Reproductive System Male Reproductive System The Scrotum Sac
































- Slides: 63

Reproductive System

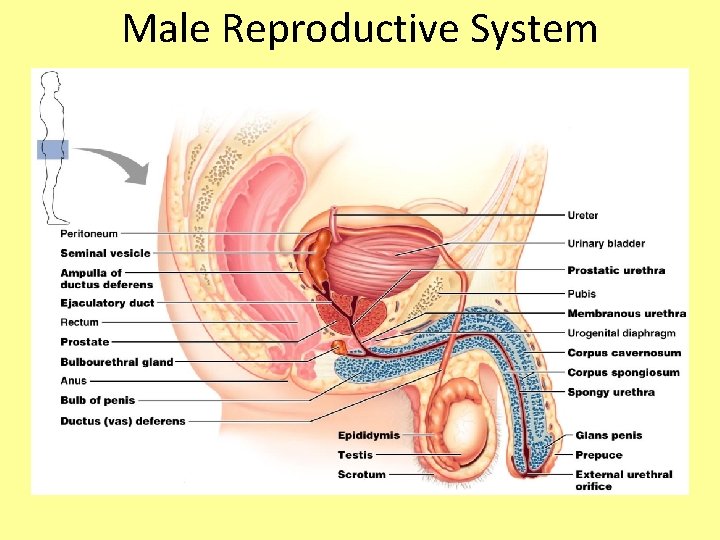
Male Reproductive System

The Scrotum • Sac of skin that hangs outside the abdominopelvic cavity at the root of the penis • Contains paired testicles separated by a midline septum • Its external positioning keeps the testes 3 C lower than core body temperature (needed for sperm production) • When external temperature is very cold, the scrotum becomes wrinkled as it is pulled closer to the warmth of the body wall

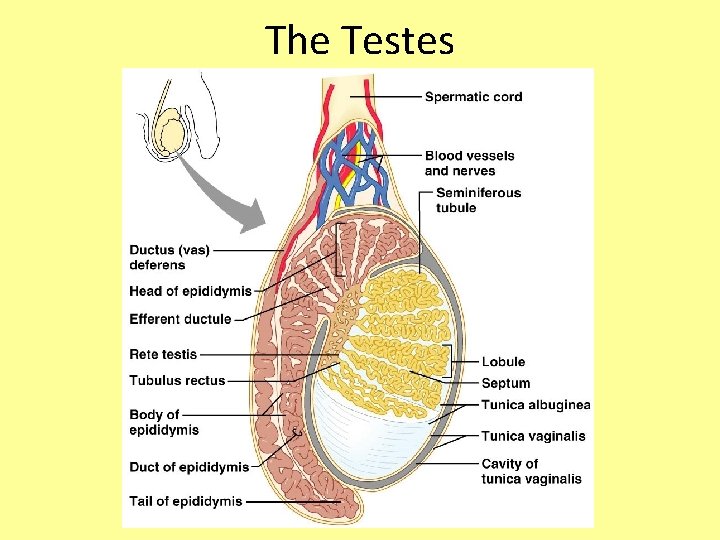
The Testes • Each testis is divided into 250 -300 lobules, each containing 1 -4 seminiferous tubules • Seminiferous tubules produce the sperm stimulated by FSH released by pituitary • Interstitial cells around the tubules produce androgens (testosterone) – stimulated by LH released by pituitary • Once the sperm are made, they continue to the epididymis

The Testes

The Epididymis • First part of male duct system • Provides a temporary storage site for the immature sperm cells – Trip through takes about 20 days – Sperm learn how to swim here! • When a male is sexually stimulated, the walls of the epididymis contract to propel sperm into the ductus deferens

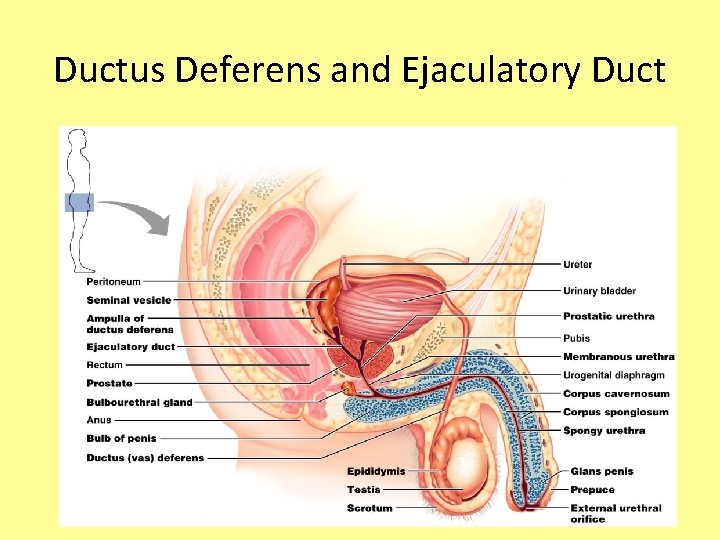
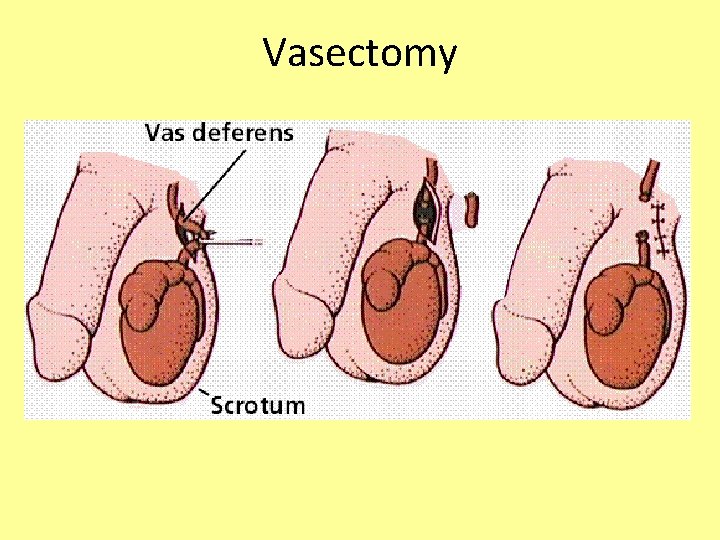
Ductus Deferens and Ejaculatory Duct • Propels sperm from the epididymis up into the pelvis, and back down to join up with the urethra • Also called the vas deferens • During an ejaculation, smooth muscles around the duct contract to create peristaltic waves that squeeze the sperm forward • Vasectomy – cutting and ligating the ductus deferens, which is a nearly 100% effective form of birth control

