1 OBSTETRICAL HEMORRHAGE Obstetrics is bloody business hemorrhage

1

OBSTETRICAL HEMORRHAGE � Obstetrics is "bloody business. " � hemorrhage still remains a leading cause of maternal mortality. � 12 % of maternal deaths were caused by obstetrical hemorrhage. � hemorrhage is the single most important cause of maternal death worldwide. � Obstetrical hemorrhage accounts for almost half of all postpartum deaths in developing countries 2

qmost maternal deaths from hemorrhage is associated with substandard care. qmany hemorrhage-related maternal deaths were preventable and were associated with inadequate facilities 4






ANTEPARTUM HEMORRHAGE q. Placental Abruption q. Placenta Previa 11

Causes of Obstetrical Hemorrhage Placental Abruption: q. Placental separation from its implantation site before delivery qvariously called placental abruption, abruptio placentae, accidental hemorrhage , abruptioplacentae 12

COMPLICATIONS �Shock � Consumptive Coagulopathy � Renal Failure � Sheehan Syndrome 13

Shock qshock sometimes seen with placental abruption was disproportionate to the amount of hemorrhage. q because placental thromboplastin enters the maternal circulation and incites intravascular coagulation qhypovolemic shock is directly due to maternal blood loss. 14

Consumptive Coagulopathy q. Placental abruption is one of the most common causes of clinically significant consumptive coagulopathy in obstetrics. q. In approximately a third of women with an abruption severe enough to kill the fetus q there are measurable changes in coagulation factors. 15

Renal Failure qit is more common if treatment of hypovolemia is delayed or incomplete. q most cases of acute kidney injury are reversible, however, acute cortical necrosis, when it occurs, is usually caused by placental abruption. q. Seriously impaired renal perfusion is the consequence of massive hemorrhage. q Because preeclampsia frequently coexists with placental abruption, renal vasospasm and hypoperfusion are likely intensified. 16

Sheehan Syndrome q. Severe intrapartum or early postpartum hemorrhage rarely is followed by pituitary failure or Sheehan syndrome. qcharacterized by : qfailure of lactation, q amenorrhea, qbreast atrophy, qloss of pubic and axillary hair, q hypothyroidism, q adrenal cortical insufficiency. qexact pathogenesis is not understood, 17

DIAGNOSIS � sonography confirmes clinical diagnosis in only 25 % of women � negative findings with sonographic examination do not exclude placental abruption 18

MANAGEMENT �with massive external bleeding, intensive resuscitation with blood plus crystalloid and prompt delivery to control hemorrhage are lifesaving for mother and hopefully, for fetus. �If the diagnosis is uncertain and the fetus is alive but without evidence of compromise, then close observation can be practiced in facilities capable of immediate intervention. �for the welfare of the distressed fetus, steps should be initiated immediately to correct maternal hypovolemia, and hypoxia to restore and maintain function of any placenta that is still implanted. 19

PLACENTA PREVIA � Placenta previa is used to describe a placenta that is implanted over or very near the internal cervical os. 20

�Kinds: • • Total placenta previa — internal os is covered completely by placenta Partial placenta previa —internal os is partially covered by placenta Marginal placenta previa —edge of the placenta is at the margin of internal os Low-lying placenta —placenta is implanted in lower uterine segment such that the placental edge does not reach the internal os, but is in close proximity to it 21

CLINICAL FINDINGS � The most characteristic event is painless hemorrhage � usually appear near the end of the second trimester and without warning � bleeding maybe appear in the onset of labor. � it may vary from slight to profuse � clinically may mimic placental abruption. � Hemorrhage from the implantation site in the lower uterine segment may continue after placental delivery because the lower uterine segment contracts poorly. 22

DIAGNOSIS � The simplest, safest, and most accurate method of placental localization is provided by transabdominal sonography. (average accuracy is 96 %) � False-positive results are often a result of bladder distension , placenta is large and extended downward all the way to the internal cervical os. � transvaginal sonography � Magnetic Resonance (MR) Imaging (useful for diagnosis of placenta accreta ) 23

MANAGEMENT q. Cesarean delivery is necessary in practically all women with placenta previa qif fetus is reasonably mature : c/s q. The fetus is preterm and there are no other indications for delivery : close observation 24

