of the foetal skull? A. B. C. D. Occipito-frontal diameter Suboccipito-bregmatic diameter Submento-bregmatic diameter Verto-mental diameter
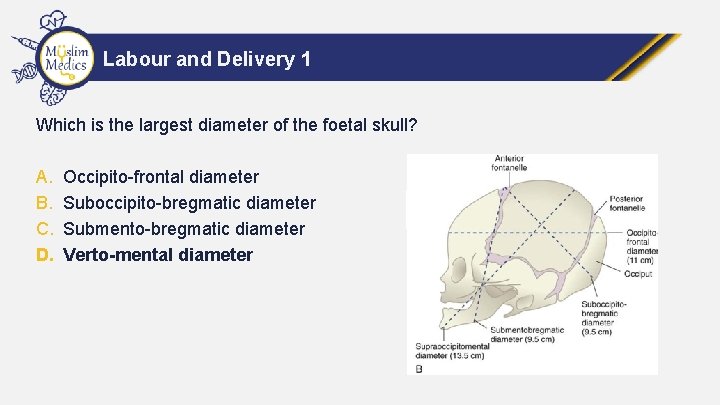
Labour and Delivery 1 Which is the largest diameter of the foetal skull? A. B. C. D. Occipito-frontal diameter Suboccipito-bregmatic diameter Submento-bregmatic diameter Verto-mental diameter

Labour and Delivery 2 A 31 year old nulliparous woman has presented to the maternity triage at 38 weeks with regular painful contractions. Her pregnancy has been uncomplicated until now and she was planning to delivery her baby in the birth center. She reports her ‘waters breaking’ 1 hour ago. On examination, she is 4 cm dilated. How often should vaginal examinations be done from now? A. B. C. D. E. Every 30 minutes Every hour Every 2 hours Every 4 hours Every 6 hours

Labour and Delivery 2 A 31 year old nulliparous woman has presented to the maternity triage at 38 weeks with regular painful contractions. Her pregnancy has been uncomplicated until now and she was planning to delivery her baby in the birth center. She reports her ‘waters breaking’ 1 hour ago. On examination, she is 4 cm dilated. How often should vaginal examinations be done from now? A. B. C. D. E. Every 30 minutes Every hour Every 2 hours Every 4 hours Every 6 hours

Labour and Delivery 3 What position does the head of the baby normally enter the pelvis during labour? A. B. C. D. E. Occipitoanterior (OA) Occipitoposterior (OP Occipitotransverse (OT) Left Occipitoanterior Right Occipitoanterior

Labour and Delivery 3 What position does the head of the baby normally enter the pelvis during labour? A. B. C. D. E. Occipitoanterior (OA) Occipitoposterior (OP Occipitotransverse (OT) Left Occipitoanterior Right Occipitoanterior

Normal Stages of Labour • 3 Stages – Stage I – Time from the diagnosis of labour to 10 cm dilatation • • LATENT PHASE – slow dilatation of cervix for first 4 cm over hours ACTIVE PHASE – more rapid dilatation until 10 cm – Stage II – Full dilatation of the cervix to delivery of the baby • • PASSIVE STAGE – from full dilatation until the head reaches the pelvic floor and there is a desire to push ACTIVE STAGE – Pushing stage until delivery of the baby – Stage III – From delivery of the baby to delivery of the placenta
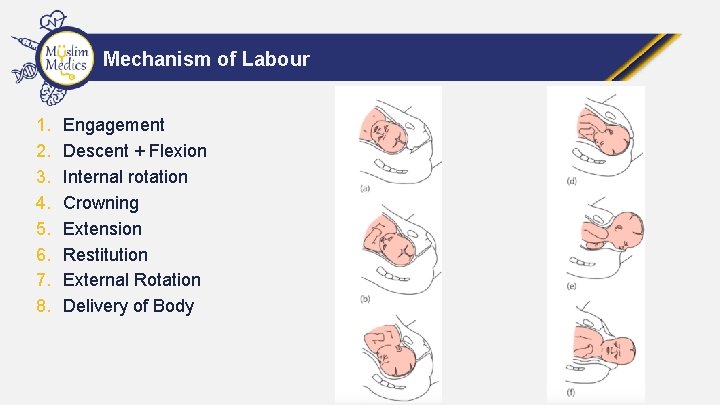
Mechanism of Labour 1. 2. 3. 4. 5. 6. 7. 8. Engagement Descent + Flexion Internal rotation Crowning Extension Restitution External Rotation Delivery of Body

Management of Normal Labour • • General observations – temperature, BP, pulse, contraction frequency Mobility – women should be encouraged to move and find a comfortable position Hydration – isotonic drinks or water Food – eating small amounts is appropriate but discourage if high risk Pyrexia - >37. 5, more common with epidural or prolonged labour Urinary tract – encourage frequent micturition, avoid retention Mental State – minimize fear and anxiety
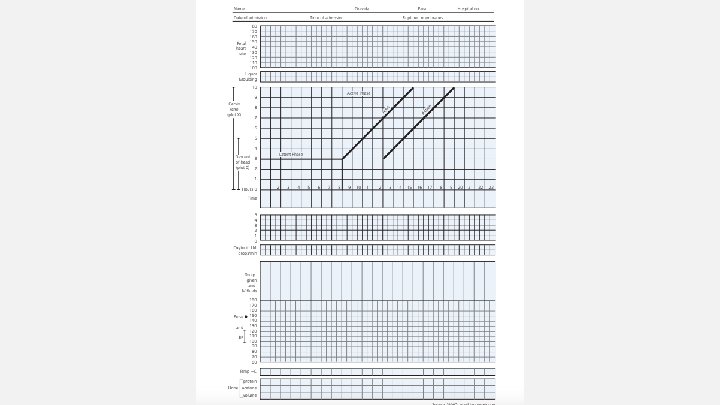
Monitoring in labour

