MRI INTERPRETATION OF PITUITARY SELLAR LESIONS Pituitary MRI





























- Slides: 53

MRI INTERPRETATION OF PITUITARY SELLAR LESIONS

Pituitary MRI interpretation • Sellar anatomy • Indications for sellar imaging • Imaging protocol • The normal pituitary on MRI • Differential diagnosis of sellar masses • Radiographic appearance & overview of sellar lesions

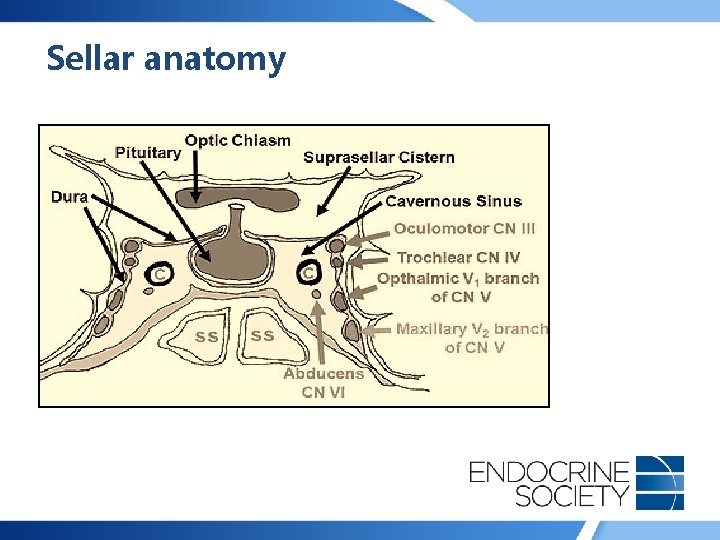
Sellar anatomy

Indications for sellar imaging • Mass effect on parasellar structures – Cranial nerve (CN) dysfunction involving CN II, IV, V, VI – Headache (especially if acute/severe or associated with cranial nerve dysfunction) • Pituitary hormone excess • Hypopituitarism

Pituitary MRI • MRI examination using a pituitary protocol is the method of choice for imaging most sellar lesions • Coronal and sagittal T 1 -SE, high resolution sequences (2 -3 mm slices; TE: 10 -15 msec, TR: 400 -600 msec) before and after gadolinium • Coronal T 2 sequences (2 -3 mm slices) helpful to detect cystic fluid or blood • Obtaining images of the rest of the brain during MRI is important, as some sellar pathologies may also involve other brain areas

Is there a role for CT imaging of the sella? • CT examination (pituitary protocol) can be helpful in sellar imaging of patients with most (non-MRI compatible) pacemakers who cannot undergo MRI • CT examination (pituitary protocol) is more helpful than MRI in imaging bone erosions, sellar calcifications or acute intrasellar hemorrhage

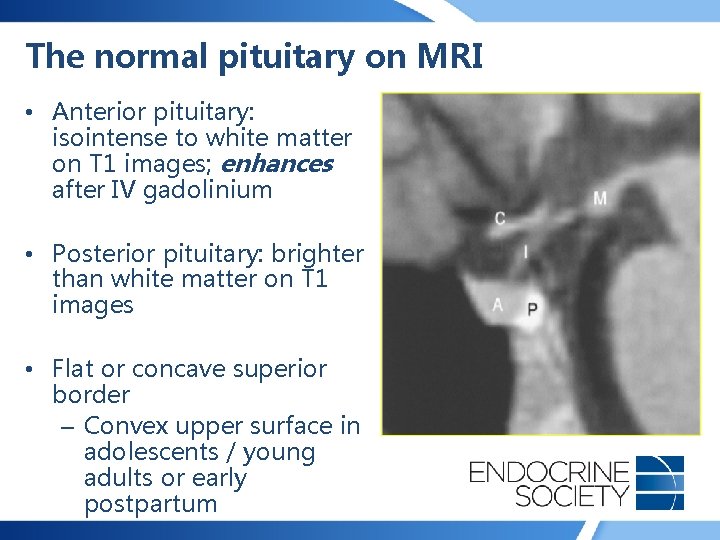
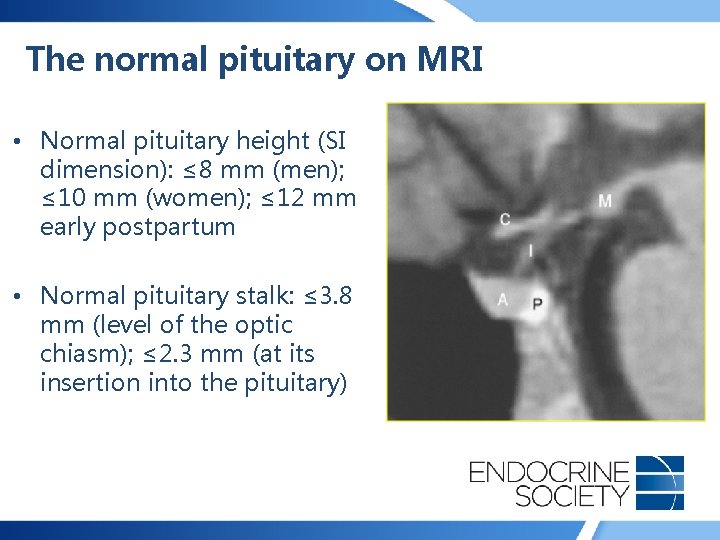
The normal pituitary on MRI • Anterior pituitary: isointense to white matter on T 1 images; enhances after IV gadolinium • Posterior pituitary: brighter than white matter on T 1 images • Flat or concave superior border – Convex upper surface in adolescents / young adults or early postpartum