Ductus Deferens and Ejaculatory Duct

Vasectomy

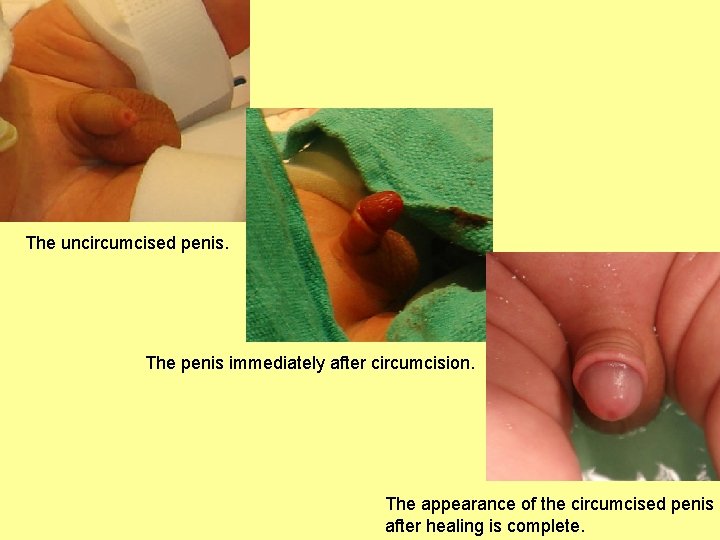
The Penis • A copulatory organ designed to deliver sperm into the female reproductive tract • Consists of an attached root and a free shaft that ends in the glans penis • Prepuce, or foreskin – cuff of skin covering the distal end of the penis – Circumcision – surgical removal of the foreskin after birth

The uncircumcised penis. The penis immediately after circumcision. The appearance of the circumcised penis after healing is complete.

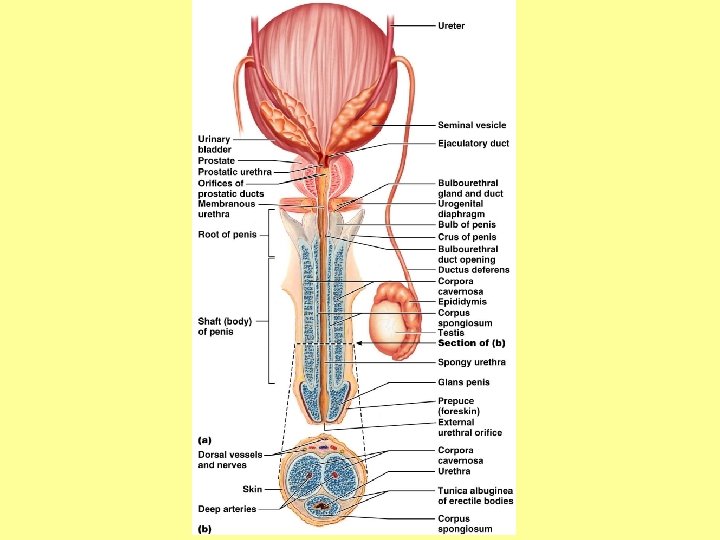
The Penis • Internal penis includes the urethra (which carries both semen and urine) and three cylindrical bodies of erectile tissue • Erectile tissue – spongy network of connective tissue and smooth muscle riddled with vascular spaces; assists with erection and ejaculation • Erection – during sexual excitement, the erectile tissue fills with blood causing the penis to enlarge and become rigid (which makes penetration easier)

The Penis

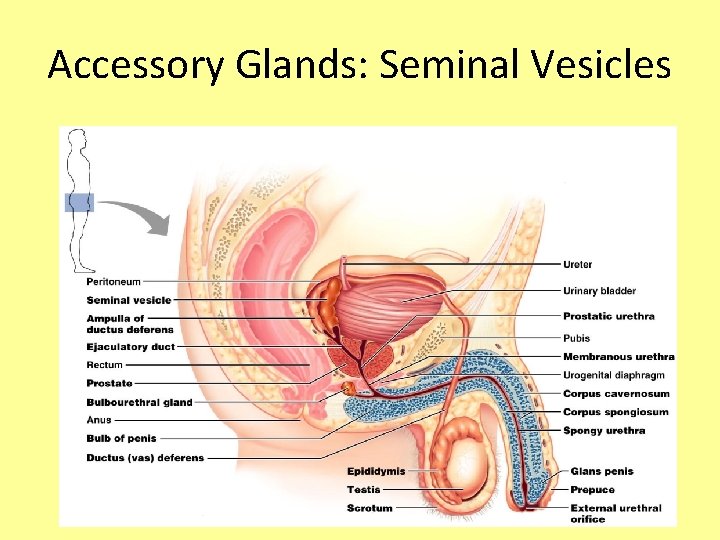
Accessory Glands: Seminal Vesicles • Lie on the posterior wall of the bladder and secretes 60% of the volume of semen • Join the ductus deferens to form the ejaculatory duct • Sperm and seminal fluid mix in the ejaculatory duct and enter the urethra during ejaculation