Labour and Delivery 4 A 31 year old nulliparous woman has presented to the maternity triage at 38 weeks with regular painful contractions. Her pregnancy has been uncomplicated until now and she was planning to delivery her baby in the birth center. She reports her ‘waters breaking’ 1 hour before arriving at the hospital. She is now 6 cm dilated but on her partogram, she was recorded at being 5 cm 4 hours ago. What is the next best step? A. B. C. D. E. Start oxytocin infusion 10 IU/500 ml Perform artificial rupture of membraes Take her to theatre for C-section No change in management Prepare for instrumental delivery

Labour and Delivery 4 A 31 year old nulliparous woman has presented to the maternity triage at 38 weeks with regular painful contractions. Her pregnancy has been uncomplicated until now and she was planning to delivery her baby in the birth center. She reports her ‘waters breaking’ 1 hour before arriving at the hospital. She is now 6 cm dilated but on her partogram, she was recorded at being 5 cm 4 hours ago. What is the next best step? A. B. C. D. E. Start oxytocin infusion 10 IU/500 ml Perform artificial rupture of membraes Take her to theatre for C-section No change in management Prepare for instrumental delivery

Problems in Labour Problems with the power • Ineffective uterine contraction – treat with augmentation either with an oxytocin infusion or ARM • Hyperactive uterine action – treat with tocolytic like salbutamol; may need CS due to foetal distress • Nulliparous mother – Passive second stage – if poor descent, an oxytocin infusion can be initiated – Active second stage – if >1 -2 hrs, SVD is less likely and traction can be applied with instruments • Multiparous mother – Problems with contractions is unlikely – More likely due to malpresentation – Higher risk of rupture – use oxytocin with caution after excluding malpresentation

Problems in Labour Problems with the passenger • Malposition – OP – occurs in 5% • • • If progression of labour is normal – no further action needed If labour is slow, augmentation can be used If prolonged second stage – instrumental delivery is achievable with manual or instrumental rotation using ventouse or Keillands forceps – OT • • Normal findings in first stage Incomplete normal rotation – must resolve to OA or OP or vaginal delivery is not possible Problem if no delivery after 1 hr of pushing Rotation with traction needed for delivery – usually with ventouse

Problems in Labour Problems with the passenger • Malpresentation – Brow presentation – 1 in 1000 • • • Extension of foetal head Presenting part has large diameter - 13 cm CS required – Face presentation – 1 in 400 • • Maximal extension of head Presenting diameter is 11 cm Vaginal delivery possible if OA Otherwise CS

Problems in Labour Problems with the passage • Cephalo-pelvic disproportion – Pelvis is simply too small – Very difficult to diagnose prior to labour – More common in large babies, very short women or if the head is high at term in a nulliparous woman – Needs CS • Pelvic variants and deformities

Labour and Delivery 5 Which of the following is NOT an indication for continuous CTG? A. B. C. D. E. Significant meconium Maternal temperature > 38 Oxytocin use OP presentation While administering epidural anaesthesia

Labour and Delivery 5 Which of the following is NOT an indication for continuous CTG? A. B. C. D. E. Significant meconium Maternal temperature > 38 Oxytocin use OP presentation While administering epidural anaesthesia

Labour and Delivery 6 A 36 year old woman is 41 weeks pregnant and in labour. She is contracting every 10 mins and her cervix is at 7 cm. She is draining significant meconium stained liquor and the midwife has started a CTG. The baseline rate is 155 bpm, with variability of 2 bpm for the past 60 mins. There are no accelerations of decelerations. What is the correct assessment of this CTG and appropriate management? A. B. C. D. Pathological CTG – expedite delivery Suspicious CTG – perform foetal blood sampling and deliver if abnormal Suspicious CTG – give IV fluids and reassess in 20 mins Suspicious CTG – reassess in 20 mins and perform foetal blood sampling if still suspicious E. Normal CTG

Labour and Delivery 6 A 36 year old woman is 41 weeks pregnant and in labour. She is contracting every 10 mins and her cervix is at 7 cm. She is draining significant meconium stained liquor and the midwife has started a CTG. The baseline rate is 155 bpm, with variability of 2 bpm for the past 60 mins. There are no accelerations or decelerations. What is the correct assessment of this CTG and appropriate management? A. B. C. D. Pathological CTG – expedite delivery Suspicious CTG – perform foetal blood sampling and deliver if abnormal Suspicious CTG – give IV fluids and reassess in 20 mins Suspicious CTG – reassess in 20 mins and perform foetal blood sampling if still suspicious E. Normal CTG

Foetal Distress • • Colour of the liquor – meconium? Foetal heart rate CTG Foetal Blood Sampling

CTG • • Baseline Rate: between 110 and 160 Baseline Variability: short term variation in FHR should be >5 bpm Accelerations: Good sign when with movement or contractions Decelerations: – Early: synchronous with contractions – Variable: vary in timing – Late: persisting after the contraction
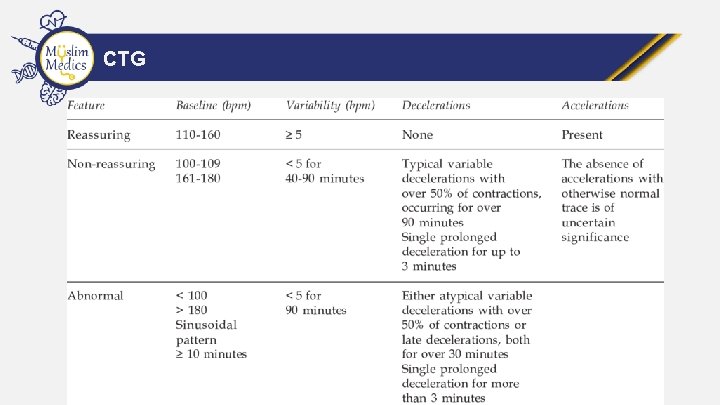
CTG