The normal pituitary on MRI • Normal pituitary height (SI dimension): ≤ 8 mm (men); ≤ 10 mm (women); ≤ 12 mm early postpartum • Normal pituitary stalk: ≤ 3. 8 mm (level of the optic chiasm); ≤ 2. 3 mm (at its insertion into the pituitary)

Sellar masses • Sellar masses may be found during the targeted investigation of related symptoms • Sellar masses may be incidental findings on imaging studies (evaluation of head injury, tinnitus and others)

Differential diagnosis Pituitary adenomas • In one surgical series, pituitary adenomas accounted for 91% of all sellar masses • Approximately 42% of these were clinically nonfunctioning pituitary adenomas • Prolactinomas (19%), growth hormone secreting adenomas (15%), corticotropin secreting adenomas (14%), and thyrotropinomas (0. 6%) were less frequent in this series

Differential diagnosis Sellar lesions other than adenomas • Neoplasms – Craniopharyngioma, meningioma, germ cell tumor, glioma, chordoma, chondrosarcoma, metastases, lymphoma • Cysts – Rathke’s cleft cyst, arachnoid cyst, epidermoid cyst, dermoid cyst • Vascular – Aneurysm, cavernous malformation • Empty sella

Differential diagnosis Sellar lesions other than adenomas • Inflammatory – Lymphocytic, granulomatous, necrotizing or xanthomatous hypophysitis; Ig. G 4 -related disease, sarcoidosis, Langerhans cell histiocytosis, granulomatosis with polyangiitis (Wegener’s granulomatosis), drug-induced • Infectious – Bacterial abscess, Whipple’s disease, tuberculosis, fungal infection, other infections (Pneumocystis, Entamoeba, cysticercosis) • Pituitary hyperplasia – Associated with pregnancy, target gland hypofunction or ectopic releasing hormone secretion

Differential diagnosis Sellar lesions other than adenomas Among 116 patients with non-adenomatous sellar masses who underwent transsphenoidal surgery at MGH (19982009): • Cystic lesions: 53% – Rathke’s cleft cysts: 42% of all cases • Benign neoplasms: 22% • Malignant neoplasms: 16% – Of these: ¼ were metastases and ¾ were primary neoplasms • Inflammatory lesions: 9% Valassi E et al, Clin Endocrinology, 2010

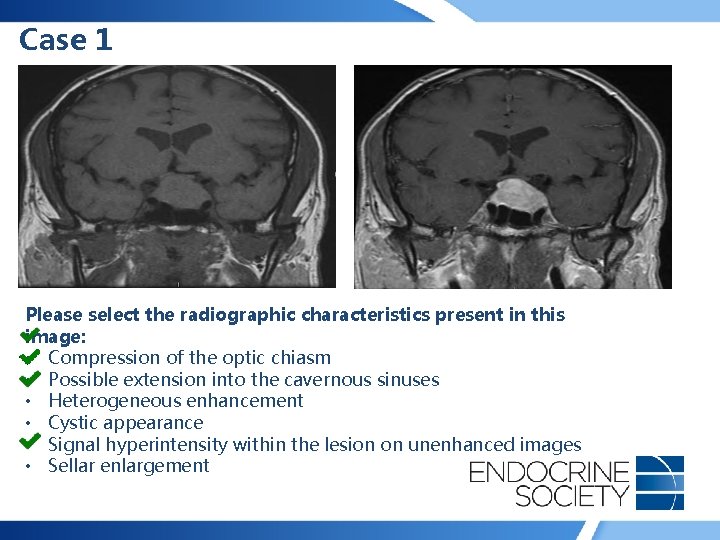
Case 1 • 45 yr man presented with decreased vision in his left eye and low libido • No headache, diplopia, weight change, history of hypertension or diabetes mellitus, or acral enlargement • Prolactin: 45 ng/m. L (0 -15); Testosterone: 160 ng/dl (270 -1070); LH: 2 U/l (1 -12); FSH: 3 U/l (1 -12)