Accessory Glands: Seminal Vesicles

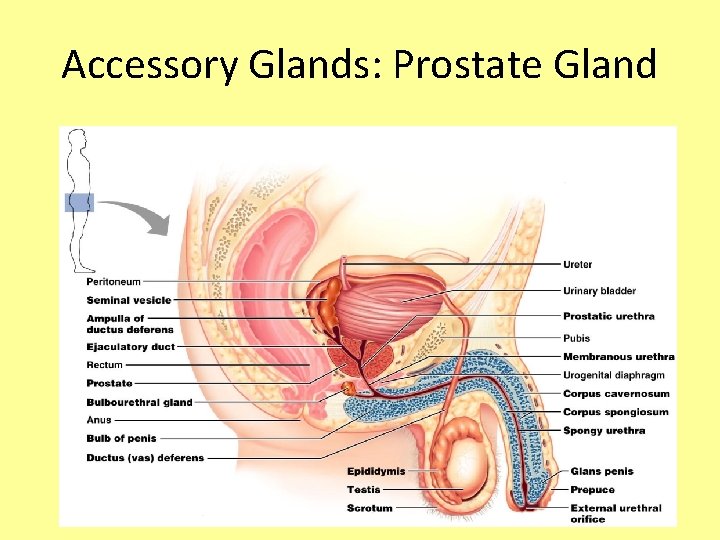
Accessory Glands: Prostate Gland • Doughnut-shaped gland that encircles part of the urethra inferior to the bladder • Its milky fluid, which contains citrate (Vitamin C), enzymes, and prostate-specific antigen (PSA), accounts for one-third of the semen volume • Fluid helps to activate sperm • Fluid made enters the urethra during ejaculation

Accessory Glands: Prostate Gland

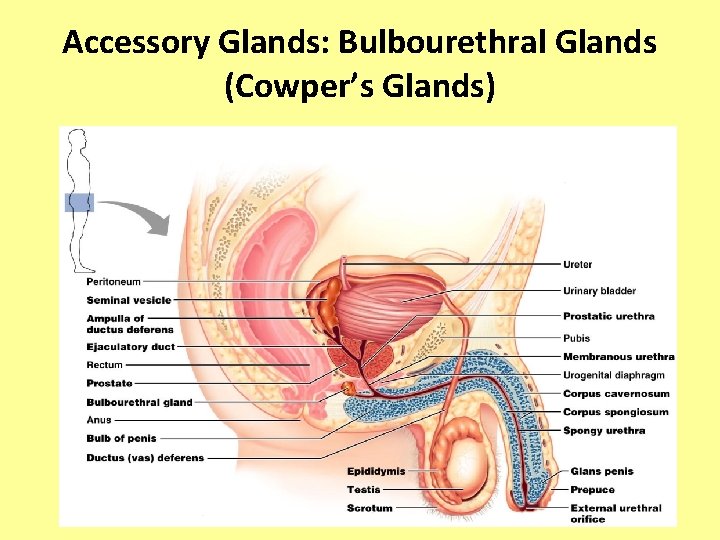
Accessory Glands: Bulbourethral Glands (Cowper’s Glands) • Pea-sized glands inferior to the prostate • Produce thick, clear mucus prior to ejaculation that neutralizes traces of acidic urine in the urethra

Accessory Glands: Bulbourethral Glands (Cowper’s Glands)

Semen • Milky white, sticky mixture of sperm and accessory gland secretions • Provides a transport medium and nutrients (fructose), protects and activates sperm, and facilitates their movement • Prostaglandins in semen: – Decrease the viscosity of mucus in the cervix – Stimulate reverse peristalsis in the uterus – Facilitate the movement of sperm through the female reproductive tract

Semen • Sperm are most active at neutral p. H, and can even die off at p. H of 4 and below! • However, vaginal p. H is normally 3. 5 -3. 9! • Seminal fluid and prostate gland fluid has a p. H of 7. 27. 6, which will help to neutralize out the vagina… but this doesn’t last forever! • p. H in vagina will drop back down to 4. 0 within 8 hours – so the lifetime of sperm in the vaginal canal is 8 hours max; lifetime in the uterus and fallopian tubes is about 48 hours • Only 2 -5 m. L of semen are ejaculated, but it contains 50 -130 million sperm per m. L

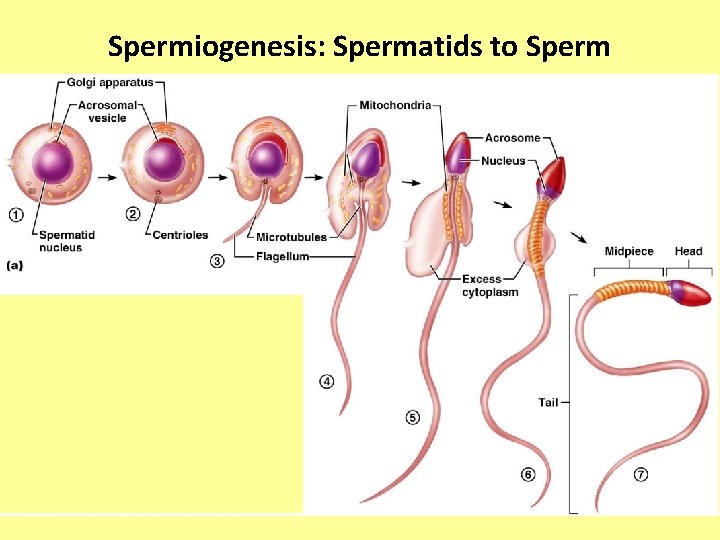
Sperm • Sperm have three major regions – Head – contains DNA and has a helmetlike acrosome containing hydrolytic enzymes that allow the sperm to penetrate and enter the egg – Midpiece – contains mitochondria spiraled around the tail filaments – Tail – a typical flagellum produced by a centriole