POSTPARTUM HEMORRHAGE 25

� The single most significant cause of maternal death worldwide � One of the top three causes of maternal mortality in all of countries � Serious morbidity may follow PPH: � ARDS, � coagulopathy, � shock, � loss � of fertility, sheehan syn. 26

Incidence The incidence varies widely: 1 -5% of deliveries 27

Definition There is no single, satisfactory definition of PPH. q PPH is excessive bleeding that makes the patient symptomatic q Most common definition: Excess blood loss (>500 ml in NVD or >1000 ml in C/S) q Decline in Hct of 10%(not a clinically useful definition) 28

Types of PPH q Primary PPH(early): in the first 24 hours, 4 -6% of pregnancies q Secondary PPH(late): between 24 h to 612 weeks, (0. 5 -2% of pregnancies) 29

Atony q The most common cause of PPH is uterine atony q Complicates 1 in 20 births q Responsible for at least 80 % of cases of PPH 30

only a small proportion of women with any risk factors for PPH develop the disorder and many women without risk factors experience hemorrhage after delivery; thus, knowledge of risk factors is not very useful clinically 31


Planning & prevention q training team q. Protocol for management of PPH qequipments of medications and instruments are readily available in Labor and delivery units 33

DIAGNOSIS � The differentiation between bleeding from uterine atony and genital tract lacerations is tentatively determined by predisposing risk factors and the condition of uterus. � If bleeding persists despite a firm, wellcontracted uterus, the cause of the hemorrhage most likely is from lacerations � Bright red blood also suggests arterial blood from lacerations. � careful inspection of the vagina, cervix, and uterus is essential. 34

Management v management of PPH is multifaceted and can involve many teams (obstetricians, nurses, anesthesiologists, blood bank personnel, laboratory medicine, surgical subspecialists, interventional radiology). v These teams are often required to work together under great stress and time pressures v Coordination is essential and can be facilitated by protocols and flow diagrams that anticipate how these teams will communicate and function together. 35

Management of postpartum hemorrhage at vaginal delivery 36

Initial Interventions q. Fundal massage q. Massage should be maintained while other interventions are being initiated q Intravenous access q Laboratory tests q CBC, fibrinogen concentration , platelet count, PT, activated PTT, typed and crossed for multiple units of packed red blood cells. 37
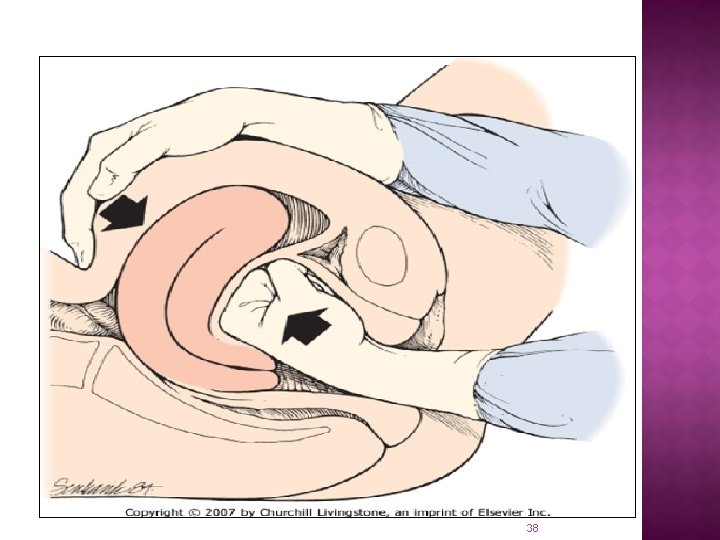
38

Fluid resuscitation and transfusion Monitoring vital signs Bladder catheter A large volume of crystalloid is infused Replacement of blood components 39

Uterotonic drugs Oxytocin • 40 units in 1 liter of normal saline • 10 units IM (including directly into the myometrium). • Higher doses of oxytocin (up to 80 units in 1000 m. L for a short duration (eg, over 30 minutes Methylergonovine • 0. 2 mg IM (or directly into the myometrium) (never IV). • May repeat at 2 -4 h intervals, as needed. If there has not been a good response to the first dose, quickly move on to a different uterotonic agent. Carboprost tromethamine (15 methyl-PGF 2α)(Hemabate) 250 mcg IM (or directly into the myometrium) every 15 -90 min, [a total dose of 2 mg (8 doses)], no asthma. (75 % respond to a single dose) move on to a different uterotonic agent if no response after one or two doses. 40