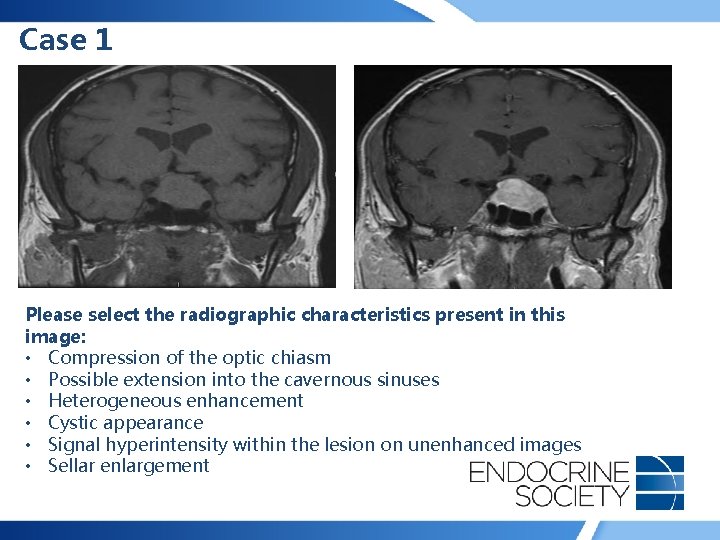
Case 1 Please select the radiographic characteristics present in this image: • Compression of the optic chiasm • Possible extension into the cavernous sinuses • Heterogeneous enhancement • Cystic appearance • Signal hyperintensity within the lesion on unenhanced images • Sellar enlargement

Case 1 Please select the radiographic characteristics present in this image: • Compression of the optic chiasm • Possible extension into the cavernous sinuses • Heterogeneous enhancement • Cystic appearance • Signal hyperintensity within the lesion on unenhanced images • Sellar enlargement

Which of the following is the correct diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

Which of the following is the correct diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

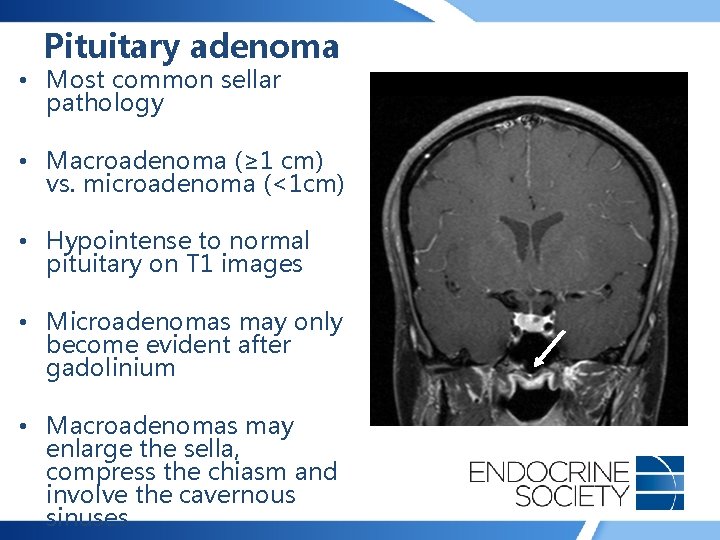
Pituitary adenoma • Most common sellar pathology • Macroadenoma (≥ 1 cm) vs. microadenoma (<1 cm) • Hypointense to normal pituitary on T 1 images • Microadenomas may only become evident after gadolinium • Macroadenomas may enlarge the sella, compress the chiasm and involve the cavernous sinuses