Spermiogenesis: Spermatids to Sperm


Secondary Male Characteristics • Deeper voice due to enlarged larynx • Increased hair growth over body, especially in axillary and pubic regions, as well as on face • Enlargement of skeletal muscles • Increased heaviness of bones • Long, narrow pelvis • All are due to testosterone levels

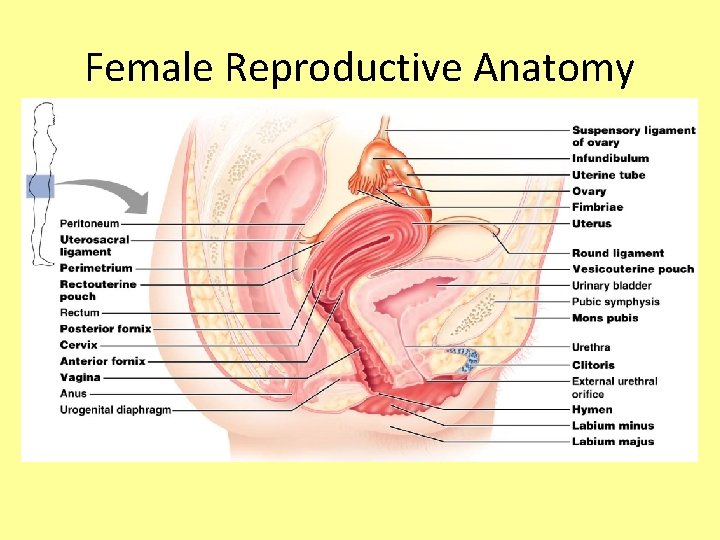
Female Reproductive Anatomy

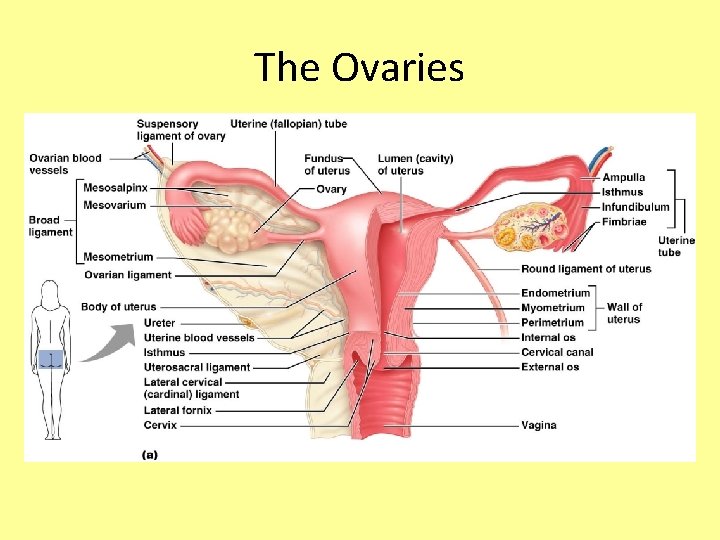
The Ovaries • Paired organs on each side of the uterus held in place by several ligaments • About the size & shape of almonds • Embedded in the ovary are follicles

The Ovaries

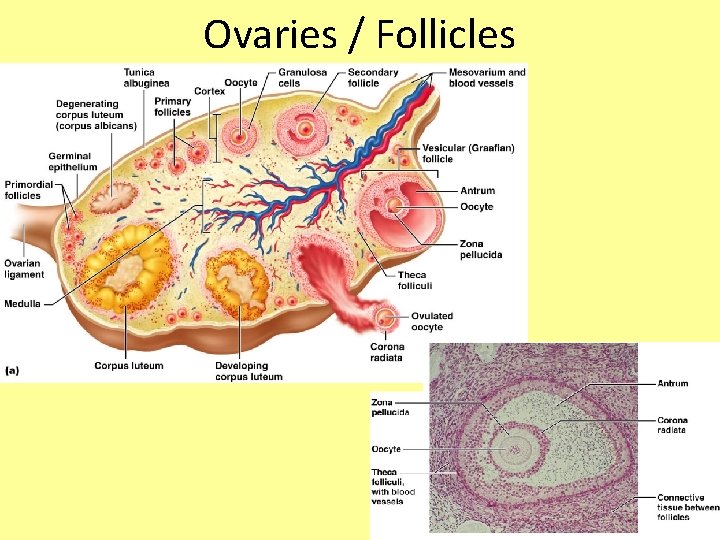
Follicles • Each follicle consists of an immature egg called an oocyte • Oocytes are surrounded by layers of follicle cells, which will mature – because of FSH released from pituitary • When follicle is mature, the developing egg (ova) will be released (ovulation) – stimulated by LH released from pituitary • After ovulation, the ruptured follicle is called a corpus luteum, which eventually degenerates