Labour and Delivery 7 Which of the following is a contraindication to epidural anaesthesia? A. B. C. D. E. Coagulopathy Previous spinal surgery Hypertension Aortic stenosis Twin birth

Labour and Delivery 7 Which of the following is a contraindication to epidural anaesthesia? A. B. C. D. E. Coagulopathy Previous spinal surgery Hypertension Aortic stenosis Twin birth
Pain Management in Labour • • Non-medical – Antenatal classes – Back rubbing – Water immersion Inhalational – Entonox – NO + O 2 Medical – Pethidine – Sometimes diamorphine Anaesthesia – Spinal – Pudendal Nerve Block – Epidural

Induction of labour • • Typically offered between 41 and 42 weeks Perform Bishops score before starting induction Methods: – prostaglandins – Amniotomy +/- oxytocin – Cervical sweep CTG monitoring

Instrumental Delivery • • • Ventouse – cup fixed to occiput by suction Forceps – ‘blades’ fit around foetal head and handles lock together Indications – Prolonged second stage – Foetal distress – Prophylactic use Type of delivery is determined by position and descent of head Failure caesarean section
Operative Delivery • • Most commonly lower segment caesarean section 4 categories Indications for Emergency CS – Foetal distress – Failure to progess in labour Indications for elective CS – Placenta praevia – Uncorrectable abnormal lie – Previous vertical CS – Twin pregnancy – Medical disease of pregnancy - GDM

Labour and Delivery 8 A 34 year old lady at 29+6 weeks have come to A&E claiming that her waters have broken. She had hyperemesis gravidarum in her first trimester but her pregnancy has been otherwise uneventful. What is the next best step? A. B. C. D. E. Give tocolytics Give corticosteroids Give erythromycin for 10 days Perform an IGFBP-1 test Perform a speculum examination

Labour and Delivery 8 A 34 year old lady at 29+6 weeks have come to A&E claiming that her waters have broken. She had hyperemesis gravidarum in her first trimester but her pregnancy has been otherwise uneventful. What is the next best step? A. B. C. D. E. Give tocolytics Give corticosteroids Give erythromycin for 10 days Perform an IGFBP-1 test Perform a speculum examination

Preterm Pre-labour Rupture of Membranes • Diagnosis – visualize liquor on sterile speculum examination or test vaginal fluid for IFGBP or PAMG-1 • Once confirmed: – Consider expectant management – Erythromycin for 10 days or until labour – Corticosteroids up to 36 weeks for foetal lung development – IV magnesium sulphate if delivery imminent for foetal neurodevelopment – Look for signs of chorioamnionitis

Amniotic Fluid Embolism • • When liquour enters maternal circulation Causes: – Collapse during labour/delivery – Acute hypotension – Respiratory distress – Acute hypoxia – Heart failure and cardiac arrest – DIC massive PPH Clinical diagnosis Management: resuscitation and supportive

Labour and Delivery 9 A 29 year old lady in labour has just delivered the head of her baby. You notice that the head retracts and is closely applied to the vulva and in the next contraction, the shoulders fail to deliver. What is the next most appropriate step? A. B. C. D. E. Call for help and ask the mother to flex and abduct her legs at the hips Call for help and ask the mother to continue pushing with her contractions Call for help and ask the mother apply fundal pressure Call for help and apply suprapubic pressure Take the mother to theatre

Labour and Delivery 9 A 29 year old lady in labour has just delivered the head of her baby. You notice that the head retracts and is closely applied to the vulva and in the next contraction, the shoulders fail to deliver. What is the next most appropriate step? A. B. C. D. E. Call for help and ask the mother to flex and abduct her legs at the hips Call for help and ask the mother to continue pushing with her contractions Call for help and ask the mother apply fundal pressure Call for help and apply suprapubic pressure Take the mother to theatre
Shoulder Dystocia • • • Obstetric emergency Baby must be delivered within 5 mins Immediately call for help


Antepartum Haemorrhage • • • Disorders of placentation Managing APH Placenta praevia Placental abruption Vasa praevia Post-partum haemorrhage

Antepartum Haemorrhage 1 A 34 year old woman has an MRI after due to an abnormality of placentation is detected on routine USS. The report states: ‘the placenta is in the lower anterior uterine wall with evidence of invasion to the posterior wall of the bladder. What is the diagnosis? A. B. C. D. E. Placenta praevia Placenta percreta Placenta increta Placenta accreta Uterine fibroid

Antepartum Haemorrhage 1 A 34 year old woman has an MRI after due to an abnormality of placentation is detected on routine USS. The report states: ‘the placenta is in the lower anterior uterine wall with evidence of invasion to the posterior wall of the bladder. What is the diagnosis? A. B. C. D. E. Placenta praevia Placenta percreta Placenta increta Placenta accreta Uterine fibroid

Antepartum Haemorrhage 2 A 25 year old lady has come for a scan at 20+2 weeks. The placenta is anterior and appears to be 17 mm from the internal os. This is her first pregnancy. What is the next step in managing her low-lying placenta? A. B. C. D. E. Repeat USS at 32 weeks Repeat USS at 36 weeks Arrange MRI scan Plan to delivery by elective CS No further management needed