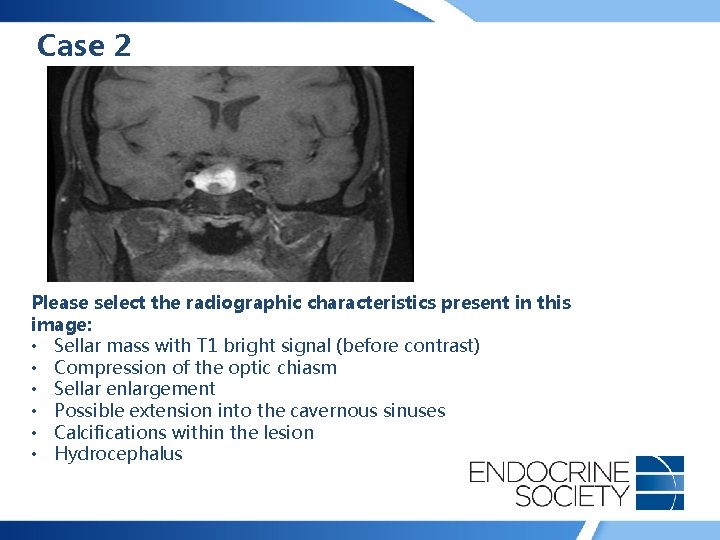
Case 2 • 52 -year-old man presented with severe headache of acute onset, decreased vision bitemporally, right ptosis, horizontal diplopia, nausea • No weight change, history of hypertension or diabetes mellitus, acral enlargement • Prolactin: 15 ng/ml (0 -15); morning cortisol: 2 mcg/dl; TSH: 1. 1 mcu/ml (0. 4 -4. 5); free T 4: 0. 6 ng/dl (0. 9 -1. 8)

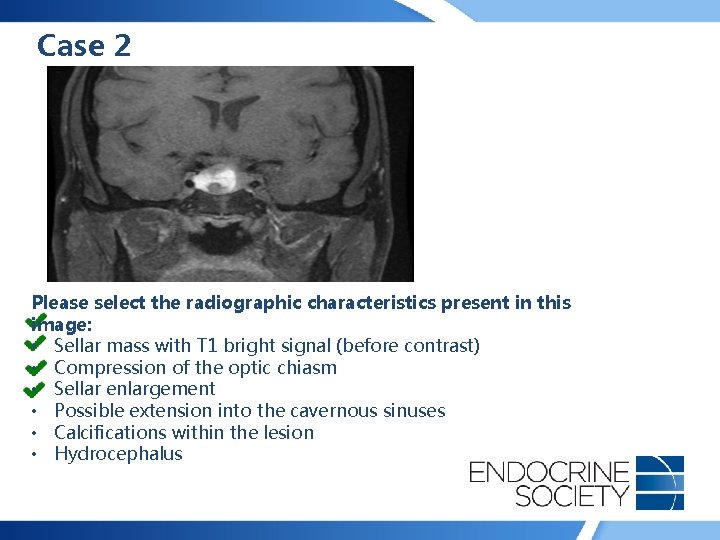
Case 2 Please select the radiographic characteristics present in this image: • Sellar mass with T 1 bright signal (before contrast) • Compression of the optic chiasm • Sellar enlargement • Possible extension into the cavernous sinuses • Calcifications within the lesion • Hydrocephalus

Case 2 Please select the radiographic characteristics present in this image: • Sellar mass with T 1 bright signal (before contrast) • Compression of the optic chiasm • Sellar enlargement • Possible extension into the cavernous sinuses • Calcifications within the lesion • Hydrocephalus

Which of the following is the correct diagnosis? A. Aneurysm B. Pituitary apoplexy C. Meningioma D. Craniopharyngioma

Which of the following is the correct diagnosis? A. Aneurysm B. Pituitary apoplexy C. Meningioma D. Craniopharyngioma

Pituitary apoplexy • Hemorrhage and/or infarction of pituitary adenoma • Severe headache of acute onset (89%), vomiting (57%) • Visual field deficits (51%) • Other (III, IV, V, VI) cranial nerve dysfunction (46%) • Fever (16%), neck stiffness (25%), impaired consciousness (14%) • Hypopituitarism very common (85%) • Neurosurgical and neuroendocrine emergency!