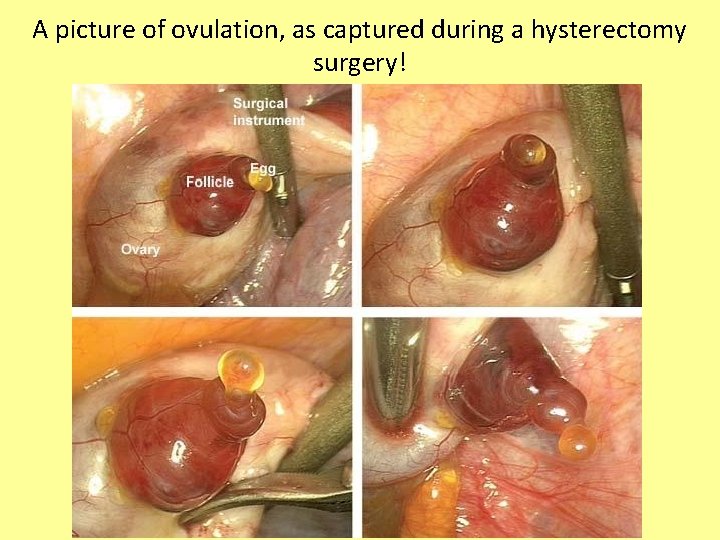
A picture of ovulation, as captured during a hysterectomy surgery!

A note about oocytes… • Females are born with approximately 700, 000 oocytes at birth combined in the two ovaries… this is the lifetime supply, and no more will develop • The number already decreases down to 400, 000 by puberty, and only about 500 eggs will be released during a woman’s lifetime • This is different than in the males, where sperm continue to be produced throughout the reproductive lifetime

Ovaries / Follicles

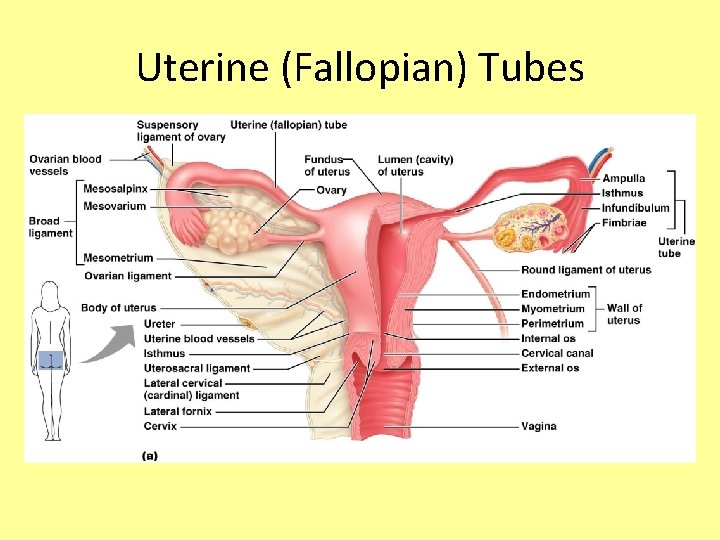
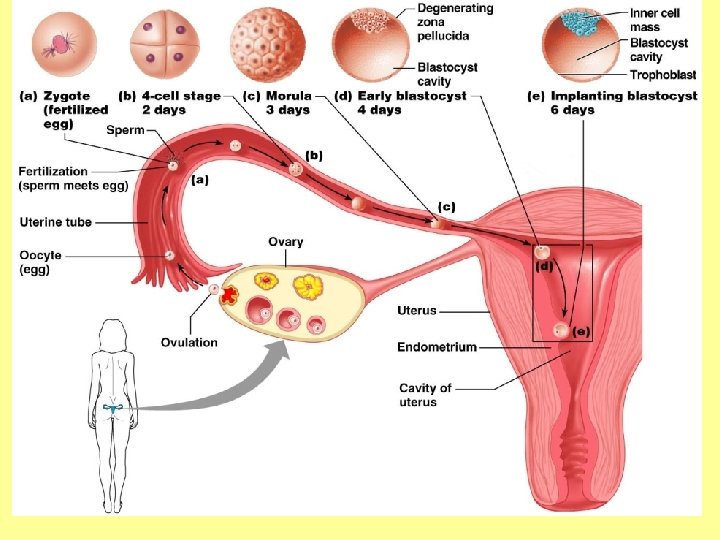
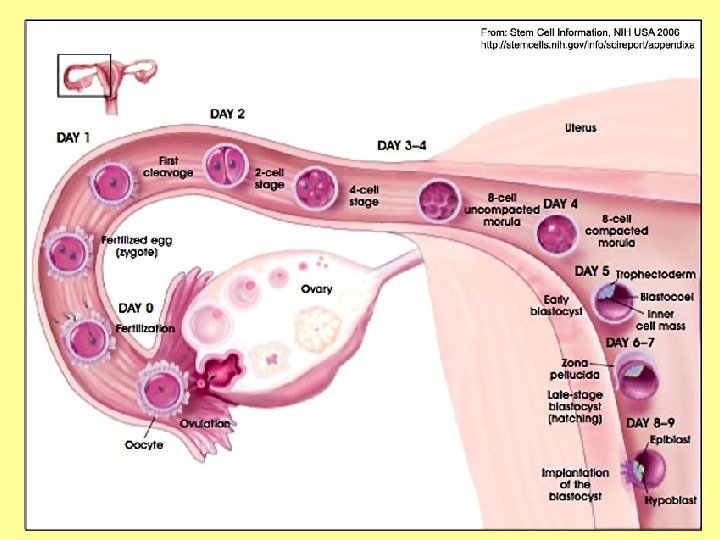
Uterine (Fallopian) Tubes • Each tube is about 10 cm long and 1 cm in diameter • Allows egg (ova) to travel from ovary to uterus • Usually the site of fertilization • End of tube near the ovary expands to form a funnel-shaped infundibulum, which has fingerlike extensions (fimbriae)