Antepartum Haemorrhage 2 A 25 year old lady has come for a scan at 20+2 weeks. The placenta is anterior and appears to be 17 mm from the internal os. This is her first pregnancy. What is the next step in managing her low-lying placenta? A. B. C. D. E. Repeat USS at 32 weeks Repeat USS at 36 weeks Arrange MRI scan Plan to delivery by elective CS No further management needed
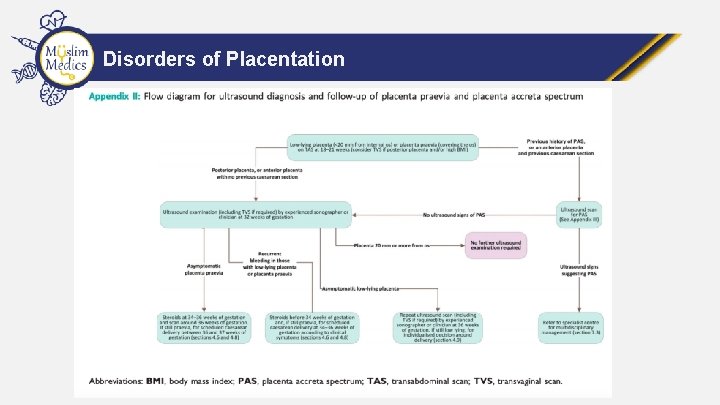
Disorders of Placentation

Antepartum Haemorrhage 3 A 30 year old nulliparous woman presents to hospital at 29 weeks following an unprovoked painless bleed of about a teaspoon. Her 20 week scan showed a lowlying placenta. Her baby is moving well and CTG is normal. What is the most appropriate management? A. Allow to go home as it was a small bleed that has now resolved B. Admit and give steroids C. Admit, give fluids, take G&S and ensure she is bleed-free for 48 hours before discharge D. Admit, perform USS scan, take G&S and give steroids if she bleeds more E. Give fluids, take bloods and review in clinic in one week

Antepartum Haemorrhage 3 A 30 year old nulliparous woman presents to hospital at 29 weeks following an unprovoked painless bleed of about a teaspoon. Her 20 week scan showed a lowlying placenta. Her baby is moving well and CTG is normal. What is the most appropriate management? A. Allow to go home as it was a small bleed that has now resolved B. Admit and give steroids C. Admit, give fluids, take G&S and ensure she is bleed-free for 48 hours before discharge D. Admit, perform USS scan, take G&S and give steroids if she bleeds more E. Give fluids, take bloods and review in clinic in one week

Antepartum Haemorrhage 4 A 25 year old lady at 32+4 weeks has presented to MAU with PV bleeding and abdominal pain. On examination, her abdomen feels hard and it is difficult to palpate the foetus. She is tachycardic, tachypnoeic and normotensive. She then loses consciousness. What is the next most appropriate step? A. B. C. D. E. Take her to theatre for EMCS Perform a CTG Give oxygen Obtain IV access Take bloods for G&S and crossmatch

Antepartum Haemorrhage 4 A 25 year old lady at 32+4 weeks has presented to MAU with PV bleeding and abdominal pain. On examination, her abdomen feels hard and it is difficult to palpate the foetus. She is tachycardic, tachypnoeic and normotensive. She then loses consciousness. What is the next most appropriate step? A. B. C. D. E. Take her to theatre for EMCS Perform a CTG Give oxygen Obtain IV access Take bloods for G&S and crossmatch

Antepartum Haemorrhage • • • PV bleeding that occurs after 24 weeks gestation Multiple causes – Placenta praevia – Placental abruption – Undetermined origin – Rare: uterine rupture, vasa praevia, genital tract pathology Things to consider: – How much? – Constant or intermittent? – Painful or painless? – Examination findings – maternal observations, CTG findings, abdominal examination
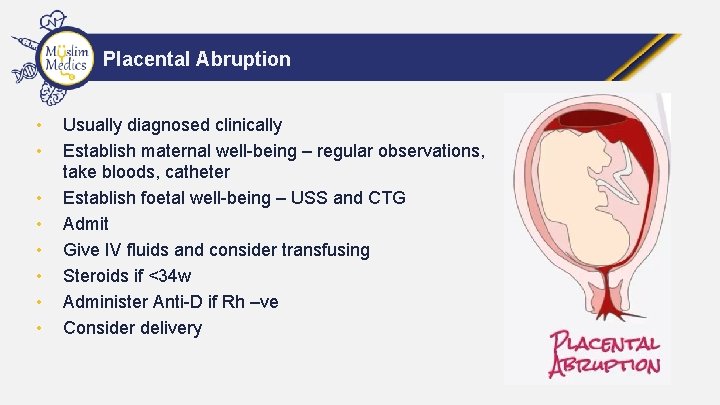
Placental Abruption • • Usually diagnosed clinically Establish maternal well-being – regular observations, take bloods, catheter Establish foetal well-being – USS and CTG Admit Give IV fluids and consider transfusing Steroids if <34 w Administer Anti-D if Rh –ve Consider delivery
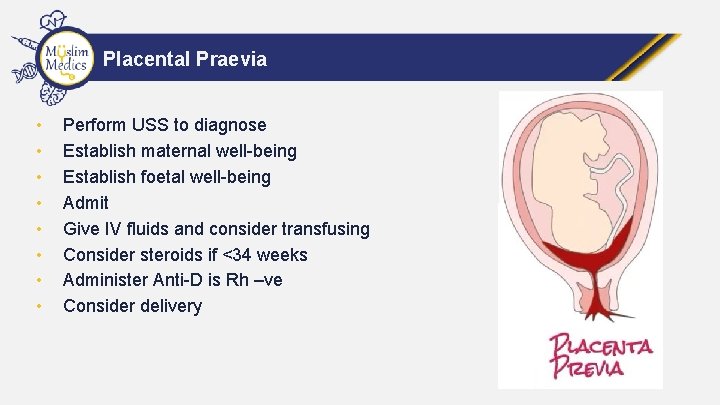
Placental Praevia • • Perform USS to diagnose Establish maternal well-being Establish foetal well-being Admit Give IV fluids and consider transfusing Consider steroids if <34 weeks Administer Anti-D is Rh –ve Consider delivery