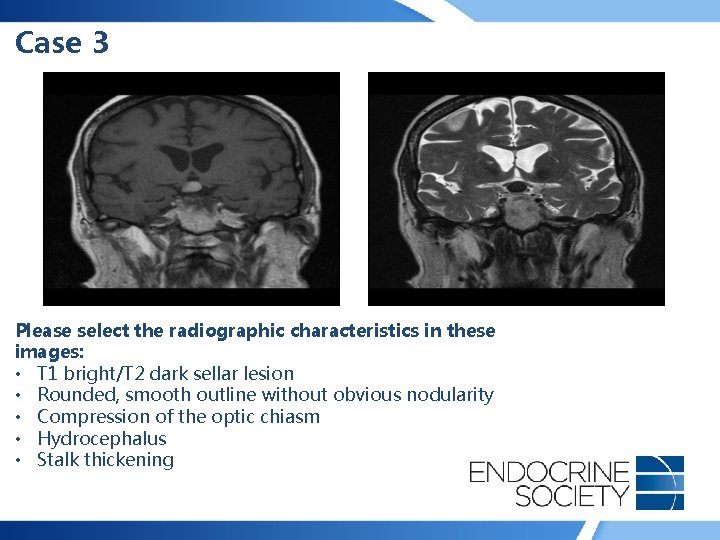
Case 3 • 24 -year-old woman presented with secondary amenorrhea and bitemporal vision loss. Menses were previously regular • No headache, weight change, history of hypertension or diabetes mellitus, acral enlargement, galactorrhea • Prolactin: 18 ng/ml (0 -20); FSH: 3 U/l (1 -20); E 2: 22 pg/ml (20 -440)

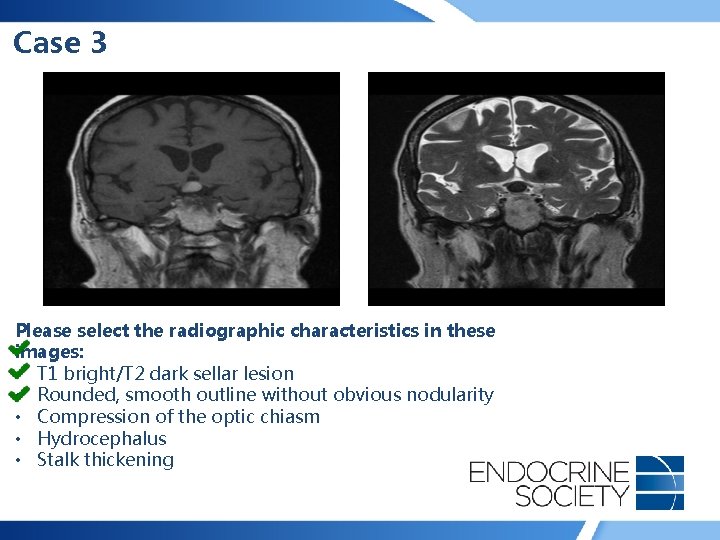
Case 3 Please select the radiographic characteristics in these images: • T 1 bright/T 2 dark sellar lesion • Rounded, smooth outline without obvious nodularity • Compression of the optic chiasm • Hydrocephalus • Stalk thickening

Case 3 Please select the radiographic characteristics in these images: • T 1 bright/T 2 dark sellar lesion • Rounded, smooth outline without obvious nodularity • Compression of the optic chiasm • Hydrocephalus • Stalk thickening

Which of the following is the most likely diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Germ-cell tumor D. Craniopharyngioma

Which of the following is the most likely diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Germ-cell tumor D. Craniopharyngioma

Rathke’s cleft cyst • Prevalence ~ 10 - 20% at autopsy • Non-neoplastic remnant of Rathke’s pouch • Approximately 10% may enlarge on serial imaging • Typically asymptomatic, but mass effect or hypopituitarism may occur • Drainage of cyst contents with limited resection of cyst wall and packing of the cavity may minimize the risk of surgical complications (including diabetes insipidus) • Recurrence (requiring re-operation) occurs in ~ 12% • Radiation therapy has been administered in small numbers of patients with recurrences (Mukherjee JJ et al, JCEM, 1997)