Uterotonic drugs(con) Misoprostol (PGE 1) § Is most useful for reducing blood loss in settings where injectable uterotonics are unavailable. § The optimum dose and route of administration are unclear. A dose of 400 mcg with the sublingual route is probably the optimal route of administration § Can be given to women with hypertension or asthma. § Maternal temperature should be monitored closely Dinoprostone (PGE 2) § 20 mg vaginal or rectal suppository is an alternative PGE to misoprostol (PGE 1). § Can be repeated at 2 -4 h intervals. Carbetocin, 41

Secondary Interventions Provide adequate anesthesia Inspect for and repair cervical and vaginal lacerations Exclude uterine rupture Remove retained products of conception Uterine tamponade 42
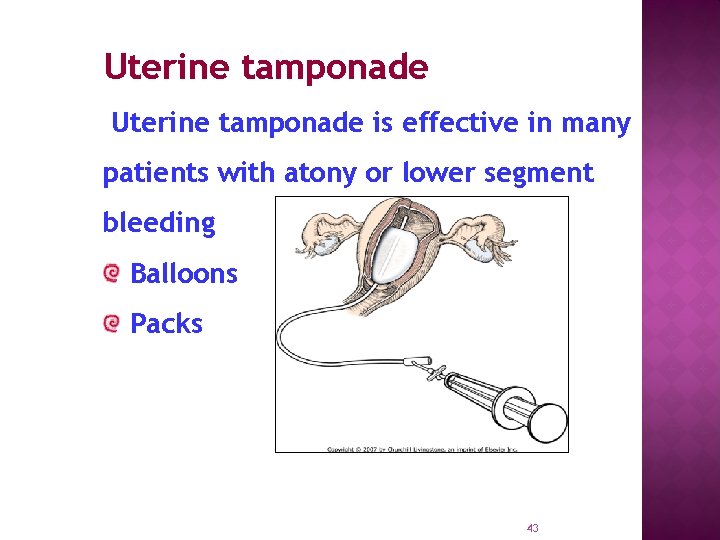
Uterine tamponade is effective in many patients with atony or lower segment bleeding Balloons Packs 43

INDICATIONS FOR LAPAROTOMY If vital signs are worse than expected for the estimated blood loss, the possibility of internal hemorrhage should be considered When a vaginal laceration has extended above the fornix Management of uterine atony unresponsive to the conservative interventions described 44

46

HYPOVOLEMIC SHOCK. 47

DEFINITIONS Hypovolemic Shock : there is an inadequate circulating blood volume resulting from hemorrhage or acute volume depletion. 48
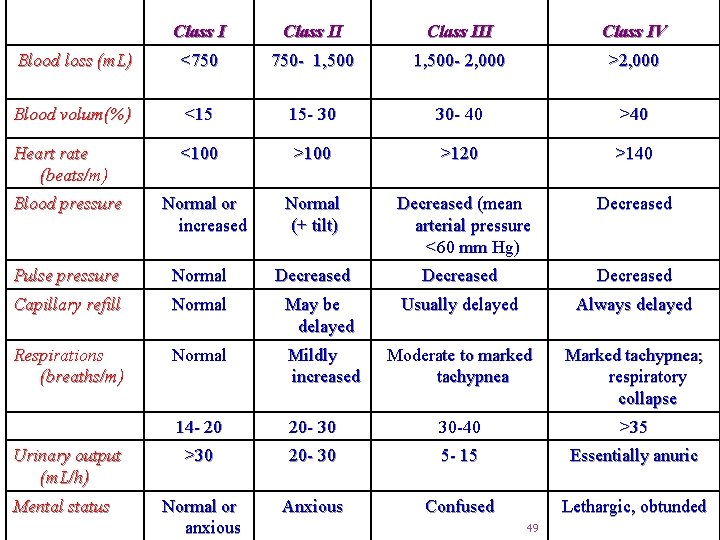
Class III Class IV Blood loss (m. L) <750 750 - 1, 500 - 2, 000 >2, 000 Blood volum(%) <15 15 - 30 30 - 40 >40 Heart rate (beats/m) <100 >120 >140 Blood pressure Normal or increased Normal (+ tilt) Decreased (mean arterial pressure <60 mm Hg) Decreased Pulse pressure Normal Decreased Capillary refill Normal May be delayed Usually delayed Always delayed Respirations (breaths/m) Normal Mildly increased Moderate to marked tachypnea Marked tachypnea; respiratory collapse 14 - 20 20 - 30 30 -40 >35 >30 20 - 30 5 - 15 Essentially anuric Normal or anxious Anxious Confused Lethargic, obtunded Urinary output (m. L/h) Mental status 49