Antepartum Haemorrhage 5 A 30 year old lady presents in spontaneous labour at 41 weeks. At 3 cm, she has spontaneous rupture of membranes with heavily blood-stained liquor. She is not in any pain. The mother feels a reduction in foetal movements and CTG shows significant abnormalities. What is the diagnosis? A. B. C. D. E. Placental Abruption Placenta praevia Vasa praevia Blood show Uterine rupture

Antepartum Haemorrhage 5 A 30 year old lady presents in spontaneous labour at 41 weeks. Her previous ultrasound scans have all been normal. At 3 cm, she has spontaneous rupture of membranes with heavily blood-stained liquor. She is not in any pain. The mother feels a reduction in foetal movements and CTG shows significant abnormalities. What is the diagnosis? A. B. C. D. E. Placental Abruption Placenta praevia Vasa praevia Blood show Uterine rupture

Vasa Praevia • • Very rare cause of APH Can be detected on USS but most are not Vessels rupture with membranes Usually painless and moderate amount of blood Accompanied by severe foetal distress Delivery must be expedited immediately with EMCS – do not wait for confirmation of diagnosis Neonatal team should be informed and present – baby will need resuscitation and blood transfusions

SBA A 36 year old lady has just given birth to a health female infant by elective Caesarean section for placenta praevia. Estimated blood loss was about 1100 ml. Later in the recovery area, she has a brisk vaginal bleed of about 1 litre. Her heart rate is 130 bpm and her BP is 95/55. What is the immediate management after calling for help? A. B. C. D. Rapid fluid resuscitation, oxytocin infusion and uterine massage Rapid fluid resuscitation, IM carboprost and vaginal assessment Rapid fluid resuscitation, rectal misoprostol, uterine massage Rapid fluid resuscitation, contact interventional radiology for uterine artery embolization E. Rapid fluid resuscitation and transport to theatre

SBA A 36 year old lady has just given birth to a health female infant by elective Caesarean section for placenta praevia. Estimated blood loss was about 1100 ml. Later in the recovery area, she has a brisk vaginal bleed of about 1 litre. Her heart rate is 130 bpm and her BP is 95/55. What is the immediate management after calling for help? A. B. C. D. Rapid fluid resuscitation, oxytocin infusion and uterine massage Rapid fluid resuscitation, IM carboprost and vaginal assessment Rapid fluid resuscitation, rectal misoprostol, uterine massage Rapid fluid resuscitation, contact interventional radiology for uterine artery embolization E. Rapid fluid resuscitation and transport to theatre

Post-Partum Haemorrhage • • Primary PPH is within 24 hrs of delivery Causes: – – • • Tone – atonic uterus Tissue – retained placenta Trauma – perineal/vaginal trauma Thrombin – coagulopathy Prevention: oxytocin/ergometrine or oxytocin alone in 3 rd stage of labour Managing minor PPH without shock – IV access and crystalloid infusion – Bloods – G&S, FBC, coag screen – 15 minute observations – Uterine massage
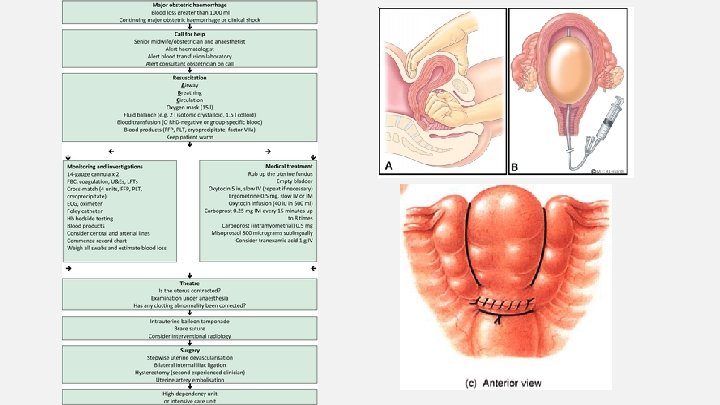
Post-Partum Haemorrhage

Abnormal Lie • Breech Presentation • Umbilical Cord Prolapse
Abnormal Lie 1 A 34 year old multiparous woman presents for a scan at 37 weeks. Previous scans show a singleton breech baby; today the baby is still breech. This lady also has gestational diabetes which is managed with metformin. Her first pregnancy also had GDM and ended in a C-section due to failure to progress in labour. What is the next best step? A. B. C. D. E. Planned C-section at 39 weeks Vaginal breech birth Wait for the baby to spontaneously turn to cephalic External cephalic version as soon as possible Admit to labour ward for monitoring
Abnormal Lie 1 A 34 year old multiparous woman presents for a scan at 37 weeks. Previous scans show a singleton breech baby; today the baby is still breech. This lady also has gestational diabetes which is managed with metformin. Her first pregnancy also had GDM and ended in a C-section due to failure to progress in labour. What is the next best step? A. B. C. D. E. Planned C-section at 39 weeks Vaginal breech birth Wait for the baby to spontaneously turn to cephalic External cephalic version as soon as possible Admit to labour ward for monitoring
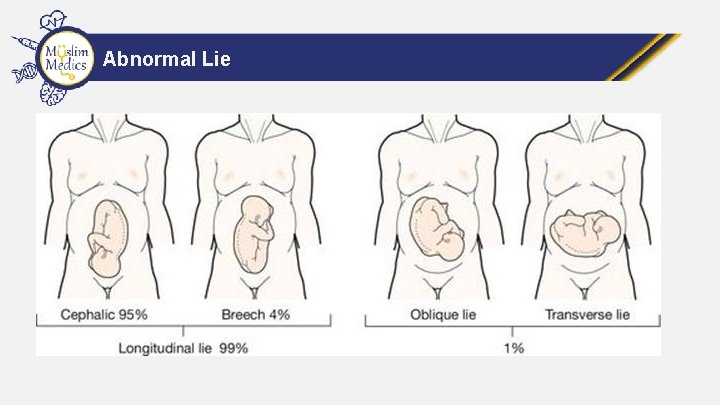
Abnormal Lie