Uterine (Fallopian) Tubes • The uterine tubes have no contact with the ovaries and the ovulated ovais cast into the peritoneal cavity • Beating cilia on the fimbriae create currents to carry the ova into the uterine tube • The ova is carried toward the uterus by peristalsis and ciliary action

Uterine (Fallopian) Tubes


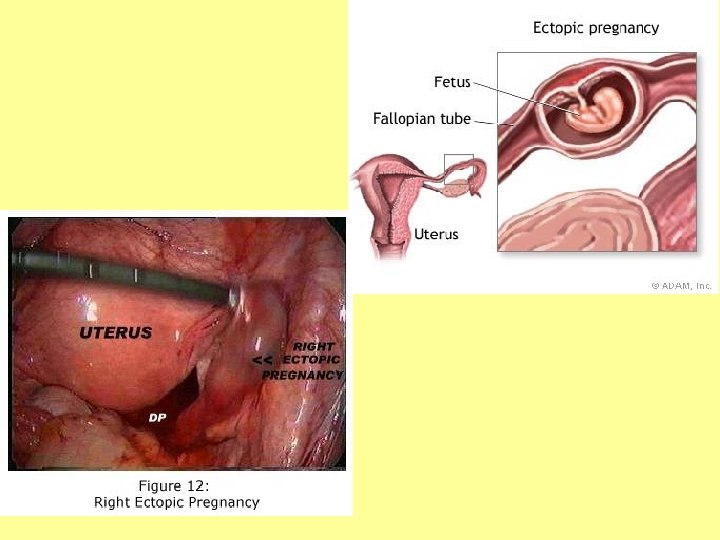
Ectopic Pregnancy • While ova get fertilized in the uterine tubes, the egg should not implant here! • If the egg is implanted anywhere other than the uterus, this is called an ectopic pregnancy • 98% of ectopic pregnancies occur in the uterine tubes • Most will resolve themselves naturally through a miscarriage, but sometimes surgery is required to remove the fetus or internal bleeding can occur


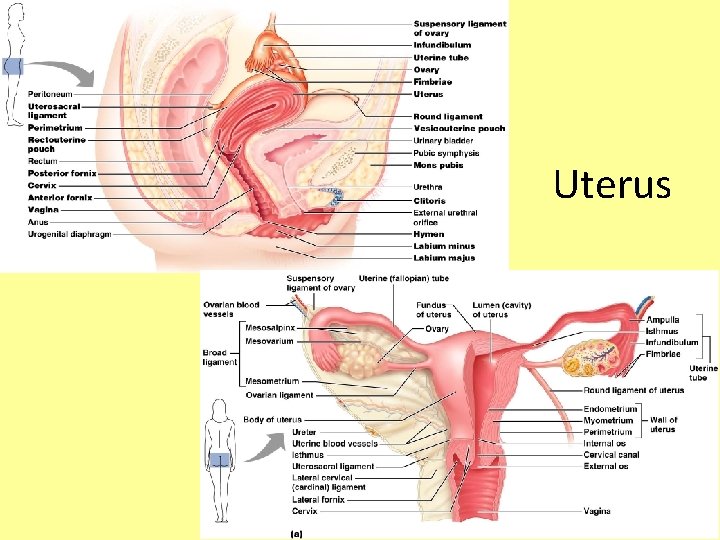
Uterus • Hollow, thick-walled organ located in the pelvis anterior to the rectum and posterosuperior to the bladder • Where implantation of fertilized ova occurs • About the size and shape of a pear • Body – major portion of the uterus • Fundus – rounded region superior to the entrance of the uterine tubes • Cervix – narrow neck which projects into the vagina inferiorly

Uterus

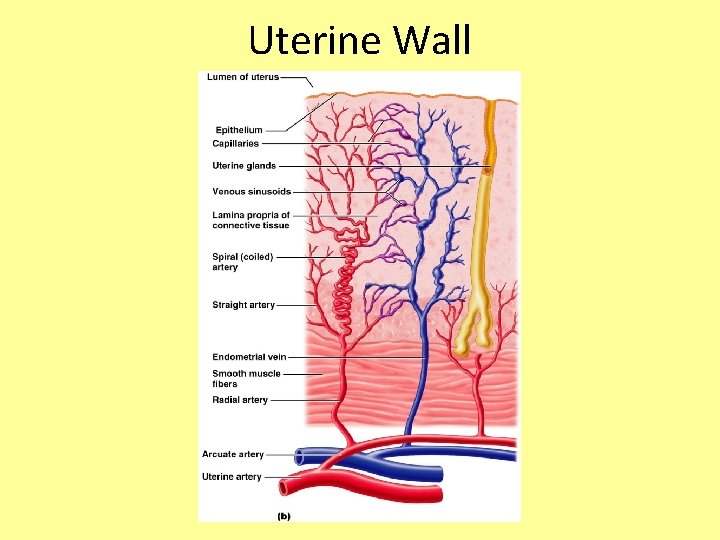
Uterine Wall • Wall composed of three layers – Perimetrium – outermost serous layer; the visceral peritoneum – Myometrium – middle layer; interlacing layers of smooth muscle; contracts during childbirth – Endometrium – mucosal lining of the uterine cavity

Uterine Wall

Endometrium • If fertilization occurs, the fertilized egg burrows into the endometrium and resides there for the rest of development • When a woman is not pregnant, the endometrial lining sloughs off periodically (approximately every 28 days) in response to hormone levels