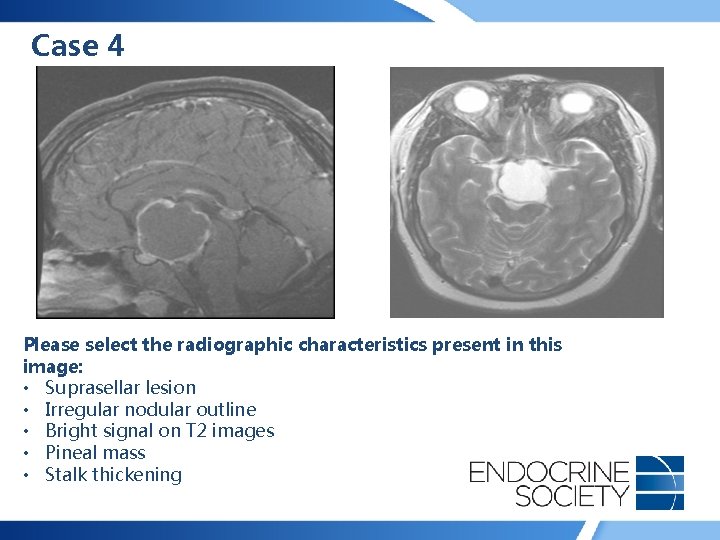
Case 4 • 19 -year-old woman presented with increased thirst, frequent urination, nocturia, and secondary amenorrhea • No headache, weight change, history of hypertension or diabetes mellitus, acral enlargement, galactorrhea • Prolactin: 25 ng/ml (0 -20); FSH: 2 U/l (1 -20); E 2 <20 pg/ml (20 -440); (morning) sodium: 147 mmol/l (135145); urine osmolality: 210 m. Osm/kg

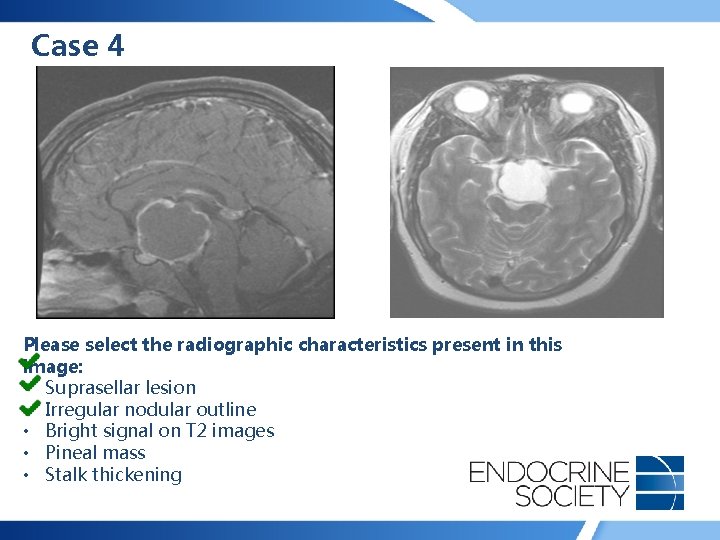
Case 4 Please select the radiographic characteristics present in this image: • Suprasellar lesion • Irregular nodular outline • Bright signal on T 2 images • Pineal mass • Stalk thickening

Case 4 Please select the radiographic characteristics present in this image: • Suprasellar lesion • Irregular nodular outline • Bright signal on T 2 images • Pineal mass • Stalk thickening

What is the diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

What is the diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

Craniopharyngiomas • Incidence ~ 0. 5 – 2. 0 cases per million annually • 30 – 50% of cases occur in children – Second incidence peak in the sixth decade of life • Derived from squamous remnants of Rathke’s pouch • Adamantinomatous tumors are mixed (cystic and solid) and more often occur in children (beta-catenin mutations in ~96%) – Tumors usually show calcifications • Papillary tumors are solid and usually occur in adults (BRAF V 600 E mutations in ~ 95%; Brastianos PK et al, Nature Gen, 2014)

Craniopharyngioma • Mass effect, diabetes insipidus, anterior hypopituitarism, hypothalamic obesity and neurocognitive deficits are common • Surgery with adjuvant radiation therapy is advised in patients with subtotal resection or recurrence (recurrence rate: 30% at 10 yr) • Might targeted therapies be effective in patients with papillary craniopharyngiomas harboring BRAF mutations? – Dabrafenib and trametinib administration (1 patient) led to a decrease in tumor size by 85% after 35 days of therapy (Brastianos PK et al, J Natl Cancer Inst, 2015) – Vemurafenib therapy (1 patient) led to a decrease in tumor size and improvement in vision (Aylwin SJ et al, Pituitary, 2015)