Abnormal Lie 2 Which of the following is NOT a contraindication to ECV? A. B. C. D. E. Placenta Praevia Twin pregnancy Labour with ROM Labour without ROM Antepartum haemorrhage in the past 7 days

Abnormal Lie 2 Which of the following is NOT a contraindication to ECV? A. B. C. D. E. Placenta Praevia Twin pregnancy Labour with ROM Labour without ROM Antepartum haemorrhage in the past 7 days
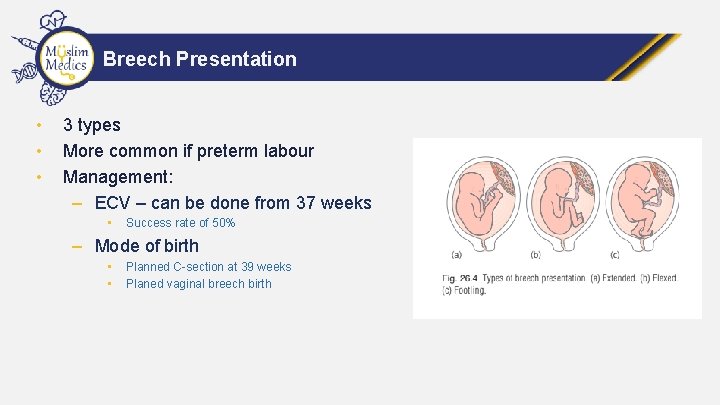
Breech Presentation • • • 3 types More common if preterm labour Management: – ECV – can be done from 37 weeks • Success rate of 50% – Mode of birth • • Planned C-section at 39 weeks Planed vaginal breech birth

Abnormal Lie 3 A 34 year old multiparous woman is admitted to labour ward with regular painful contractions. While examining her, her membranes rupture and you see the cord hanging from the vagina. She is fully dilated, the foetal position is OA and the presenting part is below the ischial spines. What should you do next? A. B. C. D. E. Gain IV access, call for help and gently place the cord back into the vagina Transfer to theatre for category 1 caesarean section Call for help and prepare for instrumental delivery Call for help, perform episiotomy and commence pushing Elevate presenting part with vaginal pack

Abnormal Lie 3 A 34 year old multiparous woman is admitted to labour ward with regular painful contractions. While examining her, her membranes rupture and you see the cord hanging from the vagina. She is fully dilated, the foetal position is OA and the presenting part is below the ischial spines. What should you do next? A. B. C. D. E. Gain IV access, call for help and gently place the cord back into the vagina Transfer to theatre for category 1 caesarean section Call for help and prepare for instrumental delivery Call for help, perform episiotomy and commence pushing Elevate presenting part with vaginal pack

Umbilical Cord Prolapse • • After ROM, cord descends below presenting part Management – Elevate presenting part – manually or by distending the bladder – Minimal handling of cord – Expedite delivery

Infections in pregnancy • • Chicken pox Herpes simplex Other teratogenic infection Group B Streptococcus UTI’s in pregnancy HIV Listeria Hepatitis B

Infections in Pregnancy 1 A 32 year old woman is 30 weeks pregnant. She visited her sister and nephew yesterday. Today, she has called the GP very worried because her nephew has developed a fever and vesicular rash this morning that looks like chicken pox. She has not had chicken pox in the past and is currently asymptomatic. What is the next best step? A. Inform her that the risk of foetal varicella syndrome is low and no further action is needed B. Advise her to go to A&E to be admitted for IV aciclovir C. Ask her to come into the GP practice for a varicella vaccine D. Ask her to come into the GP practice for a blood test E. Ask her to come into the GP practice for a VZIG injection

Infections in Pregnancy 1 A 32 year old woman is 30 weeks pregnant. She visited her sister and nephew yesterday. Today, she has called the GP very worried because her nephew has developed a fever and vesicular rash this morning that looks like chicken pox. She has not had chicken pox in the past and is currently asymptomatic. What is the next best step? A. Inform her that the risk of foetal varicella syndrome is low and no further action is needed B. Advise her to go to A&E to be admitted for IV aciclovir C. Ask her to come into the GP practice for a varicella vaccine D. Ask her to come into the GP practice for a blood test E. Ask her to come into the GP practice for a VZIG injection

Chicken Pox in Pregnancy • • Maternal risks include pneumonia, hepatitis or encephalitis Risk of neonatal chickenpox is highest if mother develops the rash in the 7 days prior to or 2 days after delivery Foetal varicella syndrome is a very rare but serious complication of VZV infection in pregnancy – it is due to infection with VZV in early pregnancy May cause – Skin scarring – Microcephaly – Limb hypoplasia – Learning difficulties – Eye defects


Listeria Monocytogenes • • • Infection can follow eating pate, soft cheeses, unpasteurized milk and dairy and pre-packed meals Causes non-specific illness: – Fever and chills – Myalgia – Nausea and vomiting Can cause fatal infection of the foetus Confirmed with blood cultures Treated with penicillins +/- gentamicin Prevention is key

Infections in Pregnancy 2 A 30 year old woman presents for her booking appointment and mentions that she has noticed a new painful, itchy vesicular rash on her vulva. Some of the vesicles have burst and are now red open sores. This is the first time she has experienced this rash. What the next best step in management? A. B. C. D. E. Explain that she will need to have a Caesarean delivery at 37 weeks Explain that this will resolve on it’s own and no further action is needed Prescribe oral aciclovir for 5 days Refer to GUM clinic for IM benzathine benzylpenicillin Advise her to have antibody testing for HSV performed