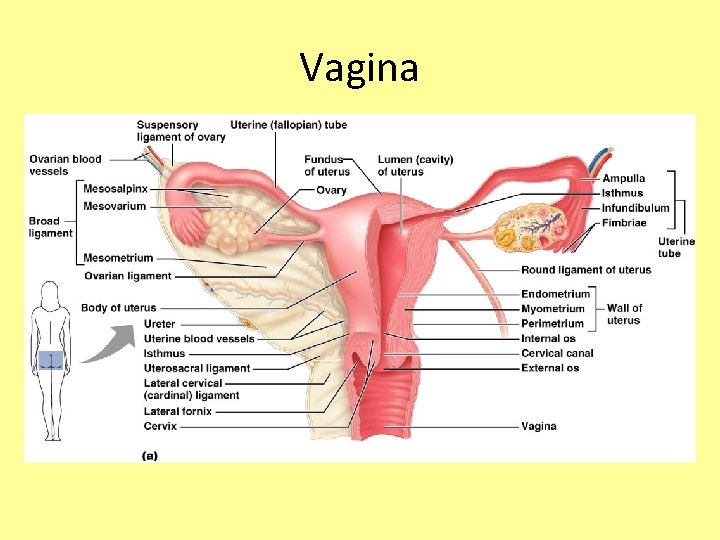
Vagina • Thin-walled tube about 3 to 4 inches long extending from the cervix to the exterior of the body • The urethra is embedded in the anterior wall • Provides a passageway for male penetration, birth, and menstrual flow • The labial folds protect the vaginal opening and the urethral opening

Vagina

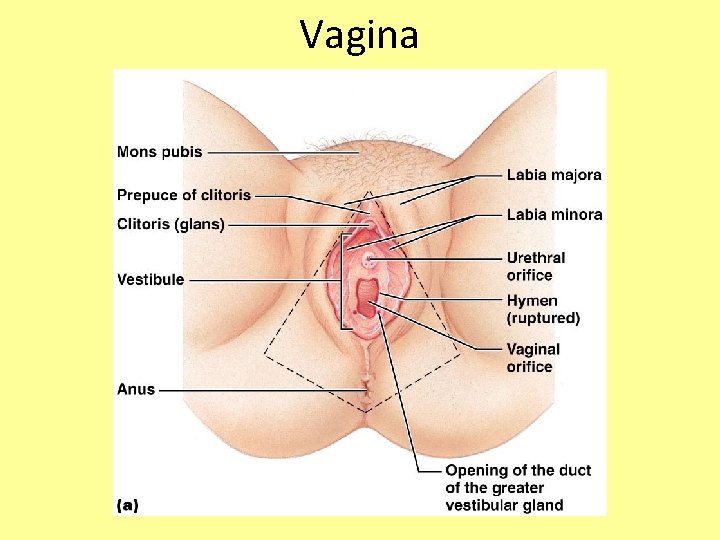
Vagina

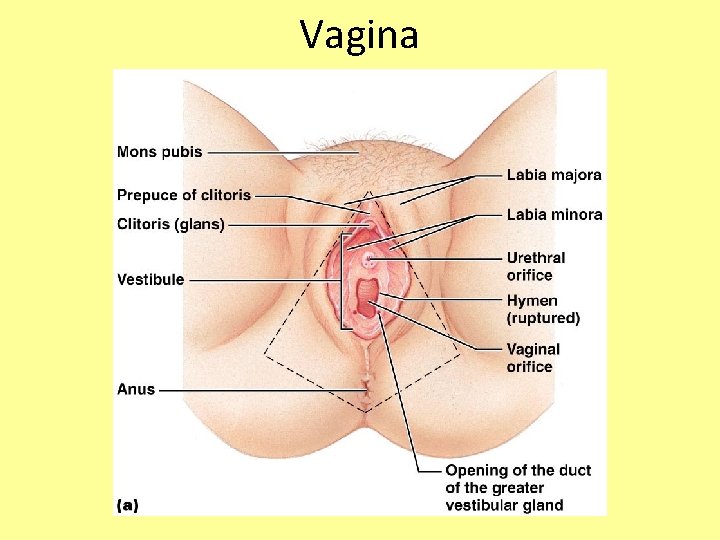
External Genitalia • Clitoris (homologous to the penis) – Erectile tissue that become swollen with blood during sexual excitement • Greater vestibular glands – Secretions lubricate the distal end of the vagina during intercourse

Vagina

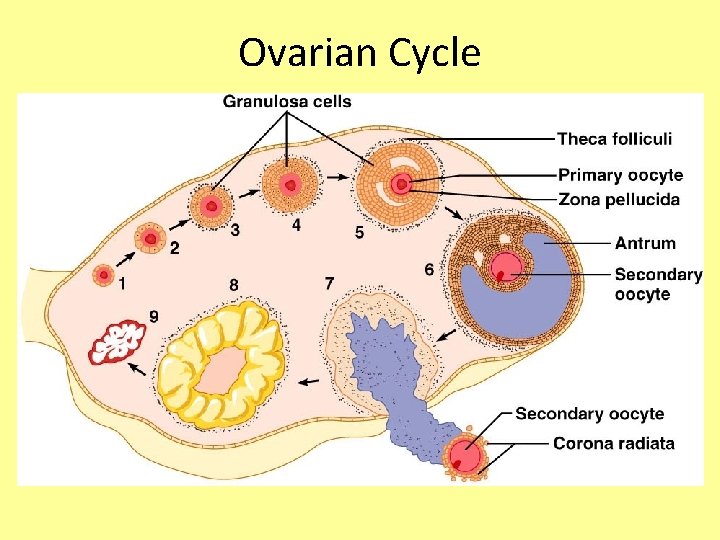
Monthly Female Cycles • Include the Ovarian Cycle and the Menstrual Cycle