Management of Shock 50

A team approach staff trained in intensive care medicine ORDER Oxygenate Restore circulatory volume Drug therapy Evaluate response to therapy Remedy the underlying cause 51

RESTORE CIRCULATING VOLUME � Rapid volume repletion is indicated. � Delayed therapy can lead to ischemic injury and possibly to irreversible shock and multiorgan system failure. � 1 - to 2 -liter fluid challenge with an isotonic electrolyte solution, preferably Ringer's lactate. � Fluid repletion continues at the initial rapid rate as long as the systemic blood pressure remains low. 52

� Clinical signs, BP, urine output, mental status, and peripheral perfusion guide resuscitation. 53

� inserting one or two large-bore (14 - or 16 -gauge) angiocatheters for volume replacement. � Trendelenburg position. � initial laboratory assessment CBC differential and platelets, electrolytes, BUN, Cr, calcium, magnesium, glucose, phosphate, and, where indicated, liver function studies, clotting profiles, serum lactate, and blood cultures. 54

� whole blood transfusion is standard. � Packed red blood cells (PRBC) have a volume of 200 to 250 m. L and a hematocrit of 70%. � normal saline+ PRBCs are the component of choice for hemorrhagic shock. 55

� oxygen-carrying capacity is met in most healthy patients with a hemoglobin of 7 g/d. L, then transfusion for moderate anemia (8 to 10 mg/d. L) is no recommended. but, correction of anemia is important. � In critically ill patients and those with significant underlying cardiac disease, RBC transfuse to maintain hemoglobin levels between 10 and 12 g/d. L 56

� For avoid the risks of hemolysis, agglutination, and clotting, all blood products should be administered through filtered lines with normal saline without electrolyte or drug additives. 57

PREVENTION OF HYPOTHERMIA �Rapid transfusion of multiple units of chilled blood may reduce the core temperature abruptly and can lead to cardiac arrhythmias. � hypothermia interfere with the normal functioning of the coagulation system. � A blood warmer should be used whenever more than three units are transfused. 58

Massive blood transfusion � Massive transfusion, defined as the replacement by transfusion of more than 50 percent of a patient's blood volume in 12 to 24 hours � Massive transfusion involves: � the selection of the appropriate amounts and types of blood components �management of bleeding and coagulation abnormalities �changes in ionized calcium, potassium, and acid-base balance. 59

RED CELL AND VOLUME REPLACEMENT � Correction of the deficit in blood volume with crystalloid volume expanders will generally maintain hemodynamic stability, while transfusion of red cells is used to improve and maintain tissue oxygenation. � Each unit of packed cells contains 200 m. L of red cells, will raise the hematocrit by 3 -4 % unless there is continued bleeding. � At rest, oxygen delivery is normally four times oxygen consumption. if intravascular volume is maintained during bleeding oxygen delivery will be adequate until the hematocrit falls below 10 percent. 60

COAGULATION PROTEINS � there will be 10 percent decrease in the concentration of clotting proteins for each 500 m. L of blood loss. � Additional bleeding based solely on dilution can occur when the level of coagulation proteins falls to 25 percent of normal. This usually requires 8 to 10 units of red cells in an adult. � Thus, the PT, a. PTT, and fibrinogen should be monitored in patients receiving massive blood transfusions of this magnitude. 61

� Two units of FFP should be given if the values exceed 1. 5 times control. � Each unit will increase the clotting protein levels by 10 percent. � Cryoprecipitate may be used when fibrinogen levels are critically low (<100 mg/d. L) 62

PLATELET COUNT �A similar dilutional effect on the platelet concentration can be seen with massive transfusion. � each 10 to 12 units of transfused red cells can produce a 50 percent fall in the platelet count; thus, significant thrombocytopenia can be seen after 10 to 20 units of blood. � with platelet counts below 50, 000/micro. L. six units of random donor platelets, or one unit of apheresis platelets, should be given. � each unit should increase the platelet count by 5000 to 10, 000/micro. L. 63

THANK YOU 64
- Slides: 62