Infections in Pregnancy 2 A 30 year old woman presents for her booking appointment and mentions that she has noticed a new painful, itchy vesicular rash on her vulva. Some of the vesicles have burst and are now red open sores. This is the first time she has experienced this rash. What the next best step in management? A. B. C. D. E. Explain that she will need to have a Caesarean delivery at 37 weeks Explain that this will resolve on it’s own and no further action is needed Prescribe oral aciclovir for 5 days Refer to GUM clinic for IM benzathine benzylpenicillin Advise her to have antibody testing for HSV performed

Herpes Simplex in Pregnancy • • • Neonatal infection has a high mortality Most commonly transmitted at vaginal delivery following recent primary infection with vesicles present Management: – Refer to GUM clinic – CS recommended if delivering within 6 weeks of primary attack/ those with genital lesions at time of delivery from primary attack – Vaginal delivery recommended for those with recurrent HSV – If in 1 st or second trimester – give oral aciclovir – Inform neonatal team at time of delivery

Infections in Pregnancy 3 A 30 year old, multiparous lady presents to her GP at 16 weeks pregnant with her 6 year old child who has developed a bright red rash on his cheeks associated with a low grade fever and runny nose. The rash has since spread across his arms and upper torso. You advise her to manage her son’s infection supportively, however you are concerned about transmission to the mother. What test should she be offered? A. B. C. D. E. Blood test for serology Nasal swab Throat swab USS of her abdomen No test is required

Infections in Pregnancy 3 A 30 year old, multiparous lady presents to her GP at 16 weeks pregnant with her 6 year old child who has developed a bright red rash on his cheeks associated with a low grade fever and runny nose. The rash has since spread across his arms and upper torso. You advise her to manage her son’s infection supportively, however you are concerned about transmission to the mother. What test should she be offered? A. B. C. D. E. Blood test for serology Nasal swab Throat swab USS of her abdomen No test is required

Parvovirus B 19 in Pregnancy • • • 50% of women are immune May present with erythema infectiosum (‘slapped cheek’) – most have arthralgia or are asymptomatic In the foetus – virus suppresses erythropoiesis severe anaemia +/thrombocytopenia; can cause foetal death Spontaneous resolution occurs in about 50% Maternal infection confirmed by testing for Ig. M Management: – Infected mothers are scanned regularly to look for signs of foetal infection – May need to give in utero transfusion if foetal hydrops detected – Severe disease associated with neurological damage – Excellent prognosis in infants who survive

Infections in Pregnancy 4 Which of the following is NOT a teratogenic infection? A. B. C. D. E. Cytomegalovirus Rubella Syphillis Toxoplasmosis HIV

Infections in Pregnancy 4 Which of the following is NOT a teratogenic infection? A. B. C. D. E. Cytomegalovirus Rubella Syphilis Toxoplasmosis HIV

Infections in Pregnancy 5 A 27 year old lady who is 13 weeks pregnant presents requesting a test for toxoplasmosis after accidentally coming into contact with cat faeces while visiting family (who have a cat). Her Ig. M test is suggestive for toxoplasmosis infection. What is the next best management step? A. B. C. D. E. Offer a termination Start spiramycin, sulfadiazine and pyrimethamine Perform amniocentesis after 20 weeks Inform her that the risk of congenital infection is low and take no further action

Infections in Pregnancy 5 A 27 year old lady who is 13 weeks pregnant presents requesting a test for toxoplasmosis after accidentally coming into contact with cat faeces while visiting family (who have a cat). Her Ig. M test is suggestive for toxoplasmosis infection. What is the next best management step? A. B. C. D. E. Offer a termination Start spiramycin, sulfadiazine and pyrimethamine Perform amniocentesis Inform her that the risk of congenital infection is low and take no further action

Teratogenic Infections • • Rubella – Very rare in the UK – Infection in early pregnancy congenital rubella syndrome – Risk and severity of CRS is very low after 16 w – TOP offered in infection occurs before 16 w – Vaccinate after pregnancy (live vaccine) Cytomegalovirus – Common cause of childhood disability and deafness – Transmission may be transplacental, during labour and delivery or through breast milk – Test with Ig. G avidity test to confirm maternal CMV – Amniocentesis to diagnose vertical transmission

Teratogenic Infections • • Syphillis – Very rare in UK – Can cause miscarriage, congenital disease and still birth – Treat with IM benzylpenicillin Toxoplasmosis – Transmitted following contact with cat faeces, soil, or eating infected meat – The earlier the infection, the worse the sequalae – Maternal disease is confirmed with Ig. M testing – spiramycin started if positive – Vertical transmission confirmed with amniocentesis after 20 weeks – Add sulphadiazine and pyrimethamine if congenital infection if confirmed – TOP may be requested

Infections in Pregnancy 6 A 24 year old woman who is HIV positive at 39 weeks pregnant has just arrived in the UK. She has had no previous antenatal care but she has not had any issues. Her CD 4 count is 180 mm/mm 3 and her viral load is 5500 copies/ml. What would you advise her regarding delivery? A. B. C. D. E. Spontaneous vaginal delivery Induction of labour as soon as possible and give HAART to baby when born Caesarean section Start HAART and await labour Start HAART and induce labour at 41 weeks

Infections in Pregnancy 6 A 24 year old woman who is HIV positive at 39 weeks pregnant has just arrived in the UK. She has had no previous antenatal care but she has not had any issues. Her CD 4 count is 180 mm/mm 3 and her viral load is 5500 copies/ml. What would you advise her regarding delivery? A. B. C. D. E. Spontaneous vaginal delivery Induction of labour as soon as possible and give HAART to baby when born Caesarean section Start HAART and await labour Start HAART and induce labour at 41 weeks