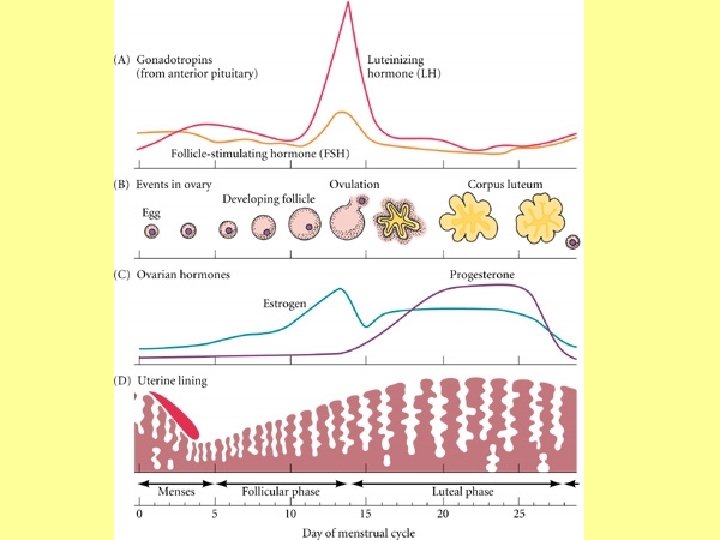
Ovarian Cycle • Monthly series of events associated with the maturation of an egg • Follicular phase – period of follicle growth (days 1– 14) – due to FSH; causes production of estrogen • Ovulation occurs midcycle due to LH – 1 -2% of ovulations release more than one ova, which if both fertilized, results in fraternal t • Luteal phase – period of corpus luteum activity (days 14– 28)

Ovarian Cycle

Luteal Phase • The corpus luteum secretes progesterone and estrogen • If pregnancy does not occur, the corpus luteum degenerates in 10 days and levels of progesterone and estrogen will decrease • If pregnancy does occur, the corpus luteum continues to produces hormones until the placenta takes over that role (at about 3 months)

Uterine (Menstrual) Cycle • Series of cyclic changes that the uterine endometrium goes through each month in response to ovarian hormones in the blood

Uterine (Menstrual) Cycle • Days 1 -5: Menstrual (Menses) Phase – uterus sheds all but the deepest part of the endometrium • Days 4 -14: Proliferative (Follicular) Phase – endometrium rebuilds itself due to rising estrogen levels (released from growing follicles) • Days 15 -28: Secretory (Luteal) phase – endometrium prepares for implantation of the embryo by increasing blood flow and nutrients due to rising progesterone levels (released from corpus luteum)

Menses • If fertilization does not occur, progesterone levels fall, depriving the endometrium of hormonal support • Arteries in uterine wall kink and go into spasms and endometrial cells begin to die • This causes the layer to disintegrate and slough off, opening up blood vessels to allow blood flow • Average blood loss during this period is 50 to 150 m. L (about ¼ to ½ cup, but can vary from woman to woman)


Secondary Female Characteristics • Development of breast tissue • Increased deposition of fat in hip and breast areas • Widening and lightening of the pelvis • Growth of armpit and pubic hair • All are due to estrogen and progesterone levels





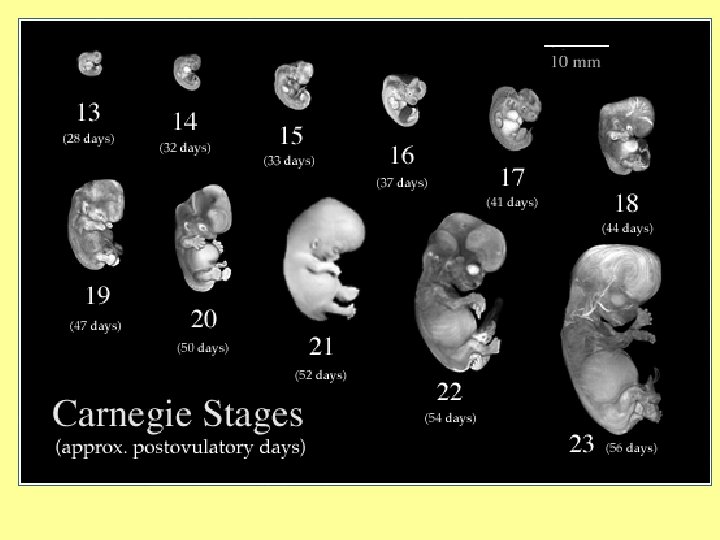
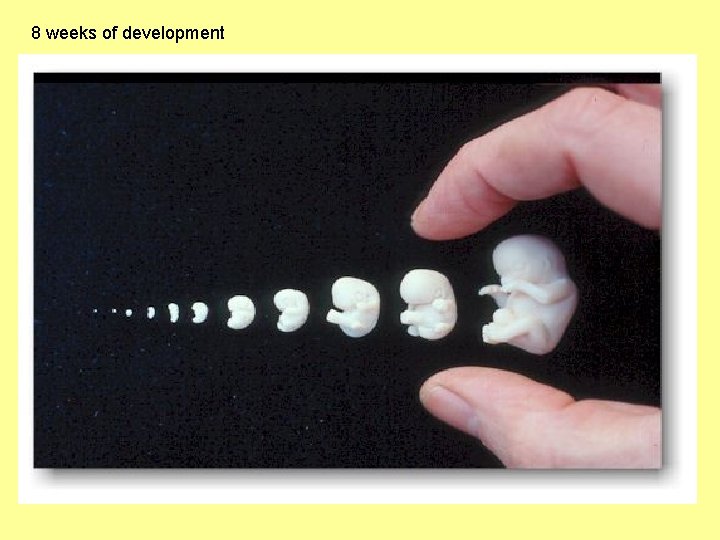
8 weeks of development