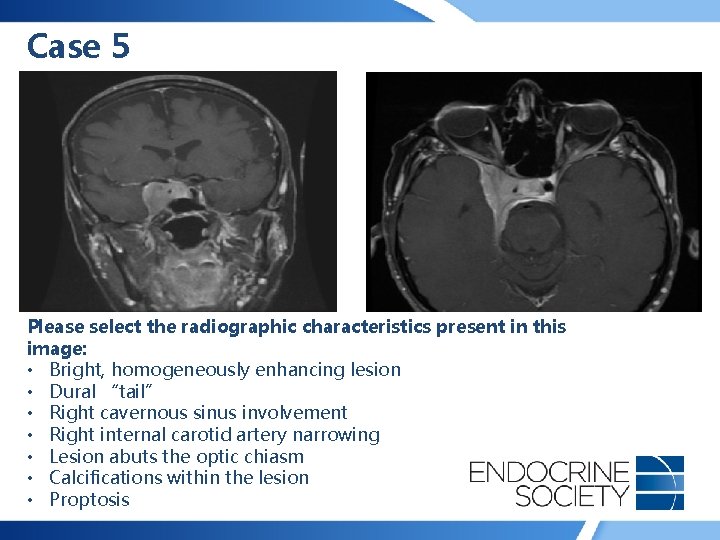
Case 5 • 62 -year-old woman presented with right eyelid ptosis and horizontal diplopia • Menses stopped at age 52 -years-old • No headache, weight change, history of hypertension or diabetes mellitus, acral enlargement, galactorrhea • No endocrine abnormalities identified on pituitary function testing

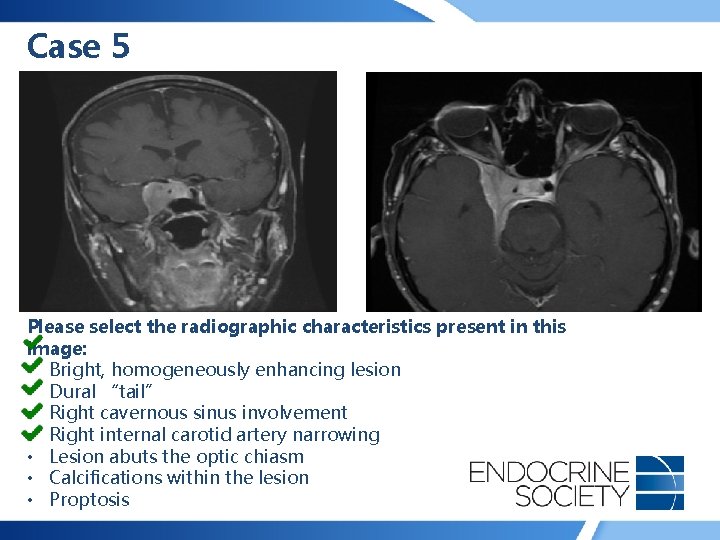
Case 5 Please select the radiographic characteristics present in this image: • Bright, homogeneously enhancing lesion • Dural “tail” • Right cavernous sinus involvement • Right internal carotid artery narrowing • Lesion abuts the optic chiasm • Calcifications within the lesion • Proptosis

Case 5 Please select the radiographic characteristics present in this image: • Bright, homogeneously enhancing lesion • Dural “tail” • Right cavernous sinus involvement • Right internal carotid artery narrowing • Lesion abuts the optic chiasm • Calcifications within the lesion • Proptosis

Which of the following is the most likely diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

Which of the following is the most likely diagnosis? A. Rathke’s cleft cyst B. Meningioma C. Pituitary adenoma D. Craniopharyngioma

Meningioma • Rare in children, increasing incidence with age throughout adulthood • Female to male incidence ratio exceeds 2 : 1 • Risk factors include previous radiation therapy and type 2 neurofibromatosis • Receptor expression (PR, ER, AR, GHR) is common • Parasellar meningiomas may arise from the planum sphenoidale, tuberculum sella, diaphragma sella or anterior clinoid processes • Surgery and/or radiation therapy are advisable for symptomatic, large or expanding lesions