HIV In Pregnancy • • Universal screening for HIV in the UK If HIV positive: – Manage with an HIV physician – Regular tests for CD 4 count and viral load – Screen for other infections – Start/continue HAART and continue throughout pregnancy and delivery – Invasive prenatal diagnostic tests should be avoided until viral load is <50 – Discuss mode of delivery – based on viral load – Consider whether intrapartum IV zidovudine is needed – Inform neonatal team – what PEP is needed? – Recommend formula feeding

Infections in Pregnancy 7 Which of the following is NOT an indication for intrapartum antibiotic prophylaxis for neonatal GBS disease? A. B. C. D. E. Asymptomatic GBS bacteriuria in current pregnancy Prolonged rupture of membranes >18 hours Positive vaginal swab for GBS, due to have an elective CS Preterm labour Maternal intrapartum fever of 38

Infections in Pregnancy 7 Which of the following is NOT an indication for intrapartum antibiotic prophylaxis for neonatal GBS disease? A. B. C. D. E. Asymptomatic GBS bacteriuria in current pregnancy Prolonged rupture of membranes >18 hours Positive vaginal swab for GBS, due to have an elective CS Preterm labour Maternal intrapartum fever of 38

GBS In Pregnancy • • • Universal screening not recommended Foetal infection occurs during labour after ROM Can cause sepsis in neonate Treatment given if risk factors for GBS present or known/incidental finding of GBS Treatment is intrapartum antibiotic prophylaxis with IV penicillins If GBS identified in a previous pregnancy offer IAP or GBS testing at 35 -37 w
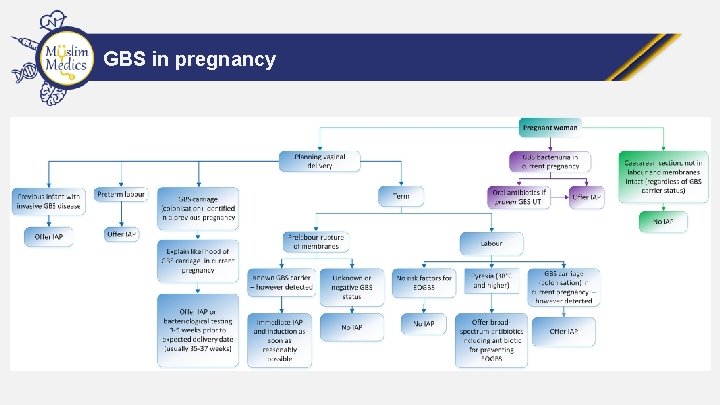
GBS in pregnancy

UTI In Pregnancy • UTI’s should be managed with: – Simple analgesia – Avoid dehydration – Antibiotics • • 1 st choice: nitrofurantoin 100 mg BD for 7 days Alternatives: amoxicillin 500 mg TDS for 7 days OR cefalexin 500 mg BD for 7 days – Urine sample to be sent for MCS – change antibiotics according to sensitivities – Urine MCS after treatment completion Asymptomatic bacteriuria should be managed with the same antibiotics – Inform antenatal team if positive for GBS

Infections in Pregnancy 8 Which of these vaccinations is safe in pregnancy? A. B. C. D. Hepatitis B Chickenpox MMR BCG Rabies

Infections in Pregnancy 8 Which of these vaccinations is safe in pregnancy? A. B. C. D. E. Hepatitis B Chickenpox MMR BCG Rabies

Infections in Pregnancy 9 The routine Hepatitis B test results for a 24 year old pregnant lady is shown below. She is fit and well and this is her first pregnancy. What is the next best step in her management? HBs. Ag negative Anti-HBc positive Anti-HBs positive A. B. C. D. E. Offer Hepatitis B vaccination Start tenofovir immediately Give hepatitis B immunoglobulin Offer TOP No further action needed

Infections in Pregnancy 9 The routine Hepatitis B test results for a 24 year old pregnant lady is shown below. She is fit and well and this is her first pregnancy. What is the next best step in her management? HBs. Ag negative Anti-HBc positive Anti-HBs positive A. B. C. D. E. Offer Hepatitis B vaccination Start tenofovir immediately Give hepatitis B immunoglobulin Offer TOP No further action needed
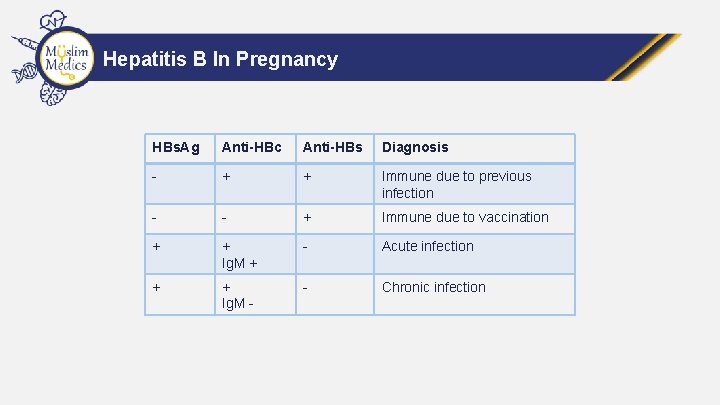
Hepatitis B In Pregnancy HBs. Ag Anti-HBc Anti-HBs Diagnosis - + + Immune due to previous infection - - + Immune due to vaccination + + Ig. M + - Acute infection + + Ig. M - - Chronic infection

Hepatitis B In Pregnancy • • • Pregnant women are routinely screened Can be vertically transmitted at delivery 90% of infected neonates become chronic carriers If mother is positive: – Manage under hepatology – Neonatal immunization – first one in first 24 hours of life – Hepatitis Ig may need to be given Very unlikely to pass Hep. B through breastfeeding
Feedback • Please leave feedback by filling out this very short survey! – http: //tiny. cc/tutorialfeedback • Year 5 – Spring Term – Specialties Management Series – Dr Adeela Ashraf
- Slides: 102