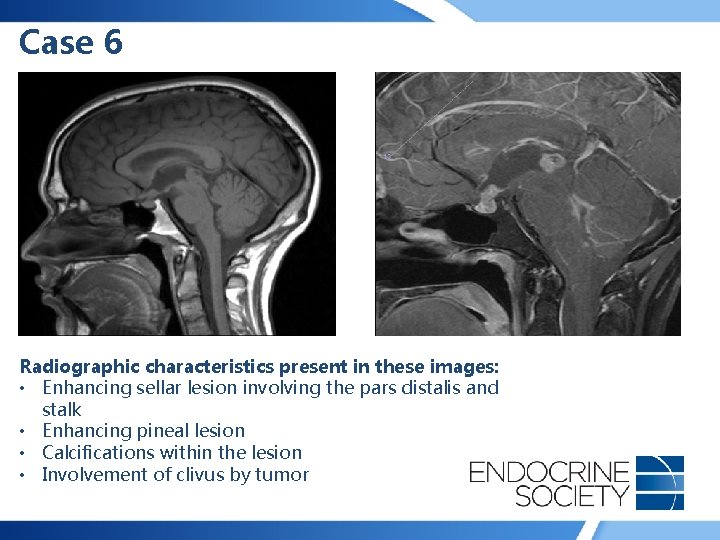
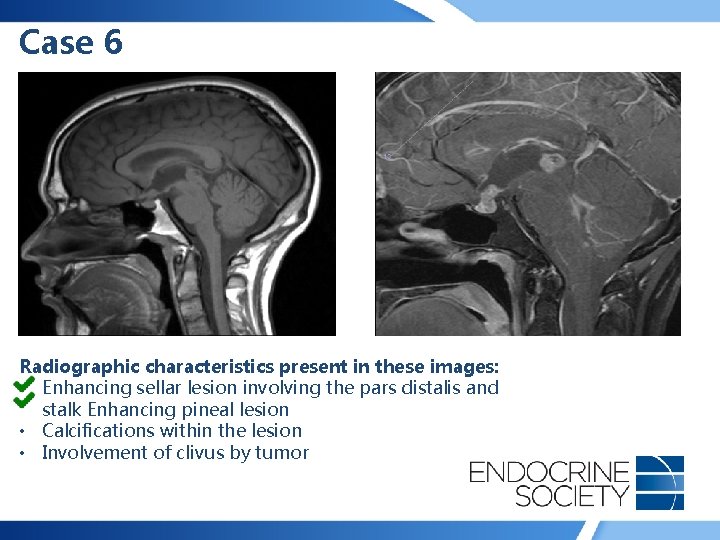
Case 6 • 18 -year-old man presented with fatigue, increased thirst and frequent urination • No headache, weight change, history of hypertension or diabetes mellitus, acral enlargement, edema • Panhypopituitarism (including central diabetes insipidus) was found on endocrine testing

Case 6 Radiographic characteristics present in these images: • Enhancing sellar lesion involving the pars distalis and stalk • Enhancing pineal lesion • Calcifications within the lesion • Involvement of clivus by tumor

Case 6 Radiographic characteristics present in these images: • Enhancing sellar lesion involving the pars distalis and stalk Enhancing pineal lesion • Calcifications within the lesion • Involvement of clivus by tumor

Which of the following is the most likely diagnosis? A. Hypophysitis B. Meningioma C. Germ-cell tumor D. Craniopharyngioma

Which of the following is the most likely diagnosis? A. Hypophysitis B. Meningioma C. Germ-cell tumor D. Craniopharyngioma

Germ cell tumor (including germinoma and non-germinomatous germ cell tumor) • Usually present in the first two decades of life • Hypothalamic or pineal mass common, but isolated stalk thickening may occur • Central DI, anterior hypopituitarism and chiasmopathy may occur • May secrete h. CG and/or AFP in the CSF and/or systemic circulation (non-germinomatous tumors) • PET scanning and biopsy may assist in diagnosis • Good response to radiation therapy (germinomas) • Adjuvant chemotherapy is often administered

Pituitary MRI interpretation • Atypical presentations of common sellar lesions or rare pathologies may occur • Consultation with an experienced neuroradiologist or pituitary surgeon is recommended for interpretation of imaging findings

Summary • Pituitary protocol MRI is the imaging method of choice for most sellar lesions • In addition to benign pituitary adenomas, which represent the majority of sellar lesions, a large number of pathologies may involve the sella • The radiographic features of a sellar mass are frequently helpful in making a presumptive diagnosis

Additional Reading • Zee CS et al. Imaging of the pituitary and parasellar region. Neurosurg Clin N Am 2003; 14: 55 -80 • Tantiwongkosi B et al. Imaging of optic neuropathy and chiasmal syndromes. Neuroimaging Clin N Am 2015; 25: 395 -410 • Bonneville JF. Magnetic resonance imaging of pituitary tumors. Front Horm Res 2016; 45: 97120 • Catford S et al. Pituitary stalk lesions: systematic review and clinical guidance. Clin Endocrinol 2016; March 7 (epub ahead of print)